Gerd Teeth: Complete Guide
Key Takeaways
- Dental health is often a window into our overall well-being, and few conditions illustrate this as clearly as the impact of Gastroesophageal Reflux Disease (GERD) on your teeth. Often dismissed as just a digestive issue, GERD's persistent acid reflux can silently erode the very foundation of your sm
Dental health is often a window into our overall well-being, and few conditions illustrate this as clearly as the impact of Gastroesophageal Reflux Disease (GERD) on your teeth. Often dismissed as just a digestive issue, GERD's persistent acid reflux can silently erode the very foundation of your smile, leading to what dentists often refer to as gerd teeth. This relentless exposure to stomach acid can cause significant and often irreversible damage to tooth enamel, resulting in increased sensitivity, disfigurement, and ultimately, tooth loss if left unaddressed. In the United States, an estimated 20% of adults experience GERD symptoms weekly, putting a substantial portion of the population at risk for these detrimental oral health effects. Understanding the connection between GERD and dental erosion is paramount for early intervention and preserving your oral health.
This comprehensive guide from SmilePedia.net will delve deep into the intricacies of gerd teeth, exploring their causes, identifying the tell-tale signs, and outlining the full spectrum of available treatment options. We’ll also equip you with crucial prevention strategies and provide insights into managing the associated costs, ensuring you have all the information needed to protect your smile from the corrosive effects of acid reflux.
Key Takeaways:
- GERD teeth result from chronic exposure to stomach acid, leading to irreversible enamel erosion and dentin damage.
- Early signs include increased tooth sensitivity, changes in tooth texture, and a yellowing appearance as enamel thins.
- Decalcification white calcium spots on teeth can be an early indicator of acid erosion or other enamel issues, requiring professional evaluation.
- Dental treatments for GERD teeth range from preventative fluoride applications (costing $30-$70 per application) and dental bonding ($100-$400 per tooth) to veneers ($900-$2,500 per tooth) or crowns ($800-$3,000 per tooth) for more severe damage.
- Managing underlying GERD through lifestyle changes, diet modifications, and medication is crucial for preventing further dental damage.
- Prompt diagnosis and intervention are vital; untreated GERD teeth can lead to extensive restorative needs and potential tooth loss, with repair timelines ranging from a single visit for bonding to several weeks for crowns/veneers.
- Dental insurance often covers essential restorative treatments, but cosmetic procedures like veneers may have limited coverage, necessitating exploration of financing options.
What It Is / Overview
Gastroesophageal Reflux Disease (GERD) is a chronic digestive disorder where stomach acid, or sometimes bile, flows back into the esophagus, irritating its lining. While often associated with heartburn and indigestion, this acidic reflux also significantly impacts oral health, giving rise to what's commonly known as gerd teeth. The highly acidic contents of the stomach, with a pH typically between 1.5 and 3.5, are powerful enough to dissolve tooth enamel, the hardest substance in the human body (which has a critical pH of 5.5). When this acid repeatedly bathes the teeth, it initiates a process called acid erosion.

Acid erosion is a chemical process, not bacterial, where the mineral structure of the tooth (primarily hydroxyapatite) is dissolved. Unlike mechanical wear from grinding or brushing, acid erosion causes a characteristic smooth, cupped, or grooved appearance on the tooth surfaces, particularly on the lingual (tongue-facing) and occlusal (biting) surfaces of the teeth, especially the molars and pre-molars. The severity of dental erosion is directly related to the frequency, duration, and acidity of the reflux episodes. Over time, the protective enamel layer thins, exposing the softer, more sensitive dentin underneath. This exposure not only increases sensitivity but also makes the teeth more vulnerable to decay, fracture, and discoloration.
It's important to differentiate acid erosion from other forms of tooth wear. Abrasion is caused by mechanical friction (e.g., aggressive brushing), attrition by tooth-to-tooth contact (e.g., grinding), and abfraction by flexural forces at the gum line. While these can coexist, acid erosion from GERD has distinct patterns of damage.
Types / Variations of Dental Erosion from Acid Reflux
While "gerd teeth" isn't a classification of teeth itself, the dental damage caused by acid reflux manifests in several identifiable patterns and severities. The type of damage often provides clues to the source and chronicity of the acid exposure.
Localized vs. Generalized Erosion
- Localized Erosion: This typically affects specific areas, often the lingual surfaces of upper front teeth (incisors), where stomach acid often pools as it refluxes. The occlusal surfaces of molars and premolars can also show erosion, particularly if reflux occurs during sleep, allowing acid to settle.
- Generalized Erosion: In severe, chronic GERD, the acid exposure can be widespread, affecting many or most teeth in the mouth. This indicates frequent and pervasive reflux episodes.
Severity Stages
Dental erosion from GERD progresses through stages:
- Early Enamel Erosion: Subtle changes, often only detectable by a dentist. The enamel may appear smoother or lose its characteristic luster. Sensitivity might be intermittent.
- Moderate Enamel Erosion: Noticeable thinning of enamel. Teeth may appear more translucent or slightly yellow as dentin becomes more visible. Increased sensitivity to hot, cold, and sweet.
- Severe Enamel Erosion with Dentin Exposure: Enamel is significantly worn down, exposing the softer dentin. This leads to pronounced sensitivity, potential changes in tooth shape (e.g., rounded cusps, cupping), and a deeper yellow or brownish discoloration. Fillings may appear to sit higher than the surrounding tooth structure because the natural tooth has eroded around them.
- Pulp Exposure/Damage: In extreme cases, the dentin wears away to expose the dental pulp, containing nerves and blood vessels. This can lead to severe pain, infection, and necessitate root canal treatment or extraction.
Erosion from Other Acidic Conditions (Similar Signs)
It's crucial to note that while GERD is a primary cause, other conditions can lead to similar bulimia teeth signs or general acid erosion, making a differential diagnosis important for proper treatment.
- Bulimia Nervosa and Other Eating Disorders: Repeated self-induced vomiting exposes teeth to highly acidic stomach contents. The pattern of erosion, often most pronounced on the lingual surfaces of the upper front teeth and occlusal surfaces, can be strikingly similar to GERD. The damage can be rapid and severe.
- Acidic Dietary Habits: Frequent consumption of highly acidic foods and beverages (e.g., sodas, sports drinks, fruit juices, citrus fruits, vinegars) can cause extrinsic acid erosion, typically affecting the labial (lip-facing) and occlusal surfaces, but can also cause generalized erosion.
- Medication Side Effects: Certain medications can cause dry mouth (xerostomia), reducing saliva's ability to buffer acids, thus exacerbating erosion. Others may directly be acidic.
- Occupational Exposure: Individuals working in industries with acidic fumes (e.g., battery manufacturing) may experience erosion.
Understanding these variations helps your dentist accurately diagnose the cause and recommend the most effective treatment and prevention strategies.
Causes / Why It Happens
The fundamental cause of gerd teeth is the persistent exposure of tooth enamel to highly acidic stomach contents. This happens when the lower esophageal sphincter (LES), a ring of muscle that acts as a valve between the esophagus and stomach, malfunctions and doesn't close properly.
Here's a breakdown of the key contributing factors:
Malfunctioning Lower Esophageal Sphincter (LES)
- Weakened LES: The LES can relax inappropriately, allowing stomach acid to flow back up into the esophagus and sometimes into the mouth. This is the primary physiological mechanism behind GERD.
- Hiatal Hernia: A condition where part of the stomach pushes up through the diaphragm, can weaken the LES and increase the likelihood of reflux.
Increased Abdominal Pressure
- Obesity: Excess weight puts pressure on the abdomen, pushing stomach contents upwards.
- Pregnancy: The growing uterus exerts pressure, and hormonal changes can relax the LES.
- Tight Clothing: Can constrict the abdomen.
- Heavy Lifting/Straining: Increases intra-abdominal pressure.
Lifestyle and Dietary Factors
- Trigger Foods and Beverages:
- Acidic Foods: Citrus fruits, tomatoes, vinegar-based dressings.
- Fatty and Fried Foods: Slow stomach emptying, increasing reflux time.
- Spicy Foods: Can irritate the esophagus.
- Chocolate: Contains methylxanthine, which can relax the LES.
- Peppermint: Also relaxes the LES.
- Carbonated Drinks: Increase stomach pressure and are often acidic.
- Caffeine: Can relax the LES.
- Alcohol: Relaxes the LES and can irritate the esophageal lining.
- Eating Habits: Large meals, eating too close to bedtime, and lying down immediately after eating can exacerbate reflux.
- Smoking: Nicotine relaxes the LES and reduces saliva production, hindering acid neutralization.
- Stress: While not a direct cause, stress can worsen GERD symptoms by affecting digestive processes.
Other Medical Conditions and Medications
- Gastroparesis: Delayed stomach emptying, where food stays in the stomach longer, increasing reflux risk.
- Zollinger-Ellison Syndrome: A rare condition causing excessive stomach acid production.
- Certain Medications: Some drugs can relax the LES (e.g., calcium channel blockers, nitrates), reduce saliva flow (e.g., antihistamines, antidepressants), or directly irritate the esophagus.
Saliva's Protective Role
Saliva plays a crucial role in protecting teeth from acid. It helps to:
- Buffer acids: Neutralizing them with bicarbonates and other compounds.
- Rinse away acid: Physically washing acid off tooth surfaces.
- Provide minerals: Contributing to remineralization of early enamel lesions.
Conditions that reduce saliva flow, such as dry mouth (xerostomia) from medications, certain diseases (e.g., Sjögren's syndrome), or salivary gland damage, can significantly accelerate acid erosion, making the teeth more vulnerable to the effects of reflux.
Signs and Symptoms
Identifying the signs of gerd teeth early is crucial for effective intervention. Many symptoms are subtle at first, often dismissed as typical wear and tear or minor sensitivity. A keen eye and regular dental check-ups are your best defense.
Visual Cues in the Mouth
- Changes in Tooth Color and Texture:
- Yellowing: As enamel erodes, the underlying dentin, which is naturally yellowish, becomes more exposed.
- Dull or Opaque Appearance: Enamel can lose its natural luster and appear dull.
- Translucency: The edges of front teeth, particularly the incisal edges, may appear more transparent.
- Smooth, Glassy Appearance: Eroded surfaces can feel unusually smooth to the tongue.
- Cupping and Grooving:
- Cupping on Occlusal Surfaces: Small, rounded depressions or "cups" may appear on the biting surfaces of molars and premolars, often surrounded by intact enamel rims.
- Grooving: Shallow grooves may form on the lingual (tongue-facing) surfaces of upper anterior teeth.
- Loss of Tooth Anatomy:
- Flattened Cusps: The pointed cusps of back teeth can become flattened and rounded.
- Shortened Teeth: Severe erosion can visibly shorten the overall length of teeth.
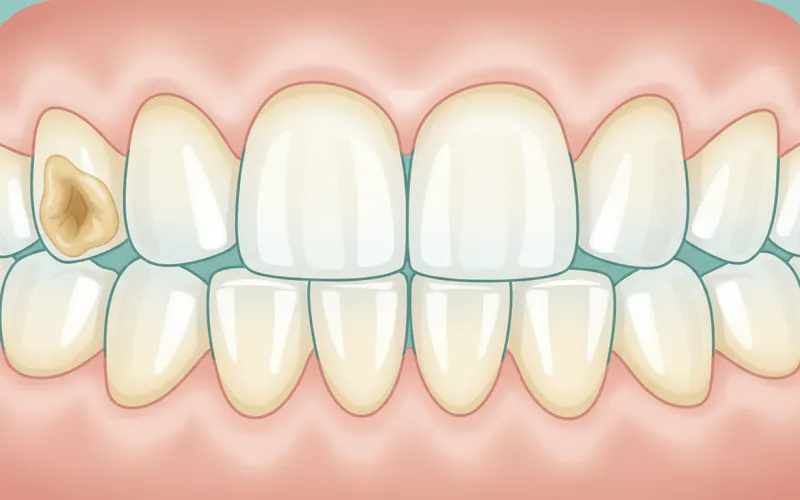
- Exposed Dentin: Patches of the softer, darker dentin may be visible through the thinned enamel.
- Raised Fillings: Existing dental fillings may appear to protrude or sit above the surrounding tooth surface because the natural tooth structure around them has eroded.
- Decalcification White Calcium Spots on Teeth: These can appear as initial signs of demineralization, sometimes from acid erosion, but also from other causes like plaque accumulation around braces. While not exclusive to GERD, acid exposure can contribute to localized mineral loss, leading to these white, chalky areas.
Oral Sensations and Discomfort
- Increased Tooth Sensitivity: This is one of the most common and earliest symptoms. Exposed dentin contains microscopic tubules leading to the tooth's nerve. Acid, hot, cold, and sweet foods or drinks can trigger sharp, fleeting pain.
- Dry Mouth: Some individuals with GERD or those taking GERD medications may experience dry mouth, which exacerbates erosion by reducing saliva's protective buffering capacity.
- Chipping and Fractures: Eroded enamel is weaker and more brittle, making teeth more susceptible to chipping or fracturing, even from normal biting forces.
- Bad Breath (Halitosis): GERD can contribute to bad breath due to refluxed stomach contents and changes in oral pH.
- Sore Throat/Hoarseness: Though not a direct dental sign, these are common symptoms of GERD, indicating acid exposure in the throat that can also affect oral tissues.
Bulimia Teeth Signs: A Specific Pattern
When considering bulimia teeth signs, the erosion pattern is very specific due to repeated self-induced vomiting. Look for:
- Severe erosion primarily on the lingual (tongue-facing) surfaces of the upper front teeth. This is where the stomach acid makes most contact as it passes through the mouth.
- Erosion on the occlusal surfaces of back teeth, though sometimes less pronounced than on the linguals of anterior teeth.
- Sensitivity and often visible shortening or thinning of the affected teeth.
- Palatal lesions: Sores or trauma to the soft palate from fingers or objects used to induce vomiting.
- Enlarged parotid glands: Swelling in the cheeks due to overworked salivary glands.
If you notice any of these signs, particularly a combination of them, it's crucial to schedule an appointment with your dentist and discuss your GERD symptoms or any history of eating disorders. Early detection can significantly limit the damage and preserve your oral health.
Treatment Options
Treating gerd teeth involves a two-pronged approach: managing the underlying GERD to halt further damage and restoring the damaged dental structures. It's a collaboration between your dentist and your medical doctor or gastroenterologist.
1. Addressing the Underlying GERD
This is the most critical step to prevent ongoing dental erosion.
- Lifestyle and Dietary Modifications:
- Dietary Changes: Avoid trigger foods (fatty, spicy, acidic, chocolate, peppermint, caffeine, alcohol, carbonated drinks).
- Eating Habits: Eat smaller, more frequent meals. Avoid eating 2-3 hours before bedtime. Elevate the head of your bed.
- Weight Management: Lose weight if overweight or obese.
- Smoking Cessation: Stop smoking.
- Medications:
- Antacids: Provide immediate, temporary relief by neutralizing stomach acid.
- H2 Blockers (e.g., famotidine, ranitidine): Reduce acid production.
- Proton Pump Inhibitors (PPIs, e.g., omeprazole, lansoprazole): Potently block acid production, often prescribed for long-term GERD management.
- Surgical Intervention: In severe cases where lifestyle changes and medications are ineffective, surgery (e.g., fundoplication) to strengthen the LES may be considered.
2. Dental Restorative Treatments
Once GERD is managed, your dentist can begin to repair the existing damage. The choice of treatment depends on the severity of the erosion.
a. Preventative and Minimally Invasive
- Fluoride Treatments:
- Description: Professional fluoride varnishes, gels, or foams applied in-office strengthen enamel and make it more resistant to acid. Prescription-strength fluoride toothpaste or mouth rinses may also be recommended for home use.
- Pros: Non-invasive, strengthens existing enamel, reduces sensitivity.
- Cons: Does not repair existing structural damage.
- Cost: $30-$70 per application in-office.
- Dental Sealants:
- Description: A protective plastic coating applied to the chewing surfaces of back teeth to shield them from acid and decay.
- Pros: Prevents further erosion in vulnerable grooves.
- Cons: Only covers occlusal surfaces.
- Cost: $30-$60 per tooth.
- Bonding (Composite Resins):
- Description: Tooth-colored resin material is applied to the eroded areas, sculpted, and hardened with a special light. Ideal for minor to moderate erosion and covering decalcification white calcium spots on teeth.
- Pros: Less invasive than crowns/veneers, preserves more natural tooth structure, often completed in one visit.
- Cons: Not as durable or stain-resistant as porcelain, may need to be repaired or replaced every 5-10 years.
- Cost: $100-$400 per tooth.
b. Moderately Invasive to Extensive Restorations
- Veneers (Porcelain or Composite):
- Description: Thin, custom-made shells (usually porcelain) are bonded to the front surface of teeth to restore shape, color, and protect from further erosion. Composite veneers are a less expensive, direct option.
- Pros: Highly aesthetic, durable (porcelain), protects extensive facial/lingual erosion.
- Cons: Irreversible (requires removal of some enamel), more expensive, porcelain can chip.
- Cost: $900-$2,500 per tooth for porcelain; $250-$1,500 per tooth for composite.
- Crowns (Caps):
- Description: A custom-made cap that covers the entire visible portion of a tooth. Used when erosion is severe, and the tooth structure is significantly compromised.
- Pros: Provides full coverage and strength, durable, can restore severely damaged teeth.
- Cons: Requires significant removal of existing tooth structure, more expensive, multi-visit procedure.
- Cost: $800-$3,000 per tooth.
- Onlays/Inlays:
- Description: Partial crowns that restore the chewing surface and/or cusps of back teeth when erosion is too extensive for a filling but not severe enough for a full crown.
- Pros: Conservative of tooth structure compared to full crowns, durable.
- Cons: More expensive than fillings, multi-visit procedure.
- Cost: $650-$1,200 per tooth.
- Root Canal Treatment and Extraction/Implants:
- Description: If erosion reaches the dental pulp, causing irreversible damage or infection, a root canal may be necessary. For severely compromised teeth that cannot be saved, extraction followed by a dental implant and crown is an option.
- Pros: Saves a tooth (root canal), replaces a lost tooth with a stable, long-lasting solution (implant).
- Cons: Invasive, expensive, multi-stage procedure for implants.
- Cost: Root canal: $700-$2,000 per tooth. Dental Implant (implant, abutment, crown): $3,000-$6,000 per tooth.
Pro Tip: Always discuss all available options with your dentist, including their pros, cons, costs, and expected lifespan, before making a decision. Consider long-term implications for your oral health and budget.
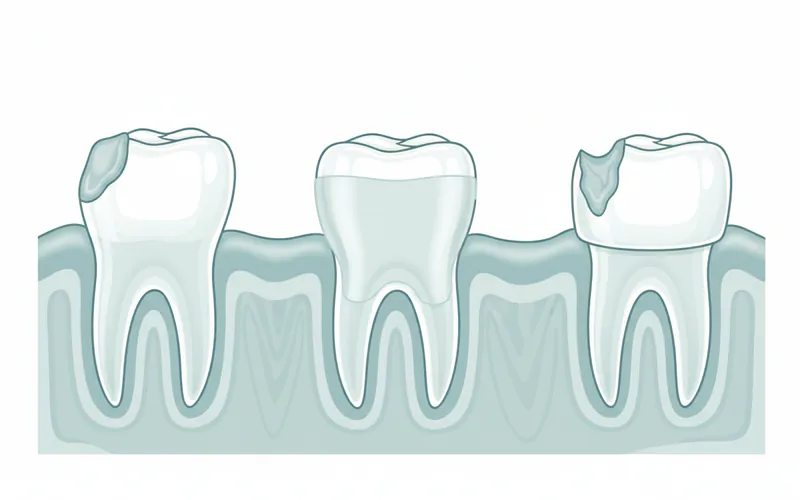
Step-by-Step Process for Dental Treatment
The treatment process for gerd teeth typically follows a structured approach, starting with diagnosis and management of the underlying condition before proceeding to dental restorations.
Step 1: Initial Consultation and Diagnosis
- Comprehensive Dental Exam: Your dentist will perform a thorough visual inspection, looking for characteristic signs of acid erosion (cupping, yellowing, translucency, raised fillings). They will also assess your overall oral health.
- Medical History Review: You'll be asked about your medical history, including any diagnosis of GERD, symptoms like heartburn or regurgitation, medication use, and dietary habits. If an eating disorder is suspected, your dentist may subtly inquire or refer you for professional evaluation.
- Imaging: X-rays may be taken to assess the extent of damage to the inner tooth structure, identify decay, or rule out other issues.
- Discussion: Your dentist will explain their findings and discuss the link between your GERD and your dental condition.
Step 2: Referral and GERD Management
- Medical Referral: If you have undiagnosed GERD or poorly managed symptoms, your dentist will likely refer you to your primary care physician or a gastroenterologist for diagnosis and treatment of the reflux itself. This is a critical step, as repairing teeth without addressing the acid source is futile.
- GERD Treatment Plan: Your medical doctor will develop a plan that may include lifestyle modifications, dietary changes, and/or medication (antacids, H2 blockers, PPIs).

Step 3: Dental Treatment Planning
- Stabilization Phase: For active erosion or severe sensitivity, your dentist might recommend immediate preventative measures like fluoride treatments or prescription-strength fluoride toothpaste to strengthen enamel and reduce discomfort while GERD is being controlled.
- Restorative Plan: Once your GERD is under control, your dentist will present a detailed treatment plan for restoring the damaged teeth. This plan will outline recommended procedures (bonding, veneers, crowns, etc.), their sequence, estimated costs, and timelines.
- Pre-Treatment Preparations: Depending on the chosen treatment, this might involve taking impressions of your teeth, creating wax-up models to visualize results, or discussing anesthesia options.
Step 4: Execution of Dental Restorations (Example: Bonding)
Let's use dental bonding as an example for a common treatment of moderately eroded teeth or decalcification white calcium spots on teeth:
- Preparation: The dentist will prepare the tooth surface by lightly etching it with an acid gel. This creates microscopic pores for the bonding material to adhere to.
- Application of Bonding Agent: A liquid bonding agent is applied to the etched tooth surface.
- Application of Composite Resin: The tooth-colored composite resin is applied in layers, carefully sculpted to match the natural contours of your tooth and fill in eroded areas or cover spots.
- Curing: Each layer of resin is hardened with a special curing light.
- Shaping and Polishing: Once all layers are applied and hardened, the dentist meticulously shapes and polishes the bonded material to ensure a natural look and feel, and proper bite. This entire process usually takes 30-60 minutes per tooth.
Other procedures like veneers or crowns involve more extensive tooth preparation (shaping the tooth), taking impressions for lab fabrication, and multiple appointments.
Step 5: Follow-up and Maintenance
- Regular Dental Check-ups: Consistent visits (every 3-6 months initially, then annually) are essential to monitor your oral health, assess the longevity of restorations, and check for any new signs of erosion.
- Oral Hygiene Education: Your dentist and hygienist will reinforce proper brushing techniques (using a soft-bristle brush, avoiding aggressive scrubbing, especially after an acidic event), flossing, and the use of fluoride products.
- Ongoing GERD Management: Continue to work with your medical doctor to ensure your GERD remains well-controlled.
Pro Tip: After an acidic reflux episode, resist the urge to brush immediately. The enamel is temporarily softened by acid, and brushing can cause more damage. Instead, rinse your mouth thoroughly with water or a fluoride mouthwash and wait at least 30-60 minutes before brushing.
Cost and Insurance
Understanding the financial aspects of treating gerd teeth is crucial, as the costs can vary significantly based on the severity of the damage and the chosen restorative treatments. All costs provided are average US ranges and can vary by region, dentist, and complexity.
Average US Cost Ranges for Treatments:
| Treatment Type | Average Cost per Tooth (USD) | Common Range (USD) |
|---|---|---|
| Fluoride Treatment (in-office) | $50 | $30 - $70 |
| Dental Sealant | $45 | $30 - $60 |
| Dental Bonding (Composite) | $250 | $100 - $400 |
| Composite Filling (for decay) | $150 | $90 - $350 |
| Inlay (Porcelain/Composite) | $750 | $650 - $1,200 |
| Onlay (Porcelain/Composite) | $900 | $800 - $1,500 |
| Porcelain Veneer | $1,700 | $900 - $2,500 |
| Porcelain/Zirconia Crown | $1,500 | $800 - $3,000 |
| Root Canal Treatment (Molar) | $1,200 | $700 - $2,000 |
| Dental Implant (incl. abutment, crown) | $4,500 | $3,000 - $6,000+ |
Insurance Coverage Details:
- Preventative Care: Most dental insurance plans cover 80-100% of preventative services like fluoride treatments, regular check-ups, and cleanings. This is a key reason to maintain regular dental visits.
- Basic Restorative Care: Procedures like dental bonding (especially to restore function or cover spots like decalcification white calcium spots on teeth that are causing sensitivity) and basic fillings are usually covered at 50-80% after your deductible.
- Major Restorative Care: Crowns, onlays, inlays, and root canals are generally covered at 50% by most plans. However, there are often annual maximums (typically $1,000-$2,000) that you may quickly reach if multiple teeth require extensive work.
- Cosmetic Procedures: Porcelain veneers are often considered cosmetic and may not be covered by insurance at all, or only to a very limited extent if there's a clear functional need documented by the dentist.
- Dental Implants: Coverage for implants varies greatly. Some plans offer partial coverage, treating it similarly to a major restorative procedure, while others offer no coverage at all.
Pro Tip: Always submit a pre-treatment estimate to your insurance company for major procedures. This will clarify your exact out-of-pocket costs before you commit to treatment.
Payment Plans and Financing Options:
If insurance doesn't cover the full cost or if you reach your annual maximum, several options are available:
- In-Office Payment Plans: Many dental offices offer interest-free payment plans, allowing you to pay for treatment over several months.
- Third-Party Financing: Companies like CareCredit or LendingClub provide healthcare credit cards or loans, often with low or 0% interest for a promotional period.
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): These tax-advantaged accounts allow you to save money specifically for healthcare expenses, including dental work.
- Dental Schools: University dental schools often provide services at a reduced cost, performed by supervised students.
- Community Dental Clinics: Some non-profit or government-funded clinics offer sliding scale fees based on income.
Recovery and Aftercare
Once your gerd teeth have received restorative treatment, proper recovery and ongoing aftercare are essential to ensure the longevity of your restorations and prevent further damage. This involves both dental care and continued management of your GERD.
Immediate Post-Treatment Care (Dental Restorations)
- Anesthesia Effects: If local anesthesia was used, avoid chewing until the numbness wears off to prevent accidentally biting your cheek or tongue.
- Sensitivity: It's common to experience some temporary sensitivity to hot or cold after procedures like fillings, bonding, veneers, or crowns, particularly if deeper erosion was present. This typically subsides within a few days to weeks. Over-the-counter pain relievers (e.g., ibuprofen, acetaminophen) can help manage discomfort.
- Temporary Restorations: If you received a temporary crown or veneer, be gentle with it. Avoid sticky or hard foods that could dislodge it. If it comes off, contact your dentist immediately.
- Bite Adjustment: If your bite feels "off" after a restoration, contact your dentist. A slight adjustment can prevent discomfort and potential damage to the restoration or opposing teeth.
Long-Term Dental Aftercare
- Maintain Excellent Oral Hygiene:
- Brush Gently, but Thoroughly: Use a soft-bristle toothbrush and non-abrasive fluoride toothpaste. Brush twice daily for two minutes.
- Floss Daily: Flossing removes plaque and food particles from between teeth and around restorations, areas where acid can still contribute to decay.
- Use Fluoride Mouthwash: A fluoride rinse can provide an extra layer of protection against demineralization.
- Protect Your Restorations:
- Avoid Hard/Sticky Foods: Be mindful of extremely hard candies, ice, or sticky caramels that can chip or dislodge restorations.
- Address Bruxism (Teeth Grinding): If you grind or clench your teeth, especially at night, your dentist may recommend a custom nightguard. Grinding can wear down both natural teeth and restorations, especially those weakened by erosion.
- Regular Dental Check-ups: Continue to visit your dentist every six months, or more frequently if recommended, for professional cleanings and examinations. Your dentist will monitor the health of your restored teeth and look for any new signs of erosion.
Ongoing GERD Management
- Adhere to Medical Advice: Continue with any prescribed GERD medications and follow your physician's recommendations for lifestyle and dietary changes. Consistent management of your reflux is the single most important factor in preventing further dental damage.
- Monitor Symptoms: Pay attention to any recurrence or worsening of GERD symptoms. If they return, consult your medical doctor promptly.
- Hydration: Drink plenty of water throughout the day, especially after meals, to help rinse away residual acids and promote saliva production.
- Chew Sugar-Free Gum: Chewing sugar-free gum after meals can stimulate saliva flow, which helps neutralize acids and remineralize enamel. Look for gums with xylitol.
Pro Tip: If you're managing bulimia teeth signs, consistent communication with both your dental and medical health teams, including therapists, is paramount. Continued vigilance against acid exposure, both internal and external, is key to preventing relapse of erosion.
Prevention
Preventing gerd teeth primarily involves controlling the underlying GERD and implementing specific oral hygiene practices to protect your enamel.
1. Control Your GERD
This is the most critical preventative step. Work closely with your medical doctor or gastroenterologist.
- Dietary Modifications:
- Identify and Avoid Trigger Foods: Common culprits include fatty foods, spicy foods, acidic foods (citrus, tomatoes), chocolate, peppermint, garlic, onions, caffeine, alcohol, and carbonated beverages.
- Eat Smaller, More Frequent Meals: This reduces the volume of food in the stomach at any one time.
- Avoid Eating Close to Bedtime: Allow at least 2-3 hours after eating before lying down.
- Lifestyle Changes:
- Maintain a Healthy Weight: Excess weight puts pressure on the stomach, increasing reflux.
- Elevate Your Head During Sleep: Use a wedge pillow to raise your head and torso by 6-8 inches.
- Quit Smoking: Nicotine relaxes the LES.
- Avoid Tight Clothing: Clothes that constrict the abdomen can worsen reflux.
- Stress Management: While not a direct cause, stress can exacerbate GERD symptoms.
- Medication Adherence: Take prescribed GERD medications (antacids, H2 blockers, PPIs) as directed by your doctor.
2. Optimize Oral Hygiene and Protection
Even with GERD under control, specific oral care practices can further protect your teeth.
- Don't Brush Immediately After Reflux: Enamel is temporarily softened by acid. Brushing immediately can cause more damage. Instead, rinse your mouth thoroughly with water or a fluoride mouthwash. Wait at least 30-60 minutes before brushing.
- Use a Soft-Bristle Toothbrush: Gentle brushing with a soft-bristle brush and non-abrasive fluoride toothpaste is key to prevent further enamel wear.
- Fluoride is Your Friend:
- Fluoride Toothpaste: Use toothpaste containing fluoride to strengthen enamel.
- Fluoride Mouthwash: Incorporate a daily fluoride mouthwash into your routine.
- Prescription Fluoride Products: Your dentist may prescribe higher-strength fluoride toothpaste or gels for extra protection, especially if you have sensitive or early eroded teeth, or decalcification white calcium spots on teeth.
- In-Office Fluoride Treatments: Regular professional fluoride applications by your dentist are highly beneficial.
- Chew Sugar-Free Gum: Chewing sugar-free gum after meals stimulates saliva flow, which is a natural acid neutralizer and helps to remineralize enamel. Look for gum containing xylitol.
- Avoid Excessive Acidic Foods/Drinks: Even if you don't have GERD, frequent consumption of sodas, sports drinks, fruit juices, and sour candies can cause erosion. Limit their intake and rinse your mouth with water afterward. If you do consume them, use a straw to minimize contact with teeth.
- Regular Dental Check-ups: Visit your dentist every six months for professional cleanings and examinations. They can detect early signs of erosion and provide preventative treatments. The ADA (American Dental Association) strongly recommends regular check-ups and cleanings for optimal oral health.
Pro Tip: If you experience dry mouth, discuss it with your dentist and physician. Saliva substitutes or specific oral hygiene products can help compensate for reduced saliva flow and protect your enamel.
Risks and Complications
Neglecting the dental effects of GERD can lead to a cascade of worsening oral health issues, making timely intervention crucial.
- Increased Tooth Sensitivity: As enamel erodes and exposes the underlying dentin, teeth become hypersensitive to hot, cold, sweet, and even acidic foods and drinks. This can significantly impact your comfort and dietary choices.
- Increased Risk of Dental Caries (Cavities): While acid erosion itself is not a cavity, the thinning enamel makes teeth more susceptible to bacterial acid attacks, leading to cavities. Once dentin is exposed, decay can progress much faster.
- Changes in Tooth Appearance: Erosion can lead to yellowing (exposed dentin), translucency of enamel edges, and alterations in the shape and length of teeth, affecting the aesthetics of your smile. This can be particularly distressing if front teeth are affected.
- Chipping and Fractures: Eroded enamel and exposed dentin weaken the tooth structure, making teeth more prone to chipping, cracking, or breaking, even from normal chewing forces. This can lead to sharp edges or loss of significant tooth structure.
- Occlusal (Bite) Problems: Severe, generalized erosion can alter the way your upper and lower teeth meet, leading to an unstable bite. This can cause issues with chewing, jaw pain (TMJ disorders), and further wear on remaining tooth structure.
- Pulpitis and Infection: If erosion progresses deep enough to reach the dental pulp (containing nerves and blood vessels), it can cause inflammation (pulpitis) and potentially lead to infection, severe pain, and the need for root canal treatment or extraction.
- Need for Extensive and Costly Restorations: Delaying treatment means more severe damage, necessitating more complex, invasive, and expensive dental procedures like multiple crowns, onlays, or even extractions and dental implants. What might have been treated with simple bonding early on could later require full mouth rehabilitation.
- Difficulty with Dental Procedures: Severely eroded teeth can be challenging to restore. There may be insufficient healthy tooth structure to support fillings, veneers, or crowns, making treatment more complex and less predictable.
- Tooth Loss: In the most severe and untreated cases, teeth can become so compromised that they cannot be saved and must be extracted, leading to permanent tooth loss.
Understanding these potential complications underscores the importance of a proactive approach to managing both your GERD and its impact on your oral health.
Comparison Tables
Table 1: Dental Restoration Options for Gerd Teeth
| Feature | Dental Bonding (Composite) | Porcelain Veneer | Dental Crown |
|---|---|---|---|
| Ideal For | Minor to moderate erosion, sensitivity, decalcification white calcium spots on teeth, small chips. | Moderate to extensive facial/lingual erosion, aesthetic improvements, protecting front teeth. | Severe erosion, significant tooth structure loss, protecting back teeth, after root canal. |
| Invasiveness | Minimally invasive (light etching, no/minimal enamel removal). | Moderately invasive (requires some enamel removal). | Highly invasive (significant enamel reduction on all sides). |
| Lifespan | 5-10 years | 10-15 years | 10-15+ years |
| Cost (per tooth) | $100 - $400 | $900 - $2,500 | $800 - $3,000 |
| Timeframe | Single visit (30-60 min). | 2-3 visits over 1-2 weeks. | 2-3 visits over 2-3 weeks. |
| Aesthetics | Good match, but can stain over time. | Excellent, highly stain-resistant. | Excellent (especially porcelain options), highly durable. |
| Durability | Moderate, susceptible to chipping or staining. | Very good, strong, but can chip. | Excellent, provides full protection and strength. |
Table 2: Strategies for GERD Management & Oral Protection
| Strategy | Description | Impact on GERD | Impact on Oral Health | Cost (approx. monthly) |
|---|---|---|---|---|
| Dietary Modification | Avoiding trigger foods (spicy, fatty, acidic, caffeine, alcohol). | Significantly reduces reflux episodes. | Reduces direct acid exposure to teeth. | Minimal to Variable |
| Lifestyle Changes | Weight loss, elevated sleeping, no eating before bed, quit smoking. | Reduces pressure on LES, strengthens LES. | Reduces frequency/severity of acid attacks on teeth. | Minimal |
| Antacids | OTC medications (e.g., Tums, Rolaids) for immediate relief. | Neutralizes stomach acid quickly. | Provides temporary protection from immediate acid exposure. | $5 - $20 |
| H2 Blockers | OTC/Prescription (e.g., Pepcid) reduces acid production. | Longer-lasting acid reduction than antacids. | Reduces total acid in reflux events over longer periods. | $10 - $40 |
| Proton Pump Inhibitors | Prescription (e.g., Omeprazole) powerfully blocks acid production. | Most effective for severe/chronic GERD. | Significantly minimizes acid exposure, allowing healing. | $15 - $100+ |
| Fluoride Treatments | Professional gels/varnishes or prescription toothpaste. | No direct impact on GERD. | Strengthens enamel, increases acid resistance, reduces sensitivity. | $0 - $70 (per application) |
| Sugar-Free Gum w/ Xylitol | Chewing after meals stimulates saliva flow. | No direct impact on GERD. | Neutralizes acids, rinses debris, promotes remineralization. | $5 - $15 |
Children / Pediatric Considerations
GERD is not just an adult condition; it can affect infants and children, and its impact on their developing dentition can be particularly concerning. Recognizing gerd teeth in children requires parents and pediatric dentists to be vigilant.
GERD in Children
Infant reflux (spitting up) is common and often resolves on its own. However, persistent or severe reflux in children can be diagnosed as GERD. Causes can include:

- Immature Digestive System: The LES in infants is not fully developed.
- Dietary Factors: Allergies to milk protein, or certain foods in older children.
- Underlying Conditions: Neurological impairments, prematurity, or genetic syndromes.
Symptoms in children can differ from adults and may include: excessive spitting up, refusal to eat, poor weight gain, arching back during or after feeds, recurrent respiratory problems (cough, wheezing), and persistent sore throat or hoarseness.
Dental Impact on Pediatric Patients
Children's primary (baby) teeth have thinner enamel than permanent teeth, making them even more susceptible to acid erosion. Damage to primary teeth can have long-term consequences:
- Early Enamel Erosion: Similar to adults, children will show signs of enamel loss, often on the lingual surfaces of primary molars and incisors.
- Increased Decay Risk: Weakened enamel is a prime target for cavities, which can spread rapidly in baby teeth.
- Sensitivity: Children may complain of tooth sensitivity, especially to cold or sweet foods.
- Impact on Permanent Teeth: Severe erosion and premature loss of primary teeth can affect the eruption pattern and alignment of permanent teeth, potentially leading to orthodontic issues.
Guidance for Parents
- Monitor Symptoms: Pay close attention to your child's feeding habits, comfort, and any signs of reflux. Discuss any concerns with your pediatrician.
- Early Dental Visits: Schedule your child's first dental visit by their first birthday. A pediatric dentist can monitor for early signs of erosion.
- Preventative Care:
- Fluoride: Ensure your child uses fluoride toothpaste (a tiny smear for children under 3, pea-sized for 3-6 years) and receives regular in-office fluoride treatments.
- Diet: Limit highly acidic drinks and snacks. Encourage water consumption.
- Brushing: Supervise brushing and ensure proper technique.
- Post-Reflux Rinse: If your child experiences reflux or vomiting, have them rinse their mouth with water immediately. Avoid brushing for at least 30 minutes.
- Communication: Maintain open communication between your pediatrician and pediatric dentist to ensure a coordinated approach to managing your child's GERD and protecting their oral health.
- Addressing Eating Disorders: In adolescents, bulimia teeth signs can manifest dramatically. If you suspect an eating disorder, seek immediate medical and psychological help. Your dentist is a key partner in this, identifying the damage and providing support.
Cost Breakdown
A dedicated look at the cost breakdown provides further clarity on the financial aspects of treating gerd teeth, especially concerning different levels of insurance coverage and alternative payment strategies.
Average US Costs (Low, Mid, High)
The range for procedures can be quite wide depending on:
- Geographic Location: Major metropolitan areas often have higher costs.
- Dentist's Experience/Specialization: Specialists may charge more.
- Materials Used: Porcelain vs. composite, different types of metal for crowns.
- Complexity: The extent of erosion and individual tooth condition.
| Procedure | Low End (USD) | Mid Range (USD) | High End (USD) |
|---|---|---|---|
| Dental Bonding (per tooth) | $100 | $250 | $400 |
| Porcelain Veneer (per tooth) | $900 | $1,700 | $2,500 |
| Porcelain Crown (per tooth) | $800 | $1,500 | $3,000 |
| Fluoride Treatment (in-office) | $30 | $50 | $70 |
| Full Mouth Reconstruction* | $15,000 | $30,000 | $80,000+ |
| *Full mouth reconstruction is needed for very severe, widespread erosion and involves a combination of crowns, veneers, inlays/onlays across most or all teeth. |
With vs. Without Insurance
- Without Insurance: You will be responsible for 100% of all costs. This is why preventative care and early intervention are so critical – addressing minor erosion is significantly cheaper than extensive damage.
- With Insurance:
- Preventative: 80-100% covered (e.g., fluoride, cleanings).
- Basic Restorative: 50-80% covered (e.g., bonding, basic fillings).
- Major Restorative: 50% covered (e.g., crowns, veneers if functionally necessary, root canals).
- Deductibles: You typically pay an annual deductible (e.g., $50-$100) before your insurance starts paying.
- Annual Maximums: Most plans have an annual limit on what they will pay (e.g., $1,000-$2,000). For extensive GERD teeth damage, you might reach this quickly, leaving significant out-of-pocket expenses.
- Waiting Periods: Some plans have waiting periods (e.g., 6-12 months) before they cover major restorative procedures.
Payment Plans and Financing Options
As discussed earlier, these are crucial for managing costs beyond insurance:
- CareCredit/LendingClub: Offer special financing for healthcare expenses.
- In-Office Plans: Discuss directly with your dental office.
- Health Savings Accounts (HSAs) & Flexible Spending Accounts (FSAs): Use pre-tax dollars for eligible medical and dental expenses.
- Dental Schools/Community Clinics: Reduced-cost services for those with limited budgets.
Cost-Saving Tips
- Prioritize Prevention: Preventing GERD teeth is always cheaper than treating them. Adhere to GERD management and optimal oral hygiene.
- Regular Check-ups: Catching erosion early means simpler, less expensive treatments.
- Understand Your Insurance: Know your plan's deductibles, annual maximums, and coverage percentages. Get pre-treatment estimates.
- Phased Treatment: If multiple teeth need work, your dentist may be able to phase out treatments over several years, allowing you to use successive annual insurance maximums.
- Shop Around (Carefully): While quality of care is paramount, comparing prices for complex procedures among reputable dentists in your area can sometimes save money.
Frequently Asked Questions
What does "gerd teeth" actually mean?
Gerd teeth refers to the dental damage, primarily acid erosion, caused by chronic exposure to stomach acid due to Gastroesophageal Reflux Disease (GERD). The acid dissolves tooth enamel, leading to sensitivity, changes in tooth shape and color, and increased vulnerability to decay.
How do I know if my teeth are being damaged by GERD?
Common signs include increased tooth sensitivity to hot, cold, or sweets, yellowing of teeth, a dull or translucent appearance, cupping or grooving on chewing surfaces, and fillings that appear "raised" because the surrounding tooth structure has worn away. A dentist can confirm the diagnosis during an exam.
Is acid erosion from GERD painful?
Initially, acid erosion might not cause pain. However, as the enamel thins and exposes the sensitive dentin underneath, many people experience increased sensitivity and sharp, fleeting pain when consuming certain foods or drinks. In severe cases where the pulp is affected, the pain can become constant and severe.
Can acid-eroded teeth be repaired?
Yes, acid-eroded teeth can be repaired. Treatment options range from fluoride treatments and dental bonding for minor erosion to veneers, crowns, or onlays for more significant damage. The best approach depends on the extent of the erosion and the specific teeth affected.
What is the average cost to fix GERD teeth?
The cost varies widely based on the severity of damage and chosen treatments. Minor issues might cost $100-$400 per tooth for bonding, while more extensive damage could require veneers ($900-$2,500 per tooth) or crowns ($800-$3,000 per tooth). Full mouth reconstruction can range from $15,000 to over $80,000.
Does dental insurance cover the repair of GERD teeth?
Dental insurance typically covers a portion of restorative treatments like bonding, fillings, crowns, and root canals, often 50-80% after a deductible, up to an annual maximum (usually $1,000-$2,000). However, highly aesthetic treatments like veneers might have limited or no coverage.
How long does it take to fix GERD teeth?
The duration depends on the treatment. Dental bonding can be done in a single 30-60 minute visit per tooth. More complex restorations like crowns or veneers usually require 2-3 visits spread over 1-3 weeks, as they involve lab fabrication. Extensive damage requiring multiple procedures can take several months.
What happens if I don't treat my GERD teeth?
Untreated GERD teeth will continue to erode, leading to worsening sensitivity, increased risk of cavities and infection, potential chipping or fracturing, changes in your bite, and ultimately, potential tooth loss. The longer you wait, the more extensive and expensive the necessary dental repairs become.
Are "decalcification white calcium spots on teeth" related to GERD?
While decalcification white calcium spots on teeth can be an early sign of enamel demineralization from various causes (e.g., plaque accumulation, fluoride excess), acid exposure from GERD can certainly contribute to localized mineral loss, leading to these white, chalky areas. Your dentist can determine the specific cause.
Can bulimia teeth signs be mistaken for GERD teeth?
Yes, the patterns of acid erosion from bulimia (repeated self-induced vomiting) and GERD can be very similar, particularly on the lingual (tongue-facing) surfaces of upper front teeth. A thorough dental and medical history is crucial for accurate diagnosis to determine the underlying cause and implement appropriate interventions.
When to See a Dentist
The insidious nature of acid erosion from GERD means that early detection is key to preventing widespread and irreversible damage. Don't wait until you're in significant pain or your teeth are visibly disfigured.
See a dentist for a routine check-up if you:
- Experience any GERD symptoms: Even if you think your reflux is mild, it can still be affecting your teeth. Regular dental visits allow your dentist to monitor for subtle changes.
- Have increased tooth sensitivity: If you notice your teeth are more sensitive to hot, cold, or sweet foods/drinks, this could be an early sign of enamel erosion.
- See changes in tooth appearance: Any yellowing, dullness, translucency, or changes in the shape or texture of your teeth warrant a dental visit. This includes noticing any decalcification white calcium spots on teeth that are new or spreading.
- Notice your existing fillings appear raised: This indicates that the natural tooth structure around the filling has eroded.
- Have frequent dry mouth: Reduced saliva flow exacerbates acid erosion, making dental monitoring even more critical.
Schedule an appointment promptly if you have any of these "red flags":
- Persistent or severe tooth pain: This could indicate advanced erosion reaching the tooth's nerve, potentially requiring more invasive treatment like a root canal.
- Chipped or fractured teeth: Especially if there's no obvious injury, this could be a sign of weakened tooth structure due to erosion.
- Difficulty chewing or changes in your bite: Significant erosion can alter how your teeth come together, leading to functional problems.
- Suspect an eating disorder: If you or a loved one exhibit bulimia teeth signs or other indications of an eating disorder, immediate consultation with both a dentist and medical/mental health professional is vital.
Emergency vs. Scheduled Appointment:
- Emergency: Severe, debilitating tooth pain, swelling around a tooth, or a significantly fractured tooth with exposed pulp generally warrants an emergency dental visit.
- Scheduled: For other signs like mild sensitivity, changes in appearance, or routine monitoring of GERD teeth, a regularly scheduled appointment is appropriate.
Remember, your dentist is your first line of defense against the oral health consequences of GERD. Regular check-ups and open communication about your health history are essential to maintaining a healthy, functional smile for life.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
What Are Calcium Deposits on Teeth
Are you one of the millions of Americans who notices a stubborn, yellowish buildup on your teeth despite regular brushing? You're likely experiencing what many refer to as "calcium deposits on teeth." This common dental concern, medically known as dental calculus or tartar, affects a vast ma
February 23, 2026
Calcium Good for Teeth: Complete Guide
More than 99% of your body's calcium resides in your bones and teeth, making it an undeniable cornerstone of skeletal and oral health. But did you know that an estimated 42% of American adults don't get enough calcium from their diet? This staggering statistic underscores a critical question
February 23, 2026
What Do Bulimia Teeth Look Like
"Bulimia teeth" refers to the specific and often severe damage that the self-induced vomiting characteristic of bulimia nervosa inflicts on a person's oral health. It's a critical issue, affecting approximately 1.5% of women and 0.5% of men in the US at some point in their lives, with many more
February 23, 2026

Erosion in Teeth: Complete Guide
Erosion in Teeth: Complete Guide
February 23, 2026