Stop Teeth Grinding: Complete Guide
Key Takeaways
- Do you wake up with a dull, constant headache or jaw soreness? Do your teeth feel sensitive, or have you noticed they look flatter or chipped? You might be one of the estimated 10% of adults and up to 15% of children who experience bruxism, commonly known as teeth grinding or clenching. This per
Stop Teeth Grinding: Complete Guide
Do you wake up with a dull, constant headache or jaw soreness? Do your teeth feel sensitive, or have you noticed they look flatter or chipped? You might be one of the estimated 10% of adults and up to 15% of children who experience bruxism, commonly known as teeth grinding or clenching. This pervasive habit, often occurring subconsciously during sleep, can lead to significant dental and overall health problems if left unaddressed. Understanding how to prevent teeth grinding and its underlying causes is crucial for preserving your oral health and preventing painful complications.
This comprehensive guide from SmilePedia.net will delve deep into the world of bruxism, exploring its different forms, the numerous factors that contribute to it, and the diverse array of effective treatments available. We will walk you through what to expect during diagnosis and treatment, discuss the associated costs and insurance considerations, and provide actionable steps you can take to alleviate symptoms and, ultimately, stop teeth grinding for good. By the end of this article, you'll have a complete understanding of this common condition and a clear roadmap to a healthier, pain-free smile.
Key Takeaways:
- Bruxism is widespread: Affects 1 in 10 adults and up to 1 in 7 children, often occurring during sleep.
- Causes are varied: Stress, anxiety, sleep disorders (like sleep apnea), certain medications, and lifestyle factors are common culprits.
- Symptoms include: Jaw pain, headaches, worn/chipped teeth, tooth sensitivity, and muscle soreness.
- Custom night guards are often the first line of defense: Costing $300-$800 (or more), they protect teeth from damage, though some insurance plans may cover a portion. OTC guards are cheaper but less effective long-term.
- Botox injections can provide relief: Targeting jaw muscles, treatments cost $400-$1,000+ per session and typically last 3-6 months.
- Lifestyle changes are critical: Stress management, improved sleep hygiene, and avoiding stimulants can significantly reduce grinding severity.
- Early intervention is key: Addressing bruxism promptly can prevent irreversible tooth damage, chronic jaw pain, and expensive restorative dental work.

What It Is / Overview
Bruxism (pronounced BRUK-siz-um) is a medical term for involuntarily grinding, clenching, or gnashing your teeth. While occasional teeth grinding may not cause harm, when it occurs regularly, it can lead to a range of dental complications, jaw disorders, headaches, and other issues. It's often a subconscious habit, meaning many people are unaware they do it until a dental professional points out the signs or a partner complains about the grinding sounds.
The force exerted during bruxism can be substantial, often many times greater than the force used during normal chewing. This immense pressure places undue stress on your teeth, jaw muscles, and temporomandibular joints (TMJs). According to the American Dental Association (ADA), bruxism is a significant concern due to its potential for cumulative, irreversible damage over time.
Types / Variations
Bruxism is generally categorized into two main types:
Sleep Bruxism (Nocturnal Bruxism)
This is the most common form, characterized by involuntary grinding or clenching during sleep. Individuals are often unaware they are doing it, and it can be quite forceful, leading to significant wear on teeth and strain on jaw muscles. Sleep bruxism is classified as a sleep-related movement disorder and is often associated with other sleep disturbances like snoring or sleep apnea. It tends to occur more frequently during periods of light sleep or during sleep arousal.
Awake Bruxism (Diurnal Bruxism)
Awake bruxism involves subconscious clenching or grinding of teeth while a person is awake. Unlike sleep bruxism, it typically does not involve the characteristic grinding sound. Instead, it manifests as chronic clenching, often in response to stress, anxiety, concentration, or even habitual behaviors like biting nails or chewing on pens. People with awake bruxism may catch themselves clenching their jaw during stressful moments or while performing focused tasks like driving or working at a computer.
While both types can lead to similar symptoms and damage, their triggers and management strategies can differ. Some individuals may experience both sleep and awake bruxism.
Causes / Why It Happens
Understanding the root teeth grinding causes is a critical step toward effective treatment and prevention. Bruxism is rarely caused by a single factor but often results from a combination of physical, psychological, and lifestyle elements.
Psychological Factors
- Stress and Anxiety: This is arguably the most common cause. High levels of stress, anxiety, anger, frustration, or tension can lead to subconscious teeth clenching and grinding, especially during sleep. The jaw muscles become a physical outlet for emotional distress.
- Personality Type: Individuals with aggressive, competitive, or hyperactive personality types may be more prone to bruxism.
Physical and Dental Factors
- Malocclusion (Misaligned Bite): While not universally accepted as a direct cause, some theories suggest that an improper bite, where teeth do not meet correctly, can trigger grinding as the jaw attempts to find a comfortable resting position.
- TMJ Disorders: Bruxism can be both a cause and a symptom of temporomandibular joint (TMJ) disorders, which affect the jaw joint and surrounding muscles.
- Neurological Conditions: Certain rare neurological conditions, such as Huntington's disease or Parkinson's disease, can be associated with bruxism.
- Growth and Development: In children, bruxism can be a temporary phase related to teething, jaw growth, or the eruption of new teeth.
Medical Conditions and Medications
- Sleep Disorders: Sleep apnea, a condition where breathing repeatedly stops and starts during sleep, is strongly linked to sleep bruxism. Other sleep disorders like restless legs syndrome can also be contributing factors.
- Gastroesophageal Reflux Disease (GERD): Some studies indicate a correlation between acid reflux and sleep bruxism.
- Certain Medications: Antidepressants, particularly selective serotonin reuptake inhibitors (SSRIs), antipsychotics, and some stimulant medications (e.g., for ADHD), can have bruxism as a side effect.
- Illicit Drugs: Amphetamines and ecstasy are known to cause severe teeth clenching and grinding.
Lifestyle Factors
- Caffeine and Alcohol: Excessive consumption of caffeinated beverages (coffee, energy drinks) and alcohol, especially before bedtime, can stimulate the central nervous system and exacerbate grinding.
- Smoking: Nicotine is a stimulant and has been linked to an increased risk of bruxism.
- Recreational Drug Use: Certain recreational drugs can induce or worsen teeth grinding.
Pro Tip: Keeping a "bruxism diary" can help identify potential triggers. Note down your stress levels, caffeine intake, alcohol consumption, and any jaw discomfort to look for patterns.
Signs and Symptoms
Recognizing the signs and symptoms of bruxism is often the first step toward seeking treatment. Because sleep bruxism occurs unconsciously, many people learn about it from a bed partner who hears the grinding sounds, or from their dentist during a routine check-up.
Common signs and symptoms include:
- Worn-down, flattened, fractured, or chipped teeth: This is one of the most visible indicators, especially on the biting surfaces.
- Increased tooth sensitivity: Due to enamel erosion and exposed dentin.
- Enlarged jaw muscles: The masseter muscles (on the sides of your jaw) can become noticeably larger and feel tender or tight to the touch.
- Jaw pain or soreness: Especially in the morning, along with tenderness in the jaw joints.
- Tired or tight jaw muscles: Making it difficult to open your mouth fully.
- Pain that feels like an earache: But with no actual problem inside the ear.
- Dull headaches: Originating in the temples, often present upon waking.
- Facial pain: Especially around the jaw, temples, and cheeks.
- Clicking, popping, or locking of the jaw joint (TMJ): Indicating potential temporomandibular joint dysfunction.
- Indentations on the tongue: From pressing against the teeth.
- Damage from chewing on the inside of the cheek: Irritation or small sores.
- Sleep disruption: For the person grinding or their bed partner.
A dentist can often diagnose bruxism by examining your teeth for wear patterns, checking for jaw tenderness, and asking about your symptoms and lifestyle. X-rays may be taken to assess the condition of your jaw joints and underlying bone.
Treatment Options
Effectively addressing bruxism often requires a multi-faceted approach, combining dental interventions with lifestyle modifications and sometimes medical treatments. The goal is to protect your teeth, alleviate pain, and reduce or eliminate the grinding habit.
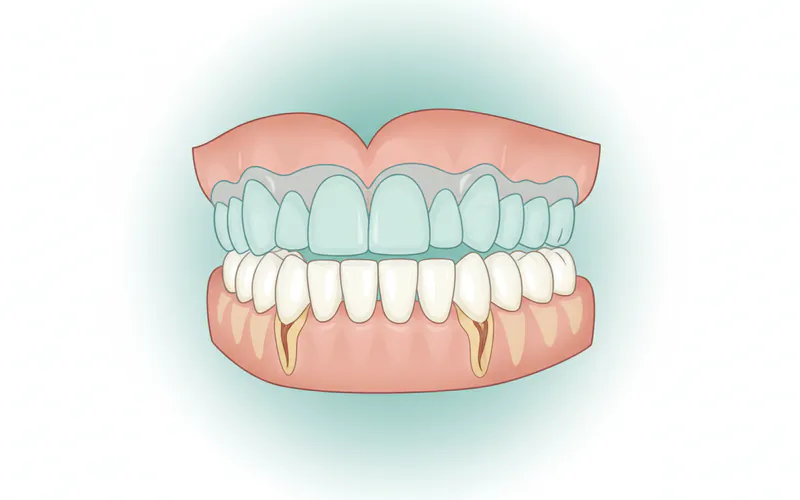
1. Dental Appliances (Night Guards / Splints)
These are the most common and often the first line of treatment. A dental appliance, typically worn over the upper or lower teeth, acts as a barrier, preventing direct tooth-on-tooth contact and distributing the forces of grinding and clenching.
- Custom-Made Night Guards: Fabricated by your dentist from an impression of your teeth, these are made of durable acrylic and fit precisely.
- Pros: Superior comfort, fit, and durability; highly effective in protecting teeth and reducing jaw strain.
- Cons: Higher cost, requires a dental visit for impressions and fitting.
- Over-the-Counter (OTC) Night Guards: Available at pharmacies, these are typically "boil-and-bite" mouthguards or pre-formed generic guards.
- Pros: Inexpensive, immediately available.
- Cons: Less comfortable, poorer fit, less durable, can sometimes exacerbate jaw problems if not fitted correctly, may not stay in place well.
- Pro Tip: While OTC guards offer temporary relief, they are not a long-term solution. A custom-fitted guard provides far better protection and comfort.
2. Stress and Anxiety Management
Since stress is a primary driver for many bruxism sufferers, managing it is crucial.
- Relaxation Techniques: Deep breathing exercises, meditation, yoga, mindfulness, and progressive muscle relaxation can help reduce overall tension.
- Counseling or Therapy: Cognitive Behavioral Therapy (CBT) can help individuals identify and change thought patterns contributing to stress and anxiety.
- Regular Exercise: Physical activity is a great stress reliever.
- Adequate Sleep: Prioritizing good sleep hygiene can reduce overall stress on the body.
3. Biofeedback
Biofeedback therapy uses electronic devices to monitor physiological responses (like muscle tension) and provide real-time feedback. For bruxism, sensors can be placed on jaw muscles, and when clenching occurs, a sound or light cue prompts the person to relax. This can help individuals become more aware of their clenching habits and learn to control them, especially for awake bruxism.
4. Medications
While no medication specifically cures bruxism, some can help manage symptoms or address underlying causes.
- Muscle Relaxants: Prescribed for short-term use to relax jaw muscles, especially before bedtime, to reduce clenching.
- Botulinum Toxin (Botox) Injections: Small amounts of Botox injected into the masseter muscles can partially paralyze them, reducing the force of clenching and grinding.
- Pros: Highly effective for severe cases, can provide significant pain relief and stop teeth grinding for several months.
- Cons: Temporary (effects last 3-6 months), requires repeated injections, relatively high cost, potential for temporary muscle weakness or changes in smile.
- Pain Relievers and Anti-inflammatories: Over-the-counter NSAIDs (e.g., ibuprofen) can help manage pain and inflammation associated with jaw soreness.
- Medications for Underlying Conditions: If bruxism is linked to sleep apnea, restless legs syndrome, or certain psychiatric conditions, treating those primary conditions with specific medications can indirectly alleviate bruxism.
5. Addressing Underlying Conditions
- Sleep Apnea Treatment: If a sleep study confirms sleep apnea, treatments like Continuous Positive Airway Pressure (CPAP) therapy or oral appliances designed for sleep apnea can significantly reduce or eliminate associated sleep bruxism.
- Orthodontic Correction: In cases where a significant malocclusion is believed to contribute to bruxism, orthodontic treatment (braces, aligners) may be considered to correct the bite. This is typically a longer-term and more expensive solution, rarely the first choice for bruxism alone.
- Medication Review: If current medications are suspected of causing bruxism, your doctor may adjust dosages or switch to alternative drugs. Never discontinue medication without consulting your prescribing physician.
6. Physical Therapy and Manual Therapies
- Stretching and Massage: Gentle stretches for the jaw and neck muscles, along with self-massage, can help relieve tension.
- Warm Compresses: Applying a warm, moist cloth to the jaw can relax muscles.
- Professional Physical Therapy: A physical therapist can provide specific exercises to strengthen jaw muscles, improve range of motion, and reduce pain, particularly if TMJ involvement is present.
- Acupuncture: Some individuals find relief from jaw pain and muscle tension through acupuncture.
Step-by-Step Process: What to Expect During Treatment
Addressing bruxism typically involves a systematic approach, starting with diagnosis and moving through treatment and ongoing management.
-
Initial Dental Consultation:
- Your dentist will take a thorough medical and dental history, asking about symptoms like jaw pain, headaches, tooth sensitivity, and any observed grinding.
- They will perform a comprehensive oral exam, looking for signs of tooth wear, fractured teeth or fillings, indentations on the tongue or cheek, and enlarged jaw muscles.
- Palpation of the jaw muscles and TMJs will assess tenderness and dysfunction.
- X-rays may be taken to evaluate the jaw joints and underlying bone structure.
- Based on these findings, a diagnosis of bruxism will be made, and a preliminary treatment plan discussed.
-
Addressing Immediate Needs (Pain Relief/Protection):
- If you're experiencing significant pain, your dentist might recommend over-the-counter pain relievers or prescribe a short course of muscle relaxants.
- The most common first step for protection is a custom-fitted night guard. Impressions of your teeth will be taken, and the guard will be fabricated in a dental lab. This typically requires two appointments: one for impressions, one for fitting and adjustments.
-
Exploring Underlying Causes:
- Your dentist will discuss potential contributing factors like stress, sleep habits, caffeine/alcohol intake, and medications.
- If sleep apnea or other sleep disorders are suspected, a referral to a sleep specialist for a sleep study (polysomnography) may be recommended.
- If specific medications are implicated, a discussion with your prescribing physician will be necessary.
-
Implementing Broader Treatment Strategies:
- Lifestyle Changes: You'll be advised on stress reduction techniques, improving sleep hygiene, and avoiding stimulants.
- Biofeedback or Physical Therapy: If recommended, these therapies will begin with a specialist.
- Botox Injections: If appropriate, your dentist or an oral surgeon will administer the injections. This is typically done in-office and takes only a few minutes.
-
Follow-up and Adjustment:
- Regular follow-up appointments will be scheduled to check the night guard's fit, assess the effectiveness of treatment, and monitor your symptoms.
- Your dentist may make adjustments to your night guard or recommend further steps based on your progress.
- If underlying conditions like sleep apnea are being treated, ongoing management with the relevant specialists will occur.
This process is highly individualized, and the exact steps and duration will vary based on the severity of your bruxism and its underlying causes.
Cost and Insurance
The cost of treating bruxism in the US can vary significantly depending on the chosen treatment, the severity of the condition, and your geographic location. Insurance coverage also plays a major role.
Typical Cost Ranges (US Dollars)
- Dental Consultation and Exam: $50 - $250 (often covered by most dental insurance plans for preventative care).
- Custom-Made Night Guard/Occlusal Splint: $300 - $800 on average. Some specialized or complex splints can cost up to $1,500 - $2,500.
- Geographic Variation: Costs tend to be higher in major metropolitan areas like New York City or Los Angeles compared to rural regions.
- Over-the-Counter (Boil-and-Bite) Night Guard: $15 - $50.
- Botox Injections for Bruxism: $400 - $1,000+ per session. The price depends on the number of units used and the provider's fees. Most patients require injections every 3-6 months.
- Sleep Study (Polysomnography): $500 - $5,000. This can vary greatly depending on whether it's an at-home test or an in-lab study, and whether you have medical insurance.
- Physical Therapy Sessions: $75 - $200 per session. A course of treatment may involve several sessions.
- Counseling/Therapy for Stress Management: $75 - $250 per session, depending on the therapist and type of therapy.
- Orthodontic Treatment: If malocclusion is a primary factor and requires correction, costs can range from $3,000 - $8,000+ for braces or clear aligners.
Insurance Coverage Details
- Dental Insurance:
- Many dental insurance plans provide partial coverage for custom-made night guards, often classifying them under "major restorative" or "preventative appliances." You might find coverage of 50% to 80% after your deductible is met, up to your annual maximum.
- Routine exams and X-rays are usually covered at a high percentage (80-100%).
- Orthodontic coverage varies widely; some plans offer limited benefits for adults.
- Medical Insurance:
- Treatment for underlying medical conditions like sleep apnea (e.g., sleep study, CPAP machine, oral appliances for sleep apnea) is typically covered by medical insurance, often subject to deductibles and co-pays.
- Botox for bruxism is generally considered an "off-label" cosmetic treatment and is usually not covered by medical insurance, making it an out-of-pocket expense. However, if bruxism is medically debilitating and causing severe TMJ dysfunction, some medical plans might cover it with prior authorization and extensive documentation.
- Physical therapy and mental health counseling for stress/anxiety are often covered by medical insurance, though co-pays and deductibles will apply.
Payment Plans and Financing Options
Many dental and medical offices offer:
- In-house payment plans: Spreading costs over several months.
- Third-party financing: Companies like CareCredit offer special healthcare financing with deferred interest options for qualified applicants.
- Health Savings Accounts (HSAs) or Flexible Spending Accounts (FSAs): These tax-advantaged accounts can be used to pay for qualified medical and dental expenses, including many bruxism treatments.
Pro Tip: Always confirm coverage with your specific insurance provider before starting any treatment to understand your out-of-pocket costs. Ask for a detailed cost estimate from your dental office.
Recovery and Aftercare
Once you begin treatment for bruxism, ongoing care and vigilance are essential for sustained relief and prevention of recurrence.
Night Guard Maintenance
- Daily Cleaning: Clean your night guard daily with a toothbrush and mild soap or non-abrasive denture cleaner. Rinse thoroughly.
- Proper Storage: Store your night guard in its protective case when not in use to prevent damage and bacterial growth.
- Regular Check-ups: Bring your night guard to your dental appointments. Your dentist will check its fit and condition, making adjustments or recommending replacement if necessary (typically every 1-5 years, depending on wear).
Lifestyle Management
- Consistent Stress Reduction: Continue practicing relaxation techniques (meditation, yoga, deep breathing) as part of your daily routine. Identify and address sources of stress in your life.
- Maintain Good Sleep Hygiene: Stick to a regular sleep schedule, create a comfortable sleep environment, and avoid screens before bed.
- Avoid Triggers: Limit or eliminate caffeine, alcohol, and nicotine, especially in the hours leading up to bedtime.
- Self-Monitoring: Be aware of your jaw position throughout the day. Try to keep your teeth slightly apart, with your tongue resting gently against the roof of your mouth.
- Jaw Exercises: Your dentist or a physical therapist may provide specific exercises to stretch and strengthen jaw muscles and improve TMJ function.
Follow-up with Specialists
- If you're undergoing treatment for sleep apnea, continue with your CPAP therapy or oral appliance as prescribed and attend follow-up appointments with your sleep specialist.
- If you receive Botox injections, schedule follow-up injections every 3-6 months to maintain the effects.
- Regular dental check-ups (typically every six months) are vital for your dentist to monitor your progress, check for any new signs of grinding, and ensure your overall oral health remains stable.
Recovery from bruxism is less about a one-time "cure" and more about effective, ongoing management. By consistently applying treatment strategies and practicing self-care, you can significantly reduce symptoms and protect your dental health long-term.
Prevention: How to Prevent Teeth Grinding
While not all cases of bruxism are preventable (e.g., those linked to certain neurological conditions), many instances, especially those related to stress and lifestyle, can be significantly mitigated or prevented through proactive measures. Here’s how to prevent teeth grinding:
-
Stress Management: This is paramount. Incorporate stress-reduction techniques into your daily life.
- Mindfulness and Meditation: Even 10-15 minutes a day can make a difference.
- Yoga or Tai Chi: These practices combine physical activity with mental relaxation.
- Deep Breathing Exercises: Simple techniques can calm your nervous system.
- Time Management: Reduce overwhelm by organizing tasks and setting realistic goals.
- Seek Professional Help: If stress or anxiety feels unmanageable, consider talking to a therapist or counselor.
-
Improve Sleep Hygiene: Good sleep habits can reduce sleep disturbances that contribute to bruxism.
- Consistent Sleep Schedule: Go to bed and wake up at the same time every day, even on weekends.
- Create a Relaxing Bedtime Routine: Take a warm bath, read a book, or listen to calming music.
- Optimize Your Sleep Environment: Ensure your bedroom is dark, quiet, and cool.
- Avoid Screens Before Bed: The blue light from phones, tablets, and computers can interfere with sleep.
- Limit Naps: If you must nap, keep it short and early in the day.
-
Avoid Stimulants and Certain Substances:
- Caffeine: Reduce or eliminate caffeine intake, especially in the afternoon and evening. This includes coffee, tea, energy drinks, and some sodas.
- Alcohol: Limit alcohol consumption, particularly close to bedtime, as it can disrupt sleep cycles and worsen bruxism.
- Nicotine: Quit smoking or using other tobacco products. Nicotine is a stimulant.
- Illicit Drugs: Avoid amphetamines and ecstasy, which are strong triggers for bruxism.
-
Conscious Awareness During the Day: For awake bruxism, becoming aware of the habit is the first step.
- Self-Monitoring: Periodically check your jaw throughout the day. Are your teeth touching?
- Jaw Rest Position: Practice keeping your teeth slightly apart, with your tongue resting on the roof of your mouth, behind your upper front teeth.
- Reminders: Use sticky notes, phone alarms, or an app to remind yourself to relax your jaw.
-
Regular Dental Check-ups: Your dentist can spot early signs of wear and tear, even before you notice symptoms, and recommend preventive measures like a night guard. They can also advise on proper jaw alignment.
-
Stay Hydrated and Maintain a Balanced Diet: Overall health contributes to stress resilience and better sleep.
By incorporating these preventive strategies into your daily life, you can significantly decrease the likelihood and severity of teeth grinding, safeguarding your oral health and overall well-being.
Risks and Complications
Left untreated, chronic bruxism can lead to a range of serious and often irreversible complications affecting your oral health and quality of life.
-
Severe Tooth Damage:
- Flattened, Fractured, or Chipped Teeth: Constant grinding wears down the chewing surfaces, potentially leading to cracks or breaks in teeth.
- Worn Enamel: Loss of enamel can expose the underlying dentin, leading to increased tooth sensitivity to hot, cold, and sweets.
- Loose Teeth: Persistent force can loosen teeth in their sockets.
- Root Damage: In extreme cases, the roots of the teeth can be damaged.
- Damage to Dental Work: Crowns, fillings, veneers, and bridges can be fractured or dislodged, requiring expensive replacement.
-
Temporomandibular Joint (TMJ) Disorders:
- Chronic stress on the TMJs can lead to inflammation, pain, and dysfunction.
- Symptoms include pain or tenderness in and around the jaw joint, clicking or popping sounds when opening or closing the mouth, limited jaw movement, and a locked jaw.
- Severe cases may require complex medical or surgical interventions.
-
Chronic Headaches and Facial Pain:
- Tension headaches, especially in the temples and behind the eyes, are common due to overworking jaw muscles.
- Generalized facial pain and neck stiffness can also develop.
-
Muscle Hypertrophy:
- The masseter muscles (jaw muscles) can become enlarged and overdeveloped, leading to a wider, more square-shaped jawline.
-
Sleep Disturbances:
- For individuals with sleep bruxism, the grinding episodes can disrupt their sleep cycle, leading to fatigue, irritability, and reduced cognitive function the next day.
- The grinding sounds can also severely disturb a bed partner's sleep.
-
Gum Recession: In some cases, the excessive force of grinding can contribute to gum recession around the teeth.
-
Speech and Chewing Difficulties: Severe pain or TMJ issues can make speaking, chewing, and swallowing uncomfortable or difficult.
Early intervention is critical to prevent these long-term, often painful, and costly complications.
Comparison Tables
Table 1: Night Guard Options Comparison
| Feature | Custom-Made Night Guard | Boil-and-Bite (OTC) Night Guard | Pre-Formed (OTC) Night Guard |
|---|---|---|---|
| Material | Durable acrylic (hard or soft-hard composite) | Thermoplastic material (softens with heat) | Softer rubber or silicone |
| Fit | Precise, covers entire arch, made from dental impressions | Molded by patient at home, often bulky | Generic fit, one-size-fits-most, often loose or ill-fitting |
| Protection | Excellent: cushions, distributes force, prevents tooth contact | Fair: provides some cushioning, but can shift | Poor: minimal protection, can be uncomfortable |
| Comfort | Superior: slim, comfortable, barely noticeable after adaptation | Moderate to poor: bulky, can irritate gums, difficult to speak | Poor: bulky, can trigger gag reflex, uncomfortable |
| Durability | High: lasts 1-5+ years with proper care | Low: typically lasts a few weeks to months | Very low: easily chewed through, short lifespan |
| Cost (US) | $300 - $800+ | $15 - $50 | $10 - $30 |
| Insurance | Often partially covered by dental insurance | Not covered | Not covered |
| Pros | Maximum protection, durable, comfortable, effective, dentist-supervised | Inexpensive, immediate availability | Very inexpensive |
| Cons | Expensive, requires multiple dental visits | Bulky, less durable, can shift, may worsen TMJ if not fitted properly | Bulky, uncomfortable, ineffective for severe grinding, high risk of misuse |
Table 2: Bruxism Treatment Options Comparison
| Treatment Option | Primary Goal | Average Cost (US) | Effectiveness (General) | Duration of Effect | Pros | Cons |
|---|---|---|---|---|---|---|
| Custom Night Guard | Protect teeth, reduce jaw strain | $300 - $800+ | High | Years (with proper care) | Non-invasive, highly protective, durable, dentist-monitored | Initial cost, requires adaptation |
| Stress Management/Therapy | Address root cause, reduce tension | $75 - $250/session | High (long-term) | Ongoing/Permanent | Holistic, no side effects, improves overall well-being | Requires consistent effort, not an immediate "cure" |
| Botox Injections | Reduce muscle force, alleviate pain | $400 - $1,000+/session | High (for muscle relaxation) | 3-6 months | Quick relief from severe clenching, reduces pain | Temporary, expensive, requires repeat visits, potential side effects |
| Sleep Apnea Treatment | Resolve sleep breathing issues | $500 - $5,000 (study & treatment) | High (if primary cause) | Ongoing | Addresses underlying sleep disorder, improves general health | Invasive (CPAP), requires compliance, initial cost |
| Physical Therapy | Alleviate pain, improve jaw function | $75 - $200/session | Moderate to High | Varies with adherence | Non-invasive, strengthens muscles, educates on self-care | Requires commitment, not a direct grinding "stopper" |
| Biofeedback | Increase awareness, retrain muscles | Varies widely (device/therapy) | Moderate (for awake bruxism) | Variable (with practice) | Non-pharmacological, empowers self-control | Requires technology/training, less effective for sleep bruxism |
Children / Pediatric Considerations
Bruxism is common in children, affecting an estimated 15% of preschoolers and up to 10% of adolescents. Unlike adult bruxism, it often presents differently and typically has a more benign prognosis.
Why It Happens in Children
- Growth and Development: Grinding can occur as baby teeth erupt and fall out, or as permanent teeth emerge and the jaw develops. It's often a temporary response to changes in their bite.
- Stress and Anxiety: Similar to adults, stress from school, new siblings, family issues, or even excitement can trigger grinding.
- Allergies and Earaches: Some children grind their teeth to relieve pressure from ear infections or allergy-related congestion.
- Sleep Disorders: Although less common than in adults, sleep apnea or other sleep-disordered breathing can contribute to bruxism in children.
- Nutritional Deficiencies: Rarely, some research suggests a link to certain vitamin deficiencies.
Signs and Symptoms in Children
Parents might notice:
- Grinding sounds during sleep.
- Complaints of jaw pain or soreness in the morning.
- Headaches (less common than in adults).
- Visible wear on baby teeth or early permanent teeth.
- Increased tooth sensitivity.
Treatment and Management for Children
For most children, bruxism is a self-limiting condition that resolves on its own by the time they are teenagers. Treatment is usually conservative and often unnecessary.
- Observation: The most common approach is "watch and wait." Regular dental check-ups are crucial to monitor tooth wear.
- Stress Reduction: Address any identifiable sources of stress or anxiety in the child's life. Encourage relaxation before bed (e.g., warm bath, reading, quiet play).
- Dental Appliances (Rarely): Night guards are generally not recommended for children unless tooth wear is severe or the child experiences significant pain, and only then for a temporary period. A growing jaw means a night guard would quickly become ill-fitting and ineffective. If prescribed, it would be custom-made and closely monitored by a pediatric dentist.
- Addressing Underlying Issues: If a sleep disorder like sleep apnea is suspected, a referral to a pediatric sleep specialist is warranted. Treating allergies or ear infections can sometimes alleviate grinding.
- Dietary Adjustments: Limit sugary drinks and caffeine.
Pro Tip for Parents: If your child is grinding their teeth, discuss it with their pediatric dentist. They can assess the severity and rule out any underlying issues, providing reassurance and guidance. Most childhood bruxism does not cause long-term damage.
Cost Breakdown (Summary)
To consolidate cost information for budgeting purposes, here's a summary of average US costs for key bruxism treatments, factoring in insurance impact.
| Treatment/Service | Average Low Cost (Without Insurance) | Average Mid Cost (Without Insurance) | Average High Cost (Without Insurance) | With Insurance (Estimated Out-of-Pocket) |
|---|---|---|---|---|
| Dental Exam/Consultation | $50 | $150 | $250 | $0 - $50 (often fully covered or low co-pay) |
| Custom Night Guard | $300 | $550 | $800+ | $100 - $400 (after deductible, 50-80% coverage typical) |
| OTC Night Guard | $15 | $30 | $50 | Not Covered |
| Botox Injections (per session) | $400 | $700 | $1,000+ | $400 - $1,000+ (usually not covered) |
| Sleep Study (in-lab) | $1,000 | $2,500 | $5,000+ | $200 - $1,500+ (depends on deductible, co-pay) |
| Physical Therapy (per session) | $75 | $125 | $200 | $20 - $75 (with medical insurance co-pay) |
| Counseling (per session) | $75 | $150 | $250 | $20 - $60 (with medical insurance co-pay) |
Payment Plans and Financing Options
- Dental Office Payment Plans: Many dental practices offer internal payment plans, allowing patients to spread the cost of treatment over several months, often without interest.
- Third-Party Medical Financing: Companies like CareCredit or Alphaeon Credit specialize in healthcare financing. They offer credit cards specifically for medical and dental expenses, often with promotional periods of 0% interest if the balance is paid within a certain timeframe (e.g., 6, 12, 18, or 24 months). Be sure to understand the terms and conditions.
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): If you have access to these employer-sponsored plans, you can use pre-tax dollars to pay for qualified medical and dental expenses, including night guards, Botox (if for a medical condition), physical therapy, and even sleep studies. This can lead to significant tax savings.
Cost-Saving Tips
- Shop Around (Carefully): While a custom night guard from your dentist is recommended, comparing prices among reputable local dentists can sometimes yield savings.
- Ask for Discounts: Some dentists offer discounts for upfront payment or for patients without insurance.
- Utilize Preventative Care: Regular dental check-ups, typically covered by insurance, can help catch bruxism early before extensive and costly damage occurs.
- Address Underlying Causes: Investing in stress management or treating sleep apnea might seem like separate expenses, but they can prevent the need for more expensive dental restorations down the line.
- Understand Your Insurance: Before committing to any treatment, call your dental and medical insurance providers to understand your exact benefits, deductibles, co-pays, and annual maximums. Get prior authorization for expensive procedures if required.
Frequently Asked Questions
### Is teeth grinding bad for you?
Yes, chronic teeth grinding (bruxism) can be very damaging. It can lead to worn, chipped, or fractured teeth, increased tooth sensitivity, severe jaw pain, headaches, and can contribute to or worsen temporomandibular joint (TMJ) disorders. Long-term, it can necessitate extensive and costly dental restorative work.
### How can I stop teeth grinding naturally?
Natural approaches focus on addressing underlying causes. Stress reduction techniques like meditation, yoga, and deep breathing are highly effective. Improving sleep hygiene, avoiding stimulants like caffeine and alcohol, and consciously practicing jaw relaxation during the day can also significantly help. Some people find relief with warm compresses on the jaw or gentle jaw stretches.
### What is the best treatment for teeth grinding?
The "best" treatment depends on the individual and the cause. Custom-fitted night guards are often the most common and effective first-line treatment, protecting teeth and reducing jaw strain. For severe cases, Botox injections can significantly reduce muscle activity. Addressing underlying issues like stress, anxiety, or sleep apnea is crucial for long-term success.
### How much does it cost to stop teeth grinding?
Costs vary widely based on treatment. A custom night guard typically costs $300-$800+. Botox injections can be $400-$1,000+ per session. A sleep study to diagnose underlying sleep disorders might range from $500-$5,000. Less expensive options include over-the-counter night guards ($15-$50) or therapies like counseling ($75-$250 per session).
### Does insurance cover bruxism treatment?
Dental insurance often provides partial coverage (e.g., 50-80%) for custom-made night guards, after your deductible. Medical insurance may cover treatments for underlying conditions like sleep apnea or physical therapy for TMJ. However, Botox injections for bruxism are typically considered cosmetic and are generally not covered by insurance.
### How long does it take to stop teeth grinding?
Stopping teeth grinding is often a management process rather than an instant cure. While a night guard provides immediate protection, reducing the habit itself can take weeks to months of consistent effort, especially when addressing stress or adopting new habits. Botox effects last 3-6 months, requiring repeat treatments.
### Is bruxism pain permanent?
No, bruxism pain is typically not permanent, especially with appropriate treatment. While chronic grinding can cause persistent jaw pain and headaches, these symptoms usually subside significantly once an effective treatment plan (like a night guard, stress management, or Botox) is implemented and adhered to.
### Can orthodontics help with teeth grinding?
In some cases where a significant malocclusion (improper bite) is a contributing factor, orthodontic treatment (braces or aligners) might be considered to correct the bite. However, this is usually a long-term solution and not the primary treatment for bruxism unless other severe dental issues are also present. It's not a guaranteed solution to stop grinding.
### Can teeth grinding cause headaches?
Yes, teeth grinding is a very common cause of tension headaches, particularly those felt in the temples or radiating from the jaw and neck. The constant clenching and grinding overwork the jaw muscles, leading to muscle fatigue and referred pain that manifests as a headache, often noticeable upon waking.
### What is the difference between clenching and grinding?
Clenching involves pressing your upper and lower teeth together firmly, often without movement. Grinding involves rubbing your teeth back and forth against each other. Both are forms of bruxism and exert excessive force on the teeth and jaw, leading to similar types of damage and symptoms.
When to See a Dentist
It's crucial to seek professional dental advice if you suspect you might be grinding your teeth. Early detection and intervention can prevent significant damage and discomfort.
You should schedule a routine dental appointment if you notice any of the following signs:
- You wake up with a dull, constant headache or soreness in your jaw.
- Your teeth appear flattened, chipped, cracked, or excessively worn.
- You experience increased tooth sensitivity to hot or cold.
- Your bed partner complains about grinding sounds during the night.
- You notice indentations on your tongue or the inside of your cheeks.
- You have persistent facial pain or tenderness in your jaw muscles.
Seek a more urgent dental consultation (within a few days) if:
- You experience sudden, sharp pain in your jaw or teeth that limits your ability to chew or speak.
- Your jaw locks in an open or closed position.
- You suspect your grinding is leading to the fracture of existing dental work (fillings, crowns) or natural teeth.
When to seek immediate medical attention (emergency care) or contact your dentist immediately:
- If you experience severe, unrelenting jaw pain accompanied by swelling or fever.
- If your jaw suddenly dislocates and you cannot close your mouth.
Always remember that your dentist is your primary resource for diagnosing and managing bruxism. They can differentiate bruxism from other conditions and guide you toward the most appropriate treatment plan for your specific needs, helping you effectively stop teeth grinding and protect your oral health.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles

What Causes Teeth Grinding in Sleep
More than one in ten adults—and even more children—clench or grind their teeth during sleep, a condition known medically as sleep bruxism. For many, it's an unconscious habit that goes unnoticed until significant damage or discomfort arises. Waking up with a dull, constant headache, jaw pain, or
February 23, 2026
How to Not Grind Teeth at Night
More than one in ten adults and a significant percentage of children experience teeth grinding, medically known as bruxism, a condition that often goes unnoticed, especially when it occurs during sleep. If you've woken up with a sore jaw, a dull headache, or noticed your teeth becoming unusually
February 23, 2026

What Is Jaw Clenching
Do you often wake up with a dull headache, a sore jaw, or unexplained tooth sensitivity? You're not alone. Approximately 1 in 10 adults and up to 3 in 10 children experience some form of bruxism, a condition characterized by grinding, gnashing, or clenching your teeth. At the heart of this wides
February 23, 2026
Severe Bruxism Molars: Complete Guide
When the quiet of the night is shattered by a grinding, grating sound, or when you wake up with an aching jaw and teeth that feel oddly sensitive, it’s often a sign of bruxism. But what happens when this condition intensifies, leading to significant damage, especially to your back teeth? This is the
February 23, 2026