Adult Tooth Eruption Chart: Complete Guide
Key Takeaways
- Did you know that by the age of 18, most adults have 28 permanent teeth, with an additional four wisdom teeth often making an appearance later? The process of teeth emerging through the gums, known as tooth eruption, is a carefully orchestrated biological event, even in adulthood. While we typically
Adult Tooth Eruption Chart: Complete Guide
Did you know that by the age of 18, most adults have 28 permanent teeth, with an additional four wisdom teeth often making an appearance later? The process of teeth emerging through the gums, known as tooth eruption, is a carefully orchestrated biological event, even in adulthood. While we typically associate eruption charts with baby teeth, understanding the adult tooth eruption chart is crucial for monitoring your oral health, identifying potential issues, and ensuring a lifetime of healthy smiles. This comprehensive guide from SmilePedia.net will demystify the stages of tooth eruption, explain what to expect, and highlight when professional dental care is needed. We’ll delve into everything from the fascinating biology behind tooth development to the common challenges like impacted wisdom teeth, offering insights into prevention, treatment, and costs.

Key Takeaways:
- Permanent Teeth Count: Adults typically have 32 permanent teeth, including four wisdom teeth, though many have wisdom teeth removed or never develop them.
- Eruption Timeline: The first permanent molars usually emerge around 6-7 years old, and the process continues until wisdom teeth erupt between 17-21 years old.
- Wisdom Teeth: These are the most common teeth to become impacted, meaning they don't fully erupt, often requiring surgical extraction. Costs for impacted wisdom tooth removal range from $225-$600 per tooth.
- Signs of Trouble: Persistent pain, swelling, difficulty chewing, or visible misalignment in adult teeth can indicate eruption problems like impaction or crowding.
- Early Intervention: Regular dental check-ups, especially during adolescence, are vital for monitoring eruption patterns and addressing issues like crowding or impaction before they become severe.
- Costs: Dental treatments for eruption issues can vary widely. Orthodontics (braces/aligners) typically cost $3,000-$8,000, while surgical exposure of an impacted tooth can range from $300-$1,000.
- Insurance Coverage: Many dental insurance plans cover a portion of diagnostic X-rays, consultations, and necessary extractions or orthodontic treatments, but coverage varies significantly.
What It Is / Overview
Tooth eruption is the biological process by which teeth move from their developmental position within the jawbone into the oral cavity, becoming visible and functional. While the initial eruption of primary (baby) teeth is a well-known phenomenon starting around six months of age, adults also experience distinct stages of tooth eruption as their permanent teeth replace the deciduous set. The adult tooth eruption chart outlines the typical chronological sequence and age ranges when each of your 32 permanent teeth is expected to emerge.
This chart serves as a critical reference for dentists, orthodontists, and even patients, providing a benchmark for normal development. Understanding this timeline helps in identifying deviations, such as delayed eruption, impaction, or malocclusion (improper bite), which can lead to various dental health issues if left unaddressed. Each tooth type – incisors, canines, premolars, and molars – has a general window of eruption, influenced by genetics, nutrition, overall health, and the space available in the jaw.
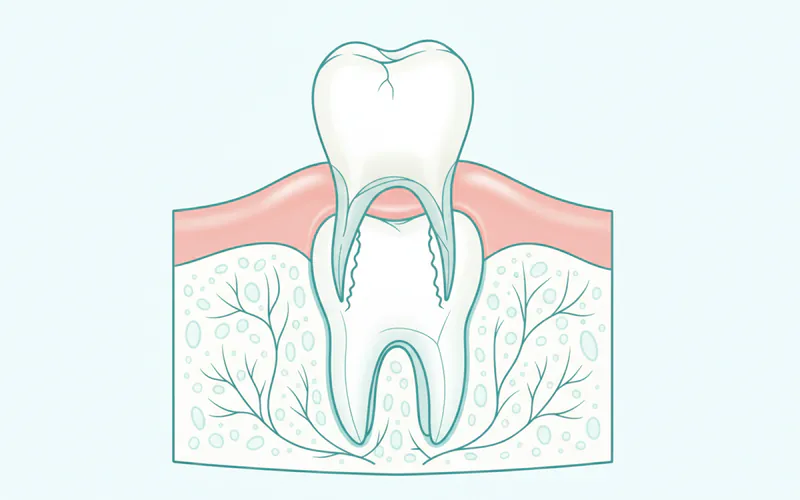
The Journey of a Permanent Tooth
The development of permanent teeth begins even before birth, with tooth buds forming deep within the jawbones. As primary teeth fall out (exfoliate), often spurred by the developing permanent tooth beneath it, the permanent tooth begins its ascent. This intricate process involves:
- Resorption of Primary Tooth Roots: The root of the primary tooth is gradually dissolved, loosening the tooth until it falls out.
- Formation of the Permanent Tooth Root: The root of the permanent tooth continues to develop, pushing the crown upwards.
- Movement Through Bone and Gum Tissue: The tooth travels through the alveolar bone and then penetrates the gum tissue, finally becoming visible in the mouth.
This entire process is carefully regulated by a complex interplay of cellular and molecular signals.
Types / Variations in Adult Tooth Eruption
While there's a general timeline for permanent tooth eruption, it's important to understand that individual experiences can vary. Not everyone follows the chart precisely, and there are several "variations" or specific scenarios that dental professionals look for.
Normal Eruption Sequence
The most common sequence for permanent tooth eruption in adults, following the loss of primary teeth, is as follows:
- First Molars: Often called "6-year molars," these are the first permanent teeth to erupt, behind the last primary molars. They typically appear between 6 and 7 years of age.
- Central Incisors: The front two teeth, usually between 6 and 8 years.
- Lateral Incisors: The teeth next to the central incisors, between 7 and 9 years.
- Canines (Cuspids): The pointed "eye teeth," usually between 9 and 12 years.
- First Premolars (Bicuspids): These replace the first primary molars, between 9 and 11 years.
- Second Premolars (Bicuspids): Replacing the second primary molars, between 10 and 12 years.
- Second Molars: Often called "12-year molars," these appear behind the first molars, between 11 and 13 years.
- Third Molars (Wisdom Teeth): These are the last teeth to erupt, at the very back of the mouth, typically between 17 and 21 years. Many adults do not develop all four wisdom teeth, or they may become impacted.
Delayed Eruption
Delayed eruption occurs when a tooth takes longer than the average timeframe to emerge. This can affect a single tooth or multiple teeth.
- Causes: Genetic factors, systemic conditions (e.g., hypothyroidism, Down syndrome), nutritional deficiencies, obstructions (such as a cyst or supernumerary tooth), or thick gum tissue.
- Consequences: Can lead to orthodontic problems, overcrowding, or functional bite issues.
Impaction
Impaction is a common variation, particularly with wisdom teeth, but can affect any tooth (most commonly canines). An impacted tooth is one that is blocked from fully erupting into its proper position.
- Causes: Lack of space in the jaw, obstruction by adjacent teeth, abnormal eruption angle, or genetic predisposition.
- Consequences: Pain, infection (pericoronitis), damage to adjacent teeth, cyst formation, or tumors.
Ectopic Eruption
Ectopic eruption occurs when a tooth erupts in an abnormal position, often outside its normal alignment.
- Causes: Jaw discrepancies, genetic factors, or developmental abnormalities.
- Consequences: Can lead to crowding, difficulty cleaning, and aesthetic concerns.
Supernumerary Teeth (Hyperdontia)
These are extra teeth that develop in addition to the normal set. They can prevent the eruption of permanent teeth or cause displacement.
- Causes: Genetic factors or developmental anomalies.
- Consequences: Impaction, displacement of adjacent teeth, cyst formation.
Causes / Why It Happens
The process of tooth eruption is incredibly complex, and numerous factors can influence whether a tooth erupts on schedule and in the correct position.
Genetic Factors
Genetics play a significant role in determining the timing and sequence of tooth eruption, as well as jaw size and tooth size. If your parents experienced late eruption or impacted wisdom teeth, you might be more prone to similar issues. Certain syndromes also have a strong genetic link to abnormal eruption patterns.
Local Factors within the Mouth
These are often the most direct causes of eruption problems:
- Lack of Space: The most common reason for impaction, especially with wisdom teeth. If the jaw isn't large enough to accommodate all 32 teeth, the last teeth to emerge will struggle.
- Presence of Primary Teeth: Sometimes, a primary tooth doesn't exfoliate (fall out) on time, physically blocking the permanent tooth beneath it.
- Supernumerary Teeth: Extra teeth can obstruct the path of normal permanent teeth.
- Cysts or Tumors: Lesions or growths in the jawbone can create a physical barrier to eruption.
- Ankylosis: A rare condition where the tooth root fuses with the bone, preventing further eruption.
- Trauma: Injury to the face or jaw in childhood can damage developing tooth buds, leading to eruption delays or abnormalities.
- Thick Gingival Tissue: In some cases, unusually dense gum tissue can make it difficult for a tooth to break through.
Systemic Factors and General Health
Overall health and certain medical conditions can also impact tooth eruption:
- Nutritional Deficiencies: Severe deficiencies in vitamins (like Vitamin D) or minerals (like calcium) essential for bone and tooth development can affect eruption timing.
- Endocrine Disorders: Conditions like hypothyroidism (underactive thyroid) or hypopituitarism can cause generalized delayed tooth eruption.
- Systemic Diseases: Chronic illnesses, particularly those affecting bone metabolism, can sometimes influence eruption.
- Syndromes: Genetic syndromes such as Down syndrome, Cleidocranial Dysplasia, or Gardner's syndrome are frequently associated with delayed or absent tooth eruption.
Pro Tip: Regular dental check-ups, especially during childhood and adolescence, are crucial for monitoring tooth development. Your dentist can identify early signs of potential eruption problems using X-rays and clinical examination.
Signs and Symptoms
For most adults, the eruption of permanent teeth (beyond wisdom teeth) occurs relatively early in life, and usually without significant discomfort once past childhood. However, issues like delayed eruption or impaction can occur, presenting specific signs and symptoms.
Signs of Normal Adult Tooth Eruption (Primarily Wisdom Teeth)
When wisdom teeth begin to erupt, you might notice:
- Mild Discomfort or Pressure: A dull ache or feeling of pressure in the back of your jaw as the tooth pushes through the gum.
- Slight Swelling or Tenderness: The gum tissue around the erupting tooth may be a little red and sensitive.
- "Growing Pains": Some people report a general sense of jaw soreness or tension.
These symptoms are usually temporary and manageable.
Signs and Symptoms of Problematic Eruption (Especially Impaction)
If a tooth, particularly a wisdom tooth, is having trouble erupting, or if any permanent tooth is impacted, you might experience more severe symptoms:
- Pain: Often a throbbing, persistent pain in the jaw, radiating to the ear, head, or neck. This is a common symptom of impacted wisdom teeth trying to emerge in a crowded space.
- Swelling and Redness: The gum tissue around the affected area may be visibly swollen, red, and tender to the touch. This indicates inflammation or potential infection.
- Difficulty Opening Mouth (Trismus): Inflammation or infection can make it painful and difficult to open your mouth fully.
- Bad Breath (Halitosis) or Unpleasant Taste: If food particles and bacteria get trapped under a partially erupted tooth (a common issue with partially impacted wisdom teeth), it can lead to infection (pericoronitis), causing bad breath and a foul taste.
- Pus Drainage: A clear sign of infection around an impacted tooth.
- Damage to Adjacent Teeth: Pressure from an impacted tooth can damage the roots or crowns of neighboring teeth, potentially leading to cavities or bone loss.
- Cyst or Tumor Formation: In rare cases, a fluid-filled sac (cyst) or even a benign tumor can form around the crown of an impacted tooth. This is usually painless but can cause jaw expansion if it grows large.
- Visible Gaps or Misalignment: If an impacted tooth is preventing other teeth from moving into their correct positions, you might notice new gaps or changes in your bite alignment.
- Headaches or Earaches: Pain from an impacted tooth can sometimes radiate and be perceived as a headache or earache.
Pro Tip: Don't ignore persistent pain or discomfort in your jaw, especially in the back of your mouth. These symptoms warrant a dental evaluation to rule out impaction or infection.
Treatment Options
When adult tooth eruption doesn't proceed normally, intervention may be necessary to prevent complications, alleviate pain, and maintain oral health. The treatment approach depends entirely on the specific issue, the affected tooth, and the patient's overall dental health.
1. Monitoring and Observation
- Description: For minor delays or partial eruption where no immediate symptoms or risks are present, your dentist might recommend a "wait and see" approach, often with regular X-rays to monitor development. This is common for wisdom teeth that are slightly delayed but show potential for full eruption.
- Pros: Non-invasive, avoids immediate procedures.
- Cons: Potential for problems to develop later if eruption fails; requires diligent follow-up.
- Cost: Minimal, primarily consultation and X-ray fees ($50-$250 per visit).
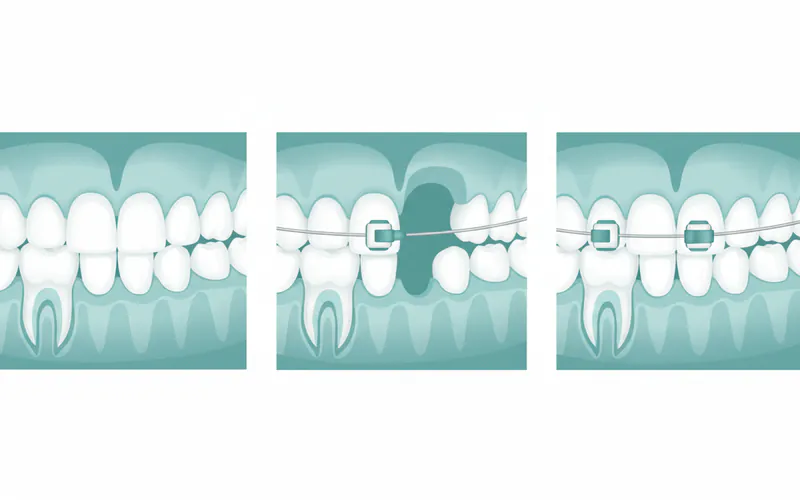
2. Surgical Exposure and Orthodontic Eruption
- Description: This treatment is often used for impacted canines or other non-wisdom teeth that are otherwise healthy and needed in the arch. An oral surgeon or periodontist performs a minor procedure to remove gum tissue and sometimes a small amount of bone covering the impacted tooth. An orthodontic bracket and chain are then attached to the exposed tooth. An orthodontist then gradually pulls the tooth into its proper position using braces or aligners.
- Pros: Saves the natural tooth, improves aesthetics and function.
- Cons: Involves both surgery and prolonged orthodontic treatment (typically 1-3 years), discomfort post-surgery.
- Cost: Surgical exposure: $300-$1,000 per tooth. Orthodontic treatment: $3,000-$8,000 for the full course.
3. Extraction (Tooth Removal)
- Description: This is the most common treatment for problematic wisdom teeth and sometimes for other severely impacted, damaged, or problematic teeth.
- Simple Extraction: For fully erupted teeth or those with minimal impaction, the tooth is loosened and removed with forceps.
- Surgical Extraction: For impacted teeth (especially wisdom teeth), the oral surgeon makes an incision in the gum, removes bone blocking the tooth, and may divide the tooth into sections for easier removal.
- Pros: Eliminates pain and infection risk, prevents damage to adjacent teeth, creates space for other teeth.
- Cons: Permanent loss of the tooth, potential for dry socket, nerve damage (rare), swelling, and discomfort during recovery.
- Cost:
- Simple extraction: $75-$250 per tooth.
- Surgical extraction (impacted wisdom tooth): $225-$600 per tooth.
- General anesthesia: Adds $200-$500 per hour if required.

4. Space Management and Orthodontics
- Description: If overcrowding is preventing a tooth from erupting, or if delayed eruption causes misalignment, an orthodontist may use appliances (e.g., expanders, braces) to create sufficient space in the dental arch. This can guide delayed teeth into eruption or correct positions. In some cases, extraction of other teeth (not the impacted one) might be considered to create space.
- Pros: Guides natural eruption, corrects bite issues, improves aesthetics.
- Cons: Can be a lengthy process (1-3 years), requires patient compliance with appliances.
- Cost: Orthodontic treatment ranges from $3,000-$8,000.
5. Removal of Obstructions
- Description: If a physical obstruction like a cyst, tumor, or supernumerary tooth is blocking eruption, it must be surgically removed. Once the obstruction is gone, the impacted tooth may erupt naturally or may still require orthodontic assistance.
- Pros: Resolves the root cause of impaction, can allow natural eruption.
- Cons: Requires surgery, potential for further intervention if the tooth doesn't erupt on its own.
- Cost: Varies widely depending on the nature and complexity of the obstruction removal, typically $200-$1,500.
Comparison of Common Treatments for Eruption Issues
| Treatment Option | Primary Use Case | Typical Duration | Average Cost (US) | Key Considerations |
|---|---|---|---|---|
| Monitoring & Observation | Mild delays, asymptomatic impactions | Ongoing until resolution or issue arises | $50-$250 (per visit/X-ray) | Low cost, non-invasive, but requires patience; potential for future intervention. |
| Surgical Exposure + Orthodontics | Impacted canines or critical non-wisdom teeth | 1-3 years (ortho) | $300-$1,000 (surgery) + $3k-$8k (ortho) | Saves natural tooth, complex, requires specialized care from multiple providers. |
| Surgical Extraction (Impacted) | Problematic wisdom teeth, severely impacted/damaged teeth | 30-90 minutes (procedure) | $225-$600 per tooth + anesthesia | Immediate relief, permanent tooth loss, common for wisdom teeth. |
| Orthodontic Space Management | Overcrowding preventing eruption, misalignment | 1-3 years | $3,000-$8,000 | Guides natural eruption, improves bite, no tooth loss (unless other extractions). |
| Obstruction Removal | Cysts, supernumerary teeth blocking eruption | 30-60 minutes (procedure) | $200-$1,500 (variable) | Resolves root cause; tooth may erupt naturally afterward or need assistance. |
Step-by-Step Process: Surgical Extraction of an Impacted Wisdom Tooth
Given that problematic wisdom tooth eruption is the most common adult eruption issue, let's detail the typical process for a surgical extraction.
-
Initial Consultation and Diagnosis:
- You'll meet with your general dentist or an oral surgeon to discuss your symptoms.
- A comprehensive oral exam will be performed.
- Dental X-rays (panoramic X-ray, sometimes 3D cone-beam CT) will be taken to visualize the impacted tooth's position, root structure, and its proximity to vital structures like nerves and sinuses.
- The dentist or surgeon will explain the findings, discuss treatment options, and recommend the best course of action.
- Cost: Consultation $50-$200; X-rays $75-$250.
-
Pre-Procedure Instructions:
- You'll receive instructions regarding food and drink restrictions (especially if sedation or general anesthesia is used).
- You may be prescribed antibiotics to start before the procedure if an infection is present.
- Arrange for transportation if you're receiving sedation.
-
Anesthesia Administration:
- Upon arrival, the team will prepare you for the procedure.
- Local Anesthesia: The area around the tooth will be numbed using injections. This is standard for all extractions.
- Sedation Options (often recommended for impacted wisdom teeth):
- Nitrous Oxide (Laughing Gas): Relaxes you, wears off quickly.
- Oral Sedation: A pill taken beforehand to make you drowsy.
- IV Sedation (Conscious Sedation): Administered intravenously to put you into a deeper state of relaxation, often called "twilight sleep." You'll be awake but won't remember much.
- General Anesthesia: You'll be completely unconscious. This is typically reserved for complex cases or multiple extractions.
-
Surgical Removal of the Tooth:
- The surgeon will make an incision in the gum tissue to expose the impacted tooth and underlying bone.
- Any bone obstructing the tooth's path will be carefully removed using specialized dental drills.
- The tooth may be sectioned (cut into smaller pieces) to facilitate easier removal, especially if it's deeply impacted or has complex roots.
- The tooth pieces are carefully extracted.
-
Site Closure:
- The socket is cleaned of any debris or remaining tissue.
- The gum flap is repositioned, and sutures (stitches) are placed to close the incision. These may be dissolvable or require removal at a follow-up appointment.
- Gauze is placed over the extraction site for pressure to aid clotting.
-
Post-Procedure Instructions:
- You'll be monitored in a recovery area until the effects of sedation wear off.
- Detailed post-operative instructions will be provided, covering pain management, diet, oral hygiene, and activity restrictions.
- You'll typically go home with gauze, prescriptions for pain medication, and possibly antibiotics.
Cost and Insurance
The cost of addressing adult tooth eruption issues in the United States can vary significantly based on the complexity of the case, the type of procedure, the number of teeth involved, the geographic location of the dental practice, and the practitioner's fees.
Average US Price Ranges
| Procedure | Average Low Cost (US$) | Average Mid Cost (US$) | Average High Cost (US$) |
|---|---|---|---|
| Dental Consultation | $50 | $100 | $200 |
| Panoramic X-ray | $75 | $120 | $200 |
| 3D Cone Beam CT Scan | $200 | $350 | $600 |
| Simple Tooth Extraction | $75 | $150 | $250 |
| Surgical Extraction (Impacted Tooth) | $225 | $400 | $600 |
| General Anesthesia (per hour) | $200 | $350 | $500 |
| Surgical Exposure of Impacted Tooth | $300 | $600 | $1,000 |
| Orthodontic Treatment (Braces/Aligners) | $3,000 | $5,500 | $8,000 |
| Removal of Supernumerary Tooth/Obstruction | $200 | $500 | $1,500 |
- Geographic Variation: Costs tend to be higher in major metropolitan areas (e.g., New York, Los Angeles) compared to rural areas.
- Specialist vs. General Dentist: Oral surgeons or orthodontists typically charge more than general dentists due to their specialized training and equipment.
Insurance Coverage Details
Most dental insurance plans in the US offer some level of coverage for medically necessary procedures related to tooth eruption issues.
- Diagnostic Services: Consultations and X-rays are usually covered at a high percentage (e.g., 80-100%) as they are considered preventive or diagnostic.
- Extractions: Routine and surgical extractions for impacted teeth are generally covered, often at 50-80% of the cost, depending on your plan's specifics and whether your annual maximum has been met.
- Anesthesia: Local anesthesia is usually included with the extraction fee. IV sedation or general anesthesia may be covered, but often at a lower percentage or only for specific medical indications. Check your policy carefully.
- Orthodontics: This is where coverage varies the most.
- Many adult dental plans do not cover orthodontics for cosmetic reasons.
- However, if orthodontic treatment (like surgical exposure and bonding an impacted tooth) is deemed medically necessary to correct a functional problem (e.g., prevent damage to other teeth, improve bite), some plans may offer partial coverage, typically 25-50%.
- Plans with an "orthodontic rider" or specific "lifetime maximum" for orthodontics are more likely to cover it.
- Waiting Periods & Deductibles: Be aware of waiting periods for major procedures (often 6-12 months) and annual deductibles that must be met before your insurance starts paying.
- Annual Maximums: Most dental plans have an annual maximum benefit (e.g., $1,000-$2,000). Once this limit is reached, you're responsible for the remaining costs for that year.
- Pre-Authorization: For complex or costly procedures, it's highly recommended to obtain a pre-authorization from your insurance company. This clarifies what they will cover before you undergo treatment.
Pro Tip: Always contact your dental insurance provider directly or have your dental office submit a pre-treatment estimate to understand your exact out-of-pocket costs.
Recovery and Aftercare
Proper recovery and aftercare are crucial following procedures for adult tooth eruption issues, especially after surgical extractions or exposures. Following your dental professional's instructions diligently will minimize complications and promote healing.
Immediate Post-Procedure (First 24-48 Hours)
- Bleeding Control: Bite firmly on the gauze pads for 30-45 minutes. Change them as needed. Slight oozing is normal; heavy bleeding is not.
- Pain Management: Take prescribed pain medication as directed. Over-the-counter options like ibuprofen (Advil, Motrin) or acetaminophen (Tylenol) can also be effective.
- Swelling Reduction: Apply an ice pack to the outside of your cheek, 20 minutes on, 20 minutes off, for the first 24-48 hours. This is most effective if started immediately.
- Rest: Avoid strenuous activities for at least 24-48 hours. Elevate your head with pillows while sleeping to help reduce swelling.
- Diet: Stick to soft, cool foods initially (e.g., yogurt, mashed potatoes, lukewarm soup, smoothies). Avoid hot, hard, crunchy, or spicy foods that could irritate the surgical site.
- Avoid Straws: The sucking motion can dislodge the blood clot, leading to a painful condition called "dry socket."
- Oral Hygiene: Do NOT rinse vigorously for the first 24 hours. After that, gentle rinsing with warm salt water (1/2 teaspoon salt in 8 ounces warm water) 2-3 times a day can help keep the area clean. Continue to brush other teeth carefully, avoiding the surgical site.
- Avoid Smoking and Alcohol: Both can significantly impede healing and increase the risk of complications.
Ongoing Recovery (Days 3-14)
- Pain and Swelling: These should gradually decrease. If pain worsens or swelling increases after 3-4 days, contact your dentist.
- Diet Progression: Gradually introduce more solid foods as comfort allows.
- Oral Hygiene: Continue gentle salt water rinses. You may be able to carefully resume normal brushing in the area, avoiding sutures.
- Sutures: If non-dissolvable sutures were used, you'll have a follow-up appointment (typically 7-10 days post-op) for their removal. Dissolvable sutures will disappear on their own.
- Orthodontic Care (if applicable): If you've had surgical exposure, your orthodontist will likely adjust your braces soon after to begin guiding the newly exposed tooth into position. Follow their specific instructions for care and adjustments.
Potential Complications to Watch For
- Dry Socket (Alveolar Osteitis): Intense, throbbing pain usually starting 2-4 days after extraction, often radiating to the ear. It occurs when the blood clot dislodges or dissolves, leaving the bone exposed. Requires dental attention.
- Infection: Increasing pain, swelling, pus, fever, or persistent bad taste/smell could indicate infection. Contact your dentist immediately.
- Numbness: Temporary numbness is common due to local anesthesia. Persistent numbness (paresthesia) in the lip, chin, or tongue, though rare, can occur if nerves are irritated or damaged during surgery.
- Excessive Bleeding: If bleeding is heavy and doesn't stop after applying pressure, seek immediate dental or medical help.
ADA Guidelines: The American Dental Association emphasizes that good oral hygiene, adherence to post-operative instructions, and regular follow-up appointments are critical for successful recovery and preventing complications after dental surgery.
Prevention
While some adult tooth eruption issues, like genetic predispositions to impaction, can't be entirely prevented, many complications can be avoided or minimized through proactive dental care and early intervention.
1. Regular Dental Check-ups
- Importance: This is the cornerstone of prevention. Regular visits, ideally every six months, allow your dentist to monitor your oral development from childhood through adulthood.
- What they do: Your dentist will perform clinical examinations and take periodic X-rays (panoramic X-rays are especially useful for visualizing developing teeth in the jaw) to identify any signs of delayed eruption, impaction, or overcrowding before they become symptomatic.
- ADA Recommendation: The ADA strongly recommends regular dental check-ups for individuals of all ages.
2. Early Orthodontic Assessment
- When: The American Association of Orthodontists recommends a first orthodontic check-up around age 7. Even if adult teeth haven't fully erupted, an orthodontist can assess jaw growth and space availability.
- Benefits: Early assessment can identify potential issues like severe crowding, disproportionate jaw growth, or the likelihood of impacted teeth (especially canines and wisdom teeth) years in advance.
- Intervention: This allows for timely intervention, such as interceptive orthodontics, expanders, or space maintainers, which can guide proper eruption and potentially avoid more complex treatments later.
3. Proper Oral Hygiene
- Impact: While good hygiene doesn't prevent impaction, it significantly reduces the risk of infection around partially erupted teeth, particularly wisdom teeth.
- Routine: Brushing twice daily and flossing daily helps remove food particles and plaque, reducing the bacterial load that can cause pericoronitis (gum infection around an erupting tooth).
- Targeted Cleaning: Pay extra attention to the very back of your mouth where wisdom teeth are trying to emerge, as these areas are often difficult to clean effectively.
4. Space Maintenance (in childhood)
- Relevance: If a primary tooth is lost prematurely due to decay or injury, a "space maintainer" can be placed by a pediatric dentist or orthodontist.
- Function: This appliance holds the space open, preventing adjacent teeth from drifting and blocking the eruption path of the permanent tooth below.
5. Timely Extraction of Primary Teeth
- Scenario: Sometimes a primary tooth's root doesn't resorb properly, or it remains firmly in place even after the permanent tooth is ready to erupt.
- Intervention: Your dentist may recommend extracting the primary tooth to clear the path for the permanent tooth, preventing impaction or ectopic eruption.
6. Nutritional Considerations
- Healthy Diet: While not a direct prevention for impaction, a balanced diet rich in essential vitamins and minerals (especially Calcium and Vitamin D) supports overall bone and tooth development, contributing to healthy eruption processes.
By being proactive and working closely with your dental team, you can significantly reduce the likelihood of complications associated with adult tooth eruption and ensure a healthier, more comfortable experience.
Risks and Complications
While tooth eruption is a natural physiological process, problems, especially with the eruption of adult teeth, can lead to various risks and complications if not properly managed.
Risks Associated with Impaction or Abnormal Eruption
- Pericoronitis: This is an infection of the gum tissue surrounding a partially erupted tooth, most commonly seen with wisdom teeth. Food and bacteria get trapped under the gum flap, leading to inflammation, pain, swelling, and sometimes pus. It can be severe, causing difficulty opening the mouth, fever, and spreading infection.
- Dental Caries (Cavities): Partially erupted or crowded teeth are harder to clean. Food and plaque can accumulate, increasing the risk of cavities on the affected tooth or the adjacent tooth.
- Damage to Adjacent Teeth: An impacted tooth pushing against the root or crown of a neighboring tooth can cause resorption (dissolving) of the adjacent tooth's root, structural damage to its crown, or contribute to gum disease and bone loss around it.
- Cysts and Tumors: In rare cases, the follicular sac (the tissue surrounding the crown of an unerupted tooth) can fill with fluid and expand, forming a dentigerous cyst. These cysts can grow large, causing bone destruction, and may even lead to the formation of benign tumors.
- Orthodontic Problems: Impacted teeth can cause misalignment of other teeth, crowding, or interfere with orthodontic treatment aimed at correcting bite issues. They can shift the entire dental arch.
- Pain and Discomfort: Pressure from an erupting or impacted tooth can cause chronic pain in the jaw, head, or ear.
- Root Resorption: The roots of adjacent teeth can be absorbed or damaged by the pressure of an impacted tooth.
- Nerve Damage: Although rare, severely impacted teeth (especially lower wisdom teeth) can be very close to the inferior alveolar nerve, which provides sensation to the lower lip, chin, and tongue. Extraction carries a small risk of temporary or, in very rare cases, permanent numbness (paresthesia).

Risks and Complications of Treatment (e.g., Surgical Extraction)
- Pain and Swelling: Expected side effects, usually managed with medication, but can be significant.
- Dry Socket (Alveolar Osteitis): As mentioned in recovery, this painful condition occurs when the blood clot in the extraction site dislodges, exposing the bone.
- Infection: While antibiotics are often prescribed, infection can still occur at the surgical site.
- Bleeding: Post-operative bleeding can occur, though usually manageable. Persistent, heavy bleeding needs immediate attention.
- Nerve Injury (Paresthesia): A rare but serious complication, especially with lower wisdom tooth removal. It can result in temporary or permanent numbness/tingling in the lip, chin, or tongue.
- Sinus Communication: For upper molars, extraction can sometimes create an opening between the mouth and the maxillary sinus. This usually heals but may require additional procedures if it doesn't close on its own.
- Jaw Fracture: Extremely rare, but possible during a very difficult extraction, especially if the jawbone is thin or weakened.
- Damage to Adjacent Teeth/Restorations: Instruments used during extraction can inadvertently damage nearby teeth or existing dental work (fillings, crowns).
Pro Tip: Discuss all potential risks and complications with your oral surgeon or dentist before undergoing any procedure. Understanding the risks allows you to make an informed decision and be prepared for recovery.
Children / Pediatric Considerations
While this article focuses on the adult tooth eruption chart, understanding the preceding stages of primary (baby) tooth eruption and their transition is crucial for ensuring healthy adult dentition. The primary tooth eruption chart lays the foundation for permanent teeth.
Primary Tooth Eruption Timeline
Primary teeth typically begin erupting around 6 months of age and complete by age 3. There are 20 primary teeth in total.
| Tooth Type | Average Age of Eruption (Mandible) | Average Age of Eruption (Maxilla) |
|---|---|---|
| Central Incisors | 6-10 months | 8-12 months |
| Lateral Incisors | 10-16 months | 9-13 months |
| First Molars | 14-18 months | 13-19 months |
| Canines | 17-23 months | 16-22 months |
| Second Molars | 23-31 months | 25-33 months |
Importance of Primary Teeth
Many parents mistakenly believe that baby teeth aren't important since they'll eventually fall out. This is a dangerous misconception! Primary teeth are vital for:
- Speech Development: They help children form sounds correctly.
- Nutrition: They enable proper chewing and digestion of food.
- Space Maintenance: They hold the necessary space in the jaws for the permanent teeth that are developing beneath them. Premature loss of a primary tooth can lead to space loss, causing permanent teeth to erupt out of alignment or become impacted.
- Guiding Permanent Teeth: Primary teeth act as guides, helping the permanent teeth erupt into their correct positions.
Transition to Permanent Dentition
The mixed dentition stage, where both primary and permanent teeth are present, typically begins around age 6 with the eruption of the first permanent molars (often called "6-year molars") and the shedding of primary central incisors. This period lasts until approximately age 12-14 when the last primary teeth are lost.
Age-Specific Guidance for Parents:
- Infancy (0-1 year): First dental visit by age 1 or when the first tooth erupts. Focus on cleaning gums, proper bottle/sippy cup use, and preventing baby bottle tooth decay.
- Toddler/Preschool (1-5 years): Establish good brushing habits (with supervision), introduce flossing, and continue regular dental check-ups. Address thumb-sucking or pacifier habits if they persist beyond age 3, as they can affect jaw development and tooth alignment.
- School Age (6-12 years): This is the crucial mixed dentition phase.
- Monitor for Losing Teeth: Ensure primary teeth are shedding naturally. If a permanent tooth is erupting but the baby tooth hasn't fallen out, consult your dentist.
- First Permanent Molars: These erupt behind the last baby teeth and are often mistaken for more baby teeth. They are susceptible to decay, so discuss sealants with your dentist.
- Orthodontic Assessment: As mentioned, an orthodontic evaluation around age 7 can identify developing issues with jaw growth or crowding, allowing for interceptive treatment.
- Space Maintainers: If a child loses a primary tooth prematurely, a space maintainer may be necessary to preserve the space for the incoming permanent tooth.
By taking an active role in monitoring your child's dental development and ensuring regular dental care, parents can significantly contribute to a healthy and well-aligned set of permanent teeth for their children.
Frequently Asked Questions
### Q1: What is a typical adult tooth eruption chart, and how does it differ from a child's?
A1: An adult tooth eruption chart outlines the typical ages when permanent teeth emerge, replacing primary (baby) teeth or erupting in new positions (like molars). It usually covers ages 6 to 21, culminating with wisdom teeth. A child's chart focuses on the eruption of primary teeth from around 6 months to 3 years of age, which are then shed to make way for the permanent set.
### Q2: How many permanent teeth does an adult usually have?
A2: Most adults have 32 permanent teeth, which includes 8 incisors, 4 canines, 8 premolars (bicuspids), and 12 molars (including 4 wisdom teeth). However, it's common for individuals to have their wisdom teeth removed or never develop all four, resulting in 28 teeth.
### Q3: Is it normal for adult teeth to erupt later than the typical chart indicates?
A3: There can be some natural variation in eruption timing, with a delay of up to six months generally considered within the normal range. However, significant delays (more than a year past the average) or asymmetry (a tooth erupting on one side but not the other) warrant a dental evaluation to rule out issues like impaction or obstructions.
### Q4: What are the signs that a wisdom tooth is erupting abnormally or is impacted?
A4: Common signs of problematic wisdom tooth eruption include persistent pain in the back of the jaw, swelling or tenderness of the gums, difficulty opening your mouth, bad breath, or a foul taste in your mouth. If you experience these symptoms, especially if they worsen, it's important to see a dentist.
### Q5: How much does it cost to have an impacted wisdom tooth removed?
A5: The cost for removing an impacted wisdom tooth in the US typically ranges from $225 to $600 per tooth. This does not include consultation, X-rays, or anesthesia costs. If general anesthesia or IV sedation is used, expect an additional $200-$500 per hour. Insurance may cover a portion, usually 50-80%, after deductibles.
### Q6: Will my insurance cover the cost of treating an impacted tooth?
A6: Most dental insurance plans cover medically necessary procedures like extractions for impacted teeth, often at 50-80%. However, coverage varies widely, and there might be waiting periods, deductibles, and annual maximums. For orthodontic treatment related to impacted teeth, coverage is less consistent and often depends on medical necessity and specific plan features.
### Q7: What is the recovery like after a surgical extraction for an impacted tooth?
A7: Recovery typically involves some pain and swelling for the first 3-5 days, managed with prescribed pain medication and ice packs. You'll need to stick to a soft diet, avoid straws, and practice gentle oral hygiene. Complete healing of the soft tissue takes about 1-2 weeks, while bone healing takes several months. Watch for signs of dry socket or infection.
### Q8: Can an adult tooth that hasn't erupted still be guided into place?
A8: Yes, for some impacted non-wisdom teeth (like canines), surgical exposure followed by orthodontic treatment can successfully guide the tooth into its proper position. This is often done if the tooth is healthy and needed for proper bite function and aesthetics. It requires collaboration between an oral surgeon and an orthodontist.
### Q9: What happens if an impacted tooth is left untreated?
A9: Leaving an impacted tooth untreated can lead to various complications, including chronic pain, infection (pericoronitis), damage to adjacent teeth (cavities or root resorption), development of cysts or tumors, and orthodontic problems like crowding or misalignment. Early intervention is generally recommended to prevent these issues.
### Q10: How can parents help ensure their children's adult teeth erupt properly?
A10: Parents can ensure proper adult tooth eruption by maintaining regular dental check-ups for their children starting by age one, teaching good oral hygiene, monitoring for timely shedding of baby teeth, and considering an orthodontic assessment around age seven. Addressing issues like premature baby tooth loss or thumb-sucking habits can also guide proper development.
When to See a Dentist
Understanding the normal adult tooth eruption chart empowers you to recognize when something might be amiss. While slight variations in timing are common, certain signs and symptoms warrant prompt professional attention.
Immediate Attention (Emergency)
Seek immediate dental care if you experience any of the following:
- Severe, Unmanageable Pain: Intense, throbbing pain in the back of your jaw or around a specific tooth that doesn't subside with over-the-counter pain relievers.
- Significant Swelling: Rapidly increasing swelling in your jaw, cheek, or around a tooth, especially if accompanied by difficulty swallowing or breathing, which could indicate a spreading infection.
- Signs of Infection: Fever, chills, pus draining from the gums, or a persistent foul taste in your mouth, which can signify a serious infection (pericoronitis or abscess).
- Difficulty Opening Your Mouth (Trismus): If you can barely open your mouth due to pain or swelling, it's a sign of significant inflammation or infection.
- Excessive Bleeding: If you've recently had a tooth extracted and experience heavy, uncontrollable bleeding that doesn't stop after applying pressure with gauze for 30 minutes.
Scheduled Appointment (Red Flags)
Schedule an appointment with your dentist soon if you notice any of these red flags, even if they aren't immediately painful:
- Persistent Mild Discomfort: A dull ache or pressure in the back of your jaw that lasts for more than a few days, even if it's not severe.
- Delayed Eruption: If a permanent tooth has not erupted by its expected timeframe, especially if a similar tooth on the opposite side of your mouth has already emerged, or if a baby tooth is still present when it shouldn't be.
- Visible Swelling or Redness without Pain: Localized gum inflammation around where a tooth should be erupting, even if it's not causing significant discomfort.
- New Gaps or Crowding: If you notice new spaces forming between your teeth, or your teeth suddenly becoming more crowded or misaligned, it could be due to an impacted tooth pushing against others.
- Bad Breath or Unpleasant Taste: If you frequently experience bad breath or a strange taste in your mouth, particularly in the back, it could indicate food entrapment and early infection around a partially erupted tooth.
- Sensitivity in Adjacent Teeth: If teeth next to an area of suspected eruption issue suddenly become sensitive to hot or cold, it could be a sign of pressure or damage.
Routine Care Guidance
Even without specific symptoms, regular dental check-ups are the best way to prevent eruption issues from becoming problematic. Your dentist can:
- Monitor Tooth Development: Use X-rays to track the development and position of unerupted permanent teeth, particularly wisdom teeth.
- Identify Potential Problems Early: Catch issues like impaction or lack of space before they cause pain or damage.
- Recommend Preventive Measures: Suggest early orthodontic consultations or timely extractions if necessary.
By staying proactive and attentive to your oral health, you can ensure that the journey of your adult teeth is as smooth and healthy as possible.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Tooth Eruption Order: Complete Guide
The journey of human teeth, from their initial emergence in infancy to the arrival of wisdom teeth in young adulthood, is a fascinating and crucial aspect of our overall health. Understanding the tooth eruption order is not just a matter of curiosity; it's a vital piece of knowledge that empower
February 23, 2026
Primary Tooth Eruption Sequence: Complete Guide
Did you know that by their third birthday, most children will have a full set of 20 primary teeth? The journey of these first teeth, from their initial appearance to their eventual replacement by permanent teeth, is a remarkable and often challenging milestone for both infants and parents. Understan
February 23, 2026
Canine Tooth Eruption: Complete Guide
Have you ever wondered about the complex process that brings your teeth into alignment, especially the prominent, pointed teeth known as canines? While often overshadowed by discussions of wisdom teeth or incisors, the canine tooth eruption process is a critical stage in your oral development, d
February 23, 2026
Permanent Tooth Eruption Sequence: Complete Guide
Welcome to SmilePedia.net, your trusted resource for comprehensive dental health information. The journey of your permanent teeth emerging into your mouth, known as the permanent tooth eruption sequence, is a fundamental aspect of oral development. Did you know that while primary (baby) teeth ty
February 23, 2026