Face Swelling From Tooth: Complete Guide
Key Takeaways
- An alarming sight for many, face swelling from a tooth is far more than just a cosmetic concern; it's a critical indicator of a potentially serious dental infection that demands immediate attention. Imagine waking up to a visibly swollen face, the pain radiating, and a sense of dread as you real
An alarming sight for many, face swelling from a tooth is far more than just a cosmetic concern; it's a critical indicator of a potentially serious dental infection that demands immediate attention. Imagine waking up to a visibly swollen face, the pain radiating, and a sense of dread as you realize the source is likely a neglected tooth. Data suggests that dental infections are among the most common reasons for emergency room visits in the U.S., with facial swelling being a primary symptom. Ignoring such swelling can lead to severe health complications, impacting not just your oral health but your entire well-being. This comprehensive guide from SmilePedia.net will delve into every aspect of facial swelling originating from a dental issue, offering you a clear understanding of what causes it, how it's treated, the associated costs, and crucial prevention strategies. We'll explore the dangers of untreated infections, from localized swelling of the gums to life-threatening conditions like Ludwig's Angina, ensuring you have the knowledge to protect yourself and your family.
Key Takeaways:
- Urgency is Paramount: Any facial swelling originating from a tooth is a dental emergency requiring immediate professional evaluation to prevent severe complications.
- Common Causes: Most often, it's due to an untreated dental abscess (periapical or periodontal) caused by deep decay, trauma, or severe gum disease.
- Spreading Infection Risk: Untreated dental infections can spread rapidly to other areas of the face, jaw, neck (causing submandibular swelling), and even to critical structures like the airway or brain.
- Treatment Options: Core treatments include draining the infection (incision and drainage), antibiotics, and definitive dental procedures like root canal therapy or tooth extraction.
- Cost & Insurance: Treatment costs can range significantly, from $150-$500 for antibiotics and simple drainage, up to $1,000-$3,000+ for root canals or extractions, often partially covered by dental insurance. Severe cases requiring hospitalization can incur tens of thousands.
- Recognize Red Flags: Seek emergency care if swelling is rapid, painful, accompanied by fever, difficulty breathing or swallowing, or causes submandibular swelling (swelling under the jaw).
- Prevention is Key: Regular dental check-ups, meticulous oral hygiene, and prompt treatment of minor dental issues are the best defenses against such infections.
What It Is / Overview
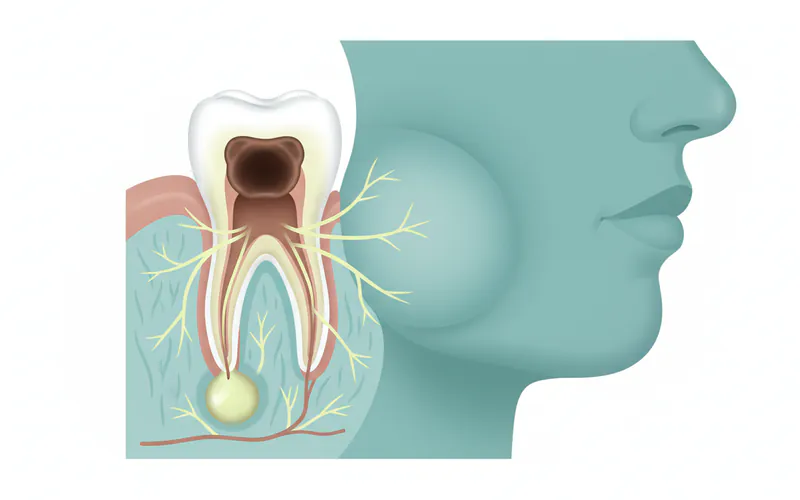
Face swelling from a tooth refers to the inflammation and enlargement of facial tissues, usually in the jaw, cheek, or neck region, as a direct result of an underlying dental problem. This swelling is almost always a sign of infection, where bacteria from an infected tooth or surrounding gum tissue have spread into the adjacent soft tissues. Medically, this condition is often an abscess or cellulitis originating from a dental source.

A dental abscess is a localized collection of pus formed by bacteria, white blood cells, and tissue debris. It typically forms at the tip of a tooth root (periapical abscess) due to untreated decay or trauma, or in the gums surrounding a tooth (periodontal abscess) due to severe gum disease. When this pus cannot drain internally, it puts pressure on surrounding tissues and seeks the path of least resistance, often creating a fistula (a small pimple-like bump that may ooze pus) or spreading into the soft tissues of the face, causing visible swelling.
The severity of the swelling can range from a subtle puffiness around the affected tooth to a dramatic, disfiguring enlargement of the entire cheek, jawline, or even the submandibular and neck regions. The presence of swelling signifies that the infection has progressed beyond the confines of the tooth itself and is now involving the facial or neck spaces, making it a more urgent concern.
Types / Variations
Facial swelling from a tooth isn't a single condition but rather a symptom that can manifest in several ways, each indicating a different level of severity and spread of infection. Understanding these variations is crucial for timely and appropriate treatment.
Dental Abscesses
The most common precursor to facial swelling is a dental abscess, which can be primarily categorized into two types:
- Periapical Abscess: This occurs at the tip of the tooth root, deep within the jawbone. It's usually the result of an untreated cavity that has allowed bacteria to penetrate the pulp (nerve and blood vessels) of the tooth. Once the pulp dies, the infection spreads out of the root tip into the surrounding bone, forming a pus pocket. If this pocket grows large enough, the pus can breach the bone and spread into the soft tissues of the face, causing significant swelling.
- Periodontal Abscess: This forms in the gum tissue next to the root of a tooth. It's typically caused by advanced gum disease (periodontitis), where bacteria accumulate in deep pockets between the tooth and gum. Food debris or calculus (hardened plaque) can become trapped, leading to an acute infection and pus formation. This can result in localized swelling of the gums (gums swelling) around the affected tooth and, if severe, can extend into the face.
Cellulitis
Cellulitis is a more widespread and dangerous form of infection. Instead of being a localized collection of pus like an abscess, cellulitis is a diffuse bacterial infection of the skin and underlying soft tissues. When a dental abscess ruptures or the infection from a tooth spreads aggressively, it can cause cellulitis of the face and neck.
- Characteristics: The affected area becomes red, warm, tender to the touch, and swollen. Unlike an abscess, cellulitis typically doesn't have a central "head" or an obvious pus-filled core. The swelling can spread rapidly and extensively.
- Severity: Facial cellulitis originating from a tooth is a serious condition that requires immediate medical attention and aggressive antibiotic therapy, often intravenously.
Ludwig's Angina
This is the most severe and life-threatening form of spreading dental infection. Ludwig's Angina is a rapidly progressive, diffuse cellulitis involving the submandibular, sublingual, and submental spaces (the areas under the jaw and tongue). It almost always originates from an infected mandibular (lower jaw) tooth, particularly molars.
- Characteristics: Patients present with a "bull neck" appearance, marked submandibular swelling, difficulty swallowing (dysphagia), drooling, and speech changes ("hot potato voice"). Critically, the swelling can push the tongue upwards and backward, potentially obstructing the airway, leading to respiratory distress.
- Severity: Ludwig's Angina is a medical emergency that necessitates immediate hospitalization, aggressive IV antibiotics, and potentially surgical intervention to drain the infection and secure the airway. Without rapid treatment, it can be fatal.
Other Causes of Localized Swelling
While less common, other dental-related issues can also cause facial or gums swelling:
- Impacted Wisdom Teeth: An impacted wisdom tooth, particularly if partially erupted, can become infected (pericoronitis). The trapped food and bacteria can lead to localized gum swelling, pain, and sometimes facial swelling in the angle of the jaw.
- Trauma: A direct blow to the face or jaw can cause swelling due to injury to soft tissues or fracture, which can become infected.
- Salivary Gland Infection (Sialadenitis): While not directly a tooth infection, an infection of the salivary glands (often triggered by a salivary stone or obstruction) can cause swelling in the cheek or under the jaw, which might be mistaken for a dental issue.
Causes / Why It Happens
The root cause of facial swelling from a tooth is almost invariably a bacterial infection that has breached the confines of the tooth itself and infiltrated the surrounding soft tissues. Several factors contribute to this process:
- Untreated Dental Decay (Cavities): This is the leading cause. When a cavity is left untreated, bacteria penetrate the enamel and dentin, eventually reaching the dental pulp (the innermost part of the tooth containing nerves and blood vessels). Once infected, the pulp dies, and the bacteria multiply, creating a pathway for infection to spread from the tooth's root tip into the jawbone and then into the facial tissues.
- Severe Periodontal Disease (Gum Disease): Advanced periodontitis leads to deep pockets between the teeth and gums where bacteria thrive. These pockets can become acutely infected, forming a periodontal abscess. If the infection is not drained, it can spread to the adjacent bone and soft tissues, causing swelling in the gums and potentially the face.
- Dental Trauma: A tooth that has suffered a severe blow, crack, or fracture may have its pulp compromised, leading to infection. Even if the tooth doesn't appear damaged, internal injury can cause the pulp to die and become a source of infection years later.
- Failed Dental Work: Occasionally, a previous root canal treatment may fail, or a filling/crown may leak, allowing bacteria to re-infect the tooth. This secondary infection can then lead to an abscess and subsequent facial swelling.
- Impacted Wisdom Teeth: When wisdom teeth are unable to fully erupt, they can become partially covered by a flap of gum tissue. Food and bacteria can get trapped under this flap, leading to an infection called pericoronitis, which can cause significant localized gums swelling and extend to the cheek and jaw.
- Compromised Immune System: Individuals with weakened immune systems (due to conditions like diabetes, autoimmune disorders, HIV, or certain medications) are more susceptible to infections and may experience more rapid and severe progression of dental infections, leading to more extensive facial swelling.
- Poor Oral Hygiene: A general lack of consistent and effective brushing and flossing allows plaque and bacteria to accumulate, increasing the risk of both cavities and gum disease, which are primary precursors to facial infections.
Signs and Symptoms
Recognizing the signs and symptoms of face swelling from a tooth is crucial for seeking timely treatment. While the most obvious sign is the swelling itself, several other indicators can help you understand the severity and nature of the problem.
Localized Symptoms:
- Visible Facial Swelling: This is the hallmark symptom. It can range from a subtle puffiness to a very noticeable bulge on one side of the face, affecting the cheek, jawline, or under the eye. The swelling may feel firm or doughy to the touch.
- Pain: Often intense, throbbing, constant, and worsening with chewing or pressure. The pain may radiate to the ear, jaw, or neck. In some cases, if the pulp has died, the pain might initially decrease, only to return as the infection spreads to surrounding tissues.
- Gums Swelling: The gum tissue directly around the affected tooth may be red, swollen, and tender. A small, pimple-like bump (fistula) might be visible on the gum, sometimes oozing pus or blood.
- Tenderness to Touch: The swollen area of the face and the affected tooth will likely be very tender.
- Tooth Sensitivity: Increased sensitivity to hot, cold, or pressure on the involved tooth.
- Bad Taste/Smell: A foul taste in the mouth or bad breath, often due to pus draining from the infection.
- Limited Mouth Opening (Trismus): Difficulty or pain when opening the mouth wide, especially if the infection is in the posterior lower jaw.
- Submandibular Swelling: Swelling underneath the jaw, often indicating involvement of the lymph nodes or a deeper spread of infection into the neck spaces.
Systemic Symptoms (Indicating a More Serious Infection):
- Fever and Chills: A sign that the infection is becoming systemic and the body is fighting it off.
- Fatigue and Malaise: General feeling of being unwell.
- Swollen Lymph Nodes: Tender, enlarged lymph nodes in the neck or under the jaw, indicating the body's immune response to infection.
- Difficulty Swallowing (Dysphagia): A critical symptom, particularly with severe submandibular swelling, as it indicates the infection may be impinging on the throat.
- Difficulty Breathing (Dyspnea): An absolute emergency. This occurs when the swelling in the neck and throat starts to compromise the airway, as seen in conditions like Ludwig's Angina.
- Rapidly Spreading Swelling: If the swelling is increasing quickly over hours, it signifies an aggressive infection.
Pro Tip: Never underestimate the significance of facial swelling, especially if accompanied by systemic symptoms. Early intervention is key to preventing potentially life-threatening complications. If you experience difficulty breathing or swallowing, head to the nearest emergency room immediately.
Treatment Options
Treating face swelling from a tooth involves a multi-pronged approach focused on eliminating the infection, managing symptoms, and addressing the underlying dental problem. The specific treatment plan will depend on the severity of the infection and its spread.
1. Antibiotics
- Description: Antibiotics are crucial for controlling the bacterial infection, especially when it has spread into the soft tissues of the face and caused swelling. Common prescriptions include penicillin, amoxicillin, clindamycin, or metronidazole.
- Pros: Reduces bacterial load, helps to contain the spread of infection, and decreases inflammation.
- Cons: Does not address the source of the infection (the tooth itself); misuse can lead to antibiotic resistance; potential side effects (nausea, diarrhea, allergic reactions).
- Important Note: Antibiotics alone are rarely a definitive cure for an abscess. They buy time and reduce the acute symptoms but the source of the infection must still be treated.
2. Incision and Drainage (I&D)
- Description: This surgical procedure involves making a small incision in the swollen area (either on the gum or facial skin, depending on where the pus has collected) to allow the pus to drain out. A rubber drain may be placed to keep the incision open and facilitate continued drainage.
- Pros: Provides immediate relief from pressure and pain, reduces the bacterial load, and helps to localize the infection. Essential for managing significant swelling and pus collection.
- Cons: Minor surgical procedure, requires local anesthesia, potential for scarring if external incision is made.
- Pro Tip: Drainage is often performed in conjunction with antibiotics for maximum effectiveness.
3. Root Canal Therapy (Endodontic Treatment)
- Description: If the infection originates from the pulp inside the tooth, a root canal is performed to save the tooth. The infected pulp tissue is removed, the root canals are cleaned, disinfected, and then filled with a biocompatible material.
- Pros: Saves the natural tooth, eliminates the source of infection, highly effective with a high success rate.
- Cons: Can be an extensive procedure, requires multiple appointments, higher cost than extraction.
- Cost Range: $700 - $2,000+ per tooth, depending on tooth type (front tooth vs. molar) and complexity.
4. Tooth Extraction
- Description: If the tooth is too severely damaged, infected, or non-restorable, extraction may be the most appropriate treatment. Removing the infected tooth eliminates the source of the infection.
- Pros: Immediate and definitive removal of the infection source, generally quicker than a root canal, often less expensive for simple extractions.
- Cons: Permanent loss of the natural tooth, may require prosthetic replacement (bridge, implant) in the future to prevent shifting of adjacent teeth and maintain bite function, which adds significant cost.
- Cost Range: $150 - $400 for a simple extraction; $250 - $800+ for surgical extraction (e.g., impacted wisdom tooth), not including replacement costs.
5. Hospitalization and Advanced Care
- Description: For severe cases like facial cellulitis or Ludwig's Angina, or if the patient has a compromised immune system, hospitalization is necessary. This involves aggressive intravenous (IV) antibiotics, close monitoring, and potentially emergency airway management (e.g., intubation or tracheostomy) if breathing is compromised.
- Pros: Provides intensive medical care for life-threatening infections.
- Cons: High cost, invasive, requires extensive medical intervention.
Comparison of Primary Treatment Options (Once Acute Infection is Controlled)
| Treatment Option | Purpose | Pros | Cons | Estimated US Cost (without insurance) |
|---|---|---|---|---|
| Root Canal Therapy | Save the tooth, remove internal infection | Preserves natural tooth, maintains chewing | Higher cost, multiple visits, requires crown afterward | $700 - $2,000+ |
| Tooth Extraction | Remove source of infection by removing tooth | Quick, definitive, often lower initial cost | Permanent tooth loss, may need replacement | $150 - $800+ |
| Incision & Drainage | Drain pus, relieve pressure, reduce swelling | Immediate relief, aids antibiotic effectiveness | Minor surgical procedure, doesn't address tooth source | $150 - $500 (often with antibiotics) |
Step-by-Step Process: What to Expect During Treatment
Dealing with face swelling from a tooth can be daunting, but understanding the typical treatment process can alleviate anxiety. While specifics vary based on the diagnosis and severity, a general sequence of events unfolds.
1. Initial Examination and Diagnosis
- Patient History: Your dentist will ask about your symptoms, when they started, pain levels, and any other medical conditions.
- Clinical Examination: The dentist will visually inspect your face for swelling, redness, and tenderness. They will also examine your mouth, teeth, and gums, looking for the source of infection (e.g., a decayed tooth, inflamed gums, a fistula). They will check for submandibular swelling and tenderness in your lymph nodes.
- X-rays: Dental X-rays (periapical, panoramic) are essential to identify the infected tooth, assess the extent of decay, check for bone loss, or locate an abscess at the root tip.
- Palpation: Gently feeling the swollen area to assess firmness, tenderness, and identify potential areas of pus collection.
- Vitality Testing: Testing the affected tooth's response to cold or electric pulp tests can help determine if the pulp is alive, inflamed, or necrotic.
2. Acute Infection Management (First Priority)
- Antibiotics: If a significant infection is present, especially with facial swelling or systemic symptoms, antibiotics will be prescribed immediately. You'll typically start a course of antibiotics to reduce the spread of bacteria. It's crucial to take the full course as prescribed, even if you start feeling better.
- Drainage (Incision and Drainage - I&D): If there's a localized collection of pus (an abscess), the dentist may perform an I&D.
- Anesthesia: The area will be numbed with local anesthetic.
- Incision: A small incision is made in the most prominent part of the swelling, allowing the pus to drain. This might be on the gum or, in rare cases, externally on the skin if the infection has spread significantly.
- Drainage: The pus is carefully evacuated. Sometimes, a small rubber drain is placed to allow continuous drainage for a few days.
- Relief: This procedure often provides immediate relief from pressure and pain.
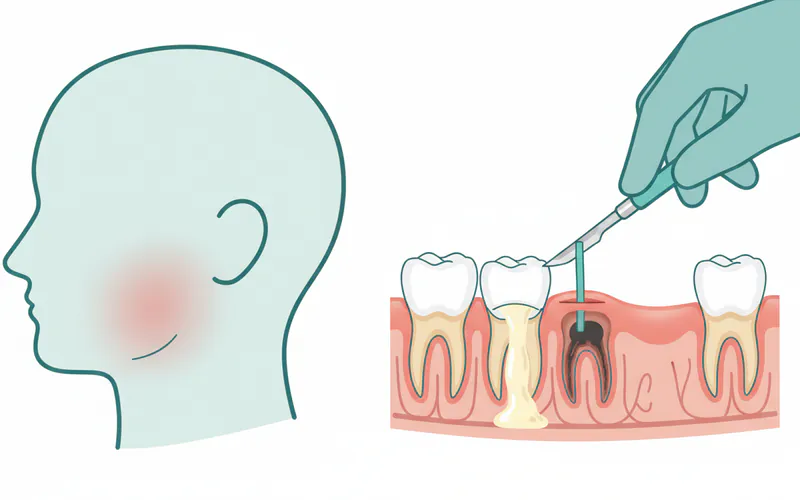
3. Definitive Treatment (Once Acute Infection is Controlled)
Once the acute infection and swelling have subsided (usually within a few days of antibiotics and/or drainage), the underlying cause must be addressed.
- Root Canal Therapy:
- Access: A small opening is made in the top of the tooth.
- Pulp Removal: The infected or necrotic pulp tissue is removed from the pulp chamber and root canals.
- Cleaning and Shaping: The canals are thoroughly cleaned, disinfected, and shaped using small files.
- Filling: The cleaned canals are filled with a biocompatible material (gutta-percha) to prevent re-infection.
- Restoration: The access opening is sealed with a filling, and often a crown is placed over the tooth for protection and strength.
- Tooth Extraction:
- Anesthesia: Local anesthetic is administered to numb the tooth and surrounding area.
- Removal: The dentist carefully loosens and removes the infected tooth.
- Post-Extraction Care: Instructions for wound care, pain management, and preventing dry socket are provided.
- Follow-up: Regardless of the definitive treatment, a follow-up appointment is typically scheduled to ensure healing, remove any drains, and assess the overall outcome.
Cost and Insurance
The financial aspect of treating face swelling from a tooth can vary significantly based on the severity of the infection, the specific procedures required, the geographic location, and whether you have dental insurance. Being prepared for these costs can ease the burden during a stressful time.
Average US Price Ranges (Without Insurance):
- Emergency Exam & X-rays: $75 - $250. This initial visit is crucial for diagnosis.
- Prescription Antibiotics: $10 - $60 (for a typical course of generic antibiotics).
- Incision and Drainage (I&D): $150 - $500. This procedure, often performed immediately, provides relief but doesn't solve the root cause.
- Simple Tooth Extraction: $150 - $400. For a visible tooth that can be removed with forceps.
- Surgical Tooth Extraction: $250 - $800+. For impacted teeth (like wisdom teeth) or those requiring bone removal.
- Root Canal Therapy:
- Front Tooth: $700 - $1,200
- Premolar: $800 - $1,500
- Molar: $1,000 - $2,000+ (Molars have more canals and are more complex).
- Dental Crown (post-root canal): $800 - $2,000+. This is often necessary to protect a root-canaled tooth from fracture.
- Hospitalization (for severe infections like Ludwig's Angina): Can range from several thousand to tens of thousands of dollars, depending on the length of stay, IV antibiotics, and any necessary surgical interventions. This is usually covered by medical insurance rather than dental insurance.
Dental Insurance Coverage Details:
Most dental insurance plans in the US categorize treatments based on complexity and necessity:
- Preventive Care (e.g., exams, X-rays): Often covered at 80-100%.
- Basic Procedures (e.g., fillings, simple extractions, I&D): Typically covered at 70-80%.
- Major Procedures (e.g., root canals, crowns, surgical extractions): Usually covered at 50-70%.
Key Terms to Understand:
- Deductible: The amount you must pay out-of-pocket before your insurance begins to cover costs.
- Co-pay: A fixed amount you pay for a covered service after your deductible has been met.
- Coinsurance: The percentage of costs you pay after your deductible is met (e.g., if insurance covers 80%, you pay 20%).
- Annual Maximum: The maximum amount your dental insurance plan will pay for covered services in a plan year. This is often $1,000 - $2,000. If your treatment exceeds this, you pay the rest out-of-pocket.
Example Scenario: If you need a root canal on a molar ($1,500) and a crown ($1,200), totaling $2,700:
- Assuming a $50 deductible, 50% coverage for major procedures, and a $1,500 annual maximum.
- You pay the $50 deductible.
- Remaining cost: $2,650.
- Insurance covers 50% of $2,650 = $1,325.
- Your out-of-pocket for these procedures would be $2,650 - $1,325 = $1,325.
- If your plan had a $1,500 annual maximum, the insurance would cover up to that amount within the year, but your portion would still be calculated based on the 50% coinsurance. In this case, you would hit your annual maximum and pay the remaining $1,325.
Cost Comparison Table for Acute Dental Infection Management
This table provides general cost estimates for the immediate management of a dental infection causing facial swelling. Definitive treatment (root canal, extraction with replacement) would be additional.
| Procedure | Average US Cost Range (without insurance) | Insurance Coverage (Typical) | Out-of-Pocket (with insurance, post-deductible) |
|---|---|---|---|
| Emergency Exam & X-rays | $75 - $250 | 80-100% | $0 - $50 |
| Antibiotics (Oral) | $10 - $60 | N/A (medical insurance often) | $10 - $60 |
| Incision and Drainage | $150 - $500 | 70-80% | $30 - $150 |
| Simple Extraction | $150 - $400 | 70-80% | $30 - $120 |
| Surgical Extraction | $250 - $800+ | 50-70% | $75 - $400+ |
| Root Canal (Molar) | $1,000 - $2,000+ | 50-70% | $300 - $1,000+ |
Pro Tip: Always call your dental insurance provider beforehand to understand your specific benefits, deductibles, co-pays, and annual maximums. Ask your dental office for an estimated cost breakdown and payment options.
Recovery and Aftercare
Proper recovery and aftercare are vital to ensure successful healing, prevent complications, and avoid recurrence after treatment for face swelling from a tooth.
Post-Procedure Care:
- Pain Management:
- Take prescribed pain medication (e.g., ibuprofen, acetaminophen, or stronger opioids if prescribed for severe pain) as directed.
- Apply a cold compress to the external cheek area for 15-20 minutes at a time, several times a day for the first 24-48 hours to help reduce swelling and discomfort.
- Antibiotics:
- Crucially, complete the entire course of antibiotics exactly as prescribed, even if your symptoms improve quickly. Stopping early can lead to a resurgence of infection or antibiotic resistance.
- Oral Hygiene:
- Maintain gentle oral hygiene. Brush your teeth carefully, avoiding the surgical site directly for the first 24 hours if you had an extraction or drainage.
- Rinse with warm salt water (1/2 teaspoon salt in 8 ounces warm water) 2-3 times a day, especially after meals. This helps to keep the area clean and promotes healing. Avoid vigorous rinsing, which can dislodge blood clots.
- Diet:
- Stick to soft, easy-to-chew foods for the first few days (e.g., yogurt, mashed potatoes, soups, scrambled eggs).
- Avoid extremely hot or cold foods and drinks if sensitivity persists.
- Avoid crunchy, hard, or sticky foods that could irritate the healing area or dislodge a clot/dressing.
- Activity:
- Avoid strenuous physical activity for at least 24-48 hours following a procedure, as this can increase bleeding and swelling.
- Rest with your head elevated to help reduce swelling.
- Smoking/Alcohol:
- Avoid smoking and alcohol, as both can significantly impair healing and increase the risk of complications like dry socket after extraction.
- Drains (if placed):
- If a rubber drain was placed during incision and drainage, follow your dentist's instructions for its care. It will usually be removed after a few days at a follow-up appointment.
What to Watch For (Signs of Complications):
- Worsening Pain or Swelling: If the pain or face swelling from a tooth increases after the initial 24-48 hours, or if new swelling appears.
- Persistent Fever: A fever that doesn't subside or worsens.
- Difficulty Swallowing or Breathing: These are emergency signs and require immediate medical attention.
- Pus Discharge: Continued pus drainage after the initial healing period.
- Excessive Bleeding: More than minor oozing after an extraction.
- Allergic Reaction: Hives, rash, difficulty breathing (call 911 immediately) from antibiotics or other medications.
- Dry Socket: Intense, throbbing pain in the extraction site 2-5 days after a tooth removal, sometimes accompanied by a foul odor.
Follow-up Appointments:
It's crucial to attend all scheduled follow-up appointments. Your dentist will monitor healing, remove any sutures or drains, and ensure the infection has completely resolved. They will also complete any restorative work (like placing a crown after a root canal).

Prevention
Preventing face swelling from a tooth boils down to meticulous oral hygiene and proactive dental care. Most instances of facial swelling stem from untreated or poorly managed dental issues that escalate into serious infections.
- Practice Excellent Oral Hygiene:
- Brush Twice Daily: Brush your teeth for at least two minutes, twice a day, using a fluoride toothpaste. Ensure you reach all surfaces of your teeth.
- Floss Daily: Floss at least once a day to remove plaque and food particles from between your teeth and under the gumline, areas your toothbrush can't reach. This is crucial for preventing gums swelling and periodontal disease.
- Use Mouthwash: An antimicrobial mouthwash can help reduce bacteria in your mouth, but it's not a substitute for brushing and flossing.
- Regular Dental Check-ups and Cleanings:
- Visit your dentist every six months, or as recommended, for professional clean-ups and examinations. These visits allow your dentist to identify and treat minor issues like cavities or early gum disease before they become severe.
- Early detection of small cavities can prevent them from progressing to deep infections that cause facial swelling.
- Prompt Treatment of Dental Problems:
- Do not ignore dental pain, sensitivity, or minor gums swelling. These are warning signs that require prompt professional attention. Delaying treatment for a small cavity or gum inflammation can lead to a severe infection and facial swelling.
- Address broken or chipped teeth, loose fillings, or failing crowns immediately, as these can create entry points for bacteria.
- Address Impacted Wisdom Teeth:
- If your wisdom teeth are impacted and causing recurrent infections (pericoronitis) or are at high risk of doing so, discuss extraction with your dentist or oral surgeon. This can prevent episodes of pain, swelling, and potential spread of infection to the jaw and face.
- Balanced Diet:
- Limit sugary foods and drinks, which feed bacteria and contribute to tooth decay.
- Eat a balanced diet rich in fruits, vegetables, and whole grains to support overall health and immune function.
- Protect Your Teeth:
- If you play contact sports, wear a custom-fitted mouthguard to protect your teeth from trauma that could lead to infection.
- If you grind or clench your teeth (bruxism), talk to your dentist about a nightguard to prevent tooth wear and fractures.
- Manage Underlying Health Conditions:
- If you have conditions like diabetes or a compromised immune system, work closely with your medical doctor and dentist to manage these conditions, as they can increase your susceptibility to dental infections.
By adhering to these preventive measures, you significantly reduce your risk of experiencing the discomfort, danger, and expense associated with face swelling from a tooth.
Risks and Complications
While treatable, face swelling from a tooth carries significant risks and can lead to severe, even life-threatening, complications if left untreated or improperly managed. Understanding these potential outcomes underscores the urgency of seeking professional dental care.
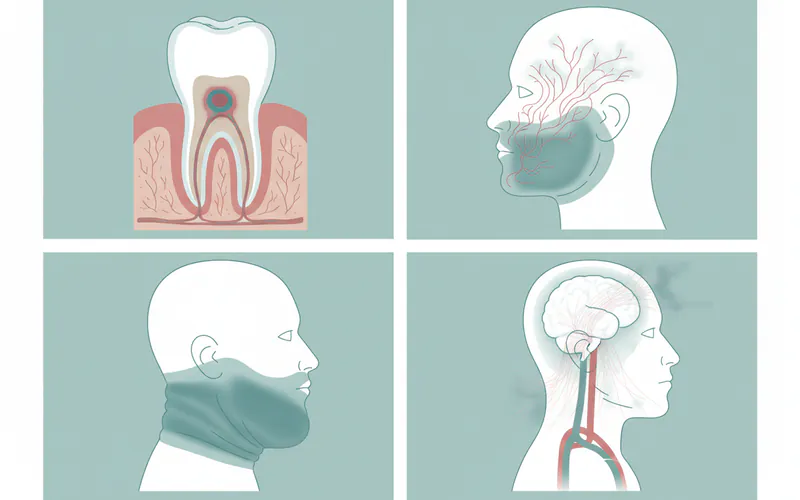
1. Spread of Infection:
This is the most critical risk. A localized dental infection can rapidly spread beyond the original site:
- Cellulitis: The infection can spread diffusely through the soft tissues of the face and neck, causing extensive redness, warmth, and tenderness. This requires aggressive antibiotic treatment.
- Ludwig's Angina: As discussed, this is a rapidly spreading cellulitis of the floor of the mouth and neck, which can cause significant submandibular swelling, push the tongue backward, and obstruct the airway, leading to difficulty breathing and potentially death. This is a medical emergency.
- Periorbital Cellulitis: Infection can spread to the tissues around the eye, leading to swelling, pain, and potentially vision problems.
- Cavernous Sinus Thrombosis: A rare but deadly complication where the infection spreads to the cavernous sinus, a large vein located behind the eyes at the base of the brain. This can lead to blood clots, vision loss, stroke, and death.
- Osteomyelitis: The infection can spread into the jawbone itself, causing inflammation and destruction of bone tissue. This is a chronic condition that can be challenging to treat.
- Sepsis: If the bacteria enter the bloodstream, it can lead to sepsis, a life-threatening whole-body inflammatory response to infection that can result in organ failure and death.
- Brain Abscess: In very rare and severe cases, the infection can travel to the brain, forming a pus pocket within brain tissue, leading to severe neurological symptoms and requiring neurosurgery.
2. Airway Obstruction:
Especially with infections in the lower jaw and floor of the mouth (like Ludwig's Angina), the swelling can rapidly compromise the airway. This is a life-threatening emergency that requires immediate medical intervention to secure breathing, potentially through intubation or tracheostomy.
3. Chronic Pain and Discomfort:
Even if the acute swelling subsides, the underlying infection will persist without definitive dental treatment, leading to chronic pain, intermittent swelling, and ongoing discomfort.
4. Tooth Loss:
If the infection severely damages the tooth structure or surrounding bone, the affected tooth may become unsalvageable and require extraction.
5. Cosmetic and Functional Impairment:
Severe swelling can cause temporary facial disfigurement. In cases requiring extensive surgical drainage, there might be scarring. Long-term, untreated infections can lead to significant bone loss, affecting facial structure and making future dental restorations more complex.
6. Antibiotic Resistance:
Repeated or improper use of antibiotics (e.g., not completing the full course) can contribute to the development of antibiotic-resistant bacteria, making future infections harder to treat.
Children / Pediatric Considerations
Facial swelling from a tooth in children presents unique concerns and often requires even more immediate attention due to several factors specific to their developing bodies.
- Faster Progression: Children's immune systems and anatomical structures are different from adults. Infections can spread more rapidly and aggressively in smaller facial spaces. What might be a slowly progressing abscess in an adult could quickly become widespread cellulitis in a child.
- Primary (Baby) Teeth Involvement: Dental decay in primary teeth is a common cause. Parents sometimes mistakenly believe that infections in baby teeth are less serious because the teeth will eventually fall out. However, an infection in a primary tooth can lead to a serious abscess and facial swelling, just like in a permanent tooth.
- Impact on Permanent Teeth: An infection in a primary tooth can damage the developing permanent tooth bud underneath, leading to enamel defects or malformation of the adult tooth.
- Difficulty in Communication: Young children may not be able to articulate their pain or specific symptoms clearly. Parents must be vigilant for signs like irritability, refusal to eat, disrupted sleep, or changes in behavior.
- Early Recognition: Parents should look for:
- Visible facial swelling, especially around the cheek or jaw.
- Gums swelling around a specific tooth.
- Fever (even low grade).
- Tenderness to touch on the face or jaw.
- Reluctance to chew on one side.
- A small "pimple" on the gum near a tooth.
- Treatment Approach:
- Antibiotics: Crucial for controlling the infection. Pediatric dentists will carefully choose appropriate antibiotics and dosages.
- Drainage: If an abscess is present, drainage may be necessary.
- Pulp Therapy (Pulpotomy/Pulpectomy): For infected primary teeth, the infected pulp can often be partially or fully removed to save the tooth, similar to a root canal in an adult. This is important for maintaining space for permanent teeth.
- Extraction: If the primary tooth is too severely damaged or infected to save, it may need to be extracted.
- Prevention is Paramount:
- Begin dental check-ups by age one or with the eruption of the first tooth.
- Ensure proper brushing and flossing habits from an early age.
- Limit sugary snacks and drinks.
- Address even small cavities promptly.
Pro Tip for Parents: If your child has facial swelling, especially with fever or difficulty eating, contact your pediatric dentist immediately. If the swelling is rapid or affects breathing, head to the nearest emergency room.
Cost Breakdown
A detailed cost breakdown for managing face swelling from a tooth illustrates the financial implications, which can vary widely. This section elaborates on average US costs, insurance impacts, and strategies for managing expenses.
Average US Costs (Without Insurance):
Let's refine and expand on costs, noting that these are estimates and can fluctuate based on the dentist's fees, specialist involvement (e.g., endodontist, oral surgeon), and geographic location (urban vs. rural).
- Initial Emergency Visit & Diagnosis:
- Emergency Exam: $75 - $150
- X-rays (periapical, panoramic): $30 - $100 per film, or $100 - $250 for a full mouth series/panoramic
- Consultation: May be included with exam or separate $50 - $100
- Total for initial visit: $100 - $400
- Acute Infection Management:
- Antibiotics: $10 - $60 for generic prescriptions (e.g., Amoxicillin, Clindamycin). More specialized antibiotics can be higher.
- Incision and Drainage (I&D): $150 - $500. This often includes local anesthesia and follow-up.
- Total for acute management (excluding initial visit): $160 - $560
- Definitive Treatment (Once Infection is Controlled):
- Simple Tooth Extraction: $150 - $400.
- Surgical Extraction (e.g., impacted tooth, bone removal needed): $250 - $800+. May require sedation, adding $200 - $800+.
- Root Canal Therapy:
- Anterior (front) tooth: $700 - $1,200
- Premolar: $800 - $1,500
- Molar: $1,000 - $2,000+
- Post-Root Canal Crown: $800 - $2,000+. (Often necessary for long-term protection of a root-canaled tooth).
- Total for definitive treatment (can be just extraction, or RCT + crown): $150 - $4,000+
- Hospitalization (Severe Cases - Ludwig's Angina, Extensive Cellulitis):
- ER Visit: $500 - $2,000+
- Hospital Stay (per day): $1,000 - $5,000+ (includes IV antibiotics, monitoring, potential surgery).
- Intubation/Tracheostomy (if needed): $5,000 - $20,000+
- Total: Tens of thousands of dollars
With vs. Without Insurance:
- Without Insurance: You are responsible for 100% of all costs. This is why many people delay care, often leading to more severe and expensive emergencies.
- With Dental Insurance:
- Coverage varies, but typically ranges from 70-100% for preventive care, 70-80% for basic procedures (like I&D, simple extractions, fillings), and 50-70% for major procedures (like root canals, crowns, surgical extractions).
- You will still have co-pays, deductibles (often $50-$100 annually), and coinsurance to pay.
- Most dental plans have an annual maximum, typically $1,000 - $2,000. If your treatment costs exceed this, you pay 100% of the remaining balance. This maximum is often easily hit with a root canal and crown.
Payment Plans and Financing Options:
- In-Office Payment Plans: Many dental offices offer interest-free payment plans for a few months for established patients.
- Dental Credit Cards (e.g., CareCredit, LendingClub): These are specialized healthcare credit cards that offer promotional financing options, often with 0% interest for a set period (e.g., 6-24 months) if paid in full. Be cautious of deferred interest rates if you don't pay it off in time.
- Personal Loans: Banks or credit unions offer personal loans, but these come with interest rates.
- Community Dental Clinics/Dental Schools: These often offer services at a reduced cost. Wait times can be longer, but they are a viable option for those with limited financial resources.
- Flexible Spending Accounts (FSA) and Health Savings Accounts (HSA): If you have access to these through your employer, you can use pre-tax dollars to pay for dental expenses, which can offer significant savings.
Cost-Saving Tips:
- Don't Delay: The single most effective cost-saving tip is to seek treatment for dental problems before they become emergencies. A small filling (under $300) is far cheaper than a root canal ($1,000+) or an emergency room visit for facial swelling.
- Get Multiple Quotes: For non-emergency, definitive treatments (like a root canal or crown), you can ask different dental offices for quotes.
- Inquire About Cash Discounts: Some practices offer a discount for patients paying in full with cash or without insurance.
- Dental Discount Plans: These are not insurance but offer a percentage discount on services from participating dentists for an annual fee.
Frequently Asked Questions
How long does facial swelling from a tooth last?
The duration of facial swelling from a tooth depends on the severity of the infection and how quickly treatment is initiated. With prompt antibiotic treatment and drainage, the swelling typically begins to subside within 24-48 hours. Complete resolution can take anywhere from a few days to a week or more, especially if the infection was widespread. Without treatment, the swelling can persist indefinitely and worsen, leading to serious complications.
Can a tooth infection spread to the brain?
Yes, though rare, a severe tooth infection can spread to the brain. The bacteria can travel from the jawbone through the facial veins, eventually reaching the brain and forming a brain abscess. This is a life-threatening complication, often preceded by severe facial cellulitis or cavernous sinus thrombosis, and requires immediate medical attention, including IV antibiotics and potentially neurosurgery.
What are the signs of a tooth infection spreading?
Signs of a spreading tooth infection include rapidly increasing facial swelling, submandibular swelling (swelling under the jaw or in the neck), fever and chills, difficulty swallowing (dysphagia), difficulty opening your mouth (trismus), and most critically, difficulty breathing (dyspnea). If you experience any of these symptoms, seek emergency medical care immediately.
Can antibiotics alone cure a dental abscess?
No, antibiotics alone cannot cure a dental abscess. While they can help control the acute bacterial infection and reduce swelling, they do not remove the source of the infection, which is the dead pulp tissue inside the tooth or the trapped bacteria in a periodontal pocket. Definitive treatment, such as root canal therapy or tooth extraction, is essential to eliminate the source and prevent recurrence.
Is facial swelling from a tooth a dental emergency?
Absolutely, yes. Any facial swelling originating from a tooth should be considered a dental emergency. It indicates that the infection has spread beyond the tooth itself and into the surrounding soft tissues, carrying the risk of further spread to critical areas like the airway, brain, or bloodstream. Immediate professional evaluation is crucial.
What helps with facial swelling from a tooth?
While waiting for a dental appointment, you can apply a cold compress to the outside of your cheek for 15-20 minutes at a time to help reduce swelling and discomfort. Over-the-counter pain relievers like ibuprofen can help manage pain and inflammation. However, these are temporary measures; they do not treat the underlying infection, and prompt dental intervention is required.
How much does it cost to treat facial swelling from a tooth?
The cost varies significantly. An emergency exam and antibiotics might be $100-$400. If incision and drainage are performed, add $150-$500. Definitive treatment like a root canal costs $700-$2,000+ (plus a crown, $800-$2,000+), or an extraction costs $150-$800+. Without insurance, the total cost for a full resolution can range from hundreds to several thousands of dollars, and tens of thousands for hospitalization.
Can I wait to see a dentist for face swelling?
No, waiting to see a dentist for face swelling from a tooth is strongly discouraged and potentially dangerous. Dental infections can spread rapidly. Delaying treatment significantly increases the risk of severe complications, including airway obstruction, widespread cellulitis, and even life-threatening conditions. Seek immediate professional dental or medical care.
What is submandibular swelling related to teeth?
Submandibular swelling refers to swelling under the jawbone. When related to teeth, it typically indicates that a dental infection (often from a lower molar) has spread into the fascial spaces of the neck, or that the lymph nodes in the neck have become enlarged and tender as they fight the infection. It's a serious sign that the infection is no longer localized and requires urgent attention.
Are there home remedies for face swelling from a tooth?
While some home remedies like cold compresses and warm salt water rinses can provide temporary symptomatic relief, they are not a cure for the underlying bacterial infection causing facial swelling. Relying solely on home remedies delays essential professional treatment, allowing the infection to worsen and increase the risk of severe, life-threatening complications. Always see a dentist.
When to See a Dentist
Given the potential severity of face swelling from a tooth, knowing when to seek professional help is critical. This is almost always a dental emergency.
Immediate Emergency Attention (Go to the Dentist or ER NOW if you experience any of these):
- Any visible facial swelling: This is the primary red flag. Whether it's a small puffiness or a large bulge on your cheek, jaw, or under your eye, it indicates a spreading infection.
- Rapidly worsening swelling: If the swelling is increasing quickly over a few hours.
- Difficulty breathing: This is a life-threatening symptom. Swelling in the neck and floor of the mouth can compromise your airway. Call 911 or go to the nearest emergency room immediately.
- Difficulty swallowing (dysphagia) or speaking: These indicate that the infection is affecting your throat and potentially your airway.
- High fever and chills: Systemic signs of a serious infection.
- Severe, unmanageable pain: Pain that doesn't respond to over-the-counter medication.
- Submandibular swelling: Swelling under the jaw or in the neck, especially if firm, red, and tender. This signals a deeper, more dangerous infection.
- Feeling generally unwell (malaise) with swelling: If you feel weak, nauseous, or have body aches in addition to facial swelling.
- Swelling extending towards your eye: This indicates the infection is spreading aggressively.
Scheduled Dental Appointment (If only these symptoms are present, but still urgent):
While the above situations demand immediate emergency care, the following also require prompt attention and should not be ignored:
- Localized gums swelling without facial involvement: If only your gums are swollen around a tooth, indicating a possible abscess or gum infection that hasn't spread yet.
- Persistent tooth pain or sensitivity without swelling: A sign of a developing cavity or pulp infection that needs to be addressed before it leads to swelling.
- A "pimple" or draining fistula on your gums: This indicates pus is draining, which can relieve pressure, but the underlying infection is still present and needs definitive treatment.
Pro Tip: When in doubt, always err on the side of caution. Call your dentist immediately. If it's after hours and you have any of the "Immediate Emergency Attention" symptoms, head to an urgent care center or emergency room without delay. Dental infections are not to be underestimated.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
How to Relieve Gum Swelling
When your gums are swollen, it can be an alarming and uncomfortable experience, often signaling an underlying issue that requires attention. Statistics from the Centers for Disease Control and Prevention (CDC) reveal that **nearly half of adults aged 30 or older in the United States have some form o
February 23, 2026
Teeth Swelling: Complete Guide
When you experience teeth swelling, it's more than just a minor discomfort; it's a clear signal from your body that something is amiss within your oral cavity, often indicating an underlying infection or inflammation that requires prompt attention. A recent survey revealed that **over 25% of adu
February 23, 2026
Submandibular Salivary Gland Swelling: Complete Guide
When you notice a peculiar lump or uncomfortable fullness beneath your jaw, it can be an alarming experience. This sensation, often accompanied by pain and difficulty swallowing, could indicate submandibular salivary gland swelling. Affecting an estimated 1 in 10,000 adults annually, conditi
February 23, 2026
What Helps With Gum Swelling
Gum swelling, medically known as gingival swelling or gingivitis, is a common yet often underestimated dental issue affecting millions of Americans. Have you ever woken up with sore, puffy gums that bleed easily when you brush? You're not alone. Research indicates that nearly **half of all a
February 23, 2026