Calcium Deficiency in Teeth: Complete Guide
Key Takeaways
- Did you know that 99% of your body's calcium resides in your bones and teeth? While often overlooked until problems arise, a lack of this vital mineral can significantly compromise your oral health, leading to a host of dental issues that extend far beyond a simple cavity. In the United States,
Calcium Deficiency in Teeth: Complete Guide
Did you know that 99% of your body's calcium resides in your bones and teeth? While often overlooked until problems arise, a lack of this vital mineral can significantly compromise your oral health, leading to a host of dental issues that extend far beyond a simple cavity. In the United States, an estimated 44% of adults do not meet their daily recommended calcium intake, setting the stage for potential systemic and dental challenges. Understanding calcium deficiency in teeth is paramount for maintaining a strong, healthy smile throughout your life.

This comprehensive guide will delve into the intricacies of how insufficient calcium affects your pearly whites, distinguishing between systemic deficiencies and localized mineral loss in enamel. We'll explore the underlying causes, recognizable signs and symptoms, and the full spectrum of modern treatment options available. From preventive measures to detailed cost breakdowns and pediatric considerations, you'll gain the authoritative knowledge needed to protect your teeth from the insidious effects of low calcium. Prepare to unlock a deeper understanding of your dental health and learn actionable strategies to ensure your smile remains strong and vibrant.
Key Takeaways:
- Enamel Demineralization: The primary dental manifestation of "calcium deficiency in teeth" is often demineralization of enamel, leading to white spots, increased sensitivity, and higher cavity risk. This is distinct from systemic calcium deficiency, though the two can be related.
- Dietary & Lifestyle Impact: Insufficient calcium intake, poor diet, certain medical conditions (e.g., celiac disease, Crohn's), and lifestyle factors (e.g., excessive soda consumption, acid reflux) are major contributors.
- Early Detection is Key: White spots on teeth, increased sensitivity to hot/cold, and recurrent cavities are early warning signs. Regular dental check-ups (typically every 6 months) can detect demineralization before it becomes a full-blown cavity.
- Treatment Varies: Treatments range from topical fluoride applications and remineralizing toothpastes for early stages, to dental fillings, crowns, or even root canals for advanced decay. Costs for treatments can vary widely, from $50-$250 for fluoride varnish to $150-$400 for a single filling, and $800-$3,000+ for crowns, often covered partially by dental insurance.
- Prevention is Paramount: A balanced diet rich in calcium and Vitamin D, excellent oral hygiene, regular dental visits, and avoiding acidic foods/drinks are crucial for preventing demineralization.
- Addressing Misconceptions: "Calcium deposits in teeth" usually refers to dental calculus (tartar), which is a buildup on teeth, not a deficiency within them. It's important to understand this distinction.
What Is Calcium Deficiency in Teeth?
When we talk about calcium deficiency in teeth, it's crucial to understand that we are often referring to two related but distinct concepts:
- Systemic Calcium Deficiency (Hypocalcemia): This is a broader condition where the body doesn't have enough calcium in the blood and bones. While teeth are incredibly hard, the enamel, which is 96% mineral, primarily hydroxyapatite (a crystalline form of calcium phosphate), is not a living tissue that can easily draw calcium from the bloodstream for repair like bones can. However, severe systemic calcium deficiencies, especially during tooth development in childhood, can lead to weakened enamel formation (enamel hypoplasia) and make teeth more susceptible to decay later in life. In adults, prolonged systemic deficiency can contribute to issues like osteoporosis, which indirectly impacts jawbone density and the stability of teeth.
- Localized Enamel Demineralization: This is the more common phenomenon directly impacting tooth structure, often mistaken for or referred to as "calcium deficiency in teeth." It occurs when acids in the mouth (produced by bacteria metabolizing sugars, or from acidic foods/drinks, or acid reflux) attack the enamel surface. These acids cause calcium and phosphate minerals to leach out of the enamel structure, weakening it. This process is called demineralization. If unchecked, this weakening can progress from white spots to full-blown cavities.
So, while systemic calcium intake is vital for overall health and healthy tooth development, the direct, day-to-day "deficiency" causing problems in adult teeth is usually about the loss of calcium and other minerals from the enamel due to acidic attacks, rather than an inability to obtain calcium. The term low calcium teeth generally refers to teeth whose enamel has been weakened by this mineral loss, making them more vulnerable.
It's also important to clarify the term "calcium deposits in teeth." This phrase often causes confusion. In a dental context, "calcium deposits" typically refers to:
- Dental Calculus (Tartar): This is hardened plaque, a mineralized bacterial biofilm that forms on the surface of teeth. It consists of calcium phosphate minerals from saliva that have crystallized within the plaque. Calculus is a sign of poor oral hygiene, not a calcium deficiency within the tooth.
- Pulp Stones (Denticles): These are calcified masses that can form within the dental pulp (the innermost part of the tooth containing nerves and blood vessels). While they are made of mineralized tissue, they are not typically symptomatic and are not related to enamel's calcium content or deficiency.
For the purpose of this article, when we discuss calcium deficiency in teeth, our primary focus will be on the processes of demineralization and the factors contributing to the loss or lack of sufficient minerals within the tooth structure, particularly the enamel, and how this impacts dental health.
Causes of Low Calcium Teeth
Understanding why teeth lose their vital minerals is key to prevention and treatment. The causes can be broadly categorized into dietary, systemic, and localized factors.
Dietary Factors
- Insufficient Calcium Intake: The most direct cause. If your diet consistently lacks calcium-rich foods (dairy, fortified plant milks, leafy greens), your body may not have enough calcium to support general health, which indirectly affects dental health over the long term, especially during development.
- ADA Recommendation: The ADA, in line with general health guidelines, emphasizes adequate calcium intake for strong bones and teeth. For adults, the recommended daily allowance (RDA) is typically 1,000 mg, increasing to 1,200 mg for women over 50 and men over 70.
- Vitamin D Deficiency: Vitamin D is crucial for the absorption of calcium from the gut into the bloodstream. Without enough Vitamin D, even a calcium-rich diet may not be sufficient.
- Vitamin K2 Deficiency: Works with Vitamin D to direct calcium to appropriate places (bones and teeth) and away from soft tissues.
- Excessive Acidic Foods and Drinks: Regular consumption of sodas, sports drinks, fruit juices, and acidic foods (citrus fruits, vinegar) directly erodes enamel. This demineralization process leaches calcium and phosphate from the tooth structure.
- High Sugar Intake: Sugars feed oral bacteria, which produce acids that demineralize enamel. This is the primary mechanism behind cavity formation.
Systemic Factors
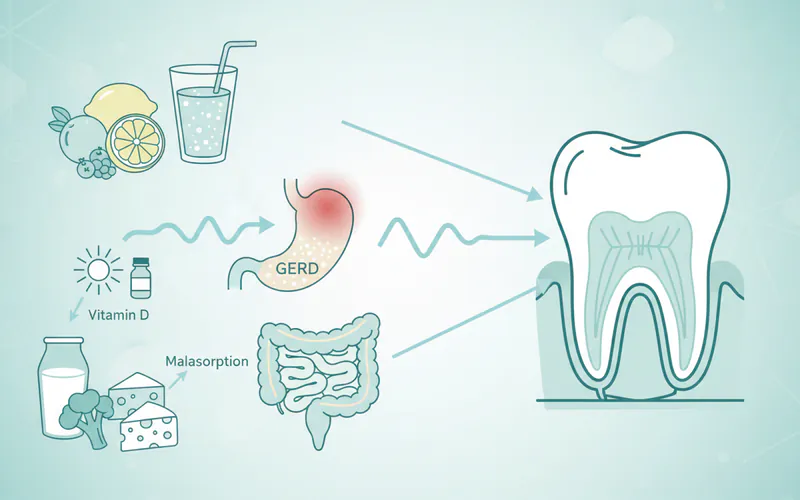
- Malabsorption Issues: Conditions like celiac disease, Crohn's disease, irritable bowel syndrome, or gastric bypass surgery can impair the body's ability to absorb calcium and Vitamin D, leading to systemic deficiency.
- Hormonal Imbalances:
- Hypoparathyroidism: A condition where the parathyroid glands produce too little parathyroid hormone, leading to low blood calcium levels.
- Menopause: Estrogen plays a role in bone density. After menopause, women often experience accelerated bone loss, which can indirectly affect jawbone density.
- Certain Medications: Long-term use of some medications, such as corticosteroids, certain diuretics, or proton pump inhibitors, can interfere with calcium absorption or metabolism.
- Kidney Disease: Impaired kidney function can affect Vitamin D activation and calcium regulation in the body.
- Eating Disorders: Anorexia nervosa and bulimia can lead to severe nutritional deficiencies, including calcium, and the frequent exposure to stomach acid (in bulimia) directly erodes enamel.
- Chronic Diseases: Some chronic diseases can affect overall nutrient absorption and bone health.
Localized Oral Environment Factors
- Poor Oral Hygiene: Inadequate brushing and flossing allow plaque to accumulate. Plaque is a sticky film of bacteria that produces acids from food particles, leading to demineralization.
- Dry Mouth (Xerostomia): Saliva plays a critical role in neutralizing acids, washing away food particles, and remineralizing enamel by delivering calcium and phosphate ions. Reduced saliva flow (due to medications, medical conditions, or radiation therapy) significantly increases the risk of demineralization and decay.
- Acid Reflux (GERD): Chronic acid reflux brings stomach acid into the mouth, which is highly erosive to enamel.
- Bruxism (Teeth Grinding): While not directly causing calcium deficiency, chronic grinding can wear down enamel, making it thinner and more susceptible to acid erosion and demineralization.
- Enamel Defects: Some individuals may have naturally weaker enamel due to genetic factors or developmental issues (e.g., amelogenesis imperfecta, fluorosis, or early childhood illness), making their teeth more prone to demineralization.
Signs and Symptoms of Calcium Deficiency in Teeth
Recognizing the early signs of mineral loss is crucial for intervention. These symptoms can range from subtle changes in appearance to discomfort and structural damage.
Early Signs
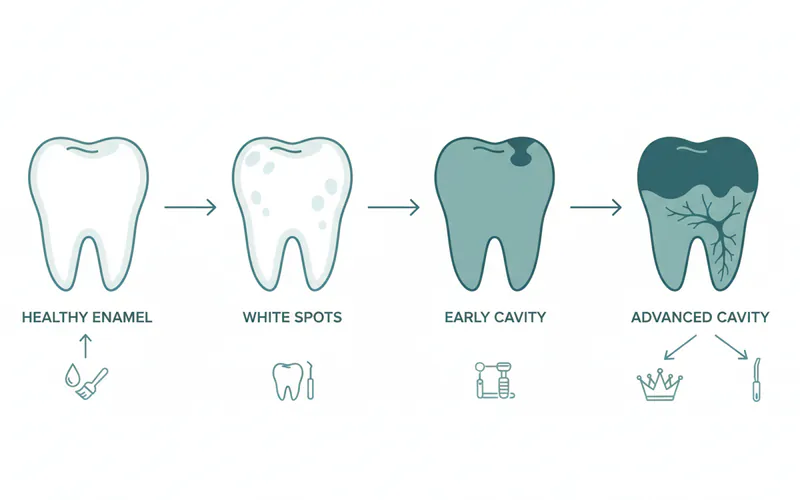
- White Spots on Teeth (Initial Caries Lesions): This is often the very first visible sign of demineralization. These chalky white or opaque areas indicate that minerals have been leached from the enamel surface, making it porous. These spots are typically duller than the surrounding healthy enamel and may appear near the gum line or on smooth surfaces.
- Increased Tooth Sensitivity: As enamel thins or becomes more porous due to mineral loss, the underlying dentin (which contains microscopic tubules leading to the nerve) becomes more exposed. This can lead to sensitivity to hot, cold, sweet, or acidic foods and drinks.
- Dull or Translucent Enamel: Healthy enamel has a certain luster. Demineralized enamel may appear duller, less vibrant, or even slightly translucent, especially at the biting edges.
Moderate to Advanced Signs
- Increased Cavity Formation (Dental Caries): Demineralized enamel is significantly weaker and more susceptible to bacterial acid attacks, leading to the rapid formation of cavities. You might notice more frequent cavities despite good oral hygiene.
- Tooth Discoloration: While white spots are an early sign, as demineralization progresses and decay sets in, the affected areas can turn yellow, brown, or even black.
- Rough or Pitted Enamel: Advanced demineralization can cause the enamel surface to feel rough or develop small pits and indentations, making it easier for plaque to adhere.
- Chipping or Cracking: Severely demineralized teeth are weaker and more brittle, making them prone to chipping, cracking, or breaking, especially when biting on hard foods.
- Gum Recession (Indirectly Related): While not a direct symptom of calcium deficiency, weakened tooth structure can sometimes exacerbate gum recession, as the supportive tissue may not be as robust, further exposing sensitive root surfaces.
Pro Tip: If you notice any persistent white spots or an increase in tooth sensitivity, schedule an appointment with your dentist promptly. Early intervention can often reverse demineralization before it becomes a cavity.
Treatment Options for Low Calcium Teeth
The approach to treating low calcium teeth depends heavily on the severity of the mineral loss, from early demineralization to advanced decay. Treatments focus on remineralization, halting decay, and restoring tooth structure.
1. Remineralization Therapies (For Early Demineralization)
These are ideal for addressing white spots and early enamel weakening before a cavity fully forms.
- Fluoride Varnish/Gel:
- Pros: Highly effective in strengthening enamel and reversing early demineralization. Fluoride incorporates into the enamel structure, making it more resistant to acid attacks. Applied professionally by a dentist or hygienist.
- Cons: Not effective for established cavities. Requires professional application.
- Cost: $25 - $75 per application, often covered by insurance for children, sometimes for adults with high risk.
- Prescription-Strength Fluoride Toothpaste/Rinses:
- Pros: Higher concentration of fluoride than over-the-counter products. Can be used daily at home.
- Cons: Requires a dentist's prescription. Not a standalone treatment for advanced issues.
- Cost: $10 - $30 per tube/bottle, usually not covered by insurance.
- CPP-ACP (Casein Phosphopeptide-Amorphous Calcium Phosphate) Products:
- Pros: Delivers high concentrations of calcium and phosphate ions to the tooth surface, helping to rebuild enamel. Found in products like MI Paste™.
- Cons: Derived from milk protein, so not suitable for individuals with milk allergies. Can be more expensive than fluoride products.
- Cost: $20 - $40 per tube.
- Silver Diamine Fluoride (SDF):
- Pros: Can halt the progression of existing cavities, particularly in children or uncooperative patients, and can prevent new lesions. Applied as a liquid directly to the tooth.
- Cons: Permanently stains decayed areas black, which can be cosmetically undesirable. Not a restorative solution.
- Cost: $25 - $75 per application, often covered by insurance.
2. Restorative Treatments (For Cavities and Structural Damage)
Once demineralization has progressed to a cavity, simple remineralization is no longer sufficient, and the lost tooth structure must be restored.
- Dental Fillings:
- Pros: Removes decayed portion of the tooth and restores its shape and function. Various materials available (composite resin, amalgam).
- Cons: Requires drilling away tooth structure.
- Cost: $150 - $400 for composite (white) fillings, $100 - $300 for amalgam (silver) fillings, largely depending on size and location. Insurance typically covers 50-80%.
- Dental Crowns:
- Pros: Covers the entire visible portion of a severely damaged or weakened tooth, protecting it from further decay and restoring strength.
- Cons: Requires significant removal of tooth structure. More expensive and time-consuming than fillings.
- Cost: $800 - $2,500 per crown (porcelain-fused-to-metal, all-ceramic, gold). Insurance usually covers 50%.
- Inlays/Onlays:
- Pros: Used for cavities too large for a filling but not severe enough for a crown. More durable than fillings.
- Cons: More expensive than fillings, requires two appointments.
- Cost: $600 - $1,200 per inlay/onlay. Insurance typically covers 50-80%.
- Root Canal Therapy and Crown:
- Pros: Saves a severely decayed or infected tooth when the pulp is involved, preventing extraction.
- Cons: Complex, multi-appointment procedure. High cost.
- Cost: $700 - $2,000 for the root canal, plus $800 - $2,500 for the subsequent crown. Insurance often covers a percentage.
- Tooth Extraction and Replacement:
- Pros: Last resort for unsalvageable teeth.
- Cons: Permanent tooth loss, requires replacement (bridge, implant) which is costly and invasive.
- Cost: $150 - $400 for simple extraction. $1,500 - $6,000+ for an implant with crown.
3. Dietary and Supplementation Approaches
- Calcium and Vitamin D-rich Diet: Increase intake of dairy products (milk, yogurt, cheese), fortified plant milks, leafy green vegetables (kale, spinach), fortified cereals, and fatty fish (salmon, tuna).
- Dietary Supplements: If diet is insufficient, supplements may be recommended by a doctor or dentist. Calcium carbonate and calcium citrate are common forms. Vitamin D supplements are often needed, especially in regions with limited sun exposure.
- Pros: Addresses underlying nutritional deficiencies.
- Cons: Supplements should be guided by a healthcare professional to avoid excessive intake, which can have adverse effects. Not a direct fix for existing cavities.
- Cost: $10 - $30 per bottle, usually not covered by insurance.
 `
`
Step-by-Step Treatment Process
Let's outline what you can expect during common treatments for calcium-deficient teeth, focusing on early demineralization and a typical filling procedure.
For Early Demineralization (e.g., Fluoride Varnish Application)
- Initial Examination and Diagnosis: Your dentist or hygienist will examine your teeth, possibly using an explorer or an intraoral camera, to identify any white spots or areas of demineralization. X-rays might be taken to rule out underlying cavities.
- Tooth Cleaning: The teeth are thoroughly cleaned to remove plaque and food debris, ensuring the fluoride can effectively contact the enamel surface.
- Application of Fluoride Varnish: A thin layer of fluoride varnish is painted onto the affected and at-risk tooth surfaces. The varnish sticks to the teeth and slowly releases fluoride over several hours.
- Drying Time: You'll be asked to keep your mouth open for a short period while the varnish dries.
- Post-Treatment Instructions: You'll typically be advised not to eat, drink, or brush your teeth for a specified time (e.g., 30 minutes to a few hours) to allow the fluoride to penetrate the enamel. You may also be advised to avoid sticky or crunchy foods for the rest of the day.
- Follow-Up: Depending on your risk level, repeat applications may be recommended every 3, 6, or 12 months.
For a Moderate Cavity (e.g., Composite Filling)
- Local Anesthesia: The dentist will numb the area around the affected tooth using a local anesthetic injection. This ensures you feel no pain during the procedure.
- Decay Removal: Using a dental drill, the dentist will carefully remove all decayed and demineralized tooth structure. The goal is to preserve as much healthy tooth as possible.
- Tooth Preparation: The remaining tooth structure is shaped to create a stable foundation for the filling material. For composite fillings, a mild acid gel may be applied to slightly etch the enamel, creating microscopic pores for better bonding.
- Bonding Agent Application: A bonding agent (adhesive) is applied to the prepared tooth surface. This liquid resin helps the composite filling material adhere strongly to the tooth.
- Composite Placement: The composite resin, which is a tooth-colored plastic mixture, is applied in layers. After each layer, a special blue light is used to harden (cure) the material. This layering and curing process ensures strength and proper shade matching.
- Shaping and Polishing: Once all the composite layers are placed and cured, the dentist will carefully shape the filling to match the natural contours of your tooth and ensure your bite is correct. The filling is then polished for a smooth, natural finish.
- Post-Treatment Instructions: You'll typically be able to eat and drink normally once the anesthesia wears off. You might experience some mild sensitivity for a few days, which is normal.
Cost and Insurance for Calcium Deficiency Treatments
The cost of treating low calcium teeth in the US can vary significantly based on the severity of the condition, the type of treatment, the dental practice's location, and whether you have dental insurance.
Average US Price Ranges (Without Insurance)
| Treatment Type | Typical US Cost Range (Without Insurance) |
|---|---|
| Fluoride Varnish Application (Per visit) | $25 - $75 |
| Prescription Fluoride Toothpaste/Rinse | $10 - $30 |
| CPP-ACP Products (e.g., MI Paste) | $20 - $40 |
| Silver Diamine Fluoride (SDF) | $25 - $75 |
| Dental Filling (Amalgam - 1 surface) | $100 - $250 |
| Dental Filling (Composite - 1 surface) | $150 - $400 |
| Dental Filling (Composite - 3+ surfaces) | $300 - $600+ |
| Inlay/Onlay (Composite/Ceramic) | $600 - $1,200 |
| Dental Crown (Ceramic, PFM) | $800 - $2,500 |
| Root Canal Therapy (Molar) | $900 - $2,000 |
| Tooth Extraction (Simple) | $150 - $400 |
Regional Cost Variations: Costs tend to be higher in metropolitan areas and on the coasts (e.g., New York, California) and lower in rural areas or the Midwest.
Dental Insurance Coverage
Most dental insurance plans categorize treatments into preventive, basic, and major services, with varying coverage percentages:
- Preventive Services (e.g., fluoride varnish, regular cleanings, exams): Often covered at 80-100%, especially for children. Many plans offer 1-2 fluoride treatments per year.
- Basic Restorative Services (e.g., fillings, SDF): Typically covered at 50-80%. The specific percentage often depends on the type of filling (amalgam vs. composite) and the number of surfaces. Some plans may cover composite fillings at the amalgam rate, leaving you to pay the difference.
- Major Restorative Services (e.g., crowns, inlays/onlays, root canals): Usually covered at 20-50%, with many plans covering around 50%. There is often an annual maximum benefit ($1,000 - $2,000 is common) that once reached, you are responsible for 100% of costs.

Pro Tip: Always check with your specific dental insurance provider beforehand to understand your exact coverage, deductibles, co-pays, and annual maximums. Ask your dental office for a pre-treatment estimate to avoid financial surprises.
Recovery and Aftercare
Proper aftercare is crucial to ensure the success of any treatment for low calcium teeth and to prevent future issues.
After Remineralization Therapies (e.g., Fluoride Varnish)
- Avoid eating/drinking for a short period: Typically 30 minutes to a few hours, as directed by your dentist, to allow the fluoride to penetrate.
- Avoid abrasive foods: For the rest of the day, stick to soft foods and avoid very hot or cold items.
- Delay brushing/flossing: Your dentist might recommend waiting 4-6 hours or even until the next morning before brushing to maximize fluoride absorption.
- Maintain oral hygiene: Once the initial waiting period is over, resume your excellent oral hygiene routine.
After Dental Fillings
- Anesthesia wears off: Expect the numbness to last for a few hours. Be careful not to bite your cheek, tongue, or lips during this time.
- Sensitivity: It's common to experience mild sensitivity to hot, cold, or pressure for a few days to a few weeks after a filling. This usually subsides. If sensitivity persists or worsens, contact your dentist.
- Chewing: Avoid chewing on the newly filled tooth until the anesthetic has completely worn off. If it's an amalgam filling, your dentist might advise avoiding heavy chewing for 24 hours to allow it to fully set.
- Bite Adjustment: If your bite feels "high" or uneven after the filling, contact your dentist for an adjustment. A high spot can cause pain and even fracture the filling or tooth.
- Oral hygiene: Resume normal brushing and flossing immediately.
General Aftercare & Prevention
- Excellent Oral Hygiene:
- Brush twice daily for two minutes with a fluoride toothpaste.
- Floss daily to remove plaque and food particles from between teeth.
- Consider an antimicrobial or fluoride mouthwash if recommended by your dentist.
- Dietary Modifications:
- Reduce intake of sugary and acidic foods/drinks.
- Choose calcium and Vitamin D-rich foods.
- Limit snacking between meals to reduce acid exposure.
- Hydration: Drink plenty of water throughout the day, especially if you suffer from dry mouth, to help rinse away acids and food debris.
- Regular Dental Check-ups and Cleanings: Schedule visits every six months (or more frequently if recommended) for professional cleaning, examination, and early detection of demineralization or decay.
- Address underlying medical conditions: Work with your physician and dentist to manage conditions like GERD, malabsorption disorders, or dry mouth that contribute to dental problems.
Prevention of Calcium Deficiency in Teeth
Preventing low calcium teeth is a lifelong commitment to good oral health and systemic well-being. Focusing on these key areas can significantly reduce your risk.
1. Optimal Dietary Intake
- Consume Calcium-Rich Foods: Ensure your diet includes adequate sources of calcium.
- Dairy Products: Milk, yogurt, cheese (low-fat options are good).
- Fortified Plant Milks: Almond, soy, oat milk fortified with calcium and Vitamin D.
- Leafy Green Vegetables: Kale, spinach, collard greens, turnip greens.
- Certain Fish: Canned sardines and salmon (with bones) are excellent sources.
- Fortified Foods: Some orange juices, cereals, and breads are fortified.
- Adequate Vitamin D: Essential for calcium absorption.
- Sunlight Exposure: 10-15 minutes of direct sunlight a few times a week (with caution for skin cancer risk).
- Fatty Fish: Salmon, mackerel, tuna.
- Fortified Foods: Milk, cereal, orange juice.
- Supplements: Consult with your doctor about Vitamin D supplements, especially if you have limited sun exposure or a diagnosed deficiency.
- Limit Acidic and Sugary Foods/Drinks: These directly contribute to demineralization and cavity formation. Rinse your mouth with water after consuming them if you can't brush immediately.
- Balanced Nutrition: A diet rich in fruits, vegetables, and whole grains provides essential vitamins and minerals for overall health, including oral health.
2. Excellent Oral Hygiene Practices
- Brush Twice Daily with Fluoride Toothpaste: Brush for two minutes each time, covering all surfaces of your teeth. Fluoride strengthens enamel and helps remineralize early lesions.
- ADA Seal of Acceptance: Look for toothpastes with the ADA Seal of Acceptance, ensuring they meet efficacy and safety standards.
- Floss Daily: Flossing removes plaque and food particles from between teeth and under the gum line, areas your toothbrush can't reach, preventing acid buildup.
- Consider a Fluoride Mouthwash: If you're at high risk for cavities or demineralization, your dentist might recommend a daily over-the-counter or prescription fluoride rinse.
- Electric Toothbrush: Many find electric toothbrushes more effective at removing plaque.
3. Regular Dental Check-ups and Professional Care
- Schedule Bi-Annual Visits: Visit your dentist every six months (or as recommended) for professional cleanings and comprehensive examinations. This allows for early detection of demineralization, cavities, or other issues.
- Professional Fluoride Treatments: Your dentist or hygienist can apply high-concentration fluoride varnishes, gels, or foams during your routine visits, especially if you are considered high risk.
- Dental Sealants: For children and sometimes adults, sealants can be applied to the chewing surfaces of molars to protect them from decay.
4. Lifestyle and Medical Management
- Manage Dry Mouth: If you suffer from dry mouth, discuss solutions with your dentist. These can include salivary stimulants, artificial saliva, or adjusting medications. Xylitol-containing gums and lozenges can also help stimulate saliva flow.
- Address Acid Reflux (GERD): Work with your physician to manage GERD, as stomach acid can severely erode enamel.
- Avoid Smoking and Excessive Alcohol: Both can negatively impact oral health, contributing to dry mouth and increasing the risk of gum disease and other issues.
- Treat Underlying Health Conditions: If you have malabsorption issues or other systemic conditions affecting calcium levels, ensure they are properly managed by a medical professional.
By integrating these preventive strategies into your daily routine, you can significantly bolster your teeth against mineral loss and maintain a strong, healthy smile.
Risks and Complications of Untreated Low Calcium Teeth
Ignoring the signs of calcium deficiency in teeth or delaying treatment can lead to a cascade of worsening dental and even systemic health problems.
Dental Complications
- Accelerated Cavity Formation (Dental Caries): The most direct consequence. Weakened enamel provides less protection against bacterial acids, leading to more frequent, larger, and deeper cavities.
- Tooth Sensitivity: Persistent and worsening sensitivity to hot, cold, sweet, and acidic stimuli can significantly impact daily comfort and enjoyment of food.
- Enamel Erosion and Wear: Beyond demineralization, continuous acid attacks will physically erode the enamel, making teeth appear smaller, rougher, or more translucent.
- Tooth Fractures and Chipping: Demineralized teeth are brittle and more prone to breaking, especially when biting on hard foods or during accidental trauma. This can lead to jagged edges that cut soft tissues or expose the inner tooth.
- Pulpitis and Tooth Abscesses: If a cavity progresses deep enough, it can reach the pulp (the tooth's nerve and blood vessels), causing inflammation (pulpitis) and potentially infection (abscess). This is extremely painful and can lead to swelling, fever, and even spread of infection.
- Tooth Loss: Untreated severe decay or fractures can render a tooth unsalvageable, necessitating extraction. This impacts chewing ability, speech, and can lead to shifting of adjacent teeth, affecting overall bite alignment.
- Periodontal Disease Exacerbation: While not a direct cause, weakened teeth can complicate the management of gum disease, and systemic calcium deficiency can impact jawbone density, further compromising tooth support.
- Increased Dental Treatment Needs: Delaying treatment almost always leads to more complex, invasive, and expensive procedures later on (e.g., fillings becoming crowns, crowns becoming root canals, or extractions).
Systemic Complications (Indirectly Related)
While "calcium deficiency in teeth" primarily refers to local enamel issues, a systemic calcium deficiency can have broader health impacts that indirectly affect oral health:
- Osteoporosis: Long-term calcium deficiency significantly increases the risk of osteoporosis, a condition characterized by weak, brittle bones. This can include the jawbone, potentially leading to tooth mobility or difficulties with dental implants.
- Nutritional Deficiencies: Dental issues can make it painful or difficult to eat certain foods, potentially leading to further nutritional deficiencies.
- Impact on Overall Health: Chronic oral infections (like abscesses) can have systemic effects, potentially contributing to cardiovascular issues, diabetes complications, and adverse pregnancy outcomes.
Pro Tip: Do not wait until you are in pain to see a dentist. Regular check-ups allow for detection and treatment of demineralization and early cavities, preventing these more severe complications.
Children / Pediatric Considerations
Calcium is profoundly important during childhood and adolescence because this is the critical period for tooth development and the formation of strong bones. Low calcium teeth in children can have lasting impacts.
Fetal and Infant Development
- Maternal Calcium Intake: A mother's calcium intake during pregnancy directly influences the development of her baby's teeth and bones. Insufficient calcium can lead to enamel hypoplasia (developmental defects in enamel) in the primary (baby) teeth.
- Early Childhood Nutrition: From infancy, adequate calcium (from breast milk, formula, and then calcium-rich foods) is crucial for the proper mineralization of primary teeth and the formation of permanent teeth developing within the jawbones.
Risks for Children
- Enamel Hypoplasia: This condition results in thinner, weaker, or rough enamel surfaces, making teeth highly susceptible to decay, even with seemingly good oral hygiene. It often manifests as pits, grooves, or discolored patches on the enamel.
- Early Childhood Caries (ECC): Often called "baby bottle tooth decay," ECC is severe decay in infants and toddlers, often linked to prolonged exposure to sugary liquids (milk, juice, formula) and insufficient fluoride. While not solely a calcium deficiency issue, weakened enamel due to poor nutrition makes teeth more vulnerable.
- Increased Cavity Risk: Children with weaker enamel or those with diets low in calcium and high in sugar are at a significantly higher risk for developing cavities, which can lead to pain, infection, difficulty eating, and speech problems.
- Impact on Permanent Teeth: Damage to primary teeth can sometimes affect the proper eruption and alignment of the underlying permanent teeth.
Prevention and Treatment for Children
- Balanced Diet: Ensure children consume a diet rich in calcium, Vitamin D, and other essential nutrients. Encourage milk, yogurt, cheese, fortified cereals, and leafy greens.
- Limit Sugary Drinks and Snacks: Reduce consumption of sodas, juices, and candies. Encourage water as the primary beverage.
- Excellent Oral Hygiene from an Early Age:
- Wipe infant's gums after feeding.
- Brush teeth twice daily with a fluoride toothpaste (a "smear" for children under 3, a "pea-size" amount for ages 3-6).
- Floss once teeth touch.
- Regular Pediatric Dental Visits: Start dental visits by the first birthday or when the first tooth erupts. Pediatric dentists are experts in managing children's oral health and can apply preventive treatments.
- Professional Fluoride Treatments: Pediatric dentists frequently apply fluoride varnish to children's teeth during routine check-ups to strengthen enamel and prevent cavities.
- Dental Sealants: Applied to the chewing surfaces of permanent molars as soon as they erupt to protect them from decay.
- Silver Diamine Fluoride (SDF): Can be a valuable tool for arresting existing cavities in primary teeth, especially for very young or uncooperative children.
Pro Tip: Parents should be proactive in managing their child's diet and oral hygiene. Early habits set the stage for a lifetime of dental health. If you notice any white spots or brown areas on your child's teeth, consult a pediatric dentist immediately.
Cost Breakdown
Understanding the financial aspect of treating low calcium teeth is important for planning. Costs vary widely based on the complexity and type of treatment.
Average US Costs (Without Insurance)
| Service Category | Example Procedures | Low Range | Mid Range | High Range |
|---|---|---|---|---|
| Preventive Care | Dental Exam, X-rays, Cleaning | $100 | $200 | $350 |
| Fluoride Varnish/Treatment | $25 | $50 | $75 | |
| Early Intervention | Silver Diamine Fluoride (SDF) | $25 | $50 | $75 |
| Prescription Fluoride Toothpaste/Rinse | $10 | $20 | $30 | |
| CPP-ACP Products (e.g., MI Paste) | $20 | $30 | $40 | |
| Basic Restorations | Amalgam Filling (1 surface) | $100 | $150 | $250 |
| Composite Filling (1 surface) | $150 | $250 | $400 | |
| Composite Filling (3+ surfaces) | $300 | $450 | $600+ | |
| Major Restorations | Inlay/Onlay (Porcelain) | $600 | $900 | $1,200 |
| Dental Crown (Porcelain-fused-to-metal) | $800 | $1,500 | $2,500 | |
| All-Ceramic/Zirconia Crown | $1,000 | $1,800 | $3,000+ | |
| Endodontic & Surgical | Root Canal Therapy (Front tooth) | $700 | $900 | $1,200 |
| Root Canal Therapy (Molar) | $900 | $1,500 | $2,000 | |
| Simple Tooth Extraction | $150 | $250 | $400 | |
| Surgical Tooth Extraction | $250 | $450 | $800+ | |
| Tooth Replacement | Dental Bridge (3 units) | $2,000 | $3,500 | $5,000+ |
| Dental Implant (Post only) | $1,500 | $2,500 | $3,000+ | |
| Dental Implant (Post, Abutment, Crown) | $3,000 | $4,500 | $6,000+ |

With Insurance
Dental insurance can significantly reduce your out-of-pocket costs.
- Preventive: Often 80-100% covered.
- Basic: Typically 50-80% covered.
- Major: Usually 20-50% covered.
Important Note: Most insurance plans have a deductible (an amount you pay before coverage begins) and an annual maximum benefit (the maximum amount your insurance will pay in a year, commonly $1,000 - $2,000). Once you reach your annual maximum, you are responsible for 100% of additional costs.
Payment Plans and Financing Options
Many dental practices understand the financial burden of extensive treatment and offer various payment solutions:
- In-house Payment Plans: Some offices offer direct payment plans, allowing you to pay for services over several months, often without interest.
- Third-Party Financing: Companies like CareCredit or LendingClub provide healthcare credit cards or loans that can cover dental expenses. These often offer interest-free periods if paid in full within a certain timeframe.
- Dental Savings Plans (Discount Plans): These are not insurance but offer a discount on services from participating dentists for an annual fee. Discounts typically range from 10-60%.
- Flexible Spending Accounts (FSAs) / Health Savings Accounts (HSAs): If you have these through your employer, you can use pre-tax dollars to pay for qualified dental expenses.
Cost-Saving Tips
- Preventive Care is Key: Regular cleanings and fluoride treatments are far less expensive than fillings or crowns. Prevention saves significant money in the long run.
- Early Detection: Addressing demineralization or small cavities early prevents them from becoming larger, more complex, and costlier problems.
- Shop Around (Carefully): Get multiple quotes for major procedures, but don't base your decision solely on price. Quality of care, dentist's experience, and patient reviews are equally important.
- Utilize Dental School Clinics: Dental schools often offer services at a reduced cost, as procedures are performed by students under the supervision of experienced faculty.
- Negotiate: For extensive treatments without insurance, some practices may be willing to offer a discount for upfront payment.
Frequently Asked Questions
What does calcium deficiency in teeth look like?
Calcium deficiency in teeth often begins as white spots on the enamel, which appear dull, chalky, or opaque compared to the surrounding tooth structure. As it progresses, these areas can become sensitive, lead to yellow, brown, or black discolorations from cavities, and in advanced stages, result in visible holes, chipping, or fractures in the tooth.
Can low calcium cause tooth sensitivity?
Yes, absolutely. When enamel loses calcium and other minerals, it becomes thinner and more porous. This exposes the underlying dentin, which contains microscopic tubules leading to the tooth's nerve. This exposure makes the tooth highly susceptible to sensitivity to hot, cold, sweet, or acidic stimuli.
Can teeth remineralize themselves?
Yes, teeth have a natural ability to remineralize, but only in the early stages of demineralization. Saliva contains calcium and phosphate ions that can deposit back into weakened enamel. Fluoride significantly enhances this process by making the enamel more resistant to acid. However, once a cavity has physically formed (a hole in the tooth), it cannot remineralize and requires professional restoration like a filling.
Is "calcium deposits in teeth" the same as calcium deficiency?
No, these terms refer to entirely different conditions. "Calcium deposits in teeth" typically refers to dental calculus (tartar), which is hardened plaque formed by minerals from saliva on the tooth surface. This is a sign of poor oral hygiene and is distinct from calcium deficiency in teeth, which involves the loss of minerals from the tooth structure, weakening the enamel.
How long does it take to fix calcium deficiency in teeth?
The timeline depends on the severity. Early demineralization (white spots) can show improvement within weeks to months with consistent fluoride applications, prescription toothpastes, and dietary changes. However, established cavities require immediate restorative treatment (like fillings), which typically takes one appointment (around 30-90 minutes). Severe cases requiring crowns or root canals can involve multiple appointments over several weeks.
How much does it cost to treat low calcium teeth?
Costs vary significantly based on the treatment. Fluoride applications can range from $25-$75. A basic filling might cost $100-$400, while a crown can be $800-$2,500. Root canal therapy can range from $700-$2,000, with an additional cost for the crown. These are without insurance, which typically covers a percentage of basic and major procedures.
Are calcium supplements good for teeth?
Calcium supplements can be beneficial if you have a diagnosed systemic calcium deficiency or your dietary intake is consistently inadequate, especially for overall bone health. However, supplements alone won't directly reverse existing enamel demineralization or cavities. For direct tooth health, topical fluoride and a balanced diet with good oral hygiene are more critical. Always consult a doctor or dentist before starting any supplements.
What foods are best for strengthening teeth with low calcium?
Foods rich in calcium include dairy products (milk, yogurt, cheese), fortified plant milks, leafy green vegetables (kale, spinach, collard greens), fortified cereals, and specific fish (canned salmon with bones). Foods rich in Vitamin D (fatty fish, fortified milk) are also crucial for calcium absorption. Reducing acidic and sugary foods is equally important to prevent mineral loss.
Can calcium deficiency lead to tooth loss?
Indirectly, yes. If calcium deficiency leads to significant enamel demineralization and widespread, untreated cavities, these teeth can become severely compromised, leading to fractures, infections, and eventually necessitating extraction. Systemic calcium deficiency can also impact jawbone density, which might indirectly affect tooth stability in the long term.
Can enamel regrow if it's demineralized?
Enamel cannot regrow in the same way bone tissue can. However, early demineralization, where minerals have only begun to leach from the surface, can be reversed or "remineralized." This means that calcium, phosphate, and fluoride ions can redeposit into the weakened enamel, strengthening it and making it more resistant to further acid attacks. This process is most effective with topical fluoride and proper oral hygiene.
When to See a Dentist
Recognizing when to seek professional dental care is critical for managing calcium deficiency in teeth and protecting your oral health.
Clear Warning Signs That Need Immediate Attention
- Persistent Toothache: Any severe, throbbing, or continuous tooth pain that doesn't subside, especially if it worsens with hot or cold, indicates a likely deep cavity or infection.
- Swelling: Swelling in your gums, face, or jaw accompanied by pain or fever could signify a serious infection (abscess) that requires urgent treatment.
- Fractured or Broken Tooth: If a tooth chips, cracks, or breaks, exposing underlying layers, it needs prompt attention to prevent infection and further damage.
- Pus or Discharge: Any visible pus around a tooth or in the gums points to an active infection.
- Difficulty Eating or Chewing: If pain or sensitivity prevents you from eating properly, it's a clear sign you need dental intervention.
Red Flags vs. Routine Care Guidance
- Red Flags (Schedule an Appointment Soon):
- New White Spots: If you notice new white, chalky areas on your teeth, particularly near the gum line or on smooth surfaces, these are early signs of demineralization. While not an emergency, addressing them quickly can prevent cavities.
- Increased or New Sensitivity: If your teeth suddenly become more sensitive to hot, cold, or sweets, it could indicate enamel erosion or early decay.
- Visible Cavities: Any dark spots or small holes in your teeth that you can see or feel with your tongue should be checked.
- Rough Spots or Changes in Tooth Texture: If your enamel feels rougher or pitted, it might indicate mineral loss.
- Persistent Bad Breath: While many causes, it can sometimes be a sign of hidden decay or infection.
- Routine Care (Regular Appointments):
- Even if you have no symptoms, schedule regular dental check-ups and cleanings every six months. This is crucial for early detection of demineralization and cavities before they become painful or severe. Your dentist can also apply preventive fluoride treatments.
By being proactive and attentive to changes in your teeth, you can prevent minor issues from escalating into major problems, maintaining a healthy and strong smile.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
What Are Calcium Deposits on Teeth
Are you one of the millions of Americans who notices a stubborn, yellowish buildup on your teeth despite regular brushing? You're likely experiencing what many refer to as "calcium deposits on teeth." This common dental concern, medically known as dental calculus or tartar, affects a vast ma
February 23, 2026
Calcium Good for Teeth: Complete Guide
More than 99% of your body's calcium resides in your bones and teeth, making it an undeniable cornerstone of skeletal and oral health. But did you know that an estimated 42% of American adults don't get enough calcium from their diet? This staggering statistic underscores a critical question
February 23, 2026
What Do Bulimia Teeth Look Like
"Bulimia teeth" refers to the specific and often severe damage that the self-induced vomiting characteristic of bulimia nervosa inflicts on a person's oral health. It's a critical issue, affecting approximately 1.5% of women and 0.5% of men in the US at some point in their lives, with many more
February 23, 2026

Erosion in Teeth: Complete Guide
Erosion in Teeth: Complete Guide
February 23, 2026