How to Not Grind Teeth at Night
Key Takeaways
- More than one in ten adults and a significant percentage of children experience teeth grinding, medically known as bruxism, a condition that often goes unnoticed, especially when it occurs during sleep. If you've woken up with a sore jaw, a dull headache, or noticed your teeth becoming unusually
More than one in ten adults and a significant percentage of children experience teeth grinding, medically known as bruxism, a condition that often goes unnoticed, especially when it occurs during sleep. If you've woken up with a sore jaw, a dull headache, or noticed your teeth becoming unusually sensitive, you might be asking how to not grind teeth at night. This article from SmilePedia.net is your comprehensive guide to understanding nocturnal bruxism and equipping you with effective strategies to stop teeth grinding at night, protecting your oral health and overall well-being. We'll delve into the causes behind this common habit, explore its wide-ranging symptoms, and meticulously outline various treatment options – from simple at-home remedies like specific massages for jaw clenching to advanced dental interventions. Our goal is to empower you with the knowledge and tools needed to reclaim peaceful sleep and a healthy, pain-free smile.
Key Takeaways:
- Prevalence: Approximately 10-15% of adults and 15-20% of children experience bruxism, often unknowingly.
- Primary Solution: Custom-fitted nightguards are often the first line of defense, costing $300-$800 (without insurance) and lasting 1-5 years.
- Underlying Causes: Stress, sleep disorders (like sleep apnea), certain medications, and bite issues are common contributors. Addressing these is crucial for long-term relief.
- Lifestyle Changes: Stress reduction techniques, avoiding stimulants, and improving sleep hygiene can significantly reduce grinding severity.
- Advanced Treatments: For severe cases, Botox injections (costing $300-$600 per treatment, lasting 3-6 months) or orthodontic interventions (ranging $3,000-$8,000+) may be recommended.
- Actionable Steps: Incorporate daily jaw relaxation exercises and massages for jaw clenching, especially before bedtime, to alleviate tension.
- When to See a Dentist: Consult a dental professional if you experience persistent jaw pain, headaches, tooth sensitivity, or visible tooth wear. Early intervention prevents further damage.
Understanding Bruxism: What It Is and Why It Matters
Bruxism is the medical term for involuntary grinding, clenching, or gnashing of teeth. It can occur during the day (awake bruxism) or, more commonly, during sleep (sleep bruxism). While occasional teeth grinding might not be harmful, chronic bruxism can lead to a host of dental and medical complications, significantly impacting your quality of life. The forces exerted during bruxism can be up to six times greater than those used for chewing, putting immense strain on your teeth, jaws, and surrounding muscles.

Ignoring bruxism can lead to serious consequences, including:
- Tooth damage: Worn down enamel, chipped teeth, fractured teeth, increased sensitivity.
- Jaw problems: Temporomandibular joint (TMJ) disorders, characterized by pain, clicking, or limited jaw movement.
- Headaches and facial pain: Often concentrated in the temples or jaw area.
- Sleep disruption: For both the individual and their sleep partner due to grinding noises.
- Muscle hypertrophy: Enlargement of the jaw muscles, leading to a squarer facial appearance.
Understanding bruxism is the first step toward effective management and prevention.
Types of Bruxism
Bruxism manifests in two primary forms, each with distinct characteristics and potential causes:
-
Awake Bruxism (Diurnal Bruxism):
- Definition: This involves consciously or subconsciously clenching or grinding teeth while awake. It's often a habitual response to stress, anxiety, concentration, or even specific tasks like driving or working on a computer.
- Characteristics: Individuals are often unaware they are doing it until symptoms like jaw tension or headaches appear. It tends to involve clenching rather than grinding.
- Management: Awareness and self-monitoring are key. Techniques like mindfulness, biofeedback, and consciously relaxing the jaw muscles can be effective.
-
Sleep Bruxism (Nocturnal Bruxism):
- Definition: This is the more common and often more damaging form, occurring involuntarily during sleep. Because it happens unconsciously, many individuals only discover they have it through a sleep partner, a dentist, or by experiencing symptoms upon waking.
- Characteristics: Involves both clenching and grinding, often in rhythmic, sustained bursts. It’s classified as a sleep-related movement disorder and is frequently associated with other sleep disturbances.
- Management: Typically requires dental interventions like nightguards, alongside addressing underlying sleep issues or medical conditions.
This article primarily focuses on how to not grind teeth at night, addressing the challenges and solutions associated with nocturnal bruxism.
Unraveling the Causes of Teeth Grinding at Night
Pinpointing the exact cause of sleep bruxism can be challenging, as it often results from a complex interplay of physical, psychological, and genetic factors. Understanding these potential triggers is vital for effective treatment.
Psychological Factors
- Stress and Anxiety: This is arguably the most common culprit. High levels of emotional stress, anxiety, frustration, anger, or tension can manifest as physical clenching and grinding during sleep. The body’s response to stress often includes muscle tension, and the jaw muscles are no exception.
- Personality Type: Some research suggests that individuals with aggressive, competitive, or hyperactive personality traits may be more prone to bruxism.
- Depression: There's a known correlation between depression and an increased incidence of bruxism, likely due to shared neurochemical pathways and stress responses.
Sleep-Related Factors
- Sleep Disorders: Sleep bruxism is strongly associated with other sleep disorders, particularly obstructive sleep apnea (OSA). In individuals with OSA, the body may clench or grind its teeth as a subconscious effort to open the airway during episodes of breathing cessation.
- Arousal from Sleep: Bruxism episodes often occur during micro-arousals from deep sleep (NREM stage 2 and REM sleep), rather than during continuous deep sleep. These brief awakenings are part of the normal sleep cycle but can trigger grinding.
- Sleep Position: While not a direct cause, some anecdotal evidence suggests certain sleep positions might exacerbate jaw tension.
Physical and Physiological Factors
- Malocclusion (Misaligned Bite): Historically, an "imperfect bite" or misaligned teeth were thought to be the primary cause of bruxism. While modern research has downplayed its sole role, significant bite discrepancies can still contribute to abnormal jaw function and muscle strain, potentially triggering grinding. The American Dental Association (ADA) acknowledges that while occlusal factors can contribute, they are rarely the sole cause.
- Dental Issues: Missing teeth, new fillings or crowns, or uneven tooth surfaces can sometimes create "high spots" that disrupt the bite and lead to grinding as the jaw attempts to find a comfortable position.
- Genetics: There's evidence of a genetic predisposition to bruxism, meaning it can run in families. If your parents or siblings grind their teeth, you might be more likely to develop the habit.
- Neurological Conditions: Rare cases of bruxism can be linked to certain neurological conditions like Parkinson's disease, Huntington's disease, or epilepsy.
Medications and Substances
- Antidepressants: Selective serotonin reuptake inhibitors (SSRIs) like Prozac, Zoloft, and Paxil, commonly prescribed for depression and anxiety, are known to induce or worsen bruxism in some individuals.
- Stimulants: Amphetamines and other stimulant medications, often used for ADHD, can increase central nervous system activity, leading to heightened muscle tension and grinding.
- Recreational Drugs: Cocaine, ecstasy (MDMA), and methamphetamine can cause severe bruxism.
- Caffeine and Alcohol: Excessive consumption of caffeine and alcohol, especially close to bedtime, can disrupt sleep patterns and increase muscle activity, potentially exacerbating grinding.
- Tobacco: Nicotine is a stimulant that can also interfere with sleep architecture and muscle relaxation, increasing the risk of bruxism.
Understanding these multifaceted causes is crucial. A thorough dental and medical evaluation by a dentist or a sleep specialist can help identify the underlying triggers for your specific case, paving the way for targeted and effective treatment.
Recognizing the Signs and Symptoms of Teeth Grinding
Because nocturnal bruxism occurs unconsciously, many people are unaware they grind their teeth until symptoms become noticeable or a partner points it out. Recognizing these signs early is crucial to prevent long-term damage.
Common Signs and Symptoms:
-
Tooth Damage:
- Worn-down, flattened, fractured, or chipped teeth: This is often the most telling sign. You might notice your teeth look shorter or have sharp edges.
- Increased tooth sensitivity: Especially to hot, cold, or sweet foods due to enamel erosion.
- Loose teeth: In severe, chronic cases, the constant force can loosen teeth.
- Abfractions: Notches or grooves near the gum line, often wedge-shaped.
- Dental restorations damage: Fractured fillings, crowns, or veneers.
-
Jaw and Facial Pain:
- Sore or tired jaw muscles: Particularly noticeable upon waking.
- Pain or tenderness in the temporomandibular joints (TMJ): The joints connecting your jaw to your skull, located just in front of your ears.
- Locked jaw: In some cases, the jaw may temporarily lock open or closed.
- Limited jaw movement: Difficulty opening your mouth wide.
- Clicking, popping, or grinding sounds: When opening or closing your mouth.
-
Headaches and Earaches:
- Dull, constant headache: Often originating in the temples and present upon waking. These are frequently tension-type headaches.
- Earaches: Even though there's no problem with the ear itself, referred pain from the jaw muscles can mimic an earache.
-
Other Symptoms:
- Sleep disruption: The grinding noises can disturb your sleep or that of your sleep partner.
- Indentation on the tongue: Scalloped edges along the sides of the tongue, caused by pressing it against your teeth.
- Cheek biting: Damage to the inside of the cheek, sometimes showing a white line where the teeth meet.
- Muscle hypertrophy: Enlarged masseter muscles (jaw muscles) can lead to a more square-shaped face.
If you or a loved one notice any of these signs, it's essential to schedule an appointment with your dentist. They can diagnose bruxism, assess the extent of the damage, and recommend appropriate treatment options. Early intervention is key to preventing further complications and improving your overall oral and general health.
Comprehensive Treatment Options to Stop Teeth Grinding at Night
Effectively managing nocturnal bruxism often involves a multi-pronged approach, targeting both the symptoms and the underlying causes. Your dentist will work with you to determine the most suitable treatment plan.
1. Dental Appliances (Nightguards or Occlusal Splints)
What they are: These are custom-made devices, typically made of hard acrylic or soft plastic, that fit over your upper or lower teeth. They act as a protective barrier, preventing direct contact between your teeth and absorbing the force of grinding and clenching. Pros:
- Protects teeth: Prevents wear, fractures, and sensitivity.
- Reduces jaw pain: Cushions the jaw joints and muscles.
- Non-invasive: Easily removable.
- Custom-fit: Superior comfort and effectiveness compared to over-the-counter options. Cons:
- Cost: More expensive than over-the-counter options.
- Adjustment period: May feel bulky initially.
- Maintenance: Requires regular cleaning.
- Doesn't cure bruxism: Manages symptoms, but doesn't address the root cause. Process: Your dentist will take impressions of your teeth, which are then sent to a dental lab to fabricate the custom appliance. You'll return for a fitting appointment to ensure proper comfort and bite alignment. Cost: Custom nightguards typically range from $300 to $800, depending on the material and complexity, and can last 1 to 5 years. Insurance may cover a portion. Pro Tip: While readily available, over-the-counter (boil-and-bite) mouthguards offer only limited protection and can sometimes worsen bite issues. Always consult your dentist for a custom-fit appliance.
2. Behavioral Therapies and Stress Management
Since stress and anxiety are major contributors to bruxism, addressing these factors is crucial. Methods:
- Stress Reduction Techniques: Yoga, meditation, deep breathing exercises, mindfulness, progressive muscle relaxation.
- Counseling/Therapy: Cognitive-behavioral therapy (CBT) can help identify and modify stressful thought patterns.
- Biofeedback: Devices that monitor jaw muscle activity and provide sensory feedback (e.g., sound) to help you learn to relax your jaw muscles.
- Awareness Training: For awake bruxism, consciously repositioning your jaw throughout the day, keeping your teeth apart. Pros:
- Addresses root cause: Can lead to long-term reduction in bruxism.
- Improves overall well-being: Benefits extend beyond bruxism.
- Non-pharmacological: Few side effects. Cons:
- Requires commitment: Effectiveness depends on consistent practice.
- May take time: Results are not immediate.
- Cost: Therapy sessions can range from $75-$200 per hour and may not be covered by dental insurance.
3. Medications
Medications are generally used as a short-term solution for severe bruxism or when other treatments haven't been effective. Types:
- Muscle Relaxants: Prescribed for a limited period to relax jaw muscles, especially before bedtime. (e.g., cyclobenzaprine).
- Botulinum Toxin (Botox): Injections into the masseter muscles (jaw muscles) can temporarily weaken them, reducing clenching force. This is not approved by the FDA specifically for bruxism, but it is a widely used off-label treatment.
- Antidepressants/Anxiolytics: In some cases, if bruxism is strongly linked to severe anxiety or depression, a physician might adjust existing medications or prescribe new ones. However, some antidepressants can cause bruxism, so careful consideration is needed. Pros:
- Rapid relief: Especially for muscle relaxants and Botox.
- Targeted relief: Botox specifically targets the jaw muscles. Cons:
- Temporary: Effects wear off, requiring repeat treatments.
- Side effects: Drowsiness, dry mouth (muscle relaxants); temporary facial weakness, asymmetry (Botox).
- Doesn't address underlying cause: Symptoms return if medication is stopped.
- Cost of Botox: $300-$600 per treatment, lasting 3-6 months. Usually not covered by dental insurance; may be covered by medical insurance if deemed medically necessary (e.g., for severe TMJ pain).
4. Dental Corrections
If malocclusion (misaligned bite) or specific dental issues are identified as significant contributing factors, your dentist may recommend corrective procedures. Methods:
- Occlusal Adjustment: Minor reshaping of tooth surfaces (selective grinding) to improve bite alignment.
- Restorations: Replacing worn or damaged teeth with crowns, onlays, or fillings to restore proper bite.
- Orthodontics: Braces or clear aligners to correct significant bite discrepancies or crowded teeth. Pros:
- Permanent solution: Addresses structural issues.
- Improves overall oral health: Enhances chewing function and aesthetics. Cons:
- Invasive: May involve permanent alteration of tooth structure.
- Time-consuming: Orthodontics can take months to years.
- Cost: Varies widely. Occlusal adjustment: $50-$300. Crowns: $800-$2,500 per tooth. Orthodontics: $3,000-$8,000+. Pro Tip: Dental corrections are usually considered after other conservative treatments have been tried, as bite issues are rarely the sole cause of bruxism. The ADA recommends careful consideration before irreversible occlusal adjustments for bruxism.
5. Treating Underlying Sleep Disorders
If sleep apnea is suspected, a sleep study (polysomnography) will be recommended. Methods:
- CPAP (Continuous Positive Airway Pressure) therapy: For sleep apnea, a device that keeps airways open during sleep.
- Oral Appliance Therapy (OAT): Custom dental devices that reposition the jaw to keep the airway open. Pros:
- Addresses a major cause: Can significantly reduce or eliminate bruxism associated with sleep apnea.
- Improves overall health: Better sleep quality, reduced risk of cardiovascular issues. Cons:
- Requires diagnosis: Needs a sleep study.
- Compliance: CPAP can be uncomfortable for some.
- Cost: Sleep studies $500-$5,000+ (in-lab vs. home test). CPAP machine $500-$3,000. Oral appliances for OSA $1,800-$3,500. Usually covered by medical insurance.
6. Physical Therapy and Self-Care (Massage for Jaw Clenching)
Physical therapy can be beneficial for alleviating jaw pain and improving muscle function. Self-care practices are vital for daily management. Methods:
- Therapeutic exercises: Stretches and strengthening exercises for jaw muscles.
- Manual therapy: Gentle massage and mobilization of jaw joints and muscles by a physical therapist.
- Heat/Cold Therapy: Applying warm compresses to the jaw can relax muscles; cold packs can reduce inflammation.
- Soft Diet: Temporarily avoid hard, chewy foods to rest the jaw.
- Massage for Jaw Clenching:
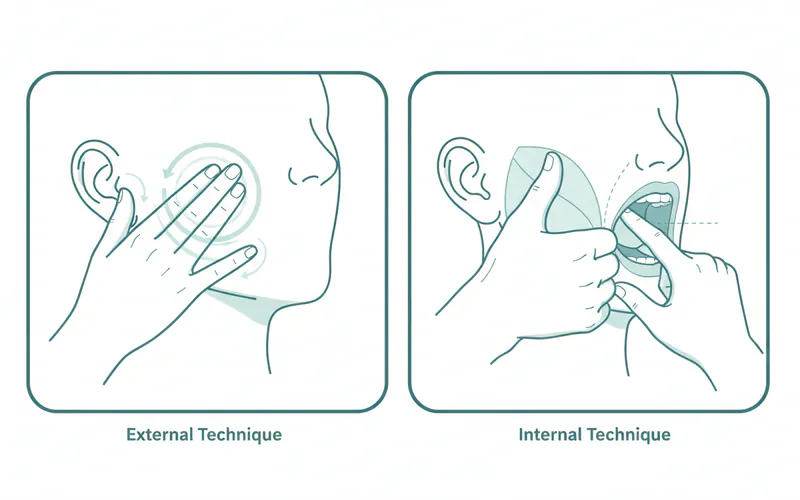
- External Massage: Use your fingers to gently massage the masseter muscles (on the sides of your jaw, just below your cheekbones) in a circular motion. You can also massage your temples and neck.
- Internal Massage (Intraoral): With clean hands, place your thumb inside your mouth against your cheek and your index finger on the outside of your cheek. Gently massage the jaw muscles from both sides, especially focusing on tender spots. This can provide significant relief for tight muscles. Perform these massages for 5-10 minutes before bed. Pros:
- Non-invasive and drug-free: Natural pain relief.
- Empowering: Gives you tools to manage symptoms.
- Cost-effective: Self-care is free. Physical therapy: $75-$200 per session, often covered by medical insurance. Cons:
- Requires consistency: Must be done regularly for results.
- May not address root cause: Primarily symptom management.
Comparison Table: Treatment Options for Bruxism
| Treatment Option | Primary Function | Typical Cost (US, without insurance) | Duration/Longevity | Pros | Cons |
|---|---|---|---|---|---|
| Custom Nightguard | Protects teeth, reduces jaw strain | $300 - $800 | 1-5 years | Highly effective for protection, non-invasive | Doesn't cure cause, requires maintenance |
| Behavioral Therapy/CBT | Addresses stress/anxiety, promotes relaxation | $75 - $200 per session | Ongoing as needed | Addresses root cause, improves overall well-being | Requires commitment, results take time |
| Botox Injections | Weakens jaw muscles, reduces clenching force | $300 - $600 per treatment | 3-6 months | Quick symptom relief, non-surgical | Temporary, potential side effects, not FDA-approved for bruxism |
| Occlusal Adjustment | Corrects minor bite discrepancies | $50 - $300 | Permanent | Permanent correction of specific bite issues | Irreversible, rarely a sole solution |
| Orthodontics | Corrects major bite problems, realigns teeth | $3,000 - $8,000+ | Permanent (with retainers) | Comprehensive bite correction | High cost, long treatment time |
| Sleep Apnea Treatment | Addresses underlying sleep breathing issues | $500 - $5,000+ (diagnosis) | Ongoing | Resolves a major bruxism cause, improves sleep | Requires diagnosis, potential compliance issues |
| Physical Therapy/Massage | Alleviates jaw pain, improves muscle function | $75 - $200 per session (PT) | Ongoing self-care | Non-invasive, empowering, immediate relief | Primarily symptom management |
Step-by-Step Process: What to Expect During Bruxism Treatment
The journey to effectively stop teeth grinding at night typically involves several steps, starting with diagnosis and leading to a tailored treatment plan.
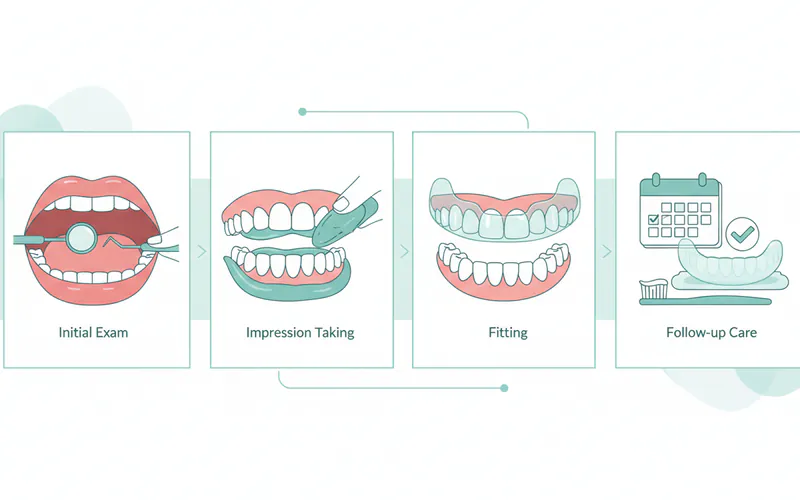
Step 1: Initial Consultation and Diagnosis (1-2 Appointments)
- Your Role: Describe your symptoms (jaw pain, headaches, tooth sensitivity), any noises heard by a sleep partner, and relevant lifestyle factors (stress, medication, caffeine intake).
- Dentist's Role:
- Oral Examination: Look for signs of bruxism, such as worn tooth enamel, chips, fractures, abfractions, tongue indentations, or cheek biting marks.
- Jaw and Muscle Palpation: Feel your jaw joints and muscles for tenderness, clicking, or limited movement.
- Bite Analysis: Assess your bite for any significant misalignments.
- X-rays: May be taken to check for bone damage or other dental issues.
- Discussion of Medical History: Inquire about sleep habits, stress levels, medications, and any other health conditions.
- Outcome: Your dentist will diagnose bruxism and discuss potential contributing factors. They may recommend further evaluation (e.g., a sleep study for suspected sleep apnea) or move directly to treatment options.
Step 2: Custom Nightguard Fabrication (1-2 Appointments) - If Recommended
- Impression Taking: Your dentist will take precise molds (impressions) of your upper and lower teeth.
- Lab Work: These impressions are sent to a dental lab where a skilled technician fabricates your custom nightguard, often from durable acrylic, ensuring a precise fit. This typically takes 1-2 weeks.
- Fitting and Adjustment: You'll return to the office to try on the nightguard. Your dentist will ensure it fits comfortably, doesn't interfere with your bite, and make any necessary minor adjustments.
- Instructions: You'll receive detailed instructions on how to wear, clean, and care for your nightguard.
- Outcome: You'll have a protective device to wear at night, which helps prevent tooth damage and reduce jaw pain.
Step 3: Addressing Underlying Causes (Ongoing)
- Stress Management: If stress is a significant factor, your dentist may recommend techniques like meditation apps, counseling, or lifestyle changes. This is an ongoing self-management process.
- Medication Review: If you're taking medications known to cause bruxism, your dentist might consult with your prescribing physician about potential alternatives or dosage adjustments. Never stop medication without consulting your doctor.
- Sleep Study (If Suspected Sleep Apnea): If sleep apnea is suspected, you'll be referred to a sleep specialist for a sleep study. If diagnosed, treatment (e.g., CPAP, oral appliance) will begin.
- Physical Therapy/Self-Care: Learn and practice jaw exercises and self-massage techniques. This can be done daily at home.
Step 4: Follow-up and Adjustment (Regular Appointments)
- Regular Dental Check-ups: Your dentist will monitor your teeth for further wear, assess the effectiveness of your nightguard, and check for improvements in jaw pain.
- Nightguard Maintenance: Your nightguard may need occasional adjustments or replacement after several years.
- Treatment Plan Modifications: Based on your progress and symptom relief, your dentist may recommend further treatments or adjustments to your current plan.
This step-by-step process ensures a holistic approach to managing bruxism, aiming not just for symptom relief but also addressing its root causes for long-term oral health and comfort.
Cost and Insurance: Navigating Bruxism Treatment Expenses
The cost of treating bruxism varies significantly based on the severity of the condition, the chosen treatment methods, your geographic location, and your insurance coverage. Understanding these factors is key to planning your care.
Average US Cost Ranges (Without Insurance)
| Treatment Type | Low End (USD) | Mid Range (USD) | High End (USD) | Notes |
|---|---|---|---|---|
| Initial Consultation & Exam | $50 | $150 | $300 | Includes X-rays, diagnosis. |
| Custom Nightguard (Occlusal Splint) | $300 | $550 | $800 | Varies by material (hard vs. soft), lab fees. |
| Over-the-Counter Mouthguard | $20 | $40 | $80 | Boil-and-bite; not custom-fit, less effective/protective. |
| Botox Injections (for Masseters) | $300 | $450 | $600 | Per treatment cycle, typically 3-6 months. Price per unit. |
| Occlusal Adjustment (Minor) | $50 | $150 | $300 | Selective grinding of few teeth. |
| Orthodontics (Braces/Aligners) | $3,000 | $5,500 | $8,000+ | Comprehensive treatment for severe bite issues. |
| Sleep Study (Home) | $500 | $1,000 | $1,500 | For suspected sleep apnea diagnosis. |
| Sleep Study (In-Lab Polysomnography) | $2,000 | $3,500 | $5,000+ | More comprehensive, often required by insurance. |
| CPAP Machine (for Sleep Apnea) | $500 | $1,500 | $3,000 | Ongoing mask and supply costs. |
| Oral Appliance Therapy (for OSA) | $1,800 | $2,500 | $3,500 | Custom-made device to manage sleep apnea. |
| Physical Therapy (per session) | $75 | $120 | $200 | Multiple sessions often required. |
| Counseling/CBT (per session) | $75 | $130 | $200 | If stress/anxiety is a major factor. |
Geographic Variation: Costs can fluctuate significantly between urban and rural areas, and different regions of the US. Major metropolitan areas (e.g., New York, Los Angeles) generally have higher costs.
Insurance Coverage Details
Navigating insurance for bruxism treatment can be complex, as different treatments may fall under dental or medical plans.
-
Dental Insurance:
- Nightguards: Many dental insurance plans offer partial coverage for custom nightguards (occlusal splints), often covering 50-80% of the cost after your deductible. You may need to meet a waiting period. Over-the-counter mouthguards are typically not covered.
- Dental Corrections: Fillings, crowns, and occlusal adjustments are usually covered by dental insurance at varying percentages (e.g., 80% for basic, 50% for major procedures).
- Orthodontics: Some plans include orthodontic benefits, but often with age limits or lifetime maximums.
-
Medical Insurance:
- Diagnosis: Initial consultations with a dentist might be covered if filed under medical, especially if it leads to a medical diagnosis like TMJ disorder.
- Sleep Studies & Sleep Apnea Treatment: If bruxism is linked to sleep apnea, diagnostic sleep studies, CPAP machines, and oral appliance therapy for OSA are typically covered by medical insurance, subject to deductibles and co-pays.
- Botox Injections: While often considered cosmetic, if Botox is prescribed by a medical doctor (e.g., neurologist, pain specialist) for severe TMJ pain or headaches associated with bruxism, it might be covered by medical insurance if deemed medically necessary and prior authorization is obtained. Dental insurance rarely covers Botox.
- Physical Therapy/Counseling: If prescribed by a physician as part of a treatment plan for TMJ disorder or stress, these might be covered by medical insurance.
Pro Tip for Insurance: Always contact your dental and medical insurance providers before starting treatment to understand your specific benefits, deductibles, co-pays, and any pre-authorization requirements. Ask for procedure codes (CDT codes for dental, CPT codes for medical) from your dentist to verify coverage accurately.
Payment Plans and Financing Options
If insurance coverage is limited or unavailable, several options can help manage costs:
- In-Office Payment Plans: Many dental offices offer installment plans, allowing you to pay for treatment over several months.
- Third-Party Financing: Companies like CareCredit or LendingClub offer specialized healthcare credit cards with deferred interest options if paid within a certain period.
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): These tax-advantaged accounts allow you to set aside pre-tax money for qualified medical and dental expenses.
- Dental Schools: University dental schools often provide services at a reduced cost, with treatment performed by students under the supervision of experienced faculty.
Recovery and Aftercare for Bruxism Management
Managing bruxism is often an ongoing process, and successful long-term outcomes depend heavily on consistent aftercare and adherence to recommended strategies.

After Nightguard Fitting:
- Adjustment Period (1-2 Weeks): It's common to experience some initial discomfort, increased salivation, or a feeling of bulkiness when you first start wearing your nightguard. This usually subsides as your mouth adjusts.
- Consistency is Key: Wear your nightguard every night, as instructed by your dentist, even if you don't feel active symptoms. Sporadic use can reduce its effectiveness.
- Cleaning and Maintenance:
- Daily: After each use, rinse your nightguard with cool water and brush it with a soft toothbrush and non-abrasive soap or a denture cleaner. Avoid hot water, which can warp the material.
- Weekly/Bi-weekly: Soak it in a specialized nightguard cleaning solution (available at pharmacies or from your dentist) to kill bacteria and prevent odors.
- Storage: Store it in its protective case when not in use to keep it clean and prevent damage.
- Regular Dental Check-ups: Bring your nightguard to every dental appointment. Your dentist will check its fit, assess for wear, and ensure your bite remains stable. They may need to make minor adjustments over time. A nightguard can last from 1 to 5 years or more, depending on the material and severity of grinding.
Post-Botox Injections (If Applicable):
- Immediate Aftercare: Avoid rubbing or massaging the injection sites for 24 hours to prevent the Botox from spreading to unintended muscles. Avoid strenuous exercise for the rest of the day.
- Onset of Effect: You may start to feel the effects (reduced clenching) within 3-7 days, with full effect usually seen in 2 weeks.
- Duration: The effects typically last 3-6 months. Plan for repeat injections as symptoms return.
- Monitoring: Report any unusual side effects (e.g., difficulty chewing, asymmetrical smile) to your provider.
Lifestyle and Behavioral Aftercare:
- Continued Stress Management: Implement stress-reduction techniques (meditation, exercise, hobbies) into your daily routine. This is a lifelong commitment.
- Mindfulness for Awake Bruxism: If you also clench during the day, regularly check in with your jaw position. Keep your teeth slightly apart, with your tongue resting gently on the roof of your mouth.
- Dietary Modifications: Continue to avoid or reduce stimulants like caffeine and alcohol, especially in the hours leading up to bedtime. Avoid hard, chewy foods if your jaw is sore.
- Jaw Exercises and Massage for Jaw Clenching: Continue to perform gentle jaw stretches and massages, particularly before bedtime. This helps relax the muscles and can significantly contribute to reducing nighttime tension. Focus on the masseter and temporalis muscles.
- Sleep Hygiene: Maintain a consistent sleep schedule, create a dark and quiet sleep environment, and avoid screens before bed. Good sleep hygiene can positively impact bruxism, especially if it's linked to sleep disturbances.
Effective recovery and aftercare are integral to successfully stopping teeth grinding at night and maintaining a healthy, comfortable smile. It’s a partnership between you and your dental care team.
Prevention: Proactive Steps to Not Grind Teeth at Night
While some causes of bruxism, like genetics, are beyond your control, many contributing factors can be managed or prevented through proactive lifestyle changes and awareness. The goal is to reduce stress, improve sleep quality, and protect your oral structures.
-
Manage Stress and Anxiety:
- Identify Triggers: Become aware of what situations or thoughts lead to increased tension and stress in your life.
- Relaxation Techniques: Incorporate daily relaxation practices such as yoga, meditation, deep breathing exercises, or progressive muscle relaxation. Even 10-15 minutes a day can make a difference.
- Regular Exercise: Physical activity is a powerful stress reliever. Aim for at least 30 minutes of moderate exercise most days of the week.
- Hobbies and Downtime: Engage in enjoyable activities that help you unwind and detach from daily pressures.
- Professional Help: If stress and anxiety are overwhelming, consider counseling or cognitive-behavioral therapy (CBT) to develop healthier coping mechanisms.
-
Practice Good Sleep Hygiene:
- Consistent Sleep Schedule: Go to bed and wake up at the same time every day, even on weekends, to regulate your body's natural sleep-wake cycle.
- Comfortable Sleep Environment: Ensure your bedroom is dark, quiet, and cool.
- Avoid Stimulants Before Bed: Refrain from caffeine, nicotine, and alcohol several hours before sleep. Alcohol might initially make you feel drowsy, but it disrupts sleep architecture later in the night.
- Limit Screen Time: Avoid electronic devices (phones, tablets, computers, TVs) for at least an hour before bed, as the blue light can interfere with melatonin production.
- Relaxing Bedtime Routine: Take a warm bath, read a book, or listen to calming music to signal to your body that it's time to wind down.
-
Adjust Your Diet and Habits:
- Reduce Stimulant Intake: Minimize consumption of caffeine and nicotine throughout the day, especially in the afternoon and evening.
- Limit Alcohol: Excessive alcohol intake can worsen sleep quality and bruxism.
- Stay Hydrated: Dehydration can sometimes contribute to muscle cramps and tension.
- Avoid Chewing Non-Food Items: Don't chew on pens, pencils, ice, or your fingernails, as these habits can train your jaw muscles for clenching.
- Chew Gum Sparingly: While gum can temporarily relieve jaw tension for some, excessive gum chewing can actually overwork and tire your jaw muscles, potentially exacerbating bruxism.
-
Practice Jaw Awareness and Relaxation:
- "Lips Together, Teeth Apart": Make a conscious effort to keep your teeth from touching throughout the day. Your lips should be gently closed, but your teeth should be slightly separated, with your tongue resting lightly on the roof of your mouth.
- Regular Jaw Stretches: Gently stretch your jaw muscles throughout the day. Simple exercises like slowly opening and closing your mouth or moving your jaw side-to-side can help maintain flexibility.
- Self-Massage: Incorporate massages for jaw clenching into your daily routine, particularly before bed. Gently massage your temples, cheeks (masseter muscles), and neck.
-
Address Underlying Medical Conditions:
- Screen for Sleep Apnea: If you snore loudly, experience daytime fatigue, or have witnessed breathing pauses during sleep, talk to your doctor about a sleep study. Treating sleep apnea can significantly reduce bruxism.
- Medication Review: If you suspect a medication is contributing to your bruxism, discuss it with your prescribing doctor. Do not stop taking any medication without professional guidance.
By integrating these preventive measures into your daily life, you can significantly reduce the likelihood and severity of nighttime teeth grinding, protecting your smile and promoting overall well-being.
Risks and Complications of Untreated Bruxism
Ignoring teeth grinding can lead to a cascade of painful and potentially irreversible problems for your oral health and overall physical comfort. The constant, excessive force exerted on your teeth and jaw can have serious long-term consequences.
Dental and Oral Complications:
- Severe Tooth Wear and Damage:
- Enamel Erosion: The outermost layer of your teeth can be worn down, exposing the softer dentin underneath, leading to increased sensitivity and a yellowish appearance.
- Chipped, Fractured, or Cracked Teeth: The immense pressure can cause parts of your teeth to break off, or even lead to hairline cracks that compromise the tooth's structural integrity.
- Loose Teeth: Chronic clenching and grinding can damage the periodontal ligaments and supporting bone, leading to tooth mobility.
- Loss of Teeth: In extreme, long-standing cases, teeth can become so damaged or loose that they need to be extracted.
- Damage to Dental Restorations: Existing fillings, crowns, bridges, and even dental implants can be fractured, loosened, or completely destroyed by grinding forces, requiring costly replacements.
- Hypersensitivity: Worn enamel exposes dentin, which contains microscopic tubules leading to the tooth's nerve. This can cause significant sensitivity to hot, cold, sweet, or acidic foods and drinks.
- Gum Recession: Grinding forces can contribute to the breakdown of gum tissue and supporting bone around the teeth, leading to gum recession and exposure of tooth roots.
Temporomandibular Joint (TMJ) Disorders:
- Pain and Tenderness: The most common complication, affecting the jaw joints (TMJ) and the muscles that control jaw movement.
- Clicking, Popping, or Grating Sounds: As the joint disc becomes displaced or damaged.
- Limited Jaw Movement: Difficulty opening or closing the mouth fully, or the jaw locking in an open or closed position.
- Ear Pain: Often misdiagnosed as an ear infection, as pain can radiate from the TMJ to the ear area.
Facial and Other Body Pain:
- Chronic Headaches: Especially tension-type headaches, often concentrated in the temples and forehead, prevalent upon waking.
- Neck and Shoulder Pain: The tension can extend beyond the jaw muscles, affecting adjacent muscle groups in the neck and shoulders.
- Facial Muscle Hypertrophy: The masseter muscles can become visibly enlarged and contribute to a squarer facial appearance.
- Sleep Disturbances: Not only can the grinding noises disturb a sleep partner, but the physiological stress of clenching can also impact the quality of the bruxer's own sleep, leading to daytime fatigue.
Psychological Impact:
- Increased Stress and Anxiety: The constant pain and discomfort from bruxism can create a vicious cycle, increasing stress, which in turn can worsen grinding.
- Reduced Quality of Life: Chronic pain and sleep disruption can severely impact daily activities, mood, and overall well-being.
The American Dental Association (ADA) emphasizes that early diagnosis and intervention are critical to mitigate these risks. If you suspect you grind your teeth, seeking professional dental advice promptly can save you from significant pain, extensive dental work, and long-term health complications.
Children and Pediatric Considerations
Bruxism is surprisingly common in children, affecting an estimated 15-20% of children, typically between the ages of 3 and 12. While it can be alarming for parents to hear grinding noises from their child's bedroom, pediatric bruxism is often benign and self-resolving.
Why Children Grind Their Teeth:
- Growth and Development: As children's jaws and teeth are still developing, they may grind as their baby teeth erupt, their permanent teeth come in, or as their bite adjusts.
- Stress and Anxiety: Similar to adults, stress from school, new siblings, changes at home, or even exciting events can manifest as grinding.
- Allergies/Illness: Nasal congestion, ear infections, or allergies can make it harder for children to breathe at night, leading to jaw adjustments and grinding.
- Malocclusion: While not the sole cause, misaligned teeth or a poor bite can sometimes contribute.
- Hyperactivity: Children with ADHD may have a higher incidence of bruxism.
- Sleep Disorders: Though less common than in adults, sleep apnea can also occur in children and may be linked to grinding.
Signs and Symptoms in Children:
The signs are similar to adults but parents should look for:
- Grinding noises during sleep.
- Complaints of jaw pain or soreness in the morning.
- Headaches upon waking.
- Tooth sensitivity (though children may not always articulate this clearly).
- Visible wear on primary (baby) teeth.
When to Be Concerned:
Most pediatric bruxism resolves on its own by age 12-13, particularly after all permanent teeth have erupted. However, consult a pediatric dentist if:
- Your child complains of persistent jaw pain or headaches.
- Their teeth show significant wear or damage.
- Their grinding is extremely loud or disrupts their sleep.
- You notice other sleep-related issues like snoring or gasping for breath (which could indicate sleep apnea).
Treatment and Management for Children:
- Observation: In most cases, the dentist will recommend monitoring the situation.
- Stress Management: Help your child identify and manage stressors. Ensure they have a relaxing bedtime routine.
- Address Underlying Issues: Treat allergies, colds, or ear infections.
- Nightguards: Custom nightguards are rarely recommended for young children due to their changing dentition. They might be considered for older children or adolescents with severe, damaging bruxism after permanent teeth have fully erupted. The cost for a pediatric nightguard is similar to adult versions, ranging from $300-$700.
- Orthodontic Consultation: If malocclusion is significant and persistent, an orthodontic evaluation may be recommended.
The primary goal in children is to protect developing teeth and ensure comfortable, healthy growth. A pediatric dentist is best equipped to guide parents through concerns about their child's teeth grinding.
Frequently Asked Questions About Stopping Teeth Grinding at Night
How can I stop teeth grinding at night naturally?
Natural approaches focus on stress reduction and jaw relaxation. Try daily meditation, deep breathing exercises, yoga, or progressive muscle relaxation before bed. Applying warm compresses to your jaw, performing gentle jaw stretches, and massaging your jaw muscles (external and internal massages for jaw clenching) can help. Avoiding stimulants like caffeine and alcohol, especially in the evening, also contributes to natural relief.
Do mouthguards really work for teeth grinding?
Yes, custom-fitted nightguards (occlusal splints) are highly effective. They don't stop the grinding itself but act as a protective barrier between your upper and lower teeth, preventing damage and distributing the forces of clenching more evenly, which reduces jaw pain and protects your teeth from wear and fractures.
Is there a specific massage for jaw clenching that I can do at home?
Absolutely. For external massage, use your fingertips to gently rub your masseter muscles (sides of your jaw below cheekbones) and your temporalis muscles (temples) in circular motions for 5-10 minutes. For internal massage, wash your hands thoroughly, then place your thumb inside your mouth against your cheek and your index finger on the outside. Gently pinch and rub the tight muscle areas.
How much does it cost to stop teeth grinding at night?
The cost varies widely based on treatment. A custom nightguard typically costs $300-$800 without insurance. Botox injections range from $300-$600 per treatment. Addressing underlying sleep apnea can involve sleep studies ($500-$5,000+) and CPAP or oral appliances ($500-$3,500). Lifestyle changes like stress management are generally low-cost or free.
Can teeth grinding be cured permanently?
A complete "cure" for bruxism is challenging, as it often has multiple contributing factors. However, effective management and reduction of symptoms are highly achievable. Addressing underlying causes like stress, sleep disorders, or bite issues, combined with protective appliances and behavioral changes, can lead to long-term relief and prevent irreversible damage.
What are the dangers of not treating teeth grinding?
Untreated bruxism can lead to severe tooth wear, chipping, and fractures, often requiring extensive and costly dental work like crowns or extractions. It can also cause chronic jaw pain, headaches, TMJ disorders (clicking, locking jaw), gum recession, and muscle hypertrophy, significantly impacting your quality of life.
Can stress relief really help stop teeth grinding?
Yes, stress relief is one of the most crucial components in managing bruxism. High levels of stress and anxiety are primary triggers for both awake and sleep bruxism. By effectively reducing stress through various techniques, you can significantly lessen the intensity and frequency of clenching and grinding episodes.
Will my insurance cover the cost of a nightguard?
Many dental insurance plans cover a portion of the cost for a custom nightguard (occlusal splint), typically 50-80% after your deductible. However, coverage varies widely, so it's essential to check with your specific insurance provider for details on your plan's benefits, waiting periods, and any pre-authorization requirements.
How long does it take to see results from bruxism treatment?
Results vary. A nightguard offers immediate physical protection and often provides quick relief from jaw pain upon waking. Behavioral changes and stress management techniques may take several weeks to months of consistent practice to show significant improvement. Botox typically takes about 2 weeks for full effect.
Are over-the-counter mouthguards effective?
Over-the-counter boil-and-bite mouthguards offer minimal protection compared to custom-fitted nightguards. They can provide a temporary barrier but are often ill-fitting, uncomfortable, and may even shift your bite over time. For serious bruxism, a custom nightguard from your dentist is always recommended for safety and effectiveness.
When to See a Dentist
While occasional jaw tension might not be a cause for immediate alarm, persistent symptoms related to teeth grinding warrant a professional evaluation. Early intervention is key to preventing long-term damage and more complex, expensive treatments.
You should make an appointment to see your dentist if you experience any of the following:
- Persistent Jaw Pain or Tenderness: If you wake up regularly with a sore jaw, pain around your ears, or difficulty opening your mouth wide.
- Frequent Headaches: Especially dull headaches that start in your temples or jaw area and are present upon waking.
- Noticeable Tooth Sensitivity: If your teeth become increasingly sensitive to hot, cold, or sweet foods and drinks.
- Visible Tooth Damage: If you notice that your teeth are visibly flattened, chipped, cracked, or if your dental fillings or crowns are frequently breaking.
- Clicking or Popping in Your Jaw: Sounds when you open or close your mouth, which could indicate a temporomandibular joint (TMJ) disorder.
- Your Sleep Partner Reports Grinding Noises: If a spouse or family member mentions that they hear you grinding your teeth at night.
- Unexplained Facial Pain: Persistent discomfort in your facial muscles that isn't attributable to other causes.
- Concerns about Your Child: If your child complains of jaw pain or headaches, or you notice significant wear on their teeth, especially if accompanied by other sleep issues like snoring.
Red Flags (Seek prompt attention):
- Acute, severe jaw pain that limits your ability to eat or speak.
- A jaw that locks open or closed and cannot be easily returned to normal position.
- Sudden, unexplained changes in your bite or difficulty bringing your teeth together.
While some self-help measures can offer temporary relief, a dental professional can accurately diagnose the extent of the problem, identify potential underlying causes, and recommend the most effective, personalized treatment plan to help you stop teeth grinding at night and protect your smile for years to come.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles

What Causes Teeth Grinding in Sleep
More than one in ten adults—and even more children—clench or grind their teeth during sleep, a condition known medically as sleep bruxism. For many, it's an unconscious habit that goes unnoticed until significant damage or discomfort arises. Waking up with a dull, constant headache, jaw pain, or
February 23, 2026

What Is Jaw Clenching
Do you often wake up with a dull headache, a sore jaw, or unexplained tooth sensitivity? You're not alone. Approximately 1 in 10 adults and up to 3 in 10 children experience some form of bruxism, a condition characterized by grinding, gnashing, or clenching your teeth. At the heart of this wides
February 23, 2026
Severe Bruxism Molars: Complete Guide
When the quiet of the night is shattered by a grinding, grating sound, or when you wake up with an aching jaw and teeth that feel oddly sensitive, it’s often a sign of bruxism. But what happens when this condition intensifies, leading to significant damage, especially to your back teeth? This is the
February 23, 2026

How to Prevent Teeth Grinding in Sleep
Teeth grinding, medically known as bruxism, is a common condition that affects millions of Americans. Often occurring subconsciously during sleep, it can lead to a host of uncomfortable and potentially serious health issues, ranging from persistent headaches and jaw pain to significant dental damage
February 23, 2026