Bicuspid
4,174 words · 14 min read
Quick Definition
Another name for a premolar tooth, which has two pointed cusps on its biting surface. Adults have eight bicuspids, located between the canines and molars.
Bicuspid: Your Definitive Guide to These Crucial Chewing Teeth
Introduction
Welcome to SmilePedia.net, your trusted resource for comprehensive dental health information. Today, we delve into a fundamental component of your smile and chewing apparatus: the bicuspid tooth. Often overshadowed by their larger molar neighbors or more prominent canines, bicuspids play a vital, transitional role in your mouth's functionality. Understanding "what is a bicuspid" and its importance is key to maintaining optimal oral health and preventing common dental issues.
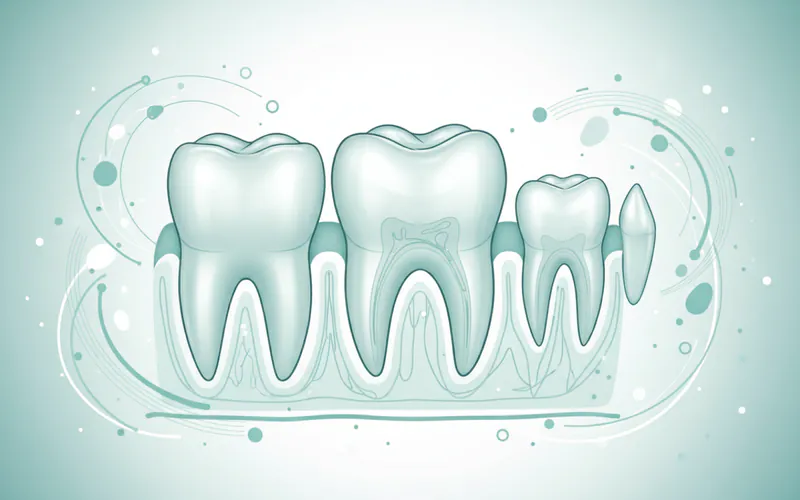
A bicuspid is a type of permanent tooth located in the middle of your dental arch, specifically situated between the sharper canine teeth and the larger molars. Its name, derived from Latin, literally means "two points," referring to the two pointed cusps prominently featured on its biting, or occlusal, surface. These unique teeth act as a bridge, designed to both tear food like canines and grind it down like molars, making them indispensable for efficient chewing and digestion.
Adults typically possess eight bicuspids – two on each side of the upper jaw and two on each side of the lower jaw. These teeth are also universally known by their more clinical term: premolars. Their strategic position and dual function mean they are frequently subjected to significant chewing forces, making them susceptible to various dental problems such as cavities, cracks, and fractures. According to the Centers for Disease Control and Prevention (CDC), over 90% of adults aged 20-64 have experienced tooth decay in their permanent teeth, and bicuspids are often among those affected due to their complex anatomy and heavy use. Recognizing their importance and understanding potential issues is paramount for everyone seeking a healthy, functional smile.
Key Takeaways:
- Bicuspids are also known as premolars. They are transitional teeth in the middle of your dental arch.
- The name "bicuspid" refers to the two pointed cusps on their biting surface.
- They are located between the canine teeth and the larger molars.
- Bicuspids are crucial for chewing, grinding, and tearing food, facilitating proper digestion.
- Adults typically have eight bicuspids – two on each side of the upper and lower jaws.
- Due to their function, bicuspids are prone to common dental issues like cavities, cracks, and fractures.
Detailed Explanation
The bicuspid tooth, or premolar, is a remarkable feat of natural engineering, perfectly positioned to handle the transition from tearing to grinding food. This section will thoroughly explore all facets of bicuspids, from their classifications to treatment and prevention.
Types and Classifications of Bicuspids
While all bicuspids share the fundamental characteristic of having two cusps, there are subtle distinctions that dentists recognize:
- First Premolars: These are located immediately adjacent to the canines. In the upper jaw (maxillary first premolars), they often have two roots, which is unique among bicuspids. Lower jaw (mandibular first premolars) typically have one root. They are primarily involved in tearing and holding food.
- Second Premolars: Situated closer to the molars, these teeth typically have a single root in both the upper and lower jaws. Their cusps are often more rounded than those of first premolars, giving them a greater grinding capacity.
Maxillary Bicuspids: The upper bicuspids generally have larger, more pronounced cusps and are often broader. Mandibular Bicuspids: The lower bicuspids can vary more in their cusp formation; the mandibular second premolar, for instance, sometimes has three cusps (though still generally considered a bicuspid/premolar based on its position and overall morphology).
Despite these minor differences, the core function remains the same: to efficiently process food particles between the canines and molars, ensuring thorough mastication before swallowing. ``
Causes and Risk Factors for Bicuspid Issues
Due to their role in chewing and specific anatomical features, bicuspids are susceptible to a range of dental problems. Understanding these causes and risk factors is crucial for prevention.
-
Dental Caries (Cavities):
- Poor Oral Hygiene: Inadequate brushing and flossing allow plaque—a sticky film of bacteria—to accumulate, producing acids that erode enamel (the tooth's hard outer layer).
- Sugary and Acidic Diet: Frequent consumption of sugary snacks, sodas, and acidic foods accelerates enamel erosion and cavity formation.
- Anatomy: The deep grooves and pits on the occlusal surface (chewing surface) of bicuspids can easily trap food particles and bacteria, making them prime locations for decay.
- Dry Mouth (Xerostomia): Reduced saliva flow, often due to medications or medical conditions, diminishes the mouth's natural ability to wash away food particles and neutralize acids, increasing cavity risk.
-
Fractures and Cracks:
- Biting on Hard Objects: Chewing ice, hard candies, or non-food items can cause sudden, forceful impacts that crack bicuspids.
- Bruxism (Teeth Grinding/Clenching): Chronic grinding or clenching, often stress-related or occurring during sleep, places immense pressure on teeth, leading to microfractures that can worsen over time.
- Large Fillings: Teeth with extensive, old fillings may have compromised structural integrity, making them more prone to cracking under chewing forces.
- Trauma: Accidents or injuries to the mouth can directly damage bicuspids.
-
Attrition and Erosion:
- Attrition: Tooth wear caused by tooth-on-tooth contact, often linked to bruxism, leading to flattened chewing surfaces.
- Erosion: Chemical wear from non-bacterial acids, such as those from highly acidic foods/drinks (citrus, sodas) or conditions like Gastroesophageal Reflux Disease (GERD) or bulimia.
-
Malocclusion (Misaligned Bite):
- Crowding: If there isn't enough space in the jaw, bicuspids can become misaligned, making them harder to clean and more susceptible to decay or abnormal wear.
- Impacted Teeth: While less common than wisdom teeth, bicuspids can sometimes fail to erupt properly.
- Missing Teeth: Gaps from missing teeth can cause adjacent teeth, including bicuspids, to shift, leading to bite problems. Bicuspids are also frequently extracted as part of orthodontic treatment to create space.
-
Gum Disease (Periodontal Disease): While not exclusive to bicuspids, untreated gum inflammation can lead to gum recession, exposing the tooth roots and increasing sensitivity and vulnerability to decay or bone loss around the tooth.
Signs and Symptoms to Watch For
Recognizing the signs of bicuspid problems early can prevent more severe complications. Pay attention to:
- Pain: Can range from a sharp, sudden pain when biting down or releasing, to a dull, constant ache. Pain that lingers after eating hot or cold foods is a red flag, indicating potential nerve involvement.
- Sensitivity: Increased sensitivity to hot, cold, sweet, or acidic foods and drinks. This can indicate enamel erosion, receding gums, or a crack.
- Visible Changes: Dark spots or visible holes (cavities), changes in tooth color, or visible cracks or chips on the tooth surface.
- Swelling or Redness: Around the affected bicuspid or in the gums surrounding it, suggesting infection or inflammation.
- Pain During Chewing: Discomfort or sharp pain when biting down on food, which may indicate a crack, cavity, or issue with a filling.
- Loose Tooth: Any noticeable movement of a bicuspid can be a sign of advanced gum disease or severe trauma.
- Bad Breath or Unpleasant Taste: Persistent bad breath (halitosis) or a foul taste in the mouth can be a symptom of infection or extensive decay.
``
Diagnosis Process — What Your Dentist Does
When you visit your dentist with concerns about a bicuspid, they will employ a systematic approach to accurately diagnose the problem:
-
Clinical Examination:
- Visual Inspection: The dentist will meticulously examine the bicuspid and surrounding teeth and gums for visible signs of decay, cracks, discoloration, swelling, or gum recession.
- Dental Probe and Mirror: A small explorer tool is used to gently check for soft spots (cavities) or rough edges, while a mirror provides a comprehensive view of all tooth surfaces.
- Percussion Test: Tapping on the tooth can help identify inflammation or infection in the tissues surrounding the tooth root.
- Palpation: Gentle pressing on the gums around the tooth can reveal swelling or tenderness.
-
Dental X-rays:
- Bitewing X-rays: These are commonly used to detect cavities between teeth (interproximal cavities) that aren't visible during a clinical exam.
- Periapical X-rays: Provide a detailed view of the entire tooth, from the crown to the end of the root, and the surrounding bone, useful for detecting root infections, abscesses, or bone loss.
- Panoramic X-rays: Offer a broad overview of the entire mouth, including all teeth, jaws, and surrounding structures, useful for overall assessment of crowded or impacted teeth.
-
Transillumination: A bright fiber-optic light can be shone through the tooth to reveal cracks or fractures that might otherwise be invisible.
-
Pulp Vitality Testing:
- Cold Test: A cold stimulus (like an ice stick) is applied to the tooth to assess the vitality of the pulp (the tooth's innermost nerve and blood vessel tissue). A healthy tooth will react briefly, while an inflamed or necrotic pulp will have a prolonged or absent response.
- Electric Pulp Tester: A small electrical current is used to stimulate the nerve, helping to determine if the pulp is alive.
-
Occlusal Analysis: The dentist will check your bite to identify any premature contacts or grinding patterns that might be contributing to tooth wear or fractures.
Treatment Options with Pros, Cons, and Costs
The treatment for a bicuspid issue depends entirely on the nature and severity of the problem. Here's an overview of common treatments:
| Treatment | Purpose | Pros | Cons | Average Cost (Without Insurance, US) |
|---|---|---|---|---|
| Dental Filling | Small to moderate cavities, minor chips. | Restores tooth structure, prevents further decay, relatively quick and affordable. | Not suitable for large defects or severe fractures; lifespan varies by material (amalgam vs. composite). | $50 - $450 |
| Dental Crown | Large cavities, extensive fractures, post-root canal, severely weakened tooth. | Protects the weakened tooth, restores full function and aesthetics, highly durable (5-15+ years). | More invasive (requires tooth reduction), higher cost, can require multiple visits. | $800 - $2,500+ |
| Root Canal Therapy (Endodontics) | Infected or inflamed pulp, deep decay reaching the nerve, severe trauma. | Saves the natural tooth, eliminates pain and infection, prevents need for extraction. | Can be a lengthy procedure, often requires a crown afterward for protection, higher cost, potential for post-treatment sensitivity. | $700 - $1,500+ (bicuspid) |
| Tooth Extraction | Severely damaged, infected, or impacted tooth beyond repair; orthodontic space creation. | Eliminates source of pain/infection, can be a definitive solution for untreatable teeth. | Loss of natural tooth, can lead to shifting teeth, bone loss over time, requires replacement (implant, bridge) to restore function and aesthetics, which adds significant cost. | $75 - $650 |
| Orthodontics | Misaligned bicuspids, crowded teeth, bite correction. | Improves alignment, bite function, aesthetics, easier oral hygiene. | Long treatment duration (months to years), significant cost, requires patient compliance (retainers). | $3,000 - $8,000+ |
| Dental Sealants | Prevention of pit and fissure decay. | Non-invasive, highly effective in preventing cavities in deep grooves, especially in children/teens. | Only effective on chewing surfaces, requires good isolation during application, can chip or wear off over time (needs reapplication). | $30 - $70 per tooth |
Cost Ranges in the US (with/without insurance): Dental costs can vary significantly based on your location, the dentist's fees, and the complexity of the procedure. The figures above represent average costs without insurance.
- With Dental Insurance: Most dental insurance plans cover a portion of restorative treatments.
- Fillings: Typically covered at 50-80% after deductible.
- Crowns: Often covered at 50% after deductible.
- Root Canal Therapy: Usually covered at 50% after deductible.
- Extractions: Can be covered at 50-80% depending on if it's considered basic or major.
- Orthodontics: Some plans include orthodontic benefits, often with a lifetime maximum and typically covering 25-50%.
- Sealants: Often fully covered for children, sometimes partially for adults.
- It's crucial to check your specific policy for exact coverage details and annual maximums.
Step-by-Step: What to Expect During Treatment
While each procedure is unique, here's a general overview of what you might expect for common bicuspid treatments:
-
Dental Filling:
- Numbing: Local anesthetic is applied to numb the tooth and surrounding area.
- Decay Removal: The dentist uses a high-speed handpiece to carefully remove all decayed or damaged tooth structure.
- Preparation: The tooth is shaped and cleaned for the filling material.
- Filling Placement: For composite fillings, a bonding agent is applied, and the resin is layered and hardened with a curing light. Amalgam is packed into the cavity.
- Shaping and Polishing: The filling is shaped to match your bite and polished smooth. The entire process typically takes 30-60 minutes.
-
Dental Crown:
- Numbing: Local anesthetic is administered.
- Tooth Preparation: The tooth is precisely reshaped by removing a layer of enamel and sometimes dentin (the layer beneath enamel) to create space for the crown.
- Impressions: Digital or traditional putty impressions are taken of your prepared tooth and opposing teeth. These are sent to a dental lab to custom-fabricate your crown.
- Temporary Crown: A temporary crown is placed to protect the tooth while the permanent one is being made.
- Placement of Permanent Crown (Second Visit): Once the custom crown arrives, the temporary is removed, and the permanent crown is cemented into place after checking its fit and bite.
-
Root Canal Therapy:
- Numbing and Isolation: Local anesthetic is given, and a rubber dam is placed around the tooth to keep it dry and free of bacteria.
- Access: A small opening is drilled into the crown of the tooth to access the infected pulp chamber.
- Pulp Removal: Special instruments are used to carefully remove the infected or inflamed pulp, nerves, and blood vessels from the pulp chamber and root canals.
- Cleaning and Shaping: The canals are thoroughly cleaned, disinfected, and shaped to prepare them for filling.
- Filling and Sealing: The cleaned canals are filled with a biocompatible material, typically gutta-percha, and sealed.
- Restoration: The access opening is sealed with a temporary or permanent filling. A dental crown is almost always recommended afterward to protect the weakened tooth.
-
Tooth Extraction:
- Numbing: The area is thoroughly numbed with local anesthetic.
- Loosening the Tooth: The dentist gently wiggles the tooth back and forth using an instrument called an elevator to loosen it from its socket.
- Removal: Dental forceps are used to grasp and remove the tooth.
- Aftercare: Gauze is placed to control bleeding, and post-operative instructions are provided.
Recovery Timeline and Aftercare
Recovery varies based on the treatment performed:
-
Fillings:
- Recovery: Numbness typically wears off within 2-4 hours. You can generally eat once the numbness subsides, but avoid chewing on the treated side for a day or two if possible.
- Aftercare: Maintain regular brushing and flossing. Minor sensitivity to hot/cold for a few days is normal.
-
Crowns:
- Recovery: Some sensitivity to hot/cold and pressure is common for 1-2 weeks after the temporary and permanent crown placements.
- Aftercare: Avoid sticky or very hard foods on the temporary crown. Once the permanent crown is placed, resume normal oral hygiene.
-
Root Canal Therapy:
- Recovery: Discomfort or mild pain for several days after the procedure is normal and manageable with over-the-counter pain relievers.
- Aftercare: Avoid chewing on the treated tooth until the permanent crown is placed. Maintain excellent oral hygiene.
-
Extraction:
- Recovery: Initial bleeding control is crucial for the first few hours. Swelling and discomfort peak in 24-48 hours and usually subside within 3-5 days. Complete soft tissue healing takes 7-10 days, bone healing takes months.
- Aftercare: Follow all post-operative instructions diligently: bite on gauze, avoid vigorous rinsing/spitting for 24 hours, eat soft foods, avoid straws and smoking for at least 48 hours (to prevent dry socket), and take prescribed medications.
Prevention Strategies for Bicuspid Health
Preventing issues with your bicuspids is far easier and less costly than treating them.
- Consistent Oral Hygiene:
- Brush twice daily for at least two minutes each time with a fluoride toothpaste.
- Floss daily to remove plaque and food debris from between teeth and below the gumline.
- Regular Dental Check-ups and Cleanings: Visit your dentist every six months for professional cleaning and examination. Early detection of problems allows for less invasive treatment.
- Balanced Diet: Limit sugary and acidic foods and drinks, which contribute to enamel erosion and decay. Opt for water, fruits, vegetables, and dairy.
- Fluoride: Ensure adequate fluoride intake through fluoridated water, toothpaste, and mouthwash to strengthen enamel.
- Dental Sealants: For children and even some adults with deep grooves on their bicuspids, dental sealants can be applied to create a protective barrier against decay-causing bacteria.
- Mouthguards:
- If you grind or clench your teeth (bruxism), a custom-fitted nightguard can protect your bicuspids from excessive wear and fracture.
- For sports activities, a protective athletic mouthguard is essential to prevent dental trauma.
- Avoid Hard Foods and Habits: Refrain from chewing on ice, hard candies, or using your teeth as tools to open packages.
For Parents / Pediatric Considerations
While bicuspids are permanent teeth, their development and care begin long before they erupt.
- Eruption Timeline: Permanent bicuspids typically erupt into the mouth around ages 10-12, replacing the primary (baby) molars. The first permanent premolars usually appear between 10-11 years, followed by the second premolars between 10-12 years.
- Importance of Primary Molars: The health of a child's primary molars directly impacts the healthy eruption and alignment of their permanent bicuspids. Early loss of baby molars due to decay can lead to space loss, causing permanent bicuspids to erupt out of alignment.
- Dental Sealants: Bicuspids, like molars, often have deep grooves on their chewing surfaces where food particles and bacteria can easily accumulate. Applying dental sealants to newly erupted permanent bicuspids is a highly effective preventive measure against cavities. Sealants are thin, plastic coatings painted onto the chewing surfaces.
- Orthodontic Space: Bicuspids are often involved in orthodontic treatment. In cases of severe crowding, one or more bicuspids (most commonly the first premolars) may be extracted to create necessary space for other teeth to align properly, achieving a balanced and functional bite. Parents should discuss these options thoroughly with an orthodontist.
- Trauma: Children and teenagers are active, making them prone to dental injuries. Encourage the use of mouthguards during sports to protect bicuspids and other teeth from trauma.
Frequently Asked Questions
How much does bicuspid treatment cost?
The cost of treating a bicuspid varies significantly depending on the specific issue and the required procedure. A simple filling might range from $50 to $450, while a dental crown could cost $800 to $2,500+. Root canal therapy for a bicuspid typically ranges from $700 to $1,500+, not including the cost of the necessary crown afterward. Extractions range from $75 to $650. These are average costs without dental insurance in the US, and specific fees can differ by location and dental practice.
Is bicuspid treatment painful?
Modern dental procedures prioritize patient comfort. For most treatments like fillings, crowns, and root canals, the area around the bicuspid will be thoroughly numbed with local anesthetic, meaning you should not feel pain during the procedure itself. Afterward, some discomfort, soreness, or sensitivity is common, especially after more invasive treatments like root canals or extractions. This post-treatment pain is usually manageable with over-the-counter pain relievers and typically subsides within a few days.
How long does bicuspid treatment take?
The duration of treatment depends on the procedure. A routine dental filling for a bicuspid usually takes 30-60 minutes. A dental crown typically requires two appointments: the first for tooth preparation and impressions (about 60-90 minutes), and the second for permanent crown placement (about 30-60 minutes), usually 1-3 weeks later. Root canal therapy for a bicuspid can often be completed in a single appointment of 60-90 minutes, or sometimes two shorter appointments. A simple extraction can be as quick as 20-30 minutes.
Are there alternatives to bicuspid extraction?
In many cases, yes. Unless a bicuspid is severely damaged, fractured beyond repair, or heavily impacted, dentists often strive to save the natural tooth. Alternatives to extraction include:
- Root Canal Therapy: For infected or severely inflamed pulp, saving the tooth from extraction.
- Dental Crowns: To protect and restore a tooth with extensive decay or fracture.
- Orthodontic Treatment: Sometimes malpositioned bicuspids can be corrected through braces or aligners rather than removal. The decision to extract is usually a last resort when other restorative options are not viable or would not provide a long-term solution.
Does dental insurance cover bicuspid treatments?
Most dental insurance plans do cover a portion of bicuspid treatments, but the coverage percentage varies widely depending on your specific plan. Generally:
- Preventive care (like sealants for children) is often covered at 80-100%.
- Basic restorative procedures (like fillings, simple extractions) are typically covered at 50-80%.
- Major procedures (like crowns, root canals, complex extractions) are usually covered at 25-50%. Orthodontic coverage, if included, often has a separate lifetime maximum. It's essential to consult your insurance provider directly or review your policy details to understand your specific coverage, deductibles, and annual maximums.
What is the difference between a bicuspid and a molar?
The primary differences between a bicuspid (premolar) and a molar lie in their location, size, and number of cusps (pointed projections on the chewing surface):
- Location: Bicuspids are located between the canines and molars. Molars are the large teeth at the very back of the mouth.
- Number of Cusps: Bicuspids typically have two cusps (hence "bicuspid"). Molars typically have four or five cusps.
- Size and Function: Bicuspids are smaller than molars and serve as transitional teeth, aiding in both tearing and initial grinding. Molars are the largest and strongest teeth, designed for heavy grinding and crushing of food.
- Roots: Most bicuspids have one root (upper first premolars sometimes have two), while molars typically have two or three roots.
Can bicuspids be sealed?
Yes, dental sealants can be applied to bicuspids, particularly if they have deep grooves or pits on their chewing surfaces. Sealants create a protective barrier that prevents food particles and bacteria from accumulating in these crevices, effectively reducing the risk of cavities. While often associated with children's molars, sealants can be beneficial for adults as well, especially on newly erupted permanent teeth or teeth with a high risk of decay.
How important are bicuspids?
Bicuspids are incredibly important for several reasons:
- Chewing Efficiency: They play a crucial role in the initial stages of breaking down food, facilitating proper digestion.
- Maintaining Bite and Alignment: They help maintain the proper spacing and alignment of adjacent teeth. Loss of a bicuspid can lead to shifting of other teeth, causing bite problems and potential jaw issues.
- Facial Structure: Like all teeth, bicuspids contribute to supporting your facial structure and maintaining the aesthetic appearance of your smile and jawline.
- Transition from Tearing to Grinding: Their unique two-cusp design allows them to bridge the gap between the tearing action of canines and the grinding action of molars, making the entire chewing process more efficient.
When to See a Dentist
Knowing when to seek professional dental care is critical for your bicuspid health.
Emergency Situations (See a dentist immediately or go to an emergency dental clinic):
- Severe, Unrelenting Pain: If you experience sudden, intense, or throbbing pain in a bicuspid that doesn't subside with over-the-counter pain relievers.
- Swelling: Any rapid swelling in your face, jaw, or gums around a bicuspid, which could indicate a serious infection or abscess.
- Trauma: A bicuspid that has been knocked out, severely fractured, or displaced due to an accident or injury.
- Difficulty Swallowing or Breathing: These symptoms, especially when accompanied by pain or swelling, could indicate a spreading infection that requires immediate medical attention.
Urgent/Routine Care (Schedule an appointment as soon as possible):
- Persistent Sensitivity: If your bicuspid is sensitive to hot, cold, or sweet for more than a few days, or if the sensitivity lingers.
- Dull, Constant Ache: A persistent, low-grade ache in a bicuspid or surrounding area.
- Visible Decay or Holes: Any dark spots, pits, or visible holes in your bicuspid's surface.
- Pain When Chewing: Discomfort or sharp pain specifically when you bite down or chew food.
- Broken Filling or Crown: If an existing filling or crown on a bicuspid comes loose or breaks.
- Food Impaction: If food frequently gets stuck between your bicuspids, causing discomfort.
Ultimately, regular dental check-ups every six months are your best defense. Your dentist can identify potential issues with your bicuspids (and other teeth) before they become painful or severe, ensuring your smile remains healthy and functional for years to come.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.