What Is a Root Canal?
Key Takeaways
- The phrase "root canal" often conjures images of pain and dread, but the reality is quite different. For millions of Americans each year, a root canal is a crucial, pain-relieving procedure that saves a damaged or infected tooth, allowing them to maintain their natural smile and oral health. Far fro
What Is a Root Canal?
The phrase "root canal" often conjures images of pain and dread, but the reality is quite different. For millions of Americans each year, a root canal is a crucial, pain-relieving procedure that saves a damaged or infected tooth, allowing them to maintain their natural smile and oral health. Far from being a painful ordeal, modern advancements in dentistry have made what is a root canal? a relatively comfortable experience, comparable to getting a routine filling. It's a highly effective endodontic treatment designed to eliminate bacterial infection from the root canal, prevent reinfection of the tooth, and save the natural tooth. Ignoring the signs of an infected tooth can lead to severe pain, abscess formation, and even the loss of the tooth. This comprehensive guide will demystify the root canal procedure, explain its symptoms, discuss costs, and provide essential information to help you understand this vital dental treatment.

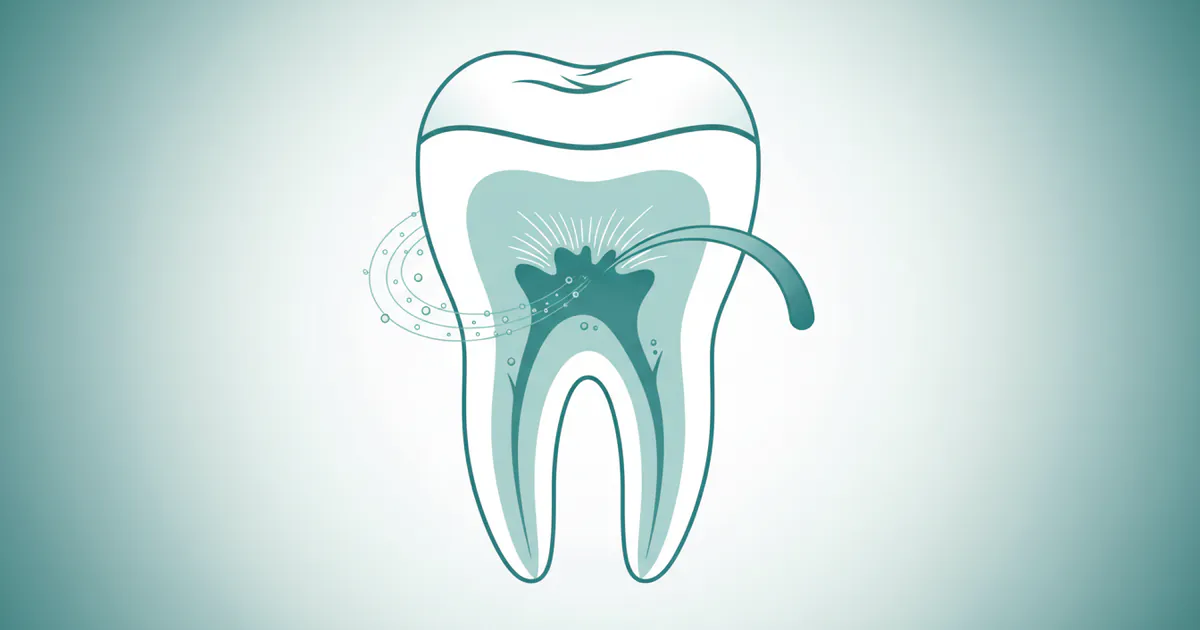
![A cross-section diagram of a tooth clearly showing the pulp chamber(/dental-anatomy/types-of-teeth-shapes-complete-guide), root canals, and surrounding bone, with an arrow pointing to an infected pulp.]
Key Takeaways:
- Purpose: A root canal (endodontic treatment) saves a tooth with infected or inflamed pulp, preventing extraction and maintaining natural function.
- Symptoms: Common root canal symptoms include persistent tooth pain, sensitivity to hot/cold, gum swelling, and discoloration of the tooth.
- Procedure: Involves removing infected pulp, cleaning and shaping the root canals, and then filling and sealing them, typically followed by a crown.
- Cost: The cost of a root canal in the US generally ranges from $700 to $1,500 for front teeth and $1,000 to $2,000+ for molars, often partially covered by dental insurance.
- Pain: The procedure is performed under local anesthesia and is generally not painful; post-procedure discomfort is manageable with over-the-counter pain relievers.
- Success Rate: With proper care, root canal treatment has a high success rate, often exceeding 95%, allowing the tooth to last a lifetime.
- Recovery: Recovery is typically quick, with most patients returning to normal activities within a day. A permanent crown is essential for long-term protection.
What It Is: Understanding the Root Canal Procedure
A root canal, clinically known as endodontic treatment, is a dental procedure designed to treat infection or inflammation in the dental pulp. To truly understand why this treatment is so important, it helps to know a bit about tooth anatomy. Each of your teeth contains a soft core called the dental pulp. This pulp consists of nerves, blood vessels, and connective tissue, extending from the crown (the visible part of the tooth) down through the root canal system, which branches into the roots embedded in your jawbone. The pulp is crucial for tooth development, providing nourishment and sensation. However, once a tooth is fully developed, it can survive without the pulp, drawing nourishment from the surrounding tissues.
When the pulp becomes infected or inflamed, usually due to deep decay, a crack, or trauma, it can cause excruciating pain and lead to an abscess (a pus-filled pocket) at the root tip. If left untreated, this infection can spread to other parts of the body, cause significant bone loss around the tooth, and eventually necessitate tooth extraction.
The primary goal of a root canal procedure is to remove the diseased pulp, thoroughly clean and disinfect the inside of the tooth, and then fill and seal the space to prevent further infection. This process effectively eliminates the source of the pain and saves your natural tooth, allowing it to continue functioning normally. Saving your natural tooth is always the preferred option, as it maintains your bite, prevents adjacent teeth from shifting, and avoids the need for more complex and costly replacement options like dental implants or bridges.
Pro Tip: Don't delay seeking dental care if you suspect you might need a root canal. Early intervention can prevent more severe pain and complications, and may even make the procedure simpler and less expensive.
Types and Variations of Endodontic Treatment
While the term "root canal" typically refers to conventional endodontic treatment, there are several variations and related procedures, each tailored to specific clinical situations.
Conventional Root Canal Treatment (RCT)
This is the most common type of root canal procedure, performed when the pulp inside the tooth becomes irreversibly inflamed or infected. It involves accessing the pulp chamber, removing the diseased tissue, cleaning and shaping the root canals, and then filling them with a biocompatible material (gutta-percha) before sealing the tooth. A permanent restoration, usually a dental crown, is then placed to protect the treated tooth.
Endodontic Retreatment
Sometimes, a tooth that has previously undergone root canal treatment may develop new problems. This can happen if the initial treatment didn't fully remove all infection, if new decay exposes the treated root to bacteria, or if the crown or filling breaks. In such cases, endodontic retreatment is performed. This involves reopening the tooth, removing the previous filling material, thoroughly cleaning and disinfecting the canals again, and then refilling and sealing them. This procedure is often more complex than the initial root canal and is frequently performed by an endodontist, a specialist in root canal treatment.
Apicoectomy (Root-End Resection)
An apicoectomy is a minor surgical procedure performed when an infection or inflammation persists around the tip of the tooth's root even after a conventional root canal or retreatment. During an apicoectomy, the gum tissue is opened to expose the bone and the infected root tip. The very end of the root is removed, along with any infected tissue, and a small filling is placed to seal the end of the root canal. This procedure is generally performed by an endodontist.
Pulpotomy and Pulpectomy (Often Pediatric, but Relevant)
While primarily associated with pediatric dentistry, understanding these procedures can provide context.
- Pulpotomy: This procedure involves removing only the diseased portion of the pulp from the crown of the tooth, leaving the healthy pulp in the root canals intact. It's often performed on primary (baby) teeth to save them from extraction due to deep decay or injury, allowing the tooth to stay in place until it naturally falls out.
- Pulpectomy: A pulpectomy is a more extensive procedure where all the pulp, both in the crown and the root canals, is removed. This is essentially a full root canal for primary teeth. After the pulp is removed, the canals are cleaned and then filled with a resorbable material that allows the tooth to eventually fall out normally. For adult teeth, this is sometimes referred to as vital pulp therapy in cases of reversible pulpitis, aiming to save the tooth's vitality.
Apexification and Apexogenesis
These are specialized endodontic procedures performed on immature permanent teeth (teeth where the root has not fully formed).
- Apexification: This procedure induces root-end closure in permanent teeth with incomplete root formation and necrotic pulp. It involves placing a medication (often MTA) in the canal to encourage the root tip to calcify and close.
- Apexogenesis: This procedure aims to promote continued root development and apex closure in vital immature permanent teeth where the pulp is still alive but has been exposed or inflamed. It involves removing the inflamed part of the pulp and placing a protective material to encourage the remaining healthy pulp to finish forming the root.
These variations highlight the nuanced approach endodontists take to preserve natural teeth, emphasizing conservative treatment whenever possible.
Causes: Why a Root Canal Becomes Necessary
The need for a root canal arises when the dental pulp, the soft tissue inside your tooth, becomes inflamed, infected, or damaged. This can happen for several primary reasons:
- Deep Decay (Dental Caries): This is the most common cause. When a cavity is left untreated, bacteria can erode through the enamel and dentin layers of the tooth, eventually reaching the pulp chamber. Once bacteria invade the pulp, they cause inflammation (pulpitis) and infection, leading to the breakdown of the pulp tissue.
- Repeated Dental Procedures on the Same Tooth: Multiple fillings, crown preparations, or other extensive dental work on a single tooth can sometimes irritate the pulp over time. While modern dental materials and techniques minimize this risk, repeated trauma or exposure to drilling and chemicals can eventually lead to irreversible pulp damage.
- Cracked or Chipped Tooth: A significant crack or chip in a tooth, especially one that extends below the gum line or into the pulp chamber, can create an opening for bacteria to enter and infect the pulp. Cracks can be subtle and difficult to detect, but they allow bacteria to penetrate the tooth's inner layers.
- Trauma to the Tooth: A direct blow to the mouth or face can damage a tooth, even if there's no visible crack or chip. The impact can sever the blood supply to the pulp, causing it to die and become necrotic. Over time, a necrotic pulp can become infected. This can happen immediately or years after the initial injury.
- Severe Gum Disease (Periodontal Disease): While less common, in advanced cases of periodontal disease, bacteria from the gums can sometimes travel up the side of the root and enter the tooth through small accessory canals, leading to pulp infection.
- Extensive Wear: Severe wear of teeth due to grinding (bruxism) or erosion can expose the dentin and, eventually, the pulp, making it vulnerable to infection and inflammation.
Understanding these causes emphasizes the importance of good oral hygiene, regular dental check-ups, and prompt treatment of any dental issues to prevent the need for a root canal.
Signs and Symptoms of a Needed Root Canal
Recognizing root canal symptoms early is crucial for effective treatment and preventing further complications. While some people experience no symptoms, a significant number will present with one or more of the following:
- Persistent Tooth Pain: This is the most common and often the most severe symptom. The pain can vary from mild to intense and may be constant or intermittent. It might radiate to your jaw, face, or other teeth. Characteristically, this pain often worsens when you lie down or apply pressure to the tooth, and it might be so severe it wakes you from sleep.
- Sensitivity to Hot and Cold: While temporary sensitivity can indicate a simple cavity, sensitivity that lingers for an extended period (minutes instead of seconds) after the hot or cold stimulus has been removed is a strong indicator of pulp damage.
- Swelling and Tenderness in the Gums: An infection in the tooth can spread to the surrounding tissues, causing the gums near the affected tooth to become swollen, tender, or red. You might also notice swelling in your face or neck.
- Pimple-Like Bump on the Gums (Fistula): This small bump, often called a "gum boil" or fistula, indicates that the infection has created a pathway for pus to drain from the root tip to the surface of the gums. This can sometimes temporarily relieve pain as pressure is released.
- Tooth Discoloration: An infected tooth, particularly one with a necrotic (dead) pulp, can appear darker or grayish. This is due to the breakdown of blood vessels and tissues within the pulp chamber, which can stain the dentin.
- Pain When Chewing or Biting: Inflammation around the root of the tooth can make it extremely painful to bite down or chew food, even soft foods. This indicates inflammation of the ligaments surrounding the tooth (periodontal ligament).
- Loose Tooth: The infection and inflammation can cause bone loss around the tooth and weaken the ligaments holding it in place, leading to increased tooth mobility.
If you experience any of these symptoms, especially persistent pain or swelling, it's vital to see a dentist immediately. Ignoring these signs can lead to the infection spreading, increased pain, and potentially the loss of the tooth.
Treatment Options: Root Canal vs. Extraction
When the dental pulp becomes irreversibly damaged or infected, you generally have two primary treatment paths: preserving the tooth with a root canal or removing the tooth entirely via extraction. Understanding the pros and cons of each is crucial for making an informed decision.
Option 1: Root Canal Treatment (RCT)
What it is: A procedure to remove the infected pulp, clean and disinfect the internal chambers, and then seal the tooth to prevent future infection. It's almost always followed by a dental crown.
Pros:
- Saves Your Natural Tooth: This is the biggest advantage. Saving your natural tooth preserves your bite, keeps adjacent teeth from shifting, and avoids the bone loss that occurs after tooth extraction.
- Prevents Spread of Infection: The treatment eliminates bacteria, halting the infection from spreading to other teeth or into your jawbone.
- Maintains Aesthetics and Function: Your natural tooth can continue to function normally, allowing you to chew efficiently and speak clearly, while maintaining your natural smile.
- High Success Rate: Modern root canals have a very high success rate, often exceeding 95%, allowing the tooth to last a lifetime with proper care.
- Less Complex Long-Term: While initially more involved than an extraction, preserving the tooth can avoid the need for more complex, costly, and time-consuming tooth replacement procedures down the line.
Cons:
- Cost: A root canal, especially when followed by a crown, can be a significant upfront investment.
- Multiple Appointments: The procedure often requires two appointments, and sometimes more, depending on the complexity.
- Potential for Complications: Though rare, complications like instrument fracture, perforation, or persistent infection can occur, potentially requiring retreatment or surgery.
- Tooth May Become Brittle: A tooth that has undergone a root canal can become more brittle because it no longer has its vital pulp. This is why a crown is almost always recommended to protect it from fracture.
Option 2: Tooth Extraction
What it is: The complete removal of the infected or damaged tooth from its socket.
Pros:
- Immediate Pain Relief: Once the tooth is extracted, the source of the infection and pain is removed.
- Lower Upfront Cost: An extraction is generally less expensive than a root canal, especially if no immediate tooth replacement is planned.
- Simpler Procedure: In many cases, a straightforward extraction is a quicker and less involved procedure than a root canal.
Cons:
- Loss of Natural Tooth: This is the major drawback. Losing a tooth affects your ability to chew and can impact your appearance.
- Bone Loss: The jawbone supporting the extracted tooth will begin to resorb (shrink) over time due to lack of stimulation, which can affect facial structure and the stability of adjacent teeth.
- Shifting of Adjacent Teeth: Without a neighboring tooth to hold them in place, surrounding teeth can drift into the empty space, affecting your bite and potentially causing new dental problems.
- Need for Replacement: To prevent the negative consequences of tooth loss, the extracted tooth often needs to be replaced with a dental implant, bridge, or partial denture, which adds significant cost and complexity.
- Impact on Chewing and Speech: A missing tooth can impair your ability to chew certain foods and may affect your speech.
Comparison Table: Root Canal vs. Extraction
To help you visualize the differences, here's a comparison:
| Feature | Root Canal Treatment (RCT) | Tooth Extraction |
|---|---|---|
| Primary Goal | Save natural tooth, eliminate infection | Remove source of infection/pain, remove tooth |
| Longevity | Tooth can last a lifetime with proper care and crown | Tooth is gone; requires replacement for long-term function |
| Impact on Jawbone | Preserves jawbone structure | Leads to bone resorption/loss over time |
| Impact on Adjacent Teeth | Prevents shifting and maintains bite | Can cause adjacent teeth to shift, affecting bite |
| Aesthetics | Maintains natural appearance and smile | Creates a gap; may require prosthetic replacement |
| Complexity of Procedure | Generally 1-2 appointments, detailed internal cleaning | Usually 1 appointment, surgical removal |
| Typical Cost (US) | $700 - $2,000 (plus crown: $800 - $2,500) | $150 - $600 (simple); $250 - $800+ (surgical) |
| Long-term Cost | Initial RCT + crown | Extraction + replacement (implant: $3,000 - $6,000; bridge: $2,000 - $5,000) |
| Recovery | Mild discomfort for a few days, back to normal quickly | Swelling, bruising, discomfort for several days; risk of dry socket |
| Success Rate | Very high (95%+) | High for removal, but creates new issues for oral health |
Given the long-term benefits of preserving your natural tooth, a root canal is almost always the recommended course of action when feasible. The American Dental Association (ADA) strongly advocates for saving natural teeth whenever possible.
Step-by-Step Process: What to Expect During Treatment
Understanding the stages of a root canal can help alleviate anxiety and prepare you for the procedure. While the exact steps might vary slightly depending on the complexity of your case and the dentist or endodontist performing the treatment, the general process remains consistent.
Step 1: Diagnosis and Treatment Planning
Your dentist will first confirm the need for a root canal. This involves:
- Clinical Examination: Visual inspection, tapping on the tooth, checking for sensitivity to hot/cold, and examining the gums.
- X-rays: Digital X-rays are crucial for identifying the extent of the infection, checking for bone loss around the root tip, visualizing the root canal anatomy, and ruling out other issues. Sometimes, a 3D cone-beam computed tomography (CBCT) scan may be used for complex cases.
- Pulp Vitality Tests: Tests like electric pulp tests or cold/heat tests help determine the vitality and health of the dental pulp.
Step 2: Anesthesia
Before starting, the tooth and surrounding area will be numbed with a local anesthetic. This ensures that you will not feel any pain during the procedure. Modern anesthetics are highly effective, making the root canal a largely pain-free experience.
Step 3: Rubber Dam Placement
Once numb, a small sheet of latex or non-latex material called a rubber dam is placed around the affected tooth. This isolates the tooth, keeping it clean and dry from saliva and bacteria in your mouth, and prevents you from accidentally swallowing small instruments.

Step 4: Access Opening
The dentist will create a small access opening through the crown of the tooth, usually using a dental drill. This opening provides direct access to the pulp chamber and the root canals.
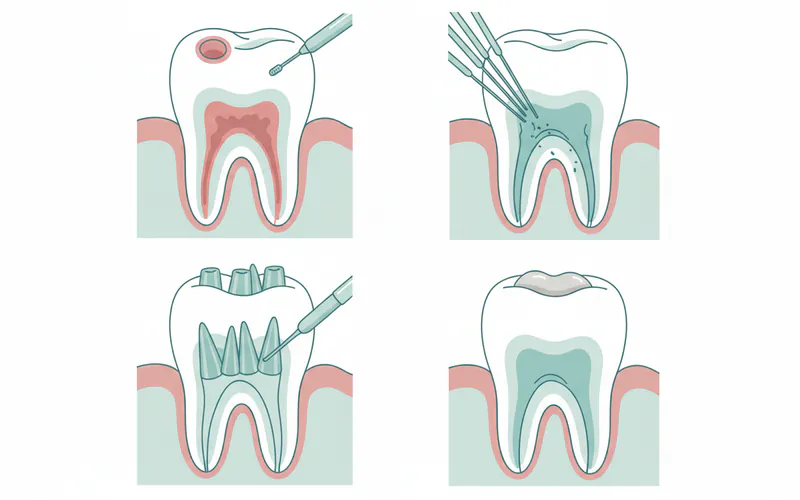
Step 5: Pulp Removal and Cleaning
Using tiny, specialized instruments called endodontic files, the infected or inflamed pulp tissue is carefully removed from the pulp chamber and root canals. The canals are then meticulously cleaned and shaped. During this process, irrigating solutions (like sodium hypochlorite, a disinfectant) are flushed into the canals to wash away debris and kill bacteria. This step is critical for ensuring all infection is eliminated.
Step 6: Filling and Sealing (Obturation)
Once the canals are thoroughly cleaned, shaped, and disinfected, they are dried. Then, they are filled with a biocompatible, rubber-like material called gutta-percha. This material is typically heated and compacted into the canals to ensure a complete, three-dimensional seal. An adhesive cement (sealer) is used to further secure the gutta-percha and prevent reinfection.
Step 7: Temporary Filling
After the root canals are filled, the access opening in the crown of the tooth is sealed with a temporary filling material. This protects the tooth until a permanent restoration can be placed.
Step 8: Permanent Restoration (Crown or Filling)
The final and crucial step occurs a few days or weeks later. A tooth that has undergone a root canal is more fragile and prone to fracture because it no longer has its vital blood supply and has been hollowed out. Therefore, a permanent restoration, typically a dental crown, is almost always necessary to protect the tooth from future damage and restore its full function. In some cases, if the tooth structure is largely intact, a permanent filling may suffice, but a crown offers superior protection, especially for back teeth that bear significant chewing forces.
Pro Tip: Do not skip the permanent crown! Waiting too long or opting out of a crown after a root canal significantly increases the risk of tooth fracture and may compromise the long-term success of the treatment.
Cost and Insurance: Understanding the Financial Aspect
The cost of a root canal is a significant concern for many patients, and it's important to understand the factors that influence it in the US market. Prices can vary widely based on the tooth's location, the complexity of the case, the dental professional performing the procedure, and geographic region.
Average US Root Canal Costs by Tooth Type
The primary factor affecting cost is the specific tooth requiring treatment:
- Front Teeth (Incisors & Canines): These teeth typically have only one root canal, making them the least complex and, therefore, the least expensive.
- Average Cost: $700 - $1,200
- Premolars (Bicuspids): These teeth often have one or two root canals.
- Average Cost: $800 - $1,500
- Molars: These teeth are located at the back of the mouth, have multiple roots (typically three or four), and are the most complex to treat, making them the most expensive.
- Average Cost: $1,000 - $2,000+
Additional Factors Affecting Cost:
- General Dentist vs. Endodontist: An endodontist is a root canal specialist who has undergone additional years of specialized training. While their expertise often leads to higher success rates for complex cases, their fees can be 10-30% higher than those of a general dentist.
- Geographic Location: Costs can be significantly higher in major metropolitan areas (e.g., New York, Los Angeles) compared to rural areas or states with lower costs of living.
- Complexity of the Case: Factors like calcified canals, unusual root anatomy, retreatment, or the presence of a severe infection can increase the time and difficulty of the procedure, thereby increasing the cost.
- Diagnostic Fees: Initial X-rays, exams, and potentially 3D scans (CBCT) are additional costs that contribute to the overall bill.
- Post-Treatment Restoration: This is a crucial, often separate cost. After a root canal, a permanent restoration, usually a dental crown, is almost always necessary to protect the treated tooth.
- Cost of a Dental Crown: $800 - $2,500 (depending on material like porcelain, ceramic, zirconia, or metal, and lab fees).
- Build-up/Core Foundation: If significant tooth structure is lost, a "build-up" or "post and core" may be needed before placing a crown, adding $200 - $500.
Dental Insurance Coverage
Most dental insurance plans do cover a portion of root canal procedures, as it's considered a major restorative treatment.
- Coverage Percentage: Typically, dental insurance covers 50-80% of the cost of a root canal.
- Deductibles: You will usually need to meet your annual deductible first (e.g., $50-$200) before your insurance starts paying.
- Annual Maximums: Most plans have an annual maximum benefit (e.g., $1,000-$2,500). If your root canal and crown costs exceed this, you'll pay the remainder out-of-pocket.
- Waiting Periods: Some plans have waiting periods for major procedures like root canals, meaning you might have to be enrolled for 6-12 months before coverage kicks in.
- Coverage for Crown: Dental crowns are also typically covered at a similar percentage (50-80%) but fall under the same annual maximum.
Pro Tip: Always contact your dental insurance provider directly or ask your dental office to run a pre-treatment estimate. This will give you a clear understanding of your out-of-pocket expenses before the procedure begins.
Cost Breakdown: Root Canal by Tooth Type and Provider (US Averages)
| Tooth Type | General Dentist (Estimated Cost) | Endodontist (Estimated Cost) | With Insurance (50% coverage, post-deductible) |
|---|---|---|---|
| Front Tooth | $700 - $1,000 | $900 - $1,200 | $350 - $600 (out-of-pocket) |
| Premolar | $800 - $1,200 | $1,000 - $1,500 | $400 - $750 (out-of-pocket) |
| Molar | $1,000 - $1,500 | $1,300 - $2,000+ | $500 - $1,000+ (out-of-pocket) |
| Dental Crown (Additional) | $800 - $2,500 | N/A (Performed by General Dentist) | $400 - $1,250 (out-of-pocket) |
| Total (Molar + Crown) | $1,800 - $4,000 | $2,100 - $4,500+ | $900 - $2,250+ (out-of-pocket) |
Note: These are average ranges and can vary widely. Always get a specific quote from your dental provider.
Payment Plans and Financing Options
If the cost is a barrier, many dental offices offer or work with third-party financing options:
- Payment Plans: Some practices offer in-house payment plans, allowing you to pay in installments.
- CareCredit/LendingClub: These are healthcare credit cards that offer special financing options, including interest-free periods if paid in full within a certain timeframe.
- Dental Schools: University dental schools often provide services at a reduced cost, as procedures are performed by students under the close supervision of experienced faculty.
- Public Health Clinics: Some community dental clinics offer sliding scale fees based on income or reduced rates.
Recovery and Aftercare: Ensuring Long-Term Success
After a root canal procedure, proper recovery and diligent aftercare are essential for ensuring the long-term success of the treatment and preventing complications.
Immediate Post-Procedure Care (First 24-72 Hours)
- Numbness: The local anesthetic will wear off gradually, typically within a few hours. Avoid chewing on the treated side until the numbness completely subsides to prevent accidental biting of your cheek or tongue.
- Discomfort and Sensitivity: It's normal to experience some mild to moderate discomfort, tenderness, or sensitivity for a few days after the procedure. This is due to the inflammation of the tissues surrounding the tooth and the healing process.
- Pain Management:
- Over-the-counter (OTC) pain relievers: Medications like ibuprofen (Advil, Motrin) or naproxen (Aleve) are usually effective for managing post-procedure pain and inflammation. Acetaminophen (Tylenol) can also be used.
- Prescription Pain Relievers: In some cases, especially if there was significant infection or inflammation, your dentist might prescribe stronger pain medication. Take as directed.
- Diet: Stick to soft foods for the first few days. Avoid hard, crunchy, or sticky foods that could dislodge the temporary filling or put excessive pressure on the healing tooth.
- Avoid Chewing on the Treated Tooth: Until the permanent crown or restoration is placed, the tooth is more fragile. Chew on the opposite side of your mouth to prevent fracture of the temporary filling or the tooth itself.
Long-Term Aftercare
- Permanent Restoration is Crucial: As mentioned, a permanent dental crown or other restoration is vital. The temporary filling is not designed for long-term use. Schedule and attend your follow-up appointment to get the permanent crown placed as soon as recommended (usually within a few weeks). Delaying this step significantly increases the risk of tooth fracture or reinfection.
- Maintain Excellent Oral Hygiene: Continue brushing twice a day with fluoride toothpaste and flossing daily. Pay particular attention to the treated tooth and the surrounding gum line to prevent new decay or gum disease.
- Regular Dental Check-ups: Continue with your routine dental check-ups and cleanings as recommended by your dentist. This allows your dentist to monitor the health of your treated tooth and address any potential issues early.
- Avoid Habits that Damage Teeth: Refrain from chewing on ice, pens, or other hard objects. If you grind or clench your teeth (bruxism), your dentist may recommend a nightguard to protect your teeth, especially the crowned tooth.
- Monitor for Complications: While most root canals are highly successful, be aware of signs that might indicate a problem, such as:
- Severe pain that doesn't subside with medication.
- Swelling, fever, or a persistent pimple on the gums.
- Signs of an allergic reaction to medication.
- Loss of the temporary or permanent filling/crown.
- Increased sensitivity to pressure or heat that lingers. If you experience any of these, contact your dentist immediately.
With proper care, a tooth treated with a root canal and restored with a crown can last a lifetime, functioning just like any other tooth. The success rate for root canal treatment is remarkably high, often exceeding 95%, making it one of the most reliable dental procedures.
Prevention: How to Avoid a Root Canal
The best treatment is prevention. By adopting good oral hygiene habits and making proactive lifestyle choices, you can significantly reduce your risk of needing a root canal.
-
Practice Excellent Oral Hygiene:
- Brush Twice Daily: Brush your teeth for two minutes, twice a day, using a fluoride toothpaste. This helps remove plaque and food debris that cause cavities.
- Floss Daily: Flossing removes plaque and food particles from between your teeth and under the gum line, areas your toothbrush can't reach. This is crucial for preventing interdental cavities and gum disease.
- Use Mouthwash: An antimicrobial mouthwash can help reduce bacteria in your mouth, though it's not a substitute for brushing and flossing.
-
Regular Dental Check-ups and Cleanings:
- Visit Your Dentist Every 6 Months: Professional cleanings remove tartar buildup that brushing alone can't. Regular check-ups allow your dentist to spot small cavities, cracks, or other issues early, before they progress to the pulp. Early detection of cavities means simpler, less invasive fillings instead of root canals.
- Get X-rays as Recommended: X-rays help your dentist see decay between teeth, under existing fillings, or potential infections at the root tips that aren't visible during a visual exam.
-
Prompt Treatment of Cavities: Don't delay treating a cavity. Even a small cavity can quickly enlarge and eventually reach the pulp if left unattended. A simple filling is far preferable to a root canal.
-
Protect Your Teeth from Trauma:
- Wear a Mouthguard for Sports: If you play contact sports or participate in activities with a risk of facial impact, a custom-fitted mouthguard can protect your teeth from chips, cracks, and avulsion (tooth knockout).
- Avoid Chewing Hard Objects: Do not chew on ice, popcorn kernels, pens, or other hard, non-food items that can crack or chip your teeth.
-
Address Bruxism (Teeth Grinding/Clenching): If you grind or clench your teeth, especially at night, this can put immense pressure on your teeth, leading to cracks, wear, and eventual pulp damage. Your dentist can recommend a nightguard to protect your teeth.
-
Maintain a Healthy Diet: Limit sugary and acidic foods and drinks. These contribute to tooth decay by creating an environment where harmful bacteria thrive. Instead, opt for a balanced diet rich in fruits, vegetables, and calcium-rich foods.
By following these preventive measures, you significantly decrease your chances of experiencing the pain and complications that necessitate a root canal, keeping your natural smile healthy and strong.
Risks and Complications
While root canal treatment boasts a very high success rate, typically above 95%, like any medical procedure, it carries potential risks and complications. Being aware of these can help you understand what to look for and when to contact your dental professional.
-
Persistent Infection or Re-infection:
- Incomplete Cleaning: Despite best efforts, tiny accessory canals or complex root anatomy might make it impossible to completely clean all bacteria.
- Leakage: A leaky temporary or permanent restoration can allow bacteria to re-enter the treated canals.
- New Decay: New cavities forming around the treated tooth, especially under the crown, can expose the sealed canals to bacteria.
- Untreated Canals: Sometimes a tooth may have more canals than initially identified and treated.
- Symptoms: Persistent pain, swelling, or a recurring pimple on the gums can indicate a failed root canal, which might require retreatment or an apicoectomy.
-
Fracture of the Tooth:
- Weakened Tooth Structure: A tooth that has undergone a root canal can become brittle because it's no longer receiving nourishment from the pulp and has been hollowed out. This is why a dental crown is almost always recommended to protect it from fracture.
- Vertical Root Fracture: In rare cases, a fracture can occur along the root of the tooth, often due to excessive biting forces or internal stress. Vertical root fractures are challenging to treat and often lead to tooth extraction.
-
Instrument Separation (Broken File):
- During the cleaning and shaping process, the small, delicate endodontic files can sometimes break off inside the root canal, especially in very narrow or curved canals.
- If the fragment is small and occurs near the tip of the root in an already clean canal, it may be left in place without causing problems. However, if it blocks access to an infected area, it can prevent proper cleaning and require specialized removal or surgical intervention.
-
Perforation:
- Occasionally, an endodontic instrument can accidentally create a small hole (perforation) through the side or bottom of the tooth's root or into the pulp chamber during the access or cleaning stage.
- Small perforations can often be repaired with a special filling material, but larger ones can compromise the tooth's long-term prognosis and may lead to extraction.
-
Discoloration:
- While less common with modern techniques, a treated tooth can sometimes darken over time. This is usually due to residual pulp tissue, blood products left in the dentin tubules, or certain filling materials.
- Discoloration can often be treated with internal tooth whitening procedures or masked with a crown or veneer.
-
Nerve Damage:
- Extremely rare, but during treatment, especially in lower back teeth where nerves are close to the root tips, there's a minimal risk of temporary or, in very rare cases, permanent nerve damage, leading to numbness or altered sensation in the lip or chin. This is more often a risk with dental extractions involving the inferior alveolar nerve.
-
Allergic Reaction:
- Allergic reactions to anesthetic agents, latex (from the rubber dam), or medications used during or after the procedure are possible, though rare.
These risks underscore the importance of choosing an experienced dentist or endodontist and following all post-treatment instructions carefully. Most complications are manageable if addressed promptly.
Children / Pediatric Considerations
While root canals are commonly associated with adult teeth, primary (baby) teeth can also develop deep decay or trauma that affects the pulp, necessitating similar endodontic procedures. For children, the goal is often to save the primary tooth until it's naturally ready to fall out, as premature loss can lead to space problems for the developing permanent teeth.
Why a Root Canal Might Be Needed for a Child's Tooth:
- Deep Cavities: Just like in adults, untreated deep cavities can reach the pulp, causing pain and infection.
- Dental Trauma: Falls or blows to the face are common in childhood and can cause cracks or fractures in primary teeth, leading to pulp exposure or necrosis.
- Pulpitis: Inflammation of the pulp, either reversible or irreversible, can occur.

Pediatric Endodontic Procedures:
-
Pulpotomy (Partial Pulp Removal):
- This is often called a "nerve treatment" or "baby root canal."
- In a pulpotomy, only the infected or inflamed pulp tissue in the crown of the tooth is removed. The healthy pulp within the root canals is left intact.
- A medicated material is then placed over the remaining pulp to help it heal, and the tooth is restored, usually with a stainless steel crown.
- Goal: To maintain the vitality of the root pulp and allow the primary tooth to remain in place until its natural exfoliation (falling out) date, preserving space for the permanent tooth.
-
Pulpectomy (Full Pulp Removal):
- If the infection has spread throughout the entire pulp system, including the root canals, a pulpectomy is performed.
- This involves removing all the pulp tissue from both the crown and the root canals.
- The canals are then cleaned, disinfected, and filled with a resorbable material (unlike the permanent gutta-percha used in adult root canals) that allows the primary tooth to resorb naturally along with its root as the permanent tooth develops.
- Goal: To eradicate infection and save the primary tooth when a pulpotomy is not sufficient, ensuring proper chewing function and maintaining space.
Importance of Saving Primary Teeth:
- Space Maintainers: Primary teeth act as natural space maintainers for permanent teeth. If a baby tooth is lost too early, adjacent teeth can drift into the empty space, leading to crowding and misalignment of the permanent teeth later on.
- Chewing and Speech: Healthy primary teeth are essential for proper chewing, nutrition, and the development of clear speech patterns.
- Self-Esteem: Avoiding premature tooth loss helps children maintain a confident smile.
Pediatric Aftercare:
- Parents should ensure their child avoids chewing on the treated tooth until the permanent crown is placed.
- Good oral hygiene practices (brushing, flossing) are paramount to prevent further decay.
- Regular pediatric dental check-ups are vital to monitor the treated tooth and the eruption of permanent teeth.
Pro Tip for Parents: If your child complains of persistent tooth pain, has swelling around a tooth, or experiences sensitivity, seek immediate dental care. Early intervention by a pediatric dentist can often save a primary tooth and prevent more complex issues down the line.
Frequently Asked Questions
Here are some common questions patients have about root canal treatment:
Is a root canal painful?
Modern root canal treatment is generally not painful. The procedure is performed under local anesthesia, completely numbing the tooth and surrounding area, making it comparable to getting a routine filling. Any discomfort during the procedure is typically from the injection, not the treatment itself. Post-procedure, mild soreness is common for a few days but is usually managed effectively with over-the-counter pain relievers. The goal of a root canal is to relieve the severe pain caused by an infected tooth, not to cause it.
How long does a root canal take?
The duration of a root canal procedure varies depending on the complexity of the case and the tooth involved. A front tooth (single canal) might take 60-90 minutes, while a molar (multiple canals) can take 90 minutes to 2 hours or more. Some complex cases or re-treatments may require two separate appointments to ensure thorough cleaning and disinfection.
How much does a root canal cost?
In the US, the cost of a root canal typically ranges from $700 to $1,500 for front teeth and $1,000 to $2,000+ for molars. These prices usually do not include the cost of a dental crown, which is often necessary and can add another $800 to $2,500. Dental insurance often covers 50-80% of the procedure after your deductible is met, but you should always verify your specific benefits.
What are the alternatives to a root canal?
The primary alternative to a root canal for an infected or severely damaged tooth is tooth extraction. While extraction provides immediate relief from pain, it results in the loss of your natural tooth and can lead to issues like bone loss, shifting teeth, and the need for costly replacements like dental implants or bridges. A root canal saves your natural tooth, which is almost always the preferred option.
How long does a root canal last?
With proper care and a timely placed permanent crown, a tooth treated with a root canal can last a lifetime. The success rate for root canal treatment is very high, often exceeding 95%. Regular brushing, flossing, dental check-ups, and avoiding habits like chewing on hard objects are crucial for its longevity.
Do I need a crown after a root canal?
In most cases, yes, a dental crown is strongly recommended after a root canal, especially for back teeth (molars and premolars) that bear heavy chewing forces. The root canal procedure removes the vital pulp, which can make the tooth more brittle and prone to fracture. A crown provides essential protection, restoring the tooth's strength and preventing future damage, thus significantly increasing the success rate and longevity of the treated tooth.
What can I eat after a root canal?
Immediately after the procedure, while your mouth is still numb, avoid eating to prevent accidentally biting your cheek or tongue. For the first few days, stick to soft foods and chew on the opposite side of your mouth. Avoid hard, crunchy, or sticky foods that could dislodge the temporary filling or fracture the weakened tooth before a permanent crown is placed. Once the permanent crown is in, you can typically resume a normal diet.
Can a root canal fail?
While highly successful, a root canal can sometimes fail. This can happen due to persistent infection from undetected canals, a new crack in the tooth, new decay exposing the treated area, or if the permanent restoration (crown) is delayed or breaks. Signs of failure include renewed pain, swelling, or a recurring pimple on the gums. In such cases, endodontic retreatment or an apicoectomy may be necessary.
Is it better to get a root canal or extract the tooth?
It is almost always better to save your natural tooth with a root canal than to extract it. Saving your tooth preserves your natural bite, prevents adjacent teeth from shifting, avoids bone loss in the jaw, and eliminates the need for more complex and costly replacement procedures like implants or bridges. Tooth extraction should generally be considered a last resort when a root canal is not feasible.
Who performs a root canal?
Root canals can be performed by either a general dentist or an endodontist. An endodontist is a dental specialist who has completed an additional two to three years of advanced training in diagnosing and treating problems related to the dental pulp and root. For complex cases, re-treatments, or surgical endodontic procedures, a general dentist will often refer you to an endodontist due to their specialized expertise and equipment.
When to See a Dentist
Recognizing the warning signs that indicate a potentially serious dental issue, such as an infected pulp, is paramount for your oral health. Prompt dental attention can prevent the escalation of pain, infection, and the loss of your tooth.
Clear Warning Signs That Need Immediate Attention:
- Severe, Persistent Tooth Pain: This is the most critical sign. If you experience intense tooth pain that is constant, throbbing, wakes you up at night, or radiates to your jaw or ear, it's an emergency. This type of pain often indicates an infection has reached the tooth's nerve.
- Swelling in the Gums, Face, or Neck: Swelling around a tooth, on your jaw, or in your face or neck is a clear sign of a spreading infection or abscess. This needs immediate evaluation as a dental infection can spread rapidly and become life-threatening if left untreated.
- Pimple-Like Bump on the Gums (Fistula): A small, tender bump on your gums, especially one that releases pus or has a foul taste, indicates a draining infection from the root of a tooth.
- Extreme Sensitivity to Hot and Cold That Lingers: While temporary sensitivity is common, if your tooth remains highly sensitive to hot or cold temperatures for minutes after the stimulus is removed, it suggests irreversible pulp damage.
- Pain When Chewing or Biting: Tenderness or severe pain when putting pressure on a tooth, or when chewing, is a strong indicator of inflammation around the root.
- Tooth Discoloration: If one of your teeth starts to look darker or grayish, it can mean the pulp inside has died, often due to infection or trauma.
Emergency vs. Scheduled Appointment Guidance:
- Emergency: If you have severe, unbearable pain, significant swelling, signs of a spreading infection (fever, difficulty swallowing or breathing), or trauma that has loosened or knocked out a tooth, seek emergency dental care immediately. Contact your dentist's office, an emergency dental clinic, or go to an urgent care center or hospital emergency room.
- Scheduled Appointment: If your symptoms are milder but persistent – such as mild, lingering sensitivity, occasional discomfort when chewing, or a subtle change in tooth color – you should schedule an appointment with your dentist as soon as possible. Don't wait for the pain to become unbearable, as early intervention can often lead to simpler treatment and a better outcome.
Ignoring dental symptoms is never advisable. The human body is remarkably resilient, but dental infections do not resolve on their own. They will almost always worsen over time, leading to increased pain, more complex treatment, and potentially the loss of the affected tooth. Your dentist is the best resource to diagnose the problem and recommend the appropriate course of action, which could very well be a root canal to save your natural tooth.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
How to Stop Throbbing Pain After Root Canal
Undergoing a root canal procedure is often a necessary step to save a tooth severely damaged by decay or infection, preventing further complications and excruciating pain. While the procedure itself is performed under local anesthesia to ensure comfort, it's common for patients to experience some le
February 22, 2026
Root Canal After Care: Complete Guide
A root canal procedure can be a tooth-saving treatment, offering relief from pain and preventing further infection. However, the success and longevity of this crucial dental intervention heavily rely on diligent root canal after care. Neglecting post-treatment instructions can lead to complicati
February 22, 2026

Can You Drive After a Root Canal
Undergoing a root canal procedure can understandably bring up a host of questions and concerns, from understanding the process itself to managing recovery. One of the most common and practical inquiries people have is: can you drive after a root canal? The answer isn't always a simple yes or no,
February 22, 2026
Is a Root Canal Painful
When facing the prospect of a root canal, one of the most common and immediate questions that comes to mind is: is a root canal painful? It's a valid concern, stemming from outdated perceptions and anecdotal stories. However, modern root canal therapy is a highly effective and generally comforta
February 22, 2026