Botox for Teeth Clenching: Complete Guide
Key Takeaways
- Do you often wake up with a dull headache, jaw pain, or find your teeth feel sensitive? You're not alone. Millions of Americans grapple with teeth clenching and grinding, a condition known as bruxism. While often dismissed as a minor nuisance, chronic bruxism can lead to severe dental damage, te
Botox for Teeth Clenching: Complete Guide
Do you often wake up with a dull headache, jaw pain, or find your teeth feel sensitive? You're not alone. Millions of Americans grapple with teeth clenching and grinding, a condition known as bruxism. While often dismissed as a minor nuisance, chronic bruxism can lead to severe dental damage, temporomandibular joint (TMJ) disorders, and debilitating pain, including persistent teeth grinding headaches. For many, traditional treatments offer insufficient relief, prompting a search for more effective solutions. This is where Botox for teeth clenching has emerged as a revolutionary therapeutic option, offering significant relief for those whose lives are impacted by this relentless condition.

At SmilePedia.net, our mission is to provide you with comprehensive, medically accurate information to empower your dental health decisions. This complete guide will delve deep into the world of Botox as a treatment for bruxism. We'll explore what causes teeth clenching, the various symptoms it presents, and a full spectrum of treatment options—from conventional approaches to the cutting-edge use of botulinum toxin type A. You'll learn how Botox works, what to expect during the procedure, typical costs, potential risks, and crucial aftercare instructions. By understanding this treatment thoroughly, you can have an informed discussion with your dental professional about whether Botox is the right path to alleviate your jaw pain and protect your smile.
Key Takeaways:
- Botox offers significant relief for chronic teeth clenching (bruxism) by relaxing the jaw muscles.
- It works by temporarily blocking nerve signals to the masseter and temporalis muscles, reducing their clenching force.
- Typical costs range from $400 to $1,500 per treatment session, depending on the number of units and provider, usually $10-$20 per unit.
- Results generally appear within 3-7 days and last 3 to 6 months, requiring repeat injections.
- Common side effects are mild and temporary, such as bruising or swelling at injection sites. Serious complications are rare.
- Many insurance plans do not cover Botox for bruxism if considered cosmetic, but medical necessity may sometimes qualify it for coverage.
- Botox can reduce teeth grinding headaches, jaw pain, and prevent further tooth damage and TMJ issues.
What is Bruxism and Teeth Clenching?
Bruxism is a common condition characterized by the involuntary clenching, grinding, or gnashing of teeth. It can occur during the day (awake bruxism) or, more commonly, at night while sleeping (sleep bruxism). While occasional teeth clenching might not cause harm, chronic bruxism can lead to a host of significant dental and medical problems.
Awake Bruxism typically involves sustained clenching of the teeth or bracing of the jaw. Individuals may not even be aware they are doing it, especially when focused on tasks, feeling stressed, or concentrating intensely. It's often related to stress, anxiety, or habitual behaviors.
Sleep Bruxism is a sleep-related movement disorder that involves rhythmic (or non-rhythmic) masticatory muscle activity during sleep. It's considered a parasomnia, meaning it's an undesirable physical event that occurs during sleep. Many individuals are unaware they grind their teeth at night until a sleeping partner notices the sound or a dentist identifies signs of wear and tear on their teeth. Sleep bruxism can be more damaging because the forces exerted on the teeth and jaw muscles can be significantly greater than during waking hours, as there's no conscious control or inhibition. The American Dental Association (ADA) recognizes bruxism as a significant concern, emphasizing the importance of early diagnosis and management to prevent long-term damage.
Why Do We Clench Our Teeth? Causes and Contributing Factors
The exact cause of bruxism isn't always clear, but it's often a multifactorial issue, meaning several factors can contribute to its development. Understanding these can help in effective management.
Psychological Factors
- Stress and Anxiety: This is arguably the most common culprit. High levels of stress, anxiety, frustration, or anger can lead to unconscious clenching during the day and grinding at night. The jaw muscles become a physical outlet for psychological tension.
- Personality Type: Individuals with aggressive, competitive, or hyperactive personality types may be more prone to bruxism.
Physical and Medical Factors
- Sleep Disorders: Sleep bruxism is strongly associated with other sleep disorders, particularly obstructive sleep apnea (OSA). People with OSA frequently experience interrupted breathing, and the body may respond by clenching or grinding teeth as it struggles to open the airway. Other sleep disturbances like snoring can also be linked.
- Malocclusion (Misaligned Bite): While historically thought to be a primary cause, current research suggests that malocclusion plays a less significant role than stress or sleep disorders. However, an improper bite can sometimes contribute to uneven forces on the teeth, potentially triggering clenching in some individuals.
- Certain Medications: Some antidepressant medications, especially selective serotonin reuptake inhibitors (SSRIs) like Prozac or Zoloft, can have bruxism as a side effect. Other drugs, including certain antipsychotics and stimulants, have also been linked.
- Substance Use: Consumption of caffeine, alcohol, nicotine, and illicit drugs like ecstasy can exacerbate or induce bruxism.
- Neurological Conditions: Rare cases of bruxism can be associated with certain neurological diseases such as Parkinson's disease, Huntington's disease, or other movement disorders.
- Genetic Predisposition: There's some evidence that bruxism may run in families, suggesting a genetic component.
- Gastroesophageal Reflux Disease (GERD): Some studies have shown a correlation between GERD and sleep bruxism, although the exact mechanism is still being investigated.
Other Factors
- Age: While bruxism can affect anyone, it's particularly common in young children and often decreases with age. However, chronic adult bruxism can persist for decades.
- Lifestyle: A high-stress lifestyle, irregular sleep patterns, and poor dietary habits can all contribute to the problem.
Identifying the underlying cause or contributing factors is a crucial first step in determining the most effective treatment plan, which may involve a combination of approaches.
The Damaging Effects of Teeth Clenching
The continuous, excessive force exerted by clenching and grinding can have widespread detrimental effects on your oral health and overall well-being. These issues can range from mild discomfort to severe, chronic pain and irreversible damage.
Dental Damage
- Tooth Wear and Fractures: The most common consequence is the wearing down of tooth enamel, exposing the sensitive dentin underneath. This can lead to chipped, flattened, or fractured teeth. In severe cases, teeth can be worn down to stumps.
- Increased Tooth Sensitivity: As enamel erodes, teeth become more sensitive to hot, cold, and sweet foods and drinks.
- Loose Teeth: Persistent force can loosen teeth in their sockets, potentially leading to tooth loss if not addressed.
- Gum Recession: The trauma can also contribute to the recession of gum tissue around the teeth.
- Damage to Dental Restorations: Fillings, crowns, bridges, and even dental implants can be damaged, cracked, or dislodged due to the intense pressure.
Temporomandibular Joint (TMJ) Disorders
The TMJ connects your jaw to your skull, acting like a sliding hinge. Chronic clenching overworks these joints and the surrounding muscles, leading to a group of conditions known as Temporomandibular Disorders (TMDs).
- Jaw Pain and Tenderness: A common symptom, often felt around the ear, in the jaw muscles, or radiating to the face.
- Clicking or Popping Jaw: The joint can make noises when opening or closing the mouth.
- Limited Jaw Movement: Difficulty opening the mouth wide, or the jaw feeling "locked" in an open or closed position.
- Facial Muscle Hypertrophy: Overworked jaw muscles, particularly the masseter muscle, can become enlarged, leading to a wider, more square-shaped jawline. This is a common indicator of significant clenching.
Headaches and Facial Pain
- Teeth Grinding Headaches: One of the most common and debilitating symptoms. Bruxism often causes tension-type headaches, particularly in the temples, forehead, and behind the eyes. These headaches are frequently present upon waking and can persist throughout the day. The constant strain on the temporalis muscles (on the sides of your head) from clenching is a primary cause.
- Migraine-like Symptoms: For some, bruxism can trigger or exacerbate migraines, leading to severe, throbbing headaches, light sensitivity, and nausea.
- Earache: Pain originating from the jaw joint and surrounding muscles can be referred to the ear, often mistaken for an ear infection.
- Neck and Shoulder Pain: The tension can extend down the neck and into the shoulders, contributing to generalized muscle soreness.
Other Symptoms
- Fatigue: The constant muscle activity during sleep can disrupt restful sleep, leaving individuals feeling tired even after a full night's rest.
- Sleep Disruption: Grinding noises can disturb a sleeping partner.
- Cheek Biting: Some individuals may unconsciously bite the inside of their cheek due to muscle tension or jaw misalignment.
Ignoring bruxism can lead to a cascade of worsening problems. Early intervention is key to preventing severe damage and improving quality of life.
Traditional Treatment Options for Bruxism
Before considering more advanced interventions like Botox, dentists typically recommend a range of conservative and traditional treatments for bruxism. These options focus on protecting teeth, reducing muscle activity, and addressing underlying causes.
1. Mouthguards and Night Guards
These are the most common and often the first line of defense.
- Custom-Fit Night Guards: Made by your dentist, these are fabricated from durable acrylic after taking impressions of your teeth. They fit precisely, are comfortable to wear, and effectively cushion the teeth, preventing direct contact and distributing pressure evenly. They also help position the jaw in a relaxed state.
- Pros: Highly effective at protecting teeth from wear and fractures, can reduce muscle strain, custom fit is comfortable and durable.
- Cons: Can be expensive (ranging from $300 to $800), requires cleaning and maintenance, some people find them bulky or uncomfortable initially, does not stop clenching, only protects against its effects.
- Boil-and-Bite Guards: Available over-the-counter (OTC) at drugstores, these guards are softened in hot water and then bitten into to mold to your teeth.
- Pros: Inexpensive (typically $20-$50), readily available.
- Cons: Less precise fit, can be bulky and uncomfortable, less durable, may not offer as much protection as custom guards, can sometimes shift the bite if not fitted correctly.
- Soft vs. Hard Guards: Dentists usually recommend harder guards for severe grinders as they are more durable and provide better stability for the jaw. Soft guards might be prescribed for mild clenching or as a temporary measure.
2. Stress Management Techniques
Since stress and anxiety are major contributors to bruxism, managing them can significantly reduce symptoms.
- Cognitive Behavioral Therapy (CBT): Helps identify and change thought patterns that contribute to stress and anxiety.
- Relaxation Techniques: Yoga, meditation, deep breathing exercises, progressive muscle relaxation.
- Biofeedback: Uses electronic monitoring to teach individuals how to control muscle activity. For bruxism, it can help people become aware of their jaw clenching and learn to relax those muscles.
- Counseling or Therapy: Addressing underlying psychological issues.
3. Physical Therapy and Myofascial Release
- Jaw Exercises: Specific exercises can help stretch and relax jaw muscles, improve range of motion, and reduce pain.
- Heat/Cold Therapy: Applying warm compresses to the jaw can soothe sore muscles, while cold packs can reduce inflammation.
- Massage: Gentle massage of the jaw, neck, and temple muscles can help release tension.
4. Medications
- Muscle Relaxants: Prescribed for short-term use, typically before bedtime, to relax jaw muscles and reduce clenching. Not a long-term solution due to potential side effects.
- Botox Injections: (Detailed below, but mentioned here as an increasingly common medical intervention).
- Anti-inflammatory Drugs: Over-the-counter pain relievers like ibuprofen can help manage pain and inflammation associated with jaw soreness and headaches.
- Antidepressants/Anti-anxiety Medications: If psychological factors are severe, a physician may prescribe these to manage the root cause, which can indirectly reduce bruxism.
5. Dental Corrections
- Correcting Misaligned Teeth: In rare cases where a significant bite issue (malocclusion) is contributing to bruxism, orthodontic treatment (braces, clear aligners) or restorative procedures (crowns, fillings) might be considered to balance the bite. This is usually pursued only after other causes have been ruled out.
Pro Tip: Always consult with your dentist or a healthcare professional to determine the best treatment path. Self-diagnosis and treatment can sometimes exacerbate the problem or delay effective relief.
Comparison Table 1: Traditional Treatments vs. Botox for Bruxism
| Feature | Custom Night Guard | Stress Management (CBT/Relaxation) | Botox Injections (Masseter/Temporalis) |
|---|---|---|---|
| Primary Goal | Protect teeth from wear; distribute pressure | Address underlying causes (stress, anxiety) | Relax muscles; reduce clenching force & pain |
| Mechanism | Physical barrier; slight jaw repositioning | Cognitive & behavioral modification | Blocks nerve signals to specific muscles |
| Effectiveness | Very high for tooth protection; moderate for pain | Variable; requires consistent effort | High for reducing clenching, pain, and headaches |
| Duration of Effect | Ongoing protection as long as worn | Long-term if habits are maintained | 3-6 months per treatment |
| Cost Range (US) | $300 - $800 (one-time) | $50 - $200+ per session (ongoing) | $400 - $1,500 per session (every 3-6 months) |
| Pros | Non-invasive, protects teeth, often effective | Addresses root cause, improves overall well-being | Highly effective for pain, prevents muscle hypertrophy, minimally invasive |
| Cons | Does not stop clenching, discomfort, maintenance | Requires commitment, not immediate relief | Temporary, requires repeat injections, cost, potential side effects, not typically covered by dental insurance |
| Side Effects | Mild discomfort, drooling | None | Temporary bruising, swelling, rare muscle weakness, smile changes |
Understanding Botox (Botulinum Toxin Type A)
Botox is a brand name for botulinum toxin type A, a neurotoxin produced by the bacterium Clostridium botulinum. While often associated with cosmetic wrinkle reduction, Botox has a wide range of therapeutic medical applications due to its unique mechanism of action.
How It Works: The Neuromodulator Effect
Botulinum toxin works by temporarily blocking the release of acetylcholine, a neurotransmitter that signals muscles to contract. When injected into a muscle, Botox causes localized muscle relaxation or paralysis. This effect is temporary because the nerve endings eventually regenerate, and new neurotransmitter receptors are formed.
Medical Uses Beyond Aesthetics
Beyond its well-known use in cosmetic dermatology, Botox has been approved by the U.S. Food and Drug Administration (FDA) for treating various medical conditions, including:
- Chronic migraines: By blocking pain signals.
- Severe underarm sweating (hyperhidrosis): By blocking nerve signals to sweat glands.
- Overactive bladder: By relaxing the bladder muscle.
- Cervical dystonia: A neurological disorder causing severe neck and shoulder muscle spasms.
- Spasticity: In conditions like cerebral palsy or post-stroke.
- Blepharospasm: Involuntary twitching of the eyelids.
Its therapeutic versatility stems from its ability to precisely target and relax specific muscles, making it an ideal candidate for managing conditions characterized by excessive muscle activity, such as bruxism.
Botox for Teeth Clenching: The Mechanism
When used for bruxism, Botox is specifically injected into the muscles responsible for jaw clenching and grinding. The primary targets are the masseter muscles (located on the sides of the jaw, near the cheeks) and sometimes the temporalis muscles (on the temples).
Targeting the Masseter and Temporalis Muscles
- Masseter Muscles: These are some of the strongest muscles in the body, responsible for closing the jaw and chewing. When overactive due to bruxism, they can become enlarged (hypertrophy), leading to a wider jawline and significant pain. Injecting Botox into the masseter muscles directly reduces their ability to contract with excessive force.
- Temporalis Muscles: These fan-shaped muscles on the sides of the head also play a crucial role in clenching and contribute significantly to teeth grinding headaches. Botox injections here can alleviate the tension that leads to these headaches.

How It Reduces Muscle Activity Without Affecting Chewing
A common concern among patients is whether Botox will interfere with essential functions like chewing or speaking. The answer is generally no, when administered correctly by an experienced practitioner.
- Precise Dosing and Placement: The goal isn't to completely paralyze the jaw muscles, but to reduce their strength and activity to a therapeutic level. Dentists and oral surgeons who administer Botox for bruxism are highly skilled in understanding facial anatomy and determining the appropriate dosage and injection points.
- Multiple Muscles for Chewing: While the masseter and temporalis muscles are powerful, other muscles (like the pterygoid muscles) also contribute to chewing. Botox selectively weakens the overactive clenching muscles without impairing the overall ability to chew, speak, or make normal facial expressions. Patients typically report a noticeable reduction in clenching intensity and frequency, without feeling like their jaw is "weak."
By relaxing these overactive muscles, Botox effectively breaks the cycle of constant muscle tension, leading to:
- Reduced Jaw Pain: The primary benefit for many.
- Alleviation of Headaches: Especially teeth grinding headaches originating from temple and jaw tension.
- Prevention of Tooth Damage: Less clenching means less wear and tear on teeth and existing dental work.
- Reduced Muscle Hypertrophy: Over time, the masseter muscles may reduce in size, leading to a softer, more oval facial contour (often a welcome aesthetic side effect for those with an enlarged jawline due to chronic clenching). This is often referred to as botox jaw clenching reduction.
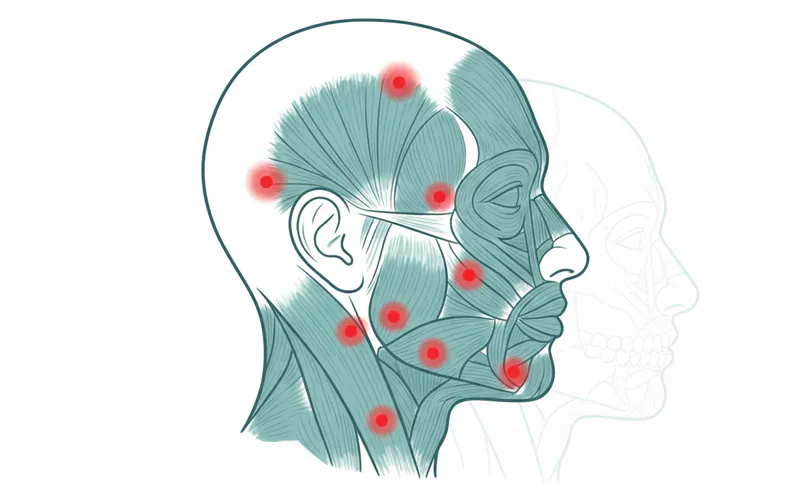
Who is a Candidate for Botox for Bruxism?
Botox for bruxism is not a universal solution, but it can be highly effective for specific groups of patients. A thorough consultation with a qualified dental or medical professional is essential to determine candidacy.
You might be a good candidate if you experience:
- Chronic, Severe Bruxism: Particularly if traditional treatments like night guards have not provided sufficient relief from pain or muscle tension.
- Persistent Jaw Pain and TMJ Symptoms: Including chronic facial pain, tenderness in the jaw muscles, clicking or popping, or limited jaw movement directly linked to clenching.
- Frequent Teeth Grinding Headaches: If you suffer from regular tension-type headaches, especially upon waking, that are attributed to clenching or grinding.
- Significant Tooth Wear or Damage: If your dentist observes accelerated wear and tear on your teeth that your night guard isn't fully preventing, or if you're prone to fractures from clenching.
- Enlarged Masseter Muscles (Masseter Hypertrophy): This often results in a wide or "square" jawline due to overactive clenching muscles.
- Unwillingness or Inability to Wear a Night Guard: While night guards are effective, some individuals find them intolerable.
- No Contraindications: You must not have any medical conditions that would make Botox unsafe.
Contraindications for Botox Treatment:
Botox is generally not recommended for:
- Pregnant or Breastfeeding Individuals: Due to insufficient research on its safety in these populations.
- Individuals with Neuromuscular Disorders: Such as Myasthenia Gravis or Lambert-Eaton Syndrome, as Botox can exacerbate muscle weakness.
- Those with Infections at the Proposed Injection Sites: Treatment should be postponed until the infection clears.
- Individuals with known allergies to any component of the Botox formulation.
- Patients on certain medications: Especially those that interfere with neuromuscular transmission (e.g., aminoglycoside antibiotics). It's crucial to disclose all medications to your provider.
It's vital that your provider conducts a comprehensive medical history review and physical examination to ensure Botox is a safe and appropriate treatment option for your specific situation.
The Botox for Bruxism Treatment Process: What to Expect
Receiving Botox for bruxism is a relatively quick and straightforward procedure, typically performed in a dental or medical office. Here's a step-by-step guide to what you can expect:
1. Initial Consultation and Assessment
Your journey begins with a thorough consultation. Your dentist or specialist will:
- Review Your Medical History: Including any medications you're taking, allergies, and pre-existing conditions.
- Discuss Your Symptoms: E.g., jaw pain, headaches, tooth sensitivity, clenching habits.
- Perform a Physical Examination: This involves palpating your jaw muscles (masseter and temporalis) to assess their size, strength, and tenderness. They may also check for signs of tooth wear and TMJ dysfunction.
- Determine Candidacy: Based on this assessment, your provider will confirm if Botox is a suitable treatment for you and explain the expected outcomes, potential risks, and costs.
- Discuss Goals: You'll discuss what you hope to achieve with the treatment (e.g., pain reduction, headache relief, preventing tooth damage).
2. Preparation
On the day of the treatment:
- Avoid Blood Thinners: You might be advised to avoid blood-thinning medications, supplements (like aspirin, ibuprofen, fish oil, Vitamin E), and alcohol for a few days beforehand to minimize bruising. Always follow your provider's specific instructions.
- Clean Skin: The injection sites will be cleaned with an antiseptic wipe.
- Numbing (Optional): While the injections are generally well-tolerated, a topical numbing cream or ice pack may be applied to the area to enhance comfort, though many patients find it unnecessary.
3. The Injection Procedure
The actual injection process is swift, usually lasting only 10-15 minutes.
- Marking Injection Sites: Your provider will ask you to clench your jaw to identify the bulkiest parts of your masseter muscles and the areas of greatest tension in your temporalis muscles. They may use a marker to pinpoint the exact injection points.
- Multiple Injections: Using a very fine needle, the Botox is injected into several points within each masseter muscle (typically 2-4 points per side) and often into the temporalis muscles (again, multiple points per side). The number of injections and units of Botox will depend on the severity of your condition and muscle mass.
- Number of Units: For bruxism, the typical dosage ranges from 20 to 50 units per side for the masseter muscles, and potentially an additional 10-20 units per side for the temporalis muscles, for a total of 40-140 units per session. Your provider will customize this based on your individual needs. The total number of units directly impacts the overall cost.
- Minimal Discomfort: Patients often describe the injections as feeling like small pinpricks or a slight stinging sensation. Most find it very tolerable.
4. Post-Procedure Guidance
Immediately after the injections, you can usually resume most normal activities.
- No Rubbing/Massaging: Avoid rubbing or massaging the treated areas for at least 24 hours to prevent the Botox from spreading to unintended muscles.
- Avoid Strenuous Exercise: Refrain from heavy exercise for 24 hours.
- Stay Upright: Avoid lying down for 2-4 hours post-treatment.
- Expect Mild Side Effects: Minor redness, swelling, or bruising at the injection sites is common and usually resolves within a few hours to a few days.
- Timeline for Results: You won't feel the effects immediately. Botox typically starts to take effect within 3-7 days, with full results visible around 10-14 days after treatment.
- Duration of Effects: The muscle-relaxing effects typically last between 3 to 6 months. As the effects wear off, muscle activity will gradually return, and you'll likely need repeat injections to maintain the benefits.
Recovery and Aftercare
The recovery period after Botox injections for bruxism is minimal, allowing most individuals to return to their daily routines almost immediately. However, proper aftercare is crucial to optimize results and minimize potential side effects.
Immediate Post-Treatment Care (First 24-48 hours)
- Avoid Touching/Rubbing: This is perhaps the most important instruction. Do NOT rub, massage, or apply pressure to the treated areas for at least 24 hours. This prevents the Botox from migrating to unintended muscles, which could lead to unwanted side effects like temporary facial asymmetry.
- Remain Upright: Try to stay in an upright position (avoid lying flat) for at least 2-4 hours after the injections. This further helps prevent product migration.
- No Strenuous Exercise: Avoid intense physical activity, heavy lifting, or anything that significantly raises your heart rate for 24 hours. Increased blood flow can potentially spread the Botox.
- Avoid Alcohol and Blood Thinners: Continue to avoid alcohol and any blood-thinning medications or supplements (if advised by your provider) for 24-48 hours to minimize bruising.
- Manage Swelling/Bruising: Mild swelling, redness, or bruising at the injection sites is normal. You can apply a cold compress gently to the area for 10-15 minutes at a time to reduce these symptoms. Avoid firm pressure.
- Discomfort: Any minor discomfort can usually be managed with over-the-counter pain relievers like acetaminophen (Tylenol). Avoid NSAIDs like ibuprofen if you are prone to bruising.
What to Expect in the Days and Weeks Following Treatment
- Onset of Action: You will not feel immediate relief. Botox begins to work gradually. You should start to notice a reduction in muscle tension and clenching intensity within 3 to 7 days.
- Full Effect: The maximum effect of the treatment is typically observed around 10 to 14 days after the injections. At this point, you should experience significant relief from jaw pain, headaches, and a noticeable reduction in the force of your clenching.
- Facial Changes (Optional): If you had significant masseter hypertrophy, you might notice a subtle softening or slimming of your jawline over several weeks as the muscle gradually atrophies due to reduced activity. This is a common and often desired "side effect" for many patients.
- Chewing Ability: Your ability to chew will remain largely unaffected. While the strong clenching muscles are relaxed, other jaw muscles still function normally for eating. You may notice a slight reduction in chewing power for very tough foods, but this is usually minor and temporary.
- Duration: The effects of Botox for bruxism typically last between 3 to 6 months. The duration can vary between individuals and depends on factors like the dosage used and how quickly your body metabolizes the toxin.
- Repeat Treatments: To maintain the benefits, repeat injections are necessary as the effects of Botox gradually wear off. Your provider will recommend a schedule for follow-up treatments, usually every 4-6 months. Consistent treatment can sometimes lead to longer-lasting results over time as the muscles remain relaxed.
Pro Tip: Keep a journal of your symptoms (pain levels, headache frequency) before and after treatment to accurately track the effectiveness of Botox and discuss it with your provider during follow-up appointments.
Risks, Side Effects, and Potential Complications
While Botox for bruxism is generally considered safe and effective when administered by a qualified professional, it's crucial to be aware of the potential risks, side effects, and rare complications.
Common, Mild, and Temporary Side Effects
These typically resolve within a few days to a couple of weeks:
- Bruising, Swelling, Redness at Injection Sites: This is the most common side effect, similar to any injection. It usually subsides quickly.
- Mild Pain or Tenderness: At the injection sites, which can be managed with over-the-counter pain relievers.
- Headache: A mild, temporary headache can occur after treatment, usually resolving within 24-48 hours.
- Dry Mouth: Some individuals might experience temporary dry mouth.
- Fatigue or Malaise: Very rarely, a generalized feeling of being unwell.
Less Common, Potentially More Noticeable Side Effects
These are usually temporary and resolve as the Botox wears off:
- Asymmetry of Smile or Facial Expression: If Botox spreads to nearby muscles that control smiling, it can temporarily affect the corners of the mouth, leading to a lopsided smile. This is rare and typically resolves as the Botox wears off.
- Weakness in Chewing: While generally not affecting eating, some individuals might experience a temporary, mild reduction in their ability to chew very tough or fibrous foods. This typically improves over a few weeks.
- Speech Changes: Rarely, if the muscles involved in articulation are affected, minor temporary speech changes can occur.
- Difficulty Swallowing: Extremely rare, but possible if the Botox spreads to the muscles involved in swallowing.
- Excessive Salivation: Very uncommon, but reported in some cases.
- Jaw Contouring Changes: While often a desired side effect, for some, the reduction in masseter muscle size might be more pronounced than anticipated, leading to a visible change in facial shape.
Rare and Serious Complications
Serious complications are exceedingly rare, especially when the procedure is performed by an experienced and qualified practitioner. They can include:
- Allergic Reaction: Though rare, a severe allergic reaction (anaphylaxis) is possible. Symptoms can include rash, itching, hives, swelling of the face, lips, or tongue, and difficulty breathing.
- Spread of Toxin (Systemic Effects): In very rare instances, the botulinum toxin can spread beyond the injection site, potentially causing generalized muscle weakness, vision problems, difficulty speaking or swallowing, or breathing problems. This is more commonly associated with high doses or off-label uses and is exceptionally rare in the doses used for bruxism.
- Infection: As with any injection, there is a very small risk of infection at the injection site.
- Nerve Damage: Extremely rare, but possible if the needle inadvertently strikes a nerve.
Pro Tip: Always choose a board-certified and experienced provider (dentist, oral surgeon, dermatologist, or plastic surgeon) who is well-versed in facial anatomy and therapeutic Botox injections. Do not hesitate to ask about their experience and qualifications. Following all pre- and post-treatment instructions rigorously can also significantly reduce your risk of complications.
Cost of Botox for Teeth Clenching and Insurance
Understanding the financial aspect of Botox for bruxism is crucial, as costs can vary significantly, and insurance coverage is often complex.
Factors Influencing Cost
The total cost of Botox for teeth clenching depends on several factors:
- Number of Units: Botox is priced per unit. For bruxism, a typical treatment might involve 40-140 units, depending on the severity of clenching and the size/strength of your masseter and temporalis muscles.
- Geographic Location: Prices per unit can vary significantly by region and city within the US. Major metropolitan areas tend to have higher costs.
- Provider's Experience and Specialty: Highly experienced and specialized practitioners (e.g., oral surgeons, neurologists, specific dentists) may charge more per unit than less experienced providers.
- Clinic Overhead: The type of facility (medspa vs. specialized dental/medical office) can influence pricing.
- Bundled Packages: Some clinics offer discounts for purchasing multiple units or for committing to a series of treatments.
Average US Price Ranges
- Per Unit Cost: Generally ranges from $10 to $20 per unit in the US.
- Total Cost Per Session: For bruxism, a single treatment session typically ranges from $400 to $1,500.
- Low End (e.g., 40-60 units): $400 - $900
- Mid-Range (e.g., 60-100 units): $600 - $1,500
- High End (e.g., 100-140+ units for severe cases or multiple muscle groups): $1,000 - $2,500+
Remember that these treatments are temporary, requiring repeat injections every 3-6 months to maintain results, so consider the annual cost.
Insurance Coverage Details
This is often the most confusing aspect for patients.
- Dental Insurance: Typically, dental insurance does NOT cover Botox injections for bruxism. Dental plans primarily cover diagnostic, preventive, and restorative dental procedures.
- Medical Insurance: Coverage under medical insurance is possible but highly variable and often challenging to obtain.
- Medical Necessity: For medical insurance to consider coverage, the Botox treatment must be deemed medically necessary to address a documented medical condition (like chronic pain from TMD, severe headaches, or severe bruxism leading to significant dental damage) rather than for cosmetic reasons.
- Prior Authorization: Your provider will usually need to submit a prior authorization request to your insurance company. This involves detailed documentation, including your diagnosis, symptoms, previous failed treatments (e.g., night guards, physical therapy), and a clear explanation of why Botox is the appropriate next step.
- Specific Codes: The provider will use specific CPT codes (Current Procedural Terminology) for Botox injections and for the medical condition being treated.
- In-Network vs. Out-of-Network: Your coverage will also depend on whether your provider is in-network with your specific insurance plan.
- Deductibles, Co-pays, and Co-insurance: Even if covered, you will still be responsible for your plan's deductibles, co-pays, and co-insurance.
Pro Tip: Before undergoing treatment, always verify coverage with your medical insurance provider. Ask your dental professional's office to assist you in this process, as they often have experience navigating these claims.
Payment Plans and Financing Options
Given that insurance coverage is not guaranteed, many clinics offer:
- Payment Plans: In-house payment plans where you can spread the cost over several months.
- Healthcare Financing: Third-party financing options like CareCredit or Alphaeon Credit, which offer low-interest or interest-free plans for a certain period.
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): These accounts allow you to use pre-tax dollars for qualified medical expenses, which often include Botox for medically necessary conditions.
Comparison Table 2: Botox Cost Breakdown by US Region & Typical Units
| Region | Average Cost per Unit | Typical Units (Masseter/Temporalis) | Estimated Total Cost per Session (Range) | Insurance Coverage Likelihood |
|---|---|---|---|---|
| Northeast | $15 - $20 | 50 - 100 | $750 - $2,000 | Low to Moderate (Medical Necessity) |
| Southeast | $12 - $18 | 40 - 80 | $480 - $1,440 | Low to Moderate (Medical Necessity) |
| Midwest | $10 - $15 | 40 - 70 | $400 - $1,050 | Low (Medical Necessity) |
| Southwest | $12 - $17 | 40 - 80 | $480 - $1,360 | Low to Moderate (Medical Necessity) |
| West Coast | $16 - $20+ | 60 - 120+ | $960 - $2,400+ | Moderate (Medical Necessity) |
Note: These are estimated ranges and can vary widely based on the specific city, clinic, and individual patient needs.
Prevention of Teeth Clenching (Beyond Botox)
While Botox provides effective relief for existing bruxism, implementing preventive strategies can significantly reduce the likelihood of clenching and potentially extend the benefits of treatment. A multi-faceted approach is often the most successful.

1. Stress Reduction and Management
Since stress is a major trigger for bruxism, adopting effective stress-reducing habits is paramount:
- Mindfulness and Meditation: Regular practice can help calm the nervous system and reduce overall tension.
- Deep Breathing Exercises: Incorporate these throughout the day to de-stress.
- Yoga or Tai Chi: These practices combine physical movement with mindfulness, promoting relaxation.
- Regular Exercise: Physical activity is a powerful stress reliever.
- Adequate Sleep: Prioritize 7-9 hours of quality sleep per night. Poor sleep hygiene can exacerbate bruxism.
- Professional Counseling: If stress and anxiety are overwhelming, seeking help from a therapist or counselor can provide valuable coping strategies.
2. Jaw Relaxation Techniques
- Awareness: Become aware of when you clench your jaw during the day. Set reminders (e.g., on your phone) to check your jaw position.
- "Lips Together, Teeth Apart": Practice keeping your lips together but your teeth slightly apart, with your jaw muscles relaxed. The tongue should rest gently on the roof of your mouth.
- Warm Compress: Apply a warm, moist towel to your jaw muscles before bed to help them relax.
- Self-Massage: Gently massage your jaw, temples, and neck muscles to release tension.
3. Dietary and Lifestyle Adjustments
- Reduce Caffeine and Alcohol: Both can disrupt sleep and exacerbate bruxism. Try to avoid them, especially in the evening.
- Avoid Chewing Gum and Hard Foods: Excessive chewing can overwork jaw muscles, making them more prone to clenching.
- Stay Hydrated: Dehydration can contribute to muscle cramps and tension.
- Quit Smoking: Nicotine is a stimulant that can worsen bruxism.
4. Optimize Sleep Environment and Habits
- Consistent Sleep Schedule: Go to bed and wake up at the same time each day, even on weekends.
- Dark, Quiet, Cool Bedroom: Create an optimal sleep environment.
- Avoid Screens Before Bed: The blue light from phones, tablets, and computers can interfere with melatonin production and sleep quality.
- Address Sleep Disorders: If you suspect you have a sleep disorder like sleep apnea, consult a medical professional. Treating sleep apnea can significantly reduce sleep bruxism.
5. Regular Dental Check-ups
- Monitor for Signs: Regular visits to your dentist allow them to monitor your teeth for signs of wear and tear, gum recession, and muscle hypertrophy. Early detection means earlier intervention.
- Discuss Symptoms: Don't hesitate to discuss any jaw pain, headaches, or clenching habits with your dentist. They can offer personalized advice and guidance.
By combining the therapeutic effects of Botox with proactive preventive measures, you can achieve more comprehensive and longer-lasting relief from teeth clenching and its associated problems.
Children / Pediatric Considerations
Bruxism is remarkably common in children, affecting a significant percentage of those under the age of 12. However, the approach to treating bruxism in children is distinctly different from adults, and Botox is generally NOT a first-line or common treatment option for pediatric bruxism.
Common Characteristics of Pediatric Bruxism
- Prevalence: Studies suggest that between 10-30% of children experience bruxism, with peaks during eruption of primary teeth and mixed dentition.
- Causes: In children, bruxism is often linked to:
- Stress and Anxiety: School pressure, family changes, or everyday worries.
- Dental Issues: Misaligned teeth, erupting teeth, or a reaction to pain from an earache or teething.
- Allergies or Upper Respiratory Issues: Nasal congestion can sometimes lead to jaw clenching.
- Sleep Disorders: Though less common than in adults, some children with sleep apnea may grind their teeth.
- Often Resolves Naturally: Most cases of childhood bruxism are temporary and resolve on their own as children grow, their permanent teeth erupt, and they develop better coping mechanisms for stress.
Traditional Treatment for Children
For children, the focus is almost exclusively on conservative, non-invasive methods:
- Monitoring: The most common approach. Dentists will monitor for signs of tooth wear and pain.
- Stress Reduction: Encouraging relaxation techniques, ensuring adequate sleep, and addressing any underlying emotional stressors.
- Mouthguards: Custom-fitted night guards may be prescribed for older children or adolescents with severe, persistent bruxism causing pain or significant tooth damage. However, they are less common for very young children due to growth and tooth changes.
- Addressing Underlying Issues: Treating allergies, ear infections, or sleep disorders if identified.
Botox for Children: Limited Role
Botox is rarely, if ever, considered for pediatric bruxism, for several reasons:
- Off-label Use: The safety and efficacy of Botox for bruxism have not been extensively studied or approved for use in children.
- Growth and Development: Children's jaws and muscles are still developing, and introducing a muscle-relaxing agent could theoretically interfere with normal growth patterns, though this is speculative.
- Temporary Nature: Botox is a temporary solution, and given that childhood bruxism often resolves on its own, a temporary, invasive treatment is generally not warranted.
- Risks vs. Benefits: The potential risks, while low in adults, are typically not justified when less invasive and equally effective treatments are available for children.
When to See a Dentist for a Child: If your child complains of jaw pain, persistent headaches, or if you notice significant teeth grinding sounds, it's always best to consult a pediatric dentist. They can assess the situation, rule out serious underlying conditions, and recommend appropriate, age-specific interventions. For the vast majority of children, Botox will not be part of their treatment plan.
Frequently Asked Questions
Q1: Is Botox for teeth clenching painful?
A: The injections typically involve minimal discomfort. Most patients describe it as a quick, mild stinging or pinprick sensation, similar to a mosquito bite. A topical numbing cream or ice can be applied beforehand to enhance comfort, though many find it unnecessary.
Q2: How long does Botox last for bruxism?
A: The effects of Botox for bruxism typically last between 3 to 6 months. The exact duration can vary based on individual metabolism, the dosage administered, and the severity of your clenching habits. Repeat treatments are necessary to maintain relief.
Q3: How many units of Botox are needed for jaw clenching?
A: The number of units varies significantly depending on the individual's muscle mass and the severity of their bruxism. A common range is 20 to 50 units per masseter muscle (40-100 total for both sides) and potentially an additional 10-20 units per temporalis muscle if those are also treated, leading to a total of 40-140 units per session.
Q4: Can I chew normally after Botox for bruxism?
A: Yes, you can typically chew normally after Botox injections for bruxism. The goal is to reduce the excessive clenching force, not to paralyze your chewing muscles entirely. You might notice a subtle reduction in strength for very tough foods, but your overall ability to eat and speak will remain unaffected.
Q5: Is Botox for bruxism covered by insurance?
A: Dental insurance generally does not cover Botox. Medical insurance may offer coverage if the treatment is deemed medically necessary for a documented condition like chronic TMJ pain or severe bruxism leading to health issues, rather than purely cosmetic reasons. Prior authorization and detailed documentation are usually required.
Q6: What are the alternatives to Botox for teeth clenching?
A: Alternatives include custom-fitted night guards, stress management techniques (like CBT, meditation), physical therapy, biofeedback, and in some cases, short-term muscle relaxants. Dental corrections for bite issues are rarely primary treatments but may be considered in specific cases.
Q7: Can Botox change my facial appearance?
A: For individuals with significantly enlarged masseter muscles due to chronic clenching (masseter hypertrophy), Botox can lead to a subtle slimming or softening of the lower jawline over several weeks. This is often a desired aesthetic side effect but is not the primary goal of the treatment for bruxism.
Q8: How quickly does Botox work for jaw clenching?
A: Botox does not work instantly. You should begin to feel the effects of reduced muscle tension and clenching within 3 to 7 days after the injections. The full therapeutic effect is typically observed around 10 to 14 days post-treatment.
Q9: Are there long-term side effects of Botox for bruxism?
A: Long-term side effects from correctly administered Botox for bruxism are generally rare. The effects are temporary, and the body fully metabolizes the toxin. Some studies suggest long-term use may lead to mild, reversible bone density changes in the jaw, but more research is needed, and this is typically not a concern with standard therapeutic doses.
Q10: Who performs Botox injections for bruxism?
A: Botox injections for bruxism should be performed by a qualified and experienced healthcare professional. This typically includes dentists (especially those with advanced training in TMD and facial aesthetics), oral and maxillofacial surgeons, neurologists, or dermatologists who have specific expertise in therapeutic Botox.
When to See a Dentist
Recognizing the signs and symptoms of bruxism and knowing when to seek professional help is critical for preventing long-term damage and managing pain. Do not wait for severe complications to arise.
You should schedule an appointment with your dentist or an oral health specialist if you experience any of the following:
- Persistent Jaw Pain: If you frequently wake up with or experience chronic pain or tenderness in your jaw, face, or around your ears.
- Frequent Headaches: Especially teeth grinding headaches that are dull, tension-type, and tend to be worse in the morning or worsen throughout the day.
- Noticeable Tooth Damage: If you observe flattened, chipped, fractured, or excessively worn-down teeth, or if your dental restorations (fillings, crowns) are repeatedly breaking.
- Increased Tooth Sensitivity: Unexplained sensitivity to hot, cold, or sweet foods.
- Loud Grinding Noises: If a sleeping partner has told you that you make grinding or clenching noises at night.
- Limited Jaw Movement: Difficulty opening your mouth wide, your jaw feeling stiff, or a sensation of your jaw locking.
- Clicking or Popping Jaw: Sounds coming from your temporomandibular joint when you open or close your mouth.
- Enlarged Jaw Muscles: If you notice your jawline appears wider or more "square" than before.
- Unsuccessful Conservative Treatments: If you've tried traditional approaches like over-the-counter night guards or stress management techniques without significant relief.
Red Flags (Seek prompt attention):
- Severe, debilitating pain that interferes with daily activities.
- Jaw locking in an open or closed position that you cannot resolve yourself.
- Signs of infection (redness, pus, fever) near your jaw or in your mouth.
Addressing bruxism early can prevent extensive dental work, chronic pain, and a significant reduction in your quality of life. Your dentist can accurately diagnose your condition, identify contributing factors, and discuss the full range of treatment options available, including whether Botox for teeth clenching is a suitable solution for you.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles

What Causes Teeth Grinding in Sleep
More than one in ten adults—and even more children—clench or grind their teeth during sleep, a condition known medically as sleep bruxism. For many, it's an unconscious habit that goes unnoticed until significant damage or discomfort arises. Waking up with a dull, constant headache, jaw pain, or
February 23, 2026
How to Not Grind Teeth at Night
More than one in ten adults and a significant percentage of children experience teeth grinding, medically known as bruxism, a condition that often goes unnoticed, especially when it occurs during sleep. If you've woken up with a sore jaw, a dull headache, or noticed your teeth becoming unusually
February 23, 2026

What Is Jaw Clenching
Do you often wake up with a dull headache, a sore jaw, or unexplained tooth sensitivity? You're not alone. Approximately 1 in 10 adults and up to 3 in 10 children experience some form of bruxism, a condition characterized by grinding, gnashing, or clenching your teeth. At the heart of this wides
February 23, 2026
Severe Bruxism Molars: Complete Guide
When the quiet of the night is shattered by a grinding, grating sound, or when you wake up with an aching jaw and teeth that feel oddly sensitive, it’s often a sign of bruxism. But what happens when this condition intensifies, leading to significant damage, especially to your back teeth? This is the
February 23, 2026