Teeth Swelling: Complete Guide
Key Takeaways
- When you experience teeth swelling, it's more than just a minor discomfort; it's a clear signal from your body that something is amiss within your oral cavity, often indicating an underlying infection or inflammation that requires prompt attention. A recent survey revealed that **over 25% of adu
When you experience teeth swelling, it's more than just a minor discomfort; it's a clear signal from your body that something is amiss within your oral cavity, often indicating an underlying infection or inflammation that requires prompt attention. A recent survey revealed that over 25% of adults in the US report experiencing some form of oral pain or discomfort annually, with swelling being a common accompanying symptom. Ignoring swelling around a tooth or your gums can escalate quickly, leading to severe pain, widespread infection, and potentially serious health complications. This comprehensive guide will explore the various causes of teeth swelling, detail the associated symptoms, outline effective treatment strategies, delve into cost implications, and provide essential advice on prevention and recovery. By understanding the intricacies of this common dental issue, you'll be better equipped to protect your oral health and know exactly when to seek professional help.
Key Takeaways:
- Teeth swelling is often a sign of infection: Most cases are due to dental abscesses (root or gum), periodontal disease, or impacted wisdom teeth. Prompt treatment is crucial to prevent spread.
- Don't delay seeking care: If swelling is accompanied by fever, difficulty breathing, or swallowing, it's a dental emergency requiring immediate attention to avoid life-threatening complications like sepsis or Ludwig's angina.
- Home remedies are temporary: While saltwater rinses or cold compresses can offer temporary relief, they do not address the root cause of swelling and should not replace professional dental care.
- Treatment costs vary widely: Simple antibiotic prescriptions might be under $50, while a root canal can range from $700 to $2,000, and an extraction from $75 to $600, depending on complexity and location. Insurance typically covers a portion, usually 50-80%, for medically necessary procedures.
- Prevention is key: Consistent oral hygiene, regular dental check-ups (every 6 months, typically $75-$200 for exam/cleaning), and addressing dental issues early can prevent most instances of teeth swelling.
- TMJ can cause facial swelling: Though less common, temporomandibular joint (TMJ) disorders can lead to swelling and pain around the jaw joint, sometimes mimicking dental issues.
What It Is / Overview
Teeth swelling refers to the inflammation and enlargement of tissues surrounding a tooth, within the gum, or even extending into the facial structures. It's not a condition in itself but rather a symptom, a warning sign that your body is reacting to an irritant, infection, or injury. This swelling can manifest in various ways: as a localized bulge in the gum, a general puffiness of the cheek, or even visible facial asymmetry.

The underlying mechanism often involves an immune response. When bacteria, trauma, or other irritants trigger inflammation, blood vessels in the affected area dilate, increasing blood flow and allowing immune cells to rush to the site. This influx of fluid, cells, and inflammatory mediators causes the tissue to expand, leading to the characteristic swelling, redness, heat, and pain. Understanding the specific location and nature of the swelling is critical for dentists to accurately diagnose the root cause and recommend appropriate treatment.
Types / Variations of Teeth Swelling
Swelling associated with your teeth can present in several forms, each pointing to different underlying issues:
Gum Swelling (Gingival Edema)
This is the most common type, where the gum tissue around one or more teeth becomes inflamed and enlarged.
- Localized Gum Swelling: Often occurs around a single tooth, frequently due to a dental abscess (periapical or periodontal), food impaction, or localized trauma.
- Generalized Gum Swelling: Affects larger areas of the gums, typically a hallmark of generalized gingivitis or periodontitis. It can also be a side effect of certain medications or systemic conditions.
Facial Swelling
When the infection or inflammation spreads beyond the immediate tooth and gum area, it can manifest as swelling in the cheek, jawline, or under the eye. This is a more serious indicator.
- Odontogenic Swelling: Directly linked to a tooth infection (abscess) that has spread into the surrounding soft tissues of the face. This can be dangerous as the infection can track into vital spaces.
- Non-Odontogenic Facial Swelling: Swelling not originating from a tooth, but perhaps from salivary gland infections, sinusitis, or even conditions like mumps. While not "teeth swelling" per se, it can be confused with it.
Swelling Around Impacted Teeth
Impacted wisdom teeth are a common culprit for localized swelling. When a wisdom tooth doesn't fully erupt, it creates a flap of gum tissue (operculum) that can trap food and bacteria, leading to an infection called pericoronitis. This causes significant localized swelling and pain around the back of the jaw.
Bone Swelling
In rare but severe cases, chronic infection can lead to inflammation and enlargement of the alveolar bone (the bone that holds the teeth). This is less common and usually associated with long-standing, untreated infections or osteomyelitis.
Causes / Why It Happens
The causes of teeth swelling are diverse, ranging from common infections to less frequent systemic issues. Identifying the specific cause is paramount for effective treatment.
1. Dental Abscesses
This is arguably the most common and urgent cause of localized teeth swelling. An abscess is a localized collection of pus formed by bacterial infection.
- Periapical Abscess: Occurs at the tip of the tooth root, usually due to deep tooth decay or trauma that has allowed bacteria to enter the tooth's pulp (nerve tissue). The infection then spreads out of the root into the surrounding bone and soft tissues, causing significant swelling, often resembling a pimple on the gum or even spreading into the face.
- Periodontal Abscess: Develops in the gum tissue itself, typically due to advanced gum disease (periodontitis). Bacteria accumulate in deep periodontal pockets, leading to infection and pus formation.
2. Gum Disease (Gingivitis and Periodontitis)
Poor oral hygiene leads to plaque and tartar buildup, irritating the gums.
- Gingivitis: The initial stage, characterized by red, swollen, and bleeding gums. The swelling is usually mild and generalized.
- Periodontitis: If gingivitis is left untreated, it progresses to periodontitis, where the infection damages the bone and ligaments supporting the teeth. This can cause more pronounced, chronic gum swelling, deep pockets, and eventually tooth mobility and loss.
3. Impacted Wisdom Teeth
As mentioned, wisdom teeth that don't erupt properly can cause pericoronitis, an infection of the gum flap covering the partially erupted tooth. This often results in painful swelling around the wisdom tooth, difficulty opening the mouth, and sometimes facial swelling in the jaw area.
4. Trauma
An injury to the mouth, such as a sports injury, fall, or blow to the face, can cause:
- Direct Gum Trauma: Leading to immediate swelling, bruising, and potential cuts.
- Tooth Trauma: If a tooth is chipped, fractured, or dislodged, it can damage the pulp, leading to infection and subsequent abscess formation and swelling weeks or months later.
5. Temporomandibular Joint (TMJ) Disorders
Can TMJ cause facial swelling? Yes, while less common than dental infections, TMJ disorders can certainly contribute to facial swelling. The temporomandibular joints are the hinges connecting your jawbone to your skull. Issues like disc displacement, arthritis, or muscle strain can cause inflammation in the joint capsule or surrounding muscles, leading to:
- Localized Swelling: Around the jaw joint, typically just in front of the ear.
- Referred Pain: Pain that mimics a toothache.
- Muscle Spasm: Leading to tenderness and a feeling of fullness in the jaw muscles. The swelling from TMJ is usually non-infectious, but the inflammation can be significant.
6. Cysts and Tumors
Though rare, non-cancerous (benign) or cancerous (malignant) growths in the jawbone or soft tissues can cause localized swelling. Cysts are fluid-filled sacs that can develop in the jaw, often associated with unerupted teeth or chronic infections.
7. Allergic Reactions
An allergic reaction to food, medication, or even dental materials can cause localized or generalized swelling of the lips, gums, or face (angioedema).
8. Systemic Conditions and Medications
- Hormonal Changes: Pregnancy, puberty, and menstruation can sometimes cause temporary gum sensitivity and mild swelling due to hormonal fluctuations.
- Certain Medications: Some drugs, particularly calcium channel blockers (used for high blood pressure) and immunosuppressants, can cause gingival hyperplasia (overgrowth of gum tissue), which appears as significant gum swelling.
- Nutritional Deficiencies: Severe vitamin C deficiency (scurvy) can lead to swollen, bleeding gums.
- Immunocompromised States: Conditions like diabetes, HIV, or cancer treatment can make individuals more susceptible to severe oral infections and subsequent swelling.
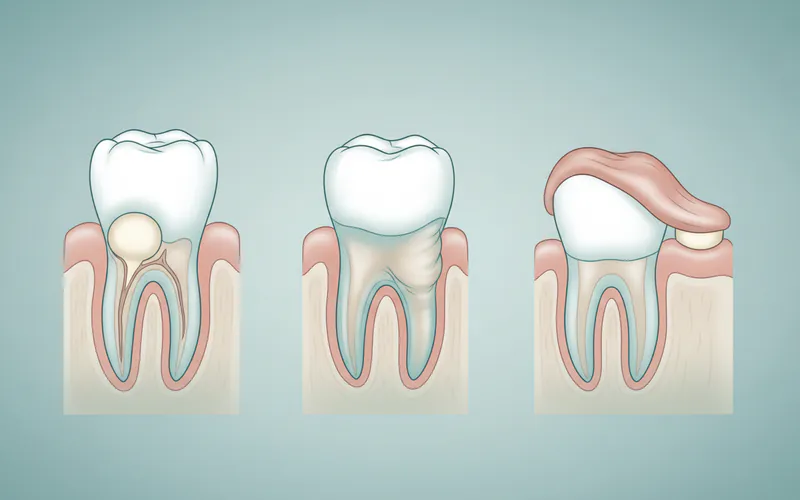
Signs and Symptoms
Recognizing the signs and symptoms of teeth swelling is crucial for timely intervention. While swelling itself is a primary symptom, it often comes with other indicators:
Primary Signs:
- Visible Swelling: A noticeable bulge or puffiness in the gum tissue, cheek, jaw, or around a specific tooth.
- Redness: The affected area often appears redder than the surrounding healthy tissue due to increased blood flow.
- Tenderness/Pain: The swollen area will typically be painful to touch or when chewing. The pain can range from a dull ache to a sharp, throbbing sensation.
- Heat: The inflamed area may feel warm to the touch.
Accompanying Symptoms:
- Pus Drainage: A foul-tasting discharge from the swollen area, sometimes forming a "pimple-like" bump (fistula) that spontaneously drains.
- Bad Taste/Halitosis: Persistent bad breath or a metallic/sour taste in the mouth, often due to infection.
- Sensitivity: Increased sensitivity to hot, cold, or pressure on the affected tooth.
- Fever: A systemic sign of infection, indicating that the body is fighting off bacteria. This is a serious symptom requiring immediate attention.
- Fatigue/Malaise: A general feeling of being unwell.
- Difficulty Chewing or Swallowing: If the swelling is extensive or affects jaw mobility, it can impede eating and drinking.
- Difficulty Opening Mouth (Trismus): Particularly common with wisdom tooth infections or severe dental abscesses that have spread to jaw muscles.
- Swollen Lymph Nodes: Lymph nodes in the neck or under the jaw may become tender and enlarged as they filter infection.
- Facial Asymmetry: When swelling is significant enough to alter the shape of your face.
- Tooth Discoloration: A tooth that has darkened might indicate pulp necrosis (death of the nerve), a common precursor to a periapical abscess.
Pro Tip: Pay close attention to how quickly the swelling develops and if it's accompanied by systemic symptoms like fever. Rapidly spreading facial swelling, especially with fever, difficulty breathing, or swallowing, constitutes a medical emergency.
Treatment Options
The treatment for teeth swelling is entirely dependent on its underlying cause. A dental professional will conduct a thorough examination, possibly including X-rays, to accurately diagnose the problem.
1. Antibiotics
- When Used: Primarily prescribed for bacterial infections like dental abscesses, pericoronitis, or severe periodontal disease to control the infection before definitive dental treatment.
- Pros: Can reduce swelling, alleviate pain, and prevent the spread of infection.
- Cons: Do not remove the source of infection (e.g., dead tooth pulp, plaque/tartar) and are therefore a temporary solution. Overuse contributes to antibiotic resistance.
- Common Examples: Amoxicillin, clindamycin, metronidazole.
- Typical Cost (without insurance): Prescription costs can range from $10 to $50 for a course.
2. Abscess Drainage
- When Used: For dental abscesses where pus has accumulated.
- Pros: Provides immediate relief from pressure and pain, and helps the infection drain. Often performed in conjunction with antibiotics.
- Cons: Must be followed by definitive treatment of the tooth.
- Process: The dentist will make a small incision in the gum to allow the pus to drain, or in the case of a periapical abscess, may drain through the tooth itself.
- Typical Cost (without insurance): $50 to $200 for simple drainage.
3. Root Canal Treatment (Endodontic Therapy)
- When Used: For periapical abscesses or deep decay that has infected the tooth's pulp.
- Pros: Saves the natural tooth, alleviating pain and eliminating the source of infection.
- Cons: Requires multiple appointments, can be costly, and the tooth may require a crown afterward.
- Process: The infected pulp is removed, the root canals are cleaned, shaped, and filled.
- Typical Cost (without insurance):
- Front tooth: $700 - $1,200
- Premolar: $800 - $1,500
- Molar: $1,000 - $2,000
- Crown after root canal: $800 - $2,500
4. Tooth Extraction
- When Used: When a tooth is severely damaged, untreatable (e.g., extensive decay below the gum line, severe fracture), or if root canal therapy is not feasible or desired. This is also common for infected or impacted wisdom teeth.
- Pros: Completely removes the source of infection.
- Cons: Creates a gap, which may require replacement (implant, bridge) to maintain bite function and prevent shifting of adjacent teeth.
- Typical Cost (without insurance):
- Simple extraction: $75 - $300
- Surgical extraction (e.g., impacted wisdom tooth): $200 - $600 per tooth, potentially more for complex cases with anesthesia.
5. Periodontal Treatment
- When Used: For gum swelling caused by gingivitis or periodontitis.
- Pros: Addresses the underlying gum disease, reduces inflammation, and prevents further bone loss.
- Cons: Requires ongoing maintenance and strict oral hygiene.
- Treatment Options:
- Scaling and Root Planing (Deep Cleaning): Removes plaque and tartar from above and below the gum line. Often involves multiple sessions.
- Cost (without insurance): $150 - $400 per quadrant, or $600 - $1,600 for the full mouth.
- Periodontal Surgery: For advanced cases to reduce pocket depth or regenerate lost tissue.
- Cost (without insurance): Can range from $500 to $4,000+ depending on the procedure.
- Scaling and Root Planing (Deep Cleaning): Removes plaque and tartar from above and below the gum line. Often involves multiple sessions.
6. TMJ Therapy
- When Used: For swelling related to Temporomandibular Joint disorders.
- Pros: Addresses joint and muscle pain, improves jaw function.
- Cons: Can be a chronic condition requiring ongoing management.
- Treatment Options:
- Conservative management: Pain relievers, muscle relaxants, heat/cold therapy, soft diet.
- Occlusal Splints (Nightguards): Custom-made devices to protect teeth and reposition the jaw.
- Cost (without insurance): $300 - $800.
- Physical Therapy: Exercises to strengthen jaw muscles and improve mobility.
- Injections: Corticosteroid or Botox injections.
- Cost (without insurance): $200 - $800 per injection.
- Surgery: Rarely needed, for severe structural problems.
- Cost (without insurance): Can range from $5,000 to $20,000+.
7. Other Treatments
- Cyst Removal: Surgical excision.
- Cost (without insurance): $500 - $2,000+.
- Allergy Management: Antihistamines, corticosteroids if allergic reaction.
- Medication Review: If a medication is causing gum overgrowth, consultation with a physician to explore alternatives.

Pro Tip: Always complete your full course of antibiotics, even if symptoms improve, to ensure the infection is fully eradicated and to prevent antibiotic resistance.
Step-by-Step Process During Treatment
The specific steps you'll experience during treatment depend heavily on the cause of your teeth swelling. Here's a general overview of what to expect for common scenarios:
For a Dental Abscess (e.g., Periapical Abscess):
- Diagnosis: Your dentist will examine the area, inquire about your symptoms, and take X-rays to pinpoint the source of the infection.
- Pain Management & Initial Infection Control: If swelling is significant or accompanied by fever, an antibiotic prescription might be given. Local anesthesia will be administered to numb the area.
- Drainage (if applicable): If a visible pus pocket is present, the dentist may make a small incision to allow pus to drain. For a periapical abscess, drainage might occur through drilling into the tooth.
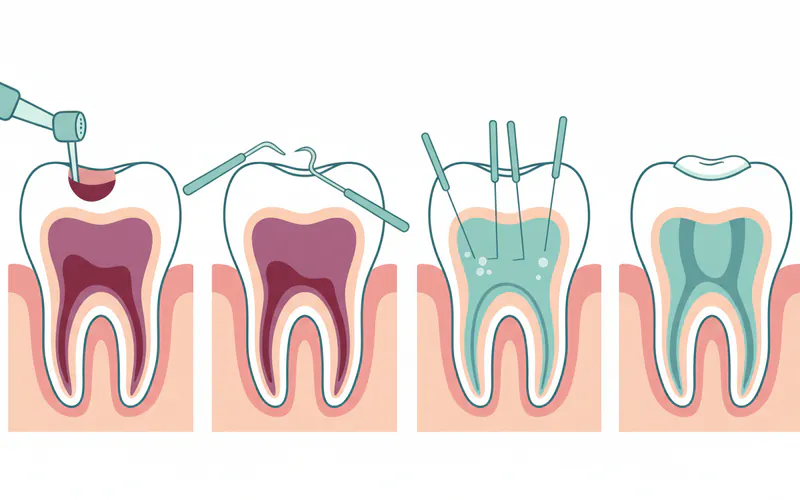
- Root Canal Treatment (if tooth is savable):
- Access: A small opening is made in the crown of the tooth.
- Cleaning: Infected pulp and bacteria are removed from the root canals using specialized instruments.
- Shaping & Disinfection: Canals are shaped and disinfected to remove any remaining bacteria.
- Filling: The cleaned canals are filled with a biocompatible material (gutta-percha) to prevent reinfection.
- Restoration: The opening in the tooth is sealed with a temporary or permanent filling. A dental crown is often recommended later to protect the treated tooth.
- Tooth Extraction (if tooth is not savable):
- Numbing: Local anesthesia is administered.
- Loosening: The tooth is gently loosened from its socket using instruments.
- Removal: The tooth is extracted.
- Post-Extraction Care: Gauze is placed to control bleeding, and post-operative instructions are provided.
For Periodontal Abscess/Gum Disease:
- Diagnosis: Examination, probing gum pockets, and X-rays to assess bone loss.
- Anesthesia: Local anesthetic may be used to numb the gums.
- Scaling and Root Planing: Using specialized instruments (ultrasonic and hand scalers), plaque and tartar are meticulously removed from above and below the gum line. The root surfaces are smoothed to remove bacterial toxins and prevent future buildup.
- Antibiotic Application (optional): In some cases, localized antibiotic gels or chips might be placed into deep pockets.
- Follow-up: Multiple appointments might be needed. Regular cleanings and maintenance are crucial afterward.
For Impacted Wisdom Tooth (Pericoronitis):
- Diagnosis: Examination and X-rays to assess the position of the wisdom tooth and the extent of infection.
- Infection Control: Antibiotics may be prescribed if the infection is severe or spreading.
- Cleaning: The area around the wisdom tooth is cleaned to remove trapped food and debris.
- Gum Flap Management: The dentist may irrigate the gum flap or, in some cases, trim it (opercolectomy).
- Extraction (definitive treatment): If the pericoronitis is recurrent or the tooth is poorly positioned, extraction of the wisdom tooth is often recommended. This is usually a surgical procedure.
Cost and Insurance
Understanding the financial aspect of treating teeth swelling is important, as costs can vary significantly based on the cause, complexity of treatment, location, and the dentist's fees.
Average US Costs (without insurance):
- Antibiotic Prescription: $10 - $50
- Simple Abscess Drainage: $50 - $200
- Dental Exam & X-rays (initial diagnosis): $75 - $250
- Root Canal Treatment:
- Front tooth: $700 - $1,200
- Premolar: $800 - $1,500
- Molar: $1,000 - $2,000
- Dental Crown (post-root canal): $800 - $2,500
- Tooth Extraction:
- Simple: $75 - $300
- Surgical (e.g., impacted wisdom tooth): $200 - $600 per tooth, can be up to $1,000+ if IV sedation is used.
- Scaling and Root Planing (Deep Cleaning): $150 - $400 per quadrant, so $600 - $1,600 for a full mouth.
- TMJ Splint/Nightguard: $300 - $800
Regional Variations:
Costs can be higher in major metropolitan areas (e.g., New York, Los Angeles) compared to rural areas or areas with a lower cost of living. For instance, a molar root canal in a large city might lean towards the $2,000 end, while in a smaller town, it might be closer to $1,200.
Insurance Coverage Details:
Most dental insurance plans in the US categorize procedures into preventive, basic, and major care, each with different coverage percentages.
- Preventive Care (e.g., exams, X-rays, routine cleanings): Often covered at 80-100%.
- Basic Restorative Care (e.g., fillings, simple extractions, root canal treatment): Typically covered at 70-80%.
- Major Restorative Care (e.g., crowns, bridges, dentures, surgical extractions): Usually covered at 50%. Periodontal surgery may also fall into this category.
- TMJ Treatment: Coverage varies widely. Some dental plans may cover occlusal splints, while others classify TMJ treatment as medical and may require billing through medical insurance, if covered at all.
Important Considerations:
- Deductibles: You'll typically need to pay an annual deductible (e.g., $50-$100) before your insurance starts paying.
- Annual Maximums: Most dental insurance plans have an annual maximum benefit (e.g., $1,000 - $2,000). Once you reach this limit, you pay 100% of subsequent costs for the year.
- Waiting Periods: Some plans have waiting periods (e.g., 6 months for basic, 12 months for major procedures) before certain benefits kick in.
- In-network vs. Out-of-network: You'll usually save money by choosing an in-network provider.
Cost-Saving Tips:
- Preventive Care: Regular check-ups and cleanings are the most effective way to prevent costly issues.
- Dental Discount Plans: These are not insurance but offer reduced fees at participating dentists for an annual membership fee.
- Dental Schools: University dental schools often provide treatment at a lower cost, performed by supervised students.
- Payment Plans/Financing: Many dental offices offer in-house payment plans or partner with third-party medical financing companies (e.g., CareCredit).
- Health Savings Accounts (HSAs) or Flexible Spending Accounts (FSAs): Use pre-tax dollars to pay for dental expenses.
Recovery and Aftercare
Proper recovery and aftercare are vital for healing, minimizing complications, and ensuring the success of your dental treatment. Instructions will vary based on the procedure.
General Aftercare Principles:
- Pain Management: Take prescribed or over-the-counter pain relievers (ibuprofen, acetaminophen) as directed.
- Swelling Reduction: Apply a cold compress or ice pack to the outside of your cheek (15-20 minutes on, 15-20 minutes off) for the first 24-48 hours.
- Oral Hygiene:
- Avoid the immediate area: For the first 24 hours, avoid brushing or flossing directly over the surgical site or extraction socket.
- Gentle Rinsing: After 24 hours, gentle warm saltwater rinses (1/2 teaspoon salt in 8 ounces warm water) 3-4 times a day can help keep the area clean and reduce swelling. Avoid vigorous rinsing, especially after extraction.
- Continue Brushing/Flossing: Maintain regular oral hygiene in other areas of your mouth.
- Diet: Stick to soft foods for a few days to a week. Avoid hot, spicy, crunchy, or chewy foods that could irritate the treated area or dislodge blood clots (after extraction).
- Activity: Avoid strenuous physical activity for 24-48 hours, as this can increase bleeding and swelling.
- Avoid Smoking/Alcohol: Both can significantly delay healing and increase the risk of complications.
Specific Recovery Notes:
- After Root Canal: You might experience some mild soreness for a few days. The tooth may be sensitive until a permanent crown is placed. Avoid chewing hard foods on the treated tooth until it's fully restored.
- After Extraction: Expect some bleeding for the first 24 hours. Bite firmly on the gauze. Avoid spitting, sucking through a straw, or smoking to prevent dry socket. Pain usually subsides within a few days, but full healing can take weeks.
- After Scaling and Root Planing: Gums may be sensitive, swollen, and bleed slightly for a few days. Use a soft-bristle toothbrush and continue good oral hygiene. Sensitivity to hot/cold may increase temporarily.
- After TMJ Treatment: Follow your dentist's specific instructions for splint wear and jaw exercises. Avoid clenching or grinding, and manage stress.
When to Contact Your Dentist During Recovery:
- Severe or worsening pain not relieved by medication.
- Persistent or increasing swelling beyond 2-3 days.
- Fever that develops or worsens.
- Pus discharge.
- Excessive bleeding.
- Difficulty breathing or swallowing.
- Any unexpected or concerning symptoms.
Prevention
Preventing teeth swelling largely revolves around maintaining excellent oral hygiene and addressing dental problems promptly. The American Dental Association (ADA) emphasizes these core preventive strategies:
1. Maintain Excellent Oral Hygiene:
- Brush Twice Daily: Use a soft-bristle toothbrush and fluoride toothpaste. Brush for at least two minutes, covering all surfaces of your teeth and gently brushing your gums.
- Floss Daily: Flossing removes plaque and food particles from between teeth and under the gum line, areas your toothbrush can't reach. This is crucial for preventing gum disease, a primary cause of swelling.
- Use Mouthwash: An antiseptic mouthwash can help reduce bacteria and inflammation, though it shouldn't replace brushing and flossing.
- Tongue Cleaning: Brush or scrape your tongue to remove bacteria that contribute to bad breath and can irritate gums.
2. Regular Dental Check-ups and Professional Cleanings:
- Every Six Months: Visit your dentist for routine examinations and professional cleanings. These appointments allow your dentist to detect early signs of decay, gum disease, or other issues before they become severe and lead to swelling.
- Early Intervention: Addressing small cavities with fillings prevents them from progressing to deep infections that cause abscesses and swelling. Professional cleanings remove hardened plaque (tartar) that home brushing cannot, preventing gum disease.
3. Balanced Diet and Hydration:
- Limit Sugary and Acidic Foods/Drinks: These contribute to tooth decay.
- Eat Nutrient-Rich Foods: A diet rich in fruits, vegetables, and whole grains supports overall health, including gum health.
- Stay Hydrated: Drinking plenty of water helps wash away food particles and maintains saliva flow, which naturally cleans teeth.
4. Protect Your Teeth:
- Mouthguards for Sports: If you play contact sports, wear a custom-fitted mouthguard to prevent dental trauma that could lead to fractured teeth or gum injuries.
- Nightguards for Grinding/Clenching: If you grind or clench your teeth (bruxism), a nightguard can protect your teeth from excessive wear and prevent strain on your TMJ, reducing the risk of related swelling.
5. Quit Smoking/Tobacco Use:
- Smoking significantly increases the risk and severity of gum disease, hinders healing, and compromises your immune response, making you more susceptible to infections that cause swelling.
6. Manage Systemic Health Conditions:
- Control diabetes, as uncontrolled blood sugar levels increase the risk of gum disease and infections.
- Discuss any medications that cause dry mouth or gum overgrowth with your physician and dentist.
Risks and Complications
While teeth swelling might seem like a localized problem, ignoring it or delaying treatment can lead to serious, even life-threatening, complications.
1. Spread of Infection (Cellulitis, Sepsis):
- Facial Cellulitis: An untreated dental abscess can spread from the tooth into the surrounding soft tissues of the face and neck, causing widespread inflammation and swelling. This can rapidly become dangerous.
- Ludwig's Angina: A severe and aggressive form of cellulitis that affects the floor of the mouth and neck. It can cause rapid swelling, obstructing the airway and leading to difficulty breathing and swallowing. This is a medical emergency requiring immediate hospitalization and intravenous antibiotics.
- Cavernous Sinus Thrombosis: In rare but grave cases, infection from an upper tooth can spread to the cavernous sinus, a large vein located behind the eyes in the brain. This can lead to blood clots, vision loss, stroke, and even death.
- Sepsis: If bacteria from an oral infection enter the bloodstream and spread throughout the body, it can trigger a systemic inflammatory response known as sepsis, a life-threatening condition.
2. Bone Loss and Tooth Loss:
- Periodontitis: Chronic gum inflammation can lead to irreversible damage to the bone and ligaments supporting your teeth, eventually causing tooth mobility and loss.
- Untreated Abscess: A long-standing periapical abscess can destroy significant amounts of jawbone around the tooth root.
3. Formation of Cysts:
- A chronic dental abscess can sometimes develop into a fluid-filled sac called a radicular cyst, which can grow and destroy surrounding bone if not removed.
4. Re-infection:
- If the source of the infection isn't fully removed (e.g., only antibiotics are used without definitive dental treatment), the infection and swelling are highly likely to recur.
5. Aesthetic and Functional Impairment:
- Chronic swelling, tooth loss, or extensive dental work can impact your appearance, ability to chew, and speech.

Comparison Table: Causes of Swelling vs. Potential Complications
| Cause of Swelling | Primary Symptoms | Definitive Treatment | Potential Risks/Complications (if untreated) |
|---|---|---|---|
| Dental Abscess (Periapical) | Localized pain, pus, sensitivity | Root Canal or Extraction | Facial cellulitis, Ludwig's Angina, sepsis, tooth loss |
| Periodontal Abscess | Gum swelling, pain, pus, bad taste | Drainage, Deep Cleaning (SRP) | Spread of infection, localized bone loss, tooth loss |
| Gingivitis/Periodontitis | Red, swollen, bleeding gums | Deep Cleaning (SRP), improved hygiene | Tooth loss, bone loss, increased systemic disease risk |
| Impacted Wisdom Tooth | Swelling, pain at back of jaw, trismus | Extraction, gum flap removal | Recurrent infection (pericoronitis), cyst formation |
| TMJ Disorder | Jaw pain, clicking, limited opening | Splint, PT, medication | Chronic pain, degenerative joint changes |
Comparison Table: Common Treatments vs. Cost & Recovery Time
| Treatment | Average Cost Range (US, w/o insurance) | Typical Recovery Time | Duration of Effect |
|---|---|---|---|
| Antibiotics (Oral) | $10 - $50 | Immediate symptom relief | Temporary (treats infection, not cause) |
| Abscess Drainage | $50 - $200 | 1-2 days (for initial relief) | Immediate (must be followed by definitive treatment) |
| Root Canal Treatment | $700 - $2,000 (per tooth) | 2-7 days of soreness | Lifelong (with proper care and crown) |
| Simple Tooth Extraction | $75 - $300 (per tooth) | 3-7 days of soreness | Permanent removal |
| Surgical Tooth Extraction | $200 - $1,000+ (per tooth) | 7-14 days of soreness/swelling | Permanent removal |
| Scaling & Root Planing (SRP) | $600 - $1,600 (full mouth) | 1-3 days of gum sensitivity | Ongoing (requires maintenance) |
| Occlusal Splint (TMJ) | $300 - $800 | Immediate comfort, long-term adjustment | As long as worn (months to years) |
Children / Pediatric Considerations
Children are also susceptible to teeth swelling, and in some cases, the causes and management differ from adults. Parents should be particularly vigilant.
Common Causes in Children:
- Teething: While not a "swelling" in the pathological sense, erupting baby teeth can cause localized gum inflammation, redness, and discomfort, sometimes with a small bulge. This is normal but can be mistaken for other issues.
- Dental Caries (Cavities): Baby teeth are highly vulnerable to decay, which can progress rapidly to infect the pulp, leading to dental abscesses and localized gum swelling, similar to adults. "Baby bottle tooth decay" is a common culprit.
- Trauma: Children are prone to falls and accidents. A blow to the mouth can injure a tooth, leading to discoloration, pain, and eventually infection and swelling. This is particularly concerning with developing permanent teeth.
- Eruption Cysts/Hematomas: Sometimes, a bluish or purplish swelling can appear over an erupting tooth, often a permanent molar. This is an eruption cyst or hematoma, usually harmless and resolves on its own as the tooth erupts, but it can be alarming.
- Abscesses: Similar to adults, periapical or periodontal abscesses can occur in children and require immediate dental attention.
Specific Considerations for Children:
- Rapid Progression: Infections in children can spread more quickly due to less dense bone structures.
- Developing Teeth: Treatment decisions (e.g., extraction vs. pulp therapy) must consider the presence of permanent tooth buds underneath baby teeth. Early loss of baby teeth can impact the alignment of permanent teeth.
- Cooperation: Children may be less cooperative during dental procedures, necessitating different approaches like sedation.
- Fever: Any swelling accompanied by fever in a child should be evaluated by a dentist or pediatrician promptly.
Prevention for Children:
- Early Oral Hygiene: Start cleaning your baby's gums even before teeth erupt. Brush with a tiny smear of fluoride toothpaste once teeth appear.
- Regular Dental Visits: The ADA recommends a child's first dental visit by age one or when the first tooth appears. Regular check-ups help identify and address issues early.
- Diet: Limit sugary snacks and drinks. Avoid putting babies to bed with bottles containing anything other than water.
- Mouthguards: For active children in sports.
Cost Breakdown (Recap and Details)
To reiterate and provide more granular detail, here's a cost breakdown often encountered for managing teeth swelling in the US.
Average US Costs (Out-of-Pocket, without Insurance)
- Initial Consultation/Emergency Exam: $75 - $250 (Includes exam and usually 1-2 X-rays)
- Prescription Antibiotics: $10 - $50 (Generic brands are cheaper)
- Pain Relievers (OTC): $5 - $20
Specific Procedure Costs:
| Procedure | Low End ($) | Mid Range ($) | High End ($) | Notes |
|---|---|---|---|---|
| Abscess Incision & Drainage | 50 | 125 | 200 | Simple, in-office procedure. |
| Simple Tooth Extraction | 75 | 175 | 300 | For visible, easily removed teeth. |
| Surgical Tooth Extraction | 200 | 400 | 600 | For impacted, fractured, or difficult-to-remove teeth. Price per tooth. |
| Wisdom Tooth Extraction (Impacted) | 250 | 450 | 700 | Per tooth. Can be higher if IV sedation ($500-$1000+) is used. |
| Root Canal (Front Tooth) | 700 | 950 | 1,200 | Less complex, fewer canals. |
| Root Canal (Premolar) | 800 | 1,150 | 1,500 | Moderately complex. |
| Root Canal (Molar) | 1,000 | 1,500 | 2,000 | Most complex, often multiple canals. |
| Dental Crown (after root canal) | 800 | 1,650 | 2,500 | Varies by material (porcelain-fused-to-metal, all-ceramic, gold). |
| Scaling & Root Planing (per quadrant) | 150 | 275 | 400 | Often requires 2-4 quadrants to be treated. |
| Occlusal Splint (Nightguard for TMJ) | 300 | 550 | 800 | Custom-fitted. |
With Insurance:
As mentioned, dental insurance typically covers a percentage of costs after your deductible is met, up to an annual maximum.
- Deductible: Usually $50 - $100 per year.
- Coverage:
- Preventive (Exams, X-rays): 80-100%
- Basic (Fillings, Simple Extractions, Root Canals): 70-80%
- Major (Crowns, Surgical Extractions, Periodontal Surgery): 50%
- Annual Maximum: Most plans cap benefits at $1,000 - $2,000 per year. This means if your treatment costs $3,000 and your maximum is $1,500, you'll pay at least $1,500 out-of-pocket (plus any deductible and co-insurance).
Payment Plans and Financing Options:
- In-Office Payment Plans: Many dental practices offer flexible payment schedules directly with the patient.
- Third-Party Financing: Companies like CareCredit or LendingClub provide healthcare credit cards or loans with various interest rates, often interest-free for an introductory period.
- Health Savings Accounts (HSAs) & Flexible Spending Accounts (FSAs): These tax-advantaged accounts allow you to set aside pre-tax money for eligible healthcare expenses, including dental care.
Cost-Saving Tips:
- Preventive Care: This is the most cost-effective "treatment." Regular cleanings and check-ups prevent expensive problems.
- Ask for Estimates: Always request a detailed cost estimate before beginning any major treatment.
- Compare Dentists: Get a second opinion and compare costs for complex procedures, especially for non-emergency situations.
- Dental Schools: As previously mentioned, a good option for lower-cost care.
Frequently Asked Questions
What should I do immediately if my tooth is swelling?
If your tooth is swelling, rinse your mouth gently with warm salt water (1/2 teaspoon salt in 8 ounces warm water) several times a day to reduce inflammation and cleanse the area. You can also apply a cold compress to the outside of your cheek for 15-20 minutes at a time to help reduce swelling. Take over-the-counter pain relievers like ibuprofen or acetaminophen if needed. Most importantly, contact your dentist immediately for an emergency appointment, as home remedies only provide temporary relief and don't address the underlying cause.
How to make gums stop swelling at home?
To temporarily alleviate gum swelling at home, gentle warm saltwater rinses are highly effective for reducing inflammation and keeping the area clean. You can also gently brush the swollen area with a soft-bristle toothbrush to remove irritants. Avoid very hot or cold foods, and refrain from irritating the area with your tongue or fingers. Remember, these are symptomatic treatments; seeing a dentist is essential to diagnose and treat the cause.
Can TMJ cause facial swelling and is it common?
Yes, TMJ disorders can cause facial swelling, particularly around the jaw joint itself (just in front of the ear) or in the surrounding jaw muscles. It's not as common as swelling from a dental infection, but it occurs due to inflammation of the joint or muscle spasms. The swelling often accompanies jaw pain, clicking, or difficulty opening your mouth. If you suspect TMJ, your dentist or an oral surgeon can provide a diagnosis and recommend appropriate treatment.
How long does dental swelling last after treatment?
The duration of swelling after treatment depends on the cause and the procedure. For a drained abscess, significant swelling reduction can occur within 24-48 hours. After a tooth extraction, swelling typically peaks at 2-3 days and then gradually subsides over 5-7 days. With root canal treatment, localized swelling might resolve within a day or two, though minor soreness could last longer. Always follow your dentist's post-operative instructions for optimal healing.
Can a swollen tooth heal on its own without a dentist?
No, a swollen tooth cannot heal on its own if the swelling is due to an infection or underlying issue. While symptoms might temporarily subside with home remedies or antibiotics, the source of the problem (e.g., infected pulp, deep periodontal pocket) remains. Without professional treatment, the infection will almost certainly return, often more severely, and can lead to serious complications like widespread infection or tooth loss.
What are the signs that teeth swelling is an emergency?
Teeth swelling becomes a dental emergency if it's accompanied by:
- Rapidly spreading facial swelling (especially if it impacts your eye or neck).
- Fever or chills.
- Difficulty breathing or swallowing.
- Severe, throbbing pain that isn't relieved by over-the-counter medication.
- Difficulty opening your mouth fully (trismus). These signs indicate a severe infection that could spread quickly and be life-threatening. Seek immediate dental or medical attention.
Does dental insurance cover the cost of treating teeth swelling?
Most dental insurance plans in the US will cover a portion of the costs for treating teeth swelling, as it's typically considered basic or major restorative care. Coverage usually ranges from 50% to 80% after you meet your annual deductible. However, plans often have annual maximums (typically $1,000-$2,000), and some may have waiting periods for major procedures. Always check with your insurance provider for specific details regarding your plan's coverage.
What's the difference between swelling from a gum infection and a tooth infection?
Swelling from a gum infection (periodontal) typically occurs within the gum tissue itself, often alongside generalized red, swollen, and bleeding gums. It might be localized to a specific pocket. Swelling from a tooth infection (periapical abscess) originates from the tooth's pulp and usually appears as a localized bump on the gum adjacent to the infected tooth, or the swelling can spread into the face around that tooth. Your dentist can differentiate between these with X-rays and examination.
Can allergies cause swelling around teeth?
Yes, allergic reactions can sometimes cause swelling around the teeth, gums, lips, or face. This is usually due to angioedema, a type of swelling beneath the skin's surface. It can be a reaction to certain foods, medications, or even dental materials. If you suspect an allergic reaction, especially if accompanied by hives or difficulty breathing, seek immediate medical attention.
What happens if I ignore teeth swelling?
Ignoring teeth swelling is extremely risky. Untreated dental infections can spread to other parts of your face, jaw, neck, or even into your bloodstream and brain. This can lead to severe complications like facial cellulitis, Ludwig's angina (a life-threatening airway obstruction), sepsis, or cavernous sinus thrombosis. You also risk irreversible bone loss, tooth loss, and chronic pain. Early intervention is critical to prevent these serious health issues.
When to See a Dentist
Recognizing when to seek professional dental care for teeth swelling is paramount to preventing minor issues from escalating into major health problems.
Immediate Dental Attention (Emergency - Call Your Dentist or Go to an Urgent Care/ER):
- Rapidly Spreading Swelling: If the swelling is increasing quickly, spreading to your eye, throat, or neck.
- Difficulty Breathing or Swallowing: This is a critical sign of a spreading infection that could compromise your airway.
- Fever or Chills: Systemic signs of a serious infection.
- Severe, Unbearable Pain: Pain that is intense, throbbing, and not relieved by over-the-counter pain medication.
- Difficulty Opening Your Mouth (Trismus): Often indicates a deep infection affecting jaw muscles.
- Facial Asymmetry: Noticeable distortion of your face due to swelling.
Prompt Dental Appointment (Within 24-48 Hours):
- Persistent Localized Swelling: If you have a noticeable bulge on your gum or around a tooth that doesn't subside with home remedies within a day.
- Pain Accompanied by Swelling: Even if not severe, persistent pain along with swelling indicates an issue that needs professional diagnosis.
- Pus Drainage: If you notice pus draining from the swollen area or a "pimple" on your gum.
- Swollen Lymph Nodes: Tender, enlarged lymph nodes under your jaw or in your neck, along with localized swelling.
- Swelling Around a Wisdom Tooth: Especially if accompanied by difficulty chewing or bad taste.
Routine Dental Appointment (Schedule at Your Earliest Convenience):
- Mild, Chronic Gum Swelling: If your gums are generally swollen, red, and bleed easily (signs of gingivitis). While not an emergency, addressing it promptly can prevent progression to periodontitis.
- Localized Swelling without Pain: Sometimes a cyst or a chronic, non-symptomatic issue can cause swelling. It still needs evaluation.
- Sensitivity to Hot/Cold: Even without obvious swelling, this could be an early sign of decay or an impending infection.
Ignoring any form of teeth swelling, especially if it's painful or accompanied by systemic symptoms, is a significant health risk. Your oral health is intrinsically linked to your overall well-being, and prompt professional care can make all the difference.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
How to Relieve Gum Swelling
When your gums are swollen, it can be an alarming and uncomfortable experience, often signaling an underlying issue that requires attention. Statistics from the Centers for Disease Control and Prevention (CDC) reveal that **nearly half of adults aged 30 or older in the United States have some form o
February 23, 2026
Submandibular Salivary Gland Swelling: Complete Guide
When you notice a peculiar lump or uncomfortable fullness beneath your jaw, it can be an alarming experience. This sensation, often accompanied by pain and difficulty swallowing, could indicate submandibular salivary gland swelling. Affecting an estimated 1 in 10,000 adults annually, conditi
February 23, 2026
What Helps With Gum Swelling
Gum swelling, medically known as gingival swelling or gingivitis, is a common yet often underestimated dental issue affecting millions of Americans. Have you ever woken up with sore, puffy gums that bleed easily when you brush? You're not alone. Research indicates that nearly **half of all a
February 23, 2026
How to Handle Knocked Out Tooth
A sudden impact, a sporting accident, or an unexpected fall – in a fraction of a second, your world can shift when you realize you've lost a tooth. A knocked out tooth, medically known as an avulsed tooth, is one of the most severe dental emergencies, and knowing **how to handle a knocked out to
February 23, 2026