Complete Guide to Dental Emergencies: Everything You Need to Know
Key Takeaways
- Imagine a sudden, searing pain in your jaw, the startling sight of a knocked-out tooth, or inexplicable gum swelling that makes eating unbearable. Dental emergencies are not just inconvenient; they can be profoundly painful, impact your overall health, and, if left untreated, lead to severe comp
Complete Guide to Dental Emergencies: Everything You Need to Know
Imagine a sudden, searing pain in your jaw, the startling sight of a knocked-out tooth, or inexplicable gum swelling that makes eating unbearable. Dental emergencies are not just inconvenient; they can be profoundly painful, impact your overall health, and, if left untreated, lead to severe complications. In fact, millions of Americans experience a dental emergency each year, often leading to frantic searches for immediate care. This comprehensive guide will equip you with crucial knowledge on how to identify, manage, and prevent various dental emergencies, helping you protect your oral health and ensure you know exactly what to do when minutes matter.
This article delves into the common types of oral crises, from an avulsed tooth to the unsettling discomfort of dry socket in mouth, providing detailed insights into causes, symptoms, and most importantly, immediate first aid and professional treatment options. We’ll cover everything from managing a severe toothache to understanding alarming conditions like submandibular gland swelling and how to effectively reduce gum swelling, ensuring you have all the information needed to navigate these challenging situations with confidence.
Key Takeaways:
- Act Fast for Avulsed Teeth: A knocked-out tooth has the best chance of re-implantation if seen by a dentist within 30-60 minutes. Keep the tooth moist in milk or saliva.
- Don't Ignore Swelling: Persistent or rapidly worsening gum swelling or salivary gland swelling can indicate a serious infection requiring immediate dental attention.
- Dry Socket Pain is Severe: If you experience intense, throbbing pain after a tooth extraction, especially 2-4 days post-procedure, it's likely a dry socket tooth. Seek prompt treatment for relief.
- Costs Vary Widely: Emergency dental visits can range from $75 - $300 for an exam, with treatments like extractions costing $200 - $600 and root canals $700 - $2,000+. Insurance significantly impacts out-of-pocket costs.
- Prevention is Key: Regular dental check-ups, good oral hygiene, and wearing mouthguards during sports can prevent many common dental emergencies.
- Know When to Seek Care: Any uncontrolled bleeding, severe pain, facial swelling, or a knocked-out permanent tooth warrants immediate emergency dental care.
- Reduce Gum Swelling at Home: Mild gum swelling can often be temporarily relieved with warm salt water rinses and cold compresses, but a dentist must diagnose the underlying cause.
``
Understanding Dental Emergencies: What You Need to Know Now
A dental emergency is any oral problem that requires immediate attention from a dental professional to save a tooth, stop bleeding, alleviate severe pain, or address an infection. Ignoring these issues can lead to irreversible damage, increased pain, and even systemic health complications.
What Constitutes a Dental Emergency?
Not every dental problem is an emergency. Understanding the difference can help you decide whether to call your dentist's emergency line, wait for regular office hours, or even visit an urgent care facility.
True Dental Emergencies require immediate attention (within hours):
- A permanent tooth that has been knocked out (avulsed).
- Severe toothache that doesn't subside with over-the-counter pain relievers, especially if accompanied by fever or swelling.
- Uncontrolled bleeding in the mouth.
- Swelling of the gums or face that is rapidly spreading or affecting breathing/swallowing.
- Suspected jaw fracture.
Urgent Dental Problems require prompt attention (within 24-48 hours):
- A chipped or fractured tooth that causes pain but no severe bleeding or facial swelling.
- Lost filling or crown, especially if it's causing sensitivity or pain.
- A loose permanent tooth without complete avulsion.
- Dental abscess "Abscess: Complete Dental Guide") (pimple-like bump on gums) that is not accompanied by severe swelling or fever.
- Dry socket in mouth after an extraction.
Non-Urgent Dental Issues can wait for a regular appointment:
- Dull toothache that comes and goes.
- Minor chip or crack in a tooth without pain.
- Food lodged between teeth.
- Broken orthodontic wire that isn't causing severe irritation.
Why Immediate Action Matters
Delaying treatment for a dental emergency can have serious consequences. For instance, a knocked-out tooth's chances of successful re-implantation decrease significantly after the first hour. An untreated infection can spread from your mouth to other parts of your body, potentially leading to life-threatening conditions like cellulitis or sepsis. Severe pain can also disrupt daily life, affecting sleep, eating, and concentration. Prompt intervention often leads to better outcomes, less invasive procedures, and lower overall treatment costs.
Common Types of Dental Emergencies and How to Respond
Navigating a dental emergency can be stressful, but knowing what to do in the first few moments can make a critical difference. Here's a breakdown of common emergencies and initial steps to take.
Avulsed (Knocked-Out) Tooth
An avulsed tooth is a permanent tooth that has been completely dislodged from its socket. This is one of the most time-sensitive dental emergencies.
- Causes: Most commonly caused by trauma, such as sports injuries, falls, or accidents.
- Immediate Steps:
- Find the tooth: Handle it only by the crown (the chewing surface), avoiding touching the root.
- Rinse gently (if dirty): If dirty, rinse the tooth very gently for no more than 10 seconds under cold, running water. Do NOT scrub or use soap.
- Re-insert (if possible): If you can, gently try to place the tooth back into its socket. Bite down gently on a piece of gauze or a clean cloth to hold it in place.
- Keep it moist: If re-insertion isn't possible, keep the tooth moist. The best options, in order of preference, are:
- In a glass of milk.
- In your mouth next to your cheek (if you're an adult and won't swallow it).
- In a sterile saline solution.
- As a last resort, in water, but this is less ideal.
- Seek immediate dental care: Get to a dentist or emergency room within 30-60 minutes for the best chance of saving the tooth.
- Treatment: The dentist will clean the tooth and socket, re-implant the tooth, and splint it to adjacent teeth for several weeks to allow the bone to heal around it. A root canal may be necessary later.
- Cost: Re-implantation, splinting, and follow-up root canal can range from $1,500 - $4,000+ without insurance, depending on the need for subsequent procedures.
``
Chipped, Cracked, or Fractured Tooth
A chipped, cracked, or fractured tooth can range from a cosmetic issue to a severe problem that exposes the tooth's sensitive inner layers.
- Causes: Biting on hard foods, trauma, teeth grinding (bruxism), or large fillings weakening the tooth structure.
- Signs and Symptoms: Sharp pain when biting or chewing, sensitivity to hot and cold, visible crack or missing piece of tooth.
- Immediate Steps: Rinse your mouth with warm water. If there's swelling, apply a cold compress to your face. Take over-the-counter pain relievers if needed. Avoid chewing on the affected side. Collect any broken tooth fragments if possible.
- Treatment Options:
- Small chips: Can often be smoothed or restored with dental bonding (composite resin).
- Moderate cracks: May require a dental crown to protect the tooth from further fracture.
- Deep fractures: If the crack extends into the pulp (nerve) or root, a root canal may be needed, followed by a crown. In severe cases, extraction might be the only option.
- Cost: Bonding: $100 - $400. Crown: $800 - $2,500. Root Canal: $700 - $2,000+. Extraction: $200 - $600.
Severe Toothache and Dental Abscess
A severe, persistent toothache is a clear sign that something is wrong, often indicating infection or decay that has reached the tooth's nerve. A dental abscess is a localized collection of pus, usually caused by a bacterial infection.
- Causes: Deep decay, trauma leading to a cracked tooth, gum disease, or failed previous dental work.
- Signs and Symptoms:
- Toothache: Throbbing, sharp, or constant pain, often worsening with hot/cold or chewing.
- Abscess: A persistent, throbbing pain, sensitivity to hot/cold, pain when chewing, fever, facial swelling, tender lymph nodes, and a small, pimple-like bump on the gums (fistula) that may periodically release pus.
- Risks: Untreated infections can spread to the jaw, neck, brain, or bloodstream (sepsis), which can be life-threatening.
- Immediate Steps: Rinse your mouth thoroughly with warm salt water to help reduce swelling and draw out pus. Do not place aspirin directly on the gum as it can burn the tissue. Take over-the-counter pain relievers (like ibuprofen or acetaminophen). Apply a cold compress to the outside of your cheek for swelling. Seek immediate dental attention.
- Treatment Options:
- Drainage: The dentist will drain the abscess to relieve pressure and remove the infection.
- Root Canal Therapy: To remove the infected pulp from inside the tooth.
- Tooth Extraction: If the tooth is too damaged to be saved.
- Antibiotics: May be prescribed to help control the infection, but they are not a substitute for removing the source of the infection.
- Cost: Abscess drainage alone: $150 - $400. Root canal: $700 - $2,000+. Extraction: $200 - $600.
Lost Filling or Crown
While not always painful, a lost filling or crown can expose the sensitive dentin or pulp of a tooth, leading to sensitivity, pain, and vulnerability to further damage or decay.
- Immediate Steps:
- For a lost filling: Clean the area gently. You can temporarily fill the cavity with over-the-counter dental cement or even a piece of sugar-free gum until you see a dentist. Avoid chewing on that side.
- For a lost crown: Try to locate the crown. If the tooth underneath is intact, you might be able to temporarily re-seat the crown using a small amount of over-the-counter dental cement (available at pharmacies) or even toothpaste. Never use super glue. Clean the crown and the tooth thoroughly beforehand.
- Treatment: The dentist will assess if the tooth can be refilled or if the crown can be re-cemented. Sometimes, a new filling or crown is necessary.
- Cost: Re-cementing a crown: $75 - $200. New filling: $100 - $400. New crown: $800 - $2,500.
Extruded (Partially Dislodged) or Luxated Tooth
An extruded tooth is one that has been pushed partially out of its socket, while a luxated tooth has been displaced but not fully extruded or avulsed.
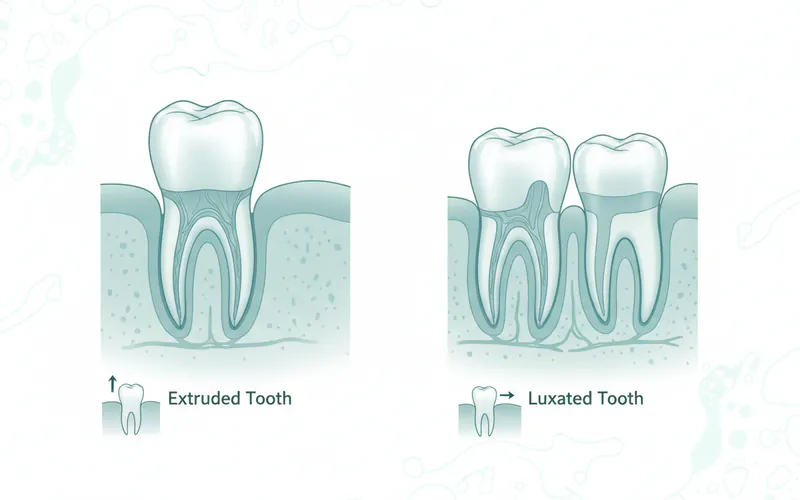
- Causes: Trauma or injury to the mouth.
- Signs and Symptoms: The tooth appears longer than adjacent teeth, is loose, and may be painful when touched or moved.
- Immediate Steps: Gently try to reposition the tooth into its normal alignment using light finger pressure. Apply a cold compress to the outside of your mouth. Seek immediate dental care.
- Treatment: The dentist will reposition the tooth and stabilize it with a flexible splint to adjacent teeth. Root canal treatment may be required later if the pulp is damaged.
- Cost: Repositioning and splinting: $300 - $800.
Soft Tissue Injuries (Gums, Cheeks, Lips, Tongue)
Cuts, punctures, and lacerations to the soft tissues of the mouth can bleed heavily due to the rich blood supply.
- Causes: Biting your tongue or cheek, sports injuries, falls, or sharp foods.
- Immediate Steps:
- Rinse: Rinse your mouth with a mild salt-water solution to clean the area.
- Control bleeding: Apply firm, direct pressure to the wound using a clean piece of gauze or cloth for at least 10-15 minutes.
- Reduce swelling: Apply a cold compress to the outside of the mouth/face.
- Seek care: If bleeding doesn't stop after 10-15 minutes, the cut is deep or wide, or you suspect something is embedded, seek emergency dental or medical attention. Stitches may be necessary.
- Treatment: The dentist or doctor may clean the wound, remove foreign objects, and suture the laceration.
Swelling of Gums and Salivary Glands
Swelling in your mouth or jaw can indicate a serious underlying problem, ranging from infection to blockages in salivary glands.
Causes of Gum Swelling
Gum swelling can be localized to a single tooth or affect a broader area.
- Infection/Abscess: A common cause is a bacterial infection, often from severe decay or periodontal disease, leading to a pocket of pus. This causes localized gum swelling around the affected tooth.
- Gingivitis/Periodontitis: Chronic inflammation of the gums due to plaque buildup. While usually not an emergency, acute flare-ups can cause significant swelling and pain.
- Impacted Wisdom Tooth: When a wisdom tooth doesn't fully erupt, the gum tissue over it can become inflamed and infected (pericoronitis), leading to localized gum swelling and pain in the back of the mouth.
- Food Impaction: Sometimes, food debris gets trapped deep under the gum line, irritating the tissue and causing swelling.
- Medication Side Effects: Certain medications can cause gum overgrowth, which can appear as swelling.
- Nutritional Deficiencies: In rare cases, severe vitamin C deficiency (scurvy) can cause swollen, bleeding gums.
Signs and Symptoms: Redness, tenderness, pain, bleeding, shiny appearance, bad breath, and sometimes fever.
How to Reduce Gum Swelling (Temporary Home Care):
- Warm Salt Water Rinses: Rinse your mouth with a solution of 1/2 teaspoon salt in 8 ounces of warm water several times a day. This helps reduce inflammation and can draw out pus.
- Cold Compress: Apply a cold compress to the outside of your face to help reduce swelling and discomfort, especially if the swelling is significant.
- Good Oral Hygiene: Gently brush and floss around the affected area to remove plaque and food debris, but avoid irritating the swollen tissue.
- Over-the-Counter Pain Relievers: Ibuprofen or acetaminophen can help manage pain and inflammation.
Pro Tip: While these home remedies can provide temporary relief, they do not address the root cause of the gum swelling. It is crucial to see a dentist for diagnosis and appropriate gum swelling treatment.
Gum Swelling Treatment:
- Deep Cleaning (Scaling and Root Planing): For gum disease, to remove plaque and calculus below the gum line.
- Antibiotics: To combat bacterial infections.
- Abscess Drainage: If a pus pocket is present, the dentist will drain it.
- Root Canal or Extraction: If the infection originates from the tooth's pulp.
- Wisdom Tooth Extraction: If an impacted wisdom tooth is the cause.
Salivary Gland Swelling
Swelling of the salivary glands can be alarming and sometimes indicate a serious condition. There are three major pairs of salivary glands: parotid (in front of ears), submandibular (under the jaw), and sublingual (under the tongue).
- Causes of Salivary Gland Swelling:
- Sialolithiasis (Salivary Stones): Small calcified masses can block the ducts of salivary glands, most commonly the submandibular gland. This causes pain and submandibular gland swelling or swelling in other glands, especially during or after eating.
- Sialadenitis (Bacterial Infection): Often caused by reduced saliva flow, leading to a bacterial infection within the gland. Can affect any gland, leading to general salivary gland swelling, pain, fever, and pus drainage.
- Viral Infections: Mumps is a classic example, causing bilateral parotid gland swelling. Other viruses like influenza, CMV, or HIV can also cause salivary gland swelling.
- Cysts or Tumors: While less common, growths can cause persistent salivary gland swelling.
- Autoimmune Diseases: Conditions like Sjögren's syndrome can cause chronic swelling and dry mouth.
Signs and Symptoms:
- Pain and tenderness in the affected gland (e.g., under the jaw for submandibular gland swelling).
- Swelling that may worsen with eating.
- Dry mouth.
- Difficulty opening the mouth or swallowing.
- Fever, chills (with infection).
- A foul taste or pus drainage into the mouth (with bacterial infection).
Treatment for Salivary Gland Swelling:
- Warm Compresses: Applied to the affected area.
- Hydration: Drink plenty of fluids.
- Gland Massage: Gentle massage of the gland can help stimulate saliva flow.
- Sour Candies/Lemon: To encourage saliva production and help dislodge stones.
- Antibiotics: For bacterial infections.
- Stone Removal: Small stones may pass on their own; larger ones may require minor surgical removal.
- Surgery: For large stones, recurrent infections, or tumors.
Dry Socket (Alveolar Osteitis)
Dry socket in mouth is a painful complication that can occur after a tooth extraction, usually 2-4 days post-procedure.
- What it is: Instead of a protective blood clot forming in the empty socket, the clot either fails to form, dislodges prematurely, or dissolves, leaving the underlying bone and nerve exposed to air, food, and fluids. This exposes the dry socket tooth area.
- Causes: Trauma to the extraction site, tobacco use, poor oral hygiene, oral contraceptives, or difficult extractions.
- Signs and Symptoms: Intense, throbbing pain that radiates to the ear, eye, temple, or neck, usually 2-4 days after extraction. A visible empty socket, foul odor from the mouth, or unpleasant taste.
- Treatment:
- Cleaning: The dentist will gently clean the socket to remove any debris.
- Medicated Dressing: A medicated paste or dressing is placed into the socket to protect the exposed bone and promote healing. This dressing needs to be changed periodically.
- Pain Management: Prescription pain medication may be necessary.
- Rinsing: Specific antiseptic mouth rinses might be prescribed.
- Prevention: Follow all post-extraction instructions meticulously: avoid smoking, drinking through a straw, vigorous rinsing, and eating hard/crunchy foods for the first few days.
- Cost: $100 - $300 per visit for cleaning and dressing. Several visits might be needed.
Orthodontic Emergencies
While typically not life-threatening, issues with braces or aligners can be painful and require prompt attention.
- Common Issues: Broken wires, loose brackets, poky wires, or lost aligners.
- Immediate Steps:
- Poky wire: Try to gently push it back into place with a cotton swab or pencil eraser. If not possible, cover the end with orthodontic wax or a small piece of cotton.
- Loose bracket: If it's still attached to the wire, leave it alone. If it comes off, save it.
- Seek Orthodontist: Contact your orthodontist as soon as possible for repair.
General Principles of Immediate First Aid for Dental Emergencies
While waiting to see a dentist, these steps can help manage the situation:
- Stay Calm: Panic can make the situation worse.
- Control Bleeding: For cuts or persistent bleeding, apply firm, direct pressure with a clean gauze or cloth for 10-15 minutes.
- Manage Pain: Over-the-counter pain relievers like ibuprofen (Advil, Motrin) or acetaminophen (Tylenol) can help. Follow dosage instructions.
- Reduce Swelling: Apply a cold compress (ice pack wrapped in a cloth) to the outside of your face or jaw in 20-minute intervals.
- Clean the Area: Rinse your mouth gently with warm water, possibly with a teaspoon of salt added, to help clean wounds and reduce inflammation.
- Protect the Tooth/Area: Avoid chewing on the affected side. If a tooth is chipped or sensitive, cover it temporarily with orthodontic wax or sugar-free gum.
When to Seek Professional Dental Care
It can be challenging to determine if your situation warrants an emergency visit. Here's a guide:
- Immediate Emergency (Call Dentist/Go to ER NOW):
- A knocked-out permanent tooth (avulsion).
- Uncontrolled bleeding from the mouth.
- Severe, rapidly spreading facial or oral swelling, especially if it affects breathing or swallowing.
- Suspected jaw fracture.
- Intense, unbearable pain that doesn't respond to OTC medication.
- Urgent Care (Call Dentist Today/Within 24-48 hours):
- Severe toothache that is persistent but not accompanied by widespread swelling or fever.
- A large chip or crack in a tooth exposing the inner layers.
- Lost filling or crown causing pain or sensitivity.
- Dry socket in mouth after an extraction.
- Localized gum swelling or salivary gland swelling that is painful or accompanied by fever.
- Routine Care (Schedule a Regular Appointment):
- Minor, painless chip or crack.
- Loose crown or filling with no pain or sensitivity.
- Dull, intermittent toothache.
Always err on the side of caution. When in doubt, call your dentist or an emergency dental clinic. Many dental practices offer emergency contact numbers outside of regular business hours.
The Dental Emergency Visit: What to Expect
When you arrive for an emergency visit, the dentist's primary goal is to diagnose the problem, alleviate pain, and prevent further complications.
Step-by-Step Process for a Typical Emergency Visit:
- Initial Assessment: The dental team will ask about your symptoms, when they started, and any relevant medical history.
- Examination: The dentist will conduct a thorough oral examination of the affected area and surrounding tissues.
- Imaging: X-rays are almost always necessary to visualize the teeth, roots, jawbone, and surrounding structures to identify the source of the problem (e.g., abscess, fracture, impacted tooth).
- Diagnosis: Based on the exam and X-rays, the dentist will make a diagnosis and explain the issue.
- Treatment Options & Plan: The dentist will discuss the recommended emergency treatment, potential alternative options, and what to expect. They will also outline any necessary follow-up care.
- Emergency Treatment: This could involve:
- Pain Relief: Administering local anesthetic to numb the area.
- Infection Control: Draining an abscess, prescribing antibiotics.
- Temporary Restoration: Placing a temporary filling or crown.
- Tooth Stabilization: Splinting an avulsed or luxated tooth.
- Extraction: If the tooth is beyond repair.
- Medicated Dressing: For dry socket in mouth.
- Post-Treatment Instructions: You'll receive specific instructions for aftercare, including pain management, dietary restrictions, and oral hygiene, along with scheduling any necessary follow-up appointments.
Pro Tip: Be prepared to provide your full medical history, including any medications you are taking, allergies, and existing medical conditions, as this can influence treatment decisions.
Costs of Dental Emergency Treatment and Insurance Coverage
The cost of dental emergency treatment in the US can vary significantly based on the type of emergency, the complexity of the procedure, the dentist's fees, geographic location, and whether you have dental insurance.
Average US Costs (Without Insurance):
- Emergency Exam & X-ray: $75 - $300
- Abscess Drainage: $150 - $400 (initial treatment, may not include definitive care)
- Simple Extraction: $200 - $400
- Surgical Extraction (e.g., impacted wisdom tooth): $300 - $600+
- Dry Socket Treatment: $100 - $300 per visit (may require multiple visits)
- Dental Bonding (small chip): $100 - $400
- Re-cementing a Crown: $75 - $200
- Root Canal Therapy (Front Tooth): $700 - $1,200
- Root Canal Therapy (Molar): $1,000 - $2,000+
- Avulsed Tooth Re-implantation & Splinting: $300 - $800 (initial procedure, excludes potential root canal later)
Impact of Insurance:
Most dental insurance plans (PPO, HMO) cover a percentage of emergency treatments after you meet your deductible. Preventive care (exams, X-rays, cleanings) is often covered at 80-100%, while basic restorative care (fillings, extractions) may be covered at 50-80%. Major procedures (root canals, crowns) might be covered at 30-50%.
- Deductible: The amount you must pay out-of-pocket before your insurance begins to cover costs, typically $50 - $150 per year.
- Co-pay: A fixed amount you pay for a service at the time of visit.
- Coinsurance: The percentage of the cost you are responsible for after meeting your deductible.
- Annual Maximum: The total amount your insurance company will pay for your dental care in a policy year, often $1,000 - $2,000.
Pro Tip: Always call your insurance provider before treatment to understand your specific benefits, deductibles, co-pays, and annual maximums for emergency services.
Payment Plans and Financing Options:
- In-Office Payment Plans: Many dental offices offer interest-free payment plans for larger treatments.
- Third-Party Financing: Companies like CareCredit or LendingClub provide healthcare credit cards with deferred interest options.
- Dental Schools: University dental schools often provide services at a reduced cost, performed by supervised students.
- Community Dental Clinics: Some community health centers offer affordable dental care based on a sliding scale.
| Procedure | Estimated Cost (No Insurance) | Typical Coverage (with PPO Insurance) | Out-of-Pocket (with Insurance, after deductible) |
|---|---|---|---|
| Emergency Exam & X-ray | $75 - $300 | 80-100% | $0 - $60 |
| Simple Tooth Extraction | $200 - $400 | 50-80% | $40 - $200 |
| Abscess Drainage (initial) | $150 - $400 | 50-70% | $45 - $200 |
| Root Canal (Molar) | $1,000 - $2,000+ | 30-50% | $500 - $1,400+ |
| Dry Socket Treatment (per visit) | $100 - $300 | 50-70% | $30 - $150 |
| Re-cementing Crown | $75 - $200 | 50-80% | $15 - $100 |
Note: Costs are estimates and can vary widely. Deductibles and annual maximums apply.
Recovery and Aftercare for Dental Emergencies
Proper aftercare is crucial for successful healing and preventing complications following a dental emergency.
- Pain Management: Follow your dentist's instructions for prescription pain relievers. Over-the-counter options like ibuprofen or acetaminophen can also be used.
- Swelling: Continue applying cold compresses in 20-minute intervals for the first 24-48 hours. After that, warm compresses can promote circulation and healing.
- Diet: Stick to soft foods for the first few days (e.g., soup, yogurt, mashed potatoes, scrambled eggs). Avoid hot, spicy, hard, or crunchy foods. Gradually reintroduce normal foods as comfort allows.
- Oral Hygiene: Gently brush and floss, avoiding the immediate treatment site for the first 24 hours or as advised. Your dentist may recommend a special antiseptic mouth rinse.
- Avoid Straws & Smoking: For extractions or dry socket prevention, avoid using straws and smoking, as the sucking action can dislodge blood clots.
- Activity: Rest and avoid strenuous activity for the first 24-48 hours.
- Follow-Up Appointments: Attend all scheduled follow-up appointments to ensure proper healing and address any concerns. This is particularly important for procedures like root canals or re-implanted teeth.
Preventing Dental Emergencies: Proactive Steps for Oral Health
Many dental emergencies are preventable. By adopting good habits and being proactive, you can significantly reduce your risk.
- Regular Dental Check-ups and Cleanings: Visiting your dentist every six months allows them to identify and treat minor issues (like small cavities or early gum disease) before they escalate into emergencies. The American Dental Association (ADA) strongly recommends these routine visits.
- Maintain Excellent Oral Hygiene:
- Brush your teeth twice a day with fluoride toothpaste for at least two minutes.
- Floss daily to remove plaque and food debris from between teeth and under the gum line.
- Use an antiseptic mouthwash to reduce bacteria.
- Wear a Mouthguard for Sports: If you play contact sports or engage in activities with a risk of facial injury, a custom-fitted mouthguard can protect your teeth from chips, fractures, and avulsion.
- Avoid Chewing Hard Objects: Don't chew on ice, popcorn kernels, hard candies, or use your teeth to open packages, as this can lead to chipped or fractured teeth.
- Address Bruxism (Teeth Grinding): If you grind your teeth at night, a nightguard can protect your teeth from excessive wear and fracture.
- Manage Existing Dental Conditions: Promptly treat cavities, gum disease, and orthodontic issues to prevent them from worsening.
- Healthy Diet: Limit sugary and acidic foods and drinks that contribute to tooth decay.
- Quit Tobacco: Smoking and tobacco use severely increase the risk of gum disease, tooth loss, and impaired healing.
Risks and Complications of Untreated Dental Emergencies
Ignoring a dental emergency can lead to a cascade of serious problems:
- Spread of Infection: An untreated dental abscess or infection can spread to the jawbone, sinuses, neck, and even the brain, leading to life-threatening conditions like cellulitis, osteomyelitis, or sepsis.
- Tooth Loss: Many emergencies, like deep fractures or severe infections, can ultimately lead to the loss of the affected tooth if not treated promptly.
- Chronic Pain: Persistent, untreated dental issues can result in chronic oral and facial pain, significantly impacting quality of life.
- Damage to Adjacent Teeth: Untreated infections can spread to neighboring teeth, affecting their health and requiring more extensive treatment.
- Systemic Health Issues: Oral health is intrinsically linked to overall health. Untreated dental infections can exacerbate existing conditions like diabetes or heart disease.
- Increased Treatment Complexity and Cost: Delaying care almost always results in more complex, invasive, and expensive treatments down the line.
Pediatric Dental Emergencies: Special Considerations for Children
Children are particularly prone to dental emergencies due to falls, playground accidents, and sports injuries. Parents need to know how to respond to protect their child's developing dentition.
- Common Pediatric Emergencies:
- Avulsed (Knocked-Out) Tooth: The critical distinction here is whether it's a primary (baby) tooth or a permanent tooth.
- Chipped/Fractured Teeth: Very common in active children.
- Intruded Tooth: A tooth pushed up into the gum line.
- Soft Tissue Injuries: Lacerations to lips, tongue, or cheeks.
- Severe Toothache: Often due to deep cavities.
Handling Avulsed Teeth in Children:
| Feature | Primary (Baby) Tooth | Permanent Tooth |
|---|---|---|
| Action | DO NOT attempt to re-implant the tooth. | Attempt to re-implant immediately if possible. |
| Why? | Re-implantation can damage the developing permanent tooth bud underneath. | Best chance of survival is if re-implanted within 30-60 minutes. |
| What to do? | Find the tooth (for dentist to examine), apply gauze to stop bleeding, contact pediatric dentist. | Handle by crown, gently rinse, try to re-insert, or place in milk/saliva. See dentist immediately. |
| Prognosis | Usually no long-term issues if the permanent tooth bud is undamaged. | Good chance of saving the tooth with prompt re-implantation and follow-up care. |
- For all dental trauma in children:
- Stay calm and comfort your child.
- Control any bleeding with gentle pressure.
- Clean the area gently with water.
- Apply a cold compress to reduce swelling.
- Contact a pediatric dentist immediately. They are specialists in treating children and managing their specific dental needs.
- Save any broken tooth fragments.
- If there's any concern about head injury, loss of consciousness, or other significant trauma, go to the nearest emergency room first.
Frequently Asked Questions
H3: How do I know if it's a dental emergency?
A dental emergency typically involves severe pain, uncontrolled bleeding, facial swelling, or a knocked-out permanent tooth. If you're unsure, call your dentist immediately; they can assess your symptoms and advise on the urgency.
H3: Can I go to an urgent care clinic for a dental emergency?
Urgent care clinics can manage pain and provide antibiotics for infections, but they generally cannot perform definitive dental procedures like extractions, root canals, or tooth re-implantation. It's best to see a dentist for specific dental issues.
H3: How much does an emergency dental visit cost without insurance?
An emergency exam and X-ray without insurance can range from $75 to $300. If a procedure like an extraction or abscess drainage is performed, the total cost will increase, often ranging from $200 to $600+ for basic interventions.
H3: What's the fastest way to stop severe tooth pain?
For immediate relief, take over-the-counter pain relievers like ibuprofen or acetaminophen. You can also apply a cold compress to the outside of your cheek and rinse your mouth with warm salt water. However, these are temporary measures; you need to see a dentist to address the cause of the pain.
H3: How long can I wait to see a dentist for a chipped tooth?
If the chip is minor and not causing pain or sensitivity, you might be able to wait a few days for a regular appointment. However, if the chip is large, causes pain, or exposes the tooth's inner layers, you should see a dentist within 24-48 hours to prevent further damage or infection.
H3: Is gum swelling always an emergency?
Not always. Mild gum swelling might be due to trapped food or gingivitis and can often be managed initially with good hygiene and salt water rinses. However, if the swelling is painful, persistent, spreading, accompanied by fever, or interferes with eating/swallowing, it requires immediate dental attention as it could indicate a serious infection like an abscess.
H3: Can a dry socket be prevented?
Yes, dry socket in mouth can largely be prevented by carefully following your dentist's post-extraction instructions. This includes avoiding smoking, drinking through a straw, vigorous rinsing, and eating hard foods for the first few days after an extraction to protect the blood clot.
H3: What should I do if a permanent tooth gets knocked out?
Handle the tooth only by the crown, gently rinse it (if dirty) for no more than 10 seconds, and try to re-insert it into its socket. If unsuccessful, keep it moist in milk or saliva and see a dentist immediately, ideally within 30-60 minutes, for the best chance of saving the tooth.
H3: Are antibiotics always necessary for a dental infection?
Antibiotics are often prescribed for spreading dental infections or abscesses, but they are typically only a temporary measure. The definitive gum swelling treatment or other infection treatment usually involves a dental procedure like drainage, root canal, or extraction to remove the source of the infection.
H3: What are the signs of a serious dental infection?
Signs of a serious dental infection include severe, throbbing pain, significant facial or jaw swelling that may be spreading, fever, chills, difficulty swallowing or breathing, and tender lymph nodes in the neck. These symptoms warrant immediate dental or medical attention.
When to See a Dentist
Knowing when to seek professional help can prevent minor issues from becoming major problems.
Call your dentist IMMEDIATELY (within hours) if you experience any of the following:
- A permanent tooth is completely knocked out (avulsed tooth).
- You have uncontrolled bleeding from your mouth.
- Severe, rapidly spreading swelling in your face or mouth, especially if it's impacting your ability to breathe or swallow.
- Intense, unbearable tooth pain that doesn't respond to pain relievers.
- Suspected jaw fracture or other significant trauma to your face/mouth.
Call your dentist URGENTLY (within 24-48 hours) for:
- A chipped or fractured tooth that causes pain or sensitivity.
- A lost filling or crown that is painful or exposes sensitive tooth structure.
- Persistent, severe gum swelling or salivary gland swelling with pain or fever.
- Symptoms of a dry socket in mouth after a tooth extraction.
- A painful dental abscess (pimple on the gums).
- A tooth that is significantly loose or displaced.
Schedule a regular appointment for:
- Minor chips or cracks that are not painful.
- A lost filling or crown that is not causing pain or sensitivity.
- Dull, intermittent toothaches.
- Any concerns about your oral health that are not causing acute pain or severe symptoms.
Your oral health is a vital component of your overall well-being. By understanding dental emergencies and how to respond, you empower yourself to act decisively and protect your smile.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
How to Relieve Gum Swelling
When your gums are swollen, it can be an alarming and uncomfortable experience, often signaling an underlying issue that requires attention. Statistics from the Centers for Disease Control and Prevention (CDC) reveal that **nearly half of adults aged 30 or older in the United States have some form o
February 23, 2026
Teeth Swelling: Complete Guide
When you experience teeth swelling, it's more than just a minor discomfort; it's a clear signal from your body that something is amiss within your oral cavity, often indicating an underlying infection or inflammation that requires prompt attention. A recent survey revealed that **over 25% of adu
February 23, 2026
Submandibular Salivary Gland Swelling: Complete Guide
When you notice a peculiar lump or uncomfortable fullness beneath your jaw, it can be an alarming experience. This sensation, often accompanied by pain and difficulty swallowing, could indicate submandibular salivary gland swelling. Affecting an estimated 1 in 10,000 adults annually, conditi
February 23, 2026
What Helps With Gum Swelling
Gum swelling, medically known as gingival swelling or gingivitis, is a common yet often underestimated dental issue affecting millions of Americans. Have you ever woken up with sore, puffy gums that bleed easily when you brush? You're not alone. Research indicates that nearly **half of all a
February 23, 2026