Swollen Gums Treatment at Home: Complete Guide

Key Takeaways
- More than 50% of American adults over 30 suffer from some form of gum disease, often starting with the common and often overlooked issue of swollen gums. While it might seem like a minor annoyance, swollen gums are your body's alarm bell, signaling underlying inflammation and potential oral heal
More than 50% of American adults over 30 suffer from some form of gum disease, often starting with the common and often overlooked issue of swollen gums. While it might seem like a minor annoyance, swollen gums are your body's alarm bell, signaling underlying inflammation and potential oral health problems that, if left unaddressed, can escalate into serious conditions like periodontitis, leading to tooth loss. If you're experiencing puffy, tender, or bleeding gums, you're likely searching for effective swollen gums treatment at home options to alleviate discomfort and restore gum health. This comprehensive guide from SmilePedia.net will equip you with medically accurate, practical advice on managing and improving swollen gums from the comfort of your home, while also knowing when professional dental care is essential. We'll delve into the causes, symptoms, best home remedies, prevention strategies, and vital information about professional treatments, costs, and recovery, empowering you to take control of your gum health.
Key Takeaways:
- Gingivitis is the primary cause: Most cases of swollen gums stem from gingivitis, an early and reversible form of gum disease caused by plaque buildup.
- Effective home remedies include: Saltwater rinses, hydrogen peroxide rinses, proper brushing/flossing, and certain herbal applications like aloe vera, offering significant gum pain relief.
- Prevention is key: Consistent oral hygiene (brushing twice daily, flossing daily), a balanced diet, and regular dental check-ups are crucial to prevent swollen gums and advanced gum disease.
- Professional intervention: If home treatments don't resolve symptoms within 7-10 days, or if you experience severe pain, persistent bleeding, or loose teeth, immediate dental consultation is necessary. Professional cleaning (scaling and root planing) can cost $150-$400 per quadrant without insurance.
- Timelines: Initial improvement with home remedies can be seen within 3-7 days, but complete resolution of gingivitis may take 2-4 weeks of diligent care. Advanced periodontitis requires professional treatment and a longer recovery.
- Cost of home care: Most home remedies cost less than $20 for supplies (salt, hydrogen peroxide, soft toothbrush), making them highly accessible for initial relief.
What Are Swollen Gums? An Overview
Swollen gums, medically known as gingival inflammation or gingivitis, occur when the gum tissue surrounding your teeth becomes enlarged, puffy, and sometimes tender or painful. This inflammation is typically a response to an irritant, most commonly plaque — a sticky film of bacteria that constantly forms on your teeth. When plaque isn't adequately removed, it hardens into tartar, which further irritates the gums and creates an environment where more bacteria can thrive.

Healthy gums are firm, pink, and fit snugly around your teeth. Swollen gums, in contrast, may appear red, purplish, or bluish, feel soft and spongy to the touch, and often bleed easily, especially during brushing or flossing. While swollen gums are a common complaint, they are a significant indicator of gum disease progression and should never be ignored. Early detection and treatment, often starting with swollen gums treatment at home, are crucial to prevent the condition from advancing to more severe forms of periodontal disease that can lead to irreversible damage and tooth loss.
Types of Gum Inflammation and Related Conditions
While "swollen gums" often refers to gingivitis, understanding the nuances of gum inflammation helps in identifying the severity and appropriate treatment.
Gingivitis
This is the most common and mildest form of gum disease, characterized by inflammation of the gums (gingiva) without loss of the bone or tissue supporting the teeth. It's almost always caused by poor oral hygiene leading to plaque accumulation.
- Symptoms: Red, swollen, tender gums that bleed easily.
- Reversibility: Fully reversible with proper oral hygiene and professional cleaning. This is where most swollen gums treatment at home remedies are effective.
Periodontitis
If gingivitis is left untreated, it can advance to periodontitis. This is a more severe infection that spreads below the gum line, affecting the bone and tissues that support your teeth.
- Symptoms: Deep pockets forming between teeth and gums, persistent bad breath, pus between teeth and gums, receding gums, loose teeth, changes in bite, eventual tooth loss.
- Reversibility: Not fully reversible in terms of tissue and bone loss, but its progression can be halted and managed with professional treatment. Home care plays a supportive role but cannot cure periodontitis.
Other Causes of Gum Swelling
Beyond plaque-induced gingivitis, other factors can cause localized or generalized gum swelling:
- Abscess: A localized collection of pus, usually due to a bacterial infection, which can cause significant swelling and pain in a specific area of the gum.
- Pericoronitis: Inflammation and swelling of the gum tissue surrounding a partially erupted tooth, most commonly wisdom teeth.
- Trauma: Physical injury to the gums, such as aggressive brushing, a burn from hot food, or an accidental poke.
- Allergic Reactions: Reactions to ingredients in toothpaste, mouthwash, or certain foods.
- Nutritional Deficiencies: Severe deficiency of Vitamin C (scurvy) or Vitamin K can lead to bleeding and swollen gums.
- Hormonal Changes: Puberty, menstruation, pregnancy, and menopause can increase gum sensitivity and inflammation due to fluctuating hormone levels.
- Medications: Certain drugs (e.g., anti-seizure medications, calcium channel blockers, immunosuppressants) can cause drug-induced gingival overgrowth, where gum tissue becomes excessively enlarged.
- Systemic Diseases: Conditions like diabetes, Crohn's disease, and certain blood disorders can manifest with gum symptoms.
- Ill-fitting Dental Appliances: Braces, dentures, or partials that rub or put pressure on the gums can cause localized irritation and swelling.
Causes: Why Your Gums Swell
Understanding the root causes of swollen gums is the first step toward effective prevention and treatment. While plaque accumulation is the most common culprit, several factors can contribute to or exacerbate the problem.
1. Plaque and Tartar Buildup (Gingivitis)
This is by far the leading cause. When you don't brush and floss regularly, bacteria in your mouth form a sticky film called plaque on your teeth. These bacteria release toxins that irritate the gum tissue, leading to inflammation, redness, swelling, and bleeding – the hallmark signs of gingivitis. If plaque isn't removed, it hardens into tartar (calculus), a rough deposit that further irritates the gums and provides a porous surface for more plaque to accumulate, perpetuating the cycle of inflammation.
2. Poor Oral Hygiene
Inadequate or incorrect brushing and flossing allow plaque to accumulate. Brushing too aggressively can also cause gum irritation and recession, making them more susceptible to inflammation. The ADA recommends brushing for two minutes, twice a day, and flossing once daily.
3. Hormonal Fluctuations
- Pregnancy: "Pregnancy gingivitis" is common due to increased hormone levels (progesterone and estrogen) that make gums more sensitive to plaque bacteria, leading to increased inflammation and bleeding.
- Menstruation/Puberty: Similar hormonal shifts can cause temporary gum swelling and sensitivity.
- Menopause: Hormonal changes can lead to dry mouth and increased gum sensitivity.
4. Nutritional Deficiencies
A lack of essential vitamins, particularly Vitamin C and Vitamin K, can compromise gum health. Vitamin C is vital for tissue repair and collagen production, and its deficiency can lead to scurvy, characterized by severely swollen, bleeding gums. Vitamin K is crucial for blood clotting, and its deficiency can exacerbate gum bleeding.
5. Certain Medications
Some medications can cause side effects that impact gum health:
- Anticonvulsants (e.g., phenytoin): Can cause gingival overgrowth (hyperplasia).
- Calcium channel blockers (e.g., nifedipine, amlodipine): Also linked to gingival overgrowth.
- Immunosuppressants (e.g., cyclosporine): Can lead to similar gum enlargement.
- Oral contraceptives: May contribute to gum sensitivity.
6. Dry Mouth (Xerostomia)
Saliva plays a crucial role in washing away food particles and neutralizing acids produced by bacteria. Reduced saliva flow, often a side effect of medications, aging, or certain medical conditions, can lead to increased plaque buildup and a higher risk of gum inflammation.
7. Tobacco Use
Smoking or using smokeless tobacco significantly increases your risk of developing gum disease. Tobacco restricts blood flow to the gums, impairs the immune system's ability to fight infection, and hinders the healing process, making it harder to recover from gingivitis.

8. Systemic Diseases
Certain medical conditions can weaken the immune system or affect the body's response to infection, making gums more vulnerable:
- Diabetes: Poorly controlled blood sugar levels can impair the body's ability to fight off bacterial infections, including those in the gums.
- Leukemia: This cancer affects blood cells and can cause swollen, bleeding gums.
- Crohn's Disease and other autoimmune disorders: Can manifest with oral symptoms, including gum inflammation.
9. Ill-fitting Dental Restorations or Appliances
Crowns, fillings, dentures, or braces that don't fit correctly can irritate gum tissue, create plaque traps, and contribute to localized inflammation.
10. Allergic Reactions
Occasionally, an allergic reaction to ingredients in toothpaste, mouthwash, or even certain foods can cause localized or generalized gum swelling and irritation.
Signs and Symptoms: What to Look For
Recognizing the signs and symptoms of swollen gums early is vital for effective swollen gums treatment at home and knowing when to seek professional help. Healthy gums are typically pale pink, firm, and do not bleed easily.
Here's what to look for if you suspect your gums are swollen:
- Redness or Darkening: Healthy gums are pink. Inflamed gums often appear bright red, purplish, or bluish. This change in color indicates increased blood flow due to inflammation.
- Swelling and Puffiness: The most obvious sign. Gums may appear enlarged, puffy, or bulging around the teeth. They might also look rounded or bulbous instead of firm and contoured.
- Tenderness or Pain: Swollen gums can be sensitive or painful to the touch, especially when brushing, flossing, or eating. You might experience a persistent dull ache.
- Bleeding Gums: One of the earliest and most common symptoms of gingivitis. Your gums might bleed easily when brushing, flossing, or even biting into hard foods.
- Receding Gums: While less common in early gingivitis, persistent inflammation can eventually lead to the gums pulling away from the teeth, making the teeth appear longer. This also exposes the sensitive tooth roots.
- Bad Breath (Halitosis): The accumulation of bacteria and food particles in inflamed gum pockets can produce volatile sulfur compounds, leading to chronic bad breath that doesn't resolve with brushing.
- Shiny Appearance: Inflamed gums can sometimes look shiny or glossy due to fluid retention and swelling.
- Loose Teeth: This is a sign of advanced gum disease (periodontitis), where the underlying bone supporting the teeth is compromised. If you notice your teeth feeling loose, see a dentist immediately.
- Pus Between Teeth and Gums: Another serious sign of infection, indicating periodontitis. This requires immediate professional intervention.
- Changes in Bite: As gum disease progresses, it can affect the stability of your teeth, potentially causing your bite to feel different or your teeth to shift.
Pro Tip: Pay close attention to how your gums feel and look during your daily oral hygiene routine. Any persistent change from their normal, healthy state warrants attention. Early intervention, often through swollen gums treatment at home, can prevent minor issues from becoming major problems.
``
Swollen Gums Treatment at Home: Effective Strategies
Addressing swollen gums early, particularly those caused by gingivitis, often involves diligent swollen gums treatment at home. These methods focus on reducing inflammation, controlling bacterial plaque, and promoting healing.
1. Improve Oral Hygiene (The Foundation)
This is the most critical step for treating and preventing plaque-induced swollen gums.
- Brush Twice Daily: Use a soft-bristled toothbrush and fluoride toothpaste. Brush gently in circular motions, paying attention to the gum line. Avoid aggressive scrubbing, which can further irritate gums. Replace your toothbrush every 3-4 months, or sooner if bristles are splayed. Consider an electric toothbrush for more effective plaque removal.
- Floss Daily: Flossing removes food particles and plaque from between your teeth and under the gum line where your toothbrush can't reach. Use a fresh section of floss for each tooth.
- Tongue Cleaning: Gently brush or scrape your tongue to remove bacteria that contribute to bad breath and can migrate to gums.
2. Saltwater Rinses
A classic and highly effective home remedy. Salt acts as a natural disinfectant and helps reduce inflammation.
- Process: Mix 1/2 teaspoon of salt in 8 ounces of warm water. Swish the solution around your mouth for 30-60 seconds, then spit it out. Do this 2-3 times a day.
- Benefits: Reduces bacteria, soothes irritated tissues, helps heal minor sores.
- Cost: Minimal (less than $5 for a box of salt).
3. Hydrogen Peroxide Rinse
Hydrogen peroxide is an antiseptic that can help kill bacteria and reduce gum inflammation. It's particularly useful for addressing gum pain relief by targeting the bacterial cause.
- Process: Mix equal parts 3% hydrogen peroxide with water (e.g., 1 tablespoon peroxide to 1 tablespoon water). Swish for 30 seconds, then spit thoroughly. Do not swallow. Limit use to 2-3 times a week, as overuse can cause irritation.
- Benefits: Kills bacteria, reduces plaque, helps whiten teeth over time.
- Cost: Low (approx. $1-$5 for a bottle).
4. Warm and Cold Compresses
These can provide symptomatic gum pain relief.
- Warm Compress: Apply a warm, damp cloth to your face over the swollen gum area to help relieve pain and increase blood flow, promoting healing.
- Cold Compress: For immediate numbing and reduction of swelling, a cold compress or ice pack applied externally can be effective.
- Process: Apply for 10-15 minutes at a time, several times a day.
- Benefits: Reduces pain and swelling.
- Cost: None.
5. Herbal Remedies (with caution)
Several natural substances have anti-inflammatory and antiseptic properties, but their scientific evidence varies. Always consult your dentist before relying heavily on herbal remedies, especially if you have existing conditions or are on medication.
- Aloe Vera: Known for its soothing and anti-inflammatory properties.
- Process: Apply pure aloe vera gel directly to the swollen gums, or use an aloe vera mouthwash.
- Benefits: Soothes inflammation, promotes healing.
- Cost: Varies, $5-$15 for a bottle of gel/mouthwash.
- Turmeric Paste: Turmeric contains curcumin, a potent anti-inflammatory compound.
- Process: Mix a small amount of turmeric powder with water to form a paste. Apply it to the gums and leave for 5-10 minutes before rinsing.
- Benefits: Reduces inflammation, antiseptic.
- Cost: Low ($5-$10 for a container of powder).
- Tea Tree Oil (Diluted): Has antiseptic and anti-inflammatory properties.
- Process: Add 1-2 drops of pure tea tree oil to a cup of warm water and use as a mouth rinse. Never swallow tea tree oil. Do not apply undiluted oil directly to gums, as it can be irritating.
- Benefits: Kills bacteria, reduces inflammation.
- Cost: Moderate ($10-$20 for a bottle of essential oil).
- Clove Oil: Traditionally used for toothache and gum pain relief due to its eugenol content (a natural anesthetic).
- Process: Dilute a few drops of clove oil in a carrier oil (like olive oil) and gently dab onto the affected area with a cotton swab.
- Benefits: Provides temporary pain relief, antiseptic.
- Cost: Moderate ($10-$20 for a bottle of essential oil).
6. Over-the-Counter Pain Relievers
For temporary gum pain relief, OTC medications can be helpful.
- NSAIDs (Nonsteroidal Anti-Inflammatory Drugs): Ibuprofen (Advil, Motrin) or naproxen (Aleve) can reduce pain and inflammation.
- Acetaminophen (Tylenol): Can help with pain, but does not reduce inflammation.
- Topical Gels: Over-the-counter numbing gels containing benzocaine (e.g., Orajel) can provide temporary localized pain relief.
- Cost: Low ($5-$15 per bottle/tube).
7. Nutritional Adjustments
- Increase Vitamin C: Found in citrus fruits, bell peppers, broccoli, and strawberries. Vitamin C is crucial for gum tissue repair and immunity.
- Increase Vitamin K: Found in leafy green vegetables like spinach and kale. Vitamin K aids in blood clotting and can help reduce gum bleeding.
- Avoid Sugary and Acidic Foods: These can contribute to plaque formation and irritate sensitive gums.
- Stay Hydrated: Drinking plenty of water helps rinse away food particles and bacteria, and prevents dry mouth.

Pro Tip: Consistency is key for any home treatment. Diligent adherence to improved oral hygiene and chosen home remedies for 7-10 days can significantly reduce symptoms of gingivitis.
Step-by-Step Process for Home Treatment
Here’s a structured approach to applying swollen gums treatment at home for general gingivitis:
- Assess Your Gums: Start by gently examining your gums in a mirror. Note the areas that are red, swollen, or appear to be bleeding. This helps you focus your efforts.
- Improve Brushing Technique (Day 1 onwards):
- Use a soft-bristled toothbrush.
- Brush for two minutes, twice a day, using gentle, circular motions.
- Angle the brush at 45 degrees towards the gum line to clean effectively without irritation.
- Ensure you clean all surfaces of your teeth and your tongue.
- Floss Daily (Day 1 onwards):
- Gently slide floss between each tooth.
- Curve the floss into a C-shape against one tooth, slide it gently under the gum line, and move it up and down. Repeat for the adjacent tooth.
- Be extra gentle if your gums bleed, but don't stop flossing; it's crucial for removing the irritants.
- Implement Saltwater Rinses (Immediately):
- Mix 1/2 teaspoon of salt in 8 oz of warm water.
- Swish for 30-60 seconds after brushing and after meals.
- Repeat 2-3 times daily for at least a week.
- Consider Hydrogen Peroxide Rinse (Optional, after a few days):
- If saltwater isn't providing enough relief or if you suspect a higher bacterial load.
- Mix equal parts 3% hydrogen peroxide and water. Swish for 30 seconds, 1-2 times daily, but no more than 2-3 times a week. Spit thoroughly.
- Apply Compresses for Pain Relief (As Needed):
- Use a warm compress for a soothing effect, or a cold compress for numbing, applied externally to the face for 10-15 minutes.
- Monitor Your Diet:
- Reduce sugary snacks and drinks.
- Increase intake of Vitamin C and K-rich foods.
- Drink plenty of water throughout the day.
- Observe for Improvement:
- You should start to see some reduction in redness and swelling, and less bleeding, within 3-7 days.
- Full resolution of gingivitis can take 2-4 weeks of consistent effort.
- When to Seek Professional Help: If, after 7-10 days of diligent home care, your symptoms haven't improved, worsen, or you experience new severe symptoms (like severe pain, pus, or loose teeth), it's crucial to schedule a dental appointment.
Professional Treatment Options
While swollen gums treatment at home is effective for mild gingivitis, more severe cases or underlying issues require professional dental intervention.
1. Professional Dental Cleaning (Prophylaxis)
- What it is: A routine dental cleaning performed by a dental hygienist. It involves removing plaque and tartar deposits from above the gum line and slightly below it using specialized instruments.
- When it's used: For healthy gums or mild gingivitis.
- Benefits: Prevents gum disease, removes irritants, helps maintain oral health.
- Drawbacks: Not sufficient for advanced gum disease.
- Cost: Generally covered by most dental insurance plans. Without insurance, typically $75-$200.
2. Scaling and Root Planing (Deep Cleaning)
- What it is: A non-surgical procedure that is considered the gold standard for treating periodontitis. Scaling involves removing plaque and tartar from above and below the gum line. Root planing smooths the root surfaces of the teeth, which helps prevent bacteria from re-adhering and allows the gums to reattach to the teeth. It's often done under local anesthesia and typically divided into quadrants of the mouth over multiple appointments.
- When it's used: For moderate periodontitis where significant plaque and tartar have accumulated below the gum line, leading to gum pockets and bone loss. This is the primary professional method for "how to cure gingivitis" that has progressed.
- Benefits: Reduces inflammation, eliminates bacterial infection, stops progression of periodontitis, can reverse early bone loss (in some cases).
- Drawbacks: Can cause temporary sensitivity, discomfort, and gum recession.
- Cost: Varies significantly based on the number of quadrants treated and region. Expect $150-$400 per quadrant (total $600-$1,600 for a full mouth deep cleaning) without insurance. Often partially covered by insurance.
``
3. Antibiotics
- What it is: Used to control bacterial infections. Can be topical (applied directly to gum pockets, e.g., antibiotic gels or chips) or oral (pills taken systemically).
- When it's used: As an adjunct to scaling and root planing, particularly in aggressive or recurrent cases of periodontitis.
- Benefits: Targets specific bacteria, reduces bacterial load.
- Drawbacks: Potential for side effects (e.g., digestive issues with oral antibiotics), risk of antibiotic resistance.
- Cost: Varies by type; generic oral antibiotics can be $10-$50, while localized antibiotic gels can be $50-$150 per application.
4. Surgical Treatments
- What it is: For advanced periodontitis, surgery may be necessary to reduce pocket depth, regenerate lost bone and tissue, or graft new tissue.
- Flap Surgery (Pocket Reduction Surgery): Gums are lifted back, tartar is removed, and irregular bone surfaces are smoothed before gums are sutured back.
- Bone Grafts: Use fragments of your own bone, synthetic bone, or donated bone to rebuild bone destroyed by periodontitis.
- Soft Tissue Grafts: Used to reinforce thin gums or fill in areas where gums have receded.
- When it's used: When non-surgical treatments are insufficient to control periodontitis or to address significant gum and bone damage.
- Benefits: Can save teeth, reduce infection, prevent further bone loss.
- Drawbacks: More invasive, longer recovery, higher cost, potential for post-surgical pain and sensitivity.
- Cost: Highly variable. Flap surgery can range from $500-$3,000 per quadrant. Bone grafts or soft tissue grafts can be $600-$2,000 per site.
5. Laser Therapy
- What it is: Lasers can be used to remove inflamed gum tissue and target bacteria in periodontal pockets.
- When it's used: Sometimes used as an alternative or adjunct to traditional scaling and root planing, or during surgical procedures.
- Benefits: Less invasive, potentially less bleeding and discomfort, faster healing.
- Drawbacks: Not all dentists offer it, effectiveness can vary, can be more expensive than traditional methods.
- Cost: Can add $200-$1,000+ to the cost of scaling and root planing or surgical procedures.
Comparison of Home vs. Professional Treatments
| Feature | Home Remedies (e.g., Saltwater, Improved Brushing) | Professional Cleaning (Prophylaxis) | Scaling & Root Planing (Deep Cleaning) |
|---|---|---|---|
| Target Condition | Mild Gingivitis, Symptomatic Relief | Mild Gingivitis, Prevention | Moderate to Severe Periodontitis |
| Effectiveness | Good for mild cases; symptom relief | Highly effective for prevention | Highly effective for stopping disease |
| Duration of Effect | Requires ongoing diligence | 6 months (typically) | Months to years with maintenance |
| Cost (US) | < $20 for supplies | $75-$200 (without insurance) | $600-$1,600 (full mouth, no insurance) |
| Pain Level | Minimal to none | Minimal | Mild to moderate (with anesthesia) |
| Required Skill | Patient self-care | Dental Hygienist/Dentist | Dentist/Periodontist |
| Reversibility | Yes, for gingivitis | Yes, for gingivitis | Can halt disease, but not bone loss |
| Time to Results | 3-7 days for symptom improvement | Immediate | Weeks for full gum healing |
Cost and Insurance: US Price Ranges
Understanding the financial aspect of swollen gums treatment is crucial. Costs vary significantly based on the type of treatment, the severity of the condition, your geographic location, and whether you have dental insurance.
Home Treatment Costs
- Basic Supplies:
- Soft-bristled toothbrush: $3-$10
- Fluoride toothpaste: $3-$8
- Dental floss: $3-$7
- Salt: $1-$5
- Hydrogen peroxide (3%): $1-$5
- Aloe vera gel/mouthwash: $5-$15
- Turmeric/Clove oil: $5-$20
- Total Initial Investment: Less than $50 for a full range of home care items. This represents the most affordable and often first-line swollen gums treatment at home.
Professional Treatment Costs (Without Insurance, US Averages)
| Treatment Type | Average Cost Range (US) | Notes |
|---|---|---|
| Routine Dental Exam | $50-$150 | Often includes X-rays, which add $25-$100 |
| Standard Cleaning (Prophylaxis) | $75-$200 | For healthy gums or mild gingivitis |
| Scaling & Root Planing (per quadrant) | $150-$400 | Typically 2-4 quadrants for a full mouth; total $600-$1600 |
| Localized Antibiotic Application (per site) | $50-$150 | Applied directly into gum pockets |
| Oral Antibiotics (prescription) | $10-$100 | Varies by medication and dosage |
| Flap Surgery (per quadrant) | $500-$3,000 | More advanced surgical intervention |
| Bone Graft (per site) | $600-$2,000 | Required for significant bone loss |
| Soft Tissue Graft (per site) | $600-$1,500 | To cover exposed roots or increase gum thickness |
| Laser-Assisted Gum Therapy (adjunct) | $200-$1,000+ | Additional cost on top of scaling or surgery |
Insurance Coverage
Most dental insurance plans in the US follow a "100-80-50" coverage model:
- 100% Coverage: Preventive care (e.g., routine exams, X-rays, standard cleanings – typically two per year). This is where your initial swollen gums treatment at home follow-up and basic professional care falls.
- 80% Coverage: Basic procedures (e.g., fillings, simple extractions).
- 50% Coverage: Major procedures (e.g., crowns, bridges, dentures, root canals, and often periodontal surgeries like scaling and root planing, grafts).

Key Points on Insurance:
- Deductibles: You'll likely need to pay an annual deductible (e.g., $50-$100) before your insurance starts paying.
- Annual Maximums: Most plans have an annual maximum benefit (e.g., $1,000-$2,000). Once you hit this, you pay 100% out-of-pocket for the rest of the year.
- Waiting Periods: Many plans have waiting periods (e.g., 6-12 months for basic procedures, 12-24 months for major procedures) before they will cover certain treatments for pre-existing conditions like periodontitis. This means if you buy insurance today, you might not be covered for deep cleaning for a year.
- Pre-authorization: For expensive procedures, your dentist will often submit a pre-treatment estimate to your insurance company to determine your exact coverage.
Payment Plans and Financing Options
If you don't have insurance or face high out-of-pocket costs, consider these options:
- Dental School Clinics: Often offer lower-cost care as procedures are performed by students under supervision of experienced faculty.
- Payment Plans: Many dental offices offer in-house payment plans, allowing you to pay for treatment in installments.
- Third-Party Financing: Companies like CareCredit offer healthcare credit cards with low or no-interest promotional periods if paid off within a certain timeframe.
- Health Savings Accounts (HSAs) / Flexible Spending Accounts (FSAs): If you have an HSA or FSA through your employer, you can use pre-tax dollars to pay for dental expenses, including deductibles, co-pays, and services not covered by insurance.
Recovery and Aftercare for Swollen Gums
Whether you're treating swollen gums at home or undergoing professional procedures, proper recovery and aftercare are essential for long-term success.
After Home Treatment for Gingivitis
If your swollen gums responded to home care:
- Maintain Excellent Oral Hygiene: This is paramount. Continue brushing twice a day with a soft brush and fluoride toothpaste, and floss daily. Consider adding an antiseptic mouthwash (e.g., chlorhexidine, prescribed by a dentist, or an OTC therapeutic mouthwash approved by the ADA).
- Regular Dental Check-ups: Schedule a dental exam and professional cleaning every six months. Your dentist can catch early signs of recurrence and remove any plaque or tartar buildup you might have missed.
- Healthy Lifestyle: Continue a balanced diet rich in vitamins, stay hydrated, and avoid smoking.
- Monitor Your Gums: Keep an eye out for any return of redness, swelling, or bleeding. Address these promptly with renewed home care or a dental visit.
After Professional Deep Cleaning (Scaling and Root Planing)
- Immediate Post-Procedure (First 24-48 hours):
- Pain and Sensitivity: It's normal to experience some tenderness, soreness, and sensitivity to hot/cold for a few days. OTC pain relievers (like ibuprofen) can help manage this.
- Bleeding: Minor bleeding may occur for a day or two. A saltwater rinse can help.
- Diet: Stick to soft foods and avoid extremely hot, cold, or spicy foods. Chew on the opposite side of the treated area if possible.
- Brushing/Flossing: Be gentle around the treated areas. Your hygienist will provide specific instructions on when and how to resume full oral hygiene.
- Longer-Term Care (Weeks to Months):
- Excellent Oral Hygiene: Your dentist or hygienist will likely provide specific instructions on brushing and flossing techniques, possibly recommending interdental brushes or specific mouthwashes. This is non-negotiable for preventing recurrence.
- Follow-up Appointments: You'll typically need a follow-up visit (often called periodontal maintenance) 4-6 weeks after deep cleaning to assess healing and remove any new plaque.
- Periodontal Maintenance Cleanings: Unlike standard cleanings, these are tailored for patients with a history of gum disease and are often recommended every 3-4 months, rather than twice a year. This is critical for preventing periodontitis from returning.
- Smoking Cessation: If you smoke, quitting is one of the most impactful steps you can take for your gum health.
- Expected Outcomes: Gums should become firmer, pinker, and less prone to bleeding. Pockets around the teeth should shrink, and gum pain relief should be significant.
After Gum Surgery
Recovery from gum surgery is more involved:
- Pain Management: Your dentist will likely prescribe pain medication. Follow instructions carefully.
- Swelling: Expect some facial swelling, which can be managed with cold compresses.
- Diet: A soft food diet is usually required for several days to weeks.
- Oral Hygiene: Very gentle cleaning as directed by your surgeon. You might use a prescription mouthwash (e.g., chlorhexidine) instead of brushing for a period.
- Stitches: If present, they will either dissolve or be removed at a follow-up appointment.
- Avoid Smoking: Crucial for optimal healing.
- Follow-up: Regular post-operative appointments are essential to monitor healing and ensure successful outcomes.
Pro Tip: Your commitment to at-home oral care after any treatment, whether home-based or professional, is the single most important factor in the long-term health of your gums.
Prevention of Swollen Gums
Preventing swollen gums, and by extension, gingivitis and periodontitis, is far easier and less costly than treating them. Most strategies for swollen gums treatment at home are also excellent preventive measures.
- Brush Twice Daily: Use a soft-bristled toothbrush and fluoride toothpaste. Brush for at least two minutes each time, covering all surfaces of your teeth and gently cleaning along the gum line.
- Floss Daily: This is non-negotiable. Flossing removes plaque and food particles from between teeth and under the gum line, areas your toothbrush can't reach.
- Use an Antiseptic Mouthwash: An ADA-accepted therapeutic mouthwash can help reduce plaque and gingivitis, complementing brushing and flossing. Look for ingredients like cetylpyridinium chloride (CPC) or essential oils.
- Regular Dental Check-ups and Professional Cleanings: Visit your dentist for a check-up and professional cleaning at least twice a year, or more frequently if recommended due to a history of gum disease. These cleanings remove hardened plaque (tartar) that cannot be removed at home.
- Eat a Balanced Diet:
- Limit Sugary and Starchy Foods: These contribute to plaque formation.
- Consume Plenty of Fruits and Vegetables: Rich in vitamins (especially Vitamin C and K) and antioxidants that support gum health and immune function.
- Drink Water: Rinse away food particles and neutralize acids.
- Avoid Tobacco Products: Smoking and chewing tobacco are major risk factors for gum disease and significantly impair the body's ability to fight infection and heal. Quitting is one of the best things you can do for your oral and overall health.
- Manage Underlying Health Conditions: If you have conditions like diabetes, keep them well-controlled, as they can impact gum health.
- Address Dry Mouth: If you suffer from dry mouth, discuss solutions with your dentist, such as artificial saliva products or medications that stimulate saliva flow.
- Avoid Overly Aggressive Brushing: Brushing too hard can damage gums and lead to recession, making them more vulnerable.
- Regularly Replace Your Toothbrush: Replace your toothbrush every 3-4 months, or sooner if the bristles are frayed. Worn bristles are less effective at cleaning and can harbor bacteria.
Risks and Complications of Untreated Swollen Gums
Ignoring swollen gums can lead to a cascade of increasingly severe oral and systemic health problems. The initial stage, gingivitis, is reversible, but if left untreated, it can advance to irreversible and destructive conditions.
Oral Health Complications
- Periodontitis: This is the most significant risk. Untreated gingivitis progresses to periodontitis, where the infection spreads below the gum line, destroying the bone and tissues that support your teeth. This process leads to:
- Gum Recession: Gums pull away from the teeth, exposing sensitive roots.
- Deep Periodontal Pockets: Spaces between teeth and gums deepen, collecting more bacteria.
- Bone Loss: The jawbone supporting the teeth erodes.
- Tooth Loosening and Loss: As bone support diminishes, teeth become loose and eventually fall out or need extraction.
- Dental Abscesses: Pockets of pus can form in the gums or bone, causing severe pain and swelling.
- Persistent Bad Breath: Chronic infection leads to foul-smelling breath.
- Increased Risk of Tooth Decay: Exposed tooth roots are more susceptible to decay than enamel-covered crowns.
- Difficulty Eating and Speaking: Loose teeth or painful gums can make chewing and articulation difficult.
Systemic Health Complications
Emerging research highlights a strong link between periodontal disease and various systemic health conditions. The bacteria and inflammation from the gums can enter the bloodstream and affect other parts of the body.
- Cardiovascular Disease: Periodontitis is associated with an increased risk of heart attack, stroke, and other cardiovascular problems. Inflammation in the gums may contribute to inflammation in the arteries.
- Diabetes Complications: Periodontal disease can make it harder for people with diabetes to control their blood sugar levels, and uncontrolled diabetes can worsen gum disease. It's a two-way street.
- Respiratory Diseases: Oral bacteria can be aspirated into the lungs, potentially leading to pneumonia or exacerbating existing respiratory conditions like COPD.
- Adverse Pregnancy Outcomes: Pregnant women with periodontitis may have a higher risk of preterm birth and low birth weight babies.
- Rheumatoid Arthritis: There's a link between periodontal disease and this inflammatory autoimmune condition.
- Alzheimer's Disease: Some studies suggest a potential link between chronic gum inflammation and an increased risk or progression of Alzheimer's disease.
The Bottom Line: While swollen gums treatment at home can address early stages, recognizing when to seek professional care is crucial to prevent these serious, long-term health consequences.
Children / Pediatric Considerations
Swollen gums are not just an adult issue; they can affect children too. Understanding the specific causes and treatments for kids is important for parents.
Common Causes of Swollen Gums in Children:
- Eruption Gingivitis: As baby teeth erupt (or permanent teeth erupt), the gums around them can become temporarily swollen, red, and tender. This is usually mild and resolves once the tooth fully emerges.
- Poor Oral Hygiene (Plaque-Induced Gingivitis): Just like adults, children can develop gingivitis if they don't brush and floss properly. Plaque buildup is the primary culprit.
- Thumb Sucking/Pacifier Use: Prolonged or aggressive habits can irritate gum tissue.
- Trauma: Children are prone to falls and bumps, which can injure the gums.
- Orthodontic Appliances: Braces can sometimes irritate gums and make cleaning more challenging, leading to inflammation.
- Diet: Frequent consumption of sugary snacks and drinks increases plaque formation.
- Canker Sores or Herpes Lesions: These can cause localized inflammation and pain on the gums.
- Nutritional Deficiencies: Rare but possible, especially vitamin deficiencies.
- Dental Abscess: An infection can cause localized gum swelling and pain, often accompanied by a pimple-like bump (fistula) on the gum. This requires immediate dental attention.
Swollen Gums Treatment at Home for Children:
- Gentle Brushing: Use a soft-bristled, child-sized toothbrush. For infants, a soft cloth or finger brush can clean gums and emerging teeth.
- Supervised Brushing: Parents should supervise and assist children with brushing until around age 7-8 to ensure thorough cleaning.
- Flossing: Introduce flossing once teeth touch each other, usually around age 2-3. Floss picks can be easier for small hands.
- Saltwater Rinses: For older children who can spit reliably, a warm saltwater rinse (1/4 teaspoon salt in 4 oz warm water) can soothe inflamed gums. Ensure they don't swallow it.
- Soft Diet: Offer soft, non-irritating foods if gums are sore.
- Avoid Sugary Snacks: Limit candies, sodas, and juices that feed bacteria.
- Cold Compresses/Teething Rings: For eruption gingivitis, cold teething rings or a gentle gum massage with a clean finger can provide relief.

When to See a Pediatric Dentist:
- Persistent Swelling: If swollen gums don't improve within a few days of diligent home care.
- Severe Pain: If your child is in significant discomfort, unwilling to eat, or has difficulty sleeping.
- Fever or Facial Swelling: These are signs of a more serious infection, like an abscess.
- Pus: Any pus from the gums indicates an infection.
- Bleeding Gums: While some bleeding during brushing can occur with gingivitis, persistent or heavy bleeding needs a check-up.
- Loose Teeth: If baby teeth are loose prematurely or permanent teeth feel loose.
- White/Red Lesions: Any unusual sores or lesions on the gums.
Pro Tip for Parents: Make oral hygiene fun and consistent. Lead by example, brush together, and use positive reinforcement. Regular dental check-ups starting by age one are crucial for preventing gum issues in children.
Frequently Asked Questions
Q1: How long does it take for swollen gums to go down with home treatment?
A1: For mild gingivitis caused by plaque, you should start to see improvement in redness, swelling, and bleeding within 3-7 days of consistent and diligent home care, including improved brushing, flossing, and saltwater rinses. Complete resolution of gingivitis can take 2-4 weeks. If there's no improvement or symptoms worsen after a week, it's time to see a dentist.
Q2: Can swollen gums be a sign of something serious?
A2: Yes, while often a sign of reversible gingivitis, persistent or severe swollen gums can indicate more serious underlying issues. These include advanced gum disease (periodontitis) which can lead to tooth and bone loss, dental abscesses, or even systemic health problems like diabetes or certain blood disorders. It's crucial to seek professional evaluation if home remedies don't help.
Q3: Is it okay to brush and floss if my gums are bleeding?
A3: Absolutely. While it might seem counterintuitive, bleeding gums are typically a sign of inflammation caused by plaque buildup. Gentle but thorough brushing and flossing are essential to remove this irritant. If you stop brushing or flossing, the condition will only worsen. Use a soft-bristled brush and floss very carefully.
Q4: Can I "cure" gingivitis at home?
A4: Yes, in many cases, mild gingivitis can be fully cured at home. This involves diligently practicing excellent oral hygiene (brushing twice daily, flossing daily) to remove plaque, combined with home remedies like saltwater rinses to reduce inflammation. However, if tartar has formed, professional cleaning is necessary, as home methods cannot remove hardened tartar.
Q5: What is the fastest way to get rid of gum pain?
A5: For immediate gum pain relief, you can try a warm saltwater rinse, applying a cold compress externally to your jaw, or using an over-the-counter pain reliever like ibuprofen. Topical numbing gels containing benzocaine can also provide temporary localized relief. However, these are symptomatic treatments; addressing the underlying cause (usually plaque) is essential for long-term relief.
Q6: Does swollen gums treatment at home include hydrogen peroxide?
A6: Yes, a diluted hydrogen peroxide rinse can be an effective part of a home treatment regimen for swollen gums. Mix equal parts 3% hydrogen peroxide with water, swish for 30 seconds, and then spit thoroughly. It acts as an antiseptic to kill bacteria and reduce inflammation. However, limit its use to 2-3 times a week, and never swallow it.
Q7: Are there any foods that make swollen gums worse or better?
A7: Sugary and acidic foods can feed bacteria and irritate inflamed gums, making the condition worse. Hard, crunchy, or spicy foods can also cause discomfort. Conversely, a diet rich in Vitamin C (citrus, berries, leafy greens) and Vitamin K (kale, spinach) can improve gum health. Staying hydrated by drinking plenty of water also helps rinse away food particles.
Q8: When should I see a dentist for swollen gums?
A8: You should see a dentist if your swollen gums don't improve after 7-10 days of diligent home care, if the swelling is severe or accompanied by intense pain, fever, pus, or if you notice any loose teeth or persistent bad breath. Any signs of an abscess or rapid worsening of symptoms warrant immediate professional attention.
Q9: Can pregnancy cause swollen gums?
A9: Yes, "pregnancy gingivitis" is a common condition due to hormonal changes, particularly increased progesterone and estrogen levels. These hormones can make gums more sensitive to plaque bacteria, leading to increased inflammation, redness, and bleeding. It typically subsides after childbirth but requires consistent oral hygiene during pregnancy.
Q10: What is the difference between gingivitis and periodontitis?
A10: Gingivitis is the early, mildest form of gum disease, characterized by inflammation, redness, and bleeding of the gums caused by plaque. It is reversible with proper oral hygiene and professional cleaning. Periodontitis is a more advanced and serious form where the infection has spread below the gum line, damaging the bone and tissues supporting the teeth, leading to irreversible bone loss and potential tooth loss. Periodontitis requires professional treatment to halt its progression.
When to See a Dentist
While swollen gums treatment at home can be highly effective for mild gingivitis, it's crucial to recognize when professional dental intervention is necessary. Ignoring severe or persistent symptoms can lead to irreversible damage.
You should schedule a dental appointment if:
- No Improvement After 7-10 Days of Home Care: If your gums continue to be swollen, red, or bleed easily despite consistent and proper home care (brushing, flossing, saltwater rinses) for over a week, it indicates that home remedies are not sufficient, and professional evaluation is needed.
- Severe or Worsening Pain: If you experience intense, throbbing pain, or if your pain increases rather than decreases.
- Visible Pus: The presence of pus oozing from your gums or around a tooth (often appearing as a pimple-like bump on the gum) is a clear sign of an infection (abscess) that requires immediate professional treatment.
- Fever or Facial Swelling: If swollen gums are accompanied by a fever or swelling that spreads to your face, jaw, or neck, this indicates a serious infection that could spread rapidly. This is an emergency.
- Loose Teeth: Any sensation of a tooth feeling loose or shifting is a critical red flag for advanced periodontitis and requires urgent dental care to prevent tooth loss.
- Persistent Bad Breath: While mild bad breath can accompany gingivitis, chronic, foul-smelling breath that doesn't improve with brushing and flossing can be a symptom of deeper infection.
- Receding Gums: If you notice your gums pulling away from your teeth, making them look longer, this is a sign of gum disease progression and bone loss.
- Difficulty Eating or Swallowing: Severe gum swelling or pain can make it hard to chew or swallow, indicating a serious issue.
Emergency vs. Scheduled Appointment Guidance:
- Emergency (Call Your Dentist Immediately or Visit an Urgent Care/ER):
- Sudden, severe, unmanageable pain.
- Rapidly spreading facial swelling.
- High fever associated with gum swelling.
- Difficulty breathing or swallowing.
- Trauma leading to significant gum injury and bleeding.
- Scheduled Appointment (Within a few days to a week):
- Persistent swollen, red, or bleeding gums that don't respond to home care.
- Signs of gum recession or minor tooth sensitivity.
- Persistent bad breath.
- Concern about medication side effects on gums.
Remember, your oral health is intrinsically linked to your overall well-being. Don't hesitate to consult a dental professional if you have any concerns about your gum health. Early diagnosis and treatment are key to preventing minor issues from becoming major problems.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
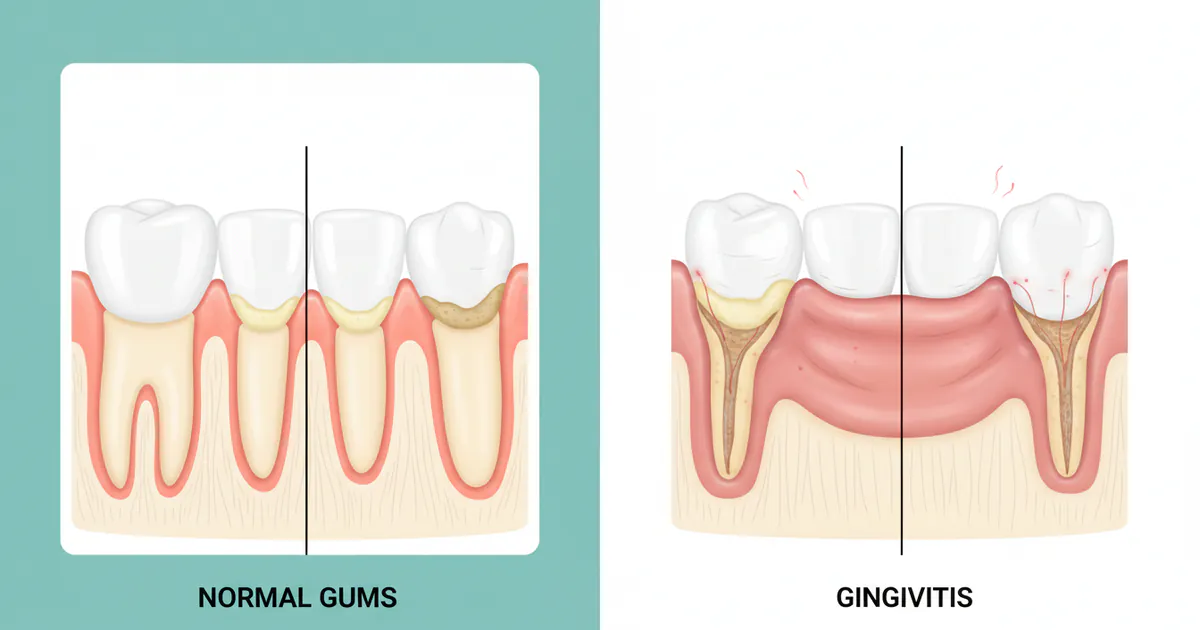
Normal Gums vs Gingivitis: Complete Comparison Guide
Did you know that nearly half of American adults over 30 show signs of gum disease, a condition that can range from mild inflammation to severe infection leading to tooth loss? Understanding the difference between healthy gums and those affected by early gum disease, known as gingivitis, is cruc
February 22, 2026
Can You Get Rid of Gingivitis
More than 50% of American adults aged 30 or older suffer from some form of gum disease, with gingivitis being the earliest and most common stage. This often silent condition, marked by inflammation of the gums, can seem daunting, leading many to wonder: can you get rid of gingivitis? The good ne
February 22, 2026
What Causes Receding Gums
Receding gums, a condition where the gum tissue surrounding the teeth pulls back or wears away, exposing more of the tooth or the tooth's root, affects a significant portion of the adult population in the United States. In fact, estimates suggest that **up to 88% of people over the age of 65 have on
February 22, 2026
Signs of Gingivitis: Complete Guide
Did you know that nearly half of American adults aged 30 and older suffer from some form of gum disease? While that statistic might sound alarming, the good news is that the earliest and most common stage, gingivitis, is entirely reversible. Recognizing the signs of gingivitis early is your
February 22, 2026