Can Adults Get Hand Foot and Mouth

Key Takeaways
- Hand, Foot, and Mouth Disease (HFMD) is often perceived as a childhood ailment, a rite of passage for toddlers in daycare. However, the notion that adults are immune to this common viral infection is a pervasive misconception. In reality, can adults get Hand Foot and Mouth disease? The unequivoc
Can Adults Get Hand Foot and Mouth?
Hand, Foot, and Mouth Disease (HFMD) is often perceived as a childhood ailment, a rite of passage for toddlers in daycare. However, the notion that adults are immune to this common viral infection is a pervasive misconception. In reality, can adults get Hand Foot and Mouth disease? The unequivocal answer is yes, and for many, the experience can be surprisingly severe and prolonged compared to what children typically endure. While instances of HFMD in adults might not dominate headlines, they are a significant concern for parents, caregivers, and anyone exposed to young children, affecting their daily lives, work, and overall well-being.

This comprehensive guide from SmilePedia.net aims to demystify Hand, Foot, and Mouth Disease in adults. We'll delve into its origins, the specific challenges it poses to adult immune systems, and why its symptoms can sometimes be more debilitating than in younger populations. We’ll explore everything from its characteristic oral sores and skin rashes to effective management strategies, prevention tactics, and when it’s crucial to seek medical or dental attention. Understanding this viral infection is vital for protecting yourself and your community, ensuring prompt diagnosis, and mitigating its impact on your health.
Key Takeaways:
- Adults can and do contract Hand, Foot, and Mouth Disease (HFMD), often experiencing more severe symptoms than children due to their mature immune responses.
- HFMD is caused by enteroviruses, primarily Coxsackievirus A16 and Enterovirus 71, and is highly contagious through direct contact, respiratory droplets, and contaminated surfaces.
- Symptoms in adults can include high fever, intense sore throat with painful oral lesions (resembling canker sores), and a distinctive rash on hands, feet, and sometimes buttocks.
- Treatment is largely supportive, focusing on pain relief with over-the-counter medications ($10-$30), hydration, and managing oral discomfort with rinses ($5-$25).
- Diagnosis typically involves a clinical exam, with lab tests rarely necessary. An urgent care or primary care visit may cost $100-$300 without insurance, while prescription relief (if needed) might add $20-$100.
- Recovery can range from 7-10 days for mild cases to several weeks for more severe adult infections, with potential complications like nail shedding or, rarely, neurological issues.
- Prevention hinges on rigorous hand hygiene, disinfection of shared surfaces, and avoiding close contact with infected individuals, especially during the contagious period.
What It Is / Overview
Hand, Foot, and Mouth Disease (HFMD) is a common infectious disease caused by a group of viruses known as enteroviruses. The most frequent culprit is Coxsackievirus A16, but other strains, particularly Enterovirus 71 (EV-A71), can also lead to more severe forms of the illness. Despite its name often associating it with young children, HFMD is a systemic viral infection that can affect individuals of any age, including adults.
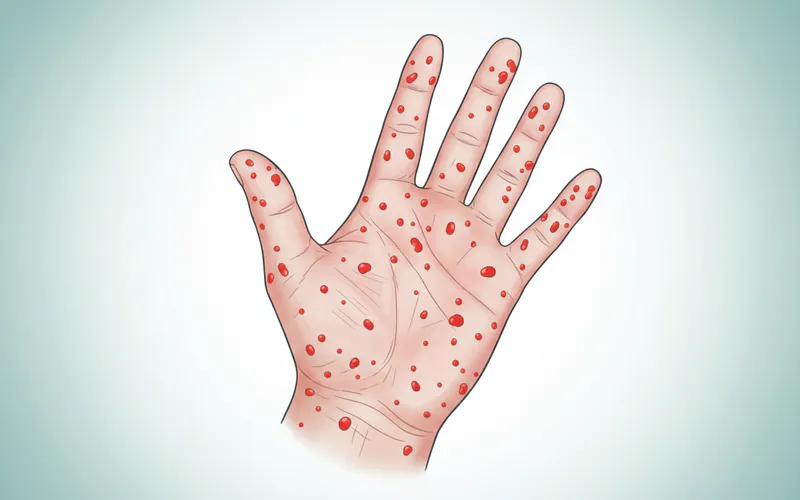
The disease manifests primarily through characteristic lesions—small, painful blisters or sores—that typically appear in the mouth, on the hands, and on the feet. In some cases, the rash can extend to the buttocks, groin, and elbows. While usually a mild, self-limiting illness in children, adults often experience a more pronounced and debilitating course of the disease due to their fully developed immune systems launching a more vigorous, and sometimes overreactive, response to the invading virus. This heightened immune response can lead to more intense inflammation and discomfort, making adult HFMD a challenging experience.
Types / Variations
While Coxsackievirus A16 is the most common cause of HFMD in the United States and Western countries, it's important to understand that several strains of enteroviruses can cause the condition.
- Coxsackievirus A16 (CVA16): This is the predominant strain globally and typically causes the classic, milder form of HFMD. Symptoms are usually self-limiting, and severe complications are rare.
- Enterovirus 71 (EV-A71): This strain is more frequently associated with severe disease and neurological complications, such as encephalitis, meningitis, or acute flaccid paralysis, particularly in Southeast Asia. While less common in the US, outbreaks can occur, and adults infected with EV-A71 may face a higher risk of complications.
- Other Coxsackievirus Strains (e.g., Coxsackievirus A6): Increasingly, other strains, like Coxsackievirus A6, are being identified as causes of HFMD. Infections with CVA6 can sometimes lead to atypical presentations, including more widespread rashes, lesions resembling chickenpox, and a higher incidence of nail shedding (onychomadesis) during recovery. This variation can make diagnosis challenging as it deviates from the classic HFMD presentation.
Another related condition, Herpangina, is also caused by enteroviruses (often Coxsackievirus A and B types). Herpangina primarily affects the throat, causing painful sores on the soft palate, tonsils, and uvula, typically without the characteristic rash on hands and feet. It can sometimes be mistaken for HFMD, especially if oral lesions are the dominant symptom. While technically distinct, both conditions highlight the diverse ways enteroviruses can manifest in the oral cavity.
Causes / Why It Happens
HFMD is highly contagious and spreads primarily through person-to-person contact. The viruses responsible are found in the nose and throat secretions (saliva, sputum, nasal mucus), blister fluid, and feces of an infected person.
The main modes of transmission include:
- Close Personal Contact: Hugging, kissing, or sharing utensils with an infected person.
- Respiratory Droplets: Coughing or sneezing releases viral particles into the air, which can be inhaled by others.
- Fecal-Oral Route: Contact with feces from an infected person, often occurring during diaper changes, then touching the mouth without proper handwashing. This is a common route of transmission in daycare settings.
- Contaminated Surfaces: Touching surfaces or objects that have been contaminated with the virus (e.g., toys, doorknobs) and then touching one's eyes, nose, or mouth.
Risk Factors for Adults:
While anyone can contract HFMD, certain adults are at a significantly higher risk:
- Parents of Young Children: This is by far the most common risk factor. Children, especially those in daycare or preschool, are often the primary vectors for HFMD due to their close contact, less developed hygiene habits, and frequent sharing of toys. Parents caring for infected children are almost inevitably exposed.
- Childcare Workers: Teachers, daycare providers, and nannies are in constant contact with young children and are highly susceptible to contracting the virus.
- Healthcare Professionals: Those working with pediatric patients may be exposed.
- Immunocompromised Individuals: Adults with weakened immune systems (e.g., due to HIV, organ transplant, chemotherapy, or certain autoimmune diseases) are more susceptible to severe infections and prolonged illness.
- Travelers: Visiting regions with ongoing HFMD outbreaks (particularly in Asia) can increase exposure risk.
The incubation period for HFMD is typically 3 to 7 days, meaning symptoms usually appear a few days after exposure to the virus. An infected person is most contagious during the first week of illness but can shed the virus in their feces for several weeks, even after symptoms have resolved. This prolonged shedding period contributes to the virus's ability to spread widely.
Signs and Symptoms
The presentation of Hand, Foot, and Mouth Disease in adults can differ significantly from children, often leading to a more challenging and uncomfortable experience. While children might have mild fever and a scattered rash, adults can suffer from severe pain and systemic symptoms.
The initial signs in adults are often non-specific and can be mistaken for other viral illnesses:
- Prodromal Symptoms (1-2 days before rash/sores):
- High Fever: Adults often experience a higher and more persistent fever, sometimes reaching 102°F to 104°F (39°C to 40°C).
- Intense Sore Throat: One of the most debilitating symptoms for adults is a severely painful sore throat, making swallowing difficult and sometimes leading to dehydration.
- Malaise and Fatigue: Profound tiredness and a general feeling of being unwell are common.
- Headache and Muscle Aches: Aches and pains throughout the body are frequently reported.
- Loss of Appetite: Due to the sore throat and general malaise.
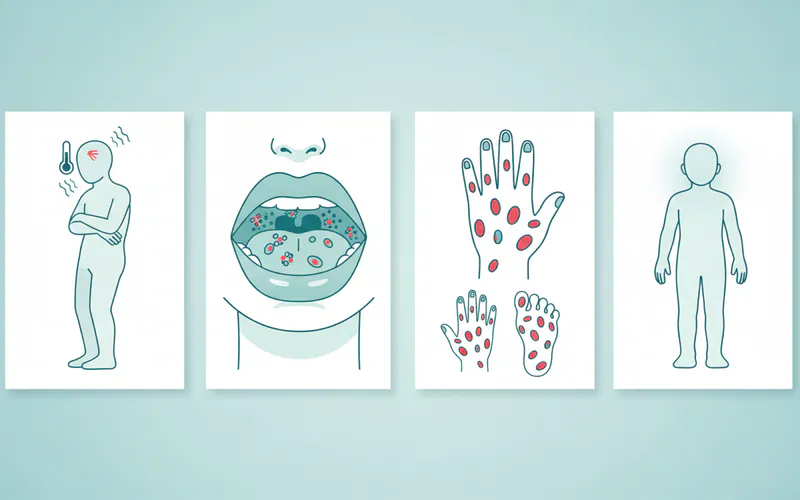
Following these initial symptoms, the characteristic rash and oral lesions begin to appear:
- Oral Lesions (Mouth Sores): These are often the first distinctive sign. Small, painful red spots develop in the mouth, particularly on the tongue, soft palate, inside of the cheeks, and gums. These quickly evolve into blisters, then shallow, ulcer-like sores that can be extremely painful. Unlike common canker sores (aphthous ulcers) which often appear individually and have a distinct pattern, HFMD oral lesions are typically numerous and widespread throughout the mouth and throat. They can make eating, drinking, and even speaking incredibly difficult.
- Skin Rash:
- Location: The rash primarily appears on the palms of the hands and soles of the feet. However, in adults, it can be much more widespread, often extending to the back of the hands, tops of the feet, arms, legs, buttocks, and even the torso.
- Appearance: The rash starts as flat red spots (macules) or small raised bumps (papules) that are often non-itchy but can sometimes be tender or painful to the touch. These can progress to small, fluid-filled blisters (vesicles) with a red halo, which may burst and crust over. The appearance can be quite dramatic in adults, with numerous, sometimes large, lesions.
- Discomfort: While the rash itself may not be itchy like chickenpox, it can be extremely sensitive, burning, or painful, particularly on the hands and feet, making walking or using hands difficult.
Severity Differences in Adults:
The mature immune system of an adult, while generally more robust, can respond to the enterovirus infection with an exaggerated inflammatory response. This often leads to:
- More Intense Pain: Especially from the oral lesions, which can be larger and more numerous.
- Higher Fever: As mentioned, fevers tend to be more significant and prolonged.
- Increased Systemic Discomfort: Greater fatigue, body aches, and general feeling of illness.
- Prolonged Duration: Adult HFMD often lasts longer, sometimes up to two weeks, or even more if complications like nail shedding occur.
Pro Tip: If you're an adult and experience a sudden onset of high fever, severe sore throat, and develop red spots or blisters on your hands and feet, especially if you've been around young children, HFMD should be high on your list of differential diagnoses. Early recognition can help you manage symptoms effectively and prevent further spread.
Treatment Options
There is no specific antiviral treatment or cure for Hand, Foot, and Mouth Disease. As a viral infection, treatment is primarily supportive, focusing on relieving symptoms and ensuring comfort while the body's immune system fights off the virus.
-
Pain and Fever Management:
- Over-the-Counter (OTC) Pain Relievers:
- Acetaminophen (Tylenol): Effective for fever and pain.
- Non-Steroidal Anti-Inflammatory Drugs (NSAIDs) like Ibuprofen (Advil, Motrin): Reduce pain, fever, and inflammation.
- Pros: Readily available, generally safe, and effective for most symptoms.
- Cons: Can have side effects (e.g., stomach upset with NSAIDs), only address symptoms, not the virus.
- Cost: Typically $5-$15 for a bottle of generics.
- Topical Anesthetics for Oral Lesions:
- Lidocaine Viscous: A prescription-strength oral rinse that numbs the mouth and throat, offering significant relief, especially before meals.
- OTC Oral Pain Relief Gels/Sprays: Products containing benzocaine (e.g., Orajel, Chloraseptic) can provide temporary numbing.
- Pros: Direct relief for painful mouth sores, allowing for better hydration and nutrition.
- Cons: Prescription lidocaine requires a doctor's visit; OTC options offer limited and temporary relief.
- Cost: OTC gels $5-$15. Prescription lidocaine viscous $20-$50.
- "Magic Mouthwash" (Compounded): A prescription mixture often containing an antacid (like Maalox), an antihistamine (like diphenhydramine), and a topical anesthetic (like lidocaine). It's swished and spit out (or sometimes swallowed) to soothe the mouth and throat.
- Pros: Highly effective for severe oral pain.
- Cons: Requires a prescription, taste can be unpleasant.
- Cost: $30-$70 depending on ingredients and pharmacy.
- Over-the-Counter (OTC) Pain Relievers:
-
Hydration and Nutrition:
- Increased Fluid Intake: Essential to prevent dehydration, especially with painful swallowing. Water, diluted juices, oral rehydration solutions (e.g., Pedialyte), and broths are recommended.
- Soft, Bland Foods: Choose foods that are easy to swallow and won't irritate mouth sores. Examples include yogurt, applesauce, mashed potatoes, popsicles, ice cream, and soups. Avoid acidic, spicy, or crunchy foods.
- Pros: Crucial for recovery and preventing complications.
- Cons: Can be challenging with severe oral pain.
-
Skin Rash Care:
- Cool Compresses: Can soothe discomfort from skin lesions.
- Calamine Lotion: May help with any itchiness or discomfort, though HFMD rash is typically not intensely itchy.
- Pros: Provides symptomatic relief.
- Cons: May not be necessary for all cases as the rash is often more painful than itchy.
- Cost: $5-$10 for Calamine lotion.
-
Rest: Adequate rest allows the body to conserve energy and focus on fighting the infection. Adults often feel more exhausted and need significant downtime.
When Medical Intervention is Necessary:
While most cases resolve on their own, seek medical attention if:
- Symptoms worsen or do not improve after 7-10 days.
- High fever persists for more than 3 days.
- Signs of dehydration develop: Decreased urination, dry mouth, sunken eyes, excessive lethargy.
- Severe headaches, stiff neck, back pain, or confusion develop: These could indicate rare neurological complications like meningitis or encephalitis.
- Difficulty breathing or chest pain.
- Pain is unmanageable with OTC medications.
For adults, the intensity of symptoms can be more debilitating, impacting work and daily activities. Consulting a healthcare provider for diagnosis and prescription-strength pain relief or "magic mouthwash" is often a worthwhile step to manage severe discomfort.
Step-by-Step Process (of managing symptoms)
Managing HFMD in adults is primarily a self-care process focused on symptom relief and preventing transmission. Here’s a step-by-step guide:
-
Confirm Diagnosis (if concerned):
- If you suspect HFMD, especially with severe symptoms, schedule an appointment with your primary care physician or visit an urgent care clinic. A dentist can also identify oral lesions. They will perform a clinical examination, looking for the characteristic rash and mouth sores. Lab tests are rarely needed but can confirm the viral strain if necessary.
- Cost: Primary care visit $50-$200 (with insurance), $100-$300 (without insurance). Urgent care visit $100-$300 (with insurance), $150-$400+ (without insurance).
-
Isolate Yourself:
- HFMD is highly contagious. Stay home from work, school, or public gatherings to prevent spreading the virus.
- Avoid close contact with others, especially young children, pregnant women, and immunocompromised individuals, until all blisters have crusted over and fever has subsided for at least 24 hours without medication. This typically lasts 7-10 days.
-
Manage Pain and Fever:
- Take acetaminophen or ibuprofen regularly as directed to reduce fever and body aches. Follow dosing instructions carefully.
- For severe oral pain, discuss prescription options like viscous lidocaine or "magic mouthwash" with your doctor. Otherwise, use OTC oral pain relief sprays or gels.
- Pro Tip: Try taking pain medication about 30 minutes before attempting to eat or drink to make swallowing more comfortable.
-
Prioritize Hydration:
- Drink plenty of fluids throughout the day. Water, coconut water, oral rehydration solutions, and clear broths are excellent choices.
- Suck on ice chips or popsicles to soothe your throat and provide fluids.
- Avoid acidic juices (orange, grapefruit, tomato) and carbonated drinks, as they can irritate mouth sores.
-
Eat Soft, Bland Foods:
- Choose foods that require minimal chewing and are unlikely to irritate your mouth. Examples: yogurt, applesauce, mashed potatoes, scrambled eggs, oatmeal, soft cheeses, and pureed soups.
- Avoid spicy, salty, crunchy, or acidic foods until your mouth sores have healed.
-
Maintain Oral Hygiene:
- Gently brush your teeth with a soft-bristled toothbrush.
- Rinse your mouth with warm salt water (1/2 teaspoon salt in 8 ounces warm water) several times a day to soothe sores and promote healing. An ADA-recommended alcohol-free mouthwash can also be helpful if it doesn't cause irritation.
- Cost: Soft toothbrush $3-$7, Salt $2-$5.
-
Care for Skin Rash:
- Keep affected areas clean and dry.
- Apply calamine lotion or cool compresses if the rash is itchy or uncomfortable. Avoid picking at blisters to prevent secondary bacterial infections.
-
Get Ample Rest:
- Your body needs energy to fight the virus. Prioritize sleep and limit strenuous activities.
-
Monitor for Complications:
- Be vigilant for signs of dehydration (decreased urination, dizziness, dry mouth), worsening pain, or neurological symptoms (severe headache, stiff neck, confusion). Seek immediate medical attention if these occur.
Cost and Insurance
The costs associated with HFMD in adults primarily stem from diagnosis, symptom management, and potential complications. Since there's no specific cure, expenditures are mainly for supportive care.
1. Diagnostic Costs:
- Primary Care Physician (PCP) Visit: For initial diagnosis and symptom assessment.
- With Insurance: Typically a co-pay of $20-$75, plus any deductible amounts.
- Without Insurance: $100-$300 for an office visit.
- Urgent Care Clinic Visit: Often chosen for quicker access, especially if symptoms are severe or during off-hours.
- With Insurance: Co-pay usually $50-$100, plus deductible.
- Without Insurance: $150-$400, sometimes more depending on services rendered (e.g., IV fluids for dehydration).
- Emergency Room (ER) Visit: Generally not necessary unless severe dehydration or neurological complications are suspected.
- With Insurance: High co-pays (e.g., $100-$500) and significant deductible application.
- Without Insurance: $500-$3,000+, making it a very expensive option for non-emergencies.
- Lab Tests: Viral swabs are rarely performed for routine HFMD diagnosis in adults as it's usually clinical. If done, they can add $100-$300 to the cost, typically covered by insurance if deemed medically necessary.
2. Medication Costs (Out-of-Pocket):
- Over-the-Counter (OTC) Pain Relievers/Fever Reducers: Acetaminophen or Ibuprofen.
- Cost: $5-$15 per bottle.
- OTC Oral Pain Relief (Sprays, Gels): Benzocaine-based products.
- Cost: $5-$15 per item.
- Prescription Oral Pain Rinses (e.g., Viscous Lidocaine, "Magic Mouthwash"):
- Cost: $20-$70, depending on pharmacy, formulation, and insurance coverage. Generics are less expensive.
- Calamine Lotion: For rash discomfort.
- Cost: $5-$10.
- Oral Rehydration Solutions (Pedialyte):
- Cost: $5-$15 per carton/powder.
3. Insurance Coverage:
Most health insurance plans in the US will cover the costs associated with diagnosing and treating HFMD, as it's a common medical condition.
- Deductibles: You will be responsible for costs until your annual deductible is met.
- Co-pays: A fixed amount you pay at the time of service for doctor visits or urgent care.
- Co-insurance: After your deductible is met, you may still pay a percentage of the remaining costs (e.g., 20%).
- Prescription Coverage: Most plans have a prescription drug benefit with tiered co-pays (e.g., $10-$50+ depending on generic vs. brand-name).
4. Cost-Saving Tips:
- Telemedicine: For initial assessment, a telehealth visit can sometimes be cheaper than an in-person visit ($40-$100 without insurance, or a lower co-pay).
- Generics: Opt for generic versions of OTC and prescription medications.
- Hydration at Home: Focus on water, clear broths, and homemade popsicles instead of expensive sports drinks or rehydration solutions unless specifically recommended by a doctor for dehydration.
- Avoid the ER: Unless it's a true emergency, an urgent care clinic or your PCP is a far more cost-effective option.
Overall, a typical adult HFMD case involving a doctor's visit and OTC medications might range from $50 (with good insurance) to $350 (without insurance and prescriptions). Severe cases requiring special prescriptions or multiple visits could reach $100-$500. Hospitalization for rare complications would, of course, be significantly higher, potentially thousands of dollars, though largely covered by insurance.
Recovery and Aftercare
The recovery period for Hand, Foot, and Mouth Disease in adults can be more protracted than in children, often ranging from 7 to 14 days, or even longer for more severe cases or if complications arise.
Typical Recovery Timeline:
- Days 1-3 (Acute Phase): High fever, severe sore throat, body aches, and the initial appearance of oral lesions. Rash may begin to emerge. This is usually the peak of discomfort.
- Days 4-7 (Lesion Development & Pain Management): Oral sores are most painful, making eating and drinking challenging. The skin rash typically becomes more prominent, with blisters forming. Fatigue can be significant.
- Days 8-14 (Healing & Resolution): Oral sores begin to heal, pain subsides, and appetite improves. Skin blisters dry up, scab over, and gradually disappear. Fever usually resolves. Energy levels start to return to normal.
- Weeks 3-8 (Post-Viral Effects - Less Common): Some adults, especially after infections with Coxsackievirus A6, may experience onychomadesis (nail shedding). This is a painless condition where fingernails and toenails detach and fall off. New nails typically grow back within a few months. This is temporary and not a sign of serious illness.
Aftercare Instructions:
- Continue Good Hygiene: Even after symptoms resolve, the virus can still be shed in stool for several weeks. Maintain meticulous handwashing with soap and water, especially after using the restroom and before eating.
- Monitor for Nail Changes: If nail shedding occurs, there's no specific treatment. Keep nails trimmed and clean. Consult a dermatologist if you have concerns, but generally, patience is key.
- Gradual Return to Activity: Listen to your body. While the acute symptoms may fade, persistent fatigue can linger. Gradually reintroduce physical activity and return to work/social activities when you feel fully recovered and are no longer contagious.
- Boost Immune System: Focus on a healthy diet, adequate sleep, and stress reduction to support your immune system post-illness.
- Dental Check-ups: If oral lesions were particularly severe or caused concerns, a dental check-up is advisable after full recovery to ensure proper oral health and address any lingering issues. An ADA-recommended routine check-up is always a good practice.
Pro Tip: Even if you feel better, continue to disinfect frequently touched surfaces in your home for a few weeks, as viral shedding can persist, especially if you have young children in the household.
Prevention
Preventing Hand, Foot, and Mouth Disease, especially in adults, centers on rigorous hygiene practices and avoiding exposure to the virus.
- Hand Hygiene:
- Wash hands frequently and thoroughly: Use soap and water for at least 20 seconds, especially after using the restroom, changing diapers, before eating, and after coughing, sneezing, or blowing your nose.
- Use alcohol-based hand sanitizers: If soap and water are not available, use a hand sanitizer with at least 60% alcohol. However, handwashing is more effective for enteroviruses.
- Disinfection of Surfaces:
- Regularly clean and disinfect: Frequently touched surfaces and objects (doorknobs, toys, countertops, remote controls, phones) in your home, especially if someone is ill.
- Use appropriate disinfectants: A solution of 1 tablespoon of bleach to 4 cups of water, or a commercial household disinfectant. Follow product instructions carefully.
- Avoid Close Contact:
- Minimize contact with infected individuals: Avoid hugging, kissing, sharing eating utensils, cups, towels, or personal items with anyone who has HFMD.
- Stay home when sick: If you have HFMD, stay home from work, school, and public places until your fever has resolved and blisters have dried up (typically 7-10 days) to prevent spreading the virus.
- Teach Children Good Hygiene:
- Educate children about proper handwashing techniques and the importance of not putting hands or toys in their mouths. This indirectly protects adults.
- Manage Oral Secretions:
- Cover your mouth and nose when coughing or sneezing. Dispose of tissues properly.
- Avoid touching your eyes, nose, and mouth with unwashed hands.
Vaccine Research: Currently, there is no vaccine available for Hand, Foot, and Mouth Disease in the United States. However, research is ongoing, particularly for Enterovirus 71 (EV-A71), which causes more severe forms of the disease. Several EV-A71 vaccines are licensed and used in some Asian countries, but they are not widely available elsewhere.
Risks and Complications
While HFMD is generally a mild, self-limiting illness, adults are not immune to potential risks and complications, some of which can be more severe than in children.
- Dehydration: Due to painful mouth sores, adults may find it extremely difficult to swallow, leading to reduced fluid intake. This can result in dehydration, especially if accompanied by high fever. Symptoms include decreased urination, dry mouth, lethargy, and dizziness.
- Secondary Bacterial Infections: Open blisters or sores, both in the mouth and on the skin, can become infected with bacteria. This can lead to increased pain, swelling, redness, pus, and may require antibiotic treatment.
- Onychomadesis (Nail Shedding): As mentioned, this is a common, though temporary, complication primarily seen a few weeks to months after infection, particularly with Coxsackievirus A6. Fingernails and toenails may loosen and fall off.
- Neurological Complications (Rare but Serious): While rare in the US, certain strains of enteroviruses (especially EV-A71) can lead to severe neurological complications. These include:
- Viral Meningitis: Inflammation of the membranes surrounding the brain and spinal cord. Symptoms include severe headache, stiff neck, fever, and light sensitivity.
- Encephalitis: Inflammation of the brain itself. This is very serious and can cause confusion, seizures, weakness, or problems with movement.
- Acute Flaccid Paralysis: A rare condition affecting the nervous system, leading to muscle weakness and paralysis.
- Myocarditis: In extremely rare cases, enteroviruses can cause inflammation of the heart muscle, known as myocarditis. This can lead to symptoms like chest pain, shortness of breath, and fatigue.
- Pregnant Women: While there is no clear evidence that HFMD during pregnancy causes severe problems for the fetus, pregnant women should take extra precautions to avoid infection, especially close to delivery. Infection during delivery could potentially transmit the virus to the newborn.
It's crucial for adults to monitor their symptoms closely and seek prompt medical attention if any signs of severe complications arise.
Comparison Tables
Here are two comparison tables to help differentiate conditions and understand treatment options.
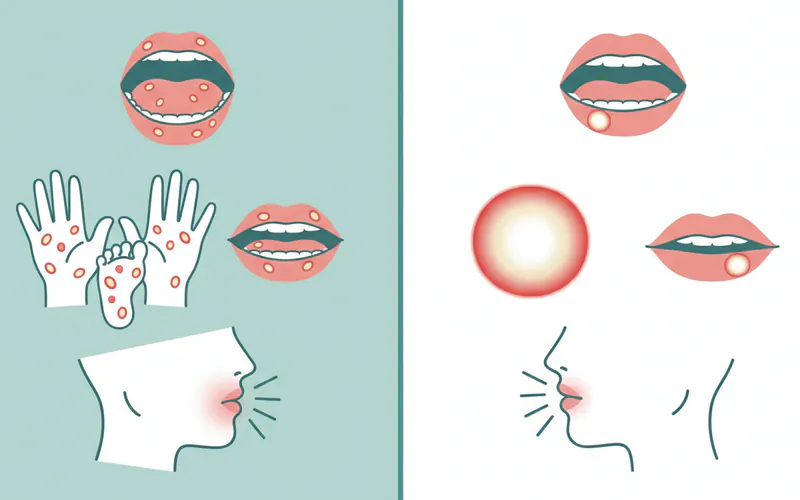
Table 1: HFMD Oral Lesions vs. Common Canker Sores
This comparison helps address the target keyword "canker sore causes" by distinguishing HFMD lesions from typical canker sores.
| Feature | Hand, Foot, and Mouth Disease Oral Lesions | Common Canker Sores (Aphthous Ulcers) |
|---|---|---|
| Causes | Enteroviruses (Coxsackievirus A16, EV-A71, etc.) | Unknown, but often linked to stress, trauma, acidic foods, nutritional deficiencies (e.g., B12, iron), certain toothpastes. |
| Location | Widespread: Tongue, soft palate, tonsils, inside cheeks, gums. Often deep in the throat. | Typically on non-keratinized tissues: Inside cheeks, lips, soft palate, tongue edges. Rarely on hard palate or gums. |
| Appearance | Start as small red spots, quickly becoming fluid-filled blisters, then shallow, painful ulcers. Often multiple. | Round or oval sores with a white/yellowish center and a red border. Usually single or a few at a time. |
| Associated Symptoms | High fever, body aches, malaise, sore throat, skin rash on hands/feet/buttocks. | No fever or systemic symptoms. Localized pain only. |
| Contagiousness | Highly contagious. | Not contagious. |
| Duration | Typically 7-10 days for oral lesions, resolves with the illness. | Usually 1-2 weeks; recurrent episodes are common. |
| Management | Symptomatic: Pain relief, hydration, soft foods, mouth rinses. | Symptomatic: Topical anesthetics, protective gels, addressing underlying triggers. |
Table 2: Symptom Management Options & Estimated US Costs
| Symptom / Treatment Category | Specific Option / Medication | Estimated Out-of-Pocket Cost (No Insurance) | Typical Duration of Use | Pros | Cons |
|---|---|---|---|---|---|
| Pain/Fever Relief | Acetaminophen (e.g., Tylenol) - OTC | $5 - $15 | As needed (7-10 days) | Widely available, effective for pain & fever. | Can cause liver damage in high doses. |
| Ibuprofen (e.g., Advil, Motrin) - OTC | $5 - $15 | As needed (7-10 days) | Reduces pain, fever, and inflammation. | Can cause stomach upset, kidney issues with prolonged use. | |
| Oral Pain Relief | OTC Benzocaine Gels/Sprays (e.g., Orajel, Chloraseptic) | $5 - $15 | As needed | Quick, localized numbing. | Temporary relief, can cause allergic reactions in some. |
| Viscous Lidocaine 2% - Prescription | $20 - $50 | As needed | Strong, effective numbing for severe oral pain. | Requires doctor's visit, can suppress gag reflex. | |
| "Magic Mouthwash" (Compounded) - Prescription | $30 - $70 | As needed | Combines anesthetics, antihistamines, antacids for comprehensive relief. | Requires doctor's visit, taste can be unpleasant. | |
| Saltwater Rinses (homemade) | <$1 (for salt) | Several times daily | Soothes, promotes healing, antibacterial effect. | No numbing effect. | |
| Rash Discomfort | Calamine Lotion - OTC | $5 - $10 | As needed | Soothes itching, dries weeping blisters. | Can be messy, not always needed for non-itchy HFMD rash. |
| Hydration Support | Oral Rehydration Solution (e.g., Pedialyte) - OTC | $5 - $15 | As needed | Replaces electrolytes, prevents dehydration. | Can be costly, many find taste unappealing. |
| Doctor's Visit | Primary Care Physician (PCP) visit - Diagnosis / Prescription | $100 - $300 | One visit | Professional diagnosis, prescription access, peace of mind. | Cost without insurance, wait times. |
| Urgent Care Clinic visit - Diagnosis / Prescription | $150 - $400+ | One visit | Faster access than PCP, especially after hours. | Higher cost than PCP, may not have patient's full history. |
Children / Pediatric Considerations
While this article focuses on adults, it's crucial to understand HFMD's impact on children, as they are often the source of adult infections. HFMD is most common in infants and children younger than 5 years old.
- Symptoms in Children: Children typically exhibit similar symptoms: fever, decreased appetite, malaise, and a sore throat, followed by mouth sores and a rash on hands and feet. However, their symptoms are often milder, and they tend to recover more quickly.
- Contagiousness in Children: Children in daycare, preschool, or school settings are highly efficient at spreading the virus due to close contact, incomplete hand hygiene, and putting toys in their mouths. They can remain contagious for several weeks after symptoms resolve due to viral shedding in stool.
- Parental Burden: Parents of infected children face the dual challenge of caring for a sick child and the high risk of contracting the disease themselves. This often means sleepless nights, missed work, and managing intense symptoms for both parent and child.
- Preventive Measures for Children: Emphasize frequent handwashing for children, especially after diaper changes and before meals. Regularly disinfect toys and surfaces that children touch. Teach children to cough and sneeze into their elbow or a tissue. If a child has HFMD, keep them home from school or daycare until their fever has resolved and blisters have dried to prevent community spread, as recommended by the American Academy of Pediatrics.
Understanding the pediatric aspect is vital for adults, as prevention strategies in children directly translate to protection for adults.
Cost Breakdown
A detailed breakdown of costs associated with adult HFMD, especially without insurance, highlights the financial impact of the illness.

Average US Costs (without insurance):
- Low-End Estimate (Mild Case, Self-Care):
- OTC pain relievers/fever reducers: $10
- OTC oral numbing gel/spray: $10
- Total: $20
- Mid-Range Estimate (Moderate Case, Doctor Visit, OTC + 1 Rx):
- Urgent Care Visit: $250
- OTC medications: $20
- Prescription (e.g., viscous lidocaine): $40
- Total: $310
- High-End Estimate (Severe Case, Multiple Visits, Multiple Rxs):
- Initial Urgent Care Visit: $300
- Follow-up PCP Visit: $200
- OTC medications: $30
- Prescription "Magic Mouthwash": $60
- Prescription for secondary bacterial infection (if needed): $50
- Total: $640
- Note: This excludes extreme cases requiring ER visits or hospitalization, which could be thousands.
With Insurance:
Costs are significantly reduced with insurance, though they vary based on your specific plan's deductible, co-pays, and co-insurance.
- Doctor Visit (PCP/Urgent Care): Typically a co-pay of $20 - $100.
- Prescription Medications: Co-pays usually range from $10 - $50 for generics, higher for brand names.
- Overall: Most insured individuals might pay between $30 - $200 for a typical case, assuming their deductible has already been met. If the deductible has not been met, they might pay more until it is satisfied.
Payment Plans and Financing Options:
For higher-cost scenarios (e.g., if a diagnostic lab test is needed, or for complications), or for those without insurance, payment plans might be available:
- Clinic Payment Plans: Many hospitals and urgent care centers offer interest-free payment plans, allowing patients to pay medical bills over several months. Inquire at the front desk or billing department.
- CareCredit: A healthcare credit card that offers promotional financing options (e.g., 0% interest for a certain period) for medical expenses.
- Hospital Financial Assistance: Non-profit hospitals often have financial assistance programs for low-income patients.
Cost-Saving Tips:
- Telehealth First: For initial symptoms, a virtual visit can often lead to a diagnosis and prescription at a lower cost than an in-person visit.
- Use Generics: Always ask for generic versions of medications.
- Compare Pharmacy Prices: Use apps or websites to compare prescription drug prices at different pharmacies.
- Avoid ER for Non-Emergencies: Reserve the emergency room for true medical emergencies to avoid exorbitant costs. An urgent care clinic is a more cost-effective alternative for most HFMD symptoms.
- Preventative Care: Investing in good hygiene and preventive measures (like regular handwashing) can save you from potential medical costs down the line.
Frequently Asked Questions
Is Hand, Foot, and Mouth Disease more severe in adults?
Yes, many adults report that HFMD symptoms are significantly more severe than in children. This is often attributed to a stronger immune response, leading to more intense inflammation, higher fevers, more widespread and painful rashes, and debilitating oral lesions that make eating and drinking very difficult. Recovery can also be more prolonged in adults.
How long is an adult contagious with HFMD?
Adults are most contagious during the first week of illness, especially when fever is present and blisters are active. However, the virus can continue to be shed in feces for several weeks, even after symptoms have resolved. It's recommended to stay home until fever has subsided for 24 hours without medication and blisters have crusted over, typically 7-10 days.
Can I get HFMD if I had it as a child?
Yes, it is possible to get HFMD multiple times, even if you had it as a child. This is because there are several different strains of enteroviruses that can cause the disease. Infection with one strain provides immunity to that specific strain but not to others. This means adults can still contract HFMD from a different viral strain.
What are the best home remedies for adult HFMD?
Effective home remedies focus on symptomatic relief. These include staying hydrated with water, broths, and oral rehydration solutions; managing pain and fever with acetaminophen or ibuprofen; using warm salt water rinses or OTC oral numbing gels for mouth sores; and eating soft, bland foods. Rest is also crucial for recovery.
Are the oral sores from HFMD similar to what causes tonsil stones?
No, the oral sores from HFMD are not similar to tonsil stones, nor do they cause them. HFMD sores are painful blisters or ulcers on various parts of the mouth and throat caused by a viral infection. Tonsil stones, on the other hand, are calcified deposits of food debris, dead cells, and bacteria that accumulate in the crypts of the tonsils, often causing bad breath but not typically pain or widespread oral lesions. While both involve the throat area, their causes, appearance, and implications are entirely different.
When should an adult with HFMD see a doctor?
An adult should see a doctor if symptoms are unusually severe, if fever persists for more than three days, if there are signs of dehydration (e.g., decreased urination, severe dizziness), if pain is unmanageable with OTC medications, or if any neurological symptoms develop (e.g., severe headache, stiff neck, confusion).
Can HFMD in adults lead to long-term health problems?
For most adults, HFMD resolves without long-term health problems. However, rare complications like viral meningitis, encephalitis, or myocarditis can have serious long-term consequences. Temporary nail shedding (onychomadesis) is a relatively common post-infection effect but is not considered a serious long-term health problem.
How much does it cost for an adult to get diagnosed and treated for HFMD?
Without insurance, an adult could expect to pay anywhere from $20 (for self-care with OTC medications) to $400-$600+ (for an urgent care visit, prescriptions, and potential follow-ups). With insurance, costs are typically much lower, often a co-pay of $20-$100 for a doctor's visit and $10-$50 for prescriptions, assuming deductibles are met.
Can HFMD affect dental health directly?
While HFMD causes painful oral lesions that can make eating and oral hygiene difficult during the illness, it generally does not cause direct long-term dental health issues. Temporary disruptions in brushing or flossing due to pain can be overcome once symptoms resolve. However, severe dehydration can impact oral health by reducing saliva flow, increasing risk of cavities, but this is an indirect effect.
Is there a vaccine for adult HFMD?
Currently, there is no vaccine for Hand, Foot, and Mouth Disease approved or widely available in the United States for adults or children. Research is ongoing, particularly for vaccines against the more severe Enterovirus 71 strain, but these are not yet globally accessible.
When to See a Dentist
While HFMD is a viral infection primarily managed by a medical doctor, certain oral aspects may warrant dental attention, or at least a dental professional can offer valuable insights.
- Severe Oral Pain Unresponsive to Home Care: If the mouth sores are so intensely painful that they prevent you from eating, drinking, or maintaining basic oral hygiene, and OTC remedies are insufficient, a dentist can assess the severity and potentially prescribe stronger topical anesthetics (like viscous lidocaine) or suggest specific oral rinses to alleviate discomfort. An ADA-recommended approach is to ensure oral pain doesn't lead to dehydration or secondary infections.
- Confusion with Other Oral Conditions: If you are unsure whether your oral lesions are due to HFMD, canker sores, cold sores, or another condition, a dental professional is highly skilled in differentiating oral pathologies. Incorrect self-diagnosis can delay proper management.
- Signs of Secondary Oral Infection: While rare, open mouth sores can sometimes develop a secondary bacterial infection. If you notice increasing redness, swelling, pus, or a foul odor from your mouth sores, a dentist can evaluate for bacterial infection and recommend appropriate treatment, which might include antibiotics.
- Concerns about Dehydration Affecting Oral Health: Prolonged difficulty drinking due to oral pain can lead to dehydration, which reduces saliva production and increases the risk of dry mouth and even tooth decay. A dentist can provide advice on managing dry mouth symptoms and maintaining oral health during recovery.
- Post-Recovery Follow-up: If the oral lesions were particularly severe or caused you significant distress, a follow-up dental check-up after full recovery can ensure that your oral tissues have healed properly and that no lingering issues are present.
Red Flags Needing Immediate Medical (or Dental if severe oral issue) Attention:
- Any signs of severe dehydration.
- Persistent high fever despite medication.
- Severe headache, stiff neck, or confusion.
- Difficulty breathing or chest pain.
- Unmanageable oral pain preventing any intake of fluids.
For most cases of adult HFMD, your primary care physician or an urgent care clinic will be the main point of contact. However, do not hesitate to consult your dentist for specific concerns related to oral health and severe mouth pain.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles

Oral Candidiasis Symptoms: Complete Guide
Oral candidiasis, commonly known as oral thrush, is a fungal infection of the mouth caused by an overgrowth of Candida yeast, most often Candida albicans. While Candida is a normal inhabitant of the human mouth in small amounts, an imbalance can lead to uncomfortable and sometimes painful symptoms
February 23, 2026
Are Cold Sores Contagious
In the United States, an estimated 67% of the population under age 50 carries the herpes simplex virus type 1 (HSV-1), the primary cause of cold sores. This means millions of Americans are susceptible to these often painful and highly visible oral lesions. Beyond the discomfort and cosmetic conc
February 23, 2026
How Long Does Hand Foot and Mouth Last
Hand, Foot, and Mouth Disease (HFMD) is a common, often uncomfortable, viral illness that can affect anyone but is particularly prevalent among young children. If you or a loved one has ever experienced the tell-tale rash or painful mouth sores, you've likely wondered: **how long does Hand Foot and
February 23, 2026
Cold Sore vs Pimple on Lip: Complete Comparison Guide
When you notice an unexpected bump or lesion on your lip, your mind might immediately jump to questions of what it is, how long it will last, and most importantly, if it's contagious. The confusion between a cold sore vs pimple on lip is incredibly common, yet the distinction is crucial for prop
February 23, 2026