Dog Bad Breath: Complete Guide

Key Takeaways
- Few things can dampen the joy of a loving pet interaction quite like a strong whiff of "dog breath." While it's commonly joked about, persistent dog bad breath—medically known as halitosis—is far more than just an unpleasant odor. It's often a critical indicator of underlying health issues, rang
Dog Bad Breath: Complete Guide
Few things can dampen the joy of a loving pet interaction quite like a strong whiff of "dog breath." While it's commonly joked about, persistent dog bad breath—medically known as halitosis—is far more than just an unpleasant odor. It's often a critical indicator of underlying health issues, ranging from prevalent dental disease to more serious systemic conditions. In fact, studies show that by the age of three, most dogs exhibit some signs of periodontal disease, the leading cause of bad breath in canines. Ignoring your dog's halitosis isn't just about tolerating a smell; it's about overlooking a potential health crisis that could impact their comfort, quality of life, and even longevity. This comprehensive guide from SmilePedia.net will delve into what causes bad breath in dogs, the various signs to look for, the most effective treatment options, and crucial prevention strategies to ensure your furry companion enjoys a healthier, fresher future.

Key Takeaways:
Key Takeaways:
- Primary Cause: Over 80% of dogs over three years old suffer from periodontal disease, the most common cause of bad breath, driven by plaque and tartar buildup.
- Early Intervention: Addressing bad breath early can prevent painful tooth loss, gum infections, and the spread of bacteria to vital organs like the heart, kidneys, and liver.
- Professional Dental Cleaning: A comprehensive veterinary dental cleaning under anesthesia, including scaling and polishing, typically costs $400-$1,200 in the US, depending on location and the severity of disease. Extractions can add $50-$300 per tooth.
- Home Care is Crucial: Daily tooth brushing with pet-specific toothpaste is the gold standard for prevention, reducing plaque by up to 70%. Start early for best results.
- Beyond Dental: If dental issues are ruled out, bad breath can signal serious conditions like kidney disease (ammonia smell), liver disease (musty smell), or diabetes (sweet, fruity smell), requiring immediate veterinary attention.
- Regular Check-ups: Annual veterinary check-ups, ideally including an oral examination, are essential for early detection and intervention, often saving significant costs and preventing severe health complications down the line.
- Pet Insurance: Many pet insurance plans cover a portion of unexpected dental procedures like extractions and advanced periodontal treatments, significantly reducing out-of-pocket expenses. Routine cleanings are often covered by wellness plans.
What It Is / Overview
Dog bad breath, or canine halitosis, refers to a persistent and noticeably unpleasant odor emanating from a dog's mouth. Unlike the occasional "doggy breath" that might occur after certain meals, true halitosis is a chronic issue that signals an underlying problem. It's not a condition in itself, but rather a symptom of something deeper, most frequently originating within the oral cavity. The primary culprits behind this offensive smell are volatile sulfur compounds (VSCs) produced by bacteria accumulating in the mouth. These bacteria thrive on food particles and cellular debris, forming plaque and subsequently hardening into tartar. Without proper intervention, this buildup creates a hostile environment ripe for infection and disease, making the breath increasingly foul.
The perception that "all dogs have bad breath" is a dangerous misconception that leads many owners to delay seeking veterinary care. A healthy dog's breath should be relatively neutral, certainly not overtly offensive. Any strong, persistent, or worsening odor is a clear indication that something is amiss and warrants investigation. Ignoring this sign can lead to advanced periodontal disease, pain, and systemic health issues, transforming a potentially manageable problem into a complex and costly one. Understanding what causes bad breath is the first step toward effective management and prevention.
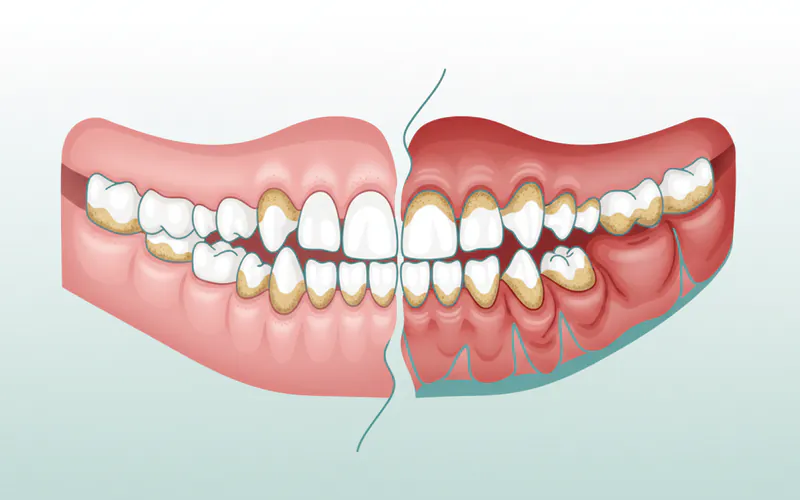
Types / Variations of Dog Bad Breath
While the symptom is consistently bad breath, the type of odor can sometimes offer clues about its origin. Understanding these variations can help you communicate more effectively with your veterinarian.
Odor Characteristics and Potential Causes:
- Rotten, Decaying Smell: This is the most common type and almost always indicates severe dental disease. It's caused by decaying food particles, bacterial growth, pus from infections, and necrotic (dead) tissue within the mouth. This odor is often accompanied by visible plaque, tartar, and inflamed gums.
- Sweet or Fruity Smell: A noticeably sweet or fruity odor, particularly if accompanied by increased thirst, urination, and weight loss despite a good appetite, is a significant red flag for diabetes mellitus. In diabetic dogs, the body cannot properly utilize glucose, leading to the production of ketones, which can give the breath a distinctive sweet scent.
- Ammonia or Urine-like Smell: If your dog's breath smells like ammonia or urine, it's a strong indicator of kidney disease. When the kidneys are failing, they can't effectively filter toxins from the blood. These toxins, including urea, build up and are excreted through other routes, including the breath.
- Musty or Stale Smell: A musty or stale odor can sometimes point to liver disease. The liver plays a crucial role in detoxification, and when it's compromised, toxins accumulate, leading to various symptoms, including a characteristic breath odor.
- Fecal Smell: This is less common but can occur if a dog has consumed feces (coprophagia), or, more seriously, if there's a severe gastrointestinal issue, an intestinal blockage, or a condition where the dog is vomiting fecal matter.
- Pungent, Sour Smell: Can be associated with gastrointestinal upset, acid reflux, or a diet that isn't sitting well with the dog.
- General "Fishy" Smell: While sometimes related to specific foods or fish oil supplements, a persistent fishy odor, especially if accompanied by anal gland issues, can also sometimes be due to systemic bacterial imbalances.
It's crucial to remember that these are just potential indicators. Only a thorough veterinary examination, including blood work and potentially dental X-rays, can accurately diagnose the underlying cause of your dog's bad breath.
Causes / Why It Happens
Understanding what causes bad breath in dogs is fundamental to addressing the issue effectively. The vast majority of cases stem from oral health problems, but systemic diseases can also manifest through distinct breath odors.
1. Oral Health Problems (The Most Common Cause)
-
Periodontal Disease (Gum Disease): This is by far the leading cause of bad breath in dogs. It begins when bacteria in the mouth mix with saliva and food particles to form a sticky film called plaque on the teeth. If plaque isn't removed regularly, it hardens into tartar (calculus). Tartar creates a rough surface that allows even more plaque to accumulate, and it's difficult to remove with brushing alone.
- Gingivitis: This is the earliest stage of periodontal disease, characterized by inflammation of the gums (gingiva). The gums may appear red, swollen, and bleed easily. At this stage, gingivitis is reversible with professional cleaning and good home care. The bacteria associated with gingivitis produce VSCs, causing bad breath.
- Periodontitis: If gingivitis is left untreated, it progresses to periodontitis. The inflammation spreads below the gum line, destroying the supporting structures of the tooth (ligaments, bone). Pockets form around the teeth where more bacteria, pus, and decaying food accumulate, leading to significant bone loss, tooth mobility, and eventually tooth loss. The putrid smell at this stage is intense.
- Bacterial Action: The anaerobic bacteria that thrive in plaque and tartar produce foul-smelling volatile sulfur compounds (VSCs), such as hydrogen sulfide, methyl mercaptan, and dimethyl sulfide, which are responsible for the characteristic odor of bad breath.
-
Food Trapped in the Mouth: Small pieces of food can become lodged between teeth or in gum pockets, especially if teeth are crowded, misaligned, or if there are already existing gum issues. These decaying food particles contribute to bad breath.
-
Oral Tumors or Growths: Malignant or benign masses in the mouth can become necrotic (die off) and infected, leading to a very foul odor. These can be difficult to spot without a thorough oral examination.
-
Foreign Bodies: Objects like splinters of bone, sticks, or even fabric can get lodged between teeth or in the soft tissues of the mouth. This can cause irritation, infection, and a strong, localized odor.
-
Abscessed Teeth: A tooth root abscess, often a complication of severe periodontal disease or a fractured tooth, involves a painful pocket of pus around the tooth root. The infection and pus generate a potent, foul smell.
-
Oral Trauma: Injuries to the mouth, such as lacerations or fractured jaws, can become infected and contribute to bad breath.
-
Stomatitis: Severe inflammation of the entire oral cavity, often seen in dogs with underlying immune system issues, leading to widespread pain and infection.
2. Dietary Factors
- Diet Type: Some raw food diets or diets rich in fish products can temporarily alter breath odor. However, a persistent foul smell usually indicates more than just diet.
- Poor Quality Food: Diets high in fermentable carbohydrates or low-quality ingredients can potentially contribute to plaque formation or digestive issues that impact breath.
- Coprophagia (Eating Feces): If your dog eats stool (their own or another animal's), their breath will naturally smell fecal. This is a behavioral issue that can also have dietary or medical underpinnings.
3. Systemic Health Conditions
While less common than dental disease, certain medical conditions outside the mouth can cause distinct breath odors:
- Kidney Disease: As mentioned, a build-up of urea in the bloodstream (uremia) due to failing kidneys can lead to an ammonia or urine-like smell on the breath. This is a serious condition requiring immediate veterinary intervention.
- Liver Disease: A compromised liver can't filter toxins effectively, leading to their accumulation and a musty, stale breath odor. Symptoms often include jaundice (yellowing of skin/eyes), lethargy, and vomiting.
- Diabetes Mellitus: Uncontrolled diabetes can lead to ketoacidosis, a dangerous metabolic state where the body produces ketones. These ketones can give the breath a distinctively sweet, fruity, or acetone-like smell. Increased thirst, urination, and weight loss are common accompanying symptoms.
- Gastrointestinal Issues: Severe gastrointestinal upset, inflammatory bowel disease, or megaesophagus can sometimes cause unusual breath odors.
- Respiratory Tract Infections: Infections in the nasal passages, sinuses, or lungs can occasionally lead to bad breath, especially if there's discharge or pus that drains into the back of the throat.
- Foreign Bodies in the Nose: A foreign object lodged in the nasal passages can cause a foul-smelling discharge that mimics bad breath.
- Cancer: Cancers of the mouth, throat, or even respiratory system can lead to necrotic tissue and secondary infections, resulting in severe halitosis.
Understanding these varied causes is crucial for both pet owners and veterinarians. What causes bad breath in one dog might be entirely different in another, necessitating a thorough diagnostic approach.
Signs and Symptoms
The most obvious sign of an issue is, of course, the bad breath itself. However, canine halitosis rarely occurs in isolation, especially when caused by dental disease. Learning what to look for can help you identify problems early.
Primary Sign:
- Persistent, Foul Breath: Ranging from mildly offensive to putrid and decaying. The smell may worsen over time.
Accompanying Oral Signs:
- Visible Plaque and Tartar Buildup: Yellow, brown, or green deposits on the teeth, especially along the gum line.
- Red, Swollen, or Bleeding Gums (Gingivitis): Gums may look inflamed, sensitive to touch, or bleed when eating or when you try to brush them.
- Receding Gums: The gum line appears to be pulling away from the teeth, exposing the tooth roots.
- Loose or Missing Teeth: A sign of advanced periodontal disease where the supporting structures of the tooth have been severely compromised.
- Excessive Drooling (Ptyalism): Especially if the saliva is bloody or tinged with pus.
- Paw-rubbing or Pawing at the Mouth: Indicates discomfort or pain.
- Reluctance to Eat or Difficulty Chewing: Especially hard kibble or toys. The dog may chew on one side of the mouth or drop food.
- Changes in Eating Habits: Less enthusiasm for meals, picking at food, or only eating soft foods.
- Discharge from the Nose or Eyes: Especially if purulent (containing pus), can indicate an oral-nasal fistula or severe infection.
- Facial Swelling: Particularly under the eye, which can indicate a tooth root abscess in an upper tooth.
- Lumps or Bumps in the Mouth: Could indicate oral tumors.
Accompanying Systemic Signs (Indicating a Non-Dental Cause):
- Increased Thirst (Polydipsia) and Urination (Polyuria): Common with diabetes and kidney disease.
- Unexplained Weight Loss: Can be a sign of diabetes, kidney disease, liver disease, or cancer.
- Lethargy or Weakness: General malaise often associated with systemic illness.
- Vomiting or Diarrhea: Can accompany severe kidney or liver disease, or gastrointestinal issues.
- Jaundice (Yellowish Skin/Gums/Eyes): A hallmark sign of liver disease.
- Changes in Appetite: Ranging from complete loss of appetite to ravenous hunger (diabetes).
Any of these signs, especially in conjunction with bad breath, should prompt an immediate visit to your veterinarian. Early detection is key to successful treatment and preventing further complications.
Treatment Options
Once the underlying cause of your dog's bad breath has been diagnosed by a veterinarian, a tailored treatment plan can be developed. How to fix bad breath truly depends on its origin, but dental cleaning is the most common and effective first step.
1. Professional Dental Cleaning (Dental Prophylaxis)
- Overview: This is the cornerstone of treating dental-related bad breath. It's performed under general anesthesia to ensure thoroughness and safety.
- Process:
- Pre-anesthetic Bloodwork: To assess organ function and ensure the dog is a good candidate for anesthesia.
- Anesthesia: General anesthesia is essential to allow for a comprehensive and pain-free examination, scaling, and polishing.
- Oral Examination: A detailed assessment of each tooth and surrounding structures.
- Scaling: Using ultrasonic and hand scalers to remove plaque and tartar from above and below the gum line. This is crucial as most disease occurs subgingivally.
- Polishing: Smoothing the tooth surface to deter future plaque adhesion.
- Fluoride Treatment/Sealants: May be applied to strengthen enamel and reduce sensitivity.
- Dental X-rays: Often performed to assess the health of tooth roots and bone structure beneath the gum line, identifying issues like abscesses, bone loss, or unerupted teeth.
- Extractions: Severely diseased or damaged teeth that cannot be saved are surgically removed.
- Pros: The most effective way to eliminate existing plaque and tartar, treat gingivitis, and address early periodontitis. Significantly improves breath and overall oral health. Prevents systemic spread of bacteria.
- Cons: Requires general anesthesia, which carries inherent, though low, risks. Can be costly.
- Pro Tip: Choose a veterinary clinic that adheres to the American Animal Hospital Association (AAHA) Dental Care Guidelines. These guidelines ensure a high standard of care, including pre-anesthetic bloodwork, IV fluids, monitoring, and dental X-rays.
2. Dental Extractions
- Overview: If periodontal disease is advanced, teeth are fractured, or abscessed, extraction is necessary to remove the source of infection and pain.
- Process: Surgical removal of the entire tooth, including its roots. This may involve gingival flaps and bone removal, followed by sutures to close the gum.
- Pros: Eliminates pain, infection, and a major source of bad breath. Prevents further systemic complications.
- Cons: Permanent loss of teeth. Requires significant post-operative care. Can be costly, especially for complex extractions.
3. Medications
- Antibiotics: Prescribed for active infections, such as abscesses or severe periodontitis, before or after dental procedures. They reduce bacterial load and inflammation. Commonly used antibiotics include clindamycin or amoxicillin-clavulanate.
- Pain Relievers/Anti-inflammatories: Non-steroidal anti-inflammatory drugs (NSAIDs) like carprofen or meloxicam are often prescribed post-extraction or for painful oral conditions to manage discomfort.
- Oral Rinses/Gels: Chlorhexidine-based rinses or gels can temporarily reduce bacteria in the mouth and help manage gingivitis. They are typically used as an adjunct to brushing, not a replacement.
4. Addressing Systemic Diseases
- Kidney Disease: Treatment focuses on managing the disease with dietary changes (low protein, phosphorus-restricted), fluid therapy, medications to control blood pressure or phosphorus levels, and potentially dialysis. The breath odor usually improves as kidney function is managed.
- Liver Disease: Treatment varies widely depending on the specific liver condition, but may involve dietary modifications, medications to support liver function, antibiotics, or anti-inflammatories.
- Diabetes Mellitus: Requires insulin therapy to regulate blood sugar levels, dietary management, and regular monitoring. As blood sugar is controlled, the sweet breath odor should resolve.
- Oral Tumors: Treatment depends on the type of tumor (benign or malignant) and its location. Options include surgical removal, radiation therapy, or chemotherapy.
- Gastrointestinal Issues: Treating the underlying GI condition (e.g., dietary modification, medications for reflux, deworming for parasites) can resolve associated breath odors.
5. At-Home Dental Care (For Prevention and Mild Cases)
- Daily Tooth Brushing: The most effective home care method. Requires a pet-specific toothbrush and toothpaste (never human toothpaste, which contains xylitol and fluoride toxic to dogs).
- Dental Chews and Treats: Products with the Veterinary Oral Health Council (VOHC) seal of acceptance have been proven to reduce plaque and/or tartar.
- Dental Diets: Specially formulated kibble that mechanically cleans teeth as the dog chews or contains ingredients that prevent plaque mineralization. Look for VOHC-approved options.
- Water Additives: Solutions added to drinking water that contain antimicrobials or anti-plaque agents. Also look for VOHC approval.
- Oral Sprays/Gels: Similar to rinses, these can help reduce bacteria and freshen breath.
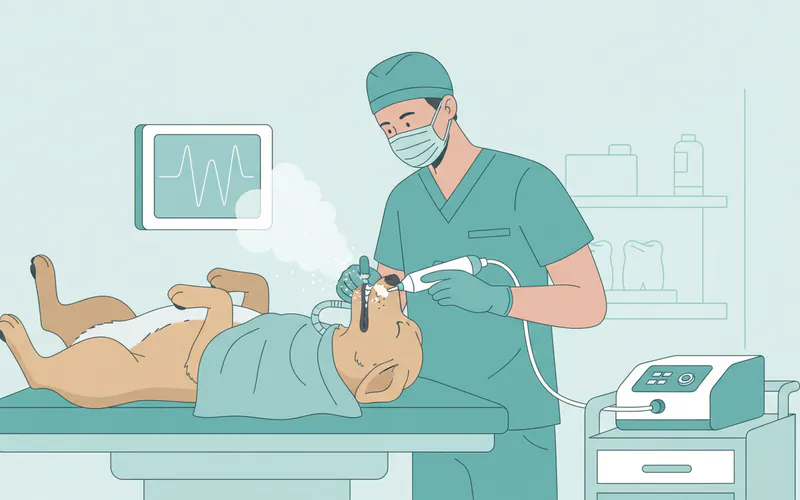
Step-by-Step Process: What to Expect During a Professional Dental Cleaning
When your veterinarian recommends a professional dental cleaning to address your dog's bad breath and oral health, here's a typical step-by-step overview of what you can expect:
1. Pre-Anesthetic Assessment (Days/Weeks Before)
- Comprehensive Physical Exam: Your vet will perform a full physical check-up to assess your dog's overall health and identify any potential risks for anesthesia.
- Blood Work: Pre-anesthetic blood tests are crucial. They evaluate organ function (liver, kidneys), check for underlying infections, and assess blood cell counts to ensure your dog can safely metabolize anesthetic drugs and clot blood normally.
- Urinalysis and ECG (Electrocardiogram): May be recommended for older dogs or those with suspected underlying health conditions to further assess kidney function and heart health.
- Discussion: Your vet will discuss the procedure, potential risks, and the estimated cost.
2. Day of the Procedure (Drop-off)
- Fasting: You will be instructed to withhold food for 8-12 hours before the procedure and water for 2-4 hours to prevent aspiration during anesthesia.
- Admittance: You'll drop your dog off at the clinic. The veterinary team will conduct a final pre-anesthetic check and may administer a mild sedative to help your dog relax.
- IV Catheter Placement: An intravenous (IV) catheter is placed, usually in the front leg, to administer fluids (which help maintain blood pressure and hydration) and provide a route for anesthetic and emergency medications.
3. Anesthesia and Monitoring
- Pre-medication: Sedatives and pain medications are given to ease anxiety and provide initial pain relief, reducing the amount of general anesthetic needed.
- Induction: An anesthetic agent is given intravenously to induce unconsciousness.
- Intubation: An endotracheal tube is inserted into the windpipe to ensure a clear airway and deliver anesthetic gas and oxygen directly to the lungs.
- Monitoring: Throughout the procedure, a dedicated veterinary technician continuously monitors your dog's vital signs, including heart rate, respiratory rate, blood pressure, oxygen saturation, and body temperature. Specialized equipment tracks these parameters.
- IV Fluids: Administered throughout the procedure to support kidney function and blood pressure.

4. The Dental Procedure Itself
- Full Oral Examination: Once under anesthesia, a thorough examination of the entire oral cavity is performed. This includes checking each tooth, gums, tongue, and other soft tissues for signs of disease, damage, or masses.
- Dental X-rays: Full-mouth dental X-rays are taken to assess the health of the tooth roots, jawbone, and structures below the gum line. This is critical as up to 60% of dental disease is hidden beneath the gum line.
- Supra- and Subgingival Scaling: An ultrasonic scaler is used to remove large deposits of plaque and tartar from above (supragingival) and below (subgingival) the gum line. Hand scalers are then used for fine scaling and to remove any remaining deposits.
- Polishing: After scaling, the teeth are polished using a special paste and polishing tool. This creates a smooth surface, which helps deter future plaque accumulation.
- Gingival Lavage: The gum line is flushed to remove any debris and bacteria.
- Extractions: If severe periodontal disease, abscesses, or fractured teeth are identified (often with the help of X-rays), surgical extractions are performed. This involves carefully removing the diseased tooth, often requiring gum flaps and bone removal, followed by suturing the gum tissue closed.
- Pain Management: Local anesthetic blocks (similar to what humans receive at the dentist) are often administered before extractions to provide extended pain relief.
5. Recovery
- Anesthesia Reversal/Wake-up: Anesthetic gas is turned off, and your dog is monitored closely as they wake up.
- Post-operative Pain Management: Additional pain medication is given as needed.
- Warmth and Comfort: Your dog will be kept warm and comfortable in a recovery area.
- Monitoring: Recovery is closely supervised until your dog is fully awake and stable.
6. Discharge and Aftercare Instructions
- Discharge: Your vet or technician will discuss post-operative care, including medication schedules (antibiotics, pain relievers), dietary recommendations (soft food temporarily), and instructions for activity restriction.
- Follow-up: A follow-up appointment is often scheduled to check healing, especially after extractions.
- Home Dental Care Plan: Your vet will recommend a long-term home dental care plan, which may include daily brushing, dental chews, and water additives, to prevent the recurrence of bad breath and dental disease.
This comprehensive process ensures that not only is the bad breath addressed, but the underlying disease is treated, and your dog's oral health is restored.
Cost and Insurance
The cost of addressing dog bad breath can vary significantly based on the severity of the underlying condition, the required treatment, your geographic location, and the veterinary clinic's pricing structure.
Average US Costs for Professional Dental Care:
The most common intervention for bad breath is a professional dental cleaning. These ranges are estimates and can fluctuate:
- Basic Dental Cleaning (Grade 1 Gingivitis, no extractions):
- Low End: $400 - $700 (includes pre-anesthetic bloodwork, anesthesia, scaling, polishing, pain meds)
- Mid-Range: $700 - $1,200 (includes all basic services, IV fluids, basic dental X-rays)
- High End: $1,200 - $1,800 (often in urban areas, includes extensive monitoring, full mouth X-rays, more comprehensive pre-anesthetic work)
- Moderate Dental Disease (Grade 2-3 Periodontitis, some extractions):
- Typically adds $200 - $800+ to the basic cleaning cost.
- Extractions: Each extraction can range from $50 - $300+, depending on the tooth's location (incisors are cheaper, molars are more complex) and the difficulty of removal (e.g., fractured roots, surgical extractions).
- Additional X-rays: If multiple X-rays are needed, costs can increase.
- Severe Dental Disease (Grade 4 Periodontitis, multiple extractions, advanced procedures):
- Can range from $1,500 - $4,000+. This often involves many extractions, advanced pain management, and extended anesthesia time.
- Referral to a Veterinary Dental Specialist: For extremely complex cases (e.g., root canal, orthodontics, oral surgery for tumors), costs can be significantly higher, often starting from $3,000 to $8,000+.
Cost Breakdown Example (Mid-Range Cleaning with 2 Extractions):
| Service | Estimated Cost Range (USD) |
|---|---|
| Pre-anesthetic Bloodwork | $100 - $250 |
| Anesthesia (including monitoring) | $300 - $700 |
| IV Fluids | $50 - $150 |
| Dental Prophylaxis (Scaling/Polish) | $200 - $400 |
| Full-Mouth Dental X-rays | $150 - $300 |
| 2 Simple Extractions (@ $100-$150/ea) | $200 - $300 |
| Post-op Medications (Pain/Antibiotics) | $50 - $150 |
| TOTAL ESTIMATE | $1050 - $2250 |
Geographic Variations:
Costs tend to be higher in major metropolitan areas (e.g., New York, Los Angeles) and on the coasts, while rural areas or the Midwest may offer slightly lower prices.
Pet Insurance Coverage:
- Routine Dental Cleanings: Most standard pet insurance policies (accident/illness) do not cover routine dental cleanings. However, many providers offer "Wellness Plans" or "Preventative Care Add-ons" that include coverage for annual dental cleanings, typically reimbursing a set amount or percentage.
- Dental Disease Treatment: If your dog develops periodontal disease, abscesses, or fractured teeth (not pre-existing conditions), these treatments are often covered by comprehensive accident/illness pet insurance policies. Coverage typically ranges from 70-90% of eligible costs after you meet your deductible.
- Important Note: Pet insurance usually has waiting periods (e.g., 6 months to a year) before dental illness coverage kicks in. Pre-existing conditions are generally not covered. Review policy details carefully.
Payment Plans and Financing Options:
- Veterinary Clinics: Some clinics offer in-house payment plans for established clients.
- Third-Party Financing: Services like CareCredit or Scratchpay offer deferred interest or low-interest payment plans specifically for healthcare costs, including veterinary bills. These can be a lifesaver for unexpected, expensive procedures.
- Emergency Funds: A dedicated savings account for pet emergencies can help cover costs.
Cost-Saving Tips:
- Preventative Home Care: Daily tooth brushing, VOHC-approved dental chews/diets/water additives can significantly delay or reduce the need for costly professional cleanings and extractions.
- Early Intervention: Addressing bad breath and early signs of dental disease with your vet can prevent the progression to more severe, expensive stages requiring multiple extractions.
- Shop Around (Carefully): Get estimates from a few reputable veterinary clinics in your area. However, prioritize quality of care, experience, and adherence to AAHA guidelines over just the lowest price, especially for anesthesia and dental procedures.
- Wellness Plans: If your dog is young and healthy, enrolling in a wellness plan that covers annual dental cleanings can be a good investment over their lifetime.
Recovery and Aftercare
Post-treatment care is crucial for your dog's comfort, healing, and the long-term success of resolving their bad breath, especially following a professional dental cleaning or extractions.
Immediate Post-Anesthesia Care (First 24-48 Hours):
- Rest: Your dog will likely be groggy and disoriented for several hours after anesthesia. Provide a quiet, comfortable, warm place for them to rest. Limit activity.
- Monitor Incisions/Extraction Sites: If extractions were performed, there might be slight bleeding or swelling. Monitor for excessive bleeding, swelling, or discharge.
- Pain Management: Administer all prescribed pain medications exactly as directed by your veterinarian. Do not skip doses, even if your dog seems comfortable. Adequate pain control is vital for healing.
- Antibiotics: If prescribed for infection or as a preventative measure, complete the full course of antibiotics.
- Diet: Offer small amounts of soft, moist food for the first few days, especially after extractions. Avoid hard kibble, bones, or chew toys that could irritate healing gums or extraction sites. Gradually reintroduce normal food as tolerated.
- Water: Ensure fresh water is always available.
- Monitor Appetite and Urination/Defecation: Call your vet if your dog refuses to eat or drink, vomits excessively, has prolonged lethargy, or doesn't urinate/defecate normally.
Long-Term Aftercare for Dental Health:
The goal after a professional cleaning is to prevent the recurrence of plaque, tartar, and bad breath. This requires consistent home dental care.
- Daily Tooth Brushing: This is the gold standard. Use a soft-bristled, pet-specific toothbrush and enzymatic pet toothpaste. Never use human toothpaste. Focus on the outside surfaces of the upper teeth, where plaque accumulates most.
- Pro Tip: Start gradually. Introduce the toothpaste flavor first, then the brush. Keep sessions short and positive, rewarding your dog afterward. Aim for 2-3 minutes daily.
- VOHC-Accepted Dental Products: Incorporate dental chews, treats, or diets that have received the Veterinary Oral Health Council (VOHC) seal of acceptance. These products have been scientifically proven to reduce plaque and/or tartar.
- Water Additives: Consider VOHC-accepted water additives that contain ingredients to inhibit bacterial growth and plaque formation.
- Oral Rinses/Gels: Your vet might recommend a chlorhexidine-based oral rinse or gel for specific issues, used as directed.
- Regular Veterinary Check-ups: Schedule annual (or more frequent, if advised) veterinary check-ups that include an oral examination. This allows your vet to monitor your dog's dental health and catch any returning issues early.
- Watch for Recurrence: Continue to monitor your dog's breath, appetite, and any signs of oral pain or discomfort. If bad breath returns quickly or oral symptoms reappear, contact your vet.
Recovery from Non-Dental Causes:
If bad breath was due to a systemic condition (kidney disease, diabetes, etc.), the recovery and aftercare will focus on managing that specific disease. This might include:
- Medication Adherence: Consistent administration of prescribed medications (e.g., insulin, kidney support drugs).
- Dietary Management: Adhering to special prescription diets for kidney, liver, or diabetic dogs.
- Regular Monitoring: Frequent vet visits, blood tests, and urinalysis to track the disease progression and the effectiveness of treatment.
Adhering to your veterinarian's post-treatment recommendations is paramount to ensuring a smooth recovery and maintaining your dog's health and fresh breath.
Prevention
Preventing dog bad breath primarily involves proactive oral hygiene and regular veterinary care. By taking steps to control plaque and tartar buildup, you can significantly reduce the risk of periodontal disease and the associated foul odor.
1. Daily Home Dental Care (The Foundation)
- Tooth Brushing: This is the single most effective method for preventing plaque and tartar.
- Frequency: Aim for daily brushing. If daily isn't possible, every other day is still beneficial.
- Tools: Use a soft-bristled toothbrush designed for dogs or a finger brush. Always use an enzymatic pet toothpaste (chicken, beef, or peanut butter flavored) – never human toothpaste, which contains fluoride and xylitol that are toxic to dogs.
- Technique: Gently lift your dog's lip and brush the outside surfaces of their teeth, especially where the gums meet the teeth. Focus on the upper, back teeth, as they tend to accumulate the most plaque. Make it a positive experience with praise and rewards.
- Start Early: Begin dental care when your dog is a puppy to acclimate them to the routine.
- VOHC-Accepted Dental Chews and Treats:
- Mechanism: These products are specially designed to either mechanically scrape plaque off teeth as the dog chews or contain ingredients that prevent plaque mineralization.
- Selection: Look for the Veterinary Oral Health Council (VOHC) Seal of Acceptance on packaging. This indicates the product has met standards for reducing plaque, tartar, or both.
- Safety: Always supervise your dog with chews to prevent choking or gastrointestinal issues. Choose appropriately sized and textured chews for your dog.
- Dental Diets:
- Mechanism: Some prescription and over-the-counter kibbles are formulated with a larger, more fibrous texture that helps to mechanically scrub the tooth surface as the dog chews. Others contain ingredients that chemically reduce plaque or tartar formation.
- Selection: Again, look for the VOHC seal. Consult your vet before switching diets, especially for dogs with specific dietary needs.
- Water Additives:
- Mechanism: These solutions contain anti-bacterial or anti-plaque agents that, when added to your dog's drinking water, help reduce the bacterial load in the mouth.
- Selection: Choose VOHC-accepted products.
- Note: Water additives are an adjunct, not a replacement for brushing.
2. Regular Veterinary Check-ups and Professional Dental Cleanings
- Annual Oral Examinations: Your veterinarian will conduct a visual oral exam during your dog's annual physical. They can spot early signs of gingivitis, plaque buildup, or other oral issues.
- Scheduled Professional Cleanings: Depending on your dog's breed, age, genetics, and home care regimen, your vet may recommend professional dental cleanings under anesthesia every 1-3 years. Small breeds are often prone to earlier and more severe dental disease and may need cleanings more frequently.
- Early Intervention: Regular vet visits allow for early detection and treatment of dental disease, preventing it from progressing to severe, painful, and costly stages.
3. Diet and Lifestyle Factors
- Balanced Diet: Feed a high-quality, balanced diet appropriate for your dog's age and breed. While kibble can help reduce some plaque, it's not a substitute for brushing.
- Avoid Harmful Chews: Rawhides can be problematic if not fully digestible. Hard objects like bones, antlers, or ice cubes can cause fractured teeth. Opt for safer, softer chews or VOHC-approved options.
- Discourage Coprophagia: If your dog eats feces, address this behavior. It could be behavioral, nutritional, or medical. Consult your vet for strategies.
Comparison Table: At-Home Dental Care Options
| Method | Effectiveness in Plaque/Tartar Reduction | Ease of Use | Cost (Annual Estimate) | Key Considerations |
|---|---|---|---|---|
| Tooth Brushing | High (up to 70% plaque reduction) | Requires Training | $20 - $50 | Gold standard; requires commitment; use pet-specific paste |
| VOHC Dental Chews | Moderate to High (product-dependent) | Very Easy | $100 - $300 | Must be VOHC-accepted; supervise use; caloric intake |
| VOHC Dental Diets | Moderate | Very Easy (as food) | $500 - $1000+ | Replaces regular food; consult vet for nutritional needs |
| Water Additives | Low to Moderate | Very Easy (add to water) | $50 - $100 | Adjunctive; VOHC-accepted preferred; monitor water intake |
| Oral Gels/Sprays | Low to Moderate | Easy | $30 - $80 | Adjunctive; may require direct application |
Consistency is key in prevention. A combination of daily home care and regular professional check-ups is the most effective strategy for maintaining good oral health and keeping your dog's breath fresh.
Risks and Complications
Ignoring dog bad breath or delaying treatment carries significant risks and can lead to serious complications, extending far beyond just a smelly mouth.
1. Complications of Untreated Periodontal Disease:
- Severe Oral Pain: Advanced gum disease is incredibly painful. Dogs are stoic and may not show obvious signs, but they suffer from chronic discomfort, especially when eating.
- Tooth Loss: As periodontal disease progresses, the bone supporting the teeth is destroyed, leading to loose, mobile, and eventually lost teeth. This impacts chewing ability and quality of life.
- Oral-Nasal Fistula: Severe infection in the root of an upper canine or premolar tooth can erode through the bone, creating an abnormal opening between the mouth and the nasal cavity. This leads to chronic nasal discharge, sneezing, and potentially infection of the nasal passages.
- Jaw Fractures: In cases of severe bone loss in the lower jaw (mandible), particularly in small breeds, the jaw can become so weakened that a simple fall or even chewing can cause a pathological fracture.
- Oral Abscesses and Cellulitis: Untreated infections can lead to painful pus-filled pockets around tooth roots (abscesses) or spread to the surrounding tissues, causing facial swelling (cellulitis).
- Systemic Infections (Bacteria Spread): The constant stream of bacteria from an infected mouth can enter the bloodstream (bacteremia) and travel to distant organs, potentially causing:
- Endocarditis: Infection of the heart valves, leading to serious heart conditions.
- Kidney Disease: Bacterial colonization in the kidneys, potentially worsening or initiating kidney dysfunction.
- Liver Disease: Liver inflammation or infection.
- Joint Infections: In rare cases, bacteria can seed joints.
- Increased Risk of Diabetes: Chronic inflammation from periodontal disease can contribute to insulin resistance.
2. Risks Associated with Anesthesia (for Dental Procedures):
While modern veterinary anesthesia is very safe, it's not without risk. These risks are generally low, especially with proper pre-anesthetic screening and monitoring.

- Allergic Reactions: To anesthetic drugs.
- Cardiac Arrhythmias: Irregular heartbeats.
- Hypotension: Low blood pressure.
- Hypothermia: Drop in body temperature.
- Aspiration Pneumonia: Inhaling stomach contents into the lungs during induction or recovery (rare, prevented by fasting).
- Organ Failure: Pre-existing conditions (e.g., kidney, liver disease) can be exacerbated by anesthesia. This is why pre-anesthetic blood work is crucial.
- Death: Extremely rare, but a possibility with any general anesthesia. The risk is significantly higher in sick, debilitated, or very old animals.
3. Complications of Untreated Systemic Diseases:
If bad breath is a symptom of conditions like kidney disease, liver disease, or diabetes, failing to diagnose and treat these conditions has severe, life-threatening implications:
- Kidney Failure: Untreated kidney disease will progress, leading to complete kidney failure and death.
- Liver Failure: Untreated liver conditions can result in irreversible liver damage and failure.
- Diabetic Ketoacidosis (DKA): Uncontrolled diabetes can lead to DKA, a life-threatening emergency characterized by severe dehydration, electrolyte imbalances, and coma.
- Cancer Progression: If bad breath is due to an oral or systemic tumor, delay in diagnosis and treatment allows the cancer to spread and worsen, often with devastating consequences.
The risks associated with ignoring bad breath in dogs are substantial. What might seem like a minor cosmetic issue can quickly escalate into a serious health crisis, causing pain, reducing quality of life, and potentially shortening your dog's lifespan. Early veterinary intervention is paramount.
Comparison Table: Risks of Untreated Bad Breath vs. Anesthesia for Dental Cleaning
| Factor | Risks of Untreated Bad Breath (Dental Disease) | Risks of Anesthesia for Dental Cleaning (with proper protocols) |
|---|---|---|
| Pain | Chronic, severe oral pain; reluctance to eat. | Temporary discomfort post-procedure (managed with pain meds). |
| Infection | Local (abscesses, gum disease); Systemic (heart, kidney, liver infections). | Low risk of infection with sterile technique and antibiotics. |
| Organ Damage | Direct damage (kidney, heart, liver) from bacterial spread. | Extremely low risk of organ damage with proper pre-anesthetic screening. |
| Quality of Life | Significantly reduced due to pain, inability to eat, chronic illness. | Brief period of grogginess/disorientation during recovery. |
| Long-term Health | Shortened lifespan; increased risk of severe systemic diseases. | Improved long-term health due to elimination of infection source. |
| Cost | Potentially higher costs for advanced disease, emergency care, long-term medication. | Upfront cost of the procedure. |
| Mortality | Increased risk of death from systemic complications. | Extremely low; significantly lower than risks of untreated severe disease. |
It is overwhelmingly clear that the risks of neglecting a dog's bad breath and underlying dental disease far outweigh the carefully managed risks of modern veterinary anesthesia for a necessary dental procedure.
Cost Breakdown (Detailed)
A detailed breakdown of costs for addressing dog bad breath, specifically focusing on professional dental care, helps owners understand where their money goes.
Average US Costs for Professional Dental Care (Without Insurance)
These costs are highly variable and can differ by state, city, and clinic type (general practice vs. specialty hospital).
- Initial Consultation & Exam: $50 - $150
- Purpose: To identify the cause of bad breath, determine the severity of dental disease, and recommend a treatment plan.
- Pre-Anesthetic Blood Work: $100 - $250
- Purpose: Essential for evaluating liver and kidney function, red and white blood cell counts, ensuring the dog can safely metabolize anesthesia and isn't fighting a systemic infection.
- Intravenous (IV) Catheter & Fluids: $50 - $150
- Purpose: For direct access to veins for administering drugs and providing continuous hydration to support blood pressure and organ function during anesthesia.
- Anesthesia (Induction, Maintenance, Monitoring): $300 - $700+
- Purpose: Includes the anesthetic drugs, the gas used for maintenance, and the constant monitoring of vital signs (heart rate, respiration, blood pressure, oxygen saturation, temperature) by a dedicated technician. Longer procedures cost more.
- Comprehensive Oral Exam & Dental Prophylaxis (Scaling & Polishing): $200 - $450
- Purpose: The actual cleaning, including ultrasonic scaling above and below the gum line, hand scaling, and polishing to smooth tooth surfaces.
- Full Mouth Dental X-rays: $150 - $350
- Purpose: Critical for identifying disease below the gum line (root abscesses, bone loss, unerupted teeth, fractured roots), which is often invisible during a visual exam.
- Dental Extractions: $50 - $300+ per tooth
- Purpose: Removal of diseased, fractured, or painful teeth. Costs vary based on the tooth (simple incisor vs. multi-rooted molar), difficulty (surgical extraction with bone removal vs. simple pull), and location. Multiple extractions can add significantly to the bill.
- Local Anesthetic Nerve Blocks: $30 - $80 (per quadrant or site)
- Purpose: Administered before extractions to provide immediate and prolonged pain relief, reducing the amount of general anesthesia needed.
- Post-Operative Medications: $50 - $150
- Purpose: Typically includes pain relievers (NSAIDs) and antibiotics to prevent infection and manage discomfort during recovery.
- Post-Operative Follow-up: $0 - $75 (sometimes included in the procedure cost, sometimes a separate charge)
- Purpose: To check healing, especially after extractions, and address any concerns.
Total Estimated Ranges (Without Insurance)
- Basic Cleaning (Healthy mouth, no extractions): $650 - $1,800
- Moderate Disease (Some extractions): $1,000 - $2,800
- Severe Disease (Multiple complex extractions, advanced care): $2,000 - $5,000+
- Referral to Specialist: $3,000 - $8,000+
With Pet Insurance
- Accident & Illness Plans: For periodontal disease or extractions due to illness/injury, pet insurance typically covers 70-90% of the eligible costs after your deductible is met.
- Example: If your bill is $1,500, your deductible is $250, and your reimbursement rate is 80%: You pay $250 deductible + 20% of ($1500-$250) = $250 + $250 = $500. Insurance covers $1,000.
- Wellness Plans/Add-ons: Many pet insurance companies offer wellness plans that cover a portion of routine dental cleanings, usually reimbursing a fixed amount (e.g., $100-$300 annually).
Payment Plans and Financing Options
- CareCredit / Scratchpay: These are popular third-party financing solutions. They offer various payment plans, including options for 0% interest if paid within a certain timeframe (e.g., 6, 12, 18 months). Interest accrues if not paid in full.
- In-house Payment Plans: Some veterinary clinics, especially those you have a long-standing relationship with, may offer their own payment arrangements. Always inquire.
- Pet Savings Account: Establishing a dedicated savings fund for your pet's health can be the most straightforward way to manage these costs without debt.
Cost-Saving Tips
- Preventative Home Care: Consistent daily brushing and VOHC-approved dental products are the best long-term cost-saving measure, delaying the need for professional cleanings.
- Early Intervention: Addressing bad breath and dental issues when they are minor (gingivitis) is far less costly than waiting until severe periodontitis and multiple extractions are required.
- Annual Exams: Regular vet check-ups can catch problems early before they become expensive emergencies.
- Compare Estimates: Get detailed estimates from a few reputable local clinics, but consider all aspects of care (anesthesia protocols, monitoring, dental X-rays) not just the bottom line.
Frequently Asked Questions
H3: What is the main cause of bad breath in dogs?
The overwhelming majority of dog bad breath cases are caused by periodontal disease, which begins with the accumulation of plaque and tartar on the teeth. This buildup provides a breeding ground for bacteria that produce foul-smelling volatile sulfur compounds. Without regular cleaning, this progresses to inflammation of the gums (gingivitis) and eventually to the destruction of the tooth's supporting structures (periodontitis).
H3: Can home remedies really fix my dog's bad breath?
While consistent daily home dental care, such as brushing with pet toothpaste and using VOHC-approved dental chews or water additives, can significantly prevent and manage mild bad breath, it usually cannot "fix" bad breath caused by established periodontal disease. Once tartar has formed, it requires professional veterinary scaling under anesthesia to remove it effectively. Home remedies are best for prevention and maintenance after a professional cleaning.
H3: Is it normal for puppies to have bad breath?
Puppies typically have relatively neutral breath. If a puppy has strong bad breath, it could indicate issues like trapped food between baby teeth, a foreign object, or even an early sign of an underlying systemic illness. Sometimes, it's associated with teething or eating things they shouldn't. Any persistent bad breath in a puppy should be checked by a veterinarian.
H3: How often should my dog get their teeth professionally cleaned?
The frequency of professional dental cleanings varies greatly depending on your dog's breed, genetics, age, diet, and the effectiveness of your home care routine. Some dogs may need annual cleanings, especially small breeds or those prone to dental disease, while others might only need them every 2-3 years. Your veterinarian will assess your dog's oral health during annual check-ups and recommend a suitable schedule.
H3: What if my dog won't let me brush their teeth?
Many dogs resist tooth brushing initially. Start slowly and make it a positive experience with treats and praise. Begin by simply letting them lick pet toothpaste off your finger, then gradually introduce a finger brush, and eventually a toothbrush. If brushing remains impossible, discuss alternative VOHC-accepted dental products like chews, diets, or water additives with your vet.
H3: Can bad breath be a sign of something serious?
Absolutely. While most cases are dental-related, bad breath can be a symptom of serious systemic diseases. A sweet, fruity smell can indicate diabetes; an ammonia-like odor might signal kidney disease; and a musty smell can point to liver disease. Oral tumors or severe infections can also cause very foul breath. Any sudden change or persistent, severe bad breath warrants immediate veterinary attention.
H3: What is the typical cost for a dental cleaning with extractions?
A professional dental cleaning with extractions in the US can range from $1,000 to $2,800 or more, depending on the number and complexity of extractions, your location, and the veterinary clinic. This cost typically includes pre-anesthetic blood work, anesthesia, IV fluids, scaling, polishing, dental X-rays, the extractions themselves, and post-operative medications.
H3: Does pet insurance cover dental cleanings?
Most standard pet insurance policies (accident/illness) do not cover routine dental cleanings. However, many providers offer "Wellness Plans" or "Preventative Care Add-ons" that do include coverage for annual dental cleanings, often reimbursing a set amount. Treatment for dental disease (e.g., extractions for periodontitis) is usually covered by accident/illness policies, provided it's not a pre-existing condition and waiting periods are met.
H3: What are VOHC-accepted products?
VOHC stands for the Veterinary Oral Health Council. Products bearing the VOHC seal of acceptance (e.g., certain dental chews, diets, water additives) have undergone rigorous scientific testing and are proven to effectively reduce plaque, tartar, or both. They are a valuable tool in maintaining your dog's oral health alongside regular brushing and vet visits.
H3: How long does it take to recover from a dental cleaning or extractions?
For a routine dental cleaning without extractions, recovery is typically within 24-48 hours, with dogs being back to their normal selves. If extractions were performed, full recovery of the gums and soft tissues can take 7-14 days. Your dog will need soft food and restricted activity during this period, and pain medication will be prescribed to manage discomfort.
When to See a Dentist (Veterinarian)
Knowing when your dog's bad breath warrants a trip to the vet is crucial. While a mild, temporary odor might be harmless, persistent or severe halitosis is a definite red flag.
Clear Warning Signs That Need Immediate Attention:
- Sudden onset of extremely foul breath: A rapid change to a very strong, putrid smell.
- Any change in breath odor to sweet/fruity, ammonia-like, or musty: These are critical indicators of potential diabetes, kidney disease, or liver disease, respectively, requiring immediate diagnostic evaluation.
- Accompanying signs of pain: Reluctance to eat, dropping food, chewing on one side, pawing at the mouth, excessive drooling (especially bloody or pus-tinged).
- Visible oral abnormalities: Red, swollen, or bleeding gums, severe plaque/tartar buildup, loose or broken teeth, visible masses/growths in the mouth.
- Facial swelling: Especially under an eye or along the jawline, indicating a potential abscess.
- Systemic illness signs: Lethargy, increased thirst and urination, unexplained weight loss, vomiting, diarrhea, or yellowing of the skin/eyes (jaundice).
Red Flags vs. Routine Care Guidance:
- Red Flag (Emergency/Urgent Appointment): If your dog exhibits any of the "Clear Warning Signs" above, particularly changes in breath odor suggesting systemic disease or signs of severe pain/infection, schedule an urgent veterinary appointment. These issues can quickly become life-threatening.
- Routine Care (Scheduled Appointment): If your dog's breath is consistently unpleasant but without any of the acute warning signs, it likely indicates progressive periodontal disease. While not an emergency, it's a chronic condition that will worsen over time. Schedule a non-urgent appointment with your veterinarian for an oral examination and to discuss a professional dental cleaning. Delaying this will only lead to more severe disease, pain, and higher treatment costs.
Pro Tip: Don't wait until your dog is obviously suffering. Dogs are masters at hiding pain. If you notice any persistent bad breath, even without other overt symptoms, it's always best to have your veterinarian assess the situation. Early detection and intervention are key to preventing discomfort, serious health complications, and expensive treatments down the line.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
What Cause Bad Breath
For many, a quick mint or a swig of mouthwash is the go-to solution for an unpleasant taste or odor in the mouth. But what if that bad breath, medically known as halitosis, is a persistent problem that no amount of peppermint can conquer? It’s a far more common issue than you might think, affecting
February 23, 2026

Dogs Bad Breath: Complete Guide
One whiff is all it takes: that distinctly unpleasant odor emanating from your beloved canine companion. If you've ever wondered, "Why does my dog's breath smell so bad?" you're not alone. It's a common concern among pet owners, with over 80% of dogs showing signs of oral disease by age three. W
February 23, 2026

Sudden Bad Breath in Toddlers: Complete Guide
When your toddler, who usually smells sweet and innocent, suddenly develops an unpleasant odor in their breath, it can be an alarming experience for any parent. Sudden bad breath in toddlers, also known as halitosis, is more common than you might think, affecting a significant number of young ch
February 23, 2026

Mouth Wash for Bad Breath: Complete Guide
Bad breath, medically known as halitosis, is an incredibly common and often embarrassing condition that affects a significant portion of the global population. In the United States alone, more than 80 million people suffer from chronic bad breath, impacting social interactions, professional conf
February 23, 2026