Halitosis
4,521 words · 15 min read
Quick Definition
Chronic bad breath that persists despite normal oral hygiene. Halitosis can originate from oral sources (bacteria, gum disease, dry mouth) or systemic conditions.
Halitosis: A Comprehensive Guide to Chronic Bad Breath
Introduction
Halitosis, commonly known as chronic bad breath, is a persistent and often distressing condition characterized by an unpleasant odor emanating from the mouth. Unlike temporary bad breath caused by strong foods like garlic or onions, halitosis doesn't simply disappear after brushing or rinsing; it lingers, affecting an individual's confidence, social interactions, and overall quality of life. More than just an embarrassing social issue, halitosis often serves as a significant indicator of underlying oral health problems or, in some cases, systemic medical conditions that require attention.


Understanding halitosis is crucial for maintaining good dental health. It is remarkably common, affecting a substantial portion of the population. Studies suggest that approximately 1 in 4 people globally experience halitosis on a regular basis, with some estimates in the US market indicating that up to 50% of adults have experienced chronic bad breath at some point. Its prevalence underscores the importance of proper diagnosis and treatment. By delving into its causes, symptoms, and effective management strategies, this definitive guide aims to empower you with the knowledge needed to address halitosis effectively and reclaim fresh breath.
Key Takeaways:
- Halitosis is persistent bad breath, not just temporary food-related odor.
- It affects a significant portion of the population (up to 50% of adults).
- The primary cause is often oral, linked to bacteria producing Volatile Sulfur Compounds (VSCs).
- It can also signal underlying dental issues like Gum Disease or systemic health problems.
- Accurate diagnosis by a dentist is crucial for effective treatment.
- Halitosis is treatable, with solutions ranging from improved oral hygiene to professional dental care and medical intervention.
Detailed Explanation
Types and Classifications of Halitosis
Halitosis is not a monolithic condition; it can be classified into several types based on its origin and perception:
-
True Halitosis: This is genuine bad breath that is objectively noticeable by others.
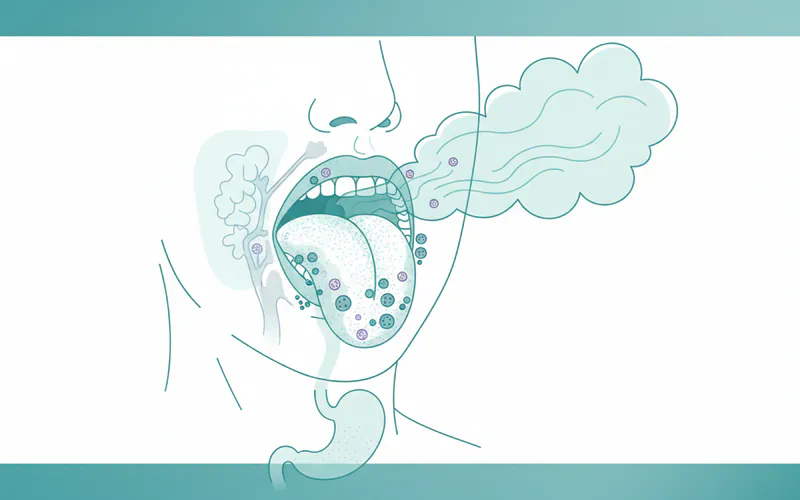
- Physiological Halitosis: This is the most common type and is primarily caused by normal bacterial activity in the mouth, particularly on the back of the tongue. These bacteria break down proteins and produce Volatile Sulfur Compounds (VSCs), such as hydrogen sulfide and methyl mercaptan, which create the foul odor. Morning breath is a classic example. While normal, it can become chronic if oral hygiene is insufficient.
- Pathological Halitosis: This type indicates an underlying disease or condition.
- Oral Pathological Halitosis: The vast majority (approximately 85-90%) of halitosis cases originate in the mouth. These are linked to dental conditions such as Gingivitis, Gum Disease (periodontitis), dental caries (cavities), oral infections (e.g., abscesses), unclean dentures, tongue coating, and dry mouth (Xerostomia). Food impaction between teeth or faulty dental restorations can also trap food debris and bacteria.
- Extra-Oral Pathological Halitosis: In about 10-15% of cases, the source of bad breath is outside the oral cavity. This can stem from systemic diseases or conditions affecting other parts of the body. Examples include upper or lower respiratory tract infections (sinusitis, tonsillitis, bronchitis, lung infections), gastrointestinal issues (GERD – gastroesophageal reflux disease, hiatal hernia), metabolic disorders (diabetes, liver failure, kidney failure), certain cancers, and various medications.
-
Pseudo-Halitosis: In this scenario, individuals perceive they have bad breath, but it is not objectively detectable by others. Despite reassurances from dental professionals and family, the patient remains convinced they have an odor. This often requires psychological counseling to manage.
-
Halitophobia: This is an extreme and irrational fear of having bad breath, even after successful treatment for true halitosis or pseudo-halitosis. Individuals with halitophobia may constantly check their breath, overuse oral hygiene products, and avoid social situations, significantly impacting their mental well-being. This condition also warrants psychological support.
Causes and Risk Factors
Understanding the various causes is critical for effective treatment:
Primary Oral Causes (Approx. 85-90% of cases):
- Bacterial Accumulation on the Tongue: The posterior dorsum (back) of the tongue is a prime breeding ground for anaerobic bacteria. These bacteria feast on food debris, dead cells, and post-nasal drip, producing VSCs as byproducts. A thick, white or yellowish coating on the tongue is a common sign.
- Gum Disease (Periodontal Disease): Both Gingivitis (inflammation of the gums) and its more severe form, periodontitis, are major contributors. As bacteria proliferate in deep gum pockets, they produce significant amounts of VSCs and other foul-smelling compounds. Bleeding gums and loose teeth are also signs of advanced Gum Disease.
- Poor Oral Hygiene: Infrequent or ineffective brushing and flossing allow food particles to remain in the mouth, promoting bacterial growth and plaque accumulation.
- Dry Mouth (Xerostomia): Saliva plays a crucial role in cleansing the mouth and neutralizing acids. Reduced salivary flow, often caused by medications, certain medical conditions (e.g., Sjogren's syndrome), mouth breathing, or dehydration, allows bacteria to thrive and food particles to linger, intensifying bad breath.
- Dental Caries (Cavities) and Abscesses: Decaying teeth provide ideal niches for bacteria to accumulate and produce odors. Deep cavities and dental abscesses (pus-filled infections) can release strong, foul smells.
- Faulty Dental Restorations: Old, cracked, or poorly fitting fillings, crowns, or bridges can create traps for food particles and bacteria, making them difficult to clean effectively.
- Oral Infections: Other infections, such as oral thrush (candidiasis), herpes simplex lesions, or healing wounds from oral surgery, can also cause transient or persistent bad breath.
- Foods and Beverages: While not chronic halitosis, strong-smelling foods like garlic, onions, spices, and coffee can leave a temporary odor after digestion, as their volatile compounds are absorbed into the bloodstream and exhaled through the lungs.
- Tobacco Products: Smoking and chewing tobacco not only leave their own distinctive odor but also increase the risk of Gum Disease and dry mouth, exacerbating halitosis.
Extra-Oral (Systemic) Causes (Approx. 10-15% of cases):
- Respiratory Tract Infections: Conditions like sinusitis, post-nasal drip, tonsillitis, pharyngitis, bronchitis, and lung infections can lead to unpleasant breath due to mucus, pus, and bacterial activity in the airways.
- Gastrointestinal Issues: Gastroesophageal reflux disease (GERD), where stomach acid flows back into the esophagus, can cause a sour or acidic breath odor. Other GI conditions like hiatal hernia or Helicobacter pylori infection may also contribute.
- Metabolic Disorders:
- Diabetes: Uncontrolled diabetes can lead to ketoacidosis, producing a distinct fruity or acetone-like breath odor.
- Kidney Disease: Kidney failure can result in a urine-like or fishy odor on the breath, due to the buildup of toxins.
- Liver Disease: Severe liver dysfunction (cirrhosis) can cause "fetor hepaticus," a distinct sweet, musty odor.
- Certain Medications: Many prescription and over-the-counter drugs can cause dry mouth as a side effect (e.g., antidepressants, antihistamines, diuretics, blood pressure medications), indirectly leading to halitosis.
- Cancer: Head and neck cancers or lung cancers can sometimes be associated with a distinctive, foul breath odor.
Signs and Symptoms to Watch For
The most obvious symptom of halitosis is an unpleasant breath odor. However, other signs often accompany it:
- Persistent Bad Odor: The primary indicator, which may be described as rotten eggs (due to hydrogen sulfide), fecal, sour, or putrid.
- Dry Mouth (Xerostomia): A feeling of stickiness or dryness in the mouth, often accompanied by difficulty swallowing or speaking.
- White or Yellowish Coating on the Tongue: Especially noticeable on the back of the tongue.
- Sour, Bitter, or Metallic Taste in the Mouth: A lingering unpleasant taste that doesn't go away.
- Increased Mucus or Post-Nasal Drip: Can contribute to bacterial growth at the back of the throat.
- Bleeding Gums or Swollen Gums: Indicative of Gingivitis or Gum Disease.
- Discomfort or Burning Sensation in the Mouth.
- Social Anxiety or Self-Consciousness: While not a physical symptom, this is a significant impact for many sufferers.
Diagnosis Process — What Your Dentist Does
Diagnosing halitosis effectively requires a systematic approach by a dental professional. Your dentist at SmilePedia.net will typically follow these steps:
- Comprehensive Medical and Dental History: Your dentist will ask about your oral hygiene habits, diet, medications, smoking and alcohol use, and any existing medical conditions. They'll also inquire about when you notice the bad breath, if it's constant, and if family members or friends have commented on it.
- Organoleptic Assessment: This is the "gold standard" for evaluating breath odor. The dentist directly smells the patient's breath from different sites (mouth, nose) at various distances. This highly subjective but experienced assessment helps determine the presence and severity of the odor and its potential source (oral vs. nasal/systemic). This is often done after a period of fasting and avoiding oral hygiene products to get an accurate baseline.
- Intraoral Examination: A thorough examination of your teeth, gums, tongue, and other oral tissues will be conducted. The dentist will look for:
- Signs of Gingivitis or Gum Disease (swelling, redness, bleeding, deep periodontal pockets).
- Dental caries (cavities) or infections.
- Faulty or old dental restorations.
- Tongue coating thickness and color.
- Signs of Xerostomia (dry mouth) like reduced saliva flow or parched oral tissues.
- Oral lesions or infections.
- Specialized Diagnostic Tests (if necessary):
- Halimeter (Portable Sulfide Monitor): This device measures the concentration of Volatile Sulfur Compounds (VSCs) in your breath, providing an objective numerical value for bad breath. It’s particularly useful for monitoring treatment effectiveness.
- Gas Chromatography: Considered the most accurate method, this laboratory technique separates and identifies individual VSCs (hydrogen sulfide, methyl mercaptan, dimethyl sulfide), offering a detailed profile of the odor-causing compounds.
- Salivary Flow Rate Test: If Xerostomia is suspected, your dentist may measure your salivary flow rate to assess salivary gland function.
- Bacterial Culture: In some cases, a swab may be taken from the tongue or periodontal pockets to identify specific odor-producing bacteria.
- Periodontal Probing and X-rays: These help assess the extent of Gum Disease and bone loss, which can be a significant source of bad breath.
- Referral (if extra-oral causes are suspected): If the dental examination doesn't reveal an adequate oral source for the halitosis, or if the breath odor has distinct characteristics (e.g., fruity, ammonia-like), your dentist will refer you to a physician for further medical evaluation and diagnosis of potential systemic conditions.
Treatment Options with Pros, Cons, and Costs
Treatment for halitosis is highly individualized and depends entirely on the underlying cause.
1. Improved Oral Hygiene (for Physiological Halitosis & Mild Oral Pathological Halitosis)
- Pros: Cost-effective, non-invasive, improves overall oral health.
- Cons: Requires consistent effort, may not be sufficient for severe cases or underlying medical issues.
- Cost: Minimal (cost of toothbrush, toothpaste, floss, tongue cleaner).
- Toothbrush: $3-$15
- Toothpaste: $3-$10
- Dental Floss: $3-$8
- Tongue Scraper/Cleaner: $5-$15
2. Professional Dental Cleanings (Prophylaxis & Deep Cleaning)
- Pros: Removes plaque, tartar, and bacteria that contribute to bad breath, essential for Gingivitis and Gum Disease management.
- Cons: Requires multiple visits for deep cleaning, some discomfort possible.
- Cost (without insurance):
- Routine Cleaning (Prophylaxis): $75 - $200
- Deep Cleaning (Scaling and Root Planing, per quadrant): $200 - $600 per quadrant (often 2-4 quadrants treated). A full mouth deep cleaning could range from $800 - $2400+.
3. Treatment of Oral Conditions (Cavities, Gum Disease, Faulty Restorations)
- Pros: Eliminates the source of infection/odor, restores oral health.
- Cons: Can be more invasive, potentially higher cost, may require multiple appointments.
- Cost (without insurance):
- Fillings (Composite): $150 - $400+ per tooth.
- Gum Disease Treatment: Varies widely from deep cleaning (above) to periodontal surgery ($500 - $4000+ per area).
- Replacing Old Restorations (Crowns, Bridges): $800 - $2,500+ per unit.
4. Mouthwashes and Oral Rinses
- Pros: Provides temporary freshness, some contain antimicrobial agents to reduce bacteria.
- Cons: Temporary effect if underlying cause isn't addressed, some contain alcohol (can dry mouth), overuse can mask serious issues.
- Cost: $5 - $20 per bottle.
- Comparison of Mouthwash Types:
| Mouthwash Type | Active Ingredients | Pros | Cons |
|---|---|---|---|
| Antiseptic/Antimicrobial | Chlorhexidine, Cetylpyridinium Chloride (CPC), Essential Oils | Kills odor-causing bacteria, reduces plaque and Gingivitis. | Can stain teeth (Chlorhexidine), some contain alcohol (drying). |
| Oxygenating | Chlorine Dioxide, Zinc compounds | Neutralizes VSCs, doesn't just mask odors. | Can have a strong taste, not effective against all bacteria. |
| Cosmetic/Breath Freshener | Flavoring agents, mint | Provides immediate but temporary fresh breath. | Does not treat the underlying cause, no antimicrobial benefits. |
| Fluoride Rinse | Sodium Fluoride | Strengthens enamel, helps prevent cavities (indirectly prevents odor from decay). | No direct anti-halitosis properties. |
5. Addressing Dry Mouth (Xerostomia)
- Pros: Restores salivary function, improves comfort, aids in natural oral cleansing.
- Cons: Management rather than cure, may require continuous use of products.
- Cost:
- Saliva Substitutes/Artificial Saliva: $10 - $30 per product.
- Xylitol Products (Mints, Gums): $5 - $15 per pack.
6. Medical Management (for Extra-Oral Halitosis)
- Pros: Treats systemic disease, resolves associated halitosis.
- Cons: Requires medical diagnosis and treatment, which can be complex and expensive depending on the condition.
- Cost: Highly variable, depends on the underlying medical condition (e.g., medication for GERD, treatment for sinusitis, diabetes management). Can range from $50 for a doctor's visit and simple prescription to thousands for chronic disease management.
Step-by-Step: What to Expect During Treatment
- Initial Consultation & Diagnosis: Your journey begins with a thorough dental exam and diagnostic tests to pinpoint the cause.
- Oral Hygiene Education: If the cause is physiological or mild oral pathological, your dentist or hygienist will provide detailed instructions on proper brushing (including effective tongue cleaning), flossing, and the use of specific mouthwashes.
- Professional Cleaning: A routine cleaning (prophylaxis) will remove plaque and tartar. If Gum Disease is present, a deep cleaning (scaling and root planing) will be performed to clean below the gum line. This may involve local anesthetic for comfort.
- Dental Restorations/Repairs: Any cavities will be filled, and faulty fillings or crowns will be repaired or replaced.
- Tongue Cleaning: Your dentist will likely recommend and demonstrate the proper use of a tongue scraper or brush to remove bacterial coating.
- Addressing Dry Mouth: If Xerostomia is a factor, recommendations will include increasing water intake, using sugar-free xylitol gums/mints, or prescribing artificial saliva products.
- Medication Review: If medications are causing dry mouth, your dentist may consult with your physician to explore alternative prescriptions or strategies to manage the side effect.
- Medical Referral: If a systemic medical condition is suspected, you will be referred to a physician (e.g., ENT specialist, gastroenterologist, endocrinologist) for further diagnosis and treatment.
- Follow-Up Appointments: Regular follow-up visits will be scheduled to monitor your progress, reinforce oral hygiene techniques, and ensure the halitosis is effectively managed.
Recovery Timeline and Aftercare
The recovery timeline for halitosis varies significantly based on its cause and the treatment provided.
- Physiological Halitosis: Improvement can be noticed within days to a week with consistent and improved oral hygiene (brushing, flossing, tongue scraping).
- Mild Oral Pathological Halitosis (e.g., Gingivitis): With professional cleaning and diligent home care, breath can improve within 1-2 weeks. Full resolution of Gingivitis typically takes a few weeks.
- Severe Oral Pathological Halitosis (e.g., Periodontitis, multiple cavities): Recovery can take several weeks to months, especially if deep cleanings, fillings, or other dental procedures are required. The key is consistent follow-up and maintenance.
- Extra-Oral Pathological Halitosis: Improvement depends entirely on the successful management of the underlying medical condition. This could take weeks, months, or be an ongoing management process.
Aftercare is crucial for preventing recurrence:
- Maintain Excellent Oral Hygiene: Brush twice daily for two minutes, floss once daily, and clean your tongue daily.
- Regular Dental Check-ups: Visit your dentist every 6 months for professional cleanings and examinations.
- Stay Hydrated: Drink plenty of water throughout the day.
- Healthy Diet: Limit sugary foods and drinks.
- Avoid Tobacco: Quitting smoking or chewing tobacco is paramount.
- Manage Underlying Conditions: Continue to work with your physician to manage any systemic health issues.
Prevention Strategies
Preventing halitosis largely mirrors the aftercare strategies:
- Brush and Floss Regularly: Brush your teeth and gums twice a day with fluoride toothpaste. Floss daily to remove food particles and plaque from between teeth.
- Clean Your Tongue: Use a tongue scraper or the back of your toothbrush to gently clean your tongue daily. This significantly reduces odor-producing bacteria.
- Stay Hydrated: Drink plenty of water to keep your mouth moist and help wash away food particles and bacteria.
- Eat a Balanced Diet: Limit sugary and acidic foods that can promote bacterial growth and decay. Include crunchy fruits and vegetables (e.g., apples, carrots) that act as natural tooth cleansers.
- Chew Sugar-Free Gum: Chewing sugar-free gum, especially those with xylitol, can stimulate saliva flow, helping to cleanse the mouth.
- Avoid Tobacco Products: Tobacco is a major contributor to bad breath and severe oral health problems.
- Regular Dental Check-ups and Cleanings: Professional cleanings remove plaque and tartar that cannot be removed by brushing alone, and allow your dentist to catch issues like cavities or Gum Disease early.
- Treat Underlying Health Conditions: Promptly address conditions like sinus infections, GERD, or diabetes under medical guidance.
Cost Ranges in the US (with/without insurance)
The cost of diagnosing and treating halitosis in the US can vary widely based on the complexity of the cause, the required procedures, the location of the dental practice, and whether you have dental insurance.
- Initial Dental Exam & Consultation (without insurance): $50 - $150. With insurance, you might pay a co-pay of $0 - $50.
- Routine Professional Cleaning (Prophylaxis) (without insurance): $75 - $200. With insurance, this is often covered at 80-100%, leaving a minimal or no out-of-pocket cost.
- Deep Cleaning (Scaling and Root Planing) (without insurance): $200 - $600 per quadrant. As a major procedure, insurance might cover 50-80% after a deductible, leaving you with a significant out-of-pocket expense of $100 - $300 per quadrant.
- Fillings (Composite) (without insurance): $150 - $400+ per tooth. Insurance often covers 50-80%.
- Tongue Scraper/Brush: $5 - $15. Not typically covered by insurance.
- Specialized Mouthwashes/Rinses: $5 - $20. Not covered by insurance.
- Saliva Substitutes/Xylitol Products: $10 - $30. Not covered by insurance.
- Medical Referrals/Tests: If referred to a physician for systemic causes, costs will depend on your medical insurance plan (co-pays, deductibles for doctor visits, specialist visits, blood tests, imaging). A specialist visit could be $100 - $300+ without insurance, or a $30 - $70 co-pay with insurance.
Important Note: Many dental insurance plans operate on a "100-80-50" coverage model, meaning preventive care (exams, cleanings) is covered at 100%, basic procedures (fillings) at 80%, and major procedures (deep cleanings, crowns) at 50%, often after a deductible is met. It's always best to check with your specific insurance provider for exact coverage details.
Comparison Table: Key Oral Hygiene Tools for Halitosis Prevention
| Oral Hygiene Tool | Primary Action | Benefit for Halitosis | Frequency of Use | Cost Range (US) |
|---|---|---|---|---|
| Toothbrush | Removes plaque and food debris from teeth/gums. | Eliminates odor-causing bacteria on teeth/gums. | Twice daily | $3 - $15 |
| Dental Floss | Cleans between teeth and under gumline. | Removes trapped food and bacteria where toothbrush can't reach. | Once daily | $3 - $8 |
| Tongue Scraper | Physically removes bacterial coating from tongue. | Directly reduces VSC production on the tongue. | Once or twice daily | $5 - $15 |
| Antimicrobial Mouthwash | Kills oral bacteria. | Reduces overall bacterial load and VSCs. | Once or twice daily | $5 - $20 |
| Xylitol Gum/Mints | Stimulates saliva, fights bacteria. | Increases natural cleansing, neutralizes acids. | Several times a day | $5 - $15 |
For Parents / Pediatric Considerations
Halitosis in children is less common than in adults, but when it occurs, it can be a source of concern for parents. While sometimes simply "morning breath," persistent bad breath in children usually points to an underlying issue.
Common Causes of Halitosis in Children:
- Poor Oral Hygiene: Just like adults, insufficient brushing and flossing allow food particles and bacteria to accumulate, especially if children are not adequately supervised.
- Tongue Coating: A thick coating on the tongue can harbor odor-producing bacteria.
- Enlarged Tonsils or Tonsillitis: Tonsils can have crypts or pockets where food debris, bacteria, and dead cells get trapped, forming "tonsil stones" (tonsilloliths) that produce a very foul odor. Chronic tonsillitis is a frequent cause of bad breath in children.
- Sinus or Nasal Infections: Children are prone to colds, allergies, and sinus infections, leading to post-nasal drip. The mucus accumulating at the back of the throat can be a breeding ground for bacteria. A foreign object lodged in the nose (e.g., a bead, a small toy) can also cause a very strong, unilateral (one-sided) foul smell.
- Dry Mouth: Less common but can be caused by certain medications, mouth breathing (due to allergies or enlarged adenoids/tonsils), or dehydration.
- Dental Issues: Untreated cavities or Gingivitis (often referred to as "childhood gingivitis") can contribute to bad breath.
- Gastroesophageal Reflux (GER): Infant reflux or GERD in older children can lead to acidic breath.
- Systemic Conditions: Very rarely, metabolic disorders like diabetes can cause characteristic breath odors.
What Parents Should Do:
- Emphasize Oral Hygiene: Ensure children brush twice daily for two minutes, floss daily, and gently brush their tongue. Supervise younger children.
- Hydration: Encourage ample water intake.
- Regular Dental Check-ups: Ensure your child has regular dental visits starting from their first tooth.
- Consult Your Pediatric Dentist: If bad breath persists despite good hygiene, schedule an appointment. The pediatric dentist can identify oral causes or refer to a pediatrician or ENT specialist if necessary. Do not ignore persistent bad breath in a child.
Frequently Asked Questions
Is halitosis curable?
Yes, in the vast majority of cases, halitosis is treatable and manageable. If it stems from oral causes (like bacteria on the tongue, Gum Disease, or cavities), addressing these issues usually resolves the problem. For halitosis caused by systemic medical conditions, effective management of the underlying disease can eliminate or significantly reduce bad breath. However, ongoing good oral hygiene and sometimes professional maintenance are often required to prevent recurrence.
How much does treatment for halitosis cost in the US?
The cost varies greatly depending on the cause and required treatment. An initial dental exam ranges from $50-$150. Routine cleanings are $75-$200. If Gum Disease requires deep cleaning, it can cost $200-$600 per quadrant, potentially $800-$2,400+ for a full mouth. Cavity fillings range from $150-$400+. Costs for treating systemic issues vary widely based on medical insurance and the condition. Many dental insurance plans cover preventive care significantly, but major procedures will involve higher out-of-pocket expenses.
Is halitosis treatment painful?
Generally, treatments for halitosis are not painful. Improved oral hygiene involves no pain. Professional cleanings are typically comfortable, though deep cleanings for Gum Disease might involve some mild discomfort or sensitivity, which can be managed with local anesthetic. Dental procedures like fillings are performed with numbing agents. If systemic medical issues are treated, any pain would be related to that specific medical treatment.
How long does it take to get rid of bad breath?
The timeline depends on the cause:
- Physiological/Poor Hygiene: Improvement can be seen within days to a week with diligent oral hygiene.
- Mild Oral Issues (Gingivitis): 1-2 weeks after professional cleaning and consistent home care.
- Severe Oral Issues (Periodontitis, multiple cavities): Several weeks to a few months, as it involves multiple appointments and healing.
- Systemic Causes: Resolution depends on the successful diagnosis and treatment of the underlying medical condition, which can range from weeks to ongoing management.
Are there natural remedies or home cures for halitosis?
While good oral hygiene is fundamental, some natural approaches can help manage symptoms or provide temporary relief:
- Hydration: Drinking plenty of water is essential.
- Chewing Fresh Herbs: Parsley, mint, or basil can temporarily freshen breath.
- Green Tea: Contains polyphenols that can help reduce sulfur compounds.
- Xylitol: Found in sugar-free gum and mints, it stimulates saliva and inhibits bacterial growth.
- Oil Pulling: While some advocate for it, scientific evidence of its effectiveness for halitosis is limited, and it should not replace regular brushing and flossing. Important: Natural remedies should supplement, not replace, professional dental and medical advice. Always consult your dentist.
Does insurance cover halitosis treatment?
Dental insurance typically covers treatments for underlying oral conditions that cause halitosis. This includes:
- Preventive care (exams, cleanings): Often covered at 80-100%.
- Basic procedures (fillings): Usually covered at 50-80%.
- Major procedures (deep cleanings, periodontal surgery, crowns): Generally covered at 50% after deductibles. If halitosis is caused by a systemic medical condition, your medical insurance would apply to the physician visits, diagnostic tests, and treatment for that condition. It's crucial to check with both your dental and medical insurance providers for specific coverage details.
What are the alternatives if standard treatments don't work?
If standard dental treatments and medical referrals don't resolve halitosis, your dentist might explore:
- More advanced diagnostic tests: Such as gas chromatography to pinpoint specific VSCs.
- Specialized mouthwash formulations: With higher concentrations of antimicrobial or oxidizing agents.
- Referral to an ENT (Ear, Nose, Throat) specialist: To rule out obscure nasal or throat conditions.
- Referral to a gastroenterologist: For in-depth investigation of gastrointestinal issues.
- Psychological counseling: If pseudo-halitosis or halitophobia is suspected. Persistent halitosis requires perseverance and a collaborative approach between dental and medical professionals.
When to See a Dentist
While occasional bad breath is normal, it's time to see a dentist about halitosis if:
- Your bad breath is persistent: It doesn't go away after brushing, flossing, or using over-the-counter mouthwash for several days or weeks.
- You frequently experience dry mouth (Xerostomia).
- You notice other symptoms: Such as a persistent bad taste in your mouth, bleeding or swollen gums, loose teeth, or a white/yellowish coating on your tongue.
- Your breath has a distinctly unusual odor: Such as a fruity smell (could indicate diabetes) or an ammonia-like smell (could indicate kidney issues).
- Your halitosis causes you significant social anxiety or impacts your quality of life.
Emergency signs that warrant immediate medical attention (not just dental) include:
- Sudden onset of extremely foul breath accompanied by fever, difficulty swallowing, or a rapidly spreading infection.
- Breath odor alongside unexplained weight loss, chronic fatigue, or severe stomach pain.
Regular dental check-ups are key to preventing and addressing halitosis early. Don't let embarrassment stop you from seeking professional help; halitosis is a common and treatable condition, and your dental team at SmilePedia.net is there to help you achieve fresh breath and optimal oral health.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.