How to Relieve Gum Swelling
Key Takeaways
- When your gums are swollen, it can be an alarming and uncomfortable experience, often signaling an underlying issue that requires attention. Statistics from the Centers for Disease Control and Prevention (CDC) reveal that **nearly half of adults aged 30 or older in the United States have some form o
When your gums are swollen, it can be an alarming and uncomfortable experience, often signaling an underlying issue that requires attention. Statistics from the Centers for Disease Control and Prevention (CDC) reveal that nearly half of adults aged 30 or older in the United States have some form of gum disease, a condition that frequently manifests with swollen, red, and tender gums. Ignoring these symptoms can lead to more severe dental problems, including tooth loss and broader health complications. Understanding how to relieve gum swelling is not just about temporary comfort; it's a crucial step in maintaining your overall oral and systemic health.
This comprehensive guide from SmilePedia.net aims to provide you with the knowledge and tools to identify, understand, and effectively manage gum swelling. We will delve into the various causes, from common plaque buildup to systemic conditions, explore immediate home remedies, detail professional treatment options, discuss associated costs and recovery, and emphasize preventive measures. By the end of this article, you will be equipped with the insights needed to address gum swelling proactively and confidently.
Key Takeaways:
- Identify the Cause: Gum swelling is a symptom, not a disease. Common causes include poor oral hygiene (gingivitis), infections (abscesses), trauma, and systemic conditions like pregnancy or diabetes.
- Home Remedies for Immediate Relief: Saltwater rinses, cold/warm compresses, and over-the-counter pain relievers can offer temporary relief for mild swelling. These typically cost $5-$20.
- Professional Dental Care is Crucial: Persistent or severe swelling, especially accompanied by pain, pus, or fever, requires immediate dental evaluation. Treatment can range from basic cleanings ($75-$200) to deep cleaning (scaling and root planing, $200-$500 per quadrant) or abscess drainage ($150-$400).
- Preventive Measures are Key: Maintaining diligent oral hygiene, including brushing twice daily and flossing once daily, along with regular dental check-ups (every 6 months, approximately $75-$200 per visit without insurance), is the best defense against gum swelling.
- Insurance Coverage: Most dental insurance plans cover preventive care and a significant portion (50-80%) of basic restorative procedures. Major procedures like periodontal surgery can have 20-50% coverage.
- Timelines: Mild, plaque-induced gingivitis may resolve within 5-7 days with improved oral hygiene and home care. Abscesses require immediate professional intervention and healing can take 1-2 weeks after treatment. Chronic periodontitis requires ongoing management.
- Don't Delay: Untreated gum swelling can escalate to severe infections, bone loss, and even impact systemic health, making early intervention critical.
What It Is / Overview: Gum Swelling Explained
Gum swelling, medically known as gingival inflammation or gingivitis, is a common oral health condition characterized by the enlargement, redness, and tenderness of the gum tissue (gingiva) surrounding the teeth. The gingiva is designed to be firm, pale pink, and tightly hug the teeth. When inflammation occurs, this healthy appearance is compromised, leading to a softer, often puffy texture that may appear bright red or purplish.

This inflammation is essentially the body's immune response to irritants, most commonly bacterial plaque buildup along the gumline. While seemingly minor, persistent gum swelling is a significant indicator that something is amiss in your oral environment. It can range from a localized swelling affecting just one area around a single tooth to a more generalized inflammation impacting the entire gum line. If left unaddressed, mild gingival swelling can progress to more severe forms of gum disease, known as periodontitis, which can have devastating consequences for your oral health, including bone loss and eventual tooth loss.
Types / Variations: Understanding Different Forms of Gum Swelling
Gum swelling isn't a singular condition; it manifests in various forms, each with distinct characteristics and underlying causes. Recognizing these variations is crucial for proper diagnosis and effective treatment.
Localized vs. Generalized Swelling
- Localized Swelling: This refers to swelling that affects only a specific area, often around a single tooth or a small group of teeth. It can indicate a localized infection, trauma, or an erupting tooth.
- Generalized Swelling: When the inflammation extends across a larger portion of the gum line, often affecting most or all of the gums, it's considered generalized. This is typically associated with widespread poor oral hygiene or systemic conditions.
Acute vs. Chronic Swelling
- Acute Swelling: Characterized by a sudden onset, often accompanied by pain and rapid progression. Dental abscesses or acute traumatic injuries are common causes of acute gum swelling.
- Chronic Swelling: Develops gradually over time and may persist for weeks, months, or even years. It often presents with less immediate pain but can lead to long-term tissue damage. Chronic gingivitis and periodontitis fall into this category.
Specific Conditions Presenting with Gum Swelling
- Gingivitis: This is the mildest form of gum disease, primarily caused by plaque accumulation. Symptoms include red, swollen, and easily bleeding gums. It's reversible with good oral hygiene and professional cleaning.
- Periodontitis: If gingivitis is left untreated, it can advance to periodontitis. This more severe form causes inflammation, gum recession, bone loss around the teeth, and can lead to tooth mobility and eventual tooth loss. The swelling here is often more chronic and can involve deeper tissues.
- Dental Abscess (Periapical or Periodontal): An abscess is a localized collection of pus caused by a bacterial infection.
- Periapical Abscess: Forms at the tip of the tooth root due to deep decay or trauma affecting the tooth's pulp. The swelling may appear on the gum near the affected tooth.
- Periodontal Abscess: Forms within the gum tissue itself, often in a periodontal pocket, and is associated with existing periodontitis. It presents as a painful, rapidly enlarging, red bump on the gum.
- Pregnancy Gingivitis: Hormonal changes during pregnancy can make gums more sensitive to plaque, leading to exaggerated inflammation, redness, and swelling. This typically resolves after childbirth but requires careful management during pregnancy.
- Medication-Induced Gingival Enlargement: Certain medications, such as some anti-seizure drugs (e.g., phenytoin), immunosuppressants (e.g., cyclosporine), and calcium channel blockers (e.g., nifedipine), can cause the gum tissue to overgrow, leading to significant swelling and making oral hygiene difficult.
- Eruption Gingivitis/Pericoronitis:
- Eruption Gingivitis: Swelling and tenderness can occur as a tooth (especially wisdom teeth in adults or primary teeth in children) emerges through the gum tissue.
- Pericoronitis: Inflammation of the gum tissue surrounding a partially erupted tooth, most commonly a wisdom tooth. Food particles and bacteria can get trapped under the flap of gum, leading to infection and significant swelling.
- Traumatic Swelling: Physical injury, such as aggressive brushing, a poke from a sharp object, or ill-fitting dental prosthetics (dentures, crowns), can cause localized gum swelling.
- Nutritional Deficiencies: While less common in developed countries, severe deficiencies in vitamins, particularly Vitamin C (scurvy) and Vitamin K, can lead to widespread gum inflammation and bleeding.
Understanding these variations helps both patients and dental professionals pinpoint the exact nature of the problem, allowing for targeted and effective treatment strategies.
Causes / Why It Happens: The Roots of Swollen Gums
Gum swelling is a symptom, not a standalone disease. Pinpointing its cause is the critical first step in effective treatment. The reasons behind swollen gums are diverse, ranging from simple hygiene issues to complex systemic diseases.
Poor Oral Hygiene and Plaque Buildup
This is by far the most common cause of gum swelling. When you don't brush and floss effectively, food particles and bacteria accumulate on your teeth, forming a sticky film called plaque. If plaque is not removed regularly, it hardens into tartar (calculus). Both plaque and tartar contain bacteria that release toxins, irritating the gum tissue and triggering an inflammatory response, leading to gingivitis. Pro Tip: Even mild plaque accumulation can initiate gum inflammation. It's a progressive process, so consistent removal is key.
Gingivitis and Periodontitis
As mentioned, gingivitis is the initial stage of gum disease, directly resulting from plaque and tartar accumulation. If gingivitis is left untreated, the inflammation progresses. The gum tissue starts to pull away from the teeth, forming "pockets" where more plaque, tartar, and bacteria can collect. This progression is known as periodontitis, a more severe infection that affects the supporting bone and ligaments around your teeth, leading to irreversible damage, bone loss, and eventually tooth loss.
Dental Abscesses
An abscess is a painful, pus-filled pocket caused by a bacterial infection.
- Periapical Abscess: Occurs at the tip of the tooth root, often due to a deep cavity or crack in the tooth that allows bacteria to infect the pulp (nerve) of the tooth. The infection can then spread out of the root and into the surrounding bone and gum tissue, causing localized swelling.
- Periodontal Abscess: Develops within the gum tissue itself, usually in a periodontal pocket, and is common in individuals with untreated periodontitis. Food and bacteria get trapped in these deep pockets, leading to a rapid and painful infection.
Trauma or Injury
Physical injury to the gums can cause localized swelling. This can result from:
- Aggressive Brushing: Using a hard-bristled toothbrush or brushing too vigorously can injure delicate gum tissue.
- Flossing Accidents: Incorrect flossing technique can cut or irritate the gums.
- Ill-fitting Dental Appliances: Dentures, partials, braces, crowns, or fillings that don't fit correctly can rub against or press into the gums, causing irritation and swelling.
- Chemical Irritation: Strong mouthwashes, certain foods, or even allergic reactions to dental materials can irritate gums.
Nutritional Deficiencies
While rare, severe deficiencies in certain vitamins can impact gum health:
- Vitamin C (Ascorbic Acid): Essential for collagen formation, which supports healthy gum tissue. A severe deficiency can lead to scurvy, characterized by spongy, swollen, and bleeding gums.
- Vitamin K: Important for blood clotting. Deficiency can contribute to bleeding gums, which may appear swollen due to inflammation.
Hormonal Changes
Fluctuations in hormone levels can make gums more sensitive and prone to inflammation:
- Pregnancy: Elevated estrogen and progesterone levels during pregnancy can increase blood flow to the gums, making them more reactive to plaque and causing "pregnancy gingivitis." This affects an estimated 60-75% of pregnant women.
- Puberty, Menstruation, Menopause: Similar hormonal shifts during these life stages can also cause temporary gum sensitivity and swelling.
Medications
Several types of medications can cause drug-induced gingival enlargement (also called gingival hyperplasia or overgrowth):
- Anti-seizure medications: e.g., Phenytoin (Dilantin)
- Immunosuppressants: e.g., Cyclosporine
- Calcium Channel Blockers: Used to treat high blood pressure and heart conditions, e.g., Nifedipine, Amlodipine. These medications can cause gum tissue to grow excessively, making it difficult to clean and thus more susceptible to inflammation.
Systemic Diseases and Conditions
Certain underlying health conditions can manifest as gum swelling or increase susceptibility to gum disease:
- Diabetes: Individuals with diabetes are more prone to infections, including gum disease, and often experience more severe and frequent gum inflammation. Poorly controlled blood sugar impairs the body's healing response.
- Leukemia: This cancer of the blood cells can cause diffuse, purplish, and very swollen gums that bleed easily.
- Crohn's Disease: An inflammatory bowel disease that can cause oral manifestations, including swollen and inflamed gums.
- Autoimmune Diseases: Conditions like lupus or Sjögren's syndrome can affect oral tissues, leading to dryness and increased susceptibility to gum inflammation.
- HIV/AIDS: Compromised immune systems make individuals more vulnerable to severe and rapidly progressing gum disease.
Tooth Eruption
- Teething in Infants: As baby teeth emerge, the surrounding gums can become swollen, red, and tender, causing discomfort for the child.
- Wisdom Teeth: When wisdom teeth (third molars) partially erupt or become impacted, the flap of gum tissue overlying them (operculum) can trap food and bacteria, leading to inflammation and infection known as pericoronitis. This can cause significant localized swelling and pain.

Allergic Reactions
Less commonly, an allergic reaction to certain ingredients in toothpaste, mouthwash, or even food items can cause the gums to swell. Dental materials used in fillings or crowns can also trigger localized allergic responses in some individuals.
Can TMJ Cause Swelling?
The target keyword "can TMJ cause swelling" is an excellent question that connects gum health to broader craniofacial issues. Temporomandibular joint (TMJ) disorders primarily affect the jaw joint and the muscles that control jaw movement. While TMJ disorders typically manifest as jaw pain, clicking/popping sounds, and difficulty chewing, they can indirectly contribute to sensations of swelling or actual localized swelling in the facial area, which might be perceived as gum swelling.
Here's how TMJ might relate to perceived or actual swelling:
- Muscle Inflammation: The muscles involved in chewing (masseter, temporalis) are close to the upper and lower jawbones. If these muscles are inflamed or overworked due to TMJ dysfunction, the swelling can sometimes be felt or seen in the cheek/jaw area, potentially radiating discomfort or a feeling of fullness that might be confused with gum swelling, especially in the posterior (back) regions of the mouth.
- Referred Pain: TMJ pain is notorious for radiating. Pain or discomfort from the jaw joint or surrounding muscles can be referred to the teeth and gums, making them feel tender or "swollen" even if there's no visible inflammation.
- Bruxism (Teeth Grinding/Clenching): Often a contributing factor to TMJ disorders, bruxism puts excessive stress on teeth and gums. This chronic stress can lead to inflammation of the periodontal ligaments and gum tissues around the stressed teeth, potentially causing localized swelling or tenderness.
- Salivary Gland Involvement: In rare cases, severe TMJ dysfunction might indirectly affect nearby structures like the parotid salivary gland, leading to swelling in the cheek area that could be misinterpreted as gum swelling.
Therefore, while TMJ doesn't directly cause gingivitis or periodontal disease, it can create symptoms or conditions (like bruxism or muscle inflammation) that lead to perceived or actual localized swelling or discomfort that might be attributed to the gums. A dentist will differentiate this from true gingival inflammation during an examination.
Signs and Symptoms: What to Look For
Recognizing the signs and symptoms of gum swelling early is key to preventing more serious complications. While the primary symptom is visible gum enlargement, there are several other indicators to watch for:
- Redness or Darkening of Gums: Healthy gums are typically pale pink. Swollen gums often appear bright red, dark red, or purplish due to increased blood flow and inflammation.
- Tenderness or Pain: The swollen area may be sensitive to touch, pressure, or when brushing/flossing. This pain can range from mild discomfort to a throbbing ache, especially in the case of an abscess.
- Bleeding Gums: One of the most common signs. Gums may bleed easily when brushing, flossing, or even when eating certain foods. This indicates inflammation and fragility of the gum tissue.
- Puffy, Bulbous, or Spongy Gums: Instead of being firm and tight around the teeth, swollen gums often look soft, puffy, and appear to "balloon" out from the tooth surface.
- Receding Gums: In more advanced cases of gum disease (periodontitis), the gums may pull away from the teeth, making the teeth appear longer. While swelling might be present, the overall gum line can be lower.
- Bad Breath (Halitosis): The accumulation of bacteria and food particles in inflamed gum pockets can release foul-smelling gases, leading to persistent bad breath.
- Pus Between Teeth and Gums: A sign of infection, especially with an abscess or advanced periodontitis. Pus may be visible when pressure is applied to the gum or may drain on its own.
- Loose Teeth: A late-stage symptom of periodontitis, where the inflammation and bone loss have compromised the support structures of the teeth.
- Difficulty Chewing: Swelling and pain can make chewing uncomfortable or impossible, especially with hard or crunchy foods.
- Fever or Swollen Lymph Nodes: These are signs of a more widespread infection, particularly with acute abscesses or severe systemic involvement, and warrant immediate medical attention.
Home Remedies and Initial Relief for Gum Swelling
When your gums first show signs of swelling, certain home remedies can provide temporary relief and help manage mild inflammation. However, it's crucial to remember that these are not substitutes for professional dental care, especially if the swelling is persistent, severe, or accompanied by other alarming symptoms.
-
Saline (Saltwater) Rinses:
- How it works: Saltwater is a natural disinfectant and can help reduce inflammation and soothe irritated gum tissue by drawing out toxins and reducing bacterial load. The warmth can also provide comfort.
- Preparation: Mix half a teaspoon of salt into 8 ounces of warm water.
- Application: Swish the solution gently in your mouth for 30-60 seconds, then spit it out.
- Frequency: Repeat 2-3 times a day, especially after meals.
- Cost: Minimal, usually less than $5 for a container of salt.
-
Warm Compress/Cold Compress:
- How it works:
- Warm compress: Can help soothe pain and increase blood flow, promoting healing, especially if there's an abscess that needs to come to a head.
- Cold compress: Excellent for reducing immediate swelling, throbbing pain, and inflammation, particularly if the swelling is due to trauma or an acute injury.
- Application:
- Warm: Soak a clean cloth in warm water, wring it out, and hold it gently against the outside of your cheek near the swollen gum area for 10-15 minutes.
- Cold: Wrap an ice pack or a bag of frozen vegetables in a thin cloth and apply it to the outside of your cheek for 10-15 minutes.
- Frequency: Apply several times a day as needed for pain and swelling relief.
- Cost: Minimal.
- How it works:
-
Over-the-Counter (OTC) Pain Relievers:
- How it works: Non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen (Advil, Motrin) can reduce both pain and inflammation. Acetaminophen (Tylenol) can alleviate pain but does not significantly reduce inflammation.
- Application: Follow the dosage instructions on the packaging.
- Cost: $5-$15 for a bottle.
-
Topical Gels:
- How it works: Gels containing benzocaine (like Orajel) or other numbing agents can temporarily reduce localized pain and discomfort. Some gels also contain antiseptic ingredients.
- Application: Apply a small amount directly to the swollen gum area with a clean finger or cotton swab.
- Cost: $8-$20.
-
Gentle Brushing and Flossing:
- How it works: While it might seem counterintuitive to clean inflamed gums, gentle and thorough oral hygiene is paramount. Removing plaque is the primary way to allow gums to heal. Aggressive brushing, however, can worsen the situation.
- Application: Use a soft-bristled toothbrush and brush with light, circular motions. Floss carefully around the affected areas to dislodge any trapped food particles or plaque.
- Pro Tip: Don't skip cleaning the affected area. It's essential for removing the irritant. If bleeding occurs, it's a sign that the gums are inflamed and need more, not less, cleaning.
-
Dietary Adjustments:
- How it works: Eating soft, non-irritating foods can reduce trauma to the swollen gums and minimize discomfort while chewing.
- Application: Avoid very hot, cold, spicy, acidic, crunchy, or sugary foods. Opt for soft foods like soups, yogurt, mashed potatoes, and smoothies.
- Cost: No additional cost, just a change in food choices.
-
Herbal Rinses (with caution):
- Some people find relief with rinses made from diluted essential oils (like tea tree oil, clove oil, or peppermint oil) or herbal infusions (like chamomile or calendula). Always dilute essential oils properly before use, as they can be irritating in concentrated forms, and consult a dentist before using herbal remedies, especially if pregnant or breastfeeding.
- Cost: $10-$30 depending on the specific product.
Remember, if gum swelling persists for more than 1-2 days despite home care, worsens, or is accompanied by severe pain, fever, pus, or difficulty swallowing, it's time to seek professional dental help immediately.
Professional Treatment Options for Gum Swelling
When home remedies aren't enough, or if the gum swelling indicates a more serious underlying issue, professional dental treatment is essential. A dentist can accurately diagnose the cause and provide targeted interventions.
Dental Cleaning (Prophylaxis)
- What it is: A routine professional cleaning performed by a dental hygienist or dentist. It involves removing plaque and tartar (calculus) from above and slightly below the gum line using specialized instruments (scalers and ultrasonic devices).
- When it's used: This is the primary treatment for mild gingivitis, where gum swelling is mainly due to plaque accumulation.
- Pros: Non-invasive, effective for preventing and reversing early gum disease, relatively inexpensive.
- Cons: Not sufficient for advanced gum disease or deep infections.
- Cost: Typically $75 - $200 without insurance.
Scaling and Root Planing (Deep Cleaning)
- What it is: A more intensive cleaning procedure than routine prophylaxis. It involves scaling (removing plaque and tartar from above and below the gum line, deep within the periodontal pockets) and root planing (smoothing the tooth root surfaces to remove bacterial toxins and prevent future plaque adhesion). It's often performed under local anesthesia.
- When it's used: The gold standard non-surgical treatment for moderate periodontitis.
- Pros: Highly effective at reducing gum inflammation and pocket depths, can halt the progression of gum disease, often avoids the need for surgery.
- Cons: More invasive than a regular cleaning, may require multiple appointments (often per quadrant), some post-procedure sensitivity is common.
- Cost: Typically $200 - $500 per quadrant (a full mouth deep cleaning could be $800 - $2,000+).
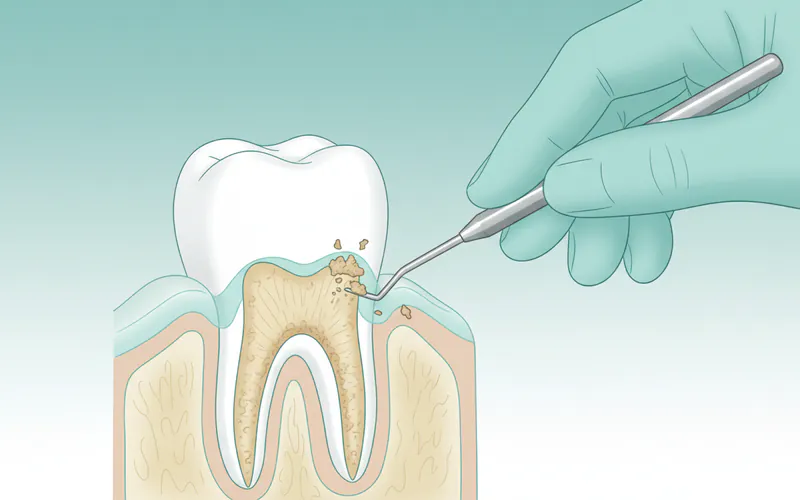
Antibiotics
- What it is: Medications that kill or inhibit the growth of bacteria. They can be prescribed systemically (oral pills) or applied locally (gels, chips, or rinses placed directly into periodontal pockets).
- When it's used: For acute infections like dental abscesses, aggressive forms of periodontitis, or when infection is spreading. Local antibiotics can supplement scaling and root planing.
- Pros: Directly targets bacterial infection, can quickly reduce severe inflammation and pain.
- Cons: Oral antibiotics can have side effects (stomach upset, yeast infections), can contribute to antibiotic resistance, local applications are not for widespread infection.
- Cost: Oral antibiotics typically $10 - $100. Local antibiotic placement $30 - $100 per site.
Drainage of Abscess
- What it is: A minor surgical procedure to release the pus from a dental abscess. This involves making a small incision in the swollen gum tissue to allow the pus to drain, followed by irrigation of the area.
- When it's used: For painful, localized gum swelling caused by a periodontal or periapical abscess.
- Pros: Provides immediate pain relief by releasing pressure, removes infection.
- Cons: May require follow-up treatment (e.g., root canal for periapical abscess, scaling and root planing for periodontal abscess).
- Cost: Typically $150 - $400.
Gingivectomy / Flap Surgery (Periodontal Surgery)
- What it is:
- Gingivectomy: Surgical removal of excess gum tissue, often performed to reduce deep gum pockets, eliminate gum overgrowth (e.g., medication-induced), or reshape the gums.
- Flap Surgery (Pocket Reduction Surgery): The gums are lifted back (a flap is created) to allow for thorough removal of tartar and bacteria from deep pockets and to reshape damaged bone. The gums are then sutured back into place, often tighter around the teeth.
- When it's used: For advanced periodontitis that doesn't respond to non-surgical treatments, severe gingival overgrowth, or when deep pockets need to be addressed surgically.
- Pros: Can significantly reduce pocket depths, eliminate infection, save teeth, improve access for home cleaning.
- Cons: More invasive, longer recovery time, higher cost, potential for post-operative pain and sensitivity.
- Cost: Gingivectomy $200 - $1,000 per tooth/quadrant. Flap surgery $500 - $3,000+ per quadrant.
Referral to Specialist
- What it is: Your general dentist may refer you to a periodontist (a gum disease specialist) for advanced cases of periodontitis, complex gum surgeries, or for issues like significant gum recession.
- When it's used: When the condition is beyond the scope of general dentistry, or requires specialized expertise.
- Pros: Access to highly specialized knowledge and techniques.
- Cons: Potentially higher specialist fees.
Addressing Underlying Causes
- Medication Review: If drug-induced gingival enlargement is diagnosed, the dentist may consult with your physician to see if alternative medications can be prescribed. Do not stop taking prescribed medications without consulting your doctor.
- Systemic Disease Management: For conditions like diabetes, uncontrolled blood sugar levels can exacerbate gum disease. Collaboration between your dentist and physician to manage the systemic condition is crucial for improving gum health.
- Correction of Ill-fitting Appliances: Dentures, crowns, or fillings that are causing irritation will need to be adjusted, repaired, or replaced.
Step-by-Step Process: What to Expect During Treatment
The path to relieving gum swelling typically follows a structured approach, starting with diagnosis and progressing through tailored treatment and follow-up.
1. Initial Consultation and Diagnosis
- Patient History: Your dentist will ask about your symptoms, duration of swelling, medical history, medications you're taking, and oral hygiene habits.
- Visual Examination: The dentist will carefully inspect your gums, teeth, and other oral tissues, looking for redness, puffiness, bleeding, and any signs of infection (like pus).
- Periodontal Probing: A small measuring tool (periodontal probe) is gently inserted into the sulcus (the space between the tooth and gum) to measure pocket depths. Depths greater than 3mm often indicate gum disease.
- X-rays: Dental X-rays may be taken to assess bone levels around the teeth, identify any deep cavities, or locate abscesses not visible during the visual exam.
- Diagnosis: Based on these findings, the dentist will determine the cause and severity of your gum swelling.

2. Treatment Plan Discussion
- Your dentist will explain the diagnosis, the recommended treatment options, their pros and cons, and what you can expect during each procedure.
- They will also discuss the estimated costs, insurance coverage, and answer any questions you may have.
3. Procedure Execution
- For Gingivitis: A routine dental cleaning (prophylaxis) will be scheduled. This is usually done in one appointment.
- For Moderate Periodontitis: Scaling and root planing will be performed. This often requires 1-4 appointments, as it's typically done quadrant by quadrant, possibly under local anesthesia.
- For Abscesses: The area will be numbed, an incision made to drain the pus, and the area cleaned. Antibiotics may be prescribed.
- For Advanced Periodontitis/Gingival Overgrowth: Referral to a periodontist for surgical procedures like gingivectomy or flap surgery may be recommended. These are more complex procedures often requiring local anesthesia and sedation, typically taking 1-2 hours per area.
4. Recovery and Aftercare Instructions
- After treatment, the dental team will provide detailed instructions on how to care for your mouth to promote healing and prevent recurrence.
- This will include advice on pain management, diet, oral hygiene techniques, and what to expect during the healing process.
5. Follow-up Appointments
- Depending on the treatment, follow-up appointments will be scheduled to monitor healing, remove sutures (if applicable), and reinforce oral hygiene practices.
- For periodontitis, "maintenance" cleanings (often called periodontal maintenance) are crucial and typically recommended every 3-4 months to prevent recurrence.
Recovery and Aftercare: Ensuring Lasting Relief
Proper recovery and diligent aftercare are essential for long-term success in relieving gum swelling and preventing its return. The specific instructions will vary based on the treatment received.
After Routine Cleaning (Prophylaxis)
- Sensitivity: You might experience minor sensitivity to hot or cold for a day or two. This is normal.
- Oral Hygiene: Continue brushing gently twice a day with a soft-bristled toothbrush and flossing once a day. Your hygienist may recommend specific brushing techniques or interdental cleaners.
- Rinsing: Continue with warm salt water rinses for a day or two to soothe gums.
- Diet: No specific dietary restrictions, but avoid overly hard or sticky foods immediately after if your gums feel sensitive.
After Scaling and Root Planing (Deep Cleaning)
- Pain and Sensitivity: Expect some discomfort, soreness, and sensitivity for several days to a week. Your dentist may prescribe pain relievers or recommend OTC options like ibuprofen.
- Swelling and Bleeding: Minor swelling and bleeding are normal immediately after the procedure. Saltwater rinses can help.
- Diet: Stick to soft, non-irritating foods for the first few days (e.g., soup, yogurt, mashed potatoes, scrambled eggs). Avoid crunchy, spicy, or acidic foods.
- Oral Hygiene: Continue brushing and flossing gently but thoroughly. An antimicrobial mouthwash might be prescribed for a short period.
- Smoking: Avoid smoking, as it significantly impairs healing.
- Follow-up: Adhere strictly to your scheduled follow-up appointments, typically 4-6 weeks after the deep cleaning, to assess healing and measure pocket depths.
- Periodontal Maintenance: After initial healing, you'll likely be placed on a periodontal maintenance schedule, requiring professional cleanings every 3-4 months, rather than the standard 6 months, to manage the disease effectively.
After Abscess Drainage or Periodontal Surgery
- Pain Management: More significant pain is expected. Your dentist will prescribe pain medication and possibly antibiotics.
- Swelling: Expect some facial swelling, which can be managed with cold compresses applied externally for the first 24-48 hours.
- Bleeding: Some oozing or light bleeding is normal for the first day. Use gauze as instructed.
- Diet: A soft-food diet is critical for several days to a week, or longer depending on the extent of the surgery. Avoid chewing on the treated side.
- Oral Hygiene: You'll receive specific instructions. This may involve avoiding brushing the surgical site for a few days, using a special soft brush, or rinsing with a prescribed antiseptic mouthwash (e.g., chlorhexidine).
- Activity: Avoid strenuous activity for the first few days to prevent increased bleeding.
- Smoking/Alcohol: Absolutely avoid smoking and alcohol, as they impede healing and increase complications.
- Sutures: If sutures (stitches) were placed, they might be dissolvable, or you'll need to return in 7-14 days for removal.
- Follow-up: Critical for monitoring healing and ensuring the success of the procedure.
Pro Tip: Consistency is paramount. Even after initial healing, maintaining excellent oral hygiene and attending all recommended follow-up and maintenance appointments are the most crucial factors in preventing gum swelling from returning. According to ADA guidelines, maintaining good oral hygiene is fundamental to preventing the recurrence of gum disease.
Prevention: Keeping Your Gums Healthy
Preventing gum swelling is far easier and less costly than treating it. A proactive approach to oral health is your best defense.
-
Excellent Oral Hygiene:
- Brush Twice Daily: Use a soft-bristled toothbrush and fluoride toothpaste. Brush for at least two minutes, covering all tooth surfaces and along the gum line. Consider an electric toothbrush, which can be more effective at removing plaque.
- Floss Daily: Flossing removes plaque and food particles from between teeth and under the gum line where your toothbrush can't reach. This is non-negotiable for gum health.
- Mouthwash: An antiseptic mouthwash can help reduce bacteria and inflammation. Look for those with ADA Seal of Acceptance. However, mouthwash is an adjunct, not a substitute for brushing and flossing.
-
Regular Dental Check-ups and Professional Cleanings:
- Visit your dentist for check-ups and cleanings every six months, or more frequently if recommended due to a history of gum disease or other risk factors. These visits allow professionals to remove stubborn plaque and tartar that you can't remove at home and to detect problems early.
-
Balanced Diet:
- Limit sugary and starchy foods, which fuel plaque-producing bacteria.
- Eat a diet rich in fruits, vegetables, and whole grains. These provide essential vitamins (like Vitamin C for gum health) and minerals.
- Stay hydrated by drinking plenty of water, which helps rinse away food particles and maintains saliva flow.
-
Avoid Tobacco Products:
- Smoking and chewing tobacco are major risk factors for gum disease. They impair gum healing, reduce blood flow, and mask symptoms, making problems harder to detect. Quitting tobacco is one of the most impactful steps you can take for your oral and overall health.
-
Manage Systemic Conditions:
- If you have conditions like diabetes, keep your blood sugar levels well-controlled. Uncontrolled diabetes significantly increases your risk and severity of gum disease.
- Work with your physician to manage other conditions that can affect oral health.
-
Stress Management:
- Chronic stress can weaken your immune system, making you more susceptible to infections, including gum disease. Practice stress-reduction techniques like exercise, meditation, or hobbies.
-
Address Dental Misalignments or Ill-fitting Restorations:
- Crooked teeth or poorly fitting crowns, fillings, or dentures can create areas where plaque accumulates easily or where gums are constantly irritated. Your dentist can recommend solutions like orthodontics or replacing restorations.
Risks and Complications of Untreated Gum Swelling
Ignoring gum swelling is never a good idea. What starts as a seemingly minor irritation can escalate into severe oral health problems and even impact your overall systemic health.
- Progression to Periodontitis: The most direct and common complication. Untreated gingivitis inevitably progresses to periodontitis, where the inflammation spreads from the gums to the deeper supporting structures of the teeth, including the periodontal ligament and alveolar bone.
- Bone Loss: Periodontitis leads to the gradual destruction of the bone that anchors your teeth. This bone loss is irreversible and can result in significant changes to your bite and facial structure.
- Tooth Loss: As bone support diminishes, teeth become loose (mobile) and eventually fall out or need to be extracted. This has significant aesthetic, functional, and financial consequences.
- Dental Abscesses: Untreated gum inflammation or deep pockets can become breeding grounds for bacteria, leading to painful pus-filled abscesses that require urgent dental intervention. These can cause severe pain, facial swelling, and even systemic symptoms like fever.
- Spread of Infection: An untreated dental infection can spread beyond the mouth to other parts of the body, leading to serious, potentially life-threatening conditions such as:
- Cellulitis: A bacterial skin infection.
- Sepsis: A life-threatening response to an infection.
- Ludwig's Angina: A serious bacterial infection in the floor of the mouth, which can cause swelling that blocks airways.
- Increased Risk of Systemic Diseases: The chronic inflammation and bacterial load associated with gum disease have been linked to an increased risk or worsening of various systemic health conditions, including:
- Cardiovascular Disease: Bacteria from the mouth can enter the bloodstream, contributing to plaque buildup in arteries.
- Diabetes: Periodontitis makes it harder to control blood sugar levels, and diabetes makes periodontitis worse.
- Respiratory Diseases: Inhaling oral bacteria can contribute to pneumonia or bronchitis.
- Adverse Pregnancy Outcomes: Links have been found to preterm birth and low birth weight.
- Rheumatoid Arthritis: A chronic inflammatory disease.
- Certain Cancers: Some studies suggest a link to pancreatic, esophageal, and head and neck cancers.
- Impact on Quality of Life: Chronic pain, difficulty eating, bad breath, and anxiety about one's appearance can significantly reduce quality of life.
Comparison Tables
Table 1: Home Remedies vs. Professional Treatments for Gum Swelling
| Feature | Home Remedies (e.g., Saltwater Rinse, Cold Compress) | Professional Dental Treatments (e.g., Cleaning, Scaling & Root Planing) |
|---|---|---|
| Severity of Swelling | Mild, temporary inflammation, initial discomfort | Persistent, severe, localized, or generalized swelling; signs of infection or advanced gum disease |
| Cost Range (US) | $5 - $20 (for basic supplies) | $75 - $3,000+ (depending on procedure, includes basic cleaning, deep cleaning, abscess drainage, or surgery) |
| Efficacy | Provides temporary relief, addresses symptoms, helps maintain hygiene; does not treat root cause if underlying issue is severe | Addresses the root cause (plaque, tartar, infection); highly effective in reversing/managing gum disease and eliminating swelling |
| Timeframe for Relief | Immediate, temporary relief for hours to 1-2 days | Initial relief within days; full resolution of swelling/symptoms typically 1-4 weeks after treatment, depending on severity |
| Actionable Data | Use 2-3x daily; apply compress 10-15 min sessions; take OTC pain relievers as directed | Schedule exam promptly; follow specific post-op instructions; attend maintenance cleanings (every 3-4 months for periodontitis) |
| Primary Goal | Soothe symptoms, support healing process | Eliminate infection, remove irritants, restore gum health, prevent recurrence, save teeth |
Table 2: Common Causes of Gum Swelling and Their Typical Treatments
| Cause | Common Symptoms | Initial Home Treatment | Professional Dental Treatment |
|---|---|---|---|
| Gingivitis (Plaque-induced) | Red, swollen, easily bleeding gums; mild tenderness | Improved brushing/flossing; saltwater rinses | Professional Dental Cleaning (Prophylaxis) |
| Periodontitis (Advanced Gum Disease) | Persistent swelling, bleeding, receding gums, bad breath, loose teeth | Saltwater rinses for temporary relief, gentle cleaning | Scaling & Root Planing (Deep Cleaning), potentially Periodontal Surgery |
| Dental Abscess (Periapical/Periodontal) | Localized, painful, rapidly spreading swelling; pus; throbbing pain; fever | Cold compress for pain; OTC pain relievers (no drainage at home) | Drainage, Antibiotics; Root Canal (periapical) or Deep Cleaning (periodontal) |
| Trauma/Injury | Localized swelling, pain after physical impact, cuts | Cold compress, gentle cleaning, soft diet | Identification & removal of irritant (e.g., adjust appliance), watchful waiting |
| Medication-Induced Gingival Overgrowth | Diffuse gum enlargement, difficulty cleaning, inflammation | Meticulous oral hygiene; antiseptic rinses | Gingivectomy (surgical gum removal), medication adjustment (with physician) |
| Erupting Tooth (e.g., Wisdom Tooth) | Localized swelling, tenderness, pain, sometimes difficulty opening mouth (pericoronitis) | Saltwater rinses, OTC pain relievers, soft diet | Dental Cleaning around tooth, antibiotics; possibly Tooth Extraction |
Children / Pediatric Considerations
Gum swelling in children is common and can be a source of concern for parents. While many causes are similar to adults, there are some unique considerations for pediatric patients.

- Teething: This is the most common cause of localized gum swelling in infants and toddlers. As primary (baby) teeth erupt through the gums, the area can become red, swollen, and tender.
- Guidance: Offer a clean teething ring (chilled, not frozen), a cold washcloth, or gently massage the gums with a clean finger. OTC pain relievers specifically formulated for infants (like acetaminophen or ibuprofen, consult pediatrician for dosage) can help. Avoid topical numbing gels containing benzocaine in children under two years due to potential side effects.
- Eruption Gingivitis: As permanent teeth emerge, particularly molars, the surrounding gum tissue can become inflamed and swollen, similar to pericoronitis in adults.
- Poor Oral Hygiene: Even young children can develop gingivitis due to inadequate brushing and flossing. Parents play a crucial role in establishing good oral hygiene habits early on.
- Guidance: Parents should brush their child's teeth twice a day from the appearance of the first tooth and supervise brushing until around age 7-8. Flossing should begin once two teeth touch.
- Thumb Sucking or Pacifier Use: Prolonged or aggressive habits can cause trauma or irritation to the gum tissue, leading to localized swelling.
- Trauma: Children are prone to falls and injuries. A blow to the mouth can cause localized gum swelling or even injure developing teeth. Seek immediate dental attention for any significant oral trauma.
- Dental Abscesses: Deep cavities can lead to dental abscesses in children, causing localized gum swelling, pain, and sometimes fever. This requires immediate professional treatment.
- Specific Childhood Gingivitis: Some children may experience more severe or unusual forms of gingivitis, sometimes linked to systemic conditions. Regular dental check-ups, starting by age one or with the eruption of the first tooth (ADA recommendation), are vital for early detection and management.
Pro Tip for Parents: Make brushing fun! Use flavored toothpaste, sing songs, or let them choose their toothbrush. Regular positive reinforcement helps establish lifelong good habits.
Cost Breakdown: Understanding the Financial Aspect of Gum Treatment
The cost of treating gum swelling in the US can vary significantly based on the underlying cause, the severity of the condition, geographic location, the specific dental provider, and whether you have dental insurance. Here's a general breakdown:
Average US Costs (Without Insurance)
- Basic Dental Exam (Initial Visit):
- Low: $50
- Mid: $100
- High: $200
- Includes visual exam, X-rays may be extra ($25-$150).
- Routine Dental Cleaning (Prophylaxis):
- Low: $75
- Mid: $125
- High: $200
- Treatment for mild gingivitis.
- Scaling and Root Planing (Deep Cleaning):
- Per Quadrant: $200 - $500
- Full Mouth (4 quadrants): $800 - $2,000+
- For moderate periodontitis.
- Antibiotic Therapy:
- Oral Antibiotics (Prescription): $10 - $100
- Local Antibiotic Placement (e.g., Arestin per site): $30 - $100
- Abscess Drainage:
- Simple Incision & Drainage: $150 - $400
- Does not include potential follow-up root canal or extraction.
- Gingivectomy (Surgical Gum Removal):
- Per Tooth/Area: $200 - $1,000
- For severe gum overgrowth or pocket reduction.
- Periodontal Flap Surgery (Pocket Reduction Surgery):
- Per Quadrant: $500 - $3,000+
- For advanced periodontitis, can include bone grafting or gum grafting which adds to the cost.
- Periodontal Maintenance Cleaning:
- Low: $100
- Mid: $175
- High: $250
- Often needed every 3-4 months after deep cleaning.
With Dental Insurance
Dental insurance plans vary significantly, but generally categorize treatments into preventive, basic, and major.
- Preventive Care (Exams, X-rays, Routine Cleanings): Typically covered at 80-100%. Many plans cover two cleanings and one exam/X-ray series per year.
- Basic Restorative Procedures (Fillings, Scaling & Root Planing, Abscess Drainage, Oral Antibiotics): Often covered at 50-80%. You will pay the remaining percentage (co-insurance) after meeting your deductible.
- Major Procedures (Periodontal Surgery, Gingivectomy): Typically covered at 20-50%. These procedures usually have a higher co-insurance and are subject to your plan's annual maximums.
Deductibles and Annual Maximums: Most dental insurance plans have a deductible (e.g., $50-$100) that you must pay out-of-pocket before insurance starts to cover services. They also have an annual maximum (e.g., $1,000-$2,000), which is the total amount the insurance company will pay for your dental care in a plan year. Once you hit this maximum, you pay 100% of subsequent costs.
Payment Plans and Financing Options
If you don't have insurance or face significant out-of-pocket costs, consider these options:
- CareCredit and Other Medical Financing: Third-party healthcare credit cards that offer promotional financing options, often with 0% interest for a set period (e.g., 6, 12, or 18 months) if the balance is paid in full.
- In-House Payment Plans: Many dental offices offer their own payment plans, allowing you to pay for treatment in installments. Discuss this with the office manager.
- Dental Savings Plans: Not insurance, but a membership plan where you pay an annual fee and get discounts (typically 10-60%) on dental services from participating providers.
- Flexible Spending Accounts (FSAs) or Health Savings Accounts (HSAs): If you have these through your employer, you can use pre-tax dollars to pay for qualified dental expenses.
Cost-Saving Tips
- Prevention is Key: The cheapest gum treatment is excellent daily oral hygiene and regular preventive check-ups. Preventing gingivitis from progressing to periodontitis saves thousands of dollars.
- Address Issues Early: Don't wait for gum swelling to become severe. Early intervention is less invasive and less expensive.
- Shop Around: While not always feasible for emergencies, for non-urgent procedures, you can get quotes from a few different dental offices.
- Ask About Discounts: Some offices offer discounts for cash payments or for seniors.
Frequently Asked Questions
How long does it take for gum swelling to go down?
The duration for gum swelling to subside depends entirely on its cause and the effectiveness of treatment. Mild, plaque-induced gingivitis can show significant improvement within 5-7 days with diligent home care and professional cleaning. More severe infections, like an abscess, may take 1-2 weeks to heal after drainage and antibiotic therapy. Chronic periodontitis requires ongoing management, and while acute swelling may resolve, the underlying disease requires continuous professional care.
What is the fastest way to reduce gum inflammation?
For immediate, temporary relief of mild inflammation, warm salt water rinses, gentle brushing, and a cold compress applied to the cheek are often the fastest home remedies. Over-the-counter anti-inflammatory pain relievers like ibuprofen can also quickly reduce discomfort and swelling. However, for a definitive and lasting reduction in inflammation, addressing the root cause through professional dental cleaning or specific treatment is essential.
Can swollen gums go away on their own?
Mild gum swelling caused by temporary irritation or a very minor accumulation of plaque might occasionally improve with extremely diligent oral hygiene. However, in most cases, swollen gums indicate a bacterial infection (gingivitis or periodontitis) or another underlying issue that will not resolve without professional intervention. Ignoring persistent swelling almost always leads to worsening conditions and more severe problems down the line.
When should I be concerned about gum swelling?
You should be concerned and seek dental attention if gum swelling persists for more than 1-2 days, is accompanied by severe pain, pus (a white or yellow discharge), fever, difficulty swallowing or breathing, a bad taste in your mouth, or if you notice receding gums or loose teeth. These are red flags that indicate a potentially serious infection or advanced gum disease requiring immediate care.
Is salt water good for swollen gums?
Yes, warm salt water rinses are an excellent home remedy for swollen gums. Salt acts as a natural antiseptic, helping to reduce bacteria in the mouth and soothe irritated tissues. The warm water can also increase blood flow to the area, aiding in the healing process. It's safe to use multiple times a day, especially after meals, but it doesn't replace professional treatment for underlying issues.
Can stress cause gum swelling?
While stress doesn't directly cause gum swelling, it can significantly contribute to its development or worsening. Chronic stress weakens the immune system, making your body less able to fight off bacterial infections that cause gum disease. Stress can also lead to habits like teeth grinding (bruxism) or neglecting oral hygiene, both of which can exacerbate gum inflammation.
How can you keep a knocked out tooth moist?
This is a critical dental emergency. If a permanent tooth is knocked out (avulsed), the most important thing is to keep it moist to preserve the cells on the root surface. The best options, in order of preference, are to reinsert it gently into its socket if possible and hold it in place. If reinsertion isn't possible, place the tooth in a cup of milk, saliva, or a saline solution (contact lens solution). Do not store it in tap water. Seek immediate dental attention, ideally within 30-60 minutes, as prompt re-implantation significantly increases the tooth's chances of survival.
Can gum swelling be a sign of something serious?
Absolutely. While often a sign of common gingivitis, gum swelling can also indicate more serious underlying conditions such as severe periodontitis (which can lead to bone and tooth loss), a dental abscess (a serious infection that can spread), or even systemic diseases like leukemia, diabetes, or autoimmune disorders. Persistent or severe gum swelling should always be evaluated by a dental professional to rule out serious health concerns.
How much does it cost to treat swollen gums?
The cost varies widely based on the cause and required treatment. For simple gingivitis, a routine dental cleaning might cost $75-$200. If it's moderate periodontitis requiring scaling and root planing, expect $200-$500 per quadrant, or $800-$2,000+ for a full mouth. An abscess drainage might be $150-$400, not including subsequent treatments like a root canal. Complex periodontal surgery can range from $500 to over $3,000 per quadrant. Dental insurance typically covers a portion, especially for preventive and basic procedures.
When to See a Dentist
While home remedies can offer temporary comfort, knowing when to seek professional dental attention is crucial to prevent minor issues from escalating into serious health problems.
See a Dentist Immediately (Emergency):
- Severe, Throbbing Pain: Especially if it's constant and not relieved by OTC pain relievers. This often indicates an acute infection or abscess.
- Visible Pus: Any white, yellow, or greenish discharge coming from your gums or around a tooth is a clear sign of infection and requires immediate drainage and treatment.
- Rapidly Spreading Swelling: If the swelling quickly spreads to your face, jaw, neck, or under your tongue, it could indicate a serious infection that requires urgent care.
- Difficulty Swallowing or Breathing: This is a medical emergency. Swelling in the floor of the mouth or throat can compromise your airway. Go to the nearest emergency room immediately.
- Fever, Chills, or General Malaise: These systemic symptoms, accompanying gum swelling, indicate a spreading infection.
- Knocked-Out Tooth: If a permanent tooth has been entirely dislodged, seek emergency dental care within minutes to maximize the chances of successful re-implantation.
Schedule an Appointment Promptly (Routine/Urgent Care):
- Persistent Swelling: If your gums remain swollen, red, or tender for more than 2 days despite diligent home care.
- Bleeding Gums: Gums that bleed consistently when brushing, flossing, or spontaneously.
- Receding Gums or Loose Teeth: These are signs of advanced gum disease.
- Bad Breath: Persistent bad breath that doesn't improve with brushing and flossing can indicate gum disease or infection.
- Pain When Chewing: This could be a sign of a dental abscess, advanced decay, or tooth fracture.
- Ill-fitting Dental Appliances: If your dentures, partials, or even braces are causing chronic irritation or swelling.
Regular Check-ups (Preventive Care):
- Even if you have no symptoms, regular dental check-ups every six months are vital. These visits allow your dentist and hygienist to identify early signs of gum inflammation, remove plaque and tartar, and provide guidance to prevent issues before they become problematic.
Ignoring gum swelling can lead to severe pain, tooth loss, and impact your overall health. When in doubt, always err on the side of caution and consult with a dental professional.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Teeth Swelling: Complete Guide
When you experience teeth swelling, it's more than just a minor discomfort; it's a clear signal from your body that something is amiss within your oral cavity, often indicating an underlying infection or inflammation that requires prompt attention. A recent survey revealed that **over 25% of adu
February 23, 2026
Submandibular Salivary Gland Swelling: Complete Guide
When you notice a peculiar lump or uncomfortable fullness beneath your jaw, it can be an alarming experience. This sensation, often accompanied by pain and difficulty swallowing, could indicate submandibular salivary gland swelling. Affecting an estimated 1 in 10,000 adults annually, conditi
February 23, 2026
What Helps With Gum Swelling
Gum swelling, medically known as gingival swelling or gingivitis, is a common yet often underestimated dental issue affecting millions of Americans. Have you ever woken up with sore, puffy gums that bleed easily when you brush? You're not alone. Research indicates that nearly **half of all a
February 23, 2026
How to Handle Knocked Out Tooth
A sudden impact, a sporting accident, or an unexpected fall – in a fraction of a second, your world can shift when you realize you've lost a tooth. A knocked out tooth, medically known as an avulsed tooth, is one of the most severe dental emergencies, and knowing **how to handle a knocked out to
February 23, 2026