Cost of Teeth Implants: Complete Price Guide 2026

Key Takeaways
- Every year, millions of Americans experience tooth loss, a challenge that impacts not just their smile, but their ability to chew, speak, and even their overall health. While traditional dentures and bridges have long been solutions, dental implants have emerged as the gold standard for tooth re
Every year, millions of Americans experience tooth loss, a challenge that impacts not just their smile, but their ability to chew, speak, and even their overall health. While traditional dentures and bridges have long been solutions, dental implants have emerged as the gold standard for tooth replacement, offering unparalleled stability, aesthetics, and longevity. However, for many, the primary concern, and often the biggest barrier, is understanding the cost of teeth implants. As we look to 2026, navigating tooth implant pricing can feel complex, with various factors influencing the final bill.
This comprehensive guide from SmilePedia.net aims to demystify the financial aspects of dental implants. We'll break down the different types of implants, the procedures involved, and the intricate factors that contribute to the overall cost. You'll gain a clear understanding of what to expect, how insurance might factor in, and strategies to make this life-changing investment more manageable. From single tooth replacements to full arch restorations, we'll provide detailed cost ranges, helping you plan your journey to a restored smile with confidence.
Key Takeaways:
- Single Tooth Implant Cost (2026): Expect to pay between $3,000 and $6,500 per tooth, including the implant, abutment, and crown. This can reach $8,000 with complex preparatory procedures like bone grafting.
- Full Arch/Mouth Implants (2026): All-on-4 or similar full-arch solutions typically range from $20,000 to $35,000 per arch (upper or lower), and up to $60,000 to $80,000 for a full mouth restoration.
- Factors Influencing Cost: Price varies significantly based on geographic location, dentist's expertise, type of implant material, number of implants, and necessary pre-procedures (e.g., bone graft, tooth extraction).
- Insurance Coverage: While most dental insurance plans offer limited coverage (typically 10-50%) for the crown or abutment, the implant post itself is often not covered. Medical insurance may cover portions if tooth loss is due to injury or disease.
- Additional Procedures: Bone grafting (ranging from $200 to $3,500+), tooth extractions ($75 to $600), and CT scans ($150 to $500) can add significantly to the total tooth implant pricing.
- Longevity & Value: Despite the initial investment, dental implants are a long-term solution, potentially lasting 20-30 years or even a lifetime with proper care, offering superior value compared to recurring costs of bridges or dentures.
- Financing Options: Many dental practices offer payment plans, third-party financing (like CareCredit), and discounts for upfront payments to help manage the cost.
What Are Dental Implants? An Overview
Dental implants are sophisticated devices designed to replace missing tooth roots, providing a strong foundation for artificial teeth that look, feel, and function like natural teeth. Unlike dentures that rest on the gums or bridges that rely on adjacent teeth for support, a dental implant is surgically placed into the jawbone, where it fuses directly with the bone through a process called osseointegration. This biological bond creates an incredibly stable and durable anchor.
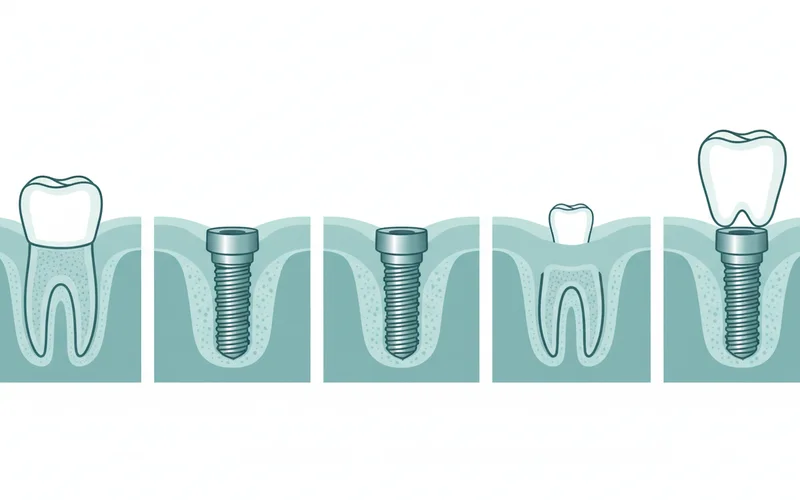
A typical dental implant consists of three main components:
- The Implant Post (Fixture): This is a small, screw-shaped post, usually made of biocompatible titanium or zirconia, that is surgically inserted into the jawbone. It acts as the artificial tooth root.
- The Abutment: This is a connector piece that screws onto the implant post and extends above the gum line. It serves as the attachment point for the visible crown, bridge, or denture.
- The Restoration (Crown, Bridge, or Denture): This is the custom-made artificial tooth or set of teeth. A single missing tooth will receive a custom crown. If multiple teeth are missing, a bridge or a full denture can be secured onto several implants.
Dental implants are a significant advancement in restorative dentistry, preserving jawbone health, maintaining facial structure, and providing a stable, comfortable, and aesthetically pleasing solution for tooth loss.
Types of Dental Implants and Their Variations
Understanding the different types of dental implants is crucial for comprehending the range in tooth implant pricing. While the basic concept remains the same, variations exist in design, material, and placement technique to address diverse patient needs and oral health conditions.
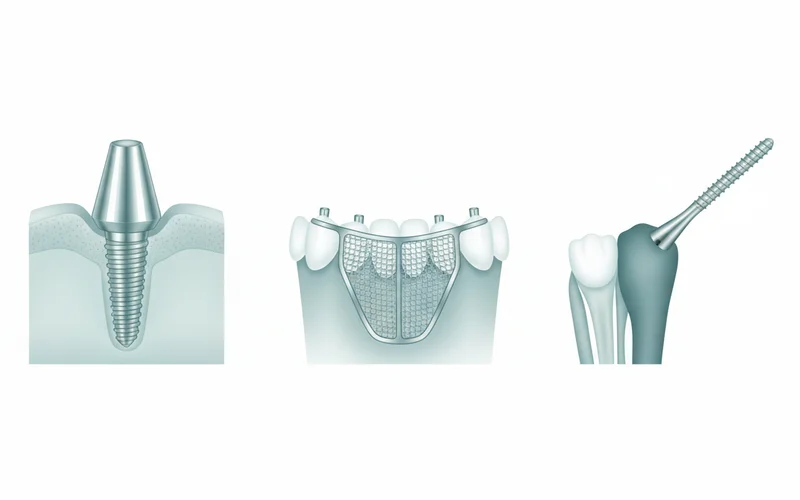
Endosteal Implants (In-Bone Implants)
These are the most common type of dental implant. They are typically shaped like small screws, cylinders, or blades and are surgically placed directly into the jawbone.
- Standard Endosteal Implants: These are the traditional titanium implants used for most single tooth replacements, multiple teeth, or full arch restorations. They require sufficient bone density for successful integration.
- Pros: High success rate, excellent stability, long-lasting.
- Cons: Requires adequate bone, involves surgery, longer healing time.
Subperiosteal Implants (On-Bone Implants)
These implants are much less common today. Instead of being placed into the bone, subperiosteal implants consist of a metal framework that is fitted on top of the jawbone, just under the gum tissue. Posts extending from the framework protrude through the gums to hold the prosthetic teeth.
- Pros: An option for patients with insufficient bone height who cannot undergo bone grafting.
- Cons: Lower long-term success rates compared to endosteal implants, more prone to complications, generally not recommended by modern dentistry.
Zygomatic Implants
These are specialized, longer implants used in the cheekbone (zygoma) when there is severe bone loss in the upper jaw, making conventional implants impossible without extensive bone grafting. They are anchored into the dense zygomatic bone.
- Pros: Avoids the need for complex and lengthy bone grafting procedures for upper jaw restoration.
- Cons: More complex surgery, fewer dentists are trained to perform them, higher cost.
Mini Dental Implants (MDIs)
MDIs are smaller in diameter than traditional implants (typically less than 3mm). They are primarily used for stabilizing lower dentures or for temporary anchorage during orthodontic treatment.
- Pros: Less invasive placement, faster recovery, often lower cost, useful for denture stabilization or narrow bone ridges.
- Cons: Less durable than traditional implants, not suitable for replacing individual teeth that bear heavy chewing forces, generally a temporary or less permanent solution.
Specialized Implant Systems and Approaches
Beyond the basic types, there are specific systems and approaches that cater to different situations:
- All-on-4® Dental Implants (or All-on-X): This revolutionary technique allows for a full arch of prosthetic teeth (upper or lower) to be supported by just four strategically placed implants (sometimes 5 or 6, hence All-on-X). The posterior implants are typically angled to maximize contact with available bone, often bypassing the need for bone grafting.
- Pros: Can restore an entire arch with fewer implants, immediate function often possible, reduces the need for extensive bone grafting, streamlined procedure.
- Cons: Higher initial cost than traditional dentures, requires specialized surgical skill.
- Immediate Load Dental Implants (Same-Day Implants): In certain favorable conditions, a temporary crown or restoration can be placed on the implant immediately after surgical placement.
- Pros: Faster aesthetic and functional results, fewer appointments.
- Cons: Not suitable for all patients, higher risk of failure if not carefully selected, requires ideal bone quality and primary stability.
- Implant-Supported Bridges: For multiple missing teeth in a row, two or more implants can support a fixed dental bridge, eliminating the need to modify adjacent healthy teeth.
- Implant-Supported Dentures (Overdentures): Removable dentures that snap onto implants, providing far greater stability and retention than conventional dentures. They can be supported by 2-6 implants per arch.
The Step-by-Step Process: What to Expect During Treatment
Embarking on the journey of receiving dental implants is a multi-stage process designed to ensure optimal success and longevity. While timelines can vary, understanding each phase will help you appreciate the comprehensive nature of tooth implant pricing.
1. Initial Consultation and Treatment Planning
Your journey begins with a thorough examination by a qualified dental professional, often an oral surgeon or periodontist, alongside your general dentist. This stage involves:
- Comprehensive Oral Examination: Assessment of your overall oral health, remaining teeth, and gum condition.
- Advanced Imaging: X-rays, 3D CT scans, and panoramic radiographs are critical to evaluate bone quality, quantity, and location of vital structures (nerves, sinuses) to plan precise implant placement.
- Medical History Review: Discussion of your general health, medications, and any conditions that might impact healing or implant success (e.g., diabetes, smoking).
- Treatment Discussion: Your dentist will explain the recommended implant type, procedure details, timeline, and associated costs.
- Custom Treatment Plan: A personalized plan is developed, outlining all necessary steps, including any preparatory procedures.
2. Preparatory Procedures (If Needed)
Some patients may require additional procedures before implant placement to ensure a successful outcome. These contribute significantly to the overall cost of teeth implants.
- Tooth Extraction: If the damaged or decayed tooth is still present, it must be carefully removed. Depending on the complexity, this can range from a simple extraction to a surgical extraction.
- Bone Grafting: If your jawbone lacks sufficient volume or density due to tooth loss, trauma, or gum disease, bone grafting is necessary to build up the bone. This involves placing bone material (from your own body, a donor, or synthetic) at the implant site. Healing can take several months.
- Sinus Lift: A specific type of bone graft performed in the upper jaw when there isn't enough bone between the jaw and the maxillary sinuses.
- Ridge Augmentation: A procedure to restore the natural contour of the jawbone after tooth loss.
- Gum Disease Treatment: Active gum disease must be treated and resolved before implant placement.
3. Dental Implant Placement Surgery
Once your jawbone is ready, the implant post is surgically placed.
- Anesthesia: Local anesthesia is typically used, often combined with sedation (oral, IV, or nitrous oxide) for patient comfort.
- Incision and Drilling: The gum tissue is opened to expose the bone, and a small pilot hole is carefully drilled into the jawbone at the precise location determined during planning. This hole is then gradually widened.
- Implant Insertion: The titanium or zirconia implant post is carefully screwed or tapped into the prepared bone socket.
- Gum Closure: The gum tissue is closed over the implant (submerged technique) or around a healing abutment (one-stage technique).
This surgical phase usually takes 1-2 hours for a single implant.
4. Osseointegration and Healing Period
This is a critical phase where the implant fuses with the surrounding jawbone.
- Duration: Osseointegration typically takes 3 to 6 months, though it can be shorter or longer depending on bone quality and individual healing rates.
- Temporary Solutions: During this time, you may wear a temporary denture or bridge to maintain aesthetics and function.
- Monitoring: Your dentist will monitor the healing progress.
5. Abutment Placement (If Not Done During Surgery)
If the implant was placed below the gum line (submerged technique), a minor follow-up procedure is needed to expose the implant and attach the abutment.
- Procedure: A small incision is made in the gum to uncover the implant, and the abutment (a small connector post) is screwed onto the implant.
- Gum Healing: The gum tissue then heals around the abutment for a few weeks, creating a natural-looking collar for the final restoration.
6. Restoration Placement (Crown, Bridge, or Denture)
Once the implant has fully integrated and the gums have healed around the abutment, your final restoration can be fabricated and placed.
- Impressions: Impressions (digital or traditional molds) of your mouth and the abutment are taken.
- Custom Fabrication: These impressions are sent to a dental lab where your custom crown, bridge, or denture is meticulously crafted to match your natural teeth in shape, size, and color. This can take several weeks.
- Final Attachment: At your final appointment, the custom-made restoration is securely attached to the abutment, completing your new smile.
- Adjustments: Your dentist will make any necessary adjustments to ensure a comfortable fit and proper bite.
Cost of Dental Implants: A Detailed Breakdown for 2026
Understanding the cost of teeth implants requires a look at not just the implant itself, but all the associated components and procedures. As of 2026, prices reflect advancements in technology, materials, and surgical expertise.
Factors Influencing Dental Implant Cost
Several variables contribute to the final tooth implant pricing:
- Geographic Location: Dental costs vary significantly by region. Major metropolitan areas and coastal cities in the US (e.g., New York, Los Angeles, Boston) typically have higher prices than rural areas or the Midwest.
- Number of Implants: A single implant is less expensive than multiple implants or a full arch restoration.
- Type of Implant: While endosteal titanium implants are standard, specialized implants like zirconia, mini implants, or zygomatic implants can have different price points.
- Type of Restoration: A single crown is less expensive than an implant-supported bridge or a full arch denture. The material of the crown (porcelain-fused-to-metal, all-ceramic, zirconia) also impacts cost.
- Brand of Implant: There are many reputable implant manufacturers (e.g., Straumann, Nobel Biocare, Zimmer Biomet). Premium brands may command higher prices due to extensive research, quality control, and long-term data.
- Dentist's Expertise and Experience: Highly experienced oral surgeons, periodontists, or prosthodontists specializing in implant dentistry may charge more for their advanced skills and higher success rates.
- Preparatory Procedures: The most significant add-ons are often bone grafts, sinus lifts, and tooth extractions.
- Diagnostic Procedures: X-rays, 3D CT scans, and digital impressions are essential for planning and add to the initial cost.
- Anesthesia and Sedation: The type of anesthesia (local, oral sedation, IV sedation, general anesthesia) chosen for the surgery will impact the overall price.
- Custom Abutments: While stock abutments are available, custom-milled abutments (especially for aesthetic areas) offer superior fit and appearance but cost more.
Average US Costs for Dental Implants (2026 Estimates)
These are general ranges, and actual costs can fall outside these figures based on the factors above.
1. Single Tooth Implant Cost
This covers the entire process for replacing one missing tooth.
-
Implant Post (Fixture) Only: $1,500 - $3,000
-
Abutment: $500 - $1,200
-
Dental Crown: $800 - $2,500 (Varies by material – PFM, E-max, Zirconia)
-
Total for a Single Tooth Implant (Implant, Abutment, Crown): $3,000 - $6,500
- With additional procedures (e.g., minor bone graft, extraction): Can reach $4,500 - $8,000+ per tooth.
2. Multiple Tooth Implants
Replacing several adjacent missing teeth often involves an implant-supported bridge.
- 2-3 Implants supporting a 3-4 Unit Bridge: $6,000 - $15,000+
- This cost includes the implants, abutments, and the custom bridge. The number of implants needed for a bridge depends on the span and location.
3. Full Arch Dental Implants (All-on-4® / All-on-X)
This is a comprehensive solution for replacing an entire arch of teeth (upper or lower).
- All-on-4®/All-on-X (per arch): $20,000 - $35,000
- This typically includes the 4-6 implants, abutments, and a fixed provisional denture that can be placed on the same day, followed by a permanent, high-quality fixed prosthesis (e.g., acrylic/titanium hybrid or zirconia).
- Full Mouth Implants (Both Arches): $40,000 - $80,000+ for a complete rehabilitation, potentially including any necessary extractions or bone contouring.
4. Implant-Supported Dentures (Overdentures)
These are removable dentures that snap onto a fewer number of implants for stability.
- Lower Arch (2-4 implants + overdenture): $6,000 - $15,000
- Upper Arch (4-6 implants + overdenture): $10,000 - $25,000 (Upper arch often requires more implants due to bone density differences and palate coverage).
Cost of Common Preparatory Procedures
These can significantly impact the final cost of teeth implants:
- Tooth Extraction (Simple): $75 - $200
- Tooth Extraction (Surgical/Impacted): $200 - $600+
- Bone Grafting (Minor/Site-specific): $200 - $1,200
- Bone Grafting (Major/Block Graft): $1,500 - $3,500+
- Sinus Lift (Internal): $1,000 - $2,000
- Sinus Lift (External/Lateral Window): $2,000 - $3,500+
- CBCT (Cone Beam Computed Tomography) Scan: $150 - $500
- IV Sedation: $300 - $800 per hour
Pro Tip: Always request a detailed, itemized treatment plan from your dentist that clearly breaks down all anticipated costs, including any potential preparatory procedures, implant components, and restorations.
Dental Insurance and Implant Coverage
Navigating insurance coverage for dental implants can be challenging because coverage varies widely.
-
Dental Insurance: Most standard dental insurance plans consider dental implants an elective cosmetic procedure or a major restorative procedure.
- Limited Coverage: Many plans offer some coverage for the dental crown or bridge that goes on top of the implant (often 10-50% of the restoration cost), but typically do not cover the implant post itself (the surgical placement and the implant fixture).
- Annual Maximums: Most dental plans have annual maximums, typically ranging from $1,000 to $2,000 per year. The full cost of an implant often exceeds this, meaning you will likely pay a substantial portion out-of-pocket.
- Waiting Periods: Some plans have waiting periods (e.g., 6-12 months) for major restorative procedures like implants.
- Employer-Sponsored Plans: If your employer offers a high-end dental plan, it might include limited implant coverage. Always check with your HR department or insurance provider directly.
- "Dental Implant Coverage" Plans: Some newer, higher-premium dental plans specifically advertise implant coverage, but it's crucial to understand the exact percentage, limits, and covered components.
-
Medical Insurance: In certain circumstances, your medical insurance might cover a portion of the implant procedure.
- Medical Necessity: If tooth loss is directly related to a medical condition (e.g., oral cancer, severe trauma, genetic defect), or if the procedure is deemed medically necessary to prevent severe health complications, your medical insurance provider might cover some aspects of the surgery.
- Documentation: This typically requires extensive documentation from your dentist and physician, proving medical necessity.
- Pre-Authorization: Always seek pre-authorization from your medical insurance provider before starting any treatment if you believe it falls under medical necessity.
Pro Tip: Before committing to treatment, contact both your dental and medical insurance providers directly. Ask for a detailed explanation of their implant coverage, including any exclusions, annual maximums, deductibles, and waiting periods. Provide them with your dentist's CDT (Current Dental Terminology) codes for each procedure.
Cost Breakdown Table (2026 Estimates)
| Procedure/Component | Average Cost (Low-Mid Range) | Average Cost (High Range) | Notes |
|---|---|---|---|
| Single Tooth Implant | |||
| Implant Post (Fixture) | $1,500 - $2,500 | $3,000 | Titanium, premium brand |
| Abutment | $500 - $1,000 | $1,200 | Standard vs. custom |
| Crown (Porcelain/Zirconia) | $800 - $1,800 | $2,500 | Material and aesthetic demands |
| Total (Single Implant) | $3,000 - $5,300 | $6,700 | Excludes complex preparatory procedures |
| Full Arch (All-on-4/X) | |||
| Per Arch (Upper or Lower) | $20,000 - $30,000 | $35,000 | Includes 4-6 implants, abutments, and fixed prosthesis (acrylic/titanium hybrid) |
| Both Arches (Full Mouth) | $40,000 - $60,000 | $80,000 | Can include extractions, advanced prosthetics |
| Implant-Supported Overdenture | |||
| Lower Arch (2-4 implants) | $6,000 - $12,000 | $15,000 | Removable, uses fewer implants |
| Upper Arch (4-6 implants) | $10,000 - $20,000 | $25,000 | Removable, often requires more implants for stability |
| Common Add-on Procedures | |||
| Tooth Extraction (Surgical) | $200 - $400 | $600 | Per tooth |
| Bone Graft (Minor Site) | $200 - $800 | $1,200 | Small area, synthetic/cadaver bone |
| Sinus Lift (Internal) | $1,000 - $1,500 | $2,000 | Less invasive, for minor bone height issues |
| Sinus Lift (External) | $2,000 - $2,800 | $3,500 | More complex, for significant bone loss |
| CBCT Scan | $150 - $300 | $500 | Essential 3D imaging |
| IV Sedation | $300 - $600 per hour | $800 per hour | For surgical comfort |
Payment Plans and Financing Options
Given the significant investment, many patients explore financing options to make dental implants affordable.
- In-Office Payment Plans: Many dental practices offer their own interest-free payment plans, allowing you to pay in installments over several months.
- Third-Party Medical/Dental Financing: Companies like CareCredit, LendingClub, or Alphaeon Credit specialize in healthcare financing. They offer various plans, including interest-free options for a set period (e.g., 6, 12, or 18 months) or longer-term plans with fixed interest rates.
- Personal Loans: Banks and credit unions offer personal loans that can be used for any purpose, including dental treatments. Interest rates depend on your credit score.
- Credit Cards: While an option, using high-interest credit cards for large expenses should be approached with caution to avoid accumulating significant debt.
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): If you have an HSA or FSA through your employer, you can use these tax-advantaged accounts to pay for dental implants. You're using pre-tax dollars, which can result in significant savings.
Cost-Saving Tips for Dental Implants
While dental implants are a premium solution, there are ways to potentially reduce the overall cost of teeth implants:
- Dental Schools: University dental schools often offer implant procedures at a reduced cost. These procedures are performed by students under the direct supervision of experienced faculty. The trade-off can be longer appointment times and a more extended treatment timeline.
- Comparison Shopping: Get quotes from several reputable dentists or specialists in your area. Don't just compare prices; also compare their experience, patient reviews, and the quality of materials they use.
- Ask for Discounts: Some practices offer discounts for upfront payment in full, or for patients without insurance. It never hurts to ask!
- Travel for Treatment: In some cases, patients consider traveling to other countries where dental work is significantly cheaper (dental tourism). However, this comes with risks regarding quality control, follow-up care, and potential language barriers. If considering this, research thoroughly and understand the potential complications.
- Maximize Insurance: Understand your benefits fully and strategize with your dental office to maximize annual maximums, potentially by spreading parts of the treatment over two calendar years if your plan renews.
- Maintain Good Oral Hygiene: Preventing further tooth loss or gum disease can avoid additional, costly procedures down the line.
Recovery and Aftercare for Dental Implants
Proper recovery and diligent aftercare are crucial for the long-term success and longevity of your dental implants, helping protect your significant investment in tooth implant pricing.
Immediate Post-Operative Care (First 24-72 Hours)
- Pain Management: Expect some discomfort. Your dentist will prescribe pain medication or recommend over-the-counter options (e.g., ibuprofen, acetaminophen). Take as directed.
- Swelling: Apply an ice pack to the outside of your cheek for 15-20 minutes on, 20 minutes off, for the first 24-48 hours to minimize swelling.
- Bleeding: Slight bleeding or oozing is normal. Bite gently on gauze pads and change them every 30-45 minutes until bleeding subsides. Avoid spitting, rinsing vigorously, or using straws as this can dislodge the blood clot.
- Diet: Stick to soft foods for the first few days (e.g., yogurt, soup, mashed potatoes, smoothies). Avoid hot foods/drinks, crunchy, spicy, or acidic foods.
- Oral Hygiene: Do NOT brush or rinse vigorously around the surgical site for the first 24 hours. After 24 hours, gentle rinsing with a prescribed antimicrobial mouthwash or warm salt water (1/2 teaspoon salt in 8 ounces warm water) can begin, up to 2-3 times a day. Brush other areas of your mouth normally, being careful near the surgical site.
- Activity: Rest and avoid strenuous physical activity for at least 48-72 hours to prevent increased bleeding and swelling.
- Smoking/Alcohol: Absolutely avoid smoking and alcohol, as they significantly impede healing and increase the risk of implant failure.
Weeks Following Surgery
- Diet: Gradually reintroduce solid foods as comfort allows, but continue to avoid chewing directly on the implant site until your dentist advises otherwise.
- Oral Hygiene: Continue gentle brushing around the implant site and using prescribed mouthwash. Your dentist may give you specific instructions for cleaning.
- Medications: Complete any prescribed antibiotics to prevent infection.
- Follow-Up Appointments: Attend all scheduled follow-up appointments so your dentist can monitor healing and remove sutures if necessary.
Long-Term Care and Maintenance
Once your dental implants are fully restored, treating them like natural teeth is key to their longevity.
- Excellent Oral Hygiene: Brush at least twice a day with a soft-bristled toothbrush and floss daily, paying special attention around the implant. Interdental brushes or water flossers can be particularly effective.
- Regular Dental Check-ups: Visit your dentist and hygienist every 6 months for professional cleanings and examinations. They will specifically check the health of your implants, surrounding gums, and bone. ADA guidelines emphasize the importance of regular professional care.
- Avoid Harmful Habits: Do not chew on ice, hard candies, or use your teeth as tools. If you grind or clench your teeth (bruxism), your dentist may recommend a nightguard to protect your implants and natural teeth.
- Healthy Lifestyle: A balanced diet and avoiding smoking will contribute to overall oral health and the long-term success of your implants.
Pro Tip: Treat your implants with the same care, if not more, than your natural teeth. Consistent oral hygiene and professional maintenance are non-negotiable for ensuring your investment lasts a lifetime.
Risks and Complications of Dental Implants
While dental implants boast a high success rate (typically over 95%), like any surgical procedure, there are potential risks and complications to be aware of. Understanding these can help you make an informed decision regarding the cost of teeth implants versus the potential issues.
Common Risks and Minor Complications:
- Infection: Although rare, infection at the implant site can occur, especially if post-operative care instructions are not followed. This is usually treatable with antibiotics or, in some cases, removal of the implant.
- Nerve Damage: During placement, there is a small risk of damaging nerves, particularly in the lower jaw. This can lead to numbness, tingling, or pain in the lips, chin, tongue, or gums. Modern 3D imaging significantly reduces this risk.
- Sinus Problems: For upper jaw implants, there's a slight risk of the implant protruding into the sinus cavity, which can lead to sinus inflammation or infection. Sinus lifts are performed to mitigate this.
- Gum Recession: Over time, the gum tissue around the implant may recede, exposing the implant collar or abutment. This can be an aesthetic concern and may require gum grafting.
- Peri-Implantitis: This is an inflammatory condition affecting the gum and bone tissues surrounding a dental implant, similar to gum disease around natural teeth. If left untreated, it can lead to bone loss and implant failure. Smoking and poor oral hygiene are major risk factors.
Less Common but Serious Complications:
- Implant Failure (Lack of Osseointegration): The implant may fail to integrate with the jawbone. This can be due to poor bone quality, excessive force during healing, infection, or underlying medical conditions. If an implant fails, it typically needs to be removed, the site allowed to heal, and then a new implant can be placed.
- Mechanical Complications: Though rare, components can loosen or break (e.g., abutment screw fracture, crown fracture). These are usually repairable or replaceable.
- Allergic Reaction: Extremely rare, but some individuals might have an allergic reaction to titanium. Zirconia implants offer an alternative for those with suspected metal sensitivities.
Your dentist will discuss these risks with you thoroughly during the consultation phase, assessing your individual risk factors and taking precautions to minimize them. Choosing a highly experienced and qualified dental professional is one of the best ways to reduce potential complications.
When to See a Dentist
Knowing when to seek professional dental attention is crucial, especially when it comes to the success and longevity of your dental implants. While regular check-ups are essential for everyone, certain signs and symptoms warrant immediate attention.
During the Healing Phase (Post-Surgery):
- Severe or Worsening Pain: While some discomfort is normal after surgery, severe pain that doesn't respond to medication or worsens significantly over time is a red flag.
- Excessive Bleeding: If bleeding is heavy, persistent, or bright red after the first 24-48 hours, contact your dentist.
- Significant Swelling or Bruising that Spreads: While some swelling is normal, rapidly increasing swelling, especially if accompanied by fever, could indicate infection.
- Pus or Discharge: Any yellow, green, or foul-smelling discharge from the surgical site is a clear sign of infection.
- Numbness or Tingling that Persists: If numbness in your lip, chin, or tongue doesn't improve within 24 hours post-surgery, it could indicate nerve involvement.
- Fever or Chills: These are signs of a systemic infection.
After Restoration Placement (Long-Term):
- Loose Implant, Abutment, or Crown: If you feel any movement in your implant, abutment, or the crown itself, contact your dentist immediately. Early intervention can often prevent further damage.
- Persistent Pain or Discomfort: While healthy implants shouldn't cause pain, persistent discomfort, throbbing, or pressure around an implant can indicate a problem like peri-implantitis or nerve irritation.
- Swelling, Redness, or Bleeding Gums Around the Implant: These are classic signs of peri-implantitis (gum disease around the implant).
- Receding Gums Around the Implant: If you notice the gum line moving up or down around your implant, exposing more of the abutment or implant collar, it needs evaluation.
- Difficulty Chewing or Biting: Any change in your bite or difficulty chewing could indicate an issue with the implant or surrounding structures.
- Chipped, Cracked, or Broken Crown/Prosthesis: While the implant itself is strong, the crown or bridge can still be damaged.
- Fractured Implant: This is rare but possible, often due to trauma or excessive biting forces.
Routine Care vs. Emergency
- Routine Care: Schedule regular dental check-ups every six months, even if your implants feel fine. These visits allow your dentist and hygienist to monitor your oral health, perform professional cleanings, and catch potential issues early.
- Emergency Care: If you experience any of the severe or persistent symptoms listed above, especially pain, swelling, discharge, or mobility, consider it an urgent matter and contact your dental professional as soon as possible. Don't wait for your next routine appointment.
The American Dental Association (ADA) emphasizes that prompt evaluation of any implant-related concerns is critical for successful long-term outcomes. Early detection and treatment of complications are key to preserving your dental implant and your overall oral health.
Frequently Asked Questions About Dental Implant Costs
Q1: Is the cost of dental implants worth it?
A1: Despite the initial higher cost of teeth implants, most patients and dentists agree they are a worthwhile investment. Implants offer superior stability, functionality, and aesthetics compared to traditional dentures or bridges. They also help preserve jawbone health and can last a lifetime with proper care, making them a cost-effective long-term solution.
Q2: What is the cheapest way to get a dental implant?
A2: The "cheapest" option might be a dental school or traveling abroad for dental tourism, but these come with potential trade-offs in terms of expertise, follow-up care, and material quality. Comparing prices from several local, reputable dentists and inquiring about payment plans or discounts for upfront payment can be a safer approach to managing tooth implant pricing.
Q3: How long do dental implants last?
A3: With excellent oral hygiene and regular dental check-ups, the implant post itself can last 20-30 years, often a lifetime. The crown, bridge, or denture attached to the implant typically lasts 10-15 years before needing replacement due to wear and tear.
Q4: Are dental implants painful?
A4: The dental implant placement procedure is performed under local anesthesia, so you should not feel any pain during the surgery itself. Post-operative discomfort, swelling, and soreness are normal but typically manageable with prescribed pain medication and over-the-counter pain relievers. Most patients report the discomfort is less than expected.
Q5: Can I get a dental implant if I have bone loss?
A5: Yes, in many cases. If you have insufficient jawbone density or height, your dentist might recommend a bone grafting procedure (such as a sinus lift or ridge augmentation) prior to implant placement. While this adds to the cost of teeth implants and extends the treatment timeline, it makes implant placement possible and successful.
Q6: What are the alternatives to dental implants?
A6: The primary alternatives to dental implants are traditional dental bridges and removable dentures. Bridges use adjacent healthy teeth for support, while dentures are removable prosthetics that rest on the gums. While less expensive upfront, these options often don't offer the same stability, comfort, bone preservation benefits, or longevity as implants.
Q7: Why do dental implants cost so much?
A7: The high cost of teeth implants reflects the precision, specialized materials (biocompatible titanium or zirconia), advanced technology (3D imaging, surgical guides), multiple surgical stages, the expertise of highly trained dental specialists (oral surgeons, periodontists, prosthodontists), and the custom fabrication of the final restoration by skilled dental labs. It's a complex, multi-faceted procedure.
Q8: Does dental insurance cover the full cost of implants?
A8: Rarely. Most dental insurance plans offer very limited coverage for implants. They might cover a percentage of the crown or abutment (e.g., 10-50%), but often exclude the implant post and surgical placement itself. Annual maximums are usually too low to cover the full cost. It's essential to verify your specific plan's benefits.
Q9: Can I get an implant immediately after tooth extraction?
A9: In some cases, yes. This is called immediate implant placement. It's only possible if there is no infection, sufficient bone quality and quantity, and the extracted tooth socket is ideal for implant stability. This can reduce the overall treatment time and sometimes the total tooth implant pricing, but it's not suitable for all patients.
Q10: How long does the entire implant process take?
A10: The complete dental implant process, from initial consultation to final restoration, typically takes 3 to 9 months. This includes healing time for any preparatory procedures (like bone grafting), osseointegration (3-6 months), and the fabrication of your custom crown or prosthesis. Some complex cases may take longer.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Implantologist: Complete Guide
Losing a tooth can be a significant setback, impacting not only your smile but also your ability to speak, chew, and maintain overall oral health. In fact, over 3 million Americans currently have dental implants, and that number is projected to grow significantly as more people seek a durable, n
March 8, 2026
Dentures Over Implants: Complete Guide
Missing multiple teeth or even an entire arch can profoundly impact your life, affecting everything from your ability to chew and speak to your self-confidence. For millions of Americans, traditional removable dentures have long been a solution, but they often come with compromises: slipping, discom
March 8, 2026
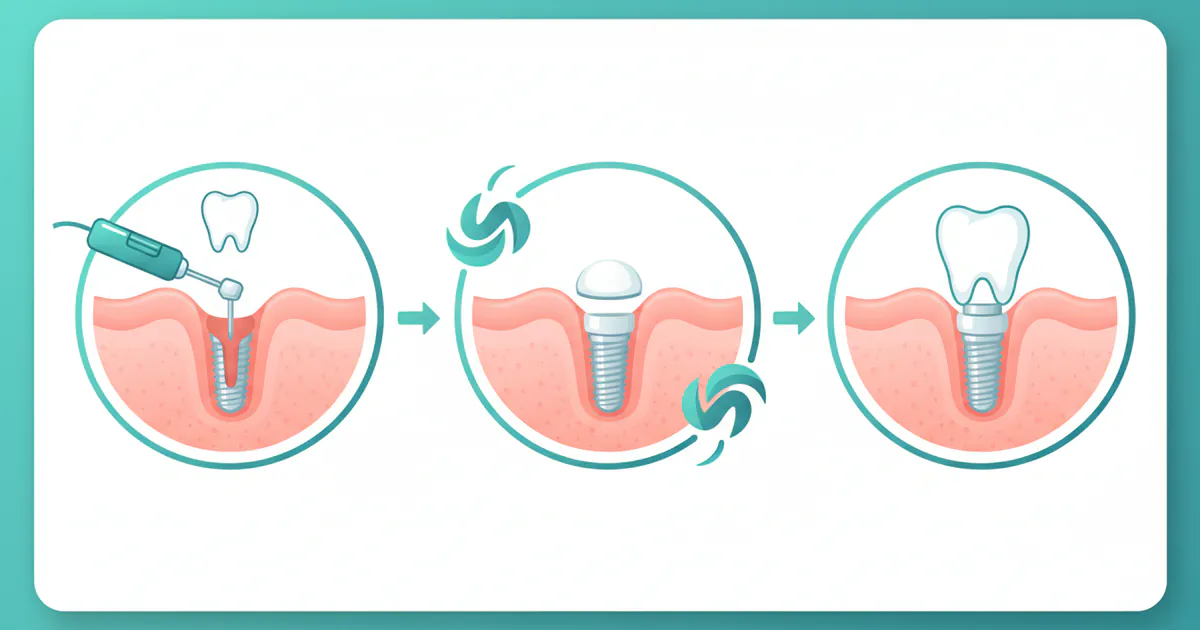
Implants Process: Complete Guide
Missing teeth can impact more than just your smile; they can affect your ability to eat, speak, and even your overall confidence. In fact, over 178 million Americans are missing at least one tooth, and about 40 million are missing all of their teeth. When faced with tooth loss, understanding the
March 8, 2026

Implants Dentaires: Complete Guide
Missing teeth can dramatically impact not just your smile, but your overall health, confidence, and quality of life. In the United States, an estimated 178 million adults are missing at least one tooth, while approximately 40 million are missing all their teeth. These statistics underscore a
March 8, 2026