Swelling Gums: Complete Guide
Key Takeaways
- Have you ever woken up to find your gums puffy, tender, or even painful? You're not alone. Swelling gums are a surprisingly common issue, affecting millions of Americans each year. While often a sign of mild irritation, gum swelling can also indicate underlying serious dental or systemic health
Swelling Gums: Complete Guide
Have you ever woken up to find your gums puffy, tender, or even painful? You're not alone. Swelling gums are a surprisingly common issue, affecting millions of Americans each year. While often a sign of mild irritation, gum swelling can also indicate underlying serious dental or systemic health problems that demand immediate attention. Ignoring swollen gums can lead to discomfort, infection, tooth loss, and even broader health complications. This comprehensive guide from SmilePedia.net will delve deep into the causes, symptoms, treatments, and prevention strategies for swelling gums, empowering you to understand this condition and protect your oral and overall health. We'll cover everything from the most common culprits like gingivitis to more complex scenarios like differentiating gum swelling from a swollen submandibular gland or lymph node, and what to do if you experience a dental emergency like a knocked out tooth.
Key Takeaways:
- Common Causes: The most frequent causes of swelling gums are gingivitis and periodontitis, often due to poor oral hygiene. Other causes include abscesses, trauma, hormonal changes, and certain medical conditions.
- Emergency Indicators: Seek immediate dental care if gum swelling is accompanied by severe pain, fever, difficulty swallowing/breathing, pus, or rapidly spreading redness. A knocked out tooth also constitutes a dental emergency requiring immediate attention within 30 minutes to an hour for best replantation success.
- Cost of Treatment: Basic treatments like professional dental cleaning (scaling and root planing) range from $250-$1,500, depending on severity and number of quadrants. More complex treatments like root canal therapy can cost $700-$2,000, and gum surgery $500-$10,000+ per quadrant.
- Prevention is Key: Diligent oral hygiene (brushing twice daily, flossing once daily), regular dental check-ups (every 6 months), and a balanced diet are crucial for preventing gum swelling.
- Diagnosis is Essential: A dentist will diagnose the cause through a visual exam, probing, X-rays, and potentially other diagnostic tests. Self-diagnosis can be misleading, especially when differentiating between gum issues and other facial swellings.
- Differentiating Swelling: Gum swelling is typically localized to the gum tissue. Swelling of a submandibular gland (under the jaw) often relates to salivary gland issues, while swollen lymph nodes (neck, jawline) are usually indicative of infection or inflammation elsewhere in the body, although they can swell in response to a dental infection.
- Treatment Timelines: Mild gingivitis can resolve within 1-2 weeks with improved hygiene and professional cleaning. Periodontitis treatment can take several weeks to months, including follow-up care.
What It Is / Overview
Swelling gums, medically known as gingival swelling or gingival edema, refers to the enlargement, inflammation, or protrusion of the gum tissue surrounding the teeth. This inflammation can range from a localized puffiness affecting a single tooth to a generalized swelling impacting all gum tissue. The texture of swollen gums may appear redder than usual, be tender to the touch, and often bleed easily, especially during brushing or flossing.
The gums, or gingiva, are vital soft tissues that protect the roots of your teeth and the underlying bone. When they become inflamed, it's a clear signal that something is amiss in your oral environment or even your overall health. This inflammation is usually a protective response by the body's immune system to irritants, bacteria, or injury. Understanding the nature and extent of the swelling is the first step toward effective diagnosis and treatment.
Types / Variations
Gum swelling can present in various forms, each offering clues to its underlying cause:
Localized vs. Generalized Swelling
- Localized Swelling: This affects a specific area, such as around a single tooth or a small segment of the gum line.
- Causes: Often due to a dental abscess, an impacted tooth, trauma, a foreign body lodged in the gum, or a localized infection.
- Generalized Swelling: This involves a larger area, often affecting all the gums in one arch (upper or lower) or even throughout the entire mouth.
- Causes: Typically associated with widespread inflammatory conditions like gingivitis or periodontitis, systemic issues, hormonal changes (e.g., pregnancy gingivitis), or nutritional deficiencies.
Acute vs. Chronic Swelling
- Acute Swelling: Appears suddenly and may be accompanied by intense pain.
- Causes: Often linked to acute infections (abscess), trauma, or allergic reactions.
- Chronic Swelling: Develops gradually over time and may persist for weeks or months, sometimes with minimal pain.
- Causes: Characteristic of long-standing conditions like chronic gingivitis or periodontitis, certain systemic diseases, or medications.
Other Presentations
- Pustule/Boil: A small, localized bump containing pus, often indicating an underlying infection (dental abscess).
- Fibrotic Enlargement: Gums appear firm and overgrown, often associated with certain medications (e.g., phenytoin, cyclosporine, nifedipine) or genetic conditions.
- Ulcerative/Necrotic: Severe inflammation with tissue breakdown, which can be seen in aggressive forms of periodontitis or specific infections.
Causes / Why It Happens
The causes of swelling gums are diverse, ranging from simple hygiene issues to serious medical conditions. Identifying the root cause is critical for effective treatment.
1. Poor Oral Hygiene (Plaque and Tartar Buildup)
- Gingivitis: This is the most common cause of gum swelling. It's an early stage of gum disease caused by the accumulation of plaque—a sticky film of bacteria—on teeth. If plaque isn't removed by regular brushing and flossing, it irritates the gums, leading to inflammation, redness, and swelling. Gingivitis is reversible with proper oral hygiene and professional cleaning.
- Periodontitis: If gingivitis is left untreated, it can progress to periodontitis, a more severe gum infection. In periodontitis, plaque and tartar spread below the gum line, causing the gums to pull away from the teeth (forming pockets) and leading to chronic inflammation, bone loss, and eventually tooth loss. Swelling in periodontitis is often more pronounced and persistent.
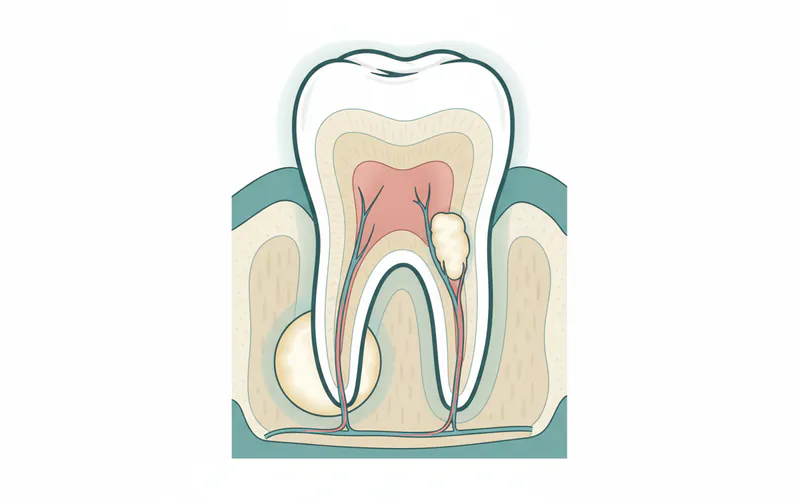
2. Dental Abscess
A dental abscess is a localized collection of pus caused by a bacterial infection.
- Periodontal Abscess: Occurs in the gum tissue itself, often due to deep periodontal pockets becoming infected or a foreign body getting lodged in the gum.
- Periapical Abscess: Forms at the tip of the tooth root, usually as a result of a deep cavity or crack that allows bacteria to infect the pulp (nerve) of the tooth. This infection can spread into the surrounding bone and gum, causing localized swelling, severe pain, and sometimes a visible "pimple" on the gum.
3. Trauma or Injury
- Physical Injury: Accidentally brushing too hard, irritation from ill-fitting dental appliances (dentures, braces), rough edges of fillings or crowns, or chemical irritation from certain products can cause localized gum swelling.
- Knocked Out Tooth (Avulsed Tooth): A severe form of trauma where a tooth is completely dislodged from its socket. The immediate impact often causes significant swelling and bleeding of the surrounding gum tissue. This is a dental emergency.
4. Hormonal Changes
- Pregnancy Gingivitis: Hormonal fluctuations during pregnancy (increased progesterone and estrogen) make gums more sensitive to plaque bacteria, leading to increased inflammation, swelling, and bleeding.
- Menstruation/Puberty: Similar hormonal shifts can temporarily increase gum sensitivity and swelling.
- Menopause: Hormonal changes can lead to dry mouth and more sensitive gums, making them prone to inflammation.
5. Nutritional Deficiencies
- Vitamin C Deficiency (Scurvy): Severe lack of vitamin C can cause gums to become swollen, bleeding, and spongy. While rare in developed countries, it can occur in individuals with extremely poor diets.
- Other Deficiencies: Deficiencies in B vitamins or Vitamin K can also impact gum health, though less directly than Vitamin C.
6. Allergic Reactions
- Dental Materials: Reactions to certain dental materials (e.g., components in fillings, crowns, or even some toothpaste ingredients) can cause localized or generalized gum swelling.
- Food/Medication Allergies: Systemic allergic reactions can sometimes manifest as oral swelling, including the gums.
7. Medications
- Drug-Induced Gingival Enlargement: Certain medications can cause the gums to overgrow and swell, a condition known as gingival hyperplasia.
- Anticonvulsants: Phenytoin (Dilantin)
- Immunosuppressants: Cyclosporine
- Calcium Channel Blockers: Nifedipine, amlodipine (used for high blood pressure)
- Other Medications: Some blood thinners can cause increased gum bleeding, which might be mistaken for or exacerbate swelling.
8. Systemic Diseases
Various systemic health conditions can manifest as gum swelling or make the gums more susceptible to inflammation:
- Diabetes: Poorly controlled diabetes impairs the body's ability to fight infection and heal, making individuals more prone to severe gum disease and swelling.
- Leukemia: This cancer of the blood-forming tissues can cause generalized gum enlargement, bleeding, and pallor.
- Crohn's Disease: An inflammatory bowel disease that can sometimes manifest with oral lesions and gum swelling.
- Autoimmune Diseases: Conditions like Lupus or Sjogren's syndrome can affect oral tissues.
- Viral/Fungal Infections: Herpes gingivostomatitis (especially in children) or candidiasis (thrush) can cause widespread gum inflammation.
9. Impacted Teeth or Erupting Wisdom Teeth
When a tooth, particularly a wisdom tooth, is impacted (unable to fully erupt) or partially erupted, it can create a flap of gum tissue (operculum) that traps food and bacteria, leading to inflammation and swelling (pericoronitis).
Differentiating Gum Swelling from Other Neck/Jaw Swelling
It's important to understand the difference between submandibular gland and lymph node swelling as these can sometimes be confused with dental issues, or be related to dental infections.
- Submandibular Gland Swelling: The submandibular glands are major salivary glands located under the jawbone on both sides. Swelling here is typically firm, tender, and localized to the area under the chin/jawline, not directly on the gum tissue.
- Causes: Salivary gland stones (sialolithiasis), infection (sialadenitis), or rarely, tumors. These can cause pain, especially during eating, and sometimes dry mouth. While a severe dental infection could indirectly cause reactive swelling in nearby structures, direct submandibular gland swelling points to a salivary gland issue.
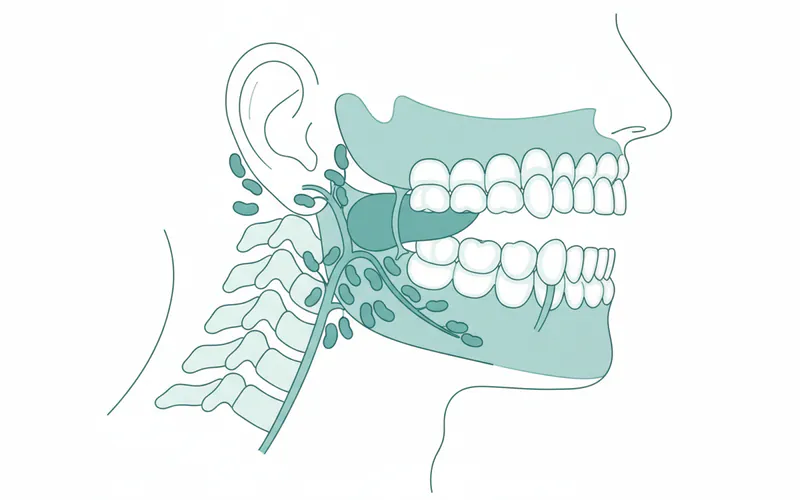
- Lymph Node Swelling: Lymph nodes are small, bean-shaped glands that are part of the immune system, found throughout the body, including in the neck, under the jaw (submandibular nodes), and in front of the ears. When they swell (lymphadenopathy), they become tender, palpable lumps, usually firm and movable, in the neck or under the jaw.
- Causes: Most commonly, swollen lymph nodes indicate an infection or inflammation elsewhere in the body, which the immune system is fighting. A severe dental infection (like an abscess) is a very common cause of reactive submandibular or cervical lymph node swelling, as the nodes drain the infected area. However, the swelling is in the node itself, not the gum.
- Causes: Most commonly, swollen lymph nodes indicate an infection or inflammation elsewhere in the body, which the immune system is fighting. A severe dental infection (like an abscess) is a very common cause of reactive submandibular or cervical lymph node swelling, as the nodes drain the infected area. However, the swelling is in the node itself, not the gum.
Key Differences: Gum swelling is directly on the gingival tissue. Submandibular gland swelling is under the jawbone. Lymph node swelling is a palpable lump, often under the jaw or in the neck, and can be a symptom of a dental infection, but isn't the gum itself.
Signs and Symptoms
Recognizing the signs and symptoms of swelling gums is crucial for timely intervention:
- Redness: Gums appear darker red or purplish instead of a healthy pink.
- Tenderness/Pain: Gums are sensitive to touch, pressure, or when brushing/flossing. Pain can range from mild discomfort to severe, throbbing pain, especially with an abscess.
- Bleeding Gums: Gums bleed easily when brushing, flossing, or even spontaneously.
- Puffiness/Enlargement: Gums appear swollen, rounded, or puffy, rather than firm and contoured around the teeth.
- Shiny Appearance: The surface of the swollen gum tissue may look taut and shiny.
- Receding Gums: While swelling, the gums may also appear to pull away from the teeth, exposing more of the tooth root.
- Bad Breath (Halitosis): Often a sign of bacterial overgrowth and gum disease.
- Pus: Presence of pus (a yellowish or whitish discharge) indicates an active infection, often associated with an abscess.
- Loose Teeth: In advanced gum disease, teeth may become loose due to bone loss.
- Taste of Metal or Pus: A foul taste in the mouth can accompany infection.
- Fever and Malaise: In cases of severe infection (abscess), systemic symptoms like fever, fatigue, and swollen lymph nodes may occur.
- Difficulty Chewing or Swallowing: Severe swelling, especially related to a wisdom tooth or large abscess, can make these activities painful or difficult.
Treatment Options
Treatment for swelling gums depends entirely on the underlying cause. A dental professional will conduct a thorough examination to determine the appropriate course of action.
1. Professional Dental Cleaning (Scaling and Root Planing)
- For Gingivitis and Mild Periodontitis:
- Description: This involves a thorough cleaning below the gum line to remove plaque and tartar (calculus) from the tooth surfaces. Scaling removes the hard deposits, and root planing smooths the root surfaces to prevent bacteria from reattaching.
- Pros: Highly effective for reversing gingivitis and managing early periodontitis, non-surgical.
- Cons: May require local anesthesia, can cause temporary sensitivity.
- Cost: Ranges from $250-$500 for a standard cleaning (prophylaxis) up to $800-$1,500 for scaling and root planing (deep cleaning) for the entire mouth (4 quadrants). Insurance typically covers a significant portion.
2. Antibiotics
- For Bacterial Infections (Abscesses, Severe Periodontitis):
- Description: Oral antibiotics (e.g., amoxicillin, clindamycin, metronidazole) may be prescribed to kill bacteria causing infection. In some cases, topical antibiotic gels or chips may be placed directly into periodontal pockets.
- Pros: Effectively clears bacterial infections, reduces inflammation.
- Cons: Potential side effects (nausea, diarrhea), risk of antibiotic resistance, not a standalone solution for plaque/tartar.
- Cost: Oral antibiotics typically cost $10-$50 for a prescription. Topical treatments can be $50-$200 per application site.
3. Incision and Drainage (I&D)
- For Dental Abscesses:
- Description: A small incision is made in the swollen gum tissue to drain the pus from an abscess. This immediately relieves pressure and pain.
- Pros: Immediate pain relief, addresses the acute infection.
- Cons: Requires local anesthesia, may need follow-up procedures (e.g., root canal or extraction).
- Cost: Typically $100-$300, often included if part of a larger procedure like a root canal.
4. Root Canal Therapy
- For Periapical Abscesses (Tooth Nerve Infection):
- Description: If an infection from a decaying tooth has spread to the pulp and caused a periapical abscess, a root canal removes the infected pulp, cleans and shapes the root canals, and fills them to prevent further infection.
- Pros: Saves the natural tooth, eliminates the source of infection.
- Cons: Multi-appointment procedure, requires a crown afterward, can be expensive.
- Cost: $700-$1,500 for a front tooth, $1,000-$2,000 for molars, not including the crown (which can add $800-$2,000).
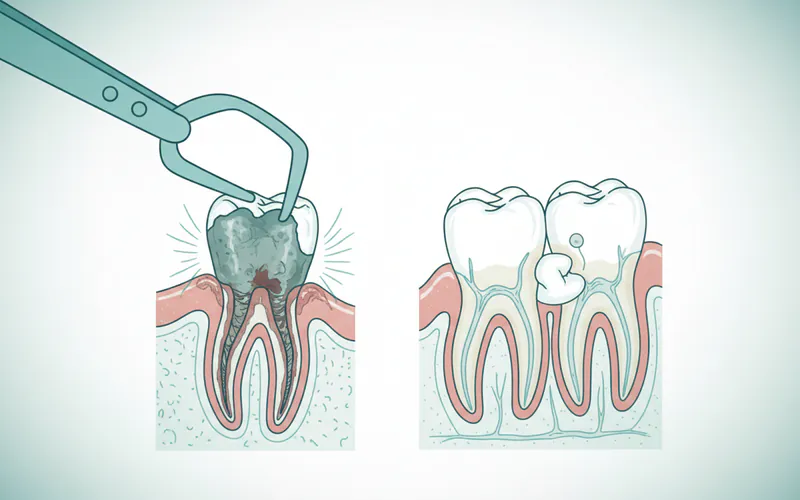
5. Tooth Extraction
- For Severely Damaged/Infected Teeth, Impacted Wisdom Teeth:
- Description: If a tooth is beyond repair, or if an impacted wisdom tooth is causing recurrent infection (pericoronitis) and swelling, extraction may be necessary.
- Pros: Removes the source of infection/irritation permanently.
- Cons: Loss of a natural tooth, may require replacement (implant, bridge) which adds cost.
- Cost: Simple extraction $75-$250, surgical extraction (for impacted teeth) $200-$600, wisdom tooth extraction $250-$800 per tooth (can be higher for complex impactions).
6. Gum Surgery (Periodontal Surgery)
- For Advanced Periodontitis:
- Description: Various surgical procedures are used to treat advanced gum disease, including flap surgery (lifting gums to clean roots and bone), bone grafting, or soft tissue grafts to repair damaged gum tissue.
- Pros: Can halt disease progression, regenerate lost bone/tissue.
- Cons: Invasive, longer recovery, more expensive.
- Cost: Highly variable, from $500-$3,000 for a single quadrant to $5,000-$10,000+ for full-mouth reconstruction.
7. Addressing Underlying Systemic Issues
- Description: If gum swelling is due to a systemic condition (e.g., diabetes, leukemia, medication side effects), treatment involves managing the underlying disease with the primary physician or adjusting medication with medical guidance.
- Pros: Addresses the root cause, improves overall health.
- Cons: May require ongoing medical management.
- Cost: Varies greatly depending on the medical condition and necessary treatments.
8. Home Care and Lifestyle Adjustments
- Description: While not a substitute for professional care, good home care is essential for prevention and as an adjunct to professional treatment. This includes proper brushing and flossing, rinsing with warm salt water, and avoiding irritants.
- Pros: Inexpensive, improves overall oral health.
- Cons: Insufficient for treating severe conditions.
Step-by-Step Process: What to Expect During Treatment
Let's outline a common scenario for addressing gum swelling:
-
Initial Consultation and Diagnosis:
- You'll provide your dental and medical history.
- The dentist will perform a thorough visual examination of your gums, teeth, and entire oral cavity.
- They will use a periodontal probe to measure the depth of gum pockets around your teeth, checking for signs of gum disease.
- Dental X-rays (bitewings, periapical, or panoramic) will be taken to assess bone levels and identify any underlying infections (like abscesses) or impacted teeth.
- If systemic causes are suspected, the dentist might refer you to a medical doctor for further evaluation.
- Pro Tip: Be completely honest about your symptoms, pain levels, medications, and any recent changes in your health. This aids in accurate diagnosis.
-
Treatment Planning:
- Based on the diagnosis, your dentist will explain the cause of your swelling gums and present various treatment options, outlining the pros, cons, and costs of each.
- For example, if gingivitis is diagnosed, a basic cleaning and oral hygiene instructions will be recommended. If an abscess is present, incision and drainage, potentially followed by root canal therapy or extraction, will be discussed.
-
Treatment Execution (Examples):
-
For Gingivitis/Mild Periodontitis:
- Professional Cleaning (Scaling & Root Planing): You'll receive local anesthesia if needed. A dental hygienist or dentist will use specialized instruments (ultrasonic scalers and hand scalers) to meticulously remove plaque and tartar from above and below the gum line. Root surfaces will be smoothed. This may take one or more appointments depending on the severity.
- Oral Hygiene Instruction: You'll be coached on proper brushing techniques (using a soft-bristled brush, angling at 45 degrees), daily flossing, and potentially interdental brushes or oral irrigators.
-
For Dental Abscess (e.g., periapical):
- Drainage: If there's a visible pus-filled bump, the dentist may make a small incision to drain the pus, providing immediate relief.
- Antibiotics: A course of antibiotics will likely be prescribed to control the infection.
- Root Canal Therapy (if tooth is salvageable): The tooth will be numbed. The dentist will create an access opening in the tooth's crown, remove the infected pulp, clean and shape the root canals, and then fill them with a biocompatible material. A temporary filling is placed, and you'll return for a permanent restoration (usually a crown).
- Extraction (if tooth is not salvageable): The tooth will be numbed and then carefully removed. Instructions for post-extraction care will be provided.
-
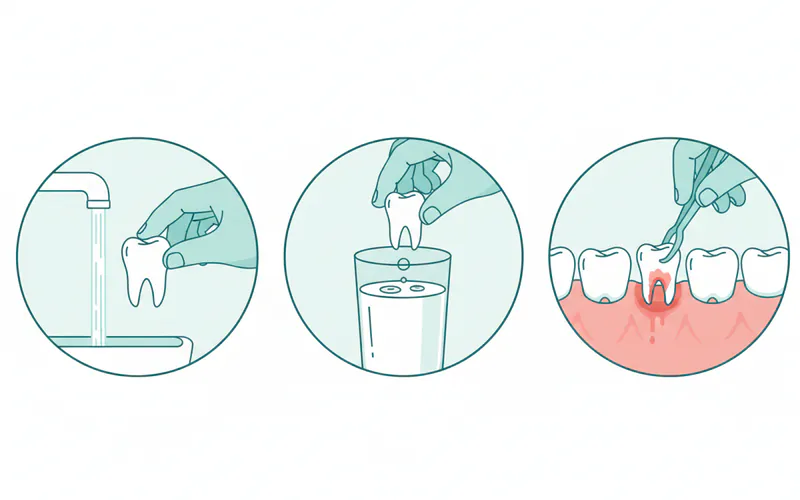
For Knocked Out Tooth:
- Immediate Action: If you have a knocked out tooth, your immediate action is crucial. Gently rinse the tooth with milk or saline (do not scrub), and attempt to reinsert it into the socket. If not possible, place it in a cup of milk, saline, or even your mouth (between cheek and gum). Get to the dentist within 30 minutes to an hour.
- At the Dentist: The dentist will clean the tooth and socket, re-implant the tooth, and splint it to adjacent teeth to stabilize it for several weeks. Follow-up appointments and potentially root canal treatment will be necessary.
-
Cost and Insurance
Dental care costs can vary significantly based on the procedure, your geographic location (major cities often have higher costs), and the dental provider.
| Procedure | Average US Cost (Without Insurance) | Insurance Coverage (Typical) |
|---|---|---|
| Routine Cleaning (Prophylaxis) | $75 - $200 | 80-100% |
| Scaling & Root Planing (per quadrant) | $200 - $400 | 50-80% |
| Oral Antibiotics | $10 - $50 | Usually covered by medical |
| Incision & Drainage (Abscess) | $100 - $300 | 50-80% (often part of larger tx) |
| Simple Tooth Extraction | $75 - $250 | 50-80% |
| Surgical Extraction (incl. wisdom tooth) | $200 - $800 | 50-70% |
| Root Canal (Anterior/Premolar) | $700 - $1,500 | 50-80% |
| Root Canal (Molar) | $1,000 - $2,000 | 50-80% |
| Dental Crown (post-root canal) | $800 - $2,000 | 50% |
| Periodontal Surgery (e.g., flap surgery) | $500 - $3,000 (per quadrant) | 30-50% |
-
Insurance Coverage:
- PPO (Preferred Provider Organization): Offers flexibility to choose any dentist, but going in-network results in lower out-of-pocket costs. Typically covers 80-100% for preventive care, 50-80% for basic procedures (fillings, extractions), and 30-50% for major procedures (crowns, root canals, surgery).
- HMO (Health Maintenance Organization): Requires you to choose a primary dentist within their network. Often has lower monthly premiums but less flexibility. May cover a broad range of services with co-pays.
- Medicaid/CHIP: State-dependent programs for low-income individuals and children. Coverage for adults can be limited to emergencies in some states, while children often have comprehensive dental benefits.
- Annual Maximums: Most dental insurance plans have an annual maximum benefit, typically ranging from $1,000 to $2,000. Once this limit is reached, you pay 100% of the costs.
- Waiting Periods: Many plans have waiting periods (e.g., 6 months for basic care, 12 months for major care) before full benefits kick in.
-
Payment Plans and Financing Options:
- Many dental offices offer in-house payment plans or work with third-party financing companies like CareCredit, which provide low-interest or interest-free payment options for qualifying patients.
- Pro Tip: Always discuss costs and your insurance benefits with your dental office's financial coordinator before commencing treatment to avoid surprises.
Recovery and Aftercare
Post-treatment care is vital for effective healing and preventing recurrence.
- Pain Management:
- Over-the-counter pain relievers (ibuprofen, acetaminophen) are usually sufficient.
- Your dentist may prescribe stronger pain medication for more invasive procedures.
- Apply a cold compress to the outside of your face for the first 24-48 hours to reduce swelling.
- Oral Hygiene:
- Follow your dentist's specific instructions. You may be advised to gently brush the treated area or use a prescribed antimicrobial mouthwash (e.g., chlorhexidine) for a limited period.
- Continue regular brushing and flossing of untreated areas.
- Diet:
- Stick to soft foods for a few days after procedures like extractions, root canals, or gum surgery.
- Avoid hot, spicy, crunchy, or acidic foods that can irritate healing tissues.
- Avoid using straws after extractions as the suction can dislodge blood clots.
- Activity:
- Avoid strenuous activity for 24-48 hours after surgery or extractions.
- Follow-Up Appointments:
- Attend all scheduled follow-up appointments to ensure proper healing and monitor for any complications.
- Lifestyle Changes:
- Quit smoking: Smoking significantly impairs healing and increases the risk of gum disease.
- Manage chronic conditions: If your gum swelling is linked to a systemic disease, diligent management of that condition is crucial.
Prevention
Preventing swelling gums largely revolves around excellent oral hygiene and regular dental care.
- Brush Twice Daily: Use a soft-bristled toothbrush and fluoride toothpaste. Brush gently in circular motions, paying attention to the gum line. The ADA recommends brushing for at least two minutes each time.
- Floss Once Daily: Flossing removes plaque and food particles from between teeth and under the gum line, where toothbrushes can't reach. This is non-negotiable for gum health.
- Regular Dental Check-ups and Cleanings: Visit your dentist every six months for a professional cleaning and examination. This allows for early detection and treatment of issues before they become severe.
- Balanced Diet: Eat a diet rich in fruits, vegetables, and whole grains. Limit sugary snacks and drinks, which contribute to plaque formation. Ensure adequate intake of vitamins, especially Vitamin C.
- Stay Hydrated: Drinking plenty of water helps wash away food particles and bacteria.
- Avoid Tobacco Products: Smoking and chewing tobacco are major risk factors for gum disease and impede healing.
- Manage Stress: Stress can weaken the immune system, potentially making you more susceptible to gum inflammation.
- Address Systemic Conditions: Work with your medical doctor to effectively manage chronic conditions like diabetes that can impact gum health.
- Be Mindful of Medications: If you're on medications known to cause gingival enlargement, discuss this with your dentist and physician. Regular, meticulous oral hygiene is even more critical in these cases.
Risks and Complications
Untreated swelling gums, especially when caused by underlying infections or gum disease, can lead to serious complications:
- Progression to Periodontitis: Untreated gingivitis will almost certainly advance to periodontitis, leading to irreversible bone loss around teeth.
- Tooth Loss: As periodontal disease progresses and bone is lost, teeth become loose and eventually fall out or require extraction.
- Spread of Infection: A dental abscess can spread to other parts of the face, neck, and even into the bloodstream (sepsis), which is a life-threatening condition.
- Impact on Systemic Health: Research has established links between severe gum disease and increased risk or worsening of systemic conditions such as:
- Heart disease and stroke
- Diabetes complications
- Respiratory diseases
- Adverse pregnancy outcomes (premature birth, low birth weight)
- Certain cancers
- Alzheimer's disease
- Receding Gums: Chronic inflammation can lead to gum recession, exposing sensitive tooth roots and increasing the risk of cavities at the root surface.
- Bone Loss in Jaw: Periodontitis directly attacks the bone supporting the teeth, leading to its gradual destruction.
- Halitosis (Chronic Bad Breath): Persistent bacterial growth contributes to offensive breath.
- Difficulty Eating and Speaking: Pain and loose teeth can impair daily functions.
Children / Pediatric Considerations
Swelling gums in children can be concerning for parents and often have different underlying causes or require specific approaches.
- Teething: This is the most common cause of gum swelling in infants and toddlers. As teeth erupt, the gums around them become red, swollen, and tender. Symptoms include irritability, drooling, and a desire to chew on objects.
- Care: Gentle gum massage, chilled teething rings, and over-the-counter pain relievers (acetaminophen or ibuprofen, consult pediatrician for dosage) can help.
- Poor Oral Hygiene: Just like adults, children can develop gingivitis due to inadequate brushing and flossing.
- Care: Parents must ensure children brush twice daily (assisting until age 7-8) and begin flossing once the teeth touch. Regular pediatric dental visits are essential.
- Herpetic Gingivostomatitis: This viral infection, often seen in young children, causes widespread, painful swelling of the gums, mouth sores, fever, and difficulty eating. It's usually caused by the herpes simplex virus.
- Care: Antiviral medications (if diagnosed early), pain relief, and ensuring hydration are key.
- Dental Abscesses/Cavities: Children are susceptible to cavities. If a cavity goes deep, it can lead to an infection and abscess, causing localized gum swelling.
- Care: Immediate dental attention for a filling, pulpotomy (nerve treatment for baby teeth), or extraction.
- Trauma: Children are prone to falls and accidents, which can injure the gums or knock out teeth.
- Care: Any significant trauma to the mouth warrants a dental visit. Follow emergency protocols for a knocked out baby tooth (do not re-implant a baby tooth, but seek a dentist immediately).
- Eruption Cysts/Hematomas: Sometimes a bluish, soft swelling appears on the gum before a tooth erupts. This is an eruption cyst or hematoma and usually resolves on its own as the tooth comes through.
- Care: Observation is typically sufficient, but a dentist can confirm the diagnosis.
Pro Tip for Parents: If your child has unexplained gum swelling, pain, or fever, consult a pediatric dentist promptly. Early intervention can prevent minor issues from becoming major problems.
Cost Breakdown
Understanding the financial aspect of dental treatment for swelling gums is critical. While general ranges were provided, let's detail how these costs might apply.
Factors Influencing Cost:
- Severity of Condition: Mild gingivitis costs far less to treat than advanced periodontitis requiring surgery.
- Location: Dental costs are generally higher in metropolitan areas compared to rural regions.
- Dentist's Fees: Experience and specialization (e.g., periodontist for gum surgery) can influence costs.
- Materials Used: For crowns or fillings, the type of material can affect the price.
| Treatment Type | Low Range (US, small town) | Mid Range (US, suburban) | High Range (US, major city/specialist) |
|---|---|---|---|
| Basic Cleaning | $75 | $120 | $200 |
| Deep Cleaning (SRP) | $200/quadrant | $300/quadrant | $400/quadrant |
| Simple Extraction | $75 | $150 | $250 |
| Surgical Extraction | $200 | $450 | $800 |
| Root Canal (Front) | $700 | $1,000 | $1,500 |
| Root Canal (Molar) | $1,000 | $1,500 | $2,000 |
| Gum Surgery (Flap) | $500/quadrant | $1,500/quadrant | $3,000/quadrant |
| Antibiotics | $10 | $30 | $50 |
With vs. Without Insurance:
- With Insurance: As mentioned, most PPO plans cover a percentage of costs after deductibles are met, up to an annual maximum. For a deep cleaning, you might pay $60-$120 per quadrant out-of-pocket, or 20-50% of a root canal. If you hit your annual maximum (e.g., $1,500), you'll pay 100% of any further costs for that year.
- Without Insurance: You are responsible for 100% of the listed costs. Many dentists offer a discount for cash payments or have membership plans that provide a discount for a yearly fee.
Payment Plans and Financing Options:
- In-Office Payment Plans: Many dental practices understand the financial burden and offer installment plans, especially for extensive treatments.
- Third-Party Medical Financing: Companies like CareCredit or LendingClub offer specialized credit lines for healthcare expenses. They often have promotional periods with 0% interest if the balance is paid within a specified timeframe (e.g., 6, 12, 18, or 24 months). Interest rates can be high if the balance isn't paid off in time.
- Dental Schools: University dental schools often provide services at a reduced cost because students perform the procedures under the close supervision of experienced faculty. This can be an excellent cost-saving option for more complex treatments, though appointments may take longer.
- Community Health Centers: Federally Qualified Health Centers (FQHCs) and other community clinics provide dental care on a sliding scale fee based on income, making it accessible to low-income individuals.
Cost-Saving Tips:
- Preventive Care: The absolute best way to save money is to prevent issues. Regular cleanings are far cheaper than treating advanced gum disease or an abscess.
- Shop Around: Get quotes from a few different dentists for major procedures.
- Utilize HSAs/FSAs: If you have a Health Savings Account (HSA) or Flexible Spending Account (FSA) through your employer, contribute to these tax-advantaged accounts to pay for dental expenses.
- Negotiate: Don't be afraid to ask about cash discounts or payment plans.
Frequently Asked Questions
What does it mean if my gums are swollen around one tooth?
Swelling around a single tooth often indicates a localized issue. Common causes include a dental abscess (infection at the tooth's root or in the gum pocket), a foreign object lodged in the gum, trauma to that specific tooth, or an impacted wisdom tooth. It's crucial to see a dentist to diagnose the exact cause and prevent the infection from spreading.
Can swollen gums go away on their own?
Mild gingivitis caused by temporary plaque buildup might subside with diligent brushing and flossing within a few days. However, swelling caused by infections (abscesses), advanced gum disease, trauma, or systemic issues will not resolve on its own and requires professional dental intervention. Ignoring persistent swelling can lead to severe complications.
How do I reduce gum swelling fast at home?
While professional treatment is essential for underlying causes, you can temporarily alleviate discomfort at home. Rinse with warm salt water (1/2 teaspoon salt in 8 ounces of warm water) several times a day. Avoid irritating foods (spicy, acidic), use a soft-bristled toothbrush, and gently massage your gums. Over-the-counter pain relievers can help with discomfort.
Is gum swelling an emergency?
Not always, but it can be. If gum swelling is accompanied by severe, throbbing pain, pus discharge, fever, difficulty swallowing or breathing, rapid onset, or facial swelling spreading beyond the gum, it is a dental emergency. Swelling after a knocked out tooth is also an emergency requiring immediate attention to save the tooth.
What is the average cost of treating swelling gums?
The cost varies greatly based on the cause. A routine cleaning for gingivitis might cost $75-$200. Scaling and root planing for mild periodontitis could be $800-$1,500 for the whole mouth. A dental abscess might require an incision and drainage ($100-$300) and potentially a root canal ($700-$2,000) or extraction ($75-$800).
What types of doctors treat swollen gums?
Your primary point of contact is a general dentist. They can diagnose and treat most causes of gum swelling. For advanced gum disease or complex cases, they may refer you to a periodontist (a gum specialist). If the swelling is linked to a systemic medical condition, your general dentist may collaborate with your primary care physician or a relevant medical specialist.
Can wisdom teeth cause gum swelling?
Yes, wisdom teeth are a common cause of localized gum swelling. When wisdom teeth are partially erupted or impacted, a flap of gum tissue can form over them, trapping food and bacteria. This can lead to an infection called pericoronitis, causing significant pain, redness, and swelling around the wisdom tooth.
How long does it take for gum swelling to go down after treatment?
For mild gingivitis, swelling can noticeably reduce within a few days to a week after a professional cleaning and improved home care. For abscesses, swelling often subsides within 2-3 days after drainage and antibiotic treatment. More extensive procedures like gum surgery will have a longer recovery period, with initial swelling reducing in a week but full healing taking several weeks or months.
Can braces cause swollen gums?
Yes, braces can contribute to gum swelling. The brackets and wires can make it harder to clean teeth effectively, leading to plaque buildup and gingivitis. Additionally, the constant pressure of braces can sometimes irritate the gum tissue, leading to localized inflammation. Meticulous oral hygiene is even more critical for individuals with braces.
What foods should I avoid if my gums are swollen?
If your gums are swollen, avoid foods that can irritate them or get stuck, such as crunchy snacks (chips, popcorn), acidic foods (citrus fruits, tomatoes), very hot or spicy foods, and sugary items. Stick to soft, cool, and non-acidic foods like yogurt, mashed potatoes, cooked vegetables, and soft fruits until the swelling subsides.
When to See a Dentist
Knowing when to seek professional help for swelling gums is critical for preventing serious complications.
Schedule a routine dental appointment if you notice:
- Gums that bleed easily when brushing or flossing.
- Persistent bad breath.
- Gums that are redder than usual and feel tender.
- Mild, generalized gum swelling that doesn't improve with improved home care after a few days.
Seek immediate dental attention (Dental Emergency) if you experience:
- Severe, throbbing pain in your gums or jaw.
- Rapidly spreading facial swelling that involves your cheek, jaw, or neck.
- Difficulty swallowing or breathing due to swelling.
- Fever or chills accompanying the gum swelling.
- Pus discharge from your gums, especially forming a visible "pimple" (abscess).
- Gums so swollen you can't close your mouth properly.
- A knocked out tooth: This is a true dental emergency, and prompt action (within 30-60 minutes) is crucial for a chance to save the tooth.
- Swelling that persists or worsens despite attempts at home care for more than a few days.
Delaying treatment for severe gum swelling can lead to the spread of infection, tooth loss, and potentially life-threatening systemic complications. Your dental health is an integral part of your overall well-being.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
How to Relieve Gum Swelling
When your gums are swollen, it can be an alarming and uncomfortable experience, often signaling an underlying issue that requires attention. Statistics from the Centers for Disease Control and Prevention (CDC) reveal that **nearly half of adults aged 30 or older in the United States have some form o
February 23, 2026
Teeth Swelling: Complete Guide
When you experience teeth swelling, it's more than just a minor discomfort; it's a clear signal from your body that something is amiss within your oral cavity, often indicating an underlying infection or inflammation that requires prompt attention. A recent survey revealed that **over 25% of adu
February 23, 2026
Submandibular Salivary Gland Swelling: Complete Guide
When you notice a peculiar lump or uncomfortable fullness beneath your jaw, it can be an alarming experience. This sensation, often accompanied by pain and difficulty swallowing, could indicate submandibular salivary gland swelling. Affecting an estimated 1 in 10,000 adults annually, conditi
February 23, 2026
What Helps With Gum Swelling
Gum swelling, medically known as gingival swelling or gingivitis, is a common yet often underestimated dental issue affecting millions of Americans. Have you ever woken up with sore, puffy gums that bleed easily when you brush? You're not alone. Research indicates that nearly **half of all a
February 23, 2026