Occlusal
3,652 words · 12 min read
Quick Definition
Relating to the biting or chewing surface of posterior teeth (premolars and molars), or to the way the upper and lower teeth come together.
Occlusal: Understanding Your Bite and Its Impact on Dental Health
Welcome to SmilePedia.net, your definitive resource for all things dental! Today, we're diving deep into a fundamental concept that underpins much of dentistry: occlusal. Often heard in the dentist's office but perhaps not fully understood, "occlusal" is central to how your teeth function, how they wear, and even your overall well-being.
At its core, occlusal refers to the biting or chewing surface of your posterior teeth – your premolars and molars. More broadly, it describes the intricate relationship between your upper and lower teeth when they come together, whether you're chewing, swallowing, or simply resting your jaw. This interaction, known as your bite, is far more complex and critical than many realize. A healthy occlusal relationship ensures efficient chewing, clear speech, proper jaw function, and can prevent a host of painful and costly dental issues.
Why does this matter so much? Because even subtle imbalances in how your teeth meet can have a ripple effect throughout your entire oral system. From excessive tooth wear and sensitivity to persistent headaches and jaw pain, an improper bite can significantly impact your quality of life. Issues related to occlusion, collectively known as malocclusion, are remarkably common, affecting an estimated 60-75% of the US population to varying degrees. While some forms are mild and asymptomatic, others require intervention to prevent progressive damage and discomfort. Understanding your occlusal health is a proactive step toward a lifetime of comfortable chewing and a pain-free smile.
Key Takeaways:
- Occlusal pertains to the chewing surfaces of your back teeth and how all your teeth fit together.
- A proper bite (occlusion) is essential for effective chewing, clear speech, and preventing dental problems.
- Malocclusion, or an improper bite, is very common, affecting a large percentage of the US population.
- Untreated occlusal issues can lead to significant tooth wear, sensitivity, jaw pain (TMJ disorders), and even headaches.
- Diagnosis involves a thorough dental exam, X-rays, and sometimes advanced bite analysis tools.
- Treatment options range from simple occlusal adjustments to orthodontics, restorative work, or even surgery, depending on the severity.
Detailed Explanation of Occlusal Health
The world of occlusal health is vast, encompassing everything from the microscopic ridges on your molars to the complex movements of your jaw joint. Let's break down the crucial aspects.
Types and Classifications of Occlusion
Dentists classify occlusion to understand deviations from the ideal. The most widely used system is Angle's Classification of Malocclusion, which categorizes the relationship between the first permanent molars:
- Class I (Neutroclusion): This is considered the ideal or normal occlusion. The mesiobuccal cusp of the maxillary (upper) first molar aligns with the buccal groove of the mandibular (lower) first molar. While considered ideal, patients can still have other minor bite irregularities like crowding or spacing within Class I.
- Class II (Distocclusion or Overbite): In this classification, the mandibular first molar is positioned distally (further back) relative to the maxillary first molar. This often results in an overbite, where the upper front teeth significantly overlap the lower front teeth. It can also involve an overjet, where the upper front teeth protrude excessively forward over the lower teeth.
- Class III (Mesiocclusion or Underbite): Here, the mandibular first molar is positioned mesially (further forward) relative to the maxillary first molar. This typically leads to an underbite, where the lower front teeth extend beyond the upper front teeth.
Beyond Angle's classification, other important terms describe specific bite relationships:
- Crossbite: One or more upper teeth bite on the inside of the lower teeth. This can be anterior (front teeth) or posterior (back teeth), and can affect one side or both.
- Open Bite: A vertical gap exists between the upper and lower teeth when the jaw is closed, meaning some teeth do not make contact. This can also be anterior or posterior.
- Deep Bite: A severe overbite where the upper front teeth completely cover the lower front teeth, sometimes even biting into the gum tissue behind the lower teeth.
- Edge-to-Edge Bite: The incisal (biting) edges of the upper and lower front teeth meet directly.
- Functional Occlusion: Refers to the dynamic contact between teeth during chewing and other jaw movements. This is arguably more important than static occlusion, as most tooth wear and damage occur during functional movements.
- Static Occlusion: The way teeth contact when the jaw is fully closed in a resting position.
Causes and Risk Factors for Occlusal Problems
A perfect bite is somewhat rare, and many factors can contribute to developing an occlusal issue:
- Genetics and Heredity: Jaw size, tooth size, and the general arrangement of teeth are often inherited traits. If parents have a specific type of malocclusion, their children are more likely to develop it.
- Childhood Habits:
- Thumb-sucking or prolonged pacifier use: Can push developing teeth out of alignment, leading to open bites or excessive overjets.
- Tongue thrusting: Where the tongue pushes against the front teeth during swallowing, can also cause an open bite.
- Mouth breathing: Can alter jaw development and lead to narrow arches and crossbites.
- Premature Tooth Loss: If a primary (baby) tooth is lost too early, the adjacent teeth can drift into the empty space, preventing the permanent tooth from erupting correctly.
- Impacted or Missing Teeth: Teeth that fail to erupt (impacted) or are congenitally missing can disrupt the natural alignment of the dental arch.
- Dental Restorations: Poorly placed or ill-fitting fillings, crowns, or bridges can alter the bite, causing premature contact points that lead to wear or pain.
- Trauma: Injuries to the face or jaw can shift teeth or damage the jaw joint, affecting occlusion.
- Temporomandibular Joint (TMJ) Disorders: Problems with the jaw joint itself can manifest as occlusal issues, or conversely, occlusal problems can exacerbate TMJ disorders.
- Bruxism (Teeth Grinding/Clenching): This involuntary habit, often stress-related, places immense force on the teeth and jaw, leading to significant wear, fractures, and changes in the bite over time.
Signs and Symptoms to Watch For
Recognizing the signs of occlusal problems early can prevent more severe complications. Pay attention to:
- Excessive Tooth Wear: Flat spots, chips, cracks, or shortening of teeth, especially the incisal edges of front teeth or the cusps of back teeth. This is often a tell-tale sign of bruxism or a destructive bite pattern.
- Tooth Sensitivity: Constant or intermittent pain when eating hot, cold, or sweet foods, often due to exposed dentin from wear or cracks.
- Pain in the Jaw, Face, Head, or Neck: Persistent headaches, earaches (without infection), or general facial pain can be symptoms of an unbalanced bite or underlying TMJ issues.
- Clicking, Popping, or Grating Sounds in the Jaw: These noises, particularly when opening or closing the mouth, indicate potential problems with the TMJ.
- Difficulty Chewing or Biting: You might find it hard to properly tear or grind food, or experience discomfort while eating.
- Gum Recession or Abfraction Lesions: Notches near the gum line of teeth, often appearing as "V" or "wedge" shapes, can be caused by excessive biting forces flexing the tooth.
- Fractured Teeth or Restorations: Repeated breakage of fillings, crowns, or even natural teeth can signal excessive stress from an improper bite.
- Loose Teeth (Mobility): While often associated with gum disease, excessive occlusal forces can also contribute to tooth mobility.
- Difficulty with Speech: Certain speech impediments can be linked to misaligned teeth or jaw positions.
Diagnosis Process — What Your Dentist Does
Diagnosing occlusal issues requires a comprehensive approach. Your dentist will act as a detective, gathering clues from various sources:
- Thorough Clinical Examination:
- Visual Inspection: Your dentist will carefully examine your teeth for signs of wear, cracks, fractures, or recession.
- Palpation: They will gently feel your jaw muscles and TMJ for tenderness, clicking, or limited movement.
- Occlusal Assessment: Using articulating paper (a thin, colored paper), they will have you bite down to identify premature or heavy contact points. They might also assess your bite in various jaw movements.
- Tooth Mobility Check: Each tooth will be gently wiggled to check for abnormal looseness.
- Dental X-rays:
- Periapical X-rays: Provide detailed images of individual teeth and surrounding bone.
- Bitewing X-rays: Show the crowns of upper and lower teeth, revealing interproximal cavities and bone levels.
- Panoramic X-ray: Offers a broad view of the entire mouth, including all teeth, jaws, and TMJs.
- Cephalometric X-ray: A specialized X-ray that shows the side view of the head, used primarily for orthodontic assessment of skeletal relationships.
- Cone Beam Computed Tomography (CBCT): A 3D imaging technique for more complex cases, especially involving the TMJ or impacted teeth.
- Dental Impressions and Models: Impressions of your upper and lower teeth are taken to create plaster models (casts). These models can be mounted on an articulator, a device that simulates jaw movements, allowing the dentist to study your bite outside of your mouth.
- Digital Occlusal Analysis (e.g., T-Scan): For more precise analysis, some dentists use digital bite registration systems. These devices measure the force and timing of occlusal contacts, providing a detailed visual map of your bite.
- TMJ Evaluation: This might involve specific tests for jaw range of motion, muscle tenderness, and listening for joint sounds.
Treatment Options with Pros, Cons, and Costs
Addressing occlusal problems requires a tailored approach based on the specific diagnosis.
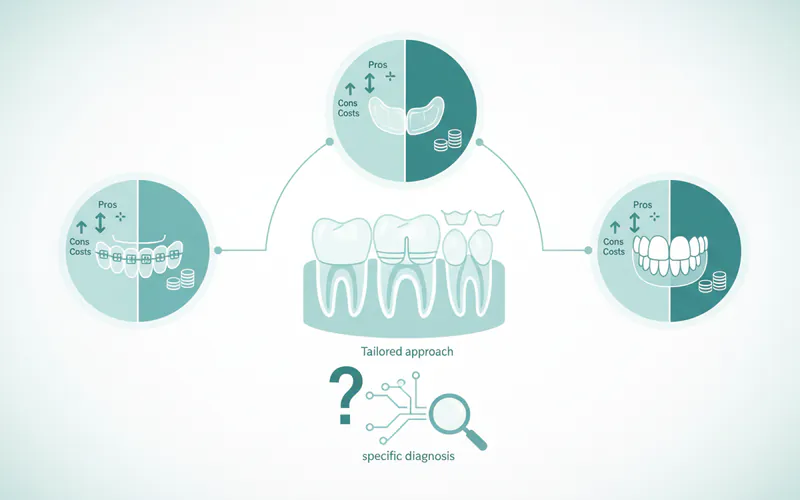
| Treatment Option | Description | Pros | Cons | Typical US Cost (without insurance) |
|---|---|---|---|---|
| Occlusal Adjustment (Equilibration) | Selective reshaping (grinding) of small amounts of tooth enamel to eliminate premature or excessive contact points. | Non-invasive, quick, often immediate relief for minor issues. | Irreversible, requires skilled hand, limited scope for severe issues, can cause temporary sensitivity. | $150 - $500 |
| Occlusal Splints / Nightguards | Custom-fitted acrylic device worn over teeth, usually at night, to protect teeth from grinding/clenching and stabilize the bite. | Non-invasive, protective, can relieve muscle pain, reversible. | Requires patient compliance, doesn't correct underlying skeletal issues, can be lost or broken. | $300 - $800 |
| Orthodontics (Braces/Aligners) | Use of braces, clear aligners (e.g., Invisalign), or other appliances to gradually shift teeth into proper alignment. | Comprehensive correction of misaligned teeth and bite. | Time-consuming (months to years), can be visible (braces), requires diligence with aligners, discomfort. | $3,000 - $8,000+ |
| Restorative Dentistry | Using fillings, crowns, bridges, or veneers to rebuild worn-down teeth, replace missing teeth, or reshape teeth for better bite. | Restores form, function, and aesthetics; durable solutions. | Can be extensive, multiple appointments, cost varies greatly per procedure, some procedures are invasive. | $200 (filling) - $3,000 (crown) per tooth |
| TMJ Therapy | Physiotherapy, medication, stress management, botox injections, or specialized splints to manage jaw joint pain. | Targets pain and dysfunction, often non-invasive. | May require ongoing management, doesn't always address underlying bite issues directly. | $50 - $300 per session/injection |
| Orthognathic Surgery (Jaw Surgery) | Surgical repositioning of the upper jaw, lower jaw, or both, to correct severe skeletal discrepancies. | Definitive correction for severe skeletal malocclusion. | Invasive, significant recovery time, high cost, potential risks of surgery. | $20,000 - $50,000+ |
Step-by-Step: What to Expect During Treatment (Focusing on Occlusal Adjustment)
If your dentist recommends an occlusal adjustment, here's a general overview of what to expect:
- Initial Assessment: Your dentist will use articulating paper to mark all contact points between your upper and lower teeth when you bite down in various positions. This helps identify areas of premature or excessive contact.
- Selective Reshaping: Using a high-speed handpiece with very fine burs, your dentist will gently and precisely remove microscopic amounts of enamel from the identified "high spots." This is done incrementally.
- Re-evaluation: After each adjustment, you'll bite down on articulating paper again to check the new contact pattern. The process is repeated until a balanced and harmonious bite is achieved, where all teeth make even contact simultaneously.
- Polishing: Once the adjustment is complete, the treated tooth surfaces will be polished smooth.
- Post-Treatment Check: Sometimes, a follow-up appointment is needed a few weeks later to ensure the bite remains comfortable and stable.
Occlusal adjustments are generally painless, as only enamel (which has no nerves) is removed. You might feel a slight vibration or pressure. For more complex cases involving widespread wear or multiple teeth, the process might be spread over a few appointments.
Recovery Timeline and Aftercare
Recovery largely depends on the type of treatment received:
- Occlusal Adjustment: Recovery is immediate. You might experience mild, temporary tooth sensitivity to hot or cold for a few days, which usually resolves on its own. Avoid extremely hard or sticky foods if sensitivity persists.
- Occlusal Splints/Nightguards: There's no recovery period. It may take a few nights to adjust to wearing the appliance. It's crucial to clean the guard daily and follow your dentist's instructions for wear.
- Orthodontics: Initial discomfort and soreness are common after adjustments or new aligner trays. This usually subsides within a few days. You'll need to follow dietary restrictions (avoid sticky, hard foods) and maintain meticulous oral hygiene.
- Restorative Dentistry: Recovery varies. A new filling might cause temporary sensitivity. A crown or bridge might require a few days to adjust to the new bite. Follow post-operative instructions for pain management and diet.
- Orthognathic Surgery: This is the most intensive. Recovery can take several weeks to months, involving a liquid or soft diet, pain management, and physical therapy.
Regardless of the treatment, regular follow-up appointments with your dentist are crucial to monitor progress and ensure the long-term stability of your bite.
Prevention Strategies
While some occlusal problems are genetic, many can be prevented or mitigated:
- Regular Dental Check-ups: Biannual visits allow your dentist to detect early signs of wear, malocclusion, or bruxism before they become severe.
- Good Oral Hygiene: Brushing and flossing prevent cavities and gum disease, which can destabilize teeth and impact your bite.
- Early Intervention for Childhood Habits: Address thumb-sucking, pacifier use, or tongue thrusting early with your pediatric dentist. Orthodontic evaluations for children are recommended around age 7 or 8 to identify and potentially intercept developing bite issues.
- Promptly Replace Missing Teeth: Gaps from missing teeth can cause adjacent teeth to shift, leading to bite instability. Dental implants, bridges, or partial dentures can prevent this.
- Wear a Mouthguard for Sports: Protect your teeth and jaws from traumatic injuries.
- Manage Stress: Stress is a major trigger for bruxism. Incorporate stress-reduction techniques like meditation, exercise, or therapy into your routine.
- Be Mindful of Your Bite: If you notice new clicking sounds, jaw pain, or changes in how your teeth meet, consult your dentist promptly.
Cost Ranges in the US (with/without Insurance)
The cost of occlusal treatment varies dramatically based on the complexity, the specific procedure, and your geographic location.
- Occlusal Adjustment: $150 - $500. Some dental insurance plans may cover a portion if deemed medically necessary.
- Occlusal Splint/Nightguard: $300 - $800. Many dental insurance plans offer partial coverage, especially if a diagnosis of bruxism or TMD is present.
- Orthodontics (Braces/Aligners): $3,000 - $8,000+. Some dental insurance plans, particularly those with orthodontic benefits, will cover a percentage (e.g., 50%) up to a lifetime maximum. Child-specific plans often have better orthodontic coverage.
- Restorative Dentistry:
- Fillings: $100 - $400 per tooth (depending on material and size).
- Crowns: $800 - $3,000 per tooth.
- Bridges: $2,000 - $5,000 per unit.
- Insurance typically covers 50-80% of these costs after deductibles are met.
- TMJ Therapy: Can range from $50 - $300 per session for physical therapy or injections. Splints are covered separately. Medical insurance may cover some aspects if linked to a medical diagnosis of TMD.
- Orthognathic Surgery: $20,000 - $50,000+. This is often covered by medical insurance if it's deemed medically necessary to correct a functional problem (e.g., severe difficulty eating or breathing), rather than purely cosmetic.
It's crucial to discuss all estimated costs with your dental provider and insurance company beforehand. Many offices offer payment plans or third-party financing options to make treatment more affordable.
For Parents / Pediatric Considerations
Occlusal health starts early, and parents play a vital role in monitoring their child's developing bite.
- Early Orthodontic Evaluation: The American Association of Orthodontists recommends that children have their first orthodontic check-up by age 7. At this age, the orthodontist can identify subtle problems with jaw growth and erupting permanent teeth. Early (Phase I) treatment can often prevent more serious issues later, guiding jaw growth and making space for permanent teeth.
- Habit Cessation: Intervening to stop prolonged thumb-sucking, pacifier use, or tongue thrusting before age 4-5 is crucial. Your dentist can offer strategies and appliances to help.
- Space Maintainers: If a primary (baby) tooth is lost prematurely due to decay or injury, a space maintainer can be placed to hold the space open for the permanent tooth, preventing adjacent teeth from drifting and causing future crowding or impaction.
- Monitoring Tooth Eruption: Keep an eye on how your child's permanent teeth are erupting. If you notice severe crowding, unusual eruption patterns, or if baby teeth are not falling out as expected, consult your dentist.
Addressing occlusal issues in childhood can simplify treatment, reduce costs, and improve long-term oral health outcomes.
Frequently Asked Questions
Is occlusal adjustment painful?
Generally, no. Occlusal adjustment involves removing only microscopic amounts of enamel, which has no nerve endings. You might feel a slight vibration or pressure, and some temporary sensitivity to hot or cold foods can occur for a few days afterward, but it typically subsides quickly.
How long does occlusal treatment take?
The duration varies widely depending on the chosen treatment. An occlusal adjustment might be completed in one to two appointments, each lasting 30-60 minutes. Wearing an occlusal splint is ongoing, typically nightly. Orthodontic treatment (braces or aligners) usually takes 18-36 months. Restorative work can range from a single appointment for a filling to several for complex crowns or bridges. Orthognathic surgery involves a lengthy preparation phase and several months of recovery.
Can malocclusion fix itself?
Rarely. While a very minor bite issue might not worsen significantly, most forms of malocclusion, especially those involving skeletal discrepancies or destructive habits like bruxism, tend to worsen over time if left untreated. This can lead to increased tooth wear, pain, and more complex treatment needs in the future.
What are the alternatives to braces for malocclusion?
For many mild to moderate cases, clear aligners (like Invisalign) offer a less noticeable alternative to traditional braces. For purely aesthetic concerns where the underlying bite isn't severely problematic, veneers can cosmetically improve the appearance of misaligned teeth, but they don't correct the actual bite. For severe skeletal malocclusion, orthognathic surgery combined with orthodontics is often the only definitive solution.
Will insurance cover occlusal treatment?
Coverage depends on your specific dental and medical insurance plans, and the nature of the treatment.
- Occlusal adjustments and splints may be partially covered if deemed medically necessary (e.g., for bruxism or TMJ disorder).
- Orthodontics often has a separate benefit with a lifetime maximum, especially for children. Some adult plans offer limited coverage.
- Restorative treatments (fillings, crowns) are typically covered 50-80% for major procedures.
- Orthognathic surgery may be covered by medical insurance if it addresses a functional impairment. Always check with your insurance provider and dental office for a pre-treatment estimate.
What happens if occlusal issues are left untreated?
Ignoring occlusal problems can lead to a cascade of worsening issues:
- Progressive tooth wear and fractures.
- Chronic tooth sensitivity.
- Increased risk of cavities and gum disease due to uneven wear or difficulty cleaning.
- Worsening TMJ disorders, leading to chronic jaw pain, headaches, and limited jaw function.
- Chewing difficulties and digestive problems.
- Altered facial aesthetics.
- Potentially costly and extensive dental work required to repair damage later.
Is an occlusal guard the same as a nightguard?
Yes, these terms are often used interchangeably. Both refer to custom-fitted oral appliances worn over the teeth, typically at night, to protect against the damaging effects of bruxism (teeth grinding and clenching) and to help stabilize the jaw joint in cases of TMJ disorders. While some over-the-counter options exist, a custom-fitted occlusal guard from your dentist offers superior protection and comfort.
When to See a Dentist
Given the potential long-term impact of occlusal problems, knowing when to seek professional help is important:
- Routine Dental Check-ups: Your dentist regularly assesses your bite during your biannual visits, often catching issues before you even notice symptoms.
- Persistent Pain: If you experience ongoing pain in your jaw, face, head, neck, or teeth without a clear cause, especially if it worsens when chewing or after waking up.
- Jaw Sounds: Any new or worsening clicking, popping, or grating sounds in your jaw when you open or close your mouth.
- Changes in Your Bite: If you suddenly notice your teeth don't fit together the same way, or if chewing feels different or difficult.
- Visible Tooth Damage: If you see excessive wear, chips, cracks, or unexplained sensitivity in your teeth.
- Difficulty with Jaw Movement: If you find it hard to open your mouth wide, or your jaw locks.
Don't wait for severe pain or extensive damage. Early detection and intervention are key to maintaining a healthy, functional bite and a comfortable smile for life.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.