Cat Has Bad Breath: Complete Guide

Key Takeaways
- A purrfect companion with a less-than-purrfect breath? If your cat has bad breath, you're not alone. Up to 80% of cats over the age of three suffer from some form of dental disease, a primary culprit behind foul feline odor. While occasional bad breath might seem minor, chronic halitosis in
A purrfect companion with a less-than-purrfect breath? If your cat has bad breath, you're not alone. Up to 80% of cats over the age of three suffer from some form of dental disease, a primary culprit behind foul feline odor. While occasional bad breath might seem minor, chronic halitosis in cats is often a significant warning sign that something deeper is amiss with their health, demanding your attention. Ignoring it can lead to severe pain, discomfort, and even systemic health issues for your beloved pet.
This comprehensive guide from SmilePedia.net will delve into every aspect of feline halitosis, from understanding its root causes—including why cat bad breath can smell like poop—to exploring various treatment options, prevention strategies, and what to expect during veterinary care. By understanding the nuances of your cat's oral health, you can ensure they live a happier, healthier life, free from the silent pain and systemic complications that often accompany neglected dental issues. We'll cover everything from diagnosis and cost implications to long-term care, empowering you to make informed decisions for your furry friend.
Key Takeaways:
- Halitosis in cats is more than just an unpleasant smell; it's often a symptom of underlying dental disease or systemic illness.
- Dental disease (plaque, tartar, gingivitis, periodontitis) is the most common cause, affecting up to 80% of cats over three.
- A "poop-like" odor can signal severe periodontal disease, foreign objects, or serious systemic issues like kidney or liver failure.
- Professional veterinary dental cleaning typically costs between $400 and $1,200 in the US, but can exceed $3,000-$5,000 for complex procedures like multiple extractions.
- Prevention is key, involving daily brushing, dental diets, water additives, and regular veterinary check-ups (annual to bi-annual).
- Early intervention can prevent pain, tooth loss, and the spread of infection to vital organs.
- Prompt veterinary consultation is crucial for diagnosis and effective treatment, as home remedies alone are often insufficient.
What It Is / Overview
Halitosis, commonly known as bad breath, is an unpleasant odor emanating from the mouth. In cats, this condition is far more than a mere nuisance; it is a critical indicator of underlying health issues. While sometimes a cat's breath can simply be a reflection of their last meal, persistent or worsening bad breath is almost always a red flag that warrants investigation by a veterinarian.

The odor itself is typically caused by the accumulation of bacteria in the mouth. These bacteria produce volatile sulfur compounds (VSCs) as they break down food particles and tissue, leading to the characteristic foul smell. In cats, the intensity and specific type of odor can provide clues about the underlying cause. For instance, a sweet, fruity smell might indicate diabetes, while an ammonia-like odor can point to kidney disease. However, the most common scent associated with feline halitosis is a generally foul, decaying smell, often linked directly to dental disease.
Understanding that halitosis is a symptom, not a disease itself, is crucial. It signals that your cat's body is struggling with an infection, inflammation, or metabolic imbalance that requires attention. Ignoring persistent bad breath not only leads to discomfort for your cat but can allow underlying conditions to progress, potentially causing severe pain, organ damage, and a reduced quality of life.
Types / Variations
Feline halitosis isn't a monolithic condition; its manifestation can vary based on the underlying cause. Understanding these variations can help you communicate more effectively with your veterinarian.
Transient vs. Chronic Halitosis
- Transient Halitosis: This is temporary bad breath, often related to a recent meal or something the cat has just eaten (e.g., strong-smelling wet food, something they scavenged). It typically resolves on its own within a few hours. This type is generally not a cause for concern unless it becomes a regular occurrence.
- Chronic Halitosis: This is persistent bad breath that does not go away. It is almost always indicative of an underlying health problem and requires veterinary attention. This is the focus of our discussion.
Odor Characteristics and Potential Meanings
The specific smell of your cat's bad breath can sometimes offer a preliminary clue to its origin:
- Foul, Decaying, or "Poop-Like" Odor: This is the most common type and is overwhelmingly associated with severe dental disease. This includes advanced periodontal disease, where bacterial plaque and tartar buildup lead to gum inflammation (gingivitis), bone loss, and tooth decay. The "poop-like" smell arises from the anaerobic bacteria thriving in decaying oral tissue, necrotic (dead) tissue, pus, and trapped food particles, creating extremely potent VSCs. In some cases, it can also indicate a foreign body lodged in the mouth or throat, or even a severe oral tumor that is necrotizing. Less commonly, it might point to gastrointestinal issues or, in very severe cases, kidney or liver disease where toxins build up and are excreted through the breath.
- Sweet or Fruity Odor: This specific scent is highly suggestive of diabetic ketoacidosis (DKA), a life-threatening complication of uncontrolled diabetes. If your cat's breath smells sweet, seek immediate veterinary care.
- Ammonia-like or Urine-like Odor: This is a hallmark sign of kidney disease. As kidneys fail to filter toxins from the blood, these waste products, including urea, accumulate and are released through the breath.
- Extremely Putrid or Liver-like Odor: A very strong, sickly sweet, or "mousy" odor can sometimes be associated with severe liver disease.
- Sour or Vomitus Odor: Can indicate gastrointestinal issues, reflux, or recent vomiting.
It's important to remember that these are general indicators. A definitive diagnosis always requires a professional veterinary examination and diagnostic tests.
Causes / Why It Happens
The causes of a cat's bad breath are numerous and can range from benign to life-threatening. Identifying the root cause is paramount for effective treatment.
1. Dental and Oral Diseases (Most Common Cause)
Periodontal Disease: This is by far the most prevalent cause of chronic halitosis in cats, affecting the majority of adult felines. It begins with: * Plaque Formation: A sticky film of bacteria, saliva, and food particles constantly forms on teeth. * Tartar (Calculus) Buildup: If plaque isn't removed, it hardens into tartar, which adheres firmly to the tooth surface. Tartar creates a rough surface that allows even more bacteria and plaque to accumulate. * Gingivitis: The bacteria in plaque and tartar irritate the gums, leading to inflammation, redness, swelling, and bleeding. This is the earliest stage of periodontal disease and is reversible. * Periodontitis: If gingivitis progresses, the inflammation spreads below the gumline, destroying the supporting structures of the teeth (ligaments, bone). Pockets form around the teeth, filling with bacteria, pus, and decaying tissue. This stage is irreversible and leads to tooth mobility, pain, and eventually tooth loss. The anaerobic bacteria thriving in these deep pockets produce highly foul-smelling volatile sulfur compounds, resulting in that distinct "poop-like" or decaying odor. * Resorptive Lesions: Also known as Feline Odontoclastic Resorptive Lesions (FORLs), these are extremely painful conditions where the dentin (the tissue beneath the enamel) of a tooth is eroded, often starting at the gumline. While not directly a cause of halitosis, the exposed pulp and subsequent infection can contribute significantly to bad breath. Up to 70% of cats may be affected by these lesions.
Other Oral Issues:
- Stomatitis: A severe, painful inflammation of the entire oral cavity, including gums, tongue, and inner cheeks. This condition is often immune-mediated and can lead to severe ulcerations, making eating extremely painful and producing a very foul odor.
- Oral Tumors/Cancers: Growths in the mouth, especially malignant ones, can become infected and necrotic (tissue death), causing a very strong, putrid smell. These can be difficult to spot without a thorough veterinary examination.
- Oral Injuries: Cuts, punctures, or fractured teeth can harbor bacteria and lead to localized infections and bad breath.
- Foreign Objects: Small bones, splinters, threads, or even grass awns can become lodged between teeth or in the gums, leading to inflammation, infection, and a very strong localized odor. This is a common cause for a sudden onset of extremely foul breath.
2. Systemic Diseases
Beyond the mouth, several non-oral health conditions can manifest as bad breath, some of which are very serious.
- Kidney Disease: As mentioned, failing kidneys cannot effectively filter waste products from the blood. Toxins like urea accumulate, leading to an ammonia-like or urine-like odor on the breath (uremic breath). This often accompanies other signs like increased thirst and urination, lethargy, and weight loss.
- Liver Disease: A severely compromised liver, unable to process toxins and metabolize nutrients properly, can lead to a very distinctive, often sickly sweet or musty odor on the breath. Symptoms can include jaundice (yellowing of skin/eyes), lethargy, vomiting, and loss of appetite.
- Diabetes Mellitus: Uncontrolled diabetes can lead to diabetic ketoacidosis (DKA), a metabolic emergency characterized by a distinctive sweet or fruity smell on the breath, along with symptoms like increased thirst, urination, and weight loss despite a good appetite.
- Gastrointestinal Disorders: Chronic vomiting, acid reflux (GERD), or certain malabsorption issues can sometimes contribute to bad breath.
- Respiratory Tract Infections: Infections in the nasal passages, sinuses, or lungs (e.g., bacterial pneumonia, rhinitis) can cause a foul smell to emanate from the respiratory system, which can be perceived as bad breath.
3. Dietary and Environmental Factors
- Diet: While generally less common as a sole cause of chronic halitosis, certain diets can contribute. Wet foods, particularly those with strong odors, can temporarily linger. Diets rich in soft, sticky carbohydrates can contribute to plaque formation. Some cats are allergic to certain food components, leading to oral inflammation.
- Coprophagia (Eating Feces): If your cat has access to and eats feces (either their own, other cats', or other animals'), their breath will temporarily smell like poop. While not a disease, it's a behavioral issue that can be a nuisance and potentially expose them to parasites.
- Grooming Habits: Cats are meticulous groomers. However, if they have an oral lesion or pain, they might groom less, allowing food debris and bacteria to accumulate. Conversely, if they groom excessively around an infected area, they might spread bacteria.
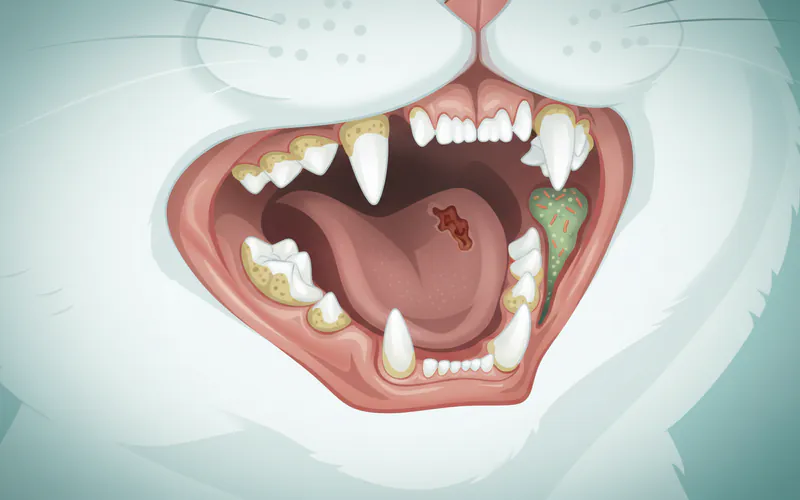
Signs and Symptoms
Beyond the obvious foul odor, your cat may exhibit other signs that indicate an underlying oral or systemic issue. Recognizing these can prompt earlier veterinary intervention.
- Visible Plaque and Tartar: Yellowish-brown buildup on the surface of the teeth, especially near the gumline.
- Red, Swollen, or Bleeding Gums (Gingivitis): Gums that look inflamed or bleed easily, especially during eating or touching.
- Drooling (Ptyalism): Excessive drooling, sometimes mixed with blood or pus, indicates oral pain or discomfort.
- Difficulty Eating (Dysphagia) or Changes in Eating Habits:
- Reluctance to eat hard food.
- Chewing on one side of the mouth.
- Dropping food from the mouth.
- Paw at the mouth while eating.
- Hissing or crying when attempting to eat.
- Loss of appetite altogether (anorexia) if pain is severe.
- Weight Loss: Due to difficulty eating or chronic illness.
- Pawing at the Face or Mouth: An attempt to relieve discomfort.
- Facial Swelling: May indicate a dental abscess (infection around the tooth root) or tumor.
- Lethargy or Behavioral Changes: Withdrawal, decreased playfulness, irritability due to chronic pain or illness.
- Loose or Missing Teeth: A sign of advanced periodontal disease.
- Oral Masses or Growths: Visible lumps or bumps in the mouth or on the gums.
- Changes in Water Consumption or Urination: Increased thirst and urination can point to kidney disease or diabetes.
Pro Tip: Regularly lift your cat's lips to inspect their teeth and gums. Doing this gently from a young age can help them tolerate it better. Look for any changes in color, swelling, or visible buildup.
Treatment Options
Treating your cat's bad breath effectively always begins with diagnosing the underlying cause. Once the cause is identified, a tailored treatment plan can be implemented.
1. Professional Veterinary Dental Cleaning (COHAT)
For most cases of dental-related halitosis, a Comprehensive Oral Health Assessment and Treatment (COHAT) under anesthesia is the gold standard.
Process:
- Pre-Anesthetic Blood Work: To assess organ function and ensure the cat is a safe candidate for anesthesia.
- Physical Examination: A thorough check of overall health.
- Anesthesia: General anesthesia is essential for a complete and safe dental procedure. This allows for thorough examination, scaling, and polishing without causing stress or pain to the cat.
- Oral Examination and Charting: Each tooth is carefully examined, and any abnormalities (e.g., plaque, tartar, gum recession, periodontal pockets, resorptive lesions) are recorded.
- Dental Radiographs (X-rays): Crucial for evaluating the health of the tooth roots and surrounding bone, which are hidden beneath the gumline. Up to 60% of dental disease in cats is found below the gumline.
- Scaling: Using ultrasonic and hand scalers, plaque and tartar are meticulously removed from both above and below the gumline.
- Polishing: The tooth surfaces are polished to smooth out microscopic scratches, making it harder for plaque to adhere.
- Subgingival Lavage: Flushing the gum pockets to remove debris and bacteria.
- Extractions: If severe periodontal disease, resorptive lesions, or fractured teeth are present, extraction may be necessary. This is performed carefully, often requiring dental surgical techniques.
- Pain Management: Anesthetic protocols include pain medications, and often local nerve blocks are administered before extractions to ensure the cat wakes up comfortably. Oral pain medication is prescribed for post-procedure recovery.
Pros:
- Most effective treatment for dental disease.
- Removes source of infection and pain.
- Prevents progression of periodontal disease.
- Improves overall health and quality of life.
Cons:
- Requires general anesthesia (though modern anesthetic protocols are very safe).
- Can be costly.
- Potential for tooth loss (extractions).
2. Medications
- Antibiotics: Prescribed for active infections, especially before or after dental procedures involving extractions or deep pocket cleaning. Also used for systemic infections contributing to halitosis (e.g., respiratory infections).
- Anti-inflammatories/Pain Relievers: Crucial for managing pain associated with dental disease, stomatitis, or recovery from extractions. Non-steroidal anti-inflammatory drugs (NSAIDs) or corticosteroids may be used, depending on the condition.
- Medications for Systemic Diseases:
- Diabetes: Insulin therapy, dietary management.
- Kidney Disease: Special renal diets, fluid therapy, phosphate binders, blood pressure medication.
- Liver Disease: Specific diets, liver protectants, antibiotics, anti-inflammatories.
- Stomatitis: Can be very challenging, often requiring multiple tooth extractions (full-mouth extraction is common and surprisingly effective), corticosteroids, immunosuppressants, or even novel therapies like laser treatment or stem cell therapy.
3. Dietary Changes
- Prescription Dental Diets: Specially formulated kibble that helps mechanically scrub teeth as the cat chews, reducing plaque and tartar buildup. Some diets also contain ingredients that chemically bind calcium in saliva, preventing tartar formation. Look for diets with the VOHC (Veterinary Oral Health Council) seal of acceptance.
- Wet Food vs. Dry Food: While wet food doesn't offer the same mechanical abrasion as kibble, it can be essential for cats with painful dental disease who struggle to eat dry food. In such cases, the primary focus is on professional dental care.
- Specific Diets for Systemic Diseases: As mentioned, prescription renal diets, diabetic diets, or liver support diets are vital for managing systemic causes of bad breath.
4. Home Oral Care
While home care cannot cure existing dental disease, it is crucial for prevention and maintaining oral health after a professional cleaning.
- Brushing: Daily tooth brushing with a vet-approved feline toothpaste (never human toothpaste!) is the single most effective home care method. Start slowly and positively.
- Dental Chews/Treats: Look for VOHC-accepted dental treats or chews that are designed to reduce plaque and tartar. Ensure they are appropriate for your cat's size and chewing style.
- Oral Rinses/Water Additives: Antiseptic rinses or water additives (containing zinc, chlorhexidine, or xylitol alternatives safe for cats) can help reduce bacteria in the mouth. Always use products specifically formulated and approved for cats.
- Dental Wipes: For cats who resist brushing, dental wipes can offer a small degree of plaque removal.
Pro Tip: Introduce brushing gradually. Start by letting your cat lick the pet toothpaste (it's often flavored like chicken or tuna). Then, introduce a finger brush, slowly working up to a small pet toothbrush. Consistency is more important than perfection. Aim for 30-60 seconds per side, focusing on the outside surfaces of the teeth near the gumline.
Comparison of Dental Treatment Options
| Treatment Option | Primary Use | Pros | Cons | Average US Cost Range (Typical) |
|---|---|---|---|---|
| Professional Dental Cleaning (COHAT) | Gold standard for dental disease, plaque, tartar, gingivitis | Thorough cleaning, addresses subgingival issues, pain relief, prevents progression | Requires general anesthesia, often needs bloodwork, cost | $400 - $1,200 (routine); $1,500 - $5,000+ (extractions) |
| Tooth Extractions | Severe periodontal disease, resorptive lesions, fractured teeth | Eliminates source of chronic pain and infection | Permanent tooth loss, higher cost, longer recovery | Included in COHAT cost, but significantly increases total |
| Antibiotics | Active oral infections, pre/post-op | Resolves bacterial infections | Potential side effects (GI upset), antibiotic resistance | $20 - $100 (course) |
| Anti-inflammatories/Pain meds | Pain relief, inflammation management | Improves comfort, encourages eating | Potential side effects (GI upset, kidney issues), careful dosing | $15 - $75 (course) |
| Dental Diets (VOHC-accepted) | Prevention of plaque/tartar after cleaning, maintenance | Easy to implement, palatable, convenient | Not a cure for existing disease, may not be suitable for all cats | $30 - $80 (per bag, depending on brand/size) |
| Tooth Brushing | Daily prevention, plaque control | Most effective home care, cost-effective | Requires cat cooperation, consistency needed | $10 - $30 (toothpaste/brush starter kit) |
| Water Additives/Rinses | Reduce bacteria, freshen breath | Easy to use, good for cats that resist brushing | Less effective than brushing, some cats dislike taste | $15 - $40 (per bottle) |
Step-by-Step Process: What to Expect During Treatment
Addressing your cat's bad breath typically follows a structured veterinary approach.
1. Initial Veterinary Consultation and Examination
- History Taking: Your vet will ask about your cat's symptoms, eating habits, general health, and any changes you've noticed. This includes specific questions about the odor's characteristics ("cat has bad breath that smells like poop").
- Physical Examination: A thorough head-to-tail exam, including a preliminary oral examination (as much as your cat tolerates). The vet will check for visible plaque, tartar, gum inflammation, and any obvious masses or pain.
- Discussion of Potential Causes: Based on the exam and history, the vet will discuss the most likely causes (dental, systemic) and recommend next steps.
- Diagnostic Recommendations: This may include blood tests (to evaluate kidney, liver, and blood sugar levels), urine tests, and potentially a recommendation for a professional dental cleaning under anesthesia for definitive oral diagnosis.
2. Pre-Anesthetic Work-up (If Dental Cleaning is Recommended)
- Blood Tests: Standard pre-anesthetic screening to ensure your cat's organs (kidneys, liver) are functioning properly and that they can safely metabolize anesthetic drugs. This is crucial, especially for older cats or those with suspected systemic issues.
- Urine Analysis: To further assess kidney function and rule out urinary tract infections.
- Other Diagnostics: In some cases, chest X-rays or an electrocardiogram (ECG) might be recommended, especially for older cats or those with known heart conditions.

3. The Professional Dental Procedure (COHAT)
- Anesthetic Induction and Monitoring: Your cat will be given pre-medications to relax them, followed by an intravenous anesthetic. Throughout the procedure, a trained veterinary technician will continuously monitor vital signs (heart rate, respiration, blood pressure, oxygen saturation, temperature).
- Dental Radiographs (X-rays): Full mouth X-rays are taken to assess the health of the teeth below the gumline. This step is non-negotiable for a thorough dental assessment.
- Oral Examination and Charting: Each tooth is carefully probed and examined, with findings meticulously recorded on a dental chart.
- Scaling and Polishing: Ultrasonic scalers remove tartar, followed by hand scaling to ensure all surfaces (especially below the gumline) are clean. Polishing creates smooth surfaces that resist new plaque formation.
- Extractions (If Necessary): If X-rays reveal severe disease, fractured roots, or painful resorptive lesions, tooth extractions are performed. This is done surgically, often with sutures to close the gum.
- Pain Management: Local nerve blocks are administered before extractions, and systemic pain medication is given during and after the procedure.
- Recovery: Your cat will be monitored closely as they recover from anesthesia.
4. Post-Procedure and Follow-up Care
- Discharge Instructions: You'll receive detailed instructions on medication administration (antibiotics, pain relievers), feeding (soft food for a period, especially after extractions), and activity restrictions.
- Monitoring at Home: Observe your cat for any signs of pain, lethargy, or refusal to eat.
- Follow-up Appointment: A follow-up visit, typically 1-2 weeks after the procedure, to check healing, suture removal (if applicable), and discuss long-term home care strategies.
- Implementation of Home Care: This is the critical next step to prevent recurrence. Daily brushing, dental diets, and other veterinarian-recommended products should be initiated.
Cost and Insurance
The cost of treating your cat's bad breath can vary significantly depending on the underlying cause, the severity of the condition, and your geographical location in the US.
Average US Price Ranges
- Initial Veterinary Consultation: $60 - $150
- Blood Work (Pre-Anesthetic): $100 - $300
- Routine Professional Dental Cleaning (COHAT - without extractions): $400 - $1,200
- This usually includes anesthesia, monitoring, scaling, polishing, and full-mouth dental X-rays.
- Dental Cleaning with Extractions: $1,500 - $5,000+
- Each extraction can add $50 - $200+ per tooth, depending on complexity. Surgical extractions (e.g., fractured teeth, deeply rooted canines) will be at the higher end.
- Additional costs for pain medication, antibiotics, and specialized surgical supplies.
- Treatment for Systemic Diseases: Highly variable.
- Diabetes management: Initial diagnosis can be $200 - $500, then ongoing costs for insulin (monthly $40 - $150), needles, and monitoring supplies.
- Kidney or Liver Disease management: Initial diagnosis $300 - $800+ (blood tests, urinalysis, imaging), then ongoing medication and prescription diets can range from $50 - $300+ monthly.
- Oral Tumors: Biopsy $200 - $600, surgery $1,000 - $4,000+, potentially chemotherapy/radiation $2,000 - $8,000+.
- Home Care Products:
- Feline Toothbrush & Toothpaste: $10 - $30 (starter kit)
- VOHC-accepted Dental Diets: $30 - $80 (per bag)
- Dental Chews/Treats: $10 - $30 (per bag/box)
- Water Additives/Oral Rinses: $15 - $40 (per bottle)
Regional Cost Variations (Estimates)
| Region (USA) | Routine COHAT (No Extractions) | COHAT with Complex Extractions |
|---|---|---|
| Northeast (e.g., NYC, Boston) | $700 - $1,500 | $2,000 - $6,000+ |
| West Coast (e.g., LA, SF) | $650 - $1,400 | $1,800 - $5,500+ |
| Midwest (e.g., Chicago, Dallas) | $500 - $1,100 | $1,500 - $4,500+ |
| Southeast (e.g., Miami, Atlanta) | $400 - $1,000 | $1,200 - $4,000+ |
These are general estimates and can vary based on the specific veterinary clinic, specialist involvement, and the cat's individual needs.
Pet Insurance Coverage
Many pet insurance plans cover unexpected illnesses and accidents, which often includes dental disease treatment if it's not pre-existing.
- What's usually covered:
- Professional dental cleanings (especially if medically necessary due to active disease).
- Extractions, root canals, and other advanced dental procedures.
- Medications for dental infections or pain.
- Diagnostics for systemic diseases causing halitosis.
- What's usually NOT covered:
- Routine preventive cleanings (unless you have a specific "wellness" rider, which adds to the premium).
- Pre-existing conditions: If your cat already has a diagnosed dental disease before you enroll in insurance, it likely won't be covered. This highlights the importance of getting insurance before problems arise.
- Cosmetic procedures.
It's crucial to thoroughly review different pet insurance policies and understand their coverage limits, deductibles, reimbursement percentages (e.g., 70-90% of eligible costs), and waiting periods.
Recovery and Aftercare
Post-treatment care is vital for a smooth recovery and to maintain your cat's improved oral health.
Immediate Post-Procedure Care (1-2 Weeks)
- Medication Administration: Follow your vet's instructions precisely for antibiotics and pain relievers. These are crucial for preventing infection and managing discomfort.
- Dietary Adjustments: If extractions were performed, your cat will likely need to eat soft food (canned food, moistened kibble) for 7-14 days to allow gum tissues to heal. Avoid hard kibble, crunchy treats, or chew toys during this period.
- Activity Restrictions: Limit strenuous play or activities that could cause injury to the healing mouth.
- Monitor for Complications: Watch for excessive drooling, refusal to eat, lethargy, swelling, or bleeding. Contact your vet immediately if you notice any concerning signs.
- Suture Care: If sutures were placed (common after extractions), your vet will advise on their removal, typically at a follow-up appointment. Most oral sutures are absorbable.
Long-Term Aftercare and Prevention
Once your cat has recovered, the focus shifts to preventing recurrence of bad breath and dental disease.
- Daily Home Oral Care: This is the cornerstone of prevention.
- Tooth Brushing: Aim for daily brushing using a feline-specific toothbrush and toothpaste. Even a few times a week is better than nothing.
- Dental Diets: Incorporate VOHC-accepted dental kibble as a primary food or as treats.
- Water Additives/Oral Rinses: Use as recommended by your vet.
- Regular Veterinary Check-ups: Annual or bi-annual wellness exams are essential. Your vet will assess your cat's overall health and perform an oral exam, catching early signs of dental issues before they become severe.
- Monitor for Re-emergence: Continue to be vigilant for any returning signs of bad breath, changes in eating habits, or visible oral issues. Early detection means less invasive and less costly treatment.
Pro Tip: Create a positive association with home dental care. Use treats, praise, and gentle handling. Short, consistent sessions are more effective than infrequent, long, stressful ones.
Prevention
Preventing bad breath and dental disease in cats is a lifelong commitment that can save your pet from pain and you from significant veterinary bills.
1. Daily Oral Hygiene
- Tooth Brushing: This is the most effective preventive measure. Aim for daily brushing with a vet-approved feline toothpaste and toothbrush. The mechanical action of the bristles physically removes plaque before it hardens into tartar.
- VOHC-Accepted Dental Products: Incorporate dental diets, chews, or water additives that have earned the Veterinary Oral Health Council (VOHC) seal of acceptance. This seal indicates that the product has been proven to reduce plaque and/or tartar.
- Dental Diets: Specially formulated kibble that helps clean teeth.
- Dental Chews: Designed to scrape plaque off teeth as the cat chews.
- Water Additives/Oral Rinses: Help reduce bacteria in the mouth.
2. Regular Veterinary Check-ups and Professional Cleanings
- Annual Wellness Exams: Your veterinarian will perform an oral examination during these visits to assess your cat's dental health and identify any early signs of disease.
- Proactive Professional Dental Cleanings: Don't wait until severe disease develops. Many vets recommend professional cleanings every 1-3 years, depending on your cat's individual predisposition to dental disease. Early intervention means less invasive procedures and better long-term oral health.
3. Balanced Diet
- While dry food doesn't replace brushing, a good quality, balanced diet is essential for overall health, which in turn supports oral health. Discuss dietary options with your veterinarian.
4. Address Underlying Systemic Issues
- If your cat has a systemic disease (diabetes, kidney disease, etc.), diligent management of that condition is crucial for preventing related bad breath and maintaining overall well-being. Regular vet visits and adherence to prescribed treatments are key.
Risks and Complications
Ignoring your cat's bad breath or delaying treatment carries significant risks and can lead to severe complications.
1. Worsening Dental Disease
- Increased Pain: Untreated periodontal disease is incredibly painful. Cats are masters at hiding pain, so you might not see obvious signs until the disease is advanced.
- Tooth Loss: As periodontal disease progresses, the supporting bone and ligaments are destroyed, leading to loose teeth that eventually fall out or require extraction.
- Oral Abscesses: Infections can track into the bone, forming painful abscesses around tooth roots, which can sometimes lead to facial swelling or drainage.
- Jaw Fractures: In severe cases of bone loss due to periodontal disease, the jaw bone can become so thin and fragile that even a minor trauma (like a fall or rough play) can cause a fracture.
2. Systemic Health Problems
The bacteria from infected gums don't stay in the mouth. They can enter the bloodstream (bacteremia) and travel to other organs, causing serious health issues:

- Heart Disease: Bacteria can attach to heart valves, leading to inflammation and damage, known as endocarditis.
- Kidney Disease: Chronic bacterial exposure can contribute to inflammation and damage in the kidneys.
- Liver Disease: Similar to kidneys, the liver can also be affected by systemic inflammation and infection originating from the mouth.
- Diabetes Management: Chronic inflammation from dental disease can make it harder to regulate blood sugar levels in diabetic cats.
3. Nutritional Deficiencies and Weight Loss
- Painful oral conditions make eating difficult. Cats may refuse to eat, leading to weight loss, malnutrition, and a weakened immune system.
4. Poor Quality of Life
- Chronic pain, difficulty eating, and general malaise due to untreated dental or systemic disease severely diminish a cat's quality of life. They may become withdrawn, irritable, or lethargic.
Frequently Asked Questions
What does it mean if my cat has bad breath that smells like poop?
A cat's breath smelling like poop is a strong indicator of severe dental disease, such as advanced periodontitis with significant bacterial overgrowth, pus, and necrotic tissue. Less commonly, it could be due to a foreign object lodged in the mouth, an oral tumor, or indicate gastrointestinal issues. In some very severe cases, it might be associated with kidney or liver disease, where toxins build up and are excreted through breath, though these often have distinct, more ammonia-like or sickly sweet odors. A veterinary visit is crucial for diagnosis.
How do you treat bad breath in cats?
Treatment depends entirely on the cause. For dental disease, a professional veterinary dental cleaning under anesthesia (COHAT) is necessary to remove plaque and tartar and address any infections or damaged teeth. If a systemic disease (like kidney disease or diabetes) is the cause, treating the underlying condition with appropriate medications, diet, and management is paramount. Home care, such as daily brushing, dental diets, and water additives, helps prevent recurrence after professional treatment.
Is my cat's bad breath an emergency?
While most cases of bad breath are not immediate emergencies, they should never be ignored. However, certain types of bad breath warrant immediate veterinary attention: a sudden onset of extremely foul odor, a sweet or fruity smell (suggesting diabetic ketoacidosis), an ammonia-like smell (suggesting kidney failure), or if bad breath is accompanied by severe lethargy, refusal to eat, excessive drooling, or facial swelling. These signs can indicate life-threatening conditions.
How much does it cost to treat cat bad breath?
The cost varies widely based on the cause. A routine professional dental cleaning (COHAT) for dental disease can range from $400 to $1,200. If extractions are needed, the cost can easily climb to $1,500 - $5,000+. Treatment for systemic diseases (e.g., diabetes, kidney failure) can involve hundreds to thousands of dollars for initial diagnosis and ongoing management. Home care products typically cost $10-$80 per item.
Can I give my cat human dental products for bad breath?
No, absolutely not. Human toothpastes often contain fluoride and xylitol, which are toxic to cats. Human mouthwashes can also be toxic. Always use veterinary-approved products specifically formulated for cats. These are safe if swallowed and are often flavored to be palatable for felines.
How often should my cat get their teeth cleaned professionally?
The frequency depends on your cat's age, breed, diet, and individual predisposition to dental disease. For many cats, an annual professional cleaning is recommended, while others might only need one every 2-3 years, and some more frequently. Your veterinarian will assess your cat's oral health during wellness exams and recommend an appropriate schedule.
Does diet affect my cat's breath?
Yes, diet can influence your cat's breath. Soft, sticky diets can contribute to plaque buildup. Conversely, certain veterinary dental diets are formulated to help reduce plaque and tartar. Strong-smelling wet foods can temporarily linger on the breath. If a cat is eating feces (coprophagia), their breath will temporarily smell like poop. For systemic diseases, prescription diets are crucial for management and can indirectly affect breath.
Is it painful for a cat to have bad breath caused by dental disease?
Yes, absolutely. Dental disease, especially periodontitis and resorptive lesions, is incredibly painful. Cats are stoic animals and often hide their pain, but the underlying inflammation, infection, and potential tooth root exposure or decay cause significant discomfort. This pain can affect their ability to eat, groom, and enjoy life.
What are the alternatives to professional dental cleaning for cats?
There are no true alternatives that can effectively remove existing plaque and tartar below the gumline or treat advanced dental disease. Home care (brushing, dental diets, water additives) is excellent for prevention and maintenance after a professional cleaning, but it cannot reverse established disease. Over-the-counter products without the VOHC seal often lack proven efficacy.
When to See a Dentist
Given the potential severity of underlying causes, it's always best to consult your veterinarian if you notice your cat has persistent bad breath. Do not attempt to diagnose or treat the issue at home without professional guidance.
Routine Care Guidance:
- Annual Wellness Exams: Even if your cat's breath seems fine, an annual veterinary check-up includes an oral examination to catch early signs of dental disease.
- Mild or Occasional Bad Breath: If the bad breath is very mild, inconsistent, and not accompanied by other symptoms, you can mention it during your next routine vet visit. In the meantime, try to implement home care.
When to See Your Vet Promptly (Scheduled Appointment):
- Persistent Bad Breath: If your cat's bad breath lasts for more than a few days, even if there are no other obvious symptoms.
- Visible Plaque/Tartar: If you can see significant yellowish or brownish buildup on the teeth.
- Red or Swollen Gums: Any signs of gingivitis.
- Changes in Eating Habits: Difficulty chewing, dropping food, favoring one side of the mouth, or reluctance to eat.
Red Flags Requiring Immediate Veterinary Attention (Emergency):
- Sudden Onset of Extremely Foul Breath: Especially if it smells like feces, pus, or decay. This could indicate a severe infection, foreign object, or tumor.
- Sweet or Fruity Breath: This is a strong indicator of diabetic ketoacidosis, a life-threatening emergency.
- Ammonia-like or Urine-like Breath: Suggests severe kidney disease.
- Facial Swelling: Could be a dental abscess.
- Excessive Drooling (especially with blood or pus): Indicates severe oral pain or infection.
- Lethargy, Weakness, or Collapse: Any severe systemic signs accompanying bad breath.
- Refusal to Eat or Drink: Indicates severe pain or illness.
Remember, your cat's bad breath is a window into their overall health. Timely veterinary intervention can prevent pain, save teeth, and even save lives.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
What Cause Bad Breath
For many, a quick mint or a swig of mouthwash is the go-to solution for an unpleasant taste or odor in the mouth. But what if that bad breath, medically known as halitosis, is a persistent problem that no amount of peppermint can conquer? It’s a far more common issue than you might think, affecting
February 23, 2026

Dogs Bad Breath: Complete Guide
One whiff is all it takes: that distinctly unpleasant odor emanating from your beloved canine companion. If you've ever wondered, "Why does my dog's breath smell so bad?" you're not alone. It's a common concern among pet owners, with over 80% of dogs showing signs of oral disease by age three. W
February 23, 2026

Sudden Bad Breath in Toddlers: Complete Guide
When your toddler, who usually smells sweet and innocent, suddenly develops an unpleasant odor in their breath, it can be an alarming experience for any parent. Sudden bad breath in toddlers, also known as halitosis, is more common than you might think, affecting a significant number of young ch
February 23, 2026

Mouth Wash for Bad Breath: Complete Guide
Bad breath, medically known as halitosis, is an incredibly common and often embarrassing condition that affects a significant portion of the global population. In the United States alone, more than 80 million people suffer from chronic bad breath, impacting social interactions, professional conf
February 23, 2026