How to Stop Gum Swelling
Key Takeaways
- When your gums are swollen, it can be more than just an uncomfortable sensation; it's often a clear signal that something is amiss with your oral health. Imagine waking up with tender, puffy gums that bleed easily, or experiencing sudden localized swelling after an injury or meal. This isn't just an
When your gums are swollen, it can be more than just an uncomfortable sensation; it's often a clear signal that something is amiss with your oral health. Imagine waking up with tender, puffy gums that bleed easily, or experiencing sudden localized swelling after an injury or meal. This isn't just an annoyance; it's a condition that demands attention, as ignoring it can lead to more serious complications affecting your overall well-being. Knowing how to stop gum swelling effectively and understanding its underlying causes is crucial for maintaining a healthy smile and preventing progression to severe dental issues.
Gum swelling, medically known as gingival swelling, is a common complaint that can range from a mild irritation around a single tooth to widespread inflammation across your entire gum line. While sometimes a minor issue, it can also be a symptom of conditions like advanced gum disease, a developing infection, or even indicate a problem with an adjacent tooth (like a tooth swelling due to an abscess). For instance, did you know that an estimated 47.2% of adults aged 30 years and older have some form of periodontal disease, the leading cause of gum inflammation and swelling? This article from SmilePedia.net will be your comprehensive guide to understanding, treating, and preventing gum swelling. We'll delve into its various causes, explore effective home remedies and professional treatments, discuss associated costs and recovery, and equip you with the knowledge to maintain optimal gum health.
Key Takeaways:
- Identify the Cause: Gum swelling often indicates underlying issues like gingivitis, periodontitis, or infection. Accurate diagnosis by a dentist is paramount for effective treatment.
- Immediate Relief: Rinsing with warm salt water (1/2 teaspoon salt in 8 ounces of water) can provide temporary relief from pain and reduce inflammation. Over-the-counter pain relievers like ibuprofen can also help.
- Professional Treatment is Key: While home remedies offer temporary comfort, professional dental care (e.g., deep cleaning, antibiotics, root canal, or extraction) is usually required to address the root cause and prevent recurrence.
- Cost Varies Widely: Treatment costs can range from $75 - $200 for an emergency exam and X-ray, to $200 - $600 per quadrant for deep cleaning (scaling and root planing), or $800 - $2,000+ for complex procedures like root canals or gum surgery.
- Prevention is Best: Consistent oral hygiene (brushing twice daily, flossing once daily), regular dental check-ups (every 6 months), and a healthy diet are crucial for preventing gum swelling.
- Don't Delay Care: Persistent or severe gum swelling, especially with pain, pus, or fever, can signal a dental emergency. Seek professional help immediately to prevent serious complications like tooth loss or systemic infections.
- Recovery Timeline: Minor swelling from gingivitis may resolve within days to weeks with improved hygiene. More complex cases, like post-surgery or deep infection, can require weeks to months for full recovery.
What It Is / Overview
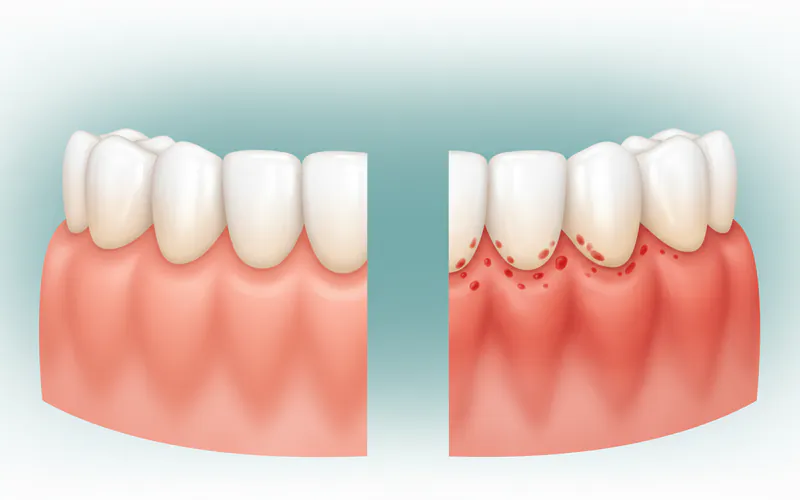
Gum swelling, or gingival edema, is a condition characterized by the enlargement, inflammation, or protrusion of the gum tissue. Healthy gums are typically firm, pink, and tightly hug the teeth. When they swell, they can appear red, puffy, glossy, and may bleed easily, especially during brushing or flossing. This swelling is a protective response by the body's immune system to irritation or infection. It signifies an increase in fluid accumulation in the gum tissues and an influx of immune cells fighting a perceived threat.

The presence of gum swelling can be localized, affecting only a small area around one tooth, or generalized, impacting the entire gum line. Understanding the difference is important as it can offer clues to the underlying cause. Localized swelling often points to specific issues like a dental abscess, an impacted tooth (such as wisdom teeth), a food particle lodged under the gum, or trauma. Generalized swelling, on the other hand, is more commonly associated with widespread conditions like gingivitis or periodontitis, nutritional deficiencies, or hormonal changes. Regardless of its extent, gum swelling should never be ignored, as it often heralds the need for dental intervention.
Types / Variations of Gum Swelling
Gum swelling can manifest in several ways, each potentially pointing to a different underlying cause:
Generalized Gum Swelling (Gingivitis or Periodontitis)
This is the most common form, affecting the gum tissue around multiple teeth or the entire mouth.
- Gingivitis: This is the earliest and most common form of gum disease, characterized by inflammation of the gums due to plaque buildup. The gums appear red, swollen, and bleed easily. It's reversible with good oral hygiene and professional cleaning.
- Periodontitis: If gingivitis is left untreated, it can advance to periodontitis, where inflammation spreads to the bone and ligaments supporting the teeth. This can lead to gum recession, the formation of pockets between teeth and gums, and eventually tooth loss. Swelling is often accompanied by deep pockets, pus, and loose teeth.
Localized Gum Swelling (Around a Single Tooth or Area)
This type of swelling is confined to a specific spot.
- Dental Abscess: A localized collection of pus, usually caused by a bacterial infection. It can form at the tip of the tooth root (periapical abscess) or in the gum tissue itself (periodontal abscess). The swelling is often very painful, tender to touch, and may form a "pimple-like" bump (fistula) that drains pus.
- Impacted Tooth: When a tooth, typically a wisdom tooth, doesn't fully erupt and remains partially or completely embedded in the jawbone or gum tissue, it can cause localized inflammation and swelling (pericoronitis). Food and bacteria can get trapped under the gum flap covering the impacted tooth, leading to infection.
- Food Impaction: A piece of food, like a popcorn kernel or a meat fiber, can get forcefully lodged under the gum line, causing irritation and localized swelling.
- Trauma: Physical injury to the gums, such as from aggressive brushing, a sharp food item, or a sports injury, can lead to localized swelling. This might also be seen when a tooth is avulsed (knocked out) and the surrounding tissues are damaged.
- Cyst or Tumor: Although less common, a cyst or benign/malignant tumor can develop in the jaw or gum tissue, presenting as localized swelling.
Swelling Associated with Tooth Issues (Tooth Swelling)
Sometimes, the gum swelling is a secondary symptom of a problem originating from the tooth itself.
- Infected Tooth: An infection deep within a tooth's pulp (root canal infection) can spread to the surrounding bone and gum tissue, causing the gum area near the infected tooth to swell. This is often accompanied by significant tooth pain.
- Eruption Cysts/Hematomas: In children, when a new tooth is about to erupt, a small, fluid-filled sac (eruption cyst) or blood-filled sac (eruption hematoma) can form over the gum, causing localized swelling.
- Root Fracture: A cracked or fractured tooth root can lead to infection and subsequent gum swelling around the affected tooth.
Recognizing the pattern and location of the swelling is the first step toward effective diagnosis and treatment.
Causes / Why It Happens
Understanding the root causes of gum swelling is essential for effective treatment and prevention. The reasons can range from simple hygiene issues to more complex medical conditions.
1. Poor Oral Hygiene
This is by far the most common cause.
- Plaque Buildup: When you don't brush and floss regularly, a sticky film of bacteria called plaque accumulates on your teeth and along the gum line.
- Tartar (Calculus): If plaque isn't removed, it hardens into tartar, which is impossible to remove with regular brushing. Both plaque and tartar irritate the gums, leading to inflammation and swelling. This irritation is the primary driver of gingivitis.
2. Gum Disease (Gingivitis and Periodontitis)
As mentioned, these are direct consequences of poor oral hygiene.
- Gingivitis: The initial stage, where gums become red, swollen, and bleed easily.
- Periodontitis: The advanced stage, where the infection spreads below the gum line, destroying the bone and supporting structures of the teeth. Gum pockets form, collecting more bacteria and leading to persistent swelling, pain, and eventually tooth loss.
3. Dental Abscess or Infection
Infections can cause localized and often severe swelling.
- Tooth Abscess (Periapical): A bacterial infection originating from the pulp of a tooth (often due to deep decay or trauma) can spread to the bone at the tip of the root, forming a pus-filled pocket. This causes significant tooth swelling and pain, often radiating to the gum tissue above or below the affected tooth.
- Periodontal Abscess: An infection that forms within the gum tissue itself, usually in a periodontal pocket, due to trapped bacteria. This results in a painful, localized swelling on the gum.
- Pericoronitis: Inflammation and infection of the gum tissue surrounding an impacted or partially erupted tooth, most commonly a wisdom tooth. Food and bacteria get trapped under the gum flap, leading to intense localized swelling, pain, and difficulty opening the mouth.
4. Nutritional Deficiencies
Certain vitamins are crucial for gum health.
- Vitamin C Deficiency (Scurvy): While rare in developed countries, severe lack of Vitamin C can lead to weakened connective tissues, causing gums to become swollen, spongy, bleed easily, and even develop ulcers.
- Vitamin K Deficiency: Important for blood clotting, a deficiency can contribute to bleeding gums.
5. Hormonal Changes
Fluctuations in hormone levels can increase gum sensitivity and inflammation.
- Pregnancy: "Pregnancy gingivitis" is common due to increased progesterone levels, which make gums more sensitive to plaque and prone to swelling and bleeding.
- Puberty, Menstruation, Menopause: Similar hormonal shifts can lead to temporary gum inflammation.
6. Medications
Some drugs can cause gum overgrowth, known as gingival hyperplasia or overgrowth.
- Phenytoin (anticonvulsant): Used for epilepsy.
- Cyclosporine (immunosuppressant): Used after organ transplants.
- Nifedipine, Amlodipine (calcium channel blockers): Used for high blood pressure and angina. When gums overgrow, they become harder to clean, increasing the risk of inflammation and swelling.
7. Allergic Reactions
- Dental Products: Sensitivity to ingredients in toothpaste, mouthwash, or even dental materials (e.g., amalgam, composites) can cause localized or generalized gum inflammation.
- Food Allergies: Less common, but certain food allergies can manifest with oral symptoms, including gum swelling.
8. Trauma or Injury
- Forceful Brushing/Flossing: Aggressive oral hygiene can irritate and damage gum tissue.
- Sharp Food: A hard piece of food (e.g., bone shard, popcorn hull) can get lodged under the gum line, causing inflammation.
- Physical Injury: A blow to the mouth, sports injury, or even a poorly fitting dental appliance (dentures, retainers) can cause localized swelling. In cases of an avulsed tooth (a tooth knocked completely out), the surrounding gum tissue will be severely traumatized and swollen.
9. Systemic Diseases
Certain medical conditions can manifest in the gums.
- Diabetes: Poorly controlled diabetes can impair the body's ability to fight infection, making individuals more susceptible to gum disease and increasing the severity of inflammation.
- Leukemia: This cancer of the blood cells can cause gums to swell, bleed, and become purplish due to the abnormal proliferation of white blood cells.
- Crohn's Disease: An inflammatory bowel disease that can sometimes present with oral manifestations, including gum swelling.
- Herpetic Gingivostomatitis: A viral infection (HSV-1) that causes widespread gum inflammation, blistering, and swelling, particularly common in children.
10. Ill-fitting Dental Appliances
Crowns, bridges, or dentures that don't fit properly can create areas where food and bacteria accumulate, or they can directly irritate the gum tissue, leading to localized swelling.
Understanding these varied causes is the first step in determining the correct approach to how to stop gum swelling and restore oral health.
Signs and Symptoms
Recognizing the signs and symptoms of gum swelling is key to seeking timely treatment. While the most obvious symptom is the visible enlargement of the gum tissue, other indicators often accompany it:
- Visible Swelling: Gums appear puffy, enlarged, or bulging. They might look like they're "pouching out" or have a "pimple" on them if an abscess is present.
- Redness: Healthy gums are typically a pale pink. Swollen gums often appear bright red, deep red, or purplish.
- Tenderness or Pain: The gums may be sore to the touch, or you might experience a dull ache or sharp pain, especially when chewing or brushing.
- Bleeding Gums: Gums that bleed easily during brushing, flossing, or even spontaneously are a classic sign of inflammation.
- Shiny or Glossy Appearance: Swollen gums can look stretched and shiny due to fluid accumulation.
- Receding Gums: In more advanced gum disease (periodontitis), the gums may pull away from the teeth, making them appear longer.
- Bad Breath (Halitosis): Bacterial buildup in inflamed gum pockets contributes to persistent bad breath.
- Unpleasant Taste in Mouth: This can be due to infection or the presence of pus draining from an abscess.
- Loose Teeth: A severe symptom of advanced periodontitis, where the supporting bone is lost, causing teeth to become mobile.
- Pus: Discharge of pus from the gum line or from a localized swelling indicates an active infection, such as a dental or periodontal abscess.
- Fever and Swollen Lymph Nodes: In cases of severe infection or abscess, you might experience systemic symptoms like fever, fatigue, and swollen, tender lymph nodes in your neck.
- Difficulty Chewing: Pain and swelling can make chewing uncomfortable or even impossible.
If you observe any of these symptoms, especially if they persist for more than a few days, it's crucial to consult a dental professional. Early intervention can prevent minor issues from escalating into serious dental emergencies.
Treatment Options for Stopping Gum Swelling
The approach to how to stop gum swelling depends entirely on its underlying cause. A dentist will first diagnose the issue before recommending the appropriate treatment plan.
1. Improved Oral Hygiene and Professional Cleaning (Scaling and Root Planing)
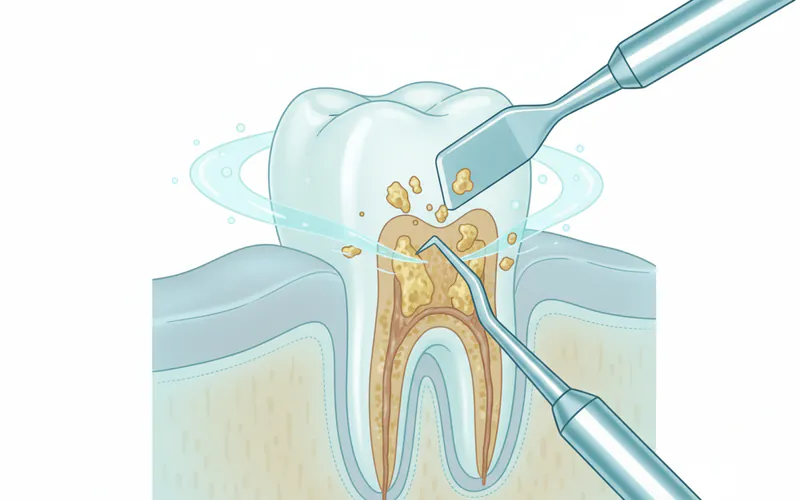
- What it involves: For gingivitis, the primary treatment is professional dental cleaning (prophylaxis) to remove plaque and tartar above and below the gum line, followed by diligent at-home oral care. For more advanced gum disease (periodontitis), a deeper cleaning called scaling and root planing (SRP) is performed. This non-surgical procedure involves scraping away tartar and plaque from both the crown and root surfaces and then smoothing the root surfaces to prevent bacteria from reattaching.
- Pros: Highly effective for early and moderate gum disease, non-invasive (prophylaxis), can reverse gingivitis, prevents progression of periodontitis.
- Cons: SRP may require local anesthesia, can cause temporary sensitivity. It doesn't regenerate lost bone or gum tissue.
- Recovery: Gums may be sensitive for a few days; full recovery within a week or two with diligent home care.
2. Antibiotics
- What it involves: If an infection (abscess, pericoronitis) is present, antibiotics may be prescribed to kill the bacteria causing the infection. This can be in pill form (oral antibiotics) or as a localized gel or chip placed directly into periodontal pockets.
- Pros: Effective at clearing bacterial infections, reduces swelling and pain.
- Cons: Can have side effects (nausea, diarrhea), risk of antibiotic resistance with overuse, doesn't address the underlying physical cause (e.g., trapped food, deep decay).
- Recovery: Symptoms typically improve within a few days of starting antibiotics.
3. Root Canal Therapy
- What it involves: If gum swelling is due to an infection within the tooth's pulp (periapical abscess), a root canal is necessary. The infected pulp is removed, the root canals are cleaned and disinfected, and then filled and sealed. A crown is usually placed over the tooth afterward.
- Pros: Saves the natural tooth, eliminates the source of infection, resolves associated gum swelling.
- Cons: Can be expensive, requires multiple appointments, may cause temporary discomfort.
- Recovery: Initial discomfort subsides within a few days; full recovery of the tooth and surrounding tissues can take weeks.
4. Tooth Extraction
- What it involves: In severe cases where a tooth is beyond repair (e.g., advanced decay, severe fracture, untreatable infection, or a problematic impacted wisdom tooth), extraction may be the only option to remove the source of infection and resolve swelling.
- Pros: Eliminates the problematic tooth and infection, immediate relief from source of pain/swelling.
- Cons: Permanent tooth loss, may require future tooth replacement (implant, bridge), can be uncomfortable during healing.
- Recovery: Socket heals within 1-2 weeks; bone healing takes several months. Swelling typically resolves quickly after extraction.
5. Periodontal Surgery
- What it involves: For advanced periodontitis where non-surgical treatments are insufficient, various surgical procedures may be performed:
- Flap Surgery (Pocket Reduction Surgery): Gums are lifted back to remove tartar and smooth damaged bone, then re-sutured to reduce pocket depth.
- Bone Grafts: To regenerate bone lost to periodontitis.
- Soft Tissue Grafts: To cover exposed roots or enhance gum tissue where recession has occurred.
- Pros: Can halt the progression of severe periodontitis, regenerates lost tissue/bone, preserves teeth.
- Cons: Invasive, more expensive, longer recovery period, potential for post-operative pain and sensitivity.
- Recovery: Weeks to months, depending on the procedure.

6. Home Remedies and Supportive Care (Temporary Relief)
While not a definitive treatment, these can provide temporary relief while awaiting professional care or during recovery.
- Warm Saltwater Rinses: Mix 1/2 teaspoon of salt in 8 ounces of warm water. Swish for 30 seconds multiple times a day.
- Over-the-Counter Pain Relievers: Ibuprofen or acetaminophen can reduce pain and inflammation.
- Cold Compress: Apply a cold pack to the outside of your cheek for 15-20 minutes at a time to reduce external swelling.
- Soft Diet: Avoid hard, crunchy, or acidic foods that can irritate swollen gums.
- Gentle Brushing/Flossing: Use a soft-bristled toothbrush and be gentle around the affected area.
Pro Tip: If your gum swelling is accompanied by a tooth swelling or severe pain, this often indicates a deeper infection. Do not delay seeing a dentist, as these infections can spread. If you've had an avulsed tooth, contact an emergency dentist immediately, as prompt re-implantation (within 30 minutes) offers the best chance of saving the tooth.
Step-by-Step Process: What to Expect During Treatment
The "step-by-step" process for stopping gum swelling varies significantly based on the diagnosis. Here's what you can generally expect for common scenarios:
Scenario 1: Gingivitis (Mild Gum Swelling)
- Initial Examination: Your dentist will visually inspect your gums, probe for bleeding, and take X-rays to check for bone loss.
- Professional Cleaning (Prophylaxis): A dental hygienist will use specialized instruments to remove plaque and tartar from above and slightly below your gum line. This typically takes 30-60 minutes.
- Oral Hygiene Instructions: You'll receive detailed instructions on proper brushing techniques (using a soft-bristled brush, brushing twice daily), flossing (once daily), and potentially mouthwash use.
- Follow-up: Your dentist may recommend a follow-up appointment in a few weeks or months to assess improvement and ensure proper home care.
- Timeline: Single appointment, resolution within 1-2 weeks with good home care.
Scenario 2: Periodontitis (Moderate to Severe Gum Swelling)
- Comprehensive Periodontal Exam: This involves measuring pocket depths around each tooth, checking for recession, bleeding, and mobility, along with X-rays to assess bone loss.
- Scaling and Root Planing (Deep Cleaning):
- Anesthesia: Local anesthetic will be administered to numb the treatment area.
- Scaling: Specialized instruments (ultrasonic and manual scalers) are used to remove plaque and tartar from above and below the gum line, deep within the periodontal pockets.
- Root Planing: The root surfaces are smoothed to remove bacterial toxins and prevent future plaque adhesion.
- Antimicrobial Agents (Optional): Your dentist may apply a localized antibiotic gel or chip into deep pockets.
- Quadrant Treatment: This procedure is often done over 2-4 appointments, treating one or two quadrants of your mouth at a time.
- Antibiotics (if infection is present): Oral antibiotics may be prescribed to target bacteria throughout your system.
- Follow-up (Periodontal Maintenance): After SRP, you'll need more frequent cleanings (every 3-4 months) to prevent recurrence and manage the disease.
- Timeline: 2-4 appointments over several weeks, followed by ongoing maintenance. Healing and reduction of swelling over several weeks.
Scenario 3: Dental Abscess or Infected Tooth
- Diagnosis: X-rays and vitality tests (e.g., cold test) will pinpoint the infected tooth and locate the abscess.
- Drainage (if applicable): If a visible "pimple" or swelling with pus is present, the dentist may gently lance it to drain the pus, providing immediate relief.
- Antibiotics: Oral antibiotics will likely be prescribed to control the infection.
- Definitive Treatment:
- Root Canal Therapy: If the tooth is savable, the dentist will perform a root canal to remove the infected pulp, clean, and seal the tooth. This typically involves 1-2 appointments.
- Extraction: If the tooth is beyond repair, it will be extracted.
- Restoration: After a root canal, a crown is typically placed on the tooth to protect it.
- Timeline: Emergency visit for diagnosis/drainage, 1-2 appointments for root canal or extraction. Swelling should subside within a few days of definitive treatment and antibiotics.
Scenario 4: Impacted Wisdom Tooth (Pericoronitis)
- Diagnosis: X-rays will show the position of the wisdom tooth and the extent of impaction.
- Cleaning and Irrigation: The dentist will clean the area around the impacted tooth, flushing out trapped food and bacteria.
- Antibiotics: If the infection is significant, antibiotics will be prescribed.
- Pain Management: Advice on warm salt water rinses and over-the-counter pain relievers.
- Definitive Treatment (often Extraction): Once the acute infection subsides, the dentist will discuss options, which usually involve extracting the wisdom tooth to prevent future flare-ups.
- Timeline: Initial visit for acute infection management (days to a week for swelling reduction), followed by extraction appointment (usually 1-2 weeks later).
Cost and Insurance
The cost to stop gum swelling in the US can vary significantly based on the underlying cause, the complexity of the treatment, your geographic location, and whether you have dental insurance.
Average US Price Ranges (Without Insurance):
| Treatment Type | Low Range | Mid Range | High Range | Notes |
|---|---|---|---|---|
| Emergency Exam & X-ray | $75 | $150 | $300 | For initial diagnosis of severe swelling/pain. |
| Standard Cleaning (Prophylaxis) | $75 | $120 | $200 | For gingivitis prevention and maintenance. |
| Scaling & Root Planing (SRP) | $200 per quadrant | $350 per quadrant | $600 per quadrant | Deep cleaning for periodontitis. Typically 2-4 quadrants are treated. Total: $800 - $2,400. |
| Oral Antibiotics | $10 | $50 | $150 | Varies greatly by medication and duration. |
| Localized Antibiotic (e.g., Arestin) | $50 per tooth | $100 per tooth | $150 per tooth | Applied directly into periodontal pockets. |
| Root Canal Therapy (Front Tooth) | $700 | $900 | $1,300 | Incisor/Canine. |
| Root Canal Therapy (Premolar) | $800 | $1,000 | $1,500 | |
| Root Canal Therapy (Molar) | $900 | $1,200 | $2,000+ | Molars are more complex, hence higher cost. |
| Dental Crown (after Root Canal) | $800 | $1,500 | $2,500+ | Varies by material (porcelain, ceramic, gold). This is additional to the root canal cost. |
| Simple Tooth Extraction | $75 | $200 | $400 | For erupted, easily removed teeth. |
| Surgical Tooth Extraction | $200 | $450 | $800 | For impacted teeth, fractured teeth, or those requiring bone removal. |
| Wisdom Tooth Extraction (Impacted) | $250 per tooth | $500 per tooth | $1,000+ per tooth | Cost depends on impaction severity, bone removal needed, and anesthesia used (local vs. general sedation). |
| Periodontal Flap Surgery | $1,000 | $2,500 | $4,000+ | Per quadrant or area, depending on complexity. |
| Soft Tissue Graft | $600 | $1,500 | $3,000+ | Per site. |
| Bone Graft | $400 | $1,200 | $3,000+ | Per site. |
Note: These are average ranges. Actual costs can vary based on the specific dentist, materials used, and geographic location (e.g., urban vs. rural areas).
Insurance Coverage Details
Most dental insurance plans in the US categorize treatments into different coverage levels:
- Preventive Care (Class I): Typically covered at 80-100%. This includes routine exams, X-rays, and standard cleanings (prophylaxis).
- Basic Procedures (Class II): Usually covered at 50-80%. This often includes scaling and root planing, simple extractions, fillings, and sometimes antibiotics.
- Major Procedures (Class III): Typically covered at 0-50%. This category includes root canals, crowns, bridges, dentures, and periodontal surgery. Wisdom tooth extractions can fall into basic or major depending on complexity.
Key points regarding insurance:
- Annual Maximums: Most plans have an annual maximum benefit, typically ranging from $1,000 to $2,000. Once you hit this limit, you pay 100% of costs until the next plan year.
- Deductibles: You may need to pay a deductible (e.g., $50-$100) before your insurance starts covering costs.
- Waiting Periods: Some plans have waiting periods (e.g., 6 months for basic, 12 months for major procedures) before certain benefits become active.
- PPO vs. HMO: PPO plans offer more flexibility in choosing dentists, while HMO plans require you to see dentists within a specific network.
- Medical Insurance for Dental: In rare cases, if the gum swelling is due to a systemic medical condition or severe facial trauma, some aspects of treatment might be covered by your medical insurance, especially if it involves hospital stays or complex oral surgery.
Cost-Saving Tips:
- Prevention: The best way to save money is to prevent gum swelling in the first place with excellent oral hygiene and regular check-ups.
- Early Intervention: Addressing gum swelling at its earliest stage (gingivitis) is far less expensive than treating advanced periodontitis or an abscess requiring a root canal.
- Payment Plans: Many dental offices offer in-house payment plans or work with third-party financing companies like CareCredit.
- Dental Schools: Dental schools often offer treatments at reduced costs, performed by supervised students.
- Community Health Clinics: These clinics may offer services on a sliding scale based on income.
- Discount Plans: Dental discount plans are an alternative to insurance, offering reduced rates for services at participating dentists for an annual fee.
Pro Tip: Always get a detailed treatment plan and estimate from your dentist, and contact your insurance provider directly to understand your specific coverage before proceeding with extensive treatment.
Recovery and Aftercare
Recovery and aftercare are crucial for ensuring the success of any treatment aimed at stopping gum swelling and preventing its recurrence. The specific instructions will depend on the procedure, but general guidelines apply.
After Professional Cleaning (Prophylaxis or Scaling & Root Planing):
- Tenderness and Sensitivity: It's normal to experience some gum tenderness, soreness, and increased tooth sensitivity to hot or cold for a few days to a week. This is especially true after scaling and root planing.
- Bleeding: Minor bleeding may occur for 24-48 hours.
- Pain Management: Over-the-counter pain relievers like ibuprofen (Advil, Motrin) or acetaminophen (Tylenol) can manage discomfort.
- Oral Hygiene: Continue brushing gently with a soft-bristled toothbrush and flossing, but be extra careful around sensitive areas. Your dentist or hygienist might recommend a therapeutic mouthwash.
- Diet: Stick to soft foods for the first day or two, avoiding extremely hot, cold, spicy, or crunchy foods.
- Avoid Smoking: Smoking significantly hinders gum healing.
After Root Canal Therapy:
- Pain and Swelling: It's common to have some soreness and mild swelling around the treated tooth for a few days. The original gum swelling related to the abscess should begin to subside within 24-48 hours.
- Pain Medication: Prescribed or over-the-counter pain medication will help manage discomfort.
- Avoid Chewing: Avoid chewing on the treated tooth until a permanent crown is placed to prevent fracture.
- Oral Hygiene: Continue regular brushing and flossing, but be gentle around the area.
- Follow-up: Return for your permanent crown placement as scheduled to protect the tooth.
After Tooth Extraction:
- Bleeding: Bite firmly on the gauze pack for 30-45 minutes immediately after the extraction to control bleeding. Change gauze as needed. Minor oozing can continue for 24-48 hours.
- Swelling: Expect some facial swelling around the extraction site. Apply a cold compress (15-20 minutes on, 20-30 minutes off) to the outside of your cheek for the first 24-48 hours to minimize swelling.
- Pain: Use prescribed pain medication or over-the-counter options as directed.
- Diet: Consume soft, cool foods for the first 24 hours. Gradually introduce regular foods as tolerated. Avoid using a straw for at least 48 hours to prevent dislodging the blood clot (dry socket).
- Oral Hygiene: Do not rinse your mouth vigorously for 24 hours. After that, gentle warm salt water rinses (1/2 tsp salt in 8 oz water) can help keep the area clean and promote healing. Brush and floss other teeth normally, but avoid the extraction site.
- Avoid Smoking/Alcohol: Both can delay healing and increase the risk of complications.
- Rest: Get plenty of rest.
- Follow-up: Your dentist may schedule a follow-up to check healing or remove sutures.
After Periodontal Surgery:
- Discomfort and Swelling: Expect more significant discomfort and swelling, potentially lasting for several days to a week.
- Pain Medication: Prescribed pain relievers are common.
- Diet: A soft diet is usually recommended for a week or more.
- Oral Hygiene: You'll receive specific instructions, which may include special rinses or gentle brushing with a soft brush only on specific areas. Avoid flossing in the surgical area until cleared by your periodontist.
- Sutures: Sutures may dissolve on their own or need to be removed at a follow-up appointment.
- Follow-up: Multiple follow-up appointments are typical to monitor healing.
General Aftercare Principles:
- Maintain Excellent Oral Hygiene: This is the most critical aspect of preventing recurrence of gum swelling, regardless of the initial cause. Brush twice daily for two minutes with a soft-bristled brush and fluoride toothpaste, and floss once daily.
- Regular Dental Check-ups: Adhere to your dentist's recommended schedule for check-ups and cleanings, typically every six months, but more frequently for those with a history of gum disease (periodontal maintenance).
- Healthy Diet: A balanced diet rich in vitamins and minerals supports overall oral and systemic health. Limit sugary snacks and drinks.
- Avoid Tobacco: Smoking and chewing tobacco are major risk factors for gum disease and significantly impair healing.
- Report Concerns: If you experience increasing pain, swelling that doesn't subside, fever, or any unusual symptoms, contact your dentist immediately.
Prevention
Preventing gum swelling is largely about maintaining consistent, excellent oral hygiene and a healthy lifestyle. Here's how you can proactively safeguard your gums:
1. Consistent and Effective Oral Hygiene
- Brush Twice Daily: Use a soft-bristled toothbrush and fluoride toothpaste. Brush for at least two minutes, gently cleaning all surfaces of your teeth and along the gum line.
- Floss Daily: Flossing removes plaque and food particles from between your teeth and under the gum line where your toothbrush can't reach. This is critical for preventing gingivitis. Consider interdental brushes for larger gaps.
- Use an Antimicrobial Mouthwash: Your dentist may recommend an over-the-counter or prescription mouthwash to help reduce plaque and gingivitis. However, mouthwash should supplement, not replace, brushing and flossing.
- Replace Your Toothbrush: Change your toothbrush every 3-4 months, or sooner if the bristles are frayed.
2. Regular Dental Check-ups and Professional Cleanings
- Schedule Every Six Months: Even with excellent home care, plaque and tartar can build up. Professional cleanings remove these hardened deposits that you can't tackle on your own.
- Early Detection: Regular visits allow your dentist to identify and address early signs of gum inflammation or other issues before they become severe.
3. Balanced Diet
- Nutrient-Rich Foods: Consume a diet rich in fruits, vegetables, lean proteins, and whole grains. Vitamins like C (for tissue repair) and K (for blood clotting) are especially important for gum health.
- Limit Sugary and Acidic Foods/Drinks: These contribute to tooth decay and create an environment conducive to bacterial growth, which can exacerbate gum inflammation.
- Stay Hydrated: Drinking plenty of water helps wash away food particles and bacteria, and promotes saliva production, which neutralizes acids.
4. Avoid Tobacco Products
- Smoking and chewing tobacco are significant risk factors for gum disease. They weaken the immune system, making it harder for gums to fight off infection, and they impair blood flow, which hinders healing. Quitting tobacco is one of the most impactful steps you can take for your oral and overall health.
5. Manage Systemic Health Conditions
- Diabetes Control: If you have diabetes, diligently managing your blood sugar levels is crucial, as uncontrolled diabetes increases susceptibility to gum disease and can worsen existing inflammation.
- Address Other Health Issues: Work with your physician to manage any other chronic conditions that might impact oral health.
6. Be Mindful of Medications
- If you're taking medications known to cause gingival overgrowth (e.g., certain anticonvulsants, immunosuppressants, calcium channel blockers), discuss this with your dentist and physician. Your dentist can monitor your gums closely and recommend strategies to manage the side effect.

7. Protect Your Teeth
- Wear a Mouthguard: If you play contact sports, a mouthguard can prevent trauma to your teeth and gums, which can cause swelling or lead to an avulsed tooth.
- Address Teeth Grinding (Bruxism): If you grind or clench your teeth, discuss a nightguard with your dentist, as excessive force can sometimes contribute to gum problems.
By integrating these preventive measures into your daily routine, you can significantly reduce your risk of experiencing gum swelling and maintain a healthy, vibrant smile.
Risks and Complications
Ignoring gum swelling or failing to treat its underlying cause can lead to a cascade of serious risks and complications, not just for your oral health but for your overall systemic well-being.
Oral Health Complications:
- Progression of Gum Disease: Untreated gingivitis inevitably progresses to periodontitis. This is a destructive disease that leads to:
- Bone Loss: The infection erodes the alveolar bone that supports your teeth.
- Gum Recession: Gums pull away from the teeth, exposing sensitive roots.
- Tooth Mobility and Loss: As bone support diminishes, teeth become loose and eventually fall out or require extraction.
- Recurrent Abscesses: Untreated infections can lead to chronic or recurring dental and periodontal abscesses, causing pain and further tissue destruction.
- Spread of Infection: A dental infection can spread beyond the mouth to other areas of the head and neck, potentially leading to:
- Cellulitis: A serious bacterial skin infection.
- Sinus Infections: If the infection originates from upper back teeth.
- Osteomyelitis: Infection of the jawbone.
- Cavernous Sinus Thrombosis: A rare but life-threatening blood clot in a vein at the base of the brain.
- Ludwig's Angina: A severe, potentially fatal infection of the floor of the mouth and neck.
- Increased Sensitivity: Exposed tooth roots due to gum recession become highly sensitive to hot, cold, and sweets.
- Chewing Difficulties: Pain, loose teeth, or missing teeth can make eating difficult, affecting nutrition.
- Cosmetic Concerns: Swollen, red gums, gum recession, and tooth loss can significantly impact the appearance of your smile.
Systemic Health Complications (Connection between Oral and General Health):
Extensive research by organizations like the American Dental Association (ADA) has highlighted the strong link between oral health and overall health. Untreated gum disease is associated with:
- Cardiovascular Disease: The bacteria from inflamed gums can enter the bloodstream, contributing to plaque buildup in arteries, increasing the risk of heart attack and stroke.
- Diabetes: Periodontal disease can make it harder for diabetics to control their blood sugar levels, and uncontrolled diabetes can worsen gum disease. It's a bidirectional relationship.
- Respiratory Diseases: Inhaling bacteria from infected gums can lead to respiratory infections like pneumonia, especially in individuals with compromised immune systems.
- Adverse Pregnancy Outcomes: Pregnant women with periodontitis have a higher risk of preterm birth and low birth weight babies.
- Rheumatoid Arthritis: Some studies suggest a link between gum disease and rheumatoid arthritis, with similar inflammatory pathways.
- Alzheimer's Disease: Emerging research indicates a potential connection between chronic gum disease and an increased risk of cognitive decline and Alzheimer's disease, possibly due to inflammation.
Comparison Table: Home Remedies vs. Professional Treatments
| Feature | Home Remedies (Temporary Relief) | Professional Dental Treatments (Definitive Solution) |
|---|---|---|
| Goal | Reduce discomfort, manage symptoms temporarily | Diagnose cause, eliminate infection, restore health, prevent recurrence |
| Effectiveness | Limited to symptom relief; does not cure underlying issue | Highly effective at addressing root cause |
| Cost | Very low (salt, OTC pain relievers) | Varies widely from $75 (exam) to $4,000+ (complex surgery) |
| Timeline for Relief | Immediate but temporary | Varies (days for antibiotics, weeks for cleaning, months for surgery) |
| Duration of Effect | Short-lived | Long-term, if proper aftercare and hygiene are maintained |
| Risks | Minimal, if used as directed | Risks associated with anesthesia, infection, sensitivity (manageable) |
| Who Can Administer | Yourself | Licensed dentist, periodontist, dental hygienist |
| Appropriate For | Mild, temporary irritation; while awaiting dental appointment | Any persistent or severe gum swelling; all stages of gum disease |
| Examples | Saltwater rinses, cold compress, OTC pain relievers | Professional cleaning, scaling & root planing, antibiotics, root canal, extraction, periodontal surgery |
Children / Pediatric Considerations
Gum swelling in children can be concerning for parents, but many causes are distinct from adults and often less severe. However, some can indicate significant issues.
Common Causes in Children:
- Eruption Gingivitis: As permanent teeth erupt, the gum tissue around the emerging tooth can become inflamed and swollen. This is usually temporary and resolves once the tooth fully erupts. Eruption cysts or hematomas (blueish swelling) are also common.
- Poor Oral Hygiene: Just like adults, plaque buildup leads to gingivitis. Children may not brush effectively, especially toddlers or those with limited dexterity.
- Trauma: Children are prone to falls and accidents, which can injure the gums, causing localized swelling. A knocked-out (avulsed) baby tooth or permanent tooth is a dental emergency.
- Herpetic Gingivostomatitis: This common viral infection, often seen in toddlers and young children, causes widespread gum inflammation, swelling, painful sores (blisters), fever, and difficulty eating. It's usually self-limiting but requires supportive care.
- Thumb Sucking/Pacifier Use: Prolonged or aggressive habits can cause gum irritation and swelling, especially on the palate or around front teeth.
- Ill-fitting Appliances: For older children with braces or retainers, poorly fitting wires or plastic can rub and irritate the gums.
- Dental Abscess: Deep decay in a baby tooth can lead to an infection and abscess, causing localized gum swelling, often appearing as a "pimple" on the gum. This requires prompt attention as it can affect the developing permanent tooth underneath.
- Impacted Teeth: Similar to adults, impacted wisdom teeth can cause pericoronitis in teenagers, but other impacted permanent teeth (like canines) can also cause localized swelling.
What Parents Should Do:
- Gentle Oral Hygiene: Help your child brush and floss, ensuring all surfaces are cleaned gently. For infants, wipe gums with a soft, damp cloth.
- Warm Saltwater Rinses: For older children, warm salt water rinses can help reduce inflammation and keep the area clean.
- Soft Diet: Offer soft, non-acidic foods if chewing is painful.
- Monitor Symptoms: Look for signs like fever, lethargy, increasing pain, or spreading swelling.
- Seek Pediatric Dental Care:
- Emergency: If the swelling is severe, rapidly spreading, accompanied by fever, difficulty breathing or swallowing, or if a tooth is avulsed, seek immediate emergency dental care.
- Prompt Appointment: For persistent localized swelling, pain around an erupting tooth, or visible "pimples" on the gums, schedule an appointment with a pediatric dentist as soon as possible.
- Educate and Supervise: Teach children proper brushing and flossing techniques and supervise them until they are old enough to do it effectively on their own (usually around age 7-8).
- Mouthguards: Ensure children wear mouthguards during sports to prevent trauma.
Pediatric dentists are specially trained to handle the unique oral health needs of children, including addressing gum swelling in a child-friendly manner.
Frequently Asked Questions
### What is the fastest way to reduce gum swelling at home?
The fastest temporary relief for gum swelling at home is often a warm salt water rinse. Mix 1/2 teaspoon of salt in 8 ounces of warm water and swish for 30 seconds several times a day. Over-the-counter pain relievers like ibuprofen can also help reduce pain and inflammation. However, these are temporary solutions and do not address the underlying cause.
### When should I be concerned about swollen gums?
You should be concerned and see a dentist if gum swelling is persistent (lasts more than a few days), painful, accompanied by bleeding, pus discharge, fever, difficulty eating or swallowing, or if it's localized and feels like a "pimple" on the gum. These can be signs of infection, advanced gum disease, or other serious issues requiring professional intervention.
### Can gum swelling go away on its own?
Mild gum swelling caused by minor irritation or early gingivitis might resolve with improved oral hygiene (diligent brushing and flossing). However, if the swelling is due to an infection, severe gum disease, an impacted tooth, or an abscess, it will not go away on its own and will likely worsen without professional dental treatment.
### Is gum swelling always a sign of gum disease?
Not always. While gum disease (gingivitis or periodontitis) is the most common cause, gum swelling can also be caused by dental abscesses, impacted teeth (like wisdom teeth), trauma, hormonal changes (e.g., pregnancy), certain medications, or even nutritional deficiencies. A dental professional can accurately diagnose the cause.
### How much does it cost to treat swollen gums?
The cost varies significantly based on the cause. A basic dental cleaning for gingivitis might cost $75-$200. Deep cleaning (scaling and root planing) for periodontitis can range from $200-$600 per quadrant. If an infection requires a root canal, costs range from $700-$2,000+, plus a crown ($800-$2,500+). Tooth extractions range from $75-$1,000+.
### Can a tooth swelling cause gum swelling?
Yes, absolutely. An infection originating from the inside of a tooth (due to deep decay or trauma) can spread to the surrounding bone and gum tissue, causing the gum area near the infected tooth to swell. This is often an indication of a dental abscess, which requires urgent dental care, usually a root canal or extraction.
### What happens if I ignore gum swelling?
Ignoring gum swelling can lead to severe complications. Mild gingivitis can progress to periodontitis, causing irreversible bone loss, gum recession, and eventually tooth loss. Untreated infections can spread to other parts of your body, leading to serious medical conditions like heart disease, stroke, and diabetes complications.
### Can an avulsed tooth lead to gum swelling?
Yes, an avulsed (knocked out) tooth causes immediate and significant trauma to the surrounding gum tissue, leading to localized swelling and bleeding. Even if the tooth is successfully re-implanted, swelling and tenderness of the gums are expected during the initial healing phase. This is a dental emergency requiring immediate attention.
### What foods should I avoid if I have swollen gums?
While your gums are swollen and sensitive, it's best to avoid hard, crunchy, sticky, spicy, very hot, or highly acidic foods that can further irritate the inflamed tissue. Opt for soft, bland, and cool foods like yogurt, mashed potatoes, cooked vegetables, soft fruits, and soups.
### Are there specific mouthwashes for swollen gums?
Yes, your dentist might recommend specific antimicrobial mouthwashes, such as those containing chlorhexidine gluconate or essential oils, to help reduce bacteria and inflammation in the gums. However, these are typically prescribed or recommended for short-term use and should be used in conjunction with, not instead of, brushing and flossing.
When to See a Dentist
Knowing when to seek professional dental help for gum swelling is crucial for preventing more serious complications. While minor, temporary irritation might resolve on its own, several warning signs indicate that you need immediate attention or at least a prompt appointment.
Immediate Emergency Dental Care (Red Flags):
Contact an emergency dentist or go to an urgent care clinic if you experience any of the following:
- Sudden, Severe Swelling: Rapidly developing or significantly painful swelling in your gums, especially if it's localized and feels like a "pimple" (indicating an abscess).
- Swelling with Fever: Gum swelling accompanied by a fever, chills, or general malaise. This suggests a spreading infection.
- Difficulty Breathing or Swallowing: If the swelling extends to your throat or face, making it hard to breathe, swallow, or open your mouth fully. This is a life-threatening emergency.
- Pus Discharge: Visible pus draining from the swollen gum area.
- Trauma/Injury: If the swelling is due to a recent injury, a blow to the mouth, or an avulsed tooth (knocked-out tooth). An avulsed permanent tooth requires immediate re-implantation within minutes for the best prognosis.
- Uncontrollable Pain: Pain that is not relieved by over-the-counter pain medication.
Prompt Scheduled Appointment (Warning Signs):
Schedule an appointment with your dentist as soon as possible if you notice:
- Persistent Swelling: Gum swelling that lasts for more than a few days, even if it's not severely painful.
- Bleeding Gums: Gums that bleed easily when brushing or flossing, or spontaneously.
- Red, Tender Gums: Gums that are consistently red, puffy, or tender to the touch.
- Receding Gums: Gums that appear to be pulling away from your teeth, making them look longer.
- Loose Teeth: Any noticeable mobility or loosening of your teeth.
- Changes in Bite: If your teeth feel different when you bite down.
- Chronic Bad Breath or Bad Taste: Persistent bad breath or an unpleasant taste in your mouth that doesn't go away with brushing.
- Sensitivity: Increased tooth sensitivity to hot or cold that persists.
Routine Care Guidance:
If your gums are generally healthy but you have occasional, very mild irritation that quickly subsides with better hygiene, continue your excellent oral care routine and ensure you maintain your regular six-month dental check-ups and cleanings. Prevention is always the best approach.
Do not attempt to self-diagnose or treat severe gum swelling with only home remedies. Only a qualified dental professional can accurately determine the cause and provide the appropriate treatment to safeguard your oral and overall health.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
How to Relieve Gum Swelling
When your gums are swollen, it can be an alarming and uncomfortable experience, often signaling an underlying issue that requires attention. Statistics from the Centers for Disease Control and Prevention (CDC) reveal that **nearly half of adults aged 30 or older in the United States have some form o
February 23, 2026
Teeth Swelling: Complete Guide
When you experience teeth swelling, it's more than just a minor discomfort; it's a clear signal from your body that something is amiss within your oral cavity, often indicating an underlying infection or inflammation that requires prompt attention. A recent survey revealed that **over 25% of adu
February 23, 2026
Submandibular Salivary Gland Swelling: Complete Guide
When you notice a peculiar lump or uncomfortable fullness beneath your jaw, it can be an alarming experience. This sensation, often accompanied by pain and difficulty swallowing, could indicate submandibular salivary gland swelling. Affecting an estimated 1 in 10,000 adults annually, conditi
February 23, 2026
What Helps With Gum Swelling
Gum swelling, medically known as gingival swelling or gingivitis, is a common yet often underestimated dental issue affecting millions of Americans. Have you ever woken up with sore, puffy gums that bleed easily when you brush? You're not alone. Research indicates that nearly **half of all a
February 23, 2026