Submandibular Salivary Gland Swelling: Complete Guide
Key Takeaways
- When you notice a peculiar lump or uncomfortable fullness beneath your jaw, it can be an alarming experience. This sensation, often accompanied by pain and difficulty swallowing, could indicate submandibular salivary gland swelling. Affecting an estimated 1 in 10,000 adults annually, conditi
When you notice a peculiar lump or uncomfortable fullness beneath your jaw, it can be an alarming experience. This sensation, often accompanied by pain and difficulty swallowing, could indicate submandibular salivary gland swelling. Affecting an estimated 1 in 10,000 adults annually, conditions related to salivary glands are more common than many realize and can range from minor irritations to serious medical emergencies. Understanding the cause and knowing when to seek professional help is crucial for your oral and overall health. Left untreated, such swelling can lead to persistent discomfort, infection, and even systemic health issues. This comprehensive guide from SmilePedia.net aims to demystify submandibular salivary gland swelling, providing you with in-depth information on its causes, symptoms, diagnosis, treatment options, and crucial preventive measures. We'll explore everything from the subtle signs to look out for, what to expect during a dental or medical consultation, and how to manage recovery, ensuring you have all the knowledge needed to safeguard your well-being.
Key Takeaways:
- Submandibular salivary gland swelling commonly results from blockages (stones), infections (sialadenitis), or underlying systemic conditions.
- Prompt diagnosis by a dental professional or physician is essential to prevent complications and determine appropriate treatment.
- Treatment options range from conservative measures like hydration and massage to medication (antibiotics) and, in some cases, surgical intervention (sialendoscopy, stone removal, gland removal).
- Cost of treatment can vary widely, from $100-$500 for conservative management to $2,000-$10,000+ for surgical procedures, with insurance typically covering a portion.
- Recovery timelines depend on the cause and treatment, from a few days for minor infections to several weeks post-surgery.
- Prevention focuses on excellent oral hygiene, adequate hydration, and addressing underlying systemic health issues.
- Seek immediate dental or medical attention if swelling is accompanied by fever, severe pain, difficulty breathing or swallowing, or rapidly worsening symptoms.
What It Is / Overview
The submandibular salivary glands are two of the three major pairs of salivary glands in your mouth, alongside the parotid and sublingual glands. Located beneath the floor of your mouth, just inside the lower jawbone (mandible), these glands produce approximately 60-65% of your saliva. Saliva is vital for digestion, lubricating the mouth, protecting teeth against decay, and washing away food particles and bacteria.
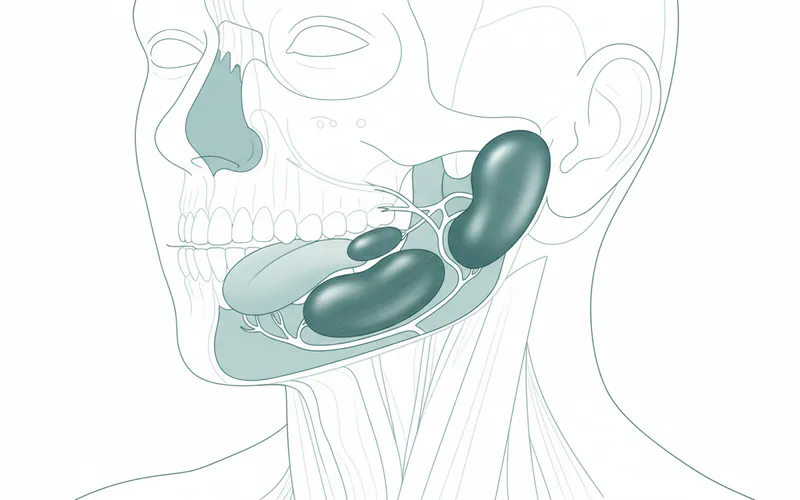
Submandibular salivary gland swelling refers to an enlargement or inflammation of one or both of these glands. This swelling can manifest as a noticeable lump under the jaw or chin, often accompanied by pain, tenderness, and sometimes changes in saliva production. It is a sign that something is interfering with the normal function of the gland, preventing saliva from flowing freely into the mouth through its duct, called Wharton's duct. While often benign, such swelling warrants professional evaluation to rule out more serious conditions and ensure proper treatment.
Types / Variations
Submandibular salivary gland swelling can arise from several distinct conditions, each with its own characteristics and implications. Understanding these variations is key to accurate diagnosis and effective treatment.
Sialolithiasis (Salivary Gland Stones)
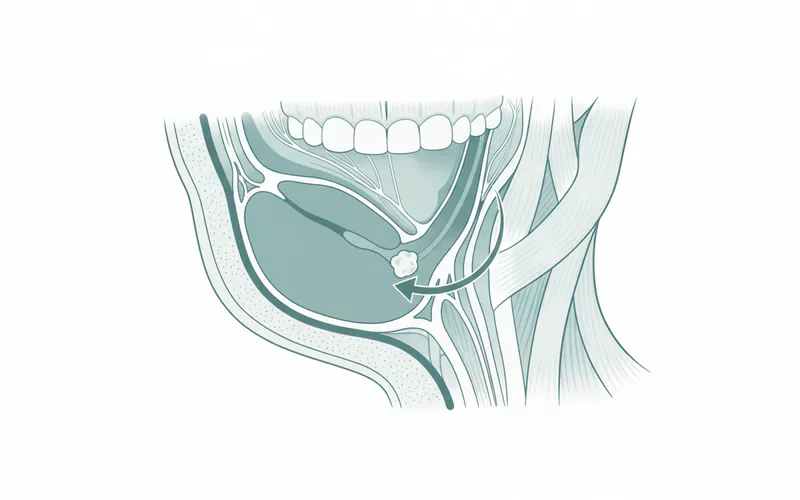
Sialolithiasis is the most common cause of submandibular gland swelling. These stones, known as sialoliths, are calcified masses that form within the salivary gland or its ducts. They are composed primarily of calcium phosphate and carbonate. Submandibular glands are particularly prone to stone formation due to their longer, more tortuous duct (Wharton's duct), the thicker, more mucinous nature of their saliva, and its higher calcium content.
- Characteristics: Often causes intermittent swelling and pain, especially during or after meals when saliva production increases, attempting to push past the obstruction. The swelling might subside between meals, only to recur.
- Prevalence: Affects approximately 1.2% of the general population.
Sialadenitis (Gland Infection)
Sialadenitis is an infection of the salivary gland, most commonly bacterial. It can occur secondary to a blockage (like a stone), which creates a stagnant environment conducive to bacterial growth, or it can be a primary infection. Dehydration, poor oral hygiene, and certain chronic illnesses can increase the risk.
- Characteristics: Typically presents with acute, painful swelling, redness, warmth over the gland, and often fever and malaise. Pus may be expressed from the duct in severe cases.
- Common culprits: Staphylococcus aureus is the most common bacterial pathogen.
Viral Infections
Certain viral infections can also cause salivary gland swelling. The most well-known example is mumps (epidemic parotitis), which primarily affects the parotid glands but can occasionally involve the submandibular glands. Other viruses like influenza, coxsackievirus, and HIV can also lead to salivary gland inflammation.
- Characteristics: Usually involves bilateral swelling, accompanied by generalized viral symptoms such as fever, muscle aches, and fatigue.
Cysts and Tumors
Both benign and malignant growths can develop in the submandibular salivary glands, leading to swelling.
- Cysts: Non-cancerous fluid-filled sacs. Ranulas, a type of mucocele, are common cysts that can occur on the floor of the mouth and sometimes involve the submandibular gland duct.
- Benign Tumors: Pleomorphic adenomas are the most common benign salivary gland tumors. They typically grow slowly and are painless.
- Malignant Tumors: Though less common, cancers like mucoepidermoid carcinoma or adenoid cystic carcinoma can develop. These may present as a rapidly growing, firm, often painless mass, sometimes accompanied by facial nerve weakness or numbness.
Systemic Conditions
Several systemic diseases can manifest with submandibular gland involvement:
- Sjögren's Syndrome: An autoimmune disorder characterized by dry eyes and dry mouth (xerostomia), often leading to chronic, bilateral salivary gland swelling and inflammation.
- Sarcoidosis: An inflammatory disease that can affect multiple organs, including salivary glands.
- HIV/AIDS: Can cause lymphoid hyperplasia within the salivary glands, leading to swelling.
- Diabetes: Poorly controlled diabetes can predispose individuals to salivary gland infections.
Other Causes
- Trauma: Injury to the jaw or mouth can cause swelling.
- Allergic Reactions: Rarely, severe allergic reactions can cause angioedema (swelling beneath the skin) affecting the face and neck, including salivary glands.
- Medication Side Effects: Certain medications, particularly those that cause dry mouth (e.g., anticholinergics, antihistamines), can increase the risk of stone formation or infection.
Causes / Why It Happens
The underlying reasons for submandibular salivary gland swelling are diverse, but they generally boil down to obstructions, infections, inflammation, or abnormal growths.
- Blockage of Saliva Flow: This is the primary mechanism for sialolithiasis. When a stone forms in Wharton's duct, it obstructs the normal outflow of saliva. During meals, the gland attempts to produce more saliva, leading to back pressure, distension, and pain. This stagnation also creates an ideal environment for bacteria, often leading to secondary infection.
- Bacterial Invasion: Sialadenitis occurs when bacteria, usually from the mouth, ascend the salivary duct into the gland. This is more likely to happen if saliva flow is reduced (due to dehydration, medications, or blockage) or if the individual has a compromised immune system.
- Viral Replication: Viruses like mumps directly infect the glandular tissue, causing inflammation and swelling as the body's immune system responds to the infection.
- Abnormal Cell Growth: Cysts result from blocked ducts or developmental anomalies, while tumors arise from uncontrolled proliferation of glandular cells.
- Immune System Dysfunction: In autoimmune diseases like Sjögren's syndrome, the body's immune system mistakenly attacks the salivary glands, causing chronic inflammation and damage.
- Dehydration and Poor Oral Hygiene: These factors contribute significantly to reduced saliva flow and increased bacterial load, predisposing individuals to sialolithiasis and sialadenitis.
- Radiation Therapy: Head and neck radiation can damage salivary gland tissue, leading to fibrosis, reduced saliva production, and an increased risk of infections.
Signs and Symptoms
Recognizing the signs and symptoms of submandibular salivary gland swelling is crucial for timely intervention. The specific symptoms can vary depending on the underlying cause.
Common Symptoms:
- Swelling under the jaw: A noticeable lump or fullness in the submandibular region, often unilateral (one side) but can be bilateral. This is the hallmark symptom of submandibular salivary gland swelling.
- Pain: Can range from dull ache to sharp, intense pain, often worse during or after eating. The pain might radiate to the ear or neck.
- Tenderness: The swollen area is often tender to the touch.
- Dry Mouth (Xerostomia): Reduced saliva production can lead to a persistent dry sensation.
- Fever and Chills: Especially common with bacterial infections (sialadenitis).
- Redness and Warmth: The skin over the swollen gland may appear red and feel warm.
- Difficulty Swallowing (Dysphagia): Severe swelling can make swallowing uncomfortable or difficult.
- Unpleasant Taste/Pus Drainage: In cases of severe infection, pus may drain into the mouth, causing a foul taste.
- Difficulty Opening Mouth (Trismus): Less common, but severe inflammation can restrict jaw movement.
- Palpable Mass: A hard lump might be felt under the jaw, particularly with stones or tumors.
- Gums Keep Swelling: While less direct, chronic swelling in the submandibular area can sometimes contribute to secondary inflammatory responses in adjacent oral tissues, potentially making it feel like gums keep swelling due to overall oral discomfort and inflammation, though primary gum swelling has different causes.
When to Suspect Specific Causes:
- Sialolithiasis: Intermittent pain and swelling during meals, often subsiding between meals.
- Acute Sialadenitis: Rapid onset of painful, red, warm swelling with fever.
- Chronic Sialadenitis: Recurrent episodes of swelling and mild pain, often due to repeated blockages or chronic inflammation.
- Tumors: Often a slowly growing, firm, usually painless lump. Rapid growth or associated nerve weakness warrants immediate attention.
- Viral Infections: Bilateral swelling with systemic viral symptoms.
Treatment Options
Treatment for submandibular salivary gland swelling depends entirely on the underlying cause. A dental professional or physician will perform a thorough examination and may order diagnostic tests to determine the best course of action.
Conservative Management (First-line for stones and mild infections):
- Hydration: Drinking plenty of water helps keep saliva thin and flowing, aiding in the natural flushing of small stones or bacteria.
- Warm Compresses: Applying warm, moist heat to the swollen area can help reduce pain and inflammation and promote blood flow.
- Massage: Gently massaging the gland and duct area can help dislodge small stones or encourage saliva flow.
- Sialogogues: Sucking on sour candies or lemon wedges, which stimulate saliva production, can help push out smaller stones.
- Pain Relief: Over-the-counter non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen or acetaminophen can manage pain and reduce inflammation.
- Oral Hygiene: Maintaining excellent oral hygiene helps reduce bacterial load in the mouth, preventing ascending infections.
Medical Management:
- Antibiotics: For bacterial sialadenitis, a course of antibiotics (e.g., amoxicillin-clavulanate, clindamycin) is prescribed. The choice depends on the severity of the infection and local resistance patterns. Treatment typically lasts 7-10 days.
- Antivirals: If a viral infection like mumps is diagnosed, antiviral medications are generally not used. Treatment focuses on supportive care to manage symptoms.
Surgical Interventions:
When conservative and medical treatments fail, or for larger stones, recurrent infections, or tumors, surgical options may be considered.
1. Sialendoscopy (Minimally Invasive)
- Description: A procedure where a tiny endoscope (a thin, flexible tube with a camera) is inserted into the salivary duct to visualize, locate, and remove stones or break up strictures (narrowings).
- Pros: Minimally invasive, preserves the gland, faster recovery, less scarring.
- Cons: Not suitable for all stones (e.g., very large or embedded ones), requires specialized equipment and trained surgeons.
- Effectiveness: Highly successful for stones less than 4mm.
2. Transoral Stone Removal
- Description: For stones located near the opening of Wharton's duct, a small incision can be made inside the mouth to extract the stone.
- Pros: Relatively simple, preserves the gland.
- Cons: Only feasible for easily accessible stones.
3. Sialadenectomy (Gland Removal)
- Description: Surgical removal of the entire submandibular salivary gland. This is typically reserved for cases of very large or deeply embedded stones, recurrent severe infections, chronic inflammation, or tumors.
- Pros: Definitive treatment for chronic or severe issues, removes source of problem.
- Cons: More invasive, requires an external neck incision, longer recovery, potential for nerve damage (marginal mandibular nerve, lingual nerve), permanent dry mouth on one side.
- Risks: Nerve damage (leading to lower lip weakness or tongue numbness), hematoma, infection, permanent dry mouth.
4. Tumor Excision
- Description: For benign or malignant tumors, surgical removal of the mass, often with a margin of healthy tissue, is necessary. The extent of surgery depends on the tumor type, size, and location.
- Pros: Curative for benign tumors, often the first line of treatment for malignant tumors.
- Cons: Similar risks to sialadenectomy, potential need for radiation therapy post-surgery for malignant tumors.
Pro Tip: Always follow your healthcare provider's instructions carefully. Do not attempt to self-diagnose or treat severe swelling, especially if accompanied by fever or difficulty breathing.
Step-by-Step Process (Typical Treatment Scenario for a Salivary Stone)
Let's consider a common scenario: you've been diagnosed with a submandibular salivary gland stone (sialolithiasis) that requires intervention beyond conservative measures.
Step 1: Initial Consultation and Diagnosis
- Your visit: You'll describe your symptoms, such as the submandibular salivary gland swelling, pain during meals, and perhaps the sensation that your gums keep swelling due to referred pain or general oral discomfort.
- Clinical Examination: The dentist or oral surgeon will visually inspect and gently palpate (feel) your jaw and neck area, and examine the floor of your mouth, looking for swelling, tenderness, and possibly feeling the stone within the duct. They might gently massage the gland to see if saliva or pus can be expressed.
- Imaging:
- X-rays (Occlusal or Panoramic): Can often detect calcified stones, especially larger ones.
- Ultrasound: Excellent for visualizing soft tissues, detecting stones, and assessing gland inflammation. It's non-invasive and radiation-free.
- CT Scan: Provides detailed cross-sectional images, useful for larger, deeply embedded stones or when a tumor is suspected.
- Sialography: Less common now, involves injecting contrast dye into the duct and taking X-rays, useful for ductal strictures but not performed if acute infection is present.
Step 2: Treatment Planning
- Based on the diagnosis (size, location of stone, presence of infection), your healthcare provider will discuss treatment options. This could range from continued conservative management to sialendoscopy or open surgery.
Step 3: Pre-Treatment Preparation (If surgery is needed)
- Medical Clearance: You may need blood tests or other evaluations to ensure you are fit for surgery, especially if general anesthesia is planned.
- Medication Review: Discuss all your medications with your surgeon, particularly blood thinners, which may need to be adjusted.
- Fasting: If general anesthesia is used, you will be instructed to fast for a certain period before the procedure.
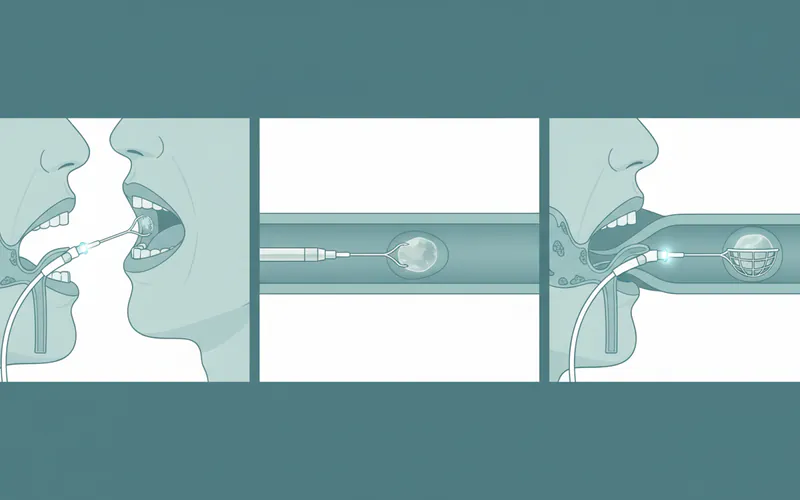
Step 4: The Procedure (Example: Sialendoscopy)
- Anesthesia: Local anesthesia with sedation or general anesthesia is administered.
- Dilation: The opening of Wharton's duct on the floor of your mouth is gently dilated.
- Endoscope Insertion: A thin sialendoscope is inserted into the duct.
- Visualization: The surgeon visualizes the duct and gland, locating the stone or stricture.
- Stone Removal: Small instruments (e.g., micro-forceps, baskets) are passed through the endoscope to grasp and remove the stone. Sometimes, a laser or micro-drill is used to fragment larger stones.
- Stent Placement (Optional): In some cases, a temporary stent (a small tube) may be placed in the duct to keep it open and prevent scarring during healing.
- Completion: The endoscope is removed, and any stent is typically removed after a few weeks.
Step 5: Post-Procedure Care and Follow-up
- Detailed instructions for recovery (pain management, diet, oral hygiene).
- Follow-up appointments to monitor healing and assess long-term success.
Cost and Insurance
Understanding the financial aspect of submandibular salivary gland swelling treatment is important for patients in the US. Costs can vary significantly based on the diagnosis, the complexity of the treatment, the geographic location, and the healthcare provider.
Average US Price Ranges:
| Treatment Type | Average Cost (Without Insurance) | Average Cost (With Insurance, Patient Share) |
|---|---|---|
| Initial Consultation/Diagnosis | $150 - $500 | $20 - $100 (Co-pay/Deductible) |
| Antibiotics/Medications | $30 - $300 | $10 - $50 (Co-pay, depending on formulary) |
| Imaging (X-ray) | $50 - $200 | $10 - $50 (Co-pay/Deductible) |
| Imaging (Ultrasound) | $200 - $600 | $50 - $150 (Co-pay/Deductible) |
| Imaging (CT Scan) | $500 - $2,000+ | $100 - $500 (Co-pay/Deductible) |
| Sialendoscopy | $2,000 - $8,000 | $500 - $2,500 (Deductible/Co-insurance) |
| Transoral Stone Removal | $1,000 - $3,000 | $200 - $1,000 (Deductible/Co-insurance) |
| Submandibular Sialadenectomy | $5,000 - $15,000+ | $1,000 - $5,000+ (Deductible/Co-insurance) |
| Biopsy / Tumor Excision (Complex) | $3,000 - $15,000+ | $500 - $5,000+ (Deductible/Co-insurance) |
Note: These are general ranges. Costs can be higher in major metropolitan areas or at specialized institutions. Emergency room visits will significantly increase initial diagnostic costs.
Insurance Coverage Details:
Most medical insurance plans (not dental insurance) will cover the diagnosis and treatment of submandibular salivary gland swelling, as it is considered a medical condition affecting a gland. However, coverage will depend on your specific plan:
- Deductibles: You will likely need to pay a certain amount out-of-pocket before your insurance begins to cover costs.
- Co-pays: A fixed amount you pay for a doctor's visit or prescription.
- Co-insurance: A percentage of the cost of a service you pay after your deductible is met (e.g., 20% of the cost of surgery).
- Out-of-Pocket Maxima: The maximum amount you will have to pay for covered services in a plan year.
It is highly recommended to contact your insurance provider directly before any procedure to understand your specific benefits, coverage limits, and any pre-authorization requirements. Many plans require prior authorization for imaging (CT scans) and surgical procedures.
Recovery and Aftercare
Recovery varies significantly based on the treatment method.
After Conservative/Medical Treatment (Stones passed, infection resolved):
- Duration: A few days to a week.
- Pain: Mild discomfort, manageable with OTC pain relievers.
- Diet: No specific restrictions, but avoid very hard or crunchy foods if your mouth is tender.
- Aftercare: Continue good hydration, warm compresses, and massage as advised by your doctor to prevent recurrence. Complete the full course of antibiotics if prescribed.
- How long does gum swelling last? If there was any related gum swelling, it should resolve as the primary submandibular issue improves, typically within a few days to a week after treatment starts.
After Sialendoscopy:
- Duration: Minimal downtime, often back to normal activities within 1-2 days.
- Pain: Mild to moderate discomfort in the mouth or under the jaw for a few days, manageable with pain medication.
- Diet: Soft diet for 24-48 hours. Avoid very hot or spicy foods.
- Aftercare:
- Hydration: Continue drinking plenty of fluids.
- Oral Hygiene: Gentle brushing, antiseptic mouthwash (e.g., chlorhexidine) if prescribed, to prevent infection.
- Saliva Stimulants: Your doctor may recommend sour candies or lemon to encourage saliva flow.
- Follow-up: Essential to ensure healing and absence of recurrence.
- Potential Symptoms: Mild swelling or bruising, temporary changes in taste are possible.
After Submandibular Sialadenectomy (Gland Removal):
- Duration: More significant recovery. Hospital stay may be 1-2 days. Full recovery can take 2-4 weeks.
- Pain: Moderate to severe pain in the neck and jaw area for the first few days, requiring prescription pain medication.
- Diet: Soft diet initially, progressing to regular food as tolerated.
- Aftercare:
- Wound Care: Keep the incision site clean and dry. Follow instructions for dressing changes.
- Activity Restrictions: Avoid strenuous activity, heavy lifting, and sudden neck movements for several weeks.
- Swelling/Bruising: Expect swelling and bruising around the incision and jaw, which will gradually subside.
- Numbness: Temporary or permanent numbness around the incision or lower lip is possible due to nerve involvement.
- Follow-up: Regular follow-up with your surgeon to monitor healing and address any concerns.
- Dental implications: If there was associated localized gums keep swelling due to inflammation, it will generally resolve as the primary surgical site heals.
Pro Tip: Always keep the surgical site clean and dry. Report any signs of infection (increased redness, pus, worsening pain, fever) to your surgeon immediately.
Prevention
Preventing submandibular salivary gland swelling primarily involves maintaining good oral hygiene and managing risk factors.
- Stay Hydrated: Drinking ample water throughout the day is crucial. Adequate hydration keeps saliva thin and flowing, reducing the risk of stone formation and bacterial stagnation. Aim for at least 8 glasses (64 ounces) of water daily.
- Practice Excellent Oral Hygiene: Brush twice a day, floss daily, and use an antiseptic mouthwash. This reduces the bacterial load in your mouth, minimizing the chance of ascending infections into the salivary ducts. Regular dental check-ups (every 6 months) are also vital.
- Stimulate Saliva Flow: If you're prone to dry mouth, chew sugar-free gum, suck on sugar-free candies (especially sour ones), or use artificial saliva products. This helps flush the ducts.
- Address Underlying Conditions: If you have systemic conditions like Sjögren's syndrome, diabetes, or HIV, managing these conditions effectively with your doctor can reduce your risk of salivary gland complications.
- Review Medications: Discuss with your doctor if any medications you are taking cause dry mouth, as this can be a risk factor for salivary gland issues. Alternative medications might be available.
- Avoid Smoking: Smoking is detrimental to overall oral health and can exacerbate inflammatory conditions.
Risks and Complications
While many cases of submandibular salivary gland swelling resolve with conservative treatment, potential risks and complications exist, especially if left untreated or in more severe cases.
- Recurrent Infections (Chronic Sialadenitis): Untreated stones or chronic inflammation can lead to repeated episodes of infection, causing significant discomfort and potentially requiring more invasive treatment.
- Abscess Formation: A severe, untreated infection can lead to the formation of an abscess (a localized collection of pus) within the gland, which requires drainage and can be dangerous if it spreads.
- Ductal Strictures: Chronic inflammation or repeated trauma from stones can cause scarring and narrowing of the salivary duct, leading to persistent blockages.
- Sepsis: In rare, severe cases, a bacterial infection can spread from the gland into the bloodstream, leading to a life-threatening systemic infection (sepsis). This is a dental emergency.
- Facial Nerve Damage: Surgical removal of the submandibular gland (sialadenectomy) carries a risk of damaging the marginal mandibular branch of the facial nerve, which can lead to temporary or permanent weakness of the lower lip.
- Lingual Nerve Damage: The lingual nerve, which provides sensation to the tongue, is also in close proximity and can be injured during surgery, causing numbness or altered taste.
- Salivary Fistula: A rare complication where a persistent opening develops, allowing saliva to drain externally through the skin.
- Ranula (Oral Cyst): A submandibular gland duct can be injured or blocked, leading to the formation of a large mucous retention cyst on the floor of the mouth.
- Malignant Transformation (Rare): While most swelling is benign, chronic inflammation in some conditions has a very low risk of contributing to malignant changes over a very long time, though this is not a direct consequence of typical salivary gland swelling. Early diagnosis of suspicious masses is paramount.
Comparison Tables
Comparison of Submandibular Swelling Causes
| Feature | Sialolithiasis (Stones) | Acute Sialadenitis (Infection) | Submandibular Tumor (Benign/Malignant) |
|---|---|---|---|
| Primary Cause | Calcified stone in duct/gland | Bacterial/viral infection | Abnormal cell growth (neoplasm) |
| Onset of Swelling | Intermittent, often linked to meals | Rapid, acute | Slow, gradual (benign); faster (malignant) |
| Pain Level | Intermittent, increases with eating, dull to sharp | Constant, moderate to severe, tenderness | Usually painless (benign); can be painful (malignant) |
| Associated Symptoms | Dry mouth, swelling subsides between meals | Fever, chills, redness, warmth, pus drainage | Firm mass, potential nerve weakness/numbness |
| Diagnosis | X-ray, Ultrasound, CT | Clinical exam, culture, Ultrasound | Clinical exam, Biopsy, CT, MRI |
| Treatment | Conservative, Sialendoscopy, Surgery | Antibiotics, hydration, warm compresses | Surgical excision, radiation (for malignancy) |
| Risk Factors | Dehydration, certain medications, smoking | Dehydration, poor oral hygiene, blockages | Age, genetics, radiation exposure |
Comparison of Surgical Treatment Options
| Feature | Sialendoscopy | Transoral Stone Removal | Submandibular Sialadenectomy |
|---|---|---|---|
| Invasiveness | Minimally invasive | Minimally invasive | Highly invasive |
| Incision | None (via duct opening) | Small intraoral incision | External neck incision (2-5 cm) |
| Anesthesia | Local with sedation or General | Local with sedation or General | General anesthesia |
| Recovery Time | 1-2 days | 2-5 days | 2-4 weeks |
| Gland Preservation | Yes | Yes | No (gland is removed) |
| Typical Cost | $2,000 - $8,000 | $1,000 - $3,000 | $5,000 - $15,000+ |
| Main Advantage | Gland preservation, quick recovery | Simple for accessible stones | Definitive for chronic/malignant issues |
| Main Disadvantage | Not for all stones, specialized skill needed | Only for superficial stones | Longer recovery, nerve damage risk, scarring |
Children / Pediatric Considerations
Submandibular salivary gland swelling in children, while less common than in adults, can occur and presents unique challenges.
- Causes: In children, viral infections (like mumps) are a more frequent cause of salivary gland swelling compared to adults. Sialadenitis can also occur, particularly in dehydrated children or those with underlying medical conditions. Sialolithiasis is rarer in children but can happen. Congenital cysts (e.g., branchial cleft cysts, dermoid cysts) can also present as neck masses that might be mistaken for salivary gland swelling.
- Diagnosis: Diagnosis can be more challenging in children due to their smaller structures and potential difficulty cooperating with imaging. Ultrasound is often the preferred imaging modality due to its non-invasive nature and lack of radiation.
- Symptoms: Children may express pain less clearly or localize it poorly. Look for irritability, refusal to eat, fever, and a visible lump under the jaw.
- Treatment: Conservative management (hydration, warm compresses, antibiotics for bacterial infections) is often the first approach. Surgical interventions are typically reserved for persistent issues, larger stones, or suspected tumors, and are performed by pediatric specialists.
- Parental Guidance: Parents should seek prompt medical attention if their child develops submandibular swelling, especially if accompanied by fever, difficulty eating, or breathing difficulties. Pediatric dentists or ENTs specializing in pediatrics are best equipped to handle these cases.
Cost Breakdown
While covered in the previous section, let's emphasize the breakdown of costs, specifically for a full diagnostic and treatment pathway.
Scenario: Acute Submandibular Sialadenitis requiring antibiotics and follow-up
- Initial Visit (Urgent Care/Dentist): $150 - $400
- Medications (Antibiotics, Pain Relievers): $30 - $150
- Follow-up Visit(s): $100 - $300
- Total (Without Insurance): $280 - $850
- Total (With Insurance, estimate for co-pays/deductibles): $50 - $200
Scenario: Sialolithiasis requiring Sialendoscopy
- Initial Consultation & Imaging (CT Scan): $650 - $2,500
- Sialendoscopy Procedure (Surgeon's fee, Anesthesia, Facility fee): $2,000 - $8,000
- Post-operative Medications: $20 - $100
- Follow-up Visit(s): $100 - $300
- Total (Without Insurance): $2,770 - $10,900
- Total (With Insurance, estimate for deductible/co-insurance): $700 - $3,500+
Payment Plans and Financing Options:
- Medical Insurance: As detailed, this is your primary coverage. Verify benefits before treatment.
- Dental Insurance: Typically does NOT cover salivary gland issues, as they are medically rather than dentally coded, unless the procedure is performed by an oral surgeon who is also a dentist and it's filed through medical.
- Payment Plans: Many hospitals and larger dental/oral surgery practices offer in-house payment plans, allowing you to pay over several months.
- Healthcare Credit Cards: Options like CareCredit offer special financing for healthcare expenses, often with deferred interest options for a period.
- Personal Loans: Banks or credit unions may offer personal loans for larger medical expenses.
- Financial Assistance Programs: Some hospitals have programs for low-income patients or those facing significant medical debt. Inquire with the hospital's financial counseling department.
Cost-Saving Tips:
- Shop Around: For non-emergency procedures, compare costs from different providers or facilities in your area.
- Generic Medications: Always ask your doctor if a generic version of a prescribed medication is available.
- In-Network Providers: Use healthcare providers and facilities that are in your insurance network to maximize coverage and reduce out-of-pocket costs.
- Understand Your EOB: Review your Explanation of Benefits (EOB) from your insurance company carefully to ensure all charges are accurate.
Frequently Asked Questions
What does submandibular salivary gland swelling feel like?
Submandibular salivary gland swelling typically feels like a firm or soft lump under the jaw, often accompanied by tenderness and pain. The pain can be dull or sharp, sometimes radiating towards the ear or neck, and often intensifies during or after eating when the gland tries to produce saliva.
Is submandibular gland swelling serious?
It can range from a minor inconvenience to a serious condition. While often benign and treatable with conservative measures, it can lead to severe infections, abscess formation, or indicate a more serious underlying issue like a tumor. Prompt medical evaluation is always recommended to determine the cause and prevent complications.
How long does submandibular gland swelling last?
The duration depends on the cause. Swelling from a small stone might subside within hours or days if the stone passes. An acute infection treated with antibiotics usually resolves within 1-2 weeks. Chronic conditions or those requiring surgery may involve intermittent swelling or a recovery period lasting several weeks to months.
Can submandibular swelling be a sign of cancer?
Yes, in rare cases, persistent or rapidly growing submandibular swelling can be a symptom of salivary gland cancer. While most swellings are benign, any new, firm, persistent, or rapidly changing lump under the jaw, especially if painless, warrants immediate investigation by a specialist.
What should I avoid eating if I have submandibular gland swelling?
During an acute episode, it's generally advisable to avoid foods that heavily stimulate saliva production (like very sour or acidic foods) if you suspect a blockage, as this can worsen pain. However, once the immediate pain subsides or if your doctor recommends it, stimulating saliva flow with sour foods can help dislodge small stones. Stick to soft, easy-to-chew foods if you have significant pain or difficulty swallowing.
Can stress cause salivary gland swelling?
Directly, no. However, chronic stress can contribute to dehydration, compromise the immune system, and potentially exacerbate conditions like Sjögren's syndrome, which in turn can indirectly increase the risk of salivary gland issues. It's not a primary cause but can be a contributing factor.
What is the recovery time after submandibular gland removal surgery?
Recovery after submandibular gland removal (sialadenectomy) typically involves a hospital stay of 1-2 days. Initial pain and swelling can last for a week, and full recovery, including resolution of tenderness and return to normal activities, usually takes 2 to 4 weeks. Adherence to post-operative instructions is crucial for proper healing.
Are there alternatives to surgery for salivary gland stones?
For small salivary stones, conservative treatments like hydration, massage, warm compresses, and saliva stimulants are often effective. For larger or persistent stones, sialendoscopy is a minimally invasive surgical alternative that preserves the gland. Open surgery is reserved for cases where these less invasive options are not feasible or fail.
How can I tell if my "gums keep swelling" is related to my salivary gland issue?
If your gums keep swelling specifically in the area near the submandibular gland and it coincides with pain and swelling under your jaw, it might be related to inflammation or referred pain from the gland. However, primary gum swelling (gingivitis, periodontitis, abscess) is usually localized to the gums themselves and has different causes. A dental professional can differentiate between these.
What is the role of the ADA in guidelines for submandibular gland issues?
The American Dental Association (ADA) provides comprehensive guidelines for oral health professionals, covering diagnosis, treatment, and referral for various oral and maxillofacial conditions, including those affecting salivary glands. They emphasize the importance of early diagnosis, appropriate imaging, and interdisciplinary collaboration with medical specialists for complex cases. Dentists often serve as the first point of contact for patients experiencing these symptoms.
When to See a Dentist
Recognizing when to seek professional help for submandibular salivary gland swelling is paramount. While some minor issues may resolve on their own, certain symptoms warrant immediate attention.
Immediate Emergency Care (Go to ER or call 911 if):
- Rapidly Worsening Swelling: If the swelling under your jaw is expanding very quickly.
- Difficulty Breathing or Swallowing: This could indicate a severe infection, abscess, or an expanding mass that is obstructing your airway or esophagus.
- High Fever with Chills: Especially if accompanied by widespread body aches, which could signal a serious infection or sepsis.
- Severe, Unbearable Pain: Pain that is not relieved by over-the-counter medication.
Urgent Dental or Medical Appointment (Within 24-48 hours if):
- New, Persistent Swelling: Any new lump or swelling under your jaw that lasts more than a day or two and doesn't improve.
- Moderate to Severe Pain: Especially if it interferes with eating or sleeping.
- Swelling accompanied by redness, warmth, or pus drainage: These are signs of infection.
- Inability to open your mouth fully (trismus).
- Numbness or weakness in the lower lip or face: This could indicate nerve involvement, potentially from a tumor.
Scheduled Dental Appointment (Routine Care, if concerns but no urgent symptoms):
- Recurrent, mild swelling: If you experience occasional, mild swelling that resolves quickly, but you're concerned about its cause or frequency.
- Persistent dry mouth (xerostomia): While not direct swelling, dry mouth is a major risk factor for salivary gland issues and should be discussed with your dentist.
- If you notice your "gums keep swelling" and you're unsure if it's related to your submandibular gland: Your dentist can rule out common gum issues and refer you if necessary.
Early intervention not only alleviates discomfort but can also prevent the progression to more serious complications. Your dental professional is often the first point of contact for these issues and can guide you to the appropriate specialist, whether it's an oral surgeon, an ENT (Ear, Nose, Throat) specialist, or another medical doctor.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
How to Relieve Gum Swelling
When your gums are swollen, it can be an alarming and uncomfortable experience, often signaling an underlying issue that requires attention. Statistics from the Centers for Disease Control and Prevention (CDC) reveal that **nearly half of adults aged 30 or older in the United States have some form o
February 23, 2026
Teeth Swelling: Complete Guide
When you experience teeth swelling, it's more than just a minor discomfort; it's a clear signal from your body that something is amiss within your oral cavity, often indicating an underlying infection or inflammation that requires prompt attention. A recent survey revealed that **over 25% of adu
February 23, 2026
What Helps With Gum Swelling
Gum swelling, medically known as gingival swelling or gingivitis, is a common yet often underestimated dental issue affecting millions of Americans. Have you ever woken up with sore, puffy gums that bleed easily when you brush? You're not alone. Research indicates that nearly **half of all a
February 23, 2026
How to Handle Knocked Out Tooth
A sudden impact, a sporting accident, or an unexpected fall – in a fraction of a second, your world can shift when you realize you've lost a tooth. A knocked out tooth, medically known as an avulsed tooth, is one of the most severe dental emergencies, and knowing **how to handle a knocked out to
February 23, 2026