Inflammation in Gums Home Remedy: Complete Guide
Key Takeaways
- More than half of American adults over the age of 30 show signs of gum disease, a condition often heralded by inflammation of gum tissue. You might have experienced it: that tell-tale tenderness, redness, or even bleeding when you brush or floss. While these symptoms can seem minor, ignoring
More than half of American adults over the age of 30 show signs of gum disease, a condition often heralded by inflammation of gum tissue. You might have experienced it: that tell-tale tenderness, redness, or even bleeding when you brush or floss. While these symptoms can seem minor, ignoring them can lead to serious oral health complications and even impact your overall systemic health. The good news is that for early stages of gum inflammation, often referred to as gingivitis, effective inflammation in gums home remedy options can provide relief and help restore gum health.
This comprehensive guide from SmilePedia.net will equip you with everything you need to understand, address, and prevent inflamed gums. We'll explore the causes, recognize the warning signs, and dive deep into medically sound home remedies and professional treatments. You'll learn how simple daily habits and targeted interventions can make a significant difference, empowering you to take control of your oral well-being and maintain a healthy, vibrant smile.
Key Takeaways:
- Gingivitis is highly common: Affecting over 50% of U.S. adults, early detection and treatment are crucial to prevent progression to more severe periodontitis.
- Home remedies offer initial relief: Simple, accessible methods like salt water rinses (costing less than $5/month) and proper oral hygiene can effectively reduce mild gum inflammation.
- Consistency is key: Daily brushing (twice), flossing (once), and regular mouthwash use are foundational for preventing and managing gum inflammation.
- Professional dental care is essential: Even with home remedies, regular dental check-ups and professional cleanings (typically $75-$200 without insurance, every 6 months) are vital to remove hardened plaque (tartar) and address underlying issues.
- Deep cleaning (Scaling and Root Planing) for moderate cases: If inflammation progresses, a deep cleaning might be necessary, costing an average of $200-$500 per quadrant without insurance.
- Early intervention saves money and prevents complications: Addressing gum inflammation promptly can prevent costly treatments like gum surgery (potentially $500-$10,000+) and systemic health risks.
- Improvement timeline: Many home remedies can show noticeable improvement in mild inflammation within 3-7 days of consistent application, though full resolution and prevention require ongoing effort.
What Is Gum Inflammation? An Overview
Gum inflammation, medically known as gingivitis, is the earliest and mildest form of periodontal (gum) disease. It occurs when plaque, a sticky film of bacteria, builds up on your teeth and irritates the surrounding gum tissue. This irritation triggers an inflammatory response, leading to the characteristic signs of red, swollen, and sometimes bleeding gums.
Think of your gums as the foundation for your teeth. When this foundation becomes inflamed, it weakens, creating an environment ripe for further bacterial invasion. If left unaddressed, gingivitis can progress to periodontitis, a more severe form of gum disease where the inflammation spreads below the gum line, damaging the bone and connective tissue that hold your teeth in place. This can eventually lead to tooth loosening and loss. Understanding the initial signs and taking prompt action with effective gums inflammation treatment is critical for preserving your oral health.
Types of Gum Inflammation (Gingivitis)
While the general term "gingivitis" refers to gum inflammation, there are several variations based on their cause:
Plaque-Induced Gingivitis
This is by far the most common type. It's directly caused by the accumulation of bacterial plaque on the teeth due, primarily, to inadequate oral hygiene. The bacteria in plaque produce toxins that irritate the gum tissue, leading to inflammation. This type is generally reversible with proper oral hygiene and professional cleaning.
Non-Plaque-Induced Gingival Lesions
These forms of gum inflammation are less common and are not primarily caused by plaque but by other factors. They might include:
- Genetic/Developmental Disorders: Conditions like hereditary gingival fibromatosis.
- Specific Infections: Viral (e.g., herpes), fungal (e.g., candidiasis), or bacterial infections (other than typical plaque bacteria).
- Inflammatory and Immune Conditions: Autoimmune diseases like lichen planus, pemphigoid, or lupus erythematosus can manifest in the gums.
- Traumatic Lesions: Injury from aggressive brushing, chemical burns, or ill-fitting dental appliances.
- Foreign Body Reactions: Inflammation around a piece of foreign material embedded in the gum.
- Systemic Conditions: Diseases like diabetes can exacerbate or alter the presentation of gingivitis.
It's important to differentiate these from plaque-induced gingivitis, as their treatment approaches will vary. A dentist can help diagnose the specific type of inflammation of gum you may be experiencing.
Causes: Why Gums Become Inflamed
The primary culprit behind most cases of gum inflammation is bacterial plaque. However, several contributing factors can increase your susceptibility:
1. Poor Oral Hygiene
This is the leading cause. When you don't brush and floss adequately, plaque accumulates along the gum line and between teeth. Over time, plaque hardens into tartar (calculus), which cannot be removed by brushing alone. Both plaque and tartar harbor bacteria that irritate the gums, leading to inflammation.
2. Hormonal Changes
Fluctuations in hormones, particularly during puberty, pregnancy, menstruation, and menopause, can make gums more sensitive and increase blood flow, leading to heightened inflammatory responses to plaque bacteria. Pregnant women, for example, often experience "pregnancy gingivitis."
3. Smoking and Tobacco Use
Smoking is a significant risk factor for gum disease. It impairs the immune system, making it harder for gum tissue to fight off infection, and restricts blood flow, masking some of the visible signs of inflammation (like bleeding). Smokers are far more likely to develop severe gum disease.
4. Certain Medications
Some medications can cause dry mouth (xerostomia), reducing saliva's protective effects and allowing plaque to build up more easily. Others, like certain anticonvulsants (e.g., phenytoin) and calcium channel blockers (e.g., nifedipine), can cause gingival overgrowth, making gums harder to clean and more prone to inflammation.
5. Systemic Diseases
Conditions such as diabetes, HIV/AIDS, and certain autoimmune diseases can compromise the immune system, making individuals more vulnerable to infections, including gum inflammation. Uncontrolled diabetes, in particular, significantly increases the risk and severity of periodontal disease.
6. Nutritional Deficiencies
While less common in developed countries, severe deficiencies in vitamins, particularly Vitamin C (scurvy), can lead to bleeding and inflamed gums.
7. Genetics
Some people are genetically predisposed to developing gum disease, making good oral hygiene even more critical for them.
8. Stress
Chronic stress can weaken the immune system, making your body less able to fight off infections, including those in your gums.
9. Misaligned Teeth or Poorly Fitting Dental Restorations
Crooked teeth, gaps, or old, ill-fitting fillings, crowns, or bridges can create areas where plaque and food particles easily accumulate and are difficult to clean, leading to localized inflammation.
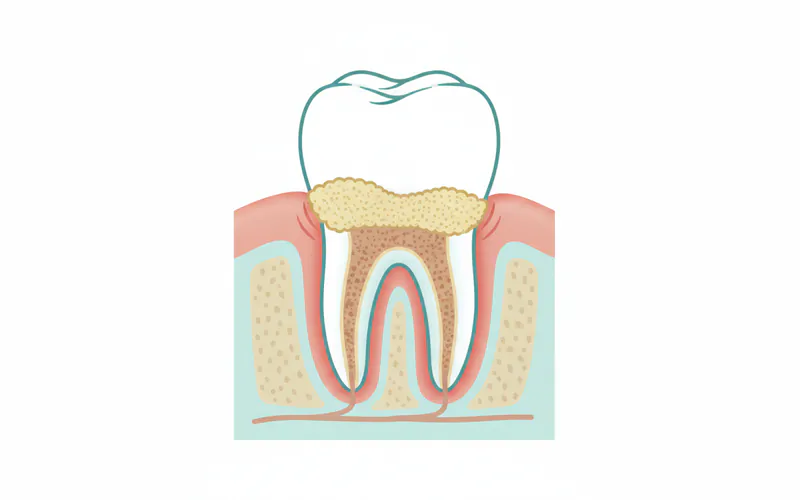
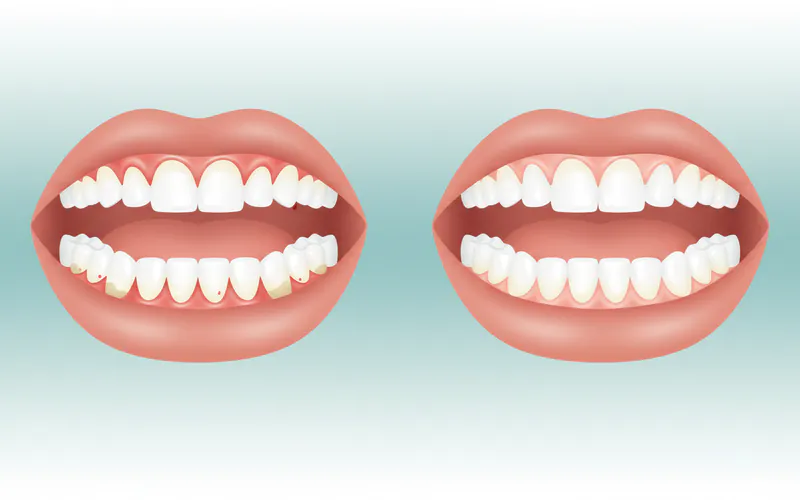
Signs and Symptoms of Inflamed Gums
Recognizing the early signs of gum inflammation is crucial for prompt treatment. Don't wait for pain to signal a problem.
Common Symptoms:
- Red or Purplish Gums: Healthy gums are typically a pale pink. Inflamed gums appear darker due to increased blood flow.
- Swollen or Puffy Gums: The gum tissue may look enlarged or distended, especially around the teeth.
- Tender or Sore Gums: Your gums might feel sensitive to touch.
- Bleeding Gums: This is one of the most common signs, particularly when brushing, flossing, or eating hard foods. Even light bleeding should not be ignored.
- Receding Gums: Over time, inflammation can cause the gum tissue to pull away from the teeth, making teeth appear longer.
- Bad Breath (Halitosis): The bacteria responsible for gum inflammation also produce foul-smelling gases.
- Metallic Taste in Mouth: Some people report a persistent unpleasant taste.
When to Be Concerned:
While some minor bleeding during aggressive brushing can happen, persistent bleeding, significant swelling, pain, or any of the above symptoms lasting more than a few days warrant attention. These are clear indicators that your gums need help.
Treatment Options for Gum Inflammation
Addressing gum inflammation typically involves a combination of professional dental care and diligent home care. For mild cases, particularly early gingivitis, inflammation in gums home remedy approaches can be very effective.
A. Home Remedies for Mild Gum Inflammation
These remedies can help reduce inflammation, soothe discomfort, and support healing, especially when combined with improved oral hygiene.
-
Salt Water Rinse:
- Description: A classic, simple, and effective remedy. Salt acts as a natural disinfectant and helps reduce swelling.
- How to Use: Dissolve ½ to 1 teaspoon of salt in 8 ounces of warm water. Swish the solution around your mouth for 30-60 seconds, then spit it out.
- Frequency: 2-3 times a day, especially after meals.
- Pro Tip: Warm water is more soothing and helps dissolve salt better.
-
Oil Pulling:
- Description: An ancient Ayurvedic practice involving swishing oil (like coconut oil, sesame oil) in the mouth. It's believed to "pull" bacteria and toxins from the mouth.
- How to Use: Swish 1 tablespoon of organic coconut oil (or sesame oil) in your mouth for 15-20 minutes, then spit it into a trash can (not sink, as it can clog pipes). Do NOT swallow.
- Frequency: Once a day, preferably in the morning before brushing.
- Evidence: While anecdotal evidence is strong, scientific studies on its direct effect on gingivitis are ongoing and mixed. It's generally considered safe as a complementary practice.
-
Aloe Vera:
- Description: Known for its anti-inflammatory and soothing properties.
- How to Use: Rinse your mouth with pure aloe vera juice (food-grade, specifically for oral use) or gently apply a small amount of aloe vera gel directly to the inflamed gums.
- Frequency: 2-3 times a day.
- Pro Tip: Ensure you're using 100% pure aloe vera that is safe for internal use and does not contain added sugars or irritants.
-
Turmeric Paste/Rinse:
- Description: Turmeric contains curcumin, a powerful anti-inflammatory and antimicrobial compound.
- How to Use: Mix a small amount of turmeric powder with water or coconut oil to form a paste. Apply it to the inflamed areas and leave for 5-10 minutes before rinsing. Alternatively, a turmeric-based mouthwash can be used.
- Frequency: Once a day for a week or two.
- Caution: Turmeric can temporarily stain teeth yellow; gentle brushing afterward can help.
-
Clove Oil:
- Description: Cloves have natural analgesic (pain-relieving) and antiseptic properties.
- How to Use: Dilute a few drops of clove oil in a carrier oil (like olive oil) or water. Apply a small amount to a cotton swab and gently dab it on the inflamed gum areas.
- Frequency: As needed for discomfort, up to 2-3 times a day.
- Caution: Clove oil is potent; always dilute it and avoid swallowing large amounts.
-
Warm or Cold Compresses:
- Description: Can help reduce swelling and pain. Warm compresses increase blood flow, promoting healing, while cold compresses can numb the area and reduce swelling directly.
- How to Use: For warmth, soak a clean cloth in warm water and hold it against your face over the affected area. For cold, wrap an ice pack in a cloth and apply.
- Frequency: As needed for comfort, 10-15 minutes at a time.
B. Professional Dental Treatments
While home remedies provide relief, professional intervention is often necessary, especially if inflammation is persistent or has progressed beyond early gingivitis.
-
Professional Dental Cleaning (Prophylaxis):
- Description: A routine cleaning where a dental hygienist or dentist removes plaque and tartar from above the gum line using specialized instruments.
- When It's Needed: Recommended every six months for most individuals as a preventative measure and for early, mild gingivitis.
- Pros: Prevents progression of gum disease, removes hard-to-reach deposits, fresh breath.
- Cons: Not sufficient for advanced gum disease.
- Cost: Typically $75-$200 without insurance.
-
Scaling and Root Planing (Deep Cleaning):
- Description: This is a non-surgical procedure that goes deeper than a regular cleaning. Scaling removes plaque and tartar from both above and below the gum line, and root planing smooths the tooth root surfaces to remove bacterial toxins and prevent future plaque adhesion.
- When It's Needed: For moderate gingivitis or early to moderate periodontitis, where pockets have formed between the gums and teeth.
- Pros: Removes deep-seated infection, helps gums reattach to teeth, can prevent the need for surgery.
- Cons: May require local anesthetic, can cause temporary sensitivity, may require multiple appointments (often 1-2 quadrants per visit).
- Cost: Average $200-$500 per quadrant (totaling $800-$2,000 for a full mouth) without insurance.
-
Antibiotics:
- Description: Oral antibiotics (e.g., doxycycline, metronidazole) or topical antibiotic gels/chips (e.g., chlorhexidine, Arestin) may be prescribed to control bacterial infection, especially after deep cleaning or in persistent cases.
- When It's Needed: For aggressive forms of periodontitis or to supplement deep cleaning in severe cases.
- Pros: Directly targets bacteria.
- Cons: Oral antibiotics can have side effects (e.g., digestive upset, yeast infections), can contribute to antibiotic resistance.
- Cost: Oral antibiotics typically $10-$100; topical antibiotics can be $50-$150 per application.
-
Surgical Treatments:
- Description: For advanced periodontitis, when non-surgical methods are insufficient, surgical options like flap surgery (pocket reduction surgery), bone grafts, soft tissue grafts, or guided tissue regeneration may be necessary.
- When It's Needed: To repair significant damage caused by severe gum disease.
- Pros: Can save teeth, regenerate lost tissue/bone.
- Cons: Invasive, higher cost, longer recovery time, potential for discomfort.
- Cost: Highly variable, ranging from $500 for a single gum graft to $10,000+ for complex full-mouth procedures.
C. Over-the-Counter Products
- Antiseptic Mouthwashes: Mouthwashes containing chlorhexidine (prescription only in some concentrations), cetylpyridinium chloride, or essential oils can help reduce bacteria.
- Fluoride Toothpaste: Strengthens enamel and can help prevent cavities, which often go hand-in-hand with gum disease.
- Soft-Bristled Toothbrushes: Essential to prevent further irritation to inflamed gums.
- Interdental Cleaners: Floss, interdental brushes, or water flossers are critical for cleaning between teeth.
Comparison Table: Home Remedies vs. Professional Treatments
| Feature | Home Remedies (e.g., Salt Water Rinse) | Professional Cleaning (Prophylaxis) | Deep Cleaning (Scaling & Root Planing) |
|---|---|---|---|
| Target Issue | Mild inflammation, symptomatic relief, adjunct to professional care | Plaque & tartar above gum line, early gingivitis prevention | Plaque & tartar below gum line, gum pockets, moderate periodontitis |
| Effectiveness | Good for mild symptoms, but doesn't remove hardened plaque | Highly effective for prevention and early gingivitis | Highly effective for halting progression of moderate gum disease |
| Cost (Avg. US) | Very low (e.g., salt $5/month) | $75 - $200 (without insurance) | $800 - $2,000 (full mouth, without insurance) |
| Timeline for Result | Days for symptomatic relief, ongoing for prevention | Immediate cleanliness, ongoing prevention (every 6 months) | Weeks to months for full gum healing |
| Skill Required | None | Dental professional | Dental professional (hygienist or dentist) |
| Primary Benefit | Immediate relief, natural approach, accessibility | Preventative, thorough removal of superficial irritants | Addresses root cause of deeper infection, saves teeth |
| Limitations | Cannot remove tartar, not sufficient for advanced disease | Cannot remove subgingival calculus or treat deep pockets | May require multiple visits, local anesthetic, temporary sensitivity |
Step-by-Step Process for Treating Inflamed Gums
Successfully treating gums inflammation treatment requires a multi-pronged approach, combining diligent home care with professional guidance.
Step 1: Assess Your Symptoms and Oral Hygiene Habits
- Self-Check: Look for redness, swelling, bleeding when brushing/flossing. Note how long these symptoms have been present.
- Review Your Routine: Are you brushing twice a day for two minutes? Flossing daily? Using an ADA-accepted toothpaste?
Step 2: Implement Home Remedies for Initial Relief (If Mild)
- Start with Salt Water Rinses: Begin rinsing with warm salt water 2-3 times daily. This is your first line of defense against mild inflammation of gum.
- Consider Oil Pulling or Aloe Vera: If comfortable, incorporate oil pulling or aloe vera rinses into your routine.
- Gentle Brushing: Use a soft-bristled toothbrush and brush gently but thoroughly, focusing on the gum line.
- Consistent Flossing: Floss daily. Expect some initial bleeding if your gums are inflamed, but this should reduce within a few days of consistent flossing.
Step 3: Schedule a Dental Appointment
- Don't Delay: If symptoms persist after a few days of consistent home care, or if they are severe (significant pain, pus, loose teeth), schedule an appointment with your dentist promptly.
- What to Expect at the Dentist:
- Comprehensive Exam: The dentist will examine your gums, teeth, and mouth. They'll use a probe to measure the depth of the pockets between your teeth and gums (pocket depth of 1-3mm is healthy).
- X-rays: May be taken to assess bone health around your teeth.
- Diagnosis: Based on the exam, the dentist will diagnose the severity of your gum inflammation (gingivitis vs. periodontitis).
- Treatment Plan: They will recommend a personalized treatment plan, which could include:
- Professional Cleaning (Prophylaxis): For mild gingivitis.
- Scaling and Root Planing (Deep Cleaning): For moderate cases with deeper pockets and tartar below the gum line.
- Prescription Mouthwash/Antibiotics: In some cases, to control infection.
- Referral to a Periodontist: For advanced periodontitis requiring surgical intervention.
Step 4: Follow Through with Professional Treatment
- Attend Appointments: Complete all recommended dental cleanings or deep cleaning sessions.
- Take Medications as Prescribed: If antibiotics are prescribed, take them exactly as directed.
Step 5: Maintain and Prevent Recurrence
- Commit to Excellent Oral Hygiene: This is paramount. Brush twice daily, floss daily, and use an antiseptic mouthwash if recommended by your dentist.
- Regular Dental Check-ups: Adhere to your dentist's recommended schedule for follow-up appointments and routine cleanings (typically every 6 months, or more frequently for periodontal maintenance).
- Lifestyle Adjustments: Quit smoking, manage systemic diseases like diabetes, and eat a balanced diet.
Cost and Insurance for Gum Inflammation Treatment in the US
Understanding the financial aspects of gums inflammation treatment is crucial for planning your dental care. Costs can vary significantly based on the severity of your condition, the type of treatment, your location, and whether you have dental insurance.
Average US Costs (Without Insurance):
- Routine Dental Cleaning (Prophylaxis):
- Range: $75 - $200 per visit.
- Frequency: Typically every 6 months.
- Scaling and Root Planing (Deep Cleaning):
- Range: $200 - $500 per quadrant. Since there are four quadrants in the mouth, a full mouth deep cleaning can range from $800 - $2,000.
- Frequency: Usually a one-time intensive treatment, followed by periodontal maintenance.
- Periodontal Maintenance:
- Range: $100 - $300 per visit.
- Frequency: Often recommended every 3-4 months after deep cleaning to prevent recurrence.
- Prescription Antibiotics (Oral):
- Range: $10 - $100 for a course.
- Topical Antibiotics (e.g., Arestin):
- Range: $50 - $150 per application site.
- Gum Surgery (e.g., Flap Surgery, Grafting):
- Range: Highly variable, from $500 to $10,000+ depending on the complexity, extent, and type of surgery.
Impact of Dental Insurance:
Most dental insurance plans in the US categorize treatments for gum inflammation as follows:
- Preventive Care (Routine Cleanings, X-rays, Exams): Often covered at 80-100%. Many plans cover two routine cleanings per year.
- Basic Procedures (Scaling and Root Planing, Fillings): Typically covered at 50-80% after a deductible is met. There might be a waiting period (e.g., 6 months) for these procedures.
- Major Procedures (Gum Surgery, Crowns): Usually covered at 20-50% after a deductible, with longer waiting periods (e.g., 12 months).
Key things to check with your insurance provider:
- Deductible: The amount you must pay out-of-pocket before your insurance starts to cover costs.
- Annual Maximum: The maximum amount your insurance will pay for your dental care in a calendar year (often $1,000-$2,000).
- Waiting Periods: How long you must be enrolled before certain procedures are covered.
- In-Network vs. Out-of-Network: Costs are usually lower with in-network providers.
Payment Plans and Financing Options:
- Dental Office Payment Plans: Many dental offices offer in-house payment plans, allowing you to pay in installments.
- Third-Party Financing (e.g., CareCredit): These programs offer credit lines specifically for healthcare costs, often with interest-free periods if paid within a certain timeframe.
- Flexible Spending Accounts (FSAs) / Health Savings Accounts (HSAs): If you have an FSA or HSA through your employer, you can use pre-tax dollars to pay for dental expenses, which can offer significant savings.
- Dental Schools: University dental schools often provide services at a reduced cost, as procedures are performed by students under the supervision of experienced faculty.
Recovery and Aftercare for Inflamed Gums
Effective recovery and aftercare are vital to ensure your gums heal properly and remain healthy. This phase involves diligent home care and adherence to professional recommendations.
After Professional Treatment (e.g., Deep Cleaning):
- Expect Sensitivity: It's normal to experience some gum soreness, tenderness, and tooth sensitivity for a few days to a week after scaling and root planing.
- Pain Management: Over-the-counter pain relievers (like ibuprofen or acetaminophen) can help manage discomfort. Your dentist might also prescribe a stronger pain medication if needed.
- Diet: Stick to soft foods for the first few days, avoiding very hot, cold, spicy, or crunchy foods that could irritate your gums.
- Oral Hygiene: Continue brushing gently with a soft-bristled toothbrush. Your dentist might recommend a special antiseptic mouthwash (e.g., chlorhexidine) for a short period to aid healing and reduce bacteria. Avoid aggressive rinsing for the first 24 hours.
- Bleeding: Minor bleeding after treatment is normal, but persistent or heavy bleeding should be reported to your dentist.
Long-Term Aftercare and Prevention:
The cornerstone of long-term gum health, whether you've had home remedies or professional treatment, is consistent and meticulous oral hygiene.
- Brush Twice Daily: Use an ADA-accepted fluoride toothpaste and a soft-bristled toothbrush. Brush gently for two minutes each time, angling the brush at 45 degrees towards the gum line to clean effectively without irritation.
- Floss Daily: This is non-negotiable for removing plaque and food particles from between teeth and under the gum line, where a toothbrush can't reach. If traditional floss is difficult, consider a water flosser or interdental brushes.
- Use Antiseptic Mouthwash: If recommended by your dentist, an antiseptic mouthwash can help control bacteria, but it should never replace brushing and flossing.
- Regular Dental Check-ups and Cleanings: Follow your dentist's recommendations, usually every 6 months for preventive care, or 3-4 months for periodontal maintenance if you've had gum disease.
- Quit Smoking: Smoking significantly hinders gum healing and increases the risk of recurrence. Quitting is one of the most impactful steps you can take for your oral and overall health.
- Manage Systemic Health Conditions: If you have diabetes or other systemic diseases, work with your medical doctor to keep them under control, as they directly impact gum health.
- Balanced Diet: A diet rich in vitamins and minerals supports overall immune function and gum health. Limit sugary foods and drinks that promote bacterial growth.
Pro Tip: Consider investing in an electric toothbrush. Many models have pressure sensors to prevent over-brushing and built-in timers to ensure you brush for the full two minutes, making your oral hygiene routine more effective.
Risks and Complications of Untreated Gum Inflammation
Ignoring gum inflammation, even if it seems minor, carries significant risks and can lead to serious complications, extending beyond your mouth.
Oral Health Complications:
- Progression to Periodontitis: The most direct risk. Untreated gingivitis inevitably progresses to periodontitis, where the inflammation spreads, destroying the bone and connective tissues that support your teeth.
- Tooth Loss: As periodontitis advances, teeth can become loose and may eventually need to be extracted or fall out spontaneously.
- Gum Recession: Chronic inflammation can cause gums to pull away from the teeth, exposing sensitive root surfaces and making teeth appear longer.
- Abscess Formation: Pockets of pus can form in the gums or around the tooth roots, leading to pain, swelling, and further infection.
- Increased Cavity Risk: Exposed tooth roots due to gum recession are more susceptible to decay.
- Dental Sensitivity: Exposed root surfaces are highly sensitive to hot, cold, and sweet stimuli.
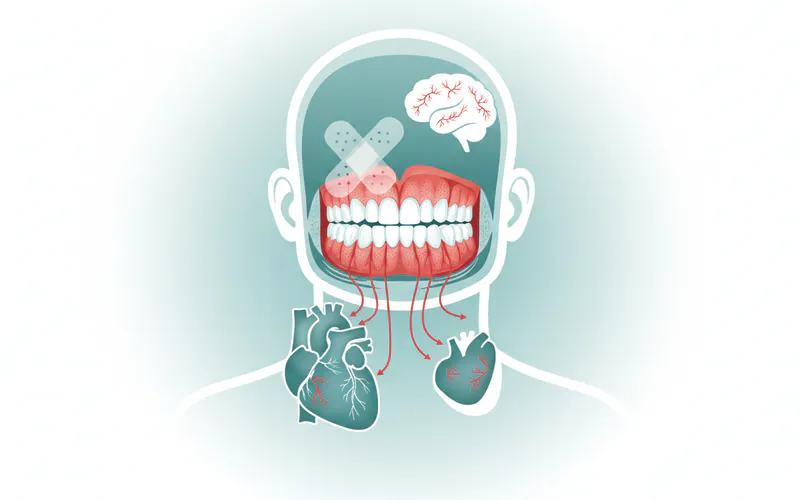
Systemic Health Complications (Oral-Systemic Link):
The inflammation and bacteria from gum disease don't stay confined to your mouth. They can enter your bloodstream and affect distant parts of your body.
- Cardiovascular Disease: Research suggests a strong link between severe gum disease and an increased risk of heart attack, stroke, and other cardiovascular problems. Bacteria from the mouth can contribute to arterial plaque formation.
- Diabetes Management: There's a bidirectional relationship. People with diabetes are more prone to gum disease, and severe gum disease can make it harder to control blood sugar levels.
- Respiratory Diseases: Oral bacteria can be inhaled into the lungs, potentially leading to respiratory infections like pneumonia, especially in older adults or those with compromised immune systems.
- Adverse Pregnancy Outcomes: Gum disease in pregnant women has been linked to an increased risk of preterm birth and low birth weight babies.
- Rheumatoid Arthritis: Some studies indicate a correlation between gum disease and an increased risk or exacerbation of rheumatoid arthritis.
- Dementia/Alzheimer's Disease: Emerging research is exploring a potential link between chronic oral inflammation and neurodegenerative diseases.
Pro Tip: The ADA emphasizes that maintaining good oral health is a critical component of your overall health and well-being. Don't underestimate the profound impact your gums can have on your entire body.
Children / Pediatric Considerations for Gum Inflammation
While less common in severe forms, children and adolescents can also experience inflammation of gum tissue, primarily gingivitis. It's crucial for parents to be aware of the signs and encourage good oral hygiene habits from an early age.
Causes in Children:
- Poor Brushing and Flossing: Just like adults, the primary cause is inadequate plaque removal. Children often need assistance or supervision with brushing until they develop sufficient dexterity (around age 7-8).
- Orthodontic Appliances: Braces and retainers create more areas for food and plaque to trap, making thorough cleaning more challenging.
- Hormonal Changes: Puberty can lead to "puberty gingivitis" due to increased hormone levels making gums more sensitive to plaque.
- Mouth Breathing: Can dry out gum tissue, making it more susceptible to inflammation.
- Certain Medications: Similar to adults, some medications can cause gingival enlargement.
- Eruption Gingivitis: Temporary inflammation around teeth that are erupting (coming through the gums).
Signs and Symptoms in Children:
Parents should look for:
- Red, swollen gums
- Bleeding when brushing or flossing (even light bleeding)
- Bad breath
- Gums that look shiny or puffy
Home Remedies and Prevention for Children:
- Supervised Brushing: Until age 7 or 8, actively supervise or assist your child with brushing. Teach them to brush for two minutes, twice a day, using a fluoride toothpaste appropriate for their age.
- Flossing Education: Introduce flossing once daily as soon as teeth touch. Use child-friendly flossers if traditional floss is too difficult.
- Healthy Diet: Limit sugary snacks and drinks, which contribute to plaque formation. Encourage water consumption.
- Regular Dental Check-ups: Children should see a dentist every six months starting from their first tooth eruption or by their first birthday. These visits help monitor gum health, provide professional cleanings, and teach proper oral hygiene techniques.
- Address Orthodontic Challenges: If your child has braces, ensure they are using special brushes and techniques recommended by their orthodontist to clean around brackets and wires.
- Salt Water Rinses: For mild inflammation, a warm salt water rinse (using a child-safe concentration, ½ tsp in 8 oz water) can be used for older children who can swish and spit without swallowing.
Pro Tip for Parents: Make oral hygiene fun! Use toothbrushes with cartoon characters, flavored toothpaste, and play songs during brushing time. Lead by example and brush and floss with your child.
Frequently Asked Questions about Gum Inflammation
### 1. Can gum inflammation heal on its own?
Mild gum inflammation (gingivitis) can often resolve with strict and consistent oral hygiene at home, including regular brushing and flossing, and sometimes with the help of home remedies like salt water rinses. However, it's crucial to address the underlying cause (plaque buildup) and typically requires professional dental cleaning to remove hardened tartar that brushing cannot. Without proper care, it's more likely to worsen.
### 2. How long does it take for inflamed gums to heal?
For mild gingivitis, you might see significant improvement in redness and bleeding within 3-7 days of consistent, excellent oral hygiene and home remedies. Complete healing and resolution of inflammation can take 1-2 weeks. If the inflammation is more severe or requires professional deep cleaning (scaling and root planing), full healing of the gum tissue can take several weeks to a few months, with ongoing maintenance.
### 3. Is bleeding gums always a sign of gum inflammation?
Yes, bleeding gums are almost always a sign of inflammation or trauma. While occasional bleeding from very aggressive brushing might occur, persistent or regular bleeding when you brush, floss, or even eat indicates that your gums are inflamed and irritated, typically due to plaque buildup. It's a critical warning sign that should not be ignored.
### 4. What's the difference between gingivitis and periodontitis?
Gingivitis is the initial, milder stage of gum disease, characterized by inflamed, red, swollen, and bleeding gums caused by plaque. It is reversible with good oral hygiene. Periodontitis is a more advanced and serious stage where the inflammation has spread below the gum line, causing the gums to pull away from the teeth, forming pockets, and damaging the bone and connective tissues supporting the teeth. Periodontitis is not reversible and requires professional intervention to manage and prevent tooth loss.
### 5. Are home remedies like oil pulling truly effective for gum inflammation?
Home remedies like salt water rinses have strong anecdotal evidence and some scientific backing for their antiseptic and anti-inflammatory effects. Oil pulling is a traditional practice with some emerging research suggesting benefits for reducing plaque and gingivitis, but more robust scientific studies are needed to confirm its efficacy. They are generally considered safe as complementary treatments but should not replace professional dental care.
### 6. What if my gums are inflamed but don't bleed?
It is possible to have inflamed gums (redness, swelling, tenderness) without immediate bleeding, especially if the inflammation is very early or if you are a smoker (smoking can constrict blood vessels, masking bleeding). However, if left untreated, bleeding will likely develop. Any persistent signs of inflammation warrant a dental check-up.
### 7. Can certain foods cause gum inflammation?
Foods high in sugar and refined carbohydrates can contribute to gum inflammation indirectly. These foods feed the bacteria in your mouth, leading to increased plaque production and acid attacks, which irritate the gums. A balanced diet rich in vitamins and minerals (especially Vitamin C) can support gum health, while poor nutrition can weaken immune response.
### 8. What's the average cost for professional gum inflammation treatment with insurance?
The average cost for professional treatment with insurance varies significantly. Routine cleanings are often covered 80-100%. Deep cleanings (scaling and root planing) are typically covered 50-80% after your deductible, meaning you might pay $160-$1,000 for a full mouth deep cleaning. More advanced surgical treatments have lower coverage, often 20-50%, and higher out-of-pocket costs, possibly in the thousands. Always check your specific plan details.
### 9. Can I use hydrogen peroxide for inflamed gums?
Diluted hydrogen peroxide can be used as a temporary oral rinse to reduce bacteria and can help with mild gingivitis, particularly for its oxygen-releasing action which can disrupt anaerobic bacteria. However, prolonged or undiluted use can irritate soft tissues, potentially cause damage, and whiten the gums. It's best used short-term (e.g., 3% solution mixed with equal parts water) and under dental guidance, not as a long-term solution.
### 10. When should I see a periodontist instead of a general dentist for gum inflammation?
You should see a periodontist (a gum specialist) if your general dentist diagnoses you with moderate to severe periodontitis, if your gum disease is aggressive, if it's not responding to initial deep cleaning treatments, or if you require advanced procedures like gum surgery, bone grafts, or soft tissue grafts. A general dentist will typically refer you to a periodontist when specialized care is needed.
When to See a Dentist
While home remedies can offer temporary relief for mild symptoms and are crucial for maintenance, it's vital to know when professional dental care is necessary. Ignoring persistent or worsening symptoms can lead to irreversible damage.
You should schedule an appointment with your dentist if you experience any of the following:
- Persistent Bleeding Gums: If your gums bleed consistently when brushing, flossing, or spontaneously, and this doesn't improve within a few days of diligent home care.
- Significant Swelling or Pain: If your gums are noticeably swollen, very red, tender to the touch, or causing you persistent pain that over-the-counter pain relievers don't alleviate.
- Receding Gums: If you notice your gums pulling away from your teeth, making your teeth look longer.
- Chronic Bad Breath or Unpleasant Taste: If you have persistent bad breath or a metallic taste in your mouth that doesn't resolve with good oral hygiene.
- Loose Teeth or Changes in Bite: These are signs of advanced gum disease (periodontitis) and require immediate professional attention.
- Pus Between Teeth and Gums: This indicates an active infection and necessitates urgent dental care.
- Symptoms Worsen Despite Home Remedies: If you've been diligently using home remedies and maintaining good oral hygiene for a week or more, and your symptoms are not improving or are getting worse.
- Any Suspected Abscess: A painful, swollen bump on your gums that might indicate a pus-filled infection.
Red Flags (Seek prompt attention, potentially emergency):
- Sudden, severe pain in your gums or teeth.
- Rapidly spreading swelling in your face or jaw.
- Difficulty swallowing or breathing due to oral swelling.
- High fever accompanied by severe gum symptoms.
Early intervention is always the best approach for gum inflammation. Don't wait for pain to become severe; regular dental check-ups are key to catching and treating issues before they escalate.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Does Oil Pulling Help Gut Health
The intricate connection between our oral health and overall well-being is a topic of growing fascination and scientific inquiry. Often, when we think of health, we focus on specific organs or systems, overlooking the crucial role of the mouth as a gateway to the rest of the body. One ancient practi
February 23, 2026
Does Oil Pulling Help With Inflammation
It's a question many health-conscious individuals ask as they explore natural remedies: does oil pulling help with inflammation? In an era where holistic approaches to wellness are gaining traction, the ancient practice of oil pulling has resurfaced, promising benefits that extend beyond oral hy
February 23, 2026
Oil Pulling for Kidney Disease: Complete Guide
Chronic kidney disease (CKD) affects an estimated 37 million adults in the United States, often progressing silently until advanced stages. What many may not realize is the profound connection between the health of their mouth and the health of their kidneys. As a bridge between traditional wisd
February 23, 2026
Oil Pulling Oral Microbiome: Complete Guide
Have you ever considered the bustling universe thriving within your mouth? This intricate community, known as the oral microbiome, consists of billions of microorganisms – some beneficial, some harmful – all playing a critical role in your oral and overall systemic health. Maintaining a balanced
February 23, 2026