Full Mouth Denture Implants: Complete Guide
Key Takeaways
- Full Mouth Denture Implants: Complete Guide
Full Mouth Denture Implants: Complete Guide
The journey to a confident, healthy smile can be challenging, especially for the millions of Americans living with significant tooth loss. According to the Centers for Disease Control and Prevention (CDC), over 17% of adults aged 65 and older have lost all their natural teeth, and many more suffer from partial edentulism that significantly impacts their quality of life. Traditional dentures offer a solution, but often come with limitations like instability, discomfort, and the need for messy adhesives. This is where full mouth denture implants emerge as a transformative option, offering unparalleled stability, comfort, and a renewed sense of confidence.
Choosing to replace an entire arch or both arches of missing teeth is a major decision, one that profoundly affects your ability to eat, speak, and smile. Understanding the intricacies of full mouth denture implants is crucial for anyone considering this life-changing procedure. This comprehensive guide from SmilePedia.net will demystify the process, exploring the types of implant-supported and implant-retained solutions available, the step-by-step journey, costs, recovery, and what you can expect from this advanced dental restoration. We aim to equip you with the knowledge needed to make an informed decision about restoring your oral health and reclaiming your smile.
Key Takeaways:
- Full mouth denture implants provide superior stability and comfort compared to traditional dentures, significantly improving chewing efficiency and speech.
- Two main types exist: Implant-Retained Overdentures (removable by patient, usually 2-4 implants per arch) and Implant-Supported Fixed Dentures (screw-retained, not removable, often 4-8 implants per arch, e.g., All-on-4®).
- The typical cost for a full arch can range from $15,000 to $50,000+ per arch, depending on the type, number of implants, materials, and additional procedures.
- The entire process, from initial consultation to final restoration, can take 4 to 12 months, including healing time for osseointegration.
- Dental implants themselves boast a success rate of over 95% and can last 20 years or a lifetime with proper care, while the prosthetic denture may need replacement every 5-15 years.
- Maintenance involves diligent oral hygiene, regular dental check-ups, and professional cleanings to prevent complications like peri-implantitis.
What It Is: Overview of Full Mouth Denture Implants
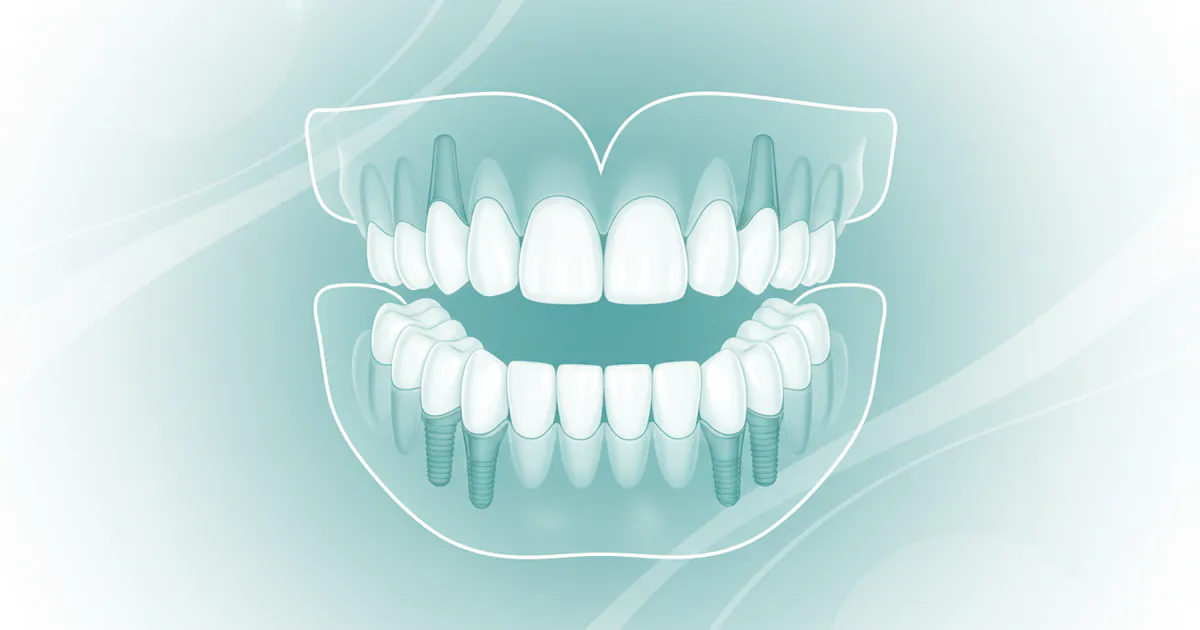
Full mouth denture implants, also commonly referred to as implant-retained dentures or implant-supported dentures, represent a sophisticated and highly effective solution for individuals who have lost all or most of their teeth in one or both dental arches. Unlike traditional dentures, which rely solely on suction and the underlying gum tissue for retention, these advanced prostheses are securely anchored to surgically placed dental implants within the jawbone.
A dental implant is a small, screw-shaped post, typically made of biocompatible titanium, that is surgically placed into the jawbone. Over several months, the implant fuses with the bone in a process called osseointegration, becoming a stable foundation much like the root of a natural tooth. For full mouth denture implants, multiple implants are strategically placed along the arch. Once integrated, these implants serve as sturdy anchors to which a custom-fabricated full denture is attached.
The primary goal of full mouth denture implants is to eliminate the common drawbacks associated with conventional removable dentures. Patients often struggle with traditional dentures slipping, causing discomfort, difficulty speaking, and significantly reduced chewing ability. The lack of stimulation to the jawbone can also lead to bone resorption, altering facial structure over time. By utilizing dental implants, these modern dentures provide:
- Exceptional Stability: No more slipping, clicking, or embarrassing moments.
- Improved Chewing Efficiency: Enjoy a wider variety of foods with confidence, leading to better nutrition.
- Enhanced Speech: Speak clearly without the worry of dentures shifting.
- Greater Comfort: Eliminate sore spots and the need for messy adhesives.
- Preservation of Jawbone: Implants stimulate the jawbone, preventing bone loss and maintaining facial structure.
- Increased Confidence: Smile, laugh, and interact socially without self-consciousness.
Essentially, full mouth denture implants offer a fixed or highly secure removable prosthetic that closely mimics the function and feel of natural teeth, providing a significant upgrade in quality of life for individuals with extensive tooth loss.
Types and Variations of Full Mouth Denture Implants
The world of full mouth denture implants offers several variations, each designed to meet different patient needs, anatomical considerations, and budget levels. The main distinction lies in how the denture attaches to the implants and whether it is removable by the patient.
1. Implant-Retained Overdentures (Removable)
Implant-retained overdentures, sometimes simply called overdentures, are a popular choice for their balance of enhanced stability and affordability compared to fixed options. These dentures are designed to "snap" onto a few strategically placed dental implants, providing significantly more retention than traditional dentures while still allowing the patient to remove them for cleaning.
- Mechanism: Typically, 2 to 4 dental implants are placed in the jawbone per arch. Once healed, abutments (connectors) are attached to these implants. The denture itself has corresponding attachments (such as ball attachments or Locator® attachments) that snap onto the abutments, holding the denture firmly in place.
- Number of Implants: Most commonly, 2 implants are used for the lower jaw (mandible) due to its denser bone, while 4 implants are often recommended for the upper jaw (maxilla) which has softer bone and often requires more support.
- Advantages:
- Improved Stability: Eliminates much of the movement and slipping associated with traditional dentures.
- Better Chewing: Enhances chewing efficiency compared to conventional dentures.
- Affordability: Generally less expensive than implant-supported fixed dentures due to fewer implants and a simpler prosthetic design.
- Ease of Cleaning: Patients can remove the denture daily for thorough cleaning of both the denture and the underlying gum tissue around the implants.
- Bone Preservation: Helps slow down or prevent further bone loss in the jaw.
- Disadvantages:
- Still Removable: Although stable, they are still removed nightly for cleaning, which some patients dislike.
- Less Secure than Fixed: While very stable, they may still have a slight degree of movement compared to fully fixed options.
- Attachments Wear: The retention clips or O-rings within the denture attachments may need periodic replacement (typically every 6-12 months) due to wear, incurring minor costs.
- Ideal Candidate: Patients seeking a significant upgrade in denture stability and comfort without the higher cost or commitment of a fixed solution, who are comfortable with daily removal for cleaning.
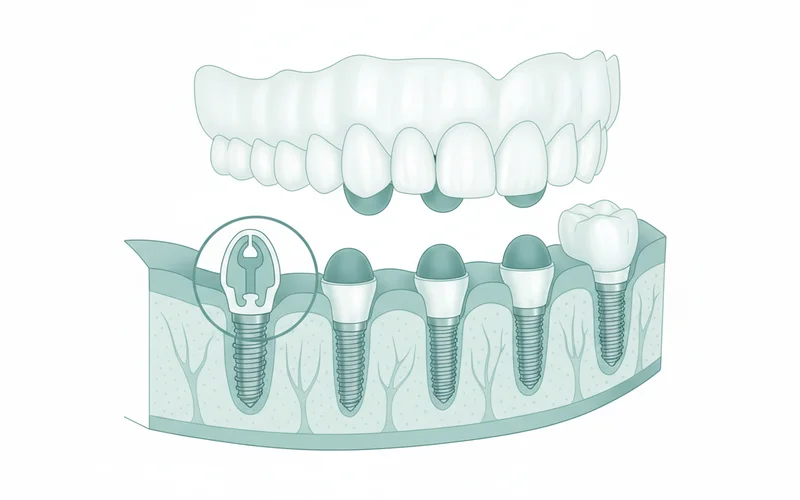
2. Implant-Supported Fixed Dentures (Non-Removable)
Also known as hybrid dentures or all-on-X solutions (e.g., All-on-4®, All-on-6®, All-on-8®), these prostheses are permanently secured to a greater number of dental implants and are not removable by the patient. They offer the closest resemblance to natural teeth in terms of function and feel.
- Mechanism: Typically 4 to 8 dental implants are strategically placed in each arch. For the popular All-on-4® technique, four implants are angled to maximize contact with existing bone, often avoiding the need for bone grafting. A custom-fabricated, full-arch prosthetic (made from acrylic, zirconia, or porcelain over a titanium framework) is then permanently screwed onto these implants.
- Number of Implants:
- All-on-4®: Uses four implants per arch, often angled to leverage existing bone. This is a very common and successful technique.
- All-on-6® / All-on-8®: Uses six or eight implants per arch, providing even greater support and distribution of biting forces, particularly beneficial for patients with higher bite forces or specific bone architecture.
- Advantages:
- Maximum Stability: Fully fixed, mimicking natural teeth. No movement whatsoever.
- Superior Chewing Power: Restores nearly full chewing efficiency, allowing a completely unrestricted diet.
- Optimal Comfort: Feels like natural teeth, no irritation from movement.
- Speech Clarity: Unimpeded speech as the denture is completely stable.
- Continuous Bone Stimulation: Excellent at preserving jawbone density over the long term.
- Convenience: No need for removal for daily cleaning (though professional cleaning is essential).
- Disadvantages:
- Higher Cost: Significantly more expensive than implant-retained overdentures due to more implants, complex surgical techniques, and advanced prosthetic materials.
- More Involved Surgery: Generally requires a more extensive surgical procedure.
- Professional Cleaning Required: While patients brush normally, specialized professional cleaning beneath the fixed bridge is crucial for long-term health.
- Difficult to Repair: If the fixed bridge gets damaged, repair can be more complex and costly.
- Ideal Candidate: Patients desiring the closest possible experience to natural teeth, prioritizing maximum stability, comfort, and chewing function, who are willing to invest in a premium, non-removable solution.
Pro Tip: Your dentist or oral surgeon will perform a thorough examination, including 3D imaging (CBCT scan), to assess your bone density and structure, helping determine which type of full mouth denture implant is best suited for your individual needs. The choice between removable and fixed solutions often depends on factors like bone quality, patient preference, and budget.
Causes: Why Full Mouth Denture Implants Become Necessary
The need for full mouth denture implants typically arises from extensive tooth loss or the failure of existing dental restorations. This widespread tooth loss, known as edentulism (complete tooth loss) or severe partial edentulism (loss of most teeth), can stem from a variety of underlying causes:
1. Advanced Periodontal (Gum) Disease
This is the leading cause of tooth loss in adults. Periodontal disease is a chronic inflammatory condition affecting the gums and supporting bone structure around teeth. If left untreated, it leads to:
- Progressive Bone Loss: The bacteria destroy the alveolar bone that holds teeth in place.
- Loose Teeth: As bone support diminishes, teeth become mobile and eventually fall out or require extraction.
- Inflammation and Infection: Persistent infection can compromise overall oral health and eventually lead to multiple extractions.
2. Severe Tooth Decay (Caries)
Widespread, untreated tooth decay can lead to the destruction of tooth structure beyond repair. Factors contributing to this include:
- Poor Oral Hygiene: Inadequate brushing and flossing allow plaque and bacteria to thrive.
- High Sugar Diet: Frequent consumption of sugary foods and drinks fuels bacterial acid production.
- Lack of Dental Care: Skipping regular check-ups and cleanings allows small cavities to progress into large, destructive lesions.
- Dry Mouth (Xerostomia): Reduced saliva flow, often a side effect of medications or medical conditions, diminishes the mouth's natural cleansing and remineralizing abilities.
3. Trauma and Injury
Accidents, sports injuries, or other forms of trauma can result in the loss of multiple teeth or severe damage that necessitates their extraction.
- Impact Injuries: Direct blows to the face can fracture teeth or dislodge them entirely.
- Extensive Fractures: Teeth fractured below the gum line often cannot be saved.
4. Congenital Conditions
Some individuals are born with conditions that lead to missing teeth or severely compromised tooth development.
- Anodontia/Oligodontia: Genetic conditions characterized by the complete or partial absence of teeth.
- Amelogenesis Imperfecta/Dentinogenesis Imperfecta: Disorders affecting enamel or dentin formation, leading to structurally weak teeth prone to early loss.
5. Failed Dental Work
Over time, extensive dental restorations such as large fillings, crowns, or bridges can fail due to recurrent decay, fractures, or underlying structural issues. When multiple restorations fail simultaneously, it can lead to the need for full arch replacement.
6. Systemic Health Conditions
Certain systemic diseases can compromise oral health and contribute to tooth loss:
- Diabetes: Uncontrolled diabetes can worsen periodontal disease and impair healing.
- Autoimmune Diseases: Conditions affecting the immune system can impact oral health.
- Cancer Treatment: Radiation therapy to the head and neck or certain chemotherapies can damage oral tissues and lead to tooth loss.
When one or a combination of these factors results in significant tooth loss, traditional removable dentures often become the initial solution. However, the subsequent bone resorption and functional limitations of these dentures frequently lead patients to seek the more stable and bone-preserving solution offered by full mouth denture implants.
Signs and Symptoms Indicating a Need for Full Mouth Denture Implants
Recognizing the signs that you might be a candidate for full mouth denture implants often involves a progression from minor discomfort to significant functional and aesthetic challenges.
For individuals with extensive natural tooth loss:
- Multiple Missing Teeth: You've lost several or all teeth in an arch, severely impacting your ability to chew and speak.
- Severely Damaged or Failing Teeth: Many remaining teeth are compromised by advanced decay, fractures, or severe gum disease, making their long-term prognosis poor.
- Difficulty Chewing a Variety of Foods: You find yourself avoiding certain foods because of pain or inability to chew effectively, leading to nutritional deficiencies.
- Speech Impairment: Missing teeth can cause lisps, whistles, or difficulty forming certain sounds.
- Changes in Facial Appearance: The absence of teeth leads to jawbone resorption, which can cause the jawline to recede, the lips to sink in, and facial muscles to sag, creating an "aged" appearance.
- Chronic Pain or Infection: Persistent pain, abscesses, or discomfort from failing teeth.
For current denture wearers:
- Loose or Ill-Fitting Dentures: Your traditional dentures constantly slip, shift, or fall out, requiring frequent use of adhesives.
- Sore Spots and Rubbing: The movement of dentures causes painful sores, ulcers, and irritation on your gums.
- Difficulty Speaking Clearly: Dentures shift while you talk, affecting your pronunciation and confidence.
- Reduced Chewing Efficiency: Even with dentures, you struggle to chew many foods, limiting your diet.
- Diminished Taste Perception: The palate coverage of upper traditional dentures can block taste buds.
- Embarrassment and Self-Consciousness: You feel self-conscious about your smile or worry your dentures might become dislodged in social situations.
- Progressive Bone Loss: You've noticed changes in your jawline or how your dentures fit over time, indicating ongoing bone resorption.
If you experience any of these signs, it's a strong indicator that you should consult with a dental professional to explore advanced tooth replacement options, including full mouth denture implants.
Treatment Options: Alternatives to Full Mouth Denture Implants
While full mouth denture implants offer a highly effective and long-lasting solution, it's important to understand the other available treatment options for extensive tooth loss. Each comes with its own set of pros and cons, which your dentist will discuss with you.
1. Traditional Full Dentures (Removable)
What it is: A complete set of prosthetic teeth and gums made from acrylic, designed to rest directly on the gum tissue. They are held in place by suction, the natural contours of the jaw, and sometimes dental adhesives.
Pros:
- Most Affordable: Generally the least expensive option for replacing an entire arch of teeth.
- Non-Invasive: No surgery required.
- Quick Fabrication: Can often be made and fitted relatively quickly.
Cons:
- Poor Stability: Prone to slipping, shifting, and falling out, especially the lower denture.
- Reduced Chewing Efficiency: Can make eating certain foods difficult or impossible, leading to dietary restrictions.
- Discomfort and Sore Spots: Can cause irritation, rubbing, and painful sores on the gums.
- Bone Loss: Does not stimulate the jawbone, leading to progressive bone resorption over time, which alters facial features and necessitates frequent relining or replacement.
- Speech Issues: May affect speech clarity until adapted to, and can still cause issues if they move.
- Daily Removal: Must be removed nightly for cleaning.
- Aesthetics: While improving appearance, they often lack the natural look and feel of implant-supported options.
2. No Treatment (Living with Extensive Tooth Loss)
What it is: Choosing not to replace missing teeth at all.
Pros:
- No Upfront Cost: Avoids the expense of dental procedures.
Cons:
- Severe Functional Impairment: Extreme difficulty chewing, leading to a severely restricted diet and poor nutrition.
- Significant Speech Problems: Can make communication very challenging.
- Accelerated Bone Loss: The jawbone will continue to resorb at an even faster rate without any stimulation.
- Facial Collapse: Leads to a sunken facial appearance, premature aging, and collapse of the bite.
- Poor Oral Health: Remaining teeth (if any) are susceptible to shifting, decay, and gum disease.
- Psychological Impact: Significant impact on self-esteem, social interaction, and overall quality of life.
3. Individual Dental Implants (for multiple single tooth replacements)
What it is: Involves placing a separate dental implant for each missing tooth, topped with individual crowns. While not a "full mouth denture implant" per se, it is an option for full mouth rehabilitation if a patient has lost most or all teeth.
Pros:
- Most Natural Feel and Function: Each implant and crown acts like an individual natural tooth.
- Optimal Bone Preservation: Each implant stimulates the bone, preventing resorption.
- Superior Aesthetics: Highly customized to match natural teeth.
- Long-Lasting: Excellent long-term success rates.
Cons:
- Highest Cost: As each tooth is replaced individually, the cost for a full arch can be extremely high, requiring 10-14 implants per arch.
- Extensive Surgery: Involves placing a large number of implants, which means more surgical sites and potentially longer recovery.
- Complexity: Requires excellent bone quantity and quality at numerous sites.
Comparison of Full Mouth Tooth Replacement Options
| Feature | Traditional Full Dentures (Removable) | Implant-Retained Overdentures (Removable) | Implant-Supported Fixed Dentures (Non-Removable) |
|---|---|---|---|
| Stability | Low (relies on suction) | High (snaps onto implants) | Excellent (screwed onto implants) |
| Comfort | Can cause sores, less natural | Much improved, less irritation | Most natural feel, no movement |
| Chewing Power | 20-25% of natural teeth | 50-70% of natural teeth | 80-95% of natural teeth |
| Bone Preservation | None (causes bone loss) | Good (implants stimulate bone) | Excellent (implants stimulate bone) |
| Maintenance | Daily removal, adhesives, relines | Daily removal, attachment clip changes | Professional cleaning, regular hygiene |
| Cost per Arch | $2,000 - $8,000 | $8,000 - $25,000 | $15,000 - $50,000+ |
| Invasiveness | None | Minor surgical procedure | Moderate surgical procedure |
| Aesthetics | Good | Very good | Excellent, highly natural |
This comparison highlights why full mouth denture implants, in their various forms, are often the preferred choice for patients seeking a significant improvement over traditional dentures, offering a blend of stability, function, and bone health preservation.
Step-by-Step Process for Full Mouth Denture Implants
The process of receiving full mouth denture implants is a multi-stage journey that requires careful planning, surgical precision, and a healing period. While specific timelines can vary, here's a general overview of what you can expect:
Step 1: Initial Consultation and Comprehensive Planning (1-2 appointments)
- Oral Examination: Your dentist or oral surgeon will perform a thorough examination of your mouth, including your gums, remaining teeth (if any), and jawbone structure.
- Imaging: X-rays, panoramic images, and crucially, a 3D Cone Beam Computed Tomography (CBCT) scan, will be taken. This provides detailed images of your bone density, nerve pathways, and sinus cavities, essential for precise implant placement.
- Health History Review: A comprehensive review of your medical history, including any medications, allergies, and systemic conditions (like diabetes or heart disease) that could affect treatment or healing.
- Discussion of Options: Your dentist will discuss the different types of full mouth denture implants (removable vs. fixed, number of implants) and tailor a personalized treatment plan, explaining the pros, cons, costs, and timeline.
- Impressions/Digital Scans: Molds or digital scans of your mouth are taken to plan the design of your temporary and final prostheses.
Step 2: Pre-Surgical Preparations (Variable)
- Extractions: If you have any remaining unhealthy teeth, they will need to be extracted. This can be done in a separate appointment or often concurrently with implant placement.
- Bone Grafting/Sinus Lift (If Needed): If your jawbone lacks sufficient volume or density to support implants, a bone grafting procedure may be necessary. For the upper jaw, a sinus lift might be performed to add bone to the posterior maxilla. These procedures require an additional healing period (typically 3-6 months) before implants can be placed.
- Temporary Denture: If you don't have existing dentures, a temporary removable denture (immediate denture) might be provided after extractions to ensure you don't go without teeth during the healing phase.
Step 3: Dental Implant Placement Surgery (1 appointment)
- Anesthesia: The procedure is typically performed under local anesthesia with sedation (oral, IV sedation, or nitrous oxide) to ensure your comfort. General anesthesia may be an option for more complex cases or patient preference.
- Surgical Incisions: The surgeon will make small incisions in your gum tissue to expose the jawbone.
- Pilot Holes: Small pilot holes are carefully drilled into the jawbone at the precise, pre-planned locations.
- Implant Insertion: The titanium dental implants are then gently screwed into these prepared sites.
- Gum Closure: The gum tissue is typically closed over the implants with sutures (submerged approach) or a healing abutment may be placed that extends through the gum tissue (one-stage approach).
Step 4: Healing and Osseointegration (3-6 months)
- Crucial Phase: This is the most critical part of the process where the dental implants fuse with your jawbone. This biological process, called osseointegration, ensures the implants become a permanent and stable part of your anatomy.
- Temporary Prosthesis: During this healing period, you will wear a temporary, often lighter-weight, denture that does not put pressure on the healing implants.
- Dietary Restrictions: You will need to follow a soft diet to avoid disturbing the implants during this delicate phase.
- Regular Check-ups: Your dentist will monitor your healing progress with follow-up appointments.
Step 5: Abutment Placement and Impression Taking (1-2 appointments)
- Exposure of Implants: If the implants were submerged, a minor procedure is performed to uncover them and attach healing abutments.
- Final Impressions: Once osseointegration is complete, new impressions or digital scans are taken of your mouth and the healed implants. These are sent to a dental lab.
- Shade and Bite Registration: The dentist will also take precise measurements of your bite and work with you to select the appropriate tooth shape, size, and shade for your final denture.
Step 6: Fabrication and Fitting of the Permanent Denture (2-4 appointments)
- Lab Fabrication: A skilled dental laboratory will custom-fabricate your final full arch denture based on the impressions and specifications provided. This process can take several weeks.
- Try-in Appointments: You will have "try-in" appointments where the dentist will check the fit, bite, aesthetics, and comfort of your new denture before it is finalized. Adjustments are made as needed.
- Final Placement: Once both you and the dentist are satisfied, your permanent full mouth denture is securely attached to the implants. For implant-retained overdentures, you'll be shown how to remove and clean them. For fixed dentures, they are permanently screwed into place.
Step 7: Follow-up and Maintenance
- Adjustment Period: There will be a brief adjustment period as you get accustomed to your new teeth. Minor adjustments may be needed after initial use.
- Regular Check-ups: Ongoing regular check-ups (typically every 6 months) are essential to monitor the health of your implants, gums, and the condition of your denture. Professional cleaning of fixed prostheses is vital.
- Oral Hygiene: You'll receive detailed instructions on how to properly care for your full mouth denture implants at home.
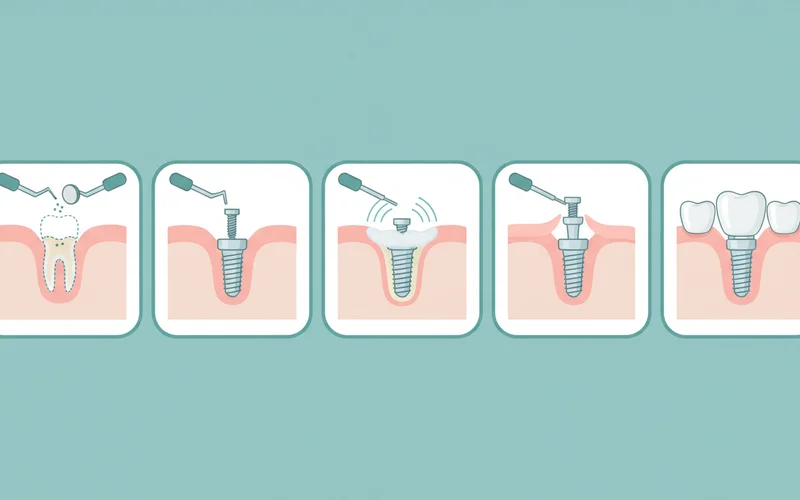
Pro Tip: Patience is key throughout this process. Rushing the healing phase can compromise the long-term success of your implants. Follow all post-operative instructions diligently.
Cost and Insurance for Full Mouth Denture Implants
Understanding the financial investment required for full mouth denture implants is a critical part of the decision-making process. The cost can vary significantly based on several factors, and insurance coverage is often limited.
Factors Influencing Cost
- Type of Denture Implant System:
- Implant-Retained Overdentures (Removable): Generally less expensive, as they typically use fewer implants (2-4 per arch) and the prosthetic itself is simpler.
- Implant-Supported Fixed Dentures (e.g., All-on-4®): More costly due to the increased number of implants (4-8 per arch), more complex surgical techniques, and the use of higher-grade, often more aesthetic and durable prosthetic materials (e.g., zirconia or porcelain over a titanium framework, as opposed to acrylic).
- Number of Implants: More implants generally mean higher cost.
- Materials Used: The quality and type of materials for both the implants and the prosthetic teeth (acrylic, composite, zirconia, porcelain) will impact the price. Zirconia and porcelain are typically more expensive than acrylic.
- Additional Procedures:
- Tooth Extractions: If you have remaining teeth that need to be removed.
- Bone Grafting: If you have insufficient jawbone volume, a bone graft (sinus lift, ridge augmentation) will add significant cost and extend treatment time.
- Sedation: The type of anesthesia chosen (oral, IV, general) will affect the overall fee.
- Geographic Location: Costs vary by region and even by specific dental practice within the United States. Major metropolitan areas tend to have higher prices.
- Dentist's Experience and Specialty: Highly experienced oral surgeons or prosthodontists specializing in full mouth rehabilitation may charge higher fees.
Average US Price Ranges (per arch)
It's important to note these are broad ranges, and a personalized quote from your dentist is essential.
-
Implant-Retained Overdenture (Removable):
- 2 Implants (Lower Arch): $8,000 - $15,000
- 4 Implants (Upper Arch): $12,000 - $25,000
- This range typically includes the implants, abutments, and the custom overdenture.
-
Implant-Supported Fixed Denture (Non-Removable, e.g., All-on-4®):
- Per Arch (e.g., All-on-4® using acrylic hybrid prosthesis): $15,000 - $35,000
- Per Arch (e.g., All-on-4® using zirconia/porcelain prosthesis): $25,000 - $50,000+
- This range usually includes the implants, temporary prosthesis, and the final fixed prosthesis.
Total Cost for Both Arches (Full Mouth): For patients requiring treatment for both the upper and lower arches, simply double the per-arch estimate. This can range from $30,000 to over $100,000 for a full mouth rehabilitation with implant-supported fixed dentures.
Insurance Coverage Details
- Dental Insurance: Most traditional dental insurance plans offer limited coverage for dental implants.
- Implants: Often categorized as a major restorative procedure, coverage typically ranges from 0% to 50%, with annual maximums often capped at $1,000 - $2,500. This means you will likely pay a significant portion out-of-pocket.
- Prosthetic (Denture): The denture portion of the treatment might have separate coverage, often similar to traditional dentures (e.g., 50% for major services).
- Related Procedures: Extractions might be covered at a higher percentage (e.g., 80%), while bone grafting may or may not be covered, depending on medical necessity and plan specifics.
- Medical Insurance: In some specific cases, if tooth loss is due to a medical condition (e.g., cancer treatment, severe trauma), parts of the procedure might be covered by your medical insurance, especially if it can be coded as a medical necessity. This is rare for routine tooth loss.
- Medicare/Medicaid: Generally, Medicare does NOT cover dental implants or most routine dental care. Medicaid coverage for dental work is typically very limited and varies greatly by state, usually not including implants.
Pro Tip: Always have your dental office submit a pre-treatment estimate to your insurance provider before starting any major procedure. This will give you a clear understanding of your out-of-pocket expenses.
Recovery and Aftercare for Full Mouth Denture Implants
Proper recovery and diligent aftercare are paramount to the long-term success and longevity of your full mouth denture implants. This phase encompasses immediate post-surgical healing and ongoing maintenance of both the implants and the prosthetic teeth.
Immediate Post-Surgical Recovery (First 1-2 Weeks)
- Pain Management: Expect some discomfort as the anesthesia wears off. Your dentist will prescribe pain medication or recommend over-the-counter options. Take medication as directed.
- Swelling: Swelling is common and typically peaks 2-3 days after surgery. Apply ice packs to the outside of your face (15 minutes on, 15 minutes off) for the first 24-48 hours.
- Bleeding: Minor bleeding or oozing is normal for the first day. Bite gently on gauze pads and change them as needed. Avoid spitting forcefully.
- Diet: Stick to a soft-food diet for several days to weeks, as advised by your dentist. Avoid chewing directly on the implant sites. Examples include mashed potatoes, yogurt, smoothies, soft scrambled eggs, and well-cooked pasta. Gradually reintroduce firmer foods as healing progresses.
- Oral Hygiene:
- First 24 Hours: Avoid rinsing, spitting, or disturbing the surgical sites.
- After 24 Hours: Gently rinse your mouth with a prescribed antimicrobial mouthwash (like chlorhexidine) or warm salt water (1/2 teaspoon salt in 8 ounces of warm water) 2-3 times a day, especially after meals. Do NOT brush directly on the surgical sites initially.
- Brushing: Brush your remaining natural teeth (if any) and the rest of your mouth gently, avoiding the surgical areas.
- Activity: Rest and avoid strenuous physical activity for at least 48-72 hours, or as recommended by your surgeon.
- Smoking/Alcohol: Absolutely avoid smoking and alcohol during the healing phase, as they can significantly impair healing and increase the risk of implant failure.
- Follow-up: Attend all scheduled follow-up appointments so your dentist can monitor healing and remove any sutures.
Long-Term Aftercare and Maintenance
Once the implants have fully integrated and your permanent denture is in place, consistent long-term care is crucial.
1. Oral Hygiene:
- Brushing:
- Implant-Retained Overdentures: Remove your denture daily (often nightly) for thorough cleaning. Brush the denture with a soft-bristled brush and non-abrasive denture cleaner. Brush around the implant sites (abutments) and your gum tissue gently with a soft toothbrush. Use a special brush or gauze to clean any attachments on the implants.
- Implant-Supported Fixed Dentures: Brush your fixed denture just as you would natural teeth, using a soft-bristled toothbrush and non-abrasive toothpaste, at least twice a day.
- Flossing/Interdental Cleaning:
- Fixed Dentures: Specialized interdental brushes, water flossers (like Waterpik), or super floss are essential for cleaning under and around the fixed prosthesis, especially where it meets the gums. This removes plaque and food debris that regular brushing can't reach. Your dentist or hygienist will demonstrate proper techniques.
- Overdentures: Use traditional floss or interdental brushes around the implant abutments.
- Mouthwash: Daily use of an antiseptic or fluoride mouthwash can be beneficial, as recommended by your dentist.
2. Regular Dental Check-ups and Professional Cleanings:
- Frequency: Visit your dentist or dental hygienist for check-ups and professional cleanings every 3-6 months, or as advised.
- Why it's Crucial: These appointments are vital for:
- Checking the health of your implants and surrounding gum tissue.
- Detecting early signs of peri-implantitis (an inflammatory condition similar to gum disease that can affect implants).
- Cleaning hard-to-reach areas of fixed prostheses, often requiring specialized tools.
- Assessing the condition of your denture and attachments.
- Making any necessary adjustments or repairs.
3. Dietary Considerations:
- With implant-supported dentures, you can generally enjoy a full and varied diet. However, it's wise to exercise caution with extremely hard foods (e.g., cracking nuts with your teeth, chewing on ice) that could potentially damage the prosthetic teeth.
- Even with fixed implants, proper chewing technique is beneficial for distributing forces evenly.
4. Protecting Your Investment:
- Nightguards: If you clench or grind your teeth (bruxism), your dentist may recommend a custom nightguard to protect your implants and denture from excessive forces.
- Avoid Abuse: Do not use your teeth as tools (e.g., opening bottles, tearing packages).
Adhering to these recovery and aftercare guidelines will significantly contribute to the long-term success and comfort of your full mouth denture implants, ensuring you enjoy your new smile for decades to come.
Prevention: Avoiding the Need for Full Mouth Denture Implants
The best way to avoid the need for full mouth denture implants is to prevent extensive tooth loss in the first place. This requires a proactive and consistent approach to oral health throughout your life.
-
Maintain Excellent Oral Hygiene:
- Brush Twice Daily: Use a soft-bristled toothbrush and fluoride toothpaste. Brush for at least two minutes, covering all tooth surfaces and the gum line.
- Floss Daily: Flossing removes plaque and food particles from between teeth and under the gum line, areas your toothbrush can't reach. This is critical for preventing gum disease and interdental decay.
- Use Mouthwash: An antimicrobial or fluoride mouthwash can provide an added layer of protection.
- Tongue Cleaning: Clean your tongue to remove bacteria that can contribute to bad breath and gum disease.
-
Regular Dental Check-ups and Professional Cleanings:
- Schedule Every 6 Months: Consistent visits to your dentist and hygienist are fundamental. They can detect and address problems like cavities or early gum disease before they escalate.
- Professional Cleanings: Remove plaque and tartar buildup that at-home brushing can't, preventing cavities and periodontal disease.
-
Address Dental Problems Promptly:
- Don't Ignore Pain: Toothaches, sensitivity, bleeding gums, or persistent bad breath are warning signs. Seek dental attention immediately.
- Treat Cavities Early: Small cavities are easier and less expensive to treat than large ones that may require root canals or extractions.
- Manage Gum Disease: If you notice signs of gingivitis (red, swollen, bleeding gums), seek treatment. Early intervention can prevent it from progressing to destructive periodontitis.
-
Healthy Diet and Lifestyle Choices:
- Limit Sugary Foods and Drinks: Sugar feeds the bacteria that cause tooth decay. Opt for water over sugary beverages.
- Eat a Balanced Diet: A diet rich in fruits, vegetables, lean proteins, and dairy (for calcium) supports overall health, including strong teeth and bones.
- Avoid Smoking and Excessive Alcohol: Both are major risk factors for gum disease, oral cancer, and contribute to tooth loss. The American Dental Association (ADA) strongly advises against tobacco use for optimal oral health.
-
Protect Your Teeth from Trauma:
- Wear a Mouthguard: If you participate in sports or activities with a risk of facial impact, wear a custom-fitted mouthguard.
- Address Bruxism (Teeth Grinding): If you clench or grind your teeth, especially at night, your dentist may recommend a nightguard to prevent excessive wear and potential tooth fractures.
- Avoid Using Teeth as Tools: Don't use your teeth to open packages, crack nuts, or bite on non-food objects.
By committing to these preventive measures, you significantly reduce your risk of developing the extensive tooth loss that would necessitate full mouth denture implants, thereby preserving your natural smile and oral health for a lifetime.
Risks and Complications Associated with Full Mouth Denture Implants
While full mouth denture implants boast a high success rate (over 95% for dental implants), it's essential to be aware of potential risks and complications, as with any surgical procedure. A thorough understanding allows you to discuss concerns with your dental professional and make informed decisions.
Surgical Risks:
- Infection: Although rare with proper sterile techniques and antibiotics, infection can occur at the implant site during or after surgery.
- Nerve Damage: In the lower jaw, there's a small risk of damage to the inferior alveolar nerve, which can lead to numbness, tingling, or pain in the lip, chin, or tongue. Careful planning with 3D imaging significantly minimizes this risk.
- Sinus Perforation: In the upper jaw, there's a risk of the implant penetrating the maxillary sinus. This is often managed during surgery or prevented with a sinus lift procedure beforehand.
- Excessive Bleeding: Some bleeding is normal, but excessive or prolonged bleeding can occur, especially if you're on blood-thinning medications.
- Adjacent Tooth/Structure Damage: While rare, there's a minimal risk of damaging existing teeth or other oral structures during implant placement.
Implant-Specific Complications:
- Implant Failure (Lack of Osseointegration): The implant may fail to fuse with the jawbone. This can be due to:
- Poor Bone Quality/Quantity: Insufficient bone to support the implant.
- Infection: Infection at the surgical site.
- Smoking: Significantly reduces success rates.
- Certain Medical Conditions: Uncontrolled diabetes, autoimmune disorders.
- Excessive Early Loading: Too much force on the implant before it has fully healed.
- If an implant fails, it typically needs to be removed, the site allowed to heal, and then a new implant (or an alternative solution) considered.
- Peri-Implantitis: This is an inflammatory disease affecting the tissues surrounding a dental implant, similar to periodontal disease around natural teeth. It's caused by bacterial infection and can lead to bone loss around the implant, potentially causing implant failure if untreated. It's often linked to poor oral hygiene and smoking.
- Mechanical Complications:
- Screw Loosening/Fracture: The screws that attach the abutment to the implant or the prosthesis to the abutment can loosen or, rarely, fracture.
- Implant Fracture: Extremely rare, but an implant itself can fracture due to excessive force or faulty materials.
Prosthetic-Related Complications (Denture/Bridge):
- Denture/Bridge Fracture or Chipping: The prosthetic teeth or the underlying framework can chip, crack, or fracture, especially with acrylic materials or if exposed to excessive biting forces.
- Attachment Wear (for Overdentures): The retention clips or O-rings in implant-retained overdentures wear out over time and need periodic replacement (typically every 6-12 months) to maintain retention.
- Denture Relining/Rebasing (for Overdentures): While less frequent than with traditional dentures, changes in gum tissue over time may still necessitate relining or rebasing an overdenture.
- Hygiene Access Issues: For fixed dentures, if the design doesn't allow adequate access for cleaning, plaque and bacteria can accumulate, increasing the risk of peri-implantitis.
General Complications:
- Allergic Reaction: Although titanium implants are highly biocompatible, rare allergic reactions to titanium or other materials can occur.
- Bruxism (Teeth Grinding): Chronic grinding or clenching can place excessive force on implants and the prosthetic, leading to mechanical complications or even implant failure. A nightguard is often recommended.
Your dental team will take extensive measures to minimize these risks, including thorough diagnostics, meticulous planning, and adherence to strict surgical protocols. Following post-operative instructions and maintaining excellent oral hygiene are your most important contributions to ensuring a successful outcome.
Children / Pediatric Considerations
Full mouth denture implants are generally not applicable to children or adolescents. Dental implants, by design, require a fully developed jawbone for successful osseointegration and long-term stability.
In younger individuals, the jawbones are still growing and developing. Placing dental implants before skeletal maturity can lead to complications such as:
- Implant Submergence: As the surrounding bone continues to grow, a stable implant can appear to "sink" relative to the adjacent teeth and jaw, leading to aesthetic and functional problems.
- Interference with Growth: The implant may interfere with the natural growth patterns of the jawbone.
Most dental professionals recommend waiting until the jawbone has reached full maturity, which typically occurs:
- Around 16-18 years old for females.
- Around 18-21 years old for males.
In rare cases where a child has congenitally missing teeth or has lost permanent teeth due to severe trauma, temporary or interim solutions such as removable partial dentures (flippers) or space maintainers are used until they reach an age where dental implants can be safely considered. For children with extensive tooth loss, close collaboration between a pediatric dentist, orthodontist, and possibly an oral surgeon will guide the multi-disciplinary treatment plan until adulthood. The focus in pediatric cases is always on preserving existing teeth, guiding jaw development, and maintaining function and aesthetics temporarily.
Cost Breakdown: Detailed US Averages and Financial Options
Delving deeper into the financial aspects of full mouth denture implants reveals a complex landscape influenced by numerous variables. Here's a more detailed look at average US costs, insurance nuances, and ways to manage the expense.
Average US Costs for a Full Arch (Ranges)
It's crucial to understand that these are national averages and can fluctuate dramatically based on the factors previously mentioned (location, dentist's expertise, materials, complexity).
| Type of Full Mouth Denture Implant | Low End (per Arch) | Mid Range (per Arch) | High End (per Arch) |
|---|---|---|---|
| Implant-Retained Overdenture | |||
| * 2 Implants (Lower)* | $8,000 | $12,000 | $15,000 |
| * 4 Implants (Upper)* | $12,000 | $18,000 | $25,000 |
| Implant-Supported Fixed Denture | |||
| * All-on-4® (Acrylic Hybrid)* | $15,000 | $25,000 | $35,000 |
| * All-on-4® (Zirconia/Porcelain)* | $25,000 | $35,000 | $50,000+ |
| * All-on-6/8 (Zirconia/Porcelain)* | $30,000 | $45,000 | $60,000+ |
Note: These figures typically include the surgical placement of implants, the abutments, and the final prosthetic. They may not always include pre-surgical extractions, bone grafting, or extensive sedation, which can add several hundred to several thousand dollars to the total. For a full mouth (both upper and lower arches), these costs are essentially doubled.
With vs. Without Insurance
As detailed earlier, dental insurance coverage for implants is often limited:
- Without Insurance: You are responsible for the entire cost. Many clinics offer cash discounts for upfront payment or through third-party financing.
- With Insurance: Even with insurance, most patients will pay a substantial portion out-of-pocket. If your plan covers 50% of major services up to a $2,000 annual maximum, on a $25,000 procedure, your insurance would pay only $2,000, leaving you with $23,000. It's critical to understand your specific plan's benefits, waiting periods, and annual maximums.
Payment Plans and Financing Options
Many dental practices recognize the significant investment involved and offer various financial solutions:
- In-House Payment Plans: Some practices offer interest-free or low-interest payment plans directly through their office.
- Third-Party Medical/Dental Financing: Companies like CareCredit®, LendingClub, or Alphaeon Credit specialize in healthcare financing. They offer various plans, including interest-free options for a specific period (e.g., 6, 12, or 18 months) if the balance is paid in full during that time, or extended payment plans with fixed interest rates.
- Personal Loans: Banks and credit unions offer personal loans that can be used to cover dental expenses.
- Health Savings Accounts (HSAs) & Flexible Spending Accounts (FSAs): If you have an HSA or FSA through your employer, these are excellent ways to pay for dental implants with pre-tax dollars, offering significant savings. You can contribute to these accounts specifically for anticipated medical and dental expenses.
Cost-Saving Tips
- Comparison Shopping: Obtain detailed treatment plans and cost estimates from 2-3 different highly qualified dentists or oral surgeons in your area. Ensure you are comparing "apples to apples" regarding the type of implant, materials, and included services.
- Dental Schools: University dental schools often provide services at a reduced cost compared to private practices. The procedures are performed by students under the direct supervision of experienced faculty. This can be a high-quality, more affordable option, though it might involve longer appointment times.
- Phased Treatment: Discuss with your dentist if the treatment can be phased over time, allowing you to spread the cost across different tax years or insurance benefit years.
- Maximize Insurance Benefits: If your procedure spans two calendar years, some costs might be covered under two separate annual maximums, effectively doubling your insurance benefit. Plan with your dental office.
- Negotiate: Some practices may be willing to offer a slight discount for upfront cash payment for the entire procedure. It never hurts to ask politely.
Pro Tip: Don't let cost be the sole determinant of your choice. The skill and experience of the dental professional, the quality of materials, and the comprehensiveness of the treatment plan are paramount for long-term success and should be weighed heavily against the price.
Frequently Asked Questions
What are full mouth denture implants?
Full mouth denture implants are a comprehensive solution for replacing all missing teeth in an arch (upper, lower, or both). They involve surgically placing several dental implants into the jawbone, which then serve as stable anchors for a custom-made full denture. This provides superior stability, comfort, and function compared to traditional removable dentures.
How long do teeth implants last?
The dental implants themselves, made from biocompatible titanium, are designed to be a permanent solution. With proper oral hygiene and regular dental check-ups, dental implants have a very high success rate (over 95%) and can last 20 years, a lifetime, or multiple decades. The prosthetic denture attached to the implants may need replacement every 5-15 years, depending on the material and wear.
Are full mouth denture implants painful?
The implant placement surgery is typically performed under local anesthesia, often with sedation, so you won't feel pain during the procedure. Post-operative discomfort is common but usually manageable with prescribed pain medication and over-the-counter anti-inflammatories. Most patients report the discomfort is less than expected and resolves within a few days to a week.
How long does the entire process take?
The full process, from initial consultation to the final placement of your permanent denture, typically spans 4 to 12 months. This timeline includes necessary extractions, the surgical placement of implants, a crucial healing period of 3-6 months for osseointegration (where implants fuse with your bone), and the fabrication and fitting of your custom prosthetic.
What is the difference between implant-retained and implant-supported dentures?
Implant-retained overdentures snap onto fewer implants (usually 2-4 per arch) and are still removable by the patient for cleaning, offering enhanced stability. Implant-supported fixed dentures (like All-on-4®) are permanently screwed onto 4-8 implants, are not removable by the patient, and provide maximum stability and chewing function, feeling much like natural teeth.
Can I get full mouth denture implants if I have bone loss?
Yes, in many cases, even with some bone loss, full mouth denture implants are still possible. Your dentist or oral surgeon will assess your bone density using 3D imaging. If significant bone loss is present, procedures like bone grafting or a sinus lift can be performed to augment the bone sufficiently to support the implants. Techniques like All-on-4® are also designed to maximize the use of existing bone.
How do I clean full mouth denture implants?
For implant-retained overdentures, you remove them daily and clean them with a soft brush and non-abrasive denture cleaner. You also gently clean around the implant abutments and gum tissue in your mouth. For implant-supported fixed dentures, you brush them like natural teeth, and use specialized tools like water flossers or interdental brushes to clean beneath the fixed bridge, along with regular professional cleanings.
What are the alternatives to full mouth denture implants?
The primary alternatives are traditional full removable dentures (less stable, cause bone loss) or, in certain very extensive cases, individual dental implants for each tooth (most expensive, highest number of implants). Living with no teeth is also an option but leads to severe functional issues and rapid facial collapse.
What is the cost of full mouth denture implants?
The cost varies significantly. For implant-retained overdentures, expect to pay roughly $8,000 to $25,000 per arch. For implant-supported fixed dentures (e.g., All-on-4®), the cost can range from $15,000 to $50,000+ per arch, depending on materials and complexity. These prices generally include the implants and the final prosthetic.
Will my insurance cover full mouth denture implants?
Most traditional dental insurance plans offer limited coverage for dental implants, often treating them as a major restorative procedure with 0-50% coverage up to an annual maximum (typically $1,000-$2,500). Some parts of the procedure, like extractions or the denture itself, might have separate coverage. It's essential to get a pre-treatment estimate from your dental office to understand your specific out-of-pocket costs.
When to See a Dentist
Determining the right time to consult a dentist about full mouth denture implants is crucial. Here’s guidance on when to seek professional advice:
Immediate Attention (Red Flags):
- Multiple Severely Damaged/Loose Teeth: If you have several teeth that are extremely loose, severely decayed, or causing constant pain, and it's clear they cannot be saved.
- Persistent Oral Pain: Unrelenting pain in your gums, jaw, or multiple teeth that isn't relieved by over-the-counter medication.
- Difficulty Eating or Speaking: If chewing becomes impossible, or your speech is severely impaired due to missing or failing teeth, impacting your nutrition and communication.
- Acute Infection: Swelling, pus, or severe tenderness around multiple teeth or in your jaw, indicating a widespread infection.
Scheduled Appointment (Routine Care or Considering Options):
- Existing Ill-Fitting Dentures: If you currently wear traditional dentures that are loose, uncomfortable, require frequent adhesive, or cause sore spots, it's time to explore more stable options.
- Progressive Tooth Loss: You've lost several teeth over time, and you're noticing a significant impact on your oral function or facial appearance.
- Difficulty Maintaining Oral Hygiene: If your remaining teeth are so compromised that proper cleaning is a challenge, leading to recurrent issues.
- Changes in Facial Structure: You've observed a sunken appearance around your mouth or a receding jawline, indicating bone loss due to missing teeth.
- Desire for Improved Quality of Life: You want to eat, speak, and smile with confidence, seeking a long-term, stable solution that closely mimics natural teeth.
- Considering a Major Investment: If you are contemplating a significant dental investment and want to understand all your tooth replacement options for extensive tooth loss.
Don't wait until your oral health is in crisis. Proactive consultation with a qualified dental professional, such as a general dentist with experience in implants, a prosthodontist (a specialist in prosthetic dentistry), or an oral surgeon, can provide you with the information and personalized treatment plan you need. They can assess your individual situation, discuss the suitability of full mouth denture implants, and guide you through the process of restoring your smile and improving your overall quality of life.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Implantologist: Complete Guide
Losing a tooth can be a significant setback, impacting not only your smile but also your ability to speak, chew, and maintain overall oral health. In fact, over 3 million Americans currently have dental implants, and that number is projected to grow significantly as more people seek a durable, n
March 8, 2026
Dentures Over Implants: Complete Guide
Missing multiple teeth or even an entire arch can profoundly impact your life, affecting everything from your ability to chew and speak to your self-confidence. For millions of Americans, traditional removable dentures have long been a solution, but they often come with compromises: slipping, discom
March 8, 2026
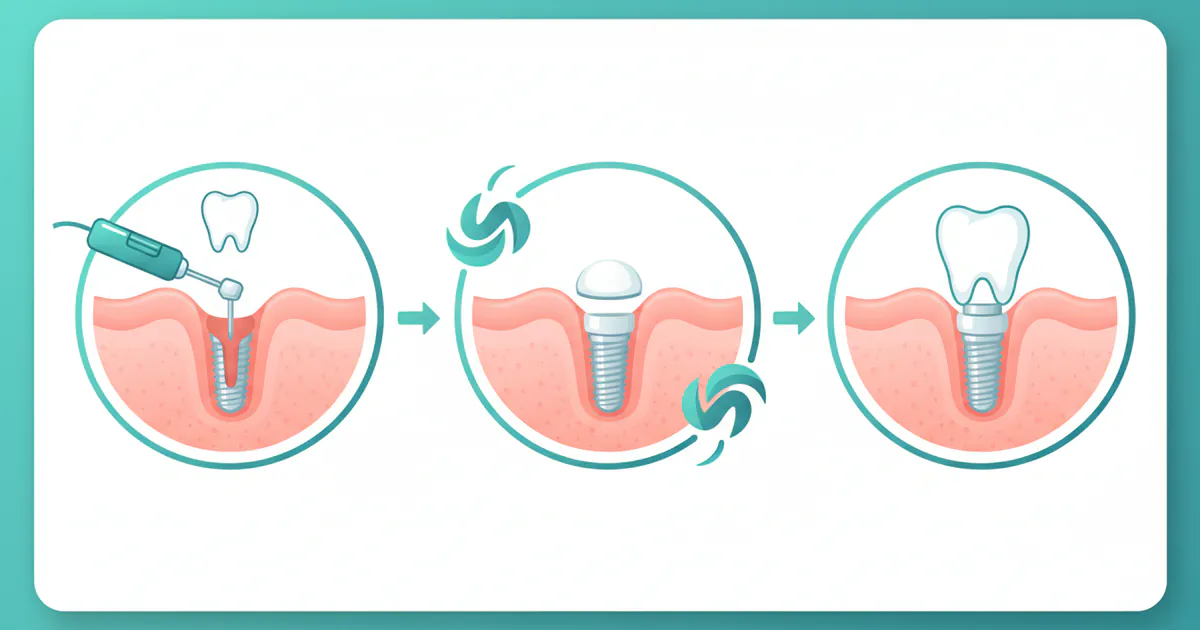
Implants Process: Complete Guide
Missing teeth can impact more than just your smile; they can affect your ability to eat, speak, and even your overall confidence. In fact, over 178 million Americans are missing at least one tooth, and about 40 million are missing all of their teeth. When faced with tooth loss, understanding the
March 8, 2026

Implants Dentaires: Complete Guide
Missing teeth can dramatically impact not just your smile, but your overall health, confidence, and quality of life. In the United States, an estimated 178 million adults are missing at least one tooth, while approximately 40 million are missing all their teeth. These statistics underscore a
March 8, 2026