Restoration
3,683 words · 12 min read
Quick Definition
Any dental procedure or material used to repair or replace damaged or missing tooth structure, including fillings, crowns, bridges, implants, and dentures.
Restoration: Rebuilding Your Smile and Health
Dental restoration is a cornerstone of modern dentistry, playing a critical role in preserving oral health, function, and aesthetics. At its core, a restoration refers to any dental procedure or material used to repair, replace, or rebuild damaged or missing tooth structure. From a simple filling to complex dental implants, these treatments are designed to restore the integrity and functionality of your teeth, ensuring you can chew, speak, and smile with confidence.
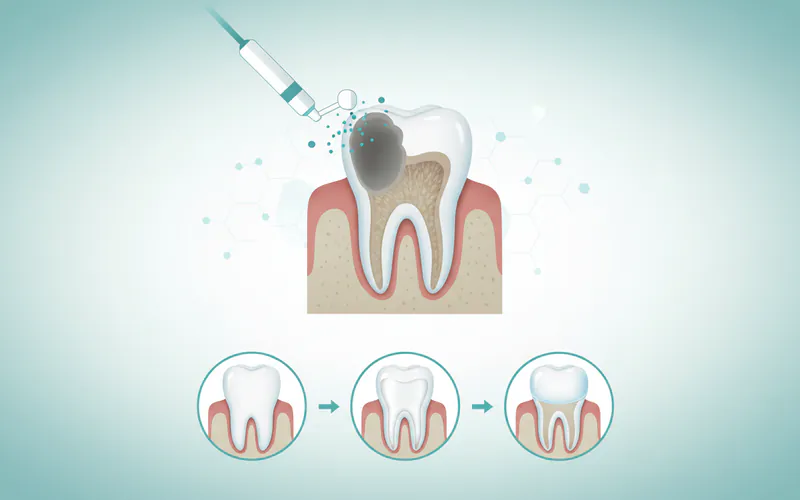
The importance of dental restorations cannot be overstated. Untreated dental problems, such as cavities or fractured teeth, can lead to severe pain, infection, further tooth loss, and even systemic health issues. By intervening with a restoration, dentists can halt the progression of disease, alleviate discomfort, and prevent more extensive and costly problems down the line. Dental restorations are incredibly common, touching the lives of nearly everyone. According to the Centers for Disease Control and Prevention (CDC), over 90% of adults aged 20-64 have had dental caries (cavities), and a significant portion of these will require some form of restorative treatment during their lifetime. This makes restorations one of the most frequently performed dental procedures, essential for maintaining the overall well-being of the US population.
Key Takeaways:
- Restoration repairs or replaces damaged/missing tooth structure.
- It includes fillings, crowns, bridges, implants, and veneers.
- Essential for preventing pain, infection, and further tooth loss.
- Over 90% of adults experience cavities requiring restorative care.
- Restorations maintain chewing function, speech, and aesthetics.
- Early intervention saves teeth and prevents more complex issues.
Detailed Explanation
Types and Classifications of Dental Restorations
Dental restorations are broadly categorized into two main groups: direct restorations and indirect restorations. The choice depends on the extent of the damage, the location of the tooth, and the patient's individual needs.
-
Direct Restorations: These are placed directly into a prepared tooth in a single dental visit.
- Fillings: The most common type of direct restoration, used to repair minor to moderate tooth decay or fractures.
- Amalgam Fillings (Silver Fillings): A durable, cost-effective mixture of metals (silver, tin, copper, mercury). Historically common, known for strength and longevity.
- Composite Fillings (Tooth-Colored Fillings): Made from a plastic and glass mixture, these fillings can be matched to the natural tooth color, offering an aesthetic advantage. They bond directly to the tooth structure.
- Glass Ionomer Fillings: Often used for smaller cavities, especially in non-load-bearing areas or for children. They release fluoride, which can help prevent further decay.
- Resin Ionomer Fillings: A hybrid of composite and glass ionomer, offering some fluoride release with improved aesthetics and strength over traditional glass ionomer.
- Fillings: The most common type of direct restoration, used to repair minor to moderate tooth decay or fractures.
-
Indirect Restorations: These require multiple dental visits because they are fabricated outside the mouth in a dental lab (or in-office with CAD/CAM technology) after the tooth is prepared and an impression is taken. They are then permanently bonded or cemented to the tooth.
- Inlays and Onlays: Used when a cavity or damage is too large for a traditional filling but not extensive enough to require a full crown.
- Crowns (Caps): Full coverage restorations that encase the entire visible portion of a damaged tooth. They are used when a tooth has significant decay, fracture, or has undergone a root canal treatment.
- Materials:
- Porcelain-Fused-to-Metal (PFM) Crowns: A metal substructure covered with porcelain for aesthetics and strength.
- All-Ceramic/All-Porcelain Crowns: Excellent aesthetics, often used for front teeth, and are metal-free.
- Zirconia Crowns: Extremely strong and durable ceramic material, increasingly popular for both front and back teeth.
- Gold Crowns: Highly durable and biocompatible, often used for back teeth due to their strength and minimal wear on opposing teeth.
- E-max Crowns: A type of all-ceramic crown known for its strength and highly aesthetic translucent properties.
- Materials:
- Bridges (Fixed Partial Dentures): Used to replace one or more missing teeth by joining artificial teeth (pontics) to crowns placed on adjacent natural teeth (abutment teeth).
- Types: Traditional (most common), Cantilever (when abutment teeth are only on one side), Maryland (uses metal or porcelain wings bonded to the back of adjacent teeth).
- Materials: Often porcelain, PFM, or zirconia.
- Dental Implants: The most advanced and durable solution for replacing missing teeth. A titanium post is surgically placed into the jawbone, acting as an artificial tooth root. After healing, a crown, bridge, or denture is attached to the implant.
- Components: Implant body (titanium screw), abutment (connector), and prosthetic crown/bridge/denture.
- Veneers: Thin, custom-made shells of porcelain or composite resin that cover the front surface of teeth. While often considered cosmetic, they can be restorative in cases of severe staining, chipping, minor fractures, or enamel erosion to protect the tooth.
Causes and Risk Factors for Tooth Damage Requiring Restoration
Various factors can lead to the need for dental restorations:
- Dental Caries (Cavities): The most common reason. Caused by bacteria in plaque producing acids that erode enamel and dentin. Risk factors include poor oral hygiene, high sugar diet, dry mouth, and genetics.
- Trauma: Accidents, falls, sports injuries, or even biting on hard objects can chip, crack, or fracture teeth, requiring immediate restorative intervention.
- Tooth Wear:
- Attrition: Tooth-to-tooth contact (e.g., grinding or clenching, known as bruxism).
- Abrasion: Wear from external objects (e.g., aggressive brushing, biting nails, using teeth as tools).
- Erosion: Chemical wear from acids (e.g., acidic foods/drinks, gastric reflux, bulimia).
- Periodontal (Gum) Disease: Advanced gum disease can lead to gum recession, bone loss, and ultimately tooth mobility or loss, necessitating extractions and replacement with bridges or implants.
- Failed Previous Restorations: Old fillings or crowns can wear down, fracture, or develop recurrent decay underneath them, requiring replacement.
- Developmental Defects: Some individuals may have naturally weaker enamel or oddly shaped teeth that are more prone to damage and require restorative solutions.
Signs and Symptoms to Watch For
Recognizing the signs of tooth damage early can lead to simpler and less expensive restorative treatments. Look out for:
- Persistent Toothache: Dull ache, sharp pain when biting, or throbbing pain.
- Sensitivity: To hot, cold, sweet foods/drinks, or pressure.
- Visible Holes or Pits: In your teeth, indicating a cavity.
- Dark Spots or Staining: On the tooth surface.
- Rough Edges or Broken Pieces: A chipped or fractured tooth.
- Loose or Missing Fillings/Crowns: Can expose sensitive tooth structure.
- Bad Breath or Unpleasant Taste: Can indicate decay or infection.
- Swelling or Redness: Around a tooth or in the gums.
- Difficulty Chewing: On one side of your mouth or specific foods.
Diagnosis Process — What Your Dentist Does
A thorough dental examination is crucial for accurate diagnosis:
- Visual Examination: Your dentist will carefully inspect your teeth and gums for visible signs of decay, cracks, discoloration, or old, failing restorations. They may use a small mirror and a dental explorer (a thin, pointed instrument) to check for soft spots or irregularities.
- Probing: Gently checking the integrity of enamel and existing fillings.
- Dental X-rays: Bitewing X-rays are excellent for detecting interproximal (between teeth) cavities and evaluating existing fillings. Periapical X-rays show the entire tooth, including the root and surrounding bone, which is vital for assessing infection or bone loss. A panoramic X-ray provides a broader view of the entire mouth and jaw structure.
- Pulp Vitality Tests: If infection or nerve damage is suspected, the dentist may perform tests to check the vitality of the pulp (the innermost part of the tooth containing nerves and blood vessels). These can include thermal tests (hot/cold) or electric pulp tests.
- Transillumination: Shining a light through the tooth can help reveal cracks.
- Intraoral Camera: A small camera can project magnified images of your teeth onto a screen, allowing you to see what the dentist sees and better understand the diagnosis.
Treatment Options with Pros, Cons, and Costs
| Restoration Type | Description | Pros | Cons | US Cost Range (Without Insurance) |
|---|---|---|---|---|
| Amalgam Filling | Silver-colored metal alloy to fill cavities. | Durable, long-lasting, cost-effective, strong. | Less aesthetic, contains mercury, slight risk of sensitivity, requires more tooth removal. | $50 - $200 |
| Composite Filling | Tooth-colored resin to fill cavities. | Aesthetic, bonds to tooth, less tooth removal, mercury-free. | Less durable than amalgam/gold (especially in large restorations), can stain over time, higher cost. | $100 - $450 |
| Glass Ionomer | Tooth-colored, releases fluoride. | Good for small, low-stress areas; fluoride release; biocompatible. | Less durable, lower strength, not suitable for large chewing surfaces. | $75 - $250 |
| Inlay/Onlay | Lab-made partial crown (porcelain, composite, gold). | More durable than fillings, preserves more tooth than a full crown, aesthetic (porcelain). | Higher cost than fillings, requires two visits. | $600 - $1,500 |
| Crown | Full tooth coverage (porcelain, ceramic, gold, PFM). | Restores strength, protects weakened teeth, highly aesthetic (ceramic). | Higher cost, requires significant tooth reduction, two visits (usually). | $800 - $3,000+ |
| Bridge | Replaces 1-3 missing teeth using adjacent crowns. | Restores chewing and speech, aesthetic, fixed solution. | Requires preparation of healthy adjacent teeth, can be difficult to clean, higher cost. | $2,000 - $5,000+ (per unit) |
| Dental Implant | Titanium post replaces root, topped with crown. | Most durable, preserves bone, feels like natural tooth, no impact on adjacent teeth. | Highest cost, surgical procedure, longer treatment time. | $3,000 - $6,000+ (per implant) |
| Veneer | Thin shell covering front of tooth (porcelain, composite). | Highly aesthetic, immediate smile improvement, durable (porcelain). | Irreversible (tooth reduction), higher cost, prone to chipping/fracture if abused. | $800 - $2,500+ (per tooth) |
Note: Costs are estimates and can vary significantly based on location, dentist's fees, material used, and complexity of the case. Dental insurance typically covers a portion of restorative treatments, with coverage levels varying widely by plan.
Step-by-Step: What to Expect During Treatment
While each restoration type has specific steps, here's a general overview:
- Anesthesia: The dentist will numb the area around the tooth using a local anesthetic to ensure you are comfortable and feel no pain during the procedure.
- Tooth Preparation:
- For Fillings: Any decayed or damaged tooth structure is carefully removed using a dental drill. The area is then cleaned and shaped to receive the filling material.
- For Inlays/Onlays/Crowns/Veneers: More tooth structure may need to be removed to create space for the restoration. The tooth is precisely shaped to ensure the restoration fits properly and blends with your bite.
- Impression (for Indirect Restorations): After preparation, an impression (mold) of your tooth is taken. This can be done using traditional putty materials or with a digital scanner. This impression is sent to a dental lab, which fabricates your custom restoration.
- For single-visit crowns (CAD/CAM technology): The impression is digital, and the crown is milled right in the office.
- Temporary Restoration (for Indirect Restorations): While your custom restoration is being made (which can take 1-2 weeks), a temporary crown or filling will be placed to protect the prepared tooth.
- Bonding/Cementation:
- For Direct Fillings: The filling material (e.g., composite) is placed directly into the prepared tooth in layers, hardened with a special light, and then shaped and polished.
- For Indirect Restorations: Once the permanent restoration arrives from the lab, the temporary is removed. The dentist will try in the new restoration to ensure a perfect fit, bite, and appearance. If everything is satisfactory, it will be permanently bonded or cemented to your tooth.
- Adjustment and Polishing: The dentist will check your bite and make any necessary adjustments to ensure comfort and proper function. The restoration will then be polished smooth.
Recovery Timeline and Aftercare
The recovery period largely depends on the type and extent of the restoration:
- Fillings: You may experience mild sensitivity to hot/cold for a few days to a few weeks. The numbing will wear off within a few hours. You can usually eat normally once the numbness subsides.
- Crowns/Bridges/Inlays/Onlays: Sensitivity may last longer, especially if significant tooth preparation was done or if the tooth was close to the pulp. Avoid chewing hard or sticky foods on temporaries. Once permanent, it should feel like a natural tooth.
- Dental Implants: This involves a surgical procedure. Initial recovery involves managing swelling and discomfort for a few days with pain medication. The implant then needs several months (3-6) to integrate with the jawbone (osseointegration) before the final crown can be placed.
- General Aftercare:
- Pain Management: Over-the-counter pain relievers (ibuprofen, acetaminophen) are usually sufficient for mild discomfort.
- Oral Hygiene: Maintain excellent oral hygiene with regular brushing (twice daily) and flossing (once daily). Use a soft-bristled toothbrush.
- Diet: Avoid overly sticky, hard, or sugary foods, especially initially, to protect the new restoration.
- Follow-Up: Attend all scheduled follow-up appointments.
- Report Issues: Contact your dentist immediately if you experience severe pain, persistent sensitivity, swelling, a loose or fractured restoration, or a change in your bite.
Prevention Strategies
Preventing tooth damage is always preferable to restoring it.
- Excellent Oral Hygiene: Brush teeth twice daily with fluoride toothpaste for two minutes each time. Floss daily to remove plaque and food particles from between teeth.
- Regular Dental Check-ups and Cleanings: Visit your dentist every six months (or as recommended) for professional cleanings and examinations to catch problems early.
- Balanced Diet: Limit sugary and acidic foods and drinks. Opt for tooth-friendly foods like fresh fruits, vegetables, and dairy products. Drink plenty of water.
- Fluoride: Use fluoride toothpaste and consider fluoride rinses if recommended by your dentist. Fluoride strengthens enamel and makes it more resistant to decay.
- Dental Sealants: For children and sometimes adults, dental sealants can be applied to the chewing surfaces of back teeth to protect against decay in the grooves.
- Mouthguards: Wear a custom-fitted mouthguard during sports to protect against traumatic injuries. If you grind or clench your teeth (bruxism), a nightguard can prevent excessive wear and fracture.
Cost Ranges in the US (with/without Insurance)
The cost of dental restorations in the US varies significantly based on factors such as:
- Type of restoration and material used
- Complexity of the procedure
- Location (urban vs. rural, different states)
- Dentist's fees and expertise
General Cost Ranges (without insurance):
- Fillings:
- Amalgam: $50 - $200
- Composite: $100 - $450
- Inlays/Onlays: $600 - $1,500
- Crowns: $800 - $3,000+ (depending on material: porcelain, zirconia, gold)
- Bridges: $2,000 - $5,000+ (per unit, a 3-unit bridge could be $6,000-$15,000)
- Dental Implants: $3,000 - $6,000+ (per implant, excluding crown and abutment, which add another $1,000 - $3,000)
- Veneers: $800 - $2,500+ (per tooth, porcelain being more expensive than composite)
With Dental Insurance:
Most standard dental insurance plans offer some coverage for restorative procedures. Coverage typically falls into tiers:
- Preventive Care: (Cleanings, exams, X-rays) Often covered at 80-100%.
- Basic Restorative Care: (Fillings, simple extractions) Usually covered at 50-80%.
- Major Restorative Care: (Crowns, bridges, dentures, root canals) Typically covered at 30-50%.
- Dental Implants and Veneers: Coverage for implants is increasing but can be limited or subject to specific criteria. Veneers are often considered cosmetic and may not be covered at all, or only partially if deemed medically necessary (e.g., to restore function after trauma).
Patients will typically pay a deductible before coverage kicks in, and then a co-insurance percentage. Many plans also have an annual maximum benefit (e.g., $1,000 - $2,500 per year), which can quickly be met with more extensive restorative work. It's crucial to check with your specific insurance provider for exact coverage details.
For Parents / Pediatric Considerations
Restorations are just as important for children's primary (baby) teeth as for adult teeth.
- Early Intervention: Addressing cavities in primary teeth is vital to prevent pain, infection, and premature tooth loss, which can affect the alignment and eruption of permanent teeth.
- Pediatric Fillings: Similar to adults, composite and glass ionomer fillings are commonly used.
- Stainless Steel Crowns (SSCs): These are frequently used for severely decayed or fractured primary molars, especially after a pulp treatment. They are durable, cost-effective, and provide full coverage protection until the tooth naturally exfoliates.
- Dental Sealants: A highly effective preventive measure, sealants are thin plastic coatings applied to the chewing surfaces of back teeth to protect against decay in pits and fissures.
- Space Maintainers: If a primary tooth is lost prematurely due to extensive decay or trauma, a space maintainer may be placed to hold the space open for the permanent tooth, preventing crowding.
- Fluoride Varnish: Applied topically to strengthen enamel and prevent decay.
Frequently Asked Questions
Q: How much does a dental restoration cost?
A: The cost varies greatly depending on the type of restoration, materials used, the complexity of the case, and your geographic location. Simple fillings can range from $50-$450, while more complex procedures like crowns can be $800-$3,000+, and dental implants can run $3,000-$6,000+ per tooth for the implant itself. Dental insurance often covers a portion, typically 50-80% for basic restorations and 30-50% for major ones, up to an annual maximum.
Q: Is dental restoration painful?
A: No, dental restorations are typically not painful during the procedure because your dentist will use a local anesthetic to numb the area. You might feel some pressure or vibration, but no sharp pain. After the numbing wears off, it's common to experience some mild sensitivity or discomfort for a few days, which can usually be managed with over-the-counter pain relievers.
Q: How long do dental restorations last?
A: The lifespan of a restoration depends on its type, material, your oral hygiene habits, and your bite.
- Composite Fillings: 5-10 years
- Amalgam Fillings: 10-15+ years
- Crowns and Bridges: 10-15+ years
- Dental Implants: 20+ years to a lifetime with proper care.
- Veneers: 10-15 years Regular dental check-ups and good oral hygiene are crucial for maximizing the longevity of any restoration.
Q: Are there alternatives to dental restorations?
A: For existing damage, the primary alternatives are often limited.
- Prevention: The best "alternative" is to prevent damage in the first place through excellent oral hygiene, regular check-ups, and a healthy diet.
- No Treatment: For very small, non-progressing lesions, sometimes "watchful waiting" or fluoride therapy can be an option, but this risks progression to larger problems.
- Extraction: If a tooth is too severely damaged to be restored, extraction (removal) may be the only option. However, missing teeth can lead to further problems like bone loss and shifting of adjacent teeth, often necessitating replacement with a bridge, implant, or denture.
Q: Does dental insurance cover restorations?
A: Yes, most dental insurance plans cover a portion of restorative procedures. The coverage level varies widely:
- Basic restorations (like fillings) are typically covered at a higher percentage (50-80%).
- Major restorations (like crowns and bridges) usually have lower coverage (30-50%).
- Dental implants and veneers may have limited or no coverage, depending on the plan and whether they are deemed medically necessary or cosmetic. It's essential to check your specific plan's details regarding deductibles, co-insurance, and annual maximums.
Q: Can restorations fall out or break?
A: Yes, while designed to be durable, restorations can sometimes fall out, chip, or break. This can happen due to:
- Recurrent decay around or under the restoration.
- New trauma or excessive biting forces (e.g., bruxism).
- Wear and tear over time.
- Improper bonding or cementation. If a restoration comes loose or breaks, it's important to contact your dentist immediately to prevent further damage to the tooth or surrounding tissues.
Q: What's the difference between a filling and a crown?
A: The main difference lies in the extent of tooth damage and coverage:
- A filling is used for minor to moderate tooth decay or damage. It fills in the prepared cavity within the tooth structure, typically involving a smaller portion of the tooth.
- A crown (or cap) is used for more extensive damage, where a significant portion of the tooth is compromised, fractured, or has undergone a root canal. A crown covers the entire visible part of the tooth, providing full protection and restoring its strength and shape.
When to See a Dentist
Regular dental check-ups, ideally every six months, are crucial for early detection of problems before they become severe. Your dentist can identify small cavities or cracks that you might not notice, preventing the need for more complex restorations.
However, you should see a dentist immediately if you experience any of the following emergency signs:
- Severe or persistent toothache: Especially if it's throbbing, keeps you awake, or doesn't subside.
- Swelling: In your gums, face, or jaw, which could indicate a serious infection or abscess.
- Knocked-out tooth: Time is critical for successful re-implantation.
- Chipped, fractured, or broken tooth: Especially if it's painful, exposes the pulp, or creates sharp edges that cut your tongue/cheek.
- Loose or lost filling, crown, or bridge: This exposes vulnerable tooth structure and needs prompt attention.
- Pain when biting or chewing: Could indicate a crack, cavity, or issue with a restoration.
- Pus or discharge: Around a tooth or in the gums.
Ignoring dental issues can lead to increased pain, infection spreading to other parts of your body, and ultimately, the loss of the tooth. Early intervention through dental restoration is key to maintaining your oral health and overall well-being.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.