Types of Teeth Problems: Complete Guide
Key Takeaways
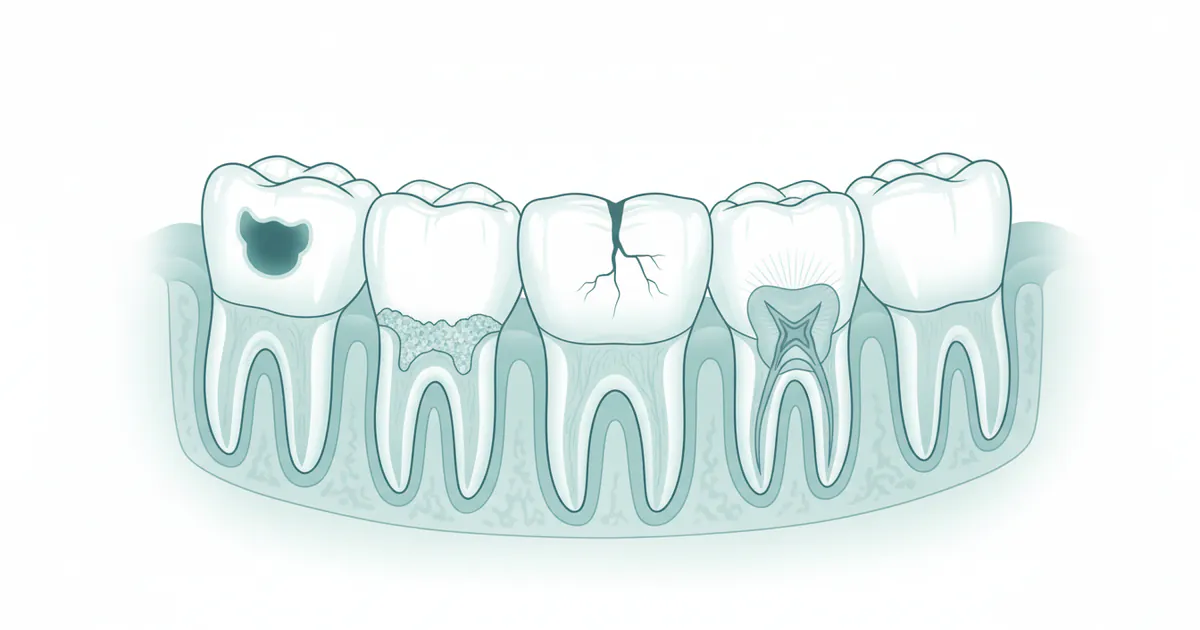
- Dental health is a cornerstone of overall well-being, yet an astonishing 30% of US adults experience daily pain in their mouth, teeth, or gums, according to the CDC. These discomforts are often tell-tale signs of underlying issues, making it crucial to understand the diverse **types of teeth pro
Dental health is a cornerstone of overall well-being, yet an astonishing 30% of US adults experience daily pain in their mouth, teeth, or gums, according to the CDC. These discomforts are often tell-tale signs of underlying issues, making it crucial to understand the diverse types of teeth problems that can affect our oral health. From the invisible battles against decay to the complex challenges of gum disease and bite irregularities, dental issues can range from minor annoyances to serious conditions impacting quality of life. This comprehensive guide will equip you with detailed knowledge about common dental ailments, their causes, symptoms, treatments, and most importantly, how to prevent them. We'll delve into the intricacies of human tooth anatomy, explore the critical process of permanent tooth eruption, and provide actionable insights to maintain a healthy, vibrant smile throughout your life.
Key Takeaways:
- Dental Caries (Cavities): Affecting nearly 90% of adults, cavities cost $90-$250 for fillings (amalgam) to $250-$4,500+ for crowns/root canals. Prevention includes regular brushing, flossing, and professional cleanings.
- Periodontal Disease (Gum Disease): Ranges from mild gingivitis to severe periodontitis, affecting nearly half of US adults over 30. Treatment can range from $200-$600 for deep cleanings (scaling & root planing) per quadrant to $500-$10,000+ for surgical interventions.
- Malocclusion (Bite Problems): Common in children and adults, often requiring orthodontic intervention. Braces can cost $3,000-$8,000, while clear aligners range from $3,500-$8,000. Treatment duration typically spans 18-36 months.
- Impacted Wisdom Teeth: A common issue during permanent tooth eruption, often requiring extraction. Costs vary from $75-$200 per tooth for simple extractions to $200-$600 per tooth for surgical removal of impacted teeth.
- Preventive Care is Key: Regular dental check-ups (every 6-12 months) and daily oral hygiene (brushing twice daily, flossing once daily) can prevent most major dental problems, saving significant time and money on future treatments.
- Dental Insurance: Can cover 50-80% of costs for basic restorative care (fillings, extractions) and 0-50% for major procedures (crowns, root canals, orthodontics), often with annual maximums of $1,000-$2,000.
- Children's Oral Health: Early dental visits (by age one) are crucial to monitor permanent tooth eruption, identify developmental issues, and prevent early childhood caries.
Understanding Human Tooth Anatomy and Development
Before diving into the various types of teeth problems, it's essential to understand the basic human tooth anatomy and how our teeth develop. This foundational knowledge helps contextualize why certain problems occur and how treatments work.

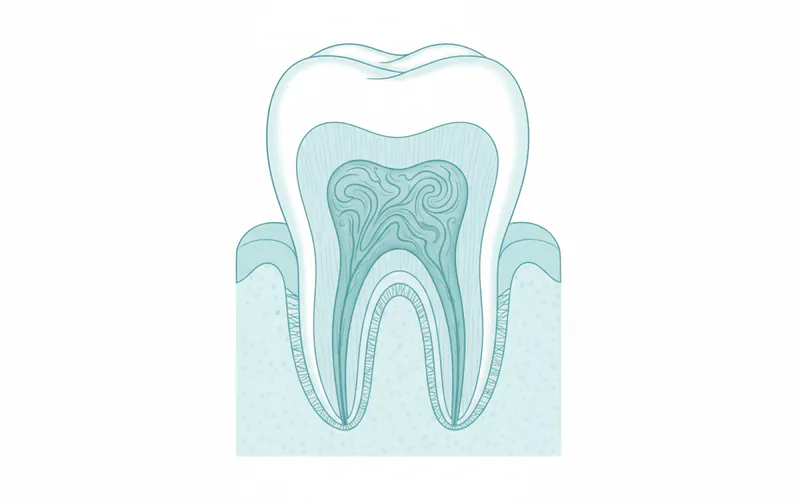
Structure of a Tooth
Each tooth is a complex organ designed for chewing, speaking, and maintaining facial structure. It consists of several distinct layers and supporting structures:
- Enamel: The outermost layer, incredibly hard and durable, protecting the inner tooth from decay and wear. It's the hardest substance in the human body.
- Dentin: Located beneath the enamel, dentin is a yellowish, porous layer that contains microscopic tubules connected to the pulp. It's softer than enamel and more susceptible to decay once exposed.
- Pulp: The innermost part of the tooth, containing nerves, blood vessels, and connective tissue. This vital tissue provides sensation and nourishment to the tooth.
- Cementum: A bone-like tissue covering the tooth root, helping to anchor it to the jawbone.
- Periodontal Ligament: A network of fibers connecting the cementum to the alveolar bone (jawbone), acting as a shock absorber and holding the tooth firmly in place.
- Gingiva (Gums): The soft tissue surrounding the teeth, protecting the roots and jawbone.
- Alveolar Bone: The part of the jawbone that holds the tooth roots.
Primary vs. Permanent Teeth Eruption Timeline
Our dental journey begins with primary (baby) teeth, which eventually make way for permanent tooth eruption. Understanding this timeline is crucial for parents and can shed light on certain dental issues.
- Primary Teeth: Typically, 20 primary teeth erupt between 6 months and 3 years of age. They serve as placeholders for permanent teeth and are vital for chewing and speech development.
- Permanent Teeth: The process of permanent tooth eruption usually begins around age 6 with the first molars and central incisors. By about age 12-14, most permanent teeth (28 total, excluding wisdom teeth) have erupted. The final set, the third molars (wisdom teeth), typically emerge between ages 17 and 25. Any deviation from this timeline or problems during eruption can lead to specific dental issues.
Common Types of Teeth Problems: A Deep Dive
Dental problems are diverse, ranging from infections to structural issues and cosmetic concerns. Here, we'll explore the most common types, providing an in-depth look at each.
Dental Caries (Cavities)
What It Is / Overview
Dental caries, commonly known as cavities or tooth decay, is the breakdown of tooth enamel due to acids produced by bacteria in the mouth. It's one of the most prevalent chronic diseases worldwide. If left untreated, a cavity can deepen, affecting the dentin and eventually the pulp, leading to pain, infection, and tooth loss.
Causes / Why It Happens
The primary cause of cavities is the interaction between bacteria, sugars, and acids in the mouth.
- Bacteria: Specific bacteria (e.g., Streptococcus mutans) naturally reside in the mouth and form plaque, a sticky film on teeth.
- Sugars/Carbohydrates: When you consume sugary foods or drinks, these bacteria feed on the sugars and produce acids.
- Acid Attack: These acids attack the tooth enamel, demineralizing it over time and creating tiny holes.
- Poor Oral Hygiene: Inadequate brushing and flossing allow plaque to accumulate, increasing acid exposure.
- Frequent Snacking: Constant exposure to sugars and acids doesn't give saliva enough time to neutralize acids and remineralize enamel.
- Dry Mouth (Xerostomia): Saliva plays a crucial role in neutralizing acids and washing away food particles. Reduced saliva flow can increase cavity risk.
Signs and Symptoms
In the early stages, cavities may be asymptomatic. As decay progresses, symptoms can include:
- Toothache, spontaneous pain, or pain without any apparent cause
- Sensitivity to hot, cold, or sweet foods and drinks
- Mild to sharp pain when biting down
- Visible pits or holes in the teeth
- Brown, black, or white staining on any surface of a tooth
Types of Cavities
Cavities can be categorized by their location:
- Smooth Surface Caries: Occur on the flat, exposed surfaces of teeth, often between teeth.
- Pit and Fissure Caries: Develop in the grooves and pits on the chewing surfaces of molars and premolars, where food and bacteria can easily get trapped.
- Root Caries: Occur on the surface of the tooth root, often when gums recede, exposing the softer cementum.
Treatment Options
Treatment depends on the severity of the cavity:
- Fluoride Treatments: For very early enamel demineralization, topical fluoride can help remineralize the enamel and reverse decay.
- Fillings: The most common treatment for established cavities. The decayed portion of the tooth is removed, and the hole is filled with a restorative material.
- Pros: Restores tooth function and aesthetics, prevents further decay.
- Cons: Requires removal of tooth structure, potential for sensitivity.
- Crowns: If a significant portion of the tooth structure is lost due to decay, a crown (a cap covering the entire tooth) may be necessary to restore strength and function.
- Pros: Highly durable, protects weakened tooth.
- Cons: More expensive, requires significant tooth reduction.
- Root Canal Therapy: If decay reaches the pulp, causing infection or inflammation, a root canal is performed to remove the infected pulp, clean and disinfect the canal, and seal it. A crown is usually placed afterward.
- Pros: Saves the natural tooth, relieves severe pain.
- Cons: Multi-appointment procedure, can be costly.
- Extraction: If a tooth is too severely damaged to be saved by a filling, crown, or root canal, extraction (removal) may be the only option.
- Pros: Eliminates infection and pain.
- Cons: Tooth loss, requires replacement (implant, bridge, denture).
Table 1: Comparing Common Filling Materials
| Filling Material | Appearance | Durability & Location | Cost (US) | Pros | Cons |
|---|---|---|---|---|---|
| Amalgam | Silver/Gray | Very Durable (Molars) | $90 - $250 | Strong, long-lasting, cost-effective | Not aesthetic, contains mercury, can expand/contract |
| Composite | Tooth-colored | Moderate (All Teeth) | $150 - $400 | Aesthetic, bonds to tooth, minimal tooth removal | Less durable than amalgam, can stain, more expensive |
| Glass Ionomer | Tooth-colored/Translucent | Weaker (Temporary, Kids) | $75 - $250 | Releases fluoride, good for root caries/temporary | Less durable, wears faster, not ideal for chewing surfaces |
| Gold | Gold | Very Durable (Molars) | $250 - $1,500+ | Highly durable, precise fit, well-tolerated | Very expensive, requires multiple visits, aesthetic |
| Porcelain | Tooth-colored | Very Durable (Inlays/Onlays/Crowns) | $600 - $1,500+ | Highly aesthetic, durable, stain-resistant | Expensive, brittle, requires lab fabrication |
Step-by-Step Process: A Standard Dental Filling
- Numbing: The dentist will numb the area around the affected tooth with a local anesthetic.
- Removal of Decay: A drill or laser is used to remove the decayed and weakened tooth structure.
- Preparation: The tooth is shaped to ensure the filling material adheres properly. For composite fillings, an etching gel and bonding agent are applied.
- Filling Placement: The chosen filling material is applied in layers (for composite) and hardened with a special light.
- Shaping and Polishing: The dentist shapes the filling to match the natural contours of your tooth and bite, then polishes it for a smooth finish.
Cost and Insurance
- Fillings:
- Amalgam: $90 - $250 per tooth
- Composite: $150 - $400 per tooth
- Crowns: $800 - $3,000+ per tooth (depending on material and complexity)
- Root Canal Therapy: $700 - $2,000+ per tooth (front vs. molars)
- Most dental insurance plans cover 50-80% of basic restorative procedures like fillings after deductibles. Major procedures like crowns and root canals typically have lower coverage (20-50%).
Recovery and Aftercare
After a filling, some sensitivity to hot, cold, or pressure is common for a few days. Avoid chewing hard or sticky foods on the filled tooth until the anesthetic wears off and any sensitivity subsides. For crowns and root canals, follow specific post-procedure instructions, which often include avoiding chewing on the treated tooth until the permanent restoration is placed.
Prevention
- Brush twice daily with fluoride toothpaste.
- Floss daily to remove plaque and food particles between teeth.
- Limit sugary and acidic foods/drinks.
- Visit your dentist for regular check-ups and cleanings (every 6-12 months).
- Consider dental sealants for chewing surfaces of molars, especially for children.
- Use fluoride mouthwash if recommended by your dentist.
Risks and Complications
- Sensitivity: Common after fillings, usually temporary.
- Allergic Reaction: Rare, but possible with certain filling materials.
- Fracture: A filling can crack, or the tooth itself can fracture around the filling.
- Secondary Decay: New decay can form around or under an existing filling.
- Pulpitis: Inflammation of the pulp, sometimes leading to the need for a root canal if the decay was deep.
Periodontal (Gum) Disease
What It Is / Overview
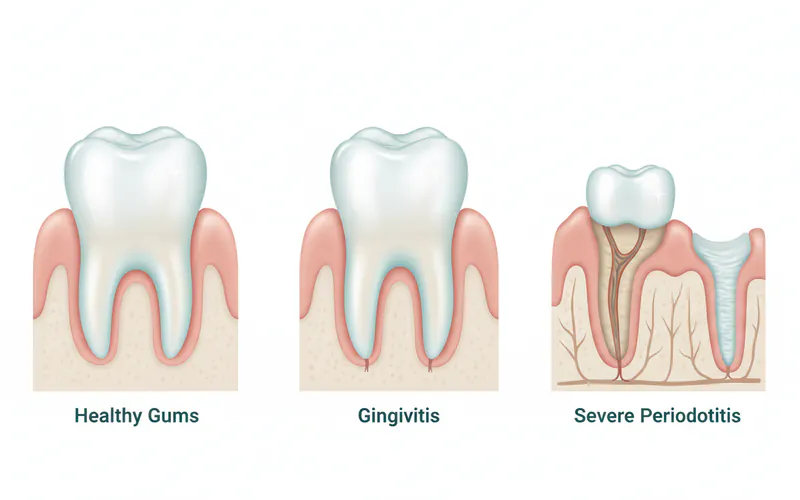
Periodontal disease, or gum disease, is an infection of the tissues that hold your teeth in place. It's primarily caused by poor oral hygiene, allowing plaque and tartar to build up on teeth. It ranges from mild inflammation (gingivitis) to severe infection (periodontitis) that can lead to tooth loss.
Causes / Why It Happens
- Plaque: A sticky film of bacteria that constantly forms on your teeth.
- Tartar (Calculus): If plaque isn't removed daily, it hardens into tartar, which can only be removed by professional cleaning.
- Bacterial Toxins: Bacteria in plaque and tartar produce toxins that irritate the gums, causing inflammation.
- Poor Oral Hygiene: Inadequate brushing and flossing are the leading causes.
- Smoking/Tobacco Use: Significantly increases the risk and severity of gum disease.
- Hormonal Changes: During pregnancy, puberty, menopause.
- Certain Medications: Some drugs can reduce saliva flow or cause gum overgrowth.
- Systemic Diseases: Diabetes, AIDS, and other conditions can weaken the immune system.
- Genetics: Some people are more genetically predisposed to gum disease.
Signs and Symptoms
- Gingivitis (Early Stage):
- Red, swollen, or tender gums
- Gums that bleed easily during brushing or flossing
- Bad breath (halitosis)
- Periodontitis (Advanced Stage):
- Receding gums (teeth appear longer)
- Formation of deep pockets between teeth and gums
- Pus between teeth and gums
- Loose or shifting teeth
- Changes in bite or fit of dentures
- Persistent bad breath or a bad taste in the mouth
Treatment Options
- Gingivitis:
- Professional Dental Cleaning: Removal of plaque and tartar by a dental hygienist.
- Improved Oral Hygiene: Consistent brushing and flossing.
- Periodontitis:
- Scaling and Root Planing (Deep Cleaning): Non-surgical procedure to remove plaque and tartar from above and below the gum line, and smooth root surfaces to prevent bacterial reattachment.
- Medications: Antibiotic gels, chips, or oral antibiotics to control bacterial infection.
- Surgical Treatments:
- Flap Surgery (Pocket Reduction Surgery): Gums are lifted back, and tartar is removed. Irregular bone surfaces may be smoothed.
- Soft Tissue Grafts: Tissue taken from the roof of the mouth or a donor source is used to cover exposed roots or enhance gum tissue.
- Bone Grafting: Used to restore bone destroyed by gum disease, using fragments of your own bone, synthetic bone, or donated bone.
- Guided Tissue Regeneration: A small piece of mesh-like fabric is inserted between the bone and gum tissue to prevent gum tissue from growing into the area where bone should be, allowing bone and connective tissue to regenerate.
- Tissue-Stimulating Proteins: Application of a gel to a diseased root to stimulate healthy bone and tissue growth.
Step-by-Step Process: Scaling and Root Planing
- Numbing: Local anesthetic is applied to numb the gums and tooth roots.
- Scaling: A specialized ultrasonic scaler and hand instruments are used to meticulously remove plaque and tartar from the tooth surfaces, both above and below the gum line.
- Root Planing: The root surfaces are then smoothed to remove bacterial toxins and rough spots, making it harder for plaque to reattach and easier for gums to heal.
- Irrigation (Optional): An antimicrobial rinse may be used to flush out bacteria.
- Follow-up: Multiple appointments may be needed, often divided into quadrants of the mouth. Regular maintenance cleanings (periodontal maintenance) are crucial afterward.
Cost and Insurance
- Professional Cleaning (Prophylaxis): $75 - $200 (often fully covered by insurance)
- Scaling and Root Planing (Deep Cleaning): $200 - $600 per quadrant (usually 4 quadrants in the mouth).
- Periodontal Surgery: $500 - $10,000+ depending on the type and extent of surgery.
- Dental insurance often covers a percentage (50-80%) of deep cleanings after deductibles. Surgical procedures typically have lower coverage (20-50%) or are subject to annual maximums.
Recovery and Aftercare
After deep cleaning, expect some tenderness, swelling, and sensitivity for a few days. Follow your dentist's instructions for pain management and oral hygiene. For surgical procedures, recovery can take longer, involving soft food diets, prescribed pain medication, and specific cleaning instructions. Lifelong rigorous oral hygiene and regular periodontal maintenance appointments (typically every 3-4 months) are crucial to prevent recurrence.
Prevention
- Brush teeth twice a day for two minutes with a soft-bristled brush.
- Floss daily.
- Use an antimicrobial mouthwash if recommended.
- Attend regular dental check-ups and professional cleanings.
- Avoid tobacco products.
- Manage underlying health conditions like diabetes.
Risks and Complications
- Recurrence: Gum disease can return if oral hygiene isn't maintained.
- Tooth Loss: Untreated periodontitis is a leading cause of tooth loss.
- Systemic Health Issues: Links between gum disease and heart disease, stroke, diabetes complications, and adverse pregnancy outcomes are well-documented.
- Increased Sensitivity: After deep cleaning or surgery.
- Gum Recession: Can expose more of the tooth root.
Malocclusion (Bite Problems)
What It Is / Overview
Malocclusion refers to any misalignment of teeth and jaws when the mouth is closed. While not directly a disease, it's a common dental problem that can lead to difficulties with chewing, speaking, and maintaining oral hygiene, as well as contributing to other issues like TMJ disorders and excessive tooth wear.
Causes / Why It Happens
Malocclusion is often hereditary, but can also be caused by environmental factors.
- Genetics: Jaw size, tooth size, and facial structure are often inherited.
- Early Loss of Primary Teeth: Can cause permanent teeth to erupt incorrectly.
- Habits: Thumb-sucking, pacifier use beyond age 2-4, tongue thrusting, and prolonged bottle feeding can alter jaw development.
- Trauma: Injuries to the jaw or teeth.
- Impacted or Missing Teeth: Can create spacing or crowding issues.
- Abnormal Jaw Growth: Due to certain medical conditions or tumors.
Signs and Symptoms
- Misaligned teeth (crooked, crowded, gapped)
- Abnormal bite (overbite, underbite, crossbite, open bite)
- Difficulty or discomfort when chewing or biting
- Speech problems (lisp)
- Breathing through the mouth
- Jaw pain or temporomandibular joint (TMJ) disorders
- Uneven wear on tooth surfaces
Types / Variations
- Class 1 Malocclusion: The most common type, where the bite is generally normal, but there are minor crowding or spacing issues.
- Class 2 Malocclusion (Overbite/Retrognathism): The upper front teeth significantly overlap the lower front teeth.
- Class 3 Malocclusion (Underbite/Prognathism): The lower jaw protrudes, causing the lower front teeth to overlap the upper front teeth.
- Crossbite: Upper teeth bite inside the lower teeth. Can affect front or back teeth.
- Open Bite: A space remains between the upper and lower teeth when the jaw is closed.
- Crowding: Not enough space for teeth, causing them to overlap or rotate.
- Spacing: Gaps between teeth due to missing teeth or an oversized jaw.
Treatment Options
Treatment typically involves orthodontics, and sometimes surgery.
- Orthodontic Appliances:
- Braces: Traditional metal, ceramic, or lingual braces use brackets and wires to gradually shift teeth into proper alignment.
- Clear Aligners (e.g., Invisalign): A series of custom-made, clear plastic trays that progressively move teeth.
- Removable Appliances: Retainers, palatal expanders, headgear – used to correct specific issues, often in conjunction with fixed braces.
- Pros: Corrects bite, improves aesthetics, facilitates oral hygiene, reduces wear and tear.
- Cons: Can be lengthy, costly, requires commitment to wear appliances.
- Tooth Extraction: Sometimes necessary to create space for crowded teeth.
- Orthognathic Surgery (Jaw Surgery): For severe skeletal discrepancies where orthodontics alone aren't sufficient, surgery realigns the jaws.
- Pros: Corrects severe bite issues, improves facial symmetry.
- Cons: Major surgery, longer recovery, higher cost.
Table 2: Comparing Common Orthodontic Treatments
| Treatment Type | Description | Cost (US) | Treatment Time | Visibility | Comfort & Maintenance |
|---|---|---|---|---|---|
| Traditional Metal Braces | Metal brackets and wires, adjusted periodically | $3,000 - $7,000 | 18-36 months | Highly Visible | Initial discomfort, diet restrictions, thorough cleaning required |
| Ceramic Braces | Tooth-colored or clear brackets, less noticeable | $3,500 - $8,000 | 18-36 months | Less Visible | Similar to metal, but brackets can stain and are more brittle |
| Clear Aligners (e.g., Invisalign) | Series of custom-made clear plastic trays | $3,500 - $8,000 | 12-24 months | Nearly Invisible | Removable for eating/cleaning, less discomfort, easy maintenance |
| Lingual Braces | Brackets placed on the inside of teeth, completely hidden | $8,000 - $12,000+ | 18-36 months | Invisible | More discomfort initially, speech can be affected, harder to clean |
Cost and Insurance
- Braces (Metal/Ceramic): $3,000 - $8,000
- Clear Aligners: $3,500 - $8,000
- Orthognathic Surgery: $20,000 - $40,000+ (often covered partially by medical insurance if medically necessary).
- Many dental insurance plans offer some orthodontic coverage, particularly for children, often covering 25-50% of the cost up to a lifetime maximum. Adult orthodontics may have less coverage.
Recovery and Aftercare
After braces or aligners, a retainer is crucial to maintain the new tooth position indefinitely. For jaw surgery, recovery involves a liquid or soft diet for several weeks, pain management, and physical therapy.
Prevention
- Early Orthodontic Evaluation: The ADA recommends an orthodontic check-up by age 7 to identify and address potential issues early.
- Limit Harmful Habits: Discourage prolonged thumb-sucking, pacifier use, or tongue thrusting.
- Maintain Primary Teeth: Prevent early loss of baby teeth through good oral hygiene.
Risks and Complications
- Root Resorption: Shortening of tooth roots during orthodontic treatment.
- Relapse: Teeth can shift back to their original position if retainers aren't worn.
- Decalcification/Cavities: Increased risk of enamel demineralization or cavities around brackets if oral hygiene is poor.
- Gum Inflammation: Gums can become inflamed around braces.
- TMJ Issues: While often improved, some individuals may develop or exacerbate TMJ symptoms.
- Surgical Risks: For orthognathic surgery, risks include nerve damage, infection, and complications from anesthesia.
Tooth Sensitivity
What It Is / Overview
Tooth sensitivity is a sharp, temporary pain in the teeth that occurs when the dentin, the softer layer beneath the enamel, becomes exposed. This exposure allows external stimuli (like hot, cold, sweet, or acidic foods) to reach the nerves in the tooth's pulp.
Causes / Why It Happens
- Receding Gums: Gums pull away from the teeth, exposing the roots which lack enamel protection.
- Enamel Erosion: Loss of enamel due to acidic foods/drinks, aggressive brushing, or bruxism.
- Cavities: Decay creates a hole, exposing the dentin.
- Cracked or Chipped Teeth: Exposes dentin or pulp.
- Worn Fillings: Old, leaky fillings can allow stimuli to reach dentin.
- Post-Treatment Sensitivity: Common after dental procedures like fillings, crowns, or professional cleanings, usually temporary.
- Aggressive Brushing: Brushing too hard can wear down enamel and expose dentin.
Signs and Symptoms
- Sharp, sudden pain when consuming hot, cold, sweet, or acidic foods/drinks.
- Pain when breathing in cold air.
- Discomfort during brushing or flossing.
Treatment Options
- Desensitizing Toothpaste: Contains compounds (e.g., potassium nitrate, strontium chloride) that block the microscopic tubules in the dentin, preventing stimuli from reaching the nerve.
- Fluoride Treatments: Applied by a dentist, can strengthen enamel and reduce sensitivity.
- Bonding/Varnishes: A tooth-colored resin material can be applied to cover exposed root surfaces.
- Gum Grafts: For significant gum recession, gum tissue can be surgically grafted to cover exposed roots.
- Root Canal: For severe, persistent sensitivity that doesn't respond to other treatments, indicating potential pulp damage.
- Treating Underlying Issues: Addressing cavities, cracks, or bruxism.
Prevention
- Use a soft-bristled toothbrush and gentle brushing technique.
- Use fluoride toothpaste daily.
- Limit acidic foods and drinks, or rinse your mouth with water afterward.
- Avoid aggressive tooth whitening products if you have sensitivity.
- Wear a nightguard if you grind your teeth.
- Regular dental check-ups to identify and treat causes early.
Bruxism (Teeth Grinding/Clenching)
What It Is / Overview
Bruxism is a condition in which you habitually grind, gnash, or clench your teeth. It can occur during the day (awake bruxism) or, more commonly, during sleep (sleep bruxism). It can lead to tooth damage, jaw pain, and headaches.
Causes / Why It Happens
- Stress and Anxiety: A common trigger for both awake and sleep bruxism.
- Personality Type: Aggressive, competitive, or hyperactive personalities may be more prone.
- Sleep Disorders: Sleep apnea and other sleep-related issues.
- Malocclusion: Misaligned bite can sometimes contribute.
- Medications: Certain antidepressants (e.g., SSRIs) can cause bruxism as a side effect.
- Substance Use: Caffeine, alcohol, and tobacco.
- Neurological Conditions: Parkinson's disease, Huntington's disease.
Signs and Symptoms
- Flattened, fractured, chipped, or loose teeth
- Worn tooth enamel, exposing deeper layers of the tooth
- Increased tooth sensitivity
- Jaw pain, tightness in the jaw muscles, or a locked jaw
- Headaches (especially temple headaches)
- Earaches (due to muscle strain)
- Facial pain
- Scalloping on the sides of the tongue
- Indentations on the inside of the cheeks
- Disrupted sleep for you or your partner (due to grinding sounds)
Treatment Options
- Nightguards/Splints: Custom-fitted acrylic appliances worn at night to create a barrier between upper and lower teeth, protecting them from grinding and clenching forces.
- Pros: Protects teeth, reduces jaw pain, non-invasive.
- Cons: Requires consistent wear, can be costly.
- Stress Management: Techniques like meditation, yoga, exercise, and therapy can help reduce stress-related bruxism.
- Biofeedback: Using electronic monitoring to teach you to control muscle activity in your jaw.
- Medications: Muscle relaxants (short-term), Botox injections into jaw muscles (for severe cases to reduce muscle activity).
- Corrective Dentistry: If bruxism has caused significant tooth wear or malocclusion, fillings, crowns, or orthodontics may be needed to reshape the biting surfaces and correct the bite.
Prevention
- Identify and manage stress.
- Avoid caffeine and alcohol, especially before bed.
- Be mindful of clenching during the day (e.g., when concentrating).
- Ensure regular sleep hygiene.
- Regular dental check-ups for early detection of wear.
Dental Abscesses and Infections
What It Is / Overview
A dental abscess is a localized collection of pus caused by a bacterial infection. It can form at the tip of the tooth root (periapical abscess) or in the gums next to a tooth (periodontal abscess). These infections are serious and can spread if not treated.
Causes / Why It Happens
- Untreated Tooth Decay: When a cavity progresses deep into the pulp, bacteria can infect the nerves and blood vessels, leading to an abscess at the root tip.
- Gum Disease: Advanced periodontal disease can cause bacteria to accumulate in gum pockets, leading to a periodontal abscess.
- Trauma: A chip or crack in the tooth can create an opening for bacteria to enter the pulp.
- Impacted Teeth: Partially erupted wisdom teeth are particularly susceptible to infection and abscess formation.
Signs and Symptoms
- Severe, persistent, throbbing toothache that can radiate to the jawbone, neck, or ear.
- Sensitivity to hot and cold temperatures.
- Sensitivity to pressure of chewing or biting.
- Fever.
- Swelling in your face or cheek.
- Tender, swollen lymph nodes under your jaw or in your neck.
- A sudden rush of foul-smelling and foul-tasting fluid in your mouth if the abscess ruptures.
- Difficulty opening your mouth or swallowing.
Treatment Options
- Drainage: The dentist may make a small incision to drain the pus, relieving pressure and pain.
- Root Canal Therapy: For periapical abscesses, this procedure removes the infected pulp, cleans the root canals, and seals the tooth to prevent re-infection.
- Extraction: If the tooth cannot be saved, it will be extracted to remove the source of infection.
- Antibiotics: Prescribed to kill the bacteria causing the infection, especially if the infection has spread or the patient has a weakened immune system.
- Saltwater Rinses: Can help soothe the area and promote drainage.
Risks and Complications
- Spread of Infection: Untreated dental abscesses can spread to the jawbone, neck, brain, or other parts of the body, potentially leading to life-threatening conditions like sepsis or cellulitis.
- Tooth Loss: If the infection is too severe.
- Osteomyelitis: Infection of the bone.
Tooth Trauma and Fractures
What It Is / Overview
Tooth trauma refers to any injury to the teeth, gums, and supporting structures. Fractures range from small chips in the enamel to severe cracks extending into the root.
Causes / Why It Happens
- Accidents: Falls, sports injuries, car accidents.
- Biting on Hard Objects: Chewing ice, popcorn kernels, hard candies.
- Bruxism: Chronic grinding/clenching can stress teeth, leading to cracks.
- Large Fillings: Teeth with extensive fillings can become weakened and more prone to fracture.
Signs and Symptoms
- Pain when chewing or biting, especially when releasing the bite.
- Sensitivity to hot, cold, or sweet foods.
- Visible crack or chip.
- Swelling of the gum around the affected tooth.
- If the pulp is affected, symptoms similar to an abscess (throbbing pain, swelling).
- Pro Tip: Cracks can be very difficult to detect visually. Dentists often use special dyes or transillumination to find them.
Treatment Options
Treatment depends on the severity and location of the fracture:
- Bonding: For small chips or cracks, a tooth-colored resin is applied and bonded to the tooth.
- Veneers: For more significant chips or cosmetic improvement, a thin shell of porcelain or composite can be bonded to the front surface of the tooth.
- Crowns: For larger cracks or fractures that have compromised the structural integrity of the tooth, a crown protects the tooth from further damage.
- Root Canal Therapy: If the fracture extends into the pulp, a root canal may be necessary to save the tooth, followed by a crown.
- Extraction: If the fracture extends deep below the gum line or is vertical, making the tooth unsalvageable, extraction is often the only option.
- Dental Implants, Bridges, or Dentures: To replace extracted teeth.
Impacted Teeth
What It Is / Overview
An impacted tooth is one that fails to fully erupt through the gum line into its proper position. This typically occurs because there isn't enough space in the jaw. While any tooth can become impacted, wisdom teeth (third molars) are the most common. This is a frequent complication during the permanent tooth eruption phase in late adolescence or early adulthood.
Causes / Why It Happens
- Lack of Space: The primary reason, especially for wisdom teeth, is that the jawbone is too small to accommodate their eruption.
- Abnormal Eruption Angle: The tooth may be growing at an angle, pushing against adjacent teeth or bone.
- Obstruction: Another tooth, dense bone, or abnormal tissue can block the eruption path.
Signs and Symptoms
- Pain or tenderness in the jaw or gums (especially in the back of the mouth).
- Red, swollen, or bleeding gums around the impacted area.
- Bad breath.
- Difficulty opening the mouth or chewing.
- Headaches or jaw stiffness.
- Infection (pericoronitis) around a partially erupted tooth.
- Cyst or tumor formation (rare but serious complication).
Treatment Options
- Monitoring: If an impacted tooth is asymptomatic and not causing problems, it may be monitored with regular X-rays.
- Extraction: The most common treatment for problematic impacted teeth, especially wisdom teeth. Surgical removal is often required, involving removal of gum tissue and sometimes bone.
- Pros: Prevents pain, infection, damage to adjacent teeth, cyst formation.
- Cons: Surgical risks (swelling, pain, dry socket, nerve damage), recovery period.
Cost and Insurance
- Simple Extraction: $75 - $200 per tooth (for non-impacted teeth)
- Surgical Extraction (Impacted): $200 - $600 per tooth (can be higher for complex cases, especially general anesthesia is used, reaching $800-$1,000+ per tooth).
- Most dental insurance plans cover a significant portion (50-80%) of extractions.
Recovery and Aftercare
After wisdom tooth extraction, expect swelling, pain, and limited jaw opening. Follow post-operative instructions carefully, which typically include:
- Biting on gauze to control bleeding.
- Using ice packs for swelling.
- Eating soft foods.
- Avoiding straws (to prevent dry socket).
- Taking prescribed pain medication and antibiotics.
- Gentle saltwater rinses after 24 hours.
Risks and Complications
- Dry Socket (Alveolar Osteitis): The blood clot dislodges from the extraction site, exposing bone, causing intense pain. Occurs in 5-10% of cases.
- Infection: Despite antibiotics, infection can occur.
- Nerve Damage: Though rare, temporary or permanent numbness (paresthesia) of the lip, tongue, or chin can occur.
- Damage to Adjacent Teeth: During extraction.
- Cyst/Tumor: Unremoved impacted teeth, especially wisdom teeth, can sometimes develop cysts or tumors.
Missing Teeth (Edentulism)
What It Is / Overview
Edentulism refers to the condition of having one or more missing teeth. This can range from a single missing tooth to complete edentulism (loss of all teeth). Missing teeth can affect chewing ability, speech, facial aesthetics, and lead to bone loss in the jaw.
Causes / Why It Happens
- Severe Decay: Untreated cavities can lead to irreparable tooth damage requiring extraction.
- Advanced Gum Disease: Periodontitis can destroy the bone and ligaments supporting teeth, causing them to loosen and fall out or require extraction.
- Trauma/Injury: Accidents can knock out teeth.
- Congenital Conditions: Some people are born with congenitally missing teeth.
- Failed Root Canals/Crowns: Sometimes a tooth cannot be saved despite previous treatments.
Signs and Symptoms
- Gaps in the smile.
- Difficulty chewing and eating certain foods.
- Speech impediments.
- Shifting or drifting of adjacent teeth into the empty space.
- Over-eruption (super-eruption) of the opposing tooth.
- Bone loss in the jaw where the tooth is missing, leading to facial changes.
Treatment Options
- Dental Implants: A titanium screw is surgically placed into the jawbone, acting as an artificial tooth root. A crown, bridge, or denture is then attached to the implant.
- Pros: Highly durable, preserves bone, feels like a natural tooth, doesn't rely on adjacent teeth.
- Cons: Invasive surgery, expensive, lengthy treatment time.
- Dental Bridges: A prosthetic tooth (pontic) is held in place by crowns cemented onto the natural teeth adjacent to the gap.
- Pros: Fixed solution, less invasive than implants, relatively quicker.
- Cons: Requires modifying healthy adjacent teeth, doesn't prevent bone loss, typically lasts 5-15 years.
- Removable Partial or Full Dentures: Artificial teeth set in an acrylic base that rests on the gums. Partial dentures attach to remaining teeth, while full dentures replace all teeth in an arch.
- Pros: Cost-effective, non-invasive, can replace multiple teeth.
- Cons: Can be less stable, requires removal for cleaning, may affect speech/eating, doesn't prevent bone loss.
Discolored and Stained Teeth
What It Is / Overview
Tooth discoloration refers to teeth that have lost their natural white or light-yellow hue, appearing darker, yellower, or stained.

Causes / Why It Happens
- Extrinsic Stains: Occur on the surface of the enamel from external factors.
- Food and Drink: Coffee, tea, red wine, dark sodas, berries, spices.
- Tobacco: Smoking or chewing tobacco.
- Poor Oral Hygiene: Plaque accumulation.
- Intrinsic Stains: Occur within the tooth structure, often due to internal factors.
- Aging: Enamel thins over time, revealing yellower dentin.
- Trauma: Can cause internal bleeding, leading to discoloration.
- Medications: Tetracycline antibiotics during tooth development can cause permanent gray-blue stains.
- Excessive Fluoride: Fluorosis can cause white or brown spots.
- Root Canal Treatment: A non-vital tooth can darken over time.
Treatment Options
- Professional Teeth Whitening (Bleaching): Using peroxide-based gels, activated by light or chemical reaction, to lighten extrinsic and some intrinsic stains.
- Pros: Effective, relatively quick, non-invasive.
- Cons: Temporary sensitivity, temporary, not effective on all stain types.
- Dental Veneers: Thin, custom-made shells of porcelain or composite material bonded to the front surface of teeth to mask severe discoloration.
- Pros: Highly aesthetic, durable, covers intrinsic stains.
- Cons: Irreversible (requires tooth reduction), expensive.
- Dental Bonding: Tooth-colored resin is applied and shaped to cover stains.
- Crowns: For severely discolored or damaged teeth.
- Internal Bleaching: For a single tooth discolored after a root canal, bleaching agents can be placed inside the tooth.
Prevention
- Good oral hygiene (brushing, flossing).
- Limit consumption of stain-causing foods and drinks, or rinse with water afterward.
- Avoid tobacco products.
- Regular professional cleanings to remove extrinsic stains.
Children and Pediatric Dental Considerations
Children's teeth, both primary and developing permanent tooth eruption, have unique vulnerabilities and requirements. Early intervention and preventive care are paramount.
Early Childhood Caries (Baby Bottle Tooth Decay)
This aggressive form of decay affects infants and toddlers, often due to prolonged exposure to sugary liquids (milk, formula, juice) in bottles or sippy cups, especially at bedtime. It can lead to severe decay in multiple primary teeth.
- Prevention: Avoid putting children to bed with bottles containing anything but water. Wipe gums and emerging teeth after feedings.
Thumb Sucking and Pacifier Use
While normal for infants, prolonged thumb-sucking or pacifier use beyond age 2-4 can affect jaw development and cause malocclusion (e.g., open bite, crossbite, protruded front teeth).
- Guidance: Most children stop on their own. If habits persist, discuss strategies with your dentist.
Teething and Eruption Issues
The process of permanent tooth eruption can sometimes be complicated:
- Impaction: As discussed earlier, especially wisdom teeth.
- Ectopic Eruption: A tooth erupts in an abnormal position.
- Supernumerary Teeth: Extra teeth that can block normal eruption.
- Ankylosis: A tooth fuses to the bone and fails to erupt or move.
- Symptoms: Discomfort, redness, mild swelling are normal during teething. Severe pain or swelling warrants a dental visit.
Dental Sealants and Fluoride
These are crucial preventive measures for children:
- Dental Sealants: Thin, protective coatings applied to the chewing surfaces of molars and premolars to prevent pit and fissure cavities, especially important as permanent molars erupt. Costs typically $30-$60 per tooth.
- Fluoride Varnish/Gel: Professional fluoride applications strengthen enamel and make teeth more resistant to decay. Often part of routine check-ups.
Dental Injuries in Children
Falls and sports injuries are common causes of chipped, fractured, or knocked-out primary or permanent teeth.
- Action: For a knocked-out permanent tooth, keep it moist (milk or saline) and seek immediate dental care within 30-60 minutes for a chance of reimplantation.
Pro Tip: The American Dental Association (ADA) recommends a child's first dental visit by their first birthday, or within six months of the first tooth erupting. This allows the dentist to monitor permanent tooth eruption, assess risk for decay, and educate parents on proper oral hygiene.
Cost Breakdown: Understanding Dental Expenses
Understanding the financial aspect of dental care in the US is crucial. Costs can vary significantly based on the procedure, location, dentist's fees, and whether you have insurance.
Average US Costs (General Estimates)
- Preventive Care (Cleanings, Exams, X-rays): $150 - $400 per visit (often fully or largely covered by insurance).
- Fillings: $90 - $400 (depending on material and size).
- Extractions: $75 - $600 (simple vs. surgical/impacted).
- Root Canals: $700 - $2,000+.
- Crowns: $800 - $3,000+.
- Dental Implants: $3,000 - $6,000+ per tooth (implant, abutment, crown).
- Orthodontics (Braces/Aligners): $3,000 - $8,000+.
- Deep Cleaning (Scaling & Root Planing): $200 - $600 per quadrant.
With vs. Without Insurance
- With Insurance: Most dental insurance plans operate on a "100-80-50" model:
- 100% Coverage: For preventive care (exams, cleanings, X-rays).
- 80% Coverage: For basic restorative care (fillings, simple extractions, sometimes root canals).
- 50% Coverage: For major restorative care (crowns, bridges, dentures) and sometimes orthodontics.
- Plans usually have a deductible (e.g., $50-$100 annually) and an annual maximum (e.g., $1,000 - $2,000).
- Without Insurance: You pay the full negotiated fee directly to the dentist. Many dentists offer a discount for cash payments.
Payment Plans and Financing Options
- In-Office Payment Plans: Many dental offices offer flexible payment schedules directly to patients.
- Third-Party Financing (e.g., CareCredit): Medical credit cards that offer interest-free periods for larger expenses if paid within a set timeframe.
- Dental Schools: Often provide discounted care by supervised students.
- Community Dental Clinics: Offer reduced-cost services for low-income individuals.
Cost-Saving Tips
- Prioritize Prevention: Regular check-ups and good home care are the best ways to avoid expensive treatments.
- Utilize Your Insurance: Understand your benefits, deductibles, and annual maximums.
- Consider a Dental Savings Plan: Not insurance, but a membership program where you pay an annual fee and get discounts on services.
- Shop Around: Get multiple quotes for expensive procedures.
- Act Early: Address dental problems when they are small and less expensive to treat.
Frequently Asked Questions
What are the most common types of teeth problems?
The most common types of teeth problems include dental caries (cavities), periodontal (gum) disease, malocclusion (bite problems), tooth sensitivity, and bruxism (teeth grinding). These issues affect a vast majority of the population at some point in their lives, often stemming from poor oral hygiene, genetic predispositions, or lifestyle factors.

How painful are dental treatments, and is anesthesia always used?
The level of pain during dental treatments varies significantly depending on the procedure and individual pain tolerance. For most restorative procedures like fillings or root canals, local anesthesia is routinely used to numb the area, making the process largely pain-free. For more invasive procedures like surgical extractions or extensive gum surgery, various sedation options, from nitrous oxide to IV sedation or general anesthesia, may be offered to ensure comfort. Post-procedure discomfort is managed with over-the-counter or prescription pain relievers.
How long do dental treatments typically last?
The duration of dental treatments can range from a single short visit for a routine cleaning or a simple filling to multiple appointments spanning several months or even years for complex cases. For example, a single dental filling might take 30-60 minutes, while orthodontics can last 18-36 months. Dental implant placement can take 3-6 months for healing before the crown is placed, and gum disease treatment often involves several deep cleaning sessions followed by ongoing maintenance.
Can diet affect my teeth problems?
Absolutely. Diet plays a critical role in dental health. Frequent consumption of sugary and acidic foods and drinks significantly increases the risk of dental caries and enamel erosion. These items provide fuel for oral bacteria to produce acids that attack tooth enamel. Conversely, a diet rich in fruits, vegetables, lean proteins, and dairy can strengthen teeth, stimulate saliva production, and provide essential nutrients for oral tissues.
What are some alternatives to traditional braces for correcting bite problems?
Beyond traditional metal braces, several effective alternatives exist for correcting malocclusion. Ceramic braces offer a less visible option, using clear or tooth-colored brackets. Lingual braces are placed on the inside surfaces of the teeth, making them completely hidden. Clear aligners, such as Invisalign, are a popular choice for their near invisibility and removability, though they require strong patient compliance. For minor issues, removable retainers or limited orthodontics might be sufficient.
How often should I see a dentist to prevent teeth problems?
The American Dental Association (ADA) recommends visiting your dentist for a routine check-up and professional cleaning at least once every six months. For individuals with a higher risk of cavities, gum disease, or other ongoing oral health issues, more frequent visits (e.g., every three or four months) may be recommended to proactively manage and prevent the progression of dental problems.
Is permanent tooth eruption always smooth, or are there common issues?
Permanent tooth eruption is not always smooth. While many permanent teeth emerge without issues, common problems include impaction (especially wisdom teeth), where a tooth gets stuck and cannot fully erupt. Other issues can include ectopic eruption (erupting in the wrong place), supernumerary teeth (extra teeth blocking eruption), or agenesis (congenitally missing teeth). Early orthodontic evaluation can help identify and address these problems.
What is the average lifespan of dental restorations like fillings or crowns?
The lifespan of dental restorations varies based on the material, the patient's oral hygiene, and chewing habits. Amalgam fillings can last 10-15 years or more, while composite fillings typically last 5-10 years. Crowns generally have a lifespan of 5-15 years, with some lasting longer with excellent care. Dental implants are designed for longevity and can last a lifetime with proper maintenance, though the crown on top may need replacement every 10-15 years.
Can bad breath be a sign of a serious teeth problem?
Yes, persistent bad breath (halitosis) can be a significant indicator of an underlying dental problem. While temporary bad breath can result from certain foods, chronic halitosis often points to issues like gum disease (gingivitis or periodontitis), which harbors odor-causing bacteria, extensive tooth decay, dental abscesses, or even dry mouth. Addressing the root cause through professional dental care and improved oral hygiene is crucial.
What should I do if my tooth is knocked out?
If a permanent tooth is knocked out (avulsed), act quickly. Gently pick up the tooth by the crown (not the root). If dirty, briefly rinse it with water (do not scrub). Try to reinsert it into its socket. If that's not possible, place it in a cup of milk, saline solution, or a tooth preservation kit. Seek immediate dental attention within 30-60 minutes for the best chance of successful reimplantation.
When to See a Dentist
Knowing when to seek professional dental care is critical for maintaining oral health and preventing minor issues from escalating into major problems.
Red Flags: Seek Immediate Attention
Certain signs and symptoms warrant immediate dental attention to prevent severe complications, infection spread, or save a tooth:
- Severe, persistent toothache: Especially if accompanied by throbbing, swelling, fever, or difficulty swallowing. This could indicate an abscess or severe infection.
- Swelling in your face, jaw, or neck: A rapidly progressing swelling can indicate a serious infection that may spread quickly.
- Knocked-out tooth: As discussed above, time is critical for successful reimplantation.
- Significant tooth fracture or trauma: Especially if accompanied by pain, visible pulp exposure, or bleeding.
- Uncontrolled bleeding from the mouth: After an injury or extraction, if bleeding doesn't stop with pressure.
- Sudden onset of extreme sensitivity: Especially if it's new and doesn't subside.
Routine Care vs. Emergency Guidance
- Routine Care: For general check-ups, professional cleanings, routine fillings, and non-urgent concerns like mild sensitivity or minor discoloration, schedule a regular appointment. This proactive approach helps prevent many dental emergencies.
- Scheduled Appointment: For issues like a chipped tooth without pain, a lost filling (without pain or sharp edges), or persistent bad breath, it's advisable to call your dentist for the earliest available appointment rather than waiting for your next routine visit.
- Emergency Care: For any of the "red flag" symptoms listed above, contact your dentist immediately. Many dental offices have an emergency line or provide guidance on what to do outside of regular hours. If your dentist is unavailable, consider visiting an urgent care center or hospital emergency room, especially if you have swelling that impedes breathing or swallowing.
Prioritizing your oral health by understanding the types of teeth problems and acting promptly when issues arise is the most effective way to ensure a lifetime of healthy smiles.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Tooth Eruption Order: Complete Guide
The journey of human teeth, from their initial emergence in infancy to the arrival of wisdom teeth in young adulthood, is a fascinating and crucial aspect of our overall health. Understanding the tooth eruption order is not just a matter of curiosity; it's a vital piece of knowledge that empower
February 23, 2026
Primary Tooth Eruption Sequence: Complete Guide
Did you know that by their third birthday, most children will have a full set of 20 primary teeth? The journey of these first teeth, from their initial appearance to their eventual replacement by permanent teeth, is a remarkable and often challenging milestone for both infants and parents. Understan
February 23, 2026
Canine Tooth Eruption: Complete Guide
Have you ever wondered about the complex process that brings your teeth into alignment, especially the prominent, pointed teeth known as canines? While often overshadowed by discussions of wisdom teeth or incisors, the canine tooth eruption process is a critical stage in your oral development, d
February 23, 2026
Permanent Tooth Eruption Sequence: Complete Guide
Welcome to SmilePedia.net, your trusted resource for comprehensive dental health information. The journey of your permanent teeth emerging into your mouth, known as the permanent tooth eruption sequence, is a fundamental aspect of oral development. Did you know that while primary (baby) teeth ty
February 23, 2026