Posterior Teeth
4,457 words · 15 min read
Quick Definition
The back teeth including premolars and molars, designed for crushing, grinding, and chewing food. Adults have 20 posterior teeth.
When you flash a smile, the teeth you typically see are your front teeth. But just behind them lies a crucial set of workhorses known as your posterior teeth. These are the unsung heroes of your oral cavity, essential for breaking down food and maintaining the integrity of your bite. For anyone searching "what is posterior teeth" or "posterior teeth dental," this comprehensive guide will demystify these vital structures and highlight their significance for your overall dental health.
Posterior teeth refers to the teeth located at the back of your mouth, specifically the premolars (also known as bicuspids) and molars. Unlike the sharp, cutting anterior teeth at the front, posterior teeth boast broad, flat surfaces designed to efficiently crush, grind, and chew food into manageable pieces for digestion. In adults, a healthy set of dentition typically includes 20 posterior teeth – 8 premolars and 12 molars (including wisdom teeth, if present). They are fundamental to chewing efficiency, speech articulation, and maintaining facial structure. Neglecting the health of your posterior teeth dental can lead to significant problems, from digestive issues to complex dental procedures. Understanding their function and how to care for them is paramount for a lifetime of healthy smiles.
Key Takeaways:
- Posterior teeth are the premolars and molars located at the back of your mouth.
- Their primary function is crushing, grinding, and chewing food.
- Adults typically have 20 posterior teeth (8 premolars, 12 molars).
- They are crucial for efficient digestion, maintaining bite alignment, and supporting facial structure.
- Due to their complex surfaces, posterior teeth are more susceptible to decay and require diligent oral hygiene.
- Regular dental check-ups and cleanings are essential for preventing issues with your posterior teeth dental.
Detailed Explanation
Types and Classifications of Posterior Teeth
The posterior teeth are broadly categorized into two main types, each with distinct characteristics and roles in the chewing process:
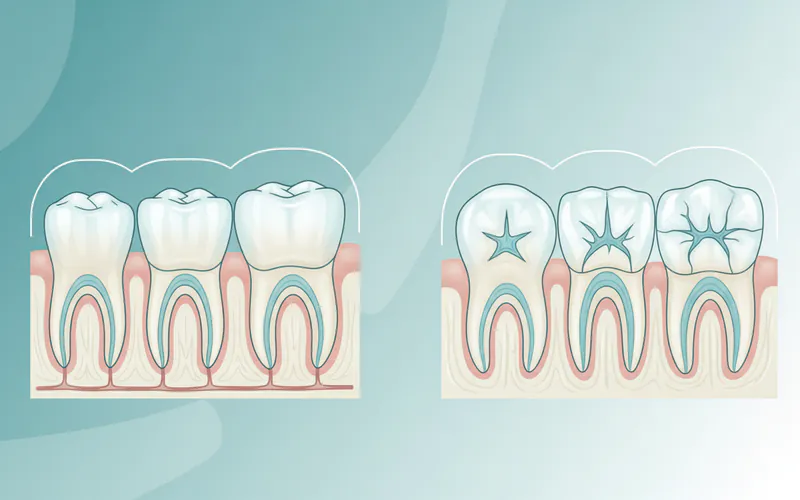
-
Premolars (Bicuspids): Situated immediately behind the canine teeth (the pointed teeth flanking the incisors), there are eight premolars in a complete adult dentition – two on each side of the upper and lower jaws. They are larger and stronger than the anterior teeth but smaller than molars. Their distinguishing feature is typically two cusps (points or bumps on the chewing surface), hence their alternative name, bicuspids. Premolars act as transitional teeth, helping to tear and grind food that has been bitten by the incisors and canines, preparing it for the molars. They play a vital role in maintaining the vertical dimension of the bite.
- First Premolars: Located closest to the canines.
- Second Premolars: Located behind the first premolars.
-
Molars: These are the largest and strongest teeth, positioned at the very back of the mouth. A complete adult set usually contains 12 molars – three on each side of the upper and lower jaws. Molars have broad, flat chewing surfaces with four or five cusps, making them ideally suited for the heavy-duty grinding and crushing of food.
- First Molars: Erupt around age 6 and are often called the "6-year molars." They are crucial for establishing the bite.
- Second Molars: Erupt around age 12 and are known as the "12-year molars."
- Third Molars (Wisdom Teeth): These are the furthest back teeth, typically erupting between ages 17 and 25. They are often problematic due to lack of space in the jaw, leading to impaction and requiring extraction. Not everyone develops all four wisdom teeth, and many have them removed proactively.
Causes and Risk Factors for Posterior Teeth Issues
The unique structure of posterior teeth, with their complex grooves and fissures, makes them particularly susceptible to certain dental problems. Several factors contribute to the risk of issues:
- Dental Caries (Cavities): The intricate pits and fissures on the chewing surfaces of molars and premolars can easily trap food particles and bacteria, making them prime targets for decay. These areas are also harder to clean thoroughly with a toothbrush.
- Periodontal (Gum) Disease: Poor oral hygiene can lead to plaque and tartar buildup around the gumline of posterior teeth, causing inflammation (gingivitis) and, if left untreated, advancing to periodontitis. This can result in bone loss, loose teeth, and eventually tooth loss.
- Bruxism (Teeth Grinding/Clenching): Chronic grinding or clenching, often stress-related or occurring during sleep, places immense pressure on the posterior teeth. This can lead to excessive wear, cracks, fractures, sensitivity, and even jaw pain (TMJ disorders).
- Trauma: Although less common than for anterior teeth, posterior teeth can sustain injuries from falls, sports accidents, or biting down on hard objects, leading to chips, cracks, or fractures.
- Malocclusion (Misaligned Bite): When teeth don't align properly, certain posterior teeth may bear excessive chewing forces, leading to uneven wear, damage, or discomfort.
- Poor Oral Hygiene: Inadequate brushing and flossing are the most significant risk factors for almost all dental problems, particularly in hard-to-reach posterior teeth.
- Diet: Frequent consumption of sugary and acidic foods and drinks erodes enamel and fuels bacteria, increasing the risk of cavities in posterior teeth dental.
- Age: Enamel naturally wears down over time, making older individuals more susceptible to issues like cracks and sensitivity.
- Lack of Fluoride: Fluoride strengthens enamel, making teeth more resistant to acid attacks. Insufficient fluoride exposure can increase cavity risk.
Signs and Symptoms to Watch For
Recognizing the early signs of problems with your posterior teeth can be crucial for timely intervention and preventing more serious issues. Be vigilant for:
- Pain: This is the most common symptom. It could be a sharp pain when biting down, a dull ache, or a throbbing sensation. Pain can indicate a cavity, crack, infection, or gum inflammation.
- Sensitivity: Increased sensitivity to hot, cold, sweet, or acidic foods and drinks can be a sign of exposed dentin due to enamel erosion, gum recession, or a developing cavity.
- Visible Holes or Pits: These are clear indicators of cavities. They might appear as dark spots or actual indentations on the chewing surface or between teeth.
- Swelling or Redness around the Gums: A sign of gingivitis or periodontitis, especially if accompanied by bleeding during brushing or flossing.
- Persistent Bad Breath or Bad Taste: Can be a symptom of bacterial buildup, gum disease, or tooth decay.
- Difficulty Chewing or Biting: If chewing becomes uncomfortable or painful, it could point to a cracked tooth, a deep cavity, or a bite problem.
- Loose Teeth: A severe sign of advanced periodontal disease or trauma.
- Dark Spots or Stains: While some stains are cosmetic, dark spots on the chewing surfaces can indicate early decay.
- Jaw Pain or Headaches: Can be associated with bruxism, especially if your posterior teeth are showing signs of wear.
Diagnosis Process — What Your Dentist Does
When you visit your dentist with concerns about your posterior teeth, or during a routine check-up, they will follow a thorough diagnostic process to identify any issues:
- Comprehensive Oral Examination: Your dentist will visually inspect all your teeth, including each premolar and molar, looking for signs of decay, cracks, excessive wear, and gum disease. They will use a small mirror and a dental explorer (a fine-tipped instrument) to check the pits and fissures for softness or stickiness, which can indicate cavities.
- Periodontal Probing: A small measuring probe will be used to measure the depth of the gum pockets around each tooth. Deeper pockets (4mm or more) can indicate gum disease.
- X-rays (Radiographs): Dental X-rays are indispensable for diagnosing problems not visible to the naked eye.
- Bitewing X-rays: These are commonly taken to detect cavities between posterior teeth and to assess bone levels.
- Periapical X-rays: Used to view the entire tooth, including the root and surrounding bone, to detect infections, abscesses, or bone loss.
- Panoramic X-rays: Provide a broad view of the entire mouth, useful for assessing wisdom teeth positions, jaw structure, and overall dental health.
- Bite Assessment: Your dentist will evaluate your bite to check for any misalignments (malocclusion) or signs of bruxism that might be affecting your posterior teeth.
- Transillumination: A bright light shone through the tooth can sometimes reveal cracks or fractures.
- Pulp Testing: If an infection is suspected, tests might be performed to check the vitality of the tooth's pulp (nerve), such as applying cold or electric pulp tests.
Treatment Options with Pros, Cons, and Costs
Treatment for posterior teeth issues varies widely depending on the nature and severity of the problem. Here's an overview of common interventions:
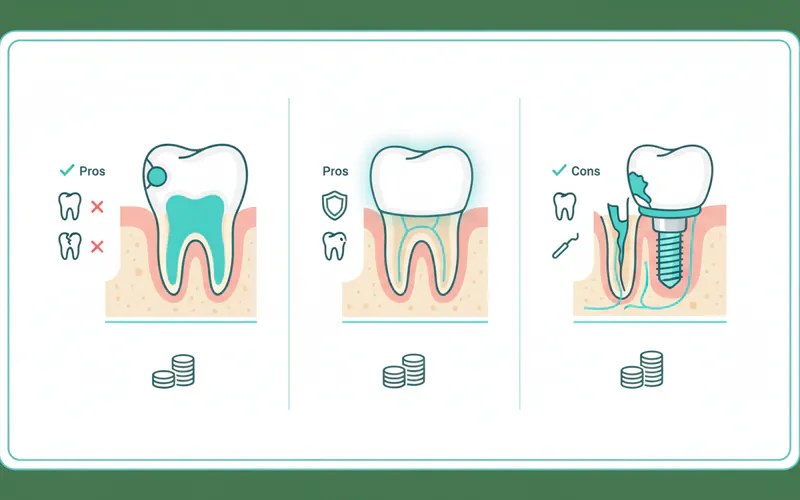
-
Dental Fillings:
- Purpose: To restore a tooth damaged by a small to medium-sized cavity.
- Pros: Restores tooth function and aesthetics, prevents further decay, relatively quick procedure.
- Cons: Not suitable for very large cavities or extensive damage; longevity depends on material (amalgam, composite, porcelain).
- Cost (US):
- Amalgam (Silver) Filling: $50 - $200 per tooth. Less common now due to aesthetics.
- Composite (Tooth-colored) Filling: $100 - $400 per tooth. More popular for aesthetics.
- With Insurance: Typically 50-80% covered.
-
Inlays and Onlays:
- Purpose: Custom-made restorations for larger cavities or damage that is too extensive for a filling but not severe enough for a full crown. Inlays fit within the cusps, onlays cover one or more cusps.
- Pros: More durable than fillings, conservative approach (preserves more tooth structure than a crown), excellent fit.
- Cons: More expensive than fillings, requires two appointments, typically made of porcelain or gold.
- Cost (US): $600 - $1,500 per tooth.
- With Insurance: Typically 20-50% covered.
-
Dental Crowns:
- Purpose: A cap placed over an entire damaged tooth (e.g., large cavity, crack, after a root canal) to restore its shape, size, strength, and appearance.
- Pros: Provides excellent strength and protection, aesthetic options (porcelain, zirconia), can significantly extend a tooth's life.
- Cons: More expensive, requires two appointments, removes more tooth structure than an inlay/onlay.
- Cost (US): $800 - $2,500 per tooth (material dependent, e.g., porcelain fused to metal, all-ceramic, zirconia).
- With Insurance: Typically 20-50% covered.
-
Root Canal Therapy:
- Purpose: To save a tooth with an infected or inflamed pulp (nerve) by removing the diseased tissue, cleaning and sealing the inside of the tooth.
- Pros: Saves the natural tooth, prevents extraction, eliminates pain.
- Cons: Can be a multi-appointment procedure, often requires a crown afterward for protection.
- Cost (US): $700 - $1,500 (for posterior teeth, which have more canals). This does not include the cost of a crown.
- With Insurance: Typically 50-80% covered for the procedure, crown coverage separate.
-
Tooth Extraction:
- Purpose: Removal of a tooth that is severely damaged, decayed beyond repair, impacted (like some wisdom teeth), or causing overcrowding.
- Pros: Eliminates source of infection/pain, prevents damage to adjacent teeth.
- Cons: Leaves a gap (which should ideally be filled to prevent shifting), can lead to bone loss, requires subsequent restoration (implant/bridge).
- Cost (US):
- Simple Extraction: $75 - $300 per tooth.
- Surgical Extraction (e.g., impacted wisdom tooth): $200 - $800+ per tooth.
- With Insurance: Typically 50-80% covered.
-
Dental Implants:
- Purpose: To replace a missing tooth by surgically placing a titanium post into the jawbone, which then supports a crown, bridge, or denture.
- Pros: Most durable and long-lasting replacement, acts like a natural tooth, preserves bone structure.
- Cons: Most expensive option, requires surgery and healing time, not suitable for everyone.
- Cost (US): $3,000 - $6,000+ per single implant (including implant, abutment, and crown).
- With Insurance: Limited or no coverage, often considered a major procedure with significant out-of-pocket costs.
-
Dental Bridges:
- Purpose: To replace one or more missing teeth by cementing a false tooth (or teeth) to crowns placed on adjacent natural teeth.
- Pros: Fills gaps, restores chewing ability and aesthetics, less invasive than implants.
- Cons: Requires modifying healthy adjacent teeth (grinding them down for crowns), can put stress on supporting teeth, not as long-lasting as implants.
- Cost (US): $1,500 - $5,000+ for a three-unit bridge (depending on materials and number of units).
- With Insurance: Typically 20-50% covered.
Step-by-Step: What to Expect During Treatment
While specific procedures vary, here's a general idea of what to expect for common posterior teeth dental treatments:
-
For a Filling (Composite):
- Numbing: Local anesthetic is applied to numb the tooth and surrounding area.
- Removal of Decay: The dentist uses a drill to remove decayed tooth structure.
- Preparation: The tooth is cleaned and sometimes etched with a mild acid for better bonding.
- Application: The composite resin is applied in layers, sculpted to the tooth's shape.
- Curing: A special light is used to harden each layer of the composite.
- Finishing: The filling is polished and adjusted to ensure a proper bite.
-
For a Crown:
- First Appointment (Preparation):
- Numbing: Local anesthetic is administered.
- Reshaping: The tooth is reshaped (filed down) to make room for the crown.
- Impressions: Molds (digital or traditional) are taken of the prepared tooth and surrounding teeth. These are sent to a dental lab.
- Temporary Crown: A temporary crown is placed to protect the prepared tooth while the permanent one is being fabricated.
- Second Appointment (Placement):
- Removal of Temporary: The temporary crown is removed.
- Fitting: The permanent crown is checked for fit, color, and bite.
- Cementation: Once satisfactory, the crown is permanently cemented onto the tooth.
- First Appointment (Preparation):
-
For Root Canal Therapy:
- Numbing: Local anesthetic is applied.
- Access: A small opening is made in the crown of the tooth to access the pulp chamber.
- Cleaning: Tiny instruments are used to remove infected pulp and clean and shape the root canals.
- Filling: The cleaned canals are filled with a rubber-like material called gutta-percha and sealed.
- Temporary Filling: A temporary filling is placed in the tooth's opening.
- Restoration: In a follow-up appointment, a permanent filling or, more commonly, a crown is placed to protect the treated tooth.
Recovery Timeline and Aftercare
Recovery and aftercare depend on the procedure:
- Fillings:
- Recovery: Numbness wears off in a few hours. Mild sensitivity to hot/cold for a few days is common.
- Aftercare: Avoid chewing on the treated tooth until numbness subsides. Maintain regular brushing and flossing.
- Inlays/Onlays & Crowns:
- Recovery: Sensitivity to temperature changes might occur for a few weeks. The bite might feel slightly different initially.
- Aftercare: Avoid sticky or hard foods on the temporary crown. Once the permanent restoration is in place, treat it like a natural tooth with diligent oral hygiene.
- Root Canal Therapy:
- Recovery: Mild soreness for a few days, manageable with over-the-counter pain relievers. Avoid chewing on the treated tooth until a permanent restoration (crown) is placed.
- Aftercare: Crucial to get the final restoration (usually a crown) promptly to prevent re-infection or fracture.
- Extractions:
- Recovery: Pain, swelling, and bleeding are common for the first 24-48 hours. Follow post-operative instructions carefully. Healing of the socket takes several weeks.
- Aftercare: Avoid vigorous rinsing, spitting, or straw use for 24-48 hours. Stick to soft foods. Manage pain with prescribed or OTC medications. Follow up with your dentist for potential tooth replacement options.
- Implants:
- Recovery: Significant healing time (3-6 months) is needed for the implant to fuse with the bone (osseointegration). Minor pain and swelling after surgery.
- Aftercare: Strict adherence to post-operative instructions, meticulous oral hygiene around the implant, and regular dental check-ups are vital for long-term success.
Prevention Strategies for Posterior Teeth
Preventing issues with your posterior teeth is far easier and less costly than treating them. A proactive approach is key:
- Maintain Excellent Oral Hygiene:
- Brush Twice Daily: Use a fluoride toothpaste and a soft-bristled brush. Pay special attention to the chewing surfaces and the gumline of your premolars and molars, where food and plaque accumulate.
- Floss Daily: Flossing is critical for cleaning between posterior teeth and below the gumline, areas your toothbrush can't reach.
- Regular Dental Check-ups and Cleanings: Visit your dentist every six months for professional cleanings and examinations. Your dentist can detect problems early, often before symptoms appear.
- Fluoride: Ensure adequate fluoride exposure through fluoridated toothpaste, mouthwash, or professional fluoride treatments.
- Dental Sealants: For children and sometimes adults, dental sealants are a highly effective preventive measure. A thin, protective coating is applied to the deep grooves and fissures of molars and premolars to prevent food and bacteria from getting trapped, drastically reducing the risk of cavities.
- Balanced Diet: Limit sugary and acidic foods and drinks. Opt for tooth-friendly snacks like fruits, vegetables, and dairy products.
- Wear a Mouthguard: If you participate in contact sports, a custom-fitted mouthguard can protect your posterior teeth from trauma. If you grind or clench your teeth (bruxism), a nightguard can prevent excessive wear and damage.
- Avoid Hard/Sticky Foods: Be cautious with extremely hard candies, ice, or sticky caramels that can crack teeth or pull out fillings.
- Quit Smoking/Tobacco Use: Tobacco products significantly increase the risk of gum disease and oral cancer, which can impact the health and longevity of your posterior teeth.
Cost Ranges in the US (with/without Insurance)
Understanding the financial aspect of dental care for posterior teeth is crucial for patients in the US. Costs vary based on geographic location, dentist's fees, and materials used.
| Procedure Type | Typical Cost Range (Without Insurance) | Estimated Cost (With PPO Insurance, 50-80% coverage) |
|---|---|---|
| Composite Filling | $100 - $400 | $20 - $200 |
| Amalgam Filling | $50 - $200 | $10 - $100 |
| Inlay/Onlay | $600 - $1,500 | $300 - $750 |
| Dental Crown | $800 - $2,500 | $400 - $1,250 |
| Root Canal (Molar) | $700 - $1,500 | $140 - $750 |
| Simple Extraction | $75 - $300 | $15 - $150 |
| Surgical Extraction | $200 - $800+ | $40 - $400+ |
| Dental Bridge (3-unit) | $1,500 - $5,000+ | $750 - $2,500+ |
| Dental Implant (Single, complete) | $3,000 - $6,000+ | $1,500 - $3,000+ (often limited coverage) |
| Dental Sealant | $30 - $70 per tooth | $0 - $35 (often 80-100% covered for children) |
Note: These are general estimates. Always get a detailed cost breakdown from your dental provider. Many insurance plans have annual maximums, deductibles, and varying coverage levels for different procedures. It's advisable to check with your insurance provider directly.
Comparison Table: Restorative Options for Posterior Teeth
When a posterior tooth is damaged, your dentist will recommend the most appropriate restoration. Here's a comparison of common options:
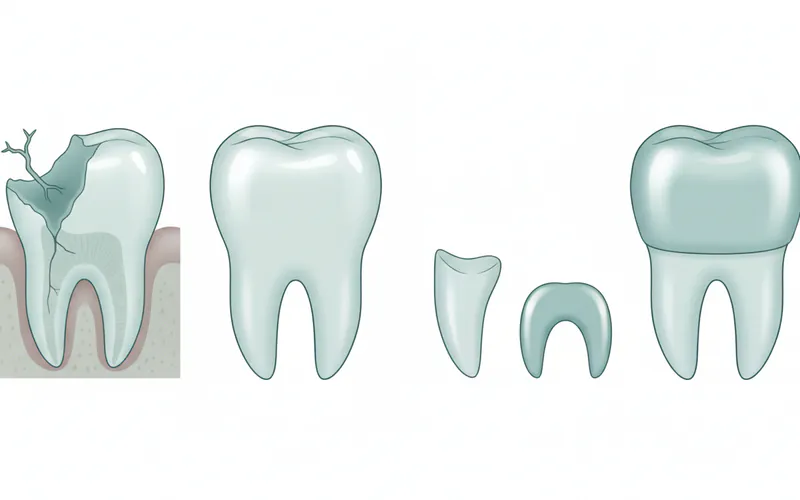
| Feature | Dental Filling (Composite) | Inlay / Onlay (Porcelain) | Dental Crown (Zirconia/Porcelain) |
|---|---|---|---|
| Damage Level | Small to moderate cavities | Moderate to large cavities, some cusp involvement | Extensive damage, cracks, post-root canal |
| Tooth Structure Preserved | High (only decay removed) | High (more than crown) | Moderate (significant tooth reshaping) |
| Strength/Durability | Good (5-10 years) | Very Good (10-15+ years) | Excellent (10-20+ years) |
| Aesthetics | Excellent (tooth-colored) | Excellent (tooth-colored) | Excellent (tooth-colored) |
| Number of Appointments | 1 | 2 | 2 |
| Cost (No Insurance) | $100 - $400 | $600 - $1,500 | $800 - $2,500 |
| Pros | Cost-effective, single visit, conservative | Durable, aesthetic, conservative than crown | Strongest, full protection, restores severe damage |
| Cons | Less durable for large defects | More expensive, 2 visits | Most invasive, most expensive, 2 visits |
For Parents / Pediatric Considerations
Posterior teeth play an especially critical role in children's oral development.
- Primary (Baby) Posterior Teeth: Children have 8 primary molars (no premolars in primary dentition) which are essential for chewing, maintaining space for permanent teeth, and guiding their eruption. Losing these primary molars prematurely due to decay or trauma can lead to space loss and misalignment of the permanent posterior teeth.
- Early Eruption of First Permanent Molars: The first permanent molars typically erupt around age 6, behind the last baby teeth. These "6-year molars" are crucial for the development of a child's bite and require immediate attention for protection.
- Dental Sealants: These thin, plastic coatings are particularly beneficial for children's posterior teeth. Applied to the chewing surfaces of molars and premolars shortly after they erupt, sealants effectively prevent food and bacteria from settling into the deep grooves and causing cavities. Studies show sealants can reduce the risk of decay by 80% in molars. They are a highly recommended preventive measure.
- Orthodontic Considerations: Early monitoring of a child's posterior teeth eruption and alignment is important. Issues like overcrowding or crossbites involving molars can impact jaw development and may require orthodontic intervention.
- Wisdom Teeth: In adolescents and young adults, wisdom teeth (third molars) may erupt. Many times, due to insufficient space, they become impacted, leading to pain, infection, or damage to adjacent second molars. Pediatric dentists or oral surgeons will monitor their development and recommend extraction if necessary.
Frequently Asked Questions
Is it more painful to have a cavity filled in a posterior tooth than an anterior tooth?
Generally, the sensation of having a cavity filled is similar for both posterior and anterior teeth once numbed. However, posterior teeth often have larger, deeper cavities due to their complex surfaces, which might require more extensive work and a longer procedure. This could lead to a bit more post-treatment sensitivity or discomfort, but during the actual procedure, local anesthetic makes it largely pain-free.
How long do posterior teeth restorations (fillings, crowns) typically last?
The lifespan of restorations varies significantly:
- Composite Fillings: 5 to 10 years, sometimes longer with excellent care.
- Amalgam Fillings: 10 to 15 years, but being phased out.
- Inlays/Onlays: 10 to 15+ years.
- Dental Crowns: 10 to 20 years, sometimes more.
- Dental Implants: Can last a lifetime with proper care, while the crown on top might need replacement after 10-15 years. Factors like oral hygiene, diet, grinding habits, and regular dental check-ups greatly influence longevity.
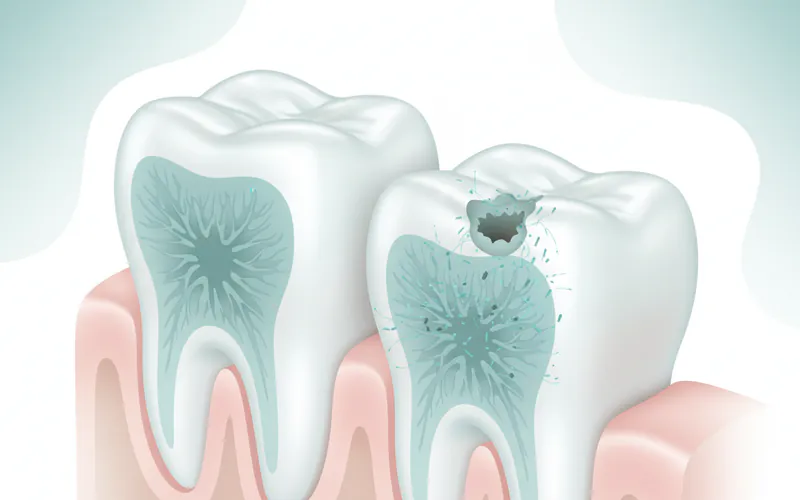
Why are posterior teeth more prone to cavities?
Posterior teeth are more susceptible to cavities primarily because of their anatomy. They have deep, intricate pits and fissures (grooves) on their chewing surfaces that are perfect traps for food particles and plaque. These areas are also harder to clean thoroughly with a toothbrush, making it easier for bacteria to thrive and cause decay. Additionally, their location at the back of the mouth makes them less accessible for cleaning.
Can I chew normally after treatment on a posterior tooth?
After a filling, you should avoid chewing on the treated tooth until the numbness wears off to prevent accidental biting of your cheek or tongue. For crowns, bridges, or root canals, you might experience some sensitivity or a slightly altered bite for a few days, but you should be able to resume normal chewing gradually. For extractions or implants, soft foods are recommended for a period, with specific dietary restrictions provided by your dentist or oral surgeon.
Are there alternatives to getting a root canal for an infected posterior tooth?
The primary alternative to a root canal for an infected tooth is extraction (removing the tooth). However, extraction is generally considered a last resort because it leaves a gap that can lead to shifting teeth, bone loss, and the need for further costly restorations like implants or bridges. Root canal therapy aims to save your natural tooth, which is always the preferred option when feasible.
Does dental insurance cover treatments for posterior teeth?
Most standard dental insurance plans in the US cover a portion of treatments for posterior teeth. Preventive care (cleanings, X-rays, sealants for children) is often covered at 80-100%. Basic restorative procedures like fillings usually have 50-80% coverage. Major restorative procedures like crowns, bridges, and root canals often have 20-50% coverage. Dental implants typically have limited or no coverage, or may fall under major restorative with lower percentage coverage. It's crucial to check your specific plan's benefits.
How do I know if my wisdom teeth need to be extracted?
Your dentist will monitor your wisdom teeth through clinical exams and X-rays, especially a panoramic X-ray. If wisdom teeth are impacted (unable to fully erupt), causing pain, infection, damaging adjacent second molars, creating cysts, or contributing to gum disease, extraction will likely be recommended. Not all wisdom teeth need to be removed; some erupt properly and function without issues.
When to See a Dentist
It's important to differentiate between routine care and urgent situations regarding your posterior teeth.
Routine Care (Schedule an Appointment Soon):
- Regular Check-ups and Cleanings: Every six months is ideal for preventing problems and catching issues early.
- Mild Sensitivity: If you notice mild, intermittent sensitivity to hot, cold, or sweets.
- New Stains or Dark Spots: These could be early signs of cavities.
- Occasional Bad Breath: Could indicate a need for better hygiene or early gum issues.
When to See a Dentist Urgently (Within 1-2 Days):
- Persistent Pain: Any toothache that doesn't go away or is severe, especially if it wakes you at night.
- Swelling: Swelling around a posterior tooth, in the gums, or in your jaw/face.
- Visible Cavity or Hole: A noticeable hole in your tooth.
- Broken or Chipped Tooth: Any significant fracture that exposes the tooth's interior or causes sharp edges.
- Lost Filling or Crown: If a restoration falls out, the exposed tooth is vulnerable.
- Pain When Biting: Consistent pain when you chew.
- Persistent Bad Taste: Could indicate infection.
Dental Emergency (Seek Immediate Care):
- Severe, Uncontrolled Pain: Pain that is excruciating and not manageable with over-the-counter pain relief.
- Facial Swelling with Difficulty Breathing or Swallowing: This could indicate a spreading infection and requires immediate medical attention.
- Traumatic Injury: A severe blow to the face or mouth that results in a knocked-out tooth or severe bleeding.
Your posterior teeth are vital for your oral health and overall well-being. Understanding their function, potential issues, and how to care for them ensures you can enjoy a lifetime of comfortable chewing and confident smiles. Regular dental visits and good home care are your best defense against problems, keeping your posterior teeth dental in excellent condition.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.