Tmj Splint: Complete Guide
Key Takeaways
- Are you experiencing persistent jaw pain, headaches, or difficulty opening and closing your mouth? You're not alone. Over 10 million Americans suffer from temporomandibular joint (TMJ) disorders, often leading to chronic discomfort in various tmj pain areas including the jaw, face, neck, and
Tmj Splint: Complete Guide
Are you experiencing persistent jaw pain, headaches, or difficulty opening and closing your mouth? You're not alone. Over 10 million Americans suffer from temporomandibular joint (TMJ) disorders, often leading to chronic discomfort in various tmj pain areas including the jaw, face, neck, and shoulders. For many, a tmj splint (also known as an occlusal splint or bite guard) offers a pathway to relief and improved quality of life. Unlike generic over-the-counter mouthguards, a custom-fitted TMJ splint is a precisely engineered oral appliance designed to address the underlying causes of your discomfort, reduce muscle tension, protect your teeth, and stabilize your jaw joint.

This comprehensive guide from SmilePedia.net will delve deep into everything you need to know about TMJ splints. We'll explore the different types available, the conditions they treat, the step-by-step process of getting one, expected costs, insurance considerations, and crucial aftercare. Our goal is to equip you with the knowledge to make informed decisions about your oral health and find lasting relief from TMD symptoms.
Key Takeaways:
- A TMJ splint is a custom-made oral appliance used to treat temporomandibular joint disorders (TMD) by stabilizing the jaw, reducing muscle tension, and protecting teeth from grinding/clenching.
- The two main types are stabilization splints (most common, worn primarily at night) and repositioning splints (used to alter jaw position, often worn more frequently).
- Costs for a custom TMJ splint in the US typically range from $300 to $2,500+, depending on the type, materials, complexity, and practitioner's fees.
- Insurance coverage for TMJ splints is variable; some medical plans may cover it for TMD treatment, while dental plans often have limitations. Pre-authorization is recommended.
- Treatment duration varies, with many patients experiencing relief within weeks to a few months, but consistent wear and follow-up adjustments are critical for long-term success.
- Potential risks include temporary discomfort and, in rare cases, changes in bite if not properly monitored, especially with repositioning splints.
- Always consult with a qualified dentist or oral surgeon for proper diagnosis and a personalized treatment plan.
What is a TMJ Splint? An Overview
A TMJ splint is a custom-fabricated oral appliance, often made of hard acrylic, that fits over your upper or lower teeth. Unlike athletic mouthguards that protect teeth from impact or over-the-counter nightguards that offer generalized protection against grinding, a TMJ splint is a therapeutic device precisely designed to address specific issues related to the temporomandibular joints (TMJs) and the muscles that control jaw movement.
The primary function of a TMJ splint is multifaceted:
- Stabilize the Jaw Joint: By providing a stable, even biting surface, it helps to properly seat the condyle (the rounded end of the jawbone) within the TMJ socket, reducing stress on the joint structures, including the articular disc.
- Reduce Muscle Activity: It can help relax the overactive jaw muscles (masseter and temporalis muscles) often responsible for clenching and grinding (bruxism), which are major contributors to TMD pain.
- Protect Teeth: While not its primary therapeutic role, a hard acrylic splint also serves to protect teeth from the destructive forces of bruxism, preventing wear, fractures, and sensitivity.
- Realign Bite (in specific cases): Certain types of splints aim to temporarily or permanently alter the jaw's position to improve the bite relationship, particularly when disc displacement is involved.
Essentially, a TMJ splint acts as an orthopedic appliance for your jaw. It creates a temporary, ideal bite relationship, allowing the jaw muscles to relax and the TMJs to rest in a more natural, unstrained position. This reduction in stress and muscle activity is key to alleviating the pain and dysfunction associated with temporomandibular disorders.
Understanding TMJ and TMD: The Root of the Problem
Before diving deeper into splint therapy, it's essential to understand the complex system a TMJ splint aims to regulate.
The Temporomandibular Joint (TMJ)
The temporomandibular joint (TMJ) is one of the most complex joints in the body. You have two TMJs, one on each side of your head, located just in front of your ears. These joints connect your lower jaw (mandible) to the temporal bone of your skull. The TMJs are unique in that they function as both a hinge (allowing up-and-down motion) and a gliding joint (allowing forward, backward, and side-to-side movements).
Within each joint, a small, oval-shaped piece of cartilage called the articular disc (or meniscus) acts as a cushion between the jawbone and the skull, ensuring smooth, frictionless movement. A network of muscles, ligaments, and nerves surrounds these joints, enabling chewing, speaking, and yawning.
Temporomandibular Disorders (TMD)
Temporomandibular Disorders (TMD) is a collective term for a range of conditions affecting the TMJs, the jaw muscles, and/or the surrounding nerves. It's important to note that "TMJ" refers to the joint itself, while "TMD" refers to the disorder.
TMD can manifest in a wide variety of symptoms, often affecting multiple tmj pain areas. This is because the jaw system is intimately connected to the head, neck, and ears. When the TMJs or associated muscles are not functioning correctly, it can lead to widespread discomfort.
Causes of TMJ Disorders
The exact cause of TMD is often difficult to pinpoint and can be multifactorial. Several factors can contribute to the development or exacerbation of these disorders:
- Bruxism (Teeth Grinding and Clenching): This is one of the most common contributing factors. Chronic clenching or grinding, especially during sleep (sleep bruxism), puts immense stress on the jaw joints, muscles, and teeth. Stress and anxiety are frequently linked to bruxism.
- Trauma: A direct blow to the jaw, head, or neck (e.g., from an accident, fall, or sports injury) can damage the TMJ, surrounding tissues, or jaw muscles. Whiplash injuries are also known to trigger TMD.
- Arthritis: Degenerative joint diseases like osteoarthritis can affect the TMJ, causing pain, stiffness, and reduced mobility. Inflammatory conditions like rheumatoid arthritis can also impact the joint.
- Disc Displacement: The articular disc within the TMJ can become displaced, either slipping forward or to the side. This can lead to clicking, popping, locking of the jaw, and pain.
- Malocclusion (Bad Bite): While historically considered a primary cause, modern research suggests that malocclusion alone is rarely the sole cause of TMD. However, a significant bite discrepancy can contribute to uneven forces on the TMJ and surrounding muscles.
- Stress and Tension: Psychological stress doesn't directly cause TMD but significantly exacerbates symptoms by increasing muscle tension and promoting clenching/grinding habits.
- Connective Tissue Diseases: Conditions that affect ligaments and cartilage throughout the body can also impact the TMJs.
- Poor Posture: Forward head posture can put strain on the neck and jaw muscles, contributing to TMD symptoms.
Signs and Symptoms of TMD: Recognizing the Need for a TMJ Splint
Recognizing the signs and symptoms of TMD is the first step toward seeking appropriate treatment. The presentation of TMD is highly varied, but common indicators often involve pain, sound, and functional limitations.
Pain and Tenderness
- Jaw Pain: Aching or throbbing pain in the jaw joint, often radiating to other tmj pain areas.
- Facial Pain: Dull, chronic aching across the face, especially in the cheekbones or temples.
- Headaches: Frequent tension headaches or even migraines, often originating near the temples or behind the eyes.
- Earaches: Pain in or around the ear that isn't due to an ear infection, sometimes accompanied by a feeling of fullness.
- Neck and Shoulder Pain: Pain and stiffness in the neck and shoulders, often due to referred pain from strained jaw muscles.
- Tooth Sensitivity: General tooth sensitivity not explained by decay or gum disease, often a result of excessive clenching or grinding.
Sounds
- Clicking or Popping: Sounds heard when opening or closing the mouth, often indicating disc displacement. This may or may not be painful.
- Grating Sounds (Crepitus): A grinding or crunching sound, which can suggest degenerative changes within the joint.
Functional Limitations
- Limited Jaw Movement: Difficulty fully opening the mouth, or a feeling of stiffness.
- Jaw Locking: The jaw getting "stuck" in an open or closed position, requiring manipulation to release.
- Difficulty Chewing: Pain or fatigue when chewing, especially tough or chewy foods.
- Tired Jaw Muscles: A persistent feeling of fatigue in the jaw muscles.
It's crucial to understand that while a patient might refer to a "TMJ pen" when describing their sharp or localized discomfort, the term "TMJ pen" isn't a medical device or a standard diagnostic tool. It's more likely a mispronunciation or a way for individuals to articulate the specific, often intense, nature of their tmj pain areas. The important aspect for diagnosis is accurately describing the location, intensity, and duration of the pain to your dental professional.
Types of TMJ Splints
TMJ splints are not one-size-fits-all. They are custom-made devices designed to address specific aspects of TMD. The most common types include stabilization splints and repositioning splints.
Stabilization Splint (Occlusal Orthotic or Flat Plane Splint)
- Purpose: This is the most commonly prescribed type of TMJ splint. Its primary goal is to provide a stable and even biting surface, which helps to relax the jaw muscles, protect the teeth from grinding and clenching, and allow the TMJ to rest in a more physiologically ideal position. It does not aim to permanently change the bite or jaw position.
- Design: Typically made of hard, clear acrylic, it covers all the teeth of either the upper or lower arch. The biting surface is flat, allowing all opposing teeth to contact it simultaneously and evenly.
- How it Works: By creating a perfect, balanced bite when worn, it encourages the jaw muscles to de-program from their learned, often dysfunctional, patterns of clenching and grinding. This reduces muscle hyperactivity and the associated pain.
- Wear Schedule: Most commonly worn at night, when involuntary grinding and clenching are prevalent. In some severe cases, a dentist might recommend daytime wear for a limited period.
- Pros: Highly effective for muscle-related TMD, bruxism, and generalized joint pain. Non-invasive and completely reversible.
- Cons: Requires consistent wear for effectiveness. Can initially feel bulky. Doesn't directly address disc displacement issues.
- Typical Cost: $300 - $1,500
Repositioning Splint (Anterior Repositioning Splint)
- Purpose: This type of splint is designed to guide the lower jaw into a specific forward or downward position. It's primarily used when there is a displaced articular disc within the TMJ, aiming to temporarily or, in some cases, facilitate the return of the disc to a more normal position.
- Design: Also typically made of hard acrylic, but its biting surface is not flat. It has ramps, indentations, or inclines that guide the lower jaw into a predetermined position.
- How it Works: By forcing the jaw into a specific position, it aims to "capture" the displaced disc, thereby eliminating clicking, popping, and improving joint function.
- Wear Schedule: Often worn more frequently than stabilization splints, sometimes even 24/7, with breaks only for eating and oral hygiene. Close monitoring is essential due to the potential for bite changes.
- Pros: Can be very effective for specific disc displacement conditions and severe jaw locking.
- Cons: Can lead to permanent changes in bite if not carefully managed and monitored, potentially requiring further orthodontic or restorative treatment. Requires a highly skilled practitioner and strict patient compliance.
- Typical Cost: $800 - $2,500+ due to complexity and closer monitoring requirements.
Soft/Resilient Splints
- Purpose: These are often softer, rubbery appliances, sometimes used for very short-term relief from acute muscle soreness.
- Design: Made from a flexible, pliable material.
- How it Works: Provides a cushion, but its soft nature can actually encourage clenching in some individuals, as the jaw muscles instinctively bite harder into a soft surface.
- Pros: Less expensive, more comfortable initially.
- Cons: Not recommended for long-term use as they can worsen bruxism over time by providing a soft surface to bite into. They don't provide the stable orthopedic support of a hard splint.
NTI-tss (Nociceptive Trigeminal Inhibition Tension Suppression System)
- Purpose: A specific type of anterior deprogrammer, the NTI-tss device prevents the back molars from coming into contact, thus inhibiting the temporal and masseter muscles from clenching with full force.
- Design: A small, custom-made device that fits over the two front upper or lower teeth.
- How it Works: By eliminating posterior tooth contact, it aims to reduce clenching intensity and relieve tension headaches and migraines related to bruxism.
- Pros: Small, less bulky than full coverage splints. Can be very effective for clenching-related headaches.
- Cons: Doesn't address all TMD issues. Potential for creating an open bite if not carefully used and monitored, as the posterior teeth can super-erupt over time if not in contact.
- Typical Cost: $300 - $800
The TMJ Splint Process: What to Expect
Getting a custom TMJ splint involves several crucial steps, emphasizing proper diagnosis and precise fabrication.
Initial Consultation and Diagnosis
Your journey begins with a thorough evaluation by a dentist or oral surgeon experienced in TMD.
- Detailed History: The dentist will ask about your symptoms (e.g., specific tmj pain areas, clicking, headaches), their duration, severity, and any aggravating or relieving factors. They will also inquire about your medical history, stress levels, and habits like teeth grinding.
- Physical Examination: This involves carefully examining your jaw joints by feeling them as you open and close your mouth, listening for sounds (clicks, pops, grating), and palpating (feeling) your jaw muscles for tenderness or spasm. Your range of motion will be assessed.
- Imaging: X-rays (panoramic), CT scans, or MRI scans may be ordered to visualize the TMJ bones, disc position, and rule out other pathologies. An MRI is particularly useful for assessing the soft tissues of the joint, including the disc.
- Diagnosis: Based on this comprehensive assessment, the dentist will arrive at a diagnosis of your specific TMD type (e.g., myofascial pain, disc displacement with reduction, degenerative joint disease). This diagnosis will guide the choice of splint and overall treatment plan.
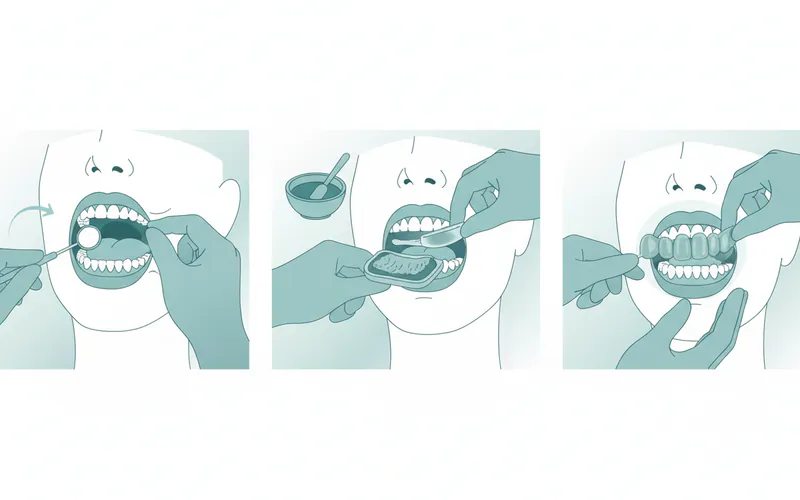
Impression Taking and Fabrication
Once a splint type is chosen, the fabrication process begins.
- Dental Impressions: Precise impressions (molds) of your teeth are taken. This can be done using traditional putty-like material or modern digital scanners. Accuracy here is paramount for a well-fitting splint.
- Bite Registration: The dentist will record your bite relationship, often using a wax wafer or other devices to capture how your upper and lower teeth meet. For some splints, they will guide your jaw into a specific therapeutic position.
- Lab Fabrication: The impressions and bite registration are sent to a specialized dental laboratory. Skilled technicians will then custom-fabricate your splint from hard acrylic, ensuring it precisely fits your teeth and meets the dentist's specifications for the desired occlusal (biting) surface.
Fitting and Adjustment
This is a critical phase where the splint is fine-tuned for optimal comfort and function.
- First Fitting: When your splint is ready, you'll return for a fitting appointment. The dentist will ensure the splint fits snugly but comfortably. They will check the bite carefully, making sure all opposing teeth contact the splint evenly and simultaneously (for stabilization splints) or that the jaw is guided to the correct position (for repositioning splints).
- Adjustments: It's common for several adjustment appointments to be needed over the first few weeks or months. As your jaw muscles relax and the joint adapts, your bite may change slightly, requiring further grinding and polishing of the splint's surface. These adjustments are vital for the splint's effectiveness and your long-term comfort.
- Wearing Instructions: You'll receive detailed instructions on when and how long to wear your splint (e.g., every night, certain hours during the day).
Follow-up and Monitoring
- Regular Check-ups: Consistent follow-up appointments are essential to monitor your progress, assess symptom relief, and make any necessary adjustments to the splint or your overall treatment plan. This allows the dentist to ensure the splint is achieving its therapeutic goals and that no adverse changes to your bite are occurring.
- Pro Tip: Be diligent in keeping all your follow-up appointments. Missing them can compromise the effectiveness of your splint therapy and potentially lead to new issues.
Treatment Options Beyond Splints: A Holistic Approach
While a TMJ splint is a highly effective treatment for many TMD sufferers, it's often part of a broader, holistic treatment plan. Depending on the specific diagnosis and severity of your condition, your dentist or oral surgeon may recommend combining splint therapy with other conservative treatments.
Conservative Therapies
These are often the first line of defense and focus on pain relief, muscle relaxation, and lifestyle modification.
- Pain Relievers: Over-the-counter non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen or naproxen can help manage pain and inflammation. In some cases, prescription-strength pain medication or muscle relaxants may be prescribed for short periods to break the cycle of pain and muscle spasm.
- Heat and Cold Therapy: Applying moist heat to the jaw and neck can relax tight muscles, while cold packs can help reduce inflammation and acute pain.
- Soft Diet: Avoiding hard, chewy, or crunchy foods can give your jaw muscles and joints a rest, especially during flare-ups.
- Stress Management: Techniques like biofeedback, meditation, yoga, and counseling can significantly reduce muscle tension and bruxism, which are often stress-related.
- Physical Therapy: Specific exercises to stretch and strengthen jaw muscles, improve posture, and increase range of motion can be highly beneficial. A physical therapist may also employ techniques like massage, ultrasound, or transcutaneous electrical nerve stimulation (TENS).
- Lifestyle Modifications: Avoiding extreme jaw movements (e.g., wide yawning, yelling), practicing good posture, and being mindful of clenching habits throughout the day.
- Pro Tip: If you notice yourself clenching during the day, try placing your tongue gently on the roof of your mouth behind your upper front teeth, and keep your teeth slightly apart. This helps relax your jaw muscles.
Injections
For localized pain and muscle spasm, injections can offer targeted relief.
- Corticosteroid Injections: Injected directly into the TMJ, these can reduce inflammation and pain within the joint, particularly in cases of arthritis or severe inflammation.
- Botulinum Toxin (Botox) Injections: When injected into hyperactive jaw muscles (masseter and temporalis), Botox can temporarily relax these muscles, significantly reducing clenching, grinding, and associated pain and headaches. Effects typically last for 3-6 months.
TMJ Surgery (Last Resort)
Surgical intervention is generally considered only when conservative treatments have failed and there is significant structural damage to the joint.
- Arthrocentesis: A minimally invasive procedure where needles are inserted into the joint to flush it with sterile fluid, removing inflammatory byproducts and potentially freeing a stuck disc.
- Arthroscopy: A minimally invasive procedure using a small camera (arthroscope) to visualize and, in some cases, repair damaged joint tissues.
- Open-Joint Surgery: Traditional surgery that involves a larger incision to directly access and repair or replace the joint structures. This is reserved for the most severe cases, such as severe degeneration, extensive scar tissue, or complete fusion of the joint (ankylosis).
Comparison Table of Common TMD Treatment Options
| Treatment Option | Primary Goal | Pros | Cons | Typical Timeline |
|---|---|---|---|---|
| TMJ Splint | Stabilize joint, relax muscles, protect teeth | Non-invasive, reversible, often highly effective for bruxism and muscle pain | Requires compliance, initial discomfort, multiple adjustments | Weeks to months |
| Pain Relievers/Muscle Relaxants | Symptom management, reduce inflammation | Quick relief, accessible | Temporary solution, side effects, doesn't address root cause | Short-term |
| Physical Therapy | Muscle rehabilitation, posture, range of motion | Non-invasive, addresses functional issues, empowers patient | Requires commitment, slower results | Weeks to months |
| Botox Injections | Reduce muscle hyper-activity | Effective for muscle-related pain/headaches, quick procedure | Temporary (3-6 months), cost, potential side effects | 3-6 months |
| Arthrocentesis/Arthroscopy | Clean/repair joint minimally invasively | Minimally invasive surgical option | Requires anesthesia, some recovery time, not for all TMD | Days to weeks |
| Open-Joint Surgery | Extensive joint repair/replacement | Can resolve severe structural issues | Highly invasive, significant recovery, last resort, risks of surgery | Months |
Cost of TMJ Splints and Insurance Coverage (US Market)
Understanding the financial aspect of TMJ splint therapy is a significant concern for many patients. The cost can vary widely, and insurance coverage is not always straightforward.

Average Costs for TMJ Splints
The price of a custom TMJ splint in the United States generally reflects the type of splint, the materials used, the complexity of its fabrication, and the fees charged by the dental professional and the laboratory.
- Stabilization Splint (Most Common): Expect to pay between $300 and $1,500. Factors at the higher end of this range might include highly specialized materials, advanced diagnostic techniques, or a practitioner with extensive TMD expertise.
- Repositioning Splint: Due to their intricate design and the need for more frequent and precise adjustments, these splints typically cost more, ranging from $800 to $2,500+. Some complex cases requiring extensive monitoring and multiple phases of treatment could exceed this.
- NTI-tss Device: These smaller appliances are generally less expensive, falling in the range of $300 to $800.
Factors Influencing Cost:
- Geographic Location: Costs can vary significantly by state and even by metropolitan area.
- Dentist's Experience/Specialization: Dentists with advanced training in TMD or those who specialize in oral and maxillofacial pain may charge higher fees.
- Materials and Lab Fees: High-quality, durable acrylic and skilled laboratory fabrication contribute to the overall cost.
- Number of Adjustments: While initial adjustments are usually included, extensive or long-term adjustments might incur additional fees.
- Diagnostic Procedures: The cost of initial consultations, X-rays, CT scans, or MRIs are typically separate from the splint cost.
Insurance Coverage
Navigating insurance coverage for TMJ splints can be complex, as it often falls into a grey area between dental and medical insurance.
- Dental Insurance: Many standard dental plans classify TMJ splints as "orthodontic appliances" or "removable prosthodontics." Coverage can be limited or subject to significant deductibles and co-pays. Some plans may not cover them at all, viewing them as a "medical" issue rather than purely "dental."
- Medical Insurance: Some medical insurance plans may offer coverage for TMD treatment, including splints, especially if the disorder is diagnosed as a medical condition (e.g., chronic pain, inflammatory arthritis of the TMJ). However, these plans often require:
- Pre-authorization: A crucial step where your dentist submits documentation to your medical insurer to justify the medical necessity of the splint before treatment begins.
- Specific Diagnostic Codes: The diagnosis must align with codes accepted by your medical insurer for coverage.
- "Medical Necessity": The splint must be proven to be medically necessary to treat a diagnosed condition rather than solely for aesthetic or orthodontic purposes.
- In-Network vs. Out-of-Network: Check if your dentist is in-network with your medical or dental plan, as this significantly impacts your out-of-pocket costs.
- Pro Tip: Always contact your insurance provider (both medical and dental) directly before starting treatment. Ask for a detailed explanation of what is covered, any limitations, deductibles, co-pays, and whether pre-authorization is required. Request all information in writing.
Payment Plans and Financing Options
If insurance coverage is limited, many dental offices offer or partner with financing options:
- CareCredit, Alphaeon Credit, LendingClub: These are common healthcare credit cards that offer low or no-interest payment plans for a specified period.
- In-Office Payment Plans: Some practices allow patients to pay for treatment in installments directly with the office.
- Flexible Spending Accounts (FSAs) and Health Savings Accounts (HSAs): These tax-advantaged accounts can be used to pay for qualified medical and dental expenses, including TMJ splints, using pre-tax dollars.
Recovery and Aftercare: Living with Your TMJ Splint
Once you receive your custom TMJ splint, consistent wear and proper care are crucial for successful treatment and long-term relief.
Initial Adjustment Period
- Temporary Discomfort: It's normal to experience some initial discomfort, pressure, or soreness in your teeth, gums, or jaw muscles for the first few days or weeks. This is your mouth adjusting to the new appliance.
- Speech Changes: You might find your speech slightly affected initially, especially with full-arch splints. Practice speaking with it in to adapt quicker.
- Increased Salivation: Some people experience temporary increased saliva production as their mouth registers the new object. This typically subsides.
- Compliance is Key: Follow your dentist's wear instructions precisely. Sporadic wear can hinder progress and even make symptoms worse.
Cleaning and Maintenance
Proper hygiene for your splint is essential to prevent bacterial buildup, odors, and maintain its integrity.
- Daily Cleaning:
- Rinse your splint thoroughly under cool water every time you remove it.
- Brush it gently with a soft-bristled toothbrush and a non-abrasive soap (like hand soap or dish soap) or a specialized denture/retainer cleaner. Avoid toothpaste, as it can be too abrasive and scratch the acrylic, creating porous surfaces for bacteria to accumulate.
- Soaking: Your dentist may recommend soaking your splint periodically (e.g., once a week) in a denture cleaner or a solution specifically designed for oral appliances. Follow product instructions carefully.
- Storage: When not in your mouth, store your splint in a clean, dry, protective case. Avoid wrapping it in tissues, as it can easily be accidentally discarded. Keep it away from pets and extreme heat, which can warp the acrylic.
- Pro Tip: Never use hot water to clean or rinse your splint, as this can cause the acrylic to warp and ruin its custom fit.
Long-term Care
- Regular Dental Check-ups: Continue with your routine dental check-ups, and bring your splint with you. Your dentist will check its condition, assess your bite, and monitor your TMD symptoms.
- Monitoring Symptoms: Pay attention to any changes in your jaw pain, clicking, or overall comfort. Report these to your dentist immediately.
- Addressing Underlying Causes: Remember that a splint manages symptoms. Continue to address any underlying causes, such as stress, poor posture, or bruxism, through appropriate therapies.
- Splint Replacement: Splints are durable but not indestructible. Over time, they can wear down, crack, or become ill-fitting. Your dentist will advise you when a replacement is needed, typically every few years depending on wear and tear.
Preventing TMD and the Need for a TMJ Splint
While not all causes of TMD are preventable, many cases are linked to habits and lifestyle factors that can be managed. Proactive steps can significantly reduce your risk of developing TMD or minimize its severity.
- Stress Management: Since stress is a major trigger for bruxism and muscle tension, incorporating stress-reducing techniques into your daily life is crucial. This could include meditation, yoga, deep breathing exercises, regular exercise, or seeking professional counseling.
- Awareness of Jaw Habits: Become mindful of habits like clenching your teeth, grinding, nail biting, lip chewing, or chewing on pens. When you catch yourself, gently separate your teeth and let your jaw muscles relax.
- Avoid Excessive Jaw Movements: Try not to open your mouth excessively wide (e.g., during yawning or eating large foods). Cut food into smaller pieces. Avoid chewing gum frequently, as this can overwork jaw muscles.
- Good Posture: Maintain proper posture, especially when working at a computer or sitting for long periods. Slouching or forward head posture can strain neck and jaw muscles. Ensure your computer screen is at eye level and your chair provides good lumbar support.
- Ergonomics: Set up your workspace ergonomically to minimize strain on your neck and shoulders.
- Regular Dental Check-ups: Regular visits allow your dentist to identify early signs of bruxism, tooth wear, or jaw joint issues before they escalate into full-blown TMD.
- Proper Nutrition and Hydration: A balanced diet and adequate hydration support overall muscle and joint health.
Risks and Complications of TMJ Splint Therapy
While TMJ splints are generally safe and effective, it's important to be aware of potential risks and complications, especially with long-term use or certain types of splints.
- Temporary Discomfort: As mentioned, initial soreness or pressure is common but usually resolves as your mouth adjusts.
- Changes in Bite (Occlusal Changes): This is the most significant potential complication, particularly with repositioning splints or if any type of splint is poorly designed or adjusted. If a splint constantly forces your jaw into a different position, your teeth may gradually shift, leading to a permanent change in your bite. This can necessitate further orthodontic treatment or restorative dentistry to correct. Close monitoring by your dentist is crucial to prevent this.
- Speech Difficulties: Temporary slurring or lisping can occur, especially with bulkier splints.
- Increased Salivation or Dry Mouth: Some individuals experience a temporary increase in saliva production, while others may notice dry mouth, particularly at night.
- Lack of Improvement or Worsening of Symptoms: If the diagnosis is incorrect, the splint is ill-fitting, or the patient is not compliant with wear instructions, the splint may not provide relief and could potentially exacerbate symptoms.
- Allergic Reactions: Though rare, some individuals may have an allergic reaction to the acrylic material used in the splint.
- Damage to Teeth or Existing Dental Work: An ill-fitting or improperly adjusted splint can put excessive pressure on certain teeth or dental restorations, potentially causing chips, cracks, or loosening.
- Dependence: In some cases, patients may become overly reliant on the splint, fearing discomfort if they don't wear it. This highlights the importance of addressing the root causes of TMD alongside splint therapy.
Comparison of TMJ Splint Types
This table provides a concise overview of the key differences between the primary types of TMJ splints.
| Feature | Stabilization Splint (Occlusal Orthotic) | Repositioning Splint (Anterior Repositioning) | NTI-tss Device |
|---|---|---|---|
| Primary Purpose | Muscle relaxation, joint stabilization, protection from bruxism | Repositioning a displaced articular disc, altering jaw position | Prevents molar contact, reduces clenching intensity for headaches |
| Design | Hard acrylic, covers all teeth on one arch, flat biting surface | Hard acrylic, covers all teeth on one arch, ramps/inclines to guide jaw position | Small, covers 2-4 front teeth, prevents posterior tooth contact |
| Wear Schedule | Primarily nightly, sometimes limited daytime wear for severe cases | Often more frequent (e.g., 24/7 with breaks for eating) for weeks/months | Primarily nightly |
| Mechanism | De-programs muscles by creating an ideal bite, reduces joint stress | Forces jaw into a specific forward/downward position to "capture" disc | Prevents full clenching power of masseter/temporalis muscles |
| Reversibility | Completely reversible (no permanent bite changes if properly used) | Can lead to permanent bite changes if not carefully managed and phased out | Potential for open bite if not properly used and monitored |
| Effectiveness | High for muscle-related pain, bruxism, general joint pain | High for specific disc displacement with reduction, jaw locking | High for clenching-related headaches/migraines |
| Typical US Cost | $300 - $1,500 | $800 - $2,500+ | $300 - $800 |
Children and Pediatric Considerations for TMJ Disorders
TMJ disorders are not exclusive to adults; they can also affect children and adolescents. While less common, the prevalence of TMD symptoms in children is estimated to be between 6% and 15%, with some studies showing higher rates for specific symptoms like clicking. Recognizing TMD in children requires careful attention, as symptoms may present differently or be more subtle than in adults.
Causes in Children
- Trauma: Injuries to the jaw or head from falls, sports, or accidents are a significant cause.
- Bruxism: Teeth grinding and clenching, often stress-related or associated with sleep disorders, can put strain on developing TMJs.
- Malocclusion: While not always the primary cause, severe bite problems can contribute.
- Habits: Thumb-sucking, prolonged pacifier use, or lip/nail biting can sometimes contribute.
- Orthodontic Treatment: In rare cases, aggressive or improperly managed orthodontic treatment might exacerbate or reveal underlying TMJ issues.
- Systemic Conditions: Juvenile idiopathic arthritis or other inflammatory conditions can affect the TMJs.
Signs and Symptoms in Children
- Pain: Children might complain of headaches, earaches, or pain in the jaw or face. They may describe it as a "sore jaw" or refuse to eat certain foods.
- Clicking/Popping: Audible sounds in the jaw joint when opening or closing. Parents might notice this during eating.
- Difficulty Chewing: Reluctance to chew tough foods, or complaints of jaw fatigue while eating.
- Limited Opening: Difficulty opening the mouth wide, which parents might observe during brushing or eating.
- Facial Swelling: In some cases, inflammation can lead to minor swelling around the jaw joint.
- Changes in Bite: Parents might notice a shift in how their child's teeth fit together.
Treatment in Children
Treatment for TMD in children typically focuses on the most conservative and reversible approaches first, given their ongoing growth and development.
- Conservative Management: This includes soft diets, warm compresses, anti-inflammatory medications (if prescribed by a pediatrician), and stress reduction techniques.
- Physical Therapy: Gentle jaw exercises can help improve muscle function and flexibility.
- Occlusal Splints (TMJ Splints): Splints can be used in children, but their design and wear schedule are carefully considered. A stabilization splint might be used to relieve muscle pain and protect teeth from bruxism. Repositioning splints are generally used with extreme caution due to the potential for altering a developing bite. The splint must be regularly monitored and adjusted as the child's jaw grows.
- Behavioral Therapy: Addressing habits like bruxism or clenching through awareness and relaxation techniques.
- Orthodontic Assessment: If malocclusion is a significant contributing factor, an orthodontist may be consulted, but orthodontic treatment is usually initiated after acute TMD symptoms are managed.
- Early Intervention: Addressing TMD early in children is crucial to prevent chronic issues and minimize impact on growth and development. Parents should consult a pediatric dentist or an oral surgeon specializing in TMD if they suspect their child has symptoms.
Frequently Asked Questions
How long does it take for a TMJ splint to work?
The timeline for relief varies widely among individuals. Many patients experience significant reduction in pain and symptoms within a few days to a few weeks of consistent splint use. However, full therapeutic effects, such as muscle de-programming and joint stabilization, can take several weeks to a few months. Long-term success also depends on adherence to the wearing schedule and follow-up adjustments.
Is wearing a TMJ splint painful?
Initially, you may experience some temporary discomfort, pressure, or soreness in your teeth, gums, or jaw muscles as your mouth adjusts to the new appliance. This is normal and usually subsides within a few days to a couple of weeks. If pain is severe or persistent, it's crucial to contact your dentist immediately, as the splint may need an adjustment.
Can a TMJ splint change my bite permanently?
A stabilization splint, when properly designed and monitored, should not cause permanent changes to your bite. Its purpose is to create a temporary ideal bite. However, repositioning splints, which aim to alter jaw position, carry a higher risk of permanent bite changes if not carefully managed, requiring further dental intervention. Close monitoring by an experienced dentist is essential to mitigate this risk.
What are the alternatives to a TMJ splint?
Alternatives to a TMJ splint include a range of conservative therapies such as pain relievers, muscle relaxants, physical therapy, stress management techniques, dietary modifications, and Botox injections. In severe, recalcitrant cases, surgical options like arthrocentesis, arthroscopy, or open-joint surgery may be considered as a last resort. The best alternative depends on the specific diagnosis and severity of your TMD.
How often do I need to wear my TMJ splint?
The wearing schedule is highly individualized and depends on the type of splint and your specific diagnosis. Most stabilization splints are worn primarily at night to prevent sleep bruxism. Repositioning splints, used for disc displacement, may require more frequent wear, sometimes even during the day, for a specific period. Always follow your dentist's precise instructions regarding your wear schedule.
Can I eat with my TMJ splint in?
Generally, no. Most TMJ splints are designed to be removed before eating. Eating with the splint in can damage the appliance, make chewing difficult, and complicate cleaning. Your dentist will provide specific instructions for your splint type, but removal for meals is standard practice.
How do I clean my TMJ splint?
You should clean your TMJ splint every time you remove it. Rinse it under cool water and gently brush it with a soft-bristled toothbrush and a non-abrasive hand soap or dish soap. Avoid using toothpaste, as its abrasive particles can scratch the acrylic. Your dentist may also recommend soaking your splint periodically in a specialized denture or retainer cleaning solution.
Will my insurance cover a TMJ splint?
Insurance coverage for TMJ splints is variable and depends on your specific dental and medical insurance plans. Some dental plans may offer limited coverage for "orthodontic appliances," while some medical plans may cover it if the TMD is classified as a medical condition and deemed medically necessary. Always contact both your dental and medical insurance providers for pre-authorization and a detailed explanation of benefits before starting treatment.
What is a "TMJ pen"?
The term "TMJ pen" is not a recognized medical term or device. It's possible it's a misspelling or misunderstanding of "TMJ pain" or "TMJ pain areas." It could also be a colloquial reference to a personal pain relief tool or a way to describe sharp, localized TMJ pain. When discussing your symptoms, it's best to describe your tmj pain areas and its characteristics (e.g., sharp, dull, throbbing) clearly to your dental professional for accurate diagnosis and treatment.
When to See a Dentist
Recognizing when to seek professional dental attention for jaw issues is crucial for preventing chronic pain and potential worsening of conditions.
You should schedule a routine appointment with your dentist if you experience any of the following:
- Persistent Jaw Pain: If you have chronic aching or tenderness in your jaw, face, neck, or around your ears that doesn't resolve with basic home care (like soft diet or warm compresses).
- Clicking, Popping, or Grating Sounds: If you consistently hear sounds from your jaw joint when opening or closing your mouth, even if they aren't painful.
- Difficulty Opening/Closing Mouth: If you notice a limited range of motion when opening your mouth, or a feeling of stiffness.
- Frequent Headaches or Earaches: If you experience headaches or earaches that don't have an identifiable cause (like vision problems or an ear infection).
- Unexplained Tooth Sensitivity or Wear: If your teeth are suddenly sensitive or you notice unusual wear patterns, especially if you suspect you're grinding or clenching.
You should seek immediate attention (or consider it an emergency, depending on severity) if you experience these red flags:
- Jaw Locks Open or Closed: If your jaw gets painfully stuck in an open or closed position and you cannot release it yourself. This may require immediate medical or dental intervention.
- Sudden, Severe Pain: A sudden onset of excruciating jaw pain, especially if accompanied by swelling.
- Difficulty Swallowing or Breathing: While rare for TMD, if jaw issues impact your ability to swallow or breathe, seek emergency medical care immediately.
- Facial Swelling with Fever: This could indicate an infection and requires urgent medical attention.
Don't wait for your symptoms to become debilitating. Early diagnosis and intervention by a qualified dental professional can often lead to more straightforward and effective treatment, preventing long-term complications and improving your overall quality of life. Always consult with a dentist or oral surgeon experienced in TMD for an accurate diagnosis and personalized treatment plan.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Tmj Massage Near Me: Complete Guide
Temporomandibular joint disorder, commonly known as TMJD, affects millions of Americans, causing debilitating pain, discomfort, and significantly impacting quality of life. If you're experiencing jaw pain, clicking, or difficulty chewing, you're not alone. Up to 15% of American adults experience
February 23, 2026
Tmd Treatment: Complete Guide
Experiencing persistent jaw pain, clicking sounds when you chew, or debilitating headaches that seem to originate from your face? You're not alone. Temporomandibular joint (TMJ) disorders, often referred to collectively as TMD, affect an estimated 10 million Americans, with women disproportionat
February 23, 2026
Tmj Nerve Damage Symptoms: Complete Guide
Experiencing persistent facial pain, numbness, or tingling can be distressing, especially when the source is unclear. While many people are familiar with general jaw pain associated with temporomandibular joint (TMJ) disorders, the less commonly understood aspect of tmj nerve damage symptoms can
February 23, 2026
Remi Night Guard: Complete Guide
Remi Night Guard: Complete Guide
February 23, 2026