What Does Gingivitis Look Like
Key Takeaways
- Gum disease is a silent, often overlooked threat to your oral and overall health. In the United States, an astonishing 47.2% of adults aged 30 years and older have some form of periodontal disease, according to the Centers for Disease Control and Prevention (CDC). Among these, the earliest and m
Gum disease is a silent, often overlooked threat to your oral and overall health. In the United States, an astonishing 47.2% of adults aged 30 years and older have some form of periodontal disease, according to the Centers for Disease Control and Prevention (CDC). Among these, the earliest and most common stage is gingivitis. But what does gingivitis look like, and how can you tell if you're experiencing its subtle — or not so subtle — signs? Recognizing the visual cues of gingivitis is the first critical step toward prevention and effective treatment, protecting your smile and preventing more severe complications.
This comprehensive guide from SmilePedia.net will dive deep into the visual and symptomatic presentation of gingivitis, equipping you with the knowledge to identify this common condition. We'll explore its causes, the various treatment avenues available, what to expect during recovery, and crucially, how to prevent it from ever taking root in your mouth. You'll also find detailed information on costs, insurance, and specific considerations for children, ensuring you have a complete picture of gum health.
Key Takeaways:
- Gingivitis is Reversible: Unlike advanced periodontitis, gingivitis can be fully reversed with proper oral hygiene and professional care, typically within 1-2 weeks of consistent treatment.
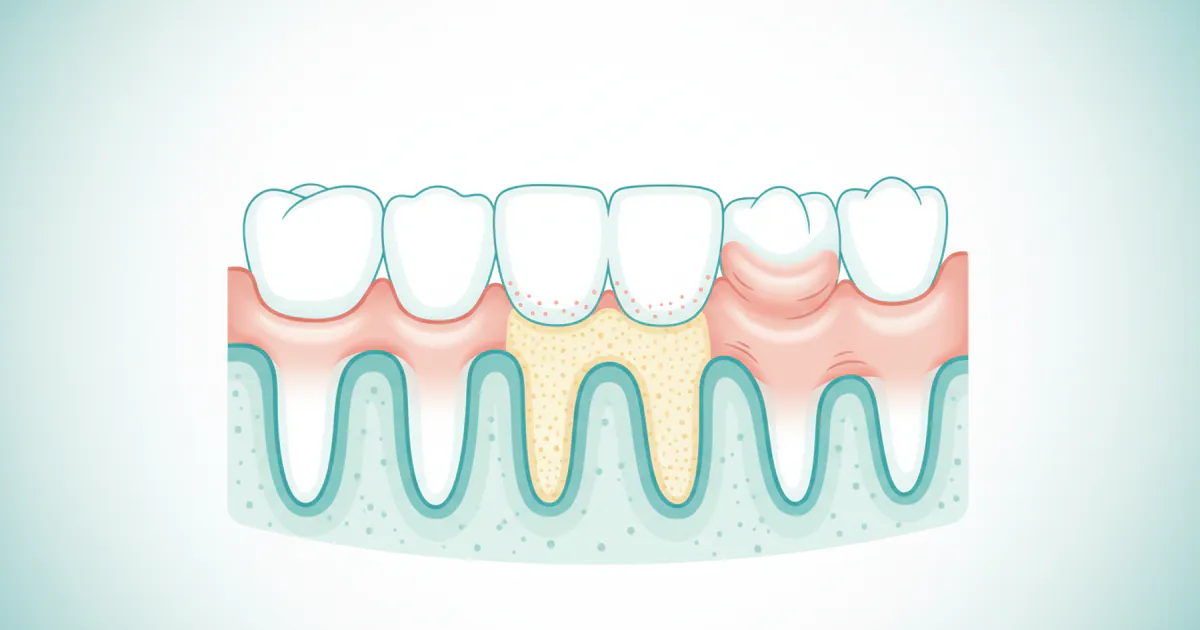
- Appearance is Key: Healthy gums are firm, pink, and don't bleed. Gingivitis manifests as red, swollen, tender, and often bleeding gums.
- Primary Cause: The overwhelming cause is plaque buildup due to inadequate brushing and flossing.
- Professional Cleaning is Essential: A dental cleaning (scaling) costing $75 - $200 (without insurance) is usually the first step to remove plaque and tartar.
- Average Treatment Cost: Initial professional treatment for gingivitis in the US generally ranges from $150 to $500, depending on severity and location.
- Prevention is Simple: Daily brushing (twice), flossing (once), and regular dental check-ups (every six months) are highly effective in preventing gingivitis.
- Don't Delay: Untreated gingivitis can progress to periodontitis, leading to irreversible gum recession and tooth loss, with treatment costs ranging from $500 to $10,000+ for advanced cases.
What Is Gingivitis? An Overview
Gingivitis is the earliest and mildest form of periodontal (gum) disease. It's an inflammatory condition specifically affecting the gingiva, which is the part of the gum surrounding the base of your teeth. Unlike its more severe cousin, periodontitis, gingivitis typically does not involve the loss of bone or connective tissue that holds your teeth in place. This crucial distinction means that gingivitis is fully reversible with diligent oral hygiene and professional dental care.
The condition is incredibly common. Studies suggest that nearly half of all adults over 30 experience some form of gum inflammation. While many might not even realize they have it in its early stages, ignoring gingivitis allows it to progress, potentially leading to much more serious and irreversible dental problems.
Understanding "what does gum disease look like" starts with recognizing gingivitis. It’s characterized by inflammation caused by bacteria in plaque, a sticky film that constantly forms on your teeth. When plaque isn't removed regularly, it hardens into tartar (calculus), which provides a rough surface for more plaque to accumulate, further irritating the gums. This bacterial assault triggers an immune response, leading to the tell-tale signs of gingivitis.
Types of Gingivitis
While the most common form of gingivitis is plaque-induced, there are variations depending on the underlying cause.
Plaque-Induced Gingivitis
This is by far the most prevalent type and the focus of most discussions about gingivitis. It is directly caused by the accumulation of bacterial plaque on the teeth, particularly along the gum line. Poor oral hygiene is the primary culprit, leading to inflammation that is usually confined to the gums without affecting the underlying bone.
Non-Plaque Induced Gingival Lesions
These are less common and are not primarily caused by plaque but by specific infections, genetic conditions, systemic conditions, or traumatic lesions. Examples include:
- Specific Bacterial, Viral, or Fungal Infections: Herpes gingivostomatitis, candidiasis.
- Genetic Disorders: Hereditary gingival fibromatosis.
- Systemic Conditions: Pemphigoid, lichen planus, certain blood disorders.
- Allergic Reactions: To dental materials, food, or toothpaste.
- Traumatic Lesions: Chemical, physical, or thermal injuries to the gums.
For the purpose of this article, we will primarily focus on plaque-induced gingivitis, as it accounts for the vast majority of cases and is highly preventable and treatable through routine dental care.
Causes: Why Gingivitis Happens
The fundamental cause of plaque-induced gingivitis is bacterial plaque buildup on the teeth. Plaque is a sticky, colorless film composed of bacteria, food particles, and saliva that constantly forms on your teeth. If plaque is not removed daily through brushing and flossing, it can lead to several problems:
- Plaque Accumulation: Bacteria in plaque produce toxins that irritate the gum tissue, triggering an inflammatory response.
- Tartar (Calculus) Formation: If plaque isn't removed within 24-72 hours, it hardens into tartar, a calcified deposit that can only be removed by a dental professional. Tartar provides a rough surface that allows even more plaque to accumulate, exacerbating the problem.
Beyond plaque, several contributing factors can increase your risk of developing gingivitis or worsen its severity:
- Poor Oral Hygiene: Inadequate or inconsistent brushing and flossing are the leading culprits.
- Smoking or Chewing Tobacco: Tobacco use significantly weakens the immune system, making it harder for gum tissue to fight off infection, and constricts blood vessels, masking the signs of inflammation.
- Hormonal Changes: Fluctuations during pregnancy, puberty, menstruation, or menopause can make gums more sensitive and prone to inflammation. Pregnancy gingivitis, for instance, is very common.
- Certain Medications: Some drugs, such as anticonvulsants, calcium channel blockers, and immunosuppressants, can cause gingival enlargement, making oral hygiene more difficult and increasing inflammation.
- Systemic Diseases: Conditions like diabetes, AIDS, and specific autoimmune disorders can impair the body's immune response, making gums more vulnerable.
- Poor Nutrition: A diet lacking essential vitamins and minerals, particularly Vitamin C, can compromise gum health.
- Crooked Teeth or Poorly Fitting Dental Restorations: These can create areas that are difficult to clean, allowing plaque and tartar to accumulate.
- Dry Mouth (Xerostomia): Saliva helps wash away food particles and neutralize acids. Reduced saliva flow can increase plaque buildup.
- Age: The risk of gum disease increases with age.
- Genetics: Some individuals may have a genetic predisposition to gum disease.
Pro Tip: Be mindful of mouthwashes containing alcohol, as they can sometimes dry out the mouth, potentially exacerbating the issue for some individuals. Opt for alcohol-free therapeutic mouthwashes if recommended by your dentist.
Signs and Symptoms: What Does Gingivitis Look Like?
Recognizing the early signs of gingivitis is paramount to successful treatment and preventing progression to more severe periodontal disease. While some symptoms can be subtle, paying close attention to your gums during your daily oral hygiene routine can make all the difference.
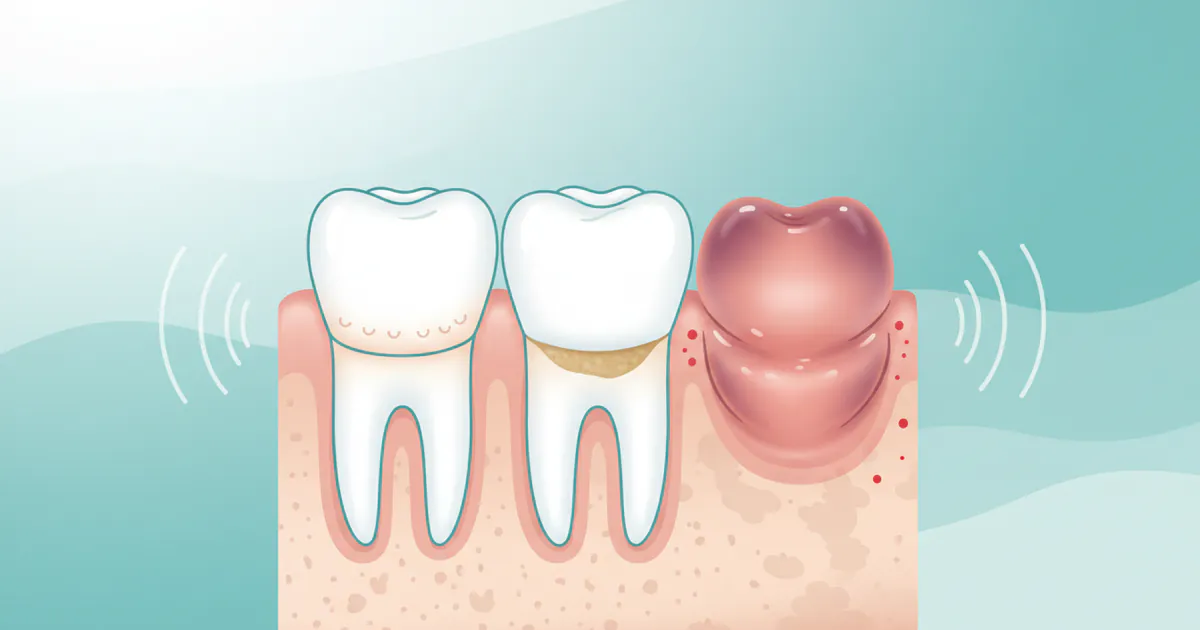
The Appearance of Healthy Gums vs. Gingivitis
To understand what does gingivitis look like, it's helpful to know what healthy gums look like:
- Color: Healthy gums are typically a uniform shade of pink, sometimes a bit darker or lighter depending on your natural complexion. They are not red or purplish.
- Texture: They appear firm and stippled, often described as having an "orange peel" texture.
- Position: Healthy gums fit snugly around the teeth, with the gum line just above the enamel. There are no significant gaps or pockets.
- Bleeding: Healthy gums do not bleed when you brush, floss, or eat.
Now, let's contrast this with the visual and symptomatic signs of gingivitis:
1. Color Change: Redness and Swelling
- Redness: One of the most prominent visual cues of gingivitis is a change in gum color. Instead of healthy pink, gingivitis-affected gums often appear red, dark red, or even purplish-red. This color change is due to increased blood flow to the area as the body's immune system responds to the bacterial infection. The redness is typically most pronounced along the gum line, where the gums meet the teeth.
- Swelling (Edema): The gums will appear swollen, puffy, or engorged. They lose their firm, tight appearance and may look somewhat "pillowy" or "rounded" at the edges, especially between the teeth (papillae). This swelling is caused by inflammation and fluid retention in the gum tissue. You might notice that the normally sharp, knife-edged contour of the gums becomes blunted and inflamed.
2. Bleeding Gums
- Spontaneous Bleeding: This is perhaps the most common and alarming symptom, and often the first sign people notice. Gums affected by gingivitis will bleed easily, often during routine activities like brushing, flossing, or even eating hard foods. Sometimes, slight pressure or even just rinsing with mouthwash can cause bleeding. The amount of bleeding can vary from a faint pink tinge on your toothbrush to more noticeable blood in the sink. This bleeding is a direct result of the inflamed, delicate blood vessels within the gum tissue becoming fragile and rupturing easily.
3. Tenderness and Discomfort
- Tenderness: The inflamed gums can feel tender or sore to the touch. You might experience mild discomfort when brushing or flossing, even if you're being gentle.
- Mild Pain: While gingivitis is generally not acutely painful, some individuals may experience a dull ache or general discomfort in their gums. This pain is usually mild and often overlooked.
4. Bad Breath (Halitosis)
- Persistent Bad Breath: The accumulation of bacteria in plaque and tartar, especially around inflamed gums, can release foul-smelling volatile sulfur compounds. This often leads to persistent bad breath (halitosis) that cannot be resolved with routine brushing or mouthwash alone.
5. Receding Gums (Advanced/Progression)
While gingivitis itself primarily causes inflammation and swelling rather than direct recession, it's crucial to address the target keyword "i healed my receding gums." Untreated gingivitis is the precursor to periodontitis, which is a major cause of gum recession. By effectively treating gingivitis, you prevent its progression to periodontitis, thereby preventing the future development of gum recession. If you already have some degree of recession, it's typically a sign that the condition has advanced beyond simple gingivitis. For existing recession, treatments are more involved than just gingivitis management. However, stopping gingivitis in its tracks is fundamental to maintaining current gum levels and preventing further loss.
``
6. Other Subtle Signs
- Puffy Gums: The gums may appear puffy or "squishy" rather than firm.
- Shiny Appearance: In some cases, the surface of the inflamed gums might look shiny due to the swelling.
- Changes in Gum Contour: The normally scalloped, knife-edge appearance of the gums may become rounded and blunted, especially the interdental papillae (the gum tissue between teeth).
It's important to note that gingivitis can sometimes be asymptomatic, especially in its very early stages. This is why regular dental check-ups are so important – dentists can spot signs you might miss.
Treatment Options
The good news is that gingivitis is highly treatable and reversible. The primary goals of treatment are to remove the source of inflammation (plaque and tartar) and establish a consistent, effective oral hygiene routine.
1. Professional Dental Cleaning (Scaling)
This is the cornerstone of gingivitis treatment. A dental hygienist or dentist will perform a thorough cleaning, often referred to as scaling.
- What it involves: Using specialized instruments (manual scalers and/or ultrasonic devices), the hygienist will remove plaque and tartar from above and below the gum line.
- Benefits: This procedure eliminates the bacterial irritants, allowing the gum tissue to heal.
- Pros: Highly effective, relatively quick, usually not painful (though local anesthetic can be used if needed), prevents progression to periodontitis.
- Cons: Requires a dental visit, may cause temporary sensitivity.
2. Improved At-Home Oral Hygiene
After professional cleaning, consistent at-home care is crucial for maintaining gum health and preventing recurrence.
- Brushing: Brush at least twice a day for two minutes each time, using a soft-bristled toothbrush and fluoride toothpaste. Angle the brush at 45 degrees towards the gum line and use gentle, circular motions. The American Dental Association (ADA) recommends replacing your toothbrush every 3-4 months, or sooner if the bristles are frayed.
- Flossing: Floss daily to remove plaque and food particles from between teeth and under the gum line, areas your toothbrush can't reach. Use a new section of floss for each tooth to avoid reintroducing bacteria.
- Antiseptic Mouthwash: Your dentist may recommend a therapeutic mouthwash containing ingredients like chlorhexidine or essential oils for short-term use to reduce bacterial load. Over-the-counter fluoride rinses can also help strengthen enamel.
3. Addressing Contributing Factors
In some cases, your dentist may recommend addressing other factors:
- Smoking Cessation: Quitting smoking is one of the most impactful steps for gum health.
- Dietary Changes: Reducing sugar intake and ensuring a balanced diet rich in vitamins (especially Vitamin C) can support gum health.
- Correction of Dental Issues: Filling cavities, fixing ill-fitting crowns or bridges, or orthodontics can eliminate areas where plaque can easily accumulate.
- Medication Review: If medication is causing gingival enlargement, your doctor may consult with your dentist to explore alternative options or management strategies.
Step-by-Step Treatment Process
If you visit your dentist suspecting gingivitis, here's a general outline of what to expect:
-
Initial Examination and Diagnosis:
- The dentist or hygienist will perform a thorough oral examination, checking your gums for redness, swelling, and bleeding.
- They will use a periodontal probe to gently measure the depth of the gum pockets around your teeth. Pockets greater than 3mm can indicate gum disease.
- X-rays may be taken to check for any underlying bone loss, which would indicate periodontitis.
- They will discuss your symptoms, medical history, and oral hygiene habits.
-
Professional Cleaning (Scaling):
- Once gingivitis is diagnosed, the primary treatment is usually a professional dental cleaning. This involves:
- Supragingival Scaling: Removal of plaque and tartar from the visible surfaces of the teeth and above the gum line.
- Subgingival Scaling: Careful removal of plaque and tartar from below the gum line, within the gum pockets. This is crucial for healing inflamed tissues.
- The hygienist will use ultrasonic scalers (which vibrate to break up deposits) and/or manual instruments (curettes and sickles) to meticulously clean each tooth surface.
- Polishing will follow to smooth the tooth surfaces, making it harder for plaque to adhere.
- Once gingivitis is diagnosed, the primary treatment is usually a professional dental cleaning. This involves:
-
Oral Hygiene Instruction:
- The dental professional will provide personalized instructions on proper brushing and flossing techniques. This might include demonstrating how to use a specific type of toothbrush, dental floss, interdental brushes, or a water flosser.
- They will emphasize the importance of consistent daily oral care.
-
Follow-Up and Maintenance:
- Depending on the severity, a follow-up appointment might be scheduled to re-evaluate your gum health and ensure proper healing.
- Regular dental check-ups (typically every six months, but sometimes more frequently initially) are essential for ongoing maintenance and early detection of any new inflammation.
Pro Tip: Don't be shy to ask your dental hygienist for a demonstration of proper flossing technique. Many people struggle with it, and a quick lesson can make a huge difference in your gum health.
Cost and Insurance
Understanding the financial aspect of dental care is crucial. Costs for gingivitis treatment can vary based on the severity of the condition, your geographic location, and whether you have dental insurance.
Average US Costs (Without Insurance)
- Routine Dental Exam: $50 - $150
- Dental X-rays (full mouth/panoramic): $50 - $250
- Professional Cleaning (Prophylaxis/Scaling): $75 - $200 (for a standard cleaning, which is usually sufficient for gingivitis)
- Fluoride Treatment: $25 - $50
- Antiseptic Mouthwash Prescription: $10 - $30 (for the medication itself)
Total initial treatment for mild to moderate gingivitis, including an exam, X-rays, and cleaning, typically ranges from $150 to $500 without insurance. More complex cases requiring multiple visits or specialized cleaning might push this higher.
Insurance Coverage
Most dental insurance plans in the US categorize gingivitis treatment as a preventive or basic service.
- Preventive Services (e.g., exams, cleanings, X-rays): Often covered at 80-100% by most plans, especially if you stick to the recommended two cleanings per year. Many plans have no deductible for these services.
- Basic Services (e.g., more frequent cleanings if prescribed, fluoride): May be covered at 70-80% after a deductible is met.
It's vital to:
- Check your specific plan: Review your Explanation of Benefits (EOB) or contact your insurance provider directly to understand your coverage details, annual maximums, and deductibles.
- In-network vs. Out-of-network: Costs can be significantly lower if you choose a dentist within your insurance network.
- Waiting periods: Some plans have waiting periods for certain services, meaning you might have to wait a few months after enrolling before full benefits kick in.
Payment Plans and Financing Options
If you don't have insurance or face significant out-of-pocket costs, consider these options:
- Payment Plans: Many dental offices offer in-house payment plans, allowing you to pay for services over several months.
- Dental Discount Plans: These are not insurance but offer reduced rates on dental services from participating providers for an annual fee.
- Health Savings Accounts (HSAs) or Flexible Spending Accounts (FSAs): If you have one of these through your employer, you can use pre-tax dollars to pay for dental expenses.
- CareCredit or similar medical credit cards: These offer special financing options, often with deferred interest if paid within a certain period.
- Dental Schools: University dental schools often provide services at a reduced cost, performed by supervised students.
Pro Tip: Don't let cost deter you from seeking treatment. Discuss your financial concerns openly with your dental office. They often have solutions or can help you navigate payment options. Early intervention for gingivitis is significantly less expensive than treating advanced periodontitis.
Recovery and Aftercare
Once gingivitis has been treated professionally and you've committed to improved oral hygiene, recovery is typically swift and straightforward.
Immediate Post-Treatment
- Temporary Sensitivity: It's common to experience some temporary tooth sensitivity, especially to hot or cold, after a deep cleaning. This usually subsides within a few days to a week. Using a desensitizing toothpaste can help.
- Gum Tenderness: Your gums might feel a bit tender or sore immediately after the cleaning. Over-the-counter pain relievers like ibuprofen can help manage any discomfort.
- Slight Bleeding: Minor bleeding might occur for a day or two after deep cleaning, but it should quickly resolve.
Long-Term Aftercare
The key to preventing gingivitis from returning and ensuring sustained gum health is unwavering commitment to daily oral hygiene and regular professional check-ups.
- Consistent Brushing: Brush twice a day for two minutes with a soft-bristled brush and fluoride toothpaste. Focus on the gum line.
- Daily Flossing: Floss every day to remove interdental plaque. Consider interdental brushes or a water flosser if you find traditional flossing difficult.
- Regular Dental Check-ups: Schedule professional cleanings and examinations every six months, or as recommended by your dentist. These visits allow your dental team to remove any new plaque and tartar buildup before it causes significant inflammation, and to monitor your gum health.
- Healthy Lifestyle: Maintain a balanced diet, limit sugary foods and drinks, and avoid tobacco products.
- Address Underlying Issues: If your gingivitis was exacerbated by medical conditions or medications, work with your dentist and physician to manage these factors.
Within 1-2 weeks of consistent, improved oral hygiene and professional cleaning, the signs of gingivitis – redness, swelling, and bleeding – should largely resolve, and your gums should return to a healthy, pink, firm state.
Prevention
Preventing gingivitis is far easier and less costly than treating it. The cornerstone of prevention is excellent oral hygiene, supported by regular dental visits and healthy lifestyle choices.
-
Brush Twice a Day:
- Use a soft-bristled toothbrush and fluoride toothpaste.
- Brush for at least two minutes, covering all surfaces of your teeth.
- Angle the brush at 45 degrees towards the gum line to clean effectively where plaque accumulates most.
- Replace your toothbrush every 3-4 months, or sooner if the bristles are frayed.
- Pro Tip: Consider an electric toothbrush; many studies show they can be more effective at removing plaque than manual brushing.
-
Floss Daily:
- Floss at least once a day to remove plaque and food debris from between your teeth and under the gum line, where your toothbrush can't reach.
- Use about 18 inches of floss, winding most of it around your middle fingers, leaving an inch or two to work with.
- Gently glide the floss between your teeth, curving it around each tooth in a "C" shape, and slide it gently beneath the gum line.
-
Regular Dental Check-ups and Cleanings:
- Visit your dentist for professional cleanings and examinations at least every six months, or more frequently if recommended.
- These appointments are vital for removing hardened plaque (tartar) that cannot be removed at home, checking for early signs of gum disease, and addressing any other oral health concerns.
-
Healthy Diet:
- Limit sugary snacks and drinks, which feed plaque bacteria.
- Eat a balanced diet rich in fruits, vegetables, and whole grains, providing essential nutrients for gum health. Vitamin C is particularly important for healthy gum tissue.
-
Avoid Tobacco Products:
- Smoking and chewing tobacco are significant risk factors for gum disease, impairing healing and masking symptoms. Quitting is one of the best things you can do for your oral health.
-
Manage Systemic Health Conditions:
- If you have conditions like diabetes, work with your doctor to manage them effectively, as they can impact your oral health.
By adhering to these preventive measures, you can significantly reduce your risk of developing gingivitis and maintain a healthy, vibrant smile.
Risks and Complications
While gingivitis is reversible, ignoring its symptoms and failing to seek treatment can lead to serious and irreversible consequences. The primary risk of untreated gingivitis is its progression to periodontitis, a more severe form of gum disease.
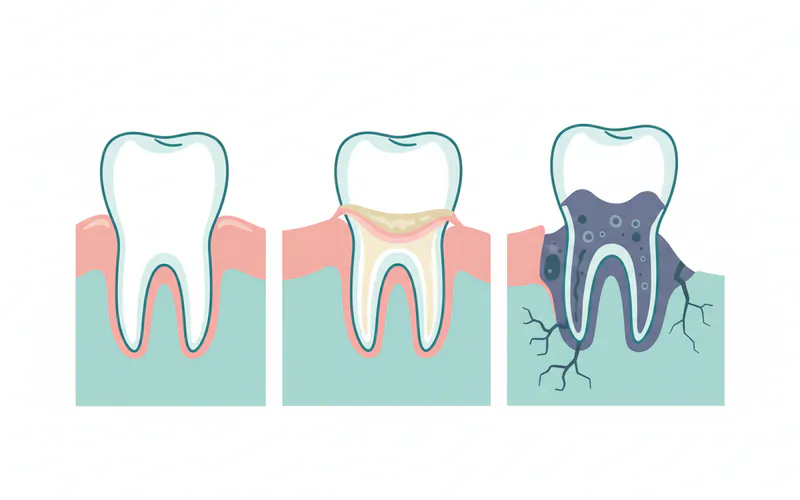
Progression to Periodontitis
- Irreversible Damage: Periodontitis involves the breakdown of the bone and connective tissue that support your teeth. Unlike gingivitis, the damage caused by periodontitis is largely irreversible.
- Pocket Formation: As the disease progresses, the inner layer of the gum and bone pull away from the teeth, forming "pockets." These pockets become deeper and collect more bacteria, plaque, and tartar.
- Bone Loss: The body's immune response to the chronic bacterial infection, combined with the bacterial toxins, begins to destroy the bone and ligaments that anchor the teeth.
- Gum Recession: As the supporting structures are lost, gums may recede, exposing more of the tooth root. This can lead to increased sensitivity and an altered appearance. This is directly related to the keyword "i healed my receding gums" – periodontitis is what causes recession, and treating gingivitis prevents this progression. Once recession occurs, specific periodontal procedures may be needed to address it.
- Loose Teeth and Tooth Loss: Eventually, without adequate bone support, teeth can become loose, shift, and may ultimately need to be extracted or fall out. This is a devastating and costly outcome.
Systemic Health Implications
The impact of untreated gum disease extends beyond the mouth. Research has established links between periodontal disease and various systemic health issues:
- Cardiovascular Disease: The inflammation and bacteria associated with gum disease can enter the bloodstream, potentially contributing to the development of heart disease, stroke, and other cardiovascular problems.
- Diabetes: There's a bidirectional relationship between diabetes and gum disease. Uncontrolled diabetes increases the risk and severity of gum disease, and severe gum disease can make it harder to control blood sugar levels.
- Respiratory Diseases: Oral bacteria can be aspirated into the lungs, potentially leading to respiratory infections like pneumonia.
- Pregnancy Complications: Pregnant women with periodontitis may have an increased risk of premature birth and low birth weight babies.
- Other Conditions: Links have also been suggested with rheumatoid arthritis, certain cancers, and even Alzheimer's disease.
Understanding these risks underscores the importance of prompt diagnosis and treatment of gingivitis. It's not just about your teeth; it's about your overall well-being.
Children / Pediatric Considerations
Gingivitis is not exclusive to adults; children and adolescents can also develop the condition. In fact, studies indicate that a significant percentage of children and teens show some signs of gingivitis, often referred to as pediatric gingivitis.
What Pediatric Gingivitis Looks Like
The signs of gingivitis in children are very similar to those in adults:
- Red, swollen, or puffy gums.
- Gums that bleed easily when brushing or flossing.
- Bad breath that persists despite brushing.
- Tenderness or discomfort in the gums.
Common Causes in Children
- Inadequate Oral Hygiene: The most common cause, just like in adults. Children may not brush or floss effectively or consistently.
- Diet: A diet high in sugary snacks and drinks increases plaque formation.
- Orthodontic Appliances: Braces, retainers, and other orthodontic devices can make it challenging to clean teeth effectively, trapping food and plaque.
- Tooth Eruption: During the eruption of permanent teeth, the surrounding gum tissue can become temporarily inflamed and tender.
- Mouth Breathing: Chronic mouth breathing can dry out the gums, especially in the front of the mouth, making them more susceptible to inflammation.
- Systemic Factors: Less commonly, certain medical conditions (like diabetes) or medications can contribute to gingivitis in children.
Parental Guidance and Prevention
Parents play a critical role in preventing and addressing pediatric gingivitis:
- Supervise Brushing and Flossing: Until around ages 7-8, children typically lack the manual dexterity to brush and floss effectively on their own. Parents should supervise or assist, ensuring they reach all tooth surfaces and the gum line.
- Teach Proper Technique: Educate children on how to brush gently yet thoroughly, and introduce flossing early (as soon as teeth touch each other).
- Regular Dental Check-ups: Take your child to the dentist for regular check-ups and cleanings, typically every six months, starting by their first birthday or when the first tooth erupts. Pediatric dentists are specially trained to handle children's unique dental needs.
- Healthy Habits: Promote a balanced diet and limit sugary treats. Encourage water intake.
- Address Orthodontic Challenges: If your child has braces, ensure they use special tools (like orthodontic toothbrushes, floss threaders, or water flossers) to keep their teeth and gums clean. Regular cleanings are even more important.
Early intervention for gingivitis in children is crucial to prevent it from progressing and impacting the developing permanent dentition.
Cost Breakdown for Gingivitis Treatment
To provide a clearer picture of potential expenses, here's a detailed cost breakdown for gingivitis treatment in the US, considering various scenarios. These are general estimates and can vary significantly by region, specific practice, and individual patient needs.
| Service/Procedure | Low Range (No Insurance) | Mid Range (No Insurance) | High Range (No Insurance) | Insurance Coverage (Typical) |
|---|---|---|---|---|
| Dental Exam (New Patient) | $50 | $100 | $150 | 80-100% |
| Full Mouth X-rays | $75 | $150 | $250 | 80-100% |
| Professional Cleaning (Prophylaxis) | $75 | $120 | $200 | 80-100% |
| Total for Initial Visit (Exam, X-rays, Cleaning) | $200 | $370 | $600 | $0 - $100 out-of-pocket |
| Fluoride Treatment | $25 | $40 | $50 | 80-100% |
| Therapeutic Mouthwash (Prescription) | $10 | $20 | $30 | Typically not covered |
| Follow-up Cleaning (if recommended) | $75 | $120 | $200 | 80-100% |
| Annual Maintenance (2 Cleanings/Year) | $150 | $240 | $400 | $0 - $50 out-of-pocket |
Note: These ranges represent typical costs for plaque-induced gingivitis. If the condition has progressed to early periodontitis requiring scaling and root planing (deep cleaning), costs would be significantly higher, often $200-$500 per quadrant of the mouth.
Cost-Saving Tips
- Preventive Care: The absolute best way to save money is to prevent gingivitis from developing in the first place through diligent daily oral hygiene.
- Regular Check-ups: Don't skip your semi-annual cleanings. They are crucial for catching issues early when they are easier and cheaper to treat.
- Utilize Insurance: Understand your dental insurance plan and maximize its benefits, especially for preventive services.
- Flexible Spending/Health Savings Accounts: Use pre-tax dollars for dental expenses if available through your employer.
- Payment Plans: Inquire about in-office payment plans to spread out costs.
- Dental Schools: Consider seeking care at accredited dental schools, which often offer reduced fees for quality treatment.
- Community Clinics: Some community dental clinics offer sliding scale fees based on income.
Frequently Asked Questions
What does gingivitis feel like?
Gingivitis typically feels tender, sore, or slightly sensitive to the touch. You might experience a dull ache or discomfort, especially when brushing or flossing. However, many people report little to no pain, making it easy to overlook in its early stages.
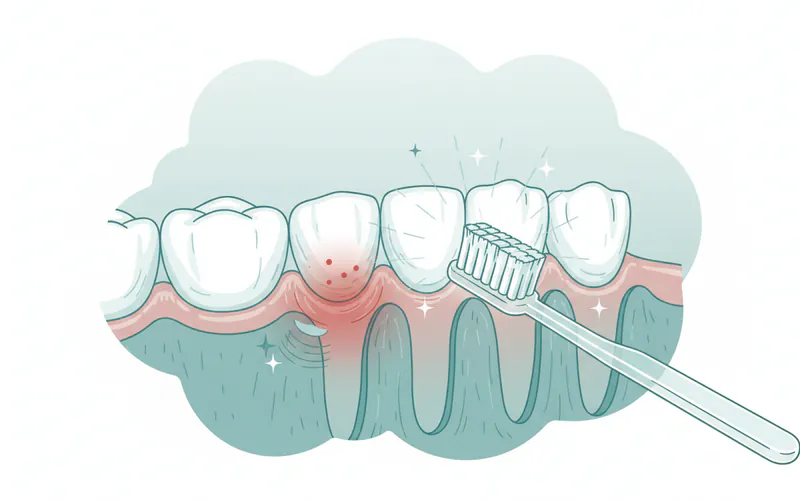
Is gingivitis painful?
Generally, gingivitis is not acutely painful. It's more commonly associated with tenderness, mild discomfort, or a feeling of puffiness in the gums. Significant pain might indicate a more advanced stage of gum disease (periodontitis) or another underlying dental issue, warranting immediate dental attention.
How long does it take to heal gingivitis?
With professional cleaning and consistent, improved oral hygiene, gingivitis can typically heal and reverse within 1 to 2 weeks. The key is diligent brushing twice daily, flossing once daily, and regular dental check-ups to prevent recurrence.
Can gingivitis go away on its own?
No, gingivitis usually does not go away on its own. While minor inflammation might temporarily subside, the underlying cause (plaque and tartar buildup) remains and will continue to irritate the gums. Professional cleaning to remove tartar is almost always necessary, followed by consistent at-home care.
What happens if gingivitis is left untreated?
If left untreated, gingivitis will likely progress to periodontitis. This more severe form of gum disease leads to irreversible damage, including gum recession, bone loss, deepening pockets around the teeth, and eventually, loosening and possible loss of teeth. It also carries systemic health risks.
Can flossing make gingivitis worse initially?
When you first start flossing regularly with gingivitis, your gums might bleed more than usual. This is a sign of inflammation and is normal. Continue flossing gently but thoroughly; consistent flossing helps remove plaque and allows the gums to heal, eventually reducing bleeding.
Are there home remedies for gingivitis?
While good oral hygiene (brushing and flossing) is the most effective "home remedy," other measures like rinsing with saltwater or specific therapeutic mouthwashes (as recommended by a dentist) can help reduce inflammation and kill bacteria. However, these are supplementary and cannot replace professional cleaning to remove tartar.
How often should I see the dentist if I have gingivitis?
Initially, your dentist might recommend a follow-up visit sooner than the standard six months, perhaps in 3-4 months, to ensure your gums are healing properly. Once your gums are healthy, you should adhere to the ADA-recommended schedule of at least twice a year for check-ups and cleanings.
Is bad breath always a sign of gingivitis?
Bad breath (halitosis) can be a symptom of gingivitis, caused by bacteria accumulating in plaque and around inflamed gums. However, bad breath can also stem from other sources like food, dry mouth, other oral infections, or even systemic health conditions. If bad breath persists, a dental visit is recommended to determine the cause.
What is the difference between gingivitis and periodontitis?
Gingivitis is the early, mildest, and reversible stage of gum disease, characterized by inflamed, bleeding gums without bone loss. Periodontitis is a more advanced and irreversible stage where the inflammation has spread to the bone and connective tissues supporting the teeth, leading to bone loss, gum recession, and potentially tooth loss.
When to See a Dentist
Recognizing the signs of gingivitis is crucial, but knowing when to seek professional help is even more important. While gingivitis is manageable, self-diagnosis and delayed treatment can lead to significant complications.
Red Flags That Need Immediate Attention:
- Persistent Bleeding Gums: If your gums bleed consistently every time you brush or floss, or if they bleed spontaneously without provocation, it's a strong indicator of gingivitis that needs professional attention.
- Significant Gum Swelling and Redness: Gums that are markedly swollen, puffy, bright red, or purplish, and feel tender, are clear signs of active inflammation.
- Persistent Bad Breath or Bad Taste: If you have chronic bad breath or a persistent foul taste in your mouth that doesn't resolve with good oral hygiene, it could indicate a bacterial infection in your gums.
- Receding Gums or Visible Pockets: If you notice your gums pulling away from your teeth, making your teeth appear longer, or if there are visible gaps or pockets between your teeth and gums, this suggests that the condition may have progressed beyond simple gingivitis to periodontitis, which requires urgent care.
- Loose Teeth: This is a late-stage symptom of periodontitis and indicates significant bone loss. If you feel any teeth wiggling, see a dentist immediately.
- Pain or Pus: While gingivitis is generally not painful, if you experience significant pain, throbbing, or notice pus oozing from your gums, it could signal an abscess or advanced infection requiring immediate intervention.
Routine Care vs. Emergency Guidance:
- Scheduled Appointment: For mild symptoms like occasional bleeding, slight redness, or tenderness, a prompt, scheduled appointment with your dentist is appropriate. The goal is early diagnosis and treatment before the condition worsens.
- Emergency Appointment (or within 24-48 hours): If you experience severe pain, pus, significant swelling that makes eating or speaking difficult, or suddenly loose teeth, this constitutes a dental emergency. Contact your dentist's office immediately or visit an urgent dental care clinic.
Remember, dental professionals are trained to identify the subtle nuances of gum health. Even if you're unsure what does gingivitis look like in your mouth, a quick check-up can provide clarity and peace of mind. Early detection and treatment of gingivitis can save you from discomfort, extensive procedures, and significant costs down the line, ensuring your smile remains healthy and strong.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
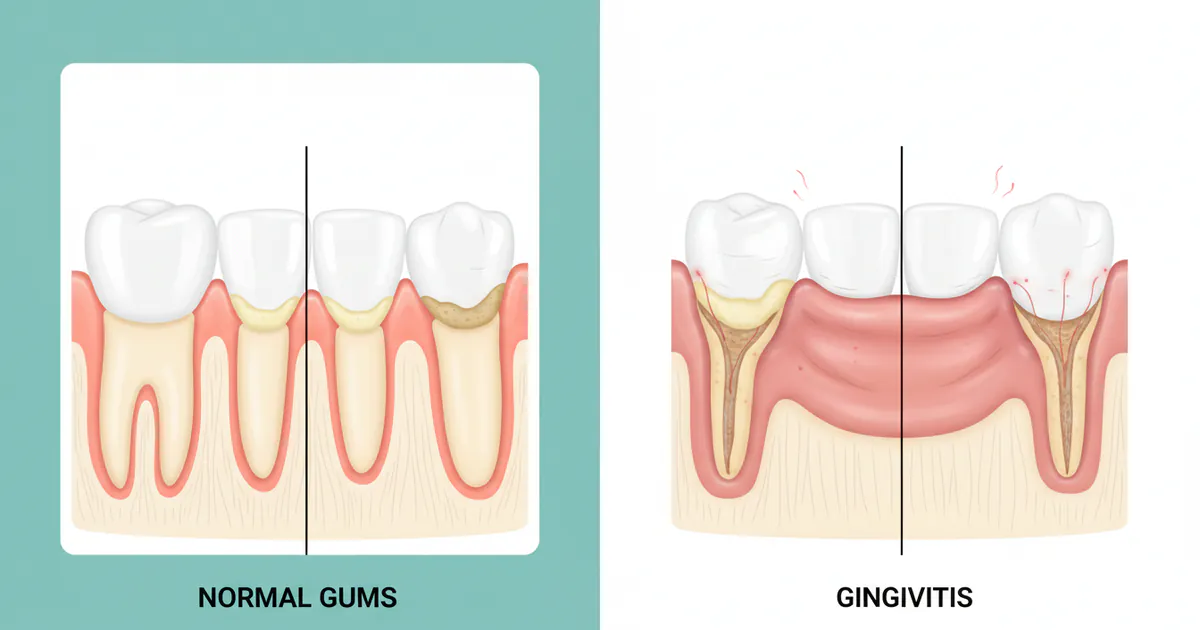
Normal Gums vs Gingivitis: Complete Comparison Guide
Did you know that nearly half of American adults over 30 show signs of gum disease, a condition that can range from mild inflammation to severe infection leading to tooth loss? Understanding the difference between healthy gums and those affected by early gum disease, known as gingivitis, is cruc
February 22, 2026
Can You Get Rid of Gingivitis
More than 50% of American adults aged 30 or older suffer from some form of gum disease, with gingivitis being the earliest and most common stage. This often silent condition, marked by inflammation of the gums, can seem daunting, leading many to wonder: can you get rid of gingivitis? The good ne
February 22, 2026
What Causes Receding Gums
Receding gums, a condition where the gum tissue surrounding the teeth pulls back or wears away, exposing more of the tooth or the tooth's root, affects a significant portion of the adult population in the United States. In fact, estimates suggest that **up to 88% of people over the age of 65 have on
February 22, 2026
Signs of Gingivitis: Complete Guide
Did you know that nearly half of American adults aged 30 and older suffer from some form of gum disease? While that statistic might sound alarming, the good news is that the earliest and most common stage, gingivitis, is entirely reversible. Recognizing the signs of gingivitis early is your
February 22, 2026