What Helps With Gum Swelling
Key Takeaways
- Gum swelling, medically known as gingival swelling or gingivitis, is a common yet often underestimated dental issue affecting millions of Americans. Have you ever woken up with sore, puffy gums that bleed easily when you brush? You're not alone. Research indicates that nearly **half of all a
Gum swelling, medically known as gingival swelling or gingivitis, is a common yet often underestimated dental issue affecting millions of Americans. Have you ever woken up with sore, puffy gums that bleed easily when you brush? You're not alone. Research indicates that nearly half of all adults aged 30 and older in the United States suffer from some form of gum disease, often starting with gingivitis, the primary cause of gum swelling. This uncomfortable condition isn't just a minor annoyance; it’s a critical indicator of underlying oral health problems that, if left unaddressed, can lead to serious complications like periodontal disease, tooth loss, and even impact your overall systemic health. Understanding what helps with gum swelling is crucial for maintaining a healthy smile and preventing more severe dental emergencies. This comprehensive guide will explore the various causes, symptoms, and effective treatment options—from home remedies to professional interventions—as well as essential prevention strategies, cost considerations, and when it’s vital to seek immediate dental care.
Key Takeaways:
- Early Action is Key: Mild gum swelling, often caused by gingivitis, can typically be resolved with improved oral hygiene within 1-2 weeks; severe cases require professional intervention.
- Home Remedies Offer Relief: Saltwater rinses and cold compresses can provide temporary symptom relief but are not cures for underlying causes.
- Professional Cleaning is Foundational: A dental cleaning (prophylaxis) for gingivitis typically costs $75-$200 without insurance, while a more intensive scaling and root planing (deep cleaning) for periodontitis can range from $250-$800 per quadrant.
- Insurance Varies: Most dental insurance plans cover preventive care like cleanings at 80-100%, but more extensive treatments like scaling and root planing might be covered at 50-80% after deductibles.
- Don't Ignore Persistent Swelling: If gum swelling persists for more than a few days, is accompanied by severe pain, fever, pus, or difficulty eating, it indicates a potential dental emergency requiring immediate professional evaluation.
- Prevention is Paramount: Regular brushing, daily flossing, and routine dental check-ups (every 6 months) are the most effective ways to prevent gum swelling and maintain long-term oral health.
- Systemic Links: Gum swelling can sometimes be a symptom of underlying systemic health issues or medication side effects; always inform your dentist about your full medical history.
What It Is: Understanding Gum Swelling
Gum swelling, known medically as gingival inflammation or gingivitis, refers to the enlargement, puffiness, or bulging of the gum tissue (gingiva) around your teeth. It’s a clear sign that something isn't right with your oral health. Healthy gums are typically firm, pink, and fit snugly around your teeth, without bleeding easily. Swollen gums, in contrast, may appear redder or darker, feel tender or painful to the touch, and often bleed when brushed or flossed. This inflammation is the body's natural immune response to irritants, most commonly bacterial plaque buildup.
The Role of Gingiva
The gingiva plays a crucial role in protecting the roots of your teeth and the underlying bone structure. It forms a protective seal around each tooth. When this tissue becomes inflamed, its protective barrier can weaken, potentially allowing bacteria to penetrate deeper and cause more significant damage, leading to conditions like periodontitis.
Causes of Gum Swelling: Why It Happens
Gum swelling can stem from a variety of factors, ranging from common oral hygiene issues to more serious underlying health conditions. Understanding the root cause is the first step toward effective treatment.
1. Poor Oral Hygiene (Gingivitis)
The most prevalent cause of gum swelling is gingivitis, an early stage of gum disease. It develops when plaque—a sticky film of bacteria, food particles, and saliva—accumulates on teeth and along the gumline. If plaque isn't removed daily through brushing and flossing, it hardens into tartar (calculus), which irritates the gums, leading to inflammation, redness, tenderness, and bleeding.
2. Periodontitis
If gingivitis is left untreated, it can advance to periodontitis, a more severe form of gum disease. In periodontitis, the inflammation spreads below the gumline, causing the gums to pull away from the teeth, forming "pockets." These pockets become infected, and the infection can destroy the bone and tissue that support the teeth, potentially leading to tooth loss. Swelling in this stage is often more persistent and can be accompanied by pain, pus, and loose teeth.
3. Dental Abscess
A dental abscess is a localized collection of pus caused by a bacterial infection. There are two main types:
- Periapical abscess: Occurs at the tip of the tooth root due to an untreated cavity, trauma, or failed root canal, leading to infection within the tooth's pulp. The swelling might appear on the gum near the affected tooth, often resembling a pimple.
- Periodontal abscess: Forms in the gum tissue itself, usually as a complication of advanced periodontitis, when bacteria get trapped in a deep gum pocket. This can cause rapid, painful swelling of the gum tissue around the tooth. Both types are dental emergencies requiring prompt treatment.
4. Trauma or Injury
Physical trauma can cause localized gum swelling. This can result from:
- Aggressive or incorrect brushing/flossing techniques.
- Ill-fitting dental appliances like dentures, retainers, or partials.
- Biting down on hard food.
- Dental procedures like extractions or deep fillings.
- Accidental injury to the mouth.
5. Nutritional Deficiencies
While less common in developed countries, severe deficiencies in certain vitamins can contribute to gum health issues:
- Vitamin C (Scurvy): Can lead to swollen, bleeding gums, tooth mobility, and impaired wound healing.
- Vitamin B (Biotin, Niacin): Deficiencies can also affect oral tissues.
6. Hormonal Changes
Fluctuations in hormone levels can make gums more sensitive and prone to inflammation:
- Pregnancy Gingivitis: Increased hormone levels (estrogen and progesterone) during pregnancy increase blood flow to the gums, making them more susceptible to plaque irritation and swelling.
- Puberty: Hormonal surges can cause temporary gum inflammation.
- Menstruation: Some women experience minor gum sensitivity and swelling around their menstrual cycle.
- Menopause: Hormonal shifts can contribute to dry mouth and gum sensitivity.
7. Medications
Certain medications can have side effects that manifest as gum swelling or overgrowth (gingival hyperplasia/overgrowth):
- Phenytoin (Dilantin): An anti-seizure medication.
- Cyclosporine: An immunosuppressant.
- Calcium Channel Blockers (e.g., Nifedipine, Amlodipine): Used for heart conditions and high blood pressure. If you're on these medications and notice gum swelling, consult your dentist and physician. Do not stop medication without professional advice.
8. Allergic Reactions
Some individuals may experience an allergic reaction to ingredients in oral hygiene products like certain toothpastes, mouthwashes, or even dental materials (e.g., components of fillings or crowns), leading to localized gum swelling, redness, and irritation.
9. Systemic Diseases
Certain systemic health conditions can weaken the immune system or affect inflammatory responses, making individuals more prone to gum swelling:
- Diabetes: Poorly controlled blood sugar impairs the body's ability to fight infection, increasing susceptibility to gum disease.
- Crohn's Disease and other Inflammatory Bowel Diseases: Can sometimes manifest with oral lesions or gum inflammation.
- Leukemia: Gum swelling and bleeding can be an early sign of leukemia due to the abnormal proliferation of white blood cells.
- Autoimmune Diseases: Conditions like Sjögren's syndrome can lead to dry mouth, increasing susceptibility to gum issues.
10. Oral Infections (Viral/Fungal)
- Herpes Simplex Virus (Primary Herpetic Gingivostomatitis): Can cause widespread gum swelling, painful sores, and fever, especially in children.
- Fungal Infections (Candidiasis/Thrush): While usually appearing as white patches, severe cases can also cause underlying gum inflammation, particularly in immunocompromised individuals.
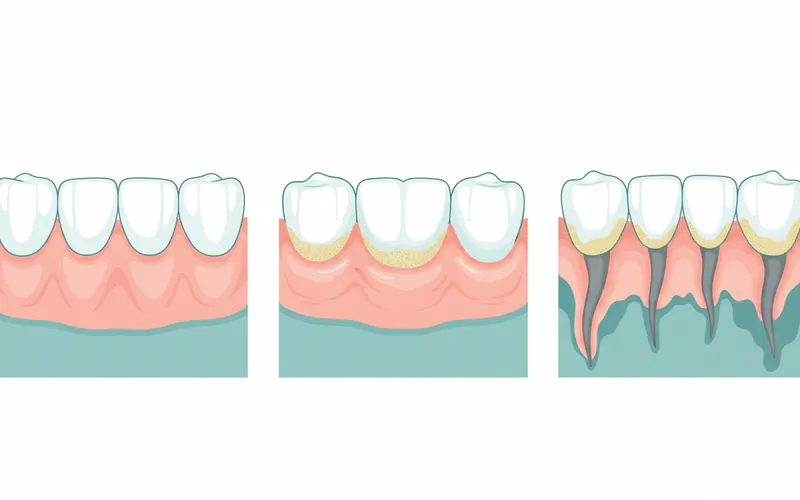
Signs and Symptoms of Gum Swelling
Recognizing the signs of gum swelling early can help you seek timely treatment. Look out for:
- Red or Darker Gums: Healthy gums are typically pink. Swollen gums often appear bright red, purplish-red, or even dark purple.
- Puffy, Bulbous, or Enlarged Gums: The gum tissue may look swollen and extend further over the teeth than usual.
- Tender or Painful Gums: The gums may feel sore or painful to the touch, or when chewing.
- Bleeding Gums: Gums that bleed easily during brushing, flossing, or even spontaneously are a hallmark sign of inflammation.
- Shiny Appearance: Inflamed gums can sometimes appear shiny due to the stretched tissue.
- Receding Gums: In more advanced cases (periodontitis), the gum tissue may pull away from the teeth, making the teeth appear longer.
- Bad Breath (Halitosis): Persistent bad breath or a bad taste in the mouth, often due to bacterial accumulation.
- Loose Teeth: A sign of advanced periodontitis, where the supporting bone and ligaments are compromised.
- Pus: Presence of pus draining from the gums, indicative of an infection or abscess.
- Fever or Facial Swelling: Especially with an abscess, you might experience systemic symptoms.
What Helps With Gum Swelling: Treatment Options
Treatment for gum swelling depends entirely on its underlying cause. It's crucial to get an accurate diagnosis from a dental professional.
Home Remedies (For Mild Inflammation & Symptom Relief)
These approaches can offer temporary relief for mild swelling, often associated with early gingivitis, but they are not substitutes for professional dental care.
-
Saltwater Rinses:
- How: Mix 1/2 teaspoon of salt in 8 ounces of warm water. Swish for 30 seconds, then spit. Repeat 2-3 times a day.
- Pros: Natural antiseptic, reduces inflammation, soothes irritated tissues, helps kill bacteria.
- Cons: Temporary relief, doesn't remove plaque/tartar, not effective for severe infections.
- Pro Tip: Use after meals and before bed for optimal cleansing.
-
Cold Compress:
- How: Apply an ice pack wrapped in a cloth to the outside of your cheek near the swollen area for 15-20 minutes, several times a day.
- Pros: Reduces swelling, numbs pain, constricts blood vessels.
- Cons: Only provides symptomatic relief, doesn't treat the cause.
- Pro Tip: Ideal for swelling caused by trauma or an acute inflammatory response.
-
Aloe Vera Gel:
- How: Apply pure aloe vera gel directly to the affected gums.
- Pros: Anti-inflammatory, antimicrobial properties, soothing.
- Cons: Efficacy varies, not a primary treatment for severe disease.
-
Turmeric Paste:
- How: Mix turmeric powder with a small amount of water to form a paste, then apply to the gums.
- Pros: Powerful anti-inflammatory and antiseptic properties due to curcumin.
- Cons: Can stain teeth temporarily, limited scientific evidence for direct gum application.
-
Oil Pulling:
- How: Swish a tablespoon of coconut, sesame, or sunflower oil in your mouth for 15-20 minutes, then spit it out.
- Pros: Anecdotal reports of reducing bacteria and inflammation.
- Cons: Lacks strong scientific backing for treating gum disease, time-consuming.
-
Improved Oral Hygiene:
- How: Gentle but thorough brushing twice a day with a soft-bristled brush, and daily flossing.
- Pros: Addresses the root cause (plaque) of gingivitis, highly effective for prevention and early stage treatment.
- Cons: Requires consistency and correct technique; may need professional guidance.
- Pro Tip: Consider an electric toothbrush for more effective plaque removal and less aggressive brushing.
Professional Dental Treatments
When home remedies aren't enough, or if the swelling is persistent, painful, or indicative of a more serious condition, professional dental intervention is necessary.
-
Professional Dental Cleaning (Prophylaxis):
- What: A routine cleaning performed by a dental hygienist or dentist to remove plaque and tartar from above and slightly below the gumline.
- When: Recommended for mild gingivitis and as preventive care.
- Pros: Removes the primary irritant (plaque/tartar), reverses early gum disease, prevents progression.
- Cons: Not sufficient for advanced periodontitis.
- Cost: ~$75 - $200 (without insurance).
-
Scaling and Root Planing (Deep Cleaning):
- What: A non-surgical procedure to remove plaque and tartar from deep gum pockets and smooth the tooth root surfaces to prevent bacterial reattachment. Often done with local anesthesia.
- When: For moderate periodontitis where gum pockets have formed.
- Pros: Halts the progression of gum disease, reduces pocket depth, helps gums reattach to teeth.
- Cons: Can cause temporary sensitivity, may require multiple appointments.
- Cost: ~$250 - $800 per quadrant (without insurance).
-
Antibiotics:
- What: Prescribed by the dentist to fight bacterial infections. Can be oral antibiotics (e.g., amoxicillin, metronidazole) or topical (e.g., antibiotic gels/chips placed directly into gum pockets).
- When: For severe gum infections, abscesses, or as an adjunct to deep cleaning.
- Pros: Directly targets infection-causing bacteria.
- Cons: Potential side effects (nausea, diarrhea), risk of antibiotic resistance with overuse.
-
Abscess Drainage:
- What: Incision and drainage of a dental abscess to release pus and relieve pressure. May be followed by root canal therapy or tooth extraction if the infection originates from the tooth.
- When: For acute dental or periodontal abscesses causing significant pain and swelling.
- Pros: Immediate pain relief, resolves infection.
- Cons: May require follow-up procedures.
- Cost: ~$150 - $400 for drainage; additional costs for root canal ($700-$2000) or extraction ($150-$500).
-
Laser Therapy:
- What: Lasers can be used as an adjunct to traditional scaling and root planing to remove inflamed tissue and kill bacteria in gum pockets.
- When: For treating gum disease, often in conjunction with other therapies.
- Pros: Minimally invasive, less bleeding, faster healing, sometimes less discomfort.
- Cons: More expensive, not always covered by insurance, long-term efficacy comparable to traditional methods is debated.
- Cost: Can add $200-$500 per quadrant to deep cleaning costs.
-
Gingivectomy/Gingivoplasty (Surgical Intervention):
- What: Surgical removal of excess gum tissue (gingivectomy) or reshaping of the gums (gingivoplasty). This might be necessary for severe gingival overgrowth (e.g., drug-induced) or to reduce deep gum pockets.
- When: For advanced periodontitis not responding to non-surgical treatments, or significant gingival enlargement.
- Pros: Reduces pocket depth, improves gum contour, allows for better oral hygiene access.
- Cons: Invasive, requires healing time, potential for discomfort.
- Cost: ~$200 - $600 per tooth or ~$1,000 - $3,000 per quadrant.
-
Treatment of Underlying Conditions:
- What: If gum swelling is due to a systemic disease (e.g., diabetes) or medication side effect, managing the underlying condition or adjusting medication (under a physician's guidance) is crucial.
- When: When a systemic link is identified.
- Pros: Addresses the root systemic cause.
- Cons: Requires collaboration between dental and medical professionals.
Comparison of Common Treatments
| Treatment Type | Primary Use Case | Typical Cost Range (US, without insurance) | Time to Relief / Resolution | Pros | Cons |
|---|---|---|---|---|---|
| Home Remedies | Mild gingivitis, temporary symptom relief | $5 - $20 (ingredients) | Hours to Days | Accessible, inexpensive, soothing | Doesn't treat underlying cause, limited efficacy for severe issues |
| Professional Cleaning | Mild gingivitis, preventive care | $75 - $200 | Days to 1-2 Weeks | Removes plaque/tartar, reverses early gum disease | Not for deep pockets, requires regular appointments |
| Scaling & Root Planing | Moderate periodontitis, deep pockets | $250 - $800 per quadrant | Weeks to Months | Stops disease progression, reduces pocket depth | Can cause sensitivity, requires multiple visits, invasive |
| Antibiotics (Oral/Topical) | Acute infections, adjunct to deep cleaning | $20 - $100 (medication) | Days to Weeks | Targets bacterial infection | Side effects, risk of resistance |
| Abscess Drainage | Acute dental abscess with pus | $150 - $400 (drainage only) | Immediate relief (pain) | Rapidly relieves pain and swelling, resolves infection | May require further treatment (root canal, extraction) |
| Gingivectomy | Severe gingival overgrowth, deep pockets (surgical) | $200 - $600 per tooth, $1k-$3k per quad | Weeks (healing) | Reduces pockets, improves gum contour, enhances hygiene | Invasive, discomfort, longer healing time, aesthetic changes |
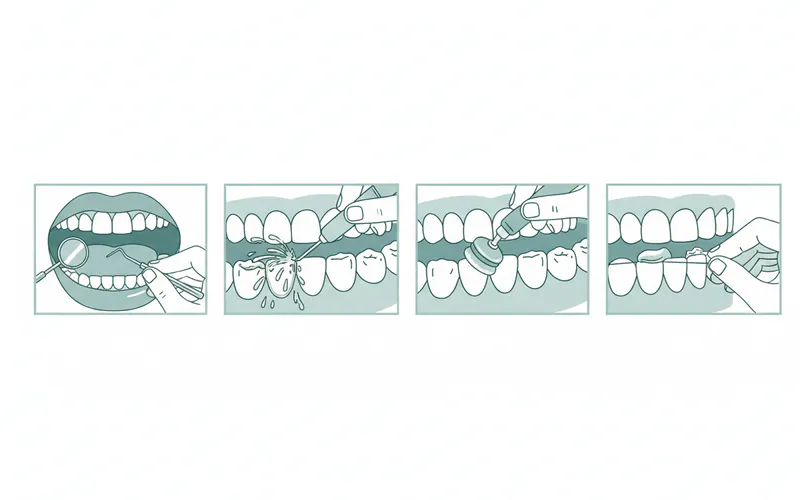
Step-by-Step Process: What to Expect During Treatment
Let's detail the process for a common and highly effective treatment for gum swelling caused by gingivitis or early periodontitis: Scaling and Root Planing (Deep Cleaning).
-
Initial Consultation and Diagnosis:
- Your dentist or periodontist will examine your gums, assess for signs of inflammation, bleeding, and gum recession.
- They will use a periodontal probe to measure the depth of the gum pockets around your teeth. Pockets deeper than 3mm often indicate gum disease.
- X-rays may be taken to check for bone loss around the tooth roots, a sign of periodontitis.
- A personalized treatment plan will be discussed, explaining why scaling and root planing is recommended.
-
Anesthesia:
- Before starting, a local anesthetic will be applied to numb the specific area (a quadrant of your mouth) that will be treated. This ensures you are comfortable throughout the procedure.
-
Scaling:
- Using specialized hand instruments (scalers) and/or an ultrasonic device (which uses high-frequency vibrations and water spray), the dental hygienist or dentist will meticulously remove plaque and tartar deposits from both above and below the gumline.
- This includes cleaning the surfaces of the teeth down into the gum pockets.
-
Root Planing:
- After scaling, the root surfaces of the teeth are planed (smoothed). This removes any remaining calculus, bacterial toxins, and rough spots, making it more difficult for plaque to reattach and promoting gum reattachment to the tooth root.
-
Irrigation (Optional):
- Sometimes, an antimicrobial rinse or irrigation with medicated solutions may be used to flush out bacteria from the pockets.
-
Medication Placement (Optional):
- In some cases, your dentist might place a local antimicrobial gel or antibiotic chip directly into deep gum pockets to deliver medication slowly over time and further reduce bacteria.
-
Post-Procedure Instructions:
- You'll receive detailed instructions on aftercare, including what to expect (e.g., sensitivity), pain management, and oral hygiene practices.
-
Follow-up Appointment:
- A follow-up appointment, usually 4-6 weeks later, is crucial to evaluate healing, re-measure pocket depths, and determine if additional treatment or maintenance is needed. Regular periodontal maintenance cleanings (often every 3-4 months) are usually recommended after deep cleaning to prevent recurrence.
Cost and Insurance: US Price Ranges
Understanding the financial aspect of gum swelling treatment is important for planning your care. Costs can vary significantly based on the severity of the condition, the type of treatment, your location, and whether you have dental insurance.
Average US Costs (Without Insurance)
- Routine Dental Cleaning (Prophylaxis): Typically ranges from $75 to $200. This is for preventive care and mild gingivitis.
- Scaling and Root Planing (Deep Cleaning): This is a more involved procedure. Costs are usually quoted per quadrant (one-fourth of your mouth).
- Per Quadrant: Expect to pay anywhere from $250 to $800 per quadrant. Many patients require 2-4 quadrants to be treated, so a full mouth deep cleaning could range from $1,000 to $3,200.
- Dental Abscess Drainage: Can cost $150 to $400, not including subsequent treatments like root canals or extractions.
- Root Canal Therapy: Varies by tooth (front vs. back) and complexity.
- Front tooth: $700 to $1,200
- Molar: $1,000 to $2,000+
- Tooth Extraction:
- Simple extraction: $150 to $400
- Surgical extraction (impacted or complex): $300 to $600+
- Gingivectomy/Gingivoplasty:
- Per tooth: $200 to $600
- Per quadrant: $1,000 to $3,000
- Prescription Antibiotics: Generally $20 to $100 depending on the specific drug and dosage.
Regional Variations: Costs can be higher in metropolitan areas and on the coasts (e.g., New York, California) compared to rural areas or the Midwest.
Insurance Coverage Details
Dental insurance can significantly reduce out-of-pocket costs, but coverage levels vary widely:
- Preventive Care (Routine Cleanings, X-rays, Exams): Most plans, especially PPO (Preferred Provider Organization) plans, cover preventive services at 80% to 100%. This is why regular check-ups are so important.
- Basic Procedures (Fillings, Simple Extractions, Scaling & Root Planing): Often covered at 50% to 80% after you've met your deductible. Scaling and root planing usually falls into this category. Be aware of waiting periods for these services, which can be 3-6 months after enrollment.
- Major Procedures (Crowns, Bridges, Dentures, Oral Surgery, Gingivectomy): Typically covered at 20% to 50%, often with higher deductibles and annual maximums.
- HMO (Health Maintenance Organization) Plans: May require you to see an in-network dentist and often have lower monthly premiums but limited choices of providers.
- Medicaid and CHIP: Coverage for adults varies by state, but children’s dental care is often comprehensively covered.
- Deductibles: The amount you must pay out-of-pocket before your insurance begins to cover costs.
- Annual Maximums: The maximum amount your insurance plan will pay for your dental care in a policy year (often $1,000 to $2,000).
Pro Tip: Always contact your dental insurance provider directly or consult your benefits handbook to understand your specific coverage before starting treatment. Ask for a pre-treatment estimate from your dentist's office.
Recovery and Aftercare
After professional treatment for gum swelling, proper recovery and aftercare are crucial to ensure healing and prevent recurrence.
- Oral Hygiene:
- Gentle Brushing: Continue brushing twice daily with a soft-bristled toothbrush. Be gentle around treated areas, especially after deep cleaning or surgery.
- Daily Flossing: Resume flossing as soon as comfortable. If advised, use special interdental brushes or water flossers, particularly around healing gum pockets.
- Antimicrobial Mouthwash: Your dentist might prescribe an antimicrobial mouthwash (e.g., chlorhexidine gluconate) for a specific period to reduce bacteria. Use as directed.
- Dietary Adjustments:
- For a few days after deep cleaning or surgery, stick to soft foods (yogurt, mashed potatoes, soup, scrambled eggs) to avoid irritating tender gums.
- Avoid extremely hot, cold, spicy, or acidic foods.
- Chew on the opposite side of your mouth if one area was treated.
- Pain and Sensitivity Management:
- It's normal to experience some sensitivity to hot and cold, and mild discomfort, especially after deep cleaning. This usually subsides within a few days to a week.
- Over-the-counter pain relievers like ibuprofen (Advil) or acetaminophen (Tylenol) can help manage discomfort.
- Desensitizing toothpastes can help with prolonged sensitivity.
- Smoking and Alcohol: Avoid smoking and alcohol consumption, as they can significantly delay healing and worsen gum health.
- Follow-Up Appointments: Adhere strictly to your dentist's recommendations for follow-up appointments, which are vital for monitoring healing and planning ongoing periodontal maintenance. For many with a history of gum disease, routine cleanings every 3-4 months are recommended instead of the standard 6 months.
Prevention: How to Keep Your Gums Healthy
Preventing gum swelling largely boils down to consistent, effective oral hygiene and a healthy lifestyle.
- Brush Twice Daily: Use a soft-bristled toothbrush and fluoride toothpaste. Brush for at least two minutes, gently cleaning all tooth surfaces and along the gumline. Replace your toothbrush every 3-4 months, or sooner if the bristles are frayed.
- Floss Daily: Flossing removes plaque and food particles from between your teeth and under the gumline, areas your toothbrush can't reach. This is non-negotiable for gum health.
- Regular Dental Check-ups and Cleanings: Visit your dentist every six months, or more frequently if recommended due to gum disease risk factors. Professional cleanings remove plaque and tartar buildup that you can't remove at home.
- ADA Guidelines: The American Dental Association (ADA) strongly recommends professional cleanings and examinations at least once a year, and ideally twice a year, for optimal oral health.
- Balanced Diet: Eat a diet rich in fruits, vegetables, and whole grains. Limit sugary snacks and drinks, which contribute to plaque formation. Ensure adequate intake of vitamins, especially Vitamin C (for gum tissue health) and calcium (for bone strength).
- Stay Hydrated: Drinking plenty of water helps rinse away food particles and bacteria, and promotes saliva production, which naturally cleanses the mouth.
- Avoid Tobacco Products: Smoking and chewing tobacco are major risk factors for gum disease, impairing blood flow to the gums and hindering healing. Quitting is one of the best things you can do for your oral and overall health.
- Manage Stress: Chronic stress can weaken the immune system, potentially making you more susceptible to infections, including gum disease.
- Address Systemic Health Conditions: If you have conditions like diabetes, ensure they are well-managed, as they directly impact oral health.
- Be Aware of Medications: If you're starting a new medication, ask your doctor or dentist if it has any oral side effects like dry mouth or gum overgrowth, so you can monitor and address them early.
Risks and Complications of Untreated Gum Swelling
Ignoring persistent gum swelling can lead to a cascade of increasingly severe problems, impacting both your oral and general health.
- Progression to Periodontitis: The most direct and common complication. Untreated gingivitis will almost certainly advance to periodontitis, characterized by deep gum pockets, bone loss, and eventually loose teeth.
- Tooth Loss: As periodontitis progresses, the bone and supporting structures around your teeth are destroyed, leading to tooth mobility and ultimately tooth extraction or spontaneous loss.
- Dental Abscesses: Untreated infections in gum pockets can lead to painful periodontal abscesses, or infections from severe tooth decay can cause periapical abscesses, both requiring urgent treatment.
- Increased Risk of Systemic Diseases: The chronic inflammation and bacteria associated with advanced gum disease can enter your bloodstream, contributing to or exacerbating various systemic health issues:
- Heart Disease: Increased risk of heart attack and stroke.
- Diabetes Complications: Worsened blood sugar control, and diabetes itself makes gum disease worse.
- Respiratory Diseases: Inhalation of oral bacteria can lead to pneumonia or bronchitis.
- Pregnancy Complications: Increased risk of premature birth and low birth weight in pregnant women.
- Other Conditions: Links to certain cancers, rheumatoid arthritis, and Alzheimer's disease are being researched.
- Pain and Discomfort: Chronic pain, tenderness, and bleeding gums significantly impact quality of life, making eating and speaking uncomfortable.
- Halitosis (Chronic Bad Breath): Persistent bad breath can be a significant social and psychological burden.
- Impact on Overall Well-being: The cumulative effect of these complications can severely diminish your quality of life, self-confidence, and ability to eat and speak normally.
Children / Pediatric Considerations
Gum swelling in children can be concerning for parents. While many causes overlap with adults, some are unique or present differently in pediatric patients.
- Teething: This is the most common cause of temporary gum swelling, redness, and discomfort in infants and toddlers. Gums may appear swollen and tender as teeth erupt.
- Relief: Cold teething rings, gentle gum massage, and infant-safe pain relievers (like acetaminophen or ibuprofen, if age-appropriate) can help.
- Poor Oral Hygiene (Gingivitis): Children can develop gingivitis if brushing and flossing are neglected. Teach proper techniques early and supervise young children.
- Primary Herpetic Gingivostomatitis: This is a common viral infection in young children, caused by the Herpes Simplex Virus. It causes widespread, painful gum swelling, ulcers throughout the mouth, fever, and difficulty eating and drinking. It's often mistaken for severe teething.
- Treatment: Supportive care, pain relief, and hydration are key. Antiviral medications may be prescribed in severe cases.
- Eruption Cysts: Sometimes, a fluid-filled sac (cyst) can form over an erupting tooth, causing a bluish-purple swelling. These usually resolve on their own when the tooth comes through.
- Trauma: Children are prone to falls and bumps, which can injure the gums and teeth, leading to swelling.
- Nutritional Deficiencies: In rare cases, severe vitamin deficiencies can affect children's gum health.
- Orthodontic Appliances: Braces and retainers can sometimes irritate the gums, leading to localized inflammation. Proper cleaning around appliances is essential.
- Dental Abscess: Untreated cavities in baby teeth can lead to dental abscesses, causing localized gum swelling. These require immediate dental attention to prevent spread of infection.
Pro Tip for Parents: If your child has gum swelling that is persistent, accompanied by fever, severe pain, difficulty eating, or if you see pus, contact a pediatric dentist immediately. Regular dental check-ups for children starting by age one are essential for early detection and prevention of oral health issues.
Cost Breakdown
To further clarify the financial implications, let's look at average US costs for key treatments, considering insurance.
Typical Cost Scenarios (US, Average Ranges)
| Procedure | Average Cost (Without Insurance) | Average Cost (With Insurance, 50-80% coverage after deductible) |
|---|---|---|
| Routine Cleaning (Prophylaxis) | $75 - $200 | $0 - $40 (often 80-100% covered) |
| Scaling & Root Planing (per quadrant) | $250 - $800 | $50 - $400 (20-50% remaining after insurance) |
| Full Mouth Scaling & Root Planing (4 quadrants) | $1,000 - $3,200 | $200 - $1,600 (depending on coverage & annual max) |
| Dental Abscess Drainage | $150 - $400 | $30 - $200 (depends on if it's considered oral surgery) |
| Root Canal (Molar) | $1,000 - $2,000+ | $500 - $1,500 (after 50% coverage) |
| Simple Tooth Extraction | $150 - $400 | $30 - $200 (after 80% coverage) |
| Gingivectomy (per tooth) | $200 - $600 | $100 - $400 (after 50% coverage) |
| Prescription Antibiotics | $20 - $100 | $0 - $50 (depends on prescription drug plan) |
Payment Plans and Financing Options
Even with insurance, out-of-pocket costs can be substantial. Many dental practices offer or accept:
- In-house Payment Plans: Installment plans arranged directly with the dental office.
- Third-Party Financing (e.g., CareCredit, LendingClub): Healthcare credit cards or loans that offer deferred interest or low-interest payment plans for medical and dental expenses.
- Dental Discount Plans: Not insurance, but a membership program where you pay an annual fee and get reduced prices on dental services from participating dentists.
- Health Savings Accounts (HSAs) or Flexible Spending Accounts (FSAs): If you have an HSA or FSA through your employer, you can use pre-tax dollars to pay for dental treatment.

Cost-Saving Tips
- Prevention is the Best Investment: Regular cleanings and good home care cost far less than treating advanced gum disease.
- Compare Dentists: Get quotes from a few different dental offices, especially for major procedures.
- Utilize Dental Schools: Dental schools often offer treatments at reduced rates, performed by supervised students.
- Seek Community Clinics: Some community health centers offer sliding-scale fees based on income.
- Negotiate: Don't be afraid to discuss payment options or potential discounts with your dentist's office, especially if paying in cash.
Frequently Asked Questions
What helps bring down gum swelling fast?
For fast relief of mild gum swelling, a warm saltwater rinse (1/2 tsp salt in 8 oz warm water, swish 30 seconds) and a cold compress applied to the outside of your cheek can help reduce inflammation and pain temporarily. However, these are symptomatic treatments; for lasting relief, addressing the underlying cause with proper oral hygiene or professional dental care is essential.
Can gum swelling go away on its own?
Mild gum swelling caused by temporary irritation or very early gingivitis can sometimes resolve with diligent and immediate improvement in oral hygiene (brushing and flossing twice daily). However, swelling that persists for more than a few days, or is accompanied by pain, bleeding, or pus, indicates an underlying issue that will not go away on its own and requires professional dental attention.
How much does it cost to treat swollen gums?
The cost to treat swollen gums varies significantly based on the cause and severity. A routine dental cleaning for gingivitis typically costs $75-$200 without insurance. If you need a deep cleaning (scaling and root planing) for periodontitis, it can range from $250-$800 per quadrant. For a dental abscess, drainage might be $150-$400, plus the cost of further treatment like a root canal ($700-$2000).
Is gum swelling painful?
Gum swelling can range from mildly tender and uncomfortable to severely painful, depending on the cause. Gingivitis usually causes tenderness and bleeding. A dental abscess, however, typically causes intense, throbbing pain, often accompanied by facial swelling and fever, due to the pressure from accumulated pus.
What home remedies are effective for gum swelling?
Effective home remedies for temporary relief include warm saltwater rinses, applying a cold compress to the outside of the cheek, and gently brushing and flossing. Some people find relief with natural anti-inflammatories like aloe vera gel or turmeric paste applied to the gums. These remedies should complement, not replace, professional dental care.
Can antibiotics cure swollen gums?
Antibiotics can help treat gum swelling that is caused by a bacterial infection, such as a dental abscess or severe gum disease. They kill the infection-causing bacteria. However, antibiotics alone are often not a complete cure; they typically need to be combined with mechanical removal of plaque and tartar (like deep cleaning) for long-term resolution and prevention of recurrence.
What are the alternatives to professional dental treatment for severe gum swelling?
For severe gum swelling caused by advanced gum disease, an abscess, or other serious conditions, there are no effective alternatives to professional dental treatment. Home remedies provide only temporary symptomatic relief and cannot address deep infections, extensive plaque/tartar buildup, or bone loss. Delaying professional treatment can lead to tooth loss and systemic health complications.
How long does it take for gum swelling to go down after treatment?
After professional treatment like a deep cleaning (scaling and root planing), mild gum swelling and sensitivity typically start to subside within a few days to a week. Complete healing and reduction of inflammation can take several weeks to a few months, depending on the initial severity and how diligently you follow aftercare instructions. Abscess drainage can provide immediate pain relief, with swelling reducing over several days.
Can gum swelling be a sign of something serious?
Yes, gum swelling can be a sign of serious underlying conditions. While often indicating gingivitis, persistent or severe swelling, especially with intense pain, pus, fever, or facial swelling, could point to a severe dental abscess, advanced periodontitis, or even systemic diseases like leukemia or diabetes complications. These situations warrant immediate dental and potentially medical evaluation.
Is it safe to brush and floss with swollen gums?
Yes, it is generally safe and crucial to brush and floss gently even with swollen gums, especially if the swelling is due to gingivitis. Gentle brushing with a soft-bristled toothbrush and daily flossing helps remove the plaque that causes inflammation. If brushing causes significant pain or excessive bleeding, or if you suspect an abscess, consult your dentist for advice on appropriate cleaning methods.
When to See a Dentist
While minor gum irritation might resolve with improved home care, certain signs indicate that you need to see a dentist promptly, or even seek emergency care.
Schedule a Dental Appointment If You Experience:
- Persistent Swelling: Gum swelling that lasts for more than a few days despite diligent home care.
- Chronic Bleeding: Gums that bleed consistently during brushing or flossing, or spontaneously.
- Tenderness or Pain: Ongoing discomfort or pain in your gums.
- Receding Gums: Gums pulling away from your teeth, making teeth appear longer.
- Bad Breath: Persistent bad breath that doesn't improve with brushing.
- Shiny or Red Gums: Gums that have changed in color or appearance.
- Loose Teeth: Any noticeable movement or looseness of your teeth.
Seek Immediate Dental Attention (Dental Emergency) If You Experience:
- Severe Pain: Intense, throbbing pain that interferes with daily activities or sleep.
- Pus Drainage: The presence of pus around your teeth or gums, often forming a "pimple" on the gum. This indicates an active infection (abscess).
- Facial Swelling: Swelling that extends beyond the gums to your cheek, jaw, or neck. This can indicate a spreading infection that requires urgent treatment.
- Fever or Chills: Systemic signs of infection accompanying gum swelling.
- Difficulty Swallowing or Breathing: This is a critical sign that a severe infection in your mouth or jaw is spreading and could be life-threatening. Go to the nearest emergency room if you cannot get immediate dental care.
Remember, early detection and treatment are paramount for effective resolution of gum swelling and the prevention of more serious oral and systemic health complications. Don't hesitate to contact your dental professional at SmilePedia.net if you have any concerns about your gum health.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
How to Relieve Gum Swelling
When your gums are swollen, it can be an alarming and uncomfortable experience, often signaling an underlying issue that requires attention. Statistics from the Centers for Disease Control and Prevention (CDC) reveal that **nearly half of adults aged 30 or older in the United States have some form o
February 23, 2026
Teeth Swelling: Complete Guide
When you experience teeth swelling, it's more than just a minor discomfort; it's a clear signal from your body that something is amiss within your oral cavity, often indicating an underlying infection or inflammation that requires prompt attention. A recent survey revealed that **over 25% of adu
February 23, 2026
Submandibular Salivary Gland Swelling: Complete Guide
When you notice a peculiar lump or uncomfortable fullness beneath your jaw, it can be an alarming experience. This sensation, often accompanied by pain and difficulty swallowing, could indicate submandibular salivary gland swelling. Affecting an estimated 1 in 10,000 adults annually, conditi
February 23, 2026
How to Handle Knocked Out Tooth
A sudden impact, a sporting accident, or an unexpected fall – in a fraction of a second, your world can shift when you realize you've lost a tooth. A knocked out tooth, medically known as an avulsed tooth, is one of the most severe dental emergencies, and knowing **how to handle a knocked out to
February 23, 2026