Gum Swelling and Pain: Complete Guide
Key Takeaways
- Experiencing gum swelling and pain can be alarming, a sign your oral health needs immediate attention. In fact, studies by the Centers for Disease Control and Prevention (CDC) indicate that nearly half of all adults aged 30 and older in the United States show signs of gum disease, a common culpr
Experiencing gum swelling and pain can be alarming, a sign your oral health needs immediate attention. In fact, studies by the Centers for Disease Control and Prevention (CDC) indicate that nearly half of all adults aged 30 and older in the United States show signs of gum disease, a common culprit behind these symptoms. While occasional tenderness might be dismissed, persistent gum swelling and pain often signal underlying issues ranging from minor irritation to severe infection that could jeopardize your teeth and overall well-being. Ignoring these symptoms is akin to ignoring a smoke detector – a small problem can quickly escalate into a dental emergency.
This comprehensive guide from SmilePedia.net aims to empower you with the knowledge needed to understand, address, and prevent gum swelling and pain. We'll explore the various causes, recognize the critical signs, detail effective treatment options, break down costs, and provide essential recovery and prevention strategies. Whether you're dealing with localized inflammation, concerned about systemic links, or wondering what does TMJ swelling look like in relation to gum discomfort, this article will serve as your definitive resource. From routine oral hygiene to understanding the urgency when a tooth is knocked out, we cover everything you need to know to protect your smile.
Key Takeaways:
- Urgency is Key: Persistent gum swelling and pain are rarely normal and often indicate an underlying issue requiring professional dental attention. Delaying treatment can lead to more severe infections, tooth loss, and higher costs.
- Common Causes: The most frequent culprits include poor oral hygiene leading to gingivitis or periodontitis, dental abscesses, trauma, and certain systemic conditions or medications.
- Treatment Varies Widely: Depending on the cause, treatments can range from professional dental cleanings (scaling and root planing) to antibiotics, root canal therapy, or even surgery.
- Cost Considerations: Treatment costs in the US can vary significantly:
- Professional Cleaning (Prophylaxis): $75 - $200 (without insurance).
- Deep Cleaning (Scaling & Root Planing): $200 - $600 per quadrant (without insurance).
- Antibiotics: $10 - $100 (prescription cost).
- Dental Abscess Drainage: $75 - $250 (often part of a larger procedure).
- Root Canal Therapy: $700 - $2,000 per tooth (without insurance, varies by tooth location).
- Tooth Extraction: $150 - $450 for simple extraction, $250 - $800 for surgical extraction.
- Insurance Coverage: Most dental insurance plans (PPO, HMO) cover a significant portion of diagnostic and preventive care (e.g., cleanings, X-rays) and 50-80% of basic restorative procedures like fillings or deep cleanings. Major procedures like root canals or extractions usually have 30-50% coverage.
- Prevention is Paramount: Consistent and effective oral hygiene (brushing twice daily, flossing once daily), regular dental check-ups, and a healthy lifestyle are your best defense against gum swelling and pain.
- Immediate Action for Emergencies: Seek immediate dental care for severe pain, fever, facial swelling, difficulty swallowing, or if a tooth has been knocked out.
What It Is / Overview
Gum swelling, medically known as gingival edema, refers to an abnormal enlargement or inflammation of the gum tissue surrounding your teeth. This swelling is often accompanied by pain, a discomforting sensation that can range from a dull ache to a sharp, throbbing pain. Together, gum swelling and pain are classic indicators of an underlying inflammatory or infectious process affecting your periodontal tissues – the structures that support your teeth.

When your gums swell, they may appear redder than usual, puffy, shiny, and may bleed easily, especially during brushing or flossing. The pain can be localized to a single tooth or area of the gum, or it can be generalized throughout the mouth. These symptoms are essentially your body's immune response to an irritant, bacterial infection, or trauma. The increased blood flow and fluid accumulation in the tissue are part of this protective mechanism, but when prolonged or severe, they signal a problem that needs professional intervention. Understanding the "what" behind these symptoms is the first step toward effective treatment and maintaining long-term oral health.
Types / Variations
Gum swelling and pain can manifest in various ways, often indicating different underlying causes and requiring specific approaches to treatment. Differentiating between these types is crucial for accurate diagnosis.
Localized vs. Generalized Swelling
- Localized Swelling: This affects a specific area, often around one tooth or a small group of teeth. It might indicate a dental abscess (an infection at the root of a tooth or in the gum tissue), an impacted tooth, a foreign object lodged in the gum (like a popcorn kernel), or trauma to a specific spot. The pain associated is typically confined to that area.
- Generalized Swelling: This involves swelling of the gums throughout the mouth or a larger section, such as an entire arch (upper or lower). This is commonly seen in widespread gum diseases like gingivitis or periodontitis, systemic conditions, or drug-induced gingival overgrowth. The pain might be more diffuse or described as a general tenderness.
Acute vs. Chronic Pain
- Acute Pain: Characterized by a sudden onset and often severe intensity. Acute gum pain can arise from an abscess, trauma (like a tooth knocked out incident), or an acute flare-up of an existing condition. It demands immediate attention as it usually signifies an active and potentially rapidly progressing issue.
- Chronic Pain: This refers to persistent pain that lasts for weeks, months, or even longer. It might be less severe than acute pain but is constant and debilitating. Chronic gum pain is frequently associated with long-standing gum disease (periodontitis), poorly fitting dental restorations, or systemic issues that cause ongoing inflammation.
Related Conditions Causing Swelling and Pain
The specific appearance and associated symptoms of gum swelling and pain are often direct clues to the underlying condition:
- Gingivitis: The mildest form of gum disease, characterized by red, swollen, and easily bleeding gums, often with minimal pain. It's caused by plaque buildup.
- Periodontitis: An advanced form of gum disease where the infection spreads below the gum line, damaging the bone and tissues supporting the teeth. Swelling is more pronounced, and pain can be significant, often accompanied by gum recession, pus, and loose teeth.
- Dental Abscess: A localized collection of pus, usually caused by a bacterial infection. It can be periapical (at the tip of the tooth root) or periodontal (in the gum tissue). The swelling is typically a distinct, painful bump, often accompanied by throbbing pain, fever, and facial swelling.
- Impacted Tooth: When a tooth, most commonly a wisdom tooth, fails to fully erupt through the gum line, the overlying gum can become inflamed, swollen, and painful (pericoronitis).
- Trauma: Physical injury to the gums, such as aggressive brushing, a burn, or a foreign object embedding itself, can cause localized swelling and pain. In cases where a tooth is knocked out, surrounding gum tissue will be bruised and swollen.
- Oral Cancer: Less common, but persistent, unexplained swelling or a lesion on the gum that doesn't heal can be a sign of oral cancer. This often presents without significant pain initially.
- Medication-Induced Gingival Overgrowth: Certain medications can cause the gum tissue to grow excessively, leading to generalized swelling and difficulty with hygiene, increasing the risk of inflammation and pain.
- Systemic Diseases: Conditions like diabetes, Crohn's disease, or specific autoimmune disorders can manifest with oral symptoms including gum inflammation and swelling.
- TMJ Disorders: While primarily affecting the jaw joint, severe temporomandibular joint (TMJ) dysfunction can sometimes lead to referred pain that patients perceive as gum or tooth pain. Swelling directly from TMJ disorders usually occurs in the area of the jaw joint itself, which is located just in front of the ear, not directly on the gums. However, chronic clenching and grinding associated with TMJ can put undue stress on teeth and gums, potentially exacerbating or indirectly contributing to gum irritation or pain. What does TMJ swelling look like? Swelling related to TMJ issues would appear as puffiness or tenderness on the side of the face, specifically around the jaw joint and cheekbone area, rather than the gum line.
Causes / Why It Happens
Understanding the root causes of gum swelling and pain is paramount for effective treatment and prevention. These symptoms are usually indicators that something in your oral environment or overall health has gone awry.
Poor Oral Hygiene (The Primary Culprit)
The most common reason for gum swelling and pain stems from inadequate oral hygiene.
- Plaque Buildup: A sticky film of bacteria constantly forms on your teeth. If not removed by regular brushing and flossing, plaque irritates the gum tissue.
- Tartar (Calculus): When plaque hardens, it turns into tartar. Tartar is porous and creates a rough surface that harbors more bacteria, making it even harder to clean.
- Gingivitis: This is the earliest stage of gum disease, caused by plaque and tartar accumulation. The gums become inflamed, red, swollen, and bleed easily. Pain is usually mild at this stage.
- Periodontitis: If gingivitis is left untreated, it progresses to periodontitis. The inflammation spreads deeper, forming pockets between the teeth and gums where bacteria thrive. This leads to breakdown of the bone and connective tissue supporting the teeth, resulting in more severe swelling, significant pain, and potential tooth loss.
Infections Beyond Gum Disease
- Dental Abscess: A localized bacterial infection.
- Periapical Abscess: Occurs at the tip of the tooth root, often due to an untreated cavity, crack, or trauma that allows bacteria to enter the pulp (nerve) of the tooth. The infection can spread to the surrounding bone and gum, causing a painful, localized swelling (often called a "gum boil").
- Periodontal Abscess: Occurs within the gum tissue itself, usually in a periodontal pocket of someone with existing gum disease. Food or bacteria get trapped in the pocket, leading to infection, swelling, and severe localized pain.
- Viral Infections: Viruses like Herpes simplex virus (HSV) can cause cold sores or herpetic gingivostomatitis, which can lead to widespread painful sores and gum inflammation.
- Fungal Infections: Oral candidiasis (thrush) can cause white patches and sometimes generalized gum redness and discomfort, though swelling is less common.
Trauma and Injury
- Accidental Injury: A hard fall, a sports injury, or biting down on something hard can damage gum tissue, leading to localized swelling and pain.
- Aggressive Brushing/Flossing: Brushing too hard or using an incorrect flossing technique can injure the gums, causing irritation, bleeding, and mild swelling.
- Ill-fitting Dental Appliances: Dentures, partials, braces, or retainers that don't fit correctly can rub against the gums, creating pressure sores, inflammation, and pain.
- Food Impaction: A piece of food (e.g., popcorn kernel, seed) lodged between a tooth and the gum can cause irritation, inflammation, and localized swelling.
- Dental Procedures: Post-operative swelling and mild pain are common after procedures like extractions, deep cleanings, or gum surgery. This is typically temporary.
- Tooth Knocked Out: If a tooth is avulsed, the trauma to the surrounding socket and gum tissue will cause significant swelling, bruising, and pain. This is a severe dental emergency.
Systemic Conditions and Medications
- Hormonal Changes: Fluctuations in hormones, such as during pregnancy, puberty, menstruation, or menopause, can make gums more sensitive to plaque and prone to inflammation and swelling (pregnancy gingivitis is common).
- Diabetes: Individuals with uncontrolled diabetes are more susceptible to infections, including gum disease, which can be more severe and harder to manage.
- Autoimmune Diseases: Conditions like Crohn's disease, lupus, or Sjogren's syndrome can sometimes manifest with oral symptoms, including gum inflammation.
- Nutritional Deficiencies: Severe vitamin C deficiency (scurvy) can lead to bleeding, swollen gums.
- Medications: Certain drugs can cause gingival hyperplasia (overgrowth of gum tissue). These include:
- Phenytoin: An anti-seizure medication.
- Cyclosporine: An immunosuppressant.
- Calcium Channel Blockers: Used for high blood pressure and heart conditions (e.g., nifedipine, amlodipine). The enlarged gums can become more difficult to clean, leading to secondary inflammation and pain.
Other Causes
- Impacted Teeth: As mentioned, wisdom teeth attempting to erupt but getting stuck can cause pericoronitis, leading to swelling and severe pain in the back of the jaw.
- Oral Cancer: Though less common, a persistent, non-healing sore or swelling on the gums that may or may not be painful should always be evaluated by a dentist to rule out oral cancer.
Signs and Symptoms
Recognizing the signs and symptoms of gum swelling and pain is crucial for early detection and timely intervention. While pain is often the most noticeable symptom, other visual and tactile clues can help you understand the severity and potential cause of the problem.
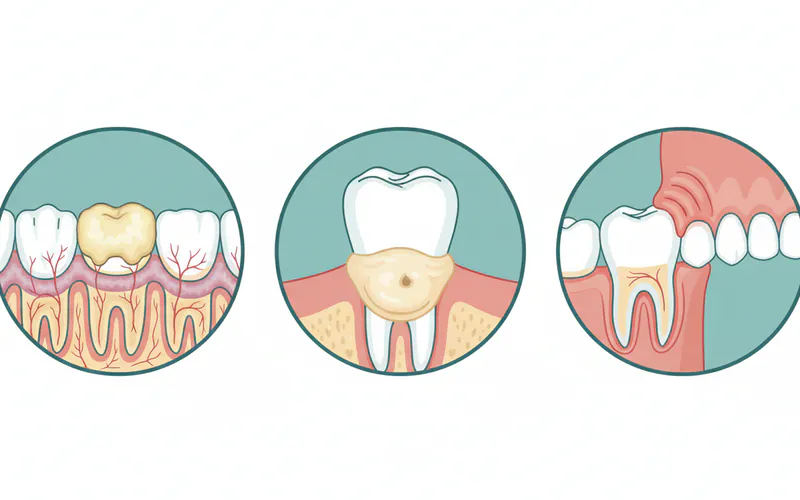
Visual Signs (What You See)
- Redness: Healthy gums are typically pink. Inflamed gums will appear reddish, sometimes even purplish-red, due to increased blood flow.
- Swelling/Puffiness (Edema): The gums may look enlarged, puffy, or bulbous instead of firm and tight around the teeth. This swelling can be localized (a single bump) or generalized.
- Shiny Appearance: Swollen gums can sometimes have a shiny, stretched appearance due to fluid accumulation.
- Bleeding Gums: Gums that bleed easily during brushing, flossing, or even spontaneously are a classic sign of inflammation, particularly gingivitis or periodontitis.
- Pus: The presence of pus, often visible as a yellowish or whitish discharge from the gum line or a swollen bump, is a clear indicator of an active infection or abscess.
- Gum Recession: In advanced gum disease (periodontitis), the gums may pull away from the teeth, making the teeth appear longer. This also exposes sensitive root surfaces.
- Changes in Gum Contour: Healthy gums have a scalloped edge. Swollen gums might lose this defined contour, becoming blunted or rolled.
- Facial Swelling: If the infection is severe and has spread, you might notice swelling in your cheek or jaw area, potentially accompanied by difficulty opening your mouth fully.
Sensory Signs (What You Feel)
- Pain/Tenderness: The most obvious symptom. This can range from a dull ache to a sharp, throbbing, or shooting pain. It might be constant or intermittent, and can worsen with chewing or touching.
- Sensitivity: Increased sensitivity to hot, cold, or sweet foods and drinks, especially if gum recession has exposed tooth roots.
- Bad Breath (Halitosis): Persistent bad breath or a foul taste in your mouth, often due to the presence of bacteria and infection.
- Metallic Taste: Some people report a metallic taste in their mouth, particularly with gum inflammation or infection.
- Loose Teeth: In advanced periodontitis, the supporting bone and ligaments are damaged, leading to teeth becoming mobile.
- Difficulty Chewing: Pain and swelling can make chewing uncomfortable or impossible, especially on the affected side.
Systemic Signs (Whole Body Effects)
- Fever: A low-grade or high fever can indicate a significant infection (e.g., a spreading dental abscess).
- Swollen Lymph Nodes: Enlarged and tender lymph nodes in the neck or under the jaw are a common sign that your body is fighting an infection.
- Fatigue/Malaise: A general feeling of being unwell or tired can accompany systemic infections.
- Headache: Sometimes, dental pain, especially from an abscess or impacted wisdom tooth, can radiate to cause headaches.
Pro Tip: Pay close attention to the duration and intensity of your symptoms. While a little tenderness after aggressive flossing might resolve quickly, persistent pain, increasing swelling, or the presence of pus are urgent warning signs that require professional dental evaluation.
Treatment Options
The treatment for gum swelling and pain is entirely dependent on the underlying cause. A thorough dental examination and diagnosis are crucial before any treatment can begin. Your dentist will assess your oral health, take X-rays, and determine the most appropriate course of action.
Home Care and Over-the-Counter Relief (Temporary Measures)
For mild, temporary irritation or as a first step before seeing a dentist:
- Saltwater Rinses: Rinse your mouth several times a day with a warm saltwater solution (1/2 teaspoon of salt in 8 ounces of warm water). This can help reduce inflammation, soothe irritated tissues, and cleanse the area.
- Over-the-Counter Pain Relievers: Ibuprofen (Advil, Motrin) or acetaminophen (Tylenol) can help manage pain and reduce inflammation. Always follow dosage instructions.
- Cold Compress: Applying a cold compress to the outside of your cheek can help reduce swelling and numb the area, especially if there's external facial swelling.
- Soft Diet: Avoid hard, crunchy, or acidic foods that might further irritate swollen gums.
- Gentle Brushing/Flossing: While it's important to continue oral hygiene, use a soft-bristled brush and be gentle around the affected area to avoid further trauma.
Pro Tip: Home remedies are for temporary relief and are not a substitute for professional dental care, especially for persistent or severe symptoms.
Professional Dental Treatments
Once the cause is identified, a dentist or periodontist will recommend specific treatments.
-
Professional Dental Cleaning (Prophylaxis):
- What it is: A routine cleaning that removes plaque and tartar from above the gum line.
- When used: For mild gingivitis, to prevent gum disease, or as part of regular maintenance.
- Pros: Non-invasive, quick, prevents progression of gum disease.
- Cons: Not sufficient for advanced gum disease or deep infections.
-
Scaling and Root Planing (Deep Cleaning):
- What it is: A non-surgical procedure where special instruments are used to remove plaque and tartar from both above and below the gum line, and smooth the root surfaces to prevent bacterial reattachment. Often performed under local anesthesia.
- When used: For moderate periodontitis where periodontal pockets have formed.
- Pros: Effectively removes deep-seated bacteria, reduces inflammation, can halt the progression of gum disease.
- Cons: Can cause temporary sensitivity and soreness; may require multiple appointments.
-
Antibiotics:
- What it is: Oral antibiotics (e.g., amoxicillin, clindamycin, metronidazole) or topical antibiotics (e.g., doxycycline gel, chlorhexidine rinse).
- When used: For acute infections, dental abscesses, or as an adjunct to deep cleaning for aggressive periodontitis.
- Pros: Directly combats bacterial infection, reduces swelling and pain.
- Cons: Potential side effects (nausea, diarrhea), can contribute to antibiotic resistance if overused.
-
Dental Abscess Drainage:
- What it is: Incision and drainage of pus from a localized abscess. This involves making a small cut in the swollen area to allow the pus to drain, relieving pressure and pain.
- When used: For a mature dental abscess (periapical or periodontal).
- Pros: Provides immediate pain relief, removes infection.
- Cons: May require follow-up treatment (e.g., root canal, extraction) to address the source of the infection.
-
Root Canal Therapy:
- What it is: A procedure to remove infected or damaged pulp from inside a tooth, clean and disinfect the internal canals, and then fill and seal them. A crown is usually placed afterwards.
- When used: For a periapical abscess where the tooth's pulp is infected or necrotic.
- Pros: Saves the natural tooth, eliminates the source of infection.
- Cons: Can be time-consuming, requires a crown; sometimes the tooth may still fail later.
-
Tooth Extraction:
- What it is: Surgical removal of a tooth.
- When used: For severely damaged, infected, or non-restorable teeth, or impacted wisdom teeth causing pericoronitis.
- Pros: Eliminates the source of infection/pain definitively.
- Cons: Permanent tooth loss, may require replacement (implant, bridge) later, which adds cost and complexity.
-
Gum Surgery (Periodontal Surgery):
- What it is: Various surgical procedures for advanced periodontitis. Examples include:
- Flap Surgery (Pocket Reduction Surgery): Gums are lifted back, tartar is removed, and irregular bone surfaces are smoothed before reattaching the gums.
- Gingivectomy: Removal of excess gum tissue, often for drug-induced gingival overgrowth or to reshape gums.
- Bone and Tissue Grafts: Used to regenerate lost bone or gum tissue due to periodontitis.
- When used: For severe periodontitis where non-surgical treatments are insufficient.
- Pros: Can halt advanced gum disease, save teeth, improve aesthetics.
- Cons: More invasive, longer recovery, higher cost, potential for post-operative discomfort and sensitivity.
- What it is: Various surgical procedures for advanced periodontitis. Examples include:
-
Management of TMJ Disorders:
- What it is: If gum pain is referred from TMJ, treatment focuses on the jaw joint. This may include custom-made oral splints or nightguards to prevent clenching/grinding, physical therapy, muscle relaxants, or in severe cases, surgery.
- When used: When TMJ is diagnosed as the primary or contributing factor to pain that might be perceived in the gums.
- Pros: Addresses the root cause of TMJ-related discomfort.
- Cons: May not directly resolve gum inflammation if other causes are also present.
Comparison of Common Treatments for Gum Swelling and Pain
| Treatment Option | Primary Indication | Procedure Overview | Typical Duration | Average US Cost (Without Insurance) | Recovery Time |
|---|---|---|---|---|---|
| Professional Cleaning | Mild gingivitis, prevention | Scaling above gum line, polishing teeth. | 30-60 min | $75 - $200 | None |
| Scaling & Root Planing | Moderate periodontitis, deep pockets | Deep cleaning above/below gum line, root smoothing (often 1-4 quadrants). | 1-2 hours per q | $200 - $600 per quadrant | 1-3 days soreness |
| Antibiotics (Oral) | Acute infection, abscess, severe gingivitis | Oral medication taken for 7-14 days. | N/A | $10 - $100 | N/A |
| Abscess Drainage | Localized dental abscess | Incision, pus drainage. | 15-30 min | $75 - $250 (plus follow-up) | 1-2 days discomfort |
| Root Canal Therapy | Infected tooth pulp, periapical abscess | Remove pulp, clean/fill canals (usually followed by a crown). | 1-2 hours | $700 - $2,000 | 2-5 days sensitivity |
| Simple Tooth Extraction | Non-restorable tooth, severe infection | Tooth removal with forceps. | 15-30 min | $150 - $450 | 3-7 days |
| Periodontal Surgery | Advanced periodontitis, extensive bone loss | Lifting gum flaps, debridement, bone reshaping, grafting. | 1-2 hours+ | $500 - $3,000+ per quadrant | 1-2 weeks significant |
Step-by-Step Process (Focus on Scaling and Root Planing)
Let's detail the process for a common treatment: Scaling and Root Planing (deep cleaning), which is often recommended for gum swelling and pain caused by moderate periodontitis.

- Diagnosis and Treatment Planning: Your dentist or periodontist will first examine your gums, measure pocket depths around your teeth, take X-rays, and review your medical history to confirm the diagnosis of periodontitis and determine if deep cleaning is appropriate. They will explain the procedure and answer any questions.
- Anesthesia: Before starting, a local anesthetic will be administered to numb the specific areas of your mouth that will be treated. This ensures you are comfortable and don't feel pain during the procedure. Depending on the extent of gum disease, the deep cleaning may be performed over two or more appointments, treating one or two quadrants of your mouth at a time.
- Scaling: Using specialized hand instruments (scalers and curettes) and often an ultrasonic scaler, the hygienist or dentist will meticulously remove plaque, calculus (tartar), and bacterial toxins from the tooth surfaces, both above and below the gum line. This includes deep within the periodontal pockets that have formed. You might feel some pressure but shouldn't experience pain due to the anesthetic.
- Root Planing: After scaling, the root surfaces of your teeth are planed (smoothed). This process removes any remaining bacterial toxins and rough spots on the roots, making it more difficult for plaque to reattach and promoting the healing and reattachment of gum tissue to the roots.
- Irrigation (Optional): Some practitioners may irrigate the periodontal pockets with an antimicrobial solution (e.g., chlorhexidine) to further reduce bacteria.
- Medication Placement (Optional): In some cases, a localized antibiotic medication (e.g., Arestin, Atridox) might be placed directly into deep periodontal pockets to provide sustained antimicrobial action.
- Post-Procedure Instructions: Once the deep cleaning is complete, your dental professional will provide detailed aftercare instructions covering pain management, dietary recommendations, oral hygiene techniques, and what to expect during the healing process.
- Follow-up Appointments: A follow-up appointment is typically scheduled a few weeks after the deep cleaning to assess healing, re-measure pocket depths, and discuss further maintenance (often called periodontal maintenance or recall cleanings), which are usually more frequent than standard prophylactic cleanings.
This detailed approach to scaling and root planing is highly effective in managing and often reversing the progression of moderate gum disease, significantly reducing gum swelling and pain.
Cost and Insurance
Understanding the financial aspect of treating gum swelling and pain is crucial for patients in the US. Costs can vary significantly based on the severity of the condition, the type of treatment needed, the geographical location of the dental practice, and whether you have dental insurance.
Average US Price Ranges (Without Insurance)
Here's a breakdown of common procedures related to gum swelling and pain:
- Initial Exam & X-rays: $50 - $200 (for new patients, includes comprehensive exam and necessary X-rays).
- Professional Cleaning (Prophylaxis): $75 - $200. This is for healthy gums or very mild gingivitis.
- Scaling and Root Planing (Deep Cleaning): This is typically charged per quadrant (a quarter of your mouth).
- Per Quadrant: $200 - $600.
- Full Mouth (4 Quadrants): $800 - $2,400.
- Antibiotics (Prescription): $10 - $100. This is for the medication itself, not the office visit.
- Dental Abscess Drainage: $75 - $250. This is often an emergency procedure, and the cost might be higher if it's done outside of regular hours or if it's part of a larger treatment plan (e.g., leading to a root canal).
- Root Canal Therapy:
- Front Tooth (incisor/canine): $700 - $1,200.
- Premolar (bicuspid): $800 - $1,500.
- Molar: $1,000 - $2,000+.
- Note: These costs do not include the post-and-core or dental crown that is almost always required after a root canal, which can add another $800 - $2,500.
- Tooth Extraction:
- Simple Extraction: $150 - $450 (for a visible, easily removable tooth).
- Surgical Extraction: $250 - $800 (for impacted teeth, fractured teeth, or those requiring bone removal).
- Periodontal Surgery (e.g., Flap Surgery): $500 - $3,000+ per quadrant, depending on complexity and whether bone grafting is needed.
Factors Affecting Cost:
- Geographic Location: Costs are typically higher in metropolitan areas and on the coasts.
- Dentist's Experience/Specialty: Specialists (e.g., periodontists, endodontists) often charge more than general dentists.
- Technology Used: Practices using advanced technology may have higher fees.
- Severity of Condition: More advanced disease requires more extensive (and expensive) treatment.
Dental Insurance Coverage Details
Most dental insurance plans in the US follow a "100-80-50" coverage model:
- Preventive Care (100% Coverage): This typically includes routine exams, X-rays (often once a year or every 6 months), and professional cleanings (usually two per year). Many plans cover these at 100% with no deductible.
- Basic Restorative Procedures (80% Coverage): This category often includes fillings, simple extractions, and scaling and root planing. You would typically pay 20% of the cost after meeting your deductible.
- Major Procedures (50% Coverage): This includes more complex treatments like root canals, crowns, bridges, dentures, and periodontal surgery. You would typically pay 50% of the cost after meeting your deductible.
Types of Plans:
- PPO (Preferred Provider Organization): Offers a network of dentists with negotiated rates. You can go out of network, but you'll pay more. Most common plan.
- HMO (Health Maintenance Organization): Requires you to choose a primary dentist from a network, and referrals are often needed for specialists. Typically has lower premiums but less flexibility.
- Medicaid & CHIP: Government programs providing dental benefits for low-income individuals and children. Coverage varies by state but generally includes basic and some major services for children, with more limited adult coverage.
- Discount Plans: Not insurance, but offer a discount on services from participating dentists. You pay an annual fee for access to these reduced rates.
Pro Tip: Always verify your specific coverage with your insurance provider before undergoing treatment. Ask your dental office for a detailed treatment plan with estimated costs and your expected out-of-pocket expenses.
Comparison Table: US Dental Procedure Costs (Estimates without Insurance)
| Procedure | Low Range | Mid Range | High Range | Common Insurance Coverage Level (after deductible) |
|---|---|---|---|---|
| Dental Exam & X-rays | $50 | $120 | $200 | 100% (Preventive) |
| Standard Cleaning (Prophylaxis) | $75 | $125 | $200 | 100% (Preventive) |
| Scaling & Root Planing (per quadrant) | $200 | $400 | $600 | 80% (Basic Restorative) |
| Dental Abscess Drainage | $75 | $150 | $250 | 80% (Basic Restorative) |
| Simple Tooth Extraction | $150 | $300 | $450 | 80% (Basic Restorative) |
| Root Canal (Molar) | $1,000 | $1,500 | $2,000+ | 50% (Major) |
| Periodontal Flap Surgery (per quadrant) | $500 | $1,500 | $3,000+ | 50% (Major) |
Recovery and Aftercare
Proper recovery and diligent aftercare are essential for optimal healing and to prevent recurrence of gum swelling and pain, regardless of the treatment you received. Your dental professional will provide specific instructions, but here are general guidelines.
After Scaling and Root Planing (Deep Cleaning)
- Pain and Discomfort: Expect mild to moderate soreness and sensitivity for a few days. OTC pain relievers (ibuprofen, acetaminophen) are usually sufficient.
- Bleeding: Slight bleeding from the gums for the first 24 hours is normal.
- Sensitivity: Teeth may be sensitive to hot, cold, or sweets for a few days to several weeks, as root surfaces are exposed. Your dentist might recommend a desensitizing toothpaste.
- Oral Hygiene: Continue brushing gently with a soft-bristled brush. Floss carefully. Your dentist may recommend an antimicrobial mouthwash (like chlorhexidine) for a short period.
- Diet: Stick to soft foods for the first few days (e.g., yogurt, soup, mashed potatoes). Avoid very hot, cold, spicy, or crunchy foods.
- Avoid: Smoking and alcohol for at least 24-48 hours, as they can impede healing.
- Follow-up: Attend all scheduled follow-up appointments (typically 4-6 weeks after treatment) for evaluation and ongoing periodontal maintenance.
After Abscess Drainage or Extraction
- Pain Management: Pain medication prescribed by your dentist or strong OTC pain relievers will be necessary.
- Swelling: Expect some facial swelling, especially for extractions or larger abscesses. Apply an ice pack to the outside of your cheek for 20 minutes on, 20 minutes off, for the first 24-48 hours.
- Bleeding: Some oozing of blood is normal. Bite gently on a gauze pad, changing it every 30-45 minutes until bleeding stops.
- Oral Hygiene: Avoid brushing directly on the surgical site for the first 24 hours. Gentle saltwater rinses (after 24 hours) can help keep the area clean. Avoid vigorous rinsing or spitting.
- Diet: Consume soft, cool foods and liquids for several days. Avoid using straws as the suction can dislodge blood clots (leading to dry socket after extraction).
- Rest: Get plenty of rest to aid healing.
- Avoid: Smoking, alcohol, and strenuous exercise for at least 48-72 hours.
- Follow-up: Attend your follow-up appointment to ensure proper healing and address any concerns.
After Root Canal Therapy
- Pain/Sensitivity: Mild pain or sensitivity is common for a few days, particularly when biting down. OTC pain relievers are usually sufficient.
- Temporary Filling/Crown: You will likely have a temporary filling or crown. Be gentle when chewing on this tooth until the permanent restoration is placed.
- Permanent Restoration: It is critical to get a permanent filling or crown placed promptly after a root canal (usually within a few weeks) to protect the treated tooth from fracture and re-infection.
- Oral Hygiene: Continue your regular brushing and flossing routines.
- Avoid: Chewing hard or sticky foods on the temporary restoration.
Pro Tip: Always follow your dentist's specific post-operative instructions carefully. If you experience excessive bleeding, severe uncontrolled pain, increasing swelling after 48 hours, or fever, contact your dentist immediately.
Prevention
Preventing gum swelling and pain primarily revolves around excellent oral hygiene and regular professional dental care. Adhering to these practices is your best defense against most causes.
1. Maintain Excellent Oral Hygiene
- Brush Twice Daily: Use a soft-bristled toothbrush and fluoride toothpaste. Brush for at least two minutes each time, covering all surfaces of your teeth and gently along the gum line. The ADA recommends replacing your toothbrush every 3-4 months, or sooner if the bristles are frayed.
- Floss Daily: Flossing is crucial for removing plaque and food particles from between teeth and under the gum line, areas your toothbrush can't reach. Use about 18 inches of floss, curving it around each tooth in a 'C' shape.
- Use Antimicrobial Mouthwash: While not a substitute for brushing and flossing, an ADA-accepted antiseptic mouthwash can help reduce bacteria and plaque. Ask your dentist if it's right for you.
- Tongue Cleaning: Gently brush or scrape your tongue to remove bacteria that can contribute to bad breath and oral infections.
2. Regular Dental Check-ups and Cleanings
- Schedule Every Six Months: Professional dental cleanings remove plaque and tartar buildup that you can't remove at home. Your dentist can also identify early signs of gum disease, cavities, and other oral health issues before they become serious.
- Periodontal Maintenance: If you've had gum disease, your dentist or periodontist may recommend more frequent cleanings (e.g., every 3-4 months) to manage the condition and prevent recurrence.
3. Adopt a Healthy Lifestyle
- Balanced Diet: Eat a diet rich in fruits, vegetables, and whole grains. Limit sugary snacks and drinks, which feed bacteria and contribute to plaque formation.
- Stay Hydrated: Drinking plenty of water helps wash away food particles and keeps your mouth moist, which is essential for saliva production and bacterial control.
- Avoid Tobacco Products: Smoking and chewing tobacco are significant risk factors for gum disease, impairing healing and making infections harder to fight. Quitting tobacco is one of the most impactful steps you can take for your oral and overall health.
- Manage Systemic Conditions: If you have conditions like diabetes, ensure they are well-managed. Work with your doctor to control blood sugar levels, as this directly impacts your susceptibility to and severity of gum disease.
- Stress Management: Chronic stress can weaken your immune system, making you more vulnerable to infections. Stress can also lead to teeth grinding or clenching (bruxism), which can exacerbate TMJ issues and put undue pressure on teeth and gums.
4. Address Specific Risks
- Wear a Mouthguard: If you grind or clench your teeth at night, a custom-fitted nightguard can protect your teeth and jaw joints, potentially alleviating related gum sensitivity.
- Proper Dental Appliances: Ensure dentures, partials, or other dental appliances fit properly. Ill-fitting devices can irritate gums and lead to swelling and sores.
- Medication Review: If you are on medications known to cause gingival overgrowth, discuss this with your doctor and dentist. Regular professional cleanings and diligent home care become even more critical.
By diligently following these preventive measures, you can significantly reduce your risk of developing gum swelling and pain and maintain a healthy, comfortable smile for years to come.
Risks and Complications
Ignoring gum swelling and pain, or delaying professional treatment, carries significant risks and can lead to a range of severe complications that extend beyond your mouth.
Local Oral Complications
- Progression of Gum Disease: Untreated gingivitis will almost certainly advance to periodontitis. This leads to the destruction of the bone and soft tissues supporting your teeth, eventually causing:
- Tooth Mobility and Loss: As bone is lost, teeth become loose and may eventually fall out or require extraction.
- Gum Recession: Gums pull away from the teeth, exposing sensitive roots and making teeth appear longer.
- Spread of Infection:
- Dental Abscesses: Untreated gum infections or cavities can lead to the formation of painful abscesses, which can cause significant localized swelling, severe pain, and sometimes a fever.
- Osteomyelitis: If a dental infection spreads to the jawbone, it can cause osteomyelitis, a serious bone infection that requires aggressive treatment.
- Cellulitis: A rapidly spreading bacterial infection of the soft tissues of the face and neck. This is a life-threatening emergency, potentially leading to airway obstruction or spread to vital organs.
- Impact on Adjacent Teeth: Infections can spread from one tooth or gum area to neighboring teeth, affecting their health and stability.
- Chronic Pain: Persistent, untreated inflammation can lead to chronic oral pain, impacting quality of life, eating, and speaking.
- Bad Breath: Chronic infections and plaque buildup are major contributors to persistent bad breath (halitosis).
Systemic Health Complications
The link between oral health and overall systemic health is well-established. Untreated gum infections can have far-reaching effects:
- Cardiovascular Disease: The bacteria and inflammation from periodontitis can enter the bloodstream, contributing to the development or worsening of heart disease, including atherosclerosis (hardening of the arteries), endocarditis (infection of the heart's inner lining), and stroke.
- Diabetes Management: Periodontitis can make it harder to control blood sugar levels in individuals with diabetes, creating a vicious cycle where gum disease worsens diabetes and vice-versa.
- Respiratory Diseases: Oral bacteria can be aspirated into the lungs, potentially leading to pneumonia or exacerbating existing respiratory conditions like COPD.
- Pregnancy Complications: Pregnant women with severe periodontitis have a higher risk of preterm birth and low birth weight babies.
- Other Conditions: Links have also been suggested between gum disease and rheumatoid arthritis, kidney disease, certain cancers, and even Alzheimer's disease.
Pro Tip: Early intervention is key. If you experience persistent gum swelling and pain, do not ignore it. Prompt dental care can prevent these serious and often costly complications. Your oral health is an integral part of your total health.
Children / Pediatric Considerations
Gum swelling and pain in children can be particularly distressing for both the child and parents. While many causes overlap with adults, there are several age-specific considerations for pediatric cases.
Common Causes in Children
- Teething: One of the most common causes of gum inflammation in infants and toddlers is teething. As teeth erupt, the gums can become red, swollen, and tender, causing discomfort and irritability.
- Poor Oral Hygiene: Just like adults, children can develop gingivitis due to inadequate brushing and flossing. Accumulation of plaque, especially around newly erupted molars, can lead to swollen, bleeding gums.
- Dental Caries (Cavities): Untreated cavities can lead to tooth infections and abscesses, which manifest as localized gum swelling (often a "gum boil") and pain, sometimes with facial swelling.
- Trauma: Children are prone to falls and accidents. A blow to the mouth can cause gum bruising, swelling, and potential damage to teeth, including a tooth knocked out (avulsion) or fractured. Even minor trauma from aggressive brushing can irritate gums.
- Erupting Teeth (Beyond Teething): As permanent teeth erupt, especially molars or wisdom teeth in older children/teens, the overlying gum tissue can become inflamed and painful (pericoronitis), similar to impacted wisdom teeth in adults.
- Herpetic Gingivostomatitis: A common viral infection (often primary herpes simplex virus infection) in young children. It causes widespread painful sores in the mouth, including severe gum swelling and redness, often accompanied by fever and difficulty eating/drinking.
- Thumb Sucking/Pacifier Use: Prolonged or aggressive non-nutritive sucking habits can sometimes cause irritation or changes in gum contour, potentially leading to inflammation.
- Food Impaction: Small food particles (e.g., popcorn hulls, seeds) can get lodged in the gum line, causing localized inflammation and pain.
- Orthodontic Appliances: Braces and retainers can sometimes rub against or irritate gum tissue, leading to localized swelling or sores.
What Parents Should Look For
- Visual Changes: Red, puffy gums; bleeding when brushing; a specific bump or blister (abscess); white sores; or signs of physical injury.
- Behavioral Cues: Irritability, refusing to eat or drink, difficulty sleeping, unusual fussiness.
- Systemic Signs: Fever, swollen lymph nodes, facial swelling (especially one-sided).
- Oral Hygiene Challenges: If the child resists brushing or flossing, or you notice persistent plaque.

When to See a Pediatric Dentist
- Persistent Symptoms: If gum swelling and pain last more than a few days, even with home remedies.
- Severe Pain: If the child is in significant distress or cannot eat/drink.
- Signs of Infection: Fever, facial swelling, pus, or a distinct "gum boil."
- Trauma: Immediately after any mouth injury, especially if a tooth is loose, fractured, or knocked out.
- Difficulty Breathing/Swallowing: These are emergency signs.
Pro Tip for Parents: Establish good oral hygiene habits early. Brush your child's teeth twice a day from the appearance of the first tooth. Schedule their first dental visit by age one or within six months of the first tooth erupting, and continue with regular check-ups. Encourage a healthy diet and discourage prolonged pacifier or thumb-sucking habits.
Cost Breakdown
While specific costs were touched upon earlier, let's provide a dedicated section to emphasize the typical range of expenses for treating gum swelling and pain in the US, with a focus on out-of-pocket costs and payment options.
Average US Costs (Low, Mid, High Estimates Without Insurance)
The cost for addressing gum swelling and pain largely depends on the diagnosis:
- Initial Consultation and X-rays:
- Low: $50 (e.g., basic exam at a large dental clinic)
- Mid: $120 (e.g., comprehensive exam, few X-rays)
- High: $200 (e.g., full mouth series X-rays, specialized consult)
- Standard Dental Cleaning (Prophylaxis):
- Low: $75
- Mid: $125
- High: $200
- Scaling and Root Planing (Per Quadrant):
- Low: $200
- Mid: $400
- High: $600
- Total for Full Mouth (4 Quadrants): $800 - $2,400
- Antibiotics (Prescription Cost):
- Low: $10 (generic with discount card)
- Mid: $50
- High: $100+ (brand name, no insurance)
- Abscess Drainage (Simple):
- Low: $75
- Mid: $150
- High: $250
- Root Canal Therapy (Molar):
- Low: $1,000
- Mid: $1,500
- High: $2,000+
- Note: Excludes the cost of a dental crown ($800 - $2,500).
- Tooth Extraction (Simple vs. Surgical):
- Simple Low: $150
- Simple Mid: $300
- Simple High: $450
- Surgical Low: $250
- Surgical Mid: $500
- Surgical High: $800
With vs. Without Insurance
The presence of dental insurance can dramatically reduce your out-of-pocket expenses.
- Without Insurance: You are responsible for 100% of all costs. Many dentists offer a cash discount for upfront payment or have in-office membership plans.
- With Insurance (e.g., PPO):
- Preventive Care (Exams, Cleanings): Often covered at 100% (or very close) after meeting a small annual deductible ($0-$100).
- Basic Procedures (Scaling & Root Planing, Simple Extractions): Typically covered at 80% after deductible. If a deep cleaning costs $400 per quadrant, your insurance might pay $320, leaving you with $80 out-of-pocket (per quadrant, plus deductible).
- Major Procedures (Root Canals, Periodontal Surgery, Crowns): Usually covered at 50% after deductible. A $1,500 root canal might mean your insurance pays $750, leaving you to cover the remaining $750 (plus deductible).
- Annual Maximums: Most dental insurance plans have an annual maximum benefit, typically ranging from $1,000 to $2,000 per year. Once this limit is reached, you are responsible for 100% of subsequent costs, even if the procedure would normally be covered. This is why extensive periodontal treatment or multiple root canals can quickly exceed annual limits.
Payment Plans and Financing Options
If you face significant costs, especially without insurance or after hitting your annual maximum, several options can help:
- In-Office Payment Plans: Many dental offices offer interest-free payment plans for a few months for established patients.
- Dental Credit Cards (e.g., CareCredit, LendingClub): These are specialized healthcare credit cards that offer deferred interest plans (0% APR for a specific period if paid in full) or low-interest financing for longer terms.
- Personal Loans: Banks or credit unions offer personal loans that can be used for dental expenses.
- Health Savings Accounts (HSAs) or Flexible Spending Accounts (FSAs): If you have a high-deductible health plan, you may have an HSA. FSAs are employer-sponsored. Both allow you to set aside pre-tax money for qualified medical and dental expenses.
- Dental Schools: University dental schools often provide high-quality care at reduced rates, as treatment is performed by students under the supervision of experienced faculty.
Cost-Saving Tips
- Preventive Care: The single best way to save money is through consistent daily oral hygiene and regular check-ups. Preventing issues is always cheaper than treating them.
- Early Intervention: Addressing gum swelling and pain at its earliest stages (e.g., gingivitis) is much less expensive than treating advanced periodontitis or a severe abscess requiring extensive procedures.
- Get Multiple Quotes: For expensive procedures, it's acceptable to get a second opinion and compare cost estimates from different dentists, especially for non-emergency treatments.
- Utilize Discount Plans: If you don't have insurance, consider a dental discount plan for reduced fees.
- Negotiate: For large cash payments, some dentists may offer a small discount if you pay upfront.
Frequently Asked Questions
What causes gum swelling and pain?
Gum swelling and pain are most commonly caused by poor oral hygiene leading to plaque and tartar buildup, which results in gingivitis or periodontitis. Other causes include dental abscesses (infections), trauma, impacted teeth, certain medications, hormonal changes, and systemic diseases like diabetes.
Is gum swelling an emergency?
It depends on the severity. Mild, temporary gum swelling and tenderness might not be an immediate emergency. However, if the swelling is severe, rapidly worsening, accompanied by intense throbbing pain, pus, fever, facial swelling, difficulty swallowing, or if it results from significant trauma (like a tooth knocked out), it is a dental emergency requiring immediate professional attention.
How long does gum swelling and pain typically last?
The duration depends entirely on the cause. Swelling from mild irritation might subside within a day or two with home care. Swelling and pain from gingivitis can persist for weeks or months until a professional cleaning. If it's due to an abscess or advanced gum disease, it will likely persist and worsen until treated by a dentist, potentially lasting indefinitely.
Can home remedies cure gum swelling and pain?
Home remedies like saltwater rinses or OTC pain relievers can offer temporary symptom relief and help with minor irritation. However, they generally do not cure the underlying cause of persistent gum swelling and pain, especially if it's due to bacterial infection, advanced gum disease, or a dental abscess. Professional dental treatment is almost always necessary for a lasting solution.
What does TMJ swelling look like?
Swelling directly related to a temporomandibular joint (TMJ) disorder would appear on the side of the face, specifically around the jaw joint (just in front of the ear) or extending down the cheek. It is typically a facial swelling, not a gum swelling. While TMJ issues can cause referred pain perceived in the teeth or gums, they do not directly cause gum tissue to swell.
Can wisdom teeth cause gum swelling and pain?
Yes, absolutely. When wisdom teeth attempt to erupt but are partially or fully impacted (stuck under the gum or bone), the overlying gum tissue can become inflamed and infected. This condition, called pericoronitis, causes significant localized swelling, severe pain, and sometimes difficulty opening the mouth or chewing.
How much does it cost to treat gum swelling and pain in the US?
Costs vary widely based on the cause and treatment. A routine dental cleaning for mild gingivitis might cost $75-$200. Scaling and root planing (deep cleaning) for periodontitis can range from $200-$600 per quadrant. Treating an abscess with a root canal can cost $700-$2,000 for the tooth (plus a crown), while an extraction might be $150-$800. These are estimates without insurance.
Will dental insurance cover the cost of treatment?
Most dental insurance plans cover a portion of the costs. Preventive care (exams, cleanings) is often 100% covered. Basic procedures like scaling and root planing or simple extractions typically have 80% coverage. Major procedures like root canals or periodontal surgery are usually covered at 50%. Most plans also have an annual maximum benefit, typically $1,000-$2,000.
What happens if gum swelling and pain are left untreated?
Leaving gum swelling and pain untreated can lead to serious complications. Untreated infections can spread to other teeth, the jawbone (osteomyelitis), or even to other parts of the body (cellulitis, sepsis), which can be life-threatening. It also leads to progressive bone loss, loosening and eventual loss of teeth, and has been linked to systemic health issues like heart disease and uncontrolled diabetes.
Is it normal for gums to bleed when swollen?
Yes, bleeding gums are a very common sign of inflammation and swelling. Healthy gums typically do not bleed. If your swollen gums bleed when you brush, floss, or even spontaneously, it's a strong indicator of gingivitis or periodontitis, and you should see a dentist for evaluation.
When to See a Dentist
It's crucial to know when to seek professional dental care for gum swelling and pain. While some minor irritation might resolve on its own, many symptoms warrant a dentist's evaluation to prevent more serious complications.
Red Flags for Immediate Attention (Dental Emergency)
Contact your dentist or an emergency dental clinic right away if you experience any of the following:
- Severe, Throbbing Pain: Pain that is constant, intense, and interferes with your daily activities or sleep.
- Rapidly Worsening Swelling: If the gum swelling is increasing quickly, especially if it's accompanied by facial swelling, swelling around your eye, or in your neck.
- Difficulty Swallowing or Breathing: This indicates a severe infection that may be spreading and could compromise your airway. This is a medical emergency; go to an urgent care clinic or emergency room if a dentist isn't immediately available.
- Fever and Chills: Systemic signs of infection spreading beyond the local area.
- Pus Drainage: Visible pus coming from the gums or a swollen area.
- Extreme Tenderness to Touch: If the area is excruciatingly painful even with light touch.
- Recent Trauma: If your gum swelling and pain resulted from an injury, especially if a tooth was knocked out or severely loosened.
- Mouth Sores that Don't Heal: Any persistent sore or lesion on your gums that lasts more than two weeks should be evaluated to rule out oral cancer.
When to Schedule a Routine Appointment (Non-Emergency)
Make an appointment to see your dentist as soon as possible, but it may not require immediate emergency care, if you experience:
- Persistent Gum Swelling: Gums that remain swollen, red, or puffy for more than a few days, even if pain is mild.
- Bleeding Gums: Gums that consistently bleed during brushing or flossing.
- Dull, Persistent Ache: A mild but nagging pain in your gums or around a tooth.
- Bad Breath: Persistent bad breath that doesn't resolve with good oral hygiene.
- Metallic Taste: A new or persistent metallic taste in your mouth.
- Sensitive Teeth: New or increased sensitivity to hot, cold, or sweets, especially if accompanied by gum recession.
- Loosening Teeth: Any noticeable changes in the stability of your teeth.
Pro Tip: When in doubt, always err on the side of caution and consult with a dental professional. Early diagnosis and treatment are the most effective ways to manage gum swelling and pain, prevent complications, and protect your oral health.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
How to Relieve Gum Swelling
When your gums are swollen, it can be an alarming and uncomfortable experience, often signaling an underlying issue that requires attention. Statistics from the Centers for Disease Control and Prevention (CDC) reveal that **nearly half of adults aged 30 or older in the United States have some form o
February 23, 2026
Teeth Swelling: Complete Guide
When you experience teeth swelling, it's more than just a minor discomfort; it's a clear signal from your body that something is amiss within your oral cavity, often indicating an underlying infection or inflammation that requires prompt attention. A recent survey revealed that **over 25% of adu
February 23, 2026
Submandibular Salivary Gland Swelling: Complete Guide
When you notice a peculiar lump or uncomfortable fullness beneath your jaw, it can be an alarming experience. This sensation, often accompanied by pain and difficulty swallowing, could indicate submandibular salivary gland swelling. Affecting an estimated 1 in 10,000 adults annually, conditi
February 23, 2026
What Helps With Gum Swelling
Gum swelling, medically known as gingival swelling or gingivitis, is a common yet often underestimated dental issue affecting millions of Americans. Have you ever woken up with sore, puffy gums that bleed easily when you brush? You're not alone. Research indicates that nearly **half of all a
February 23, 2026