Implantes: Complete Guide
Key Takeaways
- Dental implants, often referred to by their Spanish equivalent, implantes, represent a revolutionary solution for replacing missing teeth, offering a robust, long-lasting alternative to traditional bridges and dentures. The impact of tooth loss extends beyond mere aesthetics, affecting chewing a
Dental implants, often referred to by their Spanish equivalent, implantes, represent a revolutionary solution for replacing missing teeth, offering a robust, long-lasting alternative to traditional bridges and dentures. The impact of tooth loss extends beyond mere aesthetics, affecting chewing ability, speech clarity, and even the structural integrity of your jawbone. In the United States, millions of adults experience tooth loss, making the search for effective and reliable tooth replacement options a significant concern. Implantes offer a chance not just to restore a smile, but to reclaim oral health, comfort, and confidence, fundamentally improving quality of life. This comprehensive guide from SmilePedia.net will delve into every aspect of implantes, from their basic definition and various types to the detailed treatment process, associated costs, recovery expectations, and crucial prevention strategies, providing you with the knowledge needed to make informed decisions about your dental health.
Key Takeaways:
- Dental Implants (Implantes): A permanent tooth replacement solution consisting of a titanium post, an abutment, and a custom-made crown, designed to fuse with your jawbone.
- High Success Rate: Modern implantes boast a success rate of over 95% when placed by qualified professionals and properly maintained.
- Cost Variation: A single dental implant, including the implant, abutment, and crown, typically ranges from $4,000 to $8,000 in the US, with full-arch solutions like All-on-4 ranging from $20,000 to $50,000+ per arch.
- Treatment Timeline: The entire process, from initial surgery to final crown placement, can take 3 to 9 months, largely due to the required osseointegration period.
- Bone Health is Key: Adequate jawbone density is crucial for implant success; bone grafting procedures may be necessary for patients with bone loss, adding to cost and treatment duration.
- Durability & Longevity: With proper care, implantes can last 20 years to a lifetime, making them a worthwhile long-term investment compared to other tooth replacement options.
- Maintenance: Regular brushing, flossing, and professional dental check-ups are essential for preventing peri-implantitis and ensuring the longevity of your implantes.
What It Is / Overview
At its core, a dental implant, or "implante," is a sophisticated prosthetic device designed to replace a missing tooth root. Unlike other tooth replacement options that sit on top of the gums or rely on adjacent teeth for support, a dental implant surgically integrates with the jawbone, providing a stable and durable foundation for an artificial tooth. This unique process is known as osseointegration, where the bone naturally grows around and fuses with the implant post.
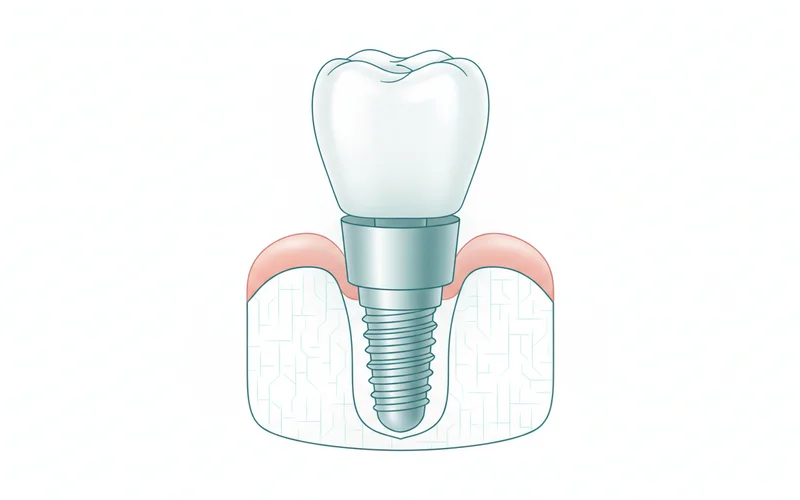
The structure of a dental implant typically comprises three main components:
- The Implant Post (Fixture): This is a small, screw-shaped post, most commonly made from biocompatible titanium (though zirconia is also used), that is surgically placed into the jawbone. Titanium is favored for its ability to integrate seamlessly with bone tissue without causing adverse reactions. This post acts as the new "root" of your replacement tooth.
- The Abutment: Once osseointegration is complete, a small connector piece called an abutment is attached to the top of the implant post. This component extends through the gum line and serves as the anchor for the final restoration.
- The Prosthesis (Crown, Bridge, or Denture): The final visible part of the implant restoration is the custom-made crown, bridge, or denture that is secured to the abutment. These prostheses are meticulously crafted to match the color, shape, and size of your natural teeth, ensuring a seamless and aesthetic integration into your smile.
Dental implants are widely regarded as the gold standard for tooth replacement due to their numerous advantages. They preserve surrounding healthy teeth, prevent bone loss in the jaw (a common consequence of missing teeth), restore chewing efficiency, improve speech, and offer superior aesthetics and comfort compared to removable alternatives. Their ability to function much like natural teeth provides an unparalleled sense of stability and confidence for patients.
Types / Variations
The field of dental implants has evolved significantly, offering several types and approaches tailored to individual patient needs, bone density, and the number of teeth requiring replacement. Understanding these variations is crucial for both patients and dental professionals.
Endosteal Implants
These are the most common type of dental implantes. "Endosteal" means "in the bone." They are typically screw-shaped, cylinder-shaped, or bladed, and are surgically placed directly into the jawbone. This type requires sufficient bone density and volume for successful integration. Endosteal implants are versatile and can be used for single tooth replacement, multiple teeth with a bridge, or to stabilize full dentures. The material is almost exclusively titanium, known for its strength and biocompatibility.
Subperiosteal Implants
"Subperiosteal" means "on the bone." These implants consist of a metal framework that is fitted onto the jawbone, just below the gum tissue. They are used primarily for patients who cannot wear conventional dentures and have insufficient bone height for endosteal implants, making bone grafting unfeasible or undesirable. While once more common, their use has declined significantly with advances in bone grafting techniques for endosteal implants.
Mini Dental Implants (MDIs)
Mini dental implants are smaller in diameter (typically less than 3mm) than traditional implants. They are often used as a temporary solution for stabilizing lower dentures, particularly for patients who may not be candidates for conventional implants due to severe bone loss or health issues. MDIs can also be used for immediate loading of temporary crowns or in areas with limited space. Their smaller size means less invasive surgery and often a quicker recovery, but they may not offer the same long-term stability as traditional implants for permanent restorations.
Zygomatic Implants
For patients with severe bone loss in the upper jaw (maxilla), where even extensive bone grafting isn't sufficient, zygomatic implants offer an advanced solution. These longer implants are anchored into the cheekbone (zygoma) instead of the maxilla. This bypasses the need for significant bone augmentation and can often facilitate immediate loading of a full arch prosthesis. Zygomatic implants are a complex procedure requiring specialized surgical expertise.
Immediate Load Dental Implants ("Teeth in a Day")
Also known as same-day implants or "Teeth in a Day," this technique allows for the placement of a temporary crown or prosthesis immediately after the implant surgery. This is possible when there is sufficient primary stability of the implant in the bone at the time of placement. While highly appealing for its instant aesthetic and functional benefits, not all patients are candidates for immediate loading. Criteria include good bone quality and quantity, a stable implant placement, and careful management of biting forces during the healing period.
All-on-4® / All-on-6® Dental Implants
These innovative techniques are designed to replace an entire arch of missing teeth (either upper or lower) using only four or six strategically placed implants. The implants are angled to maximize contact with existing bone, often eliminating the need for bone grafting. A full arch of prosthetic teeth is then attached to these implants, often on the same day as the surgery (immediate load). All-on-4 and All-on-6 provide a stable, fixed, and highly aesthetic solution for edentulous (toothless) patients, offering a dramatic improvement over traditional dentures.
Front Teeth Implants: Specific Considerations
When it comes to replacing front teeth implants, aesthetics and immediate results are often paramount. The surgical placement requires extreme precision to ensure the implant is perfectly aligned for an optimal cosmetic outcome. Factors like gum line symmetry, surrounding soft tissue contours, and the precise shade matching of the crown are critical. In some cases, a temporary crown may be placed on the same day of surgery to maintain aesthetics while osseointegration occurs. Bone grafting might be more frequently needed in the anterior (front) region to ensure sufficient bone for stable placement and natural gum contours.
Causes / Why It Happens (Tooth Loss)
Understanding the reasons behind tooth loss is crucial, as many are preventable, and prevention can often mitigate the need for future implantes. Tooth loss is a widespread issue, affecting a significant portion of the adult population in the U.S. According to the Centers for Disease Control and Prevention (CDC), over 17% of adults aged 65 and older have lost all of their natural teeth, and many more have experienced partial tooth loss.
Common causes include:
- Severe Tooth Decay (Cavities): Untreated cavities can progress deep into the tooth, infecting the pulp and eventually compromising the tooth's structural integrity to the point where extraction becomes the only option.
- Periodontal Disease (Gum Disease): This is the leading cause of tooth loss in adults. Periodontitis is an infection of the gums and supporting bone structure around the teeth. If left untreated, the inflammation and infection can destroy the bone, leading to tooth looseness and eventual loss.
- Trauma or Injury: Accidents, sports injuries, or falls can result in a tooth being knocked out (avulsed) or severely fractured beyond repair.
- Failed Root Canal Treatment: While root canals save millions of teeth each year, sometimes a treated tooth can become reinfected or fractured, leading to its eventual extraction.
- Congenital Absence: In some individuals, certain teeth never develop, a condition known as hypodontia. Implantes can provide a functional and aesthetic solution for these missing teeth.
- Bruxism (Teeth Grinding): Chronic grinding and clenching can wear down teeth, cause fractures, and stress the supporting structures, leading to tooth loss over time.
- Systemic Diseases: Certain medical conditions, such as diabetes, can increase the risk of gum disease and impair the body's healing capabilities, indirectly contributing to tooth loss.
- Aging: While not a direct cause, the cumulative effects of wear and tear, coupled with a lifetime of potential dental issues, can make older adults more susceptible to tooth loss.
Signs and Symptoms (of Missing Teeth and Their Impact)
While the "sign" of a missing tooth is obvious, the symptoms are the broader implications and consequences that highlight why tooth replacement, especially with implantes, is so vital.
- Difficulty Chewing: Missing teeth, particularly molars, significantly reduce chewing efficiency, leading to digestive issues and limiting dietary choices.
- Speech Impairment: Teeth play a crucial role in forming sounds. Missing front teeth or even posterior teeth can result in lisps, whistling, or difficulty pronouncing certain words clearly.
- Shifting of Remaining Teeth: When a tooth is lost, the adjacent teeth tend to drift into the empty space, disrupting the bite and potentially creating new gaps or crowding. The opposing tooth in the other jaw can also "over-erupt" into the space.
- Bone Resorption (Loss of Jawbone Density): This is one of the most significant consequences. When a tooth root is no longer present to stimulate the jawbone, the bone in that area begins to deteriorate or resorb. This can lead to a sunken facial appearance, especially with multiple missing teeth, and can complicate future implant placement.
- Changes in Facial Appearance: Loss of bone support, especially in the front of the mouth, can cause the lips and cheeks to sag, leading to a prematurely aged appearance.
- Increased Risk of TMJ Disorders: An unbalanced bite due to missing teeth can put undue stress on the temporomandibular joints (TMJ), leading to pain, clicking, and difficulty opening and closing the mouth.
- Psychological Impact: Missing teeth can severely impact self-confidence, leading to embarrassment, reluctance to smile, and social withdrawal.
Treatment Options (Alternatives to Implants)
While implantes are often the preferred choice, it's important for patients to understand all available tooth replacement options, along with their respective pros and cons.
1. Removable Partial Dentures (RPDs)
- Description: A removable appliance with artificial teeth attached to a gum-colored plastic base, held in place by metal clasps that hook onto natural teeth.
- Pros:
- Cost-Effective: Generally the least expensive option.
- Non-Invasive: No surgery required; no alteration of natural teeth.
- Quick to Fabricate: Can be made relatively quickly.
- Cons:
- Less Stable: Can shift or become dislodged during chewing or speaking.
- Bone Loss: Does not prevent jawbone deterioration; can accelerate it.
- Comfort: May feel bulky and less comfortable than fixed options.
- Maintenance: Requires daily removal for cleaning and soaking.
- Aesthetics: Clasps can sometimes be visible.
- Dietary Restrictions: May require avoiding certain hard or sticky foods.
2. Fixed Partial Dentures (Bridges)
- Description: Consists of one or more artificial teeth (pontics) fused between two crowns that are cemented onto the natural teeth adjacent to the gap.
- Pros:
- Fixed Solution: Non-removable, offering better stability than RPDs.
- Good Aesthetics: Can look very natural.
- Improved Chewing: Restores chewing function effectively.
- Faster Treatment: Can be completed in a few weeks.
- Cons:
- Tooth Alteration: Requires grinding down healthy adjacent teeth to serve as anchors for the crowns, making them more susceptible to decay or sensitivity.
- No Bone Stimulation: Does not prevent bone loss in the area of the missing tooth.
- Maintenance: Can be challenging to clean underneath the pontic, increasing the risk of decay in the anchor teeth.
- Lifespan: Typically lasts 10-15 years before needing replacement.
3. Full Dentures (Complete Dentures)
- Description: A removable appliance that replaces an entire arch of missing teeth, resting directly on the gums.
- Pros:
- Cost-Effective (Full Arch): More affordable than full-arch implant solutions initially.
- Non-Invasive: No surgery required.
- Quick Replacement: Can provide a full set of teeth relatively quickly.
- Cons:
- Poor Stability: Can slip, click, or fall out, especially the lower denture, leading to embarrassment and speech issues.
- Accelerated Bone Loss: Does not stimulate the jawbone, leading to accelerated bone resorption and a "sunken" facial appearance over time.
- Reduced Chewing Efficiency: Can reduce chewing force by up to 75% compared to natural teeth, severely limiting dietary options.
- Discomfort & Sore Spots: May cause irritation, sores, and require frequent adjustments.
- Maintenance: Requires daily removal for cleaning and soaking.
Comparison Table: Tooth Replacement Options
| Feature | Dental Implants (Implantes) | Fixed Bridge | Removable Partial Denture (RPD) | Full Denture |
|---|---|---|---|---|
| Stability | Excellent (fixed in bone) | Good (fixed to adjacent teeth) | Fair (clasps on teeth, can move) | Poor (rests on gums, can slip) |
| Bone Preserve | Yes (stimulates jawbone) | No (bone loss continues under pontic) | No (bone loss continues) | No (accelerates bone loss) |
| Longevity | 20+ years, often lifetime | 10-15 years | 5-10 years | 5-7 years (needs frequent relines/replacements) |
| Aesthetics | Excellent (mimics natural tooth) | Very Good (can look natural) | Good (clasps sometimes visible) | Fair to Good (can look artificial) |
| Chewing Power | Excellent (like natural teeth) | Good | Fair (reduced force) | Poor (significantly reduced force) |
| Adjacent Teeth | Not affected | Healthy teeth must be ground down | Clasps can stress adjacent teeth | Not applicable (replaces all teeth) |
| Cost (Single) | $4,000-$8,000 | $2,000-$5,000 | $700-$2,000 | N/A (for single tooth) |
| Cost (Full Arch) | $20,000-$50,000+ per arch (All-on-4/6) | N/A | $1,500-$3,000+ per arch | $1,500-$5,000+ per arch |
Step-by-Step Process (What to Expect During Treatment)
The process of getting implantes is a multi-stage journey that prioritizes precision, healing, and successful integration. While timelines can vary, the general steps remain consistent.
1. Initial Consultation and Comprehensive Examination
Your journey begins with a thorough evaluation by a dental implant specialist (often an oral surgeon or periodontist, in conjunction with a prosthodontist or general dentist).
- Medical History Review: To identify any underlying health conditions or medications that might affect treatment.
- Oral Examination: Assessment of your remaining teeth, gums, and existing restorations.
- Diagnostic Imaging: This is critical. It typically includes:
- X-rays: Panoramic and periapical views to assess bone height and width.
- 3D CT Scan (Cone Beam CT - CBCT): Provides highly detailed images of your jawbone, nerve pathways, sinus cavities, and precise bone volume, which is essential for accurate implant placement planning.
- Impressions: Digital or traditional impressions of your mouth are taken to create models for treatment planning and prosthetic fabrication.
2. Treatment Planning
Using the diagnostic images and models, your dental team will develop a personalized treatment plan. This involves:
- Determining Implant Type: Deciding on the appropriate type and size of implantes.
- Surgical Guide Fabrication: Often, a custom surgical guide (a stent that fits over your teeth or gums) is created using CAD/CAM technology to direct the implant placement with extreme accuracy, especially for front teeth implants where aesthetics are paramount.
- Addressing Ancillary Procedures: Identifying if procedures like bone grafting or a sinus lift are necessary before implant placement.
3. Pre-Surgical Procedures (If Needed)
Some patients may require preparatory procedures to create an ideal environment for the implant.
- Tooth Extractions: If damaged or decayed teeth are present, they will be extracted.
- Bone Grafting: If you have insufficient jawbone density due to long-term tooth loss or periodontal disease, bone grafting may be necessary. This involves adding bone material (synthetic, animal, or your own bone) to augment the jaw. This procedure can add 3-9 months to the overall treatment timeline for healing.
- Sinus Lift (Sinus Augmentation): For the upper jaw, if the maxillary sinuses are too close to the area where implants are needed, a sinus lift elevates the sinus membrane and places bone graft material to create sufficient height for the implant.
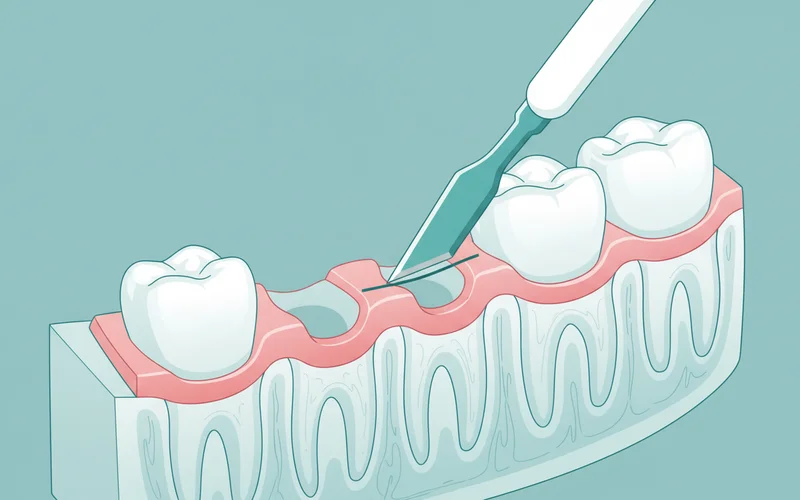
4. Implant Placement Surgery
This is the surgical phase where the implant post is placed.
- Anesthesia: Local anesthesia is typically used, often combined with sedation (oral, IV, or nitrous oxide) for patient comfort.
- Incision: A small incision is made in the gum tissue to expose the jawbone.
- Drilling: Using specialized drills, a precisely sized and shaped hole is prepared in the bone.
- Implant Placement: The titanium implant post is carefully screwed or tapped into the prepared site.
- Suturing: The gum tissue is then repositioned and sutured closed over the implant. In some cases, a healing abutment that protrudes through the gum may be placed immediately.
5. Osseointegration Period
This is the critical healing phase where the implant fuses with the jawbone.
- Duration: This process typically takes 3 to 6 months, though it can be shorter or longer depending on individual healing capabilities and bone quality.
- Temporary Solutions: During this time, patients often wear a temporary crown, bridge, or denture to maintain aesthetics and function.
- Monitoring: Your dentist will monitor the healing process to ensure successful osseointegration.
6. Abutment Placement (Second-Stage Surgery, if needed)
If the implant was fully covered by gum tissue during the initial surgery (a two-stage procedure), a second minor surgical procedure is needed to uncover the implant and attach the abutment. This involves a small incision to expose the top of the implant and secure the abutment. A healing cap is then placed to allow the gum tissue to heal correctly around the abutment.
7. Prosthesis (Crown/Bridge/Denture) Placement
Once the gums have healed around the abutment, the final restoration can be fabricated and placed.
- Impressions: New impressions (digital or traditional) are taken of the abutment and surrounding teeth.
- Fabrication: A dental lab meticulously crafts your custom crown, bridge, or denture from materials like porcelain, ceramic, or zirconia, ensuring it matches your natural teeth in color, shape, and size.
- Final Attachment: The custom prosthesis is then permanently cemented or screwed onto the abutment. Adjustments are made to ensure a comfortable and proper bite.
Pro Tip: Be patient during the osseointegration phase. Rushing this critical healing period can compromise the long-term success of your implantes. Follow all post-operative instructions diligently.
Cost and Insurance
The investment in implantes is significant, reflecting the complexity of the procedure, the quality of materials, and the specialized expertise required. Costs can vary widely depending on several factors, including geographic location, the number of implantes needed, the type of implant, the materials used for the crown, and the need for supplementary procedures.
Average US Cost Ranges:
- Single Dental Implant (Implant, Abutment, Crown):
- Low End: $4,000 - $5,000
- Mid-Range: $5,000 - $7,000
- High End: $7,000 - $8,000+
- Note: The implant post itself typically costs $1,500 - $3,000, with the abutment adding $300 - $600, and the crown adding another $1,000 - $3,000.
- Bone Grafting:
- Minor (socket preservation): $200 - $500
- Moderate: $500 - $1,500
- Major (block graft): $2,000 - $3,000+
- Sinus Lift:
- Unilateral (one side): $1,500 - $2,500
- Bilateral (both sides): $3,000 - $4,500+
- Full Arch Implants (e.g., All-on-4/6):
- Per Arch: $20,000 - $50,000+
- This includes the implants, abutments, and a full arch fixed prosthesis (often made of acrylic or zirconia).
How Much is a Gold Tooth Implant?
This is a common question, but it stems from a misunderstanding of implant materials. The implant post (the part surgically placed into your jawbone) is almost exclusively made of titanium or zirconia. These materials are chosen for their biocompatibility and ability to osseointegrate with bone, not for their aesthetic value or cost as precious metals.
However, the crown that sits on top of the implant (the visible part) can be made from various materials, including:
- Porcelain-fused-to-metal (PFM): Where a metal alloy forms the base, which can sometimes contain gold, and porcelain is fused over it.
- Full Gold Crowns: While rare for implantes today, some patients might opt for a full gold crown for a back tooth for its durability and biocompatibility, historically used before advanced ceramics.
If you are asking "how much is a gold tooth implant" because you desire a gold crown on your implant, the cost of the gold crown itself would typically be $800 - $2,500, adding to the overall implant cost. Gold crowns are generally more expensive than ceramic or porcelain options due to the material cost of gold. However, it's crucial to clarify with your dentist whether a gold crown is clinically appropriate and aesthetically desirable for your specific implant location. Most patients opt for tooth-colored ceramic or zirconia for aesthetic reasons.
Insurance Coverage Details
Dental insurance typically offers limited coverage for implantes.
- Dental Insurance: Most standard dental plans consider implants a "major procedure" and may cover 10% to 50% of the cost, often up to their annual maximum (which is frequently around $1,000 - $2,000). It's vital to check your specific policy for exclusions, waiting periods, and annual limits. Some policies may classify implants as "cosmetic" and deny coverage entirely.
- Medical Insurance: If tooth loss is due to an accident, trauma, or certain medical conditions, some components of the implant procedure (e.g., bone grafting, extractions, certain imaging) might be covered under your medical insurance. This is rare but worth investigating, especially if the oral surgeon processes claims as medical procedures.
- Supplemental Insurance: Some insurance companies offer supplemental dental plans specifically designed to provide better coverage for major procedures like implants, often with higher annual maximums.
Payment Plans and Financing Options
Due to the cost, many patients explore financing:
- In-Office Payment Plans: Many dental practices offer their own interest-free payment plans, allowing patients to spread costs over several months.
- Third-Party Financing: Companies like CareCredit or LendingClub provide healthcare credit cards or personal loans specifically for dental procedures, often with promotional periods of 0% interest.
- Health Savings Accounts (HSAs) & Flexible Spending Accounts (FSAs): These tax-advantaged accounts allow you to save and pay for qualified medical and dental expenses with pre-tax dollars, significantly reducing your out-of-pocket costs.
- Dental Schools: University dental schools often provide implant treatments at a reduced cost, as procedures are performed by students under the close supervision of experienced faculty.
Pro Tip: Always request a detailed written estimate from your dental provider that itemizes all costs, including the implant, abutment, crown, and any necessary preparatory procedures. Submit this estimate to your insurance provider for a pre-determination of benefits before commencing treatment.
Recovery and Aftercare
Successful recovery and diligent aftercare are paramount for the long-term success and longevity of your implantes. Adhering to your dentist's instructions will ensure proper healing and prevent complications.
Immediate Post-Surgery (First 24-72 Hours)
- Pain Management: You will likely experience some discomfort. Take prescribed pain medication as directed. Over-the-counter pain relievers (like ibuprofen) can also be effective.
- Swelling: Swelling is common. Apply an ice pack to the outside of your face for 15-20 minutes on, 15-20 minutes off, for the first 24-48 hours.
- Bleeding: Minor bleeding or oozing from the surgical site is normal. Bite gently on gauze pads and change them as needed. Avoid spitting forcefully.
- Rest: Get plenty of rest and avoid strenuous activities for at least 48-72 hours. Elevate your head while sleeping.
- Diet: Stick to soft foods and liquids initially. Avoid hot beverages, crunchy, hard, or spicy foods, and using a straw (which can dislodge blood clots).
- Oral Hygiene: Do NOT rinse your mouth for the first 24 hours. After that, gentle salt water rinses (1/2 teaspoon salt in 8 oz warm water) 2-3 times a day can help keep the area clean. Brush gently, avoiding the surgical site.
During Osseointegration (3-6 Months)
- Diet: You can gradually reintroduce more solid foods, but continue to avoid chewing directly on the implant site. If you have a temporary prosthesis, be extra cautious with hard or sticky foods to prevent damage or dislodgement.
- Oral Hygiene: Maintain excellent oral hygiene with regular brushing (twice daily) and flossing (at least once daily). Your dentist may recommend specific interdental brushes or water flossers for cleaning around the temporary prosthesis or adjacent teeth.
- Avoid Smoking: Smoking significantly increases the risk of implant failure by impairing blood flow and healing. It is strongly advised to quit smoking before and after implant surgery.
- Avoid Alcohol: Alcohol consumption can delay healing.
- Follow-Up Appointments: Attend all scheduled follow-up appointments with your dentist to monitor healing and osseointegration.
Long-Term Care (After Final Restoration)
Once your final crown, bridge, or denture is placed, long-term care mimics that of natural teeth, but with a few important considerations.
- Daily Oral Hygiene:
- Brushing: Brush your implantes and natural teeth twice daily with a soft-bristled toothbrush.
- Flossing: Floss daily. Special floss designed for implants or a water flosser can be very effective for cleaning around the implant crown and under bridges.
- Mouthwash: An antimicrobial mouthwash may be recommended by your dentist.
- Regular Dental Check-ups: Schedule professional cleanings and examinations every 6 months (or as recommended by your dentist/hygienist). Your dental team will specifically check the health of your implantes, assess surrounding gum tissue, and take X-rays periodically to monitor bone levels.
- Avoid Harmful Habits: Do not use your implantes (or natural teeth) to open packages, bite nails, or chew on ice. If you grind or clench your teeth (bruxism), your dentist may recommend a night guard to protect your implants and natural teeth.
- Diet: While implantes restore full chewing function, avoid excessively hard or sticky foods that could potentially damage the crown or surrounding gum tissue over time.
Pro Tip: Think of your implantes like precious natural teeth. The better you care for them, the longer they will last. Neglecting oral hygiene can lead to peri-implantitis, a serious infection that can cause implant failure.
Prevention (of Implant Failure and Tooth Loss)
Preventing implant failure largely revolves around diligent oral hygiene and lifestyle choices, while preventing original tooth loss involves general excellent dental health practices.
Preventing Implant Failure
- Strict Oral Hygiene: As highlighted in recovery and aftercare, meticulous daily brushing and flossing around your implantes is the single most important factor. This prevents the buildup of plaque and bacteria that can lead to peri-implantitis.
- Regular Professional Cleanings: Visit your dentist or dental hygienist regularly for professional cleanings. They use specialized instruments that won't scratch the implant surface and can identify early signs of problems. The American Dental Association (ADA) recommends at least annual check-ups, but implant patients often benefit from more frequent visits.
- Quit Smoking: Smoking dramatically increases the risk of implant failure due to impaired healing and reduced blood supply to the tissues around the implant.
- Manage Systemic Diseases: Conditions like diabetes can affect healing and increase susceptibility to infections. Keeping these conditions well-controlled is vital for implant success.
- Address Bruxism: If you grind or clench your teeth, wear a custom night guard as prescribed by your dentist to protect your implantes from excessive forces.
- Promptly Address Any Issues: If you notice pain, swelling, bleeding, or any looseness around your implant, contact your dentist immediately.
Preventing Tooth Loss (and thus the need for Implants)
- Maintain Excellent Oral Hygiene: Brush your teeth twice a day for two minutes each time with fluoride toothpaste. Floss daily to remove plaque and food particles from between teeth and under the gumline.
- Regular Dental Check-ups and Cleanings: Visit your dentist every six months for professional cleanings and examinations. Early detection of cavities or gum disease can prevent them from escalating to tooth loss.
- Balanced Diet: Limit sugary and acidic foods and drinks, which contribute to tooth decay. Incorporate calcium-rich foods for strong bones and teeth.
- Protect Your Teeth: Wear a mouthguard during sports activities to prevent traumatic injuries to your teeth.
- Avoid Tobacco Products: Smoking and chewing tobacco are major risk factors for gum disease and oral cancer, both of which can lead to tooth loss.
- Manage Medical Conditions: If you have conditions like diabetes, follow your doctor's advice carefully, as these can impact your oral health.
Risks and Complications
While implantes have an impressive success rate (over 95%), like any surgical procedure, they carry potential risks and complications. Being aware of these can help you identify issues early and seek prompt attention.
- Infection at the Implant Site: Although rare due to sterile techniques, bacterial infection can occur during or after surgery. Symptoms include pain, swelling, fever, and pus.
- Nerve Damage: During implant placement, there's a small risk of nerve damage, particularly in the lower jaw, which can cause numbness, tingling, or pain in the lips, gums, tongue, or chin. This is often temporary but can be permanent in rare cases. Advanced imaging (CBCT) and surgical guides help minimize this risk.
- Sinus Perforation: When placing implants in the upper jaw, there's a risk of the implant penetrating the sinus cavity. This can be managed with a sinus lift procedure, but if a perforation occurs, it can lead to complications like sinusitis.
- Implant Failure (Lack of Osseointegration): The implant may fail to fuse with the jawbone. This can be due to poor bone quality, infection, excessive force on the implant during healing, or certain medical conditions. If an implant fails, it may need to be removed, the site allowed to heal, and a new implant placed later.
- Peri-implantitis: This is a serious inflammatory condition affecting the tissues surrounding a dental implant. It's similar to periodontal disease around natural teeth and can lead to bone loss around the implant, ultimately causing implant mobility and failure if left untreated. Poor oral hygiene and smoking are primary risk factors.
- Loose Abutment or Crown: Over time, the screws connecting the abutment to the implant, or the crown to the abutment, can loosen. This is usually easily fixed by tightening or replacing the screw.
- Fracture of the Implant or Prosthesis: While implantes are strong, excessive biting forces or trauma can, in rare cases, lead to fracture of the implant itself or the prosthetic crown/bridge.
- Allergic Reaction: Although rare, some individuals might have an allergic reaction to titanium, though zirconia implants can be an alternative in such cases.
- Gum Recession: In some cases, the gum tissue around the implant may recede, exposing the top of the implant or abutment, which can be an aesthetic concern, particularly for front teeth implants.
Pro Tip: If you experience persistent pain, swelling, pus, numbness, or if your implant feels loose at any point, contact your dental implant specialist immediately. Early intervention is crucial for managing potential complications.
Children / Pediatric Considerations
Dental implants are generally not recommended for children and adolescents whose jaws are still developing. The jawbones typically continue to grow until late adolescence or early adulthood (around 18-20 years for females, and slightly later for males). Placing an implant in a growing jaw can interfere with natural bone development, causing the implant to become misaligned or "submerged" relative to the surrounding teeth as the jaw continues to grow.
For children who have lost permanent teeth due to trauma or congenital absence, temporary tooth replacement options like removable partial dentures (flippers) or space maintainers are usually preferred until full skeletal maturity is reached. Once growth is complete, implantes can then be considered as a permanent solution. Your pediatric dentist or orthodontist can monitor jaw development and advise on the appropriate timing for implant evaluation.
Frequently Asked Questions
What are implantes and how do they work?
Implantes, or dental implants, are titanium posts surgically placed into the jawbone to serve as artificial tooth roots. Through a process called osseointegration, the bone fuses with the implant, providing a stable foundation for a custom-made crown, bridge, or denture. They restore chewing function, speech, and aesthetics, acting like natural teeth.
Are implantes painful?
The implant placement surgery is typically performed under local anesthesia, so you should not feel pain during the procedure. Post-operative discomfort is managed with prescribed pain medication, and most patients report that the pain is less severe than expected, often comparable to a tooth extraction.
How long do implantes last?
With proper oral hygiene and regular dental check-ups, dental implants can last 20 years to a lifetime. The implant post itself rarely needs replacement, though the crown or prosthesis attached to it may need to be replaced after 10-15 years due to normal wear and tear.
What is the success rate of implantes?
The success rate for dental implants is remarkably high, often exceeding 95% for individual implants when performed by experienced professionals and maintained correctly. Factors like bone quality, patient health, and oral hygiene significantly influence success.
Can anyone get implantes?
While many people are candidates for implantes, it's not suitable for everyone. Good candidates generally have sufficient healthy jawbone, healthy gums, and overall good health. Factors like uncontrolled diabetes, significant smoking, or certain medical conditions can be contraindications or increase risks. A thorough evaluation by a dental professional is essential.
How do I care for my implantes?
Caring for your implantes is similar to caring for natural teeth. This involves diligent brushing twice a day, flossing daily (using special implant floss or a water flosser), and regular dental check-ups and professional cleanings every 6 months. Avoiding smoking and excessive biting on hard objects is also crucial.
Is a gold tooth implant better, and how much does it cost?
The implant post itself is made of titanium or zirconia, not gold, due to their biocompatibility and ability to fuse with bone. If you're referring to a gold crown placed on top of an implant, gold crowns are highly durable and biocompatible, making them a good option for back teeth. A gold crown can add an additional $800 to $2,500 to the overall implant cost, making it generally more expensive than porcelain or ceramic crowns.
How long does the implante process take from start to finish?
The entire implant process typically takes 3 to 9 months, from the initial surgery to the final placement of the permanent crown. This timeline includes the crucial osseointegration period (3-6 months) where the implant fuses with the jawbone, and any preparatory procedures like bone grafting, which can add several months.
What foods should I avoid with implantes?
Immediately after surgery, stick to a soft diet. Once the final prosthesis is placed and healed, implantes allow you to eat most foods comfortably. However, it's wise to avoid excessively hard candies, ice, or very sticky foods that could potentially damage the crown or place undue stress on the implant over many years.
Can I get front teeth implants, and are there special considerations?
Yes, front teeth implants are very common and highly successful. The primary special consideration for front teeth is aesthetics. Extreme precision is required during placement to ensure natural-looking gum lines and seamless integration with your smile. Sometimes, a temporary crown may be placed on the day of surgery for immediate cosmetic benefits, and bone grafting might be needed to achieve optimal gum contours.
When to See a Dentist
Knowing when to seek professional dental attention is vital for maintaining your oral health and the longevity of your implantes.
For Missing Teeth or Implant Consideration:
- You have one or more missing teeth: If you're considering tooth replacement options, especially implantes, schedule a consultation. Early intervention can prevent further bone loss and shifting of adjacent teeth.
- Your current dentures or bridges are uncomfortable or unstable: If you're struggling with loose dentures or a failing bridge, a consultation can explore more stable, fixed implant solutions.
For Existing Implantes:
- Routine Check-ups: The most important "when to see a dentist" for existing implants is your regular 6-month check-up and cleaning. These appointments are crucial for professional cleaning, monitoring the health of your implants, and detecting any issues early.
- Signs of Complication (Red Flags - Seek Immediate Attention):
- Persistent Pain or Tenderness: If you experience ongoing pain around the implant site that doesn't subside or worsens.
- Swelling or Redness: Noticeable swelling, redness, or inflammation of the gums surrounding the implant.
- Bleeding: Bleeding from the gum tissue around the implant, especially when brushing or flossing.
- Pus or Discharge: Any sign of pus or foul taste emanating from the implant area.
- Looseness: If the implant, abutment, or crown feels loose or wobbly. This is a critical sign and requires immediate professional evaluation.
- Numbness or Tingling: Persistent numbness or tingling in your lip, tongue, or jaw after implant surgery could indicate nerve involvement.
- Broken or Chipped Crown: While not an emergency, a damaged crown should be addressed promptly to prevent further issues.
Never ignore persistent symptoms around your dental implants. Early detection and treatment of complications like peri-implantitis can often save the implant and prevent more extensive and costly interventions. Contact your dental implant specialist as soon as you notice any of these warning signs.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Implantologist: Complete Guide
Losing a tooth can be a significant setback, impacting not only your smile but also your ability to speak, chew, and maintain overall oral health. In fact, over 3 million Americans currently have dental implants, and that number is projected to grow significantly as more people seek a durable, n
March 8, 2026
Dentures Over Implants: Complete Guide
Missing multiple teeth or even an entire arch can profoundly impact your life, affecting everything from your ability to chew and speak to your self-confidence. For millions of Americans, traditional removable dentures have long been a solution, but they often come with compromises: slipping, discom
March 8, 2026
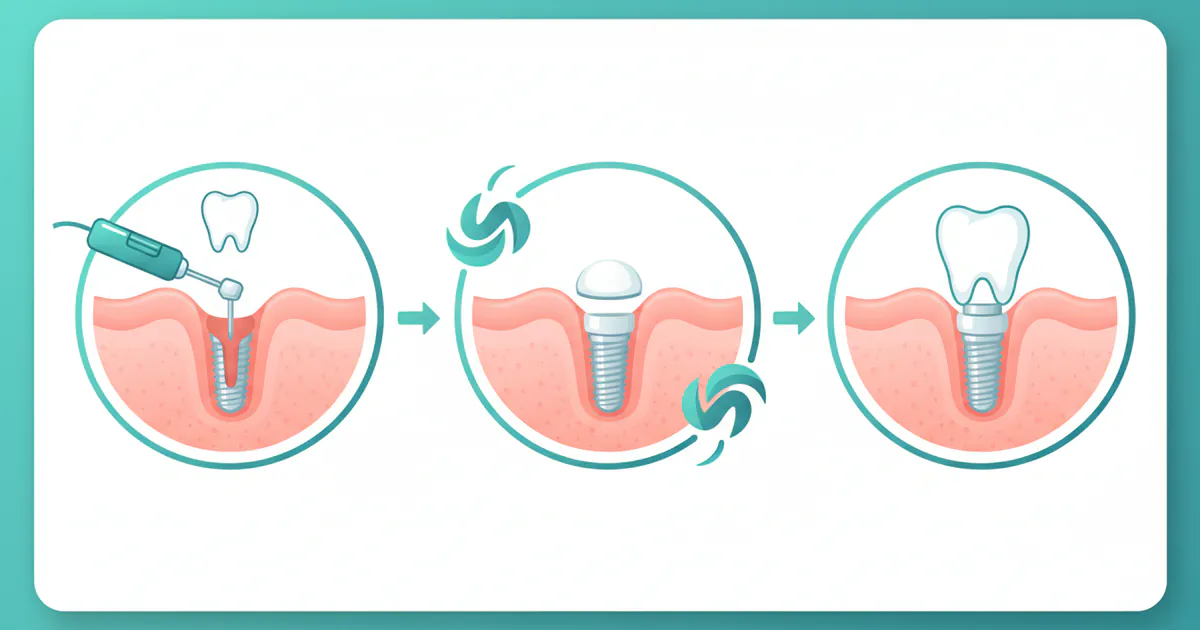
Implants Process: Complete Guide
Missing teeth can impact more than just your smile; they can affect your ability to eat, speak, and even your overall confidence. In fact, over 178 million Americans are missing at least one tooth, and about 40 million are missing all of their teeth. When faced with tooth loss, understanding the
March 8, 2026

Implants Dentaires: Complete Guide
Missing teeth can dramatically impact not just your smile, but your overall health, confidence, and quality of life. In the United States, an estimated 178 million adults are missing at least one tooth, while approximately 40 million are missing all their teeth. These statistics underscore a
March 8, 2026