Inlay
5,749 words · 19 min read
Quick Definition
A custom-made filling fabricated in a dental laboratory and cemented into a tooth cavity. Inlays fit within the cusps of a tooth, unlike onlays which extend over one or more cusps.
What is an Inlay? Your Definitive Guide to This Durable Dental Restoration
When a tooth develops a cavity that's too large for a traditional filling but not extensive enough to warrant a full crown, an inlay often emerges as the ideal solution. An inlay is a custom-made dental restoration that is precisely fabricated in a dental laboratory and then permanently cemented into the biting surface of a tooth. Unlike a direct filling, which is sculpted directly into the tooth during a single dental visit, an inlay is an indirect restoration, meaning it's made outside the mouth to exact specifications. Crucially, inlays fit within the cusps (the raised points on the chewing surface) of a tooth, distinguishing them from onlays, which extend over one or more cusps.
Inlays are celebrated for their superior strength, durability, and precise fit, offering a long-lasting alternative that restores the tooth's structure, function, and aesthetics. They are designed to withstand the significant forces of chewing, preventing further decay and fracture. While their use varies based on individual cases, dental inlays are a well-established and highly effective treatment for moderate decay or damage, helping millions of Americans preserve their natural teeth and maintain optimal oral health. Understanding what an inlay is and its benefits can empower you to make informed decisions about your dental care.
Key Takeaways:
- An inlay is a custom-made dental restoration, fabricated in a lab, and cemented into a tooth.
- It is used for cavities too large for fillings but too small for full crowns.
- Inlays fit within the cusps of a tooth, distinguishing them from onlays.
- They offer superior strength, durability, and a precise fit compared to traditional fillings.
- The process typically involves two dental visits: one for preparation and impression, one for bonding.
- Inlays are a long-term solution for restoring damaged or decayed teeth.
Detailed Explanation
Types and Classifications of Inlays
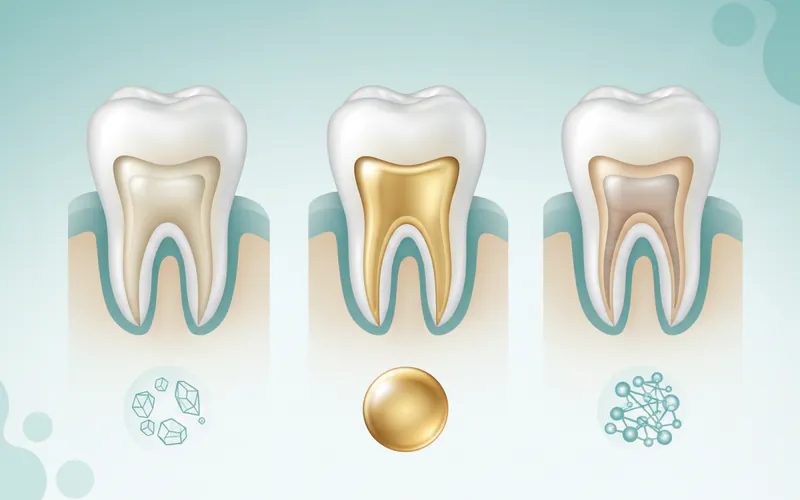
Inlays are primarily classified by the material used in their fabrication. Each material offers distinct advantages in terms of aesthetics, durability, and cost. The choice of material often depends on the tooth's location, the patient's aesthetic preferences, and budget.
-
Porcelain Inlays (Ceramic Inlays):
- Description: Made from high-strength dental ceramic, porcelain inlays are incredibly popular due to their excellent aesthetic qualities. They can be precisely color-matched to your natural tooth, making them virtually indistinguishable from surrounding teeth.
- Pros: Highly aesthetic, biocompatible, durable, resistant to staining.
- Cons: Can be more brittle than gold, potentially higher cost.
- Use: Often preferred for visible teeth due to their natural appearance.
-
Composite Resin Inlays:
- Description: Fabricated from a tooth-colored resin material, similar to direct composite fillings but cured and hardened in a lab for greater strength.
- Pros: Good aesthetics (though slightly less translucent than porcelain), more conservative tooth reduction than porcelain, generally more affordable than porcelain or gold.
- Cons: Can be more prone to staining than porcelain, may not be as durable as porcelain or gold over very long periods.
- Use: A good balance of aesthetics and cost for many patients.
-
Gold Inlays:
- Description: Made from a gold alloy, these inlays are known for their exceptional strength and longevity. Gold is highly biocompatible and wears at a rate similar to natural tooth enamel, preventing excessive wear on opposing teeth.
- Pros: Extremely durable, long-lasting (often decades), very strong, excellent fit, gentle on opposing teeth.
- Cons: Not aesthetically pleasing for many (metallic color), higher initial cost due to material.
- Use: Often recommended for molars or teeth under significant chewing force, especially for patients prioritizing durability over aesthetics.
While less common now, other materials like base metals or silver amalgam could technically be used, but gold, porcelain, and composite resin are the predominant choices for modern inlays due to their superior properties. The "indirect" nature of all these inlays—being crafted in a lab from an impression of your tooth—is a unifying characteristic that ensures a precise fit and enhanced strength compared to direct fillings.
Causes and Risk Factors for Needing an Inlay
The primary reasons a dentist might recommend an inlay revolve around the extent of tooth damage or decay. It's often a restorative choice when a tooth has suffered more significant compromise than a standard filling can effectively address but less than what would require a full crown.
- Large Cavities: The most common reason. When decay has spread beyond what a simple composite or amalgam filling can repair effectively, an inlay provides a stronger, more durable restoration. If the cavity is too wide or deep, a direct filling might compromise the tooth's structural integrity, leading to fractures.
- Failing Existing Fillings: Old, large fillings, especially amalgam ones, can weaken over time, crack, or pull away from the tooth, creating gaps where new decay can begin. When these fillings fail, an inlay can replace the compromised structure more conservatively than a full crown.
- Fractured or Cracked Teeth (Non-Cuspal): Sometimes, a tooth may suffer a fracture that is confined within the cusps, or a portion of the tooth may break off due to trauma or biting on something hard. If the damage is extensive but doesn't involve the cusps, an inlay can restore the tooth's integrity.
- Wear and Erosion: While less common than decay, significant tooth wear due to grinding (bruxism) or acid erosion can sometimes necessitate an inlay to restore lost tooth structure and protect the remaining tooth.
- Preventing Future Fractures: For teeth with large areas of lost structure, an inlay can act as a buttress, strengthening the remaining tooth walls and preventing future fractures that might occur with a weaker, direct filling.
Risk Factors that increase the likelihood of needing an inlay include:
- Poor Oral Hygiene: Inadequate brushing and flossing lead to plaque buildup and acid attacks, causing cavities.
- High Sugar Diet: Frequent consumption of sugary foods and drinks fuels decay-causing bacteria.
- Age: Older existing fillings are more prone to failure, and general wear and tear accumulate over time.
- Genetics: Some individuals may have naturally weaker enamel or a predisposition to decay.
- Dry Mouth (Xerostomia): Reduced saliva flow means less natural cleansing and buffering of acids, increasing decay risk.
- Previous Dental Work: Teeth with existing large fillings are inherently weaker and more susceptible to further damage or the failure of the existing restoration.
Signs and Symptoms to Watch For
Recognizing the signs and symptoms that might indicate a need for an inlay is crucial for timely intervention and preventing more extensive damage. Many of these symptoms are similar to those of a large cavity or a failing filling.
- Persistent Tooth Sensitivity: This is a common indicator. You might experience sharp pain or discomfort when consuming hot or cold foods and beverages, or even sweet items. This sensitivity can be mild or quite pronounced, and it may linger for a few moments after the stimulus is removed.
- Pain When Chewing or Biting: If you feel pain or discomfort specifically when biting down or chewing food on a particular tooth, it could indicate underlying decay, a crack, or a failing filling that is putting pressure on the tooth's nerve.
- Visible Hole or Pit in the Tooth: While cavities can sometimes be hidden, a larger cavity that warrants an inlay might present as a noticeable hole or pit on the chewing surface of your tooth. It may appear dark brown or black.
- Staining on the Tooth Surface: Discoloration that isn't superficial surface stain could be a sign of decay progressing underneath the enamel.
- Food Trapping: If food consistently gets stuck in a particular area of your tooth, it could be an early sign of a cavity or a gap forming around an old filling.
- Rough or Catching Surface: You might notice a rough edge with your tongue or floss getting repeatedly snagged, which could indicate a fractured tooth, a cracked filling, or a compromised tooth structure.
- Lost or Fractured Filling: If an existing filling feels loose, has fallen out, or a piece has broken off, it almost certainly signals a need for a new restoration, potentially an inlay depending on the extent of the remaining tooth structure.
- Bad Breath or Unpleasant Taste: Persistent bad breath or a foul taste in your mouth can sometimes be associated with tooth decay, as bacteria proliferate in the affected areas.
It's important to remember that not all cavities cause pain, especially in their early stages. Regular dental check-ups are essential for detecting problems before they become symptomatic and require more extensive treatment. If you experience any of these symptoms, schedule an appointment with your dentist promptly.
Diagnosis Process — What Your Dentist Does
Diagnosing the need for an inlay involves a thorough examination by your dentist, often incorporating several diagnostic tools and techniques to accurately assess the extent of the tooth's damage.
- Comprehensive Visual Examination: Your dentist will carefully inspect your teeth, looking for visible signs of decay, cracks, discoloration, or failing existing fillings. They will use a small mirror and a dental explorer (a sharp, pointed instrument) to probe tooth surfaces and identify soft spots or irregularities. They will also look for any signs of tooth sensitivity or pain response.
- Dental X-rays (Radiographs): X-rays are invaluable for detecting decay that is not visible to the naked eye, particularly between teeth or underneath existing restorations. Bitewing X-rays are commonly used to show the crowns of the upper and lower back teeth, revealing interproximal (between teeth) and occlusal (chewing surface) cavities, as well as the integrity of existing fillings. Periapical X-rays may be used if there's suspicion of a deep infection extending to the root tip.
- Transillumination: This technique involves shining a bright light through the tooth. Cracks or fractures will often block the light, appearing as dark lines, which can help in identifying damage that might otherwise be overlooked.
- Tactile Examination: Your dentist will gently probe the tooth surface and around existing fillings to feel for any areas where the explorer "catches" or for soft spots indicative of decay.
- Biting Test: If you're experiencing pain when chewing, your dentist may have you bite on a cotton roll or a specialized instrument to pinpoint the exact tooth or area causing the discomfort, which can help identify cracks or subtle fractures.
- Cavity Detection Dyes: In some cases, a special dye may be applied to the tooth. This dye temporarily stains decayed areas, making them more visible and helping the dentist differentiate between healthy and compromised tooth structure.
- Assessment of Existing Restorations: If an old filling is present, the dentist will evaluate its margins (where the filling meets the tooth), looking for signs of leakage, cracks, or recurrent decay beneath it.
Based on this comprehensive evaluation, your dentist will determine if the cavity or damage is too extensive for a traditional filling but conservative enough that a full crown is not yet necessary. If an inlay is deemed the most appropriate restoration, they will discuss the material options and the treatment plan with you.
Treatment Options with Pros, Cons, and Costs
When considering an inlay, it's helpful to understand how it compares to other common dental restorations for moderate to extensive tooth damage. The choice often depends on the extent of decay, the tooth's location, aesthetics, and budget.
| Treatment Option | Description | Pros | Cons | Estimated Cost Range (US, without insurance) |
|---|---|---|---|---|
| Direct Filling | Material (composite resin, amalgam) placed directly into the cavity and hardened in a single visit. | Pros: Single visit, most affordable, minimal tooth reduction, good for small-to-moderate cavities. | Cons: Less durable than inlays/onlays/crowns for large cavities, may not withstand heavy chewing forces, composite can stain over time, amalgam less aesthetic. | $150 - $450 (composite), $100 - $300 (amalgam) |
| Inlay | Custom-made restoration fabricated in a lab, fits within the cusps, cemented in place. (Porcelain, Composite Resin, Gold) | Pros: Superior strength and durability over large direct fillings, precise fit, excellent aesthetics (porcelain/composite), protects tooth from fracture, long lifespan (10-30+ years), conservative of tooth structure compared to crowns. | Cons: Requires two visits, generally more expensive than direct fillings, fabrication time involved, potential for initial sensitivity. Gold inlays are not aesthetic. | $600 - $1,500+ (porcelain/composite), $800 - $2,000+ (gold) |
| Onlay | Similar to an inlay but extends to cover one or more cusps of the tooth, providing more extensive coverage and strength. Also lab-fabricated. | Pros: Provides more protection and strength than an inlay, especially for weakened cusps, more conservative than a full crown (saves more natural tooth structure), excellent durability and aesthetics. | Cons: Requires two visits, more expensive than an inlay, more tooth reduction than an inlay, fabrication time. | $800 - $2,000+ (porcelain/composite), $1,000 - $2,500+ (gold) |
| Dental Crown | A cap that covers the entire visible portion of the tooth above the gum line, fully encasing it. | Pros: Maximum protection and strength for severely damaged or weak teeth, ideal for root canal-treated teeth, offers complete aesthetic restoration. | Cons: Most aggressive tooth reduction (removes the most healthy tooth structure), most expensive option, requires two visits, potential for nerve irritation. | $800 - $3,000+ (depending on material: porcelain, PFM, zirconia, gold) |
Cost Considerations: The costs listed above are general ranges in the US market without insurance. They can vary significantly based on:
- Geographic location: Dental fees are often higher in urban areas.
- Dentist's experience and specialization: Fees can differ between general dentists and specialists.
- Material chosen: Gold is often the most expensive material due to its intrinsic value, followed by high-quality porcelain and then composite resin.
- Complexity of the case: More extensive decay or difficult access can increase costs.
With insurance: Most dental insurance plans provide some coverage for inlays, often classifying them under major restorative procedures. Coverage typically ranges from 50% to 80% of the approved cost, after meeting your deductible. It's crucial to check your specific plan's benefits.
Step-by-Step: What to Expect During Treatment
Getting an inlay typically involves two dental visits. This multi-step process ensures the custom-made restoration fits perfectly and provides optimal strength and aesthetics.
Visit 1: Tooth Preparation and Impression
- Numbing: The first step involves administering a local anesthetic to numb the tooth and surrounding gum tissue, ensuring you remain comfortable throughout the procedure.
- Removal of Decay/Old Filling: Your dentist will use specialized dental instruments to carefully remove all decayed or damaged tooth structure. If you have an existing filling, it will be removed as well. The goal is to create a clean, healthy foundation for the inlay.
- Tooth Shaping: The tooth is then meticulously shaped to create a precise preparation for the inlay. This involves creating distinct walls and margins that will allow the inlay to sit perfectly within the tooth structure, ensuring a tight seal and maximum strength. This shaping is conservative, preserving as much healthy tooth as possible compared to a crown.
- Impression Taking: Once the tooth is prepared, an impression (mold) of your tooth is taken. This can be done using traditional dental putty, where you bite into a tray filled with impression material, or with a modern digital scanner that creates a 3D model of your tooth. This impression is then sent to a dental laboratory, where skilled technicians will custom-fabricate your inlay. ``
- Temporary Restoration: While your custom inlay is being made, a temporary filling or inlay will be placed over the prepared tooth. This temporary restoration protects the exposed tooth structure, prevents sensitivity, and keeps the surrounding teeth from shifting. It's important to be gentle with the temporary and avoid sticky or very hard foods.
- Color Matching (for aesthetic materials): If you've chosen a porcelain or composite resin inlay, your dentist will use a shade guide to select a color that perfectly matches your natural teeth, ensuring a seamless appearance.
Visit 2: Inlay Placement
- Numbing (Optional): While often not strictly necessary, your dentist may apply a topical anesthetic or a small amount of local anesthetic to ensure comfort when removing the temporary and seating the permanent inlay.
- Removal of Temporary: The temporary restoration is carefully removed, and any remaining temporary cement is cleaned away.
- Cleaning and Inspection: The prepared tooth is thoroughly cleaned and disinfected. Your dentist will then try in the permanent inlay to ensure a perfect fit. They will check the margins (where the inlay meets the tooth), your bite, and the overall aesthetics. Adjustments may be made to the inlay if needed at this stage.
- Bonding/Cementing: Once the fit is verified, the tooth surface is etched with a mild acid solution to create microscopic pores, and a dental adhesive (bonding agent) is applied. The inlay is then permanently bonded or cemented into place using a strong dental cement or resin. A special curing light is often used to quickly harden the adhesive.
- Polishing and Finishing: After the inlay is securely cemented, your dentist will meticulously remove any excess cement and polish the inlay and the surrounding tooth structure. They will check your bite again to ensure the inlay doesn't interfere with your natural occlusion, making any final adjustments to prevent high spots that could cause discomfort or damage. ``
The entire process, from start to finish, typically takes about two weeks between visits, allowing the lab ample time to create your custom, high-quality inlay.
Recovery Timeline and Aftercare
The recovery period after receiving an inlay is generally straightforward, but proper aftercare is crucial for the longevity of your restoration and overall oral health.
Immediate Post-Treatment (First Few Days):
- Sensitivity: It's common to experience some mild to moderate sensitivity to hot, cold, or pressure for a few days up to a couple of weeks after the inlay is cemented. This is usually due to the tooth's reaction to the bonding process and the minor trauma of the procedure. Over-the-counter pain relievers (like ibuprofen or acetaminophen) can help manage discomfort.
- Gum Soreness: Your gums around the treated tooth might be slightly tender or inflamed for a day or two. Rinsing with warm salt water can help soothe the tissues.
- Bite Adjustment: While your dentist will meticulously check your bite, sometimes after the anesthetic wears off, you might notice a subtle "high spot" on the inlay. If your bite feels off or uneven after a few days, contact your dentist. A quick adjustment can prevent discomfort or damage to the inlay or opposing teeth.
- Avoid Chewing on the Treated Side (Immediately): If your inlay was cemented with a traditional dental cement, your dentist might advise you to avoid chewing on that side for a few hours to allow the cement to fully set. With modern bonding agents, you can usually eat normally once the numbness wears off, but it's always wise to be cautious.
Long-Term Aftercare:
- Oral Hygiene is Key: Treat your inlay just like your natural teeth. Brush twice a day with a fluoride toothpaste, paying extra attention to the area around the inlay's margins to prevent plaque buildup and secondary decay. Floss daily to clean between teeth and along the gum line, ensuring food particles don't get trapped.
- Regular Dental Check-ups: Continue with your routine dental check-ups and cleanings every six months (or as recommended by your dentist). Your dentist will monitor the integrity of your inlay, check its margins, and ensure no new decay is forming.
- Avoid Hard and Sticky Foods: While inlays are very strong, excessive force on very hard candies, ice, or sticky caramels can potentially damage them, especially during the initial weeks.
- Address Bruxism (Teeth Grinding): If you clench or grind your teeth (bruxism), your dentist might recommend a nightguard. This custom-fit appliance protects your inlays (and natural teeth) from excessive forces during sleep, prolonging their lifespan.
- Dietary Choices: Limit sugary and acidic foods and drinks, as they contribute to tooth decay around the margins of any restoration.
With proper care, an inlay can last for 10 to 30 years or even longer, making it a highly durable and cost-effective restoration over its lifespan.
Prevention Strategies
Preventing the need for an inlay (or any dental restoration) starts with excellent oral hygiene and healthy lifestyle choices. The goal is to minimize decay and damage to your teeth.
-
Maintain Impeccable Oral Hygiene:
- Brush Twice Daily: Brush your teeth for two minutes, at least twice a day, using a fluoride toothpaste. Ensure you cover all surfaces of your teeth, including the chewing surfaces, outer surfaces, and inner surfaces.
- Floss Daily: Flossing is crucial for removing plaque and food particles from between your teeth and under the gum line, areas your toothbrush can't reach. This prevents interproximal (between teeth) cavities, which often require inlays or onlays.
- Use Mouthwash: An antiseptic or fluoride mouthwash can provide an extra layer of protection by killing bacteria and strengthening enamel.
-
Regular Dental Check-ups and Cleanings:
- Every Six Months: Visit your dentist for professional cleanings and examinations at least twice a year. These appointments allow your dentist to detect early signs of decay, gum disease, or issues with existing fillings or restorations before they become extensive.
- X-rays: Regular dental X-rays (typically once a year or every few years, depending on your risk factors) are essential for identifying hidden cavities, especially those between teeth or under old fillings.
-
Healthy Diet:
- Limit Sugary and Acidic Foods/Drinks: Reduce your consumption of sodas, fruit juices, sports drinks, candies, and refined carbohydrates. These fuel acid-producing bacteria in your mouth, leading to enamel erosion and decay.
- Eat Nutrient-Rich Foods: A balanced diet rich in fruits, vegetables, lean proteins, and dairy (for calcium) strengthens tooth enamel and supports overall oral health.
- Drink Water: Water helps rinse away food particles and neutralize acids. Fluoridated tap water is especially beneficial.
-
Protect Your Teeth:
- Avoid Hard Foods: Be cautious with very hard foods like ice, unpopped popcorn kernels, and hard candies, which can chip or crack teeth, potentially leading to the need for an inlay or crown.
- Address Bruxism: If you grind or clench your teeth (bruxism), talk to your dentist about a custom-made nightguard. This protects your teeth from excessive wear and potential fractures.
- Wear a Mouthguard for Sports: If you participate in contact sports, a protective mouthguard is essential to prevent traumatic injuries to your teeth.
-
Consider Sealants: For children and sometimes adults, dental sealants can be applied to the chewing surfaces of molars to fill in pits and grooves, creating a smooth surface that's easier to clean and less prone to decay. While not directly preventing the need for an inlay, they prevent initial decay that could escalate.
By adopting these preventive measures, you significantly reduce your risk of developing cavities or dental damage that would necessitate an inlay or other extensive restorations.
Cost Ranges in the US (with/without insurance)
The cost of a dental inlay in the US can vary widely based on several factors, including the material chosen, the complexity of the case, the geographic location of the dental practice, and the dentist's fees.
General Cost Ranges (without insurance):
- Composite Resin Inlay: $600 - $1,200 per tooth
- Porcelain (Ceramic) Inlay: $800 - $1,500+ per tooth
- Gold Inlay: $1,000 - $2,000+ per tooth
Factors Influencing Cost:
- Material: As noted above, gold is often the most expensive due to the cost of the metal, followed by porcelain, and then composite resin. High-quality materials and advanced lab techniques also contribute.
- Location: Dental costs are generally higher in major metropolitan areas (e.g., New York, Los Angeles) compared to rural areas.
- Dentist's Fees: Experienced dentists or those specializing in cosmetic or restorative dentistry may have higher fees.
- Complexity: A larger inlay, one in a difficult-to-access tooth, or one requiring extensive tooth preparation might incur higher costs.
- Additional Procedures: Costs might increase if other procedures are needed, such as build-up material (core foundation) if a significant amount of tooth structure is missing, or if a root canal is unexpectedly discovered.
Cost with Dental Insurance:
Most dental insurance plans in the US categorize inlays as a "major restorative" procedure. This typically means:
- Deductible: You will likely need to meet your annual deductible first (e.g., $50 - $150).
- Coinsurance: After your deductible is met, insurance plans usually cover a percentage of the cost, often 50% to 80%. For example, if your plan covers 80% of major restorative services, and the approved cost of your inlay is $1,000, you would pay $200 (20%) plus your deductible.
- Annual Maximums: Most dental insurance plans have an annual maximum benefit (e.g., $1,000 - $2,000). Once you reach this limit, you are responsible for 100% of any further dental costs for that year.
- Waiting Periods: Some plans have waiting periods (e.g., 6-12 months) for major restorative procedures like inlays, meaning you can't get coverage for these treatments immediately after enrolling.
It is highly recommended to contact your dental insurance provider directly or have your dentist's office submit a pre-treatment estimate (pre-authorization) before proceeding with the inlay. This will give you a clear understanding of your out-of-pocket expenses. Many dental offices also offer payment plans or third-party financing options to help manage costs.
For Parents / Pediatric Considerations
While inlays are less commonly used in primary (baby) teeth due to their temporary nature and the rapid growth and change in a child's mouth, they can be a viable and beneficial option for adolescents who develop extensive cavities in their permanent molars.
Key Considerations for Pediatric Patients:
- Permanent Molars: Inlays are almost exclusively considered for permanent molars in adolescents. These teeth need to last a lifetime, and for larger cavities that compromise the tooth's structure, an inlay can offer superior strength and durability compared to a large composite filling.
- Extent of Decay: If a cavity in a permanent molar is too large or deep for a conventional filling but has not reached a point where a full crown is necessary, an inlay can be a conservative and strong restoration.
- Cooperation: The inlay procedure requires a child to be cooperative for two visits, including sitting still for impressions and the bonding process. This can sometimes be challenging for very young or anxious children.
- Material Choice: For aesthetic reasons, porcelain or composite resin inlays are typically preferred for adolescents. Gold inlays, while highly durable, are less aesthetic and rarely chosen for younger patients unless specifically indicated for a very strong bite.
- Prevention is Paramount: The best "treatment" for children is prevention. Emphasize excellent oral hygiene (brushing, flossing), a balanced diet low in sugar, and regular dental check-ups with fluoride treatments and dental sealants. These preventive measures significantly reduce the risk of needing any major restoration, including an inlay.
- Orthodontic Considerations: If a child is undergoing or planning to undergo orthodontic treatment, the presence of an inlay would need to be considered by the orthodontist. While generally not an issue, specific attachments or bracket placement might require careful planning.
In summary, while not a routine pediatric procedure, an inlay can be an excellent, long-lasting solution for specific cases of extensive decay in a teenager's permanent back teeth, offering a balance of durability and tooth preservation. Your pediatric dentist will assess the individual needs of your child and recommend the most appropriate restoration.
Frequently Asked Questions
How much does an inlay cost?
The cost of an inlay in the US typically ranges from $600 to $2,000 or more per tooth without insurance. This variation depends on the material (composite resin, porcelain, or gold), the complexity of the tooth, the geographic location of the dental practice, and the dentist's fees. Gold inlays are generally the most expensive. With dental insurance, you can expect to pay a percentage of the cost (e.g., 20-50%) after meeting your deductible, up to your annual maximum benefit. It's best to get a pre-treatment estimate from your dental office.
Is getting an inlay painful?
The procedure to get an inlay is typically not painful because your dentist will use a local anesthetic to thoroughly numb the tooth and surrounding area. You might feel some pressure or vibration during the tooth preparation, but no sharp pain. After the anesthetic wears off, it's common to experience some mild to moderate sensitivity to hot/cold or pressure for a few days to a couple of weeks. Over-the-counter pain relievers usually manage this discomfort effectively.
How long does an inlay last?
With proper oral hygiene and regular dental check-ups, an inlay is a highly durable restoration that can last for a very long time. Porcelain and gold inlays are known for their exceptional longevity, often lasting 10 to 30 years or even longer. Composite resin inlays typically have a lifespan of 5 to 15 years, similar to direct composite fillings but often stronger due to lab fabrication. The lifespan can be affected by biting habits, diet, and overall oral health.
What are the alternatives to an inlay?
The primary alternatives to an inlay depend on the extent of the tooth damage:
- Direct Filling: For smaller to moderate cavities, a traditional composite or amalgam filling is a simpler, single-visit, and less expensive option. However, it may not be strong enough for larger defects.
- Onlay: If the decay or fracture extends to cover one or more cusps of the tooth, an onlay might be recommended. It's similar to an inlay but provides more coverage and strength than an inlay.
- Dental Crown: For more extensive damage, a weakened tooth (e.g., after a root canal), or significant fractures, a full crown that covers the entire tooth surface is the strongest restoration. This is generally the most aggressive and expensive option as it requires removing more healthy tooth structure.
Does dental insurance cover inlays?
Yes, most dental insurance plans typically provide coverage for inlays. Inlays are usually classified as a "major restorative" procedure. This means that after you meet your annual deductible, your insurance plan will often cover a percentage of the cost, usually 50% to 80%. Be aware of annual maximum benefits and potential waiting periods for major procedures. Always check with your specific insurance provider for detailed coverage information.
How do I care for my inlay?
Caring for your inlay is similar to caring for your natural teeth. Maintain excellent oral hygiene by brushing twice daily with fluoride toothpaste and flossing daily to clean around the inlay's margins and between teeth. Regular dental check-ups and professional cleanings every six months are crucial for monitoring the inlay's integrity. Avoid chewing on very hard foods or ice, and if you grind your teeth, consider wearing a nightguard to protect your restoration.
What's the difference between an inlay and an onlay?
The key difference lies in the extent of tooth coverage. An inlay fits within the cusps (the raised points on the chewing surface) of a tooth. It restores only the chewing surface that is contained by the cusps. An onlay, on the other hand, is a more extensive restoration that extends over one or more cusps of the tooth, providing additional protection and reinforcement to weakened cusps. Both are indirect restorations fabricated in a lab.
Can an inlay fall out?
While rare, an inlay can potentially fall out, especially if the bonding agent weakens over time, if there's recurrent decay underneath the inlay, or if the inlay is subjected to extreme biting forces or trauma. If an inlay feels loose or falls out, it's important to contact your dentist immediately. Keep the inlay if possible and bring it with you to your appointment. Your dentist will assess the situation and determine if the inlay can be re-cemented or if a new restoration is needed.
When to See a Dentist
Knowing when to seek dental care is crucial for maintaining your oral health and addressing potential issues with inlays or other restorations.
Emergency Signs (See a Dentist Immediately):
- Sudden, Severe Tooth Pain: If you experience intense, throbbing pain, especially if it's constant or wakes you up at night, it could indicate an infection, a deep cavity, or a cracked tooth.
- Lost or Fractured Inlay: If your inlay falls out completely, or a significant piece of it breaks off, expose the underlying tooth structure, seek immediate attention to protect the tooth from further damage or sensitivity.
- Swelling: Any swelling in your gums, face, or jaw, especially if accompanied by pain or fever, could indicate a serious infection that requires urgent care.
- Trauma: If you've suffered an injury to your mouth or teeth (e.g., from an accident or sports), even if there's no visible damage, it's important to be checked by a dentist.
Routine Care / When to Schedule an Appointment Soon:
- Persistent Sensitivity: If you experience lingering sensitivity to hot, cold, or sweets that doesn't subside within a few weeks after getting an inlay, or if new sensitivity develops in a previously treated tooth, schedule an appointment.
- Pain When Chewing or Biting: This could indicate a crack, an issue with your bite, or underlying decay.
- Visible Crack or Chip: If you notice a crack in your tooth or around your inlay, even if it's not painful, it's important to have it evaluated to prevent further damage.
- Rough or Catching Edges: If you feel a rough spot with your tongue or if floss repeatedly snags around your inlay, it might indicate a compromised margin or a need for adjustment.
- Changes in Bite: If your bite feels "off" or uneven after a few days of having an inlay placed, or if an old inlay suddenly feels high, contact your dentist for an adjustment.
- Discoloration around Inlay: Any new dark spots or discoloration around the edges of your inlay could signal recurrent decay.
- Routine Check-ups: The most important "when to see a dentist" is for your regular bi-annual check-ups and cleanings. These appointments are essential for preventive care, early detection of problems, and monitoring the long-term health of your inlays and other restorations.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.