Tooth Inflammation: Complete Guide
Key Takeaways
- A persistent dull ache, a throbbing pain that keeps you awake at night, or gums that bleed every time you brush – these are often more than just minor irritations. They are frequently red flags indicating tooth inflammation, a common yet serious condition affecting millions of Americans. Data fr
A persistent dull ache, a throbbing pain that keeps you awake at night, or gums that bleed every time you brush – these are often more than just minor irritations. They are frequently red flags indicating tooth inflammation, a common yet serious condition affecting millions of Americans. Data from the Centers for Disease Control and Prevention (CDC) reveals that approximately 47.2% of adults aged 30 years and older have some form of periodontal disease, a major contributor to inflammation in the mouth. Understanding tooth inflammation is crucial because if left unaddressed, it can lead to severe pain, tooth loss, and even systemic health complications impacting your heart, brain, and overall well-being.
This comprehensive guide from SmilePedia.net will demystify tooth inflammation, exploring its various forms, underlying causes, unmistakable signs, and the array of effective treatment options available. We'll delve into what to expect during treatment, recovery, and most importantly, how to prevent this often-painful condition. By the end of this article, you will be equipped with the knowledge to recognize the early warnings of inflammation in your mouth and take proactive steps to safeguard your oral and systemic health.
Key Takeaways:
- Definition: Tooth inflammation refers to the body's protective response to irritation, infection, or injury affecting the dental pulp (inside the tooth) or the surrounding gums and supporting structures.
- Common Causes: Dental cavities, gum disease (gingivitis, periodontitis), tooth trauma, cracks, and aggressive brushing are leading culprits.
- Symptoms: Look out for persistent pain (sharp, dull, throbbing), sensitivity to hot/cold, swelling in gums or face, bleeding gums, bad breath, and changes in tooth color.
- Treatment Options: Range from simple fillings (costing $75-$250) and deep cleanings ($200-$600 per quadrant) to root canal therapy ($700-$2,000) or extractions ($75-$400), depending on severity.
- Prevention is Key: Daily brushing, flossing, regular dental check-ups (typically $100-$300 without insurance for exam and cleaning), and a balanced diet can prevent most cases.
- Timeliness: Early intervention is critical. Delaying treatment can lead to more complex procedures, higher costs, and increased risk of infection spreading, potentially requiring weeks of recovery instead of days.
- Systemic Link: Oral inflammation is strongly linked to systemic conditions like heart disease, diabetes, and respiratory issues, underscoring its importance for overall health.
What It Is / Overview
Tooth inflammation, medically known as pulpitis when it affects the inside of the tooth, or a component of gingivitis and periodontitis when it affects the surrounding gum tissues, is your body's natural response to injury, irritation, or infection. This intricate process is designed to protect and heal, but when it occurs within the confined spaces of a tooth or chronically in the gums, it can cause significant pain and damage.

At its core, inflammation involves a cascade of biological events: blood vessels dilate, increasing blood flow to the affected area; immune cells rush in to combat pathogens or clear damaged tissue; and chemical mediators are released, causing redness, swelling, heat, and pain.
When inflammation impacts the dental pulp – the soft tissue deep inside your tooth containing nerves, blood vessels, and connective tissue – it is specifically termed pulpitis. The pulp is encased by hard dentin and enamel, leaving little room for swelling. This confinement intensifies pressure on the nerves, leading to the characteristic pain associated with toothaches.
Similarly, inflammation of the gums is called gingivitis, and if left untreated, it can progress to periodontitis, a more severe form of inflammation that affects the bone and ligaments supporting the teeth. Both pulpitis and periodontal inflammation are crucial indicators that something is amiss and require prompt dental attention. Ignoring these signs can lead to irreversible damage, including tooth loss and the spread of infection to other parts of the body.
Types / Variations
Tooth inflammation manifests in several distinct forms, depending on the specific tissues affected and the severity of the condition. Understanding these types is crucial for accurate diagnosis and effective treatment.
Pulpitis (Inflammation of the Dental Pulp)
Pulpitis is the inflammation of the dental pulp, the innermost part of the tooth. It is primarily categorized into two types:
-
Reversible Pulpitis: This is the milder form, where the pulp is irritated but healthy enough to recover once the irritant is removed.
- Causes: Mild tooth decay, minor trauma, recent dental work (like a new filling), or exposed dentin due to gum recession.
- Symptoms: Brief, sharp pain or sensitivity to hot, cold, or sweet stimuli that quickly subsides once the stimulus is removed. The pain does not linger.
- Treatment: Addressing the underlying cause, such as repairing a cavity with a filling, sealing exposed dentin, or adjusting a high filling. Prognosis is excellent.
-
Irreversible Pulpitis: This is a more severe form where the pulp is extensively damaged and cannot heal, even if the cause is removed. It's often the precursor to a dental abscess.
- Causes: Deep, untreated dental decay, severe tooth trauma (cracks, fractures), extensive restorative procedures, or repeated dental treatments on the same tooth.
- Symptoms: Intense, spontaneous, and lingering pain that may persist for minutes or hours after exposure to hot or cold. The pain often radiates, wakes you at night, and may be exacerbated by lying down. Pressure or chewing can also trigger discomfort.
- Treatment: Root canal therapy to remove the infected pulp and save the tooth, or tooth extraction if the tooth is beyond repair. Left untreated, it will invariably lead to pulp necrosis (death of the pulp tissue) and potentially a periapical abscess.
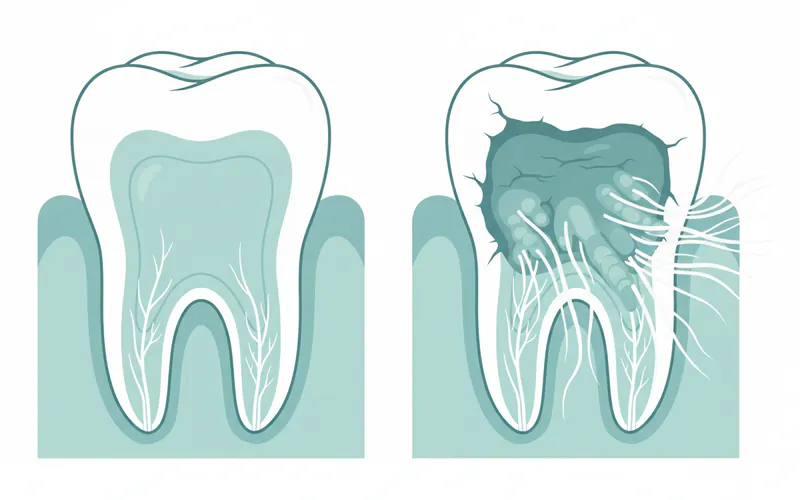
Periodontal Inflammation (Gingivitis and Periodontitis)
This category refers to the inflammation of the tissues surrounding and supporting the teeth.
-
Gingivitis: This is the earliest and mildest form of gum disease, characterized by inflammation of the gingiva (gums).
- Causes: Primarily caused by the accumulation of plaque (a sticky film of bacteria) and tartar (hardened plaque) on the teeth, leading to bacterial irritation.
- Symptoms: Red, swollen, tender, or bleeding gums, especially during brushing or flossing. Mild bad breath may also be present. There is typically no bone loss at this stage.
- Treatment: Professional dental cleaning (prophylaxis) to remove plaque and tartar, coupled with improved daily oral hygiene (brushing and flossing). Gingivitis is reversible.
-
Periodontitis: If gingivitis is left untreated, it can progress to periodontitis, a more severe and destructive form of gum disease.
- Causes: Chronic bacterial infection and inflammation that extends below the gum line, affecting the supporting bone and ligaments. Genetic factors, smoking, diabetes, and certain medications can also increase risk.
- Symptoms: Beyond the symptoms of gingivitis, periodontitis involves receding gums, persistent bad breath (halitosis), pus between teeth and gums, changes in bite, loose teeth, and eventually, tooth loss due to destruction of the supporting bone. Pockets form between the gums and teeth where bacteria thrive.
- Treatment: Deep cleaning (scaling and root planing) to remove plaque and tartar from below the gum line, antibiotics (oral or topical), and in advanced cases, surgical interventions (pocket reduction surgery, bone grafts, soft tissue grafts). Periodontitis is manageable but often not fully reversible in terms of bone loss.
Other Forms of Oral Inflammation
-
Pericoronitis: Inflammation of the gum tissue around a partially erupted tooth, most commonly wisdom teeth.
- Causes: Food impaction, bacterial accumulation, and trauma from biting on the flap of gum tissue.
- Symptoms: Pain, swelling, redness around the affected tooth, difficulty opening the mouth (trismus), and sometimes pus or fever.
- Treatment: Irrigation, antibiotics, professional cleaning, and potentially extraction of the wisdom tooth.
-
Alveolar Osteitis (Dry Socket): Inflammation of the bone after a tooth extraction.
- Causes: The blood clot at the extraction site dislodges or dissolves prematurely, exposing the underlying bone and nerves.
- Symptoms: Intense, throbbing pain days after extraction, bad breath, and a foul taste.
- Treatment: Cleaning the socket, placing medicated dressings, pain medication.
Causes / Why It Happens
Understanding the root causes of tooth inflammation is fundamental to both prevention and effective treatment. While bacterial infection is a primary culprit, several other factors contribute to the onset and progression of this condition.
1. Dental Caries (Cavities)
This is the most common cause of pulpitis. When bacteria in plaque consume sugars, they produce acids that erode tooth enamel. If left untreated, these acids create a cavity that penetrates deeper into the dentin and eventually reaches the dental pulp. Once bacteria reach the pulp, they cause infection and inflammation.
Pro Tip: Regular dental check-ups and x-rays can detect cavities early, often before they cause significant inflammation or pain, allowing for simpler and less invasive treatment.
2. Tooth Trauma
Physical injury to a tooth can directly inflame the pulp. This can include:
- Cracks or Fractures: Chips, cracks, or fractures in a tooth can expose the dentin or pulp to bacteria and irritants, leading to inflammation. These can result from biting on hard foods, accidents, or even chronic teeth grinding.
- Deep Fillings or Repeated Dental Procedures: While necessary, some extensive dental work can cause temporary pulp irritation. Repeated procedures on the same tooth can also stress the pulp.
- Traumatic Occlusion: When teeth don't meet properly, or if one tooth takes excessive biting force, it can create stress on the tooth and its supporting structures, leading to inflammation of the pulp or periodontal ligament.
3. Gum Disease (Gingivitis and Periodontitis)
As detailed earlier, plaque and tartar buildup are the primary drivers of gum inflammation.
- Plaque: A sticky, colorless film of bacteria that constantly forms on your teeth. If not removed by daily brushing and flossing, these bacteria release toxins that irritate the gum tissue.
- Tartar (Calculus): Plaque that hardens and calcifies, becoming difficult to remove with a toothbrush. Tartar creates a rough surface that harbors more plaque and provides a breeding ground for bacteria, exacerbating inflammation.
4. Bruxism (Teeth Grinding or Clenching)
Chronic grinding or clenching of teeth, often unconsciously during sleep, puts immense pressure on teeth and their supporting structures. This excessive force can lead to:
- Cracks in teeth.
- Wear and tear on enamel.
- Inflammation of the periodontal ligament (the tissue connecting the tooth to the bone).
- Irritation of the dental pulp, sometimes leading to sensitivity and even irreversible pulpitis.
5. Exposed Dentin
Dentin, the layer beneath enamel, contains thousands of microscopic tubules that lead to the dental pulp. If the enamel or gum tissue recedes, these tubules can become exposed, making the tooth sensitive to temperature changes and increasing the risk of inflammation.
- Causes: Aggressive brushing, gum recession, untreated cavities, or erosion from acidic foods and drinks.
6. Systemic Health Conditions
Certain systemic diseases can increase susceptibility to oral inflammation or exacerbate existing conditions:
- Diabetes: Individuals with diabetes are more prone to infections, including gum disease, due to impaired immune function and delayed healing. High blood sugar levels can also contribute to inflammation.
- Autoimmune Diseases: Conditions like Crohn's disease or lupus can manifest oral symptoms, including inflammation.
- Immunosuppression: Conditions or medications that suppress the immune system (e.g., organ transplant recipients, chemotherapy patients) can make individuals more vulnerable to oral infections and inflammation.
- Nutritional Deficiencies: Deficiencies in vitamins like Vitamin C (scurvy) can lead to severe gum inflammation and bleeding.
7. Tobacco Use
Smoking and other forms of tobacco use are significant risk factors for periodontitis. Tobacco impairs the immune system, reduces blood flow to the gums, and hinders healing, making smokers more susceptible to severe gum inflammation and less responsive to treatment.
8. Hormonal Changes
Fluctuations in hormones, such as during pregnancy, puberty, or menopause, can make gums more sensitive and prone to inflammation (gingivitis) due to increased blood flow to the gum tissues. This is often referred to as "pregnancy gingivitis."
Signs and Symptoms
Recognizing the signs and symptoms of tooth inflammation early is paramount for timely intervention and preventing more severe complications. While pain is a common indicator, it's not the only one.
Pain
Pain is the most overt and concerning symptom of tooth inflammation, and its characteristics can help differentiate between types:
- Sensitivity to Hot and Cold:
- Brief, sharp sensitivity: Often indicates reversible pulpitis or exposed dentin. The pain typically lasts only a few seconds after the stimulus is removed.
- Lingering pain (minutes to hours) after hot/cold: A strong sign of irreversible pulpitis, indicating significant pulp damage.
- Pain on Biting or Chewing: This can suggest a cracked tooth, an inflamed periodontal ligament (often associated with deep cavities or gum disease), or an abscess.
- Spontaneous or Throbbing Pain: Pain that arises without an obvious trigger, especially if it's dull, throbbing, and keeps you awake at night, is highly indicative of irreversible pulpitis or an acute infection/abscess.
- Referred Pain: Sometimes, the pain from an inflamed tooth can radiate to the ear, jaw, or head, making it difficult to pinpoint the exact source.
Swelling
- Localized Gum Swelling: Red, puffy gums around a specific tooth or throughout the mouth (gingivitis).
- Facial Swelling: Swelling of the cheek or jaw area indicates a more severe infection, possibly a dental abscess that has spread beyond the tooth's immediate vicinity. This is an urgent medical concern.
- Pimple-like bump on gums (fistula): This indicates a chronic infection where pus is draining from an abscess. It might temporarily relieve pain but doesn't resolve the infection.
Bleeding
- Bleeding Gums: Gums that bleed easily during brushing, flossing, or even spontaneous bleeding are a classic sign of gingivitis or periodontitis. Healthy gums do not typically bleed.
Changes in Gum Appearance
- Redness: Healthy gums are typically pink. Inflamed gums appear redder, sometimes a deep purplish-red.
- Tenderness: Gums may be sore to the touch.
- Receding Gums: Gums pulling away from the teeth, making teeth appear longer, is a sign of periodontitis and indicates bone loss.
- Pus: Presence of pus between the gums and teeth is a clear indicator of active infection (periodontitis or an abscess).
Other Symptoms
- Bad Breath (Halitosis): Persistent bad breath, even after brushing, is often caused by bacteria associated with gum disease and decaying food particles trapped in inflamed areas.
- Foul Taste in Mouth: A metallic or generally unpleasant taste can be due to pus from an infection.
- Loose Teeth: As gum disease progresses and bone support is lost, teeth may become mobile.
- Changes in Bite: Teeth may shift, or your bite may feel "off" due to bone loss or swelling.
- Fever: A fever, especially accompanied by facial swelling, indicates a serious spreading infection requiring immediate medical attention.
Pro Tip: Don't ignore persistent dental pain or gum issues. Even mild symptoms can escalate quickly. Early detection by a dentist is key to preventing major complications.
Treatment Options
The treatment for tooth inflammation depends entirely on its type, cause, and severity. A thorough dental examination, including X-rays and potentially other diagnostic tests, is crucial to determine the most appropriate course of action.
1. Dental Fillings
- Indication: Reversible pulpitis caused by small to moderate cavities.
- Process: The dentist removes the decayed tooth structure and then fills the cavity with a restorative material like composite resin, amalgam, or glass ionomer. This seals off the dentin and pulp from bacteria and irritants.
- Pros: Preserves tooth structure, relatively inexpensive, quick procedure, restores function.
- Cons: Not suitable for deep decay reaching the pulp or for irreversible pulpitis. May cause temporary sensitivity.
- Cost: $75 - $250 per filling, depending on material and size.
2. Deep Cleaning (Scaling and Root Planing - SRP)
- Indication: Gingivitis and early to moderate periodontitis.
- Process: This is a non-surgical procedure performed under local anesthesia. Scaling involves removing plaque and tartar from above and below the gum line. Root planing smooths the root surfaces to remove bacterial toxins and prevent future plaque adhesion, allowing the gums to reattach to the clean tooth surfaces. It's typically done over 2-4 appointments, treating one quadrant of the mouth at a time.
- Pros: Highly effective for controlling gum disease, less invasive than surgery, reduces gum inflammation and bleeding.
- Cons: Requires multiple appointments, may cause temporary gum sensitivity, not suitable for advanced periodontitis with significant bone loss.
- Cost: $200 - $600 per quadrant, often covered partially by insurance.
3. Root Canal Therapy (Endodontic Treatment)
- Indication: Irreversible pulpitis, infected dental pulp, dental abscess.
- Process: The dentist or endodontist (a root canal specialist) accesses the pulp chamber, removes the inflamed or infected pulp tissue, cleans and shapes the root canals, and then fills and seals them with a biocompatible material (gutta-percha). A crown is usually placed afterward to protect the weakened tooth.
- Pros: Saves the natural tooth, prevents extraction, eliminates pain and infection, highly successful (over 95% when done correctly).
- Cons: Can be an extensive procedure (1-2 appointments), requires a follow-up crown, higher cost than a filling.
- Cost: $700 - $1,500 for a front tooth, $900 - $2,000 for a bicuspid, and $1,200 - $2,500+ for a molar. The crown adds another $800 - $2,500.

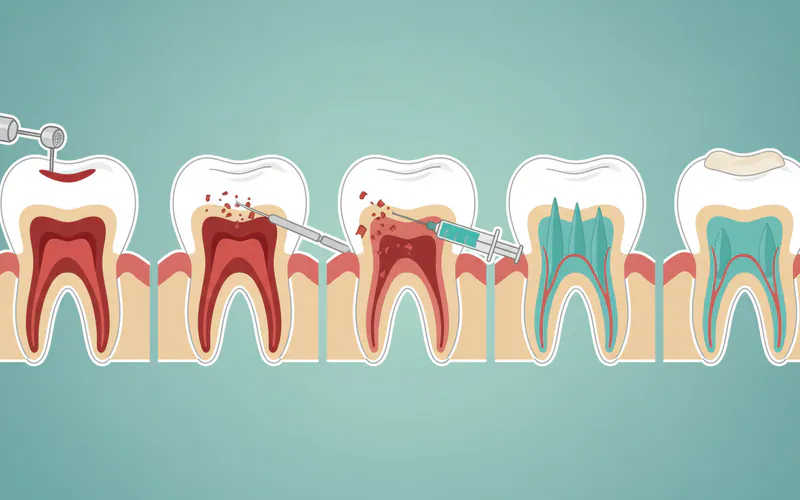
4. Tooth Extraction
- Indication: Severely damaged teeth that cannot be saved by root canal therapy (e.g., extensive decay below the gum line, severe cracks, irreparable trauma), advanced periodontitis with significant bone loss and mobility, or severe infection where root canal is not feasible.
- Process: The tooth is gently loosened and removed from its socket. Local anesthesia is always used; sedation may be an option.
- Pros: Immediate relief from the source of infection/inflammation, often a quick procedure.
- Cons: Permanent tooth loss, requires replacement (implant, bridge, partial denture) to prevent shifting of adjacent teeth, chewing problems, and bone loss. Replacement costs are additional.
- Cost: $75 - $400 for a simple extraction, $150 - $600 for a surgical extraction (e.g., impacted wisdom tooth), $800 - $2,500 for a dental implant.
5. Antibiotics
- Indication: To control acute infections spreading beyond the tooth or gums (e.g., facial swelling, fever, lymph node involvement), or as an adjunct to deep cleaning or root canal therapy in severe cases.
- Process: Oral antibiotics (e.g., Amoxicillin, Clindamycin) are prescribed for a specific duration. Topical antibiotics (e.g., Arestin) may be applied directly into periodontal pockets.
- Pros: Effective in combating bacterial infections, can reduce swelling and pain, prevents spread of infection.
- Cons: Not a standalone treatment for deep decay or chronic gum disease; must be combined with dental procedures. Risk of antibiotic resistance if overused. Can cause side effects like stomach upset.
- Cost: $10 - $50 for a course of generic oral antibiotics; topical antibiotics may be more expensive and covered by dental insurance.
6. Anti-inflammatory Medications
- Indication: To manage pain and reduce inflammation.
- Process: Over-the-counter NSAIDs (Non-Steroidal Anti-Inflammatory Drugs) like ibuprofen or naproxen are often recommended. In some cases, prescription-strength NSAIDs or corticosteroids might be used.
- Pros: Provides effective pain relief and reduces swelling.
- Cons: Does not treat the underlying cause of inflammation. Long-term use can have side effects (stomach issues, kidney problems).
- Cost: $5 - $20 for OTC medications.
Step-by-Step Process (Example: Root Canal Therapy)
To illustrate what to expect during a common treatment for severe tooth inflammation, let's detail the steps of root canal therapy:
Step 1: Diagnosis and Anesthesia
- Initial Assessment: Your dentist or endodontist will examine your tooth, take X-rays, and perform vitality tests (e.g., hot/cold sensitivity, percussion test) to confirm irreversible pulpitis or infection and determine if the tooth is a candidate for a root canal.
- Anesthesia: Local anesthetic is administered to numb the affected tooth and surrounding tissues. You should feel no pain during the procedure, only pressure.
Step 2: Isolation and Access
- Rubber Dam Placement: A small sheet of latex or non-latex material called a rubber dam is placed around the tooth. This isolates the tooth, keeps it clean and dry, and prevents bacteria from saliva from entering the treatment area. It also protects you from swallowing small instruments.
- Access Opening: A small opening is carefully drilled through the crown of the tooth to reach the pulp chamber and root canals.
Step 3: Cleaning and Shaping
- Pulp Removal: Tiny, flexible files are used to carefully remove the infected or inflamed pulp tissue from the pulp chamber and each root canal.
- Cleaning and Shaping: The root canals are meticulously cleaned, shaped, and disinfected using specialized instruments and irrigating solutions (e.g., sodium hypochlorite) to remove bacteria and debris. This step prepares the canals for filling.
Step 4: Filling and Sealing
- Obturation: Once the canals are thoroughly cleaned and dried, they are filled with a biocompatible, rubber-like material called gutta-percha, usually combined with an adhesive sealer. This material completely fills the canals, preventing future bacterial re-entry.
- Temporary Filling: A temporary filling is placed in the access opening in the crown of the tooth.
Step 5: Restoration
- Permanent Restoration: A few weeks after the root canal, you will return to your general dentist for a permanent restoration. Since a tooth that has undergone root canal therapy can become brittle and prone to fracture, a dental crown is almost always recommended to protect it and restore its full function.
- Follow-up: Your dentist will monitor the tooth with follow-up X-rays to ensure the infection has resolved and the tooth is healing properly.
This entire process can take one or two appointments, depending on the complexity of the tooth (molars have more canals than front teeth) and the extent of the infection.
Cost and Insurance
Understanding the financial aspect of dental treatments for tooth inflammation is critical for planning. Costs can vary significantly based on the type of procedure, the specific tooth involved, the region of the US, and whether you have dental insurance.
Average US Price Ranges (Without Insurance)
| Procedure | Average Low Range | Average High Range | Notes |
|---|---|---|---|
| Dental Exam & X-rays | $50 | $200 | Initial diagnosis. |
| Simple Filling (Amalgam/Composite) | $75 | $250 | For reversible pulpitis/cavities. |
| Deep Cleaning (Scaling & Root Planing) | $200 | $600 | Per quadrant (mouth divided into 4 sections). |
| Root Canal Therapy | |||
| Front Tooth (Incisor/Canine) | $700 | $1,500 | Simpler, single canal. |
| Premolar/Bicuspid | $900 | $2,000 | Typically two canals. |
| Molar | $1,200 | $2,500 | Most complex, often 3-4 canals. |
| Dental Crown (Post Root Canal) | $800 | $2,500 | Essential for protecting root canal-treated teeth. Material affects cost. |
| Simple Tooth Extraction | $75 | $400 | Non-surgical removal of visible tooth. |
| Surgical Tooth Extraction | $150 | $600 | For impacted teeth, or those requiring sectioning. |
| Dental Implant (per tooth, no crown) | $1,500 | $3,000 | Root replacement option after extraction. Crown adds $800-$2,500. |
| Antibiotics (Oral, generic) | $10 | $50 | To manage acute infection. |
Prices are estimates and can vary significantly by location (e.g., urban areas typically higher), practice, and complexity of the case.
Insurance Coverage Details
Most dental insurance plans in the US follow a "100-80-50" coverage model, though percentages can vary:
- Preventive Care (e.g., exams, X-rays, cleanings): Often covered at 80-100%. This highlights the importance of regular check-ups to catch inflammation early.
- Basic Restorative Care (e.g., fillings, simple extractions): Typically covered at 70-80% after deductible.
- Major Restorative Care (e.g., root canal therapy, crowns, deep cleanings, surgical extractions): Usually covered at 40-50% after deductible.
Important Considerations:
- Deductibles: The amount you must pay out-of-pocket before your insurance starts covering costs (e.g., $50-$150 annually).
- Annual Maximums: Most dental plans have a limit on how much they will pay in a year (e.g., $1,000-$2,000). If your treatment costs exceed this, you'll pay the remainder.
- Waiting Periods: Some plans have waiting periods (e.g., 6-12 months) for major procedures, meaning you can't get coverage immediately after signing up.
- In-Network vs. Out-of-Network: Your costs will generally be lower if you choose a dentist who is in your insurance plan's network.
- Pre-authorization: For major procedures like root canals or crowns, your dentist may submit a pre-authorization request to your insurance company to get an estimate of coverage before treatment begins.
Cost-Saving Tips:
- Preventive Care: The best way to save money is to prevent inflammation in the first place. Regular cleanings and exams cost far less than treating a root canal.
- Flexible Spending Accounts (FSAs) or Health Savings Accounts (HSAs): If you have an employer-sponsored health plan, you can use pre-tax dollars from an FSA or HSA to pay for dental expenses.
- Dental Schools: University dental schools often provide treatment at a reduced cost, as procedures are performed by students under the supervision of experienced faculty.
- Payment Plans and Financing: Many dental offices offer in-house payment plans or work with third-party financing companies (e.g., CareCredit) that offer low or no-interest payment options for qualified patients.
- Community Dental Clinics: Search for local community dental clinics or public health programs that may offer reduced-cost services, especially for lower-income individuals.
Recovery and Aftercare
Proper recovery and aftercare are crucial for ensuring the success of treatment for tooth inflammation and preventing recurrence. The specific instructions will depend on the procedure performed.
General Aftercare for Most Procedures (Fillings, SRP, Extractions)
- Pain Management:
- Over-the-counter pain relievers: NSAIDs like ibuprofen (Advil, Motrin) or acetaminophen (Tylenol) are usually sufficient to manage discomfort.
- Prescription pain medication: May be prescribed for more extensive procedures like surgical extractions or complex root canals. Take as directed.
- Swelling Reduction:
- Ice Packs: Apply an ice pack to the outside of your cheek (20 minutes on, 20 minutes off) for the first 24-48 hours to minimize swelling.
- Keep Head Elevated: Sleeping with your head slightly elevated can also help reduce swelling.
- Diet:
- Soft Foods: Stick to soft, easy-to-chew foods (yogurt, soup, mashed potatoes, scrambled eggs) for the first few days.
- Avoid: Hard, crunchy, sticky, very hot, or spicy foods, especially near the treated area.
- Straws: Avoid using straws, particularly after extractions, as the suction can dislodge blood clots.
- Oral Hygiene:
- Gentle Brushing: Brush gently around the treated area, but continue regular brushing and flossing of other teeth to maintain overall oral hygiene.
- Rinsing: Your dentist may recommend warm salt water rinses (1/2 teaspoon salt in 8 ounces warm water) starting 24 hours after the procedure, 2-3 times a day, to aid healing and keep the area clean. Avoid vigorous rinsing immediately after extraction.
- Antiseptic Mouthwash: Sometimes prescribed, especially after deep cleanings or surgery.
Specific Aftercare Instructions
- After Fillings:
- Avoid chewing on the treated tooth until the anesthetic wears off to prevent accidental biting.
- Some sensitivity to hot/cold may persist for a few days to weeks; this is normal for reversible pulpitis and should gradually subside.
- If your bite feels uneven, contact your dentist for an adjustment.
- After Deep Cleaning (SRP):
- Gums may be tender, swollen, and sensitive for several days.
- You might experience increased tooth sensitivity, especially to cold, for a few weeks; this often improves with desensitizing toothpaste.
- Continue meticulous oral hygiene as instructed by your hygienist to prevent recurrence of gum disease.
- After Root Canal Therapy:
- Avoid chewing on the temporary filling until the permanent crown is placed to prevent fracture.
- Some mild soreness or tenderness for a few days is normal.
- It is crucial to get the permanent crown or restoration placed promptly (usually within a few weeks) to protect the tooth from future damage and infection.
- After Tooth Extraction:
- Bite on gauze: Bite firmly on the gauze pad placed by the dentist for 30-60 minutes to stop bleeding and help form a blood clot. Change as needed.
- Blood Clot Protection: It is vital to protect the blood clot in the socket for the first few days to prevent dry socket. Avoid spitting, smoking, rinsing vigorously, or using straws.
- No Smoking: Avoid smoking for at least 72 hours, as it severely impairs healing and increases dry socket risk.
Pro Tip: Always follow your dentist's specific post-operative instructions diligently. If you experience severe pain, excessive bleeding, persistent swelling, fever, or any concerning symptoms, contact your dental office immediately.
Prevention
Preventing tooth inflammation is largely within your control and primarily involves consistent, diligent oral hygiene practices and regular professional dental care. Adhering to these guidelines can save you from pain, costly treatments, and potential systemic health issues.
1. Maintain Excellent Oral Hygiene
This is the cornerstone of preventing most forms of tooth and gum inflammation.
- Brush Twice Daily: Brush your teeth for at least two minutes, twice a day, using a soft-bristled toothbrush and fluoride toothpaste. Angle the brush at 45 degrees to the gum line, using gentle, circular motions. The American Dental Association (ADA) recommends replacing your toothbrush every 3-4 months, or sooner if the bristles are frayed.
- Floss Daily: Floss once a day to remove plaque and food particles from between your teeth and under the gum line where your toothbrush can't reach. This is critical for preventing gingivitis and periodontitis.
- Consider Mouthwash: An antiseptic or fluoride mouthwash can be a helpful adjunct, but it's not a substitute for brushing and flossing. Consult your dentist for recommendations.
2. Regular Dental Check-ups and Professional Cleanings
- Schedule Biannual Visits: Visit your dentist for a comprehensive examination and professional cleaning at least twice a year (every six months). These visits allow your dentist to:
- Detect and treat cavities before they lead to pulpitis.
- Remove plaque and tartar buildup that you can't remove at home, preventing gingivitis and periodontitis.
- Identify early signs of gum disease, cracks, or other issues.
- Perform oral cancer screenings.
3. Balanced Diet
- Limit Sugary and Acidic Foods/Drinks: Sugars feed the bacteria that cause tooth decay, leading to inflammation. Acidic foods and beverages can erode enamel, increasing sensitivity and vulnerability.
- Eat Nutrient-Rich Foods: A diet rich in fruits, vegetables, lean proteins, and whole grains supports overall health, including oral health. Calcium and Vitamin D are particularly important for strong teeth and bones.
4. Protect Your Teeth
- Wear a Mouthguard: If you play contact sports, always wear a custom-fitted mouthguard to protect your teeth from trauma and fractures, which can lead to pulpitis.
- Manage Bruxism: If you grind or clench your teeth (bruxism), your dentist can create a custom nightguard to protect your teeth from excessive forces, wear, and potential cracks. Addressing stress and anxiety can also help.
5. Avoid Tobacco Products
- Quit Smoking/Vaping: Tobacco use is a major risk factor for severe gum disease, impaired healing, and oral cancer. Quitting tobacco is one of the most impactful steps you can take for your oral and systemic health.
6. Address Systemic Health Issues
- Manage Chronic Conditions: If you have conditions like diabetes, ensure they are well-managed. Work with your physician and dentist to understand how your systemic health impacts your oral health.
Risks and Complications
While tooth inflammation is treatable, neglecting it or delaying treatment can lead to a cascade of serious complications, some of which extend beyond your mouth and can threaten your overall health.
1. Dental Abscess
- Periapical Abscess: An infection at the tip of the tooth root, often a direct result of untreated irreversible pulpitis.
- Periodontal Abscess: An infection in the gum tissue, often caused by advanced periodontitis.
- Risk: Abscesses are painful, can destroy surrounding bone and tissue, and can spread rapidly.
2. Spread of Infection
One of the most dangerous complications is the spread of bacterial infection from the tooth or gums to other parts of the body.
- Cellulitis: A rapidly spreading bacterial infection of the soft tissues (skin and underlying tissues) of the face, jaw, or neck. It can cause severe swelling, pain, and fever.
- Ludwig's Angina: A rare but life-threatening infection of the floor of the mouth, which can compromise the airway, making breathing difficult. This requires emergency medical attention.
- Sepsis: In rare but severe cases, the infection can enter the bloodstream, leading to sepsis, a widespread inflammatory response throughout the body that can cause organ damage and be fatal.
- Cavernous Sinus Thrombosis: A very rare but critical condition where a blood clot forms in the cavernous sinus (a large vein at the base of the brain), usually from a facial infection.
3. Tooth Loss
- Untreated Pulpitis/Abscess: If a tooth with irreversible pulpitis or an abscess is not treated (either with a root canal or extraction), the infection and structural damage will eventually lead to the tooth needing to be removed.
- Advanced Periodontitis: Chronic, uncontrolled gum disease destroys the bone and ligaments supporting the teeth, leading to loose teeth that eventually fall out or require extraction.
4. Bone Loss
- Periodontal Disease: The hallmark of periodontitis is progressive destruction of the alveolar bone that supports the teeth. This bone loss is often irreversible and can lead to a sunken appearance of the jaw, making future dental restorations (like implants) more complex.
- Abscesses: Untreated dental abscesses can also erode significant amounts of jawbone.
5. Systemic Health Complications
The link between oral inflammation and systemic health is well-established. Chronic inflammation in the mouth contributes to:
- Cardiovascular Disease: Bacteria from oral infections can enter the bloodstream and contribute to plaque formation in arteries, increasing the risk of heart attack and stroke.
- Diabetes: Periodontal disease makes it harder for individuals with diabetes to control their blood sugar, and uncontrolled diabetes, in turn, worsens gum disease.
- Respiratory Problems: Oral bacteria can be aspirated into the lungs, potentially causing pneumonia or exacerbating existing respiratory conditions.
- Adverse Pregnancy Outcomes: Periodontal disease is linked to increased risk of preterm birth and low birth weight babies.

6. Chronic Pain and Reduced Quality of Life
Living with persistent tooth or gum pain can significantly impair your quality of life, affecting your ability to eat, sleep, work, and concentrate. Chronic inflammation can also contribute to stress and anxiety.
Comparison Table: Risks of Untreated Tooth Inflammation
| Condition | Primary Oral Impact | Potential Systemic Impact | Common Treatment Costs (if delayed) | Timeline of Complication |
|---|---|---|---|---|
| Reversible Pulpitis | Develops into Irreversible Pulpitis | Minor | $700-$2500 (Root Canal) | Days to Weeks |
| Irreversible Pulpitis | Dental Abscess, Tooth Loss | Localized Swelling, Cellulitis | $700-$2500 (Root Canal) + $800-$2500 (Crown) | Weeks to Months |
| Gingivitis | Progresses to Periodontitis | Minor | $200-$600 (Deep Cleaning) | Months |
| Periodontitis | Tooth Loss, Bone Loss, Abscess | Heart Disease, Diabetes, Respiratory Issues, Sepsis | $200-$600 (Deep Cleaning) + Surgery ($500-$5000) | Months to Years |
| Dental Abscess | Extensive Bone/Tissue Damage, Tooth Loss | Facial Swelling, Cellulitis, Ludwig's Angina, Sepsis | $75-$600 (Extraction) + $1500-$3000 (Implant) | Days to Weeks (Emergency) |
Children / Pediatric Considerations
Tooth inflammation in children, while similar in underlying pathology to adults, has unique considerations due to developing teeth, different dietary habits, and specific behavioral aspects. Early detection and intervention are even more critical in pediatric dentistry.
Common Causes in Children
- Early Childhood Caries (ECC): Also known as "baby bottle tooth decay," this is severe decay in infants and toddlers, often due to prolonged exposure to sugary liquids (juice, milk) in bottles or sippy cups, especially at bedtime. This can quickly lead to pulpitis in primary teeth.
- Trauma: Children are highly active and prone to falls or accidents that can injure primary or permanent teeth, leading to cracks, fractures, or concussions that can inflame the pulp.
- Poor Oral Hygiene: Inconsistent or ineffective brushing and flossing, often due to lack of parental supervision or child non-compliance, leads to plaque buildup, cavities, and gingivitis.
- Eruption Gingivitis: As permanent teeth erupt, the surrounding gums can become temporarily inflamed, tender, and sometimes bleed. This is usually mild and resolves with good hygiene.
Signs and Symptoms in Children
- Difficulty Communicating Pain: Very young children may not articulate "toothache." Instead, look for:
- Irritability, fussiness.
- Refusal to eat, especially hard or cold foods.
- Disturbed sleep.
- Holding their cheek or constantly touching their mouth.
- Visible Swelling: Swelling around a tooth or on the face.
- Red, Bleeding Gums: Particularly noticeable during brushing.
- Changes in Tooth Color: A gray or dark discoloration could indicate a necrotic (dead) pulp, often due to trauma or deep decay.
- Pimple on the Gums: A sign of an abscess draining.
Treatment Options for Children
Treatment aims to preserve primary teeth until they are naturally lost, as they are crucial for speech, chewing, and guiding the eruption of permanent teeth.
- Fillings: For small cavities causing reversible pulpitis.
- Pulpotomy (Baby Root Canal): If decay reaches the pulp of a primary tooth, only the infected coronal (upper part) pulp is removed, and a medicated material is placed. This keeps the tooth alive until it's time for it to fall out naturally.
- Pulpectomy: For more extensive pulp infection in primary teeth, the entire pulp is removed from the root canals, similar to an adult root canal, but adapted for primary teeth.
- Stainless Steel Crowns: Often placed after a pulpotomy or pulpectomy on primary molars to protect the weakened tooth from fracture.
- Extractions: If a primary tooth is too severely damaged or infected to save, it may need to be extracted. In such cases, a "space maintainer" might be necessary to prevent adjacent teeth from shifting and blocking the eruption of the permanent tooth.
- Antibiotics: For spreading infections (facial swelling, fever).
Prevention in Children
- Early Dental Visits: The ADA recommends a child's first dental visit by their first birthday or when the first tooth erupts.
- Good Oral Hygiene Habits:
- Clean infant gums with a soft cloth.
- Brush teeth twice daily with a fluoride toothpaste (rice-grain size for under 3, pea-size for 3-6 years).
- Floss daily once teeth touch.
- Supervise brushing until age 7-8.
- Dietary Habits:
- Avoid putting babies to bed with bottles containing milk, formula, or juice.
- Limit sugary snacks and drinks.
- Encourage water consumption.
- Fluoride: Ensure adequate fluoride intake through fluoridated water, fluoride toothpaste, and professional fluoride applications.
- Dental Sealants: Applied to the chewing surfaces of permanent molars as soon as they erupt to protect them from decay.
Cost Breakdown
While individual costs were discussed earlier, let's consolidate them to provide a clearer picture of potential expenses for various scenarios, emphasizing costs with and without insurance and payment options.
Scenario-Based Cost Estimates (Without Insurance)
| Scenario | Common Procedures | Estimated Cost Range |
|---|---|---|
| Mild Inflammation (Early Cavity/Gingivitis) | Exam, X-rays, Cleaning, 1-2 Fillings | $200 - $600 |
| Moderate Inflammation (Deeper Cavity/Early Periodontitis) | Exam, X-rays, Deep Cleaning (1-2 Quads), 1 Root Canal + Crown | $2,000 - $5,000 |
| Severe Inflammation (Abscess/Advanced Periodontitis) | Emergency Exam, X-rays, Extraction, Bone Graft (optional), Implant + Crown | $3,000 - $7,000+ (per tooth) |
With Insurance: Understanding Your Out-of-Pocket
Even with insurance, you will have out-of-pocket costs due to deductibles, co-pays, and annual maximums.
- Deductible: Typically $50-$150 per person per year. You pay this amount first.
- Co-insurance: After your deductible, your insurance pays a percentage, and you pay the rest.
- Basic procedures (fillings): You might pay 20-30%.
- Major procedures (root canals, crowns, deep cleanings): You might pay 50-60%.
- Annual Maximum: Most plans cap at $1,000 - $2,000 per year. For complex issues like a root canal, crown, and deep cleaning, you could easily hit this maximum, paying the remainder yourself.
Example: For a molar root canal ($1,500) and crown ($1,500), totaling $3,000:
- Assuming a $100 deductible.
- Assuming 50% coverage for major procedures.
- You pay the $100 deductible.
- Remaining $2,900. Insurance covers 50% = $1,450.
- You pay the other 50% = $1,450.
- Total out-of-pocket for you: $100 (deductible) + $1,450 (co-insurance) = $1,550.
- If your annual maximum is $1,500, then after your insurance pays $1,450, you've almost hit the cap. You might have to pay 100% of any further treatment that year.
Payment Plans and Financing Options
Many dental practices understand the financial burden of extensive treatment and offer various solutions:
- In-Office Payment Plans: Some dentists offer interest-free payment plans, allowing you to pay in installments directly to the practice.
- Third-Party Financing (e.g., CareCredit): These companies specialize in health care financing and offer credit cards with deferred interest options (if paid within a promotional period) or low-interest plans.
- Dental Savings Plans (Discount Plans): Not insurance, but a membership program where you pay an annual fee and receive discounts (typically 10-60%) on dental services from participating providers. These are good for individuals without insurance or those who have hit their annual maximums.
Pro Tip: Always discuss treatment costs and payment options with your dental office's financial coordinator before beginning major procedures. They can often provide a detailed breakdown of costs and help you navigate your insurance benefits.
Frequently Asked Questions
What does tooth inflammation feel like?
Tooth inflammation can manifest as various types of pain: a sharp, short sensitivity to hot or cold, a lingering throbbing ache, pain when biting or chewing, or even spontaneous pain that wakes you up at night. It can also be accompanied by visible swelling in the gums or face, redness, and bad breath.
How quickly does tooth inflammation develop?
Gingivitis can develop within days to weeks of poor oral hygiene. Cavities can take months to years to become deep enough to cause significant pulp inflammation. However, once inflammation begins, severe pain and infection, like an abscess, can develop rapidly, sometimes within hours or days if left untreated.
Can tooth inflammation go away on its own?
Reversible pulpitis, often caused by minor irritation or shallow decay, can resolve if the irritant is removed (e.g., by placing a filling). However, irreversible pulpitis, periodontitis, and abscesses will not heal on their own and require professional dental intervention to prevent worsening and complications.
Is tooth inflammation contagious?
No, tooth inflammation itself is not contagious. However, the bacteria that cause certain types of inflammation, particularly those associated with gum disease, can be transmitted through saliva, though transmission alone doesn't guarantee disease development; individual susceptibility and oral hygiene play a larger role.
What are some home remedies for temporary relief?
For temporary relief, you can try rinsing with warm salt water, applying a cold compress to your cheek for swelling, or taking over-the-counter pain relievers like ibuprofen or acetaminophen. Clove oil applied to the affected tooth can also offer some numbing relief. These are only temporary measures and do not treat the underlying cause; you must still see a dentist.
Does stress contribute to tooth inflammation?
Yes, stress can indirectly contribute to tooth inflammation. High stress levels can weaken your immune system, making you more susceptible to infections like gum disease. It can also exacerbate bruxism (teeth grinding/clenching), which can lead to tooth cracks and pulp irritation.
How can I tell if my inflammation is severe enough for a root canal?
Signs that your tooth inflammation might require a root canal include severe, lingering pain after exposure to hot or cold, spontaneous pain that wakes you up, pain when biting, and facial swelling. A definitive diagnosis requires a dental exam and X-rays to assess the pulp's health and determine if the inflammation is irreversible.
What happens if I can't afford immediate dental treatment?
If you're experiencing severe pain or swelling and can't afford immediate treatment, contact your dentist or a community dental clinic. Many offer emergency appointments or payment plans. Some clinics provide services on a sliding scale. Ignoring severe inflammation can lead to life-threatening infections, making the eventual costs much higher, both financially and to your health.
How long does recovery typically take after treatment?
Recovery time varies:
- Fillings: A few days of sensitivity.
- Deep Cleaning (SRP): Gums may be sensitive for a few days to a week.
- Root Canal: Mild soreness for a few days, full recovery and crown placement within weeks.
- Extraction: A few days for initial healing, weeks to months for full tissue and bone recovery.
Can inflammation from a tooth affect other parts of my body?
Absolutely. Untreated oral inflammation, especially periodontitis and dental abscesses, can allow bacteria to enter the bloodstream. This has been linked to increased risks for systemic conditions such as heart disease, stroke, poorly controlled diabetes, respiratory infections, and complications during pregnancy.
When to See a Dentist
Knowing when to seek professional dental care is critical for managing tooth inflammation and preventing serious complications.
Immediate Attention (Emergency)
Contact your dentist or an emergency dental service immediately if you experience any of the following:
- Severe, Unbearable Pain: Especially if it's constant, throbbing, or prevents you from sleeping, and doesn't respond to over-the-counter pain medication.
- Facial Swelling: Swelling of your cheek, jaw, or around your eye. This indicates a spreading infection (abscess) that could become life-threatening if it affects your airway or spreads to other parts of your body.
- Difficulty Swallowing or Breathing: These are critical signs of a severe, rapidly progressing infection (e.g., Ludwig's Angina) and require immediate emergency medical care, potentially from an ER.
- Pimple-like bump on your gums with pus: While sometimes it provides temporary pain relief as pus drains, it signifies an active and often chronic infection that needs professional treatment.
- Fever with Dental Pain: Fever combined with tooth pain or swelling indicates a systemic infection that needs urgent attention.
- Traumatic Injury: A knocked-out tooth, significant crack, or fracture from an accident needs immediate dental evaluation.
Scheduled Appointment (Routine Care or Urgent, Non-Emergency)
Make an appointment with your dentist as soon as possible (within a few days to a week) if you notice:
- Persistent Sensitivity: If your teeth are sensitive to hot, cold, or sweets for more than a few seconds, or if the sensitivity is increasing.
- Bleeding, Red, or Swollen Gums: These are classic signs of gingivitis or early periodontitis.
- Bad Breath or Foul Taste: Persistent bad breath or a metallic/foul taste that doesn't go away with brushing.
- Pain on Biting or Chewing: This can indicate a cavity, a crack, or an issue with your bite.
- Loose Teeth: A sign of advanced gum disease.
- Receding Gums: Gums pulling away from the teeth.
Red Flags vs. Routine Care Guidance: Any pain that is persistent, worsening, or accompanied by swelling, fever, or difficulty functioning (eating, sleeping) is a red flag and warrants prompt professional evaluation. Don't wait for the pain to become unbearable. Early intervention for tooth inflammation can prevent more complex, costly, and painful procedures down the line, safeguarding both your oral and overall health.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Does Oil Pulling Help Gut Health
The intricate connection between our oral health and overall well-being is a topic of growing fascination and scientific inquiry. Often, when we think of health, we focus on specific organs or systems, overlooking the crucial role of the mouth as a gateway to the rest of the body. One ancient practi
February 23, 2026
Does Oil Pulling Help With Inflammation
It's a question many health-conscious individuals ask as they explore natural remedies: does oil pulling help with inflammation? In an era where holistic approaches to wellness are gaining traction, the ancient practice of oil pulling has resurfaced, promising benefits that extend beyond oral hy
February 23, 2026
Oil Pulling for Kidney Disease: Complete Guide
Chronic kidney disease (CKD) affects an estimated 37 million adults in the United States, often progressing silently until advanced stages. What many may not realize is the profound connection between the health of their mouth and the health of their kidneys. As a bridge between traditional wisd
February 23, 2026
Oil Pulling Oral Microbiome: Complete Guide
Have you ever considered the bustling universe thriving within your mouth? This intricate community, known as the oral microbiome, consists of billions of microorganisms – some beneficial, some harmful – all playing a critical role in your oral and overall systemic health. Maintaining a balanced
February 23, 2026