Gum Disease Treatments: Complete Guide
Key Takeaways
- Gum Disease Treatments: Complete Guide
Gum Disease Treatments: Complete Guide
Gum disease, also known as periodontal disease, affects nearly half of American adults aged 30 and older, according to the Centers for Disease Control and Prevention (CDC). This staggering statistic underscores the widespread nature of this chronic inflammatory condition, which, if left untreated, can lead to severe oral health issues, including tooth loss, and has even been linked to systemic health problems like heart disease and diabetes. Understanding the various gum disease treatments available is crucial for protecting your smile and overall well-being. From non-invasive procedures for early periodontal disease to advanced surgical interventions, modern dentistry offers a range of effective solutions designed to halt the progression of gum disease, restore gum health, and preserve your natural teeth. This comprehensive guide will walk you through everything you need to know about diagnosing, treating, and preventing gum disease, ensuring you have the knowledge to make informed decisions about your oral health. We will cover the types of gum disease, its causes, tell-tale signs like a persistent swollen gum, detailed treatment options, costs, recovery, and essential prevention strategies.
Key Takeaways:
- Early Detection is Key: Treating gingivitis (early gum disease) often involves professional cleaning and improved home care, preventing progression to periodontitis.
- Non-Surgical Treatments: Scaling and Root Planing (SRP) is the most common non-surgical treatment for moderate gum disease, costing $200-$500 per quadrant and taking 1-2 visits. Recovery is typically a few days.
- Surgical Interventions: Advanced gum disease may require procedures like flap surgery, bone grafts, or gum grafts, which can range from $500 to $4,000+ per quadrant/site. Recovery can take several weeks.
- Cost & Insurance: Gum disease treatments are often covered partially by dental insurance (50-80% for major procedures), but out-of-pocket costs can be significant. Discuss financing options with your dentist.
- Prevention is Paramount: Daily brushing, flossing, regular dental check-ups (at least twice a year), and a healthy lifestyle are essential for preventing gum disease and maintaining treatment results.
- Systemic Health Link: Untreated gum disease is linked to serious health conditions like heart disease, stroke, and diabetes, highlighting the importance of timely intervention.
- Long-Term Maintenance: Successful treatment requires ongoing periodontal maintenance appointments (typically every 3-4 months) to prevent recurrence and ensure lasting health.
What It Is / Overview
Gum disease, medically known as periodontal disease, is a progressive inflammatory condition that affects the tissues supporting your teeth. It begins with bacterial growth in your mouth and, if not properly treated, can eventually lead to tooth loss.

It primarily manifests in two main stages:
- Gingivitis: This is the earliest and mildest form of gum disease. It is characterized by inflammation of the gums, usually caused by plaque buildup along the gumline. At this stage, the gums may become red, swollen gum, tender, and bleed easily, particularly during brushing or flossing. Crucially, gingivitis typically does not involve bone loss and is reversible with professional cleaning and diligent oral hygiene.
- Periodontitis: If gingivitis is left untreated, it can advance to periodontitis. In this more severe stage, the inflammation spreads beyond the gums to the underlying bone and ligaments that support the teeth. The body's immune response, combined with bacterial toxins, begins to break down the bone and connective tissue. This leads to the formation of "pockets" between the teeth and gums, which become reservoirs for more bacteria. As the disease progresses, these pockets deepen, more bone is lost, and teeth may become loose, shift, or even fall out. Periodontitis is a chronic condition that requires ongoing management and is often irreversible in terms of lost bone, though its progression can be halted.
Types / Variations of Gum Disease
While the general progression is from gingivitis to periodontitis, periodontitis itself has several classifications based on its severity and specific characteristics:
- Chronic Periodontitis: This is the most common form, typically affecting adults but can occur at any age. It's characterized by slow to moderate progression of attachment loss and bone destruction.
- Aggressive Periodontitis: A less common but rapidly progressing form, often seen in otherwise healthy individuals, sometimes with a genetic predisposition. It involves rapid attachment loss and bone destruction and may affect specific teeth or be generalized.
- Necrotizing Periodontal Diseases: These severe forms (Necrotizing Ulcerative Gingivitis - NUG and Necrotizing Ulcerative Periodontitis - NUP) are characterized by necrosis (tissue death) of the gum tissue, periodontal ligament, and alveolar bone. They are most common in individuals with compromised immune systems (e.g., HIV/AIDS, malnutrition, severe stress).
- Periodontitis as a Manifestation of Systemic Diseases: In some cases, gum disease can be a symptom or complication of other systemic conditions, such as diabetes, certain blood disorders, or genetic syndromes.
- Periodontal Abscesses: Localized collections of pus within the gum tissue or supporting structures, often causing acute pain and swelling.
- Peri-implant Diseases: These conditions affect the soft tissues and bone surrounding dental implants, similar to how periodontitis affects natural teeth. Peri-implant mucositis is comparable to gingivitis, while peri-implantitis is analogous to periodontitis, leading to bone loss around the implant.
Causes / Why It Happens
The primary cause of gum disease is the accumulation of bacterial plaque—a sticky, colorless film that constantly forms on your teeth. If plaque is not removed daily through brushing and flossing, it hardens into tartar (calculus). Tartar cannot be removed by brushing alone and provides a rough surface where more plaque can accumulate, irritating the gums.
Beyond plaque and tartar, several factors contribute to the development and progression of gum disease:
- Poor Oral Hygiene: Inadequate brushing and flossing allow plaque to accumulate, leading to gingivitis and eventually periodontitis.
- Smoking/Tobacco Use: Smoking is one of the most significant risk factors for developing severe gum disease. It impairs the immune system, making it harder for gums to fight infection, and interferes with healing.
- Hormonal Changes: Fluctuations during pregnancy, puberty, menstruation, or menopause can make gums more sensitive and prone to inflammation.
- Certain Medications: Some drugs, such as antidepressants, heart medications, and oral contraceptives, can reduce saliva flow (dry mouth), which helps protect teeth and gums. Others can cause abnormal gum tissue growth (gingival overgrowth).
- Systemic Diseases: Conditions like diabetes, heart disease, autoimmune diseases, and HIV can weaken the immune system, making individuals more susceptible to gum infections.
- Genetics: Some people are genetically predisposed to gum disease, making them more likely to develop it even with good oral hygiene.
- Poor Nutrition: A diet lacking essential nutrients, especially Vitamin C, can compromise the immune system and make it harder for gum tissue to repair itself.
- Stress: Chronic stress can weaken the immune system, potentially making it harder to fight off infections, including gum disease.
- Bruxism (Teeth Grinding/Clenching): Excessive force on teeth can accelerate the breakdown of the periodontal ligaments and bone.
- Crooked Teeth or Fillings: Teeth that are crowded, crooked, or have ill-fitting restorations can create areas that are difficult to clean, leading to plaque buildup.
Signs and Symptoms
Recognizing the signs of gum disease early is vital for effective gum disease treatments and preventing more severe complications. Pay attention to the following indicators:
- Red, Swollen, or Tender Gums: Healthy gums are typically pink and firm. If your gums appear red, purplish, puffy, or feel tender to the touch, it's a common sign of inflammation, indicating early periodontal disease (gingivitis). A localized swollen gum could also signify an abscess.
- Bleeding Gums: Gums that bleed easily during brushing, flossing, or even when eating hard foods are a significant red flag. This is often one of the first noticeable symptoms of gingivitis.
- Persistent Bad Breath (Halitosis): The bacteria associated with gum disease produce foul-smelling gases, leading to chronic bad breath that doesn't go away with brushing or mouthwash.
- Receding Gums: If your gums appear to be pulling away from your teeth, making your teeth look longer, this is a sign of gum recession. It exposes more of the tooth root, which can lead to sensitivity.
- Pus Between Teeth and Gums: A clear sign of infection, indicating active periodontitis.
- Loose or Shifting Teeth: As the bone and supporting structures are destroyed, teeth can become mobile or change position, creating gaps or affecting your bite. This is a sign of advanced periodontitis.
- Changes in Bite: A change in how your teeth fit together when you bite down, or a change in the fit of partial dentures, can indicate underlying bone loss or shifting teeth.
- Pain while Chewing: Discomfort or pain when chewing, especially with firm foods, can be a symptom of severe gum disease.
- Increased Tooth Sensitivity: Exposed tooth roots due to gum recession can be highly sensitive to hot, cold, or sweet stimuli.
If you notice any of these symptoms, especially persistent bleeding or a chronically swollen gum, it's crucial to schedule an appointment with your dentist promptly for diagnosis and to discuss potential gum disease treatments.
Treatment Options
The approach to gum disease treatments depends largely on the severity of the disease, from early gingivitis to advanced periodontitis. The goal is always to remove plaque and tartar, reduce inflammation, eliminate bacterial infection, and prevent further damage.
A. Non-Surgical Treatments (for Gingivitis and Early to Moderate Periodontitis)
These are typically the first line of defense for less severe cases.
1. Professional Dental Cleaning (Prophylaxis)
- What it is: A routine dental cleaning performed by a dentist or dental hygienist to remove plaque and tartar from above and slightly below the gum line.
- Pros: Non-invasive, relatively quick, effective for gingivitis.
- Cons: Not sufficient for periodontitis where pockets are deep.
- Process: Your dental professional will use specialized instruments (scalers, ultrasonic devices) to meticulously clean all tooth surfaces, including areas that your toothbrush can't reach. Followed by polishing.
- Cost: Typically $75 - $200 in the US, often covered 100% by insurance if done twice a year.
2. Scaling and Root Planing (SRP) - "Deep Cleaning"
- What it is: A more intensive non-surgical procedure for early periodontal disease or moderate periodontitis. It involves scaling (removing plaque and tartar from above and below the gum line) and root planing (smoothing the root surfaces to remove bacterial toxins and prevent future plaque attachment).
- Pros: Highly effective at arresting the progression of moderate gum disease, avoids surgery, less invasive.
- Cons: Requires local anesthesia, may cause temporary sensitivity and discomfort, not suitable for advanced cases with significant bone loss.
- Process: Usually performed in 1-4 appointments, often one quadrant of the mouth at a time, under local anesthesia. The hygienist or dentist uses specialized instruments to meticulously clean the root surfaces.
- Cost: $200 - $500 per quadrant in the US. Total cost for a full mouth (4 quadrants) can be $800 - $2,000. Insurance typically covers 50-80% of the cost.
- Pro Tip: After SRP, commit to meticulous home care and regular periodontal maintenance cleanings (every 3-4 months) to prevent disease recurrence.
3. Local and Oral Antibiotics
- What it is: Antibiotics can be used as an adjunct to scaling and root planing to control bacterial infection.
- Local Delivery: Antibiotic gels, chips, or fibers (e.g., Arestin, Atridox) are placed directly into periodontal pockets after SRP, releasing medication over several days or weeks.
- Oral Antibiotics: Systemic antibiotics (e.g., amoxicillin, doxycycline, metronidazole) may be prescribed for widespread or aggressive infections.
- Pros: Targets specific bacteria, enhances the effectiveness of mechanical cleaning.
- Cons: Potential for side effects (e.g., digestive upset with oral antibiotics), risk of antibiotic resistance.
- Cost: Local antibiotics range from $50 - $150 per site/pocket. Oral antibiotics typically cost $20 - $100 for a course, depending on the drug.
4. Laser Therapy
- What it is: Lasers (like Nd:YAG or diode lasers) can be used to remove inflamed tissue and bacterial deposits from periodontal pockets.
- Pros: Less invasive than traditional surgery, may reduce bleeding and swelling, faster healing in some cases.
- Cons: Not yet universally adopted as a primary treatment, efficacy compared to traditional methods is debated, can be more expensive.
- Cost: Ranges from $200 - $1,000 per quadrant, often an add-on to SRP or a standalone procedure, potentially not fully covered by insurance.
B. Surgical Treatments (for Moderate to Advanced Periodontitis)
When non-surgical treatments are insufficient, surgery may be necessary to repair damage and prevent further tooth loss.
1. Flap Surgery (Pocket Reduction Surgery)
- What it is: The most common surgical procedure for periodontitis. The gums are lifted back, and the underlying plaque, tartar, and diseased tissue are removed. The bone surface may be reshaped, and then the gum tissue is sutured back, usually tighter around the tooth, to reduce pocket depth.
- Pros: Effectively reduces pocket depth, making it easier to clean and maintain, halts disease progression.
- Cons: More invasive, requires longer recovery, potential for gum recession and increased sensitivity.
- Process: Performed under local anesthesia, sometimes with sedation. Incisions are made, gums are folded back, roots are cleaned, bone is recontoured if needed, and gums are sutured.
- Cost: $500 - $2,000 per quadrant in the US, depending on complexity and location.
2. Bone Grafting
- What it is: Used when periodontitis has destroyed the bone supporting the teeth. Fragments of your own bone, synthetic bone, or donated bone are used to replace the lost bone and encourage regeneration.
- Pros: Can regenerate lost bone, stabilize teeth, and prepare for future implants if teeth are lost.
- Cons: Invasive, variable success rates, longer recovery period.
- Process: Often performed in conjunction with flap surgery. Graft material is placed in the defect, and gums are sutured over it.
- Cost: $600 - $3,000 per site, depending on the material and extent of bone loss.
3. Soft Tissue Grafts (Gum Grafts)
- What it is: Used to treat gum recession, where the gum tissue has pulled away from the teeth, exposing the roots. Tissue is typically taken from the roof of your mouth (palate) or a tissue bank and attached to the areas where the gum has receded.
- Pros: Covers exposed roots, reduces sensitivity, prevents further recession and bone loss, improves aesthetics.
- Cons: Invasive, two surgical sites (donor and recipient) if using your own tissue, longer healing.
- Process: A small piece of tissue is harvested or prepared, then carefully stitched over the exposed root surface.
- Cost: $700 - $3,000 per tooth/site, varies based on the type of graft and complexity.
4. Guided Tissue Regeneration (GTR)
- What it is: A surgical procedure that uses barrier membranes (resorbable or non-resorbable) to prevent gum tissue from growing into the bone defect, allowing bone and connective tissue cells to regenerate.
- Pros: Promotes regeneration of lost periodontal structures (bone, ligament, cementum).
- Cons: Complex procedure, higher cost, variable outcomes.
- Process: A membrane is placed between the gum tissue and the bone defect after cleaning the root surfaces, then the gums are sutured.
- Cost: $1,000 - $4,000 per site, often combined with bone grafting.
C. Emerging Treatments
- Growth Factors: Application of proteins (e.g., Emdogain) that stimulate tissue regeneration.
- Platelet-Rich Plasma (PRP) / Platelet-Rich Fibrin (PRF): Derived from the patient's blood, these concentrate growth factors to promote healing.
- Host Modulation Therapy: Medications that modify the body's inflammatory response to gum disease, rather than directly killing bacteria.
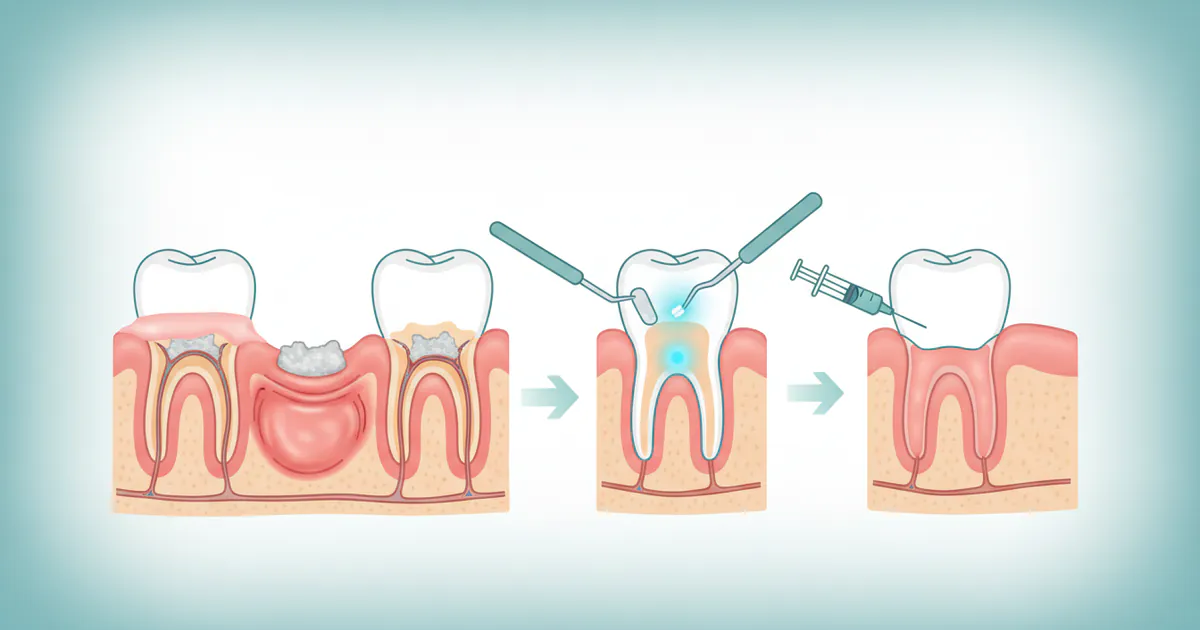
Step-by-Step Process: What to Expect During Treatment
Let's detail the typical journey for a patient undergoing gum disease treatments, focusing on scaling and root planing (SRP) as a common initial intervention, and then a general overview of a surgical procedure.

Step-by-Step: Scaling and Root Planing (Deep Cleaning)
-
Initial Examination and Diagnosis:
- Your dentist or periodontist will perform a thorough examination, including measuring pocket depths around your teeth using a periodontal probe. Pocket depths greater than 3mm usually indicate gum disease.
- X-rays will be taken to assess bone loss.
- Based on these findings, they will determine the extent of your gum disease and recommend SRP if appropriate.
-
Anesthesia:
- Before the procedure, local anesthesia will be administered to numb the specific area(s) of your mouth being treated (often one quadrant at a time). This ensures you are comfortable and feel no pain during the cleaning.
-
Scaling:
- Using an ultrasonic scaler (a device that uses high-frequency vibrations and water to break up and wash away plaque and tartar) and/or specialized hand instruments (curettes and sickles), the hygienist or dentist will meticulously remove all plaque, tartar, and bacterial toxins from the tooth surfaces, both above and below the gum line, extending into the periodontal pockets.
-
Root Planing:
- After scaling, the root surfaces are carefully planed (smoothed). This step is crucial as it removes any remaining bacterial toxins and rough spots on the root where bacteria can easily re-attach. A smooth root surface also allows the gum tissue to reattach more firmly, reducing pocket depth.
-
Irrigation (Optional):
- Sometimes, an antimicrobial rinse or local antibiotic might be applied directly into the pockets after scaling and root planing to further reduce bacteria.
-
Post-Procedure Instructions:
- You will receive detailed instructions on aftercare, including managing sensitivity, avoiding certain foods, and continuing excellent home oral hygiene.
- A follow-up appointment (usually 4-6 weeks later) will be scheduled to assess healing and re-measure pocket depths.
Step-by-Step: Periodontal Surgery (e.g., Flap Surgery)
-
Pre-Surgical Consultation:
- The periodontist will explain the procedure, potential risks, benefits, and expected recovery.
- You may be given specific instructions regarding medication, eating, and drinking before surgery.
-
Anesthesia:
- Local anesthesia will be administered to numb the surgical area. Sedation (oral or IV) may also be offered to help you relax.
-
Incisions and Gum Lifting:
- Small incisions are made in the gum tissue, allowing the periodontist to gently lift back a section of the gum (a "flap") to expose the root surfaces and underlying bone.
-
Cleaning and Reshaping:
- All plaque, tartar, and diseased tissue are thoroughly removed from the root surfaces and inside the bone defects.
- If necessary, irregular bone surfaces may be smoothed or reshaped to reduce pockets, or bone graft material/membranes may be placed to encourage regeneration.
-
Suturing and Dressing:
- The gum flap is then repositioned against the teeth and secured with sutures (stitches), often bringing the gum line slightly lower to reduce pocket depth.
- A surgical dressing (a putty-like material) may be placed over the sutures to protect the surgical site and promote healing.
-
Post-Operative Care:
- You will receive comprehensive instructions on pain management, diet restrictions (soft foods), oral hygiene (gentle brushing, special rinses), and how to care for the surgical site.
- Follow-up appointments will be scheduled to remove sutures (if non-resorbable) and monitor healing.
Cost and Insurance
The cost of gum disease treatments in the US can vary significantly based on the type and severity of the disease, the specific procedure, the geographic location (urban vs. rural, high cost of living areas), and the dental professional's fees (general dentist vs. periodontist).
Average US Price Ranges (Out-of-Pocket, without insurance)
- Routine Dental Cleaning (Prophylaxis): $75 - $200
- Scaling and Root Planing (SRP):
- Per quadrant: $200 - $500
- Full mouth (4 quadrants): $800 - $2,000
- Local Antibiotic Application (e.g., Arestin): $50 - $150 per site/pocket
- Flap Surgery (Pocket Reduction Surgery): $500 - $2,000 per quadrant
- Bone Grafting: $600 - $3,000 per site
- Soft Tissue Graft (Gum Graft): $700 - $3,000 per tooth/site
- Guided Tissue Regeneration (GTR): $1,000 - $4,000 per site
- Periodontal Maintenance Cleaning (after active treatment): $100 - $300 (typically every 3-4 months)
Regional Variations
Costs can be higher in major metropolitan areas (e.g., New York City, Los Angeles, Boston) due to higher overheads and cost of living. For example:
- Northeast/West Coast: SRP might lean towards the higher end of $400-$500 per quadrant.
- Midwest/South: SRP might be closer to $200-$350 per quadrant.
Insurance Coverage Details
Dental insurance often plays a significant role in making gum disease treatments more affordable. Coverage levels vary greatly depending on your plan (PPO, HMO, Fee-for-Service).
- Diagnostic & Preventive (e.g., exams, routine cleanings, X-rays): Often covered at 80-100%.
- Basic Procedures (e.g., fillings, simple extractions): Typically covered at 70-80%.
- Major Procedures (e.g., SRP, periodontal surgery, crowns): Usually covered at 50%.
Key Considerations for Insurance:
- Deductibles: The amount you must pay out-of-pocket before your insurance begins to pay.
- Annual Maximums: The maximum amount your insurance will pay in a given year (often $1,000 - $2,000 for most plans).
- Waiting Periods: Some plans have waiting periods (e.g., 6-12 months) before covering major procedures.
- Pre-authorization: For major procedures, your dentist may need to submit a pre-treatment estimate to your insurance company to determine coverage beforehand.
Pro Tip: Always confirm your specific benefits with your insurance provider and discuss treatment costs and payment plans with your dental office before starting any significant gum disease treatments. Many offices offer in-house payment plans or work with third-party financing companies like CareCredit.
Recovery and Aftercare
Proper recovery and diligent aftercare are essential for the success of gum disease treatments and preventing recurrence. What to expect varies significantly between non-surgical and surgical procedures.
After Scaling and Root Planing (SRP):
- Discomfort: You may experience mild soreness, tenderness, and gum sensitivity for a few days. Over-the-counter pain relievers (e.g., ibuprofen, acetaminophen) can help.
- Sensitivity: Teeth may be sensitive to hot or cold for a few days to a few weeks, especially if roots were previously exposed. Desensitizing toothpaste can be beneficial.
- Bleeding: Minor bleeding is possible for a day or two.
- Swelling: Slight gum swelling might occur.
- Eating: Stick to soft, non-spicy foods for the first day or two. Avoid very hot or cold foods if sensitivity is an issue.
- Oral Hygiene: Continue gentle brushing and flossing immediately, but avoid aggressive brushing around sensitive areas. Your dentist may recommend an antimicrobial mouthwash.
- Follow-up: A follow-up appointment (typically 4-6 weeks) is crucial to assess healing and the effectiveness of the treatment.

After Periodontal Surgery (e.g., Flap Surgery, Bone/Gum Grafts):
Recovery is generally more extensive and longer than for non-surgical treatments.
- Pain & Swelling: Moderate pain and swelling are common for several days. Your periodontist will likely prescribe stronger pain medication and recommend ice packs for swelling.
- Bleeding: Some oozing or bleeding from the surgical site is normal for the first 24-48 hours.
- Diet: A soft food diet is essential for at least 1-2 weeks, avoiding chewing on the surgical side. Avoid crunchy, sticky, or very hot foods.
- Oral Hygiene: You'll be instructed to avoid brushing or flossing the surgical site for a specified period (e.g., 1-2 weeks). Instead, you'll use a prescribed antimicrobial mouthwash (e.g., chlorhexidine) to keep the area clean.
- Activity: Avoid strenuous exercise for a few days to a week to prevent increased bleeding or discomfort.
- Smoking: Absolutely avoid smoking, as it severely impairs healing and dramatically increases the risk of complications and treatment failure.
- Sutures & Dressings: If surgical dressings were placed, they typically remain for 1-2 weeks. Non-resorbable sutures will be removed at a follow-up appointment, usually 7-10 days post-surgery.
- Healing Timeline: Initial healing takes 1-2 weeks, but complete tissue maturation can take several months. Bone grafting takes many months to integrate.
- Follow-up: Multiple follow-up appointments will be scheduled to monitor healing, remove sutures, and provide further instructions.
Long-Term Aftercare for All Treatments:
Regardless of the initial treatment, the long-term success of managing gum disease hinges on consistent oral hygiene and regular periodontal maintenance appointments. These specialized cleanings (typically every 3-4 months, compared to twice a year for healthy individuals) are critical to remove new plaque and tartar buildup and monitor gum health, preventing the disease from recurring.
Prevention
Preventing gum disease is largely within your control and is far simpler and less costly than undergoing gum disease treatments. The foundation of prevention is excellent oral hygiene combined with a healthy lifestyle.
-
Brush Your Teeth Twice Daily:
- Use a soft-bristled toothbrush and fluoride toothpaste.
- Brush for at least two minutes each time, covering all surfaces of your teeth and gently along the gum line.
- Consider an electric toothbrush, as many are more effective at removing plaque than manual brushing.
-
Floss Daily:
- Flossing removes food particles and plaque from between your teeth and under the gum line, areas your toothbrush can't reach. This is critical for preventing early periodontal disease.
- If traditional floss is difficult, consider interdental brushes, water flossers, or other interdental cleaning aids recommended by your dentist.
-
Use an Antimicrobial Mouthwash:
- An ADA-accepted therapeutic mouthwash can help reduce plaque and gingivitis. It's an adjunct to brushing and flossing, not a replacement.
-
Regular Dental Check-ups and Professional Cleanings:
- Visit your dentist at least every six months (or more frequently if you have risk factors or a history of gum disease).
- Professional cleanings remove tartar buildup that cannot be removed at home, effectively preventing gingivitis from progressing.
-
Maintain a Healthy Diet:
- Eat a balanced diet rich in vitamins and minerals, especially Vitamin C, which is important for gum health.
- Limit sugary foods and drinks, which feed the bacteria that produce plaque.
-
Avoid Tobacco Products:
- Smoking and other tobacco use are major risk factors for severe gum disease. Quitting dramatically improves your gum health and the success rate of any gum disease treatments.
-
Manage Systemic Health Conditions:
- If you have conditions like diabetes, control them effectively, as they can significantly impact gum health.
- Discuss any medications you're taking with your dentist, as some can affect your gums.
-
Address Bruxism (Teeth Grinding):
- If you grind or clench your teeth, discuss this with your dentist. A nightguard can protect your teeth and supporting structures from excessive force.
Pro Tip: Consistency is key. Even minor lapses in daily oral hygiene can allow plaque to accumulate and lead to inflammation, especially for those prone to gum disease.
Risks and Complications
While gum disease treatments are generally safe and effective, like any medical procedure, there are potential risks and complications, especially if the disease is advanced or if post-treatment care is neglected.
During/Immediately After Treatment:
- Infection: Though rare, any surgical procedure carries a risk of infection.
- Excessive Bleeding: Can occur during or after surgery.
- Pain and Swelling: Expected but can be more severe or prolonged in some cases.
- Nerve Damage: Extremely rare, but possible with invasive surgery, leading to temporary or permanent numbness.
- Adverse Reaction to Anesthesia: A rare but possible risk.
Post-Treatment Complications:
- Increased Tooth Sensitivity: Very common after SRP and surgery, particularly with exposed root surfaces. Usually temporary but can be persistent.
- Gum Recession: Especially after flap surgery, gums may recede further, making teeth appear longer. This can increase sensitivity and affect aesthetics.
- Tooth Loosening/Loss: In severe cases, even after extensive treatment, teeth may remain loose or eventually need extraction if the supporting bone loss is too great.
- Re-infection/Recurrence: Without diligent home care and regular periodontal maintenance, gum disease can recur, necessitating further treatment.
- Failure of Graft: Bone and soft tissue grafts may not always integrate successfully.
- Cosmetic Concerns: Changes in gum contour or tooth length can sometimes be aesthetically unpleasing.
- Systemic Complications (if untreated): Persistent gum disease is linked to an increased risk of heart disease, stroke, poorly controlled diabetes, respiratory disease, and adverse pregnancy outcomes (e.g., premature birth, low birth weight).
The best way to minimize risks is to choose an experienced dental professional, follow all pre- and post-treatment instructions diligently, and maintain open communication with your dental team.
Comparison Tables
Table 1: Non-Surgical vs. Surgical Gum Disease Treatments
| Feature | Non-Surgical Treatments (e.g., SRP) | Surgical Treatments (e.g., Flap Surgery, Grafts) |
|---|---|---|
| Typical Stage | Gingivitis, Early to Moderate Periodontitis | Moderate to Advanced Periodontitis (deep pockets, significant bone/tissue loss) |
| Primary Goal | Remove plaque/tartar, reduce inflammation, halt disease progression | Reduce pocket depth, regenerate lost bone/tissue, stabilize teeth, improve aesthetics |
| Invasiveness | Low (deep cleaning, local anesthesia) | Moderate to High (incisions, sutures, local/IV sedation) |
| Cost Range (US) | $200 - $2,000 (full mouth SRP) | $500 - $4,000+ (per quadrant/site) |
| Recovery Time | Few days (soreness, sensitivity) | 1-2 weeks for initial healing; several months for complete tissue maturation |
| Effectiveness | Highly effective for early stages; can prevent progression | Effective for advanced cases where non-surgical methods fail; can restore structures |
| Key Advantage | Less invasive, lower cost, quicker recovery | Can address severe damage, regenerate tissues, save teeth previously deemed unsalvageable |
| Key Disadvantage | Not effective for deep pockets or significant bone loss | More invasive, higher cost, longer/more complex recovery, potential for recession |
Table 2: US Cost Comparison for Key Gum Disease Procedures by Region (Estimated Ranges)
| Procedure | Northeast (e.g., NYC, Boston) | Midwest (e.g., Kansas City, Cleveland) | West Coast (e.g., LA, Seattle) | South (e.g., Atlanta, Houston) |
|---|---|---|---|---|
| Routine Cleaning | $120 - $200 | $90 - $150 | $110 - $190 | $80 - $140 |
| SRP (per quadrant) | $350 - $500 | $250 - $350 | $320 - $480 | $220 - $320 |
| Flap Surgery (per q) | $1,200 - $2,000 | $800 - $1,500 | $1,100 - $1,800 | $700 - $1,300 |
| Bone Graft (per site) | $1,500 - $3,000 | $1,000 - $2,000 | $1,400 - $2,800 | $900 - $1,800 |
| Gum Graft (per site) | $1,400 - $2,800 | $900 - $1,800 | $1,300 - $2,500 | $800 - $1,700 |
| Perio Maintenance | $150 - $300 | $110 - $200 | $140 - $280 | $100 - $180 |

Note: These are estimated out-of-pocket ranges and can vary based on individual practice, complexity, and specific materials used.
Children / Pediatric Considerations
While periodontal disease is primarily associated with adults, children and adolescents can also develop gum inflammation and, in rare cases, more severe forms of gum disease. However, the prevalence and typical presentation differ significantly.
- Gingivitis in Children: This is the most common form of gum disease in children and is usually related to inadequate oral hygiene. Symptoms are similar to adults: red, swollen gum, and bleeding. It's often reversible with improved brushing and flossing habits and professional cleaning. The American Dental Association (ADA) emphasizes early education on proper brushing and flossing techniques from a young age.
- Early Periodontal Disease in Adolescents: Some adolescents may develop forms of periodontitis, particularly "Localized Aggressive Periodontitis," which can affect specific permanent molars and incisors. This often has a genetic component and can lead to rapid bone loss.
- Periodontitis Associated with Systemic Conditions: Children with certain systemic diseases (e.g., diabetes, Down syndrome, Papillon-Lefèvre Syndrome) or immune deficiencies are at higher risk for severe and early-onset periodontitis.
- Treatment Approach: Treatment for children typically starts with conservative non-surgical methods like professional cleanings, scaling and root planing, and intensive oral hygiene instruction for both the child and parents. Antibiotics may be used for aggressive forms. Surgical interventions are less common but may be considered in severe, localized cases.
Parents should:
- Ensure their children brush twice daily and floss once daily.
- Take children for regular dental check-ups starting from their first tooth.
- Be vigilant for signs like a swollen gum, bleeding, or persistent bad breath.
- Discuss any concerns with their pediatric dentist, who can assess risk factors and recommend appropriate gum disease treatments or referrals to a periodontist if necessary.
Cost Breakdown: Navigating Affordability
As discussed, the cost of gum disease treatments can be substantial. Understanding the full cost breakdown and available financial options is key.
Average US Costs (Low, Mid, High)
- Mild Gum Disease (Gingivitis): Requires 1-2 professional cleanings: $75 - $400.
- Moderate Gum Disease (Early to Moderate Periodontitis): Requires Scaling and Root Planing for 2-4 quadrants, potentially local antibiotics: $800 - $2,500.
- Severe Gum Disease (Advanced Periodontitis): May require SRP, multiple surgical procedures (flap surgery, bone/gum grafts), and ongoing periodontal maintenance: $3,000 - $10,000+ over the course of treatment, not including potential tooth extractions or implants.
With vs. Without Insurance
- With Insurance: As outlined earlier, insurance typically covers 50-80% of major procedures after deductibles and up to annual maximums (often $1,000-$2,000). For a $2,000 SRP procedure, you might pay $400-$1,000 out-of-pocket, assuming you've met your deductible and haven't maxed out your benefits. For more expensive surgeries, insurance may only cover a fraction of the total cost, leaving several thousands of dollars as patient responsibility.
- Without Insurance: You are responsible for 100% of the cost. This emphasizes the importance of prevention and early intervention to avoid costly advanced gum disease treatments.
Payment Plans and Financing Options
Many dental offices understand the financial burden of extensive dental work and offer solutions:
- In-house Payment Plans: Some practices allow patients to pay for treatments in installments directly to the office, often with no interest.
- Third-Party Medical Financing: Companies like CareCredit or LendingClub offer specialized healthcare credit cards or loans with various interest rates and repayment terms. Some offer interest-free periods if the balance is paid within a certain timeframe.
- Dental Discount Plans: These are not insurance but offer a percentage discount on services from participating dentists for an annual fee. Discounts typically range from 10-60%.
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): If you have an HSA or FSA through your employer, you can use pre-tax dollars to pay for qualified dental expenses, including gum disease treatments.
Cost-Saving Tips
- Early Intervention: Addressing early periodontal disease (gingivitis) with a routine cleaning is far cheaper than treating advanced periodontitis. Don't ignore a swollen gum or bleeding.
- Preventative Care: Consistent brushing, flossing, and regular check-ups prevent the need for expensive treatments down the line.
- Shop Around (with caution): Get second opinions and compare treatment plans and costs from different periodontists or general dentists. However, prioritize expertise and reputation over the lowest price.
- Utilize Insurance Benefits: Understand your plan, use your annual maximums, and get pre-authorizations for major procedures.
- Discuss Options with Your Dentist: Be open about your financial concerns. They may be able to stage treatments or suggest alternative, more affordable options where medically appropriate.
- Dental Schools: Dental schools often offer treatments at a reduced cost, performed by supervised students. This can be a viable option for those with limited financial resources.
Frequently Asked Questions
What is the most common gum disease treatment?
The most common and fundamental gum disease treatment is scaling and root planing (SRP), often referred to as a "deep cleaning." This non-surgical procedure effectively removes plaque and tartar from below the gum line and smooths the tooth roots, helping to halt the progression of early to moderate periodontal disease. It's often the first step before considering more invasive options.

Is gum disease treatment painful?
While scaling and root planing and surgical procedures involve active treatment, they are typically performed under local anesthesia to minimize discomfort. You might feel pressure or vibration, but not sharp pain. After the procedure, some soreness, tenderness, and sensitivity are common, which can usually be managed with over-the-counter pain relievers. Surgical recovery might involve more significant discomfort requiring prescribed medication.
How long does gum disease treatment take?
Non-surgical treatments like scaling and root planing are usually completed in 1 to 4 appointments, depending on the extent of the disease, with each appointment lasting about 1-2 hours. Surgical treatments may involve a single procedure for a specific area, followed by several weeks to months of healing and follow-up visits. The overall duration of your treatment plan, including ongoing maintenance, can span many months or even years to ensure long-term stability.
Can gum disease be cured completely?
Gingivitis, the earliest stage of gum disease, is typically reversible with professional cleaning and diligent home care. However, once it progresses to periodontitis, the damage (especially bone loss) is generally irreversible. While periodontitis cannot be "cured" in the sense of complete restoration, it can be effectively managed and arrested through appropriate gum disease treatments and rigorous long-term maintenance, preventing further progression and preserving your teeth.
What are the alternatives to gum disease surgery?
For early to moderate gum disease, alternatives to surgery include non-surgical methods like scaling and root planing, local or systemic antibiotics, and laser therapy. These are often tried first. However, for advanced periodontitis with deep pockets and significant bone loss, surgery may be the only effective option to save teeth, reduce infection, and prevent further deterioration.
How much does gum disease treatment cost without insurance?
Without insurance, routine cleanings range from $75-$200. Scaling and root planing can cost $800-$2,000 for a full mouth. Surgical procedures like flap surgery, bone grafts, or gum grafts can range from $500 to $4,000+ per site/quadrant. These costs can quickly accumulate for extensive treatment plans, making prevention and early intervention financially advantageous.
Can a swollen gum indicate serious gum disease?
Yes, a persistently swollen gum is a classic symptom of gum inflammation, which can range from mild gingivitis to more serious periodontitis. If the swelling is localized and painful, it could indicate an abscess, which is a sign of acute infection and requires immediate dental attention. Any unexplained or persistent gum swelling should be evaluated by a dentist.
Will my teeth become loose after gum disease treatment?
While gum disease itself causes teeth to become loose due to bone loss, effective gum disease treatments aim to stabilize teeth by reducing inflammation and preventing further bone loss. However, teeth that were already significantly compromised before treatment may remain slightly mobile or, in very advanced cases, may eventually need extraction. Post-treatment sensitivity is more common than immediate loosening.
How effective are non-surgical gum disease treatments for early periodontal disease?
Non-surgical treatments, particularly scaling and root planing, are highly effective for early periodontal disease (gingivitis and mild to moderate periodontitis). They can significantly reduce inflammation, decrease pocket depths, and halt the progression of the disease. Their success heavily relies on the patient's commitment to excellent home oral hygiene and consistent follow-up periodontal maintenance appointments.
How often do I need follow-up appointments after gum disease treatment?
After active gum disease treatments, patients typically enter a phase of "periodontal maintenance." These specialized cleanings and check-ups are usually recommended every 3 to 4 months, rather than the standard twice-a-year cleaning. This frequent monitoring is crucial to prevent the recurrence of gum disease and maintain the results achieved through treatment.
When to See a Dentist
Recognizing when to seek professional dental care for gum-related issues is critical for preserving your oral health and preventing the progression of gum disease.
Routine Care Guidance:
- Regular Check-ups: Everyone should visit their dentist for a comprehensive examination and professional cleaning at least twice a year. These routine visits are essential for early detection of problems like gingivitis before they escalate.
- Signs of Gingivitis: If you occasionally notice a slightly swollen gum, mild bleeding during brushing, or persistent bad breath, schedule a non-emergency appointment soon. These are often signs of early periodontal disease that can be reversed with prompt attention.
Red Flags Needing a Scheduled Appointment Soon (within days to a week):
- Persistent Bleeding: Gums that bleed consistently every time you brush or floss, or bleed spontaneously.
- Chronic Swelling or Redness: Gums that remain red, puffy, or tender for more than a few days, even with improved home care.
- Receding Gums: If you notice your teeth appearing longer or increased sensitivity due to gum recession.
- Persistent Bad Breath: Halitosis that doesn't improve with regular brushing and mouthwash.
- Changes in Bite: If your teeth feel like they're shifting or your bite feels "off."
Emergency vs. Scheduled Appointment Guidance (Needs Immediate Attention, within 24-48 hours):
- Severe Pain: Intense, throbbing pain in your gums or around a tooth, especially if it worsens with chewing or pressure.
- Localized, Rapid Swelling (Abscess): A suddenly very swollen gum area that might have a pus-filled bump on it, accompanied by severe pain, fever, or facial swelling. This could indicate a periodontal abscess, which requires urgent drainage and treatment to prevent serious infection spread.
- Loose or Shifting Teeth with Acute Pain: If a tooth suddenly feels very loose or has significantly shifted, accompanied by pain, it could be a sign of acute infection or trauma to already compromised supporting structures.
Do not ignore symptoms of gum disease. The sooner you seek gum disease treatments, the more effectively and conservatively the condition can be managed, potentially saving your teeth and preventing broader health implications. Your dental team at SmilePedia.net is here to guide you toward optimal oral health.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
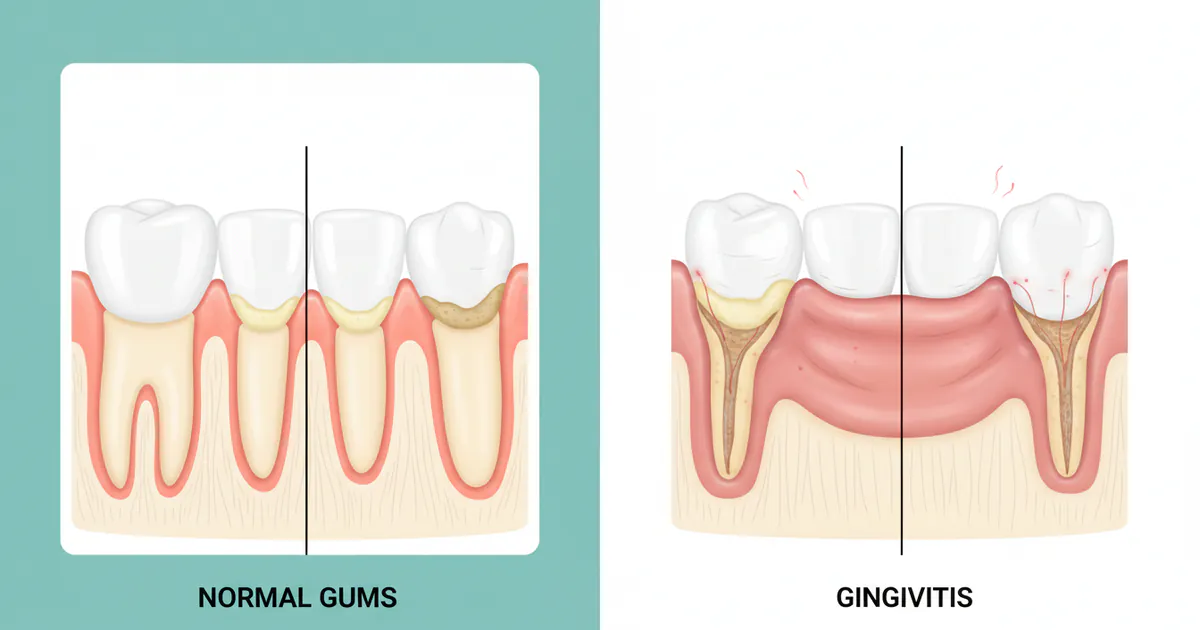
Normal Gums vs Gingivitis: Complete Comparison Guide
Did you know that nearly half of American adults over 30 show signs of gum disease, a condition that can range from mild inflammation to severe infection leading to tooth loss? Understanding the difference between healthy gums and those affected by early gum disease, known as gingivitis, is cruc
February 22, 2026
Can You Get Rid of Gingivitis
More than 50% of American adults aged 30 or older suffer from some form of gum disease, with gingivitis being the earliest and most common stage. This often silent condition, marked by inflammation of the gums, can seem daunting, leading many to wonder: can you get rid of gingivitis? The good ne
February 22, 2026
What Causes Receding Gums
Receding gums, a condition where the gum tissue surrounding the teeth pulls back or wears away, exposing more of the tooth or the tooth's root, affects a significant portion of the adult population in the United States. In fact, estimates suggest that **up to 88% of people over the age of 65 have on
February 22, 2026
Signs of Gingivitis: Complete Guide
Did you know that nearly half of American adults aged 30 and older suffer from some form of gum disease? While that statistic might sound alarming, the good news is that the earliest and most common stage, gingivitis, is entirely reversible. Recognizing the signs of gingivitis early is your
February 22, 2026