Canker Sore on Gum: Complete Guide
Key Takeaways
- A canker sore on gum tissue can be an incredibly painful and disruptive oral lesion, affecting daily activities like eating, speaking, and even smiling. While many people experience canker sores (aphthous ulcers) throughout their lives, their appearance directly on the sensitive gum line or attached
A canker sore on gum tissue can be an incredibly painful and disruptive oral lesion, affecting daily activities like eating, speaking, and even smiling. While many people experience canker sores (aphthous ulcers) throughout their lives, their appearance directly on the sensitive gum line or attached gingiva can be particularly bothersome. In fact, approximately 1 in 5 Americans will experience recurrent aphthous stomatitis, the medical term for canker sores, at some point, making this a prevalent oral health concern.
Understanding what causes these unwelcome guests, how to effectively treat them, and most importantly, how to prevent their recurrence, is crucial for maintaining good oral health and comfort. This comprehensive guide from SmilePedia.net will delve into every aspect of canker sores on the gum, from their underlying causes and various types to cutting-edge treatment options, cost considerations, and essential preventive strategies. We'll also clarify the distinctions between a canker sore on gum tissue and other oral lesions, such as cold sore inside mouth manifestations or ulcers related to hand foot and mouth disease in adults, ensuring you have all the information needed to confidently manage and overcome this common oral challenge.
Key Takeaways:
- Canker sores (aphthous ulcers) on the gum are painful, non-contagious oral lesions, distinct from cold sores.
- They typically heal within 1-3 weeks for minor types, but major or herpetiform ulcers can take longer.
- Common triggers include oral trauma, stress, nutritional deficiencies (iron, B12, folate), certain foods, and genetics.
- Treatment focuses on pain relief, accelerating healing, and preventing recurrence, ranging from OTC remedies (e.g., Kanka, Orajel, costs $5-$20) to prescription medications (e.g., corticosteroids, costs $10-$50 for generic) and professional laser therapy (costs $75-$250 per session).
- Prevention involves avoiding triggers, maintaining good oral hygiene, and addressing any underlying nutritional deficiencies or systemic issues.
- Persistent, unusually large, or frequently recurring canker sores warrant a dental visit to rule out other conditions and discuss advanced management.
- Insurance coverage for canker sore treatment is often limited to diagnostic visits, with specific treatment costs typically out-of-pocket.
What It Is / Overview
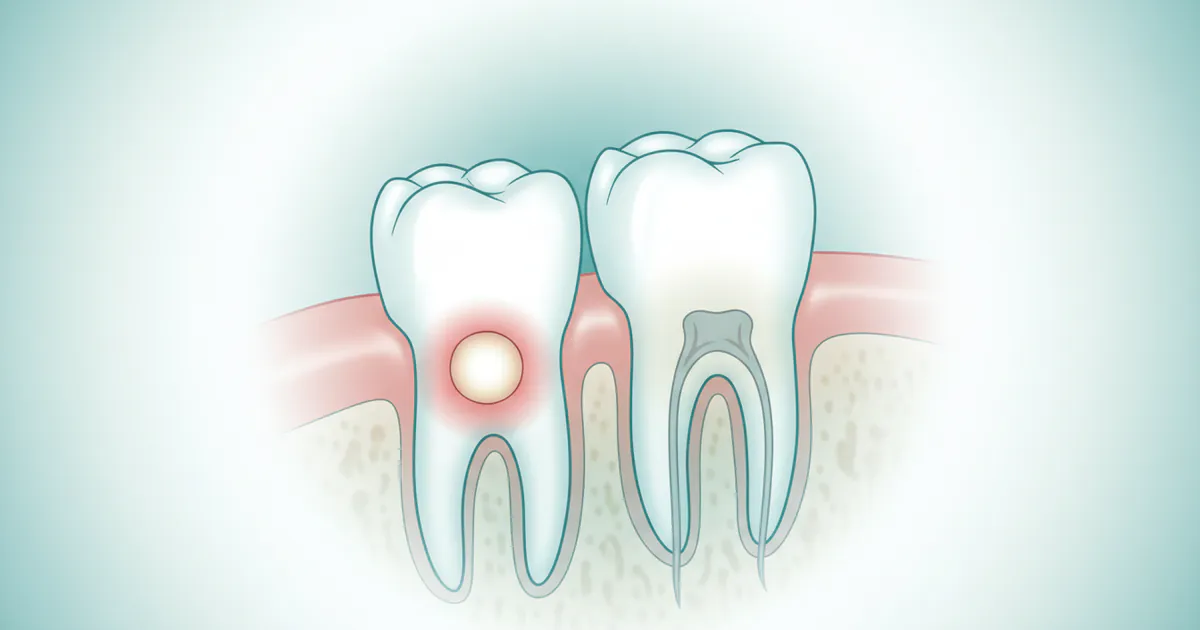
A canker sore on gum refers to an aphthous ulcer that forms specifically on the gingival tissue, which is the soft tissue surrounding your teeth. These ulcers are characterized by a painful, round or oval lesion with a white, yellowish-gray center and a distinct red border. Unlike cold sores, which are caused by the herpes simplex virus and typically appear outside the mouth on the lips or around the nose, canker sores are not contagious and are not caused by a virus. They are a type of inflammatory lesion that can occur anywhere in the mouth, but when they develop on the sensitive gum line or attached gingiva, they can be particularly uncomfortable due to the constant movement during eating and speaking.

Medically known as recurrent aphthous stomatitis (RAS), canker sores are among the most common oral mucosal diseases. While the exact cause remains elusive, they are believed to result from a complex interplay of genetic predisposition, immune system dysfunction, and environmental triggers. They can range in size from tiny pinpricks to over a centimeter in diameter and typically heal on their own, but their presence on the gum can significantly impair quality of life during their active phase.
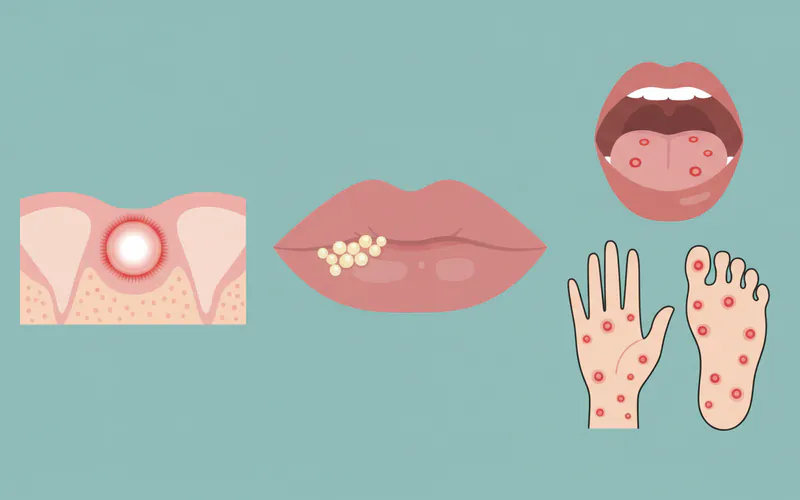
Understanding the Difference: Canker Sore vs. Cold Sore vs. Hand, Foot, and Mouth Disease
It's crucial to differentiate a canker sore on gum from other oral lesions that might appear similar:
-
Canker Sore (Aphthous Ulcer):
- Location: Inside the mouth, on soft, non-keratinized tissues like gums, inner cheeks, lips, tongue, or soft palate.
- Appearance: White or yellowish-gray center with a red halo.
- Contagion: Not contagious.
- Cause: Not viral; linked to immune response, trauma, stress, nutrition.
- Pain: Often very painful.
-
Cold Sore (Herpes Labialis/Oral Herpes):
- Location: Outside the mouth, typically on the lips, around the mouth, or on keratinized tissue like the hard palate or attached gingiva. Less commonly, they can occur inside the mouth, but usually on fixed tissue. If you suspect a cold sore inside mouth, it's important to differentiate its presentation from a canker sore. Cold sores inside the mouth often appear as small, clustered blisters that break open to form ulcers, whereas canker sores are typically solitary or a few distinct ulcers without an initial blister phase.
- Appearance: Starts as small, fluid-filled blisters that then burst, crust over, and heal.
- Contagion: Highly contagious, caused by herpes simplex virus (HSV-1).
- Cause: Viral infection.
- Pain: Painful, tingly, or itchy sensation often precedes appearance.
-
Hand, Foot, and Mouth Disease (HFMD):
- Location: Oral lesions typically appear on the tongue, cheeks, and palate, but can also extend to the gums. Characteristic rashes appear on the palms of the hands and soles of the feet, and sometimes buttocks.
- Appearance: Small, red spots that blister and then ulcerate. Often accompanied by fever and malaise.
- Contagion: Highly contagious, caused by coxsackieviruses.
- Cause: Viral infection.
- Pain: Oral lesions are very painful.
- Note on Adults: While common in children, hand foot and mouth disease in adults can occur and often presents with more severe symptoms, including significant oral pain. The presence of lesions on hands and feet is key to distinguishing it from a canker sore.
Types / Variations
Canker sores, including those that appear on the gum, are generally categorized into three main types based on their size, number, and duration:
1. Minor Aphthous Ulcers (MiAU)
- Prevalence: Account for 80-85% of all canker sores.
- Size: Small, typically less than 1 centimeter in diameter (3-10 mm).
- Appearance: Oval or round with a well-defined red border and a yellowish-gray center.
- Location: Can appear anywhere in the mouth, including on the gums.
- Duration: Heal spontaneously within 1 to 2 weeks without scarring.
- Pain Level: Mild to moderate pain.
2. Major Aphthous Ulcers (MaAU)
- Prevalence: Less common, accounting for about 10% of cases.
- Size: Larger, usually greater than 1 centimeter in diameter (10 mm or more).
- Appearance: Deeper, irregular borders, and often more painful.
- Location: Can occur on the gums, soft palate, tonsils, or pharynx.
- Duration: Can take 2 to 6 weeks or even longer to heal and may leave scars.
- Pain Level: Severe pain, significantly impacting eating and speaking.
3. Herpetiform Aphthous Ulcers (HAU)
- Prevalence: The least common type, making up about 5-10% of cases.
- Appearance: Characterized by multiple (10-100 or more) small, pinpoint ulcers (1-3 mm in diameter) that often cluster together, resembling herpes lesions (hence "herpetiform"). However, they are NOT caused by the herpes virus.
- Location: Can appear anywhere in the mouth, including extensively on the gums.
- Duration: Heal within 1 to 3 weeks, often without scarring.
- Pain Level: Can be extremely painful due to the sheer number of lesions.
Pro Tip: While herpetiform canker sores might look like a cold sore inside mouth due to their clustered appearance, remember the key difference: cold sores are preceded by blisters and are contagious. Canker sores are not. If unsure, always consult your dentist.
Causes / Why It Happens
The exact cause of canker sores, particularly a canker sore on gum, remains complex and multifactorial. However, a combination of genetic predisposition, immune system irregularities, and various environmental triggers is widely accepted. Here's a breakdown of common contributing factors:
1. Oral Trauma and Injury
- Mechanical Irritation: This is a very common trigger for a canker sore on gum. Accidental biting of the cheek or lip, aggressive tooth brushing, sharp edges from broken teeth, ill-fitting dentures, or even irritation from dental braces can damage the delicate gum tissue, leading to an ulcer.
- Chemical Irritation: Certain ingredients in oral hygiene products, particularly sodium lauryl sulfate (SLS), a foaming agent found in many toothpastes and mouthwashes, can irritate oral tissues and contribute to canker sore development in susceptible individuals.
2. Nutritional Deficiencies
- Key Deficiencies: A lack of essential vitamins and minerals has been strongly linked to canker sore formation. These include:
- Iron: Crucial for oxygen transport and cell growth.
- Vitamin B12 (Cobalamin): Important for nerve function and red blood cell production.
- Folate (Folic Acid): Essential for DNA synthesis and cell division.
- Zinc: Plays a vital role in immune function and wound healing.
- Impact: These deficiencies can impair the body's ability to maintain healthy mucosal tissue and mount an appropriate immune response, making individuals more prone to ulcers.
3. Stress and Emotional Factors
- Physiological Impact: Periods of high psychological stress, anxiety, or emotional distress are frequently cited by patients as triggers for canker sore outbreaks. Stress can alter the immune system, potentially leading to an exaggerated inflammatory response in the mouth.
- Anecdotal Evidence: While the exact mechanism is not fully understood, the link between stress and canker sores is widely recognized clinically and anecdotally.
4. Food Sensitivities and Allergies
- Acidic Foods: Highly acidic foods and beverages like citrus fruits (oranges, lemons), tomatoes, pineapples, and some spicy foods can irritate the oral mucosa and trigger canker sores in sensitive individuals.
- Food Allergens: Less commonly, specific food allergies or sensitivities to ingredients like chocolate, coffee, cheese, nuts, or highly processed foods might precipitate outbreaks.
5. Hormonal Fluctuations
- Menstrual Cycle: Some women report a correlation between canker sore outbreaks and their menstrual cycle, with lesions appearing more frequently during certain phases.
- Pregnancy/Menopause: Hormonal shifts during pregnancy or menopause can also influence oral health and potentially contribute to canker sore development, though this link is less consistent.
6. Genetic Predisposition
- Familial Tendency: There is a clear genetic component to recurrent aphthous stomatitis. If one or both parents have a history of canker sores, their children are significantly more likely to develop them, suggesting an inherited susceptibility.
7. Systemic Diseases and Underlying Health Conditions
- Immune System Disorders: Conditions that affect the immune system can increase susceptibility. These include:
- Autoimmune diseases: Such as lupus, inflammatory bowel diseases (Crohn's disease, ulcerative colitis), and Behçet's disease.
- Immunodeficiency states: Like HIV/AIDS.
- Other Conditions: Celiac disease (an autoimmune reaction to gluten) and certain gastrointestinal disorders can also be associated with recurrent oral ulcers.
- Viral Infections: While canker sores themselves are not viral, some viral infections can weaken the immune system or cause general inflammation that might indirectly trigger an outbreak. For instance, while distinct, severe cases of hand foot and mouth disease in adults might involve extensive oral lesions that could be confused with multiple canker sores.
8. Medications
- Side Effects: Certain medications, including some non-steroidal anti-inflammatory drugs (NSAIDs), beta-blockers, and chemotherapy agents, can sometimes list oral ulcers as a side effect.
Understanding these varied causes is essential for effective management and prevention, often requiring a multi-pronged approach tailored to the individual.
Signs and Symptoms
Identifying a canker sore on gum usually isn't difficult due to the distinctive pain and appearance. Here's what to look for:
Initial Signs (Prodromal Stage)
- Tingling or Burning Sensation: Many individuals report a localized tingling, burning, or pricking sensation on the gum tissue a day or two before the ulcer becomes visible.
- Tenderness: The area may feel tender or slightly swollen even before any visible lesion appears.
Visible Signs and Symptoms
- Painful Sore: The most prominent symptom is localized pain, which can range from mild discomfort to severe, sharp pain, especially when eating, drinking, speaking, or brushing teeth. The pain is often disproportionate to the size of the lesion.
- Round or Oval Lesion: A distinct round or oval-shaped ulcer appears on the gum.
- White or Yellowish-Gray Center: The center of the sore will typically be covered by a white or yellowish-gray membrane, which is a fibrin clot protecting the underlying tissue.
- Red Border (Halo): The ulcer is surrounded by a noticeable red, inflamed border or "halo."
- Location: Specifically on the soft tissues of the gums, which can be the attached gingiva (firm tissue around teeth) or the unattached alveolar mucosa (looser tissue towards the cheek/lip).
- Swelling: The immediate area around the sore might appear slightly swollen.
- Difficulty Eating/Speaking: Due to pain, you might find it difficult or uncomfortable to chew, swallow, or speak clearly.
- Irritation: Certain foods (acidic, spicy, salty) or even hot liquids can exacerbate the pain.
Less Common or Accompanying Symptoms (Especially with Major/Herpetiform or Systemic Involvement)
- Fever: While rare for minor canker sores, a low-grade fever might accompany more severe outbreaks (major or herpetiform aphthae) or indicate an underlying systemic condition.
- Swollen Lymph Nodes: Lymph nodes in the neck might become tender and swollen as a response to the inflammation.
- General Malaise: Feeling unwell or fatigued can occur, particularly with severe or numerous lesions.
- Difficulty Swallowing (Dysphagia): If the canker sore is very large or multiple lesions are present near the throat, swallowing can become painful and difficult.
Pro Tip: If you experience frequent or unusually severe oral sores accompanied by symptoms like fever, skin rashes, joint pain, or gastrointestinal issues, it's crucial to consult a healthcare professional. These could be signs of an underlying systemic condition that requires medical attention. Remember that conditions like hand foot and mouth disease in adults will present with oral ulcers AND characteristic skin lesions on hands and feet.
Treatment Options
Treating a canker sore on gum primarily focuses on relieving pain, reducing inflammation, promoting faster healing, and preventing recurrence. While most minor canker sores heal on their own, treatments can significantly improve comfort.
1. Over-the-Counter (OTC) Remedies
These are readily available and often the first line of defense for minor canker sores.
- Topical Anesthetics:
- Products: Benzocaine-containing gels (e.g., Orajel, Kanka), lidocaine gels.
- Mechanism: Numb the area temporarily to reduce pain.
- Pros: Quick pain relief, easy to apply.
- Cons: Short-acting, can sting initially, some people are sensitive to benzocaine.
- Cost: $5-$20
- Protective Pastes/Gels:
- Products: Orabase, Zilactin-B, Canker-X.
- Mechanism: Form a protective barrier over the sore, shielding it from irritation and promoting healing.
- Pros: Provides a physical barrier, can reduce irritation.
- Cons: Can be difficult to keep in place, especially on mobile gum tissue.
- Cost: $10-$25
- Antiseptic Rinses:
- Products: Chlorhexidine gluconate (e.g., Peridex - prescription strength, but weaker OTC versions exist), diluted hydrogen peroxide, saline rinse.
- Mechanism: Help keep the area clean, reduce bacterial load, and prevent secondary infection.
- Pros: Good for overall oral hygiene during an outbreak.
- Cons: Can sometimes sting, chlorhexidine can stain teeth with prolonged use.
- Cost: $5-$15 for OTC, $15-$30 for prescription strength.
- Debriding Agents:
- Products: Gly-Oxide.
- Mechanism: Help clean and debride the ulcer, promoting healing.
- Pros: Aids in cleaning.
- Cons: Specific usage instructions, may not be suitable for all.
- Cost: $8-$15
2. Prescription Medications
For more severe, persistent, or frequent canker sores, a dentist or doctor may prescribe stronger medications.
- Topical Corticosteroids:
- Products: Fluocinonide gel (e.g., Lidex), triamcinolone acetonide dental paste (e.g., Oracort E), clobetasol gel.
- Mechanism: Reduce inflammation and pain, speed up healing.
- Pros: Highly effective for reducing inflammation and discomfort.
- Cons: Requires prescription, potential for localized side effects (e.g., fungal infection) with prolonged use, should be applied carefully to the sore.
- Cost: $10-$50 for generic, higher for brand names.
- Systemic Medications (for severe, recurrent cases):
- Products: Oral corticosteroids (e.g., Prednisone), colchicine, thalidomide (rare, for severe refractory cases), immunosuppressants.
- Mechanism: Reduce widespread inflammation or modulate the immune response.
- Pros: Can manage widespread and severe outbreaks.
- Cons: Significant potential for systemic side effects, require careful medical supervision, usually reserved for major or frequently recurring cases unresponsive to other treatments.
- Cost: Varies widely, $20-$200+ depending on medication and dosage.
- Pain Medications:
- Products: Prescription-strength oral analgesics if OTC options are insufficient.
- Mechanism: Manage severe pain.
- Pros: Effective for intense pain.
- Cons: Potential side effects, dependency risk for opioids.
- Cost: Varies.
3. Professional Treatments
These are performed in a dental office.
- Laser Therapy:
- Products: Diode lasers, Nd:YAG lasers.
- Mechanism: A low-level laser is applied directly to the canker sore. It works by reducing pain, decreasing inflammation, and stimulating cell regeneration, often providing immediate relief and accelerating healing.
- Pros: Often provides immediate pain relief, significantly speeds up healing, no anesthesia usually needed, quick procedure.
- Cons: Requires a dental visit and specialized equipment.
- Cost: $75-$250 per session, often not covered by insurance.
- Silver Nitrate Application:
- Mechanism: Cauterizes the ulcer, providing a protective barrier and reducing pain.
- Pros: Can provide instant pain relief by destroying nerve endings at the surface.
- Cons: Can be very painful during application, can cause tissue discoloration, often not preferred due to potential for deeper tissue damage if not applied carefully.
- Cost: Typically included in office visit fee, $50-$150 if a specific charge.
4. Home Remedies and Supportive Care
- Saltwater Rinses: Dissolve 1/2 teaspoon of salt in a glass of warm water and rinse several times a day. Helps to clean the area and promote healing.
- Baking Soda Paste/Rinse: Mix baking soda with a little water to form a paste and apply to the sore, or dissolve in water for a rinse. Helps neutralize acids and reduce inflammation.
- Milk of Magnesia: Dab a small amount onto the sore a few times a day to coat and soothe.
- Ice Chips: Sucking on ice chips can temporarily numb the area and reduce discomfort.
- Dietary Modifications: Avoid acidic, spicy, salty, or abrasive foods that can irritate the sore. Stick to soft, bland foods.
- Nutritional Supplements: If deficiencies are suspected, your dentist or doctor might recommend supplements for iron, vitamin B12, folate, or zinc. Always consult a healthcare professional before starting new supplements.
Comparison of Common Canker Sore Treatments
| Treatment Type | Mechanism | Pros | Cons | Average US Cost (Range) | Healing Time Impact |
|---|---|---|---|---|---|
| Topical Anesthetics | Numb pain receptors | Fast, temporary pain relief, OTC | Short-acting, can sting | $5-$20 | No direct impact |
| Protective Pastes | Barrier against irritation | Protects, allows healing, OTC | Can be difficult to keep on | $10-$25 | Modest acceleration |
| Antiseptic Rinses | Cleans, reduces bacteria | Maintains oral hygiene, OTC/Rx | Can sting, chlorhexidine stains teeth | $5-$30 | Modest acceleration |
| Topical Steroids | Reduces inflammation/pain | Highly effective, Rx | Requires prescription, localized side effects | $10-$50 (generic) | Speeds healing significantly |
| Laser Therapy | Reduces pain, stimulates healing | Often immediate pain relief, fast healing | Requires dental visit, may not be insured | $75-$250/session | Speeds healing significantly |
| Home Remedies | Soothes, cleans, reduces irritation | Inexpensive, readily available | Varies in effectiveness, not for severe cases | Minimal | Modest acceleration |
Step-by-Step Process (What to Expect During Treatment)
If you're dealing with a canker sore on gum, here’s a typical progression of management, from initial self-care to professional intervention:

1. Initial Self-Care (First 1-3 Days)
- Observe and Identify: Confirm it's likely a canker sore (white/gray center, red border, painful, non-blistering, on soft tissue). Rule out other lesions like a cold sore inside mouth or signs of hand foot and mouth disease in adults (e.g., widespread rash).
- Over-the-Counter Application: Apply an OTC topical anesthetic gel (e.g., Orajel, Kanka) directly to the sore using a clean finger or cotton swab. Reapply as directed, typically every 4-6 hours.
- Rinse Regularly: Begin rinsing your mouth with warm salt water (1/2 tsp salt in 8 oz water) or a diluted hydrogen peroxide rinse (equal parts 3% hydrogen peroxide and water) 2-3 times a day. This helps keep the area clean and can soothe.
- Dietary Modifications: Avoid hot, spicy, acidic, or abrasive foods. Opt for soft, bland foods and cool beverages.
- Oral Hygiene: Continue brushing gently, avoiding direct contact with the sore. Use a soft-bristled toothbrush. Consider switching to an SLS-free toothpaste.
2. If Symptoms Persist or Worsen (Day 3-7)
- Consult Your Dentist: If the pain is severe, the sore is unusually large, doesn't show signs of healing, or you experience multiple sores, it's time to schedule a dental appointment.
- Dental Examination: Your dentist will examine the sore, review your medical history, and discuss potential triggers. They may take measurements or photos for comparison.
- Prescription Treatment: Depending on the severity, your dentist may prescribe:
- A stronger topical corticosteroid paste or gel (e.g., triamcinolone, fluocinonide) to reduce inflammation and pain. You'll receive instructions on how to apply this to the specific sore, often after meals and before bed.
- A prescription-strength antiseptic mouthrinse (e.g., chlorhexidine) for enhanced microbial control.
- In-Office Treatment (Optional):
- Laser Therapy: If available, your dentist might recommend a quick laser treatment. You'll wear protective eyewear, and the dentist will use a small handheld laser device to gently treat the sore. This typically takes only a few minutes and often provides immediate pain relief.
- Silver Nitrate: Less common, but if chosen, the dentist will carefully apply silver nitrate to the lesion to cauterize it.
3. Recovery and Healing (Post-Treatment/Ongoing)
- Follow Instructions: Adhere strictly to your dentist's instructions for medication application or rinsing.
- Monitor Healing: Most minor canker sores treated with prescription medication or laser therapy should show significant improvement within a few days and completely heal within 1-2 weeks. Major aphthae may take several weeks.
- Continued Prevention: Once healed, focus on identifying and avoiding your specific triggers. This might include dietary changes, stress management, or switching oral hygiene products.
Pro Tip: Early intervention is key. The sooner you start treatment, especially with prescription medications or laser therapy, the faster you can get relief and speed up the healing process of a canker sore on gum.
Cost and Insurance
Understanding the financial aspect of treating a canker sore on gum is important, as costs can vary significantly based on the severity of the condition, the type of treatment chosen, and your insurance coverage.
Average US Price Ranges
| Treatment Type | Average Cost (Without Insurance) | Average Cost (With Insurance) | Notes |
|---|---|---|---|
| OTC Topical Gels/Pastes | $5 - $25 | Not applicable (OTC) | Widely available, often the first line of defense. |
| OTC Antiseptic Rinses | $5 - $15 | Not applicable (OTC) | Saline rinses are virtually free. |
| Dental Consultation/Exam | $50 - $150 | $20 - $75 (co-pay/deductible) | Essential for diagnosis, especially for recurrent or severe sores. Often covered by basic dental plans. |
| Prescription Topical Steroid | $10 - $50 (generic) | $5 - $20 (co-pay) | Highly effective, often the next step after OTC. Generics are much cheaper. |
| Prescription Antiseptic Rinse | $15 - $30 | $5 - $15 (co-pay) | Chlorhexidine rinse. |
| Laser Treatment (per session) | $75 - $250 | Rarely covered | Often provides immediate relief and faster healing. Considered elective by many insurers. |
| Silver Nitrate Application | $50 - $150 | Sometimes covered | Less common, often included in exam fee if performed. |
| Systemic Medications | $20 - $200+ | $10 - $100+ (co-pay) | For severe, recurrent cases (e.g., oral corticosteroids, colchicine). Varies greatly by drug. |
| Nutritional Supplements | $10 - $40/month | Not covered | If a deficiency is identified (e.g., B12, iron, folate, zinc). |
Insurance Coverage Details (US)
- Dental Insurance:
- Diagnostic Visits: Most dental insurance plans will cover a portion (50-100%) of the cost of a dental exam and consultation (D0120, D0140, D0150) if you visit a dentist for a canker sore on gum. This helps determine the nature of the lesion.
- Prescription Medications: Dental insurance typically does not cover prescription medications. These would fall under your medical insurance pharmacy benefits, if you have them.
- Laser Therapy: This is frequently considered an elective or experimental treatment for aphthous ulcers by dental insurance companies and is rarely covered. You should expect to pay for this out-of-pocket.
- Silver Nitrate: Some plans may cover this if it's coded as a palliative treatment, but it's not universally covered.
- Medical Insurance:
- Prescription Medications: If you have medical insurance with a prescription drug plan, it will likely cover a portion of the cost for prescription topical steroids, antiseptic rinses, or systemic medications, usually after a co-pay or deductible.
- Specialist Referrals: If your dentist determines an underlying systemic condition is causing your canker sores (e.g., Crohn's disease, Behçet's disease) and refers you to a medical specialist, your medical insurance would cover those visits according to your plan.
Payment Plans and Financing Options
- Dental Office Payment Plans: Many dental offices offer in-house payment plans for more expensive treatments, allowing you to pay in installments.
- Third-Party Financing: Options like CareCredit are popular in dental practices. These medical credit cards offer promotional financing options, often with deferred interest if paid in full within a certain period.
- Health Savings Accounts (HSAs) & Flexible Spending Accounts (FSAs): If you have an HSA or FSA through your employer, you can use these tax-advantaged accounts to pay for qualified medical and dental expenses, including prescription medications and professional treatments for canker sores.
Cost-Saving Tips
- Start with OTC: For minor canker sores, try effective and inexpensive OTC remedies first.
- Inquire About Generics: If a prescription is needed, always ask your dentist or pharmacist if a generic version is available, as these are significantly cheaper than brand-name drugs.
- Check Your Insurance: Before any costly treatment like laser therapy, contact both your dental and medical insurance providers to clarify coverage.
- Discuss Options with Your Dentist: Be open about your budget concerns. Your dentist can help you explore the most effective and affordable treatment options for your specific situation.
Recovery and Aftercare
Once a canker sore on gum has been treated, either with home remedies, prescription medications, or professional procedures like laser therapy, focusing on recovery and diligent aftercare is crucial for complete healing and preventing recurrence.
Immediate Aftercare (Post-Treatment)
- Follow Specific Instructions: If you received professional treatment (e.g., laser therapy, silver nitrate application), your dentist will provide specific post-procedure instructions. Adhere to them carefully. Laser therapy often requires no special aftercare beyond continued good oral hygiene, but silver nitrate might require a few days of very soft foods.
- Medication Adherence: If prescribed topical or systemic medications, ensure you use them exactly as directed. Skipping doses or stopping early can hinder healing.
- Gentle Oral Hygiene: Continue to brush your teeth very gently, especially around the healing sore. Use a soft-bristled toothbrush. Avoid harsh brushing techniques that could re-traumatize the area.
- Rinse Regularly: Continue with warm salt water rinses (1/2 teaspoon salt in 8 ounces warm water) several times a day. This helps keep the area clean, reduces bacterial load, and promotes a healthy healing environment. If prescribed an antiseptic rinse, use it as directed.
During Healing (1-3 Weeks)
- Dietary Adjustments: Remain mindful of your diet. Avoid:
- Acidic Foods: Citrus fruits, tomatoes, vinegar.
- Spicy Foods: Hot peppers, strong spices.
- Salty Foods: Chips, pretzels, heavily salted dishes.
- Abrasive Foods: Hard crusts, crispy snacks, nuts.
- Hot Beverages: Very hot coffee or tea can irritate.
- Opt for soft, bland foods like yogurt, mashed potatoes, cooked vegetables, and lean proteins.
- Hydration: Drink plenty of water to keep your mouth moist and aid in overall healing.
- Avoid Irritants: Refrain from using tobacco products (smoking, chewing) and alcohol, as they can severely irritate the healing tissue and delay recovery.
- Stress Management: If stress is a known trigger for your canker sores, practice stress-reducing techniques like meditation, yoga, or deep breathing exercises.
- Monitor Progress: Observe the sore for signs of healing:
- Decreased pain.
- Shrinking size.
- Disappearance of the white/yellowish center, gradually replaced by healthy pink tissue.
- The red border becoming less inflamed.
Long-Term Aftercare and Prevention
- Identify and Avoid Triggers: This is the most crucial aspect of preventing future outbreaks. Keep a "canker sore diary" to note potential triggers (foods, stress levels, products).
- Nutritional Support: If identified deficiencies (iron, B12, folate, zinc) were a cause, continue with prescribed supplements and maintain a balanced diet rich in these nutrients.
- Oral Hygiene Products: If SLS in toothpaste or mouthwash is a suspected trigger, switch to SLS-free alternatives.
- Regular Dental Check-ups: Maintain your routine dental visits. Your dentist can identify potential issues (e.g., sharp tooth edges, ill-fitting appliances) that could cause trauma and predispose you to canker sores.
- Address Underlying Conditions: If systemic diseases (e.g., Crohn's, celiac, Behçet's) are contributing factors, ongoing management of these conditions with your medical doctor is paramount.
Pro Tip: Even after a canker sore on gum has healed, scar tissue may be present, especially with major aphthae. If you notice any unusual changes in your gum tissue or have persistent concerns, always follow up with your dentist.
Prevention
Preventing a canker sore on gum largely involves identifying and managing the triggers specific to you. While complete prevention may not always be possible for those with a strong genetic predisposition, these strategies can significantly reduce the frequency and severity of outbreaks.
1. Minimize Oral Trauma
- Gentle Brushing: Use a soft-bristled toothbrush and brush gently, especially along the gum line. Avoid aggressive scrubbing.
- Dental Appliances: If you wear braces, dentures, or other oral appliances, ensure they fit properly. Your orthodontist or dentist can provide wax or adjust appliances to prevent irritation.
- Avoid Biting: Be mindful when eating to avoid accidentally biting your cheeks, tongue, or gums.
- Sharp Edges: If you have a broken tooth or a sharp filling, see your dentist promptly to smooth it out.
2. Dietary Adjustments
- Avoid Trigger Foods: If you've identified certain foods (acidic fruits, spicy foods, salty snacks, chocolate, coffee, nuts) as triggers, limit or avoid them, especially during periods of stress or when you feel an outbreak might be starting.
- Balanced Diet: Ensure your diet is rich in essential vitamins and minerals, particularly iron, vitamin B12, folate, and zinc. Whole grains, lean meats, leafy green vegetables, and dairy products are good sources.
- Consider Supplements: If dietary intake isn't sufficient or if deficiencies have been identified, discuss appropriate supplements with your dentist or doctor.
3. Choose Oral Hygiene Products Wisely
- SLS-Free Products: Switch to toothpastes and mouthwashes that do not contain sodium lauryl sulfate (SLS). For many individuals, SLS is a significant irritant that can trigger canker sores. Look for labels indicating "SLS-free" or "sensitive formula."
- Alcohol-Free Mouthwash: Choose mouthwashes that are alcohol-free, as alcohol can be drying and irritating to oral tissues.
4. Stress Management
- Practice Relaxation Techniques: Incorporate stress-reducing activities into your daily routine, such as meditation, yoga, deep breathing exercises, regular exercise, or hobbies you enjoy.
- Adequate Sleep: Ensure you get sufficient restorative sleep, as chronic sleep deprivation can weaken the immune system and increase stress levels.
5. Address Underlying Health Conditions
- Regular Medical Check-ups: If you have a systemic condition (e.g., celiac disease, inflammatory bowel disease, Behçet's disease, or even chronic stress leading to hand foot and mouth disease in adults if immunity is compromised), work with your medical doctor to manage it effectively. Controlling the underlying disease can often reduce the frequency of oral ulcers.
- Nutritional Screening: Discuss with your doctor or dentist if nutritional screening for deficiencies (iron, B12, folate, zinc) is appropriate, especially if you experience recurrent canker sores.
6. Good Oral Hygiene
- Consistent Brushing and Flossing: While not a direct preventive measure for all canker sores, good oral hygiene reduces the overall bacterial load in the mouth, which can help prevent secondary infections and promote faster healing if an ulcer does occur. ADA guidelines emphasize brushing twice a day and flossing once a day.
Pro Tip: Keeping a detailed diary of when you get canker sores, what you ate, your stress levels, and any new products you used can be highly effective in identifying personal triggers and tailoring your prevention strategy.
Risks and Complications
While a canker sore on gum is generally a benign condition that resolves on its own, certain risks and complications can arise, especially with recurrent, severe, or untreated lesions.
1. Severe Pain and Discomfort
- Impact on Quality of Life: The primary complication is significant pain, which can interfere with essential daily functions such as eating, drinking, speaking, and swallowing. This can lead to nutritional deficiencies if pain prevents adequate food intake.
- Difficulty with Oral Hygiene: Pain can make brushing and flossing difficult, potentially leading to plaque buildup, gum inflammation (gingivitis), and an increased risk of cavities in the surrounding teeth.
2. Secondary Infection
- Bacterial/Fungal Overgrowth: The open wound of a canker sore provides an entry point for bacteria or fungi naturally present in the mouth. While less common, secondary bacterial infection can occur, leading to increased pain, swelling, pus formation, and delayed healing.
- Signs of Infection: Look for worsening pain, spreading redness, pus, fever, or swollen lymph nodes.
3. Scarring
- Major Aphthous Ulcers: Larger or deeper canker sores (major aphthae), particularly those on the gums, can sometimes heal with noticeable scar tissue. This scarring can be uncomfortable and, in severe cases, might slightly alter the contour of the gum.
4. Nutritional Deficiencies
- Inadequate Intake: Chronic or severe canker sores, especially in children or the elderly, can lead to a reluctance to eat due to pain, resulting in unintended weight loss and deficiencies in essential nutrients.
- Exacerbation: This can create a vicious cycle where poor nutrition makes future canker sore outbreaks more likely.
5. Psychological Impact
- Anxiety and Stress: Frequent, painful outbreaks can cause significant anxiety and stress, impacting social interactions and overall well-being.
- Social Embarrassment: Some individuals may feel self-conscious about their oral lesions.

6. Misdiagnosis or Delayed Diagnosis of Underlying Conditions
- Masking Serious Illness: Recurrent oral ulcers can be a symptom of more serious underlying systemic diseases, such as inflammatory bowel disease (Crohn's disease, ulcerative colitis), celiac disease, Behçet's disease, or immune deficiencies. If canker sores are continually dismissed without proper investigation, the diagnosis and treatment of these primary conditions can be delayed.
- Confusion with Other Lesions: Misidentifying a cold sore inside mouth (which is contagious) or mistaking lesions from hand foot and mouth disease in adults for common canker sores can lead to inappropriate treatment or a missed opportunity to manage a communicable viral infection.
7. Oral Cancer
- Persistent Lesions: While canker sores are benign, any persistent, non-healing oral ulcer (lasting more than 2-3 weeks), especially one with irregular borders, color changes, or associated lumps, should be immediately evaluated by a dentist or oral surgeon. These could be early signs of oral cancer.
Pro Tip: Never ignore a persistent oral lesion. If a canker sore on gum or any other oral sore doesn't heal within 2-3 weeks, or if it recurs frequently, consult your dentist for a thorough examination to rule out any serious underlying conditions.
Children / Pediatric Considerations
A canker sore on gum can be particularly distressing for children and their parents. While the underlying causes are similar to adults, children often react differently to pain and treatment.
Commonality in Children
- Canker sores are common in children, with some studies suggesting up to 30% of children experiencing them by age 5.
- They often start presenting in school-aged children and teenagers.
Unique Challenges in Children
- Pain Management: Children may have a lower pain threshold or difficulty articulating their discomfort, leading to irritability, refusal to eat or drink, and disrupted sleep. This can quickly lead to dehydration or nutritional deficiencies.
- Diagnosis Difficulty: Distinguishing a canker sore from other common pediatric oral conditions like herpes gingivostomatitis (a severe initial cold sore infection), chickenpox, or hand foot and mouth disease can be challenging. HFMD, in particular, often presents with oral lesions that can be confused with canker sores, but the presence of fever and rashes on hands/feet are key differentiators.
- Compliance with Treatment: Applying topical medications or using mouth rinses can be difficult with young children who may resist or not understand the importance of the treatment.
Pediatric-Specific Treatment and Care
- Gentle Oral Hygiene: Emphasize very gentle brushing with a soft-bristled toothbrush. For very young children, a clean, damp cloth can be used.
- Dietary Choices: Encourage soft, bland, cool foods. Avoid anything acidic, spicy, or crunchy. Ice cream, yogurt, mashed fruits/vegetables, and soups are often well-tolerated.
- Hydration is Key: Offer plenty of cool liquids. Sucking on ice pops or ice chips can help numb the area and encourage fluid intake.
- OTC Pain Relief: Children's acetaminophen (Tylenol) or ibuprofen (Motrin, Advil) can help manage pain, but always follow dosing instructions based on age and weight.
- Topical Anesthetics: Use benzocaine-free topical gels specifically formulated for children (if available and recommended by a dentist/pediatrician). Benzocaine use in children under 2 is generally discouraged due to risk of methemoglobinemia, and caution is advised for older children. Lidocaine is generally safer but should also be used sparingly and as directed.
- Saltwater Rinses: For older children who can rinse and spit, warm salt water rinses are effective and safe.
- Dentist Consultation: Always consult a pediatric dentist or pediatrician if:
- The child refuses to eat or drink.
- Sores are very large, numerous, or persistent (over a week).
- The child has a high fever or appears unusually ill.
- You suspect a cold sore inside mouth or other viral infection.
- The child has swollen lymph nodes or signs of secondary infection.
- Avoid SLS: Recommend SLS-free toothpastes for children, especially if they have recurrent canker sores.
- Nutritional Assessment: If canker sores are recurrent, discuss with the pediatrician whether blood tests for nutritional deficiencies (iron, B12, folate) are warranted.
Pro Tip: When a child has a canker sore on gum, make sure to distinguish it from the highly contagious hand foot and mouth disease in adults (or children). HFMD presents with lesions on hands and feet in addition to oral sores, and usually includes fever, which is less common with typical canker sores.
Cost Breakdown
While covered generally in the "Cost and Insurance" section, let's elaborate on the financial aspects of treating a canker sore on gum in the US market, focusing on average costs, insurance implications, and financing.
Average US Costs (Low, Mid, High Estimates)
| Service/Treatment | Low Estimate | Mid Estimate | High Estimate | Notes |
|---|---|---|---|---|
| Initial Dental Exam/Consultation | $50 | $100 | $150 | Diagnostic visit to confirm diagnosis and rule out other conditions. |
| OTC Topical Pain Relief (gel/paste) | $5 | $15 | $25 | For a single tube/bottle. |
| OTC Antiseptic Mouthrinse | $5 | $10 | $15 | For a standard bottle. |
| Prescription Topical Corticosteroid | $10 (generic) | $30 | $50 (brand) | Price for a small tube. |
| Prescription Antiseptic Rinse | $15 (generic) | $20 | $30 (brand) | Chlorhexidine rinse. |
| Laser Treatment (per sore/session) | $75 | $150 | $250 | Highly effective for rapid relief and healing. |
| Silver Nitrate Application | $50 | $100 | $150 | Often included in the exam fee or charged separately as a palliative procedure. |
| Blood Test for Deficiencies | $50 | $150 | $300+ | If ordered by a medical doctor, often covered by medical insurance. |
| Systemic Medication (e.g., Prednisone) | $20 (generic) | $75 | $200+ (brand) | For severe or widespread cases. Varies greatly by drug and dosage. |
| Nutritional Supplements (monthly) | $10 | $25 | $40 | Varies by brand and type of supplement (e.g., B12, iron, zinc). |
With vs. Without Insurance
- Without Insurance: You will pay the full cash price for all services and medications. OTC products are never covered by insurance. Prescription medications will be full price unless you use discount cards (e.g., GoodRx).
- With Dental Insurance:
- Diagnostic Visits: Typically covered at 50-100% after deductible, so your out-of-pocket would be $0 - $75.
- Treatments: Procedures like laser therapy are generally not covered. Silver nitrate might be partially covered.
- With Medical Insurance (for Prescriptions):
- Prescription Medications: After meeting your deductible, you'd typically pay a co-pay ranging from $5 - $60 per prescription, depending on whether it's generic or brand name and your plan's formulary.
- Blood Tests/Specialist Referrals: If underlying medical conditions are suspected, medical insurance would cover related blood tests or consultations with specialists (e.g., gastroenterologist), subject to your plan's deductible and co-pays.
Payment Plans and Financing Options
For higher-cost treatments or if you lack adequate insurance, several options exist:
- In-Office Payment Plans: Many dental practices offer flexible payment schedules directly with the office, especially for procedures like laser therapy. This avoids interest if paid on time.
- Third-Party Financing (e.g., CareCredit): These specialized healthcare credit cards allow you to pay for treatments over time, often with promotional periods of 0% interest if the balance is paid within 6, 12, or 18 months.
- Health Savings Accounts (HSAs) & Flexible Spending Accounts (FSAs): These tax-advantaged accounts are excellent for covering medical and dental expenses. Contributions are tax-deductible, and withdrawals for qualified expenses are tax-free. They can be used for co-pays, deductibles, prescription medications, and even many OTC products (if prescribed by a doctor).
Cost-Saving Tips
- Communicate with Your Dentist: Discuss your financial situation openly. Your dentist can recommend the most effective yet affordable treatment plan.
- Generic Prescriptions: Always ask for generic versions of medications. They are chemically identical to brand names but significantly cheaper.
- GoodRx and Pharmacy Discount Programs: These programs can offer substantial discounts on prescription medications if you don't have insurance or if your insurance co-pay is high.
- Preventive Measures: Investing in preventive strategies (e.g., SLS-free toothpaste, stress management) can reduce the frequency of outbreaks and thus the need for costly treatments.
- Early Intervention: Addressing a canker sore early with simple remedies can prevent it from worsening into a major aphthous ulcer that might require more extensive and costly treatment.
Frequently Asked Questions
Is a canker sore on gum contagious?
No, a canker sore on gum is not contagious. Unlike cold sores, which are caused by the herpes virus and can be transmitted through contact, canker sores are not infectious and cannot be spread to others or to other parts of your body.
How long does a canker sore on gum typically last?
Minor canker sores on the gum usually heal on their own within 1 to 2 weeks without leaving scars. Larger or major aphthous ulcers can take 2 to 6 weeks or longer to heal and may leave scarring. Herpetiform ulcers also generally resolve within 1 to 3 weeks.
Can stress cause canker sores on the gums?
Yes, stress is a very common trigger for canker sores, including those on the gums. High levels of psychological stress or anxiety can alter the body's immune response, making individuals more susceptible to developing these painful oral lesions.
What's the best way to relieve pain from a canker sore on the gum?
The most effective ways to relieve pain include applying over-the-counter topical anesthetic gels (like benzocaine or lidocaine products), using prescription topical corticosteroids to reduce inflammation, or undergoing professional laser therapy, which often provides immediate pain relief. Rinsing with warm salt water can also offer some comfort.
Are there specific foods I should avoid if I have a canker sore on my gum?
Yes, you should avoid acidic foods (citrus fruits, tomatoes), spicy foods, salty snacks, and abrasive items (chips, hard bread) as they can irritate the sore and intensify the pain. Opt for soft, bland, and cool foods during an outbreak.
What's the difference between a canker sore and a cold sore inside the mouth?
A canker sore (aphthous ulcer) occurs inside the mouth, often on soft tissues like the gums, and is not contagious. A cold sore inside mouth is rare, usually appears on fixed tissue (hard palate/attached gingiva), starts as clustered blisters, and is caused by the contagious herpes simplex virus. A true canker sore never starts as a blister.
Can nutritional deficiencies lead to canker sores on the gum?
Absolutely. Deficiencies in certain vitamins and minerals, particularly iron, vitamin B12, folate, and zinc, are well-known contributing factors to recurrent canker sores. Addressing these deficiencies through diet or supplements can help reduce outbreaks.
When should I consider professional treatment like laser therapy for a canker sore?
Consider professional treatment like laser therapy if you experience severe pain, if the sore is large or persistent, if you have frequent recurrences, or if you want to accelerate healing and get immediate pain relief. Laser therapy is a quick, in-office procedure that is highly effective.
Is laser treatment for canker sores covered by dental insurance?
Generally, no. Laser treatment for canker sores is often considered an elective or palliative procedure by dental insurance companies and is typically not covered. Patients should be prepared to pay the cost, which can range from $75 to $250 per session, out-of-pocket.
Could a canker sore on my gum be a sign of something more serious?
While most canker sores are benign, recurrent or unusually persistent oral ulcers (lasting more than 2-3 weeks) can sometimes be a symptom of an underlying systemic condition, such as inflammatory bowel disease, celiac disease, or an immune disorder. In rare cases, a non-healing sore might even be an early sign of oral cancer. Always consult your dentist for any persistent or suspicious oral lesion.
When to See a Dentist
While many canker sores on gum can be managed with home remedies and over-the-counter treatments, there are clear warning signs and situations where professional dental attention is necessary. Delaying a dental visit in these cases could lead to prolonged discomfort, complications, or a missed diagnosis of a more serious condition.
Clear Warning Signs That Need Immediate Attention:
- Persistent Sores: Any canker sore on your gum or elsewhere in your mouth that does not show signs of healing and persists for longer than 2 to 3 weeks must be evaluated by a dentist. This is the most crucial red flag, as persistent lesions could indicate oral cancer or other serious conditions.
- Unusual Size or Appearance: If a sore is unusually large (larger than 1 centimeter), has irregular borders, or appears significantly different from past canker sores.
- Extreme Pain: If the pain is debilitating, preventing you from eating, drinking, speaking, or maintaining adequate oral hygiene.
- Frequent Recurrence: If you experience canker sore outbreaks very often (e.g., several times a month) or if new sores appear before old ones have healed, indicating recurrent aphthous stomatitis that requires professional management.
- Accompanying Systemic Symptoms: If oral sores are accompanied by other symptoms such as:
- High fever
- Skin rash (especially on hands and feet, which could indicate hand foot and mouth disease in adults)
- Joint pain
- Diarrhea or other gastrointestinal issues
- Unexplained weight loss
- General feeling of malaise or fatigue
- Swollen lymph nodes in the neck or jaw.
- Difficulty Swallowing: If the sore or sores are making it genuinely difficult or painful to swallow.
- Signs of Secondary Infection: Increased redness, swelling, warmth, or pus around the sore, or if you develop a fever.
- Suspected Trauma-Related Sore: If the sore is due to a sharp tooth, a broken filling, or an ill-fitting dental appliance, your dentist can address the source of trauma.
Red Flags vs. Routine Care Guidance:
- Red Flag: A persistent, non-healing sore. Action: Schedule an urgent diagnostic appointment.
- Red Flag: Systemic symptoms (fever, rash). Action: Contact your dentist or medical doctor immediately.
- Routine Care: Minor, occasional canker sores that heal within a week or two. Action: Self-care with OTC remedies is usually sufficient, but discuss at your next routine check-up if they are bothersome.
Emergency vs. Scheduled Appointment Guidance:
- Emergency Dental Visit (Same-day or next-day): For severe, debilitating pain, inability to eat or drink due to pain, rapid worsening of symptoms, or signs of severe secondary infection (fever, pus, spreading redness).
- Scheduled Dental Appointment (Within a few days to a week): For persistent sores (beyond 7-10 days), frequent recurrence, unusually large sores without emergency symptoms, or a desire to explore advanced treatment options like laser therapy or prescription medications.
Pro Tip: Don't hesitate to contact your dentist's office with any concerns about a canker sore on gum. They can provide guidance over the phone or advise you on whether an in-person examination is necessary. When in doubt, it's always best to get a professional opinion to ensure your oral health is not compromised.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles

Oral Candidiasis Symptoms: Complete Guide
Oral candidiasis, commonly known as oral thrush, is a fungal infection of the mouth caused by an overgrowth of Candida yeast, most often Candida albicans. While Candida is a normal inhabitant of the human mouth in small amounts, an imbalance can lead to uncomfortable and sometimes painful symptoms
February 23, 2026
Are Cold Sores Contagious
In the United States, an estimated 67% of the population under age 50 carries the herpes simplex virus type 1 (HSV-1), the primary cause of cold sores. This means millions of Americans are susceptible to these often painful and highly visible oral lesions. Beyond the discomfort and cosmetic conc
February 23, 2026
How Long Does Hand Foot and Mouth Last
Hand, Foot, and Mouth Disease (HFMD) is a common, often uncomfortable, viral illness that can affect anyone but is particularly prevalent among young children. If you or a loved one has ever experienced the tell-tale rash or painful mouth sores, you've likely wondered: **how long does Hand Foot and
February 23, 2026
Cold Sore vs Pimple on Lip: Complete Comparison Guide
When you notice an unexpected bump or lesion on your lip, your mind might immediately jump to questions of what it is, how long it will last, and most importantly, if it's contagious. The confusion between a cold sore vs pimple on lip is incredibly common, yet the distinction is crucial for prop
February 23, 2026