Teeth Whitening Kit: Complete Guide
Key Takeaways
- Did you know that over 80% of Americans wish they had whiter teeth? A bright, confident smile isn't just about aesthetics; it significantly impacts self-esteem, social interactions, and even professional opportunities. For many, achieving that dazzling smile often begins with exploring a **teeth
Did you know that over 80% of Americans wish they had whiter teeth? A bright, confident smile isn't just about aesthetics; it significantly impacts self-esteem, social interactions, and even professional opportunities. For many, achieving that dazzling smile often begins with exploring a teeth whitening kit. These popular at-home solutions promise to lighten tooth discoloration and enhance your smile without requiring multiple dental visits. But with a dizzying array of options on the market, understanding which kit is right for you, how to use it safely, and what results to expect can be overwhelming. This comprehensive guide from SmilePedia.net will demystify the world of at-home teeth bleaching, helping you make informed decisions about rejuvenating your smile. We'll delve into the different types of kits, how they work, potential risks, cost considerations, and crucial steps to ensure safe and effective whitening, ultimately empowering you to achieve the radiant smile you've always desired.
Key Takeaways:
- Effectiveness & Safety: At-home teeth whitening kits can effectively lighten extrinsic stains by several shades, but professional guidance is always recommended to ensure safety and rule out underlying dental issues.
- Active Ingredients: Most kits use hydrogen peroxide or carbamide peroxide. Hydrogen peroxide acts faster, while carbamide peroxide is more stable and has a longer shelf life. Concentrations typically range from 3-20% for hydrogen peroxide and 10-35% for carbamide peroxide.
- Types & Costs: Options include whitening strips (approx. $20-$70), brush-on gels (approx. $15-$50), tray-based systems (approx. $40-$200), and LED light kits (approx. $50-$300). Custom-fitted trays from a dentist can cost $300-$600.
- Timeline for Results: Visible results often appear within a few days to two weeks of consistent use, with optimal results typically seen after 2-4 weeks. Maintenance treatments may be needed every 3-6 months.
- Potential Side Effects: Temporary tooth sensitivity and gum irritation are common but usually subside after discontinuing or reducing use. Using products with fluoride and desensitizing agents can help.
- Insurance & Alternatives: Teeth whitening is generally considered cosmetic, so dental insurance rarely covers the cost. For severe discoloration or intrinsic stains, alternatives like professional in-office whitening ($400-$1,500) or cosmetic dental solutions like veneers teeth ($800-$2,500 per tooth) may be necessary.
- ADA Guidance: Always look for products with the American Dental Association (ADA) Seal of Acceptance, indicating they meet safety and efficacy standards when used as directed.

What is a Teeth Whitening Kit? An Overview
A teeth whitening kit is a collection of products designed for at-home use to lighten the shade of natural tooth enamel. These kits typically contain a whitening agent, most commonly hydrogen peroxide or carbamide peroxide, along with an application method such as strips, gels, trays, or a combination of these, sometimes paired with an LED light accelerator. The goal of a teeth whitening kit is to remove extrinsic (surface) stains caused by food, drinks, and tobacco, and in some cases, to penetrate the enamel to lighten intrinsic (deeper) discoloration.
The process of teeth bleaching relies on these peroxide-based chemicals to break down chromogens, the colored molecules responsible for stains, into smaller, colorless molecules. This chemical reaction occurs on the tooth surface and within the microscopic pores of the enamel, resulting in a visibly brighter smile. While professional in-office whitening treatments use much higher concentrations of whitening agents under controlled conditions, at-home kits provide a more convenient and cost-effective alternative for individuals seeking a noticeable improvement in tooth brightness. It's crucial to understand that these kits are most effective on natural teeth and will not whiten existing dental restorations such as fillings, crowns, or veneers teeth.
Types of Teeth Whitening Kits / Variations
The market for at-home teeth whitening kits is vast, offering a variety of application methods and active ingredients. Each type has its own advantages, disadvantages, and suitability for different users. Understanding these variations is key to choosing the right kit for your needs.
Whitening Strips
Whitening strips are thin, flexible pieces of polyethylene plastic coated with a peroxide-based whitening gel. They are designed to adhere directly to the front surfaces of your teeth.
- How they work: Users peel a strip from its liner and press it onto the teeth, typically wearing them for 30 minutes to an hour, once or twice daily, for a period of 7 to 14 days. The peroxide gel is in direct contact with the tooth enamel.
- Pros: Very convenient, easy to use, widely available, and generally affordable. Many brands carry the ADA Seal of Acceptance.
- Cons: May not cover all tooth surfaces, especially between teeth or on irregularly shaped teeth, leading to uneven whitening. Can cause temporary gum irritation if placed too far onto the gums. Peroxide concentration is typically lower (around 3-10% hydrogen peroxide), meaning results can be more gradual.
Whitening Gels (Brush-on and Tray-based)
Whitening gels offer a versatile approach, allowing for more controlled application.
Brush-On Whitening Gels
- How they work: These gels come in a tube with a brush applicator. Users simply brush a thin layer of gel directly onto the tooth surfaces, often twice a day. The gel typically dries quickly and stays on the teeth.
- Pros: Allows for targeted application, good for minor touch-ups or specific stained areas. Generally very affordable and discreet.
- Cons: The gel can be easily rubbed off by lips or saliva, reducing contact time and effectiveness. Peroxide concentration is usually low, requiring longer treatment periods for noticeable results.
Tray-Based Whitening Gels
- How they work: This method involves applying a whitening gel into a dental tray, which is then placed over the teeth. Kits either come with boil-and-bite trays (which mold to your teeth after softening in hot water) or, less commonly in OTC kits, pre-filled disposable trays. Dentists can provide custom-fitted trays for a superior fit.
- Pros: Ensures more consistent and prolonged contact of the whitening gel with the tooth surfaces compared to strips or brush-on gels. Higher concentrations of peroxide are often available in professional tray-based systems, leading to faster and more dramatic results.
- Cons: Boil-and-bite trays may not fit perfectly, potentially leading to gel leakage and gum irritation. Custom trays are more effective but significantly more expensive. Can be messier than strips.
LED Light Whitening Kits
These kits combine a whitening gel (often applied via a syringe into a tray or directly onto teeth) with an LED light device.
- How they work: After applying the whitening gel to the teeth or a tray, the user positions an LED light device in their mouth. The light is marketed to accelerate the chemical reaction of the peroxide, speeding up the whitening process.
- Pros: Many users report faster results due to the perceived catalytic effect of the light. Can provide noticeable whitening in a shorter timeframe compared to gel-only applications.
- Cons: The scientific evidence supporting the efficacy of LED lights in accelerating at-home whitening (especially low-power consumer devices) is mixed and often debated within the dental community. The primary whitening action still comes from the peroxide gel. These kits are generally more expensive. Poorly designed lights or gels can cause uneven results or excessive sensitivity.
Whitening Pens
- How they work: Similar to brush-on gels, these pens contain a whitening gel dispensed via a brush tip. They are typically used for quick touch-ups or on-the-go application.
- Pros: Extremely convenient and portable. Ideal for maintaining results or addressing minor new stains.
- Cons: Very low peroxide concentration means limited whitening power for significant discoloration. Requires consistent, frequent application for any noticeable effect.
Whitening Toothpastes and Mouthwashes (Often Not True "Kits")
While not typically considered a "kit," these products contain mild abrasive or chemical polishing agents to remove surface stains.
- How they work: They typically rely on gentle abrasives (like silica) or chemical agents (like blue covarine) to polish the tooth surface and lift superficial stains. They do not significantly change the inherent color of the tooth.
- Pros: Everyday oral hygiene products, very easy to incorporate into a routine. Affordable.
- Cons: Only effective for extrinsic stains and typically only by one or two shades, if at all. Do not contain peroxide in concentrations high enough for true teeth bleaching.
Pro Tip: For the most effective and safest at-home whitening, consult your dentist. They can recommend professional-grade take-home kits with custom-fitted trays and higher-concentration gels, or discuss whether alternatives like veneers teeth are more appropriate for your aesthetic goals, especially if you have resistant staining or intrinsic discoloration.
Causes of Tooth Discoloration / Why It Happens
Understanding why teeth become discolored is crucial for effective whitening and long-term prevention. Tooth discoloration can be broadly categorized into extrinsic and intrinsic stains.
Extrinsic Stains (External)
These are stains that accumulate on the surface of the tooth enamel. They are the most common type of discoloration and are generally the most responsive to teeth whitening kit treatments.
- Dietary Habits: Consuming dark-colored foods and beverages regularly is a primary culprit. Examples include:
- Coffee and Tea: Tannins and chromogens in these drinks penetrate microscopic pores in the enamel.
- Red Wine: Its dark pigments and acidity contribute to staining.
- Dark-Colored Berries: Blueberries, blackberries, and cherries contain strong pigments.
- Sauces: Soy sauce, tomato sauce, and balsamic vinegar.
- Soda/Soft Drinks: Even clear sodas can be acidic, eroding enamel and making it more susceptible to staining.
- Tobacco Use: Smoking cigarettes, cigars, or using chewing tobacco introduces tar and nicotine, which create stubborn yellow and brown stains that are particularly difficult to remove.
- Poor Oral Hygiene: Inadequate brushing and flossing allow plaque and tartar to build up. This rough surface is more prone to absorbing stains from foods and drinks.
- Chromogenic Bacteria: Certain bacteria in the mouth can produce colored compounds that contribute to surface stains, especially in children.
Intrinsic Stains (Internal)
These stains occur within the tooth structure, either in the enamel or the dentin (the layer beneath the enamel). Intrinsic stains are often more challenging to treat with at-home whitening kits and may require professional intervention or alternative cosmetic solutions like veneers teeth.
- Aging: As we age, the outer layer of enamel thins, revealing more of the yellowish dentin underneath. Additionally, dentin naturally darkens over time.
- Trauma: A direct blow to a tooth can cause internal bleeding and changes in the dentin, leading to a gray or brown discoloration.
- Medications:
- Tetracycline Antibiotics: If taken during tooth development (childhood or pregnancy), tetracycline can cause permanent gray-blue or brown banding on the teeth.
- Minocycline (a tetracycline derivative): Can cause discoloration in adults.
- Chlorhexidine (antiseptic mouthwash): Prolonged use can cause brown surface stains, which can sometimes penetrate deeper.
- Excessive Fluoride Intake (Fluorosis): Overexposure to fluoride during tooth development can result in white spots, streaks, or brown pits on the enamel.
- Genetics: Some individuals naturally have brighter or darker enamel than others.
- Dental Restorations: Old amalgam (silver) fillings can stain surrounding tooth structure, giving a grayish hue.
- Root Canal Treatment: A tooth that has undergone a root canal can darken over time if the pulp tissue wasn't completely removed or due to internal bleeding.
Understanding the cause of your tooth discoloration is crucial. If you suspect intrinsic staining, especially from medication or trauma, an at-home teeth whitening kit may not yield the desired results, and a consultation with your dentist is highly recommended to explore more effective options.
Signs and Symptoms of Tooth Discoloration
The primary "sign" of tooth discoloration is, quite simply, teeth that are not as white as you'd like them to be. However, discoloration isn't always uniform and can manifest in various shades and patterns, offering clues about its underlying cause.
What to look for:
- Overall Yellowish Hue: This is the most common type of discoloration, often caused by aging, diet, and poor oral hygiene. It typically responds well to most teeth whitening kit applications.
- Brownish Stains: Often associated with heavy coffee, tea, red wine, or tobacco use. These can be more stubborn than yellow stains but are still considered extrinsic.
- Grayish or Blue-Gray Hue: This can indicate intrinsic staining, often linked to tetracycline use or a past tooth injury. These types of stains are much harder to whiten with over-the-counter kits and may require professional treatment or cosmetic solutions like veneers teeth.
- White Spots or Streaks: These can be a sign of dental fluorosis (excessive fluoride exposure during tooth development) or enamel hypoplasia (a defect in enamel formation). While not strictly "stains," they contribute to uneven tooth color. Whitening can sometimes make these spots more prominent temporarily, as the surrounding enamel whitens faster.
- Dark Spots or Pits: These might indicate cavities, old fillings leaking at the margins, or severe fluorosis. Whitening will not resolve these issues; a dentist needs to address them.
- Uneven Staining: Sometimes teeth stain differently. For example, the canine teeth (eyeteeth) are naturally a shade darker than the incisors due to thicker dentin. Also, individual teeth might have specific areas of discoloration.
- Darkening Around Existing Restorations: If you have composite fillings (white fillings), crowns, or veneers teeth, you might notice that your natural teeth are darkening around them. This is because whitening kits only affect natural tooth structure, and the restorations themselves do not change color, leading to a mismatch.
If you notice any unusual or sudden discoloration, or if your teeth are sensitive or painful along with discoloration, it's always best to consult a dentist. They can diagnose the cause and recommend the most appropriate and safest course of action, which may or may not involve an at-home teeth bleaching product.
Treatment Options
While this article focuses on the teeth whitening kit, it's important to understand the full spectrum of treatment options for tooth discoloration. The best choice depends on the type and severity of stains, your budget, and your aesthetic goals.
A. At-Home Teeth Whitening Kits (Focus of this Guide)
As detailed above, these are over-the-counter or dentist-prescribed kits used at home.

- Pros:
- Convenience: Can be used on your own schedule.
- Cost-Effective: Generally much cheaper than in-office treatments.
- Accessibility: Widely available at pharmacies, supermarkets, and online.
- Cons:
- Lower Concentration: Generally less potent than professional treatments, meaning slower or less dramatic results.
- Potential for Uneven Results: Especially with strips or ill-fitting trays.
- Temporary Side Effects: Sensitivity and gum irritation are common if used incorrectly or excessively.
- Not for All Stains: Less effective on intrinsic stains.
- No Professional Supervision: Increases the risk of misuse or exacerbating existing dental problems.
B. Professional In-Office Whitening
Performed by a dentist in a dental office.
- How it works: A high-concentration peroxide gel (often 25-40% hydrogen peroxide) is applied to the teeth. Gums and soft tissues are carefully protected. Sometimes a special light (LED, laser, or UV) is used to activate or accelerate the gel.
- Pros:
- Fastest Results: Significant whitening can be achieved in a single 1-2 hour session.
- Most Dramatic Results: Due to higher peroxide concentrations.
- Safest Option: Performed under professional supervision, minimizing gum irritation and ensuring proper application.
- Addresses Deeper Stains: More effective on intrinsic discoloration than at-home kits.
- Cons:
- Cost: Significantly more expensive, typically ranging from $400 to $1,500 per session.
- Temporary Sensitivity: Can be more pronounced due to the higher concentration of whitening agents.
- Multiple Sessions: May require more than one visit for optimal results, depending on the desired shade.
C. Dentist-Prescribed Take-Home Whitening Kits
These kits bridge the gap between over-the-counter options and in-office treatments.
- How it works: Your dentist takes impressions of your teeth to create custom-fitted whitening trays. You receive professional-strength whitening gel (e.g., 10-20% carbamide peroxide) and instructions for home use, typically wearing the trays for a few hours daily or overnight for 1-2 weeks.
- Pros:
- Custom Fit: Trays ensure excellent contact of the gel with teeth and minimize leakage onto gums, reducing irritation.
- Higher Potency: Gels are stronger than OTC options, leading to better and faster results than non-custom kits.
- Professional Guidance: Dentist monitors progress and addresses any concerns.
- More Affordable than In-Office: Typically costs $300-$600.
- Cons:
- Still Requires Home Use: Not an instant solution.
- Upfront Cost: More expensive than OTC kits.
D. Dental Veneers
For severe or intrinsic stains that resist teeth bleaching, or for patients seeking to correct other cosmetic imperfections (gaps, chips, misalignments), veneers teeth are an excellent alternative.
- How they work: Veneers are thin, custom-made shells, typically made of porcelain or resin composite, that are bonded to the front surface of the teeth. They completely cover the natural tooth, masking any discoloration.
- Pros:
- Permanent Whitening: The color is chosen by you and is permanent, resistant to future stains.
- Masks Severe Discoloration: Ideal for tetracycline stains, severe fluorosis, or teeth that are otherwise non-responsive to whitening.
- Addresses Other Cosmetic Issues: Can correct shape, size, and minor alignment problems.
- Durable: Porcelain veneers are very strong and can last 10-15 years or more with proper care.
- Cons:
- Irreversible: Requires removal of a small amount of tooth enamel, making the process irreversible.
- Cost: Significant investment, ranging from $800 to $2,500 per tooth for porcelain veneers.
- Not for Everyone: Requires healthy underlying tooth structure.
E. Dental Bonding
Similar to veneers, but uses a tooth-colored resin material.
- How it works: A composite resin material is applied directly to the tooth, sculpted, hardened with a light, and then polished.
- Pros:
- Less Invasive: Less enamel removal than veneers.
- More Affordable: Typically $100-$400 per tooth.
- Can be done in one visit.
- Cons:
- Less Durable: More prone to chipping and staining than porcelain veneers.
- Shorter Lifespan: Typically lasts 5-7 years.
- Not ideal for widespread severe discoloration.
Pro Tip: Before pursuing any whitening treatment, especially an at-home teeth whitening kit, it's crucial to have a dental check-up. Your dentist can identify the cause of your stains, check for cavities or gum disease (which need to be treated before whitening), and determine if your existing restorations will create an uneven appearance after whitening.
Step-by-Step Process for Using a Teeth Whitening Kit
While specific instructions vary by product, a general step-by-step guide can help you understand what to expect when using a typical at-home teeth whitening kit. Always read and follow the manufacturer's instructions precisely for your chosen product.
1. Pre-Treatment Preparation
- Consult Your Dentist (Highly Recommended): Before starting any teeth bleaching regimen, schedule a dental check-up. Your dentist can assess your oral health, identify the cause of your stains, and advise if a whitening kit is suitable for you. They can also address any underlying issues like cavities or gum disease that could be exacerbated by whitening agents.
- Brush and Floss Thoroughly: Always clean your teeth thoroughly before applying any whitening product. This removes plaque and food debris, allowing the whitening gel to make direct contact with your enamel. Wait at least 30 minutes after brushing before applying to avoid gum irritation from toothpaste ingredients.
- Dry Your Teeth (Optional but Recommended): For some kits, especially those involving gels applied directly to the teeth or strips, gently drying your teeth with a tissue can help the product adhere better and prevent dilution by saliva.
2. Application (Varies by Kit Type)
For Whitening Strips:
- Open Packet: Carefully peel the whitening strip from its backing. You'll usually have separate strips for upper and lower teeth.
- Apply to Teeth: Align the strip with the gum line on your front teeth. Gently press and mold the strip to ensure good contact with all tooth surfaces, especially between teeth. Fold the excess strip material over the back of your teeth to secure it.
- Wear for Recommended Time: Leave the strips on for the duration specified by the manufacturer, typically 30-60 minutes. Avoid eating, drinking, or talking excessively during this time.
For Tray-Based Gels (Boil-and-Bite or Custom Trays):
- Prepare Trays (Boil-and-Bite): If using boil-and-bite trays, follow the instructions to soften them in hot water and then bite into them to create an impression of your teeth. Trim any excess plastic that irritates your gums.
- Load Gel: Dispense a small bead of whitening gel into each tooth compartment of the tray, typically a thin line along the front surface. Be careful not to overfill, as excess gel can leak onto your gums.
- Insert Trays: Place the trays firmly over your teeth. Gently press to ensure the gel spreads evenly. Wipe away any excess gel that seeps onto your gums with a clean finger or cotton swab.
- Wear for Recommended Time: Wear the trays for the duration specified, which can range from 30 minutes to several hours, or even overnight, depending on the gel concentration.
For Brush-On Gels or Whitening Pens:
- Twist/Click to Dispense: Follow product instructions to dispense a small amount of gel onto the brush tip.
- Apply Thin Layer: Brush a thin, even layer of gel directly onto the front surfaces of your teeth. Ensure good coverage.
- Allow to Dry/Set: Keep your lips away from your teeth for the recommended drying time (usually 30 seconds to a minute) to allow the gel to set and prevent it from being wiped off.
- Avoid Eating/Drinking: Refrain from eating or drinking for a specified period (e.g., 30 minutes) after application to allow the gel to work.
For LED Light Kits:
- Apply Gel: Depending on the kit, you'll either apply gel directly to your teeth, load it into a tray, or use pre-filled trays.
- Position Light: Insert the LED light device into your mouth, ensuring it's positioned correctly over your teeth.
- Activate Light: Turn on the LED light and keep it in place for the recommended duration, often 10-30 minutes per session.
3. Post-Application Care
- Remove Product: After the recommended treatment time, remove strips, trays, or simply rinse your mouth thoroughly with water to remove any remaining gel.
- Clean Trays (if applicable): If using reusable trays, rinse them with cool water and store them in a clean, dry case.
- Avoid Staining Foods/Drinks: For at least 30 minutes to an hour after whitening (and ideally for the first 24-48 hours, especially if you experience sensitivity), avoid highly pigmented foods and beverages to prevent re-staining. This is often called the "white diet."
- Manage Sensitivity: If you experience tooth sensitivity, use a desensitizing toothpaste, reduce the frequency or duration of your whitening sessions, or take breaks between treatments.
4. Consistency and Monitoring
- Follow Schedule: Use the kit as directed by the manufacturer, typically daily for 7-14 days. Consistency is key for achieving optimal results.
- Monitor Results: Many kits come with a shade guide. Use it to track your progress.
- Don't Overuse: Resist the temptation to whiten longer or more frequently than recommended, as this can increase sensitivity and gum irritation without significantly enhancing results.
Pro Tip: If you notice any burning, prolonged sensitivity, significant gum irritation, or other adverse reactions, stop using the teeth whitening kit immediately and contact your dentist.
Cost and Insurance
Understanding the financial aspect of teeth whitening is crucial, as dental insurance rarely covers cosmetic procedures.
Cost of Teeth Whitening Kits
The cost of a teeth whitening kit varies significantly based on the brand, type of kit, and where you purchase it.
- Whitening Strips:
- Low: $20 - $35 (e.g., generic brands, smaller packs)
- Mid: $35 - $50 (e.g., popular brands like Crest 3D White)
- High: $50 - $70+ (e.g., advanced formulas, larger packs, sensitivity-focused options)
- Brush-on Gels / Whitening Pens:
- Low: $15 - $30
- Mid: $30 - $40
- High: $40 - $50+
- Tray-Based Systems (OTC with boil-and-bite trays):
- Low: $40 - $80
- Mid: $80 - $150
- High: $150 - $200+
- LED Light Kits (with gel):
- Low: $50 - $100 (basic models)
- Mid: $100 - $200 (more advanced features, better brands)
- High: $200 - $300+ (premium brands, often including custom-like trays)
- Dentist-Prescribed Take-Home Kits (custom trays and professional gel):
- Average: $300 - $600
Cost of Professional Whitening and Alternatives
For comparison, and as alternatives if kits aren't suitable:
- In-Office Professional Whitening:
- Average: $400 - $1,500 per session (can vary significantly by region and dental practice, often higher in metropolitan areas like New York or Los Angeles).
- Dental Veneers (Porcelain):
- Average: $800 - $2,500 per tooth (cost varies greatly depending on material, lab fees, and dentist's expertise).
- Dental Bonding:
- Average: $100 - $400 per tooth.
Insurance Coverage
- Teeth Whitening Kits (and all forms of teeth bleaching): Dental insurance typically does not cover the cost of teeth whitening, whether it's an at-home kit, dentist-prescribed take-home kit, or in-office professional treatment. Whitening is almost universally classified as a cosmetic procedure, not medically necessary for oral health.
- Veneers and Bonding:
- Cosmetic: If veneers or bonding are done purely for aesthetic reasons (e.g., to whiten teeth or close minor gaps), insurance will likely not cover them.
- Restorative: If veneers or bonding are deemed medically necessary to restore a damaged tooth (e.g., a severely chipped tooth from an accident), some portion of the cost might be covered. You would need to check with your specific insurance provider.

Payment Plans and Financing Options
Since dental insurance rarely covers these cosmetic procedures, many dental offices offer various payment solutions:
- In-Office Payment Plans: Some dentists allow patients to pay for more expensive treatments (like professional whitening or veneers) in installments directly through their office.
- Third-Party Financing: Companies like CareCredit or LendingClub provide specialized healthcare credit cards with low or no-interest financing options for qualified patients over a set period.
- Dental Savings Plans: These are membership programs where you pay an annual fee and get discounts (typically 10-60%) on dental procedures, including cosmetic ones, from participating dentists. These are not insurance but can offer significant savings.
Pro Tip: Always get a detailed cost estimate from your dentist before committing to any professional whitening or cosmetic procedure. Ask about all-inclusive pricing and inquire about any available payment options.
Recovery and Aftercare
Once you've achieved your desired shade using a teeth whitening kit, proper aftercare is essential to maintain your results and minimize any temporary side effects.
Managing Temporary Sensitivity
Tooth sensitivity is one of the most common side effects of teeth bleaching, affecting up to 70% of users. It typically manifests as a sharp, shooting pain when teeth are exposed to cold, hot, or sweet stimuli.
- Use a Desensitizing Toothpaste: Many toothpastes contain ingredients like potassium nitrate or strontium chloride, which block the tubules in the dentin that lead to the tooth's nerve. Use these for a few weeks before, during, and after whitening.
- Reduce Whitening Frequency/Duration: If sensitivity becomes uncomfortable, try reducing the amount of time you wear your trays or strips, or whiten every other day instead of daily.
- Take a Break: A few days' break from whitening can often resolve sensitivity.
- Apply Fluoride Gel: Your dentist might prescribe or recommend an over-the-counter fluoride gel or rinse, which can help strengthen enamel and reduce sensitivity.
- Avoid Extreme Temperatures: For a day or two after whitening, try to avoid very hot or very cold foods and drinks.
- Over-the-Counter Pain Relievers: Ibuprofen or acetaminophen can help manage discomfort if needed.
Maintaining Your New White Smile ("White Diet")
To prolong the results from your teeth whitening kit, pay attention to your diet and habits, especially immediately after treatment.
- Avoid Staining Foods and Drinks: For at least 24-48 hours after your final whitening session, your teeth are more susceptible to staining. Adhere to a "white diet" by avoiding:
- Coffee, tea, red wine, dark sodas
- Berries (blueberries, blackberries, raspberries)
- Dark sauces (soy sauce, balsamic vinegar, tomato sauce)
- Artificial food colorings
- Tobacco products (smoking, chewing tobacco)
- Drink with a Straw: When consuming staining beverages, using a straw can help minimize contact with your front teeth.
- Rinse Immediately: If you do consume staining foods or drinks, rinse your mouth with water immediately afterward.
- Good Oral Hygiene: Continue to brush twice daily and floss once daily. Consider using a whitening toothpaste designed for maintenance (which typically contains mild abrasives, not bleaching agents).
Long-Term Maintenance
- Regular Dental Check-ups and Cleanings: Visiting your dentist every six months for professional cleanings will help remove new surface stains before they become deeply embedded.
- Touch-Up Treatments: The effects of a teeth whitening kit are not permanent. Most people find they need touch-up treatments every 3-6 months, or annually, depending on their diet and habits. You can use your remaining kit materials or purchase a new one for maintenance.
- Address Habits: Reducing or eliminating tobacco use and moderating consumption of highly staining foods and drinks will significantly extend your whitening results.
Prevention of Tooth Discoloration
While teeth whitening kits can reverse existing stains, preventing them in the first place is the most effective strategy for maintaining a bright smile.
- Maintain Excellent Oral Hygiene:
- Brush Twice Daily: Use a fluoride toothpaste and brush for at least two minutes each time.
- Floss Daily: Flossing removes plaque and food particles from between teeth, areas often prone to staining and decay.
- Use an Antiseptic Mouthwash: Can help reduce bacteria that contribute to plaque and stains. Look for alcohol-free options to avoid drying out your mouth.
- Limit Staining Foods and Beverages:
- Reduce Consumption: Cut back on coffee, tea, red wine, dark sodas, and highly pigmented fruits like berries.
- Rinse After Consumption: If you consume staining items, rinse your mouth with water immediately afterward to wash away pigments before they can set.
- Use a Straw: For beverages like soda or iced coffee, a straw can help bypass your front teeth.
- Avoid Tobacco Products: Smoking and chewing tobacco are major contributors to severe extrinsic stains and numerous other oral and systemic health problems. Quitting tobacco is one of the most impactful steps you can take for your oral health and teeth brightness.
- Regular Dental Check-ups and Cleanings: Professional dental cleanings every six months (or as recommended by your dentist) are crucial. Your hygienist can remove plaque, tartar, and surface stains that regular brushing can't tackle, preventing them from accumulating and causing discoloration.
- Be Mindful of Medications: If you are prescribed medications known to cause tooth discoloration (like certain antibiotics), discuss alternatives or preventive strategies with your doctor and dentist.
- Protect Your Enamel: Enamel erosion makes teeth more susceptible to staining.
- Avoid Acidic Foods/Drinks: Citrus fruits, sodas, and highly acidic foods can weaken enamel.
- Don't Brush Immediately After Acidic Foods: The enamel is softened by acid; brushing too soon can abrade it. Wait at least 30 minutes.
- Use a Soft-Bristle Toothbrush: Hard brushing can wear down enamel over time.
- Address Bruxism (Teeth Grinding): Grinding can wear down enamel, exposing the darker dentin. Your dentist might recommend a nightguard.
By adopting these preventive measures, you can significantly reduce the need for frequent teeth bleaching and keep your smile naturally brighter for longer.
Risks and Complications of Teeth Whitening Kits
While generally safe when used as directed, teeth whitening kits are not without potential risks and complications. Being aware of these can help you use products safely and know when to consult a dentist.
1. Tooth Sensitivity
- Description: This is the most common side effect, characterized by a sharp, temporary pain when teeth are exposed to hot, cold, sweet, or acidic stimuli. It occurs when the peroxide penetrates the enamel and dentin, irritating the pulp (nerve) of the tooth.
- Risk Factors: Pre-existing sensitivity, receding gums, cracks in enamel, high peroxide concentration, prolonged application time.
- Management: Reduce application time, use less frequently, use a desensitizing toothpaste, take breaks, consult your dentist.
2. Gum Irritation (Chemical Burn)
- Description: The whitening gel, if it comes into prolonged contact with soft tissues, can cause irritation, redness, and even chemical burns on the gums. This is more common with ill-fitting trays or excess gel from strips/pens.
- Risk Factors: Overfilling trays, strips placed too far onto gums, high peroxide concentration.
- Management: Ensure proper fit and application, wipe away excess gel immediately, reduce concentration or frequency, stop use if irritation persists. Usually resolves within a few days once contact with the whitening agent is stopped.
3. Uneven Whitening
- Description: Sometimes, due to the shape of the teeth, application method, or presence of dental restorations, whitening can appear patchy or uneven.
- Risk Factors: Crooked teeth, strips not covering entire tooth surface, presence of fillings, crowns, or veneers teeth (which do not whiten).
- Management: Professional whitening or alternatives like veneers teeth may be needed for uniform results, especially if existing restorations are an issue.
4. Damage to Dental Restorations
- Description: Whitening agents do not lighten existing dental work such as composite fillings, dental crowns, or veneers teeth. This can lead to a noticeable color mismatch between your natural teeth and your restorations. While generally not "damaging" to the restorations themselves, it can necessitate their replacement if you desire a uniform bright smile.
- Risk Factors: Any existing dental work on front teeth.
- Management: Consult your dentist before whitening if you have restorations. They can advise on potential color mismatch and discuss options like replacing restorations after whitening.
5. Enamel Erosion (Rare with Proper Use)
- Description: While most studies show minimal to no permanent damage to enamel when ADA-approved products are used as directed, overuse or misuse of high-concentration whitening agents could potentially lead to minor surface changes or increased susceptibility to erosion over time.
- Risk Factors: Extremely high concentrations, prolonged exposure times far exceeding recommendations, acidic formulations, pre-existing enamel issues.
- Management: Always follow manufacturer instructions, do not exceed recommended treatment times or frequencies. Choose products with the ADA Seal of Acceptance.
6. Relapse of Stains
- Description: The effects of whitening are not permanent. Over time, teeth will naturally begin to re-stain due to dietary habits, tobacco use, and aging.
- Risk Factors: Continued consumption of staining foods/drinks, smoking, poor oral hygiene.
- Management: Regular touch-up treatments, good oral hygiene, and preventive measures.

When to Seek Professional Advice
It is always advisable to consult your dentist before starting any teeth bleaching regimen, especially if you have:
- Pre-existing tooth sensitivity or gum issues.
- Cavities, gum disease, or exposed tooth roots.
- Many dental restorations (fillings, crowns, veneers teeth).
- Intrinsic stains (e.g., from tetracycline or trauma).
- Any unusual pain, prolonged sensitivity, or severe gum irritation during treatment.
Your dentist can provide a professional assessment, recommend suitable options (including professional treatments or custom take-home kits), and address any underlying issues that could be negatively affected by a teeth whitening kit.
Comparison Tables
To help visualize the differences between popular teeth whitening options, here are two comparison tables: one for different types of at-home kits and another for comparing at-home kits with professional treatments and veneers teeth.
Table 1: At-Home Teeth Whitening Kit Comparison
| Feature | Whitening Strips | Tray-Based Gels (OTC) | LED Light Kits | Whitening Pens/Brush-on Gels |
|---|---|---|---|---|
| Active Ingredient | Hydrogen Peroxide (HP) or Carbamide Peroxide (CP) | HP or CP | HP or CP | HP or CP (often lower conc.) |
| Concentration Range | HP: 3-10%, CP: 10-20% | HP: 10-20%, CP: 15-35% | HP: 5-20%, CP: 15-35% | HP: <5%, CP: <10% |
| Application Method | Flexible strips adhere to teeth | Gel placed in boil-and-bite trays | Gel in tray/direct apply + LED light | Gel brushed directly onto teeth |
| Typical Cost (US) | $20 - $70 | $40 - $200 | $50 - $300 | $15 - $50 |
| Treatment Time | 30-60 min, 1-2x/day, for 7-14 days | 30 min - 2 hrs, 1-2x/day, for 7-21 days | 10-30 min, 1-2x/day, for 7-14 days | 2x/day, quick dry, for 7-21 days |
| Results | Good for extrinsic stains, 2-5 shades lighter | Very good for extrinsic, 3-7 shades lighter | Potentially faster/more dramatic, 3-8 shades | Mild for extrinsic, 1-2 shades lighter |
| Pros | Convenient, easy to use, affordable | Better coverage than strips, good control | Perceived faster results | Very convenient, portable, good for touch-ups |
| Cons | Uneven coverage, gum irritation if misplaced | Boil-and-bite trays can fit poorly, messy | Efficacy of light debated, higher cost | Low efficacy for significant stains, rubs off |
| Best For | First-time users, mild-moderate stains | Moderate-heavy stains, consistent results | Those seeking accelerated initial results | Minor touch-ups, on-the-go maintenance |
Table 2: At-Home Kits vs. Professional Treatments & Veneers
| Feature | At-Home Teeth Whitening Kit | Dentist-Prescribed Take-Home Kit | Professional In-Office Whitening | Veneers Teeth |
|---|---|---|---|---|
| Who Applies | You (patient) | You (patient) | Dentist/Hygienist | Dentist (prepared and bonded by professional) |
| Peroxide Concentration | Low (HP 3-20%, CP 10-35%) | Moderate (HP 10-20%, CP 15-40%) | High (HP 25-40%) | N/A (no whitening agent) |
| Typical Cost (US) | $20 - $300 | $300 - $600 | $400 - $1,500 | $800 - $2,500 per tooth (porcelain) |
| Insurance Coverage | Rarely/Never | Rarely/Never | Rarely/Never | Rarely/Never (if purely cosmetic) |
| Speed of Results | Gradual (days to weeks) | Moderate (1-2 weeks) | Fast (1-2 hours) | Immediate (after placement) |
| Degree of Whitening | Moderate (2-8 shades) | Very good (4-10 shades) | Excellent (5-12+ shades) | Complete masking of original color, permanent |
| Customization | Limited (generic strips, boil-and-bite trays) | High (custom-fitted trays) | High (professionally applied, protected gums) | Highest (custom-designed for shape, size, color) |
| Suitable For | Extrinsic stains, budget-conscious | Extrinsic/mild intrinsic, consistent results | Extrinsic/intrinsic, fast/dramatic results | Severe intrinsic stains, aesthetic issues (chips, gaps, misalignment) |
| Durability of Results | 3-6 months (with maintenance) | 6-12 months (with maintenance) | 6-24 months (with maintenance) | 10-15+ years (permanent color) |
| Irreversibility | Reversible | Reversible | Reversible | Irreversible (requires enamel removal) |
Children / Pediatric Considerations
Teeth whitening, particularly with peroxide-based teeth bleaching products, is generally not recommended for children and adolescents under the age of 16. There are several important reasons for this guideline:
- Developing Teeth: Young teeth have larger pulp chambers (the innermost part of the tooth containing nerves and blood vessels) and more permeable enamel compared to adult teeth. This makes them more susceptible to sensitivity and potential damage from whitening agents. Using a teeth whitening kit on developing teeth could lead to prolonged or severe sensitivity.
- Mixed Dentition: Most children and pre-teens have a mix of primary (baby) teeth and permanent teeth. Whitening agents only affect natural tooth structure, leading to an uneven appearance where the primary teeth may whiten differently or faster than the emerging permanent teeth.
- Irregular Eruption: Permanent teeth erupt at different stages. Whitening before all permanent teeth have fully erupted and settled can result in an inconsistent color, and areas that haven't been whitened will stand out later.
- Enamel Development Issues: Conditions like fluorosis (white spots from excessive fluoride during development) or enamel hypoplasia might become more noticeable after whitening, as the healthy enamel whitens faster than the areas with developmental defects.
- Compliance and Supervision: Younger children may not be able to reliably follow the detailed instructions for using a teeth whitening kit, increasing the risk of misuse, swallowing the whitening gel, or gum irritation.
When to Consider Whitening for Young Individuals
In rare cases, a dentist might recommend supervised whitening for adolescents with severe discoloration caused by trauma or certain medical conditions, especially if it significantly impacts their self-esteem. However, this would always be:
- Under Strict Dental Supervision: The dentist would assess the child's oral health, explain the risks, and provide professional-grade, lower-concentration products with custom-fitted trays to minimize gum exposure.
- Once Permanent Dentition is Complete: Ideally, waiting until all permanent teeth have fully erupted and calcified is preferred.
Alternatives for Children's Stains
For children experiencing tooth discoloration, parents should first consult a pediatric dentist. The cause of the stain needs to be identified.
- Extrinsic Stains: For surface stains caused by diet or poor hygiene, professional dental cleanings and improved brushing/flossing techniques are usually sufficient and highly effective.
- Intrinsic Stains: For intrinsic stains, especially those caused by trauma, your dentist might suggest waiting until the child is older to consider options like bonding, veneers teeth, or internal bleaching if suitable.
Pro Tip for Parents: Focus on prevention. Encourage good oral hygiene habits from an early age, limit sugary and staining foods/drinks, and ensure regular dental check-ups. If you're concerned about your child's tooth color, always speak to their dentist before attempting any at-home whitening solutions.
Cost Breakdown
While covered in the "Cost and Insurance" section, let's provide a clear, aggregated breakdown of average US costs for various whitening and cosmetic options, highlighting the financial implications.
At-Home Teeth Whitening Kits (Over-the-Counter)
These are the most accessible and affordable options.
- Average Cost: $20 - $300
- Whitening Strips: $20 - $70
- Brush-on Gels/Pens: $15 - $50
- Tray-Based Systems (Boil-and-Bite): $40 - $200
- LED Light Kits: $50 - $300
- Insurance Coverage: None.
- Payment Plans: Not applicable for OTC products.
Professional/Dentist-Supervised Options
These offer higher efficacy and safety but come at a higher price point.
- Dentist-Prescribed Take-Home Whitening Kit:
- Average Cost: $300 - $600 (includes custom trays and professional-strength gel)
- Insurance Coverage: None.
- Payment Plans: Some dental offices may offer in-house payment options or recommend third-party financing.
- In-Office Professional Whitening:
- Average Cost: $400 - $1,500 per session
- Insurance Coverage: None.
- Payment Plans: Often available through the dental office or third-party medical financing companies (e.g., CareCredit).
Cosmetic Alternatives for Severe Discoloration
For stains resistant to teeth bleaching or for comprehensive smile makeovers.
- Dental Bonding:
- Average Cost: $100 - $400 per tooth
- Insurance Coverage: Rarely, unless deemed restorative (e.g., repairing a chipped tooth).
- Payment Plans: May be available for multiple teeth, typically via dental office or financing.
- Porcelain Veneers Teeth:
- Average Cost: $800 - $2,500 per tooth
- Insurance Coverage: Rarely, unless deemed restorative for severe damage.
- Payment Plans: Most dental offices offer payment plans or third-party financing options due to the significant cost.
With vs. Without Insurance
As established, dental insurance typically does not cover cosmetic procedures like teeth bleaching or veneers teeth (if purely for aesthetics). Therefore, the "with insurance" cost is essentially the "without insurance" cost for these treatments, meaning you'll pay 100% out-of-pocket. Always confirm with your specific insurance provider, but generally, expect to cover the full cost.
Payment Plans and Financing Options
For more expensive procedures, consider:

- Dental Office Payment Plans: Many practices offer interest-free installment plans for a few months.
- Third-Party Medical Financing: Companies like CareCredit are widely accepted in dental offices and offer deferred interest or low-interest plans for healthcare expenses.
- Flexible Spending Accounts (FSA) / Health Savings Accounts (HSA): If you have an FSA or HSA through your employer, you can often use pre-tax dollars to pay for dental care, though cosmetic procedures may not always qualify. Check your plan's specific guidelines.
Cost-Saving Tips
- Start with OTC: For mild to moderate extrinsic stains, an affordable teeth whitening kit is a great starting point.
- Shop Around: Prices for professional services can vary between dental practices. Get consultations from a few trusted dentists.
- Dental Schools: University dental schools often offer services at a reduced cost, with treatment provided by supervised students.
- Dental Savings Plans: Consider joining a dental savings plan for discounts on various procedures.
- Focus on Prevention: The best way to save money on whitening is to prevent stains in the first place through excellent oral hygiene and smart dietary choices.
Frequently Asked Questions
What is the difference between teeth whitening and teeth bleaching?
While often used interchangeably, "teeth whitening" broadly refers to restoring a tooth's surface color by removing dirt and debris, often through abrasive toothpastes. "Teeth bleaching" specifically refers to using peroxide-based chemicals (like hydrogen peroxide or carbamide peroxide) to lighten the intrinsic color of the tooth enamel beyond its natural shade. Most teeth whitening kit products are actually considered teeth bleaching agents.
How long does it take for a teeth whitening kit to work?
Results vary by product concentration and individual tooth porosity. Most users see noticeable improvements within a few days to a week of consistent use. Optimal results typically take 2-4 weeks of daily application, following the manufacturer's instructions. Patience and consistency are key.
Will a teeth whitening kit work on veneers, crowns, or fillings?
No, teeth whitening kit products only work on natural tooth enamel. Existing dental restorations such as porcelain veneers teeth, dental crowns, or composite fillings will not change color. Whitening your natural teeth may result in a noticeable color mismatch, making your restorations appear darker than your newly whitened teeth. Consult your dentist if you have restorations.
Is teeth whitening painful?
Most people experience temporary tooth sensitivity and/or mild gum irritation during or after using a teeth whitening kit, but it's rarely described as "painful" in a severe sense. This sensitivity is usually manageable, subsides once treatment is stopped, and can be alleviated with desensitizing toothpastes or by taking breaks between applications. If you experience severe or prolonged pain, stop use and see your dentist.
How long do the results of at-home whitening last?
The results are not permanent and typically last anywhere from 3 to 12 months, depending on your diet, oral hygiene habits, and whether you smoke. Regular touch-up treatments, often every 3-6 months, and avoiding highly staining foods and beverages can help maintain your bright smile longer.
Are there any risks or side effects to using a teeth whitening kit?
Yes, the most common side effects are temporary tooth sensitivity and gum irritation. Other, rarer risks include uneven whitening, especially if the product isn't applied correctly, and potential for enamel erosion if products are used excessively or incorrectly. Always follow directions and consult your dentist if you have concerns or pre-existing conditions.
Can I whiten my teeth if I have sensitive teeth?
If you have pre-existing sensitive teeth, proceed with caution. Many teeth whitening kit brands offer formulas specifically designed for sensitive teeth, often with lower peroxide concentrations or added desensitizing agents. Using a desensitizing toothpaste for a few weeks before starting, and during the whitening process, can help. Your dentist can also provide professional advice and stronger desensitizing treatments.
How often should I use a teeth whitening kit?
You should always follow the specific instructions provided with your chosen teeth whitening kit. Generally, kits are designed for daily use for a specified period (e.g., 7-14 days). Overuse or using more frequently than recommended can increase the risk of sensitivity and gum irritation without providing significantly better or faster results.
What are alternatives to at-home teeth whitening kits?
Alternatives include professional in-office whitening by a dentist for faster and more dramatic results, dentist-prescribed take-home kits with custom-fitted trays for superior control, or cosmetic solutions like dental bonding or veneers teeth for severe intrinsic stains, chips, or alignment issues that teeth bleaching cannot address.
Should I consult a dentist before using a teeth whitening kit?
Yes, it is highly recommended to consult your dentist before starting any teeth whitening kit regimen. Your dentist can assess your oral health, identify the cause of your stains, check for cavities or gum disease (which must be treated first), and advise if whitening is appropriate and safe for your specific situation. They can also recommend products with the ADA Seal of Acceptance.
When to See a Dentist
While teeth whitening kits are popular and generally safe for at-home use, there are specific situations when it's crucial to consult a dental professional. Ignoring these signs could lead to exacerbated dental problems or unsatisfactory results.
Before Starting Any Whitening Treatment:
- You Have Existing Dental Work: If you have composite fillings, crowns, bridges, or especially veneers teeth on your front teeth, they will not whiten. Your dentist can advise you on the potential color mismatch and discuss options if you desire a uniform bright smile.
- You Have Untreated Dental Issues: Cavities, gum disease (gingivitis or periodontitis), exposed tooth roots, or cracked teeth should be treated before any whitening procedure. Whitening agents can penetrate these areas, causing severe pain, infection, or further damage.
- You Have Known Tooth Sensitivity: If your teeth are already sensitive to hot, cold, or sweets, a dentist can help identify the cause and recommend a desensitizing regimen or suggest a milder whitening approach.
- You Have Intrinsic Stains: If your teeth have deep gray or brown discoloration, or uneven white spots (e.g., from tetracycline antibiotics or fluorosis), an at-home teeth whitening kit may not be effective. Your dentist can diagnose the type of stain and recommend professional-grade options or alternatives like veneers teeth.
- You Are Pregnant or Breastfeeding: While no definitive studies confirm harm, most dentists and manufacturers advise against teeth bleaching during pregnancy or breastfeeding as a precautionary measure.
During or After Using a Teeth Whitening Kit:
- Severe or Persistent Sensitivity: If your tooth sensitivity becomes unbearable, lasts for more than a few days after stopping the product, or doesn't improve with desensitizing toothpaste, stop using the kit and see your dentist.
- Significant Gum Irritation or Chemical Burns: While mild irritation is common, persistent redness, swelling, bleeding gums, or visible white patches on your gums (chemical burns) require immediate dental attention.
- Uneven or Patchy Whitening: If your teeth are whitening unevenly, or you notice new white spots that appear starker after whitening, consult your dentist for advice on achieving a more uniform result.
- Allergic Reaction: Though rare, if you experience swelling of the lips, tongue, or throat, difficulty breathing, or a rash after using a teeth whitening kit, seek emergency medical care immediately.
- No Improvement After Recommended Use: If you've diligently followed the instructions for your teeth whitening kit and seen no noticeable improvement in tooth shade, your dentist can help determine why the treatment wasn't effective and suggest alternative solutions.
Red Flags vs. Routine Care Guidance:
- Routine Care: Mild, temporary sensitivity; slight gum tingling/irritation; gradual whitening over weeks. These are generally normal.
- Red Flags: Sharp, throbbing pain; severe, persistent sensitivity; bleeding gums; significant gum swelling or white lesions; sudden, extreme unevenness; lack of any whitening despite proper use. These warrant a dental visit.
When in doubt, a quick call to your dentist's office is always the safest course of action. They are your primary resource for ensuring your oral health and cosmetic dental endeavors are both safe and effective.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
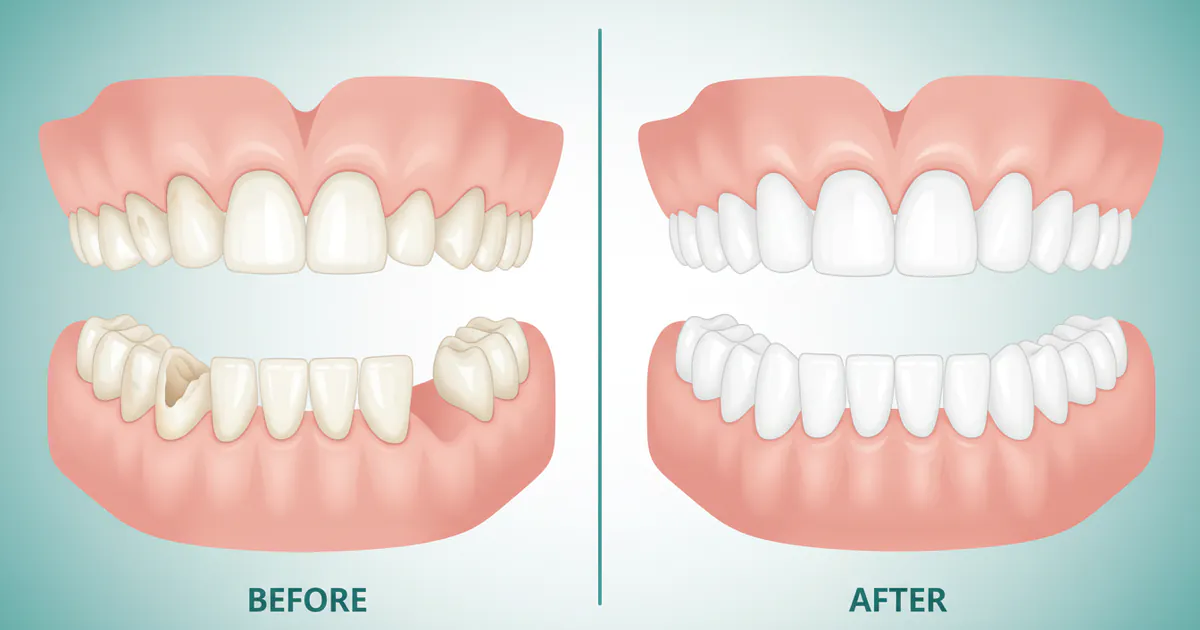
Before and After Dentures: Complete Guide
For many Americans, a vibrant smile isn't just about aesthetics; it's fundamental to speaking clearly, enjoying favorite foods, and maintaining self-confidence. Yet, over 36 million Americans are completely edentulous (have no natural teeth), and millions more suffer from significant tooth loss,
February 22, 2026

Teeth Whitening Cost: Complete Price Guide 2026
Brighter smiles are more than just a fleeting trend; they're a significant confidence booster and a common aesthetic goal for many Americans. In fact, a recent survey indicated that over 80% of adults aged 18-49 believe a beautiful smile is important for success, and teeth whitening remains one
February 22, 2026
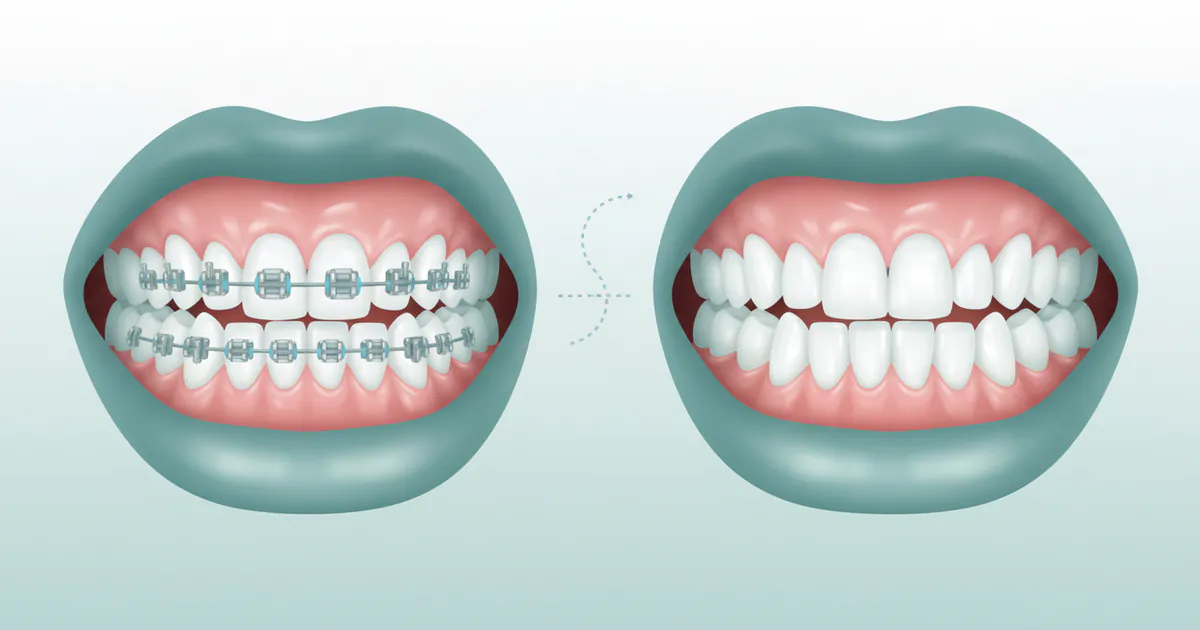
Braces Before and After: Complete Guide
For many, the journey to a confident, healthy smile begins with orthodontics. The transformation seen in braces before and after photos isn't just cosmetic; it represents improved oral health, function, and self-esteem. Crooked teeth, misaligned bites, and gaps can lead to a host of problems, fr
February 22, 2026

Natural Teeth Whitening: Complete Guide
A radiant smile is often considered a sign of health and confidence, which is why teeth whitening has become one of the most popular cosmetic dental procedures in the United States. In fact, surveys suggest that a significant majority of Americans, around 80%, desire whiter teeth, and the teeth
February 22, 2026