What Is a Dry Socket in Your Mouth
Key Takeaways
- Approximately 20-25% of individuals who undergo wisdom tooth extraction, and 2-5% of all dental extractions, may experience a painful post-operative complication known as a dry socket. Imagine enduring a dental extraction, anticipating relief, only to be met with intensifying pain a few days lat
Approximately 20-25% of individuals who undergo wisdom tooth extraction, and 2-5% of all dental extractions, may experience a painful post-operative complication known as a dry socket. Imagine enduring a dental extraction, anticipating relief, only to be met with intensifying pain a few days later, radiating throughout your jaw and head. This debilitating discomfort is often the tell-tale sign of what is a dry socket in your mouth, a condition far more severe than typical post-extraction soreness. Understanding this potential complication is crucial for anyone undergoing a tooth removal, as early recognition and proper care can significantly impact your recovery and prevent unnecessary suffering.
A dry socket, medically termed alveolar osteitis, occurs when the protective blood clot that should form in the tooth socket after an extraction either dislodges or dissolves prematurely, exposing the underlying bone and nerves to air, food, and bacteria. This article from SmilePedia.net aims to be your definitive guide to understanding dry socket, covering everything from its causes and symptoms to effective treatment options, prevention strategies, and managing associated discomfort like mouth swelling. We’ll delve into the science behind this condition, equip you with the knowledge to reduce your risk, and provide clear guidance on when to seek professional dental care to ensure a smooth and healthy recovery.
Key Takeaways:
- What it is: A dry socket (alveolar osteitis) is a painful complication following a tooth extraction where the protective blood clot dislodges or dissolves, exposing bone and nerves.
- Prevalence: It affects approximately 2-5% of all dental extractions, rising to 20-25% for wisdom tooth removals.
- Symptoms: Intense, throbbing pain typically starts 2-4 days post-extraction, radiating to the ear, eye, or neck, accompanied by a foul taste and odor.
- Treatment: Involves cleaning the socket, applying medicated dressings (e.g., Alvogyl), and pain management. Treatment costs typically range from $75 to $300 per visit without insurance, often requiring multiple appointments.
- Recovery: Pain relief is usually immediate after treatment, but full resolution may take 7-10 days as new tissue forms.
- Prevention: Avoid smoking, using straws, vigorous rinsing, and eating hard/crunchy foods for at least 48-72 hours post-extraction. Follow all post-operative instructions carefully.
- Risk Factors: Smoking, poor oral hygiene, oral contraceptives, difficult extractions, and previous dry socket history significantly increase risk.
What It Is / Overview
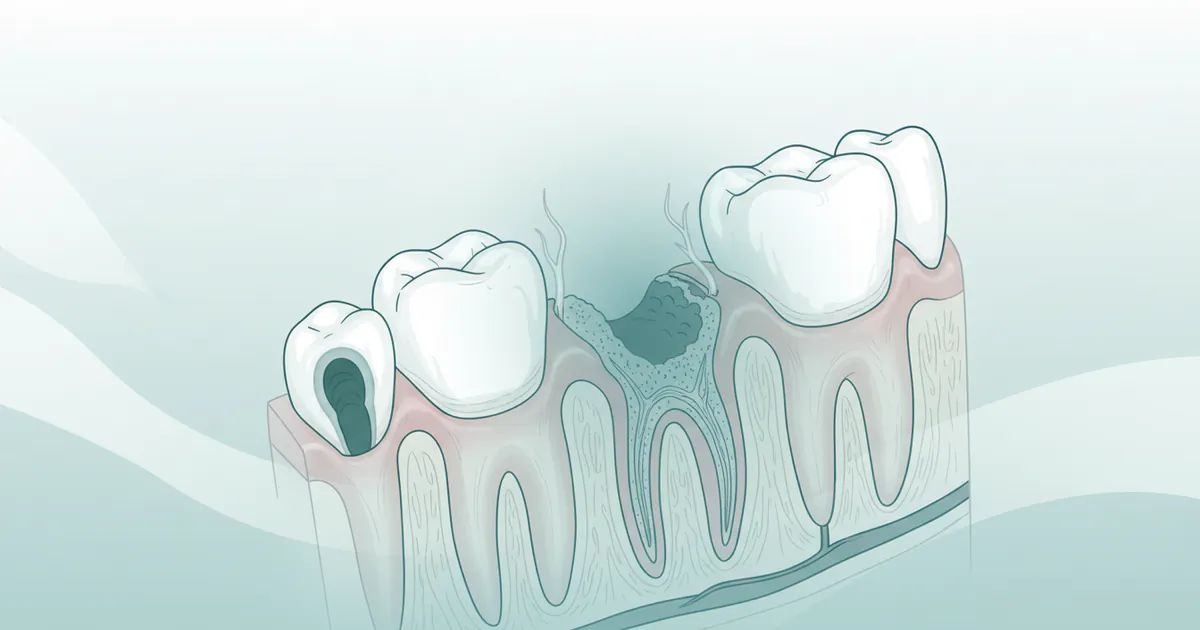
At its core, what is a dry socket in your mouth is a failure of the body's natural healing process following a tooth extraction. When a tooth is removed, it leaves an empty space in the jawbone, known as the tooth socket. Immediately after the extraction, the body initiates a crucial healing cascade, the first step of which is the formation of a blood clot within this socket. This blood clot is not just a stopper; it's a vital biological bandage that serves several critical functions:
- Protection: It shields the delicate underlying bone, nerve endings, and newly forming tissues from the oral environment, including food particles, bacteria, and saliva.
- Foundation for Healing: It acts as a scaffold for new bone and soft tissue to grow, gradually filling in the empty socket.
- Pain Reduction: By covering the exposed nerve endings, it significantly minimizes post-operative pain.

A dry socket occurs when this essential blood clot is either dislodged prematurely or fails to form adequately, or dissolves before the underlying tissues have had a chance to protect themselves. This exposes the raw bone and nerve endings in the socket to the oral cavity. The lack of protection leads to inflammation, intense pain, and delayed healing. Unlike normal post-extraction pain, which typically subsides within a few days, dry socket pain usually begins to intensify 2-4 days after the extraction and can be excruciating, radiating beyond the immediate extraction site. It's a localized osteitis, meaning an inflammation of the bone in the socket.
Types / Variations (Stages of Healing vs. Dry Socket)
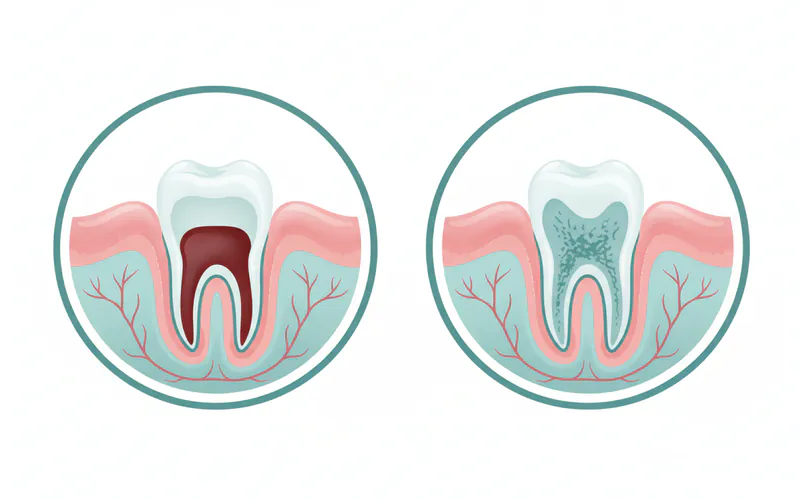
While there aren't distinct "types" of dry socket, it's more accurate to understand it in contrast to the normal healing process and to recognize that its severity can vary. Recognizing the difference is key to knowing what is a dry socket in your mouth versus what is normal post-operative discomfort.
Normal Post-Extraction Healing
Immediately after a tooth extraction, a healthy blood clot forms within minutes to hours. This clot is typically dark red, firm, and fills the socket. Over the next 24-48 hours, mild discomfort, slight mouth swelling, and minimal bleeding are common. Pain should gradually decrease each day. The clot slowly begins to organize, and within 7-10 days, granulation tissue (early healing tissue) starts to replace it. Over weeks to months, this tissue matures into new bone and gum tissue.
Dry Socket (Alveolar Osteitis)
In contrast, a dry socket represents a breakdown in this process.
- Partial vs. Complete Dislodgement: In some cases, only a portion of the clot may be lost, leading to milder symptoms. However, most symptomatic dry sockets involve significant or complete loss of the clot.
- Severity of Pain: The intensity of pain is a primary differentiator. Normal pain is manageable with over-the-counter medication and subsides; dry socket pain is severe, persistent, and often unresponsive to typical pain relievers.
- Appearance of the Socket: Instead of a dark, intact blood clot, a dry socket often appears as an empty-looking socket, sometimes with visible bone that can be pale or gray.
- Odor and Taste: A distinct foul odor and unpleasant taste in the mouth are hallmark signs of a dry socket, resulting from bacterial activity on the exposed bone.
Pro Tip: Do not attempt to "re-form" a blood clot yourself if you suspect a dry socket. This can introduce infection or further damage the area. Always consult your dentist.
Causes / Why It Happens
Understanding the underlying causes is paramount for prevention. A dry socket isn't typically caused by a single factor but often a combination of conditions and activities that compromise the integrity of the blood clot.
Direct Dislodgement of the Blood Clot
The most straightforward cause is physical disruption of the clot.
- Vigorous Rinsing or Spitting: Within the first 24-48 hours, any forceful action in the mouth can literally suck or push the clot out of the socket.
- Sucking Actions: Using a straw, smoking, or even aggressively sipping liquids creates negative pressure in the mouth, which can dislodge the clot.
- Physical Trauma: Accidentally poking the extraction site with your tongue, a toothbrush, or food can also disturb the clot.
Dissolution of the Blood Clot
Sometimes, the clot doesn't dislodge but dissolves prematurely due to enzymatic activity.
- Bacterial Contamination: High levels of bacteria in the mouth, often associated with poor oral hygiene, can release enzymes that break down the blood clot. This is particularly common in the posterior areas of the mouth (e.g., wisdom tooth sites).
- Inflammation: Pre-existing infection at the extraction site or excessive inflammation can contribute to clot breakdown.
Contributing Factors / Risk Factors
Several factors significantly increase an individual's susceptibility to developing a dry socket:
- Smoking and Tobacco Use: This is one of the strongest risk factors. Nicotine constricts blood vessels, reducing blood supply to the healing area, which impairs clot formation and stability. The act of inhaling also creates suction that can dislodge the clot. Smokers are up to 4-5 times more likely to develop a dry socket.
- Oral Contraceptives: High estrogen levels in some oral contraceptives can interfere with blood clotting, increasing the risk.
- Poor Oral Hygiene: A mouth laden with bacteria prior to extraction increases the likelihood of bacterial breakdown of the clot.
- Difficult or Traumatic Extractions: Extractions that require significant force, bone removal, or prolonged surgical time can increase inflammation and reduce blood supply to the socket, making it harder for a stable clot to form.
- Previous History of Dry Socket: If you've had a dry socket before, you are more likely to experience it again with subsequent extractions.
- Inadequate Blood Supply: Certain medical conditions or medications that affect blood flow can increase risk.
- Steroid Use: Some studies suggest a potential link, though less strong than other factors.
- Age: While extractions are common at all ages, the risk of dry socket is generally higher in older individuals.
- Bone Density: Denser bone, often seen in older patients, can complicate extractions and increase the risk.
- Certain Medications: Some medications, particularly those affecting blood coagulation, can indirectly impact clot stability. Always inform your dentist of all medications you are taking.
ADA Guideline: The American Dental Association (ADA) emphasizes careful post-operative instructions, particularly advising against smoking and vigorous rinsing, as key to preventing dry socket.
Signs and Symptoms
Recognizing the signs and symptoms of a dry socket is critical for prompt diagnosis and treatment. Unlike the typical discomfort that follows an extraction, dry socket pain is distinct and often debilitating.
Key Indicators to Watch For:
- Intense, Throbbing Pain: This is the most defining symptom. The pain typically starts 2-4 days after the extraction, not immediately. It's often described as a deep, aching, throbbing pain that can be significantly more severe than the initial post-operative pain.
- Pain Radiating: The pain doesn't stay confined to the extraction site. It commonly radiates to the ear on the same side, the eye, temple, or down the neck.
- Visible Empty Socket: When you look in the mirror (or a dentist examines it), the socket will appear empty. Instead of a dark red blood clot, you might see exposed bone, which can look pale or grayish.
- Foul Taste and Odor: A very unpleasant, often putrid, taste in your mouth and a corresponding bad breath (halitosis) are strong indicators. This is due to the breakdown of exposed tissue and bacterial activity in the open socket.
- Pain Unresponsive to Over-the-Counter Pain Relievers: While normal post-extraction pain usually responds to ibuprofen or acetaminophen, dry socket pain often persists despite these medications.
- Swollen Lymph Nodes: In some cases, especially if there's significant inflammation or infection, you might experience swollen and tender lymph nodes under the jaw or in the neck.
- Mild Fever (rare): While not typical, a low-grade fever might occur in some instances due to generalized inflammation.
How to Distinguish from Normal Post-Extraction Discomfort:
| Feature | Normal Healing After Extraction | Dry Socket (Alveolar Osteitis) |
|---|---|---|
| Pain Onset | Starts immediately after surgery, gradually decreases over 2-3 days. | Typically begins 2-4 days post-extraction, intensifies rapidly. |
| Pain Intensity | Mild to moderate, manageable with OTC pain relievers. | Severe, throbbing, excruciating, often unresponsive to OTCs. |
| Pain Radiation | Localized to the extraction site. | Radiates to ear, eye, temple, neck on the affected side. |
| Socket Appearance | Dark red, intact blood clot or early granulation tissue. | Empty socket, visible pale or grayish bone. |
| Taste/Odor | Normal, or slight metallic taste from residual bleeding. | Foul, putrid taste and severe bad breath. |
| Swelling | Localized mouth swelling or bruising, gradually subsides. | May have some swelling, but pain is disproportionately severe. |
| Response to Meds | Responds well to prescribed or OTC pain medication. | Minimal relief from standard pain medication. |
Pro Tip: If you experience any of the severe symptoms listed for dry socket, especially pain that worsens significantly a few days after extraction, contact your dentist immediately. Do not wait for it to improve on its own.
Treatment Options
Effective treatment for a dry socket aims to alleviate pain, protect the exposed bone, and promote healing. It is crucial to have a dentist or oral surgeon address the condition, as home remedies are generally insufficient.
1. Irrigation and Cleaning
- Description: The first step is for the dentist to gently irrigate (flush) the socket with a saline solution or an antiseptic rinse (like chlorhexidine) to remove any food debris, bacteria, and necrotic tissue. This cleansing is vital to reduce infection and prepare the site for medication.
- Pros: Immediately cleanses the site, reducing bacterial load and irritation.
- Cons: Does not provide long-term pain relief on its own.
2. Medicated Dressings
- Description: After irrigation, the dentist will pack the socket with a medicated dressing. This dressing typically contains an analgesic (pain reliever) and sometimes an antiseptic. Common medications include:
- Alvogyl: A paste containing eugenol (clove oil derivative for pain relief), iodoform (antiseptic), and butamben (local anesthetic). It's self-eliminating, meaning it slowly dissolves over time.
- Zinc Oxide-Eugenol (ZOE) paste: Similar to Alvogyl, eugenol provides strong analgesic properties.
- Gauze impregnated with various medications: Sometimes a simple gauze strip soaked in a pain-relieving solution is used.
- Pros: Provides rapid and significant pain relief by protecting the exposed bone and delivering medication directly to the site. Promotes a sterile environment for healing.
- Cons: Dressings usually need to be changed every 24-48 hours initially, then less frequently, requiring multiple dental visits. Some patients may dislike the taste of the medication.
3. Pain Management
- Description: In addition to the medicated dressing, your dentist may prescribe stronger pain medication, such as prescription-strength NSAIDs (e.g., ibuprofen 600-800mg) or, in severe cases, opioids for short-term use.
- Pros: Addresses systemic pain that might persist despite the local dressing.
- Cons: Potential side effects (gastrointestinal upset, drowsiness) and risk of dependence with opioids.
4. Antibiotics (Rarely Needed)
- Description: Antibiotics are generally not prescribed for dry socket itself, as it is an inflammatory condition, not typically a bacterial infection requiring systemic antibiotics. They may only be considered if there is evidence of a secondary bacterial infection spreading beyond the socket, or in immunocompromised patients.
- Pros: Necessary for actual infections.
- Cons: Overuse contributes to antibiotic resistance; generally ineffective for dry socket pain.
5. At-Home Care
- Gentle Rinsing: Your dentist might instruct you to gently rinse with warm salt water or a prescribed antiseptic mouthwash (like chlorhexidine) to keep the area clean. This is very different from vigorous rinsing.
- Cold Compress: While often used for initial swelling, a cold compress may still offer some comfort for mouth swelling associated with the surrounding inflammation.
- Avoid Irritants: Absolutely no smoking, alcohol, or using straws. Stick to soft foods.
- Oral Hygiene: Continue careful brushing and flossing, avoiding the immediate extraction site.
Comparison of Treatment Approaches:
| Treatment Method | Primary Action | Duration/Frequency | Pain Relief (Speed) | Advantages | Disadvantages |
|---|---|---|---|---|---|
| Irrigation & Cleaning | Removes debris, reduces bacteria | One-time per visit | Minimal immediate | Essential first step, prevents further irritation | No sustained pain relief, requires follow-up |
| Medicated Dressing | Protects bone, delivers analgesic | Replaced every 1-3 days (multiple visits) | Rapid & significant | Highly effective for pain, promotes healing | Requires multiple dental visits, taste/odor |
| Prescription Pain Meds | Systemic pain reduction | As directed | Hours | Addresses overall discomfort, complements local | Side effects, potential for dependence (opioids) |
| Antibiotics (rare) | Fights bacterial infection | As directed | Days | Only if infection is present | Ineffective for dry socket, risk of resistance |
Pro Tip: Always complete the full course of dental visits for dressing changes as recommended by your dentist. Stopping treatment too soon can lead to prolonged pain and delayed healing.
Step-by-Step Process: What to Expect During Treatment
When you visit your dentist for a suspected dry socket, here’s a typical outline of what you can expect during the treatment process:
-
Examination and Diagnosis:
- Your dentist will ask about your symptoms, when they started, and the intensity of your pain.
- They will then gently examine the extraction site. They'll look for an empty socket, exposed bone, and assess for any signs of infection. The distinctive appearance and the specific type of pain are usually enough for a diagnosis.
-
Anesthesia (if needed):
- While dry socket is painful, often the pain is localized enough that simple irrigation can be done without anesthesia. However, if the area is extremely sensitive or if extensive cleaning is required, your dentist might administer a local anesthetic to numb the area around the socket.
-
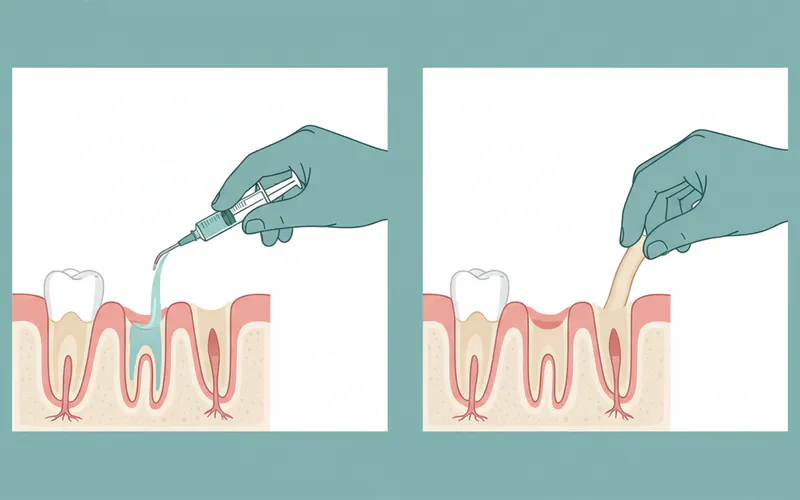
Gentle Irrigation:
- Using a syringe, your dentist will gently flush the empty socket with warm saline solution or an antiseptic rinse (like chlorhexidine). This step is crucial to remove any trapped food particles, bacteria, and debris that might be irritating the exposed bone. You might feel a cool sensation during this process.
-
Placement of Medicated Dressing:
- After cleaning, the dentist will carefully place a medicated dressing into the socket. This dressing is typically a small piece of gauze or a special paste (like Alvogyl) impregnated with pain-relieving (analgesic) and sometimes antiseptic agents. The dressing acts as a protective barrier, shields the exposed bone from the oral environment, and delivers medication directly to the painful site.
- You should feel significant pain relief relatively quickly after the dressing is placed.
-
Post-Treatment Instructions:
- Your dentist will provide specific instructions for at-home care, which will include:
- Avoiding vigorous rinsing, spitting, or using straws.
- Eating only soft foods to prevent dislodging the dressing or irritating the site.
- Gentle oral hygiene, avoiding brushing the immediate area.
- Taking prescribed pain medication as directed.
- Instructions for follow-up appointments.
- Your dentist will provide specific instructions for at-home care, which will include:
-
Follow-Up Appointments:
- A single treatment is rarely enough. You will typically need to return to the dental office every 1-3 days for several days for the dressing to be changed and the socket re-cleaned. This is important to ensure continuous pain relief and to monitor healing. As healing progresses, the frequency of dressing changes will decrease.
- The goal is for the socket to eventually heal enough to no longer require a dressing, and for new tissue to start forming.
Cost and Insurance
The cost of treating a dry socket in the US can vary significantly based on your location, the dentist's fees, and whether you have dental insurance. It's important to understand these factors to plan for potential expenses.
Average US Costs (Without Insurance):
- Per Visit Cost: A single visit for dry socket treatment (irrigation and placement of medicated dressing) typically ranges from $75 to $300.
- Total Treatment Cost: Since multiple visits are usually required (often 3-5 visits over a week or two), the total out-of-pocket cost for treating a dry socket can accumulate to $225 to $1,500.
- Factors Influencing Cost:
- Geographic Location: Costs are generally higher in metropolitan areas and on the coasts (e.g., California, New York) compared to rural areas or the Midwest.
- Complexity: If the dry socket is particularly stubborn or involves a secondary infection requiring additional interventions, the cost may increase.
- Dentist's Fees: Specialist oral surgeons may charge more than general dentists.

Insurance Coverage:
- Most dental insurance plans do cover dry socket treatment, as it is considered a post-operative complication of an extraction.
- Coverage Levels: Coverage typically falls under "basic services" or "restorative procedures," meaning plans often cover 50% to 80% of the cost after your deductible is met.
- Deductibles and Co-pays: You will likely be responsible for your annual deductible (if not already met) and any co-pays or co-insurance percentages specified by your plan.
- Pre-Authorization: While not usually required for emergency dry socket treatment, it's always wise to check with your insurance provider or have the dental office assist you in verifying coverage.
Example Cost Scenario:
Let's assume a total treatment cost of $600 for multiple visits.
- Without Insurance: You pay the full $600.
- With Insurance (80% coverage after $100 deductible):
- You pay the first $100 (deductible).
- Remaining balance: $600 - $100 = $500.
- Insurance pays 80% of $500 = $400.
- You pay the remaining 20% of $500 = $100.
- Total Out-of-Pocket: $100 (deductible) + $100 (co-insurance) = $200.
Recovery and Aftercare
Once dry socket treatment has begun, proper at-home recovery and aftercare are crucial to ensure effective healing and prevent recurrence. The primary goal is to maintain the integrity of the medicated dressing and keep the socket clean.
Immediate Post-Treatment:
- Pain Relief: You should experience significant pain relief almost immediately after the medicated dressing is placed. This relief is often profound compared to the prior pain.
- Follow Instructions: Strictly adhere to all post-treatment instructions provided by your dentist.
Ongoing Home Care:
- Medication: Take any prescribed pain medication as directed. Do not wait for the pain to become severe before taking it.
- Diet: Stick to a soft diet for several days. Avoid hard, crunchy, sticky, or very hot foods that could dislodge the dressing or irritate the socket. Examples include mashed potatoes, yogurt, applesauce, smoothies (without a straw!), and soft scrambled eggs. Gradually reintroduce firmer foods as healing progresses.
- Oral Hygiene:
- Continue brushing and flossing gently, but avoid brushing directly over the extraction site.
- Your dentist may recommend very gentle rinsing with warm salt water (1/2 teaspoon salt in 8 ounces warm water) or a prescribed antimicrobial mouthwash (like chlorhexidine) starting 24 hours after treatment. Do NOT rinse vigorously, as this can dislodge the dressing. Simply let the water pool in your mouth over the site and gently tip your head to let it drain.
- Avoid Irritants:
- Absolutely NO smoking or vaping. This is the most critical instruction. Nicotine restricts blood flow, and the sucking action can dislodge the dressing. The chemicals in smoke are also highly irritating.
- Do NOT use straws. The suction created can dislodge the dressing.
- Avoid alcohol for at least 24-48 hours, as it can interfere with healing and medications.
- Rest: Get plenty of rest. Avoid strenuous physical activity for at least the first 24-48 hours after treatment, as it can increase blood pressure and potentially disturb the healing site.
- Manage Mouth Swelling: While dry socket itself often has less swelling than a normal extraction, some inflammation may still be present. You can apply a cold compress to the outside of your cheek for 20 minutes on, 20 minutes off, during the first 24-48 hours, but for dry socket the priority is addressing the exposed bone. After 48 hours, warm compresses can help with stiffness and encourage blood flow.
Duration of Recovery:
- Pain relief from the dressing is usually immediate, but the dry socket itself takes time to heal. You can expect to need dressing changes for 7-10 days, or until the socket is no longer painful and signs of healthy granulation tissue are visible.
- Complete healing of the socket, where new bone and gum tissue fill the space, can take several weeks to a few months.
Pro Tip: If the pain returns or worsens between dressing changes, or if your dressing comes out prematurely, contact your dentist immediately. Do not try to reinsert a dislodged dressing yourself.
Prevention
Preventing a dry socket is far easier and less painful than treating one. Most preventive measures focus on protecting the blood clot and minimizing factors that lead to its dislodgement or dissolution.
Before the Extraction:
- Inform Your Dentist: Be completely honest about your medical history, including all medications, smoking habits, and if you've had a dry socket before.
- Oral Contraceptives: If you take oral contraceptives, discuss this with your dentist. They might recommend scheduling your extraction during a specific time in your cycle (e.g., days 23-28, when estrogen levels are lower) to reduce risk, although this remains a debated topic in dentistry.
- Excellent Oral Hygiene: Ensure your mouth is as clean as possible before the procedure to reduce the bacterial load. Your dentist might prescribe an antiseptic mouthwash like chlorhexidine to use for a few days before and after the extraction.
After the Extraction (Critical Period: First 48-72 Hours):
- Protect the Blood Clot: This is the paramount rule.
- No Smoking or Vaping: This is the absolute most important instruction. Avoid all tobacco and nicotine products for at least 72 hours, preferably longer. The suction from inhaling and the chemicals significantly increase dry socket risk.
- No Straws: Avoid using straws for at least 5-7 days. The suction created can dislodge the clot.
- Avoid Vigorous Rinsing or Spitting: For the first 24-48 hours, do not rinse your mouth vigorously or spit forcefully. If you need to rinse (e.g., after the initial 24 hours with warm salt water), do so very gently.
- Avoid Touching the Site: Do not poke the extraction site with your fingers or tongue.
- Diet: Stick to soft foods for the first few days. Avoid hard, crunchy, or sticky foods that might dislodge the clot or get stuck in the socket.
- Oral Hygiene:
- Brush your teeth gently, avoiding the extraction site directly for the first 24 hours. You can gradually resume gentle brushing around the area afterward.
- Your dentist may recommend a prescription chlorhexidine rinse or gentle warm salt water rinses (after 24 hours) to keep the area clean, but always use with caution and without vigorous swishing.
- Rest: Get plenty of rest and avoid strenuous physical activity for the first 24-48 hours. Elevated heart rate and blood pressure can sometimes affect the clot.
- Manage Swelling: Applying a cold compress to the outside of your cheek for 20 minutes on, 20 minutes off, for the first 24 hours can help minimize mouth swelling and discomfort, which also supports a stable clot.
- Follow Post-Operative Instructions: Your dentist will provide specific, detailed instructions. Follow them meticulously. This is your best defense against developing a dry socket.
Comparison of Key Prevention Strategies:
| Activity | Recommendation (First 72 hours) | Why It's Important |
|---|---|---|
| Smoking/Vaping | Absolutely AVOID. | Nicotine constricts blood vessels, impairs healing. Sucking action dislodges clot. |
| Using Straws | Absolutely AVOID. | Creates negative pressure (suction) in the mouth, pulling the blood clot out. |
| Vigorous Rinsing/Spitting | Absolutely AVOID. (Especially first 24-48 hrs) | Forceful movement can dislodge the protective blood clot. Gentle rinses after 24 hours if advised. |
| Hard/Crunchy Foods | AVOID. Stick to soft foods. | Can dislodge the clot, get stuck in the socket, or irritate the healing tissue. |
| Oral Contraceptives | Discuss with dentist (potential scheduling considerations). | Higher estrogen levels may interfere with blood clot formation and stability. |
| Alcohol Consumption | AVOID. | Can interfere with healing, interact with medications, and contribute to dehydration. |
| Strenuous Activity | AVOID. Rest is crucial. | Can increase blood pressure, potentially causing bleeding or dislodging the clot. |
| Oral Hygiene | Gently brush, avoiding extraction site. Use recommended rinses. | Reduces bacteria. Gentle approach prevents physical disruption of the clot. |
Risks and Complications
While a dry socket itself is a complication of an extraction, a prolonged or untreated dry socket can lead to further issues. Recognizing these potential risks underscores the importance of prompt professional care.
1. Prolonged Pain and Discomfort
- This is the most immediate and common complication. Without treatment, the severe pain associated with dry socket can persist for several days to weeks, significantly impacting quality of life, sleep, and ability to eat.
2. Delayed Healing
- The primary role of the blood clot is to serve as a matrix for new tissue growth. When the clot is lost, the healing process is significantly delayed. The open socket remains vulnerable and takes much longer to fill in with new bone and gum tissue.
3. Infection
- While a dry socket itself is primarily an inflammatory condition rather than an infection, the exposed bone and open socket are more susceptible to secondary bacterial infections. Food particles and bacteria can easily accumulate in the exposed area, potentially leading to:
- Localized Infection (Osteomyelitis): An infection of the bone itself, though rare, can be a serious complication of an untreated dry socket, especially in immunocompromised individuals. This would manifest as increased pain, swelling, pus discharge, and potentially fever.
- Cellulitis: A spreading bacterial infection of the soft tissues, which would require aggressive antibiotic treatment.
4. Halitosis (Bad Breath) and Dysgeusia (Bad Taste)
- The breakdown of tissue and accumulation of bacteria in the exposed socket can lead to a persistent foul odor and taste in the mouth, which can be socially embarrassing and further diminish appetite.
5. Increased Cost and Treatment Time
- Untreated or prolonged dry socket leads to more frequent dental visits, additional medications, and increased overall treatment costs and time.
6. Anxiety and Dental Phobia
- The intense pain and prolonged recovery associated with dry socket can exacerbate dental anxiety or even lead to the development of dental phobia, making future dental treatments more challenging for the patient.
Pro Tip: If you experience any signs of spreading infection, such as fever, significant facial swelling that extends beyond the immediate area, or difficulty swallowing, seek emergency dental or medical attention immediately.
Children / Pediatric Considerations
Dry socket is significantly less common in children than in adults, primarily because most extractions in children involve deciduous (baby) teeth, which have shallower roots and often heal more rapidly. The bone structure in children is also more vascular (has a richer blood supply), which aids in faster clot formation and healing. Furthermore, wisdom teeth, which are the most common sites for dry socket in adults, are typically not extracted in children.
However, dry socket can still occur in adolescents who have permanent teeth extracted, especially if risk factors like smoking or poor post-operative care are present.
Key Considerations for Parents:
- Education is Key: If your child needs a tooth extraction, your dentist will provide specific post-operative instructions. As a parent, it's crucial to understand and enforce these instructions diligently.
- Monitoring for Symptoms: While less likely, be aware of the signs. If your child complains of severe, throbbing pain that worsens 2-4 days after an extraction, especially if accompanied by a bad taste or odor, contact your dentist. Children may describe the pain differently, perhaps as a persistent "ouchie" that won't go away, or complain of earache or headache.
- Preventive Measures for Children:
- No Straws: Ensure children do not use straws after an extraction.
- No Spitting/Vigorous Rinsing: Supervise them to prevent forceful spitting or rinsing.
- Soft Diet: Encourage a soft diet and avoid hard, crunchy snacks for several days.
- Oral Hygiene: Help them maintain gentle oral hygiene, carefully avoiding the extraction site.
- Smoking/Vaping: This is a major risk factor in adolescents. If your teenager smokes or vapes, the extraction provides a critical opportunity to discuss the heightened risks and enforce abstinence for optimal healing.
- Communication: Maintain open communication with your child about their discomfort. Children may not always articulate pain as clearly as adults.
Pro Tip for Parents: If your child undergoes an extraction, ensure they understand why they need to follow the post-operative instructions. Explaining it in simple terms ("we need to protect the special bandage in your mouth") can increase compliance.
Cost Breakdown
While dry socket treatment is usually covered by dental insurance (as discussed above), understanding the specific cost breakdown can help in planning, especially for those without coverage or with high deductibles. The actual cost is highly variable, but here's a general framework.

Factors Contributing to Cost:
- Initial Consultation/Exam Fee: If it's a new issue, there will be a fee for the examination and diagnosis. This can range from $50 to $150.
- Irrigation and Debridement: The process of cleaning out the socket is a distinct procedure. This can cost $50 to $150 per visit.
- Medicated Dressing Placement: The cost for placing the medicated dressing (which often includes the dressing material itself) can range from $25 to $100 per dressing.
- Follow-Up Visits: Each subsequent visit for dressing changes and re-evaluation will incur charges for irrigation and dressing placement.
- Prescription Medications: Any prescribed pain medication will be an additional cost, covered by your medical insurance or out-of-pocket (e.g., $10-$50 for a generic prescription).
- X-rays (if necessary): If the dentist needs to rule out other complications, an X-ray might be taken, adding $25-$100.
Average US Cost Ranges (Without Insurance):
| Service Item | Low Range (USD) | Mid Range (USD) | High Range (USD) |
|---|---|---|---|
| Initial Exam/Diagnosis | $50 | $100 | $150 |
| Irrigation & Dressing (per visit) | $75 | $125 | $200 |
| Total for 3 Visits | $225 | $375 | $600 |
| Total for 5 Visits | $375 | $625 | $1000 |
| Prescription Pain Medication | $10 | $30 | $75 |
| Total Estimated Treatment (3-5 visits) | $285 | $755 | $1,825 |
(Note: These are estimates and actual costs can vary greatly. The "Total Estimated Treatment" includes the initial exam and potential prescription costs alongside multiple treatment visits.)
Payment Plans and Financing Options:
- In-house Payment Plans: Many dental offices offer interest-free payment plans for a few months, especially for established patients.
- Dental Credit Cards: Options like CareCredit allow you to finance dental procedures, often with promotional periods of 0% interest if paid in full within a certain timeframe (e.g., 6-24 months).
- Personal Loans: Banks or credit unions offer personal loans, but these typically come with interest rates.
- Health Savings Accounts (HSAs) / Flexible Spending Accounts (FSAs): If you have an HSA or FSA through your employer, you can use these tax-advantaged accounts to pay for dry socket treatment.
Cost-Saving Tips:
- Preventative Care: The absolute best way to save money is to prevent dry socket in the first place by meticulously following all post-operative instructions.
- Prompt Treatment: Address dry socket symptoms immediately. Delaying treatment can lead to more severe pain, more complications, and therefore more complex and expensive treatment.
- Ask for an Itemized Bill: Request a detailed breakdown of costs before treatment if possible.
- Inquire About Discounts: Some offices offer discounts for upfront cash payments.
- Negotiate: In certain situations, especially for those without insurance or facing significant financial hardship, it may be possible to negotiate the fee with the dental office.
Frequently Asked Questions
### How long does dry socket pain last?
Untreated dry socket pain can last for 7-10 days, sometimes even longer, as the exposed bone is continually irritated. However, with proper dental treatment, significant pain relief typically occurs within minutes to hours after the medicated dressing is placed, though the underlying healing still takes about 1-2 weeks.
### Can I treat a dry socket at home?
No, it is highly recommended to seek professional dental care for a dry socket. While some gentle rinsing with salt water might be advised by your dentist as part of home care, an actual dry socket requires professional cleaning and the application of a medicated dressing to effectively relieve pain and promote healing. Home remedies are generally ineffective and can sometimes worsen the condition.
### What does a dry socket look like?
A dry socket typically appears as an empty-looking tooth socket, devoid of the dark blood clot that should normally be present. You might see exposed bone, which can look pale white or gray, rather than the healthy red or dark appearance of a healing clot. There might also be visible food debris trapped within the socket.
### How soon after extraction can a dry socket occur?
Dry socket symptoms usually begin to manifest 2 to 4 days after the tooth extraction. It is uncommon for it to develop immediately after the procedure or much later than five days post-extraction. The delay is because the initial blood clot needs time to dislodge or dissolve for the symptoms to emerge.
### Will my dry socket heal on its own?
While the socket will eventually heal on its own over a longer period, it will do so very slowly and with persistent, severe pain. Professional treatment is crucial not only for immediate pain relief but also to protect the exposed bone from infection and accelerate the healing process by providing a clean, protected environment for new tissue to form.
### Is dry socket always accompanied by bad breath or taste?
Yes, a distinct foul odor and an unpleasant, often putrid, taste in the mouth are very common and often diagnostic symptoms of a dry socket. This is due to bacterial activity and the breakdown of tissues in the exposed, unhealed socket, making it a reliable indicator in addition to severe pain.
### Can I still get a dry socket if I follow all post-op instructions?
While strictly following post-operative instructions significantly reduces the risk, it does not guarantee complete immunity. Some factors, such as a very traumatic extraction, pre-existing inflammation, or individual healing variations, can still contribute to a dry socket even with perfect adherence to instructions, though this is less common.
### How does dry socket affect mouth swelling?
Dry socket typically causes less overall mouth swelling than a normal extraction initially, as there is no intact blood clot leading to fluid accumulation. However, the exposed bone and surrounding inflammation can cause localized swelling around the extraction site and along the jaw. The primary symptom is pain, not necessarily extensive swelling.
### Are there alternatives to the medicated dressing?
The medicated dressing is the gold standard for immediate pain relief and protection in dry socket treatment. While some dentists might use different types of medicated pastes or gels, the principle remains the same: to cover the exposed bone and deliver pain-relieving agents. There are no widely accepted effective alternatives that don't involve some form of local protection and medication directly in the socket.
### Can dry socket lead to more serious complications?
While relatively rare, an untreated or prolonged dry socket can potentially lead to secondary bacterial infections, such as localized osteomyelitis (bone infection) or spreading cellulitis. It also results in prolonged pain, significantly delayed healing, and increased costs due to extended treatment. Prompt professional care minimizes these risks.
When to See a Dentist
Knowing when to seek professional dental attention is crucial for managing dry socket and other post-extraction complications.
Immediate Attention (Emergency Situation - Call Dentist ASAP):
- Intensifying Pain 2-4 Days Post-Extraction: This is the hallmark sign. If your pain, instead of decreasing, significantly worsens 2 to 4 days after your tooth extraction, and especially if it's severe, throbbing, and radiates to your ear, eye, or neck.
- Pain Unresponsive to Medication: If over-the-counter pain relievers or even prescribed post-operative pain medication are not providing relief from the severe pain.
- Foul Taste and Odor: A persistent, putrid taste in your mouth or severe bad breath originating from the extraction site.
- Visible Empty Socket: If you look at the extraction site and see exposed bone instead of a dark blood clot.
- Signs of Spreading Infection: While rare for dry socket itself, if you experience:
- High fever.
- Significant and rapidly increasing facial mouth swelling that extends beyond the immediate jaw area.
- Pus discharge from the socket.
- Difficulty swallowing or breathing.
- Swollen lymph nodes in your neck or under your jaw that are increasingly painful.
Routine Care Guidance:
- Normal Post-Operative Discomfort: Mild pain, mouth swelling, and minor bleeding for the first 1-2 days are normal. Manage this with prescribed medications and cold compresses.
- Follow-Up Appointments: Attend all scheduled follow-up appointments after your extraction, even if you feel fine. Your dentist needs to monitor your healing.
- Minor Concerns: For very minor concerns, like a small amount of persistent bleeding (after 24 hours) or irritation, you can call your dentist's office for advice during business hours.
Red Flags vs. Routine Care: The key differentiator for dry socket is the delayed onset and severity of pain, coupled with the specific symptoms of an empty socket and foul taste/odor. Do not dismiss these symptoms as "normal healing." When in doubt, it is always safer to contact your dental professional. Early intervention for dry socket leads to much faster pain relief and a smoother recovery.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
How to Relieve Gum Swelling
When your gums are swollen, it can be an alarming and uncomfortable experience, often signaling an underlying issue that requires attention. Statistics from the Centers for Disease Control and Prevention (CDC) reveal that **nearly half of adults aged 30 or older in the United States have some form o
February 23, 2026
Teeth Swelling: Complete Guide
When you experience teeth swelling, it's more than just a minor discomfort; it's a clear signal from your body that something is amiss within your oral cavity, often indicating an underlying infection or inflammation that requires prompt attention. A recent survey revealed that **over 25% of adu
February 23, 2026
Submandibular Salivary Gland Swelling: Complete Guide
When you notice a peculiar lump or uncomfortable fullness beneath your jaw, it can be an alarming experience. This sensation, often accompanied by pain and difficulty swallowing, could indicate submandibular salivary gland swelling. Affecting an estimated 1 in 10,000 adults annually, conditi
February 23, 2026
What Helps With Gum Swelling
Gum swelling, medically known as gingival swelling or gingivitis, is a common yet often underestimated dental issue affecting millions of Americans. Have you ever woken up with sore, puffy gums that bleed easily when you brush? You're not alone. Research indicates that nearly **half of all a
February 23, 2026