Does Osteoporosis Affect Your Teeth and Gums
Key Takeaways
- Osteoporosis, a silent disease characterized by progressive bone loss, is often associated with fractures of the hip, spine, and wrist. Yet, its reach extends beyond these commonly recognized areas, potentially impacting your oral health in significant and often overlooked ways. Many individuals, es
Osteoporosis, a silent disease characterized by progressive bone loss, is often associated with fractures of the hip, spine, and wrist. Yet, its reach extends beyond these commonly recognized areas, potentially impacting your oral health in significant and often overlooked ways. Many individuals, especially in the US where over 54 million people are affected by low bone mass or osteoporosis, are unaware of the profound connection between their skeletal health and the strength of their jawbones, the stability of their teeth, and the health of their gums. You might be asking, "does osteoporosis affect your teeth and gums?" The answer is a resounding yes, and understanding this relationship is crucial for maintaining both your bone density and your radiant smile.
This comprehensive guide from SmilePedia.net will delve into the intricate link between osteoporosis and oral health, exploring how diminishing bone density can compromise the very foundation supporting your teeth. We will uncover the specific ways osteoporosis can manifest in your mouth, from increased risk of periodontal disease to challenges with dental procedures. We'll also provide detailed insights into diagnostic methods, effective treatment strategies, preventive measures, and practical advice on what helps with tooth inflammation and inflammation gums home remedy. By the end of this article, you will have a clear roadmap to protect your oral health while managing osteoporosis.
Key Takeaways:
- Osteoporosis significantly impacts oral health by reducing jawbone density, increasing the risk of tooth loss and periodontal disease.
- Women, especially post-menopausal, are at higher risk due to hormonal changes affecting both systemic and oral bone health.
- Early signs of oral osteoporosis can include receding gums, loose teeth, and difficulty with dentures, often detectable during routine dental X-rays.
- Bisphosphonate medications, while effective for osteoporosis, carry a rare but serious risk of Osteonecrosis of the Jaw (ONJ), requiring careful dental and medical coordination.
- Treatment for osteoporosis-related oral issues can range from enhanced periodontal therapy ($200-$1,000 per quadrant) to bone grafting ($400-$1,500 per site) and modified dental implant protocols.
- Effective prevention involves a bone-healthy diet, adequate calcium and Vitamin D, regular exercise, excellent oral hygiene, and consistent dental check-ups (typically $75-$200 for a routine exam and cleaning without insurance).
- For gum inflammation, home remedies like saltwater rinses and diligent brushing can help, but persistent or severe inflammation warrants immediate professional dental evaluation.
Understanding Osteoporosis and Oral Health
To fully grasp how osteoporosis affects your teeth and gums, it's essential to first understand the disease itself and the fundamental connection between your systemic bone health and your oral structures.
What is Osteoporosis?
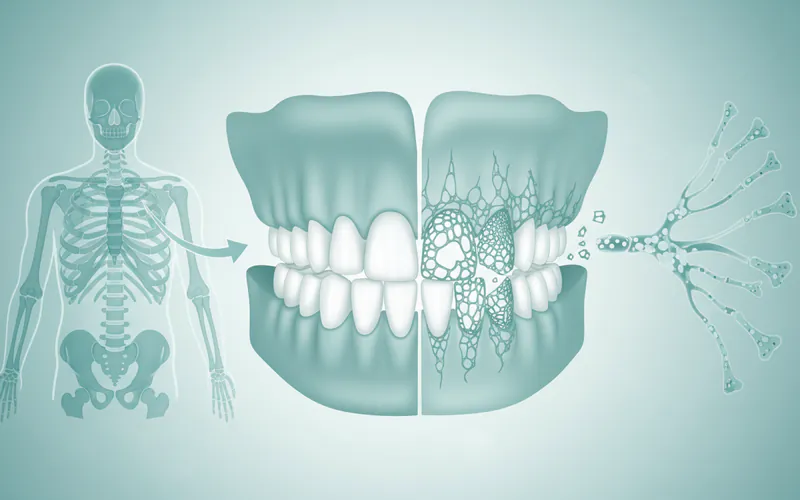
Osteoporosis, meaning "porous bone," is a condition characterized by a decrease in bone density and mass, leading to weakened bones that are more susceptible to fractures. Our bones are living tissues constantly undergoing a process called remodeling, where old bone is removed (resorption) and new bone is formed. In osteoporosis, the balance shifts, with more bone being lost than gained. This leads to bones becoming fragile and brittle over time.
According to the National Osteoporosis Foundation, approximately 10 million Americans have osteoporosis, and another 44 million have low bone density (osteopenia), placing them at increased risk. The disease is often called a "silent killer" because it typically has no symptoms until a fracture occurs. While commonly associated with hips, spine, and wrists, the bones of the jaw are just as susceptible to this systemic bone loss.
The Link Between Bone Health and Oral Health
The human jaw consists of two main bones: the maxilla (upper jaw) and the mandible (lower jaw). These bones contain the alveolar bone, which is the specialized bone tissue that surrounds and supports the roots of your teeth. The health and density of the alveolar bone are paramount for tooth stability. When systemic conditions like osteoporosis lead to a reduction in overall bone mineral density, the alveolar bone in your jaw is not immune.
Think of your teeth as trees planted in soil. If the soil (alveolar bone) becomes sparse and weak, the trees (teeth) will lose their firm anchor and become wobbly or even fall out. The same biological processes that govern bone density in your hips and spine also apply to your jaw. Calcium, phosphorus, vitamin D, and various hormones (like estrogen, parathyroid hormone, and calcitonin) play crucial roles in maintaining bone strength throughout the body, including the oral cavity. Any imbalance in these factors due to osteoporosis can directly compromise the structural integrity of your jawbones, creating a domino effect on your teeth and gums. This fundamental link is why dentists are increasingly vigilant about identifying potential signs of osteoporosis during routine oral examinations.
How Osteoporosis Specifically Impacts Your Teeth and Gums
The effects of osteoporosis on oral health are multifaceted, impacting everything from the integrity of your jawbone to the susceptibility of your gums to disease. Understanding these specific mechanisms helps clarify why does osteoporosis affect your teeth and gums is such a critical question.
Bone Loss in the Jaw: Alveolar Bone
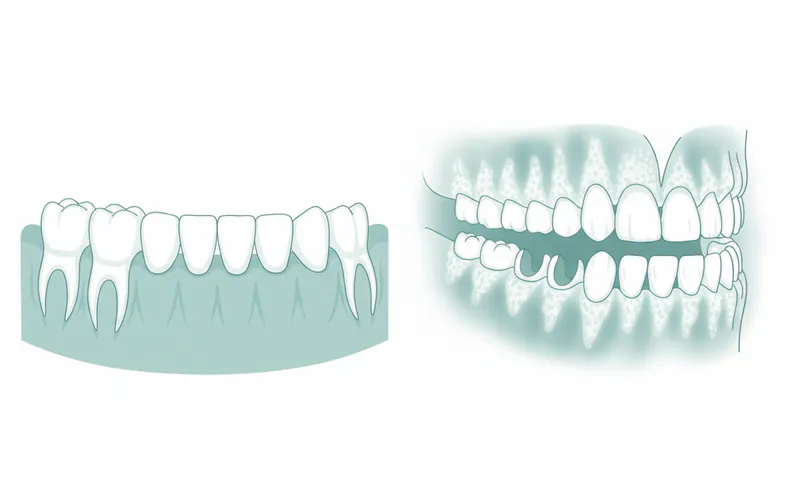
The alveolar bone is the crucial bony ridge that holds your tooth roots in place. In individuals with osteoporosis, the overall reduction in bone mineral density can lead to a significant decrease in the density and quantity of this alveolar bone. This weakened foundation can no longer adequately support the teeth, making them more vulnerable to shifting, loosening, and eventual loss.
Studies have shown that individuals with osteoporosis may experience a threefold increase in alveolar bone loss compared to those without the condition. This bone loss often manifests as a reduction in jaw height and width, which can be visible on dental X-rays. For patients who wear dentures, this diminished bone structure means there's less ridge to support the prosthesis, leading to ill-fitting dentures, discomfort, and difficulty eating and speaking. The progressive loss of alveolar bone mass due to osteoporosis makes it a primary concern for long-term tooth retention.
Increased Risk of Periodontal Disease
Periodontal disease, commonly known as gum disease, is an infection of the tissues that hold your teeth in place. It begins with gingivitis (inflammation of the gums) and, if left untreated, can progress to periodontitis, where the infection damages the bone and connective tissue supporting the teeth.
Osteoporosis doesn't directly cause periodontal disease, which is primarily initiated by bacterial plaque. However, it acts as a significant compounding factor. When the alveolar bone is already weakened by osteoporosis, it becomes less resistant to the inflammatory processes triggered by bacterial infection. The weakened bone provides a less stable environment, accelerating the progression of periodontitis and making it more aggressive. In essence, the osteoporotic bone becomes more susceptible to breakdown when confronted with the inflammation of gum disease, leading to faster attachment loss and deeper pockets around the teeth. Research indicates that women with osteoporosis are up to three times more likely to experience moderate to severe periodontal disease than those without the condition. This synergistic effect highlights the importance of rigorous oral hygiene and proactive dental care for individuals with osteoporosis.
Tooth Loss and Denture Complications
The combined effect of reduced alveolar bone density and an increased susceptibility to severe periodontal disease directly translates to a higher risk of tooth loss for individuals with osteoporosis. As the bone supporting the teeth deteriorates and gum disease advances, teeth lose their anchor and become mobile. Eventually, they may need to be extracted or can fall out spontaneously.
For patients who have already experienced tooth loss and rely on dentures, osteoporosis presents unique challenges. Dentures depend on the underlying jawbone ridge for stability and retention. When osteoporosis causes this bone to resorb or shrink, dentures that once fit perfectly can become loose, uncomfortable, and difficult to manage. This poor fit can lead to chronic irritation, sores, and further bone loss due to constant trauma. Adjusting or replacing dentures becomes a more frequent necessity, and in severe cases, adequate denture stability can become extremely difficult to achieve without surgical intervention.
Challenges with Oral Surgery and Implants
Oral surgical procedures, such as tooth extractions, bone grafting, and dental implant placement, require healthy, robust bone for successful outcomes. Osteoporosis can complicate all of these.
When bone density is significantly reduced, the healing process after extractions can be impaired, leading to slower recovery and increased risk of complications. Dental implants, which are titanium posts surgically placed into the jawbone to replace missing teeth, rely on a process called osseointegration, where the implant fuses directly with the surrounding bone. In osteoporotic bone, the success rates of implants can be lower, and the time required for osseointegration may be prolonged. The bone may simply not be dense enough to provide a stable foundation for the implant. Therefore, dentists must carefully evaluate a patient's bone density and systemic health before recommending implant procedures for individuals with osteoporosis. This often involves advanced imaging like 3D cone-beam CT scans to assess bone quality and quantity.
Signs and Symptoms of Osteoporosis Affecting Your Oral Health
Recognizing the oral manifestations of osteoporosis early can prompt timely intervention, potentially slowing progression and preserving oral health. While some signs are subtle, others are quite evident.
Receding Gums
One of the earliest and most common signs is gingival recession, where the gum tissue pulls back or wears away, exposing more of the tooth's root. While many factors can contribute to receding gums (such as aggressive brushing or periodontal disease), osteoporosis can exacerbate this condition by weakening the underlying bone that supports the gums. When the alveolar bone diminishes, the gum tissue has less foundation and may recede more easily, making teeth appear longer and increasing sensitivity.
Loose Teeth
As the alveolar bone that anchors your teeth begins to lose density and mass due to osteoporosis, your teeth can become mobile. You might notice a slight wiggle when you push on them, or they may shift when you chew. This looseness can range from mild to severe, and in advanced stages, teeth may feel like they are "floating" or even fall out. This is a direct consequence of the weakened bony support structure.
Difficulty with Dentures
If you wear dentures, a telltale sign of osteoporosis affecting your jawbone could be a progressive change in how your dentures fit. What once felt secure might now feel loose, slip frequently, or cause sore spots on your gums. This happens because the underlying jawbone, which provides the foundation for the denture, is slowly shrinking. As the bone resorbs, the shape of your jaw changes, making the denture no longer conform to the new contours, necessitating adjustments or even a complete replacement.
General Jaw Bone Weakness
Beyond the specific signs around teeth and gums, osteoporosis can lead to a generalized weakness in the jawbone. While not something you can typically feel directly, this can be observed on dental X-rays as a decrease in bone density or a more porous appearance of the bone. This weakness makes the jaw more susceptible to fractures from minor trauma and can complicate any necessary dental procedures that involve the bone.
Pro Tip: If you're experiencing any of these symptoms, especially if you have a diagnosis of osteoporosis, inform your dentist immediately. Early detection and communication between your dental and medical teams are key to managing these challenges.
Diagnosing Oral Manifestations of Osteoporosis
Identifying the impact of osteoporosis on your oral health often involves a combination of routine dental examinations and specific diagnostic tools.
Dental X-rays and Bone Density
Routine dental X-rays, such as panoramic X-rays or periapical films, can provide valuable clues about the density of your jawbone. While not as precise as a medical DEXA scan (dual-energy X-ray absorptiometry) for diagnosing systemic osteoporosis, dentists can observe specific features. These include:
- Reduced bone height: The distance between the roots of your teeth and the lower border of your jawbone may decrease.
- Increased radiolucency: The bone may appear darker or more "washed out" on the X-ray, indicating lower density.
- Changes in trabecular pattern: The fine, lacy network of bone within the jaw might appear less dense or coarse.
- Thinning of the cortical bone: The outer layer of the jawbone, particularly at the lower border of the mandible, may appear thinner.
- Panoramic X-rays can sometimes reveal calcifications in the carotid arteries, which may be a sign of increased risk for cardiovascular disease, a condition that shares risk factors with osteoporosis.
When these signs are observed, especially in patients with known risk factors for osteoporosis (e.g., post-menopausal women, individuals on certain medications), your dentist may recommend further medical evaluation, including a DEXA scan, to confirm a systemic diagnosis.
Periodontal Probing
During a routine dental check-up, your dentist or dental hygienist will use a small measuring probe to assess the depth of the pockets around your teeth. Healthy gum pockets are typically 1-3 millimeters deep. Deeper pockets (4mm or more) indicate periodontal disease, which, as discussed, can be exacerbated by osteoporosis. Along with probing depths, the dental professional will check for gum inflammation, bleeding, and any signs of receding gums or tooth mobility. Consistent findings of deeper pockets and significant attachment loss, particularly when bone density is visually reduced on X-rays, strongly suggest a link between your systemic bone health and oral disease.
Referral to a Physician
If your dentist identifies oral signs highly suggestive of osteoporosis, they will likely recommend a referral to your primary care physician or an endocrinologist. This is crucial because a dental office cannot formally diagnose systemic osteoporosis. The medical professional can then order a DEXA scan, blood tests (to check calcium, vitamin D, and hormone levels), and other necessary evaluations to confirm a diagnosis or adjust existing osteoporosis management plans. This collaborative approach between your dental and medical care providers ensures comprehensive treatment for your overall health.
Treatment and Management Strategies
Managing the oral health implications of osteoporosis requires a coordinated approach that addresses both the systemic bone condition and its local effects in the mouth.
Medical Treatments for Osteoporosis
The primary goal of medical treatment for osteoporosis is to slow bone loss, increase bone density, and reduce the risk of fractures. These treatments can have a profound impact on maintaining jawbone health. Common medications include:
- Bisphosphonates: Such as alendronate (Fosamax), risedronate (Actonel), and zoledronic acid (Reclast). These drugs work by inhibiting osteoclasts, the cells that break down bone, thereby reducing bone resorption.
- Denosumab (Prolia): A monoclonal antibody that also inhibits osteoclasts, similar to bisphosphonates but with a different mechanism of action.
- Hormone Therapy: Estrogen therapy can help prevent bone loss in post-menopausal women, though it's typically prescribed for short durations due to other health risks.
- Anabolic Agents: Such as teriparatide (Forteo) and romosozumab (Evenity), which stimulate new bone formation. These are usually reserved for severe cases.
Bisphosphonates and Oral Health Considerations
While highly effective in treating osteoporosis, bisphosphonate medications, particularly those administered intravenously (IV), carry a rare but serious risk of Medication-Related Osteonecrosis of the Jaw (MRONJ), previously known as Bisphosphonate-Related Osteonecrosis of the Jaw (BRONJ). MRONJ is a condition characterized by exposed bone in the jaw that fails to heal for more than eight weeks following minor trauma (like a tooth extraction) or spontaneously.
The risk of MRONJ is significantly higher with IV bisphosphonates (used for cancer patients to manage bone metastases) than with oral bisphosphonates (used for osteoporosis). For individuals on oral bisphosphonates, the risk is extremely low (estimated at 0.1% or less), but it's still a critical consideration.
Key considerations for patients on bisphosphonates:
- Inform your dentist: Always disclose your medication history, including bisphosphonates, to your dental team.
- Proactive Dental Care: Maintain excellent oral hygiene to minimize the need for invasive dental procedures, especially extractions.
- Timing of Invasive Procedures: If an invasive procedure (like an extraction) is necessary, your dentist and physician may discuss a "drug holiday" (temporarily stopping the medication) or alternative strategies to minimize risk, although the effectiveness of drug holidays is debated and should only be done under medical supervision.
- Ongoing Monitoring: Regular dental check-ups are vital for early detection of any oral issues.
Dental Treatments for Associated Oral Issues
Beyond managing systemic osteoporosis, specific dental treatments address the oral complications that arise.
-
Enhanced Periodontal Therapy: Given the increased susceptibility to periodontitis, aggressive and consistent periodontal therapy is crucial. This includes:
- Scaling and Root Planing (Deep Cleaning): Removes plaque and tartar from above and below the gum line, smoothing root surfaces to reduce bacterial accumulation. This may cost $200-$1,000 per quadrant without insurance, depending on severity and region.
- Antibiotics: Localized antibiotic gels or systemic antibiotics may be used to target specific bacteria.
- Periodontal Maintenance: More frequent recall appointments (every 3-4 months instead of 6) are often recommended to monitor gum health and prevent recurrence.
- Laser Therapy: Sometimes used as an adjunct to traditional scaling and root planing to reduce bacteria and inflammation.
-
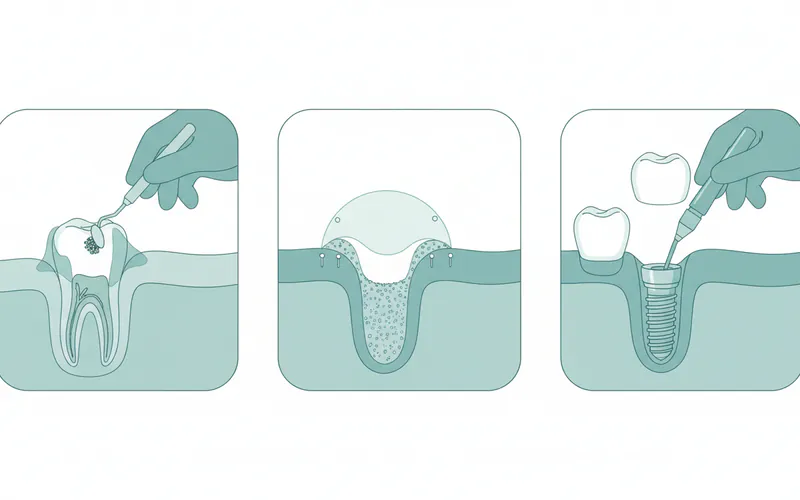
Bone Grafting: If significant jawbone loss has occurred, bone grafting procedures may be necessary to rebuild the bone structure. This is often done to prepare the jaw for dental implants or to provide better support for dentures. Materials for grafting can come from your own body, a donor, or synthetic sources. Costs for bone grafting vary significantly, typically ranging from $400-$1,500 per site.
-
Dental Implants (with precautions): While possible, implant placement in osteoporotic bone requires careful planning.
- Thorough Evaluation: Advanced imaging (CBCT scans) and assessment of bone density are paramount.
- Potential for Longer Healing: Osseointegration may take longer, and a longer healing period before loading the implant may be advised.
- Medication Review: A thorough review of osteoporosis medications (especially bisphosphonates) is critical to assess MRONJ risk before implant surgery. In some cases, a medical consultation regarding a "drug holiday" may be considered, though it's a complex decision.
- Cost: Single dental implants typically range from $3,000-$6,000 per tooth (including abutment and crown), with bone grafting adding to the total.
-
Denture Adjustments/Replacements: For patients with ill-fitting dentures due to jawbone changes, regular relining or rebasing of the denture is essential. In cases of significant bone loss, new dentures may be fabricated, or implant-supported overdentures (dentures anchored by a few strategically placed implants) might be an option to provide greater stability and comfort, albeit at a higher cost. A denture reline usually costs $200-$400, while new dentures can range from $1,000-$3,000 per arch.
Comparison of Dental Interventions for Osteoporosis-Related Issues
To help you understand the options, here's a comparison of common dental interventions for issues exacerbated by osteoporosis.
| Treatment Option | Primary Goal | Typical Cost (US, without insurance) | Approximate Timeline | Pros | Cons |
|---|---|---|---|---|---|
| Scaling & Root Planing | Reduce inflammation, remove bacteria, treat periodontal disease | $200-$1,000 per quadrant | 1-2 appointments (1-2 hours each) | Non-surgical, highly effective for early-moderate gum disease, preserves natural teeth | May require multiple visits, not suitable for advanced bone loss, regular maintenance needed |
| Bone Grafting | Rebuild jawbone volume and density | $400-$1,500 per site | 1-2 hours surgery, 4-9 months healing | Creates foundation for implants/dentures, improves facial aesthetics | Invasive surgical procedure, significant healing time, potential for complications, added cost |
| Dental Implant Placement | Replace missing teeth with stable, long-lasting solution | $3,000-$6,000 per tooth | 3-9 months (surgery to crown) | High success rate in healthy bone, preserves adjacent teeth, excellent function and aesthetics | Surgical, higher cost, longer treatment time, increased risk in osteoporotic bone (MRONJ concern) |
| Denture Relining/Replacement | Improve fit and comfort of existing/new dentures | $200-$400 (reline), $1,000-$3,000 (new) | 1-2 visits (reline), 3-5 visits (new) | Non-invasive (reline), restores function and aesthetics, affordable option for tooth replacement | Less stable than implants, ongoing adjustments may be needed, does not prevent bone loss |
Preventing Oral Complications of Osteoporosis
Prevention is always better than cure, especially when it comes to the complex interplay between osteoporosis and oral health. A proactive approach can significantly reduce your risk of complications.
Optimizing Bone Health
The most direct way to prevent oral complications from osteoporosis is to manage the underlying systemic condition. This includes:
- Regular Medical Check-ups: Ensure your osteoporosis is being actively monitored and treated by your physician.
- Adherence to Medication: Take any prescribed osteoporosis medications exactly as directed.
- Bone Density Screenings: Regular DEXA scans help track bone density changes and effectiveness of treatment.
- Avoid Smoking and Excessive Alcohol: Both habits are known to impair bone formation and accelerate bone loss, exacerbating osteoporosis and increasing the risk of periodontal disease.
Excellent Oral Hygiene
Maintaining meticulous oral hygiene is paramount for individuals with osteoporosis to mitigate the increased risk of periodontal disease.
- Brush Twice Daily: Use a soft-bristled toothbrush and fluoride toothpaste. Brush gently but thoroughly for two minutes each time, reaching all tooth surfaces and along the gum line. Consider an electric toothbrush for enhanced plaque removal.
- Floss Daily: Flossing removes plaque and food particles from between teeth and under the gum line, areas your toothbrush can't reach. This is critical for preventing gum inflammation and periodontal disease.
- Antiseptic Mouthwash: Using an ADA-accepted antiseptic mouthwash can help reduce bacterial load in your mouth, providing an extra layer of protection against gum disease.
- Tongue Cleaning: Gently brush or scrape your tongue to remove bacteria and freshen breath.
Regular Dental Check-ups
Consistent dental visits are crucial for early detection and intervention.
- Bi-annual Exams: Schedule professional cleanings and examinations at least twice a year, or more frequently if recommended by your dentist due to periodontal concerns. During these visits, your dentist will:
- Examine your gums for signs of inflammation, recession, and pocketing.
- Assess tooth mobility.
- Review your dental X-rays for changes in jawbone density.
- Screen for any other oral health issues.
- Communicate with Your Dentist: Always inform your dentist about your osteoporosis diagnosis, any medications you are taking (especially bisphosphonates), and any changes in your overall health. This information allows your dental team to tailor your care plan and monitor for specific risks.
- Average Cost: A routine dental exam and cleaning typically costs $75-$200 without insurance, while a full set of X-rays might add $50-$150.
Diet and Supplements
Nutrition plays a vital role in bone health.
- Calcium: Ensure adequate dietary intake of calcium-rich foods such as dairy products, fortified plant milks, leafy greens (kale, spinach), and fortified cereals. The recommended daily intake for adults is typically 1,000-1,200 mg.
- Vitamin D: Vitamin D is essential for calcium absorption. Good sources include fatty fish (salmon, mackerel), fortified foods, and sunlight exposure. Many individuals require vitamin D supplements. The recommended daily intake is 600-800 IU, but some with osteoporosis may need more, as determined by their physician.
- Other Nutrients: Magnesium, Vitamin K, and phosphorus also contribute to bone health. A balanced diet rich in fruits, vegetables, and whole grains supports overall health, including bone density.
Home Remedies and Supportive Care for Gum Inflammation
Even with diligent care, individuals with osteoporosis may experience episodes of gum inflammation due to their increased susceptibility. Knowing what helps with tooth inflammation and effective inflammation gums home remedy options can provide relief and support professional treatment.
Effective Home Practices
These home remedies can help manage mild gum inflammation (gingivitis) and reduce discomfort:
- Saltwater Rinses: One of the simplest and most effective home remedies. Mix 1/2 teaspoon of salt in 8 ounces of warm water. Swish for 30 seconds and spit, repeating 2-3 times a day. Saltwater acts as a natural disinfectant, reduces inflammation, and can help heal irritated gum tissue.
- Good Oral Hygiene: As emphasized earlier, consistent and gentle brushing and flossing are paramount. Removing plaque is the primary way to reduce inflammation. Use a soft-bristled brush to avoid irritating already sensitive gums.
- Warm Compresses: For localized pain or swelling, a warm, moist compress applied to the outside of your cheek can provide temporary relief.
- Herbal Rinses: Some studies suggest that rinses made with certain herbs like aloe vera, chamomile, or tea tree oil may have anti-inflammatory and antimicrobial properties. Always dilute essential oils and ensure they are safe for oral use.
- Over-the-Counter Pain Relievers: Non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen can help manage pain and reduce inflammation in the short term. Always follow dosage instructions.
When Home Remedies Aren't Enough
While home remedies can offer temporary relief and support, they are not a substitute for professional dental care, especially if you have osteoporosis.
- If gum inflammation persists for more than a few days, worsens, or is accompanied by severe pain, bleeding, pus, or tooth mobility, it's crucial to see your dentist immediately.
- These symptoms could indicate a progression to periodontitis, which requires professional scaling and root planing, and potentially other advanced treatments.
- Delaying professional treatment when you have osteoporosis can lead to accelerated bone loss, increased risk of tooth loss, and more complex, costly interventions down the line.
Pro Tip: For mild gum discomfort, try a warm saltwater rinse multiple times a day. However, if symptoms don't improve within 2-3 days, or if they are severe, schedule an appointment with your dentist promptly.
Risks and Complications
Understanding the potential risks and complications associated with osteoporosis and its treatment, particularly concerning oral health, is crucial for informed decision-making and preventive care.
Osteonecrosis of the Jaw (MRONJ)
As discussed earlier, Medication-Related Osteonecrosis of the Jaw (MRONJ) is the most serious and well-known oral complication associated with osteoporosis medications, particularly bisphosphonates and denosumab. It involves the painful exposure and death of jawbone tissue, often triggered by minor dental procedures (like extractions) or appearing spontaneously.
- Risk Factors: Higher doses and longer duration of medication use (especially IV bisphosphonates), existing periodontal disease, poor oral hygiene, smoking, and diabetes increase the risk.
- Symptoms: Exposed bone in the mouth, pain, swelling, numbness, infection, or loosening teeth.
- Management: Treatment involves managing pain, controlling infection (antibiotics), and often conservative surgical removal of the affected bone. Prevention through meticulous oral hygiene and careful dental planning for patients on these medications is paramount.
Increased Infection Risk
Individuals with osteoporosis, especially those with advanced disease or compromised immune systems (which can sometimes co-occur), may have an increased susceptibility to oral infections. Periodontal disease itself is an infection, and the weakened bone structure can make it harder for the body to fight off the invading bacteria effectively. This can lead to more aggressive and rapid progression of gum disease, potentially resulting in abscesses and widespread infection.
Implant Failure
While dental implants can be a viable option for replacing missing teeth, osteoporosis, especially if not well-controlled, can increase the risk of implant failure.
- Poor Osseointegration: The weakened and less dense bone may not integrate successfully with the titanium implant, leading to instability.
- Perii-Implantitis: Similar to periodontitis, an infection around the implant (perii-implantitis) can lead to bone loss around the implant, ultimately causing it to loosen and fail. Individuals with osteoporosis may be more susceptible to this inflammatory response.
- Mechanical Failure: The compromised bone may not be strong enough to withstand the biting forces, leading to mechanical stress and eventual failure of the implant.
Close collaboration between your dentist, oral surgeon, and physician is essential to assess these risks and determine the most appropriate treatment plan if dental implants are being considered.
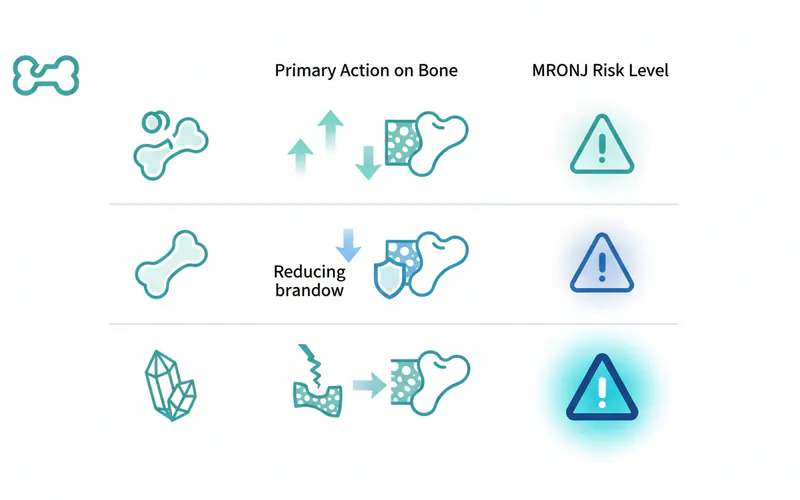
Comparison of Osteoporosis Medications and Their Oral Impact
Here's a simplified comparison of common osteoporosis medication classes and their general impact on oral health, particularly concerning MRONJ risk. This is a generalization, and individual cases may vary.
| Medication Class | Examples | Mechanism of Action | Primary Use | MRONJ Risk (General) | Key Oral Health Considerations |
|---|---|---|---|---|---|
| Oral Bisphosphonates | Alendronate, Risedronate, Ibandronate | Decrease bone breakdown (osteoclast inhibition) | Osteoporosis treatment | Very Low (0.01% - 0.1%) | Must inform dentist; maintain excellent oral hygiene; caution with extractions |
| IV Bisphosphonates | Zoledronic Acid (higher doses) | Decrease bone breakdown (stronger inhibition) | Cancer bone metastases, severe osteoporosis | Moderate-High (1% - 15% in cancer patients) | High vigilance; pre-treatment dental clearance; meticulous follow-up; significant MRONJ risk |
| Denosumab (Prolia) | Denosumab | Monoclonal antibody, inhibits osteoclasts | Osteoporosis treatment | Low (similar to oral bisphosphonates, but continuous) | Similar to bisphosphonates, but drug holiday not as straightforward; continuous risk with therapy |
| Teriparatide (Forteo) | Teriparatide | Anabolic, builds new bone | Severe osteoporosis | Extremely Low/Not established (no increased risk) | Generally considered safe for oral procedures; may even improve bone healing |
| Romosozumab (Evenity) | Romosozumab | Anabolic, builds new bone & reduces breakdown | Severe osteoporosis | Low (less than bisphosphonates, but observed in trials) | New medication, ongoing monitoring; caution with invasive procedures, less data than bisphosphonates |
| Hormone Therapy (Estrogen) | Estradiol | Replaces estrogen, reduces bone loss | Post-menopausal osteoporosis | Not increased (no direct link to MRONJ) | Generally safe for oral health; may indirectly support bone health |
Cost Breakdown
Understanding the costs associated with managing osteoporosis and its oral manifestations is crucial for financial planning, especially for those without comprehensive dental insurance. Prices can vary significantly based on geographic location, the specific dental provider, the complexity of the procedure, and whether any specialists are involved.
Average US Costs (Low, Mid, High)
Here's a general overview of common dental procedures related to osteoporosis, with typical cost ranges without insurance:
- Routine Dental Exam & Cleaning:
- Low: $75
- Mid: $150
- High: $250
- Full Mouth Dental X-rays:
- Low: $50
- Mid: $100
- High: $150
- Scaling and Root Planing (Deep Cleaning) per Quadrant:
- Low: $200
- Mid: $400
- High: $1,000+ (for complex cases or multiple visits)
- Bone Grafting per Site:
- Low: $400
- Mid: $800
- High: $1,500+ (depending on material and complexity)
- Single Dental Implant (Post, Abutment, Crown):
- Low: $3,000
- Mid: $4,500
- High: $6,000+ (does not include grafting)
- Denture Reline (Hard):
- Low: $200
- Mid: $300
- High: $400
- New Full Denture (per arch):
- Low: $1,000
- Mid: $2,000
- High: $3,000+ (for premium materials or custom fits)
With vs. Without Insurance
- With Insurance: Most dental insurance plans offer coverage for preventive care (exams, cleanings, X-rays) at 80-100%. Basic restorative procedures (fillings, extractions) may be covered at 50-80%. Major procedures (periodontal surgery, bone grafting, implants, dentures) often have lower coverage, typically 20-50%, and are subject to annual maximums (often $1,000-$2,000). You will pay the deductible and co-pay/co-insurance.
- Without Insurance: You are responsible for 100% of the costs. This is where the listed ranges apply. It's why many people seek out dental discount plans or consider payment options.
Payment Plans and Financing Options
- In-Office Payment Plans: Many dental offices offer their own payment plans for larger treatments, often requiring an initial down payment and then monthly installments.
- Third-Party Financing: Companies like CareCredit or LendingClub offer specialized healthcare credit cards with deferred interest or low-interest payment options for medical and dental expenses.
- Dental Schools: University dental schools often provide services at a reduced cost, as procedures are performed by students under the supervision of experienced faculty. This can be a significantly more affordable option, though appointment availability and treatment timelines might be longer.
- Community Health Centers: Federally qualified health centers (FQHCs) and other community clinics often provide dental care on a sliding scale based on income.
Cost-Saving Tips
- Prioritize Prevention: Regular cleanings and good home care are the most cost-effective ways to avoid expensive treatments down the line.
- Dental Discount Plans: These are not insurance but offer a percentage discount on services from participating dentists for an annual fee.
- Discuss Options with Your Dentist: Ask about different treatment approaches and their associated costs. Sometimes, a less expensive alternative might be available.
- Inquire About Senior Discounts: Some dental practices offer discounts for senior citizens.
Frequently Asked Questions
Is it safe to get dental implants if I have osteoporosis?
Yes, it can be safe, but it requires careful evaluation and planning. Your dentist or oral surgeon will assess your jawbone density using X-rays or a CBCT scan and review your medical history, especially any osteoporosis medications you're taking. They may recommend bone grafting to improve bone quality before implant placement. Success rates can be slightly lower than in individuals with healthy bone density, and healing times might be longer.
What are the earliest signs of osteoporosis affecting my mouth?
The earliest signs often include receding gums, increased tooth mobility (feeling like teeth are loose), and difficulty with the fit of existing dentures. You might also notice more frequent gum inflammation or slower healing after minor dental procedures. Dental X-rays may reveal a subtle decrease in jawbone density.
Can osteoporosis cause my teeth to fall out?
While osteoporosis doesn't directly cause teeth to fall out, it significantly increases the risk. By weakening the alveolar bone that supports your teeth, it makes them more susceptible to loss, especially when combined with periodontal disease. The reduced bone density creates an unstable foundation, leading to tooth mobility and eventual loss if not managed.
What home remedies can help with gum inflammation if I have osteoporosis?
For mild gum inflammation, a warm saltwater rinse (1/2 teaspoon salt in 8 ounces of warm water, swished 2-3 times daily) can be very effective due to its antiseptic and anti-inflammatory properties. Maintaining diligent oral hygiene, including gentle brushing and daily flossing, is also crucial. However, persistent or severe inflammation warrants professional dental attention.

Do osteoporosis medications affect dental procedures?
Yes, certain osteoporosis medications, particularly bisphosphonates (both oral and intravenous) and denosumab, can impact dental procedures due to the rare risk of Medication-Related Osteonecrosis of the Jaw (MRONJ). It is vital to inform your dentist about all medications you are taking, especially before any invasive procedures like tooth extractions or implant placement.
How often should I see my dentist if I have osteoporosis?
It is generally recommended for individuals with osteoporosis to have dental check-ups and professional cleanings every six months, or even more frequently (e.g., every three to four months) if you have signs of periodontal disease or other oral health concerns. Regular visits allow your dentist to monitor your jawbone health and address any issues promptly.
Is osteoporosis related to periodontal disease?
Osteoporosis doesn't cause periodontal disease, which is primarily bacterial. However, it acts as a significant risk factor, accelerating the progression and severity of periodontal disease. The weakened jawbone due to osteoporosis becomes less resistant to the inflammation and bone destruction caused by gum infection, leading to faster attachment loss and deeper pockets.
Can a dentist diagnose osteoporosis from an X-ray?
A dentist cannot definitively diagnose systemic osteoporosis from a dental X-ray, as a medical DEXA scan is required for that. However, dentists can observe signs suggestive of reduced bone density in the jaw (like thinning jawbone, changes in bone pattern) and may be the first to recommend a medical evaluation with your physician if they notice these indicators.
When to See a Dentist
Given the significant link between osteoporosis and oral health, knowing when to seek professional dental care is paramount. Don't wait for severe pain or major complications.
Schedule a routine check-up and inform your dentist about your osteoporosis diagnosis if:
- You have recently been diagnosed with osteoporosis or osteopenia.
- You are starting or have changed medications for osteoporosis (especially bisphosphonates or denosumab).
- You haven't had a dental check-up in the last six months to a year.
- You want to discuss preventive strategies tailored to your condition.
See your dentist promptly (within a few days) if you notice any of these warning signs:
- Persistent gum inflammation or bleeding: Gums that are consistently red, swollen, or bleed easily, especially if not improving with diligent home care.
- Receding gums: Gums that appear to be pulling away from your teeth, making them look longer.
- Loose or shifting teeth: Any noticeable movement of your teeth when chewing or pushing on them, or if your bite feels different.
- Ill-fitting dentures: If your dentures suddenly feel loose, uncomfortable, or cause sore spots, requiring frequent adjustments.
- Persistent jaw pain or discomfort: Any ongoing pain in your jaw that doesn't resolve.
Seek immediate emergency dental care if you experience:
- Severe, sudden toothache or jaw pain.
- Swelling in your face or jaw that is rapidly spreading or affecting your breathing.
- Exposed bone in your mouth, especially after a recent dental procedure (a potential sign of MRONJ).
- Signs of an abscess (a pimple-like bump on your gums, pus discharge, severe throbbing pain).
Your dental team is a crucial partner in managing your overall health, particularly when you have osteoporosis. Regular communication and proactive care can help preserve your oral health and quality of life.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Does Oil Pulling Help Gut Health
The intricate connection between our oral health and overall well-being is a topic of growing fascination and scientific inquiry. Often, when we think of health, we focus on specific organs or systems, overlooking the crucial role of the mouth as a gateway to the rest of the body. One ancient practi
February 23, 2026
Does Oil Pulling Help With Inflammation
It's a question many health-conscious individuals ask as they explore natural remedies: does oil pulling help with inflammation? In an era where holistic approaches to wellness are gaining traction, the ancient practice of oil pulling has resurfaced, promising benefits that extend beyond oral hy
February 23, 2026
Oil Pulling for Kidney Disease: Complete Guide
Chronic kidney disease (CKD) affects an estimated 37 million adults in the United States, often progressing silently until advanced stages. What many may not realize is the profound connection between the health of their mouth and the health of their kidneys. As a bridge between traditional wisd
February 23, 2026
Oil Pulling Oral Microbiome: Complete Guide
Have you ever considered the bustling universe thriving within your mouth? This intricate community, known as the oral microbiome, consists of billions of microorganisms – some beneficial, some harmful – all playing a critical role in your oral and overall systemic health. Maintaining a balanced
February 23, 2026