Bulimia Teeth Damage: Complete Guide
Key Takeaways
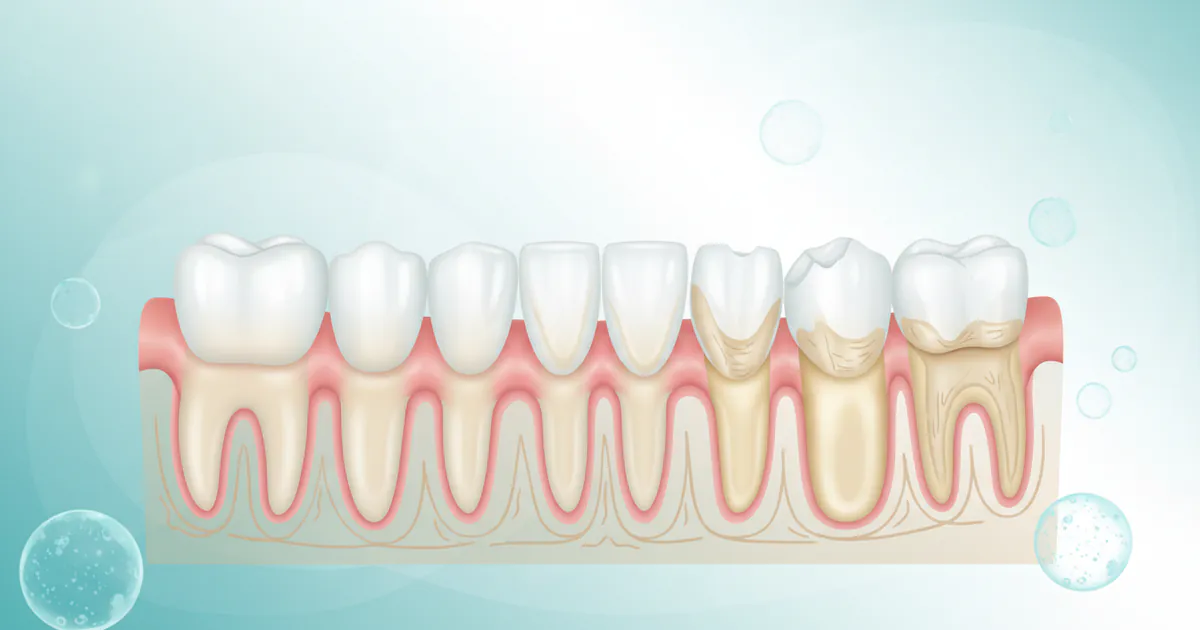
- Bulimia Nervosa, a serious eating disorder characterized by cycles of binge eating followed by compensatory behaviors like self-induced vomiting, excessive exercise, or laxative abuse, inflicts profound damage far beyond its immediate psychological and nutritional impacts. While the focus often lies
Bulimia Nervosa, a serious eating disorder characterized by cycles of binge eating followed by compensatory behaviors like self-induced vomiting, excessive exercise, or laxative abuse, inflicts profound damage far beyond its immediate psychological and nutritional impacts. While the focus often lies on systemic health, the oral cavity bears a direct and often irreversible brunt of this disorder. Studies indicate that up to 89% of individuals with bulimia nervosa exhibit significant dental erosion, making bulimia teeth damage a critical, yet frequently overlooked, health concern. This comprehensive guide from SmilePedia.net aims to shed light on the intricate ways bulimia affects your oral health, from the tell-tale signs of acid erosion to the comprehensive treatment and prevention strategies available. We'll delve into understanding the mechanisms of damage, exploring effective restorative and preventive dental treatments, discussing cost implications, and providing actionable advice on protecting your smile. Your journey to understanding and mitigating the effects of bulimia on your teeth begins here, empowering you with the knowledge to seek timely intervention and preserve your oral health.
Key Takeaways:
- Primary Damage: Acid erosion (perimylolysis) from frequent vomiting is the hallmark of bulimia teeth damage, leading to irreversible loss of tooth enamel.
- Common Signs: Watch for increased tooth sensitivity, changes in tooth color/translucency, chipped or fractured teeth, enlarged salivary glands, dry mouth, and chronic sore throat.
- Restoration Costs: Dental treatments for erosion can range from $150-$500 per tooth for bonding, $800-$2,500 per tooth for veneers, and $800-$3,000 per tooth for crowns, depending on severity and location. Full-mouth reconstruction can easily exceed $15,000-$50,000.
- Prevention is Key: Early intervention for bulimia is paramount. Dentally, focus on reducing acid exposure, meticulous oral hygiene, daily fluoride use, and regular dental check-ups.
- Remineralization: While you can't truly "increase calcium in teeth" that's been lost, topical fluoride and calcium-phosphate products can help remineralize weakened enamel, strengthening existing tooth structure.
- Insurance Coverage: Many restorative treatments are partially covered by dental insurance (typically 50-80% for major procedures), but cosmetic procedures like veneers may have limited coverage.
- Multidisciplinary Approach: Effective management of bulimia-related dental issues requires collaboration between dentists, medical doctors, and mental health professionals.
Understanding Bulimia Nervosa and Its Dental Impact
Bulimia Nervosa (BN) is a serious and potentially life-threatening eating disorder. Individuals with BN engage in cycles of binge eating—consuming an unusually large amount of food in a short period—followed by compensatory behaviors to prevent weight gain. These behaviors can include self-induced vomiting, misuse of laxatives, diuretics, enemas, fasting, or excessive exercise. The recurrent exposure of teeth to gastric acid, coupled with other associated habits, creates a unique and devastating pattern of bulimia teeth damage.
What It Is: The Oral Manifestations of Bulimia
The most defining characteristic of bulimia's impact on dental health is perimylolysis, which is the erosion of tooth enamel and dentin due caused by exposure to stomach acids. When an individual vomits frequently, the highly acidic gastric contents (pH of 1.0-2.0) wash over the teeth, particularly the lingual (tongue-facing) and palatal (roof of the mouth-facing) surfaces of the upper front teeth and the chewing surfaces of the back teeth. This acid gradually dissolves the hard mineral structure of the tooth, leading to irreversible loss of tooth tissue.
Beyond acid erosion, bulimia contributes to a cascade of other oral health issues:
- Xerostomia (Dry Mouth): Dehydration from vomiting and diuretic abuse, as well as the use of certain medications (e.g., antidepressants, anxiety medications) often prescribed for bulimia, can severely reduce saliva flow. Saliva is crucial for neutralizing acids, washing away food particles, and remineralizing enamel. Its absence exacerbates dental decay and gum problems.
- Enlarged Salivary Glands: The parotid glands, located near the ears, can become noticeably swollen and tender due to repeated stimulation from vomiting. This is sometimes referred to as "chipmunk cheeks."
- Oral Trauma: Repeated insertion of fingers or objects into the mouth to induce vomiting can cause lacerations, sores, or calluses (known as Russell's sign) on the knuckles and fingers. This can also lead to trauma to the soft tissues of the mouth, including the palate and pharynx.
- Increased Risk of Cavities: While acid erosion is distinct from cavities caused by bacteria, the combination of enamel weakening, dry mouth, and potential sugary food binges makes individuals with bulimia highly susceptible to conventional tooth decay.
- Gum Disease: Dry mouth, poor nutrition, and compromised immune function can contribute to gingivitis (gum inflammation) and periodontitis (more severe gum disease leading to bone loss).
Types of Damage: Variations in Oral Impact
While self-induced vomiting is the primary driver of most bulimia teeth damage, other compensatory behaviors can also contribute:
- Laxative and Diuretic Abuse: These can lead to severe dehydration and electrolyte imbalances, contributing to xerostomia and overall systemic health issues that indirectly affect oral health.
- Excessive Brushing: Some individuals, concerned about the acidity, may immediately brush their teeth after vomiting. Brushing immediately after acid exposure can further abrade softened enamel, worsening erosion. It's recommended to wait at least 30-60 minutes and rinse with water or fluoride mouthwash instead.
- Dietary Habits: During binge episodes, individuals may consume highly acidic or sugary foods and drinks, which, when combined with reduced salivary flow and acid exposure, can accelerate enamel damage and cavity formation.
Why It Happens: The Root Causes
While understanding the dental impact is crucial, it's important to briefly acknowledge the underlying causes of bulimia nervosa. Bulimia is a complex mental health disorder influenced by a combination of genetic, biological, psychological, and social factors. These can include:
- Genetics: A family history of eating disorders or other mental health conditions.
- Psychological Factors: Low self-esteem, body image dissatisfaction, perfectionism, impulsivity, anxiety, depression, and trauma.
- Social and Cultural Pressures: Societal emphasis on thinness and certain body ideals.
- Brain Chemistry: Imbalances in brain chemicals, such as serotonin, can play a role.
Addressing these root causes through mental health treatment is fundamental to halting the progression of both the eating disorder and its associated dental damage.
Signs and Symptoms of Bulimia Teeth Damage
Recognizing the signs of bulimia-related dental damage early is crucial for effective intervention and to prevent further, more extensive, and costly harm. Many individuals may not immediately connect these oral symptoms to an eating disorder, highlighting the importance of dentists in identification.
What to Look For: Oral Indicators
-
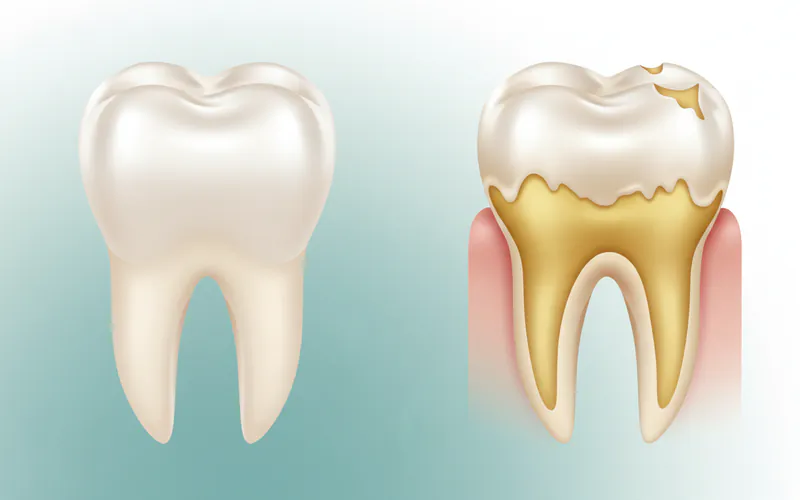
Dental Erosion (Perimylolysis):
- Appearance: Teeth may appear smooth, shiny, and translucent, especially on the biting surfaces and the inside surfaces of the upper front teeth. Over time, teeth can become shorter, rounded, or develop distinct "cupping" on the biting surfaces where the enamel has worn away, exposing the softer dentin underneath.
- Color Changes: As enamel thins and dentin is exposed, teeth may appear more yellow.
- Sensitivity: Increased sensitivity to hot, cold, sweet, or acidic foods and drinks due to exposed dentin.
- Changes in Bite: Significant tooth loss can alter the way upper and lower teeth meet.
- Chipping/Fracturing: Eroded teeth become weaker and more brittle, making them prone to chipping or fracturing, especially at the edges.
-
Enlarged Salivary Glands:
- Appearance: Swelling in the cheeks or jaw area, particularly around the ears, due to enlarged parotid glands. This can give the face a puffy, "chipmunk-like" appearance.
- Sensation: The swollen glands may be tender or painful.
-
Xerostomia (Dry Mouth):
- Sensation: Persistent feeling of dryness in the mouth, difficulty speaking, chewing, or swallowing.
- Appearance: Lips may appear dry or cracked, and the tongue may look red and fissured.
- Halitosis: Bad breath, often a consequence of reduced saliva flow and increased bacterial activity.
-
Oral Lesions and Trauma:
- Russell's Sign: Calluses, abrasions, or sores on the knuckles or backs of the fingers from repeated friction against the teeth during self-induced vomiting.
- Palatal Lacerations: Red marks, scratches, or small tears on the soft palate (roof of the mouth) or back of the throat.
- Petechiae: Small, pinpoint red or purple spots on the soft palate, caused by broken capillaries from the pressure of vomiting.
-
Gum Inflammation and Bleeding:
- Appearance: Red, swollen, or tender gums that bleed easily during brushing or flossing.
- Cause: Often exacerbated by dry mouth, poor oral hygiene, and nutritional deficiencies.
-
Increased Cavity Rate:
- Appearance: New or recurrent cavities, especially at the gumline or on surfaces previously considered less susceptible.
- Cause: Compromised enamel, reduced saliva, and acidic environment create a perfect storm for bacterial decay.
General Systemic Signs of Bulimia
While dentists focus on oral signs, understanding the broader picture is vital for comprehensive care and referral:
- Fluctuations in Weight: While often within a normal range, weight may fluctuate due to binge-purge cycles.
- Electrolyte Imbalance: Can lead to fatigue, muscle weakness, heart irregularities, and even life-threatening cardiac arrest.
- Gastrointestinal Issues: Chronic sore throat, acid reflux, stomach pain, constipation from laxative abuse.
- Menstrual Irregularities: Missed or irregular periods in females.
- Psychological Symptoms: Depression, anxiety, irritability, social withdrawal, preoccupation with body weight and shape.
Dental Treatment Options for Bulimia Teeth Damage
Addressing bulimia teeth damage requires a two-pronged approach: first, stopping the damaging behaviors through mental health intervention, and second, repairing the existing dental damage. Dental treatments aim to restore function, aesthetics, and prevent further deterioration.
A. Initial Assessment and Stabilization
- Comprehensive Dental Examination: Your dentist will perform a thorough examination, including X-rays, to assess the extent of erosion, cavities, and gum health. They will also look for characteristic signs like salivary gland swelling or Russell's sign.
- Oral Hygiene Instruction: Personalized guidance on gentle brushing techniques, recommended toothbrushes (soft-bristled), and non-abrasive toothpaste. Crucially, advise against brushing immediately after vomiting.
- Fluoride Therapy:
- At-home: Prescription-strength fluoride toothpaste (e.g., 5000 ppm fluoride) or daily fluoride mouthwashes.
- In-office: Professional fluoride varnish or gel applications. Fluoride helps remineralize weakened enamel, making it more resistant to acid attacks.
- Cost: At-home prescription fluoride toothpaste: $15-$30 per tube. In-office fluoride treatment: $30-$75 per application, often covered by insurance for high-risk patients.
- Saliva Stimulation/Dry Mouth Management:
- Over-the-counter products: Artificial saliva sprays, gels, or lozenges.
- Prescription medications: Pilocarpine or cevimeline to stimulate saliva flow (if salivary glands are functional).
- Lifestyle changes: Frequent sips of water, chewing sugar-free gum with xylitol.
- Cost: OTC products: $5-$25 per item. Prescription medications: $50-$150 per month, varies by insurance.
- Referral for Mental Health Treatment: This is the most critical step. Dentists play a vital role in identifying potential eating disorders and referring patients to a multidisciplinary team including medical doctors, psychologists, psychiatrists, and dietitians. No amount of dental work will be permanent without addressing the underlying disorder.
B. Restorative Dental Treatments
Once the damaging behaviors are under control and the oral environment is stabilized, restorative procedures can begin. The choice of treatment depends on the severity of the erosion and the affected teeth.
-
Dental Bonding (Composite Resin):
- Description: A tooth-colored resin material is applied to the tooth surface, sculpted to shape, and hardened with a special light. Ideal for minor to moderate erosion and repairing small chips.
- Pros: Least invasive, most affordable, completed in one visit.
- Cons: Less durable and more prone to staining than other options, may need replacement every 5-10 years.
- Cost: $150-$500 per tooth, depending on the extent of damage and tooth location.
-
Veneers (Porcelain or Composite):
- Description: Thin, custom-made shells that cover the front surface of the teeth. Porcelain veneers are highly aesthetic and durable; composite veneers are more affordable.
- Pros: Excellent aesthetics, good durability (especially porcelain), can correct shape, color, and minor alignment issues.
- Cons: Irreversible (porcelain requires enamel removal), higher cost than bonding, porcelain requires multiple appointments.
- Cost: $800-$2,500 per tooth for porcelain veneers, $250-$1,000 per tooth for composite veneers.
-
Dental Crowns (Caps):
- Description: A tooth-shaped cap placed over the entire tooth to restore its shape, size, strength, and appearance. Used for severely eroded, fractured, or weakened teeth.
- Pros: Highly durable, provides full coverage and protection, restores function effectively.
- Cons: Requires significant removal of tooth structure, higher cost, multiple appointments.
- Cost: $800-$3,000 per tooth, depending on material (porcelain, ceramic, metal-ceramic, gold) and complexity.
-
Inlays and Onlays (Partial Crowns):
- Description: Lab-fabricated restorations used when the damage is too extensive for a filling but not severe enough for a full crown. Inlays fit within the cusps (points) of the chewing surface, while onlays cover one or more cusps.
- Pros: Conserves more natural tooth structure than a full crown, durable.
- Cons: More expensive than fillings, requires two appointments.
- Cost: $600-$1,500 per tooth.
-
Full-Mouth Reconstruction:
- Description: For severe cases of widespread erosion, multiple teeth may need extensive restorative work, combining crowns, veneers, and possibly root canal therapy or dental implants. This is a complex, multi-stage process involving specialized prosthodontic planning.
- Pros: Restores full oral function, aesthetics, and long-term stability.
- Cons: Very extensive, time-consuming, and highly expensive.
- Cost: Can range from $15,000 to over $50,000, depending on the number of teeth involved and the specific procedures.
C. Addressing Related Issues
- Gum Disease Treatment: Scaling and root planing (deep cleaning) for gingivitis or periodontitis, guided by a periodontist if severe.
- Cavity Fillings: Standard dental fillings for new or existing cavities.
- Root Canal Therapy: If erosion or fracture has led to nerve damage or infection within a tooth.
Step-by-Step Process for Dental Restoration
The journey to restore teeth damaged by bulimia typically involves several steps, emphasizing a holistic and patient-centered approach.
-
Initial Consultation and Comprehensive Exam (1-2 visits):
- Assessment: Your dentist will conduct a thorough examination, including a detailed medical and dental history, oral cancer screening, periodontal (gum) assessment, bite analysis, and often photographs and X-rays. They will carefully assess the extent of erosion, identify sensitive areas, and check for any signs of salivary gland swelling or soft tissue trauma.
- Discussion: This is where the dentist will discuss their findings, explain the potential link to an eating disorder (if not already disclosed), and emphasize the importance of addressing the underlying bulimia.
- Mental Health Referral: If an eating disorder is suspected or confirmed, the dentist will strongly recommend or facilitate a referral to a medical doctor and mental health professional for parallel treatment.
-
Stabilization and Preventive Phase (Ongoing):
- Oral Hygiene Education: Detailed instructions on how to brush gently, floss effectively, and use recommended products. Emphasis on not brushing immediately after vomiting (wait 30-60 minutes).
- Fluoride and Remineralization Therapy: Prescription fluoride toothpaste, mouth rinses, and in-office fluoride applications will be initiated to strengthen enamel and reduce sensitivity.
- Saliva Management: Recommendations for artificial saliva products or prescription medications to combat dry mouth.
- Addressing Acute Issues: Any active infections, severe pain, or immediate concerns (e.g., fractured tooth causing sharp edges) will be handled first.
-
Treatment Planning (1-2 visits):
- Customized Plan: Based on the severity of damage and the patient's individual needs and budget, the dentist will develop a comprehensive treatment plan. This might involve a combination of bonding, veneers, crowns, or other procedures.
- Discussion: The dentist will explain each recommended procedure, its pros and cons, expected outcomes, timeline, and associated costs. They may use diagnostic wax-ups or digital smile design to show potential aesthetic improvements.
- Prioritization: Treatment is often phased, prioritizing urgent needs, followed by functional restoration, and then aesthetic improvements.
-
Restorative Procedures (Multiple Visits, varies based on complexity):
- Preparation: Depending on the chosen restoration (e.g., veneers, crowns), teeth will be carefully prepared. This may involve removing a small amount of enamel for veneers or shaping the tooth for a crown.
- Impressions/Scans: Digital or traditional impressions are taken to create custom-fit restorations.
- Temporary Restorations: If applicable, temporary crowns or veneers will be placed while permanent ones are being fabricated in a dental lab.
- Placement of Permanent Restorations: Once the custom restorations arrive from the lab, they are carefully fitted, adjusted, and permanently bonded or cemented to the teeth.
- Direct Restorations: For bonding or direct composite veneers, the material is applied, sculpted, and hardened in a single visit.
-
Recovery and Aftercare (Ongoing):
- Post-Procedure Instructions: Guidance on caring for new restorations, managing sensitivity, and maintaining oral hygiene.
- Regular Follow-ups: Scheduled appointments to monitor the health of the teeth and restorations, provide ongoing preventive care, and address any new concerns. This includes continued fluoride application and dry mouth management.
Pro Tip: Consistency with mental health treatment is paramount. Dental restorations are only as durable as the oral environment allows. If purging behaviors continue, new damage will occur, potentially undoing expensive and time-consuming dental work.
Cost and Insurance for Bulimia Teeth Damage Treatment
The cost of treating bulimia teeth damage can be substantial, varying widely based on the extent of the damage, the types of restorations needed, the materials used, and the geographic location of the dental practice in the US.
Average US Costs for Common Treatments
| Treatment Type | Average Cost Range (Per Tooth) | Notes |
|---|---|---|
| Dental Bonding (Composite) | $150 - $500 | For minor erosion, chips. Least expensive. |
| Composite Veneer | $250 - $1,000 | Direct application, less durable than porcelain. |
| Porcelain Veneer | $800 - $2,500 | Highly aesthetic, durable. Requires lab work. |
| Dental Crown | $800 - $3,000 | Covers entire tooth. Price varies by material (porcelain, Zirconia, gold, PFM). |
| Inlay/Onlay | $600 - $1,500 | Partial crown. Lab-fabricated. |
| Prescription Fluoride (at home) | $15 - $30 | Per tube/bottle. |
| In-Office Fluoride Treatment | $30 - $75 | Per application. |
| Fillings (Amalgam/Composite) | $100 - $400 | For cavities caused or exacerbated by bulimia. |
| Full-Mouth Reconstruction | $15,000 - $50,000+ | For severe, widespread damage. Highly variable. |
Cost Variation Factors:
- Geographic Location: Major metropolitan areas (e.g., New York, Los Angeles) typically have higher dental costs than rural areas.
- Dentist's Experience/Specialty: Specialists (prosthodontists) may charge more for complex reconstructions.
- Materials Used: Zirconia or Emax porcelain crowns are more expensive than traditional porcelain-fused-to-metal (PFM) or metal crowns.
- Extent of Damage: More teeth involved and greater tissue loss will increase the overall cost.
Insurance Coverage Details
Dental insurance coverage for bulimia-related damage can be complex:
- Preventive/Basic Care: Routine exams, cleanings, and fluoride treatments are generally well-covered (often 80-100%).
- Major Restorative Care: Procedures like crowns, inlays/onlays, and fillings are usually covered at a lower percentage (typically 50-80%). Many plans have annual maximums ($1,000-$2,000 per year) which can quickly be met with extensive restorative work.
- Cosmetic Procedures: Veneers, especially when primarily for aesthetic reasons, may have limited or no insurance coverage. If the veneer is deemed medically necessary to restore tooth function due to severe erosion, some coverage may apply, but this requires thorough documentation from your dentist.
- Pre-Authorizations: For expensive treatments like crowns or full-mouth reconstruction, your dentist will likely submit a pre-authorization to your insurance company to determine the exact coverage and your out-of-pocket costs before treatment begins.
- Medical vs. Dental Insurance: In some rare and severe cases, if the dental damage is directly linked to a diagnosed medical condition (like an eating disorder), parts of the treatment might be covered under medical insurance, especially for procedures like parotid gland swelling reduction or surgical interventions. This is highly specific and requires detailed communication between your medical doctor, dentist, and insurance provider.
Payment Plans and Financing Options
Many dental offices offer or partner with financing options to help manage significant treatment costs:
- In-Office Payment Plans: Some practices allow you to pay in installments.
- Third-Party Financing: Companies like CareCredit or LendingClub provide low- or no-interest payment plans for healthcare expenses, if paid within a specified promotional period (e.g., 6, 12, or 18 months).
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): These tax-advantaged accounts allow you to set aside pre-tax money for eligible healthcare expenses, including most dental treatments.
Pro Tip: Always discuss financial options with your dentist's office manager before starting extensive treatment. Understanding your insurance benefits and exploring payment plans can significantly alleviate the financial burden.
Recovery and Aftercare
Successful dental restoration for bulimia teeth damage is only part of the solution; diligent recovery and aftercare are essential for the longevity of your dental work and to prevent future problems.
Post-Treatment Care Instructions
- Maintain Excellent Oral Hygiene:
- Gentle Brushing: Use a soft-bristled toothbrush and a low-abrasive, fluoride toothpaste. Brush gently twice a day for two minutes.
- Flossing: Floss daily to remove plaque and food debris from between teeth and around restorations.
- Special Cleaning: If you have extensive restorations, your dentist may recommend specific interdental brushes or water flossers.
- Continue Fluoride Regimen: Your dentist will likely prescribe or recommend daily use of a high-fluoride toothpaste or mouthwash to continue strengthening enamel and protecting against acid attacks.
- Manage Dry Mouth:
- Stay Hydrated: Drink plenty of water throughout the day.
- Sugar-Free Products: Chew sugar-free gum with xylitol or suck on sugar-free lozenges to stimulate saliva.
- Saliva Substitutes: Use over-the-counter or prescription artificial saliva products as needed.
- Avoid Immediate Brushing After Vomiting: This is critical. If purging occurs, rinse your mouth thoroughly with plain water or a fluoride mouthwash (ideally one containing baking soda to neutralize acid) and wait at least 30-60 minutes before brushing.
- Dietary Modifications:
- Limit Acidic Foods/Drinks: Reduce consumption of sodas, fruit juices, sports drinks, and highly acidic foods (e.g., citrus fruits, vinegar). If consumed, do so quickly and rinse with water afterward.
- Avoid Sticky/Sugary Snacks: These contribute to cavity formation, especially in a compromised oral environment.
- Hard/Crunchy Foods: Be cautious with extremely hard or crunchy foods that could chip or damage new restorations, especially veneers or bonding.
- Regular Dental Check-ups: Schedule routine check-ups and professional cleanings every 3-6 months, or as recommended by your dentist. These visits allow your dentist to monitor your oral health, check the integrity of restorations, and provide preventive care.
- Address Grinding/Clenching: If you grind or clench your teeth (bruxism), often exacerbated by stress, your dentist may recommend a nightguard to protect your teeth and restorations from excessive force.
- Commitment to Mental Health Treatment: This is non-negotiable. Ongoing therapy, medication, and support group participation are essential to prevent relapse of bulimic behaviors, which would otherwise undermine all dental efforts.
Prevention of Bulimia Teeth Damage
Preventing bulimia teeth damage primarily involves preventing or stopping the eating disorder itself. However, for individuals who are struggling or in recovery, there are crucial dental strategies to minimize harm.
Primary Prevention: Addressing Bulimia Itself
- Early Intervention: Recognizing the signs of an eating disorder and seeking professional help immediately is the most effective prevention. This involves a multidisciplinary team: medical doctor, mental health professional (psychologist, psychiatrist), and dietitian.
- Mental Health Awareness: Promoting positive body image, self-esteem, and healthy coping mechanisms can reduce the risk of developing eating disorders.
- Education: Informing individuals, especially adolescents, about the severe health consequences of eating disorders, including dental damage.
Secondary Prevention: Minimizing Damage
For individuals with ongoing bulimia or those in early recovery, these dental strategies are vital:
- Avoid Brushing Immediately After Vomiting: As emphasized, this is paramount. Gastric acid softens enamel, and brushing immediately abrades it further.
- Rinse Immediately and Thoroughly: After purging, rinse your mouth vigorously with:
- Plain Water: The simplest and most immediate step.
- Fluoride Mouthwash: Helps remineralize enamel and reduce acid effects.
- Baking Soda Rinse: Mix a teaspoon of baking soda in a glass of water. Baking soda is alkaline and effectively neutralizes stomach acid.
- Daily Fluoride Use:
- Prescription Toothpaste: Your dentist may prescribe a high-fluoride toothpaste for daily use.
- Fluoride Mouthwash: Use an over-the-counter fluoride rinse daily.
- Manage Dry Mouth: Follow the strategies outlined in the "Recovery and Aftercare" section to maintain adequate saliva flow.
- Neutralize Acidic Foods/Drinks:
- Limit frequency.
- Use a straw for acidic beverages to minimize contact with teeth.
- Rinse with water after consuming acidic items.
- Regular Dental Check-ups (Every 3-4 months): More frequent visits allow your dentist to monitor for new damage, apply professional fluoride treatments, and provide necessary interventions early.
- Dental Sealants: For children and adolescents at high risk, sealants can be applied to the chewing surfaces of molars to protect them from decay and erosion.
- Protective Splints/Mouthguards: In some cases, a custom-fitted mouthguard can be worn overnight or during periods of high risk to provide a physical barrier against acid, though this isn't a primary solution.
Pro Tip: Creating a "rescue kit" with a small bottle of water, a fluoride mouthwash, or baking soda for immediate rinsing after purging can be a practical step towards harm reduction.
Risks and Complications of Untreated Bulimia Teeth Damage
Ignoring the dental consequences of bulimia can lead to a cascade of worsening problems, impacting not only oral health but overall well-being.
Progressive Dental Deterioration
- Severe Enamel and Dentin Loss: Continued acid exposure will lead to irreversible loss of tooth structure, making teeth shorter, weaker, and more prone to chipping and fracture.
- Pulp Exposure and Infection: As erosion progresses, the protective layers of enamel and dentin can wear away, exposing the sensitive dental pulp (nerve and blood vessels) inside the tooth. This can lead to severe pain, infection, and necessitate root canal treatment or even tooth extraction.
- Tooth Loss: In advanced stages, teeth may become so severely damaged they cannot be restored and must be extracted, leading to gaps in the smile and further complications like bone loss.
- Occlusal Collapse: Widespread tooth wear can alter the bite, leading to problems with the temporomandibular joint (TMJ), muscle pain, and difficulty chewing.
- Increased Risk of Cavities and Gum Disease: The compromised oral environment makes teeth highly vulnerable to bacterial decay and advanced gum disease (periodontitis), leading to further tooth loss.
Systemic Health Complications Exacerbated by Poor Oral Health
- Nutritional Deficiencies: Severely damaged or missing teeth impair the ability to chew properly, potentially worsening nutritional deficiencies already common in bulimia.
- Oral Pain and Discomfort: Chronic sensitivity, jaw pain, and gum inflammation can significantly reduce quality of life and make eating, speaking, and even sleeping uncomfortable.
- Impact on Self-Esteem and Mental Health: Visible dental damage can be a source of shame and embarrassment, further exacerbating psychological distress and social anxiety associated with bulimia. This can create a vicious cycle where a damaged smile reinforces negative self-perception, hindering recovery.
- Increased Susceptibility to Other Health Issues: Poor oral health has been linked to systemic inflammation and an increased risk of cardiovascular disease, diabetes complications, and respiratory infections.
- Economic Burden: Delaying treatment leads to more extensive and expensive procedures, such as full-mouth reconstruction or dental implants, costing tens of thousands of dollars.
Comparison of Damage Progression and Treatment Levels
| Stage of Damage | Characteristics | Typical Dental Findings | Recommended Treatment Levels | Estimated Cost (US, without insurance) |
|---|---|---|---|---|
| Early/Mild Erosion | Increased sensitivity, slight translucency, minor chips. | Visible enamel erosion (e.g., palatal surfaces), no dentin exposure. | Preventive care (fluoride, rinses), small bonding. | $50 - $500 |
| Moderate Erosion | Persistent sensitivity, yellowing, visible cupping. | Dentin exposure, noticeable wear on chewing surfaces, some small fractures. | Bonding, composite veneers, possibly some inlays/onlays. | $500 - $3,000 per tooth |
| Severe Erosion | Severe sensitivity, extreme wear, short teeth, multiple fractures. | Extensive dentin exposure, pulp involvement possible, bite collapse. | Crowns, porcelain veneers, root canals, full-mouth reconstruction. | $3,000 - $10,000+ per tooth or $15,000 - $50,000+ for full mouth |
Children / Pediatric Considerations
Bulimia nervosa can affect adolescents and even younger children, though it's more prevalent in older teens and young adults. Bulimia teeth damage in younger patients presents unique challenges due to developing dentition and differing psychological factors.
Age-Specific Guidance for Parents
- Early Recognition is Crucial: Parents should be acutely aware of general bulimia signs (preoccupation with weight, secretive eating, frequent bathroom visits after meals, unusual food disappearances, changes in mood or social behavior). Oral signs like unexplained tooth sensitivity, translucent tooth edges, or frequent mouth sores should prompt immediate dental and medical evaluation.
- Developing Permanent Teeth: Erosion in adolescents can affect newly erupted permanent teeth, which have thinner enamel initially, making them more vulnerable to rapid and severe damage. Early damage can impact the long-term health and aesthetics of these teeth throughout adulthood.
- Orthodontic Treatment Challenges: If a child or teen is undergoing orthodontic treatment (braces), the brackets and wires can trap acids, potentially leading to more localized erosion around the appliances. The treatment itself may be complicated if severe tooth damage is present.
- Behavioral Considerations: Discussing an eating disorder with a child or teen requires extreme sensitivity. The dentist should communicate findings to the parents, who can then work with medical and mental health professionals. Direct confrontation in the dental chair can be counterproductive.
- Parental Involvement in Aftercare: Parents play a critical role in supervising oral hygiene, ensuring adherence to fluoride regimens, monitoring dietary habits, and ensuring consistent attendance at both dental and mental health appointments.
- Protective Measures: For high-risk adolescents, dental sealants on molars and fluoride varnish applications can provide an extra layer of protection against decay and erosion. Custom-made mouthguards might be considered as a temporary protective barrier if purging is ongoing and professional help is being sought.
- Long-Term Impact: Dental damage sustained during adolescence can have profound and lasting effects on a child's confidence, social interactions, and overall health into adulthood, often requiring extensive and costly restorative work later in life.
Pro Tip: If you suspect your child has an eating disorder, seek help from their pediatrician immediately. The pediatrician can then coordinate referrals to a mental health specialist and a dentist experienced in pediatric oral health issues.
Frequently Asked Questions
What are the earliest signs of bulimia teeth damage?
The earliest signs often include increased tooth sensitivity to hot, cold, or sweet foods, a slight yellowing or translucency of the tooth edges, and subtle changes in the shape or texture of the inside surfaces of the upper front teeth. Some individuals might also notice frequent canker sores or a persistent sore throat.
Can teeth recover from bulimia damage naturally?
No, once enamel is lost due to acid erosion, it cannot naturally regenerate. The damage is irreversible. However, the remaining enamel can be strengthened and made more resistant to further acid attacks through remineralization strategies like fluoride therapy, which helps incorporate minerals back into the weakened tooth structure.
How do I increase calcium in teeth if I have bulimia?
You cannot directly "increase calcium" in the form of regrowing lost enamel. However, you can strengthen the existing tooth structure by using fluoride products (prescription-strength toothpaste, mouthwashes, professional varnishes) and certain calcium-phosphate containing products. These help to remineralize weakened enamel, making it more robust against acid, reducing sensitivity, and preventing further demineralization.
What causes calcium build up on teeth, and is it related to bulimia?
"Calcium build-up" on teeth typically refers to dental calculus or tartar, which forms when plaque calcifies due to minerals in saliva. This is primarily a hygiene issue, not directly caused by bulimia. In fact, bulimia causes loss of tooth minerals (erosion). While an individual with bulimia can still develop calculus if oral hygiene is poor, it's distinct from the primary acid erosion damage.
How long does it take for bulimia to damage teeth?
Significant damage can occur relatively quickly, often within a year or two of frequent purging. However, the severity and speed of damage depend on the frequency, duration, and method of purging, as well as individual factors like saliva quality and existing dental health.
Is dental treatment for bulimia teeth damage painful?
Most restorative dental treatments are performed under local anesthesia, so you should not feel pain during the procedure. You might experience some sensitivity or discomfort after the anesthesia wears off, which can usually be managed with over-the-counter pain relievers. Root canals or extractions might have more post-operative discomfort.
How much does full-mouth reconstruction for bulimia cost?
Full-mouth reconstruction is extensive and highly variable, typically ranging from $15,000 to over $50,000 without insurance. The exact cost depends on the number of teeth involved, the specific restorative procedures (crowns, veneers, implants, root canals), materials chosen, and the complexity of the case.
Does dental insurance cover treatments for bulimia teeth damage?
Dental insurance typically covers a portion of preventive care (cleanings, fluoride) and major restorative procedures (crowns, fillings, inlays/onlays), often 50-80%, up to an annual maximum (usually $1,000-$2,000). Cosmetic procedures like veneers may have limited or no coverage unless deemed medically necessary to restore function due to severe erosion.
What are the alternatives to full-mouth reconstruction for severe damage?
If full-mouth reconstruction is not feasible, alternatives might include treating only the most symptomatic teeth, using more affordable materials like composite bonding instead of porcelain crowns/veneers, or in severe cases, tooth extraction followed by partial dentures or dental implants for missing teeth, though these are typically less ideal.
Can a dentist tell if I've been vomiting?
Yes, dentists are often the first healthcare professionals to notice the tell-tale signs of frequent vomiting, such as acid erosion on specific tooth surfaces (especially the back of the upper front teeth), enlarged salivary glands, dry mouth, and oral lesions. They are trained to recognize these patterns and may gently inquire about eating habits or refer you for further evaluation.
When to See a Dentist
Given the irreversible nature of bulimia teeth damage, timely dental intervention is critical.
Clear Warning Signs for Immediate Attention
- Sudden Increase in Tooth Sensitivity: Especially to hot, cold, or sweet stimuli, indicating enamel loss.
- Visible Changes in Tooth Appearance: Teeth appearing more yellow, translucent, rounded, or shorter. Noticing chips or fractures in previously healthy teeth.
- Persistent Dry Mouth: A chronic feeling of oral dryness not relieved by drinking water.
- Chronic Sore Throat or Hoarseness: Could indicate acid reflux from purging.
- Swollen Glands: Noticeable swelling in the jaw or cheek area, particularly near the ears.
- Any Oral Pain or Discomfort: Including toothaches, gum soreness, or persistent sores in the mouth.
- Difficulty Chewing or Changes in Bite: Indicating significant tooth wear or loss.
Red Flags vs. Routine Care Guidance
- Red Flags (Schedule an appointment ASAP): Any of the "Immediate Attention" signs, especially if they are new, worsening, or associated with general health concerns. If you know you are struggling with bulimia, even without dental symptoms, a dental check-up is crucial for preventive care and early detection.
- Routine Care Guidance: Even in the absence of obvious symptoms, individuals with a history of bulimia or those in recovery should maintain more frequent dental check-ups (every 3-4 months instead of 6). These regular visits allow your dentist to monitor your oral health, provide proactive fluoride treatments, and intervene at the earliest signs of new damage.
Emergency vs. Scheduled Appointment Guidance
- Emergency (Seek immediate dental care):
- Severe, unrelenting tooth pain that wakes you up at night or is not relieved by over-the-counter pain medication.
- A knocked-out or severely fractured tooth that causes sharp pain or bleeding.
- Swelling in the face or jaw accompanied by fever, which could indicate a severe infection.
- Uncontrolled bleeding from the mouth.
- Scheduled Appointment (Book as soon as possible, but not emergency):
- Increased tooth sensitivity.
- Visible changes in tooth shape or color.
- Persistent dry mouth.
- Signs of gum inflammation.
- Concerns about your chewing ability or bite.
Remember, your dental team is there to help, not to judge. Open communication with your dentist is the first step toward preserving your oral health and supporting your overall recovery journey from bulimia.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
What Are Calcium Deposits on Teeth
Are you one of the millions of Americans who notices a stubborn, yellowish buildup on your teeth despite regular brushing? You're likely experiencing what many refer to as "calcium deposits on teeth." This common dental concern, medically known as dental calculus or tartar, affects a vast ma
February 23, 2026
Calcium Good for Teeth: Complete Guide
More than 99% of your body's calcium resides in your bones and teeth, making it an undeniable cornerstone of skeletal and oral health. But did you know that an estimated 42% of American adults don't get enough calcium from their diet? This staggering statistic underscores a critical question
February 23, 2026
What Do Bulimia Teeth Look Like
"Bulimia teeth" refers to the specific and often severe damage that the self-induced vomiting characteristic of bulimia nervosa inflicts on a person's oral health. It's a critical issue, affecting approximately 1.5% of women and 0.5% of men in the US at some point in their lives, with many more
February 23, 2026

Erosion in Teeth: Complete Guide
Erosion in Teeth: Complete Guide
February 23, 2026