Erosion Tooth: Complete Guide
Key Takeaways
- Tooth enamel, the hardest substance in the human body, is remarkably resilient but not invincible. It faces daily assaults, and one of the most insidious threats is dental erosion. If you've ever felt a sudden sensitivity to cold or noticed your teeth looking a bit more translucent, you might be exp
Tooth enamel, the hardest substance in the human body, is remarkably resilient but not invincible. It faces daily assaults, and one of the most insidious threats is dental erosion. If you've ever felt a sudden sensitivity to cold or noticed your teeth looking a bit more translucent, you might be experiencing the effects of erosion tooth, a widespread issue that silently diminishes the protective layers of your teeth.
According to the American Dental Association (ADA), tooth erosion affects a significant portion of the US population, with studies suggesting that anywhere from 20% to 45% of adults show signs of moderate to severe enamel erosion. This condition, often caused by frequent exposure to acids, gradually wears away the enamel, leading to a host of dental problems ranging from heightened sensitivity to eventual tooth loss if left untreated. Understanding teeth acid erosion is crucial because, unlike cavities, which are caused by bacteria, erosion is a chemical process that can impact anyone, regardless of their brushing habits.
This comprehensive guide from SmilePedia.net will demystify dental erosion, exploring its various forms, the underlying causes, unmistakable signs, and the full spectrum of available treatment options. We'll also delve into crucial preventive strategies, including the vital role of nutrition and how maintaining adequate vitamin D teeth health can fortify your defenses. By the end, you'll have a complete roadmap to protect your smile from the silent threat of erosion.
Key Takeaways:
- Definition: Dental erosion is the irreversible loss of tooth hard tissue due to chemical dissolution by acids, not involving bacteria.
- Primary Causes: Frequent consumption of acidic foods/drinks (extrinsic) and medical conditions like acid reflux or bulimia (intrinsic) are the leading culprits.
- Early Signs: Increased tooth sensitivity to hot, cold, or sweet, and a yellowish discoloration (due to exposed dentin) are common early indicators.
- Treatment Options: Range from conservative measures like fluoride varnishes and bonding (starting around $100-$400 per tooth for bonding) to restorative solutions like fillings, crowns, or veneers (costing $250-$2,500+ per tooth).
- Prevention is Key: Dietary modifications, proper oral hygiene habits (especially after acid exposure), and addressing underlying medical conditions can significantly slow or halt progression.
- Diagnosis & Timeline: Diagnosis typically involves a dental exam and diet/medical history review. Treatment timelines vary from a single visit for minor bonding to multiple appointments over several weeks for extensive restorations.
- Vitamin D & Oral Health: Adequate Vitamin D intake is crucial for calcium absorption and strong enamel, playing a supportive role in preventing erosion by enhancing tooth resilience.
What Is Dental Erosion? An Overview
Dental erosion, also known as erosive tooth wear, is the irreversible loss of tooth structure due to chemical dissolution by acids, without the involvement of bacterial action. This critical distinction sets it apart from dental caries (cavities), which are caused by acids produced by bacteria metabolizing sugars. In erosion, acids directly attack the mineral content of the tooth enamel and underlying dentin, dissolving the hydroxyapatite crystals that give teeth their hardness and strength.

The outermost layer of your teeth, the enamel, is incredibly strong but highly susceptible to acid. Once enamel is lost, it cannot regenerate. Beneath the enamel lies the dentin, a softer, yellowish tissue that is even more vulnerable to acid attack. As erosion progresses, it thins the enamel, exposes the dentin, and can eventually lead to significant structural damage, affecting both the aesthetics and function of your smile.
Think of it like this: if you pour a strong acid onto a piece of chalk (which is also primarily calcium carbonate), it will bubble and dissolve. Your teeth are made of a similar, albeit much harder, mineral composition. When acids come into contact with your teeth for extended periods or with high frequency, they begin to "melt" away the protective layers. This process is often slow and insidious, making it difficult for individuals to notice until significant damage has occurred.
Types of Teeth Acid Erosion
Dental erosion can be broadly categorized based on the source of the acid attacking the teeth:
Extrinsic Erosion
This type of erosion occurs when acids originate from outside the body. These are the most common culprits and are primarily linked to dietary habits and environmental factors.
- Dietary Acids: This is the most prevalent cause of extrinsic erosion. Foods and beverages with a low pH (high acidity) can directly demineralize enamel.
- Soft Drinks: Colas, lemon-lime sodas, and even diet sodas are highly acidic, often with pH levels below 3.0. Frequent consumption, especially sipping over long periods, bathes teeth in acid.
- Fruit Juices: Citrus juices (orange, grapefruit, lemon) and even apple juice are acidic. While natural, their high acid content can be damaging, especially without proper moderation. For example, orange juice typically has a pH of 3.3-4.2.
- Citrus Fruits: Direct consumption of lemons, limes, or grapefruits can lead to localized erosion.
- Sports Drinks: Many sports drinks, designed for electrolyte replenishment, contain citric acid and other acids to improve flavor, often with pH levels similar to soft drinks.
- Vinegars: Apple cider vinegar, balsamic vinegar, and other vinegars are highly acidic and can cause significant erosion if consumed frequently or swished.
- Sour Candies: These candies are formulated with high levels of acids (citric, malic, tartaric) to create their distinctive sour taste, directly attacking enamel.
- Environmental Factors:
- Occupational Exposure: Individuals working in industries involving acid fumes (e.g., battery factories, electroplating, certain chemical plants) or those frequently exposed to highly chlorinated swimming pools (where chlorine can lower pH) may experience erosion.
- Medications: Certain medications, particularly some vitamin C chewable tablets, aspirin (chewed), and some iron preparations, can be acidic.
Intrinsic Erosion
This type of erosion is caused by acids originating from within the body, primarily from stomach acids.
- Gastroesophageal Reflux Disease (GERD): Often referred to as acid reflux, GERD is a chronic condition where stomach acid flows back up into the esophagus and can reach the mouth. The pH of stomach acid is extremely low (around 1.5-3.5), making it highly destructive to tooth enamel. Patients with GERD often show erosion patterns on the lingual (tongue-side) surfaces of their upper teeth and occlusal (biting) surfaces.
- Bulimia Nervosa and Anorexia Nervosa: These eating disorders involve frequent self-induced vomiting, which exposes teeth to potent stomach acids. The pattern of erosion is typically severe on the lingual surfaces of the upper front teeth.
- Chronic Alcoholism: Frequent vomiting associated with excessive alcohol consumption can also lead to intrinsic erosion.
- Hiatal Hernia: This condition can contribute to GERD, thereby increasing the risk of intrinsic erosion.
- Pregnancy-Related Nausea and Vomiting: While temporary, severe and prolonged morning sickness can cause enamel erosion.
Understanding the type of erosion is crucial for effective diagnosis and treatment planning, as addressing the underlying cause is paramount to preventing further damage.
Causes: Why Your Teeth Are Eroding
The fundamental cause of teeth acid erosion is exposure to acids. However, it's the frequency, duration, and method of exposure, combined with individual factors, that determine the severity.
Dietary Habits
As discussed, acidic foods and drinks are major contributors. Factors that worsen their effect include:
- Frequency: Sipping on a soft drink throughout the day is far more damaging than consuming it quickly with a meal. Each exposure triggers demineralization.
- Duration: Holding acidic liquids in the mouth or swishing them around prolongs acid contact.
- Method of Consumption: Chewing ice or hard foods immediately after consuming acidic items can cause further mechanical wear on softened enamel. Using a straw can help reduce direct contact with front teeth.
- Saliva Flow: Saliva acts as a natural buffer, neutralizing acids and helping to remineralize enamel. Conditions that reduce saliva flow, such as dry mouth (xerostomia) caused by certain medications (e.g., antihistamines, antidepressants), Sjögren's syndrome, or radiation therapy, significantly increase erosion risk.
Medical Conditions
Beyond GERD and eating disorders, other health issues can contribute:
- Gastric Conditions: Any condition causing frequent vomiting or reflux, even if not diagnosed as GERD, can contribute to intrinsic erosion.
- Drug Use: Methamphetamine ("meth mouth") causes severe dry mouth and often includes consumption of sugary, acidic drinks to quench thirst, leading to rapid, widespread erosion and decay.
- Acidic Medications: As mentioned, certain chewable medications can locally erode enamel.
Lifestyle Factors
- Professional Exposure: Occupations involving acid fumes (e.g., battery makers, galvanizers) or competitive swimmers exposed to highly chlorinated water can lead to erosion.
- Aggressive Brushing: While not a direct cause of erosion, brushing vigorously immediately after consuming acidic foods or experiencing reflux can mechanically abrade already softened enamel, accelerating wear. It's often recommended to wait at least 30-60 minutes after acid exposure before brushing to allow saliva to neutralize acids and begin remineralization.
Genetic Predisposition
While not a primary cause, some individuals may have thinner enamel or a genetic predisposition to weaker enamel, making them more susceptible to acid erosion. However, lifestyle and medical factors are overwhelmingly more significant.
Signs and Symptoms: What to Look For
Recognizing the signs of erosion tooth early is crucial, as early intervention can prevent more extensive and costly damage. The symptoms often develop gradually, making them easy to overlook initially.
Common Signs
- Tooth Sensitivity: This is often the first noticeable symptom. You might experience sharp, fleeting pain when consuming hot, cold, sweet, or acidic foods and drinks. As enamel wears away, the underlying dentin, which contains microscopic tubules leading to the nerve, becomes exposed, leading to sensitivity.
- Discoloration: Enamel is translucent, and as it thins due to erosion, the yellowish dentin beneath becomes more visible, making your teeth appear darker or more yellow.
- Rounded or Smooth Edges: The sharp, distinct edges of your teeth (especially incisal edges of front teeth) may become rounded, smoothed, or appear "worn down."
- Transparent Appearance: The biting edges of your front teeth may look translucent or "glassy" as enamel thins.
- Cupping: Small indentations or "cups" may form on the chewing surfaces of your teeth, often surrounded by raised enamel. This is a classic sign of advanced erosion.
- Fillings Appearing Raised: If you have silver (amalgam) fillings, they might appear to sit "on top" of the tooth structure, as the surrounding enamel has eroded away.
- Cracks and Chips: Eroded enamel is weaker and more prone to chipping or cracking, especially at the edges of teeth.
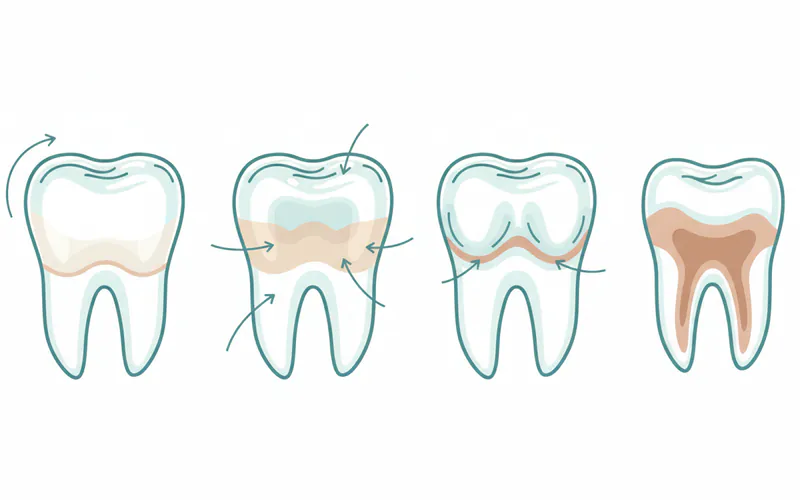
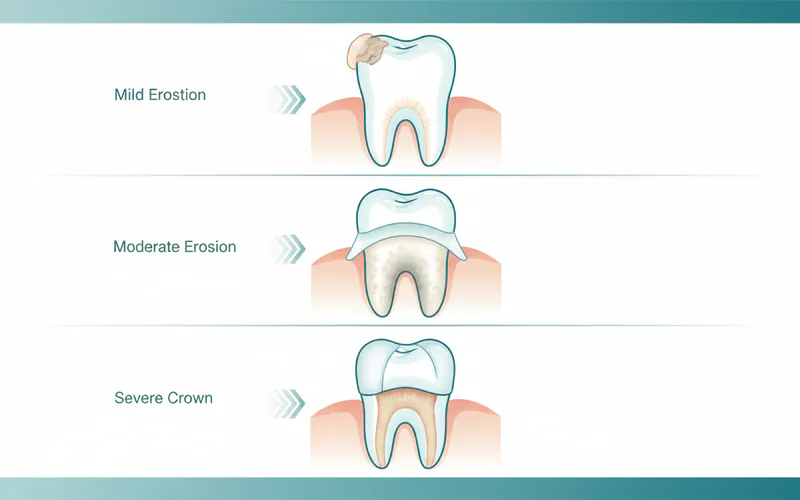
Severity Scale of Erosion
Dentists often use indices like the Basic Erosive Wear Examination (BEWE) to classify the severity of erosion:
- Score 0: No erosive tooth wear.
- Score 1: Initial loss of enamel surface texture.
- Score 2: Distinct defect, hard tissue loss less than half of the surface.
- Score 3: Hard tissue loss more than half of the surface or pulp exposure.
Regular dental check-ups are vital for early detection, as a dentist can often spot subtle signs before you notice significant symptoms.
Treatment Options for Erosion Tooth
The approach to treating erosion tooth depends on the severity of the damage, the underlying cause, and the patient's individual needs and preferences. Treatment aims to halt progression, alleviate symptoms, and restore tooth structure and aesthetics.
1. Conservative Management
For mild to moderate erosion, especially in its early stages, conservative approaches focus on prevention and strengthening remaining enamel.
- Fluoride Treatments:
- Professional Fluoride Varnishes/Gels: Applied by your dentist, these highly concentrated fluoride treatments can significantly strengthen enamel and reduce sensitivity. They work by enhancing remineralization and making the enamel more resistant to acid attacks.
- Prescription Fluoride Toothpastes/Rinses: Dentists may prescribe toothpastes with higher fluoride concentrations (e.g., 5000 ppm) than over-the-counter options, or fluoride rinses for daily use at home.
- Pros: Non-invasive, relatively inexpensive (professional application typically $25-$75 per treatment, often covered by insurance for children, sometimes for adults), effective in early stages.
- Cons: Not a restorative solution; won't rebuild lost tooth structure. Requires ongoing application.
- Dental Bonding (Composite Resin):
- For minor to moderate enamel loss, especially on front teeth or at the gumline, composite resin (tooth-colored plastic material) can be bonded directly to the tooth surface. This can restore shape, protect exposed dentin, and improve aesthetics.
- Pros: Minimally invasive, relatively inexpensive ($100-$400 per tooth depending on size and location), quick (often one visit), good aesthetic match.
- Cons: Less durable than porcelain, can stain over time, may need replacement every 5-10 years.
- Dental Sealants:
- While primarily used for cavity prevention in molars, sealants can sometimes be used on eroded biting surfaces to protect them from further acid attack and wear.
- Pros: Protective barrier, non-invasive.
- Cons: Limited applicability for widespread erosion, primarily for pits and fissures.
- Remineralizing Agents:
- Products containing calcium and phosphate (like casein phosphopeptide-amorphous calcium phosphate, CPP-ACP) can help rebuild mineral content in weakened enamel. These are often available in pastes or chewing gums.
- Pros: Supports natural repair, non-invasive.
- Cons: Best for very early stages, not a substitute for fluoride.
2. Restorative Treatments
For more advanced erosion tooth where significant tooth structure has been lost, restorative procedures are necessary to protect the remaining tooth, restore function, and improve aesthetics.
- Fillings (Composite or Amalgam):
- If erosion has created distinct cavities or deep cupping, fillings can be used to restore the lost tooth structure. Composite resin is preferred for aesthetic reasons.
- Pros: Restores function and prevents further decay.
- Cons: Does not cover the entire tooth, may still leave other areas vulnerable if erosion continues.
- Cost: $150-$450 per tooth for composite; $100-$300 per tooth for amalgam (less common now).
- Dental Veneers:
- Thin, custom-made shells (usually porcelain or composite) that cover the front surface of teeth. Veneers are an excellent option for restoring aesthetics and protecting anterior teeth with moderate to severe erosion, especially if discoloration or shape changes are prominent.
- Pros: Highly aesthetic, durable (porcelain), strong protection for front teeth.
- Cons: Irreversible (requires removal of some enamel), more expensive, not suitable for very severe erosion or posterior teeth.
- Cost: $900-$2,500 per tooth for porcelain veneers; $250-$1,500 per tooth for composite veneers.
- Dental Crowns:
- A full-coverage "cap" that encases the entire visible portion of a tooth. Crowns are used for severely eroded teeth, especially molars and premolars, where there's extensive loss of tooth structure, risk of fracture, or when a tooth requires significant structural integrity. Crowns can be made from porcelain, ceramic, metal, or a combination.
- Pros: Provides maximum protection and strength, restores full function and aesthetics.
- Cons: More invasive (requires significant tooth reduction), most expensive option.
- Cost: $800-$2,500 per tooth, depending on material and complexity.
- Onlays/Inlays:
- These are indirect restorations (made in a lab and then bonded to the tooth) used when erosion is too extensive for a filling but not severe enough for a full crown. Inlays fit within the cusps of the tooth; onlays cover one or more cusps.
- Pros: More conservative than crowns, durable, good fit.
- Cons: More expensive than fillings, requires multiple visits.
- Cost: $600-$1,200 per tooth.
Pro Tip: Always address the underlying cause of erosion first. No restoration will last if the acidic environment persists. Your dentist may collaborate with your physician if medical conditions like GERD or eating disorders are the root cause.
Step-by-Step Process: What to Expect During Treatment
The journey to treating erosion tooth typically follows a structured process, starting with diagnosis and leading to tailored treatment.
1. Initial Consultation and Diagnosis
- Comprehensive Oral Examination: Your dentist will visually inspect your teeth, looking for tell-tale signs of erosion (sensitivity, discoloration, cupping, rounded edges, exposed dentin).
- Patient History: A detailed discussion about your dietary habits (acidic food/drink consumption, frequency, duration), lifestyle (e.g., occupation, sports), and medical history (GERD, eating disorders, medications causing dry mouth) is crucial. This helps identify the source of the acid.
- Diagnostic Tools: X-rays may be taken to assess the internal health of the tooth and rule out other issues. Intraoral photos can document the extent of erosion for future comparison. Sensitivity tests might be performed.
- Treatment Planning: Based on the diagnosis and the severity of the erosion, your dentist will present a personalized treatment plan, explaining the recommended options, their pros and cons, costs, and expected outcomes.
2. Treatment Implementation (Examples)
For Conservative Treatments (e.g., Fluoride Varnish, Bonding)
- Fluoride Varnish: The dentist will dry your teeth and paint a thin layer of fluoride varnish onto the affected surfaces. It sets quickly and you'll be advised to avoid brushing or eating hard foods for a few hours.
- Dental Bonding:
- Preparation: The tooth surface is gently etched with an acid gel to create microscopic pores, allowing the resin to adhere securely.
- Bonding Agent: A liquid adhesive (bonding agent) is applied to the etched tooth surface.
- Resin Application: Tooth-colored composite resin is applied to the tooth, molded into the desired shape, and then hardened with a special curing light.
- Finishing: The bonded resin is trimmed, shaped, and polished to match the surrounding teeth and ensure a smooth, natural finish.

For Restorative Treatments (e.g., Crowns, Veneers)
- Crown or Veneer Placement (typically 2 visits):
- Visit 1 (Preparation & Impression):
- Numbing: The tooth is numbed with a local anesthetic.
- Preparation: The dentist carefully reshapes and reduces the tooth structure to make space for the crown or veneer. The amount of reduction depends on the type of restoration.
- Impression: A digital scan or traditional impression material is used to create a precise mold of your prepared tooth. This impression is sent to a dental lab where your custom crown or veneer will be fabricated.
- Temporary Restoration: A temporary crown or veneer is placed to protect the prepared tooth while the permanent one is being made.
- Visit 2 (Placement of Permanent Restoration):
- Removal of Temporary: The temporary restoration is carefully removed.
- Trial Fit: The permanent crown or veneer is placed on the tooth to check for proper fit, bite, and aesthetics. Adjustments may be made.
- Bonding/Cementation: Once satisfactory, the restoration is permanently bonded or cemented onto the tooth.
- Final Adjustments: The bite is checked again, and any necessary final adjustments and polishing are completed.
- Visit 1 (Preparation & Impression):
Pro Tip: Don't hesitate to ask your dentist questions at each stage of the process. Understanding what to expect can ease any anxiety.
Cost and Insurance for Dental Erosion Treatment
The cost of treating erosion tooth in the US can vary widely based on the severity of the erosion, the type of treatment chosen, the materials used, the dentist's fees, and your geographic location.
Average US Price Ranges (Per Tooth)
| Treatment Type | Average Cost Range (Without Insurance) |
|---|---|
| Preventative/Conservative | |
| Fluoride Varnish (Per application) | $25 - $75 |
| Dental Bonding (Composite) | $100 - $400 |
| Dental Sealants | $30 - $60 |
| Restorative | |
| Composite Filling | $150 - $450 |
| Amalgam Filling | $100 - $300 |
| Porcelain Veneer | $900 - $2,500 |
| Composite Veneer | $250 - $1,500 |
| Inlay / Onlay | $600 - $1,200 |
| Dental Crown | $800 - $2,500 |
These are general ranges. Costs in major metropolitan areas like New York or Los Angeles tend to be higher than in rural areas.
Insurance Coverage Details
Dental insurance typically categorizes procedures into three tiers:
- Preventative: Includes exams, cleanings, X-rays, and often fluoride treatments or sealants. Usually covered at 80-100%.
- Basic Restorative: Includes fillings, simple extractions, and sometimes dental bonding (if considered restorative, not cosmetic). Usually covered at 50-80%.
- Major Restorative: Includes crowns, bridges, inlays/onlays, dentures, and often veneers (if deemed medically necessary, not purely cosmetic). Usually covered at 20-50%, often after a deductible is met.
-
PPO vs. HMO:
- PPO (Preferred Provider Organization): Offers more flexibility in choosing dentists. You typically pay a deductible and then a percentage of the cost (co-insurance) after the plan starts paying.
- HMO (Health Maintenance Organization): Requires you to choose a dentist within their network. Costs are generally lower, often with fixed co-pays, but your choice of provider is limited.
-
Annual Maximums: Most dental insurance plans have an annual maximum benefit, typically ranging from $1,000 to $2,000. Once you reach this limit, you are responsible for 100% of additional costs for that year.
-
Waiting Periods: Many plans have waiting periods (e.g., 6-12 months for basic, 12-24 months for major procedures) before certain benefits become active.
Pro Tip: Contact your insurance provider directly before starting any major treatment to understand your specific coverage, deductibles, co-pays, and annual maximums. Get a pre-treatment estimate from your dentist to avoid surprises.
Recovery and Aftercare
Recovery and aftercare instructions for erosion tooth treatments vary depending on the procedure, but the overarching goal is to maintain oral hygiene, protect the treated teeth, and prevent further erosion.
General Aftercare for Restorative Treatments (Fillings, Crowns, Veneers)
- Sensitivity: It's common to experience some temporary sensitivity to hot or cold after a filling, crown, or veneer. This usually subsides within a few days or weeks. Over-the-counter pain relievers can help.
- Numbness: If local anesthetic was used, your mouth may be numb for several hours. Avoid chewing hard foods until the numbness wears off to prevent accidental biting of your cheek or tongue.
- Bite Adjustment: Your bite might feel slightly off initially. If it persists or feels uncomfortable, contact your dentist for an adjustment. A proper bite is crucial for the longevity of the restoration.
- Oral Hygiene: Continue regular brushing (twice daily with fluoride toothpaste) and flossing (once daily). Be gentle around new restorations, especially for the first day or two.
- Dietary Modifications: For the first 24-48 hours after a filling or bonding, avoid very hard, sticky, or chewy foods. With crowns and veneers, most patients can resume a normal diet quickly, but it's always wise to avoid excessively hard foods that could chip or dislodge the restoration.
Long-Term Aftercare and Prevention of Further Erosion
- Dietary Changes: This is paramount.
- Reduce Acidic Foods/Drinks: Limit consumption of sodas, fruit juices, sports drinks, citrus fruits, and vinegars. When you do consume them, do so quickly and ideally with meals.
- Use a Straw: For acidic beverages, a straw can help bypass direct contact with the front teeth.
- Rinse with Water: After consuming acidic foods or drinks, rinse your mouth thoroughly with water to neutralize acids and wash away residues.
- Avoid Brushing Immediately: Wait at least 30-60 minutes after acid exposure (including reflux episodes) before brushing to allow saliva to remineralize the softened enamel.
- Oral Hygiene Routine:
- Soft-Bristled Toothbrush: Use a soft-bristled toothbrush and gentle technique to avoid abrasion, especially on already weakened enamel.
- Fluoride Toothpaste: Use a fluoride toothpaste to strengthen enamel. Your dentist may recommend a prescription-strength fluoride toothpaste.
- Fluoride Rinse: Consider an over-the-counter fluoride mouthrinse for daily use.
- Address Underlying Medical Conditions: Work with your dentist and physician to manage conditions like GERD or eating disorders that cause intrinsic erosion. This might involve medication, lifestyle changes, or therapy.
- Saliva Stimulation: If you suffer from dry mouth, chew sugar-free gum, use saliva substitutes, or discuss medications that stimulate saliva flow with your doctor.
- Regular Dental Check-ups: Schedule routine dental visits (typically every 6 months) for professional cleanings and examinations. Your dentist can monitor the condition of your teeth and restorations and provide additional preventive treatments like fluoride applications.
Pro Tip: Consider integrating foods rich in calcium and vitamin D teeth health into your diet. Vitamin D is essential for the absorption of calcium and phosphate, minerals that contribute to strong teeth and bones, and support enamel remineralization. Dairy products, fortified foods, and fatty fish are good sources.
Prevention of Dental Erosion
Preventing teeth acid erosion is far more effective and less costly than treating it. A multi-faceted approach involving dietary adjustments, excellent oral hygiene, and addressing underlying health conditions is key.
1. Dietary Modifications
- Limit Acidic Beverages: Reduce or eliminate sodas, sports drinks, energy drinks, and excessive fruit juices. When consumed, do so quickly and ideally during meals.
- Use a Straw: When drinking acidic beverages, use a straw to minimize contact with tooth surfaces.
- Rinse with Water: After consuming acidic foods or drinks, rinse your mouth with water to help neutralize acids and dilute their effects. Chewing sugar-free gum can also stimulate saliva flow to help neutralize acids.
- Avoid Prolonged Exposure: Don't sip on acidic drinks for extended periods. Finish them quickly.
- Choose Tooth-Friendly Snacks: Opt for cheese, nuts, plain yogurt, or vegetables instead of highly acidic fruits or sugary snacks between meals.
- Increase Calcium-Rich Foods: Dairy products (milk, cheese, yogurt) are excellent sources of calcium, which helps remineralize enamel and provides a protective buffer.
2. Optimal Oral Hygiene Practices
- Wait to Brush: Avoid brushing immediately after consuming acidic foods or drinks, or after episodes of acid reflux/vomiting. Wait at least 30-60 minutes to allow saliva to naturally neutralize acids and start the remineralization process. Brushing softened enamel can cause further abrasion.
- Soft-Bristled Toothbrush: Use a soft-bristled brush and brush gently to prevent mechanical wear on enamel.
- Fluoride Toothpaste: Use a fluoride toothpaste. Fluoride strengthens enamel and makes it more resistant to acid attacks.
- Fluoride Mouthrinse: Consider using an over-the-counter fluoride mouthrinse daily. Your dentist may prescribe a stronger fluoride rinse if needed.
3. Address Underlying Medical Conditions
- GERD Management: If you suffer from acid reflux, work with your physician to manage the condition. This might involve dietary changes, medication, or lifestyle adjustments (e.g., elevating your head during sleep).
- Eating Disorder Treatment: Seek professional help for eating disorders. A multi-disciplinary approach involving medical, psychological, and dental professionals is essential.
- Dry Mouth: If you have dry mouth, identify the cause (e.g., medications, medical conditions) and discuss solutions with your doctor and dentist. Saliva substitutes, humidifiers, and staying hydrated can help.
4. Regular Dental Check-ups
- Professional Cleanings and Exams: Regular visits allow your dentist to monitor for early signs of erosion, provide professional fluoride treatments, and offer personalized preventive advice.
- Protective Appliances: In some cases, a custom-fitted mouthguard might be recommended if you experience severe nocturnal reflux, to protect your teeth during sleep.
5. Nutrition for Strong Teeth: The Role of Vitamin D
Adequate nutrition plays a crucial role in overall dental health, and vitamin D teeth resilience is a significant aspect.
- Calcium Absorption: Vitamin D is essential for the body to absorb calcium and phosphate from the diet. These minerals are the building blocks of strong enamel and dentin. Without sufficient Vitamin D, calcium cannot be effectively utilized, potentially leading to weaker enamel that is more susceptible to erosion.
- Bone Density: Vitamin D also supports healthy bone density, including the alveolar bone that supports your teeth.
- Sources of Vitamin D:
- Sunlight Exposure: The primary natural source.
- Dietary Sources: Fatty fish (salmon, mackerel, tuna), fortified milk, orange juice, cereals, and some dairy products.
- Supplements: If dietary intake and sun exposure are insufficient, your doctor or dentist may recommend vitamin D supplements.
Pro Tip: Consult with your dentist or a nutritionist for personalized advice on dietary modifications and supplementation to ensure optimal oral health and strengthen your teeth against erosion.
Risks and Complications of Untreated Erosion
Ignoring erosion tooth can lead to a cascade of worsening dental problems, significantly impacting your oral health, general well-being, and even your financial resources.
- Increased Tooth Sensitivity: As enamel erodes, the dentin becomes exposed, leading to persistent and often severe sensitivity to temperature changes and sweet or acidic foods. This can make eating and drinking uncomfortable.
- Tooth Discoloration: The yellowish dentin becomes more visible as enamel thins, making teeth appear duller and less aesthetic.
- Changes in Tooth Shape and Appearance: Teeth can become rounded, shorter, or develop characteristic "cupping" on chewing surfaces. This alters the natural appearance of your smile.
- Weakened Tooth Structure: Eroded teeth are structurally weaker, making them more prone to chipping, cracking, or fracturing, even during normal chewing.
- Increased Risk of Cavities: While erosion itself is not bacterial, exposed and demineralized dentin is more susceptible to bacterial plaque accumulation and cavity formation. Enamel is the primary shield against decay.
- Pulpitis (Inflammation of the Nerve): As erosion progresses deeper, it can reach the pulp (the innermost part of the tooth containing nerves and blood vessels). This can cause severe pain, infection, and may necessitate a root canal treatment or even tooth extraction.
- Occlusal Problems (Bite Issues): Significant tooth wear can alter your bite, leading to jaw pain (TMJ issues), headaches, and difficulty chewing properly.
- Increased Cost of Treatment: Early, mild erosion can often be managed conservatively and affordably. Untreated, severe erosion requires extensive and costly restorative procedures like multiple crowns, veneers, or even full mouth rehabilitation.
- Tooth Loss: In the most severe and prolonged cases, erosion can weaken teeth to the point where they cannot be saved and must be extracted, leading to the need for costly tooth replacement options like implants or bridges.
Children / Pediatric Considerations for Dental Erosion
Dental erosion is not just an adult problem; it can significantly affect children and adolescents, whose developing enamel may be particularly vulnerable. Early detection and intervention are crucial to protect their growing smiles.
Why Children are Vulnerable
- Thinner Enamel: Primary (baby) teeth have thinner enamel compared to permanent teeth, making them more susceptible to acid attack. Even permanent teeth in adolescents may not be fully mineralized, offering less resistance.
- Dietary Habits: Children often consume a higher frequency of sugary and acidic beverages and foods (fruit juices, sodas, sports drinks, sour candies). Parents may not realize the erosive potential of "healthy" options like 100% fruit juice if consumed excessively.
- Medications: Some pediatric medications, especially chewable vitamin C or liquid iron supplements, can be acidic.
- Medical Conditions: Children can also suffer from GERD, although symptoms might be different from adults. Eating disorders can also begin in adolescence.
- Oral Hygiene: Children may not have fully developed brushing habits, or they might brush too aggressively, especially after acidic intake.
Signs of Erosion in Children
- Increased Sensitivity: Similar to adults, sensitivity to hot, cold, or sweet.
- Dull or Yellowish Teeth: As enamel wears, the underlying dentin shows through.
- Chipping or Cracking: Children's teeth may chip more easily.
- Changes in Shape: Teeth may appear shorter or have rounded edges.
Prevention and Management for Children
- Dietary Education for Parents: Educate parents on the erosive potential of common children's foods and drinks. Encourage water as the primary beverage.
- Limit fruit juice to mealtimes and dilute it if given.
- Discourage sipping on bottles or sippy cups filled with juice or milk for extended periods.
- Proper Oral Hygiene:
- Teach children to brush gently with a soft-bristled toothbrush.
- Supervise brushing, especially for younger children.
- Emphasize waiting 30-60 minutes after acidic foods/drinks before brushing.
- Ensure they use an age-appropriate fluoride toothpaste.
- Fluoride Application:
- Regular professional fluoride varnishes are highly beneficial for children, especially if they show signs of erosion or are at high risk.
- Consider fluoride supplements if recommended by a pediatrician or dentist in areas with non-fluoridated water.
- Dental Sealants: Sealants are very effective in protecting the chewing surfaces of permanent molars, which are often targets of erosion and decay.
- Address Medical Conditions: Work with a pediatrician to manage conditions like reflux.
- Regular Pediatric Dental Visits: Routine check-ups are essential for early detection and intervention. A pediatric dentist can provide tailored advice and apply preventive treatments.

Pro Tip: Make water the default drink for children. Encourage them to drink tap water (if fluoridated) throughout the day to keep teeth strong and clean.
Cost Breakdown for Dental Erosion Treatments
Understanding the financial implications is a major concern for many patients. Here's a more detailed look at the costs associated with treating erosion tooth, broken down by procedure and considering insurance.
Average US Costs (Ranges)
As previously outlined, the range for treatments can be significant. Here's a summary:
| Treatment Category | Example Procedures | Low End (USD) | Mid Range (USD) | High End (USD) |
|---|---|---|---|---|
| Preventative/Early Stage | Fluoride Varnish (per application) | $25 | $50 | $75 |
| Dental Bonding (per tooth) | $100 | $250 | $400 | |
| Dental Sealant (per tooth) | $30 | $45 | $60 | |
| Moderate Erosion | Composite Filling (per tooth) | $150 | $300 | $450 |
| Inlay/Onlay (per tooth) | $600 | $900 | $1,200 | |
| Composite Veneer (per tooth) | $250 | $800 | $1,500 | |
| Severe Erosion | Porcelain Veneer (per tooth) | $900 | $1,700 | $2,500 |
| Dental Crown (per tooth) | $800 | $1,600 | $2,500 | |
| Full Mouth Reconstruction | $20,000 | $40,000 | $80,000+ |
Note: Full mouth reconstruction is for extreme cases requiring multiple crowns, veneers, and possibly implants.
With vs. Without Insurance
- Without Insurance: You will be responsible for 100% of the listed costs. This can be substantial, especially for multiple restorative procedures.
- With Insurance: As detailed in the "Cost and Insurance" section, coverage varies by procedure category (preventative, basic, major) and your specific plan (PPO, HMO).
- Preventative: Often 80-100% covered.
- Basic Restorative: Often 50-80% covered.
- Major Restorative: Often 20-50% covered after deductible.
- Annual Maximums: Most plans have a maximum annual benefit (e.g., $1,000-$2,000). Once reached, you pay 100%.
Example Scenario: Imagine you need 4 composite fillings for moderate erosion.
- Total Cost without insurance: 4 x $300 (mid-range) = $1,200.
- With insurance (70% coverage for basic, $50 deductible):
- You pay $50 deductible.
- Remaining balance: $1,200 - $50 = $1,150.
- Insurance pays 70% of $1,150 = $805.
- You pay 30% of $1,150 = $345.
- Your total out-of-pocket: $50 (deductible) + $345 (co-insurance) = $395.
- This assumes you haven't reached your annual maximum and met any waiting periods.
Payment Plans and Financing Options
For extensive treatments, many dental offices offer:
- In-house Payment Plans: Staggered payments over several months, often interest-free.
- Third-Party Financing: Companies like CareCredit or LendingClub offer specialized healthcare credit cards with deferred interest or low-interest payment options for larger expenses.
- Dental Schools: University dental schools often provide services at a reduced cost, as treatments are performed by supervised students.
- Community Health Clinics: Some clinics offer reduced fees for low-income individuals.
Cost-Saving Tips
- Preventative Care: The absolute best way to save money is to prevent erosion or catch it early with regular dental check-ups and good home care.
- Utilize Insurance Benefits: Understand and maximize your annual insurance benefits.
- Compare Costs: Get quotes from a few different dentists, especially for major procedures.
- Negotiate: Don't be afraid to discuss payment options or potential discounts with your dental office, especially if paying in cash.
Frequently Asked Questions About Erosion Tooth
Q1: What is the main difference between dental erosion and cavities?
Dental erosion is the loss of tooth structure due to direct chemical dissolution by acids, without bacterial involvement. Cavities (dental caries), on the other hand, are caused by acids produced by bacteria metabolizing sugars in food, creating holes in the tooth. While both involve acid, their origin and mechanisms are distinct.
Q2: How painful is it to treat a tooth with erosion?
The pain level depends on the severity of the erosion and the chosen treatment. Mild erosion treated with fluoride or bonding is usually minimally uncomfortable. Restorative treatments like fillings, crowns, or veneers typically involve local anesthetic, so you won't feel pain during the procedure. You might experience some temporary sensitivity after treatment, which can be managed with over-the-counter pain relievers.
Q3: How long do treatments for erosion last?
The longevity of treatments varies significantly. Dental bonding typically lasts 5-10 years. Fillings can last 7-15 years or more. Porcelain veneers and crowns are generally very durable, lasting 10-15 years, and often much longer with excellent care. The key factor in all treatments is addressing the underlying cause of erosion to prevent damage to the treated tooth or adjacent teeth.
Q4: Can dental erosion be reversed?
No, once tooth enamel is lost due to erosion, it cannot naturally regenerate. The damage is irreversible. However, the progression of erosion can be halted or significantly slowed down through preventive measures and early intervention. Fluoride treatments and remineralizing agents can help strengthen existing enamel and make it more resistant, but they cannot rebuild lost tooth structure.
Q5: Is it safe to whiten teeth that have erosion?
Whitening teeth with existing erosion is generally not recommended without prior dental assessment and treatment. The whitening agents can increase sensitivity in already eroded areas and potentially cause further irritation or discomfort. Your dentist will likely recommend treating the erosion first, restoring the enamel, and then discussing whitening options.
Q6: What role does Vitamin D play in preventing dental erosion?
Vitamin D is critical for the body's absorption of calcium and phosphate, which are the essential minerals for strong tooth enamel and dentin. Adequate vitamin D levels help ensure that teeth are properly mineralized and thus more resistant to acid attacks. While not a direct anti-erosive agent, it indirectly fortifies teeth against erosion by promoting overall enamel strength.
Q7: Can dry mouth contribute to dental erosion?
Yes, dry mouth (xerostomia) significantly increases the risk of dental erosion. Saliva acts as a natural buffer, neutralizing acids in the mouth and washing away food debris. It also contains minerals that help remineralize enamel. Reduced saliva flow means less acid neutralization and less remineralization, leaving teeth more vulnerable to acid attack.
Q8: Are there any home remedies for dental erosion?
There are no effective home remedies to reverse or treat existing dental erosion. While rinsing with water after acidic intake and using fluoride toothpaste are beneficial preventive measures, once erosion has occurred, professional dental treatment is necessary. Avoid unproven remedies, as some (like lemon juice or apple cider vinegar rinses) can actually worsen erosion.
Q9: Does insurance cover all erosion treatments?
Dental insurance coverage varies. Preventative treatments (fluoride, sealants) are typically well-covered. Basic restorations (fillings, bonding) usually have decent coverage. Major restorations (crowns, veneers, onlays) often have lower coverage percentages and may be subject to annual maximums and waiting periods. Cosmetic aspects, if not deemed medically necessary, might not be covered. It's crucial to check with your specific provider.
Q10: What happens if I don't treat my erosion tooth?
Untreated erosion will progressively worsen, leading to increased sensitivity, aesthetic concerns, weakened tooth structure, higher risk of cavities, and potentially severe complications like pulp inflammation, tooth fracture, and even tooth loss. The longer erosion is left untreated, the more extensive and costly the required restorative treatments will become.
When to See a Dentist
Recognizing when to seek professional dental care for erosion tooth can save you discomfort, prevent further damage, and reduce future treatment costs.
Routine Care & Early Concerns (Schedule a regular appointment):
- New or Increased Sensitivity: If you notice your teeth becoming more sensitive to hot, cold, sweet, or acidic foods/drinks. This is often an early sign.
- Changes in Tooth Appearance: If you observe your teeth appearing more yellow, dull, translucent at the edges, or if existing fillings seem to stand out more.
- Dietary or Lifestyle Changes: If you've recently increased your intake of acidic foods/drinks, started new medications that cause dry mouth, or developed habits like frequently sipping sodas.
- Diagnosis of Acid Reflux/Eating Disorder: If a physician diagnoses you with GERD, bulimia, or another condition that exposes your teeth to stomach acid, schedule a dental check-up promptly to assess and prevent erosion.
- Routine Check-ups: Even without specific symptoms, regular dental examinations (every 6 months) are vital. Your dentist can identify early signs of erosion before you even notice them.
Warning Signs Requiring Prompt Attention (Call your dentist soon):
- Persistent Pain: If you experience ongoing toothache, especially if it's dull, throbbing, or interferes with sleep, it could indicate deeper erosion affecting the tooth's pulp.
- Visible Chips or Cracks: If your teeth start to chip or crack, particularly without significant trauma, it suggests weakened enamel due to erosion.
- Difficulty Chewing: If the shape of your teeth has changed so much that it affects your bite or makes chewing uncomfortable.
- Rapid Progression: If you notice a sudden and significant worsening of any erosion symptoms or tooth wear.
Emergency Situations (Seek immediate dental care):
- Severe, Unbearable Pain: Intense, debilitating tooth pain that doesn't subside with over-the-counter pain relievers.
- Tooth Fracture or Loss: If a significant portion of a tooth breaks off, or a tooth becomes loose due to severe erosion.
- Signs of Infection: Swelling around a tooth, pus, or a fever accompanied by tooth pain could indicate an infection related to severe erosion exposing the pulp.
Don't wait until erosion becomes severe. Early detection and proactive management are the most effective ways to protect your smile and maintain long-term oral health.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
What Are Calcium Deposits on Teeth
Are you one of the millions of Americans who notices a stubborn, yellowish buildup on your teeth despite regular brushing? You're likely experiencing what many refer to as "calcium deposits on teeth." This common dental concern, medically known as dental calculus or tartar, affects a vast ma
February 23, 2026
Calcium Good for Teeth: Complete Guide
More than 99% of your body's calcium resides in your bones and teeth, making it an undeniable cornerstone of skeletal and oral health. But did you know that an estimated 42% of American adults don't get enough calcium from their diet? This staggering statistic underscores a critical question
February 23, 2026
What Do Bulimia Teeth Look Like
"Bulimia teeth" refers to the specific and often severe damage that the self-induced vomiting characteristic of bulimia nervosa inflicts on a person's oral health. It's a critical issue, affecting approximately 1.5% of women and 0.5% of men in the US at some point in their lives, with many more
February 23, 2026

Erosion in Teeth: Complete Guide
Erosion in Teeth: Complete Guide
February 23, 2026