What Is a Canker Sore
Key Takeaways
- Imagine biting into a crisp apple, only to be met with a searing pain from a small, angry spot inside your mouth. Or perhaps you wake up with a tender, raw area on your tongue that makes talking or eating a chore. These common, often debilitating oral lesions are known as canker sores, and understan
Key Takeaways:
- Canker sores, medically known as aphthous ulcers, are common, painful, non-contagious sores that appear inside the mouth. They typically have a white or yellowish center with a red border.
- Approximately 20% of the US population experiences canker sores, with women and adolescents being more susceptible.
- There are three main types: minor (most common, 7-14 days healing), major (larger, deeper, up to 6 weeks healing with potential scarring), and herpetiform (clusters of tiny ulcers, not related to the herpes virus).
- Common causes include oral trauma, stress, certain foods, nutritional deficiencies (iron, B12, folate, zinc), and an immune response. They are distinct from mouth herpes (cold sores), which are viral and contagious.
- Treatment ranges from over-the-counter pain relievers and protective gels (typically $5-$30) to prescription corticosteroids (up to $100) and in-office laser therapy ($100-$400 per session) for faster healing and pain relief. Insurance rarely covers OTC remedies but may contribute to prescription costs or a dental visit.
- Prevention involves identifying and avoiding triggers, maintaining excellent oral hygiene with SLS-free products, managing stress, and ensuring a balanced diet.
- Consult a dentist if a canker sore is unusually large, extremely painful, lasts longer than two weeks, recurs frequently, or is accompanied by other systemic symptoms like fever or difficulty swallowing.
What Is a Canker Sore: An Overview
Imagine biting into a crisp apple, only to be met with a searing pain from a small, angry spot inside your mouth. Or perhaps you wake up with a tender, raw area on your tongue that makes talking or eating a chore. These common, often debilitating oral lesions are known as canker sores, and understanding what is a canker sore is the first step toward effective management and relief. Far more than just an inconvenience, these small ulcers can significantly impact your quality of life, making basic functions like eating, drinking, and speaking uncomfortable, sometimes even painful. In fact, research indicates that up to one in five Americans will experience a canker sore at some point in their lives, making them one of the most prevalent non-contagious oral conditions.

Medically referred to as aphthous ulcers (or recurrent aphthous stomatitis, RAS, when they appear frequently), canker sores are distinct from other oral lesions like cold sores (mouth herpes), which are caused by a virus and are contagious. Canker sores develop on the soft tissues inside your mouth—on the tongue, inner cheeks, lips, soft palate, or at the base of your gums. They typically present as round or oval lesions with a white or yellowish center and a bright red, inflamed border. While generally harmless and self-healing, their recurring nature and the significant discomfort they cause necessitate a comprehensive understanding of their causes, types, treatments, and prevention strategies. This article will delve deep into every aspect of canker sores, from their subtle beginnings to advanced management, ensuring you have the knowledge to navigate this common oral challenge.
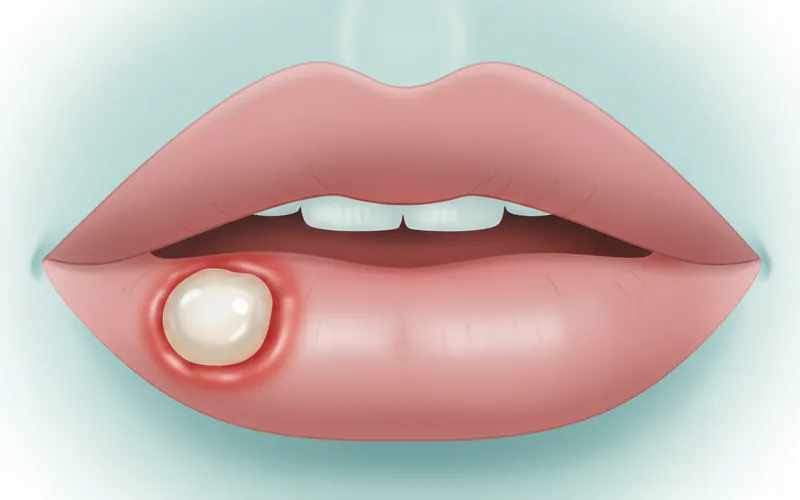
Types of Canker Sores
While all canker sores share some common characteristics, they are not all the same. Understanding the specific type can influence the severity of symptoms, healing time, and appropriate treatment approach. Dentists classify recurrent aphthous stomatitis into three primary types: minor, major, and herpetiform.
Minor Aphthous Ulcers (MiAU)
Minor aphthous ulcers are the most common type, accounting for about 80-85% of all canker sores. They are generally small, typically ranging from 1 to 5 millimeters in diameter, though they can sometimes reach up to 10 mm.
- Appearance: They are usually oval or round with a distinct white or yellowish center surrounded by a bright red, inflamed halo.
- Location: Most often found on the non-keratinized, soft tissues of the mouth, such as the inside of the lips, cheeks, the floor of the mouth, and the sides or tip of the tongue.
- Symptoms: Minor canker sores are painful but generally cause manageable discomfort. They do not usually cause systemic symptoms like fever.
- Healing Time: These sores typically heal on their own within 7 to 14 days (1 to 2 weeks) without scarring. Recurrence is common, but usually, only one or a few appear at a time.
Major Aphthous Ulcers (MaAU)
Also known as Sutton's ulcers, major aphthous ulcers are much less common, making up about 10% of canker sore cases, but they are significantly more severe.
- Appearance: These are larger, deeper, and more irregular in shape than minor sores, often exceeding 10 millimeters (up to 30 mm) in diameter. Their centers may be deeper and more necrotic (tissue death) with raised, irregular borders.
- Location: While they can appear anywhere, major sores are often found on the softer parts of the mouth, including the soft palate, tonsillar pillars, and the back of the throat, as well as the lips and cheeks.
- Symptoms: Major canker sores are exceedingly painful and can interfere with eating, drinking, and speaking. They may be accompanied by systemic symptoms such as fever, malaise, or swollen lymph nodes due to their size and inflammatory response.
- Healing Time: Due to their depth and size, major aphthous ulcers can take two weeks to six weeks or even longer to heal. They frequently leave scars, and multiple lesions can appear simultaneously, sometimes merging into larger, more complex ulcers.
Herpetiform Aphthous Ulcers (HuAU)
Despite their name, herpetiform aphthous ulcers are not caused by the herpes virus and are not contagious like mouth herpes (cold sores). They are named "herpetiform" because they resemble the clusters of small blisters seen in herpetic infections. This type is the rarest, representing about 5-10% of cases.
- Appearance: These sores manifest as multiple tiny, pinpoint ulcers (1-3 mm each) that often cluster together to form a larger, irregular-shaped lesion. There can be anywhere from 10 to 100 small ulcers in a single outbreak.
- Location: They can occur anywhere in the mouth, including areas typically associated with minor and major aphthae, but also on the more rigid (keratinized) tissues like the hard palate or gums, although this is less common than with viral herpes.
- Symptoms: Herpetiform ulcers can be extremely painful due to the sheer number of lesions.
- Healing Time: They typically heal within one to four weeks, often without scarring, though recurrence is very common.
Causes and Contributing Factors
The exact cause of canker sores remains unknown, leading to their classification as idiopathic (of unknown origin). However, extensive research points to a multifactorial etiology, meaning a combination of factors contributes to their development. It's believed that an abnormal immune response is at the heart of aphthous ulcers, triggered by various internal and external stimuli.
Genetic Predisposition
Genetics play a significant role. If one or both parents suffer from canker sores, their children have a 90% increased likelihood of developing them. This suggests a hereditary component that influences an individual's immune response to certain triggers.
Oral Injury or Trauma
Physical injury to the mouth lining is a very common trigger. This can include:
- Accidental biting of the cheek, lip, or tongue.
- Aggressive tooth brushing or using a toothbrush with hard bristles.
- Dental work, such as fillings, extractions, or orthodontic appliances (braces).
- Sharp edges from broken teeth or dental restorations.
Nutritional Deficiencies
Deficiencies in certain essential vitamins and minerals are strongly linked to canker sore development. These include:
- Iron: Essential for red blood cell formation and tissue health.
- Vitamin B12 (Cobalamin): Crucial for nerve function and DNA synthesis; deficiency can lead to anemia and oral lesions.
- Folate (Folic Acid): Important for cell growth and replication.
- Zinc: Vital for immune function and wound healing.
- Pro Tip: If you experience recurrent canker sores, ask your dentist or physician about blood tests to check for these deficiencies.
Food Sensitivities
Certain foods, particularly those that are acidic, spicy, or abrasive, can trigger canker sores in susceptible individuals. Common culprits include:
- Acidic fruits: oranges, lemons, pineapples, tomatoes.
- Spicy foods.
- Chocolate.
- Coffee.
- Nuts (especially walnuts, almonds).
- Cheese.
- Gluten (in individuals with celiac disease or gluten sensitivity).
Stress and Hormonal Changes
Psychological stress is a well-documented trigger for canker sores. Periods of high anxiety, emotional upheaval, or physical stress can disrupt the immune system, making individuals more prone to outbreaks. Hormonal fluctuations, such as those experienced during menstruation, pregnancy, or menopause, can also influence susceptibility, particularly in women.
Immune System Response
Canker sores are often considered an inflammatory condition where the immune system overreacts to something it perceives as a threat. This is why individuals with certain systemic diseases that affect the immune system are more prone to them:
- Inflammatory Bowel Diseases (IBD): Crohn's disease and ulcerative colitis are often associated with oral manifestations, including canker sores.
- Celiac Disease: An autoimmune disorder triggered by gluten, often presenting with oral lesions.
- Behçet's Disease: A rare chronic inflammatory disorder characterized by recurrent oral ulcers, genital ulcers, and eye inflammation.
- HIV/AIDS: Individuals with compromised immune systems are more susceptible to severe and persistent canker sores.
- Lupus: Another autoimmune disease that can cause oral lesions.
Sodium Lauryl Sulfate (SLS) in Toothpaste
Sodium lauryl sulfate (SLS) is a foaming agent commonly found in many toothpastes and mouthwashes. Some studies suggest that SLS can irritate the delicate oral mucosa, making it more susceptible to canker sores or prolonging their healing. Switching to an SLS-free toothpaste may reduce the frequency of outbreaks for some individuals.
Medications
Certain medications can contribute to canker sore development as a side effect. These include:
- Non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen.
- Beta-blockers.
- Nicorandil (a potassium channel activator used for angina).
- Chemotherapy drugs.
Signs and Symptoms
Identifying a canker sore is usually straightforward due to its characteristic appearance and the discomfort it causes. The onset of a canker sore typically follows a predictable pattern:
- Prodromal Stage (12-48 hours before appearance): Many individuals report a tingling, burning, or pricking sensation in a specific area of the mouth before any visible lesion appears. This forewarns of an impending canker sore.
- Lesion Development:
- Initially, a small red bump or spot develops.
- Within a day or so, this spot breaks open to form an open ulcer.
- The ulcer typically has a white or yellowish center, which is a fibrin membrane covering the exposed tissue, surrounded by a distinct bright red, inflamed halo. This red halo is a key distinguishing feature.
- Location: Canker sores almost exclusively occur on the non-keratinized (soft and movable) tissues of the mouth. This includes:
- Inside the cheeks and lips.
- On or under the tongue.
- The soft palate (the back, soft part of the roof of the mouth).
- The floor of the mouth.
- The base of the gums.
- Crucial distinction: Unlike cold sores (mouth herpes), which appear on the outside of the lips or on the hard (keratinized) palate and gums, canker sores are almost always inside the mouth on soft tissues.
- Pain Level: Canker sores are characteristically painful, especially when touched, during eating, or while speaking. The pain intensity can range from mild annoyance with minor aphthae to severe and debilitating with major aphthae, making it difficult to perform basic oral functions.
- Size: As discussed, sizes vary by type:
- Minor: 1-5 mm, up to 10 mm.
- Major: >10 mm, often larger.
- Herpetiform: Clusters of 1-3 mm lesions that merge.
- Associated Symptoms (especially with major aphthae or underlying conditions):
- Difficulty eating, drinking, and swallowing (dysphagia).
- Difficulty speaking (dysphonia).
- Swollen and tender lymph nodes in the neck.
- Fever.
- General feeling of illness (malaise).
- Fatigue.
Diagnosing Canker Sores
Diagnosing canker sores is primarily a clinical process, based on the characteristic appearance of the lesions and a thorough patient history. There isn't a specific laboratory test to confirm a canker sore, as there is for viral infections like mouth herpes.
-
Clinical Examination: Your dentist or doctor will visually inspect your mouth for the presence, location, size, and appearance of the ulcers (white/yellow center with a red halo). They will also look for signs of other oral conditions.
-
Patient History: The healthcare provider will ask about:
- Recurrence: How often do you get these sores?
- Duration: How long do they typically last?
- Triggers: Have you noticed any specific foods, stress, or trauma preceding an outbreak?
- Family History: Do other family members get canker sores?
- Associated Symptoms: Are you experiencing fever, swollen glands, gastrointestinal issues, or other systemic symptoms?
- Medications: A list of all current medications.
-
Distinguishing from Other Oral Lesions: This is a crucial step to rule out other conditions that may resemble canker sores but require different treatments.
- Cold Sores (Mouth Herpes): Caused by HSV-1, highly contagious, appear on outer lips or hard palate/gums, start as blisters that burst and crust over.
- Oral Thrush (Candidiasis): Fungal infection, presents as white, creamy patches that can be wiped away, often seen in infants, immunocompromised individuals, or those on antibiotics/steroids.
- Traumatic Ulcers: Single, non-recurring ulcers caused by a specific injury (e.g., biting cheek), heal once the cause is removed.
- Oral Cancer: Persistent, non-healing sores, often irregular in shape, typically not painful in early stages, may bleed easily. Requires immediate biopsy.
- Hand, Foot, and Mouth Disease: Viral infection common in children, characterized by painful mouth sores (often resembling canker sores) accompanied by a rash on the hands and feet, and sometimes fever. The distinction between canker sores and oral lesions associated with stages of hand foot and mouth disease is critical, especially in pediatric cases, due to differing contagiousness and systemic impact.
-
Further Investigations (if atypical or severe):
- Blood Tests: If nutritional deficiencies (iron, B12, folate, zinc) are suspected as a cause of recurrent canker sores, blood tests can confirm these.
- Biopsy: Rarely, if a lesion is persistent (lasts more than 3 weeks), unusually large, or has an atypical appearance, a biopsy may be performed to rule out more serious conditions like oral cancer or specific inflammatory diseases.
- Referral to Specialist: For severe or recurring cases, a referral to an oral pathologist, dermatologist, or gastroenterologist might be necessary to investigate underlying systemic conditions such as inflammatory bowel disease or Behçet's disease.
Treatment Options for Canker Sores
While most minor canker sores heal on their own, various treatments can alleviate pain, promote healing, and reduce the frequency of recurrence. The approach depends on the type, severity, and frequency of the sores.
Over-the-Counter (OTC) Remedies
These are the first line of defense for most minor canker sores.
- Topical Anesthetics: Products containing benzocaine (e.g., Orajel, Kank-A), lidocaine, or tetracaine provide temporary pain relief by numbing the area.
- Pros: Readily available, instant pain relief.
- Cons: Short-acting, doesn't promote healing, can sting initially.
- Oral Rinses:
- Saltwater Rinse: A classic home remedy, 1 teaspoon of salt in 8 ounces of warm water. Soothes irritation and has mild antiseptic properties.
- Baking Soda Rinse: 1 teaspoon of baking soda in 8 ounces of warm water. Neutralizes acids and reduces inflammation.
- Hydrogen Peroxide Rinse: Diluted (1 part 3% hydrogen peroxide to 1 part water). Used as an antiseptic to clean the sore. Avoid swallowing.
- Pros: Inexpensive, accessible, can keep the area clean.
- Cons: Limited pain relief, doesn't directly treat the sore's cause.
- Protective Pastes/Gels: Products forming a protective barrier over the sore (e.g., Orabase, Zilactin-B). These shield the sore from irritation caused by food, drink, and tooth friction.
- Pros: Protects the sore, can reduce pain, aids healing by preventing further irritation.
- Cons: Can be difficult to apply, may not adhere well in all areas.
- Milk of Magnesia: Applying a small amount a few times a day can help soothe and reduce acidity.
Prescription Medications
For more severe, persistent, or recurrent canker sores, a dentist or doctor may prescribe stronger medications.
- Topical Corticosteroids: These reduce inflammation and pain, and can speed healing. Common examples include fluocinonide gel, triamcinolone acetonide dental paste (Kenalog in Orabase), and clobetasol gel.
- Pros: Highly effective at reducing inflammation and pain, promotes healing.
- Cons: Requires prescription, potential for fungal infection (thrush) with prolonged use, not for viral sores.
- Oral Rinse (Dexamethasone): A potent corticosteroid rinse used for multiple or difficult-to-reach sores.
- Pros: Treats widespread lesions effectively.
- Cons: Can be absorbed systemically, requires careful use, potential for side effects if swallowed.
- Sucralfate Suspension: Used to treat stomach ulcers, it can coat oral ulcers to provide protection and promote healing.
- Pros: Forms a protective barrier, helps healing.
- Cons: Requires prescription, can have a chalky taste.
- Systemic Medications: For very severe or frequent major aphthae, oral medications might be considered:
- Oral Corticosteroids: Prednisone may be prescribed for short durations to control severe outbreaks.
- Cimetidine: An H2 blocker sometimes used off-label to reduce recurrence in severe cases by modulating the immune response.
- Colchicine, Dapsone, Pentoxifylline: Other immunomodulators used for severe, intractable cases, often managed by specialists.
- Pros: Highly effective for severe cases.
- Cons: Significant potential side effects, generally reserved for extreme situations.
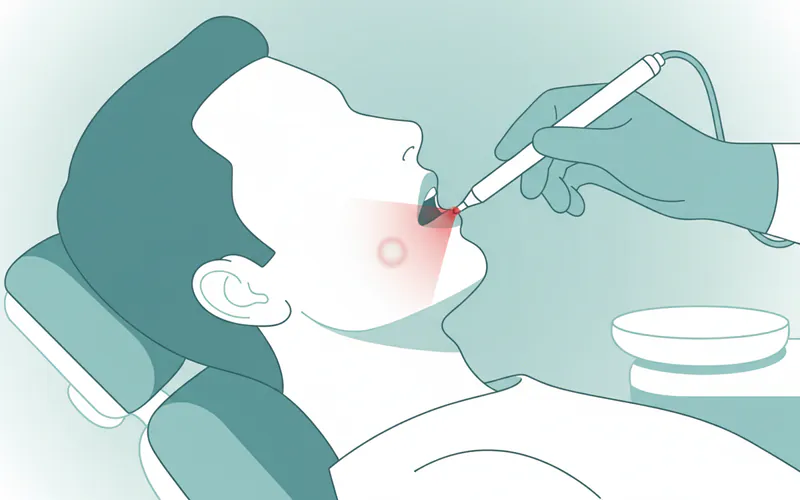
Laser Treatment
Dental lasers (e.g., diode lasers) can be used to treat canker sores in-office.
- Process: A low-level laser is directed at the sore for a few minutes. The laser energy helps to seal nerve endings, reduce inflammation, and promote faster healing.
- Pros: Immediate pain relief, significantly reduces healing time (often to 1-3 days), no anesthesia usually required, reduces recurrence in the treated spot.
- Cons: Requires a dental visit, higher upfront cost compared to OTC or prescription topicals.
- Pro Tip: Early laser treatment (at the first sign of a tingling sensation) can sometimes prevent a full canker sore from developing.
Nutritional Supplementation
If deficiencies are identified through blood tests, your doctor may recommend supplements.
- Iron, Vitamin B12, Folate, Zinc: Taken orally as directed.
- Pros: Addresses underlying cause, can reduce recurrence.
- Cons: Takes time to see results, must be taken consistently.
Lifestyle Modifications
- Dietary Changes: Identify and avoid trigger foods (acidic, spicy, abrasive).
- SLS-Free Products: Switch to toothpaste and mouthwash that do not contain sodium lauryl sulfate.
- Stress Management: Techniques like meditation, yoga, regular exercise, and adequate sleep can reduce stress-related outbreaks.
- Good Oral Hygiene: Gentle brushing with a soft-bristled toothbrush to prevent trauma.
Step-by-Step Treatment Process
The treatment process for canker sores largely depends on their severity and frequency.
-
Initial Assessment (Self-Care or Dentist Visit):
- Minor, infrequent sores: Most individuals start with self-care at home using OTC remedies.
- Large, painful, frequent, or persistent sores: A visit to your dentist or doctor is recommended for professional diagnosis and treatment.
- During a dental visit: The dentist will conduct an oral examination, review your medical history, and discuss your symptoms and potential triggers. They will differentiate the canker sore from other oral lesions like mouth herpes or signs of stages of hand foot and mouth disease.
-
For Minor Sores (Self-Care):
- Pain Relief: Apply topical anesthetic gels (e.g., benzocaine) directly to the sore as needed for temporary relief.
- Rinsing: Rinse your mouth several times a day with saltwater or baking soda solution, especially after meals, to keep the area clean and soothe irritation.
- Protection: Use protective pastes or gels to cover the sore, reducing friction and pain from food or teeth.
- Avoid Triggers: Steer clear of acidic, spicy, or abrasive foods, and ensure gentle brushing.
- Monitor: Observe the sore for healing within 1-2 weeks. If it doesn't improve or worsens, contact your dentist.
-
For Moderate to Severe Sores (Professional Treatment):
- Prescription Topicals: Your dentist may prescribe a corticosteroid gel or paste.
- Application: Apply a small amount directly to the sore, usually 2-4 times a day, preferably after meals and before bedtime. Ensure the area is as dry as possible for better adhesion.
- Prescription Rinses: For multiple or hard-to-reach sores, a dexamethasone rinse may be prescribed.
- Application: Swish the rinse in your mouth for 1-2 minutes, then spit it out. Do not swallow. Usually prescribed 2-3 times a day.
- Laser Treatment: If available and recommended, the dentist will perform a quick laser procedure.
- Process: The laser light targets the sore. Patients typically feel a warming sensation, but it's generally painless. The entire procedure usually takes only a few minutes.
- Immediate Benefits: Many report significant pain reduction immediately after treatment, with accelerated healing over the next 24-72 hours.
- Prescription Topicals: Your dentist may prescribe a corticosteroid gel or paste.
-
Addressing Underlying Causes:
- If nutritional deficiencies are identified, you will be advised to take specific supplements as prescribed.
- If certain systemic conditions are suspected, the dentist may refer you to a specialist (e.g., gastroenterologist for IBD, rheumatologist for autoimmune diseases).
-
Follow-Up:
- For minor sores, no formal follow-up is usually needed if they heal as expected.
- For severe or treated sores, your dentist may schedule a follow-up visit, especially if systemic medications are involved or to reassess healing and recurrence patterns.
- ADA Recommendation: The American Dental Association (ADA) emphasizes the importance of regular dental check-ups, which can help identify recurrent oral lesions early and ensure proper diagnosis and management.
Recovery and Aftercare
Recovery from a canker sore primarily involves waiting for the lesion to heal and managing symptoms during that period. Aftercare focuses on promoting healing, preventing secondary infections, and minimizing recurrence.

-
Healing Timelines:
- Minor Aphthous Ulcers: Typically heal within 7 to 14 days (1-2 weeks).
- Major Aphthous Ulcers: Can take significantly longer, from 2 weeks to 6 weeks or even more, often resulting in scarring due to their depth.
- Herpetiform Aphthous Ulcers: Usually heal within 1 to 4 weeks.
- Laser-Treated Sores: Pain relief is often immediate, and visible healing can be accelerated to 1-3 days.
-
Maintaining Oral Hygiene:
- Gentle Brushing: Continue to brush your teeth twice daily with a soft-bristled toothbrush to avoid further irritation to the sore. Consider using an SLS-free toothpaste.
- Regular Rinsing: Continue saltwater or baking soda rinses, especially after meals, to keep the area clean and reduce bacterial load. This is crucial for preventing secondary bacterial infections.
-
Dietary Recommendations During Healing:
- Soft, Bland Foods: Stick to foods that are easy to chew and swallow, such as mashed potatoes, yogurt, soups, scrambled eggs, and smoothies.
- Avoid Irritants: Continue to avoid acidic fruits and juices, spicy foods, very hot foods, crunchy or abrasive foods (like chips or toast), and alcohol, as these can irritate the sore and delay healing.
- Hydration: Drink plenty of water to stay hydrated, which supports overall healing.
-
Pain Management:
- Continue to use topical anesthetics or prescribed medications as needed for pain relief until the sore is fully healed.
- Over-the-counter pain relievers like acetaminophen (Tylenol) or ibuprofen (Advil, Motrin) can also help manage general discomfort.
-
Monitoring for Complications:
- Keep an eye on the sore for any signs of worsening, such as increased redness spreading beyond the sore, pus formation, or prolonged pain after the expected healing time. These could indicate a secondary bacterial infection, which may require antibiotics.
- Report any new or persistent symptoms, especially fever or swollen glands, to your dentist or doctor.
Prevention Strategies
While eliminating canker sores entirely might not be possible for those genetically predisposed, many strategies can significantly reduce their frequency and severity.
-
Identify and Avoid Triggers:
- Food Diary: Keep a log of foods you eat before an outbreak to identify potential dietary triggers (acidic foods, chocolate, nuts, etc.) and then avoid them.
- Trauma Prevention:
- Use a soft-bristled toothbrush and brush gently.
- Be mindful when chewing to avoid biting your cheeks or tongue.
- If you have sharp teeth or dental appliances (e.g., braces, ill-fitting dentures) that cause irritation, consult your dentist for adjustments.
- Use dental wax for orthodontic brackets.
-
Choose SLS-Free Oral Care Products:
- Switch to toothpastes and mouthwashes that do not contain sodium lauryl sulfate (SLS), as this foaming agent can irritate the oral mucosa in some individuals. Many brands now offer SLS-free options.
-
Manage Stress:
- Since stress is a major trigger, incorporating stress-reduction techniques into your daily routine can be highly beneficial. This may include:
- Meditation or mindfulness.
- Yoga or tai chi.
- Regular physical exercise.
- Adequate sleep (7-9 hours per night for adults).
- Spending time in nature.
- Since stress is a major trigger, incorporating stress-reduction techniques into your daily routine can be highly beneficial. This may include:
-
Maintain a Balanced Diet and Address Deficiencies:
- Eat a diet rich in fruits, vegetables, and whole grains to ensure adequate nutrient intake.
- If diagnosed with specific nutritional deficiencies (iron, Vitamin B12, folate, zinc), take supplements as prescribed by your doctor.
- Consider a daily multivitamin if your diet is often lacking.
-
Practice Excellent Oral Hygiene:
- Brush twice daily and floss once daily to keep your mouth clean and reduce bacterial load, which can help prevent secondary infections and promote overall oral health.
- Regular dental check-ups (every 6 months) allow your dentist to monitor your oral health, address any potential issues early, and provide personalized advice.
-
Stay Hydrated:
- Drinking plenty of water helps maintain oral moisture and overall health.
Risks and Complications
While generally harmless, canker sores, particularly recurrent or severe forms, can lead to several risks and complications if not managed appropriately.
- Secondary Infection: The open ulcer of a canker sore creates an entry point for bacteria, fungi, or even viruses already present in the mouth. This can lead to a secondary bacterial infection, characterized by increased pain, redness, pus formation, and delayed healing. This might require antibiotic treatment.
- Scarring: Major aphthous ulcers, due to their size and depth, frequently heal with scarring. This can alter the texture of the oral mucosa and, in severe cases, lead to tissue distortion or functional impairment if they occur in critical areas.
- Difficulty Eating and Drinking: The pain associated with canker sores, especially large or multiple lesions, can make it extremely difficult and painful to chew, swallow, or even drink. This can lead to:
- Malnutrition: If the difficulty eating persists over time.
- Dehydration: Due to reduced fluid intake.
- Weight Loss: In chronic or severe cases.
- Pain and Discomfort: Chronic or recurrent canker sores can significantly impact quality of life, leading to ongoing pain, sleep disturbances, and general malaise. This persistent discomfort can affect daily activities, work, and social interactions.
- Misdiagnosis or Delay in Diagnosis of Underlying Systemic Disease: Since recurrent or severe canker sores can be a symptom of various systemic conditions (e.g., Crohn's disease, Behçet's disease, celiac disease, HIV/AIDS, certain autoimmune disorders), attributing them solely to "just canker sores" can delay the diagnosis and treatment of a more serious underlying health issue.
- Psychological Impact: The chronic pain and recurrence of canker sores can lead to frustration, anxiety, and even depression, impacting mental well-being.
- Increased Risk of Oral Cancer (extremely rare and not directly caused by canker sores): While canker sores themselves are not precancerous, any persistent, non-healing oral lesion (lasting more than 2-3 weeks) should be evaluated by a dentist or doctor to rule out oral cancer. The concern here is about confusing a persistent canker sore with a cancerous lesion.
Comparison: Canker Sore vs. Other Oral Lesions
Distinguishing canker sores from other common oral lesions is crucial for proper diagnosis and treatment. Confusion often arises with cold sores (mouth herpes) and the oral lesions of hand, foot, and mouth disease.
| Feature | Canker Sore (Aphthous Ulcer) | Cold Sore (Mouth Herpes) | Oral Thrush (Candidiasis) | Hand, Foot, and Mouth Disease (Oral Lesions) |
|---|---|---|---|---|
| Cause | Unknown (immune response, trauma, stress, deficiencies) | Herpes Simplex Virus Type 1 (HSV-1) | Candida albicans (fungus) | Coxsackievirus A16 or Enterovirus 71 |
| Appearance | Round/oval, white/yellow center, red halo. Single or multiple. | Clusters of fluid-filled blisters that burst, crust, then heal. | Creamy white, cottage cheese-like patches, can be wiped away. | Small red spots that turn into blisters, then ulcers (similar to canker sores), usually on back of mouth/throat. |
| Location | Inside mouth on soft, non-keratinized tissues (lips, cheeks, tongue, soft palate, throat). | Outside mouth (lips), or on hard palate/gums (keratinized tissue). | Anywhere in mouth, often tongue, inner cheeks, roof of mouth. | Mouth (tongue, cheeks, hard/soft palate, tonsils), hands, feet. |
| Contagiousness | Not contagious | Highly contagious (via direct contact with lesions or saliva) | Generally not contagious (overgrowth of normal flora) | Highly contagious (via saliva, mucus, blister fluid, stool) |
| Symptoms | Painful, burning/tingling prodrome. Pain with eating/speaking. | Tingling/itching prodrome, pain, often fever/malaise with primary infection. | Pain, burning, cottony feeling in mouth, taste changes. | Fever, sore throat, malaise, rash on hands/feet, painful mouth sores. |
| Duration | 1-2 weeks (minor), 2-6 weeks (major) | 7-14 days | Varies, often persistent without treatment | 7-10 days |
| Treatment | OTC pain relief, prescription steroids, laser therapy. | Antiviral medications (topical/oral). | Antifungal medications (topical/oral). | Symptomatic relief (pain, fever), hydration. |
Children and Canker Sores: Pediatric Considerations
Canker sores are a common occurrence in children, often causing significant distress for both the child and their parents due to the pain and difficulty eating. While the general characteristics are similar to adults, there are specific considerations for pediatric cases.
- Prevalence: Canker sores can affect children as young as toddlers, and their incidence tends to increase during school-age and adolescence. Children whose parents get canker sores are more likely to develop them, highlighting the genetic link.
- Causes in Children:
- Oral Trauma: This is a very frequent cause in children. Accidental biting during play, vigorous toothbrushing, or injuries from dental appliances (braces) are common.
- Nutritional Deficiencies: Children, especially picky eaters, may be more susceptible to deficiencies in iron, Vitamin B12, or folate, which can trigger canker sores.
- Stress: Academic pressure, social issues, family changes, or even excitement can manifest as physical stress, leading to outbreaks.
- Food Sensitivities: Children may also be sensitive to acidic or spicy foods.
- Distinguishing from Hand, Foot, and Mouth Disease (HFMD): This is a critical distinction in children. Hand, foot, and mouth disease is a common viral infection in young children, characterized by fever, malaise, sore throat, and a distinctive rash on the hands and feet, along with painful oral lesions. These oral lesions can sometimes resemble canker sores.
- Key Differences:
- Location of Sores: HFMD sores often appear on the back of the mouth, throat, tonsils, and sometimes the tongue and cheeks, but are always accompanied by the characteristic hand and foot rash. Canker sores are exclusively oral and don't involve other body parts.
- Contagiousness: HFMD is highly contagious; canker sores are not.
- Systemic Symptoms: HFMD almost always includes fever and other flu-like symptoms; canker sores usually do not, unless they are major aphthae or indicate an underlying condition.
- Key Differences:
- Pain Management for Children:
- Gentle Approaches First: Start with warm saltwater rinses (if the child is old enough to rinse and spit), or gently dab milk of magnesia on the sore.
- Over-the-Counter Gels: Topical numbing gels containing benzocaine can be used sparingly for immediate pain relief, but avoid excessive use, especially in very young children, and always follow package directions or pediatrician advice.
- Dietary Adjustments: Offer soft, bland, cool foods like yogurt, ice cream, popsicles, pureed fruits, and soft pasta. Avoid acidic juices, carbonated drinks, and spicy foods.
- Hydration: Ensure the child drinks plenty of fluids to prevent dehydration, which can be a risk if eating/drinking is very painful.
- Acetaminophen/Ibuprofen: Child-appropriate doses of over-the-counter pain relievers can help with discomfort.
- When to See a Pediatric Dentist or Doctor:
- If the child is in extreme pain, refusing to eat or drink, or showing signs of dehydration.
- If the sore is unusually large, persistent (over 10 days), or recurs very frequently.
- If the child has a fever, swollen glands, or a rash on other parts of the body (to rule out HFMD or other conditions).
- If you suspect nutritional deficiencies.
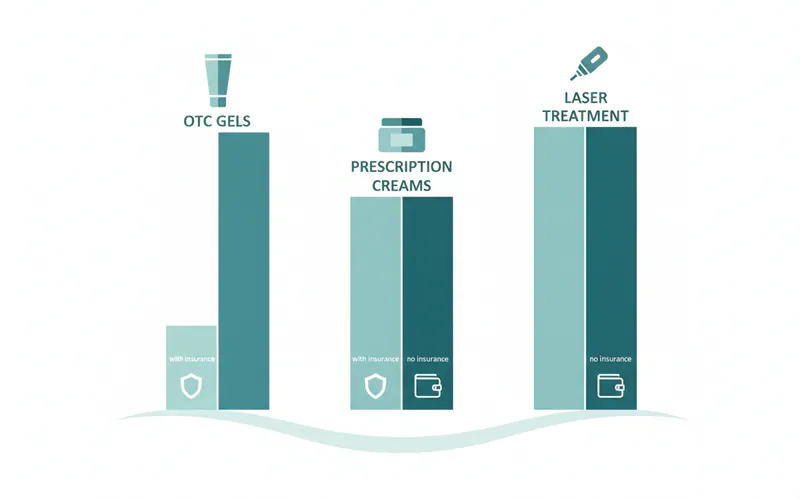
Cost Breakdown of Canker Sore Treatment
The cost of treating canker sores in the US can vary widely, depending on the severity of the condition, the type of treatment chosen, and whether professional intervention is required.
Over-the-Counter (OTC) Costs
- Topical Anesthetic Gels (e.g., Orajel, Kank-A): Typically range from $5 to $20 per tube.
- Protective Pastes (e.g., Orabase): Usually cost between $10 and $30.
- Oral Rinses (e.g., Peroxyl, specialized canker sore rinses): Can range from $8 to $25.
- Home Remedies (Salt, Baking Soda): Virtually free, costing pennies.
- OTC Pain Relievers (Acetaminophen, Ibuprofen): $5 to $15 per bottle.
- Insurance Coverage: OTC products are generally not covered by dental or medical insurance plans.
Prescription Medication Costs
- Topical Corticosteroid Gels/Pastes (e.g., Kenalog in Orabase, fluocinonide gel): Without insurance, these can cost anywhere from $20 to $100 per tube, depending on the medication and pharmacy. With insurance, a co-pay might be $10-$50.
- Prescription Oral Rinses (e.g., Dexamethasone): Can range from $30 to $150 without insurance. With insurance, a co-pay could be $15-$60.
- Systemic Medications (e.g., Cimetidine, Prednisone): Costs vary significantly depending on the drug and dosage, often ranging from $30 to $200+ for a course without insurance, with insurance co-pays being similar to other prescription drugs.
- Insurance Coverage: Many prescription medications are covered by medical insurance plans, subject to deductibles and co-pays.
Professional Treatment Costs
- Dental Office Visit/Consultation: A standard exam and consultation to diagnose a canker sore typically costs between $50 and $200 without insurance. If other services (e.g., X-rays to rule out other issues) are performed, the cost will increase.
- Insurance Coverage: Most dental insurance plans will cover a portion of diagnostic exams, often 50-80% after deductible.
- Laser Treatment: This is often considered a "cosmetic" or elective procedure by insurance, but many dentists consider it a therapeutic treatment.
- Cost per session: Laser treatment for a single canker sore generally ranges from $100 to $400 per session. For multiple or larger sores, the cost might be higher.
- Insurance Coverage: Laser treatment for canker sores is rarely covered by dental or medical insurance. Patients usually pay out-of-pocket.
Nutritional Supplements
- Iron, Vitamin B12, Folate, Zinc Supplements: Monthly supply typically costs $10 to $40, depending on the brand and dosage.
- Insurance Coverage: Generally not covered unless specifically prescribed for a documented medical deficiency and the supplement is from an approved formulary.
Cost-Saving Tips
- Utilize Home Remedies: For minor sores, saltwater or baking soda rinses are very effective and nearly free.
- Generic Medications: Opt for generic versions of prescription medications, which are often significantly cheaper than brand-name drugs.
- Ask About Samples: Your dentist or doctor may have free samples of prescription topical treatments.
- Dental School Clinics: These often offer lower-cost services compared to private practices, though wait times may be longer.
- Payment Plans and Financing: Some dental offices offer in-house payment plans, or you can explore third-party financing options like CareCredit for larger treatment costs.
Comparison Table: Canker Sore Treatment Cost & Coverage
| Treatment Type | Average Cost Range (US, out-of-pocket) | Typical Insurance Coverage | Pros | Cons |
|---|---|---|---|---|
| OTC Topical Gels/Pastes | $5 - $30 | None | Readily available, instant pain relief | Temporary, doesn't speed healing |
| OTC Rinses | $8 - $25 | None | Cleanses, soothes irritation, inexpensive | Limited pain relief, doesn't directly treat cause |
| Prescription Topicals | $20 - $100 | Partial (co-pay $10-$50) | Reduces inflammation, speeds healing, effective | Requires prescription, potential side effects |
| Prescription Systemic Meds | $30 - $200+ | Partial (co-pay $15-$60+) | Highly effective for severe/recurrent cases | Significant side effects, last resort |
| Laser Treatment (1 session) | $100 - $400 | Generally none (patient pays full) | Immediate pain relief, significantly faster healing, reduced recurrence | Higher upfront cost, requires dental visit |
| Dental Consultation | $50 - $200 | Partial (50-80% after deductible) | Professional diagnosis, rules out serious issues | Cost for exam if no insurance |
| Nutritional Supplements | $10 - $40/month | Rare | Addresses underlying deficiency, prevents recurrence | Takes time to show effect, not for all causes |
Frequently Asked Questions
Are canker sores contagious?
No, canker sores are not contagious. Unlike cold sores (mouth herpes), which are caused by a virus and can spread through direct contact, canker sores are non-viral and cannot be transmitted from person to person.
How long do canker sores last?
Minor canker sores typically heal on their own within 7 to 14 days. Major canker sores can last much longer, from 2 weeks to 6 weeks or more, and often leave scars. Herpetiform canker sores usually resolve within 1 to 4 weeks.
What foods should I avoid if I have a canker sore?
While you have a canker sore, avoid acidic foods (like citrus fruits, tomatoes), spicy foods, very hot foods, and abrasive or crunchy foods (like chips or toast). These can irritate the sore, increase pain, and delay healing.
Can stress cause canker sores?
Yes, stress is a well-known trigger for canker sores. Periods of high emotional or psychological stress can weaken the immune system or alter oral conditions, making you more susceptible to outbreaks. Managing stress through relaxation techniques can help reduce their frequency.
When should I worry about a canker sore?
You should see a dentist or doctor if a canker sore is unusually large, extremely painful, lasts longer than two weeks, recurs very frequently, or is accompanied by other symptoms like fever, diarrhea, rash, or difficulty swallowing.
Is it a canker sore or mouth herpes?
Canker sores appear inside the mouth on soft tissues (cheeks, tongue) and are not contagious. Mouth herpes (cold sores) are caused by the herpes virus, usually appear outside the mouth on the lips or on hard oral tissues (gums, hard palate), start as blisters, and are highly contagious. A dental professional can accurately diagnose the difference.
Can canker sores be a sign of something serious?
While most canker sores are harmless, recurrent or unusually severe outbreaks can sometimes be a symptom of an underlying systemic condition, such as inflammatory bowel disease (Crohn's, celiac), Behçet's disease, or nutritional deficiencies. Persistent non-healing sores should always be checked to rule out oral cancer.
Are there home remedies that actually work for canker sores?
Yes, some home remedies can help alleviate pain and promote healing. Rinsing with warm saltwater or a baking soda solution several times a day can soothe irritation and keep the area clean. Applying a small amount of milk of magnesia can also offer relief.
What is the fastest way to heal a canker sore?
For the fastest healing and pain relief, especially for persistent or painful sores, professional laser treatment is often highly effective, sometimes reducing healing time to just 1-3 days. Prescription topical corticosteroids can also significantly speed up the healing process compared to just waiting.
How much does laser treatment for a canker sore cost?
Laser treatment for a single canker sore typically costs between $100 and $400 per session in the US. This is usually an out-of-pocket expense as most dental and medical insurance plans do not cover it.
When to See a Dentist
While most minor canker sores resolve on their own with home care, there are specific situations where seeking professional dental attention is crucial. Don't hesitate to contact your dentist or doctor if you experience any of the following:
- Sores that are unusually large: Major aphthae are larger, deeper, and more painful, often requiring medical intervention to manage pain and prevent scarring.
- Sores that are unusually persistent: Any oral sore that lasts longer than two weeks should be evaluated. This is a red flag, as persistent lesions could indicate something more serious, including oral cancer.
- Sores that are extremely painful: If the pain is so severe that it interferes with eating, drinking, or speaking, and over-the-counter remedies aren't providing relief, a dentist can offer stronger treatments.
- Sores that recur frequently: If you get canker sores very often (e.g., several times a year, or new ones appear before old ones heal), it's important to investigate potential underlying causes, such as nutritional deficiencies or systemic diseases.
- Sores accompanied by other symptoms: If your canker sore is accompanied by fever, swollen lymph nodes, skin rash, headache, or gastrointestinal problems (like diarrhea or abdominal pain), it could be a sign of a systemic illness that needs medical diagnosis and treatment. This is especially true for children, where these symptoms could indicate stages of hand foot and mouth disease or other infections.
- Difficulty eating or drinking: If the pain prevents adequate nutritional or fluid intake, leading to weight loss or dehydration.
- Sores that look unusual: If the sore has an irregular border, appears very deep, or is in an atypical location (e.g., on the hard palate or gums, which might suggest mouth herpes or another condition), it warrants professional examination.
- Lack of improvement with self-care: If you've tried home remedies and OTC products for a week or more without any significant improvement, it's time to see a professional.
Timely consultation ensures proper diagnosis, effective pain management, and can identify any underlying health conditions that may be contributing to your canker sores. Your dentist can provide targeted treatments and guidance tailored to your specific situation.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles

Oral Candidiasis Symptoms: Complete Guide
Oral candidiasis, commonly known as oral thrush, is a fungal infection of the mouth caused by an overgrowth of Candida yeast, most often Candida albicans. While Candida is a normal inhabitant of the human mouth in small amounts, an imbalance can lead to uncomfortable and sometimes painful symptoms
February 23, 2026
Are Cold Sores Contagious
In the United States, an estimated 67% of the population under age 50 carries the herpes simplex virus type 1 (HSV-1), the primary cause of cold sores. This means millions of Americans are susceptible to these often painful and highly visible oral lesions. Beyond the discomfort and cosmetic conc
February 23, 2026
How Long Does Hand Foot and Mouth Last
Hand, Foot, and Mouth Disease (HFMD) is a common, often uncomfortable, viral illness that can affect anyone but is particularly prevalent among young children. If you or a loved one has ever experienced the tell-tale rash or painful mouth sores, you've likely wondered: **how long does Hand Foot and
February 23, 2026
Cold Sore vs Pimple on Lip: Complete Comparison Guide
When you notice an unexpected bump or lesion on your lip, your mind might immediately jump to questions of what it is, how long it will last, and most importantly, if it's contagious. The confusion between a cold sore vs pimple on lip is incredibly common, yet the distinction is crucial for prop
February 23, 2026