Severe Bruxism Molars: Complete Guide
Key Takeaways
- When the quiet of the night is shattered by a grinding, grating sound, or when you wake up with an aching jaw and teeth that feel oddly sensitive, it’s often a sign of bruxism. But what happens when this condition intensifies, leading to significant damage, especially to your back teeth? This is the
When the quiet of the night is shattered by a grinding, grating sound, or when you wake up with an aching jaw and teeth that feel oddly sensitive, it’s often a sign of bruxism. But what happens when this condition intensifies, leading to significant damage, especially to your back teeth? This is the reality of severe bruxism molars, a pervasive and often debilitating condition affecting millions of Americans. Studies suggest that bruxism, or teeth grinding and clenching, affects an estimated 10% to 15% of adults and a higher percentage of children. When it progresses to a severe stage, the molars – your strongest teeth, designed for chewing – bear the brunt of immense, repetitive forces, leading to accelerated wear, fractures, and chronic pain.
Understanding severe bruxism, particularly its impact on your molars, is crucial not just for preserving your dental health but for your overall well-being. This guide from SmilePedia.net will delve into every aspect of severe bruxism affecting your molars, from its underlying causes of teeth grinding to the diverse range of effective treatments available. We will explore the tell-tale signs, including the distinct teeth grinding sound that can often be heard, and provide actionable insights into prevention, recovery, and financial considerations. By the end of this comprehensive article, you'll have a clear roadmap to manage and overcome the challenges posed by severe bruxism.
Key Takeaways:
- Severe bruxism molars involve excessive grinding or clenching that significantly damages your back teeth, affecting millions globally.
- Common causes of teeth grinding include stress, sleep disorders like sleep apnea, malocclusion, and certain medications.
- Key symptoms include flattened, sensitive molars, jaw pain (TMJ), headaches, and a distinctive teeth grinding sound.
- Treatment options range from custom nightguards (costing $300-$800) and Botox injections (typically $300-$1,000 per session) to restorative dentistry (crowns: $800-$3,000 per tooth) and orthodontic correction.
- Custom-fitted nightguards are often the first line of defense, providing a protective barrier and helping to retrain jaw muscles.
- Recovery can involve managing discomfort for a few days to weeks post-procedure, with ongoing commitment to behavioral changes.
- Prevention focuses on stress management, improving sleep hygiene, and regular dental check-ups to catch issues early.
What It Is / Overview: Understanding Severe Bruxism Molars
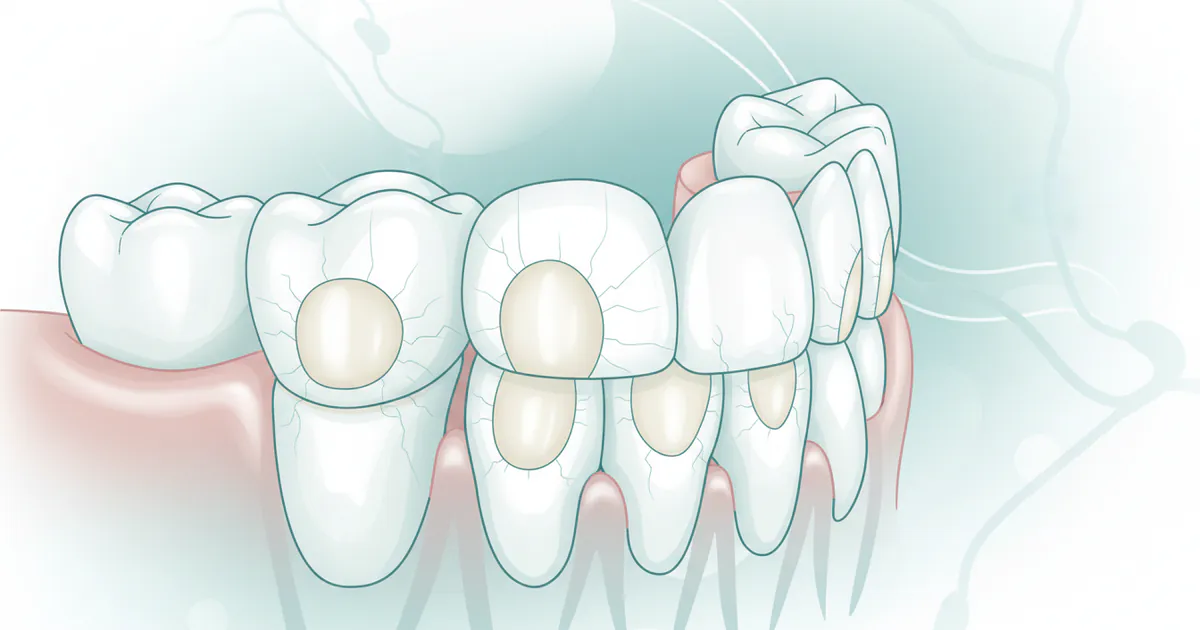
Bruxism is the medical term for grinding, clenching, or gnashing your teeth. While occasional teeth grinding might not cause significant harm, chronic and severe bruxism can lead to a host of dental and overall health problems. When we talk about severe bruxism molars, we are specifically referring to the advanced stage of this condition where the excessive force exerted by the jaw muscles primarily impacts the molars – the large, flat teeth at the back of your mouth responsible for crushing and grinding food.

These forces, often far exceeding normal chewing pressures, can be exerted for prolonged periods, especially during sleep (nocturnal bruxism), leading to accelerated wear and tear. Imagine rubbing two pieces of sandpaper together repeatedly; over time, their surfaces will erode. Similarly, the enamel and dentin of your molars, despite being the hardest substances in your body, are gradually worn down. This leads to flattened chewing surfaces, sharp edges, cracks, and even complete loss of tooth structure. The damage isn't just cosmetic; it can compromise the structural integrity of your teeth, expose sensitive underlying layers, and contribute to chronic pain in the jaw and surrounding areas. The constant pressure can also cause micro-fractures in the tooth enamel, making teeth more susceptible to decay and breakage.
The Mechanics of Grinding and Clenching
Bruxism involves two main actions:
- Grinding: This refers to the side-to-side movement of the lower jaw against the upper jaw, causing the teeth to rub together. This is the primary action responsible for the distinctive teeth grinding sound and severe wear on molar surfaces.
- Clenching: This involves tightly clamping the upper and lower teeth together without significant movement. While it doesn't produce a grinding sound, clenching can exert immense, sustained pressure on the teeth and jaw muscles, leading to fractures, muscle fatigue, and temporomandibular joint (TMJ) disorders.
Both grinding and clenching can severely damage molars. The average human jaw can exert a force of up to 200 pounds per square inch (psi), but during bruxism, these forces can be amplified and sustained for hours without the conscious protective reflexes present during waking hours. This relentless pressure often manifests as significant wear facets, which are flattened, polished areas on the chewing surfaces of your molars, indicating chronic abrasion.
Types / Variations of Bruxism
Bruxism is not a monolithic condition; it presents in different forms, each with its own characteristics and implications for your molars.
Nocturnal (Sleep) Bruxism vs. Diurnal (Awake) Bruxism
- Nocturnal Bruxism (Sleep Bruxism): This is the more common and often more damaging form. It occurs involuntarily while you sleep, making you largely unaware of it. This lack of awareness means protective reflexes are diminished, allowing grinding and clenching forces to be much stronger and more prolonged. It's often reported by partners who hear the characteristic teeth grinding sound. Because it happens for hours each night, nocturnal bruxism is a major contributor to severe bruxism molars, leading to widespread wear, fractures, and jaw pain upon waking.
- Diurnal Bruxism (Awake Bruxism): This occurs when you clench or grind your teeth while awake. It's often a subconscious habit linked to stress, concentration, or certain activities. While you might be more aware of it, and thus able to consciously relax your jaw, persistent diurnal clenching can still cause significant dental wear, muscle fatigue, and headaches. However, the forces are typically less intense and shorter in duration compared to sleep bruxism, making its impact on molars generally less severe unless the habit is extremely frequent and forceful.
Primary vs. Secondary Bruxism
- Primary Bruxism: This type occurs without an identifiable underlying medical condition or external cause. It's believed to be idiopathic, meaning it arises on its own, possibly due to a complex interplay of genetic factors, stress, and central nervous system activity.
- Secondary Bruxism: This form is a symptom or side effect of another condition, medication, or substance. Examples include bruxism linked to sleep disorders (like obstructive sleep apnea), neurological diseases (e.g., Parkinson's), psychiatric medications (especially SSRIs), and substances like caffeine or alcohol. Identifying and addressing the primary condition is crucial for managing secondary bruxism.
Clenching vs. Grinding
As mentioned earlier, while both fall under bruxism, their impact can differ:
- Clenching: Primarily causes vertical pressure. This can lead to abfraction lesions (wedge-shaped defects near the gum line), cracks in teeth, muscle fatigue, and TMJ pain.
- Grinding: Involves horizontal, abrasive forces, leading to widespread flattening of chewing surfaces, significant enamel loss, and the distinctive teeth grinding sound. Both can severely compromise molars.
Causes / Why It Happens: Unraveling the Roots of Teeth Grinding
The causes of teeth grinding are multifaceted, often involving a combination of physical, psychological, and lifestyle factors. Understanding these root causes is essential for effective diagnosis and treatment.
Psychological Factors: Stress and Anxiety
Perhaps the most common trigger, psychological stress and anxiety are highly correlated with bruxism. Daily pressures, emotional tension, anger, frustration, or even focused concentration can lead to subconscious clenching and grinding, both awake and asleep. During sleep, the body may process stress, leading to increased jaw muscle activity. High-stress professions, personal crises, or generalized anxiety disorders often exacerbate bruxism symptoms, accelerating molar wear.
Sleep Disorders
- Obstructive Sleep Apnea (OSA): This is a significant contributing factor, especially for nocturnal bruxism. OSA involves repeated episodes of airway obstruction during sleep. The body's reflex response to try and open the airway often includes jaw movements, which can manifest as grinding or clenching. Treating OSA can often alleviate or significantly reduce bruxism. The National Sleep Foundation estimates that bruxism occurs in 25% of individuals with OSA.
- Other Sleep Disturbances: Insomnia, restless leg syndrome, and other sleep-related movement disorders can also contribute to teeth grinding by disrupting normal sleep architecture.
Malocclusion (Misaligned Bite)
Traditionally, malocclusion (a "bad bite" or misaligned teeth) was thought to be a primary cause of bruxism. While its direct causative role is debated among dental professionals, it can certainly be a contributing factor. If your teeth don't fit together properly, your jaw muscles might work harder to find a comfortable resting position or to compensate for uneven contact points, leading to increased clenching and grinding. This can be particularly true for molars that bear an uneven load. The American Dental Association (ADA) emphasizes the importance of a balanced bite for overall oral health.
Medications and Substances
Several medications and substances can induce or worsen bruxism:
- Antidepressants (SSRIs): Selective serotonin reuptake inhibitors like fluoxetine (Prozac), paroxetine (Paxil), and sertraline (Zoloft) are known to cause bruxism as a side effect in some individuals.
- Stimulants: Medications for ADHD (e.g., Adderall, Ritalin) and illicit stimulants like ecstasy or cocaine can significantly increase jaw muscle activity.
- Caffeine: High intake of caffeine, especially close to bedtime, can act as a stimulant, increasing jaw tension.
- Alcohol: While it may initially seem to relax you, alcohol disrupts normal sleep cycles and can intensify bruxism episodes.
- Tobacco: Nicotine is a stimulant that can contribute to jaw clenching. Studies have shown a significantly higher prevalence of bruxism in smokers compared to non-smokers.
Neurological Conditions
Certain neurological and neurodegenerative disorders can have bruxism as a symptom. These include Parkinson's disease, Huntington's disease, and epilepsy. In these cases, bruxism is often part of a broader spectrum of motor control issues.
Genetic Predisposition
Research suggests there might be a genetic component to bruxism, particularly nocturnal bruxism. If one or both of your parents experienced teeth grinding, you might be more predisposed to developing the condition.
Age
Bruxism can affect people of all ages, including children, but severe forms leading to significant molar damage are more commonly seen in adults, especially those who have experienced bruxism for many years without intervention.
Signs and Symptoms: What to Look For
Recognizing the signs and symptoms of bruxism, especially its severe impact on your molars, is the first step toward seeking effective treatment. Often, you might not be aware of the problem yourself, particularly with sleep bruxism, until a partner points out the teeth grinding sound or your dentist identifies the damage.
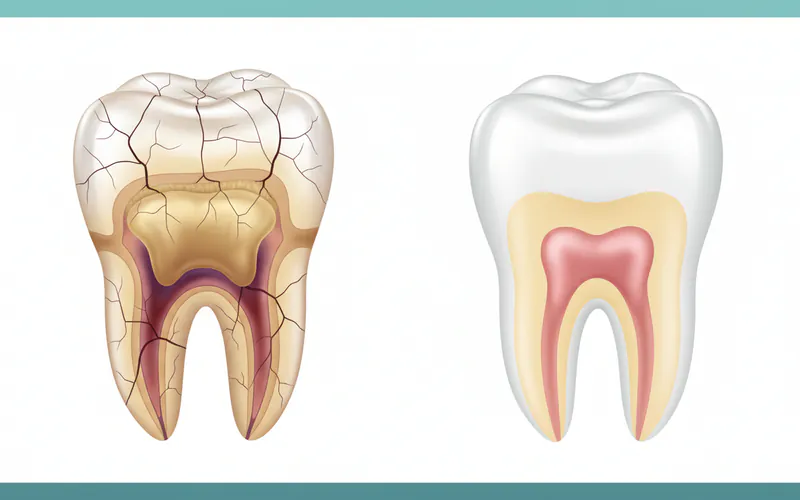
Dental Wear and Damage
- Flattened, Fractured, or Chipped Molars: This is the hallmark of severe bruxism. The chewing surfaces of your back teeth may appear flat, smooth, and shiny instead of having their natural cusps and grooves. Small chips or fractures in the enamel are also common.
- Increased Tooth Sensitivity: As enamel wears away, the underlying dentin, which contains microscopic tubules leading to the tooth's nerve, becomes exposed. This can cause sharp pain or discomfort when consuming hot, cold, sweet, or acidic foods and drinks.
- Abfraction Lesions: These are wedge-shaped or V-shaped notches near the gum line, often indicating excessive clenching forces that cause the tooth to flex at the neck.
- Loose or Mobile Teeth: Chronic, severe grinding can loosen the periodontal ligament fibers that hold teeth in their sockets, making teeth feel wobbly.
- Receding Gums: The constant pressure can contribute to gum recession, exposing more of the tooth root.
- Indentation on the Tongue or Cheeks: You might notice scalloped edges on your tongue or white lines/indentations on the inside of your cheeks (linea alba), caused by pressing soft tissues against your teeth during clenching.
Jaw and Facial Pain
- Sore or Tired Jaw Muscles: Waking up with a stiff or aching jaw, especially around the temples and cheeks, is a strong indicator of nocturnal bruxism. The masseter and temporalis muscles, responsible for chewing, become fatigued from overuse.
- Temporomandibular Joint (TMJ) Disorders: The TMJ connects your jawbone to your skull. Severe bruxism puts immense strain on this joint, leading to pain, clicking or popping sounds when opening or closing your mouth, limited jaw movement, and even locking of the jaw.
- Difficulty Opening Your Mouth Wide: Muscle stiffness can make it challenging to yawn or eat certain foods.
Headaches and Earaches
- Tension Headaches: Many bruxism sufferers experience chronic tension headaches, especially in the temples, forehead, or back of the head. These often originate from the overused jaw muscles.
- Earaches: Pain in the ear region can be referred pain from the TMJ or surrounding muscles, rather than an actual ear infection. This can be confusing and lead to misdiagnosis.
The Teeth Grinding Sound
This is often the most direct and undeniable sign of nocturnal bruxism. A partner, family member, or even roommate might report hearing a loud, grating, or clicking teeth grinding sound while you are asleep. This sound can be quite disruptive and indicates significant forces being applied to your molars.
Treatment Options: Restoring Your Oral Health
Treating severe bruxism molars requires a comprehensive approach, often combining several strategies to protect teeth, alleviate symptoms, and address underlying causes. The specific treatment plan will be tailored to your individual needs by your dentist.
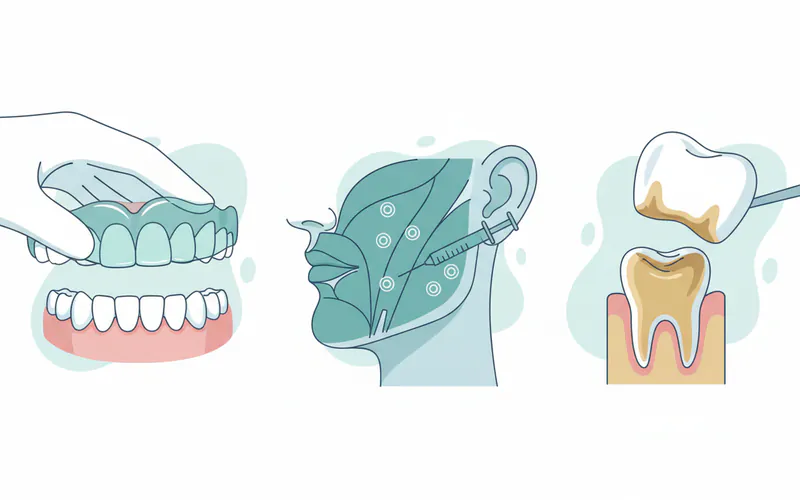
Dental Appliances: Nightguards and Splints
Custom-fitted dental appliances are often the first line of defense against bruxism.
- Nightguards (Occlusal Guards): These are custom-made acrylic or plastic devices worn over the upper or lower teeth, primarily during sleep.
- Pros: They create a protective barrier between your molars, preventing direct contact and absorbing the grinding forces. They can also help reposition the jaw, relieving muscle tension and promoting a more relaxed bite. Custom nightguards fit precisely and are comfortable for long-term use.
- Cons: Can be expensive (compared to over-the-counter options), require diligent cleaning, and some initial adjustment period. They treat the symptoms, not the underlying cause.
- Occlusal Splints (Stabilization Splints): Similar to nightguards but often more rigid and precisely calibrated to create a specific bite relationship. They are designed to stabilize the jaw joint and muscles.
- Pros: Highly effective for TMJ pain, precise fit, and durability.
- Cons: Can be more expensive and require more frequent adjustments by the dentist.
Pro Tip: Avoid generic "boil-and-bite" mouthguards found in pharmacies. While cheaper ($20-$100), they rarely fit properly, can exacerbate bite issues, and offer inadequate protection against severe bruxism forces. A custom-fitted nightguard from your dentist, costing typically $300-$800, is a worthwhile investment in your long-term dental health.
Restorative Dentistry
Once molars are damaged, restorative treatments are necessary to repair them and prevent further deterioration.
- Dental Fillings: For minor chips or areas of wear, composite resin fillings can restore tooth shape and protect exposed dentin.
- Pros: Less invasive, relatively quick procedure.
- Cons: Not suitable for extensive damage, may wear down over time with continued bruxism.
- Dental Crowns: If a molar has significant wear, fractures, or loss of tooth structure, a dental crown (cap) can fully cover and protect the entire tooth. Crowns are typically made of porcelain, ceramic, or zirconia.
- Pros: Restores tooth strength, function, and aesthetics; highly durable.
- Cons: Requires removal of some healthy tooth structure, more expensive, may need replacement after many years.
- Onlays/Inlays: These are partial crowns used when the damage is too extensive for a filling but doesn't require a full crown. They restore the cusps or biting surface of the molar.
- Pros: More conservative than a full crown, strong and durable.
- Cons: More expensive than fillings, requires laboratory fabrication.
- Root Canal Treatment: If bruxism causes a tooth to fracture deeply and expose the pulp (nerve), or if chronic irritation leads to pulp inflammation or infection, a root canal may be necessary before placing a crown.
- Pros: Saves the natural tooth.
- Cons: Invasive, requires subsequent crown placement, can be costly.
- Tooth Extraction and Replacement: In rare cases of extreme, irreparable damage or vertical root fractures, the molar may need to be extracted and replaced with a dental implant or bridge.
- Pros: Replaces severely damaged or lost teeth.
- Cons: Most invasive and expensive option, involves surgical procedures.
Orthodontics
If malocclusion is identified as a significant contributing factor to your bruxism, orthodontic treatment can help create a balanced bite.
- Pros: Addresses a potential root cause, improves overall dental alignment and function.
- Cons: Long treatment duration (months to years), significant cost, requires patient compliance.
Behavioral Therapies and Stress Management
Addressing the psychological components of bruxism is critical.
- Stress Reduction Techniques: Yoga, meditation, deep breathing exercises, mindfulness, and regular physical activity can help manage stress levels.
- Biofeedback: This technique uses electronic sensors to monitor muscle activity, allowing you to become more aware of jaw clenching and learn to relax those muscles.
- Cognitive Behavioral Therapy (CBT): A therapist can help identify triggers for stress and bruxism, and develop coping mechanisms.
- Habit Reversal: For awake bruxism, consciously repositioning your jaw (tongue resting on the roof of your mouth, teeth slightly apart) can help break the habit. Setting reminders on your phone can be helpful.
Medications
- Muscle Relaxants: Prescribed for short-term use to alleviate acute jaw pain and muscle spasms, especially before bedtime.
- Botulinum Toxin (Botox) Injections: Small amounts of Botox injected into the masseter muscles (jaw muscles) can temporarily weaken them, reducing the force of clenching and grinding.
- Pros: Highly effective for severe cases, significant pain relief, lasts typically 3-6 months.
- Cons: Temporary, requires repeat injections, can be costly, potential for temporary muscle weakness or asymmetry.
- Anti-inflammatory Drugs: Over-the-counter NSAIDs (ibuprofen, naproxen) can help manage pain and inflammation from jaw muscles.
Physical Therapy
For persistent jaw pain and limited movement, a physical therapist specializing in craniomandibular disorders can teach exercises, stretches, and manual techniques to improve jaw function and reduce muscle tension.
Step-by-Step Process: What to Expect During Treatment
While treatments vary, here's a general process for managing severe bruxism molars:
1. Initial Consultation and Diagnosis
Your dentist will conduct a thorough examination, including:
- Visual Inspection: Looking for signs of wear, fractures, gum recession, and muscle tenderness.
- Palpation: Checking jaw muscles and the TMJ for pain and tenderness.
- Dental X-rays: To assess tooth roots, bone health, and detect any underlying issues like cysts or infections.
- Patient History: Discussing your symptoms, lifestyle, stress levels, sleep habits, and medications. You may be asked if a partner has noticed the teeth grinding sound.
- Bite Analysis: Evaluating how your upper and lower teeth meet.
- Referral (if needed): For suspected sleep apnea, a sleep study might be recommended. For chronic pain, referral to an orofacial pain specialist, physical therapist, or ENT may occur.
2. Treatment Planning
Based on the diagnosis, your dentist will recommend a personalized treatment plan. This might involve a single intervention or a combination of approaches. They will discuss the pros, cons, costs, and expected outcomes of each option.
3. Implementation of Primary Treatment (e.g., Nightguard)
- Impressions: For a custom nightguard, your dentist will take precise impressions or digital scans of your teeth.
- Fabrication: These impressions are sent to a dental lab where your custom nightguard or splint is fabricated. This typically takes 1-2 weeks.
- Fitting and Adjustment: You'll return for a fitting appointment to ensure the appliance is comfortable and fits correctly. Your dentist will make any necessary adjustments. You'll receive instructions on how to wear and care for it.
4. Restorative Procedures (if necessary)
- Preparation: If crowns or fillings are needed, the damaged tooth structure will be prepared. This may involve shaping the molar to accommodate a crown.
- Impressions for Restorations: Impressions are taken for lab-fabricated crowns or onlays.
- Temporary Restorations: Temporary crowns or fillings may be placed to protect the teeth while permanent ones are being made (typically 1-3 weeks).
- Placement of Permanent Restorations: Once ready, the permanent crowns, onlays, or fillings are bonded to your molars.
5. Adjunctive Therapies
- Botox Injections: If recommended, these are performed in the dental office. A series of small injections are strategically placed in the masseter muscles.
- Behavioral Coaching: Your dentist or a referred specialist will provide guidance on stress management and habit awareness.
6. Follow-up and Monitoring
Regular follow-up appointments are crucial to monitor your progress, adjust appliances, check the integrity of restorations, and re-evaluate your bruxism symptoms. Your dentist will ensure that your molars are protected and your overall oral health is improving.

Cost and Insurance: Navigating Financial Aspects in the US
The cost of treating severe bruxism molars in the United States can vary significantly based on the severity of damage, the chosen treatment modalities, the materials used, and your geographic location. Understanding these costs and how insurance plays a role is essential.
Average US Price Ranges for Key Treatments
| Treatment Type | Average US Cost Range (Without Insurance) | Notes |
|---|---|---|
| Custom Nightguard | $300 - $800 | Price varies by material (hard acrylic usually more durable and effective than soft plastic) and complexity. Essential for protecting molars. |
| Occlusal Splint | $600 - $1,500 | More rigid and precise than a standard nightguard, often used for significant TMJ involvement. |
| Boil-and-Bite Mouthguard | $20 - $100 | Over-the-counter. Not recommended for severe bruxism due to poor fit and lack of effectiveness for long-term protection. |
| Dental Filling (Composite) | $150 - $400 per tooth | For minor chips or wear. Cost depends on size and location of the filling. |
| Dental Crown (Porcelain/Zirconia) | $800 - $3,000 per tooth | For extensively damaged molars. Cost varies by material, lab fees, and dentist's location. Porcelain fused to metal is typically on the lower end, full zirconia or all-ceramic on the higher. |
| Dental Onlay | $700 - $1,800 per tooth | For moderate damage, more conservative than a full crown. |
| Root Canal Treatment | $700 - $1,500 (molars) | If bruxism leads to nerve damage. This cost is in addition to the cost of a subsequent crown. |
| Dental Implant (Single Tooth) | $3,000 - $6,000+ | Includes implant, abutment, and crown. For replacement of a severely damaged molar that cannot be saved. Does not include extraction or bone grafting if needed. |
| Botox Injections | $300 - $1,000 per session | For jaw muscle relaxation. Requires repeat injections every 3-6 months. Cost depends on the number of units used. |
| Orthodontics (Braces/Aligners) | $3,000 - $8,000+ | For correcting significant malocclusion. Comprehensive treatment, usually over 1-3 years. |
| Physical Therapy (TMJ) | $75 - $200 per session | Often requires multiple sessions. |
Insurance Coverage Details
Dental insurance coverage for bruxism treatment can be complex and varies widely depending on your specific plan (PPO, HMO, etc.), deductible, and annual maximums.
- Diagnostic Services: Initial exams, X-rays, and consultations are typically covered at 80-100% after your deductible.
- Nightguards/Occlusal Splints: Many dental insurance plans offer some coverage for custom nightguards, often classifying them under "major restorative" or "appliance" categories. Coverage usually ranges from 20-50%, but some plans may not cover them at all if considered "preventive" or "comfort" rather than medically necessary. It's crucial to check with your provider.
- Restorative Procedures (Fillings, Crowns, Onlays): These are usually covered under "basic" or "major" services.
- Fillings: Often covered at 70-80%.
- Crowns/Onlays: Typically covered at 50-70% after your deductible.
- Root Canals: Generally covered at 50-80%.
- Dental Implants: Coverage is often limited or non-existent for implants, sometimes requiring a separate medical insurance claim if it's considered medically necessary after a trauma or severe disease. Some plans may cover the implant crown but not the implant post itself.
- Orthodontics: Coverage for orthodontics is highly variable. Some plans include it, often with a lifetime maximum benefit, while many adult plans do not. Pediatric plans are more likely to offer coverage.
- Botox Injections: Dental insurance typically does not cover Botox for bruxism. It might be covered by medical insurance if deemed medically necessary for a severe TMJ disorder and if you meet specific criteria, but this is rare. You will likely pay out-of-pocket for this treatment.
- Physical Therapy: May be covered by medical insurance, not dental, depending on your plan and the diagnosis (e.g., TMJ disorder).
Pro Tip: Always contact your dental insurance provider directly before starting any major treatment. Ask for a pre-determination of benefits (PDB) for specific procedures your dentist recommends. This will give you a clear estimate of what your plan will cover.
Recovery and Aftercare: Protecting Your Investment
Recovery from bruxism treatment involves both immediate post-procedure care and long-term habits to maintain your oral health and prevent recurrence of damage.
After Nightguard/Splint Placement
- Initial Adjustment: It's normal to feel a bit awkward or have slight difficulty speaking or swallowing initially. Some people experience increased saliva production. This usually subsides within a few days to a week.
- Jaw Soreness: You might experience some mild jaw soreness as your muscles adjust to the new bite position. This is typically temporary.
- Wearing Schedule: Adhere strictly to your dentist's instructions, usually wearing the appliance every night. Consistency is key for effectiveness.
- Cleaning: Clean your nightguard daily with a toothbrush and mild soap or non-abrasive denture cleaner. Avoid harsh chemicals or hot water, which can damage the material. Store it in its case when not in use.
- Regular Check-ups: Bring your nightguard to all dental appointments for evaluation and adjustments. Over time, it may need to be relined or replaced (typically every 5-10 years, depending on material and bruxism severity).
After Restorative Work (Fillings, Crowns, Onlays)
- Sensitivity: It's common to experience temporary sensitivity to hot or cold after a filling or crown, which should resolve within a few days to weeks.
- Bite Adjustment: Your bite will be checked and adjusted during placement. If it feels "off" after the numbing wears off, contact your dentist for further adjustment, as an uneven bite can exacerbate bruxism or cause discomfort.
- Oral Hygiene: Continue diligent brushing and flossing, paying close attention around new restorations. While crowns protect the tooth underneath, the surrounding gum tissue and margins can still be susceptible to decay or gum disease.
- Protecting Restorations: Even with restorations, it's crucial to continue managing bruxism (e.g., wearing your nightguard) to protect your new fillings or crowns from being damaged by grinding forces.
General Aftercare and Lifestyle Adjustments
- Pain Management: For any residual jaw pain, applying moist heat or a cold compress to the jaw muscles can provide relief. Over-the-counter pain relievers like ibuprofen or naproxen can also help.
- Soft Diet: For a few days after extensive restorative work or if jaw muscles are particularly sore, stick to softer foods that require less chewing.
- Jaw Relaxation Exercises: Your dentist or physical therapist may recommend gentle jaw stretches and exercises to improve flexibility and reduce tension.
- Stress Management: Continually practice stress-reducing techniques. Consider incorporating regular meditation, yoga, or professional counseling into your routine.
- Avoid Stimulants: Reduce or eliminate caffeine, alcohol, and nicotine, especially in the hours leading up to bedtime.
- Sleep Hygiene: Maintain a regular sleep schedule, create a comfortable sleep environment, and address any diagnosed sleep disorders like sleep apnea.
- Regular Dental Visits: Continue with your routine dental check-ups (typically every 6 months) so your dentist can monitor your bruxism, assess your restorations, and address any new concerns promptly.
Prevention: Stopping Bruxism Before It Starts (or Worsens)
Preventing severe bruxism molars involves a proactive approach to managing triggers and protecting your teeth. While not all causes are preventable (e.g., neurological conditions), many lifestyle and psychological factors can be controlled.
Stress Reduction Techniques
Given that stress is a primary cause of teeth grinding, implementing effective stress management strategies is paramount:
- Mindfulness and Meditation: Practice daily meditation or mindfulness exercises to calm your nervous system. Even 10-15 minutes a day can make a difference.
- Yoga and Deep Breathing: These practices promote relaxation and can reduce overall muscle tension, including in the jaw.
- Regular Exercise: Physical activity is a proven stress reliever. Aim for at least 30 minutes of moderate exercise most days of the week.
- Adequate Sleep: Ensure you get 7-9 hours of quality sleep each night. Poor sleep exacerbates stress and can worsen bruxism.
- Professional Help: If stress or anxiety feels overwhelming, consider counseling or therapy. A mental health professional can provide tools and strategies for coping.
Improve Sleep Hygiene
Good sleep habits can significantly reduce nocturnal bruxism:
- Consistent Sleep Schedule: Go to bed and wake up at the same time every day, even on weekends.
- Relaxing Bedtime Routine: Create a calming routine before bed, such as reading, taking a warm bath, or listening to soothing music.
- Optimize Sleep Environment: Ensure your bedroom is dark, quiet, and cool.
- Avoid Screens Before Bed: The blue light from phones, tablets, and computers can interfere with melatonin production.
- Limit Stimulants: Avoid caffeine, alcohol, and heavy meals several hours before sleep.
- Address Sleep Disorders: If you suspect you have sleep apnea or another sleep disorder, consult a medical doctor for diagnosis and treatment.
Dental Care and Awareness
- Regular Dental Check-ups: Visit your dentist every 6 months for routine exams and cleanings. Your dentist is often the first to spot early signs of bruxism-related tooth wear.
- Correct Malocclusion: If your dentist identifies a significant bite problem that could contribute to bruxism, discuss orthodontic solutions.
- Conscious Awareness (for awake bruxism): Throughout the day, occasionally check your jaw position. Your teeth should not be touching unless you are chewing or swallowing. Practice resting your tongue lightly on the roof of your mouth, with your teeth slightly apart.
- Avoid Hard, Chewy Foods: If you are prone to bruxism, temporarily avoiding excessively hard or chewy foods can give your jaw muscles a rest.
- Stay Hydrated: Dehydration can sometimes contribute to muscle cramps and tension.
Risks and Complications: What Can Go Wrong
Untreated or poorly managed severe bruxism can lead to a cascade of serious and painful complications, impacting not only your dental health but your overall quality of life.
- Severe Tooth Wear and Loss: The most direct complication. Molars can be worn down to stumps, requiring extensive restorative work or even extraction. Loss of vertical dimension (the distance between your upper and lower jaws) can also occur, leading to a collapsed bite and an older facial appearance.
- Tooth Fractures and Cracks: The intense forces can cause teeth to crack, sometimes extending into the root. These fractures can be painful, lead to infections, and often result in tooth loss.
- Increased Tooth Sensitivity: Exposure of dentin and pulp due to wear or cracks makes teeth highly sensitive to temperature changes and sweets.
- Temporomandibular Joint (TMJ) Disorders: Chronic strain on the TMJ can lead to inflammation, dislocation of the joint disk, pain, clicking, popping, limited jaw movement, and even locking of the jaw. This can become a debilitating chronic pain condition.
- Jaw Muscle Hypertrophy: Overuse of jaw muscles can cause them to become enlarged and bulge, affecting facial aesthetics.
- Chronic Headaches and Facial Pain: Persistent tension headaches, migraines, and generalized facial pain are common, significantly impacting daily function and sleep.
- Gum Recession and Bone Loss: The constant pressure can contribute to the gums pulling away from the teeth and even localized bone loss around the roots, making teeth unstable.
- Dental Infections: Cracked teeth can allow bacteria to enter the inner pulp, leading to painful infections that require root canals or extraction.
- Impact on Restorations: Existing fillings, crowns, and bridges can be damaged, loosened, or fractured by bruxism, requiring costly repairs or replacements.
- Sleep Disruption: While bruxism often occurs during sleep, the pain and discomfort it causes can ironically disrupt sleep further, creating a vicious cycle.
- Nutritional Deficiencies: In severe cases, pain and sensitivity can make eating difficult, leading to a reluctance to consume certain foods and potentially impacting nutrition.
Children / Pediatric Considerations
Bruxism is surprisingly common in children, affecting up to 30% of children at some point, particularly between the ages of 3 and 10. While most children outgrow it without intervention, severe cases affecting molars do occur and warrant attention.
Common Causes in Children
- Growth and Development: As children's jaws and teeth develop, misalignments or changes in bite can trigger grinding. Teething, especially of molars, can also be a factor.
- Stress and Anxiety: Just like adults, children can experience stress from school, family changes, or emotional issues, leading to bruxism.
- Allergies and Ear Infections: Congestion or pain can cause children to adjust their jaw position, leading to grinding.
- Sleep Disorders: Sleep apnea or other sleep disturbances, including restless leg syndrome, can be linked to bruxism in children.
- Medical Conditions: Certain medical conditions, like cerebral palsy, can increase the likelihood of bruxism.
Signs and Symptoms in Children
- Teeth Grinding Sound: Often noticed by parents during sleep.
- Worn or Flattened Teeth: Visible wear on primary (baby) teeth or even newly erupted permanent molars.
- Jaw Pain or Fatigue: Child may complain of a sore jaw in the morning.
- Headaches: Vague complaints of headaches.
- Tooth Sensitivity: Child might avoid certain foods.
Treatment for Children
For most children, bruxism is temporary and does not require extensive treatment. However, if there is significant molar wear, pain, or functional issues, a dentist may recommend intervention.
- Monitoring: Regular dental check-ups are essential to monitor tooth wear and jaw development.
- Stress Management: Help children manage stress through relaxation techniques, open communication, and ensuring a secure home environment.
- Addressing Underlying Issues: Treating allergies, ear infections, or sleep disorders can often resolve bruxism.
- Nightguards (Rarely): Custom nightguards are generally reserved for severe cases in older children with permanent teeth, due to constant jaw growth and potential interference with tooth eruption. When used, they must be frequently monitored and adjusted.
- Nocturnal Alarms: Some dentists might suggest simple behavioral alarms to interrupt grinding during sleep for older children.
Pro Tip for Parents: If you notice your child grinding their teeth, observe them for a few weeks and mention it to their pediatric dentist. Most times, it's a phase, but persistent grinding, especially with pain or visible wear, needs professional evaluation.
Cost Breakdown: A Deeper Look at Financial Considerations
Beyond the individual treatment costs, understanding the overall financial landscape of managing severe bruxism molars is crucial for budgeting and planning.
Average US Costs: Low, Mid, and High Estimates
A comprehensive treatment plan for severe bruxism molars, encompassing diagnosis, immediate protection, and restorative work, can range significantly.
- Low-End Estimate ($800 - $3,000): This might include a custom nightguard ($300-$800), initial exam and X-rays ($150-$400), and a few composite fillings ($150-$400 each) for minor wear. This assumes no severe tooth damage or TMJ issues.
- Mid-Range Estimate ($3,000 - $10,000): This often involves a custom nightguard, more extensive restorative work like 2-4 dental crowns or onlays ($800-$3,000 each), and potentially some follow-up Botox injections ($300-$1,000 per session) for muscle pain. This range is common for individuals with moderate to severe molar damage.
- High-End Estimate ($10,000 - $30,000+): For very severe cases with widespread molar damage, significant TMJ involvement, or teeth that need to be extracted and replaced with implants ($3,000-$6,000+ per tooth), the costs can escalate dramatically. Orthodontics ($3,000-$8,000+) to correct a severe malocclusion might also be included here. This range often reflects a need for multiple specialists and long-term treatment.
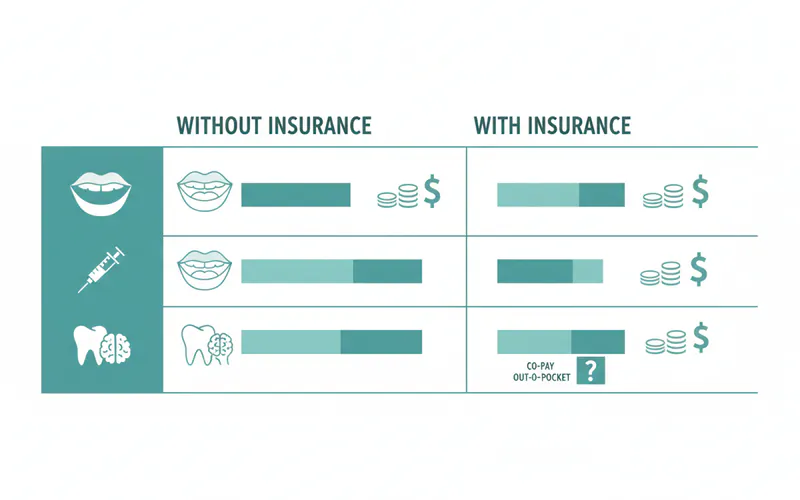
With vs. Without Insurance
- With Insurance: As discussed, insurance can significantly reduce your out-of-pocket expenses for certain procedures (e.g., fillings, crowns, nightguards typically 20-80% coverage). However, deductibles (usually $50-$250) and annual maximums (often $1,000-$2,000 per year) mean you will still pay a substantial portion, especially for extensive work. For treatments like Botox or implants, coverage is often minimal or non-existent, leaving you responsible for the full cost.
- Without Insurance: You will be responsible for 100% of all costs. This makes understanding pricing and seeking financing even more critical.
Payment Plans and Financing Options
Many dental offices recognize the significant investment required for comprehensive bruxism treatment and offer various payment solutions:
- In-Office Payment Plans: Some practices allow you to pay for treatment in installments over several months, often without interest, directly through their office.
- Third-Party Financing (e.g., CareCredit): Companies like CareCredit offer special healthcare financing with deferred interest options if paid within a certain timeframe (e.g., 6, 12, or 18 months). Interest rates can be high if the balance isn't paid off in time.
- Personal Loans: Banks and credit unions offer personal loans that can be used for dental expenses, often with competitive interest rates depending on your credit score.
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): If you have an HSA or FSA through your employer, you can use these tax-advantaged accounts to pay for qualified dental expenses, including bruxism treatment.
Cost-Saving Tips
- Preventive Care: The best cost-saving measure is prevention. Regular check-ups and early intervention prevent minor issues from becoming costly severe bruxism molars.
- Utilize Insurance Benefits: Maximize your annual dental insurance benefits. If you have extensive treatment planned, you might be able to split it across two calendar years to take advantage of two annual maximums.
- Shop Around (Carefully): Get quotes from a few different reputable dentists for major procedures. However, prioritize quality and trust over the absolute lowest price, especially for complex restorative work.
- Dental Schools: University dental schools often offer services at a reduced cost, as procedures are performed by students under the close supervision of experienced faculty.
- Payment Plan Discussion: Don't hesitate to discuss payment concerns and options with your dental office's financial coordinator. They often have solutions or can guide you.
Frequently Asked Questions
Is severe bruxism curable?
While there isn't a single "cure" for bruxism in the sense of permanently eliminating the habit, severe bruxism can be effectively managed and controlled to prevent further damage and alleviate symptoms. Treatment focuses on protecting your teeth, reducing muscle activity, and addressing underlying causes like stress or sleep disorders. For many, long-term management with a nightguard and lifestyle adjustments is key.
How long does a custom nightguard last, and how often do I need to replace it?
A well-made custom nightguard typically lasts between 5 to 10 years, depending on the material, the severity of your bruxism, and how well you care for it. Over time, the plastic may show significant wear, thinning, or even holes. Your dentist will evaluate its condition during your regular check-ups and advise you when it's time for replacement.
Can insurance cover Botox for bruxism?
Generally, dental insurance does not cover Botox injections for bruxism. In some rare cases, medical insurance might provide coverage if the Botox is deemed medically necessary for a severe TMJ disorder and meets specific criteria, but this is uncommon. Most patients should expect to pay for Botox treatments out-of-pocket, which usually requires repeat injections every 3-6 months.
Is teeth grinding a sign of sleep apnea?
Yes, there is a strong correlation between nocturnal teeth grinding and obstructive sleep apnea (OSA). While not everyone who grinds their teeth has sleep apnea, bruxism is a common symptom in individuals with OSA. If you experience severe bruxism along with snoring, gasping for air during sleep, or daytime fatigue, your dentist may recommend a sleep study to rule out or diagnose sleep apnea.
What are the alternatives to wearing a nightguard?
While a custom nightguard is often the most effective and direct method for protecting teeth from grinding forces, alternatives or complementary treatments include stress management techniques, biofeedback, physical therapy, Botox injections to relax jaw muscles, and addressing underlying sleep disorders. For some, orthodontic treatment to correct bite issues might also be considered. However, for direct tooth protection, a nightguard is typically unsurpassed.
Does severe bruxism ever go away on its own?
In adults, severe bruxism rarely disappears completely on its own without intervention, especially if it has led to significant molar damage. While minor or occasional bruxism might resolve, chronic severe grinding usually requires ongoing management. In children, however, bruxism is often temporary and many outgrow it as their dental arches develop.
Can severe bruxism cause permanent facial changes?
Yes, chronic severe bruxism, particularly clenching, can lead to permanent changes. The masseter muscles (jaw muscles) can hypertrophy (enlarge) from overuse, giving the lower face a wider, squarer appearance. Additionally, severe wear of molars can lead to a loss of vertical facial dimension, making the face appear shorter and contributing to a prematurely aged look.
How painful is bruxism treatment?
The pain associated with bruxism treatment varies. Wearing a nightguard might cause mild, temporary jaw soreness as you adjust. Restorative procedures like fillings and crowns are performed under local anesthesia, so you won't feel pain during the procedure, but some sensitivity or soreness might occur afterward. Botox injections involve minor needle pricks, similar to a bee sting, with minimal discomfort. Overall, the pain is usually manageable and far less than the chronic pain caused by untreated severe bruxism.
When to See a Dentist
It's crucial to understand when to seek professional dental care for bruxism to prevent severe damage and address underlying issues.
Schedule a routine dental appointment if you notice any of the following signs:
- Persistent jaw pain or soreness, especially upon waking.
- Frequent headaches (tension headaches) or earaches without an ear infection.
- Tooth sensitivity to hot, cold, or sweets, which wasn't present before.
- Your partner mentions hearing a teeth grinding sound from you at night.
- You notice any flattening, chipping, or unusual wear patterns on your molars.
- You experience difficulty or pain when opening your mouth wide, or a clicking/popping sound in your jaw.
- You have dental restorations (fillings, crowns) that frequently break or loosen.
Seek immediate attention or an emergency appointment if you experience:
- Sudden, severe, and excruciating tooth pain that persists, especially if it feels like a sharp, shooting pain upon biting down, which could indicate a fractured tooth.
- A jaw that locks open or closed, preventing normal function.
- Swelling in your jaw or face, which could indicate an infection related to a cracked tooth.
- Acute and debilitating TMJ pain that significantly interferes with eating or speaking.
Don't wait until the damage is severe. Early diagnosis and intervention by a qualified dental professional can save your molars, prevent chronic pain, and improve your overall quality of life. The American Dental Association (ADA) strongly recommends regular dental check-ups for early detection and management of bruxism and other oral health concerns.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles

What Causes Teeth Grinding in Sleep
More than one in ten adults—and even more children—clench or grind their teeth during sleep, a condition known medically as sleep bruxism. For many, it's an unconscious habit that goes unnoticed until significant damage or discomfort arises. Waking up with a dull, constant headache, jaw pain, or
February 23, 2026
How to Not Grind Teeth at Night
More than one in ten adults and a significant percentage of children experience teeth grinding, medically known as bruxism, a condition that often goes unnoticed, especially when it occurs during sleep. If you've woken up with a sore jaw, a dull headache, or noticed your teeth becoming unusually
February 23, 2026

What Is Jaw Clenching
Do you often wake up with a dull headache, a sore jaw, or unexplained tooth sensitivity? You're not alone. Approximately 1 in 10 adults and up to 3 in 10 children experience some form of bruxism, a condition characterized by grinding, gnashing, or clenching your teeth. At the heart of this wides
February 23, 2026

How to Prevent Teeth Grinding in Sleep
Teeth grinding, medically known as bruxism, is a common condition that affects millions of Americans. Often occurring subconsciously during sleep, it can lead to a host of uncomfortable and potentially serious health issues, ranging from persistent headaches and jaw pain to significant dental damage
February 23, 2026