Tooth Dry Socket: Complete Guide
Key Takeaways
- Imagine enduring a dental extraction, anticipating relief, only to be met with escalating, throbbing pain days later. This distressing scenario is precisely what happens with a tooth dry socket, a common yet painful complication following tooth removal. While dental extractions are generally saf
Tooth Dry Socket: Complete Guide
Imagine enduring a dental extraction, anticipating relief, only to be met with escalating, throbbing pain days later. This distressing scenario is precisely what happens with a tooth dry socket, a common yet painful complication following tooth removal. While dental extractions are generally safe, approximately 2-5% of all extractions, and up to 30% of wisdom tooth extractions, can result in this condition, technically known as alveolar osteitis. This unexpected turn can disrupt daily life, causing significant discomfort and anxiety, and can lead to confusion about what exactly is going wrong inside your mouth.

Understanding dry socket is crucial for anyone undergoing a tooth extraction, especially since its symptoms can sometimes mimic other issues or simply be mistaken for typical post-operative soreness. This comprehensive guide from SmilePedia.net aims to demystify dry socket, offering you a clear, authoritative, and medically accurate resource. We'll delve into what dry socket is, why it occurs, how to recognize its tell-tale signs, and most importantly, the effective treatment options available. We'll also cover essential recovery tips, preventive measures, and a detailed breakdown of costs and insurance considerations, empowering you to navigate this dental emergency with confidence and ensure a swift return to comfort and oral health.
Key Takeaways:
- What it is: Dry socket (alveolar osteitis) occurs when the protective blood clot dislodges or dissolves prematurely after a tooth extraction, exposing bone and nerve endings.
- Symptoms: Intense, throbbing pain, often radiating to the ear, temple, or neck, typically starting 2-4 days post-extraction. Foul odor/taste and visible empty socket are common.
- Prevalence: Affects 2-5% of all extractions, but up to 30% of wisdom tooth extractions, particularly lower molars.
- Treatment: Involves cleaning the socket, applying medicated dressings (e.g., eugenol-impregnated gauze), pain management, and sometimes antibiotics for infection.
- Pain Relief: Significant relief is usually felt within hours of professional treatment, with full resolution within 7-10 days.
- Cost: Initial treatment for dry socket typically ranges from $75 to $300 per visit, often requiring multiple visits. This is usually covered by dental insurance.
- Prevention: Strict adherence to post-operative instructions (avoiding smoking, straw use, vigorous rinsing, and maintaining good oral hygiene) significantly reduces risk.
What It Is / Overview
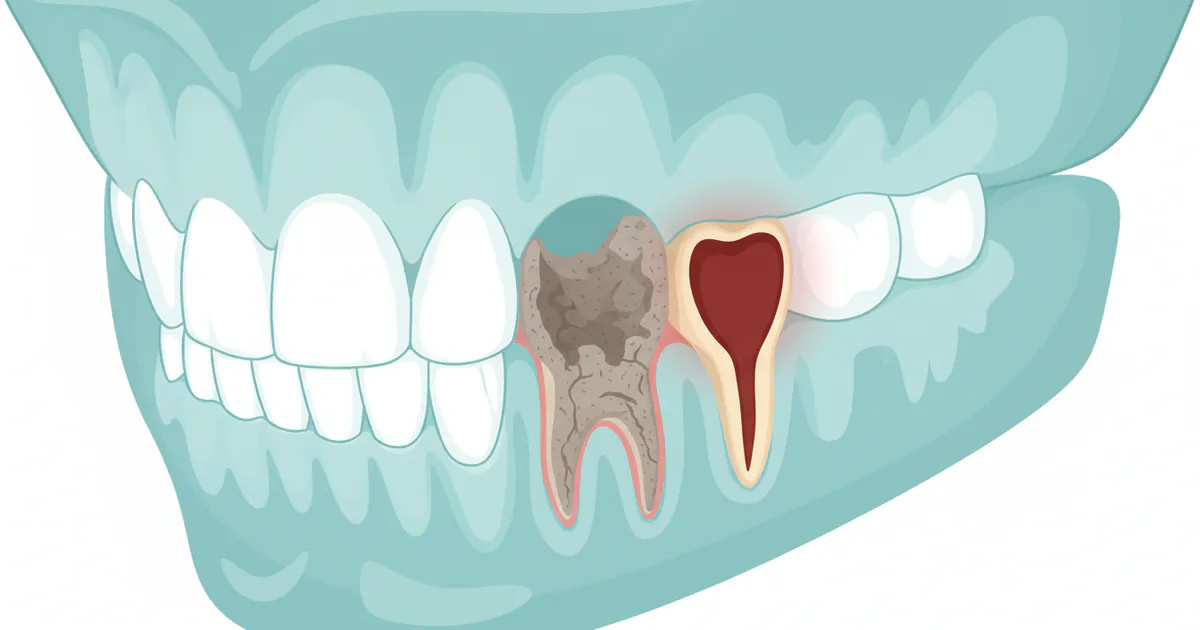
A tooth dry socket, medically termed alveolar osteitis, is a painful condition that can develop after a permanent adult tooth has been extracted. Normally, after a tooth is removed, a blood clot forms in the empty socket. This blood clot is vital for the healing process; it protects the underlying bone and nerve endings, acting as a natural bandage and scaffold for new tissue growth. When a dry socket occurs, this critical blood clot either fails to form, becomes dislodged, or dissolves prematurely, typically within 2 to 4 days post-extraction.
Without this protective clot, the underlying bone and nerve endings in the socket are exposed to air, food particles, and bacteria. This exposure leads to inflammation and intense pain, which can be significantly more severe than the expected discomfort after a routine extraction. The condition is most common after the extraction of lower wisdom teeth (mandibular third molars) due to the dense bone structure and the more traumatic nature often involved in their removal.
While not an infection in itself, dry socket creates an ideal environment for bacteria, increasing the risk of secondary infection. It's important to differentiate dry socket from a normal, healthy healing process. Normal healing involves mild to moderate pain manageable with over-the-counter pain relievers, gradually diminishing over several days. Dry socket pain, by contrast, often intensifies over time and is characterized by a deep, throbbing ache that radiates beyond the immediate extraction site.
Understanding dry socket is the first step towards recognizing its symptoms and seeking timely treatment. It is a manageable condition, but professional dental care is essential for pain relief and proper healing.
Causes / Why It Happens
The precise mechanism leading to a tooth dry socket is not always fully understood, but it is primarily attributed to the premature loss or failure of the blood clot that forms in the extraction socket. Several factors can contribute to this unfortunate occurrence:
Mechanical Dislodgement of the Blood Clot
- Sucking Action: Activities that create negative pressure in the mouth can dislodge the blood clot. This includes using straws, spitting vigorously, or smoking, particularly in the first 24-48 hours after extraction.
- Vigorous Rinsing: Aggressive rinsing or swishing with mouthwash too soon after surgery can also disturb the fragile clot.
- Touching the Site: While less common, probing the extraction site with fingers or the tongue can mechanically dislodge the clot.
Chemical and Biological Factors
- Smoking and Tobacco Use: Nicotine and other chemicals in tobacco products restrict blood flow, impairing clot formation and dissolution. The act of smoking itself (sucking action) is also a significant risk factor. Studies show smokers are significantly more likely to develop dry socket.
- Oral Contraceptives: High estrogen levels, present in some oral contraceptives, can interfere with normal blood clot formation and stability, increasing the risk for women.
- Poor Oral Hygiene: Pre-existing bacterial infections in the mouth, such as periodontitis (gum disease) or pericoronitis (inflammation around a partially erupted wisdom tooth), can lead to an increased bacterial load in the socket. This bacteria can break down the blood clot prematurely.
- Traumatic Extraction: A difficult or prolonged tooth extraction that involves significant manipulation of the surrounding bone can lead to increased inflammation and a less stable blood clot. This is particularly true for impacted wisdom teeth.
- Inadequate Blood Supply: In some cases, the blood supply to the extraction site may be compromised, leading to a weaker or smaller blood clot that is more prone to dislodging or dissolving.
Other Contributing Factors
- Previous History of Dry Socket: Individuals who have experienced dry socket after a prior extraction are at a higher risk of developing it again.
- Bone Density: Extractions from dense bone, such as the lower jaw, are more prone to dry socket.
- Steroid Use: Some research suggests a potential link between systemic steroid use and increased risk, though more studies are needed.
- Age: While dry socket can occur at any age, adults are more commonly affected than children.
Understanding these causes is vital for prevention, allowing both patients and dental professionals to take proactive steps to minimize the risk of developing this painful complication.
Signs and Symptoms
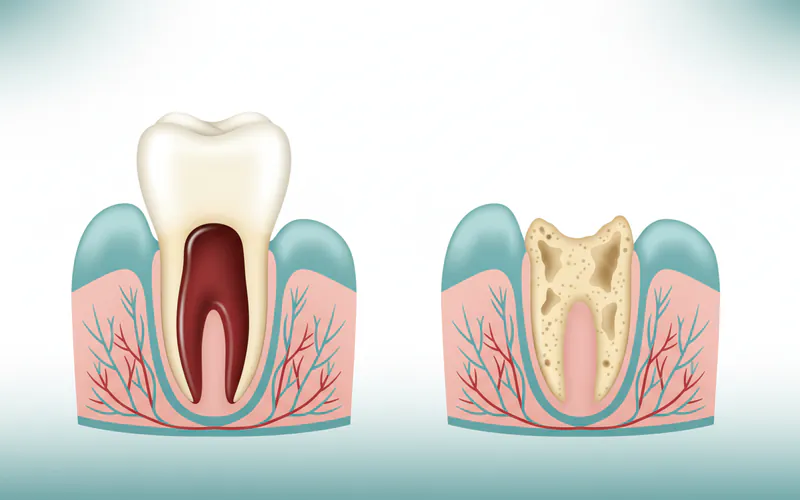
Recognizing the signs and symptoms of a dry socket is crucial for prompt diagnosis and treatment. While some pain is normal after an extraction, dry socket pain is distinct and often debilitating.
Key Indicators to Watch For:
-
Severe Pain: This is the hallmark symptom. Unlike the dull, manageable ache of a normal extraction, dry socket pain is typically:
- Intense and throbbing: Described as a deep, aching, or throbbing pain.
- Starts 2-4 days post-extraction: Normal post-op pain usually peaks within 24-48 hours and then gradually subsides. Dry socket pain often worsens or begins several days later.
- Radiating: The pain often radiates from the extraction site to the ear, temple, eye, or neck on the same side of the face.
- Unresponsive to standard pain medication: Over-the-counter pain relievers or even prescribed narcotics might provide little to no relief.
-
Visible Empty Socket: When you look into your mouth, you might see an empty, whitish-looking socket where the tooth was removed. Instead of a dark red or brownish blood clot, you might see bare bone. This is a clear indicator that the clot is missing.
-
Foul Odor and Unpleasant Taste: The exposed bone and trapped food particles can lead to a very noticeable bad breath (halitosis) and a foul, metallic, or generally unpleasant taste in your mouth. This is due to bacterial activity and tissue breakdown in the exposed socket.
-
Tenderness of Gums and Nearby Tissues: The gum tissue around the dry socket may be tender to the touch, and there might be mild swelling, though significant swelling is less common unless an infection has developed.
-
Difficulty Eating and Speaking: Due to the severe pain, eating, drinking, and even speaking can become very challenging and uncomfortable.
-
Lymph Node Swelling (Rare, but possible with secondary infection): While dry socket itself is not an infection, the exposed bone can become a breeding ground for bacteria. If a secondary infection develops, you might experience submandibular gland swelling causes if the infection spreads to nearby lymph nodes or soft tissues, or swelling in the neck and jaw area. However, dry socket primarily causes localized pain and the distinctive empty socket appearance.
It's important not to confuse dry socket with other issues like cold sore swelling. Cold sores (herpes labialis) are viral infections that cause blisters, typically on or around the lips, and are unrelated to dry socket. While both can cause oral discomfort and potentially localized swelling, their causes, appearance, and treatment are entirely different. Dry socket pain is deep within the bone, whereas cold sore pain is superficial on the skin/mucosa.
If you experience any of these symptoms, especially severe, radiating pain that starts a few days after your tooth extraction, contact your dentist immediately.
Treatment Options
Treating a tooth dry socket focuses primarily on relieving pain, promoting healing, and preventing infection. While the condition is temporary, professional dental intervention is essential to manage symptoms and ensure proper recovery.
Professional Dental Treatment
-
Cleaning the Socket (Irrigation): The first step in treating dry socket is for the dentist to gently irrigate (flush out) the socket. This removes any trapped food particles, debris, and bacteria that may be irritating the exposed bone and nerves. Saline solution, medicated rinses, or chlorhexidine gluconate are commonly used for this.
-
Medicated Dressings: After cleaning, the dentist will pack the socket with a medicated dressing. This dressing serves several purposes:
- Pain Relief: Many dressings contain eugenol (clove oil derivative), which acts as a powerful local anesthetic and antiseptic, providing almost immediate pain relief.
- Protection: It covers the exposed bone and nerve endings, protecting them from food, air, and further irritation.
- Promotes Healing: While not directly forming a new clot, it helps create an environment conducive to granulation tissue formation.
- Common materials: Alveogyl (a paste containing eugenol, iodoform, and butamben), medicated gauze strips, or other proprietary dry socket pastes.
- Pros: Provides rapid and significant pain relief; protects the socket; helps prevent further complications.
- Cons: Requires professional application; dressings need to be changed every 24-72 hours until symptoms subside; can sometimes leave an unpleasant taste.
-
Pain Management:
- Prescription Pain Relievers: Your dentist may prescribe stronger pain medication, such as opioids (e.g., hydrocodone, oxycodone) or strong NSAIDs (e.g., ibuprofen 800mg), especially during the initial stages when pain is most severe.
- Over-the-Counter Pain Relievers: For milder discomfort or as the pain subsides, over-the-counter NSAIDs like ibuprofen (Advil, Motrin) or naproxen (Aleve) can be effective.
- Pros: Directly addresses the severe pain; can improve quality of life during healing.
- Cons: Prescription medications carry risks of side effects, dependence, or abuse; OTC meds may not be sufficient for severe dry socket pain.
-
Antibiotics (If Infection is Present): Dry socket itself is typically not an infection, but the exposed bone can become infected. If there are signs of infection (pus, significant swelling, fever), your dentist may prescribe antibiotics to eliminate the bacteria.
- Pros: Addresses secondary bacterial infection, preventing its spread and further complications.
- Cons: Unnecessary antibiotic use can contribute to antibiotic resistance; may have side effects (e.g., gastrointestinal upset).
Home Care Support (Under Dental Guidance)
- Gentle Rinsing: Your dentist may recommend gentle rinsing with warm salt water several times a day to keep the area clean. This is not vigorous swishing but a gentle holding and tilting action.
- Continued Oral Hygiene: Maintain careful brushing and flossing around the other teeth, avoiding the extraction site directly.
- Dietary Modifications: Stick to soft foods that are easy to chew and swallow, avoiding crunchy, hard, or very hot/cold items that could irritate the socket.
- Avoid Irritants: Continue to avoid smoking, using straws, and spitting until the socket has fully healed.
Comparison of Treatment Approaches
| Treatment Option | Description | Pros | Cons | Typical Duration |
|---|---|---|---|---|
| Medicated Dressing | Professional cleaning and placement of medicated paste/gauze | Rapid pain relief, protection, promotes healing | Requires professional visits, dressings need changing, unpleasant taste | Until pain subsides (2-7 days), usually 2-4 visits |
| Pain Medication | Prescribed narcotics or strong NSAIDs | Directly targets severe pain, improves comfort | Side effects, potential for dependence, may not address underlying issue | As needed, usually 3-7 days |
| Antibiotics | Prescribed oral antibiotics | Treats secondary bacterial infection if present | Side effects, risk of resistance, only for infection | Typically 7-10 days course |
| Home Care | Gentle rinsing, soft diet, avoiding irritants | Supports healing, maintains hygiene, complements professional care | Not sufficient as sole treatment, requires discipline | Throughout healing (1-2 weeks or more) |
The treatment plan for dry socket is highly individualized based on the severity of your symptoms and the specific findings during examination. Your dentist will guide you through the process, ensuring the most effective and comfortable recovery.
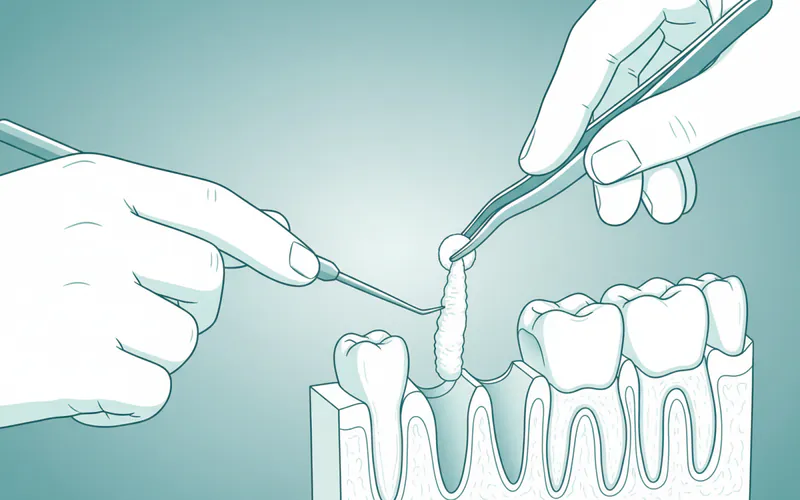
Step-by-Step Process (What to Expect During Treatment)
When you visit your dentist for suspected dry socket, here's a typical step-by-step breakdown of what you can expect during your appointment and the overall treatment period:
Initial Dental Visit: Diagnosis and First Treatment
- Examination and Medical History Review: Your dentist will first ask about your symptoms (when they started, severity, what makes them better or worse) and review your medical history, including any medications you're taking.
- Oral Examination: The dentist will carefully examine your mouth, paying close attention to the extraction site. They will look for the absence of a blood clot, exposed bone, and any signs of infection (pus, significant swelling). They might gently probe the area to assess tenderness.
- Anesthesia (if needed): If the pain is very severe, or if the cleaning process is expected to be uncomfortable, the dentist may administer a local anesthetic to numb the area around the socket.
- Irrigation and Cleaning: The dentist will gently flush the empty socket using a sterile saline solution, medicated rinse (like chlorhexidine), or water. This thoroughly cleanses the socket, removing food debris, bacteria, and any necrotic (dead) tissue. This step is crucial for preparing the site for medication.
- Application of Medicated Dressing: Once clean, the socket will be packed with a medicated dressing. This typically consists of a sterile gauze strip or sponge impregnated with a soothing agent like eugenol (clove oil derivative) and often other pain-relieving and antiseptic ingredients. The dressing is carefully placed to cover the exposed bone and nerve endings.
- Pain Medication and Aftercare Instructions: Your dentist will likely prescribe stronger pain medication if your current regimen isn't working. You'll receive specific instructions on home care, including how to manage pain, what to eat, and what to avoid. You will also be scheduled for follow-up appointments.
Follow-Up Visits: Ongoing Care
- Dressing Changes: The medicated dressing usually needs to be changed every 24-72 hours, depending on the type of dressing and your symptoms. During these follow-up visits, the old dressing will be removed, the socket will be re-irrigated, and a new dressing will be applied. This process continues until your pain significantly diminishes and the socket begins to heal.
- Monitoring Healing: Your dentist will monitor the healing progress. As healing advances, the pain will lessen, and you might observe new tissue starting to form in the socket. Eventually, the need for dressings will decrease, and your dentist will advise when they are no longer necessary.
Recovery Period: What to Expect
- Immediate Relief: Most patients experience significant pain relief within a few hours of the first medicated dressing application.
- Gradual Improvement: Pain will continue to subside with each subsequent dressing change.
- Total Healing Time: While pain relief is relatively quick, the full healing of the dry socket itself, meaning the socket is no longer exposed and new tissue has started to form, can take approximately 7 to 10 days. Complete soft tissue healing can take a few weeks, and bone remodeling continues for months.
- Commitment to Follow-Ups: Adhering to your dentist's follow-up schedule is crucial for effective treatment and to prevent complications. Do not attempt to remove or replace dressings yourself unless explicitly instructed.
This structured approach ensures that your dry socket is properly managed, leading to a faster and more comfortable recovery.
Cost and Insurance
Understanding the financial aspects of dry socket treatment is important for patients in the US. The cost can vary based on several factors, including the severity of the condition, the number of necessary follow-up visits, the type of dental professional (general dentist vs. oral surgeon), and geographic location.
Average US Cost Ranges for Dry Socket Treatment
A single visit for dry socket treatment, which typically involves irrigation and placement of a medicated dressing, usually ranges from $75 to $300. However, it's important to remember that most dry socket cases require multiple follow-up visits for dressing changes and monitoring.
- Low End (1-2 visits, simple case): $75 - $200
- Mid-Range (2-4 visits, moderate case): $200 - $600
- High End (4+ visits, complex case, including potential antibiotics): $600 - $1,000+
These figures generally cover the cost of the examination, irrigation, medicated dressing, and a follow-up visit. Additional costs might include:
- Prescription Pain Medication: This is typically covered by your medical insurance or paid out-of-pocket at a pharmacy, ranging from $10 to $50+ depending on the drug and quantity.
- Antibiotics: Similar to pain medication, these are covered by medical insurance or are an out-of-pocket cost, usually $10 to $60+.
- Emergency Fee: Some practices may charge an emergency or after-hours fee if you require immediate attention outside of regular business hours, which can add $50 to $150 to the total.
Insurance Coverage Details
Most standard dental insurance plans in the US do cover dry socket treatment because it is considered a post-operative complication of an already covered procedure (tooth extraction).

- Diagnostic & Preventative Care: The initial exam might be covered at a high percentage (e.g., 80-100%).
- Basic Restorative Care: Dry socket treatment often falls under "basic restorative" or "minor oral surgery aftercare" categories, which are usually covered at 70-80% after you meet your deductible.
- Deductibles and Co-pays: You will likely be responsible for your annual deductible before insurance coverage kicks in, and then a co-payment for each visit. For example, if your plan covers 80% and the visit costs $150, you would pay $30 (20% co-pay) after meeting your deductible.
- Annual Maximums: Be aware of your plan's annual maximums, although dry socket treatment costs are generally low enough not to exceed these unless you have other extensive dental work done in the same year.
- Medical vs. Dental Insurance: While the treatment itself is dental, any prescribed medications (painkillers, antibiotics) may fall under your medical insurance pharmacy benefits.
Pro Tip: Always contact your dental insurance provider before your appointment if possible, or have the dental office verify your benefits. Ask specific questions about coverage for "alveolar osteitis treatment" or "post-operative complication care" to understand your out-of-pocket expenses.
Comparison of Costs (with vs. without insurance)
| Service | Average Cost (Without Insurance) | Average Cost (With Insurance, 80% Coverage After Deductible) |
|---|---|---|
| Initial Exam & Diagnosis | $50 - $150 | $10 - $30 |
| Per Visit (Irrigation & Dressing) | $75 - $300 | $15 - $60 |
| Prescription Pain Meds (Out-of-Pocket) | $10 - $50 | $10 - $50 (Medical Insurance) |
| Total for 3 Visits (Estimated) | $275 - $1050 | $55 - $210 + deductible |
- Note: "Total for 3 Visits" includes an initial exam and two follow-up treatment visits.
Payment Plans and Financing Options
If you do not have dental insurance or if your out-of-pocket costs are higher than anticipated, many dental offices offer:
- Payment Plans: In-house payment plans allowing you to pay the balance in installments.
- Third-Party Financing: Options like CareCredit, which offers interest-free or low-interest financing for medical and dental expenses.
- Dental Discount Plans: These are not insurance but offer a percentage discount on services from participating dentists.
Don't let financial concerns prevent you from seeking treatment for dry socket. The pain is significant, and delaying treatment can prolong discomfort and potentially lead to secondary infections. Discuss your financial options openly with your dental office staff.
Recovery and Aftercare
Effective recovery and diligent aftercare are paramount for healing from a tooth dry socket and preventing its recurrence. While your dentist will manage the immediate treatment, your actions at home play a significant role in a smooth and speedy recovery.
Key Aftercare Instructions
- Follow Medicated Dressing Instructions: Your dentist will provide specific instructions regarding the medicated dressing. This will include how often it needs to be changed and whether you should return for professional replacement or if you'll be instructed on very gentle rinsing at home. Do not attempt to remove or replace the dressing yourself unless explicitly told to do so.
- Pain Management:
- Take Prescribed Medication: Adhere strictly to the dosage and schedule of any prescribed pain medication. Do not wait for the pain to become unbearable before taking the next dose.
- Over-the-Counter Pain Relievers: For milder pain as you heal, NSAIDs like ibuprofen or naproxen can be very effective. Always follow package directions.
- Cold/Warm Compresses: Applying a cold compress to the outside of your jaw for 15-20 minutes at a time (with 20-minute breaks) can help with residual swelling and discomfort in the first day or two. After that, a warm, moist compress can sometimes soothe the radiating pain.
- Gentle Oral Hygiene:
- Saltwater Rinses: Your dentist will likely recommend gentle rinsing with warm salt water (1/2 teaspoon of salt in 8 ounces of warm water) 2-3 times a day, especially after meals. This helps keep the socket clean and promotes healing. Do not rinse vigorously; just let the water gently swish in your mouth or tilt your head.
- Brushing: Continue to brush your other teeth normally, but be very gentle around the extraction site. Avoid direct brushing of the socket itself until instructed otherwise.
- Dietary Modifications:
- Soft Foods: Stick to a soft diet for several days after treatment, gradually reintroducing solid foods as comfort allows. Examples include yogurt, smoothies, mashed potatoes, scrambled eggs, and soft pasta.
- Avoid Crunchy, Hard, or Spicy Foods: These can irritate the socket or dislodge any fragile healing tissue.
- Avoid Extremely Hot or Cold Foods/Drinks: Temperature extremes can cause sensitivity or discomfort.
- Avoid Irritants and Disruptive Actions:
- No Smoking or Tobacco Products: This is critical. Smoking significantly impedes healing and can worsen dry socket. Avoid it entirely during recovery.
- No Straws: Continue to avoid using straws, as the sucking action can dislodge healing tissue or irritate the socket.
- No Spitting: Avoid forceful spitting.
- Minimize Physical Activity: Strenuous exercise can increase blood pressure, potentially disrupting healing and increasing discomfort. Rest as much as possible for the first few days after treatment.
- Alcohol: Avoid alcohol as it can interfere with medications and dehydrate you.
Timeline for Recovery
- Pain Relief: Often within hours of the first medicated dressing.
- Reduced Symptoms: Significant improvement usually seen within 2-3 days of consistent treatment.
- Full Resolution of Dry Socket: Typically 7-10 days, after which the pain should be gone, and the socket should be visibly filling in with new tissue.
- Complete Healing of Socket: Soft tissue healing can take 2-3 weeks, with bone remodeling continuing for several months.
Pro Tip: Even if you feel significantly better after a day or two, do not skip follow-up appointments or prematurely discontinue home care as advised by your dentist. Consistent follow-up ensures complete healing and prevents relapse. If pain or other symptoms worsen, contact your dentist immediately.
Prevention
Preventing a tooth dry socket is significantly easier and less painful than treating it. By understanding the risk factors and adhering to specific guidelines, you can greatly reduce your chances of developing this post-extraction complication.
Before Your Extraction
- Inform Your Dentist:
- Smoking/Tobacco Use: Be honest about your smoking habits. Your dentist may advise you to stop or significantly reduce smoking several days before and after the extraction.
- Medications: Disclose all medications, especially oral contraceptives, blood thinners, or steroids.
- Previous Dry Socket: Inform your dentist if you've experienced dry socket before, as this increases your risk.
- Medical Conditions: Mention any systemic conditions like diabetes or immune disorders.
- Oral Hygiene: Ensure excellent oral hygiene before the extraction. A clean mouth with minimal bacteria reduces the risk of clot breakdown. Your dentist may prescribe a chlorhexidine mouthwash to use before and/or after the procedure.
- Discuss Prophylactic Measures: Your dentist might use specific techniques or materials to help prevent dry socket, especially during more complex extractions:
- Antiseptic Rinses: Pre-operative chlorhexidine rinses.
- Placement of Absorbable Materials: Some dentists place absorbable materials (e.g., gel foam, collagen plug) in the socket after extraction to help stabilize the blood clot.
- PRP/PRF: Platelet-Rich Plasma or Platelet-Rich Fibrin, derived from your own blood, can sometimes be used to enhance healing and stabilize the clot.
- Antibiotics: In high-risk cases (e.g., infected site, immunocompromised patient, traumatic extraction), prophylactic antibiotics might be prescribed, although this is not routine for all extractions.
After Your Extraction (Crucial Steps)
- Protect the Blood Clot (First 24-48 hours are most critical):
- Avoid Sucking Actions: Do NOT use straws, spit vigorously, or smoke. These actions create negative pressure that can dislodge the crucial blood clot. If you smoke, this is the most important time to refrain.
- Avoid Vigorous Rinsing: For the first 24 hours, do not rinse your mouth. After that, only gentle saltwater rinses as directed by your dentist.
- Avoid Touching the Site: Do not poke or prod the extraction site with your fingers or tongue.
- Manage Bleeding: Gently bite down on the gauze pad placed by your dentist for at least 30-60 minutes, changing it as needed. Pressure helps the clot form.
- Dietary Modifications:
- Soft Foods: Stick to a soft food diet for the first few days.
- Chew on Opposite Side: Try to chew on the side of your mouth opposite the extraction site.
- Avoid Hot Liquids: Hot beverages can dissolve the blood clot and increase bleeding.
- Oral Hygiene:
- Brush Gently: Brush your teeth carefully, avoiding the extraction site for the first day. After 24 hours, you can gently brush the adjacent teeth.
- Warm Saltwater Rinses: After 24 hours, gently rinse your mouth with warm salt water several times a day (1/2 teaspoon salt in 8 ounces warm water). Do not swish forcefully.
- Rest and Recuperation: Avoid strenuous activity for at least 24-48 hours. Rest helps your body conserve energy for healing.
- Stay Hydrated: Drink plenty of fluids, but avoid alcohol and sugary drinks.
- Medication Adherence: Take any prescribed medications (pain relievers, antibiotics) as directed by your dentist.
Pro Tip: If you are a smoker, consider this an excellent opportunity to quit or at least significantly reduce your intake. The risks associated with dry socket are a strong motivator, and your overall health will benefit immensely. Discuss nicotine replacement therapy with your doctor prior to your extraction if you anticipate difficulty.
By following these guidelines diligently, you can significantly lower your risk of developing a dry socket and ensure a smoother, more comfortable recovery after your tooth extraction.
Risks and Complications
While a tooth dry socket is primarily a painful condition, it is typically not life-threatening. However, ignoring its symptoms or delaying treatment can lead to prolonged discomfort and potentially more serious complications.
Primary Risks Associated with Dry Socket
- Intense and Prolonged Pain: This is the most immediate and significant risk. The severe, radiating pain can be debilitating, impacting your ability to eat, sleep, work, and concentrate, lasting for days or even weeks if untreated.
- Increased Risk of Infection: While dry socket itself is not an infection, the exposed bone and open socket are highly susceptible to bacterial contamination from the mouth. Food debris can accumulate, providing a breeding ground for bacteria, leading to a secondary infection in the socket (osteomyelitis) or surrounding soft tissues.
- Delayed Healing: The absence of a blood clot and subsequent irritation of the bone significantly delays the natural healing process of the extraction site. What might normally heal in a week or two can take much longer.
- Bad Breath and Taste (Halitosis and Dysgeusia): The exposed tissue and bacterial activity contribute to a foul odor and unpleasant metallic taste, which can be embarrassing and further impact quality of life.
Potential (Less Common) Complications if Untreated
- Osteomyelitis: If a secondary infection in the dry socket spreads to the jawbone itself, it can lead to osteomyelitis, a severe bone infection. This is a rare but serious complication requiring aggressive antibiotic therapy and sometimes surgical debridement (removal of infected bone). Symptoms might include persistent fever, pus discharge, significant swelling, and extreme pain.
- Spread of Infection: In very rare cases, an untreated infection originating from a dry socket could potentially spread to surrounding tissues, including the face and neck. This could cause cellulitis (skin infection), abscess formation, or even deeper space infections, which are medical emergencies.
- Damage to Nearby Teeth or Bone: Although not a direct complication of dry socket, the prolonged inflammation and potential infection could theoretically compromise the health of adjacent teeth or delay the integration of future dental implants if the site is intended for restoration.
- Nutritional Deficiencies/Dehydration: Due to severe pain, individuals with dry socket may struggle to eat and drink adequately, potentially leading to temporary nutritional deficiencies or dehydration, especially in vulnerable populations like the elderly or those with underlying health issues.
Pro Tip: Do not attempt to self-diagnose or self-treat dry socket beyond very gentle home care while awaiting a dental appointment. Over-the-counter remedies or improper attempts to clean the socket can worsen the condition or introduce infection. Always consult your dentist immediately if you suspect you have a dry socket. Early intervention is key to minimizing discomfort and preventing complications.
Children / Pediatric Considerations
Dry socket is significantly less common in children and adolescents compared to adults, primarily because dental extractions in younger patients are usually simpler, involving deciduous (baby) teeth or permanent teeth that are not impacted. The bone is also less dense and heals more rapidly in younger individuals, reducing the risk of clot instability. However, it can still occur, and parents should be aware of the signs.
Why It's Less Common in Children:
- Simpler Extractions: Most extractions in children involve primary teeth, which have shallower roots and typically resorb naturally, making their removal less traumatic.
- Faster Healing: Children's bodies generally have a more robust and faster healing response.
- Less Dense Bone: The alveolar bone in children is less dense, promoting better blood supply and clot stability.
- Fewer Risk Factors: Children are less likely to smoke or use oral contraceptives, which are major adult risk factors.
Signs and Symptoms in Children:
The symptoms of dry socket in children are similar to those in adults:
- Intense Pain: Unexplained, severe pain that starts 2-4 days after an extraction and does not respond well to typical children's pain relievers (e.g., children's ibuprofen or acetaminophen).
- Pain Radiating: The child may complain of pain extending to the ear or jaw on the affected side.
- Foul Odor/Taste: Parents might notice bad breath or the child complaining of a bad taste in their mouth.
- Difficulty Eating/Sleeping: Due to pain.
- Visible Empty Socket: Although children might not articulate this, parents might observe an empty socket where a dark blood clot should be.
Parental Guidance:
- Strict Adherence to Post-Extraction Instructions: This is the most crucial preventive measure. Ensure your child avoids:
- Straws: Explain to them why sucking is harmful.
- Spitting: Encourage gentle swallowing.
- Vigorous Rinsing: Supervise saltwater rinses, ensuring they are gentle.
- Hard/Crunchy Foods: Stick to soft foods as recommended.
- Monitor Pain Levels: While some pain is normal, be vigilant for escalating or prolonged pain that seems disproportionate to a simple extraction.
- Observe Oral Hygiene: Ensure your child maintains gentle oral hygiene, including supervised gentle brushing around the extraction site and gentle saltwater rinses if prescribed.
- Contact Pediatric Dentist Immediately: If you suspect your child has a dry socket, contact their pediatric dentist without delay. Do not try to treat it at home.
Treatment for Children:
Treatment for dry socket in children follows similar principles as for adults:
- Gentle Irrigation: Cleaning the socket to remove debris.
- Medicated Dressing: Placement of a pain-relieving dressing (often eugenol-based).
- Pain Management: Prescription of appropriate pain medication for children.
- Follow-Up: Regular follow-up appointments for dressing changes and monitoring healing.
Pediatric dentists are skilled in managing dry socket in children, using age-appropriate techniques and communication to ensure the child's comfort and cooperation throughout the treatment process. Prompt action ensures a quick return to comfort for your child.
Cost Breakdown
While dry socket treatment is usually manageable, a clear breakdown of potential costs helps in financial planning. This section reiterates and expands on the financial aspects, focusing on average US costs.
Average US Costs for Dry Socket Treatment
The cost of treating dry socket is generally categorized by individual visits or services.

- Initial Emergency Exam: If you need an unscheduled or emergency visit for diagnosis, this typically costs $75 - $150. This covers the dentist's time for evaluation and diagnosis.
- Dry Socket Treatment (Per Visit): Each visit involving irrigation and the placement of a medicated dressing usually costs $75 - $300. The total cost will depend on the number of follow-up visits required. Most cases require 2-4 visits.
- Prescription Medications:
- Pain Relievers (e.g., Tramadol, Hydrocodone): $10 - $50+ depending on the drug and quantity.
- Antibiotics (if infection present): $10 - $60+ for a typical course.
- Additional Procedures (Rare): If severe infection leads to complications like an abscess, additional procedures might be needed, which would incur significantly higher costs (e.g., drainage procedures $200 - $500, surgical debridement $500 - $1500+), but these are not typical for routine dry socket.
Example Scenario Cost Estimation:
- Simple Case (1-2 visits):
- Initial Exam: $100
- 1 Treatment Visit: $150
- Total: $250
- Moderate Case (3-4 visits + meds):
- Initial Exam: $100
- 3 Treatment Visits x $150: $450
- Prescription Pain Meds: $20
- Total: $570
With vs. Without Insurance
The impact of dental insurance is significant for dry socket treatment.
- Without Insurance: You will be responsible for 100% of the costs detailed above.
- With Insurance: Most dental insurance plans cover dry socket treatment as a basic restorative service.
- Deductible: You'll likely pay your annual deductible first (common deductibles range from $50 - $150).
- Coverage Percentage: After the deductible, your plan typically covers 70-80% of the cost. You pay the remaining 20-30% (co-payment).
- Example: For a $150 treatment visit, if your deductible is met and coverage is 80%, you would pay $30.
- Medical Insurance for Prescriptions: Prescription medications are usually covered by your medical insurance's pharmacy benefits, often with a co-pay (e.g., $5 - $30).
Payment Plans and Financing Options
For those without insurance or facing high out-of-pocket costs:
- In-House Payment Plans: Many dental offices offer flexible payment arrangements, allowing you to pay your balance over a few months.
- Third-Party Medical/Dental Credit Cards: Companies like CareCredit or LendingClub offer specialized credit options for healthcare expenses. They often have interest-free promotional periods if paid in full within a certain timeframe (e.g., 6 or 12 months).
- Dental Discount Plans: These are membership programs where you pay an annual fee to get a discounted rate on services from participating dentists (typically 10-50% off).
- Community Dental Clinics: Some non-profit or dental school clinics offer services at reduced rates.
Cost-Saving Tips
- Prevent, Prevent, Prevent: The absolute best way to save money is to prevent dry socket in the first place by strictly following post-extraction instructions.
- Verify Insurance Benefits: Always call your insurance provider to confirm coverage details before treatment.
- Ask for an Estimate: Request a detailed cost estimate from your dental office before treatment begins.
- Discuss Options: Don't hesitate to discuss payment concerns with your dental office. They often have solutions or can refer you to resources.
- Prescription Savings: Use generic versions of medications if available, and check pharmacy discount programs (e.g., GoodRx) for better prices on prescriptions.
Frequently Asked Questions
Is dry socket an emergency?
While not life-threatening, dry socket is considered a dental emergency due to the severe pain it causes and the potential for secondary infection. It requires prompt professional dental attention to relieve discomfort and initiate proper healing. You should contact your dentist immediately if you suspect you have it.
How long does dry socket pain last after treatment?
Most patients experience significant pain relief within a few hours of the first medicated dressing application. With subsequent dressing changes and proper home care, the pain usually subsides completely within 2-3 days, with full resolution of the dry socket typically taking 7-10 days.
Can dry socket heal on its own without a dentist?
Technically, a dry socket can eventually heal on its own, but it will be an incredibly painful and prolonged process, potentially lasting weeks. It also carries a much higher risk of developing a secondary bacterial infection. Professional treatment is highly recommended for pain relief, faster healing, and complication prevention.
What does dry socket look like?
When you look into your mouth, you might see an empty, whitish-looking socket where the tooth was removed. Instead of a dark red or brownish blood clot, you might see exposed bone. Sometimes there might be some gray debris in the socket.
Can I get dry socket from a top tooth extraction?
Yes, while dry socket is significantly more common after lower wisdom tooth extractions, it can occur after any permanent tooth extraction, including upper teeth. The risk factors, symptoms, and treatment remain the same regardless of the tooth's location.
How much does it cost to treat dry socket without insurance?
Without insurance, a single visit for dry socket treatment (irrigation and dressing) typically costs between $75 and $300. Since multiple visits are usually required, the total cost for treatment can range from $250 to over $600, not including prescription medications.
What's the difference between normal extraction pain and dry socket pain?
Normal extraction pain is usually a dull ache that peaks within 24-48 hours and gradually improves. It's manageable with over-the-counter pain relievers. Dry socket pain, however, is an intense, throbbing pain that often starts 2-4 days post-extraction, worsens over time, radiates to the ear/jaw, and is poorly relieved by standard pain medications.
Can food get stuck in a dry socket?
Yes, food particles and other debris can easily get trapped in an open dry socket because there's no blood clot to protect it. This can exacerbate pain, introduce bacteria, and make the situation worse, highlighting the importance of gentle cleaning and protective dressings.
Are there any alternatives to professional dry socket treatment?
There are no effective alternatives to professional dental treatment for dry socket. Home remedies, while they might offer very temporary, mild relief (like saltwater rinses), cannot adequately clean the socket, protect the exposed bone, or provide the necessary local anesthesia and healing agents found in medicated dressings.
Can dry socket cause bad breath?
Yes, dry socket commonly causes very noticeable bad breath (halitosis) and an unpleasant taste in the mouth. This is due to the exposed bone and potential accumulation of food debris and bacteria within the empty socket. This is a key diagnostic symptom.
When to See a Dentist
Knowing when to seek professional help for post-extraction discomfort is crucial. While some pain and swelling are normal after a tooth extraction, certain signs indicate a dry socket or another complication requiring immediate dental attention.
Immediate Contact with Your Dentist if You Experience:
- Severe, Throbbing Pain: This is the most significant indicator. If your pain is intense, deep-seated, and throbbing, especially if it starts 2-4 days after your extraction and is unresponsive to prescribed or over-the-counter pain medication.
- Radiating Pain: If the pain from the extraction site spreads to your ear, temple, eye, or neck on the same side of your face.
- Visible Empty Socket: If you look into your mouth and see exposed bone (a whitish area) where the blood clot should be in the extraction site.
- Foul Odor or Unpleasant Taste: A distinctly foul smell coming from your mouth or a bad, metallic, or strange taste that persists.
- Signs of Infection: While less common for dry socket itself, if you notice pus draining from the socket, significant and increasing swelling around the jaw or face, fever, or chills, these could indicate a secondary infection.
Red Flags vs. Routine Post-Operative Symptoms:
| Symptom | Routine Post-Op (Normal) | Red Flag (See Dentist Immediately) |
|---|---|---|
| Pain | Mild to moderate, peaks in 24-48 hrs, gradually subsides | Severe, throbbing, escalating 2-4 days post-op, radiating, unresponsive to meds |
| Swelling | Mild to moderate, peaks in 24-48 hrs, gradually subsides | Significant, increasing swelling of face/jaw, particularly with pus or fever |
| Bleeding | Oozing for 24-48 hrs | Heavy, uncontrolled bleeding |
| Taste/Odor | Mildly altered taste or breath | Foul, persistent bad breath or unpleasant taste |
| View of Socket | Dark red/brown blood clot | Empty socket, exposed bone (whitish) |
| Fever | No fever or very low-grade (99-100°F) | Persistent fever (over 100.4°F), chills |
Emergency vs. Scheduled Appointment Guidance:
- Dry socket is generally considered an urgent condition. You shouldn't wait for a routine scheduled appointment if you suspect you have it. The pain warrants immediate attention, and prompt treatment will significantly improve your comfort and healing trajectory.
- Call your dental office right away. Explain your symptoms to the receptionist or nurse. They will advise you on the best course of action, which typically involves an emergency or same-day appointment.
- If your dental office is closed and you are in severe pain or have signs of infection, seek care at an urgent dental care clinic or an emergency room. While an ER might not treat the dry socket directly, they can provide pain management and antibiotics for infection until you can see your dentist.
Your dental health is important, and prompt attention to post-extraction complications like dry socket can prevent unnecessary suffering and ensure a smooth recovery.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
How to Relieve Gum Swelling
When your gums are swollen, it can be an alarming and uncomfortable experience, often signaling an underlying issue that requires attention. Statistics from the Centers for Disease Control and Prevention (CDC) reveal that **nearly half of adults aged 30 or older in the United States have some form o
February 23, 2026
Teeth Swelling: Complete Guide
When you experience teeth swelling, it's more than just a minor discomfort; it's a clear signal from your body that something is amiss within your oral cavity, often indicating an underlying infection or inflammation that requires prompt attention. A recent survey revealed that **over 25% of adu
February 23, 2026
Submandibular Salivary Gland Swelling: Complete Guide
When you notice a peculiar lump or uncomfortable fullness beneath your jaw, it can be an alarming experience. This sensation, often accompanied by pain and difficulty swallowing, could indicate submandibular salivary gland swelling. Affecting an estimated 1 in 10,000 adults annually, conditi
February 23, 2026
What Helps With Gum Swelling
Gum swelling, medically known as gingival swelling or gingivitis, is a common yet often underestimated dental issue affecting millions of Americans. Have you ever woken up with sore, puffy gums that bleed easily when you brush? You're not alone. Research indicates that nearly **half of all a
February 23, 2026