Erosion on Teeth: Complete Guide
Key Takeaways
- Have you ever noticed your teeth looking a little duller, more translucent, or even feeling sensitive to cold or sweet foods? You might be experiencing erosion on teeth, a common yet often overlooked dental problem that can severely impact your oral health and overall well-being. According to th
Erosion on Teeth: Complete Guide
Have you ever noticed your teeth looking a little duller, more translucent, or even feeling sensitive to cold or sweet foods? You might be experiencing erosion on teeth, a common yet often overlooked dental problem that can severely impact your oral health and overall well-being. According to the American Dental Association (ADA), dental erosion is a growing concern, affecting a significant portion of the adult population in the United States. This condition, characterized by the irreversible loss of tooth structure due to chemical dissolution by acids, not bacteria, can weaken your teeth, make them more susceptible to decay, and even lead to severe pain and tooth loss if left untreated. Understanding the causes, recognizing the early signs, and knowing the effective treatment and prevention strategies are crucial steps toward protecting your smile.
This comprehensive guide from SmilePedia.net will delve deep into the world of dental erosion, exploring everything from its fundamental definition and various types to the underlying causes, including lifestyle factors and medical conditions like eating disorder teeth. We'll walk you through the tell-tale signs and symptoms, detail the array of available treatment options, break down the associated costs and insurance considerations, and empower you with essential prevention tips. By the end of this article, you'll have a complete understanding of how to safeguard your teeth against the destructive effects of acid erosion and maintain a healthy, vibrant smile for years to come.
Key Takeaways:
- Dental Erosion Defined: Irreversible loss of tooth enamel and dentin due to acid exposure, distinct from decay caused by bacteria.
- Common Causes: Frequent consumption of acidic foods/drinks (citrus, sodas, sports drinks), acid reflux (GERD), and certain medical conditions like eating disorders (bulimia nervosa).
- Early Signs: Increased tooth sensitivity, dullness, transparency at the biting edges, and eventual cupping or grooving on the tooth surface.
- Treatment Options: Range from fluoride applications and bonding to veneers, crowns, or full mouth reconstruction, depending on severity.
- Cost Range: Treatment costs vary widely, from $50 - $250 for fluoride treatments, $200 - $600 per tooth for bonding, $800 - $2,500 per tooth for veneers, and $1,000 - $3,000+ per tooth for crowns. Full mouth reconstruction can cost $15,000 - $60,000+.
- Prevention is Key: Modifying diet, improving oral hygiene techniques, managing underlying medical conditions, and regular dental check-ups are vital for preventing further erosion.
- Timelines: Initial diagnosis and minor treatment (e.g., fluoride) can be resolved in 1-2 visits. More extensive treatments like veneers or crowns may require 2-4 appointments over several weeks.
What It Is: Understanding Dental Erosion
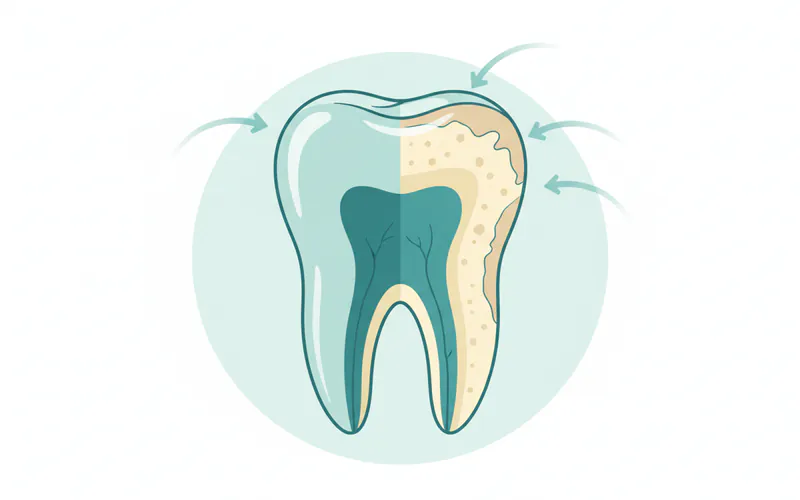
Dental erosion refers to the progressive, irreversible loss of tooth hard tissue (enamel and dentin) due to chemical processes not involving bacteria. Unlike dental caries (cavities), which are caused by acids produced by bacteria metabolizing sugars, erosion is caused by direct exposure to non-bacterial acids from various sources. These acids dissolve the mineral content of the tooth, primarily calcium and phosphate, leading to a softening and eventual wearing away of the tooth structure.
Enamel, the hardest substance in the human body, is the first line of defense. Once the enamel is worn away, the underlying dentin, which is softer and more sensitive, becomes exposed. This exposure can lead to increased tooth sensitivity, changes in tooth appearance, and a higher risk of further damage, including fractures and decay. The impact of acid erosion on teeth can range from subtle aesthetic changes to severe structural damage requiring extensive restorative work.
Types of Dental Erosion
Dental erosion is broadly categorized by the source of the acid:
Intrinsic Erosion
Intrinsic erosion occurs when acids originate from within the body. The most common cause is gastric acid, which can enter the mouth through:
- Gastroesophageal Reflux Disease (GERD): Chronic acid reflux, where stomach acid flows back into the esophagus and sometimes reaches the mouth, is a significant contributor to intrinsic erosion. People with GERD may not always experience heartburn, making the dental damage the first noticeable symptom.
- Eating Disorders: Conditions like bulimia nervosa, characterized by recurrent self-induced vomiting, expose teeth to highly corrosive stomach acid. This leads to a distinct pattern of erosion, often affecting the palatal (tongue-side) surfaces of the upper front teeth and occlusal (biting) surfaces of molars. This is why the term "eating disorder teeth" is often used to describe the specific dental manifestations of these conditions.
- Rumination: A rare disorder involving the regurgitation of undigested food from the stomach, which is then re-chewed and re-swallowed or spit out.
- Alcoholism: Chronic alcohol abuse can lead to frequent vomiting, similar to bulimia, causing significant erosion.
Extrinsic Erosion
Extrinsic erosion occurs when acids originate from outside the body. Common sources include:
- Dietary Acids: This is the most prevalent cause. Frequent consumption of highly acidic foods and beverages can erode enamel over time. Examples include:
- Soft Drinks/Sodas: Carbonated beverages, especially colas and diet sodas, are highly acidic.
- Fruit Juices: Citrus juices (orange, lemon, grapefruit) and even apple juice can be acidic.
- Sports and Energy Drinks: Many of these are laden with acids and sugars, posing a double threat.
- Acidic Foods: Citrus fruits, vinegar (found in salad dressings, pickles), sour candies, and some berries.
- Environmental/Occupational Acids: Individuals working in certain industrial settings (e.g., battery factories, electroplating plants, vineyards) may be exposed to airborne acids that can cause erosion. Swimmers in improperly chlorinated pools may also experience erosion.
- Medications: Some medications, particularly chewable vitamin C tablets and certain acid-containing asthma inhalers, can contribute to erosion.
Causes: Why Erosion on Teeth Happens
Understanding the specific causes behind erosion on teeth is crucial for both prevention and effective treatment. It's often a multifactorial problem, meaning several factors can contribute simultaneously.
Dietary Habits
The most common cause of extrinsic erosion is an acidic diet. Your saliva naturally buffers acids and helps remineralize enamel, but constant or prolonged acid exposure overwhelms this natural defense.
- Frequency of Acid Exposure: Sipping on a sugary soda or acidic juice throughout the day is far more damaging than consuming it quickly. Each exposure drops the pH level in your mouth, initiating demineralization.
- Contact Time: The longer acidic substances remain in contact with your teeth, the greater the potential for damage. Swishing acidic drinks or holding them in your mouth prolongs this contact.
- Temperature: Cold acidic drinks can be more damaging as cold liquids tend to be held in the mouth longer.
- Abrasive Habits: Brushing immediately after consuming acidic foods or drinks can exacerbate erosion. The softened enamel is more vulnerable to abrasive forces.
Medical Conditions
Several health issues can significantly contribute to dental erosion:
- GERD (Gastroesophageal Reflux Disease): Chronic reflux of stomach acid is a major intrinsic cause. The prevalence of GERD in the U.S. adult population is estimated to be between 18.1% and 27.8%, highlighting its widespread impact on dental health.
- Eating Disorders: Bulimia nervosa and anorexia nervosa (often accompanied by self-induced vomiting) are highly destructive. The frequency and duration of vomiting episodes directly correlate with the severity of eating disorder teeth manifestations.
- Hiatal Hernia: A condition where part of the stomach pushes up through the diaphragm, often leading to GERD symptoms.
- Pregnancy (Morning Sickness): Frequent vomiting during pregnancy can cause temporary, but significant, exposure to stomach acids.
- Alcoholism: As mentioned, frequent vomiting due to alcohol abuse can lead to severe erosion.
- Certain Medications: Antihistamines, aspirin, and some iron preparations can reduce salivary flow, diminishing the mouth's natural acid-buffering capacity.
Lifestyle Factors
Beyond diet and medical conditions, certain lifestyle choices play a role:
- Low Salivary Flow (Xerostomia): Saliva is vital for neutralizing acids, washing away food particles, and delivering minerals for enamel remineralization. Conditions or medications that reduce salivary flow (e.g., Sjögren's syndrome, radiation therapy, antidepressants) increase erosion risk.
- Bruxism (Teeth Grinding/Clenching): While not a direct cause of erosion, bruxism can exacerbate the problem by wearing down already softened enamel more rapidly.
- Poor Oral Hygiene (Paradoxically): While good hygiene is important, aggressive brushing or brushing immediately after acid exposure can worsen erosion.
- Excessive Mouth Breathing: Can lead to a dry mouth, reducing the protective effects of saliva.
Signs and Symptoms: What to Look For
Recognizing the early signs of acid erosion on teeth is crucial for timely intervention. Unfortunately, early erosion can be subtle and often goes unnoticed by the individual until the damage is more extensive.
Early Symptoms
- Increased Sensitivity: This is often the first noticeable sign. When enamel wears away, the underlying dentin, which contains thousands of microscopic tubules leading to the tooth's nerve, becomes exposed. This can cause sharp, fleeting pain when consuming hot, cold, sweet, or acidic foods and drinks.
- Dullness or Discoloration: Enamel is naturally translucent. As it thins, the yellowish dentin underneath becomes more visible, making the teeth appear duller or more yellow.
- Transparency at Incisal Edges: The biting edges of your front teeth may start to look translucent, almost glass-like.
Advanced Symptoms
- Cupping: Small, shallow depressions or indentations develop on the chewing surfaces of the teeth, particularly molars. These "cups" often correspond to the cusps (points) of the opposing teeth, where the enamel has been worn away and the softer dentin is exposed.
- Rounded or Worn Appearance: Teeth may lose their natural contours, appearing more rounded or smoothed out.
- Cracks and Chips: Eroded teeth become weaker and more brittle, making them prone to chipping or cracking, especially at the edges.
- Shortening of Teeth: In severe cases, significant tooth structure can be lost, leading to visibly shorter teeth.
- Restoration "Standing Proud": If you have fillings, they may appear to "stand proud" or rise above the surrounding tooth structure. This is because the tooth enamel around the filling has eroded, while the filling material (which is more acid-resistant) remains intact.
- Pain and Discomfort: As erosion progresses, sensitivity can become more constant and severe, impacting daily activities like eating and speaking.
- Dental Abscesses/Infections: If erosion progresses deep enough to expose the pulp (nerve) of the tooth, bacterial infection can occur, leading to abscesses and requiring root canal treatment.
Treatment Options for Erosion on Teeth
The approach to treating erosion on teeth depends heavily on the severity of the damage, the underlying cause, and the patient's individual needs. Treatment goals include preventing further erosion, alleviating sensitivity, restoring tooth structure, and improving aesthetics.
1. Preventive & Minimally Invasive Treatments
These are often recommended for early stages of erosion or when the primary goal is to prevent further progression.
-
Fluoride Treatments: Professional fluoride applications (varnishes, gels, foams) strengthen enamel and make it more resistant to acid attacks. Prescription fluoride toothpastes and mouth rinses may also be recommended.
- Pros: Non-invasive, affordable, helps remineralize and strengthen enamel.
- Cons: Not a restorative solution for existing structural loss, requires consistent application.
- Cost: $50 - $150 per application (often covered by insurance during routine cleanings).
-
Bonding (Composite Resins): For minor erosion or localized areas of sensitivity, a tooth-colored composite resin material can be bonded to the eroded surface.
- Pros: Esthetic, relatively conservative, can be done in one visit.
- Cons: Less durable than porcelain, can stain over time, may need replacement every 5-10 years.
- Cost: $200 - $600 per tooth, depending on size and location.
-
Sealants: Can be applied to the chewing surfaces of molars and premolars, especially in children and adolescents, to protect pits and fissures from acid attacks.
- Pros: Effective at protecting vulnerable surfaces, non-invasive.
- Cons: Limited to specific tooth surfaces, can wear off over time.
- Cost: $30 - $60 per tooth.
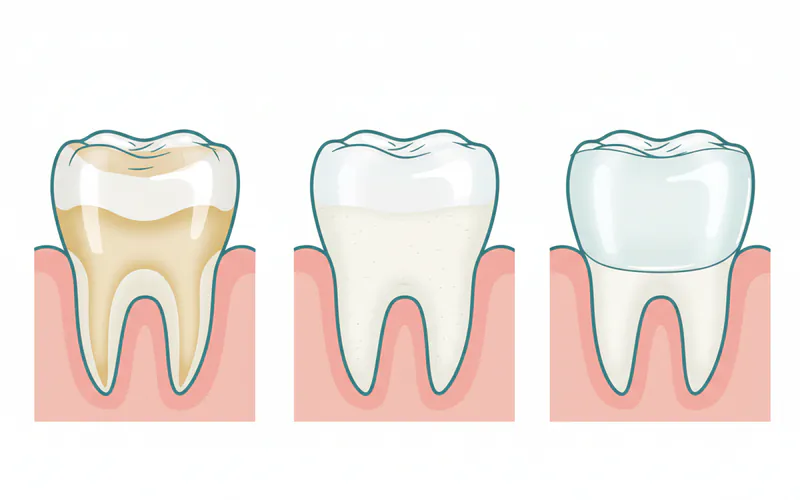
2. Restorative Treatments
For moderate to severe erosion where significant tooth structure has been lost, restorative options are necessary.
-
Dental Veneers: Thin, custom-made shells (usually porcelain or composite) that cover the front surface of teeth. They are excellent for restoring aesthetics and protecting eroded front teeth.
- Pros: Highly aesthetic, durable (porcelain veneers can last 10-15+ years), resistant to staining.
- Cons: Irreversible (requires some enamel removal), higher cost.
- Cost: $800 - $2,500 per tooth for porcelain veneers, $250 - $1,500 per tooth for composite veneers.
-
Dental Crowns: Caps that completely cover an entire tooth. Crowns are used when a tooth has lost substantial structure, is severely weakened, or requires significant aesthetic improvement.
- Pros: Provides strength and protection for severely damaged teeth, highly durable.
- Cons: More invasive (requires significant tooth reduction), higher cost, typically requires 2 visits.
- Cost: $1,000 - $3,000+ per tooth, depending on material (porcelain, ceramic, gold, PFM) and location.
-
Onlays/Inlays: Partial crowns used when the damage is too extensive for a filling but not severe enough for a full crown. Inlays fit within the cusps, while onlays cover one or more cusps.
- Pros: More conservative than crowns, durable, good fit.
- Cons: Higher cost than fillings, requires 2 visits.
- Cost: $600 - $1,500 per tooth.
-
Full Mouth Reconstruction: For cases of widespread, severe erosion affecting most or all teeth, a comprehensive treatment plan involving multiple veneers, crowns, onlays, and potentially orthodontics or gum contouring may be necessary.
- Pros: Restores complete oral health, function, and aesthetics.
- Cons: Very extensive, high cost, lengthy treatment time.
- Cost: $15,000 - $60,000+, depending on complexity and number of teeth involved.
3. Management of Underlying Causes
Crucially, treating the erosion itself without addressing the root cause will only lead to recurrence.
- Dietary Counseling: Education on acidic foods/drinks, smart consumption habits (e.g., using a straw, rinsing with water after acidic intake).
- Management of GERD: Working with a physician to control acid reflux through medication, diet, and lifestyle changes.
- Eating Disorder Treatment: This requires a multidisciplinary approach involving medical doctors, therapists, and nutritionists to address the underlying psychological and physical aspects of the disorder. Dental professionals play a supportive role in monitoring and managing oral health.
Step-by-Step Process for Treating Advanced Erosion (e.g., with Veneers or Crowns)
For significant erosion on teeth, the restorative process typically involves several stages:
Step 1: Comprehensive Examination and Diagnosis
Your dentist will conduct a thorough oral examination, take X-rays, and possibly intraoral photographs. They will assess the extent of the erosion, identify the primary causes, and discuss your symptoms and aesthetic goals. This initial appointment is crucial for developing a personalized treatment plan.
Step 2: Treatment Planning and Discussion
Based on the examination, your dentist will present a detailed treatment plan, outlining the recommended procedures (e.g., veneers, crowns, onlays), estimated costs, and expected timelines. This is your opportunity to ask questions and understand all aspects of the treatment. For complex cases, a wax-up or digital mock-up might be created to visualize the final result.
Step 3: Tooth Preparation
- Local Anesthesia: The area around the affected teeth will be numbed to ensure your comfort.
- Reshaping: A precise amount of enamel will be removed from the tooth surface to make space for the restorative material. The amount removed depends on the type of restoration (e.g., veneers require less reduction than crowns).
- Impressions: Digital scans or traditional putty impressions of your prepared teeth are taken. These impressions are sent to a dental lab, where your custom veneers, crowns, or onlays will be fabricated.
Step 4: Temporary Restorations (If Needed)
While your permanent restorations are being made (which typically takes 1-3 weeks), temporary veneers or crowns may be placed to protect the prepared teeth, maintain aesthetics, and prevent sensitivity.
Step 5: Placement of Permanent Restorations
- Removal of Temporaries: If temporaries were placed, they are carefully removed.
- Try-in: Your dentist will carefully try in the permanent restorations to check for fit, bite, and aesthetics. Any necessary adjustments will be made at this stage.
- Bonding/Cementation: Once you and your dentist are satisfied, the restorations are permanently bonded or cemented to your teeth using a strong dental adhesive.
- Final Polishing: The restorations are polished, and your bite is checked one last time to ensure proper occlusion and comfort.
Cost and Insurance: US Price Ranges
The cost of treating acid erosion on teeth in the US can vary significantly based on the severity of the erosion, the type of treatment chosen, the number of teeth involved, the materials used, the dentist's fees, and your geographic location.
Typical US Cost Ranges
| Treatment Type | Average Cost Per Tooth (Without Insurance) | Estimated Insurance Coverage |
|---|---|---|
| Fluoride Varnish | $50 - $150 | Often 80-100% (preventative) |
| Dental Bonding (Composite) | $200 - $600 | Often 50-80% |
| Dental Sealants | $30 - 60 | Often 80-100% (preventative, usually for children) |
| Composite Veneer | $250 - $1,500 | Limited, often 0-20% (cosmetic) |
| Porcelain Veneer | $800 - $2,500 | Limited, often 0-20% (cosmetic) |
| Inlay/Onlay | $600 - $1,500 | Often 50-80% |
| Dental Crown | $1,000 - $3,000+ | Often 50-80% |
| Root Canal (if needed) | $700 - $2,000+ | Often 50-80% |
| Full Mouth Reconstruction | $15,000 - $60,000+ (overall) | Varies, often 50-80% for restorative components, less for cosmetic. |
Insurance Coverage Details
Most standard dental insurance plans follow a "100-80-50" coverage model:
- 100% Coverage: Typically for preventative care, such as routine exams, cleanings, and fluoride treatments.
- 80% Coverage: Usually for basic restorative procedures like fillings (including bonding for minor erosion) and sometimes sealants.
- 50% Coverage: For major restorative procedures, which often include crowns, inlays, onlays, and sometimes root canals.
Important Considerations:
- Cosmetic vs. Restorative: Many insurance companies categorize veneers as purely cosmetic, offering little to no coverage. However, if veneers or crowns are deemed medically necessary to restore function due to severe erosion, your dentist may be able to submit a claim with a detailed explanation, which might lead to partial coverage.
- Annual Maximums: Most dental insurance plans have an annual maximum benefit, typically ranging from $1,000 to $2,000. For extensive treatments like full mouth reconstruction, you will likely exceed this maximum and incur significant out-of-pocket costs.
- Waiting Periods: Some plans have waiting periods (e.g., 6-12 months) before major restorative procedures are covered.
- Pre-authorization: For expensive treatments, your dentist may need to submit a pre-authorization request to your insurance company to determine your exact coverage and out-of-pocket expenses before beginning treatment.
Recovery and Aftercare
After receiving treatment for erosion on teeth, proper aftercare is essential to ensure the longevity of your restorations and prevent future erosion.
Immediate Aftercare (Post-Restoration)
- Sensitivity: It's normal to experience some temporary sensitivity to hot or cold after dental procedures, especially with bonding or crown preparations. This usually subsides within a few days or weeks.
- Bite Adjustment: Your bite might feel slightly different initially. If you notice any high spots or discomfort when biting, contact your dentist for an adjustment.
- Avoid Hard/Sticky Foods: For temporary restorations or immediately after permanent placement, avoid very hard, sticky, or chewy foods that could dislodge them.
Long-Term Aftercare and Prevention
The key to preventing recurrent erosion and protecting your new restorations lies in diligent oral hygiene and lifestyle modifications.
- Maintain Excellent Oral Hygiene:
- Brush twice daily with a soft-bristled toothbrush and a fluoride toothpaste.
- Floss daily.
- Consider an electric toothbrush for gentle but effective cleaning.
- Dietary Modifications:
- Reduce or eliminate acidic foods and drinks, especially sodas, sports drinks, and excessive citrus.
- If you consume acidic items, do so in moderation and preferably with meals.
- Use a straw for acidic beverages to minimize contact with teeth.
- Rinse your mouth with water immediately after consuming acidic foods or drinks to help neutralize acids.
- Wait at least 30-60 minutes before brushing after acidic intake, allowing saliva to naturally remineralize enamel.
- Manage Underlying Medical Conditions: Continue to work with your physician to manage GERD, eating disorders, or other health issues contributing to erosion. Adherence to medical treatment plans is paramount.
- Regular Dental Check-ups: Schedule routine dental exams and cleanings (typically every six months) so your dentist can monitor your oral health, check your restorations, and detect any signs of new erosion early.
- Use Fluoride Products: Your dentist may recommend prescription-strength fluoride toothpaste or mouth rinses to enhance enamel strength.
- Nightguard (If Bruxism is Present): If you grind or clench your teeth, a custom-fitted nightguard can protect your teeth and restorations from excessive wear.
- Stay Hydrated: Drinking plenty of water helps maintain good salivary flow, which is crucial for neutralizing acids.
Pro Tip: Chewing sugar-free gum after meals can stimulate saliva production, aiding in acid neutralization and remineralization. Look for gums containing xylitol.
Prevention: How to Avoid Erosion on Teeth
Prevention is always better than cure, especially when it comes to irreversible conditions like dental erosion. Taking proactive steps can significantly reduce your risk.
Dietary Prevention
- Limit Acidic Foods & Drinks: Reduce consumption of sodas, sports drinks, fruit juices, and sour candies.
- Mindful Consumption: If you do consume acidic items, do so quickly and ideally during meals. Avoid sipping slowly throughout the day.
- Use a Straw: When drinking acidic beverages, a straw can help bypass your teeth, minimizing direct contact with enamel.
- Rinse with Water: Immediately after consuming acidic foods or drinks, rinse your mouth thoroughly with plain water to dilute and wash away acids.
- Chew Sugar-Free Gum: This stimulates saliva flow, which helps neutralize acids and remineralize enamel.
- Avoid Brushing Immediately: Wait at least 30 minutes after consuming acidic foods or drinks before brushing. Your enamel is softened by acid, and brushing too soon can abrade it.
Oral Hygiene Practices
- Soft-Bristled Toothbrush: Always use a soft-bristled toothbrush to prevent abrasive damage, especially to already softened enamel.
- Fluoride Toothpaste: Use a fluoride toothpaste twice daily. Fluoride strengthens enamel and makes it more resistant to acid.
- Proper Brushing Technique: Brush gently with small, circular motions, rather than aggressive scrubbing.
- Fluoride Mouthwash: Consider using an over-the-counter fluoride mouthwash daily, or a prescription-strength one if recommended by your dentist.
Medical & Lifestyle Prevention
- Manage GERD: If you suffer from acid reflux, work closely with your physician to manage the condition through diet, lifestyle changes, and medication.
- Seek Help for Eating Disorders: If you or someone you know struggles with an eating disorder, seek professional medical and psychological help immediately. This is critical for both overall health and preventing severe dental damage.
- Address Dry Mouth: If you experience dry mouth, consult your dentist or physician to identify the cause and discuss solutions, such as salivary stimulants or artificial saliva products.
- Protective Appliances: If you clench or grind your teeth (bruxism), a custom nightguard can protect your teeth from further wear.
- Regular Dental Check-ups: Consistent visits allow your dentist to monitor your oral health, identify early signs of erosion, and provide timely interventions or preventive advice.
Risks and Complications of Untreated Erosion
Ignoring erosion on teeth can lead to a cascade of worsening problems, significantly impacting your oral health and quality of life.
Worsening Sensitivity
As erosion progresses and more dentin is exposed, tooth sensitivity can become severe and chronic, making it painful to eat, drink, or even breathe cold air.
Increased Risk of Decay
While erosion is not caused by bacteria, eroded teeth are more vulnerable to decay. The thinner enamel offers less protection, and exposed dentin is softer and more porous, making it easier for bacteria to penetrate and form cavities.
Structural Weakness and Tooth Fracture
Significant enamel and dentin loss weakens the tooth structure, making teeth more susceptible to chipping, cracking, or even breaking under normal chewing forces.
Changes in Appearance and Aesthetics
Eroded teeth can become discolored (yellowish), dull, translucent, and visibly shorter. This can impact self-confidence and overall facial aesthetics.
Bite Problems (Occlusal Collapse)
Severe erosion, especially affecting the chewing surfaces, can alter your bite. As teeth wear down, your jaw may overclose, leading to issues with the temporomandibular joint (TMJ), muscle pain, and further tooth damage.
Need for Extensive and Costly Treatment
The longer erosion goes untreated, the more extensive and expensive the necessary restorative work becomes. What might have been prevented with simple lifestyle changes could eventually require multiple crowns, veneers, or even full mouth reconstruction.
Pulp Exposure and Infection
In the most severe cases, erosion can wear through the dentin and expose the tooth's pulp (the innermost part containing nerves and blood vessels). This leads to severe pain, infection, and often necessitates root canal therapy or even tooth extraction.
Children / Pediatric Considerations
Erosion on teeth is not just an adult problem; it's increasingly observed in children and adolescents in the US. The developing enamel of primary (baby) teeth and newly erupted permanent teeth is particularly vulnerable to acid attack.
Common Causes in Children
- Frequent Acidic Drinks: The widespread consumption of sodas, fruit juices, and sports drinks among children is a primary driver of extrinsic erosion. Parents often underestimate the acidity of seemingly "healthy" juices.
- "Grazing" Habits: Sipping on acidic beverages or snacking on acidic foods throughout the day, rather than at specific meal times, prolongs acid exposure.
- Medications: Some children's medications (e.g., chewable vitamin C, iron supplements) can be acidic.
- Medical Conditions: Though less common than in adults, GERD can affect children and should be monitored. Eating disorders can also begin in adolescence.
- Enamel Defects: Some children are born with developmental enamel defects (e.g., amelogenesis imperfecta, Molar Incisor Hypomineralization) which make their teeth inherently weaker and more susceptible to erosion.
Signs of Erosion in Children
- Sensitivity: Children may complain of toothache when eating cold or sweet foods.
- Dull or Yellowish Teeth: Parents might notice changes in the color or luster of their child's teeth.
- Transparent Edges: The biting edges of front teeth may appear clear or thin.
- Cupping: Small indentations on the chewing surfaces of molars.
Prevention and Management for Parents
- Limit Acidic Beverages: Encourage water or milk as primary beverages. Offer fruit juices only at meal times and in moderation. Avoid sodas and sports drinks.
- Straw Usage: Encourage children to use a straw for acidic drinks to minimize contact with teeth.
- Rinse with Water: Teach children to rinse their mouth with water after consuming acidic foods or drinks.
- Proper Brushing: Ensure children use a soft-bristled toothbrush and fluoride toothpaste. Supervise brushing to ensure proper technique and timing (waiting after acidic intake).
- Regular Dental Visits: Early and consistent dental check-ups are vital for detecting erosion or enamel defects.
- Dental Sealants: Your pediatric dentist may recommend sealants for the chewing surfaces of molars and premolars to provide an extra layer of protection.
- Address Underlying Conditions: If GERD or an eating disorder is suspected, seek immediate medical and psychological evaluation.
- Educate and Model: Teach children about healthy eating habits and demonstrate good oral hygiene practices.
Frequently Asked Questions
What's the difference between dental erosion and cavities?
While both involve tooth decay, cavities (dental caries) are caused by acids produced by bacteria breaking down sugars. Erosion is the non-bacterial loss of tooth structure due to direct chemical dissolution by acids, often from diet or stomach acid, independent of bacterial activity.
Can erosion be reversed?
No, the loss of tooth enamel due to erosion is irreversible. Once enamel is gone, it cannot grow back. However, early intervention with fluoride can help remineralize and strengthen softened enamel, and treatments like bonding, veneers, or crowns can restore lost tooth structure and protect against further damage.
Does brushing too hard cause erosion?
Aggressive brushing, especially with a hard-bristled toothbrush, can cause abrasion, which is physical wear of the tooth. If you brush too hard immediately after consuming acidic foods or drinks, when your enamel is softened, you can significantly accelerate the erosive process by physically removing the softened enamel.
How painful is the treatment for erosion?
Most treatments for dental erosion are performed under local anesthesia, so you should not feel pain during the procedure. You might experience some temporary sensitivity or discomfort after treatment, particularly with more invasive procedures like crowns, but this usually subsides within a few days to a few weeks.
How long do restorations for eroded teeth last?
The lifespan of restorations varies. Dental bonding typically lasts 5-10 years. Porcelain veneers and crowns can last 10-15 years or even longer with excellent oral hygiene and regular dental check-ups. Maintaining good habits and managing the underlying causes of erosion are crucial for the longevity of any restoration.
Is dental insurance likely to cover treatment for eroded teeth?
Coverage depends on the type of treatment and your specific plan. Preventative treatments like fluoride are often fully covered. Restorative treatments like bonding, inlays, onlays, and crowns typically receive 50-80% coverage. Cosmetic treatments like veneers often have limited or no coverage unless deemed medically necessary to restore function due to severe erosion.
Can teeth become sensitive to the air due to erosion?
Yes, as erosion progresses and more enamel is lost, the underlying dentin becomes exposed. Dentin contains microscopic tubules that lead directly to the tooth's nerve, making it highly sensitive to external stimuli, including cold air, hot liquids, and sweet or acidic foods.
What are some natural remedies for acid erosion?
While no natural remedy can reverse existing erosion, certain practices can help prevent further damage. These include rinsing with plain water after acidic intake, chewing sugar-free xylitol gum to stimulate saliva, and maintaining a diet low in highly acidic foods and drinks. Always consult your dentist for proper diagnosis and treatment.
Can stress cause acid erosion?
Stress itself doesn't directly cause erosion, but it can contribute indirectly. Stress can exacerbate conditions like GERD (acid reflux) or lead to habits like teeth grinding (bruxism), which can worsen the effects of erosion. Some people also tend to consume more acidic comfort foods/drinks when stressed.
What happens if I ignore mild tooth erosion?
Ignoring mild tooth erosion can lead to its progression. Over time, what started as slight sensitivity or dullness can worsen, leading to increased pain, significant tooth structure loss, chipping, fractures, and eventually the need for more complex, costly, and invasive restorative treatments like crowns or even root canal therapy if the pulp becomes exposed.
When to See a Dentist
It's vital to seek professional dental care if you suspect you have erosion on teeth. Early detection and intervention can prevent minor issues from becoming major problems.
Schedule a Routine Appointment If:
- You notice any increased sensitivity to hot, cold, sweet, or acidic foods and drinks that persists.
- Your teeth appear duller, more yellow, or have translucent edges.
- You observe any subtle changes in the shape or texture of your teeth, such as small indentations or a smoothed-out appearance.
- You have a history of GERD, an eating disorder, or frequently consume acidic foods and beverages.
- You have existing fillings that seem to "stand proud" or are higher than the surrounding tooth surface.
Seek Immediate Attention (Emergency or Prompt Visit) If:
- You experience severe, sharp, or throbbing tooth pain that doesn't subside, which could indicate a deep erosion nearing the tooth's nerve or an infection.
- A tooth chips or fractures unexpectedly, especially if it's due to weakened tooth structure.
- You develop swelling, redness, or pus around a tooth, which could be a sign of infection or abscess resulting from severe erosion.
- Your sensitivity becomes unbearable, significantly impacting your ability to eat, drink, or speak comfortably.
Remember, your dental professional at SmilePedia.net is your best resource for diagnosing and treating dental erosion. Don't wait until the damage is extensive; proactive care can preserve your smile and prevent future complications.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
What Are Calcium Deposits on Teeth
Are you one of the millions of Americans who notices a stubborn, yellowish buildup on your teeth despite regular brushing? You're likely experiencing what many refer to as "calcium deposits on teeth." This common dental concern, medically known as dental calculus or tartar, affects a vast ma
February 23, 2026
Calcium Good for Teeth: Complete Guide
More than 99% of your body's calcium resides in your bones and teeth, making it an undeniable cornerstone of skeletal and oral health. But did you know that an estimated 42% of American adults don't get enough calcium from their diet? This staggering statistic underscores a critical question
February 23, 2026
What Do Bulimia Teeth Look Like
"Bulimia teeth" refers to the specific and often severe damage that the self-induced vomiting characteristic of bulimia nervosa inflicts on a person's oral health. It's a critical issue, affecting approximately 1.5% of women and 0.5% of men in the US at some point in their lives, with many more
February 23, 2026

Erosion in Teeth: Complete Guide
Erosion in Teeth: Complete Guide
February 23, 2026