Do Teeth Have Calcium
Key Takeaways
- When you flash a confident smile, what are you truly showing? Many people might assume their teeth are solid, unchanging structures made primarily of bone, or even pure calcium. But do teeth have calcium? The answer is a resounding yes, though not in the simplistic way some might imagine. Calciu
When you flash a confident smile, what are you truly showing? Many people might assume their teeth are solid, unchanging structures made primarily of bone, or even pure calcium. But do teeth have calcium? The answer is a resounding yes, though not in the simplistic way some might imagine. Calcium is, in fact, the fundamental building block of your teeth, forming the very hard minerals that protect them. Without adequate calcium, combined with other vital minerals and proper care, your teeth become vulnerable, particularly to a pervasive threat known as acid erosion in teeth.
Imagine the incredible strength required for your teeth to withstand years of biting, chewing, and grinding – a feat made possible by calcium and phosphate minerals. However, this formidable fortress isn't invincible. Everyday dietary choices, certain health conditions, and even inadequate oral hygiene can challenge its integrity, leading to demineralization where essential minerals, including calcium, are lost from your tooth structure. This process weakens the enamel, making your teeth sensitive, prone to decay, and potentially shortening their lifespan. Understanding the intricate role of calcium, the mechanisms of demineralization and remineralization, and how to effectively combat acid erosion is crucial for maintaining a healthy, vibrant smile for life.
In this comprehensive guide, we'll delve deep into the mineral composition of your teeth, clarifying exactly how calcium contributes to their strength and resilience. We'll explore the causes and signs of calcium loss and acid erosion, walk through effective prevention strategies, and discuss various treatment options available when damage has already occurred. By the end, you'll have a clear understanding of how to safeguard your dental calcium and protect your smile.
Key Takeaways:
- Teeth are primarily composed of calcium phosphate in the form of hydroxyapatite crystals, making calcium absolutely essential for their structure and strength. They are not pure calcium, but calcium is the main mineral component.
- Enamel, the outermost layer, is the hardest substance in the human body due to its high mineral content (up to 96% hydroxyapatite), making it highly dependent on calcium.
- Acid erosion in teeth is the primary way teeth lose calcium and other minerals, caused by acids from food, drinks, or medical conditions, leading to enamel weakening and sensitivity.
- Remineralization is a natural process where saliva, rich in calcium, phosphate, and fluoride, helps deposit minerals back into enamel, reversing early stages of demineralization.
- Preventive measures are key and include dietary modifications (reducing acidic foods), good oral hygiene (brushing gently, using fluoride toothpaste), and regular dental check-ups (typically every 6 months).
- Dental treatments for acid erosion range from fluoride applications ($30-$70 per treatment) and dental bonding ($150-$600 per tooth) for minor damage to fillings ($100-$400), crowns ($800-$3,000), or veneers ($900-$2,500 per tooth) for more significant destruction.
- Most dental insurance plans offer coverage for preventive care and typically cover 50-80% of basic restorative procedures after a deductible, though cosmetic treatments like veneers may have limited or no coverage.
What Are Teeth Made Of? An Overview of Calcium's Role
To truly understand if and how do teeth have calcium, it's essential to look at their remarkable composition. Your teeth are complex structures, far more intricate than simple bone. While calcium is a major player, it’s integrated into an even stronger mineral compound.

The primary mineral that makes up your teeth, giving them their incredible hardness and strength, is hydroxyapatite. This is a crystalline form of calcium phosphate. So, while teeth aren't pure calcium, calcium is the most abundant element within this vital mineral.
Let's break down the layers of a tooth and where calcium plays its part:
Enamel: The Outer Shield
Enamel is the visible, outermost layer of your tooth crown, and it's the hardest substance in the entire human body. It’s composed of approximately 96% mineral content, with hydroxyapatite crystals arranged in a dense, interlocking structure. The high concentration of calcium within these crystals is what makes enamel so durable, allowing it to withstand chewing forces and protect the sensitive inner layers. This makes it crucial to protect your enamel from acid erosion in teeth, as once enamel is lost, it cannot regenerate naturally.
Dentin: The Bulk of the Tooth
Beneath the enamel lies the dentin, which forms the bulk of the tooth structure. Dentin is also composed of hydroxyapatite crystals, but it's less mineralized than enamel, consisting of about 70% mineral content. Unlike enamel, dentin contains microscopic tubules that connect to the pulp, allowing for sensation. This is why when enamel is eroded, exposure of the dentin often leads to sensitivity.
Cementum: Anchoring the Tooth
The root surfaces of your teeth are covered by cementum, a bone-like tissue that helps anchor the tooth to the jawbone via the periodontal ligament. Cementum is roughly 45-50% mineral content, again primarily hydroxyapatite. It's less dense than enamel or dentin but crucial for the stability of your teeth.
Pulp: The Living Core
At the very center of your tooth is the pulp, which is soft tissue containing nerves, blood vessels, and connective tissue. The pulp is the living part of the tooth, providing nutrients and sensation. While not mineralized itself, it's surrounded by and nourishes the dentin, playing an indirect role in maintaining the health of the mineralized structures.
So, to reiterate, are teeth calcium? No, not purely, but they are predominantly made of calcium phosphate minerals (hydroxyapatite). This distinction is important because while consuming calcium is vital, it must be available in the right forms and supported by other minerals like phosphate and often fluoride, to be effectively incorporated into tooth structure.
![Cross-section of a human tooth showing enamel, dentin, cementum, and pulp(/glossary/glossary-pulp), highlighting the mineral layers.]
The Dynamic Process of Demineralization and Remineralization
Your teeth are not static structures. Every day, they undergo a continuous process of mineral exchange with your saliva, known as demineralization and remineralization. Understanding this balance is key to comprehending how teeth lose calcium and how to prevent damage.
Demineralization: The Loss of Tooth Calcium
Demineralization occurs when acids in your mouth dissolve the calcium and phosphate minerals from the enamel and dentin. This process weakens the tooth structure, making it softer and more porous.
Causes / Why It Happens: The primary culprits behind demineralization and acid erosion in teeth include:
- Dietary Acids: Foods and drinks high in acid content are the most common cause.
- Soft Drinks and Sports Drinks: These are highly acidic, with pH levels as low as 2.5-3.5, and often contain large amounts of sugar which further fuels bacteria.
- Citrus Fruits and Juices: Lemons, limes, oranges, and grapefruits, along with their juices, are naturally acidic.
- Vinegar: Found in salad dressings, pickles, and some condiments.
- Wine: Both red and white wines are acidic.
- Carbonated Water: Even unsweetened carbonated water can be mildly erosive due to carbonic acid.
- Bacterial Acids (Caries/Cavities): Oral bacteria metabolize sugars from your diet, producing lactic acid and other acids. These acids create localized areas of demineralization, leading to dental caries (cavities). While different from generalized acid erosion, the end result is the same: loss of tooth mineral.
- Medical Conditions:
- Gastroesophageal Reflux Disease (GERD): Chronic acid reflux brings stomach acids into the mouth, which are highly corrosive.
- Bulimia and Anorexia: Frequent vomiting exposes teeth to potent stomach acids.
- Dry Mouth (Xerostomia): Saliva is crucial for neutralizing acids and remineralization. Conditions or medications that reduce saliva flow increase demineralization risk.
- Sjögren's Syndrome: An autoimmune disease causing dry mouth.
- Mechanical Factors: Aggressive brushing immediately after consuming acidic foods can further abrade softened enamel.
Remineralization: Restoring Tooth Calcium
Fortunately, your body has a natural defense mechanism: remineralization. This is the process by which calcium, phosphate, and fluoride ions in your saliva are deposited back into the demineralized areas of the enamel, helping to repair and strengthen the tooth structure.
How it Works:
- Saliva: Your saliva is a natural superpower. It contains calcium and phosphate ions and buffers acids, raising the pH in your mouth. After an acid attack, saliva works to neutralize the acids and bathe the teeth in protective minerals.
- Fluoride: Fluoride is a game-changer for remineralization. When fluoride is present, it gets incorporated into the hydroxyapatite crystal structure, forming fluoroapatite. Fluoroapatite is more resistant to acid dissolution than regular hydroxyapatite, making the enamel stronger and more resilient. This is why fluoride is a critical component of most toothpastes and many public water supplies (water fluoridation).
The balance between demineralization and remineralization dictates the health of your enamel. When demineralization outpaces remineralization, the enamel starts to weaken, leading to erosion and ultimately cavities.
Signs and Symptoms of Calcium Loss and Acid Erosion
Recognizing the early signs of calcium loss and acid erosion in teeth is vital for timely intervention. Many symptoms are subtle at first but can progress to more severe issues if left unaddressed.
What to Look For:
- Increased Tooth Sensitivity: This is often one of the first and most common signs. As enamel thins due to acid erosion, the underlying dentin (with its microscopic tubules) becomes more exposed. You might experience sharp, sudden pain or discomfort when consuming hot, cold, sweet, or acidic foods and drinks, or even when breathing in cold air.
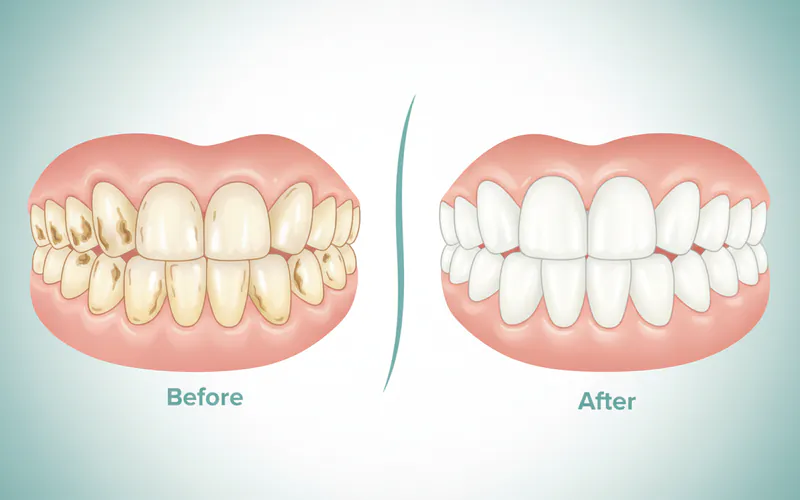
- Discoloration: Healthy enamel is naturally translucent, allowing some of the yellowish color of the dentin to show through. As enamel erodes, the yellow dentin becomes more prominent, making teeth appear darker or yellower.
- Transparency: The biting edges of your front teeth, particularly the incisors, may start to look translucent or glass-like as the enamel thins out.
- Rounded Edges or "Cupping": The biting surfaces of your teeth, especially molars, may develop small, concave depressions or "cups" where fillings might even appear to stand proud of the tooth surface. The overall shape of the tooth may also appear more rounded due to the loss of sharp edges.
- Cracks or Chips: Weakened enamel is more susceptible to fracturing. You might notice small chips or cracks on the edges of your teeth.
- Rough Tooth Surfaces: Enamel that has undergone demineralization can feel rough or grainy to the tongue rather than smooth.
- Toothache or Persistent Pain: If the erosion progresses to expose the dentin fully or even the pulp, it can lead to more constant and severe toothaches.
- Reduced Tooth Size: In advanced cases of severe acid erosion, teeth can visibly shorten or become noticeably smaller.
Pro Tip: Take note if symptoms appear suddenly or worsen over time. Keeping a food and drink diary can help you identify potential dietary culprits if you suspect acid erosion. Regular dental check-ups are essential for detecting these changes early, often before you even notice them yourself. Your dentist can spot initial signs of demineralization or erosion that are invisible to the untrained eye.
Preventing Calcium Loss and Acid Erosion
Prevention is undeniably the best strategy when it comes to safeguarding your dental calcium and protecting against acid erosion in teeth. Adopting mindful habits and a proactive approach can significantly reduce your risk.
Dietary Modifications:
- Limit Acidic Foods and Drinks: Reduce your intake of sodas, sports drinks, fruit juices (especially citrus), wine, and vinegar-based foods.
- Drink Water: Make water your primary beverage. If you must consume acidic drinks, use a straw to minimize contact with teeth.
- Neutralize Acids: After consuming acidic foods or drinks, rinse your mouth thoroughly with water or chew sugar-free gum (which stimulates saliva production) to help neutralize acids and wash away food particles. The ADA recommends chewing sugar-free gum for 20 minutes after meals to help prevent tooth decay.
- Avoid Brushing Immediately: Wait at least 30-60 minutes after consuming acidic foods or drinks before brushing your teeth. Acids temporarily soften enamel, and brushing too soon can cause further abrasion.
- Balance Your Diet: Ensure a diet rich in calcium-containing foods like dairy products (milk, cheese, yogurt), fortified plant-based milks, leafy greens (kale, spinach), and calcium-fortified cereals. These provide the necessary building blocks for remineralization.
- Vitamin D: Adequate Vitamin D is essential for the absorption of calcium. Ensure you get enough through sunlight exposure, fortified foods, or supplements if necessary, as advised by your healthcare provider.
Oral Hygiene Practices:
- Brush with Fluoride Toothpaste: Use a toothpaste containing fluoride at least twice a day. Fluoride strengthens enamel and aids in the remineralization process, making teeth more resistant to acid attacks.
- Gentle Brushing Technique: Use a soft-bristled toothbrush and brush gently in circular motions, paying attention to all tooth surfaces. Aggressive brushing can contribute to enamel wear, especially if enamel is already softened by acid.
- Floss Daily: Flossing removes plaque and food particles from between teeth and below the gumline, preventing bacterial acid production in these areas.
- Use Fluoride Mouthwash: If you're at high risk for erosion or cavities, your dentist might recommend a fluoride mouthwash as an additional protective measure.
Professional Dental Care:
- Regular Check-ups and Cleanings: Visit your dentist every six months for professional cleanings and examinations. Your dentist can spot early signs of erosion or demineralization and provide targeted preventive advice.
- Fluoride Treatments: Your dentist can apply professional-strength fluoride varnishes or gels to your teeth, providing a higher concentration of fluoride than over-the-counter products, enhancing remineralization and acid resistance.
- Dental Sealants: For children and sometimes adults, sealants can be applied to the chewing surfaces of back teeth to protect them from decay and erosion in the pits and fissures.
- Manage Underlying Conditions: If you suffer from GERD, bulimia, or dry mouth, work with your medical doctor and dentist to manage these conditions, as they significantly contribute to acid erosion.
Pro Tip: If you frequently consume acidic foods or drinks, consider rinsing your mouth with plain water or a fluoride mouthwash immediately afterward (but wait to brush!). This helps to dilute acids and facilitate remineralization.
Treatment Options for Calcium Loss and Acid Erosion
When prevention isn't enough, or if damage from calcium loss and acid erosion in teeth has already occurred, several treatment options are available. The choice of treatment depends on the severity of the erosion and the extent of the damage.
1. Remineralization Strategies (For Early Stage Erosion)
- Fluoride Varnish/Gel Applications: Your dentist can apply highly concentrated fluoride directly to your teeth. This professional treatment significantly boosts the enamel's ability to remineralize and become more acid-resistant.
- Pros: Non-invasive, quick, highly effective for early-stage erosion and sensitivity.
- Cons: Requires professional application, temporary, needs repeat treatments.
- Prescription-Strength Fluoride Toothpaste/Mouthwash: For individuals at high risk, dentists may prescribe toothpaste or mouthwash with a higher fluoride concentration than over-the-counter products.
- Pros: Can be used at home, effective for ongoing protection.
- Cons: Requires consistent use, may cause mild staining in rare cases.
- Calcium Phosphate Products (e.g., MI Paste, Recaldent™): These products contain calcium and phosphate ions that can help rebuild and strengthen enamel. Often used in conjunction with fluoride.
- Pros: Non-invasive, helps reduce sensitivity, enhances remineralization.
- Cons: Can be costly, requires consistent application, effectiveness varies depending on individual.
2. Dental Bonding (For Moderate Erosion)
Dental bonding involves applying a tooth-colored composite resin material to the eroded areas of the teeth. The resin is then shaped, hardened with a special light, and polished to match your natural teeth.
- Pros: Minimally invasive, relatively inexpensive compared to crowns/veneers, can improve aesthetics and reduce sensitivity.
- Cons: Not as durable as crowns or veneers, can stain over time, may need replacement every 5-10 years.
3. Dental Fillings (For Cavities Resulting from Erosion)
If acid erosion has progressed to form a cavity (a hole in the tooth), a dental filling will be necessary. The decayed or eroded portion of the tooth is removed, and the space is filled with a restorative material, typically composite resin or amalgam.
- Pros: Stops decay progression, restores tooth function and shape, prevents further damage.
- Cons: Involves removing part of the tooth structure, may require replacement over time.
4. Dental Crowns (For Severe Erosion with Significant Tooth Loss)
For teeth with extensive erosion, significant structural loss, or weakened structure, a dental crown (a cap) may be recommended. The crown covers the entire visible portion of the tooth, restoring its shape, size, strength, and appearance.
- Pros: Highly durable, restores full function, excellent aesthetics (especially porcelain crowns), protects the remaining tooth structure.
- Cons: More invasive (requires significant tooth reduction), higher cost, multiple appointments often required.

5. Dental Veneers (For Aesthetic Concerns and Moderate Erosion on Front Teeth)
Veneers are thin, custom-made shells of porcelain or composite resin that are bonded to the front surface of teeth. They are primarily used to improve aesthetics but can also cover eroded surfaces on front teeth.
- Pros: Excellent aesthetic results, can correct discoloration and minor shape irregularities, durable.
- Cons: Irreversible (requires some enamel removal), high cost, typically for front teeth only.
Step-by-Step Process: Receiving a Composite Filling (Common for Erosion-Induced Cavities)
- Diagnosis: Your dentist will examine your teeth and use X-rays to assess the extent of the erosion and potential cavity formation.
- Anesthesia: A local anesthetic will be administered to numb the tooth and surrounding area, ensuring you don't feel any pain during the procedure.
- Removal of Damaged Tooth Structure: Using a dental drill, the dentist will carefully remove any demineralized, softened, or decayed tooth material.
- Cleaning and Preparation: The area will be thoroughly cleaned and disinfected. If a composite filling is used, a conditioning liquid (etchant) may be applied to the tooth surface to create microscopic pores for better bonding, followed by a bonding agent.
- Application of Filling Material: For composite fillings, the tooth-colored resin material is applied in layers.
- Curing: A special blue light is used to harden (cure) each layer of the composite resin.
- Shaping and Polishing: Once all layers are applied and cured, the dentist will shape the filling to match the natural contours of your tooth and ensure your bite is correct. The filling is then polished for a smooth, natural finish.
- Final Check: The dentist will check your bite and make any necessary adjustments.
Cost and Insurance for Treating Calcium Loss and Acid Erosion
Understanding the financial aspects of treating calcium loss and acid erosion in teeth is crucial for patients in the US. Costs can vary significantly based on the severity of the condition, the type of treatment chosen, geographic location, and whether you have dental insurance.
Average US Price Ranges (Without Insurance):
| Treatment Type | Average Cost Range (Per Tooth) | Notes |
|---|---|---|
| Fluoride Varnish/Gel (Professional) | $30 - $70 (per application) | Often covered by insurance as preventive care, may be included in cleaning. |
| Prescription Fluoride Toothpaste | $15 - $30 (per tube) | Not always covered by insurance. |
| Dental Bonding (Composite Resin) | $150 - $600 | Used for minor to moderate erosion, often lasts 5-10 years. |
| Composite Filling (1 surface) | $100 - $250 | For small cavities resulting from erosion. |
| Composite Filling (2+ surfaces) | $200 - $400 | For larger cavities. |
| Porcelain Veneer | $900 - $2,500 | Primarily cosmetic, often not covered by insurance. |
| Porcelain Crown | $800 - $3,000 | Covers entire tooth, for extensive damage. Price varies by material (porcelain, zirconia, PFM). |
Geographic Variation: Costs tend to be higher in major metropolitan areas (e.g., New York, Los Angeles) and on the coasts, compared to rural areas or the Midwest. For example, a porcelain crown might cost $1,500-$3,000 in NYC but $800-$1,800 in Kansas City.
Dental Insurance Coverage:
Most standard dental insurance plans typically categorize treatments into tiers:
- Preventive Care (e.g., fluoride treatments, cleanings): Often covered at 80-100% with no deductible or a low co-pay. This is where early intervention for acid erosion symptoms can save you significant money.
- Basic Restorative Care (e.g., fillings, bonding for structural repair): Usually covered at 50-80% after you meet your deductible. Many plans view bonding as basic restorative if it addresses structural integrity or sensitivity due to erosion.
- Major Restorative Care (e.g., crowns): Typically covered at 50% after your deductible.
- Cosmetic Procedures (e.g., veneers for aesthetic reasons): Generally not covered by most dental insurance plans unless there's a clear functional or restorative need (e.g., veneer is the only viable way to restore a severely eroded front tooth's function).
Understanding Your Plan:
- Deductible: The amount you must pay out-of-pocket before your insurance begins to cover costs.
- Annual Maximum: The maximum amount your insurance company will pay for your dental care in a calendar year (often ranges from $1,000 to $2,000).
- Waiting Periods: Some plans have waiting periods (e.g., 6-12 months) before they will cover major restorative procedures.
Pro Tip: Always contact your dental insurance provider directly before any major treatment to understand your specific benefits, coverage percentages, deductibles, and annual maximums. Your dental office staff can often help you with this process and submit pre-treatment estimates.
Payment Plans and Financing Options:
For those without insurance or facing high out-of-pocket costs, several options can make treatment more affordable:
- In-Office Payment Plans: Many dental practices offer interest-free payment plans, allowing you to pay for treatment in installments over a few months.
- Third-Party Financing (e.g., CareCredit): These healthcare credit cards offer special financing options, often with deferred interest for a specific period.
- Dental Schools: Dental schools often offer treatments at reduced rates, performed by supervised students.
- Community Dental Clinics: Non-profit or government-funded clinics may offer care on a sliding scale based on income.
Recovery and Aftercare for Treated Acid Erosion
Once you've undergone treatment for calcium loss and acid erosion in teeth, proper recovery and diligent aftercare are essential to ensure the longevity of your restorations and prevent further damage.
Immediate Post-Treatment Care:
- Anesthesia Effects: If local anesthetic was used (common for fillings, bonding, crowns), avoid chewing on the treated side until the numbness completely wears off to prevent accidentally biting your cheek or tongue. This usually takes 1-3 hours.
- Sensitivity: It's normal to experience some temporary sensitivity to hot or cold foods/drinks after a filling or bonding, especially if the erosion was deep. This typically subsides within a few days to a couple of weeks. Over-the-counter pain relievers (like ibuprofen or acetaminophen) can help manage discomfort.
- Bite Adjustment: If you feel your bite is "off" or uneven after a filling or crown, contact your dentist. Minor adjustments may be needed to ensure proper occlusion and prevent discomfort or damage to the restoration.
Long-Term Aftercare:
- Maintain Excellent Oral Hygiene: This is paramount. Continue to brush twice daily with a fluoride toothpaste and a soft-bristled brush. Floss daily. Proper technique is crucial – gentle, thorough cleaning protects restorations and prevents new erosion.
- Continue Dietary Modifications: Stick to the preventive diet strategies outlined earlier. Minimize acidic foods and drinks, rinse with water after acidic consumption, and avoid constant snacking. Your restorations are not immune to acid attacks.
- Regular Dental Check-ups: Adhere to your dentist's recommended schedule for check-ups and cleanings, typically every six months. These visits allow your dentist to monitor the health of your teeth, assess your restorations, and reapply professional fluoride treatments if needed.
- Protect Against Grinding/Clenching: If you clench or grind your teeth (bruxism), especially at night, your dentist may recommend a custom-fitted nightguard. This protects your natural teeth and restorations from excessive wear and potential fracture.
- Address Underlying Medical Conditions: Continue to manage conditions like GERD or dry mouth in collaboration with your medical doctor. Effective management of these systemic issues is critical for long-term dental health.
- Avoid Harmful Habits: Refrain from habits like chewing on ice, biting fingernails, or using your teeth as tools, as these can chip or damage both natural teeth and restorations.
- Fluoride and Remineralizing Products: Your dentist may recommend continued use of prescription fluoride toothpaste or over-the-counter remineralizing products (like those containing CPP-ACP) to further strengthen enamel and protect against future erosion.
Pro Tip: Composite fillings and bonding can sometimes stain over time, especially with heavy consumption of coffee, tea, red wine, or tobacco. Regular professional cleanings can help minimize this, and good home care can slow down the process.
Risks and Complications of Untreated Calcium Loss and Acid Erosion
Ignoring calcium loss and acid erosion in teeth can lead to a cascade of increasingly serious dental problems, affecting not only your oral health but potentially your overall well-being.
What Can Go Wrong:
- Increased Tooth Sensitivity: As enamel continues to wear away, dentin exposure increases, leading to persistent and often severe sensitivity to hot, cold, sweet, and acidic stimuli. This can significantly impact your daily comfort and dietary choices.
- Tooth Decay (Cavities): Once the protective enamel layer is significantly eroded, teeth become highly vulnerable to bacterial acid attacks, leading to cavities. The softer dentin is less resistant to decay than enamel, meaning cavities can progress rapidly once they breach the enamel.
- Tooth Discoloration: Progressive enamel loss will make your teeth appear increasingly yellow or dull due to the underlying dentin becoming more prominent. This can significantly affect your smile aesthetics.
- Fractures and Chipping: Weakened, demineralized enamel is brittle and more prone to chipping, cracking, or even fracturing during normal biting and chewing forces.
- Changes in Bite and Jaw Issues: Significant tooth structure loss can alter your bite, leading to problems with your temporomandibular joint (TMJ), causing jaw pain, headaches, and difficulty chewing.
- Pulp Exposure and Infection: In severe cases, erosion can wear through both enamel and dentin, exposing the pulp (the living nerve and blood vessel tissue inside the tooth). This can cause intense pain, pulp inflammation (pulpitis), and ultimately lead to a tooth infection or abscess, requiring root canal therapy or even tooth extraction.
- Tooth Loss: If erosion and subsequent decay or infection are left untreated, the tooth may become so compromised that it cannot be saved and must be extracted. This leads to further complications like shifting teeth, difficulty chewing, and the need for costly replacements (implants, bridges, dentures).
- Increased Dental Costs: Delaying treatment invariably leads to more extensive and expensive procedures down the line. A small fluoride treatment or bonding for early erosion costs far less than a crown, root canal, or implant for a severely damaged tooth.
Pro Tip: Early detection and intervention are key to avoiding these severe complications. If you notice any signs of sensitivity, discoloration, or changes in your tooth structure, schedule an appointment with your dentist promptly.
Comparison Table: Common Restorative Options for Acid Erosion
This table compares common dental treatments used to address various levels of acid erosion in teeth and calcium loss, helping you understand the differences in cost, durability, and invasiveness.
| Feature | Fluoride Treatment (Professional) | Dental Bonding (Composite Resin) | Composite Filling (for Cavity) | Porcelain Crown | Porcelain Veneer (Front Teeth) |
|---|---|---|---|---|---|
| Purpose | Remineralize, strengthen enamel, reduce sensitivity | Restore minor to moderate erosion, improve aesthetics, reduce sensitivity | Repair cavities caused by erosion | Restore severely eroded/damaged tooth | Cosmetic restoration for front teeth, moderate erosion |
| Invasiveness | Non-invasive, topical application | Minimally invasive (etching) | Invasive (removes decayed tissue) | Highly invasive (significant tooth reduction) | Moderately invasive (enamel removal) |
| Durability | Temporary (weeks-months) | Moderate (5-10 years) | Moderate (5-10 years) | High (10-15+ years) | High (10-15+ years) |
| Cost Range (US) | $30 - $70 (per application) | $150 - $600 (per tooth) | $100 - $400 (per tooth) | $800 - $3,000 (per tooth) | $900 - $2,500 (per tooth) |
| Insurance Cov. | High (80-100% as preventive) | Moderate (50-80% as basic restorative) | Moderate (50-80% as basic restorative) | Moderate (50% as major restorative) | Low/None (often considered cosmetic) |
| Aesthetics | No direct aesthetic change | Good, tooth-colored | Good, tooth-colored | Excellent, custom-matched | Excellent, custom-matched |
| Ideal for | Early demineralization, sensitivity, prevention | Minor chips, worn edges, surface erosion | Holes in teeth from advanced erosion | Extensive tooth loss, weakened structure | Discolored, mildly eroded, misaligned front teeth |
Children / Pediatric Considerations: Calcium and Developing Teeth
Calcium's role in dental health is particularly critical for children, as their teeth are still forming and developing. Ensuring adequate calcium intake and preventing acid erosion in teeth from an early age sets the foundation for a lifetime of healthy smiles.
Developing Teeth:
- Primary (Baby) Teeth: Even before birth, calcium and other minerals are being deposited to form your baby's primary teeth. These teeth typically begin to erupt around 6 months of age. While temporary, they are crucial for chewing, speech development, and holding space for permanent teeth.
- Permanent Teeth: The mineralization process for permanent teeth begins shortly after birth and continues through early childhood, with most permanent teeth erupting between ages 6 and 12. During this period, a consistent supply of calcium is absolutely vital for the development of strong, acid-resistant enamel.
Importance of Calcium for Children:
- Strong Enamel Formation: Adequate dietary calcium (and Vitamin D for absorption) ensures that the hydroxyapatite crystals in developing enamel are robust and densely packed, creating strong teeth from the start.
- Bone Health: Calcium is also essential for developing strong jawbones, which support the teeth.
Pediatric Prevention and Care:
- Balanced Diet: Encourage a diet rich in calcium-fortified foods, dairy products, and leafy greens. Limit sugary drinks, fruit juices (even "100% juice" can be very acidic and sugary), and acidic snacks, which contribute to acid erosion and cavities.
- Fluoride Protection:
- Fluoridated Water: If your community water supply is fluoridated, it's an excellent, convenient source of fluoride.
- Fluoride Toothpaste: Start brushing with a small, rice-sized smear of fluoride toothpaste as soon as the first tooth erupts. For children aged 3-6, use a pea-sized amount. Supervise brushing to ensure they spit out the toothpaste and don't swallow too much.
- Professional Fluoride Treatments: Pediatric dentists often apply fluoride varnishes during routine check-ups to strengthen young enamel.
- Dental Sealants: The ADA recommends dental sealants for children as soon as their permanent molars erupt (around age 6 and again around age 12). Sealants act as a protective barrier against decay and erosion on the chewing surfaces.
- Early Dental Visits: Schedule your child's first dental visit by their first birthday or when their first tooth appears. Regular check-ups allow the dentist to monitor tooth development, provide preventive care, and catch early signs of demineralization or erosion.
- Avoid Bottle Propping: Never put a baby to bed with a bottle containing anything other than water, as prolonged exposure to sugary liquids (even milk or formula) can lead to severe "baby bottle tooth decay" which is a form of rampant demineralization.
- Address Thumb Sucking/Pacifier Use: While not directly related to calcium loss, prolonged habits can affect jaw development and bite, potentially leading to areas more vulnerable to wear.
Pro Tip for Parents: Make brushing fun! Use age-appropriate toothbrushes, play a song, or use a timer to ensure they brush for the recommended two minutes. Lead by example with good oral hygiene habits.
Cost Breakdown: Detailed Averages for Acid Erosion-Related Treatments
Let's consolidate and detail the average costs you might encounter for various treatments related to calcium loss and acid erosion in teeth in the US, along with insurance implications and cost-saving tips.
Average US Costs (Without Insurance):
| Procedure | Low Range | Mid Range | High Range | Notes |
|---|---|---|---|---|
| Preventive / Early Intervention | ||||
| Dental Exam & Cleaning (Routine) | $75 | $120 | $200 | Often covered 100% by insurance; essential for early detection. |
| Full Mouth X-rays (Every few years) | $100 | $150 | $250 | Varies based on number and type of X-rays; often covered 80-100%. |
| Professional Fluoride Application | $30 | $50 | $70 | Often done during cleanings, may be covered 100%. |
| Dental Sealant (Per Tooth) | $40 | $60 | $80 | Common for children's molars; covered 80-100% for pediatric patients. |
| Basic Restorations | ||||
| Dental Bonding (Composite, 1-2 surfaces) | $150 | $300 | $600 | Can address minor erosion, chips, or discoloration. |
| Composite Filling (1 Surface) | $100 | $175 | $250 | For small cavities resulting from erosion. |
| Composite Filling (2+ Surfaces) | $200 | $300 | $400 | For larger cavities. |
| Major Restorations | ||||
| Porcelain Crown | $800 | $1,500 | $3,000 | For extensive erosion or structural damage, restores full tooth. |
| Porcelain Veneer (Per Tooth) | $900 | $1,500 | $2,500 | Primarily cosmetic, but can cover eroded front teeth. |
| Inlay/Onlay (Porcelain/Composite) | $600 | $1,000 | $1,500 | More extensive than a filling, less than a crown, often for molars with moderate damage. |
| Root Canal (If erosion reaches pulp) | $700 (front) | $1,000 (pre-molar) | $2,000+ (molar) | Varies significantly by tooth type and location. A crown is usually needed afterward. |

With Dental Insurance:
As mentioned, most insurance plans cover preventive care (cleanings, exams, fluoride) at 80-100%. Basic restorative procedures (fillings, bonding for repair) are typically covered at 50-80%, and major restorative procedures (crowns) at 50%.
Example Scenario (Composite Filling for a cavity due to erosion):
- Total Cost: $250
- Insurance Coverage: 80%
- Your Deductible: Let's say you have a $50 deductible which you haven't met yet.
- Your Out-of-Pocket: $50 (deductible) + (20% of $200 remaining after deductible) = $50 + $40 = $90
Payment Plans and Financing Options:
- In-Office Plans: Many dental offices offer interest-free payment plans for up to 6-12 months. This allows you to spread the cost of larger treatments.
- Third-Party Healthcare Financing (e.g., CareCredit, LendingClub): These companies offer credit cards specifically for healthcare expenses, often with promotional periods of 0% APR if paid in full within a certain timeframe (e.g., 6, 12, 18, or 24 months). If not paid within the promotional period, high-interest rates can apply.
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): If you have an HSA or FSA through your employer, you can use these tax-advantaged accounts to pay for dental expenses with pre-tax dollars, saving you money on your income tax.
- Dental Schools and Community Clinics: These provide lower-cost care as previously mentioned, though wait times may be longer, and selection of services more limited.
Cost-Saving Tips:
- Prioritize Prevention: The single most effective way to save money is to prevent erosion and decay in the first place through excellent home care and regular check-ups.
- Address Issues Early: Don't wait for a small sensitivity to become a large cavity. Early intervention is always less expensive.
- Maximize Insurance Benefits: Understand your annual maximums and deductible. Plan larger treatments around these to get the most coverage.
- Ask About Cash Discounts: Some dental offices offer a discount for patients who pay in full with cash at the time of service, especially if they don't have insurance.
- Get Multiple Opinions: For complex or expensive treatments, getting a second opinion can confirm the diagnosis and treatment plan and provide alternative cost estimates.
Frequently Asked Questions
Are teeth made of pure calcium?
No, teeth are not made of pure calcium. They are primarily composed of a mineral called hydroxyapatite, which is a crystalline form of calcium phosphate. Calcium is the most abundant mineral element within this structure, making up about 35-39% of the weight of enamel, alongside phosphate, magnesium, and other trace elements.
Can calcium supplements rebuild lost tooth enamel?
While calcium supplements are vital for strong bones and can support overall oral health by providing essential building blocks, they cannot directly rebuild lost tooth enamel in the way that fluoride treatments or dental restorations can. Enamel loss due to acid erosion in teeth is primarily a surface-level demineralization process. Supplements contribute to the calcium in your saliva, which can aid in natural remineralization, but they don't grow back entire layers of enamel.
What foods and drinks cause the most acid erosion in teeth?
Highly acidic foods and drinks are the main culprits. These include soft drinks (soda), sports drinks, energy drinks, citrus fruits and juices (lemon, orange, grapefruit), vinegar-based foods (pickles, salad dressing), and wine. Even unsweetened carbonated water can be mildly acidic due to carbonic acid.
How long does it take for acid erosion to damage teeth?
The rate of acid erosion in teeth varies widely among individuals, depending on dietary habits, oral hygiene, and saliva production. It can be a slow, progressive process taking years to show noticeable damage, or it can advance rapidly in cases of frequent exposure to strong acids (e.g., severe GERD or bulimia). Early signs like sensitivity can appear within months or even weeks of consistent exposure.
Is calcium good for both teeth and bones?
Yes, calcium is absolutely crucial for both teeth and bones. It forms the primary mineral component (hydroxyapatite) of both structures, providing strength and rigidity. However, while bones are constantly remodeling and can release calcium into the bloodstream, teeth are mostly inert once formed. Sufficient calcium intake, especially during childhood, is vital for proper development of strong teeth and bones, and lifelong intake helps maintain bone density and supports the remineralization process in teeth.
Can acid erosion be reversed naturally?
Early stages of demineralization, where the enamel has not yet formed a cavity, can often be reversed or arrested through natural remineralization processes. Saliva, rich in calcium and phosphate, coupled with fluoride (from toothpaste, water, or professional treatments), can help deposit minerals back into the enamel. However, once enamel is physically worn away or a cavity forms, it cannot regrow or fully repair itself naturally and requires dental intervention.
How painful is treatment for acid erosion?
The pain level for treatment of acid erosion in teeth varies greatly depending on the severity of the erosion and the type of treatment. Non-invasive treatments like fluoride varnishes are painless. Dental bonding and fillings are performed under local anesthesia, so you shouldn't feel pain during the procedure, only pressure. Crowns and veneers also involve local anesthesia. Some temporary sensitivity after treatment is common but usually manageable with over-the-counter pain relievers.
Does drinking milk or eating cheese after an acidic meal help?
Yes, consuming dairy products like milk or cheese after an acidic meal can be beneficial. Milk helps to neutralize acids in the mouth, and both milk and cheese are rich in calcium, phosphate, and casein protein, which can promote remineralization and help protect enamel from further acid attacks.
How often should I get professional fluoride treatments?
The frequency of professional fluoride treatments depends on your individual risk for cavities and acid erosion in teeth. For most adults, a fluoride treatment every 6-12 months during routine check-ups is sufficient. However, if you have a high risk of decay, severe dry mouth, or active acid erosion, your dentist might recommend more frequent applications, such as every 3-4 months.
Can braces cause acid erosion or calcium loss?
Braces themselves do not directly cause acid erosion or calcium loss. However, they can make it more challenging to clean your teeth thoroughly, leading to plaque accumulation around the brackets and wires. This plaque produces acids that can cause demineralization, often appearing as white spots on the enamel once the braces are removed. Meticulous oral hygiene and frequent fluoride use are crucial for individuals with braces to prevent this.
When to See a Dentist
Recognizing the signs that warrant a professional dental visit can make a significant difference in managing calcium loss and acid erosion in teeth, preventing minor issues from escalating into major problems.
Clear Warning Signs That Need Immediate Attention:
- Sudden or Severe Tooth Sensitivity: If you experience sharp, persistent pain when consuming hot, cold, sweet, or acidic foods, or even when breathing cold air, it's a strong indicator of enamel erosion or exposed dentin.
- Noticeable Changes in Tooth Appearance: If you observe your teeth appearing more yellow or dull, developing transparent edges, or showing small "cups" or indentations on the chewing surfaces, these are visual cues of erosion.
- New Chips or Cracks: Any new chips, cracks, or rough spots on your teeth could signal weakened enamel.
- Persistent Toothache: A constant or throbbing toothache could indicate that erosion has progressed to a cavity or even reached the tooth's pulp, requiring urgent attention.
- Bleeding or Swollen Gums Alongside Tooth Changes: While not directly erosion-related, these symptoms suggest gum disease, which can further complicate oral health if combined with erosion.
Red Flags vs. Routine Care Guidance:
- Routine Care: Regular dental check-ups every six months are essential for everyone. During these visits, your dentist can identify early, subtle signs of demineralization or erosion that you might not notice. They can also provide preventive fluoride treatments and personalized advice.
- Red Flags: The warning signs listed above fall under "red flags" – situations where you should schedule an appointment sooner rather than later. Don't wait for your next routine cleaning if you're experiencing new or worsening symptoms related to sensitivity or visible tooth changes.
- Emergency Care: A severe, debilitating toothache, facial swelling, or a knocked-out tooth constitutes a dental emergency. While directly linked to calcium loss, these scenarios often stem from severe tooth compromise that erosion can contribute to over time. Contact your dentist immediately or seek emergency dental care.
Pro Tip: Your body often gives you signals when something is wrong. Listen to your teeth and don't dismiss increasing sensitivity or visible changes as "normal." Early detection and intervention are always less invasive, less costly, and more effective in preserving your natural teeth.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
What Are Calcium Deposits on Teeth
Are you one of the millions of Americans who notices a stubborn, yellowish buildup on your teeth despite regular brushing? You're likely experiencing what many refer to as "calcium deposits on teeth." This common dental concern, medically known as dental calculus or tartar, affects a vast ma
February 23, 2026
Calcium Good for Teeth: Complete Guide
More than 99% of your body's calcium resides in your bones and teeth, making it an undeniable cornerstone of skeletal and oral health. But did you know that an estimated 42% of American adults don't get enough calcium from their diet? This staggering statistic underscores a critical question
February 23, 2026
What Do Bulimia Teeth Look Like
"Bulimia teeth" refers to the specific and often severe damage that the self-induced vomiting characteristic of bulimia nervosa inflicts on a person's oral health. It's a critical issue, affecting approximately 1.5% of women and 0.5% of men in the US at some point in their lives, with many more
February 23, 2026

Erosion in Teeth: Complete Guide
Erosion in Teeth: Complete Guide
February 23, 2026