Cat Bad Breath: Complete Guide

Key Takeaways
- A sweet, fresh breath is rarely a characteristic of our feline companions. However, if your cat's breath has taken a sudden turn for the worse, becoming strikingly offensive, it's a significant warning sign that something isn't right. This pervasive and foul odor, commonly referred to as **cat bad b
A sweet, fresh breath is rarely a characteristic of our feline companions. However, if your cat's breath has taken a sudden turn for the worse, becoming strikingly offensive, it's a significant warning sign that something isn't right. This pervasive and foul odor, commonly referred to as cat bad breath or feline halitosis, isn't just an unpleasant inconvenience; it's often a direct indicator of underlying health issues that demand your attention. In fact, studies show that over 70% of cats over the age of three suffer from some form of dental disease, a primary culprit behind pungent breath. Ignoring this seemingly minor problem can lead to severe pain, tooth loss, and even systemic health complications that could drastically impact your cat's quality of life and longevity. Understanding the causes, recognizing the symptoms, and knowing the appropriate treatment and prevention strategies are crucial for maintaining your beloved pet's overall well-being. This comprehensive guide will delve into every aspect of feline halitosis, from its diverse origins, including the oft-overlooked bad breath from throat issues, to the range of effective interventions, helping you protect your cat's health and restore their comfort. We will explore the various types of bad breath smells your cat might exhibit, what each could signify, and what steps you need to take to address them.
Key Takeaways:
- Prevalence: Over 70% of cats over three years old suffer from dental disease, the leading cause of bad breath.
- Early Detection is Key: Recognizing subtle changes in breath odor and oral behavior can prevent advanced disease.
- Comprehensive Veterinary Exam: A thorough dental exam, often requiring sedation, is essential for accurate diagnosis. Costs typically range from $50-$200 for the exam alone, prior to any procedures.
- Professional Dental Cleaning: Anesthesia-based dental cleanings are the gold standard for treating dental disease. Expect costs to range from $500-$1,200 for a routine cleaning, potentially rising to $1,500-$3,000+ if extractions or advanced procedures are needed.
- Home Dental Care: Regular brushing (daily is ideal), dental diets, and approved water additives can significantly reduce plaque and tartar buildup, costing $10-$50 monthly.
- Systemic Links: Bad breath can signal serious non-dental issues like kidney disease, diabetes, or liver problems, requiring immediate veterinary attention and potentially ongoing management.
- Prevention Strategy: A combination of annual veterinary check-ups (including oral exams), consistent home dental care, and a balanced diet is the most effective prevention against bad breath and associated diseases, with a commitment of lifelong care.
What Is Cat Bad Breath / Feline Halitosis?
Cat bad breath, clinically known as feline halitosis, is an unpleasant and persistent odor emanating from a cat's mouth. Unlike the relatively neutral breath of a healthy feline, halitosis in cats often presents as a strong, foul, or unusual smell that can range from decaying meat to ammonia-like or even sweet and fruity. It's important to understand that while cats naturally have a certain "cat breath" odor, a significantly offensive or sudden change in smell is never normal and almost always indicates an underlying health problem.

The primary cause of bad breath in cats stems from the accumulation of bacteria in the mouth. These bacteria, often found in plaque and tartar buildup on the teeth, release volatile sulfur compounds (VSCs) as they metabolize food particles and oral tissues. These VSCs are responsible for the characteristic foul odor. However, halitosis can also be a symptom of more serious systemic diseases affecting organs like the kidneys, liver, or pancreas, or even issues originating higher up in the digestive or respiratory tract, potentially leading to bad breath from throat complications. Recognizing the specific scent can provide critical clues about the root cause, guiding your veterinarian toward an accurate diagnosis and effective treatment plan.
Types / Variations of Cat Bad Breath Smells
The specific odor of your cat's bad breath can provide valuable clues about its origin. While all types signal a problem, some smells are more indicative of dental issues, while others point towards systemic diseases. Understanding these nuances is crucial for identifying potential health concerns early.
1. Decaying, Putrid, or Fishy Odor (Most Common)
This is the most frequent type of cat bad breath and is almost invariably linked to oral disease.
- Causes:
- Plaque and Tartar Buildup: The primary culprits. Bacteria accumulate on teeth, forming plaque, which hardens into tartar. These bacteria produce volatile sulfur compounds (VSCs) that smell foul.
- Gingivitis: Inflammation of the gums, often caused by plaque accumulation, leading to redness, swelling, and bleeding.
- Periodontal Disease: Advanced gum disease where infection extends below the gumline, destroying the supporting structures of the teeth. This often leads to deep pockets of infection, pus, and tissue decay, resulting in a strong, putrid smell.
- Tooth Resorption: A painful condition where a cat's tooth structure erodes. Exposed nerves and infected tissue can produce a foul odor.
- Stomatitis: Severe, widespread inflammation of the oral cavity, often extremely painful, leading to significant tissue destruction and a very offensive odor.
- Oral Abscesses or Infections: Localized pockets of pus from infected teeth or wounds.
- Oral Tumors: Malignant or benign growths in the mouth can become necrotic or infected, emitting a decaying smell.
- Trapped Food Particles: Food caught between teeth or in gum pockets can rot and contribute to the smell.
2. Ammonia-Like or Urine-Like Odor
This is a distinct and serious smell that typically indicates systemic illness rather than just dental disease.
- Causes:
- Kidney Disease: When a cat's kidneys fail to filter toxins from the blood effectively, waste products like urea accumulate. These can be exhaled, leading to an ammonia or urine-like smell. This is a strong indicator of severe kidney impairment and requires immediate veterinary attention.
3. Sweet or Fruity Odor
A less common but equally serious type of bad breath.
- Causes:
- Diabetes Mellitus: In uncontrolled diabetes, the body starts burning fat for energy, producing ketones. These ketones can be exhaled, giving the breath a distinctively sweet or fruity smell, similar to nail polish remover. This is a medical emergency requiring urgent diagnosis and treatment.
4. Musty, Moldy, or "Death-like" Odor
This extremely offensive smell is often associated with severe organ dysfunction.
- Causes:
- Liver Disease: When the liver isn't functioning properly, toxins can build up in the bloodstream. These toxins, if not processed, can cause a very distinct, musty, and often described as "death-like" or "cadaverous" odor to the breath. This is a grave sign and necessitates immediate veterinary intervention.
5. Feculent or Vomit-Like Odor
While less common as a persistent breath odor, it can occur.
- Causes:
- Gastrointestinal Issues: Severe vomiting, intestinal obstruction, or other digestive problems can sometimes cause a reflux of stomach contents or accumulation of foul-smelling gases that can manifest as bad breath.
- Coprophagia (eating feces): While more common in dogs, some cats may engage in this, leading to a temporary fecal odor on their breath.
Understanding these different types of bad breath smells can help you communicate more effectively with your veterinarian, providing crucial diagnostic clues. Any persistent or dramatically changed odor warrants a professional examination.
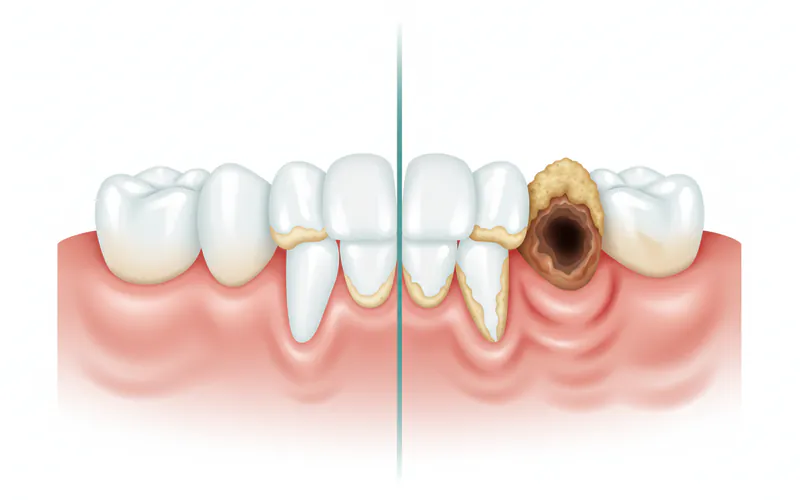
Causes / Why It Happens
Cat bad breath is a symptom, not a disease itself. It's a critical indicator that something is amiss with your feline friend's health. The causes are broadly categorized into oral/dental issues and systemic diseases.
A. Oral and Dental Diseases (Most Common Cause)
The vast majority of cat bad breath cases originate in the mouth. These conditions are progressive and, if left untreated, can lead to significant pain, tooth loss, and systemic health problems.
-
Plaque and Tartar Accumulation:
- Mechanism: After eating, food particles, saliva, and bacteria mix to form a sticky film called plaque on the teeth. If plaque isn't removed regularly (e.g., by brushing), it mineralizes within 24-72 hours into a hard, yellowish-brown substance called tartar (calculus). Tartar cannot be removed by brushing and provides a rough surface for more bacteria to adhere to.
- Impact: The bacteria trapped in plaque and tartar produce volatile sulfur compounds (VSCs) which are the primary source of the foul odor. This also irritates the gums.
-
- Mechanism: This is the initial stage of periodontal disease, characterized by inflammation of the gums (gingiva) in response to bacterial plaque accumulation.
- Impact: Gums appear red, swollen, and may bleed easily. While reversible with professional cleaning and good home care, it will progress if ignored, intensifying the bad breath.
-
- Mechanism: If gingivitis is left untreated, the inflammation and infection spread below the gumline, affecting the supporting structures of the tooth (ligaments, bone). This leads to the formation of periodontal pockets, where bacteria thrive and destroy tissue.
- Impact: This is the most common and significant cause of severe halitosis. It's incredibly painful, can lead to bone loss, receding gums, loose teeth, and eventually tooth loss. The chronic infection releases bacteria and inflammatory mediators into the bloodstream, potentially affecting vital organs like the heart, kidneys, and liver.
-
Tooth Resorption (FORLs - Feline Odontoclastic Resorptive Lesions):
- Mechanism: A common and agonizing condition where the cat's own body starts to break down and absorb the tooth structure, often starting at the gumline.
- Impact: These lesions are extremely painful, often covered by inflamed gum tissue, and can become infected, leading to severe bad breath. Estimates suggest over 50% of cats over 5 years old are affected.
-
Stomatitis:
- Mechanism: A severe and chronic inflammatory condition affecting the entire oral cavity, including the gums, palate, and back of the throat. The exact cause is unknown but is thought to be an overreaction of the cat's immune system to plaque bacteria.
- Impact: Causes extreme pain, difficulty eating, drooling, and a very strong, offensive odor due to widespread inflammation and potential ulceration. This condition can also lead to bad breath from throat as the inflammation extends into the pharynx.
-
Oral Injuries, Abscesses, and Tumors:
- Mechanism: Wounds from trauma (e.g., chewing on hard objects, falls), infected tooth roots forming abscesses, or cancerous/non-cancerous growths in the mouth can become necrotic or infected.
- Impact: Decaying tissue and bacterial infection within these lesions produce a very strong, putrid smell.
-
Foreign Objects:
- Mechanism: A small piece of food, string, bone fragment, or even plant material can get lodged between teeth, in the gums, or at the back of the throat.
- Impact: The trapped object can cause irritation, infection, and decay, leading to localized bad breath.
B. Systemic Diseases (Non-Oral Causes)
While less common than dental issues, systemic diseases are often more serious and life-threatening. The bad breath in these cases is a metabolic byproduct or a sign of organ failure.
-
Kidney Disease:
- Mechanism: Failing kidneys are unable to filter waste products (like urea) from the blood effectively.
- Impact: These waste products build up and are exhaled through the lungs, causing an ammonia-like or urine-like smell on the breath. This is a critical sign of severe kidney impairment.
-
Diabetes Mellitus:
- Mechanism: In uncontrolled diabetes, the body cannot utilize glucose for energy and begins to break down fat, producing ketones.
- Impact: These ketones are exhaled, giving the breath a distinctive sweet or fruity smell, often compared to nail polish remover. This indicates diabetic ketoacidosis, a life-threatening complication.
-
Liver Disease:
- Mechanism: A compromised liver cannot properly detoxify the body, leading to a buildup of various toxins in the bloodstream.
- Impact: These toxins can give the breath a musty, moldy, or "death-like" odor. Severe liver disease is a very serious condition.
-
Gastrointestinal Problems:
- Mechanism: Conditions like megacolon, foreign body obstruction, or severe inflammatory bowel disease can sometimes lead to the reflux of foul-smelling stomach contents or the accumulation of gases that cause a feculent odor.
- Impact: While not the most common cause of chronic bad breath, severe GI issues can contribute to it, especially if accompanied by vomiting or regurgitation.
-
Respiratory Tract Infections:
- Mechanism: Infections in the nasal passages, sinuses, or lungs (e.g., bacterial or fungal infections, viral conditions like feline calicivirus) can produce discharge and inflammation that contribute to foul odors, potentially causing bad breath from throat or nasal discharge that a cat licks.
- Impact: While primarily affecting the respiratory system, the proximity to the oral cavity means these can influence breath odor, especially if there's post-nasal drip.
-
Cancer (Oral or Systemic):
- Mechanism: Tumors anywhere in the body, but particularly in the mouth or digestive tract, can become necrotic (tissue dies) or infected.
- Impact: The decaying tissue and secondary infections produce a very strong, often putrid, odor.
Understanding these diverse causes highlights why a thorough veterinary examination is essential when you notice your cat has bad breath. Self-diagnosis can be dangerous, as the underlying condition could range from a treatable dental issue to a life-threatening systemic disease.
Signs and Symptoms
The most obvious sign of feline halitosis is the foul odor itself. However, because cats are masters at hiding pain and discomfort, it's crucial to look for other subtle signs and symptoms that might accompany bad breath, indicating an underlying problem.
1. The Odor Itself:
- Persistent Foul Smell: A strong, unpleasant odor from the mouth that doesn't dissipate.
- Specific Odors: Ammonia-like (kidney), sweet/fruity (diabetes), musty/putrid (liver, severe dental).
2. Changes in Eating Habits:
- Difficulty Chewing: Reluctance to eat hard food, preferring soft food, or dropping food from the mouth.
- Eating on One Side: Chewing only on one side of the mouth to avoid painful areas.
- Decreased Appetite: Reduced interest in food or refusal to eat due to pain.
- Weight Loss: A secondary symptom if pain or systemic illness prevents adequate food intake.
3. Oral Discomfort and Pain:
- Excessive Drooling (Ptyalism): Saliva may be thicker, discolored, or bloody.
- Pawing at the Mouth: Cats might rub their face or paw at their mouth frequently.
- Head Shyness: Reluctance to have their head or mouth touched.
- Gagging or Swallowing Difficulties: Especially if issues extend to the back of the throat.
- Bleeding Gums: Noticed on toys, food bowls, or during attempted brushing.
4. Visible Oral Changes:
- Red, Swollen, or Bleeding Gums (Gingivitis): Inflamed gum tissue, sometimes receding.
- Tartar Buildup: Yellowish-brown crusts on the teeth, especially near the gumline.
- Missing or Loose Teeth: Indicative of advanced periodontal disease.
- Discolored Teeth: Yellow, brown, or gray teeth can indicate trauma or decay.
- Oral Masses or Growths: Lumps, bumps, or ulcers inside the mouth, on the gums, tongue, or palate.
- Tooth Resorption Lesions: May appear as reddish "holes" or defects at the gumline, often covered by inflamed gum tissue.
5. Behavioral Changes:
- Irritability or Aggression: Due to chronic pain and discomfort.
- Lethargy or Reduced Activity: A general sign of illness, especially with systemic diseases.
- Hiding: Cats often hide when they are unwell or in pain.
- Changes in Grooming: Reduced grooming due to pain in the mouth, leading to a dull or unkempt coat.
6. Systemic Signs (Indicating Non-Oral Causes):
- Increased Thirst and Urination (Polydipsia/Polyuria): Common with kidney disease or diabetes.
- Vomiting or Diarrhea: Can be associated with gastrointestinal issues or severe systemic illness.
- Jaundice (Yellowing of Gums, Skin, Eyes): A sign of liver disease.
- Changes in Coat Quality: Dullness or poor condition.
If you observe any of these signs in conjunction with your cat's bad breath, it's imperative to schedule a veterinary appointment promptly. Early diagnosis and intervention can prevent further suffering and improve treatment outcomes.
Treatment Options
Treating cat bad breath effectively means addressing the underlying cause. Given that dental disease is the most common culprit, professional dental cleaning under anesthesia is often the first and most crucial step. However, treatment plans can vary widely depending on the diagnosis.
A. Professional Dental Cleaning (Anesthesia-Based)
This is the gold standard for treating dental disease and removing the primary source of foul breath in most cases.
- Description: Performed under general anesthesia for the cat's safety and to allow thorough examination and cleaning. It involves:
- Pre-Anesthetic Blood Work: To assess organ function and ensure the cat is a good candidate for anesthesia.
- Anesthesia and Monitoring: Comprehensive monitoring of heart rate, respiration, blood pressure, and oxygen saturation.
- Oral Examination: A detailed examination, often with dental X-rays, to assess the extent of disease below the gumline (where most periodontal disease resides).
- Scaling: Using ultrasonic and hand scalers to remove plaque and tartar from above and below the gumline.
- Polishing: Smoothing the tooth surfaces to prevent new plaque adhesion.
- Fluoride Treatment: To strengthen enamel and reduce sensitivity.
- Subgingival Lavage: Flushing periodontal pockets to remove debris and bacteria.
- Pros: Thorough cleaning, addresses subgingival disease, allows for full oral examination and X-rays, removes pain source.
- Cons: Requires general anesthesia (though modern anesthetic protocols are very safe), cost can be significant.
- Cost Range (US): Typically $500-$1,200 for a routine cleaning, potentially more in urban areas or with extensive pre-anesthetic work.
B. Dental Extractions
- Description: If teeth are severely diseased (e.g., advanced periodontal disease, severe tooth resorption, fractures), extraction may be necessary. This involves surgically removing the affected tooth.
- Pros: Eliminates the source of chronic pain and infection, prevents further systemic spread.
- Cons: Irreversible, requires advanced surgical skills, can be more costly and involve a longer recovery.
- Cost Range (US): Each extraction can add $50-$300+ to the overall dental procedure, depending on the tooth and complexity.
C. Antibiotics
- Description: Used to treat active oral infections (e.g., abscesses, severe gingivitis) or as part of a post-extraction regimen. Also used for systemic infections causing bad breath.
- Pros: Fights bacterial infection, reduces inflammation and pain.
- Cons: Can have side effects (GI upset), risk of antibiotic resistance with overuse, doesn't address the underlying cause of plaque/tartar buildup.
- Cost Range (US): $20-$100 depending on the type and duration of the prescription.
D. Anti-Inflammatory / Pain Medication
- Description: Non-steroidal anti-inflammatory drugs (NSAIDs) or other pain relievers may be prescribed pre- and post-procedure for pain management and to reduce inflammation.
- Pros: Improves comfort, speeds recovery, reduces swelling.
- Cons: Potential side effects (GI upset, kidney issues), requires careful dosing and monitoring.
- Cost Range (US): $15-$70 for a typical course.
E. Treatment for Systemic Diseases
If bad breath is due to non-dental causes, the treatment focuses on managing the primary condition:
- Kidney Disease: Dietary changes (prescription kidney diets), fluid therapy (subcutaneous fluids), medications to manage blood pressure and phosphorus levels.
- Diabetes Mellitus: Insulin therapy, dietary changes, regular monitoring of blood glucose levels.
- Liver Disease: Dietary modifications, liver support supplements, medications to manage symptoms (e.g., anti-nausea).
- Gastrointestinal Issues: Dietary changes, specific medications to treat inflammation, motility issues, or infections.
- Respiratory Infections: Antibiotics, antivirals, or antifungals depending on the cause, supportive care.
- Oral Tumors: Surgical removal, radiation therapy, or chemotherapy, depending on the type and stage of cancer.
- Pros: Addresses the life-threatening underlying condition, improves overall health.
- Cons: Often requires lifelong management, can be very costly and time-consuming, potential for side effects from medications.
- Cost Range (US): Highly variable, from $100s to $1,000s monthly for ongoing management of chronic diseases.
F. Home Dental Care (Adjunctive to Professional Treatment)
- Description: Essential for maintaining oral health after professional cleaning and preventing recurrence. Includes daily tooth brushing, dental diets, dental treats, and water additives. (Detailed under "Prevention")
- Pros: Reduces plaque/tartar, maintains fresh breath, cost-effective in the long run.
- Cons: Requires commitment, some cats resist.
- Cost Range (US): $10-$50 monthly for products.

Pro Tip: Never attempt to clean your cat's teeth with human toothpaste, as it contains fluoride and detergents that are toxic if swallowed by cats. Always use veterinary-approved feline toothpaste.
Step-by-Step Process: What to Expect During a Dental Procedure
When your veterinarian recommends a professional dental cleaning or other oral surgery for your cat, it’s natural to feel anxious. Understanding the step-by-step process can help alleviate concerns and prepare you for what to expect.
Step 1: Pre-Anesthetic Consultation and Diagnostics (Days to Weeks Before)
- Initial Exam: Your veterinarian will perform a thorough physical examination to assess your cat's overall health and discuss their dental history.
- Blood Work: Before any anesthesia, blood tests are crucial to evaluate organ function (kidneys, liver) and ensure your cat can safely metabolize anesthetic drugs. Urine analysis and sometimes an ECG may also be recommended, especially for older cats or those with suspected underlying conditions.
- Discussion: The vet will explain the procedure, potential risks, costs, and answer any questions you have. This is when the likely extent of dental work, including potential extractions, might be estimated.
Step 2: Admission and Pre-Sedation (Morning of Procedure)
- Fasting: You'll typically be instructed to withhold food for 8-12 hours before the procedure (water can usually be given until a few hours prior). This reduces the risk of vomiting and aspiration during anesthesia.
- Admission: You'll drop your cat off at the veterinary clinic.
- Pre-Medication: Your cat will receive pre-anesthetic medications (e.g., sedatives, pain relievers, anti-anxiety drugs) to help them relax, reduce stress, and minimize the amount of anesthetic gas needed. An intravenous (IV) catheter will be placed for fluid administration and emergency access.
Step 3: Anesthesia and Monitoring (During Procedure)
- Induction: Your cat will be given an injectable anesthetic to allow for intubation (placement of a breathing tube into the trachea).
- Maintenance: Anesthesia is maintained using inhalant gas (isoflurane or sevoflurane) delivered through the breathing tube.
- Comprehensive Monitoring: Throughout the procedure, a dedicated veterinary technician will continuously monitor your cat's vital signs:
- Heart rate and rhythm (ECG)
- Blood pressure
- Oxygen saturation (pulse oximetry)
- Carbon dioxide levels (capnography)
- Body temperature
- Respiration rate
- IV Fluids: Administered intravenously to maintain hydration, support blood pressure, and help with drug elimination.
- Pain Management: Local anesthetic blocks (e.g., bupivacaine) are often given to numb the mouth and provide effective, localized pain relief for hours post-procedure, reducing the overall need for systemic pain medication.
Step 4: Oral Examination and Dental Radiography (X-rays)
- Visual Exam: Once under anesthesia, the veterinarian performs a much more thorough visual examination of the entire oral cavity, including the back of the throat, which is impossible in an awake cat.
- Dental X-rays: Full-mouth dental X-rays are taken. This is critical because up to 60% of dental disease lies below the gumline and is invisible to the naked eye. X-rays reveal bone loss, root damage, unerupted teeth, and tooth resorption.
Step 5: Scaling, Polishing, and Extractions
- Ultrasonic Scaling: An ultrasonic scaler is used to remove large deposits of plaque and tartar from the tooth surfaces, both above and below the gumline.
- Hand Scaling: Fine hand instruments are used to meticulously clean periodontal pockets and root surfaces.
- Polishing: After scaling, a special paste is used to polish the tooth surfaces, smoothing out microscopic scratches created during scaling. This makes the teeth less receptive to new plaque accumulation.
- Extractions (if necessary): If X-rays or examination reveal severely diseased or damaged teeth that cannot be saved, they will be extracted. This is a surgical procedure involving careful elevation of the tooth, often sectioning multi-rooted teeth, cleaning the socket, and suturing the gum tissue.
Step 6: Recovery (Post-Procedure)
- Anesthesia Recovery: Your cat will be moved to a warm, quiet recovery area and continuously monitored as they wake up from anesthesia.
- Pain Management: Post-operative pain medication will be administered as needed, based on the extent of the procedure.
- Discharge: Once fully awake and stable, your cat will be discharged, typically later the same day. You'll receive detailed discharge instructions, including medication schedules, feeding guidelines, and signs to watch for.
The entire process, from admission to discharge, usually takes a full day. While the thought of anesthesia can be daunting, the benefits of addressing painful and infected dental disease far outweigh the minimal risks involved with modern veterinary protocols.
Cost and Insurance
The cost of treating cat bad breath can vary significantly depending on the underlying cause, the severity of the condition, your geographic location, and the specific veterinary clinic. Understanding these costs and insurance options is crucial for financial planning.
Average US Cost Ranges for Dental Procedures:
| Procedure / Service | Low Range (US$) | Mid Range (US$) | High Range (US$) | Notes |
|---|---|---|---|---|
| Initial Exam & Consult | $50 | $80 | $150 | For assessment of bad breath, general health check. |
| Pre-Anesthetic Blood Work | $100 | $180 | $300 | Essential for safety; includes CBC, chemistry profile, sometimes urinalysis. |
| Routine Dental Cleaning | $500 | $850 | $1,200 | Includes anesthesia, monitoring, scaling, polishing, fluoride, IV fluids. No extractions. |
| Dental X-rays (Full Mouth) | $150 | $250 | $400 | Often included in dental cleaning price, but sometimes separate. Crucial for subgingival disease. |
| Simple Tooth Extraction | $50 | $150 | $250 | Per tooth. For single-rooted teeth, no complications. |
| Complex Tooth Extraction | $200 | $350 | $500+ | Per tooth. For multi-rooted teeth, severe root damage, surgical extractions. |
| Stomatitis Treatment | $1,000 | $2,500 | $4,000+ | Often requires full-mouth extractions. Very costly. |
| Medications (Antibiotics/Pain) | $15 | $50 | $100 | Post-procedure. |
| Total for Moderate Dental Disease (Cleaning + 1-2 Extractions) | $800 | $1,500 | $2,500+ | A common scenario. |
- Regional Variations: Costs in major metropolitan areas (e.g., New York, Los Angeles) tend to be at the higher end, while rural areas may offer slightly lower prices.
- Clinic Type: Specialty veterinary dental practices will often have higher fees due to advanced equipment and expertise.
Costs for Systemic Disease Management:
These are highly variable and often ongoing.
- Kidney Disease: Monthly costs can range from $100-$500+ for prescription diets, fluid therapy, and medications.
- Diabetes: Initial diagnosis and stabilization can be $300-$800, with ongoing monthly costs of $100-$300 for insulin, syringes, and special food.
- Liver Disease: Similar to kidney disease, ongoing management can be $100-$500+ per month for medications and specific diets.
Pet Insurance Coverage:
- Dental Coverage: Many pet insurance plans offer coverage for dental illnesses (e.g., periodontal disease, extractions, root canals) if the condition is not pre-existing. Routine dental cleanings (preventative) are often not covered by standard accident/illness plans but can be added via a "wellness package" or "preventative care rider" for an additional monthly fee (typically $15-$40).
- Systemic Disease Coverage: Most comprehensive pet insurance plans will cover the diagnosis and treatment of systemic diseases like kidney disease, diabetes, or liver disease, provided they are not pre-existing conditions.
- Deductibles and Reimbursement: You will typically pay a deductible (e.g., $250-$1,000) and then be reimbursed for a percentage of the remaining costs (e.g., 70-90%) after your claim is processed.
- Waiting Periods: Be aware of waiting periods (e.g., 14 days for illness, 6 months for orthopedic conditions) before coverage kicks in. This means if you sign up for insurance after your cat develops bad breath, it might be considered pre-existing.
Payment Plans and Financing Options:
- Veterinary Payment Plans: Some clinics offer in-house payment plans, though these are less common for large expenses.
- CareCredit / Scratchpay: These are third-party financing options specifically designed for veterinary and medical expenses. They offer various payment plans, including interest-free options for a certain period, for qualifying applicants.
- Pet Savings Accounts: Many owners establish dedicated savings accounts for pet emergencies and routine care.
- Veterinary Charities: In cases of financial hardship, local animal shelters or national organizations may offer grants or assistance.
Pro Tip: Enroll in pet insurance when your cat is young and healthy to ensure potential future conditions, including dental and systemic diseases, are covered. Preventative care riders are a wise investment to help offset the cost of routine dental cleanings.
Recovery and Aftercare
Recovery from a professional dental procedure, especially if extractions were involved, is crucial for your cat's comfort and long-term oral health. Aftercare also extends to managing bad breath caused by systemic diseases.
A. Post-Dental Procedure Recovery (for Oral Causes):
- Immediate Post-Anesthesia:
- Grogginess: Your cat will likely be groggy, wobbly, and may seem disoriented for 12-24 hours. Keep them in a quiet, warm, and safe space away from stairs or other pets.
- Feeding: Offer small amounts of soft, moist food once they are fully awake and can swallow normally (usually a few hours after arriving home). Avoid hard kibble for at least 7-14 days, or longer if extensive extractions were performed.
- Water: Ensure fresh water is readily available.
- Pain Management:
- Medication: Administer prescribed pain medications (NSAIDs, opioids) exactly as directed by your veterinarian. Do not skip doses, even if your cat seems fine, as pain can be internal.
- Local Blocks: The local anesthetic blocks given during the procedure will provide pain relief for several hours post-op, but systemic pain medication is still vital.
- Antibiotics:
- Medication: If prescribed, complete the full course of antibiotics, even if your cat seems better, to prevent recurrence of infection.
- Surgical Sites (if extractions):
- Check Daily: Briefly and gently check your cat's mouth daily for any signs of excessive swelling, redness, bleeding, or discharge.
- Sutures: Most oral sutures are dissolvable and will disappear on their own within 2-4 weeks. Do not attempt to remove them.
- Avoid Irritation: Prevent your cat from chewing on hard toys or objects during the healing period.
- Follow-up:
- Scheduled Recheck: A follow-up appointment is often scheduled 7-14 days post-procedure to ensure healing is progressing well.
B. Long-Term Oral Aftercare (Prevention of Recurrence):
This is perhaps the most critical component for preventing future cat bad breath.
- Daily Tooth Brushing:
- Method: This is the most effective way to remove plaque. Use a feline-specific toothbrush (finger brush or small soft-bristled brush) and enzymatic cat toothpaste.
- Frequency: Aim for daily brushing. Even a few times a week is better than none. Start slowly, making it a positive experience with treats and praise.
- Technique: Gently lift the lip and brush the outer surfaces of the teeth, especially where the tooth meets the gumline, at a 45-degree angle. Focus on the canine teeth and the large molars in the back.
- Dental Diets:
- Description: Prescription dental diets (e.g., Hill's T/D, Royal Canin Dental) are formulated with larger kibble that mechanically scrubs the teeth as the cat chews. They also contain ingredients that inhibit plaque mineralization.
- Benefit: Can significantly reduce plaque and tartar buildup.
- Dental Treats:
- Description: Look for treats approved by the Veterinary Oral Health Council (VOHC). These products have been scientifically proven to reduce plaque and/or tartar.
- Benefit: Can supplement brushing, but are not a substitute.
- Water Additives:
- Description: Products added to your cat's drinking water that contain antiseptics or anti-plaque ingredients. Also VOHC-approved options available.
- Benefit: Easy to administer, helps reduce bacteria throughout the mouth.
- Regular Veterinary Check-ups:
- Frequency: Annual or bi-annual wellness exams include an oral check. Your vet can spot early signs of dental disease.
- Professional Cleaning Schedule: Your vet will advise on the frequency of professional cleanings, which might be annually or every 2-3 years depending on individual needs and home care effectiveness.
C. Aftercare for Systemic Diseases:
- Medication Adherence: Administer all prescribed medications for conditions like kidney disease, diabetes, or liver disease exactly as directed, often for life.
- Dietary Management: Strict adherence to prescription diets is paramount for conditions like kidney disease or diabetes.
- Regular Monitoring: Frequent veterinary visits and diagnostic tests (blood work, urine tests) will be necessary to monitor the progression of the disease and adjust treatment as needed.
- Supportive Care: Provide a comfortable, low-stress environment. Ensure adequate hydration.
- Home Dental Care: Even with systemic disease, maintaining good oral hygiene is important to prevent secondary dental issues.
Effective aftercare and long-term preventative measures are crucial investments in your cat's health, comfort, and fresh breath.
Prevention
Preventing cat bad breath is primarily about preventing the underlying causes, especially dental disease. A proactive approach combining home dental care with regular veterinary check-ups is your best strategy.
1. Daily Home Dental Care:
This is the cornerstone of prevention and can dramatically reduce plaque and tartar buildup.
- Tooth Brushing (Daily):
- Why: Mechanically removes plaque before it hardens into tartar.
- How: Use a feline-specific toothbrush (small, soft bristles or a finger brush) and enzymatic cat toothpaste (never human toothpaste).
- Technique: Gently lift the cat's lip and brush the outside surfaces of the teeth, focusing on the gumline. Even a few seconds of brushing on a few teeth is beneficial.
- Training: Start early with kittens, making it a positive experience with rewards. If your adult cat resists, introduce it gradually.
- Veterinary Oral Health Council (VOHC) Approved Products:
- Dental Diets: Specific kibble designs and ingredients help scrub teeth and reduce plaque. Examples include Hill's Prescription Diet t/d, Royal Canin Dental, Purina Pro Plan Veterinary Diets DH.
- Dental Treats: Designed to have a specific texture or active ingredients that reduce plaque and/or tartar. Look for the VOHC seal.
- Water Additives: Contain antimicrobials or anti-plaque agents that help reduce bacteria in the mouth.
- Why VOHC: These products have undergone rigorous scientific testing to prove their efficacy in reducing plaque and/or tartar. They are not a substitute for brushing but are excellent adjuncts.
2. Regular Veterinary Check-ups:
- Annual Oral Examinations: Your veterinarian will conduct a visual inspection of your cat's mouth during their annual wellness exam. They can spot early signs of gingivitis, tartar, or other oral problems.
- Professional Dental Cleanings: Even with excellent home care, most cats will require professional dental cleanings under anesthesia every 1-3 years. This removes hardened tartar and addresses disease below the gumline that can't be reached at home. Your vet will advise on the appropriate frequency based on your cat's individual needs.
3. Balanced Diet:
- High-Quality Cat Food: Feeding a nutritionally complete and balanced diet is essential for overall health, which indirectly supports oral health.
- Avoid Table Scraps: Human food can contribute to dental problems, upset digestion, and is often not nutritionally appropriate for cats.
- Dental-Specific Diets: As mentioned, these can be a crucial part of prevention, especially for cats prone to dental issues.
4. Provide Safe Chew Toys:
- Caution: Cats are not natural chewers like dogs, and many chew toys can be too hard, leading to fractured teeth.
- Recommendation: If offering chew toys, choose those specifically designed for feline dental health, made from softer, pliable materials, and always supervise your cat. Avoid anything that won't bend, such as bones, hard plastic toys, or antlers.
5. Monitor for Other Health Issues:
- Watch for Systemic Signs: Be vigilant for signs of systemic diseases (increased thirst, urination, lethargy, changes in appetite) that can cause bad breath. Early detection and treatment of these conditions are vital.
- Regular Blood Work: For older cats, annual or bi-annual blood work can help detect kidney disease, diabetes, or liver disease in their early stages, before severe bad breath develops.
By integrating these preventive measures into your cat's routine, you can significantly reduce the risk of cat bad breath and, more importantly, protect them from the pain and serious health consequences of untreated oral and systemic diseases.
| Prevention Method | Effectiveness (Dental Disease) | Ease of Implementation | Cost (Monthly) | Notes |
|---|---|---|---|---|
| Daily Tooth Brushing | High (Gold Standard) | Difficult initially | ~$10-$20 (toothpaste/brush) | Requires training and consistency. Most effective plaque removal. |
| VOHC Dental Diet | Moderate to High | Easy | ~$30-$60 (food cost) | Replaces regular kibble. Some cats may not like texture/flavor. |
| VOHC Dental Treats | Low to Moderate | Easy | ~$10-$20 | Supplement only, not a substitute. Can add calories. |
| VOHC Water Additives | Low to Moderate | Very Easy | ~$10-$20 | Least invasive, but also least effective as a standalone. |
| Regular Vet Check-ups | High (Early Detection) | Easy | ~$0 (included in annual exam) | Crucial for identifying issues and scheduling professional cleanings. |
Risks and Complications
Ignoring cat bad breath or delaying treatment carries significant risks and can lead to severe complications, impacting not only your cat's oral health but their overall systemic well-being.

A. Risks Associated with Untreated Oral Disease:
- Chronic Pain: Dental disease is inherently painful. Cats often hide pain, but chronic oral pain severely diminishes their quality of life, leading to changes in eating, grooming, and behavior.
- Tooth Loss: Advanced periodontal disease destroys the bone and ligaments supporting teeth, leading to loose, painful teeth that eventually fall out or require extraction.
- Jaw Fractures: Severe bone loss in the jaw due to periodontal disease, especially in the thin lower jaw, can weaken the bone to the point where even minor trauma (or chewing) can cause a pathological jaw fracture.
- Oral-Nasal Fistulas: Infections from upper canine teeth can erode through the bone into the nasal cavity, creating a permanent opening (fistula) between the mouth and nose. This leads to chronic nasal discharge and potential respiratory infections.
- Ocular Issues: In some cases, a severe tooth root abscess, particularly of an upper molar, can extend into the eye socket, causing pain, swelling, and potential vision impairment or loss.
- Systemic Infection (Bacteremia): Bacteria from infected teeth and gums can enter the bloodstream (bacteremia) and travel to distant organs.
- Heart Disease: Can lead to bacterial endocarditis, an infection of the heart valves.
- Kidney Disease: Chronic bacterial inflammation can strain and damage the kidneys.
- Liver Disease: The liver can be affected by chronic infection and inflammation.
- Reduced Quality of Life: Persistent pain, difficulty eating, and general malaise significantly impact a cat's happiness and interaction with their owners.
- Anorexia and Malnutrition: Painful mouths can lead to reduced food intake, resulting in weight loss, muscle wasting, and nutritional deficiencies.
B. Risks Associated with Anesthesia (for Dental Procedures):
While modern veterinary anesthesia is very safe, there are always inherent risks, though serious complications are rare.
- Adverse Drug Reactions: Allergic reactions or unexpected responses to anesthetic agents.
- Cardiovascular Complications: Arrhythmias, hypotension (low blood pressure), or, in rare severe cases, cardiac arrest. Pre-anesthetic blood work and careful monitoring minimize these risks.
- Respiratory Complications: Aspiration pneumonia (inhaling stomach contents), hypoventilation (decreased breathing). Intubation helps prevent aspiration.
- Hypothermia: Cats can lose body heat during anesthesia. Warming measures are always used to prevent this.
- Prolonged Recovery: Some cats may take longer to wake up, especially if they are very old or have underlying health conditions.
- Undiagnosed Conditions: While pre-anesthetic testing reduces the risk, sometimes an underlying, undiagnosed condition can complicate anesthesia.
C. Risks of Untreated Systemic Diseases:
If bad breath is a symptom of a systemic disease, neglecting it can have far more serious, life-threatening consequences.
- Kidney Failure: Untreated kidney disease will progress, leading to end-stage renal failure, uremic poisoning, and death.
- Diabetic Ketoacidosis (DKA): Untreated diabetes or unmanaged DKA is a metabolic emergency that can be fatal if not rapidly addressed.
- Liver Failure: Progressive liver disease can lead to severe organ dysfunction, jaundice, neurological signs, and ultimately death.
- Cancer Metastasis: Untreated oral or systemic cancer can spread rapidly throughout the body, making prognosis poor.
Pro Tip: Discuss all potential risks with your veterinarian before any procedure or treatment plan. The benefits of treating dental disease and addressing systemic illnesses almost always outweigh the risks, especially when performed with comprehensive safety protocols. The American Dental Association (ADA) emphasizes the importance of professional dental care for overall health, and this principle extends to our feline patients as well, underscoring that veterinary dental care follows similar best practices to human dentistry.
Cost Breakdown (Summary)
To consolidate and provide clarity on the financial aspects of addressing cat bad breath, here’s a summary of the typical costs you might encounter in the US. These are average ranges and can fluctuate based on location, clinic, and your cat's specific needs.
Average US Costs – Low to High Range:
- Initial Veterinary Examination for Bad Breath: $50 - $150
- What it includes: Physical exam, oral check, discussion of symptoms.
- Pre-Anesthetic Blood Work (for dental procedures): $100 - $300
- What it includes: CBC, Chemistry Panel, sometimes Urinalysis or Thyroid testing (for older cats). Essential safety measure.
- Routine Professional Dental Cleaning (without extractions): $500 - $1,200
- What it includes: Anesthesia, comprehensive monitoring, IV fluids, full-mouth dental X-rays, ultrasonic scaling above and below the gumline, polishing, fluoride treatment.
- Tooth Extractions:
- Simple Extraction (per tooth): $50 - $250
- Complex/Surgical Extraction (per tooth): $200 - $500+
- What it includes: Surgical removal, local anesthetic blocks, suturing, pain management.
- Post-Procedure Medications (Antibiotics, Pain Relievers): $15 - $100
- What it includes: Typical course for 7-14 days.
- Total for Moderate Dental Disease (Cleaning + a few extractions): $800 - $2,500+
- This is a common scenario for many cats over 3-5 years old.
Costs for Treating Systemic Diseases (beyond dental care):
- Kidney Disease Management (monthly): $100 - $500+
- Includes: Prescription diet, subcutaneous fluids, medications, monitoring blood work.
- Diabetes Management (monthly): $100 - $300
- Includes: Insulin, syringes, special diet, glucose monitoring supplies. Initial diagnostic work-up and stabilization can be $300-$800.
- Liver Disease Management (monthly): $100 - $500+
- Includes: Prescription diet, supplements, medications, monitoring.
With vs. Without Pet Insurance:
- Without Insurance: You are responsible for 100% of the costs at the time of service. This can lead to significant out-of-pocket expenses.
- With Insurance:
- Wellness/Preventative Riders: If you have a wellness plan, routine dental cleanings (and sometimes exams/blood work) may be partially or fully covered, often after a co-pay. Expect to pay $15-$40 extra per month for this rider.
- Accident & Illness Plans: These typically cover unexpected illnesses, including advanced dental disease (e.g., extractions due to periodontal disease, stomatitis), and systemic diseases (kidney, liver, diabetes). You pay a deductible ($250-$1,000) and then are reimbursed for a percentage (70%-90%) of the vet bill.
- Crucial Note: Most insurance plans consider dental disease or systemic illnesses "pre-existing" if symptoms were present before enrollment or the waiting period ended. This means they won't cover treatment for a condition that already exists.
Payment Plans and Financing Options:
- CareCredit / Scratchpay: These are popular medical credit cards designed for veterinary expenses. They often offer short-term (6-24 months) interest-free financing if paid in full within that period, or longer-term options with interest. Approval depends on your credit history.
- Veterinary Clinic Payment Plans: Some individual clinics may offer internal payment arrangements, though this is less common for large amounts. It's always worth asking.
- Emergency Funds / Pet Savings Accounts: Proactive saving for your pet's healthcare is an excellent way to prepare for unexpected costs.
- Veterinary Assistance Programs: Non-profits like The Pet Fund, RedRover, or specific breed rescues may offer financial aid for owners in need, particularly for emergency or life-saving treatments.
Cost-Saving Tips:
- Preventative Care: Consistent home dental care (brushing, VOHC products) and regular vet check-ups can prevent minor issues from becoming costly major problems.
- Early Intervention: Addressing bad breath as soon as you notice it can prevent the progression of disease, saving money on more extensive treatments later.
- Comparison Shopping (for non-emergencies): For routine procedures like dental cleanings, it's acceptable to get quotes from a few different reputable veterinary clinics, provided they use similar quality anesthesia, monitoring, and dental radiography standards.
- Pet Insurance: Enroll when your cat is young and healthy to maximize coverage for future conditions.
Investing in your cat's dental and overall health early can save significant emotional and financial stress in the long run.
Frequently Asked Questions
What does "cat bad breath" smell like?
Cat bad breath, or halitosis, can have several distinct odors. Most commonly, it smells putrid, like decaying meat or rotten fish, due to bacterial buildup and infection in the mouth. However, it can also smell like ammonia or urine (indicating kidney disease), sweet or fruity (suggesting diabetes), or very musty and "death-like" (pointing to liver disease). The specific smell can offer clues about the underlying health problem.
Is bad breath in cats always a sign of serious illness?
While often indicating dental disease, which can be severe and painful, bad breath can also be a symptom of more serious, life-threatening systemic illnesses such as kidney disease, diabetes, or liver failure. Therefore, any persistent or unusually strong bad breath in your cat warrants an immediate veterinary examination to determine the cause.
How much does it cost to fix cat bad breath?
The cost varies widely depending on the cause. A routine professional dental cleaning under anesthesia typically ranges from $500 to $1,200. If extractions are needed, add $50-$500+ per tooth. If the bad breath is due to systemic disease, ongoing monthly management can range from $100 to $500+ for medications, special diets, and monitoring.
Is professional dental cleaning painful for cats?
Professional dental cleanings are performed under general anesthesia, so your cat feels no pain during the procedure. Post-procedure, pain medication (NSAIDs, local anesthetic blocks) is administered to ensure comfort during recovery. While some discomfort is expected after extensive extractions, proper pain management keeps it controlled.
Can I brush my cat's teeth to get rid of bad breath?
Yes, daily tooth brushing with a feline-specific toothbrush and enzymatic toothpaste is the most effective way to prevent plaque buildup and reduce bad breath. However, if tartar has already formed, or if there's significant dental disease, brushing alone won't suffice, and a professional cleaning will be necessary first.
What if my cat won't let me brush their teeth?
If your cat resists brushing, don't force it. Try introducing it very gradually, rewarding them heavily. Alternatively, use VOHC-approved dental diets, dental treats, or water additives, which can help reduce plaque and tartar, though they are not as effective as brushing. Regular veterinary check-ups remain crucial regardless of your home care routine.
How long does it take for bad breath to go away after treatment?
If the bad breath is due to dental disease, it typically improves almost immediately after a professional dental cleaning and extractions. For systemic diseases, breath odor will improve as the underlying condition is brought under control through ongoing medical management, which can take days to weeks.
Are there alternatives to anesthesia for cat dental cleaning?
No, anesthesia-free dental cleanings are not recommended by the American Veterinary Dental College (AVDC) or the American Dental Association (ADA) for pets. They only address the visible tooth surface, leaving painful and dangerous disease below the gumline untouched. A thorough dental cleaning and examination require a cat to be safely anesthetized.
Does diet play a role in cat bad breath?
Yes, diet can play a role. A poor diet might contribute to plaque buildup, and certain prescription dental diets can actively help reduce plaque and tartar. More significantly, prescription diets are crucial for managing systemic diseases like kidney disease, diabetes, or liver disease, which can be the root cause of bad breath.
When should I consider pet insurance for dental care?
Consider pet insurance early in your cat's life, ideally before any dental issues arise. Most insurance plans have waiting periods and won't cover pre-existing conditions. Look for plans with a "wellness rider" or "preventative care add-on" if you want coverage for routine dental cleanings. Standard accident/illness plans typically cover dental issues only if they result from an illness or injury and are not pre-existing.
When to See a Veterinarian
It's critical to know when your cat's bad breath warrants a veterinary visit. While occasional mild bad breath might be benign, persistent or significantly foul odors are red flags that require professional attention.
Immediate Attention (Emergency/Urgent):
- Sudden Onset of Severely Foul Breath: Especially if accompanied by other acute symptoms.
- Ammonia, Sweet/Fruity, or Musty Odor: These are strong indicators of potentially life-threatening systemic diseases (kidney, diabetes, liver) and require immediate veterinary evaluation.
- Severe Pain or Discomfort: If your cat suddenly stops eating, drools excessively, paws at their mouth, or cries out when eating.
- Visible Oral Injury or Swelling: Such as a broken tooth, severe gum bleeding, or a noticeable mass in the mouth.
- Concurrent Systemic Signs: Vomiting, diarrhea, increased thirst/urination, lethargy, sudden weight loss, or yellowing of gums/eyes alongside bad breath. These could indicate a severe systemic crisis.
Scheduled Appointment (Routine Care/Non-Emergency):
- Persistent Mild to Moderate Bad Breath: If the breath has a consistently unpleasant smell that isn't indicative of a systemic issue, but isn't acute pain.
- Visible Tartar Buildup: Yellowish-brown crusts on the teeth, even if your cat isn't showing obvious signs of pain. This indicates developing dental disease.
- Red or Swollen Gums (Gingivitis): Early signs of gum inflammation.
- Changes in Eating Habits (Gradual): Such as preferring softer foods, chewing slowly, or dropping food.
- Overdue for Annual Dental Check-up: Even without overt symptoms, regular check-ups are essential for preventative care.
The Bottom Line: Never dismiss bad breath in your cat as merely "normal cat breath." A significantly offensive or changing odor is your cat's way of telling you something is wrong. Early intervention can prevent minor issues from escalating into major health crises, saving your cat from pain and potentially saving their life. When in doubt, always err on the side of caution and consult your veterinarian.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
What Cause Bad Breath
For many, a quick mint or a swig of mouthwash is the go-to solution for an unpleasant taste or odor in the mouth. But what if that bad breath, medically known as halitosis, is a persistent problem that no amount of peppermint can conquer? It’s a far more common issue than you might think, affecting
February 23, 2026

Dogs Bad Breath: Complete Guide
One whiff is all it takes: that distinctly unpleasant odor emanating from your beloved canine companion. If you've ever wondered, "Why does my dog's breath smell so bad?" you're not alone. It's a common concern among pet owners, with over 80% of dogs showing signs of oral disease by age three. W
February 23, 2026

Sudden Bad Breath in Toddlers: Complete Guide
When your toddler, who usually smells sweet and innocent, suddenly develops an unpleasant odor in their breath, it can be an alarming experience for any parent. Sudden bad breath in toddlers, also known as halitosis, is more common than you might think, affecting a significant number of young ch
February 23, 2026

Mouth Wash for Bad Breath: Complete Guide
Bad breath, medically known as halitosis, is an incredibly common and often embarrassing condition that affects a significant portion of the global population. In the United States alone, more than 80 million people suffer from chronic bad breath, impacting social interactions, professional conf
February 23, 2026