How to Prevent Teeth Grinding in Sleep

Key Takeaways
- Teeth grinding, medically known as bruxism, is a common condition that affects millions of Americans. Often occurring subconsciously during sleep, it can lead to a host of uncomfortable and potentially serious health issues, ranging from persistent headaches and jaw pain to significant dental damage
Teeth grinding, medically known as bruxism, is a common condition that affects millions of Americans. Often occurring subconsciously during sleep, it can lead to a host of uncomfortable and potentially serious health issues, ranging from persistent headaches and jaw pain to significant dental damage. If you've ever woken up with a sore jaw, unexplained headaches, or noticed your teeth appear flattened, you might be wondering how to prevent teeth grinding in sleep. This comprehensive guide from SmilePedia.net will delve into the intricacies of bruxism, exploring its causes, symptoms, and, most importantly, effective strategies and treatments to protect your smile and overall well-being. We'll cover everything from simple lifestyle adjustments to advanced dental interventions, ensuring you have the knowledge to take control of your nocturnal habits and safeguard your dental health.
Key Takeaways:
- Prevalence: Approximately 10-15% of adults and up to 30% of children experience sleep bruxism.
- Common Causes: Stress, anxiety, sleep disorders (like sleep apnea), certain medications, and lifestyle factors (caffeine, alcohol) are primary contributors.
- Primary Treatment: Custom-fitted nightguards are often the first line of defense, costing $300-$800 (or more for specialized designs) and lasting 1-5 years. Over-the-counter options are less effective and cost $20-$100.
- Beyond Nightguards: Stress management techniques, biofeedback, Botox injections (costing $300-$1,000 per treatment, lasting 3-6 months), and addressing underlying sleep disorders are crucial for long-term prevention.
- Dental Damage: Unmanaged bruxism can lead to tooth wear, fractures, gum recession, and temporomandibular joint (TMJ) disorders, potentially requiring extensive dental work costing thousands of dollars.
- Headache Connection: Can teeth grinding cause headaches? Absolutely. Muscle tension from clenching is a significant cause of tension-type headaches and migraines.
- Actionable Step: If you suspect you grind your teeth, schedule an appointment with your dentist promptly for diagnosis and personalized prevention strategies.
What It Is: Understanding Bruxism (Teeth Grinding)
Bruxism (teeth grinding) refers to the habitual clenching, grinding, or gnashing of teeth, typically without conscious awareness. While some people experience bruxism during waking hours (awake bruxism), the more common and often more damaging form occurs involuntarily during sleep (sleep bruxism). It's a sleep-related movement disorder that can exert tremendous force on your teeth, jaw, and surrounding muscles, far exceeding the forces generated during chewing.
The impact of sleep bruxism can be insidious, slowly eroding tooth enamel, flattening chewing surfaces, and even fracturing teeth over time. Because it happens while you're asleep, many individuals are unaware they have the condition until a dental professional points out the characteristic signs during a routine check-up, or a sleeping partner complains about the grinding noises. Understanding this often-invisible habit is the first step toward effective prevention and treatment.
![A person sleeping with a subtle overlay of jaw(/glossary/glossary-jaw) clenching/grinding]
Types of Bruxism: Awake vs. Sleep
Bruxism isn't a single condition but rather a spectrum of habits that manifest in different ways. Recognizing the specific type you experience can help in tailoring the most effective prevention strategies.
Awake Bruxism
Awake bruxism involves clenching or grinding your teeth while you are conscious. This often happens in response to stress, anxiety, concentration, or even just out of habit. Unlike sleep bruxism, individuals with awake bruxism can often learn to control it through conscious effort, biofeedback, and stress-reduction techniques once they become aware of the habit. It typically involves clenching rather than grinding, and while it can cause muscle tension and headaches, it generally results in less severe tooth wear than its nocturnal counterpart.
Sleep Bruxism
Sleep bruxism is the involuntary clenching or grinding of teeth during sleep. It's classified as a sleep-related movement disorder and is often associated with other sleep disturbances, such as sleep apnea. Because it occurs during an unconscious state, the forces exerted can be significantly higher and prolonged, leading to more extensive dental damage, jaw pain, and other systemic issues. Individuals may cycle through episodes of grinding throughout the night, often during transitions between sleep stages.
Primary vs. Secondary Bruxism
- Primary Bruxism: This type has no identifiable underlying medical cause. It's often linked to psychological factors like stress and anxiety, or genetic predisposition.
- Secondary Bruxism: This occurs as a side effect of another condition, medication, or substance. Examples include certain antidepressant medications (e.g., SSRIs), neurological disorders (e.g., Parkinson's disease), or substance use (e.g., caffeine, alcohol, tobacco).
Why It Happens: Root Causes and Contributing Factors
Understanding the various factors that contribute to bruxism is crucial for effective prevention. It's rarely a single cause but rather a complex interplay of physical, psychological, and lifestyle elements.
1. Psychological Factors
- Stress and Anxiety: This is arguably the most common culprit. High levels of daily stress, anxiety, frustration, or anger can manifest as teeth clenching or grinding, especially during sleep when the body processes tension.
- Personality Type: Some studies suggest that individuals with competitive, aggressive, or hyperactive personality traits may be more prone to bruxism.
2. Sleep-Related Factors
- Sleep Apnea and Other Sleep Disorders: There's a strong correlation between sleep bruxism and obstructive sleep apnea (OSA). The body may clench or grind in an attempt to open the airway during apneic episodes. Other sleep disturbances like snoring, restless leg syndrome, and periodic limb movement disorder can also contribute.
- Sleep Position: While less definitive, some research suggests certain sleep positions might influence bruxism.
3. Medications and Substances
- Antidepressants (SSRIs): Selective serotonin reuptake inhibitors (SSRIs) like Prozac, Zoloft, and Paxil, while effective for depression and anxiety, can sometimes increase bruxism as a side effect.
- Stimulants: Amphetamines and other stimulants used for ADHD or narcolepsy can heighten jaw clenching.
- Caffeine: High intake of caffeine, especially close to bedtime, acts as a stimulant and can contribute to muscle hyperactivity.
- Alcohol: While alcohol might initially feel relaxing, it disrupts normal sleep patterns and can increase bruxism activity.
- Tobacco: Nicotine is a stimulant and a known risk factor for sleep bruxism.
- Recreational Drugs: Cocaine and ecstasy are potent stimulants that can induce severe bruxism.
4. Dental and Anatomical Factors
- Malocclusion (Misaligned Bite): While historically considered a primary cause, modern research suggests malocclusion plays a less significant role in adult sleep bruxism than previously thought. However, a misaligned bite can exacerbate the effects of grinding and contribute to discomfort.
- Missing or Crooked Teeth: These can alter the bite and create uneven pressure points, potentially leading to clenching.
- Temporomandibular Joint (TMJ) Disorders: While bruxism can cause TMJ disorders, pre-existing TMJ issues can also make an individual more susceptible to grinding.
5. Other Medical Conditions
- Neurological Conditions: Certain conditions like Parkinson's disease, Huntington's disease, and epilepsy can be associated with bruxism.
- Gastroesophageal Reflux Disease (GERD): Some studies suggest a link between GERD and bruxism, possibly due to the body's response to acid reflux during sleep.
Signs and Symptoms: What to Look For
Since sleep bruxism often occurs without your conscious awareness, recognizing its signs and symptoms is key to seeking timely intervention. Many symptoms are often overlooked or attributed to other causes until the real culprit is identified.
- Worn-Down, Flattened, Chipped, or Fractured Teeth: This is one of the most definitive signs. Over time, the constant friction and pressure can visibly alter the shape and integrity of your teeth. You might notice your incisors are shorter or your molars appear flattened.
- Increased Tooth Sensitivity: As enamel wears away, the underlying dentin becomes exposed, leading to sensitivity to hot, cold, or sweet foods and drinks.
- Jaw Pain or Soreness: Waking up with a stiff, tired, or sore jaw is a classic indicator. The muscles of mastication (chewing muscles) are overworked throughout the night.
- Facial Pain or Fatigue: Beyond the jaw, the muscles around your temples and cheeks can also ache from constant clenching.
- Dull Headaches: Can teeth grinding cause headaches? Absolutely. Many people suffering from bruxism experience tension-type headaches, especially in the temples or forehead, which are often worse in the morning. Chronic migraines can also be exacerbated.
- Earache-like Pain: While not directly an ear problem, the intense muscle activity and jaw joint stress can refer pain to the ear area.
- Clicking, Popping, or Locking of the Jaw Joint (TMJ Symptoms): The temporomandibular joint can become inflamed or damaged, leading to sounds or difficulty opening and closing your mouth.
- Sleep Disruption: While you might not know you're grinding, your sleep quality can suffer. A sleeping partner might also complain about the audible grinding sounds.
- Indentations on the Tongue or Cheeks: The pressure from clenching can leave scalloped edges on the sides of your tongue or lines/sores on the inside of your cheeks.
- Gum Recession: Chronic grinding can put stress on the gums and supporting bone, potentially contributing to gum recession and even tooth mobility.
Pro Tip: If a partner reports hearing grinding noises during your sleep, take it seriously. It's often the first definitive clue for someone unaware they have bruxism.
Treatment Options: Protecting Your Smile and Well-being
Addressing bruxism typically involves a multi-faceted approach, combining dental interventions with lifestyle modifications and sometimes medical treatments. The goal is to reduce grinding activity, protect teeth from further damage, and alleviate symptoms.
1. Dental Approaches
- Nightguards (Occlusal Splints): This is the most common and often first-line treatment. A nightguard is a custom-fitted acrylic appliance worn over the upper or lower teeth during sleep.
- Pros: Creates a physical barrier to protect teeth from grinding forces, distributes pressure evenly, and can help reposition the jaw to relieve muscle tension. Very effective for symptom reduction and preventing tooth wear.
- Cons: Can take time to adjust to, requires cleaning, and doesn't address the root cause of bruxism.
- Cost: Custom-fitted guards from a dentist range from $300 to $800, depending on material and complexity. Over-the-counter (boil-and-bite or ready-made) options are $20-$100 but are generally less comfortable, less effective, and can sometimes exacerbate TMJ issues if not properly fitted.
- Occlusal Adjustments: In cases where a specific tooth or a few teeth are causing an uneven bite that contributes to bruxism, your dentist might recommend minor reshaping (equilibration) to create a more balanced bite. This is less common as a primary bruxism treatment but can be helpful for specific bite issues.
- Restorative Dentistry: For teeth already damaged by bruxism, restorative treatments may be necessary. This could include dental bonding, crowns, onlays, or veneers to restore tooth shape, function, and aesthetics. This is usually done after bruxism is managed to prevent further damage.
- Cost: Varies widely, from $100-$300 for bonding to $800-$3,000 per tooth for crowns or veneers.
2. Behavioral & Lifestyle Modifications
These are crucial for addressing the underlying causes, especially stress and anxiety.
- Stress Management Techniques:
- Cognitive Behavioral Therapy (CBT): Helps identify and change thought patterns that contribute to stress and anxiety.
- Relaxation Techniques: Yoga, meditation, deep breathing exercises, mindfulness.
- Regular Exercise: A great stress reliever.
- Warm Baths: Before bed can relax muscles.
- Biofeedback: Special sensors monitor jaw muscle activity. You learn to reduce this activity through visual or auditory feedback, especially useful for awake bruxism but can be adapted for sleep.
- Sleep Hygiene Improvement:
- Maintain a regular sleep schedule.
- Create a dark, quiet, cool bedroom environment.
- Avoid screens before bed.
- Limit naps.
- Dietary Adjustments: Reduce or eliminate caffeine, alcohol, and nicotine, especially in the hours leading up to bedtime.
3. Medical Interventions
- Medications:
- Muscle Relaxants: Your doctor might prescribe a muscle relaxant for a short period to help relax jaw muscles, particularly before sleep. These are typically not for long-term use due to potential side effects.
- Botox (Botulinum Toxin Injections): Injections of Botox into the masseter muscles (jaw muscles) can temporarily paralyze or weaken them, reducing the force of clenching and grinding.
- Pros: Highly effective for severe bruxism, can provide significant relief from pain and protect teeth. Effects last 3-6 months.
- Cons: Temporary, requires repeat injections, cost can be high, and not covered by most dental insurance (may be covered by medical insurance if considered medically necessary for TMJ disorders).
- Cost: $300-$1,000 per treatment session, depending on the number of units used and location.
- Addressing Underlying Sleep Disorders: If sleep apnea or other sleep disorders are identified as contributors, treating them (e.g., with a CPAP machine or an oral appliance for sleep apnea) can significantly reduce bruxism.
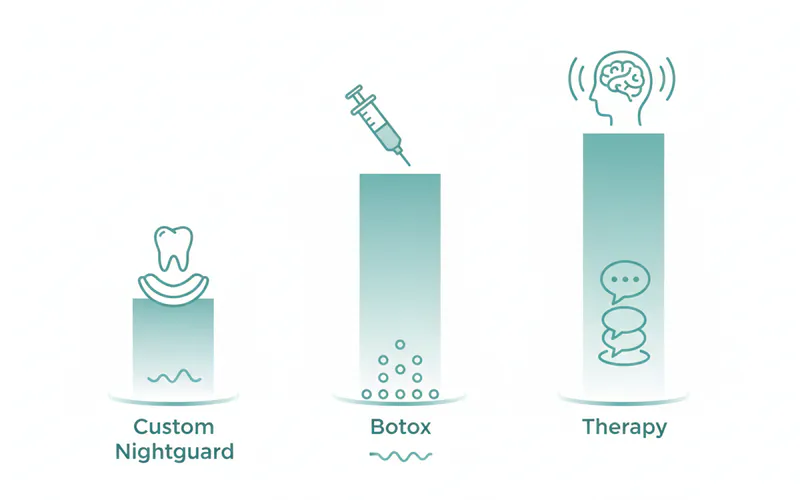
Comparison of Common Bruxism Treatments
| Treatment Option | Description | Pros | Cons | Average US Cost (Range) | Duration of Effect |
|---|---|---|---|---|---|
| Custom Nightguard | Hard acrylic guard fitted by a dentist | Excellent tooth protection, reduces muscle strain, durable | Can take adjustment, requires consistent use, doesn't cure root cause | $300 - $800 | 1-5 years |
| OTC Nightguard | Boil-and-bite or ready-made options | Inexpensive, easily accessible | Less comfortable, poor fit, can exacerbate TMJ issues, less protective | $20 - $100 | 1-6 months |
| Botox Injections | Relaxes jaw muscles by injection | Highly effective for severe pain/grinding, protects teeth | Temporary (3-6 months), high cost, not typically covered by dental ins | $300 - $1,000 per session | 3-6 months |
| Stress Management | CBT, meditation, exercise, relaxation techniques | Addresses root cause, improves overall well-being, no side effects | Requires consistent effort, results vary individually | Varies (e.g., therapy $75-$250/hr) | Ongoing |
| Sleep Apnea Treatment | CPAP, oral appliances, lifestyle changes | Addresses underlying breathing issue, improves sleep quality | Requires diagnosis, CPAP can be cumbersome, compliance is key | CPAP $800-$3,000, Oral Appliance $1,800-$3,000 | Ongoing |
| Dental Restorations | Crowns, veneers, bonding to repair damaged teeth | Restores tooth function and aesthetics | Does not prevent future grinding, often needed after bruxism is managed | $100-$3,000 per tooth | 5-15 years (restoration) |
Step-by-Step Process: What to Expect During Treatment
If you suspect you have bruxism, here's a general outline of what the diagnostic and treatment process typically involves:
- Initial Dental Examination: Your dentist will examine your teeth for signs of wear, fractures, or damage. They'll also check your jaw muscles and temporomandibular joints for tenderness, pain, clicking, or limited movement. They will ask about your symptoms (headaches, jaw pain) and lifestyle habits (stress, caffeine, sleep). Pro Tip: Be honest about your stress levels and medication use; these are critical clues for your dentist.
- Diagnosis Confirmation: Based on the examination and your reported symptoms, your dentist can often diagnose bruxism. In some cases, they might recommend a sleep study (polysomnography) if sleep apnea or other sleep disorders are suspected, or if the bruxism is severe and unresponsive to initial treatments.
- Treatment Planning: Your dentist will discuss various options based on the severity of your bruxism, your symptoms, and any identified contributing factors. This plan often starts with a nightguard.
- Nightguard Creation (if chosen):
- Impressions: Your dentist will take impressions (molds) of your upper and/or lower teeth.
- Fabrication: These impressions are sent to a dental lab where your custom nightguard is precisely fabricated. This usually takes 1-2 weeks.
- Fitting: You'll return to the dentist for a fitting appointment. The dentist will ensure the nightguard fits comfortably and doesn't interfere with your bite. Adjustments may be made.
- Instructions: You'll receive instructions on how to wear, clean, and care for your nightguard.
- Addressing Underlying Causes:
- If stress is a major factor, your dentist might recommend stress management techniques, refer you to a therapist, or suggest relaxation practices.
- If medication is suspected, they'll advise you to consult with your prescribing physician about potential alternatives or dosage adjustments (never stop medication without consulting your doctor).
- If sleep apnea is diagnosed, you'll be referred to a sleep specialist for treatment.
- Follow-up Appointments: Regular dental check-ups are essential to monitor the effectiveness of treatment, check for new signs of wear, and ensure your nightguard is still fitting correctly. Your dentist can also evaluate your overall progress in managing bruxism.
Cost and Insurance: US Price Ranges and Coverage
Understanding the financial aspect of bruxism treatment is vital. Costs can vary significantly based on the type of treatment, geographic location, and the complexity of your case.
Average US Costs for Bruxism Treatments:
| Treatment Type | Low Range | Mid Range | High Range | Notes |
|---|---|---|---|---|
| Custom Nightguard | $300 | $500 | $800+ | From a dentist, often hard acrylic. Price can exceed $1,000 for specialized designs. |
| OTC Nightguard | $20 | $50 | $100 | Boil-and-bite or ready-made. Less effective, short-term. |
| Botox Injections | $300 per session | $600 per session | $1,000+ per session | Performed by a qualified medical professional; typically 3-6 month duration. |
| Dental Restorations | $100 (bonding) | $800 (crown) | $3,000+ (complex) | Per tooth, varies by material and extent of damage. |
| Stress Management | $0 (self-guided) | $75 (group therapy) | $250+ (individual CBT) | Per session for therapy; apps, books are minimal cost. |
| Sleep Study (in-lab) | $1,000 | $3,000 | $5,000+ | Often covered by medical insurance if medically necessary. |
| CPAP Machine | $800 | $1,500 | $3,000+ | If sleep apnea is diagnosed. |
Insurance Coverage Details:
- Dental Insurance:
- Custom Nightguards: Many dental insurance plans offer partial coverage for custom nightguards, as they are considered a preventative measure against further dental damage. Coverage can range from 50% to 80%, depending on your plan's specifics (often listed under "major services" or "orthodontic appliances"). Be prepared for a co-pay or deductible.
- Restorations: Standard dental procedures like fillings, crowns, and veneers are typically covered by dental insurance at varying percentages (often 50-80% for major services), but this is for repairing damage, not preventing bruxism itself.
- OTC Nightguards: Generally, over-the-counter options are not covered by dental insurance.
- Medical Insurance:
- Botox for Bruxism: This is typically considered an "off-label" use for bruxism and is rarely covered by dental insurance. Medical insurance might cover it if it's deemed medically necessary for a diagnosed TMJ disorder (e.g., chronic migraines related to TMJ), but this requires pre-authorization and often extensive documentation. You should always check with your medical insurer directly.
- Sleep Studies & Sleep Apnea Treatment: If bruxism is linked to an underlying medical condition like sleep apnea, the diagnostic sleep study and treatment (e.g., CPAP machine, certain oral appliances for sleep apnea) are generally covered by medical insurance, subject to your plan's deductibles and co-pays.
- Therapy/Counseling: Mental health services for stress and anxiety are typically covered by medical insurance plans.
Pro Tip: Always contact your dental and medical insurance providers before starting any expensive treatment to understand your specific coverage, deductibles, co-pays, and out-of-pocket maximums. Obtain pre-treatment estimates from your dental office.
Recovery and Aftercare: Maintaining Your Progress
Managing bruxism is an ongoing process, not a one-time fix. Consistent aftercare and adherence to prevention strategies are crucial for long-term success.
- Nightguard Care:
- Cleanliness: Clean your nightguard daily with a toothbrush and mild soap or non-abrasive denture cleaner. Rinse thoroughly.
- Storage: Store it in its protective case when not in use to prevent damage and keep it sanitary.
- Avoid Heat: Never expose your nightguard to hot water, direct sunlight, or high heat, as it can warp.
- Regular Checks: Bring your nightguard to every dental check-up so your dentist can assess its fit and wear.
- Monitor Symptoms: Pay attention to your body. Are your headaches less frequent? Is your jaw less sore in the morning? Are you still experiencing tooth sensitivity? Track your progress and discuss any persistent or new symptoms with your dentist.
- Continue Stress Management: Don't abandon stress-reduction techniques once symptoms improve. Make mindfulness, exercise, or therapy a regular part of your routine. Stress is a recurring factor, and proactive management is key.
- Maintain Good Sleep Hygiene: Stick to a consistent sleep schedule, create a relaxing bedtime routine, and avoid stimulants before bed.
- Regular Dental Check-ups: These are critical for monitoring tooth wear, checking your nightguard, and addressing any new dental issues that arise. Your dentist can spot subtle signs of bruxism and adjust your prevention plan as needed.
- Jaw Exercises and Stretches: Your dentist or a physical therapist might recommend specific exercises to stretch and strengthen jaw muscles, improve range of motion, and reduce tension. Examples include gentle jaw opening and closing exercises, side-to-side movements, and self-massage of the masseter and temporal muscles.
Prevention: How to Prevent Teeth Grinding in Sleep
Proactive prevention is the most effective approach to managing bruxism and protecting your dental health. Here's a comprehensive guide on how to prevent teeth grinding in sleep.
1. Master Stress and Anxiety Management
As stress is a primary driver of bruxism, learning to manage it effectively is paramount.
- Practice Relaxation Techniques: Incorporate daily mindfulness meditation, deep breathing exercises, or progressive muscle relaxation into your routine. Apps like Calm or Headspace can be excellent resources.
- Regular Physical Activity: Exercise is a powerful stress reliever. Aim for at least 30 minutes of moderate activity most days of the week.
- Cognitive Behavioral Therapy (CBT): If stress and anxiety are overwhelming, a therapist can provide tools and strategies to reframe negative thought patterns and develop coping mechanisms.
- Adequate "Me Time": Schedule time for hobbies, reading, or anything that helps you unwind and de-stress.
- Journaling: Writing down your thoughts and feelings can help process emotions and reduce nocturnal stress.
2. Optimize Your Sleep Environment and Habits
Good sleep hygiene can significantly reduce the likelihood of sleep disturbances, including bruxism.
- Consistent Sleep Schedule: Go to bed and wake up at roughly the same time every day, even on weekends.
- Create a Relaxing Bedtime Routine: This could involve a warm bath, reading a book, or listening to calming music.
- Dark, Quiet, Cool Bedroom: Ensure your sleep environment is conducive to uninterrupted rest.
- Avoid Stimulants Before Bed: Refrain from caffeine, alcohol, and nicotine several hours before sleep. These substances can disrupt natural sleep cycles and increase jaw muscle activity.
- Limit Screen Time: The blue light emitted from phones, tablets, and computers can interfere with melatonin production, making it harder to fall asleep. Avoid screens for at least an hour before bed.
3. Dietary and Lifestyle Adjustments
- Reduce Caffeine Intake: Coffee, tea, energy drinks, and some sodas contain caffeine. Minimize consumption, especially in the afternoon and evening.
- Limit Alcohol: While it may initially feel relaxing, alcohol disturbs sleep patterns and can increase bruxism.
- Quit Smoking: Nicotine is a stimulant and a known risk factor. Seek support if you need help quitting.
- Stay Hydrated: Dehydration can sometimes contribute to muscle cramps and tension.
4. Jaw Relaxation Techniques and Awareness
For awake bruxism, becoming aware of the habit is the first step. For sleep bruxism, these techniques can help reduce overall jaw tension.
- "Lips Together, Teeth Apart": Practice keeping your lips together but your teeth slightly separated, with your tongue resting gently against the roof of your mouth. This is the natural resting position for your jaw and helps prevent clenching.
- Jaw Massage and Stretches: Gently massage the muscles around your jaw, temples, and neck. Your dentist can provide specific stretching exercises to release tension.
- Warm Compress: Apply a warm, moist washcloth to your jaw before bed to relax muscles.
5. Address Underlying Medical Conditions
- Sleep Apnea Screening: If you snore loudly, experience daytime fatigue, or have observed breathing pauses during sleep, get screened for sleep apnea. Treating sleep apnea can often resolve or significantly reduce bruxism.
- Medication Review: If you suspect a medication is contributing to your bruxism, discuss alternatives or dosage adjustments with your prescribing doctor. Never stop taking medication without medical advice.
6. Regular Dental Check-ups
Your dentist is your first line of defense. Regular visits (every 6 months) allow them to:
- Identify early signs of bruxism-related damage.
- Monitor your jaw and bite.
- Provide custom nightguards if needed.
- Offer personalized advice and referrals for other specialists (e.g., sleep specialists, therapists).
Risks and Complications: What Can Go Wrong
Ignoring bruxism can lead to a cascade of painful and costly dental and health complications over time.
- Severe Tooth Wear and Damage: Chronic grinding literally grinds down your teeth. This can lead to:
- Flattened, Fractured, or Chipped Teeth: Especially molars and premolars.
- Loss of Tooth Enamel: Exposing the sensitive dentin underneath.
- Cracked or Broken Fillings, Crowns, and Bridges: Restorations are not immune to these forces.
- Loosened Teeth: In severe cases, constant force can cause teeth to become mobile.
- Tooth Loss: The ultimate consequence of untreated, severe damage.
- Increased Tooth Sensitivity: Due to enamel wear and exposure of dentin.
- Temporomandibular Joint Disorders (TMJ/TMD): The prolonged strain on the jaw joint can lead to pain, clicking, popping, limited jaw movement, and even locking of the jaw. This can become a chronic, debilitating condition.
- Chronic Headaches and Facial Pain: The constant clenching overworks the muscles of the jaw, head, and neck, leading to persistent tension headaches, migraines, and widespread facial pain. Can teeth grinding cause headaches? Yes, it is a very common cause of chronic headaches.
- Gum Recession: The forces from grinding can put stress on the supporting structures of the teeth, contributing to gum recession and potentially exposing tooth roots.
- Sleep Disruption: While you may not be aware of the grinding, the physical stress and associated pain can lead to poor sleep quality, daytime fatigue, and irritability.
- Referred Pain: Pain from bruxism can radiate to the ears, neck, and shoulders, leading to misdiagnosis of other conditions.
Children / Pediatric Considerations
Bruxism is common in children, affecting up to 30% at some point in their development. While often a temporary phase, parents should be aware of its signs and potential implications.
Prevalence and Onset
- Most common in toddlers and preschoolers, often during sleep.
- Typically resolves by adolescence as the permanent teeth emerge and the jaw develops.
Causes in Children
- Stress and Anxiety: Similar to adults, stress from school, new siblings, or even exciting events can trigger grinding.
- Misaligned Teeth or Bite Issues: Can be a factor, especially if the primary teeth are erupting or being lost.
- Allergies: Nasal congestion or allergies can cause a child to breathe through their mouth, potentially affecting jaw position and leading to grinding.
- Underlying Medical Conditions: Rare cases may be linked to certain medical conditions or medications.
- Response to Pain: Earaches or teething pain might cause a child to grind.
Signs and Symptoms in Children
- Audible grinding sounds during sleep.
- Complaints of jaw pain or soreness in the morning.
- Facial pain.
- Headaches (less common than in adults but can occur).
- Flattened or worn primary (baby) teeth.
- Tooth sensitivity (though often hard for young children to articulate).
Treatment and Prevention in Children
- Observation: In many cases, pediatric bruxism is mild and self-resolving, requiring only observation by parents and the dentist.
- Stress Reduction: Help children manage stress through calming routines, open communication, and ensuring sufficient playtime and rest.
- Addressing Underlying Issues: Treat allergies, ear infections, or other health concerns.
- Dental Interventions: Nightguards are rarely used for primary teeth unless the grinding is severe and causing significant pain or damage to permanent tooth buds. Custom mouthguards may be considered for older children with persistent bruxism affecting permanent teeth, but this is less common than in adults.
- Regular Pediatric Dental Check-ups: A pediatric dentist can monitor tooth wear and jaw development, providing guidance and reassurance to parents.
Pro Tip for Parents: If your child regularly grinds their teeth, especially if they complain of pain or if you notice significant tooth wear, consult with their pediatric dentist. They can help determine if intervention is needed.
Cost Breakdown: Detailed US Costs for Bruxism Management
As previously detailed, the costs associated with managing bruxism can vary widely. Here's a more consolidated breakdown to help you budget.
General Cost Ranges in the US:
- Low Cost (Preventative/OTC): $20 - $100
- Boil-and-bite or generic nightguards.
- Self-guided stress management (apps, books).
- Mid-Range Cost (Initial Professional Intervention): $300 - $1,000
- Custom-fitted nightguard from a dentist.
- Initial consultations with a therapist for stress management.
- A single session of Botox injections.
- High Cost (Comprehensive/Advanced Treatment): $1,000 - $5,000+
- Extensive dental restorations (multiple crowns, veneers).
- Ongoing Botox treatments.
- Treatment for underlying sleep apnea (e.g., CPAP machine or specialized oral appliance).
- Long-term therapy or specialized TMJ treatment.
With vs. Without Insurance:
- With Dental Insurance: Expect to pay a co-pay or deductible. For a custom nightguard, coverage might be 50-80%, reducing your out-of-pocket cost to $100-$400. Dental restorations are often covered similarly.
- Without Dental Insurance: You will be responsible for 100% of the costs. This highlights the importance of preventative measures and regular check-ups to avoid more expensive treatments later.
- Medical Insurance (for specific cases): If bruxism is linked to a diagnosed medical condition (like TMJ or sleep apnea), your medical insurance might cover parts of treatment like Botox, sleep studies, or certain oral appliances, usually after meeting your deductible. Mental health therapy is often covered by medical insurance.
Payment Plans and Financing Options:
- Dental Office Payment Plans: Many dental practices offer in-house payment plans, allowing you to pay for treatment in installments.
- Third-Party Financing: Companies like CareCredit or LendingClub provide specialized healthcare credit cards with low or no-interest financing options for qualified patients.
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): These tax-advantaged accounts allow you to set aside pre-tax money for eligible healthcare expenses, including dental care and bruxism treatments.
- Dental Schools: University dental schools often provide services at a reduced cost, performed by supervised students.
Cost-Saving Tips:
- Preventative Care: Regular dental check-ups can catch bruxism early before extensive and costly damage occurs.
- Understand Your Benefits: Always verify what your insurance covers before treatment.
- Ask for Estimates: Request a detailed cost estimate from your dentist for any recommended treatment.
- Inquire About Discounts: Some dental offices offer discounts for upfront payment or for patients without insurance.
Frequently Asked Questions
### What causes teeth grinding in sleep?
Teeth grinding in sleep, or sleep bruxism, is often caused by a combination of factors. High stress and anxiety levels are significant contributors, as are certain lifestyle habits like consuming caffeine, alcohol, or nicotine, especially before bedtime. Underlying sleep disorders such as sleep apnea, and even some medications like SSRI antidepressants, can also trigger or exacerbate bruxism.
### Can teeth grinding cause headaches and jaw pain?
Yes, absolutely. Teeth grinding places immense strain on the jaw muscles and temporomandibular joints (TMJ). This prolonged tension can lead to chronic headaches, particularly tension headaches that affect the temples and forehead, and can also cause significant jaw pain, soreness, and fatigue upon waking.
### How quickly does a nightguard work for bruxism?
A custom-fitted nightguard provides immediate physical protection for your teeth as soon as you start wearing it. For symptom relief like jaw pain and headaches, many individuals experience noticeable improvement within a few days to a few weeks of consistent use. However, full relief from long-standing symptoms might take longer as muscles de-stress.
### Is teeth grinding a sign of stress?
Yes, teeth grinding is very often a direct physical manifestation of stress, anxiety, anger, or frustration. When the body is under psychological tension, it can manifest as muscle clenching, and for many, this translates into involuntary jaw clenching and grinding, especially during sleep.
### Can teeth grinding be cured naturally?
While there's no single "cure" for bruxism, especially if it has underlying medical causes, many natural and behavioral strategies can effectively manage and often resolve it. These include stress reduction techniques (meditation, exercise), improving sleep hygiene, avoiding stimulants, and practicing jaw relaxation exercises. These approaches can significantly reduce or eliminate grinding without medication.
### Are over-the-counter nightguards as effective as custom ones?
Generally, no. Over-the-counter (OTC) nightguards (like boil-and-bite types) offer some temporary protection but are rarely as effective as custom-fitted ones. Custom nightguards from a dentist provide a precise fit, better comfort, and more effective distribution of pressure, reducing the risk of further dental damage and potential TMJ issues that can arise from poorly fitting appliances.
### What if a nightguard doesn't stop the grinding?
If a nightguard doesn't fully stop your grinding or alleviate symptoms, it indicates that the underlying cause might need further attention. Your dentist might recommend exploring other treatments such as Botox injections, referring you to a sleep specialist to rule out sleep apnea, or suggesting professional stress management like Cognitive Behavioral Therapy (CBT).
### What are the long-term consequences of untreated teeth grinding?
Untreated teeth grinding can lead to severe and costly long-term consequences. These include significant tooth wear, fractures, chipped teeth, loosened teeth, gum recession, increased tooth sensitivity, chronic headaches, and temporomandibular joint (TMJ) disorders, which can cause severe jaw pain and dysfunction.
### Can children outgrow teeth grinding?
Yes, most children outgrow teeth grinding. It's quite common in toddlers and young children, often related to teething, stress, or jaw development, and typically resolves by the time they reach adolescence. However, parents should still monitor symptoms and consult a pediatric dentist if there's pain or significant tooth wear.
### How much does it cost to fix teeth damaged by grinding?
The cost to fix teeth damaged by grinding varies significantly depending on the extent and type of damage. Minor chips might be repaired with dental bonding for $100-$300 per tooth. More severe wear or fractures could require dental crowns, costing $800-$3,000 per tooth. If multiple teeth are affected or complex restorative work is needed, the total cost can easily climb into several thousands of dollars.
When to See a Dentist
It's crucial to seek professional dental advice if you suspect you or a loved one is grinding teeth, as early intervention can prevent serious complications.
Schedule a routine appointment with your dentist if you experience any of the following:
- Persistent jaw pain, soreness, or fatigue, especially in the morning.
- Frequent tension headaches, particularly upon waking.
- Noticing signs of tooth wear, flattening, or small chips on your teeth.
- Increased tooth sensitivity to hot or cold.
- If a sleeping partner reports hearing you grind your teeth at night.
- Any clicking, popping, or locking sensation in your jaw joint.
- Difficulty opening or closing your mouth fully.
Consider an earlier or more urgent appointment if you experience:
- Sudden, severe, or debilitating jaw pain that interferes with eating or speaking.
- A tooth that suddenly breaks, cracks, or becomes very loose.
- Your jaw locks in an open or closed position.
- Unmanageable pain that over-the-counter remedies do not alleviate.
While occasional teeth clenching might not be cause for alarm, persistent bruxism warrants professional evaluation. Your dentist can accurately diagnose the condition, assess any existing damage, and help you develop a personalized prevention and treatment plan to safeguard your oral health and overall well-being.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles

What Causes Teeth Grinding in Sleep
More than one in ten adults—and even more children—clench or grind their teeth during sleep, a condition known medically as sleep bruxism. For many, it's an unconscious habit that goes unnoticed until significant damage or discomfort arises. Waking up with a dull, constant headache, jaw pain, or
February 23, 2026
How to Not Grind Teeth at Night
More than one in ten adults and a significant percentage of children experience teeth grinding, medically known as bruxism, a condition that often goes unnoticed, especially when it occurs during sleep. If you've woken up with a sore jaw, a dull headache, or noticed your teeth becoming unusually
February 23, 2026

What Is Jaw Clenching
Do you often wake up with a dull headache, a sore jaw, or unexplained tooth sensitivity? You're not alone. Approximately 1 in 10 adults and up to 3 in 10 children experience some form of bruxism, a condition characterized by grinding, gnashing, or clenching your teeth. At the heart of this wides
February 23, 2026
Severe Bruxism Molars: Complete Guide
When the quiet of the night is shattered by a grinding, grating sound, or when you wake up with an aching jaw and teeth that feel oddly sensitive, it’s often a sign of bruxism. But what happens when this condition intensifies, leading to significant damage, especially to your back teeth? This is the
February 23, 2026