What Is Tmj Disorder
Key Takeaways
- Few things are as disruptive to daily life as persistent pain, especially when it affects fundamental actions like eating, speaking, or even smiling. If you've ever experienced a clicking jaw, chronic headaches, or an aching face, you might be among the estimated 10 million Americans affected by
What Is TMJ Disorder
Few things are as disruptive to daily life as persistent pain, especially when it affects fundamental actions like eating, speaking, or even smiling. If you've ever experienced a clicking jaw, chronic headaches, or an aching face, you might be among the estimated 10 million Americans affected by a temporomandibular joint (TMJ) disorder. But what is TMJ disorder exactly? It's a complex condition impacting the joints that connect your jawbone to your skull, as well as the surrounding muscles and ligaments. Understanding this common yet often misunderstood ailment is the first step toward finding relief and restoring your quality of life. This comprehensive guide from SmilePedia.net will delve deep into the world of TMJ disorders, exploring their causes, symptoms, diverse treatment options, and crucial prevention strategies to empower you with the knowledge you need.

Key Takeaways:
- What it is: TMJ disorder (TMD) affects the temporomandibular joints, jaw muscles, and nerves, leading to pain and dysfunction in the jaw and surrounding areas.
- Prevalence: Affects approximately 10 million Americans, predominantly women aged 20-40.
- Common Symptoms: Jaw pain, clicking/popping sounds, headaches, earaches, limited jaw movement, and facial pain.
- Initial Treatments: Most cases respond to conservative, non-invasive treatments like self-care, physical therapy, pain medication, and custom TMJ mouth guards (splints).
- Cost Range: Initial consultations and basic treatments can range from $100 to $500. Custom oral appliances typically cost between $300 and $2,500. More advanced temporomandibular joint dysfunction treatments, such as injections or surgery, can range from $500 to over $10,000.
- Treatment Timeline: Conservative treatments often show improvement within weeks to a few months, with long-term management sometimes required. Surgical recovery can take several months.
- Prevention: Stress management, avoiding hard or chewy foods, maintaining good posture, and addressing habits like teeth grinding can help prevent or mitigate symptoms.
What Is TMJ Disorder?
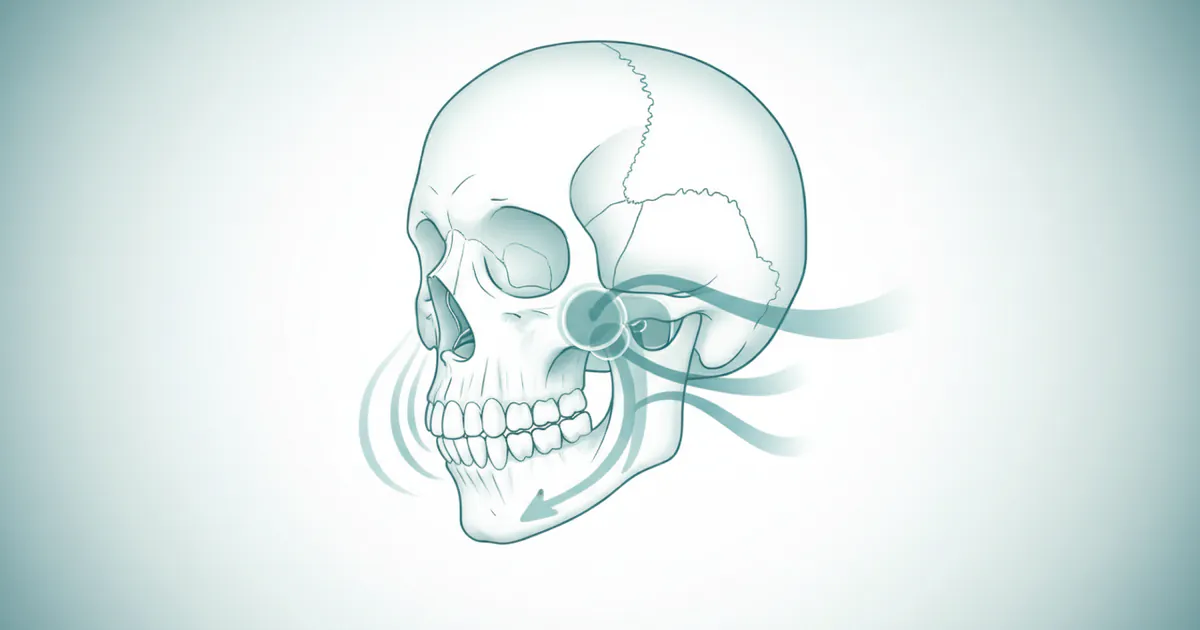
The temporomandibular joints (TMJs) are two small, hinge-like joints located on either side of your head, just in front of your ears. These joints are among the most complex in the body, responsible for the intricate movements of your jaw — up and down, side to side, and forward and back. They enable you to chew, speak, yawn, and swallow. A TMJ disorder, often referred to as TMD (Temporomandibular Disorder) or sometimes mistakenly as "TMJ" itself, refers to a group of conditions that cause pain and dysfunction in the jaw joint and the muscles that control jaw movement.
It's crucial to understand that "TMJ" refers to the joint itself, while "TMD" describes the disorder. However, "TMJ disorder" has become the common, interchangeable term understood by most patients and even some medical professionals. These disorders can be acute (short-term) or chronic (long-term) and can significantly impact a person's quality of life due to persistent pain and restricted jaw function.
The TMJ itself is composed of several key structures:
- The Condyle: The rounded upper end of the lower jawbone (mandible).
- The Articular Fossa: A socket in the temporal bone of the skull where the condyle rests.
- The Articular Disc (Meniscus): A small, oval-shaped piece of cartilage located between the condyle and the fossa. This disc acts as a shock absorber, ensuring smooth movement and preventing bone-on-bone friction.
- Muscles and Ligaments: A complex network of muscles (masseter, temporalis, medial and lateral pterygoid muscles) and ligaments stabilize the joint and facilitate its movements.
When any of these components become compromised — whether due to injury, inflammation, or structural problems — a TMJ disorder can arise, leading to a range of uncomfortable and often debilitating symptoms.
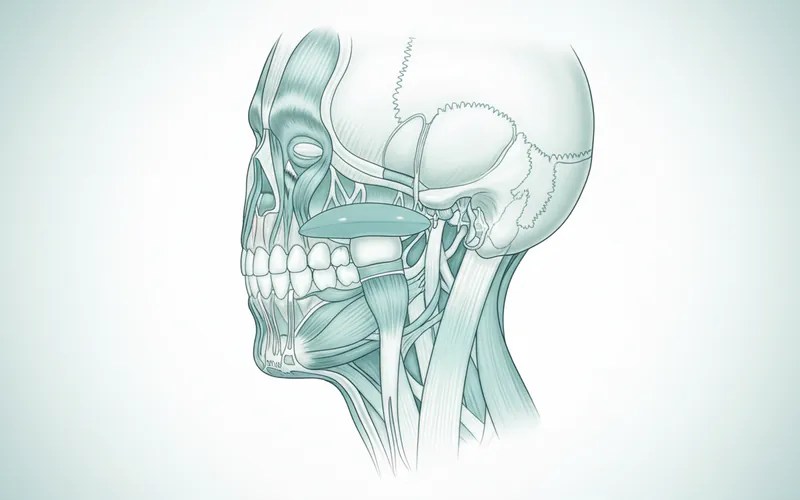
Types and Classifications of TMJ Disorders
TMJ disorders are not a single condition but rather a group of related issues. The National Institute of Dental and Craniofacial Research (NIDCR) classifies TMD into three main categories, although many patients experience a combination of these:
1. Myofascial Pain (Muscle-Related TMJ Disorder)
This is the most common type of TMJ disorder, characterized by pain or discomfort in the muscles that control jaw function (the masticatory muscles) and the muscles of the neck and shoulder.
- Characteristics: Dull, aching pain in and around the jaw, temples, neck, and shoulders. Often accompanied by muscle tenderness, stiffness, and fatigue. Headaches, particularly tension-type headaches, are very common.
- Causes: Often linked to muscle overuse, stress, teeth grinding (bruxism), teeth clenching (awake or asleep), or sustained awkward postures.
- Prevalence: Up to 70% of TMD cases fall into this category.
2. Internal Derangement of the Joint (Joint-Related TMJ Disorder)
This category involves structural problems within the TMJ itself, most commonly an issue with the articular disc.
- Disc Displacement with Reduction: The disc slips out of its normal position when the jaw is closed but moves back into place with a "click" or "pop" when the mouth is opened wide or moved in certain ways. This can cause discomfort and sounds.
- Disc Displacement Without Reduction: The disc remains displaced even when the jaw moves. This can lead to limited jaw opening (often called "closed lock"), pain, and no clicking sound as the disc isn't "reducing" back into place.
- Causes: Trauma (e.g., a blow to the jaw, whiplash), degenerative changes, repetitive stress, or hypermobility of the joint.
3. Degenerative Joint Disease (Arthritis-Related TMJ Disorder)
This refers to conditions that cause deterioration of the joint's hard tissues, such as osteoarthritis or rheumatoid arthritis.
- Osteoarthritis: The cartilage in the joint breaks down over time, leading to bone-on-bone friction, pain, stiffness, and a grating sensation (crepitus). It is common in older adults.
- Rheumatoid Arthritis: An autoimmune disease that can affect the TMJs, causing inflammation, pain, swelling, and eventually joint destruction.
- Other Inflammatory Conditions: Less common forms of arthritis or other inflammatory conditions can also affect the TMJ.
- Characteristics: Chronic pain, stiffness, limited movement, and grating or grinding sounds (crepitus) during jaw movement.
It's important to note that these categories are not mutually exclusive. A patient might experience myofascial pain alongside disc displacement or develop degenerative changes as a result of long-standing internal derangement. A thorough diagnosis by a qualified dental professional is essential to determine the specific type of TMJ disorder affecting an individual.
Causes of TMJ Disorder
The exact cause of TMJ disorders is often complex and multifactorial, meaning several factors can contribute to its development. Sometimes, the cause is clear, but in many cases, it's difficult to pinpoint a single origin.
Primary Causes and Contributing Factors:
- Trauma: A direct blow to the jaw, head, or neck (e.g., from an accident, sports injury, or whiplash) can damage the TMJ, its disc, or the surrounding muscles. Even a minor trauma, if repetitive, can contribute.
- Bruxism and Clenching: Grinding your teeth (bruxism) or clenching your jaw, often unconsciously during sleep or stress, puts immense pressure on the TMJs and surrounding muscles. This can lead to muscle fatigue, inflammation, and disc displacement. This is a very common contributing factor.
- Stress and Anxiety: Psychological stress is a significant trigger for TMJ symptoms. Stress often leads to unconscious muscle tension, clenching, and grinding, exacerbating pain and discomfort in the jaw muscles.
- Malocclusion (Bite Issues): While not considered a primary cause by all researchers, some believe that an improper bite (how your upper and lower teeth meet) can contribute to TMJ issues by creating uneven pressure on the joints. This includes misaligned teeth, missing teeth, or poorly fitting dental work.
- Arthritis: As mentioned earlier, various forms of arthritis can affect the TMJ:
- Osteoarthritis: Degeneration of joint cartilage due to wear and tear.
- Rheumatoid Arthritis: An autoimmune disease causing inflammation of the joint lining.
- Psoriatic Arthritis, Gout: Less common but can also involve the TMJ.
- Connective Tissue Diseases: Conditions like Ehlers-Danlos syndrome or lupus can affect the elasticity and integrity of the connective tissues, including those in the TMJ, leading to hypermobility or instability.
- Habitual Behaviors: Habits such as nail-biting, chewing gum frequently, jaw thrusting, or biting on foreign objects can strain the jaw joint and muscles over time.
- Hormonal Factors: TMJ disorders are significantly more common in women, particularly those of childbearing age (20-40). This suggests a possible link to hormonal influences, though the exact mechanism is not fully understood. Estrogen receptors are present in the TMJ, and fluctuations might play a role.
- Genetics: Some individuals may have a genetic predisposition to developing chronic pain conditions, including TMD.
- Postural Problems: Poor posture, especially forward head posture (often seen with prolonged computer use), can strain neck and shoulder muscles, which in turn can affect the position and function of the jaw.
It's important to understand that in many cases, a combination of these factors contributes to the onset and persistence of TMJ disorder. For example, a person with a genetic predisposition to arthritis might develop symptoms after a minor trauma and worsened by stress-induced clenching.
Signs and Symptoms of TMJ Disorder
The symptoms of a TMJ disorder can vary widely in intensity and manifestation, often mimicking other conditions, which can make diagnosis challenging. However, certain hallmark signs should prompt you to seek professional evaluation.
Common Signs and Symptoms:
- Pain or Tenderness:
- Jaw Pain: Aching or dull pain in the jaw joint itself, often radiating to the face, neck, and shoulders. It can be worse in the morning or after periods of clenching/grinding.
- Facial Pain: Generalized aching or sharp pain in the face, cheekbones, or around the temples.
- Ear Pain: Often mistaken for an ear infection, TMJ pain can manifest as aching in or around the ear, sometimes accompanied by a feeling of fullness.
- Headaches: Chronic headaches, especially tension-type headaches, are a very common symptom. Migraine-like headaches can also occur.
- Neck and Shoulder Pain: Pain and stiffness in the neck and shoulders due to muscle tension often accompany jaw pain.
- Jaw Sounds:
- Clicking or Popping: A distinct click or pop when opening or closing your mouth. This might not always be painful but can indicate disc displacement.
- Grating or Grinding (Crepitus): A rough, sand-like, or grinding sound when moving the jaw, often indicative of degenerative changes within the joint (e.g., bone-on-bone friction).
- Limited Jaw Movement and Lockjaw:
- Restricted Opening: Difficulty opening your mouth wide, making it hard to eat or yawn.
- Jaw Locking: The jaw getting "stuck" in an open or closed position, making it temporarily impossible to move it. This can be painful and frightening.
- Difficulty Chewing:
- Pain while chewing, especially hard or chewy foods.
- Feeling that your bite is "off" or uncomfortable.
- Fatigue in jaw muscles after eating.
- Other Symptoms:
- Tinnitus: Ringing in the ears.
- Dizziness or Vertigo: While less common, some patients report dizziness.
- Hearing Changes: Temporary changes in hearing perception.
- Swelling: Swelling on the side of the face.
- Tooth Sensitivity: Can be caused by excessive clenching or grinding.
- Changes in Bite: A sudden change in how your upper and lower teeth fit together.
Pro Tip: Keeping a symptom diary can be incredibly helpful for your dentist or doctor. Note when the pain occurs, its intensity, what makes it better or worse, and any associated sounds or limitations in movement.
Diagnosing TMJ Disorder
Diagnosing a TMJ disorder requires a thorough evaluation, as symptoms can overlap with other conditions. There isn't a single definitive test; rather, diagnosis is often a process of elimination and careful clinical assessment.
1. Clinical Examination:
- Patient History: Your dentist will ask about your symptoms, their duration, severity, any past injuries, dental history, habits (like clenching or grinding), and stress levels.
- Palpation: The dentist will gently feel your jaw joints and muscles (masseter, temporalis, pterygoid muscles) for tenderness, swelling, and muscle spasms.
- Jaw Movement Assessment: They will listen for clicks, pops, or grating sounds as you open and close your mouth, and observe your jaw's range of motion, checking for any deviations or limitations.
- Bite Analysis: Your bite will be evaluated to see how your teeth come together.
2. Imaging Studies:
- Dental X-rays: Standard dental X-rays (like panoramic X-rays) can help rule out other dental problems and provide a general view of the jaw bones and joints.
- Computed Tomography (CT) Scan: Provides detailed images of the bone structure of the joint, useful for detecting fractures, arthritis, or other bony changes.
- Magnetic Resonance Imaging (MRI): The gold standard for visualizing the soft tissues of the TMJ, including the articular disc, muscles, and ligaments. An MRI can show if the disc is displaced, torn, or degenerated, and can assess inflammation.
- Arthrography: Less common, this involves injecting a contrast dye into the joint space before an X-ray or CT scan to better visualize the joint structures and movement.
3. Other Diagnostic Tools:
- Electromyography (EMG): Measures the electrical activity of muscles, which can help assess muscle function and identify overactive muscles associated with bruxism or clenching.
- Diagnostic Injections: Sometimes, a local anesthetic is injected into a specific muscle or joint space. If the pain is relieved, it helps confirm that area as the source of the problem.
- Sleep Studies: If sleep bruxism is suspected, a sleep study (polysomnography) can help monitor jaw activity during sleep.
Differential Diagnosis:
A key part of diagnosis is ruling out other conditions that can cause similar symptoms, such as:
- Sinus infections
- Ear infections
- Trigeminal neuralgia (a nerve disorder)
- Cluster headaches or migraines
- Salivary gland problems
- Dental abscesses or other tooth-related pain
Your dentist will carefully evaluate your symptoms and use a combination of these diagnostic methods to arrive at an accurate diagnosis and develop an appropriate treatment plan. The American Dental Association (ADA) emphasizes a conservative approach to diagnosis, starting with clinical examination before resorting to advanced imaging unless clinically indicated.
Treatment Options for TMJ Disorder
Fortunately, most cases of TMJ disorder respond well to conservative, non-invasive treatments. The goal of treatment is to reduce pain, restore normal jaw function, and improve your quality of life. Treatment plans are highly individualized, depending on the specific cause and type of your TMJ disorder.
Conservative Treatments (First-Line Approach)
The vast majority of patients find relief with one or more of these reversible treatments.
1. Self-Care and Lifestyle Modifications:
- Soft Diet: Avoid hard, chewy, or crunchy foods (e.g., nuts, candy, bagels, tough meats) to reduce strain on the jaw.
- Heat/Cold Therapy: Apply moist heat (e.g., a warm compress) to the jaw muscles for relaxation, or ice packs for acute pain and swelling.
- Jaw Exercises: Gentle stretching and strengthening exercises, often recommended by a dentist or physical therapist, can improve jaw mobility and reduce muscle tension.
- Stress Reduction: Techniques like meditation, yoga, deep breathing, and mindfulness can help manage stress, which often exacerbates clenching and grinding.
- Avoid Extreme Jaw Movements: Limit wide yawning, excessive singing, or chewing gum.
- Good Posture: Maintain proper head and neck posture, especially when working at a computer or reading.
2. Medications:
- Over-the-Counter (OTC) Pain Relievers: Non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen (Advil, Motrin) or naproxen (Aleve) can reduce pain and inflammation.
- Prescription Medications:
- Muscle Relaxants: Such as cyclobenzaprine (Flexeril) or tizanidine (Zanaflex), can help alleviate muscle spasms and tension, often prescribed for short-term use.
- Tricyclic Antidepressants: Low doses of drugs like amitriptyline can help manage pain, improve sleep, and reduce teeth grinding, even if you don't have depression.
- Corticosteroids: Oral corticosteroids or injections into the joint can reduce inflammation and pain.
- Anti-anxiety medications: In some cases, to help manage stress and related muscle tension.
3. Physical Therapy (PT):
A physical therapist specializing in craniomandibular disorders can provide targeted treatment:
- Manual Therapy: Massage, joint mobilization, and stretching to reduce muscle tension and improve joint mobility.
- Therapeutic Exercises: Specific exercises to strengthen jaw muscles, improve posture, and increase range of motion.
- Modalities: Ultrasound, TENS (Transcutaneous Electrical Nerve Stimulation), or cold laser therapy may be used to reduce pain and inflammation.
4. Oral Appliances (Splints or TMJ Mouth Guard):
Often referred to as occlusal splints or night guards, these custom-made devices are worn over the teeth, typically at night, to help manage TMJ symptoms.
- Stabilization Splints: The most common type, designed to create an ideal bite relationship, reduce muscle activity, protect teeth from grinding, and redistribute forces across the joint. They are typically made of hard acrylic and cover all upper or lower teeth.
- Repositioning Splints: Less commonly used, these are designed to temporarily reposition the jaw to encourage the disc to return to a more favorable position. Their long-term effectiveness and potential for permanent bite changes are debated, and they are usually used for short periods under careful supervision.
Pro Tip: If you're considering a TMJ mouth guard, ensure it's a custom-fitted device made by your dentist. Over-the-counter boil-and-bite guards might offer temporary relief but can sometimes worsen symptoms or cause bite changes if not properly adjusted.
| Feature | Custom-Fitted TMJ Mouth Guard (Splint) | Over-the-Counter (Boil-and-Bite) Night Guard |
|---|---|---|
| Fit | Precisely molded to your teeth by a dentist | Self-molded at home; less precise and secure |
| Material | Durable, medical-grade acrylic or composite | Softer, less durable plastic |
| Effectiveness | Highly effective for reducing muscle activity, stabilizing bite, protecting teeth, and relieving joint stress | May offer temporary relief but can shift bite or worsen symptoms long-term |
| Comfort | Designed for maximum comfort and minimal interference with speech | Can be bulky, uncomfortable, and difficult to keep in place |
| Durability | Lasts for several years with proper care | Wears down quickly, often needs frequent replacement |
| Cost | $300 - $2,500 (depending on type and complexity) | $20 - $100 |
| Professional Oversight | Essential for proper fitting, adjustment, and monitoring | None; relies on user's ability to fit correctly |
| Risk of Bite Changes | Low, especially with stabilization splints and regular adjustments | Higher risk if worn improperly or for extended periods |
5. Botulinum Toxin (Botox) Injections:
- Mechanism: Botox can be injected directly into the jaw muscles (masseter, temporalis) to relax them and reduce their strength, thereby decreasing clenching, grinding, and muscle-related pain.
- Effectiveness: Provides temporary relief (typically 3-6 months) and can be very effective for myofascial pain that hasn't responded to other conservative treatments.
- Cost: $400 - $1,500 per treatment, depending on the number of units used and the provider. Not always covered by insurance.
Minimally Invasive Procedures
If conservative treatments are insufficient, your doctor might recommend these less invasive options.
1. Arthrocentesis (Joint Lavage):
- Process: Involves inserting small needles into the joint space and flushing it with sterile fluid (saline or Ringer's lactate). This washes out inflammatory byproducts and can help relieve pain and improve joint mobility, especially in cases of "closed lock" due to disc displacement.
- Cost: $500 - $2,000 per joint, often covered by medical insurance if deemed medically necessary.
- Recovery: Quick, often same-day.
2. TMJ Arthroscopy:
- Process: A surgeon makes a small incision and inserts a thin, lighted tube (arthroscope) with a camera into the joint space. This allows for direct visualization of the joint. Small instruments can be used to remove inflamed tissue, flush the joint, or even reposition a displaced disc in some cases.
- Use: Primarily for diagnosis and treatment of internal derangements or inflammatory conditions that haven't responded to arthrocentesis.
- Cost: $2,000 - $7,000 per joint, often covered by medical insurance.
- Recovery: A few days to a week for initial recovery, with full functional recovery over several weeks.
Surgical Interventions (Last Resort)
Surgery is rarely necessary for TMJ disorders and is typically considered only after all other conservative and minimally invasive approaches have failed and the patient has persistent, severe pain and dysfunction.
1. Arthroplasty (Open-Joint Surgery):
- Process: This involves making an incision in front of the ear to directly access the TMJ. The surgeon can then repair or remove damaged tissue, reshape bone, reposition the disc, or remove adhesions.
- Use: For severe structural problems, extensive disc damage, or degenerative joint disease that is causing significant symptoms.
- Risks: Higher risks compared to less invasive procedures, including infection, nerve damage (facial nerve), bleeding, and longer recovery times.
- Cost: $5,000 - $15,000+ per joint, depending on complexity, typically covered by medical insurance.
2. Total Joint Replacement:
- Process: In very severe cases where the joint is completely damaged (e.g., due to severe arthritis, trauma, or failed previous surgeries), the TMJ can be replaced with a prosthetic joint.
- Use: Reserved for extreme joint degeneration or dysfunction.
- Risks: Significant surgical risks and long recovery.
- Cost: $20,000 - $50,000+ per joint, making it one of the most expensive temporomandibular joint dysfunction treatments. Usually covered by medical insurance for severe cases.
| Treatment Type | Description | Approximate Cost (US, without insurance) | Typical Recovery/Timeline | Pros | Cons |
|---|---|---|---|---|---|
| Self-Care | Lifestyle changes, diet modification, exercises | $0 - $100 (for basic supplies) | Ongoing | Low cost, no side effects, patient-controlled | Requires discipline, may not be sufficient alone |
| OTC Meds | NSAIDs, pain relievers | $10 - $30 per month | Short-term relief | Readily available, inexpensive | Can have side effects (GI issues), not for chronic pain |
| Prescription Meds | Muscle relaxants, antidepressants, corticosteroids | $20 - $200+ per month | Varies | Targeted relief, improved sleep | Side effects (drowsiness, dry mouth), may require ongoing prescription |
| Physical Therapy | Manual therapy, exercises, modalities | $50 - $200 per session | Weeks to months | Non-invasive, addresses root causes, long-term benefits | Requires commitment, multiple sessions needed |
| TMJ Mouth Guard | Custom-fitted oral appliance (splint) | $300 - $2,500 | Immediate protection, long-term use | Non-invasive, protects teeth, stabilizes joint, reduces muscle activity | Initial discomfort, requires adjustment, can be lost, not always covered by dental insurance |
| Botox Injections | Injections into jaw muscles | $400 - $1,500 per treatment | 3-6 months (temporary) | Effective for muscle pain, minimally invasive | Temporary, requires repeat injections, not always covered by insurance |
| Arthrocentesis | Flushing the joint with fluid | $500 - $2,000 | Days | Minimally invasive, rapid relief for some | May require repeat procedures, not effective for all types of TMD |
| TMJ Arthroscopy | Camera-guided surgery, minor joint repairs | $2,000 - $7,000 | Weeks | Minimally invasive surgery, direct visualization | Surgical risks (infection, nerve damage), limited scope for severe issues |
| Open-Joint Surgery | Direct access to joint for major repair/reconstruction | $5,000 - $15,000+ | Months | Addresses severe structural problems | Major surgery, higher risks (nerve damage), longer recovery, last resort |
| Joint Replacement | Replacement with prosthetic joint | $20,000 - $50,000+ | Months to years | Solution for irreparable joint damage | Major surgery, highest risks, long-term maintenance, rare procedure |
Step-by-Step Process for TMJ Disorder Treatment
The journey to relief from TMJ disorder typically follows a structured, step-wise approach, starting with the least invasive methods.
1. Initial Consultation and Diagnosis:
- First Appointment: Your primary care physician or dentist is usually the first point of contact. They will conduct a thorough physical examination, take a detailed medical history, and discuss your symptoms.
- Referral: If TMJ disorder is suspected, you may be referred to a specialized dentist (like an oral and maxillofacial surgeon, prosthodontist, or orofacial pain specialist) or an ENT (ear, nose, throat) doctor.
- Diagnostic Imaging: Depending on the initial findings, X-rays, CT scans, or MRI may be ordered to assess the joint's condition and rule out other issues.
- Diagnosis: Based on the clinical exam and imaging, a specific diagnosis of the type of TMJ disorder will be made.
2. Conservative Management Phase (Weeks to Months):
This is the most common and often effective first line of treatment.
- Patient Education: You'll receive information about TMJ disorder, self-care strategies, and realistic expectations for treatment.
- Self-Care Implementation: Begin with warm/cold compresses, soft diet, stress reduction techniques, and avoiding habits like gum chewing.
- Medication Trial: OTC pain relievers (NSAIDs) will likely be recommended first. If insufficient, your doctor might prescribe muscle relaxants, low-dose antidepressants, or stronger anti-inflammatory drugs.
- Oral Appliance (TMJ Mouth Guard): If bruxism or clenching is a significant factor, a custom-fitted stabilization splint (mouth guard) will be fabricated.
- Impression Taking: Your dentist will take impressions of your teeth.
- Fabrication: The impression is sent to a dental lab to create a custom appliance. This usually takes 1-2 weeks.
- Fitting and Adjustment: You'll return for a fitting appointment where the dentist ensures the guard fits comfortably and your bite is correct. Multiple adjustment appointments may be needed over the first few weeks to ensure optimal fit and effectiveness.
- Physical Therapy Referral: Many patients benefit from specific jaw exercises and manual therapy from a physical therapist specializing in craniomandibular disorders.
- Monitoring and Adjustment: You'll have follow-up appointments (e.g., every 2-4 weeks initially) to monitor your symptoms, adjust medications, or refine your oral appliance.
3. Intermediate Interventions (If Conservative Fails - Months):
If conservative measures don't provide sufficient relief after several weeks or months, the next steps may include:
- Botox Injections: If muscle pain is persistent, Botox injections may be administered into the masticatory muscles. This is typically an in-office procedure.
- Arthrocentesis: This minimally invasive procedure involves flushing the joint and is usually performed in an outpatient setting. You may experience some soreness for a day or two.
4. Advanced/Surgical Interventions (Last Resort - Months to Years):
Only considered after all other treatments have been thoroughly explored and failed.
- TMJ Arthroscopy: An outpatient surgical procedure that involves small incisions and a camera to visualize and treat minor joint issues. Recovery typically involves a few days of rest and a gradual return to normal activities over several weeks.
- Open-Joint Surgery (Arthroplasty): A more invasive procedure requiring a longer recovery. Hospital stay might be one or two nights. Recovery can involve a period of soft diet, physical therapy, and pain management for several months.
- Total Joint Replacement: The most complex and invasive option, requiring a hospital stay and an extensive rehabilitation period.
Throughout the entire process, clear communication with your healthcare team is vital. Be sure to report any changes in your symptoms, side effects of medications, or discomfort from appliances. The goal is to find the least invasive yet most effective treatment strategy for your specific condition.
Cost and Insurance for TMJ Disorder Treatments
Understanding the financial aspects of TMJ disorder treatment in the US can be complex, as costs vary widely and insurance coverage depends on whether your condition is classified as a medical or dental issue.
Average US Price Ranges (Without Insurance):
- Initial Consultation & Diagnosis:
- General Dentist/Physician: $100 - $300
- Specialist (Oral & Maxillofacial Surgeon, Orofacial Pain Specialist): $200 - $500
- X-rays: $50 - $200
- MRI: $500 - $2,500 (can be higher in some regions)
- CT Scan: $300 - $1,500
- Conservative Treatments:
- OTC Medications: $10 - $30 per month
- Prescription Medications: $20 - $200+ per month (generic vs. brand, insurance plan)
- Physical Therapy: $50 - $200 per session (average 6-12 sessions initially)
- Custom TMJ Mouth Guard (Oral Appliance/Splint): $300 - $2,500 (depends on material, complexity, and region)
- Minimally Invasive Procedures:
- Botox Injections: $400 - $1,500 per treatment (requires repeat injections every 3-6 months)
- Arthrocentesis: $500 - $2,000 per joint
- TMJ Arthroscopy: $2,000 - $7,000 per joint
- Surgical Interventions:
- Open-Joint Surgery (Arthroplasty): $5,000 - $15,000+ per joint
- Total Joint Replacement: $20,000 - $50,000+ per joint
Regional Variations: Costs can be significantly higher in major metropolitan areas (e.g., New York, Los Angeles) compared to rural areas or states with lower costs of living.
Insurance Coverage Details:
- Medical vs. Dental Insurance: This is often the biggest hurdle.
- Medical Insurance: Typically covers medically necessary procedures. TMJ disorders are often classified as medical conditions, especially when they involve pain, joint dysfunction, or require injections, physical therapy, or surgery.
- Dental Insurance: Primarily covers routine dental care, fillings, crowns, and sometimes simple extractions. Many dental plans do not cover treatment for TMJ disorders, especially custom splints or advanced procedures, unless it's specifically listed as a benefit. However, if the cause of your TMJ is directly related to a dental issue (e.g., severe malocclusion requiring orthodontics, or damaged teeth from grinding), some dental plans might cover portions.
- Pre-authorization: For most TMJ treatments beyond basic consultations and X-rays, especially for oral appliances, injections, or any surgery, insurance companies almost always require pre-authorization. This means your dentist or doctor must submit documentation to your insurance company to prove medical necessity before treatment begins. Without pre-authorization, your claim may be denied.
- Deductibles, Co-pays, and Co-insurance: You will still be responsible for your plan's deductible (the amount you pay before insurance kicks in), co-pays for office visits or medications, and co-insurance (a percentage of the cost after your deductible is met).
- "Experimental" Treatments: Some insurance companies may consider certain TMJ treatments (like some types of splints or specific injections) "experimental" or "investigational" and may deny coverage. Your doctor may need to provide strong justification.
- HMO vs. PPO:
- HMO (Health Maintenance Organization): Typically requires referrals from your primary care physician and limits you to a network of providers. Costs are generally lower, but choice is restricted.
- PPO (Preferred Provider Organization): Offers more flexibility in choosing providers (in-network or out-of-network) but usually has higher deductibles and co-insurance for out-of-network services.
Pro Tip: Always call your medical and dental insurance providers directly to understand your specific benefits for TMJ diagnosis and treatment. Ask specific questions about:
- Coverage for oral appliances (splints/mouth guards) – ask if it's covered under "medical" or "dental" and what codes they typically approve.
- Coverage for physical therapy.
- Coverage for specific injections (e.g., Botox, corticosteroids).
- Coverage for diagnostic imaging (MRI, CT).
- Requirements for pre-authorization or referrals.
Recovery and Aftercare
Recovery from TMJ disorder treatment is highly variable, depending on the severity of the condition and the type of treatment received. However, ongoing aftercare is almost always necessary to maintain relief and prevent recurrence.
Post-Treatment Care Instructions:
- Conservative Treatments (Medications, Physical Therapy, Oral Appliances):
- Consistency is Key: Continue wearing your TMJ mouth guard as prescribed, even if you feel better. Stopping prematurely can lead to symptom relapse.
- Adherence to PT: Diligently perform prescribed jaw exercises and stretches at home.
- Medication Schedule: Follow your medication regimen carefully. Do not stop without consulting your doctor.
- Soft Diet: Continue with a soft diet for a period after pain subsides, gradually reintroducing tougher foods. Avoid extremely hard or chewy items long-term.
- Stress Management: Integrate stress-reduction techniques into your daily routine. This is crucial for long-term management.
- Regular Follow-ups: Attend all scheduled follow-up appointments with your dentist or specialist for adjustments to your oral appliance or treatment plan.
- Minimally Invasive Procedures (Botox, Arthrocentesis, Arthroscopy):
- Pain Management: You may experience soreness, swelling, or bruising for a few days. Follow your doctor's instructions for pain medication.
- Ice Packs: Apply ice to the treated area to reduce swelling.
- Soft Diet: Maintain a soft diet initially, gradually transitioning back to normal foods as comfort allows.
- Restricted Movement: Your doctor might advise limiting wide jaw movements for a short period.
- Physical Therapy: Often recommended after these procedures to restore full range of motion and strengthen muscles.
- Follow-up Appointments: Essential to monitor healing and ensure treatment effectiveness.
- Surgical Interventions (Open-Joint Surgery, Joint Replacement):
- Hospital Stay: Expect a hospital stay (1-7 days) depending on the extent of the surgery.
- Significant Pain Management: Prescription pain medication will be necessary.
- Dietary Restrictions: A liquid or very soft diet will be mandatory for an extended period (weeks to months).
- Physical Therapy/Rehabilitation: This is a critical component of recovery, starting soon after surgery and continuing for several months to regain jaw function.
- Activity Restrictions: Avoid strenuous activities, heavy lifting, and any impact to the jaw.
- Incision Care: Follow specific instructions for caring for the surgical incision to prevent infection.
- Long-Term Follow-up: Regular and long-term follow-up with your surgeon and physical therapist is essential to monitor healing, prevent complications, and optimize functional outcomes.
Long-Term Management:
Even after successful treatment, many TMJ disorder patients benefit from ongoing vigilance. This may include:
- Continued use of a night guard for bruxism protection.
- Periodic dental check-ups to monitor bite and joint health.
- Ongoing stress management practices.
- Maintaining good posture.
- Avoiding habits that strain the jaw.

The goal is not just to alleviate immediate symptoms but to establish a sustainable lifestyle that supports jaw health and minimizes the risk of future flare-ups.
Prevention of TMJ Disorder
While not all TMJ disorders are preventable (e.g., those caused by severe trauma or autoimmune diseases), many cases, particularly those related to muscle pain and disc displacement, can be mitigated or prevented by adopting certain habits and practices.
Key Prevention Strategies:
- Manage Stress: Since stress is a major trigger for teeth clenching and grinding, finding healthy ways to manage it is paramount. This includes:
- Regular exercise
- Meditation or mindfulness
- Yoga or tai chi
- Adequate sleep
- Seeking counseling or therapy if stress is overwhelming
- Avoid Jaw Overuse and Habits:
- Limit Chewing Gum: Frequent gum chewing overworks the jaw muscles.
- Avoid Hard/Chewy Foods: Minimize foods like hard candies, tough meats, nuts, and ice that require excessive chewing force.
- Break Bad Habits: Stop nail-biting, pen-chewing, or habitually propping your chin on your hand.
- Avoid Extreme Jaw Movements: Try not to open your mouth too wide when yawning or singing.
- Address Bruxism and Clenching:
- Awareness: Become aware of when you are clenching or grinding, especially during the day (e.g., when concentrating, driving, or stressed). Consciously relax your jaw.
- Night Guards: If you clench or grind at night, a custom TMJ mouth guard (night guard) can protect your teeth and jaw joints from excessive force. Your dentist can fabricate one.
- Maintain Good Posture: Poor posture, particularly forward head posture, can strain the neck and jaw muscles.
- Ergonomics: Ensure your workstation is ergonomically sound, with your computer screen at eye level and your chair supporting your lower back.
- Head Position: Keep your head balanced over your spine, avoiding prolonged jutting forward.
- Protect Your Jaw from Trauma: Wear a mouthguard during contact sports to protect your teeth and jaw from impact.
- Regular Dental Check-ups: Regular visits allow your dentist to monitor your bite, identify early signs of bruxism or malocclusion, and recommend preventative measures.
- Balanced Diet and Hydration: A healthy diet supports overall joint health, and proper hydration can help muscle function.
- Limit Caffeine and Alcohol: These can sometimes exacerbate clenching or disrupt sleep, both of which can worsen TMJ symptoms.
By being mindful of these factors and proactively incorporating preventative measures into your lifestyle, you can significantly reduce your risk of developing a TMJ disorder or manage existing symptoms more effectively.
Risks and Complications of TMJ Disorder and Its Treatments
While most TMJ disorders are manageable, and treatments are generally safe, it's important to be aware of potential risks and complications, both from the untreated condition and the interventions.
Risks and Complications of Untreated TMJ Disorder:
- Chronic Pain: Persistent jaw, facial, head, and neck pain can become debilitating, severely impacting quality of life, sleep, and mental well-being.
- Permanent Joint Damage: Long-standing disc displacement, inflammation, or degenerative changes can lead to irreversible damage to the joint cartilage and bone.
- Limited Jaw Function: Progressive loss of ability to open the mouth wide, making eating, speaking, and oral hygiene difficult. Permanent "closed lock" can occur.
- Malnutrition: Due to severe pain or inability to chew, some individuals may struggle to maintain a balanced diet.
- Psychological Impact: Chronic pain conditions, including TMJ disorder, are strongly linked to anxiety, depression, and social isolation.
- Dental Issues: Untreated bruxism can lead to cracked teeth, excessive tooth wear, sensitivity, and damage to existing dental work.
Risks and Complications of TMJ Treatments:
- Medications:
- NSAIDs: Long-term use can cause gastrointestinal issues (ulcers, bleeding), kidney problems, and increased risk of cardiovascular events.
- Muscle Relaxants/Antidepressants: Drowsiness, dizziness, dry mouth, constipation, and other side effects.
- Corticosteroid Injections: While effective, repeated injections into the joint can potentially weaken joint tissues or lead to bone degradation.
- Oral Appliances (TMJ Mouth Guards):
- Incorrect Fit: A poorly fitted mouth guard can worsen pain, shift your bite, or even damage teeth. This emphasizes the importance of custom-made appliances from a qualified dentist.
- Initial Discomfort: Some people experience temporary discomfort, increased saliva, or difficulty speaking initially.
- Dependency: In rare cases, some individuals feel "dependent" on their guard for comfort.
- Botox Injections:
- Temporary Weakness: Temporary weakness of surrounding muscles, leading to difficulty chewing certain foods or a "frozen" facial expression (rare with experienced injectors).
- Bruising/Swelling: At the injection site.
- Asymmetry: Very rarely, temporary facial asymmetry.
- Allergic Reaction: Rare.
- Minimally Invasive Procedures (Arthrocentesis, Arthroscopy):
- Infection: Risk is low but present with any invasive procedure.
- Nerve Damage: Potential for temporary or, rarely, permanent damage to small nerves around the joint, leading to numbness.
- Bleeding/Swelling: Common but usually resolves quickly.
- Limited Effectiveness: May not fully resolve symptoms for all patients, or symptoms may recur.
- Surgical Interventions (Open-Joint Surgery, Joint Replacement):
- Higher Surgical Risks: General anesthesia risks, infection, significant bleeding, scarring.
- Facial Nerve Damage: The facial nerve runs very close to the TMJ, making it vulnerable during surgery. Damage can lead to temporary or permanent facial paralysis or weakness.
- Ear Canal Damage: Proximity to the ear canal carries a risk of damage, affecting hearing or balance.
- Failed Surgery: Symptoms may not improve, or new problems may arise after surgery.
- Hardware Complications: For joint replacements, issues like loosening, fracture, or infection of the prosthetic components can occur.
- Extended Recovery: Long and often challenging recovery periods with significant dietary and activity restrictions.
Always discuss the potential risks and benefits of any recommended treatment with your healthcare provider. The ADA generally advocates for the least invasive, reversible treatments first due to the potential for complications with more aggressive interventions.
Children and Pediatric Considerations
TMJ disorders are not exclusive to adults; they can also affect children and adolescents, though the presentation and management may differ. It's crucial for parents and pediatricians to recognize the signs, as early intervention can prevent long-term complications.
How TMJ Affects Children:
- Symptoms: Children may experience similar symptoms to adults, including jaw pain, headaches (often misdiagnosed as tension headaches), earaches, clicking or popping sounds in the jaw, and difficulty opening their mouth. However, they might express pain differently or simply avoid certain foods.
- Prevalence: Studies suggest that TMJ symptoms can be present in a significant percentage of children and adolescents, with some research indicating up to 10-15% of adolescents report some form of TMJ pain or dysfunction. Girls are more commonly affected than boys, similar to adults.
- Growth and Development: TMJ disorders in children can potentially impact facial growth and development, making early diagnosis even more critical.
Unique Challenges in Children:
- Diagnosis Difficulty: Children may struggle to articulate their symptoms precisely, and parents or pediatricians might not immediately consider TMJ disorder. Symptoms like headaches or earaches are often attributed to more common childhood ailments.
- Causes: While bruxism (teeth grinding) is common in children, often resolving on its own, persistent and symptomatic bruxism can contribute to TMJ issues. Trauma (sports injuries, falls) and orthodontic treatments (though often beneficial, can sometimes temporarily exacerbate symptoms) are also potential factors.
- Treatment Approach: Treatment in children is almost always conservative and focuses on supporting normal growth and development while alleviating symptoms.
Diagnosis and Treatment Differences:
- Diagnosis: A thorough clinical examination by a pediatric dentist or an oral and maxillofacial surgeon with experience in children is essential. Imaging is used judiciously due to radiation concerns, often starting with less invasive options like panoramic X-rays before considering MRI if absolutely necessary.
- Conservative Treatments:
- Education: Teaching parents and children about jaw health, posture, and stress management.
- Soft Diet: Encouraging a diet that doesn't strain the jaw.
- Gentle Exercises: Simple jaw exercises to improve mobility.
- Oral Appliances: Custom-made pediatric TMJ mouth guards (splints) may be used, particularly for night grinding, carefully designed to not interfere with erupting teeth or jaw growth.
- Physical Therapy: Specialized pediatric physical therapy may be recommended.
- Medications: Over-the-counter pain relievers are usually the first choice, with prescription medications used very cautiously and for short durations.
- Orthodontics: If malocclusion is a significant contributing factor, orthodontic treatment might be considered, but often after TMJ pain has been managed, not as a primary treatment for the TMJ disorder itself.
- Surgery: Surgical interventions are extremely rare in children and are only considered in cases of severe trauma, ankylosis (fusion of the joint), or significant developmental abnormalities that cannot be addressed by other means.
Parents who suspect their child may have a TMJ disorder should seek an evaluation from a dentist or specialist experienced in pediatric orofacial pain. Early detection and conservative management can make a significant difference in a child's comfort and long-term oral health.
Cost Breakdown of TMJ Disorder Treatments
To provide a clearer picture of potential expenses, here's a detailed cost breakdown for common TMJ treatments in the US, considering both insured and uninsured scenarios, along with strategies for managing costs.
Average US Costs (Ranges):
| Service/Treatment | Low End (US$) | Mid Range (US$) | High End (US$) | Notes |
|---|---|---|---|---|
| Initial Consultation | 100 | 250 | 500 | Specialist visits tend to be higher. |
| Panoramic X-ray | 50 | 150 | 250 | Basic imaging. |
| TMJ MRI | 500 | 1,500 | 2,500+ | Gold standard for soft tissue, highly variable by region/facility. |
| TMJ CT Scan | 300 | 800 | 1,500 | For bone assessment. |
| Custom TMJ Mouth Guard (Splint) | 300 | 1,200 | 2,500 | Material, complexity, and adjustments included. |
| Physical Therapy (per session) | 50 | 120 | 200 | Typically 6-12 sessions initially. |
| Botox Injections (per treatment) | 400 | 800 | 1,500 | Depends on units used and provider. Repeat treatments needed. |
| Arthrocentesis (per joint) | 500 | 1,200 | 2,000 | Outpatient procedure. |
| TMJ Arthroscopy (per joint) | 2,000 | 4,500 | 7,000 | Minimally invasive surgery. |
| Open-Joint Surgery (per joint) | 5,000 | 10,000 | 15,000+ | Includes surgeon fees, anesthesia, facility fees. |
| Total Joint Replacement (per joint) | 20,000 | 35,000 | 50,000+ | Very complex, includes prosthetic components. |
With vs. Without Insurance:
- Without Insurance: You will be responsible for 100% of the costs. This is why many people opt for the most conservative treatments first. Negotiating cash prices with providers may be an option.
- With Insurance (Medical):
- After meeting your deductible (which could range from $500 to $7,000+ for high-deductible plans), your medical insurance typically covers a percentage of the "allowed amount" (often 80-90% for in-network providers) for medically necessary services like consultations, imaging (MRI, CT), physical therapy, Botox injections, arthrocentesis, and surgery.
- You will pay a co-pay for office visits (e.g., $20-$75) and a co-insurance (e.g., 10-20% of the cost after deductible).
- Check your out-of-pocket maximum, as once you reach this limit, your insurance should cover 100% of approved costs for the remainder of the year.
- With Insurance (Dental):
- Dental insurance rarely covers comprehensive TMJ treatment beyond basic diagnostic X-rays or potentially a portion of a custom night guard (if categorized as an "occlusal guard for bruxism" rather than TMJ treatment).
- Coverage for oral appliances, if available, is often limited to a percentage (e.g., 50%) after a deductible, and may have a lower annual maximum benefit (e.g., $1,000-$2,000).
Payment Plans and Financing Options:
- In-Office Payment Plans: Many dental and medical offices offer interest-free payment plans for a limited period or flexible payment schedules.
- Healthcare Credit Cards: Services like CareCredit or Alphaeon Credit offer special financing options with deferred interest for healthcare expenses, if paid off within a certain timeframe.
- Personal Loans: Banks or credit unions offer personal loans, but these come with interest.
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): If you have an HSA or FSA through your employer, you can use these tax-advantaged accounts to pay for qualified medical expenses, including TMJ treatments.
Cost-Saving Tips:
- Verify Insurance Coverage: This is the most crucial step. Call both your medical and dental insurance companies.
- Seek Referrals Wisely: Start with your general dentist, who may offer more affordable initial assessments or referrals to in-network specialists.
- Shop Around for Imaging: For MRI or CT scans, ask if different imaging centers have varying prices, even within the same insurance network.
- Consider Academic Institutions: Dental schools or university hospitals sometimes offer lower costs for treatment, often with highly experienced specialists overseeing student care.
- Generic Medications: Always ask for generic alternatives for prescription medications to save costs.
- Second Opinions: Especially for costly or invasive procedures, getting a second opinion can help ensure the recommended treatment is truly necessary and cost-effective.
- Preventative Care: Investing in early preventative measures (e.g., a good TMJ mouth guard to prevent further damage from bruxism) can save significant money down the line by avoiding more complex and expensive treatments.
Frequently Asked Questions
What is the primary cause of TMJ disorder?
The exact cause of TMJ disorder is often multifactorial, meaning several factors contribute. Common causes include trauma to the jaw, head, or neck; teeth grinding (bruxism) and clenching; stress; various forms of arthritis (like osteoarthritis); and structural problems within the joint, such as disc displacement.
Can a TMJ mouth guard really help with TMJ pain?
Yes, a custom-fitted TMJ mouth guard (also known as an occlusal splint or night guard) is one of the most common and effective conservative treatments. It works by creating a stable bite, reducing the impact of teeth grinding and clenching, and allowing the jaw muscles to relax, thereby alleviating pain and protecting the joint.
What are the main temporomandibular joint dysfunction treatments available?
Treatments range from conservative to surgical. First-line treatments include self-care (soft diet, warm/cold packs, stress management), medications (NSAIDs, muscle relaxants), physical therapy, and custom oral appliances like a TMJ mouth guard. If these fail, options like Botox injections, arthrocentesis, or arthroscopy may be considered, with open-joint surgery or total joint replacement reserved as a last resort for severe cases.
How long does it take to recover from TMJ disorder?
Recovery time varies greatly. For mild cases treated with conservative methods like self-care and a mouth guard, improvement can be seen within weeks to a few months. More invasive procedures, like TMJ arthroscopy, may require a few weeks of recovery, while open-joint surgery or total joint replacement can involve several months to a year of rehabilitation.
Is TMJ pain constant, or does it come and go?
TMJ pain can be either constant or intermittent. Many people experience flare-ups during periods of stress, after eating certain foods, or upon waking if they've been clenching their jaw at night. Others might experience persistent, chronic pain that fluctuates in intensity throughout the day.
Can TMJ disorder affect my ears or hearing?
Yes, TMJ disorder can commonly cause symptoms that mimic ear problems. These include earaches, a feeling of fullness in the ear, ringing in the ears (tinnitus), and sometimes even temporary changes in hearing. This is because the TMJ is located very close to the ear canal, and muscle spasms or inflammation can irritate nearby nerves and structures.
Is TMJ disorder always accompanied by clicking or popping sounds?
No, not all TMJ disorders involve clicking or popping sounds. While these sounds are common indicators of disc displacement within the joint, many people with TMJ disorder primarily experience pain, muscle tenderness, or limited jaw movement without any audible clicks or pops.
Will my insurance cover TMJ treatments?
Insurance coverage for TMJ treatments can be tricky. Medical insurance often covers diagnosis, physical therapy, medications, and surgical procedures if deemed medically necessary. However, coverage for oral appliances (like a TMJ mouth guard) can fall into a grey area, sometimes covered by medical, sometimes by dental, or sometimes not at all. Always contact both your medical and dental insurance providers for specific benefit details and pre-authorization requirements.
Can stress cause TMJ disorder?
While stress itself doesn't directly cause TMJ disorder, it is a significant contributing factor and can severely exacerbate symptoms. Stress often leads to unconscious jaw clenching and teeth grinding (bruxism), which puts excessive strain on the TMJ and surrounding muscles, leading to pain and inflammation. Managing stress is a crucial part of both preventing and treating TMJ disorders.
What happens if TMJ disorder is left untreated?
If left untreated, TMJ disorder can lead to chronic pain, progressive damage to the jaw joint (including irreversible cartilage and bone degeneration), severely limited jaw movement, and persistent headaches and facial pain. It can also significantly impact chewing ability, sleep quality, and overall mental health due to chronic discomfort. Early intervention is generally recommended to prevent these complications.
When to See a Dentist
Recognizing when to seek professional help for jaw discomfort is crucial for preventing a TMJ disorder from worsening and for finding effective relief.
Clear Warning Signs That Need Attention:
- Persistent Jaw Pain: If you experience ongoing pain or tenderness in your jaw, face, ear, or neck that doesn't improve with basic self-care (like soft diet, warm compresses) within a few days or weeks.
- Difficulty Chewing or Swallowing: If eating becomes painful, challenging, or your bite feels consistently "off."
- Limited Jaw Movement: If you struggle to open your mouth wide, or if your jaw feels stiff and restricted.
- Frequent Clicking, Popping, or Grating Sounds (with Pain): While occasional, painless jaw sounds can be normal, if these sounds are accompanied by pain, discomfort, or lockjaw, it's a sign to see a professional.
- Jaw Locking: If your jaw locks in an open or closed position, making it impossible to move, this warrants immediate attention.
- Chronic Headaches or Earaches: If you experience recurrent headaches, migraines, or earaches that aren't explained by other conditions (like sinusitis or ear infections), TMJ disorder could be the underlying cause.
- Facial Swelling: Unexplained swelling on one side of your face around the jaw joint.
- Changes in Bite: A sudden, noticeable change in how your upper and lower teeth fit together.
Red Flags vs. Routine Care Guidance:
- Routine Care: If you have mild, occasional jaw discomfort that resolves quickly with self-care (e.g., after eating a particularly chewy meal), you can mention it at your next regular dental check-up. Your dentist can monitor for signs of bruxism or clenching.
- Red Flags/Emergency: Jaw locking, severe acute pain, or pain accompanied by facial weakness, fever, or vision changes should prompt a more urgent visit to your dentist, an oral surgeon, or even an emergency room if symptoms are severe and rapidly escalating.
Don't ignore persistent jaw discomfort. Your general dentist is usually the best first point of contact, as they can accurately assess your condition, rule out dental issues, and refer you to a TMJ specialist (like an oral and maxillofacial surgeon, prosthodontist, or orofacial pain specialist) if needed. Early diagnosis and intervention can significantly improve outcomes and prevent the condition from progressing to more severe or chronic stages.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Tmj Massage Near Me: Complete Guide
Temporomandibular joint disorder, commonly known as TMJD, affects millions of Americans, causing debilitating pain, discomfort, and significantly impacting quality of life. If you're experiencing jaw pain, clicking, or difficulty chewing, you're not alone. Up to 15% of American adults experience
February 23, 2026
Tmd Treatment: Complete Guide
Experiencing persistent jaw pain, clicking sounds when you chew, or debilitating headaches that seem to originate from your face? You're not alone. Temporomandibular joint (TMJ) disorders, often referred to collectively as TMD, affect an estimated 10 million Americans, with women disproportionat
February 23, 2026
Tmj Nerve Damage Symptoms: Complete Guide
Experiencing persistent facial pain, numbness, or tingling can be distressing, especially when the source is unclear. While many people are familiar with general jaw pain associated with temporomandibular joint (TMJ) disorders, the less commonly understood aspect of tmj nerve damage symptoms can
February 23, 2026
Remi Night Guard: Complete Guide
Remi Night Guard: Complete Guide
February 23, 2026