Tartar
3,708 words · 12 min read
Quick Definition
Hardened dental plaque that has calcified on tooth surfaces, also called calculus. Tartar forms above and below the gumline and can only be removed by professional dental instruments.
Tartar: The Hardened Threat to Your Smile
Introduction
Welcome to SmilePedia.net, your definitive resource for understanding crucial aspects of dental health. Today, we delve into tartar, a common yet often misunderstood adversary to a healthy smile. Simply put, tartar is hardened dental plaque that has calcified on tooth surfaces. It's a rough, porous deposit that can range in color from yellow to brown to black, and it forms both above and below the gumline. Once formed, tartar, also known as calculus, cannot be removed by brushing or flossing alone. It requires professional removal by a dental hygienist or dentist using specialized instruments.
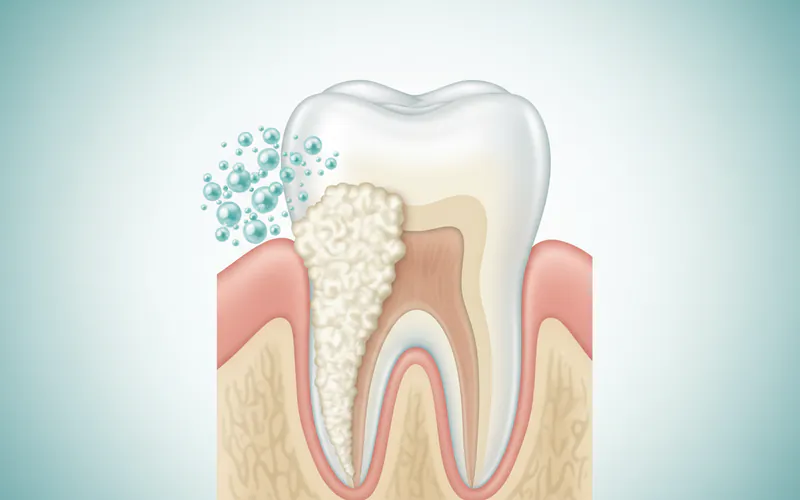
Understanding what tartar is and why it matters is fundamental to maintaining good oral hygiene. Tartar acts as a breeding ground for bacteria, leading to a cascade of oral health problems, including bad breath, gum inflammation (gingivitis), and eventually more severe conditions like periodontal disease and tooth loss. This calcified menace affects a significant portion of the US population. Statistics show that nearly 70% of adults will experience some level of tartar buildup in their lifetime, highlighting its pervasive nature and the critical need for effective prevention and treatment. This article will serve as your comprehensive guide to everything you need to know about tartar, from its formation to its removal and prevention.
Key Takeaways:
- Tartar (or calculus) is hardened dental plaque that sticks firmly to teeth.
- It cannot be removed by regular brushing or flossing once formed.
- Tartar creates a rough surface that attracts more plaque and bacteria.
- It is a primary cause of gingivitis (gum inflammation) and can lead to more severe gum disease.
- Professional dental cleanings are the only way to effectively remove tartar.
- Regular oral hygiene and dental check-ups are crucial for prevention.
Detailed Explanation
Types and Classifications of Tartar (Calculus)
Tartar is broadly classified into two main types based on its location:
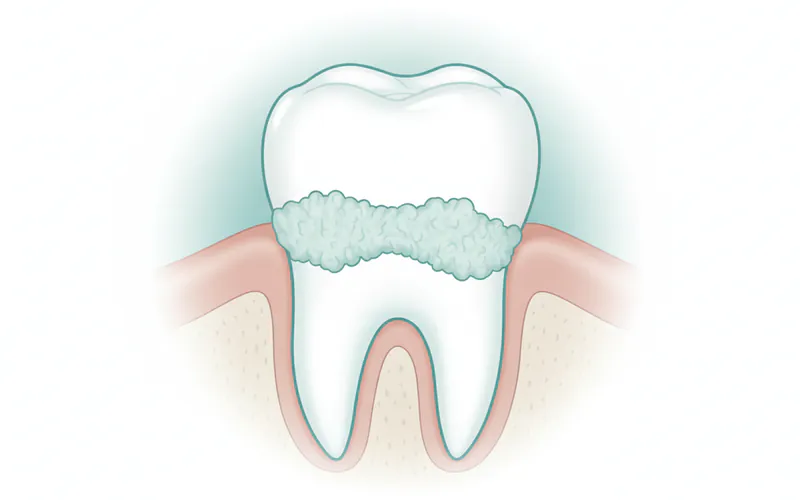
-
Supragingival Calculus: This type of tartar forms above the gumline and is typically visible to the naked eye. It often appears as a yellowish or brownish deposit, particularly on the inner surfaces of the lower front teeth and the outer surfaces of the upper molars (areas close to salivary gland ducts, where minerals for calcification are abundant). Supragingival calculus is generally easier to detect and remove during a routine dental cleaning. Its rough surface readily absorbs stains from food, beverages, and tobacco, contributing to tooth discoloration.
-
Subgingival Calculus: This type of tartar forms below the gumline, within the periodontal pockets that form as gums pull away from the teeth. It is often darker, ranging from dark brown to black, due to the presence of blood pigments. Subgingival calculus is more insidious as it is not visible and its presence directly irritates the gum tissues, contributing significantly to gingivitis and the progression of periodontal disease. Its removal requires specialized instruments and techniques, often part of a deeper cleaning procedure known as scaling and root planing. This type of tartar is particularly dangerous because it harbors harmful bacteria deep within the gum pockets, making it difficult for the body's immune system to fight off the infection.
Causes and Risk Factors for Tartar Formation
Tartar doesn't appear out of nowhere; it's the end product of a biological process involving dental plaque. Plaque is a soft, sticky film of bacteria that constantly forms on your teeth. If plaque is not removed regularly through proper brushing and flossing, it begins to absorb minerals from your saliva (primarily calcium and phosphate). This mineralization process causes the plaque to harden into tartar, typically within 24 to 72 hours of plaque formation.
Several factors can increase your risk of developing tartar:
- Poor Oral Hygiene: Inadequate or infrequent brushing and flossing are the primary culprits. If plaque isn't mechanically removed, it will inevitably calcify.
- Diet: A diet high in sugary and starchy foods provides fuel for plaque-forming bacteria. Acidic foods and drinks can also weaken enamel, making it easier for plaque to adhere.
- Smoking and Tobacco Use: Tobacco products significantly increase the risk of tartar formation, gum disease, and other oral health issues. Smokers tend to accumulate more plaque and tartar than non-smokers.
- Dry Mouth (Xerostomia): Saliva helps wash away food particles and neutralize acids. Reduced saliva flow, often a side effect of certain medications or medical conditions, can lead to increased plaque and tartar buildup.
- Genetics: Some individuals are genetically predisposed to produce more mineral-rich saliva, which can accelerate tartar formation.
- Age: As we age, our teeth and gums become more susceptible to plaque and tartar accumulation.
- Systemic Diseases: Certain systemic conditions, such as diabetes, can compromise the immune system, making individuals more vulnerable to oral infections and increased tartar.
- Crooked Teeth: Misaligned or crowded teeth can create hard-to-reach areas where plaque and tartar can easily accumulate.
- Lack of Regular Dental Check-ups: Professional cleanings are essential for removing existing tartar and identifying potential problem areas early.
Signs and Symptoms to Watch For
Since tartar often forms in less visible areas or below the gumline, it's important to be aware of the signs.
- Rough Texture on Tooth Surfaces: Run your tongue over your teeth. If they feel rough or bumpy, especially near the gumline, it's likely tartar has formed. Clean teeth should feel smooth.
- Visible Yellow, Brown, or Black Deposits: You might notice a discoloration or crusty buildup, particularly on the inner surfaces of your lower front teeth or outer surfaces of your upper back molars.
- Persistent Bad Breath (Halitosis): Tartar's porous surface acts as a haven for odor-producing bacteria, leading to chronic bad breath that doesn't resolve with brushing or mouthwash.
- Red, Swollen, or Bleeding Gums: Tartar irritates the gum tissue, leading to inflammation (gingivitis). You might notice your gums are redder than usual, swollen, tender to the touch, or bleed easily when brushing or flossing.
- Receding Gums: As tartar progresses, it can cause the gum tissue to pull away from the teeth, making your teeth appear longer.
- Sensitivity: While not a direct symptom of tartar, receding gums due to tartar can expose tooth roots, leading to increased tooth sensitivity to hot or cold temperatures.
Diagnosis Process — What Your Dentist Does
Diagnosing tartar buildup is a routine part of every dental check-up. Your dental hygienist or dentist will employ several methods:
- Visual Inspection: They will visually examine your teeth and gums for any visible signs of tartar, discoloration, or gum inflammation. A small mirror is used to inspect all surfaces of your teeth.
- Dental Explorer: A specialized instrument called a dental explorer (a thin, hooked metal tool) is used to gently probe along the tooth surface, feeling for rough, hard deposits, especially along the gumline and in crevices.
- Periodontal Probing: A periodontal probe is used to measure the depth of the gum pockets around each tooth. Healthy gum pockets are typically 1-3 millimeters deep. Deeper pockets (4mm or more) often indicate the presence of subgingival calculus and potential gum disease.
- X-rays: While not always necessary for routine tartar detection, dental X-rays can sometimes reveal significant subgingival calculus or bone loss associated with advanced periodontal disease.
Treatment Options with Pros, Cons, and Costs
Once tartar has formed, it must be removed professionally. This process is commonly known as scaling.
-
Dental Prophylaxis (Routine Cleaning):
- Description: This is the standard preventive cleaning performed by a dental hygienist. It involves removing plaque, calculus (tartar), and stains from the tooth surfaces above and just below the gumline.
- Pros: Prevents gum disease, maintains oral health, removes surface stains, relatively quick and comfortable.
- Cons: Only effective for supragingival and mild subgingival tartar; not sufficient for advanced gum disease.
- Cost Range (US): Typically $75 - $200 without insurance. Most dental insurance plans cover two prophylaxis cleanings per year at 80-100%.
-
Scaling and Root Planing (Deep Cleaning):
- Description: This is a non-surgical procedure used to treat early to moderate periodontal disease. It involves meticulously removing plaque and tartar from both above and below the gumline (scaling) and then smoothing the tooth root surfaces (root planing). Smoothing the root surfaces helps remove bacterial toxins and makes it harder for plaque to reattach. This procedure is often performed under local anesthesia and may require multiple appointments.
- Pros: Effectively removes deep-seated subgingival tartar, reduces gum inflammation, helps gums reattach to teeth, can halt the progression of periodontal disease.
- Cons: More invasive than a regular cleaning, can cause temporary sensitivity and discomfort, more expensive, may require local anesthesia.
- Cost Range (US): This is typically charged per quadrant (quarter of the mouth). Each quadrant can cost $200 - $500, so a full mouth deep cleaning can range from $800 - $2000+ without insurance. Dental insurance usually covers a percentage (e.g., 50-80%) after a deductible.
Comparison Table: Routine Cleaning vs. Deep Cleaning (Scaling and Root Planing)
| Feature | Dental Prophylaxis (Routine Cleaning) | Scaling and Root Planing (Deep Cleaning) |
|---|---|---|
| Purpose | Preventive care, removes plaque & mild tartar | Treats periodontal disease, removes deep plaque & tartar |
| Target Area | Above gumline, slight below gumline | Above and significantly below gumline, root surfaces |
| Anesthesia | Generally not needed | Often uses local anesthesia |
| Duration | 30-60 minutes | 1-2 hours per quadrant, often multiple appointments |
| Instrumentation | Hand scalers, ultrasonic scalers | Specialized hand scalers, ultrasonic scalers, curettes |
| Discomfort | Minimal | Moderate to significant, managed with anesthesia |
| Cost (US, w/o ins.) | $75 - $200 | $200 - $500 per quadrant (total $800 - $2000+ for full mouth) |
| Insurance Coverage | Usually 80-100% (2x/year) | Often 50-80% after deductible |
| Outcome | Maintains health, prevents disease | Reduces gum inflammation, halts disease progression, reattachment |
Step-by-Step: What to Expect During Treatment
Whether you're undergoing a routine cleaning or a deep cleaning, here's a general overview of what to expect:
- Examination: The hygienist or dentist will first examine your mouth to identify areas of plaque and tartar buildup, gum inflammation, and pocket depths.
- Anesthesia (for deep cleaning): If you are having scaling and root planing, local anesthesia will be administered to numb the areas being worked on. This ensures comfort during the procedure.
- Scaling:
- Ultrasonic Scaling: A specialized instrument called an ultrasonic scaler uses high-frequency vibrations and a fine stream of water to break down and wash away tartar and plaque. This tool is very effective for dislodging larger deposits.
- Hand Scaling: Following or in conjunction with the ultrasonic scaler, your hygienist will use various hand scalers and curettes – small, hooked metal instruments – to meticulously scrape away any remaining tartar from the tooth surfaces, both above and below the gumline. They work carefully to ensure all deposits are removed without damaging the tooth or gum tissue.
- Root Planing (for deep cleaning): Once tartar is removed from the root surfaces, the hygienist will use specialized instruments to smooth these surfaces. This process removes bacterial toxins and makes it more difficult for new plaque and bacteria to adhere, promoting gum reattachment.
- Polishing: After all tartar is removed, your teeth will be polished using a small rotating rubber cup and a gritty paste. This removes surface stains and leaves your teeth feeling smooth and clean.
- Flossing: The hygienist will then thoroughly floss your teeth to remove any remaining polishing paste and check for any missed spots.
- Fluoride Treatment (optional): A fluoride treatment may be applied to help strengthen tooth enamel and reduce sensitivity.
Recovery Timeline and Aftercare
For Routine Prophylaxis:
- Recovery: There is generally no downtime. You can resume normal activities immediately.
- Aftercare: Your teeth might feel exceptionally clean and smooth. Some temporary sensitivity, especially to cold, is normal but usually subsides within a few hours. Continue your regular oral hygiene routine.
For Scaling and Root Planing (Deep Cleaning):
- Recovery:
- Immediate (first few hours): Numbness from local anesthesia will wear off. You may experience some discomfort, soreness, and mild bleeding from the gums.
- First few days: Gums may remain tender, swollen, and sensitive. Pain relievers (e.g., ibuprofen) can help manage discomfort. Avoid very hot, cold, or hard, crunchy foods.
- First week: Sensitivity to hot and cold may persist but should gradually decrease. Gums will begin to heal, and inflammation will reduce.
- Aftercare:
- Oral Hygiene: Continue gentle brushing and flossing. Your dentist or hygienist may recommend a special antimicrobial mouthwash.
- Follow-up: You will likely have a follow-up appointment within 4-6 weeks to check gum healing and pocket depths.
- Maintenance: Regular periodontal maintenance cleanings (often every 3-4 months) will be crucial to prevent the recurrence of tartar and manage gum disease long-term.
Prevention Strategies
Preventing tartar is largely within your control and relies on consistent, effective oral hygiene:
- Brush Twice Daily: Use a soft-bristled toothbrush and fluoride toothpaste. Brush for at least two minutes each time, ensuring you clean all tooth surfaces, especially along the gumline. Electric toothbrushes are often more effective at removing plaque.
- Floss Daily: Flossing is crucial for removing plaque and food particles from between your teeth and under the gumline, areas your toothbrush can't reach.
- Use an Antimicrobial Mouthwash: While not a substitute for brushing and flossing, an ADA-approved antimicrobial mouthwash can help reduce bacteria in your mouth and fight plaque.
- Regular Dental Check-ups and Professional Cleanings: Visit your dentist for check-ups and prophylaxis cleanings at least twice a year (every six months). This allows for early detection and removal of plaque and tartar before it causes significant problems. Individuals with a history of periodontal disease may require more frequent cleanings (e.g., every 3-4 months).
- Healthy Diet: Limit sugary and starchy foods and drinks. These feed the bacteria that form plaque. Choose a balanced diet rich in fruits, vegetables, and lean proteins.
- Avoid Tobacco Products: Smoking and chewing tobacco are significant risk factors for tartar buildup and gum disease. Quitting can dramatically improve your oral and overall health.
- Stay Hydrated: Drinking plenty of water helps rinse away food particles and bacteria.
Cost Ranges in the US (with/without Insurance)
The cost of tartar removal varies based on the severity of the buildup, the type of procedure, and your insurance coverage. All costs are estimates and can vary by location and provider.
-
Routine Dental Prophylaxis (Cleaning):
- Without Insurance: Typically ranges from $75 to $200.
- With Insurance: Most dental insurance plans cover 80-100% of routine cleanings, often allowing for two per year. You might pay a small co-pay or nothing.
-
Scaling and Root Planing (Deep Cleaning):
- Without Insurance: This is usually charged per quadrant of the mouth. Each quadrant can cost between $200 and $500. For a full mouth deep cleaning (4 quadrants), the total could range from $800 to $2000+.
- With Insurance: Insurance plans usually classify deep cleaning as a "major procedure" or "basic procedure" and typically cover 50-80% after you meet your deductible. This means you could still be responsible for a significant portion, potentially $400 to $1000 or more for a full mouth.
-
Periodontal Maintenance (after deep cleaning):
- Without Insurance: Often slightly more expensive than a regular cleaning, ranging from $100 to $250 per visit.
- With Insurance: Coverage varies, but often similar to routine cleanings or a slightly higher co-pay/percentage. These are typically required more frequently (every 3-4 months).
It's always recommended to check with your specific dental insurance provider and your dental office for an exact cost estimate before any procedure.
For Parents / Pediatric Considerations
Tartar isn't just an adult problem; children can also develop it, though it's less common than in adults. The primary cause in children is usually inadequate oral hygiene, especially around the time permanent teeth erupt.
- Early Formation: Tartar can start forming in children around the age of 6 or 7, often appearing on the lower front teeth.
- Risk Factors: Similar to adults, poor brushing and flossing, frequent consumption of sugary snacks and drinks, and even certain medications can contribute to tartar buildup in children.
- Prevention is Key:
- Start Early: Begin cleaning your baby's gums even before teeth emerge. Brush with a soft infant toothbrush and a tiny smear of fluoride toothpaste as soon as the first tooth appears.
- Supervised Brushing: Supervise children's brushing until they are about 7 or 8 years old to ensure thoroughness. Make sure they are using an ADA-approved fluoride toothpaste.
- Flossing: Introduce flossing once two teeth touch.
- Regular Dental Visits: Take your child to the dentist for their first check-up by their first birthday or within 6 months of the first tooth erupting. Regular check-ups (every 6 months) are crucial for professional cleanings and early detection of tartar.
- Treatment: If a child develops tartar, it needs to be removed by a pediatric dentist or hygienist using similar scaling techniques as in adults, often with gentler instruments. Early removal is vital to prevent gingivitis and set the stage for good long-term oral health.
Frequently Asked Questions
Q1: Is removing tartar painful?
A: The sensation of tartar removal depends on the amount of tartar, its location, and the individual's pain tolerance. For routine cleanings with mild to moderate tartar, discomfort is usually minimal, often described as a scraping or tickling sensation. If you have significant subgingival tartar and gum inflammation, a deep cleaning (scaling and root planing) may be necessary. This procedure is often performed with local anesthesia to numb the gums and ensure comfort. After the anesthesia wears off, some soreness and sensitivity are common but can be managed with over-the-counter pain relievers.
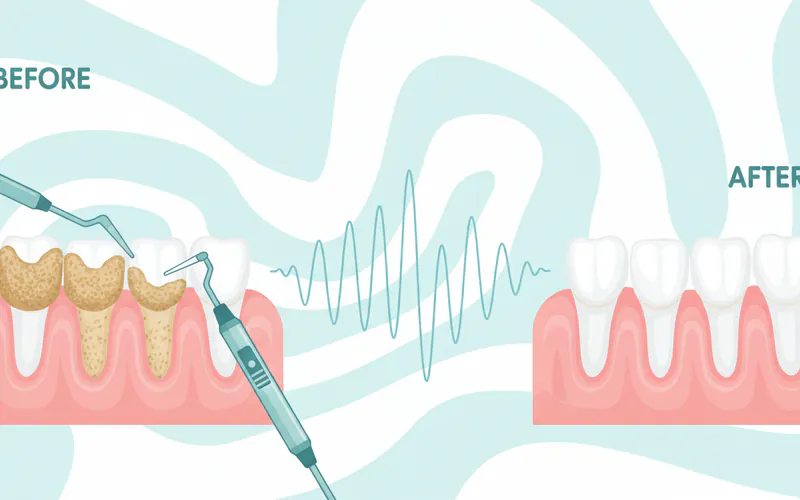
Q2: Can I remove tartar myself at home?
A: No, you cannot safely or effectively remove tartar yourself at home. Tartar is calcified and firmly adhered to the tooth surface. Attempting to scrape it off with sharp objects can damage your tooth enamel, scratch your gums, or introduce bacteria, leading to infections. Over-the-counter "tartar control" toothpastes and mouthwashes can help prevent new tartar formation by reducing plaque mineralization, but they cannot remove existing tartar. Professional dental instruments and techniques are required for proper removal without causing harm.
Q3: How long does a tartar removal appointment take?
A: A routine dental cleaning (prophylaxis) to remove plaque and supragingival tartar typically takes between 30 to 60 minutes. If you require a deep cleaning (scaling and root planing) for significant subgingival tartar, it is often performed over multiple appointments, with each appointment (covering one or two quadrants of the mouth) lasting between 1 to 2 hours. The exact duration depends on the severity of the tartar buildup and the individual's needs.
Q4: Why does tartar keep coming back even after a cleaning?
A: Tartar formation is a continuous process because plaque is constantly forming on your teeth. If even tiny amounts of plaque are missed during daily brushing and flossing, they can quickly calcify into new tartar. Certain individuals are also more prone to tartar buildup due to factors like saliva composition, genetics, and diet. While professional cleanings remove existing tartar, diligent at-home oral hygiene and regular dental check-ups (often more frequent, e.g., every 3-4 months, for those prone to heavy buildup) are essential to minimize its recurrence.
Q5: Are there any alternatives to professional scaling for tartar removal?
A: For existing, calcified tartar, there are no effective alternatives to professional scaling by a dental hygienist or dentist. "Tartar control" toothpastes and mouthwashes can help prevent new tartar from forming, but they cannot dissolve or remove established calculus. Some alternative medicine practitioners may suggest natural remedies, but these are not scientifically proven to remove tartar and may delay necessary professional treatment, potentially leading to more severe dental problems.
Q6: Does dental insurance cover tartar removal?
A: Yes, most dental insurance plans cover tartar removal to some extent.
- Routine Prophylaxis (standard cleaning): Typically covered at 80-100%, often allowing for two cleanings per year with little to no out-of-pocket cost.
- Scaling and Root Planing (deep cleaning): This is usually considered a "basic" or "major" procedure and may be covered at 50-80% after you meet your deductible. This means you will likely have a co-payment for this service.
- Periodontal Maintenance: Coverage varies; some plans treat it like a regular cleaning, while others may have a different coverage percentage. It's crucial to consult your specific insurance policy and speak with your dental office's financial coordinator to understand your exact coverage and potential out-of-pocket expenses.
When to See a Dentist
Regular dental check-ups and cleanings are the cornerstone of preventing and managing tartar. It is recommended to visit your dentist at least twice a year (every six months) for a prophylaxis cleaning and examination.
However, certain signs and symptoms warrant immediate attention, beyond your routine care:
- Visible Tartar: If you can see hard, discolored deposits on your teeth, particularly near the gumline.
- Persistent Bad Breath: If bad breath doesn't improve with regular brushing and flossing, it could be a sign of significant tartar buildup and bacterial overgrowth.
- Red, Swollen, or Bleeding Gums: These are classic signs of gingivitis, which is often caused by tartar. If your gums bleed when you brush or floss, or feel tender and puffy, schedule an appointment promptly.
- Pain or Discomfort: Any persistent pain, sensitivity, or discomfort in your teeth or gums.
- Receding Gums or Loose Teeth: These are signs of advanced periodontal disease, which tartar significantly contributes to.
- Changes in Bite: If your teeth feel different when you bite down, or you notice new spaces developing between teeth.
Do not wait for these symptoms to worsen. Early intervention is key to preventing the progression of gum disease and maintaining your overall oral health. Your dental team at SmilePedia.net encourages you to be proactive about your oral hygiene and seek professional care regularly.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.